Abstract.
|
|
|
- Gregory Bruce Ramsey
- 5 years ago
- Views:
Transcription
1 The efficacy of pharmaceutical combination of glucose, insulin, potassium, and magnesium along with thrombolytic therapy on the mortality of patients with acute myocardial infarction Mohammad Garakyaraghi (1), Mojgan Kianjoo (2), Mojgan Mortazavi (3), Nizal Sarrafzadegan (4), Hassan Shemirani (5), Mansour Shahparian (6) Abstract BACKGROUND: Despite conventional treatment methods of acute myocardial infarction, its complications and mortality rates are still very high. Finding new cost-effective treatments like regulation of ischemic muscle metabolism at the time of thrombolytic therapy can meet this requirement to some extent. This study investigated the efficacy of the pharmaceutical combination of glucose, insulin, potassium (GIK) and magnesium along with thrombolytic therapy. METHODS: In a double-blind, controlled clinical trial, 200 patients with acute myocardial infarction who had the indication for thrombolytic treatment were selected and divided to 6 groups of almost 30 people. A specific treatment protocol was designed for each group. The patients in the first 5 groups were compared with the ones in the sixth group as the control group in terms of frequency of complications and in-hospital mortality and also mortality during 3 and 6 months after the treatment. RESULTS: Mean age of the patients was ± 2.6 years. Males constituted 77% of the study population. Heart failure, in-hospital arrhythmia and ejection fraction (EF) at discharge showed favorable results in the five groups which received metabolic regulations as compared to the control group. In-hospital mortality of no groups was different from that of the control group (P > 0.05). Three months after the treatment, mortality of the group that received GIK and magnesium was lower than that of the control group (P < 0.05). After 6 months, none of the patients who received high-dose GIK and magnesium along with thrombolytic therapy died while the mortality rate of the control group was 44.4% (P < 0.05). CONCLUSION: The infusion of GIK and magnesium solution along with thrombolytic therapy can lead to a decrease in the long-term mortality and complications in patients with acute myocardial infarction. Keywords: Acute Myocardial Infarction, Glucose, Insulin, Potassium, Magnesium, Thrombolytic Therapy, Cardiovascular Diseases, Clinical Trial. ARYA Atherosclerosis Journal 2012, 7(Suppl): S36-S41 Date of submission: 5 Jan 2012, Date of acceptance: 26 Feb 2012 Introduction Despite conventional treatment methods for acute myocardial infarction, its complications and mortality rates are still very high. 1 Therefore, it is essential to find new and cost-effective treatments in this regard. Besides conventional treatments (like thrombolytic therapy), two metabolic treatments have been introduced for treating the patients with acute myocardial infarction. These two methods include the infusion of a solution of glucose, insulin, potassium (GIK), and magnesium (Mg). Recently, the perfusion measurement of myocardial tissue has shown that at the beginning of acute myocardial infarction, perfusion of myocardial tissue is at a very low level but it is not zero. 2 Since the infarction area has the minimum sufficient flow for the release of substrate, lactic acid wash would provide a basis for the intervention in the infarction flow using GIK method. The studies conducted by insulin and glucose with low-flow ischemia have shown that at the time 1- Associate Professor, Cardiac Rehabilitation Research Center, Isfahan Cardiovascular Research Institute, Isfahan University of Medical Sciences, Isfahan, Iran 2- Cardiac Rehabilitation Research Center, Isfahan Cardiovascular Research Institute, Isfahan University of Medical Sciences, Isfahan, Iran 3- Assistant Professor, Isfahan Kidney Diseases Research Center, Department of Internal Medicine, Isfahan University of Medical Sciences, Isfahan, Iran. 4- Professor, Isfahan Cardiovascular Research Center, Isfahan Cardiovascular Research Institute, Isfahan University of Medical Sciences, Isfahan, Iran. 5- Associate Professor, Hypertension Research Center, Isfahan Cardiovascular Research Institute, Isfahan University of Medical Sciences, Isfahan, Iran. 6- Assistant Professor, Department of Internal Medicine, School of Medicine, Isfahan University of Medical Sciences, Isfahan, Iran. Correspondence To: Nizal Sarrafzadegan, nsarrafzadegan@gmail.com S36
2 M. Garakyaraghi, M. Kianjoo, M. Mortazavi, N. Sarrafzadegan, H. Shemirani, M. Shahparian of acute myocardial infarction, the increase of glycosylated substrate, which is accessible by the tissue, has useful effects. 3 High glucose substrate has been found to cause an increase in resistance of myocytes to toxic effects of cellular calcium which is produced during hypoxia. 4 The results of a review study in 1997 demonstrated that GIK prescription led to 28-42% reduction in the in-hospital mortality of myocardial infarction patients. 5 However, thrombolytic therapy was not conventional at that time and it is not evident whether using GIK in treating myocardial infarction was essential at the presence of current thrombolytic treatments or not. After this study, only one other study in 1998 in South America evaluated the value of using high-dose GIK along with thrombolytic therapy and angioplasty in treating acute myocardial infarction. 6 The indication for using Mg in treating myocardial infarction is the overall reduction of Mg in the body. 7 The reasons for this reduction include receiving insufficient Mg, taking diuretics, old age, and trapping free Mg in fat cells as a result of released fatty acids by fat cells at the beginning of infarction. 7,8 Various researches in 1996 have suggested Mg infusion immediately after myocardial infarction and adding Mg salts to the diet of the patients for 2 years after myocardial infarction to possibly decrease the mortality and complications of the condition. 9 Nevertheless, the results of some other studies have indicated ineffectiveness of Mg on decreasing of the mortality and complications of myocardial infarction. 10 In the present study, the effects of the combined usage of GIK and Mg with thrombolytic therapy was compared with thrombolytic therapy alone. Materials and Methods This study was a double-blind clinical trial. Participants were patients who referred to the emergency department and coronary care unit (CCU) of Noor, Feiz, and Alzahra Hospitals, affiliated to Isfahan University of Medical Sciences (Isfahan, Iran), between late January 2000 and late July All subjects suffered from acute myocardial infarction and had the indications for thrombolytic treatment. A total number of 240 patients were enrolled in the study. They were randomly divided into 6 groups using sealed envelopes in which the number of group was randomly placed. Moreover, each envelop was numbered between 1 and 240 to correspond the 240 patients. After obtaining informed consent forms signed by patients, two residents of internal medicine who participated in this study opened the envelopes related to each patient and placed the subjects in one of the six treatment groups based on the number inside the envelope. The six treatment groups included: 1) low-dose GIK + thrombolytic; 2) high-dose GIK + thrombolytic; 3) low-dose GIK + Mg + thrombolytic; 4) high-dose GIK + Mg + thrombolytic; 5) Mg + thrombolytic; and 6) thrombolytic alone (control group). Low-dose GIK contained 1 liter of 10% glucose solution plus 20 units of insulin crystal (human or nonhuman) plus 40 MEq potassium, which were infused at the rate of 1 ml per kg of body weight per hour. High-dose GIK contained 1 lit of 25% glucose solution plus 50 units of insulin crystal (human or non-human) plus 80 milliequivalents (meq) of potassium which were infused at the rate of 1.5 ml per kg of body weight per hour. Mg solution contained 8 grams of magnesium sulfate in 1 liter of 5% serum dextrose which was infused for 24 hours. After determining the treatment group of the patients, all characteristics, symptoms, and examination results of the patient were recorded in a questionnaire by internal medicine residents. The patients were then treated according to the protocol designed for their own groups either simultaneous with or shortly after the beginning of thrombolytic therapy. Thrombolytic therapy was performed using 1.5 million units of intravenous streptokinase. GIK, Mg and streptokinase were infused via separate veins. To maintain double-blindness, the placebo (5% glucose serum) was used. Therefore, each patient received three solutions. In other words, only one solution of 5% glucose serum was used in the first, second, and fifth treatment groups. On the other hand, the sixth treatment group received glucose serum through 2 veins while the third and fourth groups did not receive any 5% glucose serum. After infusing the solutions, the patients were examined by two internal medicine residents participating in the study for mortality and in-hospital complications including a second myocardial infarction, congestive heart failure, secondary arrhythmia, in-hospital death, cerebrovascular complications, and major bleeding. Echocardiography was also performed by a heart specialist before the patients were discharged and the results (ejection fraction) were recorded in the questionnaire. The patients were followed for mortality and percutaneous transluminal coronary angioplasty (PTCA) requirement. Echocardiography was repeated at 3 and 6 months after the discharge. All echocardiograms were performed by a specific specialist at Isfahan Cardiovascular Research Center (Isfahan, Iran). Each patient was provided with a special follow-up card on which the dates of the 3- and 6-month reference were written. If the patients did S37
3 The efficacy of pharmaceutical combination of glucose, insulin, potassium magnesium not show up on the determined days, the information was achieved by phone calls or referring to their address. Considering the exclusion criteria (kidney failure, hyperkalemia, bradycardia, and hypotension) and unavailability during the follow-up, 40 patients were excluded from the study. Consequently, the data of 200 patients was analyzed. To analyze the data, Fisher's exact, chi-square, Dunnett's, Kruskal-Wallis, Dunn's, and Mann-Whitney tests were used. The minimum error of less than 0.05 was considered for rejecting the null hypothesis. Results The mean age of the patients (77% males and 23% females) was 58.7 ± 2.6 years. The characteristics of the patients in terms of risk factors and conducted clinical examinations in each group are demonstrated in table 1. The results obtained from 6 types of mentioned treatments were compared with one another in three stages. No significant difference was observed between the 6 treatment groups with regard to mortality rate during their hospital stay. The lowest mortality rate (none out of 32 patients) was in the fourth treatment group (high-dose GIK + Mg + thrombolytic). The highest mortality rate (8 from 36 patients) was observed in the sixth treatment group (only thrombolytic therapy) (Table 2). Minimum and maximum numbers of patients with heart failure were detected in the fourth treatment group (with 2 cases) and in the sixth treatment group (with 20 cases), respectively. Using Dunnett's test to compare groups 1 to 5 with group 6 (control group), it was found that heart failure rate in the control group was higher than that in treatment groups 1 (low-dose GIK + thrombolytic), 2 (high-dose GIK + thrombolytic), and 4 (high-dose GIK + Mg + thrombolytic) (P < 0.05). However, no significant difference was observed between the control group and treatment groups 3 (low-dose GIK + Mg + thrombolytic) and 5 (Mg + thrombolytic) (P > 0.05). Moreover, no difference was found between treatment groups 1 and 2 (Table 2). Table 1. Frequency distribution of risk factors, physical findings, and demographic characteristics among patients who received low-dose glucose, insulin, and potassium (GIK), high-dose GIK, low-dose GIK and magnesium, high-dose GIK and magnesium, magnesium, and placebo plus thrombolytic therapy (groups 1-6, respectively) Variables Treatment groups Total number Age (year) ± ± ± ± ± ± 2.90 Male gender Diabetes Mellitus Smokers Hyperlipidemia Obesity Hypertension Family history of cardiovascular diseases (Yes) Myocardial Infarction S S Rhonchus JVP Edema Hepatomegaly Values are expressed as mean ± SD or frequency. Table 2. Relative frequency of in-hospital complications among patients who received low-dose glucose, insulin, and potassium (GIK), high-dose GIK, low-dose GIK and magnesium, high-dose GIK and magnesium, magnesium, and placebo plus thrombolytic therapy (groups 1-6, respectively) Treatment group Total number Heart failure* Arrhythmia Repeated myocardial infarction Stroke Death Major bleeding *Heart failure based on clip criterion (higher than 2); PTCA: Percutaneous transluminal coronary angioplasty PTCA S38
4 M. Garakyaraghi, M. Kianjoo, M. Mortazavi, N. Sarrafzadegan, H. Shemirani, M. Shahparian The maximum and minimum frequencies of arrhythmia were observed in the control group (14 cases from 32 patients) and of the fourth group (no cases), respectively (Table 2). While the frequency of arrhythmia decreased in the fourth group, it did not differ significantly between other groups and the control group. No differences were observed between the treatment groups regarding the frequencies of repeated myocardial infarction, stroke, in-hospital major bleeding, and PTCA requirement during the hospital-stay (P > 0.05). Left ventricular ejection fraction was different in the six treatment groups (Table 3). The maximum (49%) and minimum (37%) mean values of ejection fraction belonged to groups 2 and 4 and the control group, respectively. A significant difference was seen between treatment groups 2 and 4 and the control group in terms of left ventricular ejection fraction (Table 2). Mortality rate after discharge until the 3-month follow-up was not different between the 6 groups (Table 4). The maximum and minimum mortality rates were seen in the control group (27.8%) and group 4 (no cases), respectively. Only mortality rate of group 4 was different from that of the control group (P < 0.05). The need for PTCA from admission until 3 months after discharge was not different between the 6 groups. The minimum and maximum rates of needed PTCA were observed in treatment groups 1 (35.7%) and 5 (64.3%), respectively. At the 3-month follow-up, left ventricular ejection fraction was different between the 6 treatment groups (Table 3). The maximum and minimum mean values were calculated in treatment groups 2 (50%) and 4 (51%) and in the control group (37.9%), respectively. In all groups except group 3, left ventricular ejection fraction was different from that of the control group (P < 0.05). Mortality rate during 3 to 6 months after discharge was not different between the 6 treatment groups. The highest and lowest mortality rates from admission until the 6-month follow-up were found in the control group (16 cases) and group 4 (zero cases). The mortality rate in groups 2 and 4 was significantly lower than the control group (P < 0.05). With regard to the need for PTCA from admission until discharge, there was no difference between groups 1 to 5 and the control group (P > 0.05). The maximum and minimum need for PTCA were in the treatment group 5 (24 cases from 28 people) and in group 4 (8 cases from 26 people), respectively (Table 4). Table 3. Left ventricular ejection fraction before discharge, and 3 and 6 months after the treatment in patients who received low-dose glucose, insulin, and potassium (GIK), high-dose GIK, low-dose GIK and magnesium, high-dose GIK and magnesium, magnesium, and placebo plus thrombolytic therapy (groups 1-6, respectively) Treatment Before discharge 3 months after discharge 6 months after discharge group 1 47 ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± 2.58 Table 4. Relative frequency of mortality and percutaneous transluminal coronary angioplasty (PTCA) requirement 3 and 6 months after discharge in patients who received low-dose glucose, insulin, and potassium (GIK), high-dose GIK, low-dose GIK and magnesium, high-dose GIK and magnesium, magnesium, and placebo plus thrombolytic therapy (groups 1-6, respectively) 3 months after discharge 3 to 6 months after discharge Treatment Total PTCA PTCA Death Number Death group number requirement requirement Number S39
5 The efficacy of pharmaceutical combination of glucose, insulin, potassium magnesium The maximum and minimum left ventricular ejection fraction values after 6 months of follow-up were observed in the treatment group 4 (53.5%) and control group (39.4%), respectively. Left ventricular ejection fraction was higher in group 4 compared to the control group (P < 0.05). Discussion The results of this study revealed that the in-hospital complications of secondary arrhythmia and severe heart failure decreased in the groups that received metabolic intervention in addition to thrombolytic therapy. Furthermore, ventricular function at the time of discharge showed considerable improvement as compared to the control group. Long-term mortality of the patients with acute myocardial infarction also significantly decreased in these patients as compared with the group that only received thrombolytic therapy. Moreover, the ventricular function of the people in the mentioned groups increased as compared to the control group. The fourth treatment group which received high-dose GIK and Mg demonstrated favorable results in general while in some cases, other groups did not show any differences with the control group. Although no significant difference was found among the groups that received high and low doses of GIK, it is difficult to reach a final conclusion and more precise studies on larger sample sizes are required. In a similar study entitled ECLA in Latin America, two groups received high and low doses of GIK without Mg and were compared with a control group that only received thrombolytic therapy. The results showed that high-dose GIK was more effective for decreasing long-term mortality after treatment as compared with the low-dose GIK. In addition, in comparison with the control group, high and low doses of GIK significantly decreased both mortality and in-hospital complications and also the mortality of the patients one year after the treatment. 6 Another similar study entitled DIGAMI demonstrated reduced mortality in patients who received insulin and glucose at the time of infarction and also received long-term insulin in addition to thrombolytic treatment. 11 It is noteworthy that the above-mentioned studies were conducted while using thrombolytic as a treatment for acute myocardial infarction. Thus far, no studies have been undertaken based on simultaneous application of GIK and Mg. However, the LIMIT-2 study reported a significant decrease in in-hospital mortality during 4.5 years after thrombolytic therapy accompanied by Mg compared to thrombolytic therapy alone. Moreover, in a study in India, patients were compared in 4 groups. Thrombolytic therapy was combined with Mg in one group and with potassium in another. Considerable reductions in mortality, cardiovascular events, and ventricular ectopy were detected in the mentioned groups compared to the placebo group. 12 In another study, the effects of intravenous Mg in acute myocardial infarction were investigated randomly and in a double-blind way. Since no difference was observed between the group that received Mg and the control group in terms of mortality and conduction disorders, it was concluded that the study was not comprehensive enough. 10 Considering the findings of this study, metabolic intervention is recommended to be performed in combination with other conventional treatments of acute myocardial infarction, especially thrombolytic therapy. In addition, to obtain stronger results about the required dose of GIK, comparisons should be made between groups receiving high and low doses of GIK + Mg and a group receiving Mg along with thrombolytic therapy. Acknowledgements The authors would like to acknowledge the cooperation of Dr. Peyman Adibi who provided invaluable recommendations at all stages of this research and Dr. Shahram Oveis Qaran who analyzed the data and provided precious recommendations. We also thank all internal medicine and cardiology residents who helped us in collecting and guiding the participants and Dr. Sadeghi who followed the patients up and performed echocardiography. Moreover, the cooperation of all the respected nursing staff in emergency and CCU departments of Noor and Feiz Medical Centers should be mentioned. We acknowledge the cooperation of Ms. Tafazzoli in the Cardiovascular Research Center for collecting and following up the patients. The Persian version of this article has been previously published in Iranian Journal of Medical Education: 2010 No: 5; Conflict of Interests Authors have no conflict of interests. References 1. Burton E, Sobel M. Diffinition and historical consideration of acute myocardial infarction. In: Goldman L, Bennett JC, Editors. Pocket Companion to Cecil Textbook of Medicine. Philadelphia: S40
6 M. Garakyaraghi, M. Kianjoo, M. Mortazavi, N. Sarrafzadegan, H. Shemirani, M. Shahparian Saunders; Milavetz JJ, Giebel DW, Christian TF, Schwartz RS, Holmes DR, Jr., Gibbons RJ. Time to therapy and salvage in myocardial infarction. J Am Coll Cardiol 1998; 31(6): Eberli FR, Weinberg EO, Grice WN, Horowitz GL, Apstein CS. Protective effect of increased glycolytic substrate against systolic and diastolic dysfunction and increased coronary resistance from prolonged global underperfusion and reperfusion in isolated rabbit hearts perfused with erythrocyte suspensions. Circ Res 1991; 68(2): Kondo RP, Apstein CS, Eberli FR, Tillotson DL, Suter TM. Increased calcium loading and inotropy without greater cell death in hypoxic rat cardiomyocytes. Am J Physiol 1998; 275(6 Pt 2): H2272-H Fath-Ordoubadi F, Beatt KJ. Glucose-insulinpotassium therapy for treatment of acute myocardial infarction: an overview of randomized placebocontrolled trials. Circulation 1997; 96(4): Díaz R, Paolasso EA, Piegas LS, Tajer CD, Moreno MG, Corvalán R, et al. Metabolic Modulation of Acute Myocardial Infarction The ECLA Glucose- Insulin-Potassium Pilot Trial. Circulation 1998; 98: Arsenian MA. Magnesium and cardiovascular disease. Prog Cardiovasc Dis 1993; 35(4): Antman E. Randomized trials of magnesium in acute myocardial infarction: big numbers do not tell the whole story. AMJ cardiol 1995; 75: Singh RB, Singh NK, Niaz MA, Sharma JP. Effect of treatment with magnesium and potassium on mortality and reinfarction rate of patients with suspected acute myocardial infarction. Int J Clin Pharmacol Ther 1996; 34(5): Urek R, Halle J, Frank B, Goles T, Tomicic D, Mirat J, et al. Intravenous magnesium in acute myocardial infarct. Lijec Vjesn 1996; 118(11-12): Malmberg K, Ryden L, Hamsten A, Herlitz J, Waldenstrom A, Wedel H. Effects of insulin treatment on cause-specific one-year mortality and morbidity in diabetic patients with acute myocardial infarction. DIGAMI Study Group. Diabetes Insulin- Glucose in Acute Myocardial Infarction. Eur Heart J 1996; 17(9): Woods KL, Fletcher S, Roffe C, Haider Y. Intravenous magnesium sulphate in suspected acute myocardial infarction: results of the second Leicester Intravenous Magnesium Intervention Trial (LIMIT- 2). Lancet 1992; 339(8809): S41
Is thromboprophylaxis effective in reducing the pulmonary thromboembolism?
 Is thromboprophylaxis effective in reducing the pulmonary thromboembolism? Fereshteh Rajabi (1), Masoumeh Sadeghi (2), Fereshteh Karbasian (3), Ali Torkan (4) Abstract BACKGROUND: Deep vein thrombosis
Is thromboprophylaxis effective in reducing the pulmonary thromboembolism? Fereshteh Rajabi (1), Masoumeh Sadeghi (2), Fereshteh Karbasian (3), Ali Torkan (4) Abstract BACKGROUND: Deep vein thrombosis
Cardiovascular Diseases and Diabetes
 Cardiovascular Diseases and Diabetes LEARNING OBJECTIVES Ø Identify the components of the cardiovascular system and the various types of cardiovascular disease Ø Discuss ways of promoting cardiovascular
Cardiovascular Diseases and Diabetes LEARNING OBJECTIVES Ø Identify the components of the cardiovascular system and the various types of cardiovascular disease Ø Discuss ways of promoting cardiovascular
An Open Randomized Study Prague-5 ˆ
 Next Day Discharge After Successful Primary Angioplasty for Acute ST Elevation Myocardial Infarction An Open Randomized Study Prague-5 Radovan JIRMÁR, 1 MD, Petr WIDIMSKÝ, 1 MD, Jan CAPEK, 1 MD, Ota HLINOMAZ,
Next Day Discharge After Successful Primary Angioplasty for Acute ST Elevation Myocardial Infarction An Open Randomized Study Prague-5 Radovan JIRMÁR, 1 MD, Petr WIDIMSKÝ, 1 MD, Jan CAPEK, 1 MD, Ota HLINOMAZ,
Lecture 8 Cardiovascular Health Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors
 Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
Evaluation of Anthropometric Indices of Patients with Left Ventricle Dysfunction Fallowing First Acute Anterior Myocardial Infarction
 Journal of Cardiovascular and Thoracic Research, 2012, 4(1), 11-15 doi: 10.5681/jcvtr.2012.003 http://jcvtr.tbzmed.ac.ir Evaluation of Anthropometric Indices of Patients with Left Ventricle Dysfunction
Journal of Cardiovascular and Thoracic Research, 2012, 4(1), 11-15 doi: 10.5681/jcvtr.2012.003 http://jcvtr.tbzmed.ac.ir Evaluation of Anthropometric Indices of Patients with Left Ventricle Dysfunction
Accelerating impact of diabetes mellitus on mortality in the years following an acute myocardial infarction
 European Heart Journal (1999) 20, 973 978 Article No. euhj.1999.1530, available online at http://www.idealibrary.com on Accelerating impact of diabetes mellitus on mortality in the years following an acute
European Heart Journal (1999) 20, 973 978 Article No. euhj.1999.1530, available online at http://www.idealibrary.com on Accelerating impact of diabetes mellitus on mortality in the years following an acute
Complications of Acute Myocardial Infarction
 Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
The ACC 50 th Annual Scientific Session
 Special Report The ACC 50 th Annual Scientific Session Part One From March 18 to 21, 2001, physicians from around the world gathered to learn, to teach and to discuss at the American College of Cardiology
Special Report The ACC 50 th Annual Scientific Session Part One From March 18 to 21, 2001, physicians from around the world gathered to learn, to teach and to discuss at the American College of Cardiology
PRIMARY CORONARY ANGIOPLASTY VERSUS INTRAVENOUS THROMBOLYSIS FOR ACUTE MYOCARDIAL INFARCTION - A COMPARATIVE STUDY AT QUEEN ALIA HEART INSTITUTE
 PRIMARY CORONARY ANGIOPLASTY VERSUS INTRAVENOUS THROMBOLYSIS FOR ACUTE MYOCARDIAL INFARCTION - A COMPARATIVE STUDY AT QUEEN ALIA HEART INSTITUTE Walid Sawalha MD, MBBS (Lond), MRCP(UK)* ABSTRACT Objectives:
PRIMARY CORONARY ANGIOPLASTY VERSUS INTRAVENOUS THROMBOLYSIS FOR ACUTE MYOCARDIAL INFARCTION - A COMPARATIVE STUDY AT QUEEN ALIA HEART INSTITUTE Walid Sawalha MD, MBBS (Lond), MRCP(UK)* ABSTRACT Objectives:
Objectives. Systolic Heart Failure: Definitions. Heart Failure: Historical Perspective 2/7/2009
 Objectives Diastolic Heart Failure and Indications for Echocardiography in the Asian Population Damon M. Kwan, MD UCSF Asian Heart & Vascular Symposium 02.07.09 Define diastolic heart failure and differentiate
Objectives Diastolic Heart Failure and Indications for Echocardiography in the Asian Population Damon M. Kwan, MD UCSF Asian Heart & Vascular Symposium 02.07.09 Define diastolic heart failure and differentiate
OUTCOME OF THROMBOLYTIC AND NON- THROMBOLYTIC THERAPY IN ACUTE MYOCARDIAL INFARCTION
 OUTCOME OF THROMBOLYTIC AND NON- THROMBOLYTIC THERAPY IN ACUTE MYOCARDIAL INFARCTION FEROZ MEMON*, LIAQUAT CHEEMA**, NAND LAL RATHI***, RAJ KUMAR***, NAZIR AHMED MEMON**** OBJECTIVE: To compare morbidity,
OUTCOME OF THROMBOLYTIC AND NON- THROMBOLYTIC THERAPY IN ACUTE MYOCARDIAL INFARCTION FEROZ MEMON*, LIAQUAT CHEEMA**, NAND LAL RATHI***, RAJ KUMAR***, NAZIR AHMED MEMON**** OBJECTIVE: To compare morbidity,
ORIGINAL ARTICLE. STUDY OF ARRHYTHMIAS IN ACUTE INFERIOR WALL MYOCARDIAL INFARCTION Ravikumar T. N 1, Anikethana G. V 2
 STUDY OF ARRHYTHMIAS IN ACUTE INFERIOR WALL MYOCARDIAL INFARCTION Ravikumar T. N 1, Anikethana G. V 2 HOW TO CITE THIS ARTICLE: Ravikumar T. N, Anikethana G. V. Study of Arrhythmias in Acute Inferior Wall
STUDY OF ARRHYTHMIAS IN ACUTE INFERIOR WALL MYOCARDIAL INFARCTION Ravikumar T. N 1, Anikethana G. V 2 HOW TO CITE THIS ARTICLE: Ravikumar T. N, Anikethana G. V. Study of Arrhythmias in Acute Inferior Wall
10/8/2018. Lecture 9. Cardiovascular Health. Lecture Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor
 Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
and Treatment in Emergency Care) Trial: Intravenous Glucose, Insulin & Potassium (GIK) in Emergency Medical Services
 Results of the IMMEDIATE (Immediate Myocardial Metabolic Enhancement DuringInitial Assessment and Treatment in Emergency Care) Trial: A Double Blinded Randomized Controlled Trial of Intravenous Glucose,
Results of the IMMEDIATE (Immediate Myocardial Metabolic Enhancement DuringInitial Assessment and Treatment in Emergency Care) Trial: A Double Blinded Randomized Controlled Trial of Intravenous Glucose,
Subsequent management and therapies
 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation Subsequent management and therapies Marco Valgimigli, MD, PhD University of Ferrara ITALY
ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation Subsequent management and therapies Marco Valgimigli, MD, PhD University of Ferrara ITALY
Current Advances and Best Practices in Acute STEMI Management A pharmacoinvasive approach
 Current Advances and Best Practices in Acute STEMI Management A pharmacoinvasive approach Frans Van de Werf, MD, PhD University Hospitals, Leuven, Belgium Frans Van de Werf: Disclosures Research grants
Current Advances and Best Practices in Acute STEMI Management A pharmacoinvasive approach Frans Van de Werf, MD, PhD University Hospitals, Leuven, Belgium Frans Van de Werf: Disclosures Research grants
Original Article. Abstract INTRODUCTION. Dhanesh M. Mhaskar, Sanket K. Mahajan, Komal C. Pawar
 Original Article Significance of serum magnesium levels in reference to acute myocardial infarction and role of intravenous magnesium therapy in prevention of cardiac arrhythmias following myocardial infarction
Original Article Significance of serum magnesium levels in reference to acute myocardial infarction and role of intravenous magnesium therapy in prevention of cardiac arrhythmias following myocardial infarction
Chapter 10. Learning Objectives. Learning Objectives 9/11/2012. Congestive Heart Failure
 Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM
 REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
PROCORALAN MAKING A STRONG ENTRY TO THE NEW ESC GUIDELINES FOR THE MANAGEMENT OF HEART FAILURE
 Press Release Issued on behalf of Servier Date: June 6, 2012 PROCORALAN MAKING A STRONG ENTRY TO THE NEW ESC GUIDELINES FOR THE MANAGEMENT OF HEART FAILURE The new ESC guidelines for the diagnosis and
Press Release Issued on behalf of Servier Date: June 6, 2012 PROCORALAN MAKING A STRONG ENTRY TO THE NEW ESC GUIDELINES FOR THE MANAGEMENT OF HEART FAILURE The new ESC guidelines for the diagnosis and
University of Groningen
 University of Groningen Computer assisted decision support in acutely ill patients. Application in glucose management and quantification of myocardial reperfusion Vogelzang, Mathijs IMPORTANT NOTE: You
University of Groningen Computer assisted decision support in acutely ill patients. Application in glucose management and quantification of myocardial reperfusion Vogelzang, Mathijs IMPORTANT NOTE: You
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Managing HTN in the Elderly: How Low to Go
 Managing HTN in the Elderly: How Low to Go Laxmi S. Mehta, MD, FACC The Ohio State University Medical Center Assistant Professor of Clinical Internal Medicine Clinical Director of the Women s Cardiovascular
Managing HTN in the Elderly: How Low to Go Laxmi S. Mehta, MD, FACC The Ohio State University Medical Center Assistant Professor of Clinical Internal Medicine Clinical Director of the Women s Cardiovascular
Curriculum Vitae. Saeed Alipour Parsa, M.D., Associate Professor of Cardiology
 Curriculum Vitae Saeed Alipour Parsa, M.D., Associate Professor of Cardiology Department of Interventional Cardiology Shahid Modarres hospital Shahid Beheshti University of Medical Sciences PERSONAL DATA
Curriculum Vitae Saeed Alipour Parsa, M.D., Associate Professor of Cardiology Department of Interventional Cardiology Shahid Modarres hospital Shahid Beheshti University of Medical Sciences PERSONAL DATA
Acute myocardial infarction. Cardiovascular disorders. main/0202_new 02/03/06. Search date August 2004 Nicholas Danchin and Eric Durand
 main/0202_new 02/03/06 Acute myocardial infarction Search date August 2004 Nicholas Danchin and Eric Durand QUESTIONS Which treatments improve outcomes in acute myocardial infarction?...4 Which treatments
main/0202_new 02/03/06 Acute myocardial infarction Search date August 2004 Nicholas Danchin and Eric Durand QUESTIONS Which treatments improve outcomes in acute myocardial infarction?...4 Which treatments
Mortality as an Efficacy or Safety Endpoint : Lessons Learned from the Heart Failure Trials
 Mortality as an Efficacy or Safety Endpoint : Lessons Learned from the Heart Failure Trials Christopher M. O Connor, MD Professor of Medicine Director, Duke Heart Center Acting Chief, Division of Cardiology
Mortality as an Efficacy or Safety Endpoint : Lessons Learned from the Heart Failure Trials Christopher M. O Connor, MD Professor of Medicine Director, Duke Heart Center Acting Chief, Division of Cardiology
Echocardiography analysis in renal transplant recipients
 Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS
 GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS Table of Contents List of authors pag 2 Supplemental figure I pag 3 Supplemental figure II pag 4 Supplemental
GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS Table of Contents List of authors pag 2 Supplemental figure I pag 3 Supplemental figure II pag 4 Supplemental
Does quality of life predict morbidity or mortality in patients with atrial fibrillation (AF)?
 Does quality of life predict morbidity or mortality in patients with atrial fibrillation (AF)? Erika Friedmann a, Eleanor Schron, b Sue A. Thomas a a University of Maryland School of Nursing; b NEI, National
Does quality of life predict morbidity or mortality in patients with atrial fibrillation (AF)? Erika Friedmann a, Eleanor Schron, b Sue A. Thomas a a University of Maryland School of Nursing; b NEI, National
Ischemic Heart Disease Mortality, Morbidity and Risk Factors of Coronary Care Unit Patients
 Ischemic Heart Disease Mortality, Morbidity and Risk Factors of Coronary (MBCHB, DM, FICMS) 1 Abstract Background: Ischemic heart disease (IHD) is the commonest type of heart disease.it causes more deaths
Ischemic Heart Disease Mortality, Morbidity and Risk Factors of Coronary (MBCHB, DM, FICMS) 1 Abstract Background: Ischemic heart disease (IHD) is the commonest type of heart disease.it causes more deaths
Antialdosterone treatment in heart failure
 Update on the Treatment of Chronic Heart Failure 2012 Antialdosterone treatment in heart failure 전남의대윤현주 Chronic Heart Failure Prognosis of Heart failure Cecil, Text book of Internal Medicine, 22 th edition
Update on the Treatment of Chronic Heart Failure 2012 Antialdosterone treatment in heart failure 전남의대윤현주 Chronic Heart Failure Prognosis of Heart failure Cecil, Text book of Internal Medicine, 22 th edition
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Clinical perspective It was recently discovered that small RNAs, called micrornas, circulate freely and stably in human plasma. This finding has sparked interest in the potential
SUPPLEMENTAL MATERIAL Clinical perspective It was recently discovered that small RNAs, called micrornas, circulate freely and stably in human plasma. This finding has sparked interest in the potential
Contrast Induced Nephropathy
 Contrast Induced Nephropathy O CIAKI refers to an abrupt deterioration in renal function associated with the administration of iodinated contrast media O CIAKI is characterized by an acute (within 48 hours)
Contrast Induced Nephropathy O CIAKI refers to an abrupt deterioration in renal function associated with the administration of iodinated contrast media O CIAKI is characterized by an acute (within 48 hours)
International Journal of Basic and Applied Physiology
 Cardiovascular Health Screening Of A Of Adults Residing In Ahmedabad City A Study Of Correlation Between Exercise, Body Mass Index And Heart Rate Jadeja Upasanaba*, Naik Shobha**, Jadeja Dhruvkumar***,
Cardiovascular Health Screening Of A Of Adults Residing In Ahmedabad City A Study Of Correlation Between Exercise, Body Mass Index And Heart Rate Jadeja Upasanaba*, Naik Shobha**, Jadeja Dhruvkumar***,
Evidence Supporting Post-MI Use of
 Addressing the Gap in the Management of Patients After Acute Myocardial Infarction: How Good Is the Evidence Supporting Current Treatment Guidelines? Michael B. Fowler, MB, FRCP Beta-adrenergic blocking
Addressing the Gap in the Management of Patients After Acute Myocardial Infarction: How Good Is the Evidence Supporting Current Treatment Guidelines? Michael B. Fowler, MB, FRCP Beta-adrenergic blocking
Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes
 Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes Seung-Jae Joo and other KAMIR-NIH investigators Department of Cardiology, Jeju National
Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes Seung-Jae Joo and other KAMIR-NIH investigators Department of Cardiology, Jeju National
Admission Hyperglycemia and Acute Myocardial Infarction: Outcomes and Potential Therapies for Diabetics and Nondiabetics
 Admission Hyperglycemia and Acute Myocardial Infarction: Outcomes and Potential Therapies for Diabetics and Nondiabetics The Harvard community has made this article openly available. Please share how this
Admission Hyperglycemia and Acute Myocardial Infarction: Outcomes and Potential Therapies for Diabetics and Nondiabetics The Harvard community has made this article openly available. Please share how this
Heart Failure and Cardiomyopathy Center, Division of Cardiology, North Shore University Hospital, Manhasset, NY
 NEUROHORMONAL ANTAGONISTS IN THE POST-MI PATIENT New Evidence from the CAPRICORN Trial: The Role of Carvedilol in High-Risk, Post Myocardial Infarction Patients Jonathan D. Sackner-Bernstein, MD, FACC
NEUROHORMONAL ANTAGONISTS IN THE POST-MI PATIENT New Evidence from the CAPRICORN Trial: The Role of Carvedilol in High-Risk, Post Myocardial Infarction Patients Jonathan D. Sackner-Bernstein, MD, FACC
Thornton Natural Healthcare s Better Health News
 February, 2011 Volume 6, Issue 2 Special Interest Articles: Magnesium and CHF Insulin insensitivity and sleep Congestive heart failure CoQ 10, carnitine and CHF Arginine and congestive heart failure Hawthorn
February, 2011 Volume 6, Issue 2 Special Interest Articles: Magnesium and CHF Insulin insensitivity and sleep Congestive heart failure CoQ 10, carnitine and CHF Arginine and congestive heart failure Hawthorn
Heart failure hospitalizations with preserved or reduced ejection fraction
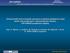 Clinical profile and in-hospital outcomes in patients admitted for heart failure with preserved or reduced ejection fraction. EPI-CARDIO prospective registry Tajer, C; Mariani, J; de Abreu, M; Charask,
Clinical profile and in-hospital outcomes in patients admitted for heart failure with preserved or reduced ejection fraction. EPI-CARDIO prospective registry Tajer, C; Mariani, J; de Abreu, M; Charask,
ST-elevation myocardial infarctions (STEMIs)
 Guidelines for Treating STEMI: Case-Based Questions As many as 25% of eligible patients presenting with STEMI do not receive any form of reperfusion therapy. The ACC/AHA guidelines highlight steps to improve
Guidelines for Treating STEMI: Case-Based Questions As many as 25% of eligible patients presenting with STEMI do not receive any form of reperfusion therapy. The ACC/AHA guidelines highlight steps to improve
CHAPTER - III METHODOLOGY
 74 CHAPTER - III METHODOLOGY This study was designed to determine the effectiveness of nurse-led cardiac rehabilitation on adherence and quality of life among patients with heart failure. 3.1. RESEARCH
74 CHAPTER - III METHODOLOGY This study was designed to determine the effectiveness of nurse-led cardiac rehabilitation on adherence and quality of life among patients with heart failure. 3.1. RESEARCH
Role of Early 2D Echocardiography in Patient with Acute Myocardial Infarction in Correlation with Electrocardiography and Clinical Presentation
 MVP Journal of Medical Sciences, Vol 1(2), 51 55, July 2014 Role of Early 2D Echocardiography in Patient with Acute Myocardial Infarction in Correlation with Electrocardiography and Clinical Presentation
MVP Journal of Medical Sciences, Vol 1(2), 51 55, July 2014 Role of Early 2D Echocardiography in Patient with Acute Myocardial Infarction in Correlation with Electrocardiography and Clinical Presentation
Impact of Nicorandil on Renal Function in Patients With Acute Heart Failure and Pre-Existing Renal Dysfunction
 Impact of Nicorandil on Renal Function in Patients With Acute Heart Failure and Pre-Existing Renal Dysfunction Masahito Shigekiyo, Kenji Harada, Ayumi Okada, Naho Terada, Hiroyoshi Yoshikawa, Akira Hirono,
Impact of Nicorandil on Renal Function in Patients With Acute Heart Failure and Pre-Existing Renal Dysfunction Masahito Shigekiyo, Kenji Harada, Ayumi Okada, Naho Terada, Hiroyoshi Yoshikawa, Akira Hirono,
Hospital and 1-year outcome after acute myocardial infarction in patients with diabetes mellitus and hypertension
 (2003) 17, 665 670 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Hospital and 1-year outcome after acute myocardial infarction in patients with
(2003) 17, 665 670 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Hospital and 1-year outcome after acute myocardial infarction in patients with
APPENDIX F: CASE REPORT FORM
 APPENDIX F: CASE REPORT FORM Instruction: Complete this form to notify all ACS admissions at your centre to National Cardiovascular Disease Registry. Where check boxes are provided, check ( ) one or more
APPENDIX F: CASE REPORT FORM Instruction: Complete this form to notify all ACS admissions at your centre to National Cardiovascular Disease Registry. Where check boxes are provided, check ( ) one or more
9 Diabetes care. Back to contents
 Back to contents Diabetes is a major risk factor for the development of peripheral vascular disease and 349/628 (55.6%) of the patients in this study had diabetes. Hospital inpatients with diabetes are
Back to contents Diabetes is a major risk factor for the development of peripheral vascular disease and 349/628 (55.6%) of the patients in this study had diabetes. Hospital inpatients with diabetes are
Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA
 Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA Case History A 50-year-old man with type 1 diabetes mellitus and hypertension presents after experiencing 1 hour of midsternal chest pain that began after
Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA Case History A 50-year-old man with type 1 diabetes mellitus and hypertension presents after experiencing 1 hour of midsternal chest pain that began after
Key words: Acute coronary syndrome, diabetes mellitus, insulin infusion systems, Iran, nursing
 Original Article Impacts of insulin infusion protocol on blood glucose level and outcomes in acute coronary syndrome patients with diabetes mellitus Fakhri Sabouhi 1, Mahboubeh Maleki 2, Masoud Amini 3,
Original Article Impacts of insulin infusion protocol on blood glucose level and outcomes in acute coronary syndrome patients with diabetes mellitus Fakhri Sabouhi 1, Mahboubeh Maleki 2, Masoud Amini 3,
Management of cardiovascular disease. Acute coronary syndromes and intensive care. Lars Rydén Karolinska Institutet Stockholm, Sweden
 Management of cardiovascular disease Acute coronary syndromes and intensive care Lars Rydén Karolinska Institutet Stockholm, Sweden Hyperglycemia and acute coronary syndromes Changing fenotype GAMI Study
Management of cardiovascular disease Acute coronary syndromes and intensive care Lars Rydén Karolinska Institutet Stockholm, Sweden Hyperglycemia and acute coronary syndromes Changing fenotype GAMI Study
Polypharmacy - arrhythmic risks in patients with heart failure
 Influencing sudden cardiac death by pharmacotherapy Polypharmacy - arrhythmic risks in patients with heart failure Professor Dan Atar Head, Dept. of Cardiology Oslo University Hospital Ullevål Norway 27.8.2012
Influencing sudden cardiac death by pharmacotherapy Polypharmacy - arrhythmic risks in patients with heart failure Professor Dan Atar Head, Dept. of Cardiology Oslo University Hospital Ullevål Norway 27.8.2012
There is no conflict of interests for the following presentation
 There is no conflict of interests for the following presentation Inflammation and Left Ventricular Diastolic Dysfunction Cho-Kai Wu MD National Taiwan University Hospital, Taipei, Taiwan Diastolic heart
There is no conflict of interests for the following presentation Inflammation and Left Ventricular Diastolic Dysfunction Cho-Kai Wu MD National Taiwan University Hospital, Taipei, Taiwan Diastolic heart
Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient
 Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient Dr. Peersab.M. Pinjar 1, Dr Praveenkumar Devarbahvi 1 and Dr Vasudeva Murthy.C.R 2, Dr.S.S.Bhat 1, Dr.Jayaraj S G 1
Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient Dr. Peersab.M. Pinjar 1, Dr Praveenkumar Devarbahvi 1 and Dr Vasudeva Murthy.C.R 2, Dr.S.S.Bhat 1, Dr.Jayaraj S G 1
Study of the relationship between hyperglycemia and hyperlipidemia and ACS in patients referring to a hospital in Tehran
 ISSN: 2347-3215 Volume 2 Number 7 (July-2014) pp. 209-214 www.ijcrar.com Study of the relationship between hyperglycemia and hyperlipidemia and ACS in patients referring to a hospital in Tehran Ali Mohammadshahi
ISSN: 2347-3215 Volume 2 Number 7 (July-2014) pp. 209-214 www.ijcrar.com Study of the relationship between hyperglycemia and hyperlipidemia and ACS in patients referring to a hospital in Tehran Ali Mohammadshahi
Takotsubo Cardiomyopathy
 Advances in Heart Disease 2008 Takotsubo Cardiomyopathy Mary O. Gray, MD, FAHA, FACC Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training Faculty Divisions
Advances in Heart Disease 2008 Takotsubo Cardiomyopathy Mary O. Gray, MD, FAHA, FACC Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training Faculty Divisions
A Comparative Study on the Effect of Ranolazine and Ivabradine on High Sensitivity C - reactive protein In Cardiac Patients
 Human Journals Mini Review March 2017 Vol.:8, Issue: 4 All rights are reserved by Prof. Dr. Mathew George et al. A Comparative Study on the Effect of Ranolazine and Ivabradine on High Sensitivity C - reactive
Human Journals Mini Review March 2017 Vol.:8, Issue: 4 All rights are reserved by Prof. Dr. Mathew George et al. A Comparative Study on the Effect of Ranolazine and Ivabradine on High Sensitivity C - reactive
Management of Acute Myocardial Infarction
 Management of Acute Myocardial Infarction Prof. Hossam Kandil Professor of Cardiology Cairo University ST Elevation Acute Myocardial Infarction Aims Of Management Emergency care (Pre-hospital) Early care
Management of Acute Myocardial Infarction Prof. Hossam Kandil Professor of Cardiology Cairo University ST Elevation Acute Myocardial Infarction Aims Of Management Emergency care (Pre-hospital) Early care
Patient characteristics Intervention Comparison Length of followup
 ISCHAEMIA TESTING CHAPTER TESTING FOR MYCOCARDIAL ISCHAEMIA VERSUS NOT TESTING FOR MYOCARDIAL ISCHAEMIA Ref ID: 4154 Reference Wienbergen H, Kai GA, Schiele R et al. Actual clinical practice exercise ing
ISCHAEMIA TESTING CHAPTER TESTING FOR MYCOCARDIAL ISCHAEMIA VERSUS NOT TESTING FOR MYOCARDIAL ISCHAEMIA Ref ID: 4154 Reference Wienbergen H, Kai GA, Schiele R et al. Actual clinical practice exercise ing
The importance of follow-up after a cardiac event: CARDIAC REHABILITATION. Dr. Guy Letcher
 The importance of follow-up after a cardiac event: CARDIAC REHABILITATION Dr. Guy Letcher The National Medicare Experience Mortality After Angioplasty 225,915 patients Mortality After Bypass Surgery 357,885
The importance of follow-up after a cardiac event: CARDIAC REHABILITATION Dr. Guy Letcher The National Medicare Experience Mortality After Angioplasty 225,915 patients Mortality After Bypass Surgery 357,885
The role of insulin therapy and glucose normalisation in patients with acute coronary syndrome
 Neth Heart J (2011) 19:79 84 DOI 10.1007/s12471-010-0065-1 REVIEW ARTICLE The role of insulin therapy and glucose normalisation in patients with acute coronary syndrome J. A. Lipton & A. Can & S. Akoudad
Neth Heart J (2011) 19:79 84 DOI 10.1007/s12471-010-0065-1 REVIEW ARTICLE The role of insulin therapy and glucose normalisation in patients with acute coronary syndrome J. A. Lipton & A. Can & S. Akoudad
Topic Page: congestive heart failure
 Topic Page: congestive heart failure Definition: congestive heart f ailure from Merriam-Webster's Collegiate(R) Dictionary (1930) : heart failure in which the heart is unable to maintain an adequate circulation
Topic Page: congestive heart failure Definition: congestive heart f ailure from Merriam-Webster's Collegiate(R) Dictionary (1930) : heart failure in which the heart is unable to maintain an adequate circulation
Diabetes mellitus (DM) is a well-established risk factor for death
 Continuous insulin infusion reduces mortality in patients with diabetes undergoing coronary artery bypass grafting Anthony P. Furnary, MD, a,d Guangqiang Gao, MD, a Gary L. Grunkemeier, PhD, b YingXing
Continuous insulin infusion reduces mortality in patients with diabetes undergoing coronary artery bypass grafting Anthony P. Furnary, MD, a,d Guangqiang Gao, MD, a Gary L. Grunkemeier, PhD, b YingXing
Continuing Medical Education Post-Test
 Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Impact of metabolic syndrome on hospital in acute myocardial infarction patients
 Original Article Impact of metabolic syndrome on hospital in acute myocardial infarction patients Pravin Rohidasrao Bhagat 1*, Shubhangi Virbhadra Swami 2 outcomes { 1 Assistant Professor, Department of
Original Article Impact of metabolic syndrome on hospital in acute myocardial infarction patients Pravin Rohidasrao Bhagat 1*, Shubhangi Virbhadra Swami 2 outcomes { 1 Assistant Professor, Department of
Myocardial Infarction In Dr.Yahya Kiwan
 Myocardial Infarction In 2007 Dr.Yahya Kiwan New Definition Of Acute Myocardial Infarction The term of myocardial infarction should be used when there is evidence of myocardial necrosis in a clinical setting
Myocardial Infarction In 2007 Dr.Yahya Kiwan New Definition Of Acute Myocardial Infarction The term of myocardial infarction should be used when there is evidence of myocardial necrosis in a clinical setting
Can point of care cardiac biomarker testing guide cardiac safety during oncology trials?
 Can point of care cardiac biomarker testing guide cardiac safety during oncology trials? Daniel J Lenihan, MD Professor, Division of Cardiovascular Medicine Director, Clinical Research Vanderbilt University
Can point of care cardiac biomarker testing guide cardiac safety during oncology trials? Daniel J Lenihan, MD Professor, Division of Cardiovascular Medicine Director, Clinical Research Vanderbilt University
CHRONIC HEART FAILURE : WHAT ELSE COULD WE OFFER TO OUR PATIENTS? Cardiac Rehabilitation Society of Thailand
 CHRONIC HEART FAILURE : WHAT ELSE COULD WE OFFER TO OUR PATIENTS? Cardiac Rehabilitation Society of Thailand ENHANCED EXTERNAL COUNTER PULSATION Piyanuj Ruckpanich, MD. Cardiac Rehabilitation Center Perfect
CHRONIC HEART FAILURE : WHAT ELSE COULD WE OFFER TO OUR PATIENTS? Cardiac Rehabilitation Society of Thailand ENHANCED EXTERNAL COUNTER PULSATION Piyanuj Ruckpanich, MD. Cardiac Rehabilitation Center Perfect
Diabetes and the Heart
 Diabetes and the Heart Association of Specialty Professors April 4, 2013 Jorge Plutzky, MD Co-Director, Preventive Cardiology Director, The Lipid Clinic Cardiovascular Division Brigham and Women s Hospital
Diabetes and the Heart Association of Specialty Professors April 4, 2013 Jorge Plutzky, MD Co-Director, Preventive Cardiology Director, The Lipid Clinic Cardiovascular Division Brigham and Women s Hospital
Prolonged Oral Morphine Therapy for Severe Angina Pectoris
 Vol. 19 No. 5 May 2000 Journal of Pain and Symptom Management 393 Clinical Note Prolonged Oral Morphine Therapy for Severe Angina Pectoris Meir Mouallem, MD, Eli Schwartz, MD, and Zvi Farfel, MD Department
Vol. 19 No. 5 May 2000 Journal of Pain and Symptom Management 393 Clinical Note Prolonged Oral Morphine Therapy for Severe Angina Pectoris Meir Mouallem, MD, Eli Schwartz, MD, and Zvi Farfel, MD Department
Risk of sudden cardiac death. Original Article
 Risk of sudden cardiac death Roxana Sadeghi (1), Nadia Adnani (2), Mohammad-Reza Sohrabi (3), Saeed Alipour Parsa (1) Abstract Original Article BACKGROUND: The aim of this study was to determine characteristics
Risk of sudden cardiac death Roxana Sadeghi (1), Nadia Adnani (2), Mohammad-Reza Sohrabi (3), Saeed Alipour Parsa (1) Abstract Original Article BACKGROUND: The aim of this study was to determine characteristics
ANTIHYPERTENSIVE DRUGS USED BY HYPERTENSIVE PATIENTS IN THE PROVINCIAL CITIES OF ISFAHAN, NAJAFABAD AND ARAK
 ANTIHYPERTENSIVE DRUGS USED BY HYPERTENSIVE PATIENTS IN THE PROVINCIAL CITIES OF ISFAHAN, NAJAFABAD AND ARAK Keywords Hypertension Adults Antihypertensive drugs Combinational regimens ARYA Journal, 2006,
ANTIHYPERTENSIVE DRUGS USED BY HYPERTENSIVE PATIENTS IN THE PROVINCIAL CITIES OF ISFAHAN, NAJAFABAD AND ARAK Keywords Hypertension Adults Antihypertensive drugs Combinational regimens ARYA Journal, 2006,
12 Lead EKG Chapter 4 Worksheet
 Match the following using the word bank. 1. A form of arteriosclerosis in which the thickening and hardening of the vessels walls are caused by an accumulation of fatty deposits in the innermost lining
Match the following using the word bank. 1. A form of arteriosclerosis in which the thickening and hardening of the vessels walls are caused by an accumulation of fatty deposits in the innermost lining
Shervin Ziabakhsh Tabary., Asian Journal of Pharmaceutical Technology & Innovation, 02 (05); 2014; 01-08
 Shervin Ziabakhsh Tabary., Asian Journal of Pharmaceutical Technology & Innovation, 02 (05); 2014; 01-08 Asian Journal of Pharmaceutical Technology & Innovation ISSN: 2347-8810 Received on: 18-02-2014
Shervin Ziabakhsh Tabary., Asian Journal of Pharmaceutical Technology & Innovation, 02 (05); 2014; 01-08 Asian Journal of Pharmaceutical Technology & Innovation ISSN: 2347-8810 Received on: 18-02-2014
Hyperglycemia in ACS. Dr. Imhemed Eljazwi
 Hyperglycemia in ACS 2012-5-8 Dr. Imhemed Eljazwi Percentage of Population (n = 1181) Prevalence of Hyperglycemia in 181 Cardiac Patients Without Known Diabetes 100% 75% 50% 66% of AMI patients have
Hyperglycemia in ACS 2012-5-8 Dr. Imhemed Eljazwi Percentage of Population (n = 1181) Prevalence of Hyperglycemia in 181 Cardiac Patients Without Known Diabetes 100% 75% 50% 66% of AMI patients have
Treating the patient with acute heart failure. What do we really know? Principles of acute heart failure treatment
 ESC 2012 27Aug - 3Sep, 2012, Munich, Germany Treating the patient with acute heart failure. What do we really know? Principles of acute heart failure treatment Marco Metra, MD, FESC Cardiology University
ESC 2012 27Aug - 3Sep, 2012, Munich, Germany Treating the patient with acute heart failure. What do we really know? Principles of acute heart failure treatment Marco Metra, MD, FESC Cardiology University
Study of rhythm disturbances in acute myocardial infarction in Government Dharmapuri Medical College Hospital, Dharmapuri
 Original Research Article Study of rhythm disturbances in acute myocardial infarction in Government Dharmapuri Medical College Hospital, Dharmapuri P. Sasikumar * Department of General Medicine, Govt.
Original Research Article Study of rhythm disturbances in acute myocardial infarction in Government Dharmapuri Medical College Hospital, Dharmapuri P. Sasikumar * Department of General Medicine, Govt.
Supplementary Material to Mayer et al. A comparative cohort study on personalised
 Suppl. Table : Baseline characteristics of the patients. Characteristic Modified cohort Non-modified cohort P value (n=00) Age years 68. ±. 69.5 ±. 0. Female sex no. (%) 60 (0.0) 88 (.7) 0.0 Body Mass
Suppl. Table : Baseline characteristics of the patients. Characteristic Modified cohort Non-modified cohort P value (n=00) Age years 68. ±. 69.5 ±. 0. Female sex no. (%) 60 (0.0) 88 (.7) 0.0 Body Mass
Heart Failure with Preserved Ejection Fraction (HFpEF): Natural History and Contemporary Management
 Heart Failure with Preserved Ejection Fraction (HFpEF): Natural History and Contemporary Management Jason L. Guichard, MD, PhD Greenville Health System Department of Medicine, Carolina Cardiology Consultants
Heart Failure with Preserved Ejection Fraction (HFpEF): Natural History and Contemporary Management Jason L. Guichard, MD, PhD Greenville Health System Department of Medicine, Carolina Cardiology Consultants
Ultrafiltration in Decompensated Heart Failure. Description
 Subject: Ultrafiltration in Decompensated Heart Failure Page: 1 of 7 Last Review Status/Date: September 2016 Ultrafiltration in Decompensated Heart Failure Description Ultrafiltration is a technique being
Subject: Ultrafiltration in Decompensated Heart Failure Page: 1 of 7 Last Review Status/Date: September 2016 Ultrafiltration in Decompensated Heart Failure Description Ultrafiltration is a technique being
The PAIN Pathway for the Management of Acute Coronary Syndrome
 2 The PAIN Pathway for the Management of Acute Coronary Syndrome Eyal Herzog, Emad Aziz, and Mun K. Hong Acute coronary syndrome (ACS) subsumes a spectrum of clinical entities, ranging from unstable angina
2 The PAIN Pathway for the Management of Acute Coronary Syndrome Eyal Herzog, Emad Aziz, and Mun K. Hong Acute coronary syndrome (ACS) subsumes a spectrum of clinical entities, ranging from unstable angina
Coronary heart disease
 1 of 9 12/30/2012 10:58 PM PubMed Health. A service of the National Library of Medicine, National Institutes of Health. A.D.A.M. Medical Encyclopedia. Atlanta (GA): A.D.A.M.; 2011. Coronary heart disease
1 of 9 12/30/2012 10:58 PM PubMed Health. A service of the National Library of Medicine, National Institutes of Health. A.D.A.M. Medical Encyclopedia. Atlanta (GA): A.D.A.M.; 2011. Coronary heart disease
Citation for published version (APA): Horst, J. C. C. V. D. (2005). Metabolic interventions in acute myocardial infarction. s.n.
 University of Groningen Horst, Johannes Cornelis Clemens van der IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Horst, Johannes Cornelis Clemens van der IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
The Incidence and Predictors of Postoperative Atrial Fibrillation After Noncardiothoracic Surgery
 ORIGINAL ARTICLE DOI 10.4070 / kcj.2009.39.3.100 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology The Incidence and Predictors of Postoperative Atrial Fibrillation
ORIGINAL ARTICLE DOI 10.4070 / kcj.2009.39.3.100 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology The Incidence and Predictors of Postoperative Atrial Fibrillation
Andrew Cohen, MD and Neil S. Skolnik, MD INTRODUCTION
 2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT
 NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT CONTENTS PATIENTS ADMITTED WITH HEART FAILURE...4 Demographics... 4 Trends in Symptoms... 4 Causes and Comorbidities
NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT CONTENTS PATIENTS ADMITTED WITH HEART FAILURE...4 Demographics... 4 Trends in Symptoms... 4 Causes and Comorbidities
During normoxia, ATP delivery to the myofilaments and
 ATP Synthesis During Low-Flow Ischemia Influence of Increased Glycolytic Substrate Alison C. Cave, PhD; Joanne S. Ingwall, PhD; Jan Friedrich, MD, DPhil; Ronglih Liao, PhD; Kurt W. Saupe, PhD; Carl S.
ATP Synthesis During Low-Flow Ischemia Influence of Increased Glycolytic Substrate Alison C. Cave, PhD; Joanne S. Ingwall, PhD; Jan Friedrich, MD, DPhil; Ronglih Liao, PhD; Kurt W. Saupe, PhD; Carl S.
Populations Interventions Comparators Outcomes Individuals: With diagnosed heart disease. rehabilitation
 Protocol Cardiac Rehabilitation in the Outpatient Setting (80308) Medical Benefit Effective Date: 01/01/17 Next Review Date: 05/18 Preauthorization No Review Dates: 07/07, 07/08, 05/09, 05/10, 05/11, 05/12,
Protocol Cardiac Rehabilitation in the Outpatient Setting (80308) Medical Benefit Effective Date: 01/01/17 Next Review Date: 05/18 Preauthorization No Review Dates: 07/07, 07/08, 05/09, 05/10, 05/11, 05/12,
The role of internist in heart failure management bridging the quality gaps
 The role of internist in heart failure management bridging the quality gaps Mohammad AlQahtani.MD,FACP Associate professor and head of internal medicine, KSAU-HS/KAMC Consultant internal medicine/hf Deputy
The role of internist in heart failure management bridging the quality gaps Mohammad AlQahtani.MD,FACP Associate professor and head of internal medicine, KSAU-HS/KAMC Consultant internal medicine/hf Deputy
Comparison of Lipoprotein (a) and Apolipoproteins in Children with and without Familial History of Premature Coronary Artery Disease
 Short Comunication Iran J Pediatr Jun 2008; Vol 18 ( No 2), Pp:159-162 Comparison of Lipoprotein (a) and Apolipoproteins in Children with and without Familial History of Premature Coronary Artery Disease
Short Comunication Iran J Pediatr Jun 2008; Vol 18 ( No 2), Pp:159-162 Comparison of Lipoprotein (a) and Apolipoproteins in Children with and without Familial History of Premature Coronary Artery Disease
Blood Pressure Targets: Where are We Now?
 Blood Pressure Targets: Where are We Now? Diana Cao, PharmD, BCPS-AQ Cardiology Assistant Professor Department of Clinical & Administrative Sciences California Northstate University College of Pharmacy
Blood Pressure Targets: Where are We Now? Diana Cao, PharmD, BCPS-AQ Cardiology Assistant Professor Department of Clinical & Administrative Sciences California Northstate University College of Pharmacy
Product: Omecamtiv Mecarbil Clinical Study Report: Date: 02 April 2014 Page 1
 Date: 02 April 2014 Page 1. 2. SYNOPSIS Name of Sponsor: Amgen Inc. Name of Finished Product: Omecamtiv mecarbil injection Name of Active Ingredient: Omecamtiv mecarbil (AMG 423) Title of Study: A double-blind,
Date: 02 April 2014 Page 1. 2. SYNOPSIS Name of Sponsor: Amgen Inc. Name of Finished Product: Omecamtiv mecarbil injection Name of Active Ingredient: Omecamtiv mecarbil (AMG 423) Title of Study: A double-blind,
WHI Form Report of Cardiovascular Outcome Ver (For items 1-11, each question specifies mark one or mark all that apply.
 WHI Form - Report of Cardiovascular Outcome Ver. 6. COMMENTS To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: OMB# 095-044 Exp: 4/06 -Affix label here- Clinical Center/ID:
WHI Form - Report of Cardiovascular Outcome Ver. 6. COMMENTS To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: OMB# 095-044 Exp: 4/06 -Affix label here- Clinical Center/ID:
A study of left ventricular dysfunction and hypertrophy by various diagnostic modalities in normotensive type 2 diabetes mellitus patients
 Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 8:102-106 A study of left ventricular dysfunction and hypertrophy by various
Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 8:102-106 A study of left ventricular dysfunction and hypertrophy by various
Statistical analysis plan
 Statistical analysis plan Prepared and approved for the BIOMArCS 2 glucose trial by Prof. Dr. Eric Boersma Dr. Victor Umans Dr. Jan Hein Cornel Maarten de Mulder Statistical analysis plan - BIOMArCS 2
Statistical analysis plan Prepared and approved for the BIOMArCS 2 glucose trial by Prof. Dr. Eric Boersma Dr. Victor Umans Dr. Jan Hein Cornel Maarten de Mulder Statistical analysis plan - BIOMArCS 2
Sudden death as co-morbidity in patients following vascular intervention
 Sudden death as co-morbidity in patients following vascular intervention Impact of ICD therapy Seah Nisam Director, Medical Science, Guidant Corporation Advanced Angioplasty Meeting (BCIS) London, 16 Jan,
Sudden death as co-morbidity in patients following vascular intervention Impact of ICD therapy Seah Nisam Director, Medical Science, Guidant Corporation Advanced Angioplasty Meeting (BCIS) London, 16 Jan,
Ischemic Postconditioning During Primary Percutaneous Coronary Intervention Mechanisms and Clinical Application Jian Liu, MD FACC FESC FSCAI Chief Phy
 Ischemic Postconditioning During Primary Percutaneous Coronary Intervention Mechanisms and Clinical Application Jian Liu, MD FACC FESC FSCAI Chief Physician, Professor of Medicine Department of Cardiology,
Ischemic Postconditioning During Primary Percutaneous Coronary Intervention Mechanisms and Clinical Application Jian Liu, MD FACC FESC FSCAI Chief Physician, Professor of Medicine Department of Cardiology,
Questions and Answers: The NIH Trial of EDTA Chelation Therapy for Coronary Heart Disease
 Questions and Answers: The NIH Trial of EDTA Chelation Therapy for Coronary Heart Disease Results from the Trial to Assess Chelation Therapy will be published in the Journal of the American Medical Associatio
Questions and Answers: The NIH Trial of EDTA Chelation Therapy for Coronary Heart Disease Results from the Trial to Assess Chelation Therapy will be published in the Journal of the American Medical Associatio
Catheter-based mitral valve repair MitraClip System
 Percutaneous Mitral Valve Repair: Results of the EVEREST II Trial William A. Gray MD Director of Endovascular Services Associate Professor of Clinical Medicine Columbia University Medical Center The Cardiovascular
Percutaneous Mitral Valve Repair: Results of the EVEREST II Trial William A. Gray MD Director of Endovascular Services Associate Professor of Clinical Medicine Columbia University Medical Center The Cardiovascular
