Gastrointestinal Intervention
|
|
|
- Anabel Barton
- 6 years ago
- Views:
Transcription
1 Gastrointest Interv 2013; 2:24 29 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: Review Article Self-expandable metal stents for endoscopic ultrasound-guided drainage of peripancreatic fluid collections Daisy Walter, * Frank P. Vleggaar, Peter D. Siersema abstract Endoscopic ultrasound (EUS)-guided transmural drainage has evolved as an important treatment modality for peripancreatic fluid collections (PFCs). Recently, self-expandable metal stents (SEMS) have been introduced as an alternative for the traditionally used double-pigtail plastic stents, for endoscopic drainage. Due to the larger diameter (>10 mm) of SEMS, a wide drainage opening can be created, with a potentially reduced risk of stent occlusion and associated complications, and a direct access route if endoscopic necrosectomy is indicated. The use of different types of SEMS has been reported in several case reports and small case series. Although the results of these studies seem promising, the available results to date are limited and need critical appraisal. Large prospective and randomized trials are needed to evaluate the efficacy and safety of the placement of SEMS for endoscopic drainage of PFCs. Copyright Ó 2013, Society of Gastrointestinal Intervention. Published by Elsevier. All rights reserved. Keywords: Pancreatic necrosis, Pancreatic pseudocyst, Peripancreatic fluid collection, Self-expandable metal stents, Transmural drainage Introduction Peripancreatic fluid collections (PFCs) may complicate the course of acute and chronic pancreatitis, pancreatic surgery or trauma. They develop due to disruption of the pancreatic duct, with subsequent fluid leakage, or as a consequence of maturation of (peri)pancreatic necrosis. 1 3 Over the past decade, endoscopic ultrasound (EUS)-guided transmural drainage has evolved as an important treatment modality for PFCs. 4 The aim of this review is to give an overview of EUS-guided treatment modalities for the different types of PFCs, with special focus on the use of self-expandable metal stents (SEMS). Definitions of peripancreatic fluid collections The use of precise terminology and strict definitions for different types of PFCs is important, since each form requires a distinct treatment strategy. Moreover, a universal classification system is essential for comparing results of studies. In 1992, the widely accepted Atlanta Classification was introduced as a clinically based classification system for PFCs that occur as a complication of acute pancreatitis. 1 Definitions were proposed for the following types of collections: acute fluid collection, pseudocyst, pancreatic abscess and pancreatic necrosis. In order to describe the evolution of pancreatic necrosis and acute fluid collections to a more organized, partially encapsulated state, Baron et al subsequently introduced the term, organized pancreatic necrosis, in Although this term for describing PFCs was not defined in the 1992 Atlanta Classification, it has been widely adopted from then on. 5 The original Atlanta Classification is considered to be a milestone in the classification of PFCs. Nonetheless, new insights into the pathophysiology of acute pancreatitis, improved imaging techniques, and the emergence of minimally invasive techniques for the management of PFCs, made it necessary to revise the Atlanta Classification in 2008 (Table 1). 6,7 In the revised Atlanta Classification, PFCs were defined by the presence or absence of necrosis. This distinction between fluid and nonliquefied collections is important, as the therapeutic strategy and clinical outcome differ between collections containing fluid alone and those containing necrotic debris as well. Subsequently, collections were further subdivided according to whether the contents are infected or sterile Acute collections, developing within the first 4 weeks after the onset of acute pancreatitis, are referred to as either acute peripancreatic fluid collections (APFC) or as acute necrotic collections (ANC). APFCs are extrapancreatic homogeneous collections without nonliquefied components, i.e., debris or necrosis, and lack a welldefined wall. The majority of these APFCs are reabsorbed spontaneously within several weeks and only a minority matures into a pancreatic pseudocyst (PP). Drainage is only indicated in the rare Department of Gastroenterology and Hepatology, University Medical Center Utrecht, Utrecht, The Netherlands Received 7 January 2013; Accepted 15 January 2013 * Corresponding author. Department of Gastroenterology and Hepatology, University Medical Center Utrecht, P.O. Box 85500, 3508 GA Utrecht, The Netherlands. address: d.walter@umcutrecht.nl (D. Walter) /$ see front matter Copyright Ó 2013, Society of Gastrointestinal Intervention. Published by Elsevier. All rights reserved.
2 Daisy Walter et al. / SEMS for transmural drainage 25 Table 1 Comparison of Atlanta Classification 1992 and Revised Atlanta Classification 2008 Atlanta Classification 1992 Working Group Classification 2008 <4 wk after onset of acute pancreatitis Acute fluid collection Acute peripancreatic fluid collections (APFC) Pancreatic necrosis Acute necrotic collection (ANC) 4 wk after onset of acute pancreatitis Pancreatic pseudocyst (PP) Pancreatic pseudocyst Pancreatic abscess Organized pancreatic necrosis* Walled-off pancreatic necrosis (WOPN) * Introduced by Baron et al. (1996). case that an APFC becomes infected. 7,12 In contrast, ANCs contain both fluid and necrotic material in various proportions, due to gradual liquefaction of necrotic tissue. These collections are not encapsulated and infected necrosis in these collections is an indication for drainage. 7,11 Within a period of approximately 4 weeks, acute collections mature and become encapsulated. These mature collections are subdivided into a PP and walled-off pancreatic necrosis (WOPN). PPs are defined as homogeneous fluid collections surrounded by a well-defined nonepithelialized fibrous wall, without nonliquefied components. They usually contain increased amylase and lipase levels, due to communication with the pancreatic ductal system. Sealing of such ductal disruptions explains the spontaneous resolution of the majority of PPs. Intervention is only indicated for PPs causing pain, jaundice or gastric outlet obstruction, due to compression on the biliary or gastrointestinal tract or fever due to infection WOPN represents the late stage of an AFPC, previously referred to as organized pancreatic necrosis. 2 A thickened wall, without an epithelial lining, forms the interface between necrosis and adjacent viable tissue. WOPN usually require drainage to effectively control sepsis, whereas in patients with sterile WOPN, the need for drainage is based on the same symptoms as for a PP. 7,12,13 Treatment modalities The management of PFCs has changed considerably over the last decades. Until the introduction of endoscopic drainage of PFCs in the late 1980s, treatment options were limited to surgical and percutaneous drainage. Since then, endoscopic transmural drainage has emerged as an important minimally invasive treatment modality. 4,16,17 Surgical drainage Surgery of PP involves internal drainage by creating an anastomosis between the cyst and a small-bowel loop, a cyst-enteric anastomosis. Although success rates are excellent, the procedure is associated with significant morbidity and mortality rates of 24% and 5.8%, respectively. 18,19 Furthermore, surgical drainage of PP is associated with a longer hospital stay compared to EUS-guided drainage. 20 The main role of surgical drainage for PP is, therefore, adjunctive to an endoscopic procedure or as salvage therapy. 4 The traditional surgical approach for WOPN is an open surgical necrosectomy. This invasive procedure is associated with high morbidity (34 95%) and mortality (11 39%) rates. 21 Minimally invasive surgical techniques, including laparoscopic necrosectomy and video-assisted retroperitoneal debridement (VARD), have gained wide popularity as alternatives due to lower morbidity and mortality rates (25 88% and 0 25%, respectively). 21,22 A recent randomized pilot study, comparing surgical necrosectomy to endoscopic necrosectomy, showed a higher pro-inflammatory response as well as higher morbidity and mortality rates for the surgical approach in cases of infected necrosis. 23 Despite these results, to date, surgical necrosectomy still has an important role in the step-up treatment algorithm for WOPN. 21,24 Percutaneous drainage A less invasive alternative to surgery is percutaneous drainage, performed under radiological guidance. Although clear fluids can be drained effectively via the percutaneous drain, a drawback of this technique is the inability to clear the necrotic content from the cyst. 4 In approximately half of patients with infected WOPN, drainage of the infected fluid provides adequate control of sepsis and the necrotic material will be reabsorbed without formal necrosectomy. However, additional necrosectomy is needed in the other patients. 21,24 27 Risks associated with percutaneous drainage include puncture of adjacent viscera, secondary infection and bleeding. Furthermore, a prolonged need for an external draining catheter may result in a considerable risk of developing a pancreaticocutaneous fistula. For collections which cannot be accessed endoscopically, or those without a mature wall, percutaneous drainage may be of additive value. 4,26 Endoscopic drainage As mentioned above, endoscopic transmural drainage of PPs was introduced in the 1980s. 16,17 The first endoscopic necrosectomy for WOPN followed in 1996, by Baron et al. 2 Since the first reports, much more experience has been gained and endoscopic techniques have evolved. Endoscopic drainage entails the creation of a fistulous tract between the PFC and the lumen of the upper gastrointestinal tract, followed by placement of double-pigtail stents and eventually a nasocystic catheter to facilitate drainage. To be eligible for this approach, PFCs should have a well-defined wall and be located within 1 cm of the duodenal, esophageal or gastric wall. Furthermore, the presence of a luminal bulge is a prerequisite when performing endoscopic drainage without EUS-guidance, since this is a relatively blind approach. Due to direct sonographic visualization, the introduction of EUS-guidance enables drainage of nonbulging PFCs, without an increased risk of perforation or puncture of other organs. Moreover, intervening vessels can be identified by using Doppler ultrasound and avoided at the puncture site, with a potential reduction of the bleeding risk. 4,28 Apart from access and safety, performing EUS before endoscopic drainage can provide essential information to rule out alternative diagnoses and differentiate between WOPN and PPs. 29,30 Two randomized trials have compared endoscopy-guided, with EUS-guided, drainage for PPs. In the EUS-guided group, fewer complications were reported; however, this difference was not statistically significant. The technical success rates were significantly higher for EUS-guided drainage (94 100%) than for endoscopy-guided drainage (33 72%) (P < 0.05). This difference was mainly due to a high failure rate for nonbulging PP in the endoscopy group. 31,32 Although some other studies have reported technical success rates to be equal for both endoscopy-guided and EUSguided drainage, EUS-guidance is increasingly being used for drainage. 28,33 The success rate of EUS-guided drainage is highly dependent on the type of PFC drained. The use of different nomenclature, leads to
3 26 Table 2 EUS-guided Drainage of Peripancreatic Fluid Collections (PFC) Using Self-expandable Metal Stents (SEMS) Authors No. Type of stent Stent lumen (mm) Type of collection (n) Technical success (%) Puncture site (n)* Clinical success n (%) Complications (n) Fully covered biliary SEMS Talreja et al (2008) VIABIL 10 PFC 94% 17 (94%) Bleeding (2) Stent migration (1) Superinfection (5) Tarantino et al (2009) 37 1 Wallstent 10 WOPN 100% TD 1 (100%) Fabbri et al (2012) WallFlex/Niti-S 10 Abscess (6) PP (12) WOPN (2) Berzosa et al (2012) 39 7 VIABIL 10 PP (5) WOPN (2) 100% TG (12) TD (6) TG þ TD (2) 100% TG 7 (100%) 19 (95%) Superinfection (2) Stent migration (1) Surgical stent removal (1) Tarantino et al (2012) 42 1 Taewoong 8 PP 100% TG þ TD 1 (100%) Penn et al (2012) WallFlex 10 PP (20) 100% TG 17 (85%) Stent migration (3) Superinfection (2) Post-drainage fever (1) Weilert et al (2012) WallFlex 10 Abscess (8) 100% 14 (78%) Superinfection (3) Acute collection (7) PP (3) Partially covered biliary SEMS Barresi et al (2012) 44 1 Wallstent 10 PP 100% TG 1 (100%) Surgical stent removal (1) Nici et al (2012) 45 1 WallFlex 10 PP 100% TG 1 (100%) Other SEMS Antillon et al (2009) 47 1 Alimaxx-E Esophagus 22 WOPN 100% TG 1 (100%) Belle et al (2010) 48 4 Leufen WOPN (4) 100% TG (3) 1 (100%) TD (1) Perez-Miranda et al (2007) 46 4 Hanaro tracheal (2) Hanaro enteral (2) Abscess (1) WOPN (3) 100% TG 3 (75%) Piece-meal stent removal (1) Transmural SEMS Itoi et al (2012) AXIOS 15 PP (15) 100% TG (12) TD (3) Itoi et al (2012) 50 1 NAGI 16 WOPN 100% TG 1 (100%) Total /112 (99%) 99/112 (88%) 15 (100%) Stent migration (1) Oozing at stent removal (3) Gastrointestinal Intervention (1), PP, pancreatic pseudocyst; TD, transduodenal; TG, transgastric; WOPN, walled-off pancreatic necrosis.
4 Daisy Walter et al. / SEMS for transmural drainage 27 a direct comparison of studies not always being easy, although it is clear that adequate treatment of WOPN is much more challenging than draining PPs. 8,9 In larger series, the technical success rate of EUS-guided drainage of PPs ranges from 90% to 100%. Treatment success, defined as clinical improvement or complete resolution on imaging, is observed in >90% of patients. Complication rates range from 0% to 31%, and include bleeding, infection, pneumoperitoneum and stent-related complications, such as stent migration or occlusion. 4 The need for necrosectomy in addition to drainage alone, in most cases of (infected) WOPN, makes the treatment of this type of PFC more challenging. For endoscopic drainage alone, success rates as low as 25% have been reported. 4 A much higher resolution rate (76%) has been reported for WOPN treated with endoscopic necrosectomy. Furthermore, with a mortality rate of 5% and a morbidity rate of 30%, this can be considered as a relatively safe procedure. 34 SEMS To further improve endoscopic treatment of PFCs, SEMS have recently been used as an alternative for the traditionally used double-pigtail stents (Table 2). The use of plastic pigtail stents is limited by the small diameter of the stent lumen (7 10F). Several studies have shown that placement of multiple stents ensures a wider drainage opening, with a low risk of obstruction of the fistula tract, resulting in better clinical success rates. Furthermore, there is a reduced risk of stent migration, which also reduces the risk of premature closure of the fistula tract. 35,36 Since SEMS have a larger diameter (>10 mm), placement of a single SEMS can already provide a wide drainage opening. Furthermore, due to the larger stent lumen, there is a reduced risk of stent occlusion, especially for collections containing a significant amount of debris. As a result, complications due to stent occlusion, for example, infection of the PFC, are expected to be reduced. Lastly, SEMS can provide an enduring direct access route for endoscopic transmural necrosectomy. The use of different types of SEMS has been described in several case reports and small case series. Biliary SEMS Fully covered biliary SEMS with a 10 mm diameter, are the most frequently used SEMS for endoscopic drainage of PFCs. Experience with this type of stent has been reported in seven reports comprising 85 patients with PFCs All but two stent placements were performed under EUS-guidance and placement failed in one patient. To prevent migration of the fully covered stents, plastic pigtail stents were placed through or alongside the SEMS in 38 patients 40,43 and a plastic stent with flaps was placed through the stent in one patient. 42 Stent migration was reported in four (10%) patients with an anchoring stent to prevent migration, whereas only one (3%) stent migration was reported in patients without additional stents. Clinical success, defined as complete resolution of symptoms and resolution on imaging, was achieved in 76 of 85 patients (89%) In five of these, endoscopic necrostomy was performed before resolution was achieved. The SEMS was removed before necrosectomy and replaced by plastic pigtails after the procedure. 41 Surgery was required in the other patients to effectively control sepsis. 38,40,41,43 In one patient, endoscopic stent removal was not possible due to inflammatory tissue ingrowth, and surgical removal was indicated. 38 The use of partially covered biliary SEMS has been reported in two case reports. 44,45 Tissue ingrowth in the uncovered stent end was thought to reduce the risk of migration in these stents. However, severe tissue ingrowth may cause problems during stent removal. Barresi et al reported this as early as 1 month after placement of the SEMS. The stent was embedded in the gastric wall and completely covered by gastric mucosa, which was described as a buried stent. The stent was removed through a surgical procedure. 44 Nici et al did not experience any problems with removal of the partially covered SEMS 3 weeks after placement. 45 Other SEMS To provide an even wider drainage opening than with biliary SEMS, other types of SEMS have been used for PFC drainage. Perez- Miranda et al report on the use of a 15-mm covered tracheal SEMS (n ¼ 2) and a 18-mm covered enteral SEMS (n ¼ 2) for EUS-guided drainage of PFCs. Double pig-tail stents, and/or a nasocystic drain, were placed through the stent to reduce migration risk, although one stent migration was reported. Endoscopic irrigation and necrosectomy was performed through the lumen of the SEMS. Clinical success was seen in three of four patients (75%) while in one patient, the stent had to be removed in a piece-meal way. 46 A 22-mm esophageal SEMS with flared ends was used by Antillon at al to facilitate drainage in one patient. Previously placed doublepigtail plastic stents and a nasocystic drain were left in place alongside. With ongoing irrigation, symptom resolution was achieved within 2 weeks and all stents could easily be removed. 47 Belle et al reported their experiences with specially designed 18-mm to 25-mm partially covered SEMS in four patients. Subsequent endoscopic procedures, including necrosectomy and lavage, were performed through the stent. Resolution of symptoms was achieved in all patients and the partially covered SEMS were easily removed. 48 Dedicated transmural stents To overcome the limitations associated with the use of tubular SEMS for transmural drainage, such as migration and tissue ingrowth, novel drainage SEMS have been developed. Both the AXIOS stent (Xlumena Inc, Mountain View, CA, USA) and the NAGI stent (Taewoong Company, Seoul, Korea) are specifically developed for transmural drainage (Fig. 1). They both have a saddle-shape design, with bilateral flanges, and a stent length between those flanges of 10-mm and 20-mm, respectively. The flanges are designed to provide lumen-to-lumen anchoring, thereby reducing the risk of migration and leakage alongside the stent. Furthermore, both stents are fully covered to prevent tissue ingrowth and to enable easy removal. The diameter of the stents, 10-mm or 15-mm for the AXIOS stent and 16-mm for the NAGI-stent, enables direct necrosectomy through the lumen of the stent. Itoi et al 49 retrospectively reported on the use of the AXIOS stent in 15 patients with symptomatic PFCs. Stents were successfully placed in all patients and the stents were used as access portals for a diagnostic endoscope (<10 mm) to perform necrosectomy and irrigation. Dislodgement or removal of the stent during these interventions was not observed. However, stent migration to the stomach was reported in one patient. The cystogastrostomy tract in this patient was dilated up to 15-mm before placement of a 10-mm stent, which might be an explanation for migration. Resolution of the PFCs was achieved in all patients and stents could be removed without complications. The experience with the NAGI stent is limited to one case report, for drainage of an infected WOPN, also by Itoi et al. 50 Stent placement was performed using a transgastric approach. Necrosectomy was performed during two subsequent endoscopy sessions, whereby a standard upper endoscope was inserted through the stent. No complications were reported and the stent was easily removed after 3 weeks.
5 28 Gastrointestinal Intervention (1), Fig. 1. Dedicated transmural stents: the AXIOS-stent (Xlumena Inc, Mountain View, CA, USA) and the NAGI-stent (Taewoong Company, Seoul, Korea). Discussion The use of SEMS for EUS-guided drainage of PFCs seems promising, based on the overall clinical success rate of 88% and only one placement failure in the above mentioned studies. However, the available results to date are limited and need critical appraisal. First, the use of SEMS has been reported for drainage of both WOPN, containing significant amounts of necrotic debris, as well as for PPs. However, as for drainage of PPs with plastic stents, excellent clinical success rates have been reported, it remains to be established whether the use of SEMS has any added clinical value for this indication. Second, the use of SEMS is, in many cases, probably not costeffective, as they are far more expensive than plastic stents. It is thought, however, that the higher initial costs for SEMS will be offset by a reduction in the number of repeat endoscopies. This reduction will than probably be more distinctive for WOPN than for PPs. However, the number of repeat endoscopies is difficult to compare, since in some studies, necrosectomy and irrigation was performed at preset moments, whereas in other studies, repeat endoscopy was only performed based on clinical symptoms. Third, a wide variety of SEMS is currently available. Fully covered SEMS are the most commonly used stents, mainly since they have the lowest risk of tissue ingrowth. To prevent migration of the stent, some preventative measures can be used, including placement of double pigtail plastic stents in or alongside the stent, the use of stents with bilateral flares, or not performing dilation before stent placement. Also, partially covered SEMS have been used, as they are less prone to migration, which is thought to be due to tissue ingrowth at the uncovered stent ends. However, hyperplastic tissue ingrowth can also lead to significant problems during endoscopic removal, and in some cases, surgery is required. 44 In order to prevent tissue ingrowth as well as migration, dedicated SEMS for transmural drainage have been developed. However, even with these devices, stent migration has been reported as well. 49 Last, the studies that have been published on the use of SEMS for PFC drainage all have limitations, such as the inclusion of small numbers of patients, the lack of a control group, the use of different stent designs, the absence of preset endpoints, no long-term follow-up results, a retrospective design, etc. Well designed prospective studies and randomized trials are therefore needed to validate the initial promising results on the use of SEMS for endoscopic drainage of PFCs. A comparison should be made with conventional drainage using plastic stents and also a clear distinction should be made for the different types of PFCs, using well established criteria. Apart from the efficacy and safety, a cost analysis should be performed to elucidate whether the more expensive SEMS are indeed cost-effective, as compared to plastic stents, when used for the drainage of PFCs. Conflicts of interest P. D. Siersema serves as an advisor to Boston Scientific Corp., USA and receives research support from Cook Medical Ltd., Ireland. All other authors report that they have no disclosures relevant to this publication. References 1. Bradley III EL. A clinically based classification system for acute pancreatitis. Summary of the International Symposium on Acute Pancreatitis, Atlanta, Ga, September 11 through 13, Arch Surg. 1993;128: Baron TH, Thaggard WG, Morgan DE, Stanley RJ. Endoscopic therapy for organized pancreatic necrosis. Gastroenterology. 1996;111: Kloppel G. Pseudocysts and other non-neoplastic cysts of the pancreas. Semin Diagn Pathol. 2000;17: Seewald S, Ang TL, Kida M, Teng KY, Soehendra N. EUS 2008 Working Group document: evaluation of EUS-guided drainage of pancreatic-fluid collections (with video). Gastrointest Endosc. 2009;69(Suppl 2):S Bollen TL, Besselink MG, van Santvoort HC, Gooszen HG, van Leeuwen MS. Toward an update of the Atlanta classification on acute pancreatitis: review of new and abandoned terms. Pancreas. 2007;35: Bollen TL, van Santvoort HC, Besselink MG, van Leeuwen MS, Horvath KD, Freeny PC, et al. The Atlanta classification of acute pancreatitis revisited. Br J Surg. 2008;95: Acute Pancreatitis Classification Working Group. Revision of the Atlanta classification of acute pancreatitis (3rd revision); Baron TH, Harewood GC, Morgan DE, Yates MR. Outcome differences after endoscopic drainage of pancreatic necrosis, acute pancreatic pseudocysts, and chronic pancreatic pseudocysts. Gastrointest Endosc. 2002;56: Hookey LC, Debroux S, Delhaye M, Arvanitakis M, Le MO, Deviere J. Endoscopic drainage of pancreatic-fluid collections in 116 patients: a comparison of etiologies, drainage techniques, and outcomes. Gastrointest Endosc. 2006;63: Beckingham IJ, Krige JE, Bornman PC, Terblanche J. Long term outcome of endoscopic drainage of pancreatic pseudocysts. Am J Gastroenterol. 1999;94: Banks PA, Bollen TL, Dervenis C, Gooszen HG, Johnson CD, Sarr MG, et al. Classification of acute pancreatitis 2012: Revision of the Atlanta classification and definitions by international consensus. Gut. 2013;62: Thoeni RF. The revised Atlanta classification of acute pancreatitis: its importance for the radiologist and its effect on treatment. Radiology. 2012;262: Seewald S, Ang TL, Teng KC, Soehendra N. EUS-guided drainage of pancreatic pseudocysts, abscesses and infected necrosis. Dig Endosc. 2009;21(Suppl 1): S Baron TH. Endoscopic drainage of pancreatic fluid collections and pancreatic necrosis. Gastrointest Endosc Clin N Am. 2003;13: Warshaw AL, Rattner DW. Timing of surgical drainage for pancreatic pseudocyst. Clinical and chemical criteria. Ann Surg. 1985;202: Sahel J, Bastid C, Pellat B, Schurgers P, Sarles H. Endoscopic cystoduodenostomy of cysts of chronic calcifying pancreatitis: a report of 20 cases. Pancreas. 1987; 2: Cremer M, Deviere J, Engelholm L. Endoscopic management of cysts and pseudocysts in chronic pancreatitis: long-term follow-up after 7 years of experience. Gastrointest Endosc. 1989;35: Bergman S, Melvin WS. Operative and nonoperative management of pancreatic pseudocysts. Surg Clin North Am. 2007;87: ix. 19. Bhattacharya D, Ammori BJ. Minimally invasive approaches to the management of pancreatic pseudocysts: review of the literature. Surg Laparosc Endosc Percutan Tech. 2003;13:141 8.
6 Daisy Walter et al. / SEMS for transmural drainage Varadarajulu S, Lopes TL, Wilcox CM, Drelichman ER, Kilgore ML, Christein JD. EUS versus surgical cyst-gastrostomy for management of pancreatic pseudocysts. Gastrointest Endosc. 2008;68: van BS, Bakker OJ, Besselink MG, Bollen TL, Fockens P, Gooszen HG, et al. Treatment of necrotizing pancreatitis. Clin Gastroenterol Hepatol. 2012;10: Werner J, Feuerbach S, Uhl W, Buchler MW. Management of acute pancreatitis: from surgery to interventional intensive care. Gut. 2005;54: Bakker OJ, van Santvoort HC, van BS, Geskus RB, Besselink MG, Bollen TL, et al. Endoscopic transgastric vs surgical necrosectomy for infected necrotizing pancreatitis: a randomized trial. JAMA. 2012;307: van Santvoort HC, Bakker OJ, Bollen TL, Besselink MG, Ahmed AU, Schrijver AM, et al. A conservative and minimally invasive approach to necrotizing pancreatitis improves outcome. Gastroenterology. 2011;141: van Baal MC, van Santvoort HC, Bollen TL, Bakker OJ, Besselink MG, Gooszen HG. Systematic review of percutaneous catheter drainage as primary treatment for necrotizing pancreatitis. Br J Surg. 2011;98: Bradley III EL, Howard TJ, van SE, Fotoohi M. Intervention in necrotizing pancreatitis: an evidence-based review of surgical and percutaneous alternatives. J Gastrointest Surg. 2008;12: van Santvoort HC, Besselink MG, Bakker OJ, Hofker HS, Boermeester MA, Dejong CH, et al. A step-up approach or open necrosectomy for necrotizing pancreatitis. N Engl J Med. 2010;362: Kahaleh M, Shami VM, Conaway MR, Tokar J, Rockoff T, De La Rue SA, et al. Endoscopic ultrasound drainage of pancreatic pseudocyst: a prospective comparison with conventional endoscopic drainage. Endoscopy. 2006;38: Baron TH. Drainage of pancreatic fluid collections: is EUS really necessary? Gastrointest Endosc. 2007;66: Fockens P, Johnson TG, van Dullemen HM, Huibregtse K, Tytgat GN. Endosonographic imaging of pancreatic pseudocysts before endoscopic transmural drainage. Gastrointest Endosc. 1997;46: Varadarajulu S, Christein JD, Tamhane A, Drelichman ER, Wilcox CM. Prospective randomized trial comparing EUS and EGD for transmural drainage of pancreatic pseudocysts (with videos). Gastrointest Endosc. 2008;68: Park DH, Lee SS, Moon SH, Choi SY, Jung SW, Seo DW, et al. Endoscopic ultrasound-guided versus conventional transmural drainage for pancreatic pseudocysts: a prospective randomized trial. Endoscopy. 2009;41: Sanchez CE, Maalak A, Le MO, Baize M, Delhaye M, Matos C, et al. Endoscopic cystenterostomy of nonbulging pancreatic fluid collections. Gastrointest Endosc. 2002;56: Haghshenasskashani A, Laurence JM, Kwan V, Johnston E, Hollands MJ, Richardson AJ, et al. Endoscopic necrosectomy of pancreatic necrosis: a systematic review. Surg Endosc. 2011;25: Cahen D, Rauws E, Fockens P, Weverling G, Huibregtse K, Bruno M. Endoscopic drainage of pancreatic pseudocysts: long-term outcome and procedural factors associated with safe and successful treatment. Endoscopy. 2005;37: Voermans RP, Ponchon T, Schumacher B, Fumex F, Bergman JJ, Larghi A, et al. Forward-viewing versus oblique-viewing echoendoscopes in transluminal drainage of pancreatic fluid collections: a multicenter, randomized, controlled trial. Gastrointest Endosc. 2011;74: Tarantino I, Barresi L, Fazio V, Di PM, Traina M. EUS-guided self-expandable stent placement in 1 step: a new method to treat pancreatic abscess. Gastrointest Endosc. 2009;69: Fabbri C, Luigiano C, Cennamo V, Polifemo AM, Barresi L, Jovine E, et al. Endoscopic ultrasound-guided transmural drainage of infected pancreatic fluid collections with placement of covered self-expanding metal stents: a case series. Endoscopy. 2012;44: Berzosa M, Maheshwari S, Patel KK, Shaib YH. Single-step endoscopic ultrasonography-guided drainage of peripancreatic fluid collections with a single self-expandable metal stent and standard linear echoendoscope. Endoscopy. 2012;44: Penn DE, Draganov PV, Wagh MS, Forsmark CE, Gupte AR, Chauhan SS. Prospective evaluation of the use of fully covered self-expanding metal stents for EUS-guided transmural drainage of pancreatic pseudocysts. Gastrointest Endosc. 2012;76: Weilert F, Binmoeller KF, Shah JN, Bhat YM, Kane S. Endoscopic ultrasoundguided drainage of pancreatic fluid collections with indeterminate adherence using temporary covered metal stents. Endoscopy. 2012;44: Tarantino I, Di PM, Barresi L, Curcio G, Granata A, Traina M. Covered self expandable metallic stent with flared plastic one inside for pancreatic pseudocyst avoiding stent dislodgement. World J Gastrointest Endosc. 2012;4: Talreja JP, Shami VM, Ku J, Morris TD, Ellen K, Kahaleh M. Transenteric drainage of pancreatic-fluid collections with fully covered self-expanding metallic stents (with video). Gastrointest Endosc. 2008;68: Barresi L, Tarantino I, Curcio G, Granata A, Traina M. Buried stent: new complication of pseudocyst drainage with self-expandable metallic stent. Dig Endosc. 2012;24: Nici AJ, Hussain SA, Kim SH, Mehta P. Unique usage of a partially covered metal stent for drainage of a pancreatic pseudocyst via endosonography-guided transcystgastrostomy. Dig Endosc. 2012;24: Perez-Miranda M, Mata L, Saracibar E, Sanchez-Antolin G, Barrio J, Caro- Paton A. Temporary access fistulas (TAFs) using covered self-expandable metal stents (csems): a feasible tool for interventional pancreaticobiliary endoscopy (abstract). Gastrointest Endosc. 2007;65. AB Antillon MR, Bechtold ML, Bartalos CR, Marshall JB. Transgastric endoscopic necrosectomy with temporary metallic esophageal stent placement for the treatment of infected pancreatic necrosis (with video). Gastrointest Endosc. 2009;69: Belle S, Collet P, Post S, Kaehler G. Temporary cystogastrostomy with selfexpanding metallic stents for pancreatic necrosis. Endoscopy. 2010;42: Itoi T, Binmoeller KF, Shah J, Sofuni A, Itokawa F, Kurihara T. Clinical evaluation of a novel lumen-apposing metal stent for endosonography-guided pancreatic pseudocyst and gallbladder drainage (with videos). Gastrointest Endosc. 2012; 75: Itoi T, Reddy DN, Yasuda I. New fully-covered self-expandable metal stent for endoscopic ultrasonography-guided intervention in infectious walled-off pancreatic necrosis (with video). J Hepatobiliary Pancreat Sci. 2013;20:403 6.
Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections
 REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 1-6 Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections Rashmee Patil a, Mel A. Ona b, Charilaos Papafragkakis
REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 1-6 Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections Rashmee Patil a, Mel A. Ona b, Charilaos Papafragkakis
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Mild. Moderate. Severe
 2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
Original Article INTRODUCTION
 Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Endoscopic Ultrasound-Guided Transluminal Drainage for Peripancreatic Fluid Collections: Where Are We Now?
 Gut and Liver, Vol. 8, No. 4, July 2014, pp. 341-355 Review Endoscopic Ultrasound-Guided Transluminal Drainage for Peripancreatic Fluid Collections: Where Are We Now? Hiroshi Kawakami*, Takao Itoi, and
Gut and Liver, Vol. 8, No. 4, July 2014, pp. 341-355 Review Endoscopic Ultrasound-Guided Transluminal Drainage for Peripancreatic Fluid Collections: Where Are We Now? Hiroshi Kawakami*, Takao Itoi, and
Safety and Efficacy of Endoscopic Ultrasound-Guided Drainage of Pancreatic Fluid Collections With Lumen-Apposing Covered Self-Expanding Metal Stents
 All studies published in Clinical Gastroenterology and Hepatology are embargoed until 3PM ET of the day they are published as corrected proofs on-line. Studies cannot be publicized as accepted manuscripts
All studies published in Clinical Gastroenterology and Hepatology are embargoed until 3PM ET of the day they are published as corrected proofs on-line. Studies cannot be publicized as accepted manuscripts
Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection
 Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Does it matter what we drain?
 Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Endoscopic Management of Acute Pancreatitis. Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018
 Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal Extension
 Gut and Liver, Vol. 4, No. 1, March 2010, pp. 140-145 Case report EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal
Gut and Liver, Vol. 4, No. 1, March 2010, pp. 140-145 Case report EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Endosonography guided management of pancreatic fluid collections
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i41.11842 World J Gastroenterol 2015 November 7; 21(41): 11842-11853 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i41.11842 World J Gastroenterol 2015 November 7; 21(41): 11842-11853 ISSN 1007-9327
Review Article Fully Covered Self-Expandable Metal Stents for Treatment of Both Benign and Malignant Biliary Disorders
 Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
Endoscopic ultrasound guided gastrojejunostomy
 Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
VIDEO ASSISTED RETROPERITONEAL DEBRIDEMENT IN HUGE INFECTED PANCREATIC PSEUDOCYST
 Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Endoscopic ultrasonography-guided endoscopic treatment. treatment of pancreatic pseudocysts and walled-off necrosis:
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i43.16191 World J Gastroenterol 2014 November 21; 20(43): 16191-16196 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i43.16191 World J Gastroenterol 2014 November 21; 20(43): 16191-16196 ISSN 1007-9327
Sepsis in Acute Pancreatitis. MD Smith Department of Surgery University of the Witwatersrand, Johannesburg Chris Hani Baragwanath Academic Hospital
 Sepsis in Acute Pancreatitis MD Smith Department of Surgery University of the Witwatersrand, Johannesburg Chris Hani Baragwanath Academic Hospital Introduction Self limiting disease in 85% Minority develop
Sepsis in Acute Pancreatitis MD Smith Department of Surgery University of the Witwatersrand, Johannesburg Chris Hani Baragwanath Academic Hospital Introduction Self limiting disease in 85% Minority develop
AXIOS Stent and Delivery System
 PRESCRIPTIVE INFORMATION AXIOS Stent and Delivery System Warning REFER TO THE DEVICE DIRECTIONS FOR USE FOR COMPLETE INSTRUCTIONS ON DEVICE USE. RX ONLY. CAUTION: FEDERAL LAW (USA) RESTRICTS THIS DEVICE
PRESCRIPTIVE INFORMATION AXIOS Stent and Delivery System Warning REFER TO THE DEVICE DIRECTIONS FOR USE FOR COMPLETE INSTRUCTIONS ON DEVICE USE. RX ONLY. CAUTION: FEDERAL LAW (USA) RESTRICTS THIS DEVICE
U Nordic Forum - Trauma & Emergency Radiology. Lecture Objectives. MDCT in Acute Pancreatitis. Acute Pancreatitis: Etiologies
 Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
The first stents designed for use in the biliary tree and
 Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm
 Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
efficacy. Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience
 E76 THIEME Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience Authors Institutions Amy Tyberg, Manuel Perez-Miranda, Ramon Sanchez-Ocaña,
E76 THIEME Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience Authors Institutions Amy Tyberg, Manuel Perez-Miranda, Ramon Sanchez-Ocaña,
and Transmural Drainage
 HPB Surgery, 2000, Vol. 11, pp. 333-338 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
HPB Surgery, 2000, Vol. 11, pp. 333-338 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report
 CASE REPORT Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report Rodrigo Azevedo Rodrigues, Lucianna Pereira da Motta Pires Correia,
CASE REPORT Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report Rodrigo Azevedo Rodrigues, Lucianna Pereira da Motta Pires Correia,
Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents
 REVIEW ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents Alessandro Mussetto a, Alessandro Fugazza b, Lorenzo
REVIEW ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents Alessandro Mussetto a, Alessandro Fugazza b, Lorenzo
EUS- Gallbladder Drainage: is it time to replace percutaneous drainage?
 EUS- Gallbladder Drainage: is it time to replace percutaneous drainage? Jessica Widmer, DO 1, Juveria Abdullah 1, Michel Kahaleh, MD. 1 Division of Gastroenterology and Hepatology, Department of Medicine,
EUS- Gallbladder Drainage: is it time to replace percutaneous drainage? Jessica Widmer, DO 1, Juveria Abdullah 1, Michel Kahaleh, MD. 1 Division of Gastroenterology and Hepatology, Department of Medicine,
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
AXIOS Stent and Electrocautery Enhanced Delivery System *
 Advancing Pancreaticobiliary Disease Management AXIOS Stent and Electrocautery Enhanced Delivery System * Select a Menu Option Below Features & Benefits Expanding Innovation Ordering Information & Resources
Advancing Pancreaticobiliary Disease Management AXIOS Stent and Electrocautery Enhanced Delivery System * Select a Menu Option Below Features & Benefits Expanding Innovation Ordering Information & Resources
Updated Imaging Nomenclature for Acute Pancreatitis
 Residents Section Structured Review Murphy et al. Imaging Nomenclature for Acute Pancreatitis Residents Section Structured Review Residents inradiology Kevin P. Murphy 1,2 Owen J. O Connor 1,2 Michael
Residents Section Structured Review Murphy et al. Imaging Nomenclature for Acute Pancreatitis Residents Section Structured Review Residents inradiology Kevin P. Murphy 1,2 Owen J. O Connor 1,2 Michael
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures
 E96 THIEME Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures Authors Institution Shounak Majumder, Navtej S. Buttar, Christopher Gostout, Michael J.
E96 THIEME Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures Authors Institution Shounak Majumder, Navtej S. Buttar, Christopher Gostout, Michael J.
Colorectal stenting. Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy
 Colorectal stenting Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Metal Stents for Obstructing Colorectal Cancer Dohomoto was credited as the first to report
Colorectal stenting Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Metal Stents for Obstructing Colorectal Cancer Dohomoto was credited as the first to report
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Transluminal endoscopic necrosectomy after acute pancreatitis: a multicentre study with long-term follow-up (the GEPARD Study)
 See Commentary, p 1180 1 Department of Internal Medicine, Oldenburg Municipal Hospital, Oldenburg, Germany; 2 Central Interdisciplinary Endoscopy Unit, Department of Gastroenterology, Charité Medical University
See Commentary, p 1180 1 Department of Internal Medicine, Oldenburg Municipal Hospital, Oldenburg, Germany; 2 Central Interdisciplinary Endoscopy Unit, Department of Gastroenterology, Charité Medical University
Electrocautery vs non-electrocautery dilation catheters in endoscopic ultrasonography-guided pancreatic fluid collection drainage
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4253/wjge.v8.i13.458 World J Gastrointest Endosc 2016 July 10; 8(13): 458-465 ISSN 1948-5190
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4253/wjge.v8.i13.458 World J Gastrointest Endosc 2016 July 10; 8(13): 458-465 ISSN 1948-5190
Therapeutic EUS: today & tomorrow Pietro Fusaroli
 Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Keywords. Abstract. Introduction
 The Safety of Endoscopic Ultrasonography-Guided Drainage of Pancreatic Fluid Collections Without Fluoroscopic Control: a Single Tertiary Center Experience Andrada Seicean 1, Roxana Stan-Iuga 1, Radu Badea
The Safety of Endoscopic Ultrasonography-Guided Drainage of Pancreatic Fluid Collections Without Fluoroscopic Control: a Single Tertiary Center Experience Andrada Seicean 1, Roxana Stan-Iuga 1, Radu Badea
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance for Extraluminal Complicated Cysts
 Gastroenterology Research and Practice Volume 2016, Article ID 1249064, 8 pages http://dx.doi.org/10.1155/2016/1249064 Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance
Gastroenterology Research and Practice Volume 2016, Article ID 1249064, 8 pages http://dx.doi.org/10.1155/2016/1249064 Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance
EUS-guided cholecystoduodenostomy for acute cholecystitis with an anti-stent migration and anti-food impaction system; a pilot study
 609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Robotic transgastric cystgastrostomy and pancreatic debridement in the management of pancreatic fluid collections following acute pancreatitis
 Review Article on Pancreatic Surgery Robotic transgastric cystgastrostomy and pancreatic debridement in the management of pancreatic fluid collections following acute pancreatitis Russell C. Kirks Jr,
Review Article on Pancreatic Surgery Robotic transgastric cystgastrostomy and pancreatic debridement in the management of pancreatic fluid collections following acute pancreatitis Russell C. Kirks Jr,
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) Endosonographic imaging of pancreatic pseudocysts before endoscopic transmural drainage Fockens, P.; Johnson, T.G.; van Dullemen, H.M.; Huibregtse, K.; Tytgat, G.N.J.
UvA-DARE (Digital Academic Repository) Endosonographic imaging of pancreatic pseudocysts before endoscopic transmural drainage Fockens, P.; Johnson, T.G.; van Dullemen, H.M.; Huibregtse, K.; Tytgat, G.N.J.
Endoscopic ultrasound-guided drainage of postoperative intra-abdominal abscesses
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i11.3402 World J Gastroenterol 2015 March 21; 21(11): 3402-3408 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i11.3402 World J Gastroenterol 2015 March 21; 21(11): 3402-3408 ISSN 1007-9327
Comparative evaluation of structural and functional changes in pancreas after endoscopic and surgical management of pancreatic necrosis
 ORIGINAL ARTICLE Annals of Gastroenterology (2014) 27, 162-166 Comparative evaluation of structural and functional changes in pancreas after endoscopic and surgical management of pancreatic necrosis Surinder
ORIGINAL ARTICLE Annals of Gastroenterology (2014) 27, 162-166 Comparative evaluation of structural and functional changes in pancreas after endoscopic and surgical management of pancreatic necrosis Surinder
Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W.
 UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE. T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar
 ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice
 CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY?
 Endoscopy 2006 Update and Live Demonstration Berlin, 04. 05. Mai 2006 CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY? J. F. Riemann A. Rosenbaum Medizinische Klinik C, Klinikum Ludwigshafen
Endoscopy 2006 Update and Live Demonstration Berlin, 04. 05. Mai 2006 CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY? J. F. Riemann A. Rosenbaum Medizinische Klinik C, Klinikum Ludwigshafen
Hui-Yun Zhu 1, Pei Xie 1,2, Ying-Xiao Song 1, Zhao-Shen Li 1,2,3,4*, Zhen-Dong Jin 1,2,3,4* and Yi-Qi Du 1,2,3,4*
 Zhu et al. Trials (2018) 19:549 https://doi.org/10.1186/s13063-018-2901-3 STUDY PROTOCOL Open Access Lumen-apposing metal stents (LAMS) versus plastic stents for EUS-guided drainage of walled-off necrosis
Zhu et al. Trials (2018) 19:549 https://doi.org/10.1186/s13063-018-2901-3 STUDY PROTOCOL Open Access Lumen-apposing metal stents (LAMS) versus plastic stents for EUS-guided drainage of walled-off necrosis
Recurrence of Pancreatic Pseudocyst following Endoscopic Ultrasonography-Guided Drainage
 Shimane J. Med. Sci., Vol.34 pp.73-80, 2017 73 Recurrence of Pancreatic Pseudocyst following Endoscopic Ultrasonography-Guided Drainage Ahmed SELIM 1,2), Nobuhiko FUKUBA 1), Ichiro MORIYAMA 3), Hiroki
Shimane J. Med. Sci., Vol.34 pp.73-80, 2017 73 Recurrence of Pancreatic Pseudocyst following Endoscopic Ultrasonography-Guided Drainage Ahmed SELIM 1,2), Nobuhiko FUKUBA 1), Ichiro MORIYAMA 3), Hiroki
A multi institutional consensus on how to perform endoscopic ultrasound-guided peri-pancreatic fluid collection drainage and endoscopic necrosectomy
 Consensus A multi institutional consensus on how to perform endoscopic ultrasound-guided peri-pancreatic fluid collection drainage and endoscopic necrosectomy Jintao Guo, Adrian Saftoiu 1, Peter Vilmann
Consensus A multi institutional consensus on how to perform endoscopic ultrasound-guided peri-pancreatic fluid collection drainage and endoscopic necrosectomy Jintao Guo, Adrian Saftoiu 1, Peter Vilmann
Title. CitationSurgical Endoscopy, 26(6): Issue Date Doc URL. Rights. Type. File Information. surgery
 Title Endoscopic ultrasound-guided transmural drainage for surgery Onodera, Manabu; Kawakami, Hiroshi; Kuwatani, Masaki Author(s) Eto, Kazunori; Nasu, Yuya; Tanaka, Eiichi; Hirano, S CitationSurgical Endoscopy,
Title Endoscopic ultrasound-guided transmural drainage for surgery Onodera, Manabu; Kawakami, Hiroshi; Kuwatani, Masaki Author(s) Eto, Kazunori; Nasu, Yuya; Tanaka, Eiichi; Hirano, S CitationSurgical Endoscopy,
JMSCR Volume 03 Issue 01 Page January 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Pancreatic Pseudocyst: A Surgical Dilemma Authors Dr. Ketan Vagholkar 1, Dr. Madhavan Iyengar 2, Dr. Rahulkumar Chavan 3 Dr. Abhishek
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Pancreatic Pseudocyst: A Surgical Dilemma Authors Dr. Ketan Vagholkar 1, Dr. Madhavan Iyengar 2, Dr. Rahulkumar Chavan 3 Dr. Abhishek
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Best of UEG week 2017 (Pancreas-biliary)
 Best of UEG week 2017 (Pancreas-biliary) Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Best of UEG week 2017 (Pancreas-biliary) Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Enteral stenting for gastric outlet obstruction and afferent limb syndrome following pancreaticoduodenectomy
 CASE SERIES Annals of Gastroenterology (2014) 27, 1-5 Enteral stenting for gastric outlet obstruction and afferent limb syndrome following pancreaticoduodenectomy Wilson T. Kwong a, Syed M. Fehmi a, Andrew
CASE SERIES Annals of Gastroenterology (2014) 27, 1-5 Enteral stenting for gastric outlet obstruction and afferent limb syndrome following pancreaticoduodenectomy Wilson T. Kwong a, Syed M. Fehmi a, Andrew
Overview. Doumit S. BouHaidar, MD ACG/VGS/ODSGNA Regional Postgraduate Course Copyright American College of Gastroenterology 1
 Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction
 Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
Original Article. Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome
 Tropical Gastroenterology 2015;36(1):31 35 Original Article Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome Surinder S Rana 1, Vishal Sharma 1, Deepak
Tropical Gastroenterology 2015;36(1):31 35 Original Article Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome Surinder S Rana 1, Vishal Sharma 1, Deepak
CURRICULUM VITAE
 CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
Endoscopic versus percutaneous drainage of symptomatic pancreatic fluid collections: a 14-year experience from a tertiary hepatobiliary centre
 Surg Endosc (2016) 30:3730 3740 DOI 10.1007/s00464-015-4668-x and Other Interventional Techniques Endoscopic versus percutaneous drainage of symptomatic pancreatic fluid collections: a 14-year experience
Surg Endosc (2016) 30:3730 3740 DOI 10.1007/s00464-015-4668-x and Other Interventional Techniques Endoscopic versus percutaneous drainage of symptomatic pancreatic fluid collections: a 14-year experience
Optimizing the step-up approach for infected necrotizing pancreatitis van Grinsven, A.H.J.
 UvA-DARE (Digital Academic Repository) Optimizing the step-up approach for infected necrotizing pancreatitis van Grinsven, A.H.J. Link to publication Citation for published version (APA): van Grinsven,
UvA-DARE (Digital Academic Repository) Optimizing the step-up approach for infected necrotizing pancreatitis van Grinsven, A.H.J. Link to publication Citation for published version (APA): van Grinsven,
BILIARY CANNULATION FOR the treatment of biliary
 Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Jennifer Hsieh 1, Amar Thosani 1, Matthew Grunwald 2, Satish Nagula 1, Juan Carlos Bucobo 1, Jonathan M. Buscaglia 1. Introduction
 How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Endoscopic transluminal drainage of pancreatic pseudocyst and pancreatic necrosectomy Removing dead tissue from
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Endoscopic transluminal drainage of pancreatic pseudocyst and pancreatic necrosectomy Removing dead tissue from
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal Stent for Acute Cholecystitis: A Systematic Review
 REVIEW Clin Endosc 2018;51:450-462 https://doi.org/10.5946/ce.2018.024 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal
REVIEW Clin Endosc 2018;51:450-462 https://doi.org/10.5946/ce.2018.024 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal
ORIGINAL ARTICLE: Clinical Endoscopy
 ORIGINAL ARTICLE: Clinical Endoscopy Anchoring flap versus flared end, fully covered self-expandable metal stents to prevent migration in patients with benign biliary strictures: a multicenter, prospective,
ORIGINAL ARTICLE: Clinical Endoscopy Anchoring flap versus flared end, fully covered self-expandable metal stents to prevent migration in patients with benign biliary strictures: a multicenter, prospective,
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
ESPEN Congress Brussels Stenting of the esophagus and small bowel. Jean-Marc Dumonceau
 ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
Hajhamad M 1, Reynu R, Kosai NR, Mustafa MT, Othman H 2
 Successful conservative management of pancreatico-colonic fistula following videoscopic assisted retroperitoneal debridement of infected pancreatic necrosis. Case report and review of literature. Hajhamad
Successful conservative management of pancreatico-colonic fistula following videoscopic assisted retroperitoneal debridement of infected pancreatic necrosis. Case report and review of literature. Hajhamad
Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic Duct Obstruction: Is Endoscopic Sphincterotomy Needed?
 Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Endoscopic management of sleeve leaks
 Endoscopic management of sleeve leaks Mr Damien Loh Oesophagogastric and Bariatric Surgeon The Alfred The clinical problem Incidence 0.1-7% Inpatient mortality 2-5% High morbidity Prolonged ICU and in-hospital
Endoscopic management of sleeve leaks Mr Damien Loh Oesophagogastric and Bariatric Surgeon The Alfred The clinical problem Incidence 0.1-7% Inpatient mortality 2-5% High morbidity Prolonged ICU and in-hospital
The Use of Double Lasso, Fully Covered Self-Expandable Metal Stents with New Anchoring Flap System in the Treatment of Benign Biliary Diseases
 DOI 10.1007/s10620-014-3158-7 ORIGINAL ARTICLE The Use of Double Lasso, Fully Covered Self-Expandable Metal Stents with New Anchoring Flap System in the Treatment of Benign Biliary Diseases B. Mangiavillano
DOI 10.1007/s10620-014-3158-7 ORIGINAL ARTICLE The Use of Double Lasso, Fully Covered Self-Expandable Metal Stents with New Anchoring Flap System in the Treatment of Benign Biliary Diseases B. Mangiavillano
Endoscopic Ultrasound-Guided Fine Needle Aspiration Used for the Diagnosis of a Retroperitoneal Abscess. A Case Report
 EUS guided fine needle aspiration of a retroperitoneal abscess CASE REPORTS Endoscopic Ultrasound-Guided Fine Needle Aspiration Used for the Diagnosis of a Retroperitoneal Abscess. A Case Report Adrian
EUS guided fine needle aspiration of a retroperitoneal abscess CASE REPORTS Endoscopic Ultrasound-Guided Fine Needle Aspiration Used for the Diagnosis of a Retroperitoneal Abscess. A Case Report Adrian
The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis. William H. Nealon M.D.
 The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis William H. Nealon M.D. Students and Trainees: Guide to Creativity, Productivity and Innovation in a Clinical Career Choose
The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis William H. Nealon M.D. Students and Trainees: Guide to Creativity, Productivity and Innovation in a Clinical Career Choose
International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches
 E175 International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches Authors Mouen A. Khashab 1, Ahmed A. Messallam 1,
E175 International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches Authors Mouen A. Khashab 1, Ahmed A. Messallam 1,
Pi Liu *, Jun Song, Hua-jing Ke, Nong-hua Lv, Yin Zhu, Hao Zeng, Yong Zhu, Liang Xia, Wen-hua He, Ji Li, Xin Huang and Yu-peng Lei
 Liu et al. BMC Gastroenterology (2017) 17:155 DOI 10.1186/s12876-017-0717-3 TECHNICAL ADVANCE Open Access Double-catheter lavage combined with percutaneous flexible endoscopic debridement for infected
Liu et al. BMC Gastroenterology (2017) 17:155 DOI 10.1186/s12876-017-0717-3 TECHNICAL ADVANCE Open Access Double-catheter lavage combined with percutaneous flexible endoscopic debridement for infected
Introduction E1111. Background and study aim Gallbladder drainage in patients
 Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis with a silicone-covered nitinol short bilaterally flared stent: a case series Authors Raffaele Manta 1, Claudio Zulli 2,AngeloZullo
Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis with a silicone-covered nitinol short bilaterally flared stent: a case series Authors Raffaele Manta 1, Claudio Zulli 2,AngeloZullo
Slide 1. Slide 2. Slide 3 Pancreatic Cancer- Case #1. Endoscopic management of GI malignancy. Endoscopic approaches in GI malignancy- Agenda
 Slide 1 A teaching hospital of Harvard Medical School Endoscopic management of GI malignancy Tyler Berzin MD, MS Center for Advanced Endoscopy Division of Gastroenterology Beth Israel Deaconess Medical
Slide 1 A teaching hospital of Harvard Medical School Endoscopic management of GI malignancy Tyler Berzin MD, MS Center for Advanced Endoscopy Division of Gastroenterology Beth Israel Deaconess Medical
Jintao Guo, Siyu Sun, Xiang Liu, Sheng Wang, Nan Ge, and Guoxin Wang. 1. Introduction. 2. Patients and Methods
 Gastroenterology Research and Practice Volume 2016, Article ID 9469472, 6 pages http://dx.doi.org/10.1155/2016/9469472 Clinical Study Endoscopic Ultrasound-Guided Biliary Drainage Using a Fully Covered
Gastroenterology Research and Practice Volume 2016, Article ID 9469472, 6 pages http://dx.doi.org/10.1155/2016/9469472 Clinical Study Endoscopic Ultrasound-Guided Biliary Drainage Using a Fully Covered
Lumen-apposing metal stents for gastrointestinal luminal strictures: current use and future directions
 REVIEW ARTICLE Annals of Gastroenterology (2019) 32, 1-6 Lumen-apposing metal stents for gastrointestinal luminal strictures: current use and future directions Brian Larson, Douglas G. Adler University
REVIEW ARTICLE Annals of Gastroenterology (2019) 32, 1-6 Lumen-apposing metal stents for gastrointestinal luminal strictures: current use and future directions Brian Larson, Douglas G. Adler University
Necrotizing Pancreatitis: Current Management and Therapies
 REVIEW Clin Endosc 2017;50:357-365 https://doi.org/10.5946/ce.2016.152 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Necrotizing Pancreatitis: Current Management and Therapies Christine Boumitri
REVIEW Clin Endosc 2017;50:357-365 https://doi.org/10.5946/ce.2016.152 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Necrotizing Pancreatitis: Current Management and Therapies Christine Boumitri
Endoscopic Management of Perforations
 Endoscopic Management of Perforations Gregory G. Ginsberg, MD Professor of Medicine University of Pennsylvania Perelman School of Medicine Gastroenterology Division Executive Director of Endoscopic Services
Endoscopic Management of Perforations Gregory G. Ginsberg, MD Professor of Medicine University of Pennsylvania Perelman School of Medicine Gastroenterology Division Executive Director of Endoscopic Services
EXPERIMENTAL AND THERAPEUTIC MEDICINE 14: , 2017
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 14: 4397-4404, 2017 Predictive factors of pancreatic necrosectomy following percutaneous catheter drainage as a primary treatment of patients with infected necrotizing
EXPERIMENTAL AND THERAPEUTIC MEDICINE 14: 4397-4404, 2017 Predictive factors of pancreatic necrosectomy following percutaneous catheter drainage as a primary treatment of patients with infected necrotizing
Gastrointestinal Intervention
 Gastrointest Interv 2012; 1:11 18 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided
Gastrointest Interv 2012; 1:11 18 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided
Endoscopic Ultrasound-Guided Pancreatic Duct Intervention
 FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
Author's response to reviews
 Author's response to reviews Title: Fully covered self-expandable metal stents (SEMS), partially covered SEMS and self-expandable plastic stents for the treatment of benign esophageal ruptures and anastomotic
Author's response to reviews Title: Fully covered self-expandable metal stents (SEMS), partially covered SEMS and self-expandable plastic stents for the treatment of benign esophageal ruptures and anastomotic
Endoscopic ultrasound criteria to predict the need for intervention in pancreatic necrosis
 Jürgensen et al. BMC Gastroenterology 2012, 12:48 RESEARCH ARTICLE Endoscopic ultrasound criteria to predict the need for intervention in pancreatic necrosis Open Access Christian Jürgensen 1*, Alexander
Jürgensen et al. BMC Gastroenterology 2012, 12:48 RESEARCH ARTICLE Endoscopic ultrasound criteria to predict the need for intervention in pancreatic necrosis Open Access Christian Jürgensen 1*, Alexander
Double Bypass Surgery vs Endotherapy for Irresectable Pancreatic Cancer
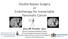 Double Bypass Surgery vs Endotherapy for Irresectable Pancreatic Cancer Jones AO Omoshoro-Jones General & Hepatopancreatobiliary Surgery Chris Hani-Baragwanath Academic Hospital Faculty of Health Sciences,
Double Bypass Surgery vs Endotherapy for Irresectable Pancreatic Cancer Jones AO Omoshoro-Jones General & Hepatopancreatobiliary Surgery Chris Hani-Baragwanath Academic Hospital Faculty of Health Sciences,
Acute Pancreatitis. Falk Symposium 161 Dresden
 Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
