Management of Carotid Stenosis
|
|
|
- Melinda Reed
- 6 years ago
- Views:
Transcription
1 C l i n i c a l D e c i s i o n s Interactive at Management of Carotid Stenosis This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed by specific clinical options, none of which can be considered either correct or incorrect. In short essays, experts in the field then argue for each of the options. In the online version of this feature, available at readers can participate in forming community opinion by choosing one of the options and, if they like, providing their reasons. C ase Vignet te A 67-year-old man with a history of hypertension and hyperlipidemia is seen for a routine examination. His medications include hydrochlorothiazide (25 mg daily), simvastatin (20 mg daily), and aspirin (81 mg daily). He drinks alcohol rarely and does not smoke. His body-mass index (the weight in kilograms divided by the square of the height in meters) is 27, consistent with overweight. His blood pressure is 140/85 mm Hg, and his heart rate is 72 beats per minute and regular. His cardiac examination is normal. Auscultation of the neck shows normal carotid upstrokes but reveals a middle-pitched bruit only in systole at the angle of the right jaw. A detailed neurologic examination is normal. On questioning, the patient does not report any history of transient neurologic deficits specifically, no unilateral weakness or sensory symptoms, visual disturbances, or speech or language difficulty. Noninvasive testing of the carotid arteries reveals a stenosis of 70 to 80% of the proximal right carotid artery with an irregular plaque and peak velocity of 339 cm per second. There is 20% stenosis in the left proximal carotid artery. Which one of the following initial treatment options, any of which could be considered correct, would you find most appropriate for this patient? Base your choice on the published literature, your past experience, recent guidelines, and other sources of information, as appropriate. 1. Medical management. 2. Carotid stenting. 3. Carotid endarterectomy. To aid in your decision making, each of these approaches to treatment is defended by an expert in the management of carotid stenosis in the following short essays. Given your knowledge of the condition and the points made by the experts, which treatment approach would you choose? Make your choice on our Web site (www. nejm.org). Treatment Op tion 1 Medical Management Cathy A. Sila, M.D. Recommendations for the treatment of a patient with asymptomatic carotid stenosis of 70 to 80%, such as the patient in the case vignette, should be based on an understanding of the adverse events that are most likely to occur and the benefits and risks of the treatment over time. The best outcome-based data for patients with asymptomatic carotid stenosis come from the Asymptomatic Carotid Atherosclerosis Study (ACAS) and the Asymptomatic Carotid Surgery Trial (ACST; Current Controlled Trials number, ISRCTN ). 1,2 Although stroke may be the most feared consequence of carotid disease, the most common adverse event in these studies was death from myocardial infarction or other (nonstroke) cardiovascular causes. Nonfatal myocardial infarctions were not reported separately, but the rate of fatal events alone is consistent with a high risk of coronary heart disease according to the Framingham model (>20% over a 10-year period). Fatal or nonfatal strokes were the next-most-common adverse events, but only one third to one half of these strokes were ischemic and ipsilateral and could be attributed to the carotid stenosis. n engl j med 358;15 april 10,
2 Aggressive medical management of vascular risk factors can reduce both coronary and cerebrovascular events in patients with carotid disease, although the definition and execution of medical therapy vary from trial to trial. In five randomized clinical trials (including ACAS and ACST) of medical therapy alone for asymptomatic carotid stenosis as compared with endarterectomy plus medical therapy, the medical therapy consisted of an antiplatelet regimen and counseling about risk factors, but the subsequent care of patients was delegated to the primary physician. Although the degree of compliance with antiplatelet therapy was reported, the degree of success with control of risk factors was not. In the ACST, the definition of best medical therapy evolved during the study, with patients in the final cohort receiving antiplatelet therapy (given to 90% of patients), antihypertensive therapy (81%), and lipid-lowering therapy (70%). Three of the five trials, including a total of 925 patients with asymptomatic carotid stenosis of more than 50%, showed no significant reduction in the risk of stroke or death with endarterectomy as compared with medical therapy alone. In the two larger trials, including a total of 4782 patients with asymptomatic carotid stenosis of 60 to 99% or 70 to 99%, adding endarterectomy to medical therapy did reduce the combined rate of ipsilateral stroke at 5 years and perioperative stroke and death (11.0 to 11.8% reduced to 5.1 to 6.4%), with low procedural risk (2.3 to 3.1%). However, the goal of preventing a disabling or fatal stroke with the use of surgery was achieved only in ACST, and that reduction of 0.5% per year means that 40 patients would need to be treated to prevent one major stroke over a 5-year period. Medical therapy alone should be recommended if procedural risks (of surgery as well as angiography) are expected to exceed 3.0%. Unfortunately, in contrast to rates in the trials discussed above, rates as high as 4.7 to 6.7% have been reported with endarterectomy in other clinical trials and in the Medicare population. 3 Published postapproval carotid-stenting registries have also reported procedural risks exceeding the safety threshold set by the American Heart Association and the American Academy of Neurology. Currently, carotid stenting for asymptomatic stenosis in low-risk patients is reimbursed by the Centers for Medicare and Medicaid Services only in the context of a clinical trial approved by the Food and Drug Administration (FDA). Such patients should be referred to ongoing randomized trials the Carotid Revascularization Endarterectomy versus Stenting Trial (CREST; ClinicalTrials.gov number, NCT ) or the Carotid Stenting vs. Surgery of Severe Carotid Artery Disease and Stroke Prevention in Asymptomatic Patients (ACT I) trial (ClinicalTrials. gov number, NCT ). Also, since the risks of revascularization are immediate, whereas the benefit to an asymptomatic patient is accrued only over time, high-risk asymptomatic patients with poor 5-year survival (e.g., those with previous vascular surgery, claudication, cardiac disease, an abnormal electrocardiogram, diabetes mellitus, or older age) should also be treated medically. 4 Available data from the clinical trials probably underestimate the benefit that could be derived from medical intervention. For the patient in the case vignette, I would encourage lifestyle modifications including weight and girth loss, dietary counseling, and lipid-lowering therapy to achieve a low-density lipoprotein level of less than 100 mg per deciliter (2.6 mmol per liter) (with consideration of a target of <70 mg per deciliter [1.8 mmol per liter]), a triglyceride level of less than 150 mg per deciliter (1.7 mmol per liter), and a high-density lipoprotein level of more than 40 mg per deciliter (1.0 mmol per liter). For patients who smoke, I also recommend smoking cessation. Antihypertensive therapy should be adjusted to maintain blood pressure below 140/90 mm Hg or, if there is evidence of diabetes or kidney disease, below 130/80 mm Hg. Diabetes screening should be performed and hyperglycemia treated, with a target glycated hemoglobin level of less than 7%. Given the high risk of concomitant coronary heart disease, provocative testing should be performed before initiation of a moderate-intensity aerobic physical exercise program ( 30 minutes most days of the week). 5 Patients and their families should be educated about the symptoms of transient ischemic attack and stroke, which require urgent reevaluation and treatment. No potential conflict of interest relevant to this article was reported. From the Neurological Institute Case Medical Center, Case Western Reserve University School of Medicine, Cleveland n engl j med 358;15 april 10, 2008
3 Clinical Decisions Treatment Op tion 2 Carotid Stenting Randall T. Higashida, M.D. Carotid atherosclerotic disease is responsible for a significant proportion of major disabling strokes and death. Effective prevention by means of revascularization is the best course of treatment, if performed at a center with an acceptably low procedural complication rate. The ACAS, published in 1995, involved 1662 patients with asymptomatic carotid stenosis of more than 60%. 1 Patients were prospectively, randomly assigned to undergo either surgical revascularization or aggressive medical management. The primary outcome was any major stroke or death; the median follow-up was 2.7 years. The aggregate risk of any stroke or perioperative death over a 5-year period favored revascularization (5.1%, vs. 11.0% for medical therapy; 95% confidence interval [CI], 0.9 to 9.1; relative risk reduction, 53.6%). The authors concluded that elective surgical revascularization will reduce the 5-year risk of ipsilateral stroke if performed at a center associated with a perioperative morbidity rate of less than 3%. In 2004, the results of the ACST, a confirmatory randomized trial of 3120 patients with asymptomatic stenosis of more than 60%, were published. 2 An absolute reduction of 5.3% (95% CI, 3.0 to 7.8) in the rate of the primary end point any stroke or perioperative death at 5 years with early treatment translated into a significant relative risk reduction of 54.0% (P<0.001). Over the past decade, numerous clinical trials have compared surgery with an alternative, less invasive treatment: carotid-artery stenting with the use of distal-protection devices. The Carotid and Vertebral Artery Transluminal Angioplasty Study (CAVATAS) involved the random assignment of 504 patients to undergo either angioplasty, with or without stenting, or surgery. The 30-day rates of stroke and death were similar in the two groups. In the Stenting and Angioplasty with Protection in Patients at High Risk for Endarterectomy (SAPPHIRE) trial, 334 patients who had symptomatic stenosis of more than 50% or asymptomatic stenosis of more than 80% and who were highrisk surgical candidates were randomly assigned to undergo either stenting or surgery. 6 The primary end point of stroke, death, or myocardial infarction within 30 days after the procedure, or ipsilateral stroke between 31 days and 1 year after, strongly favored stenting over surgery (12.2% of patients vs. 20.1%; absolute difference, 7.9%; 95% CI, 16.4 to 0.7; P = for noninferiority and P = for superiority). A Cochrane analysis in 2005 evaluated data from five randomized trials, involving 1269 patients, comparing the safety and efficacy of endovascular stenting with that of surgery. 7 The 30-day and 1-year safety data showed no significant difference between the two groups in the odds of having a treatment-related stoke or the odds of any stroke, death, or both. In addition, the rates of cranial nerve injury and minor complications were significantly lower with stenting than with surgery. On the basis of these studies, the FDA granted approval in 2005 for carotid stenting for both symptomatic and asymptomatic patients who are high-risk surgical candidates and are enrolled in postapproval studies, and the Centers for Medicare and Medicaid Services approved payment for these procedures. 8 The ongoing National Institutes of Health sponsored CREST, a prospective, multicenter, randomized study of 2500 patients, is nearing completion. This trial may provide clinically directive information about the relative safety and efficacy of surgery, as compared with carotid stenting, for both symptomatic and asymptomatic patients. The advantages of carotid stenting are numerous. Stenting is performed under local anesthesia, permitting continuous neurologic monitoring, and is considered minimally invasive, involving only a small opening (<3 mm in diameter) in the femoral artery, as compared with the much larger, open incision across the neck required for endarterectomy. Direct surgical exposure of the neck vessels increases the risks of wound infection, cranial nerve deficits, vocal cord paralysis, hoarseness, and dysphagia; 8 to 10% of surgical patients experience one or more of these complications. Scarring and other major surgical complications are significantly less common with stenting. Complete recovery time is much shorter with stenting, averaging 2 to 4 days, as compared with 2 to 4 weeks with surgery. As the design of both stents and distal-protection devices improves, so do the outcomes. Large database registries indicate that the n engl j med 358;15 april 10,
4 real-world experience of stenting in both symptomatic and asymptomatic patients makes it acceptable for routine clinical use. The patient in the case vignette should be counseled that with the best medical therapy, his risk of a major stroke or death over a 5-year period is 11 to 12% and that by undergoing a revascularization procedure he can reduce his risk to approximately 5 to 6%. There are now two viable revascularization options: open surgery, requiring a large incision across the neck, and the much less invasive stenting procedure, which is performed under local anesthesia. Although this patient is not considered to be at high surgical risk, private insurance companies and Medicare will consider, on a case-by-case basis, payment for carotid-artery stenting performed in qualified centers or as part of a clinical trial. Both procedures, when performed in centers with capable and experienced physicians, have a periprocedural rate of major complications of less than 3%. I would strongly advise the patient to undergo carotidartery stenting as definitive therapy to improve his longevity and quality of life. Dr. Higashida reports being the National Co-Principal Investigator of the Medtronic Self-Expanding Carotid Stent System with Distal Protection in the Treatment of Carotid Stenosis (MAVERIC) trials I, II, and III and participating in the Abbott Carotid Artery Stent Trial and Guidant s Capture 2 Post Market Carotid Artery Stenting Registry. No other potential conflict of interest relevant to this article was reported. From the Division of Interventional Neurovascular Radiology and the Departments of Radiology, Neurology, Neurological Surgery, and Anesthesiology, University of California, San Francisco, Medical Center, San Francisco. T r e a t m e n t O p t i o n 3 Carotid Endarterectomy G. Patrick Clagett, M.D. The patient in the case vignette is an ideal candidate for carotid endarterectomy to prevent stroke because of the favorable benefit-to-risk ratio. Two large-scale, rigorous trials evaluating the use of carotid endarterectomy in asymptomatic patients with advanced stenoses (>60%) reached similar conclusions despite being carried out on different continents a decade apart. 1,2 In both, as compared with the best medical therapy, the use of carotid endarterectomy resulted in a significantly reduced rate of stroke and death at 5 years (absolute risk reduction, 5.4 to 5.9%; relative risk reduction, 46.0 to 53.0%; P<0.001). Because the patient has a low operative risk, there is no reason that he should not realize the benefit of carotid endarterectomy. He is also unlikely to be harmed by the procedure. In the U.S. trial, 1 the 30-day rate of perioperative stroke or death was 1.1%, after exclusion of the 1.2% rate of stroke from arteriography, a procedure that is rarely performed today in patients with carotid occlusive disease. It has been argued that these results, showing exceptionally low morbidity and mortality, are unlikely to be replicated in routine clinical practice because of the rigorous selection and vetting of surgeons participating in clinical trials. However, recent, large-scale database analyses from the United States 9 and Canada 10 document overall rates of stroke and death in patients undergoing carotid endarterectomy to be well within the range of those found in clinical trials, with stroke rates as low as 0.5%. The absolute reduction in the risk of stroke or death of 5 to 6% with carotid endarterectomy in asymptomatic patients, although significant, is relatively modest and suggests that approximately 17 patients would need to undergo surgery to prevent one stroke or death. This has led to unsuccessful attempts to define more precisely the patients with asymptomatic carotid stenosis who would most likely benefit from the operation. The converse identifying patients who may be less likely to benefit and more likely to suffer complications from surgery has been more feasible. Symptomatic disease, age older than 75 years, female sex, contralateral occlusion, left-sided procedure, severe systolic hypertension, and previous angina or congestive heart failure have all been associated with an increased risk of perioperative stroke or death. 11 Our hypothetical patient has none of these risk factors for adverse outcomes. Other strategies to treat this patient are possible, but none have been shown to be as effective as carotid endarterectomy. The most compelling alternative is intensive medical therapy with aggressive suppression of platelet function, targeted blood-pressure control (possibly with the addition of beta-blockade and an angiotensin-converting enzyme inhibitor), and statin therapy. The argument has been made that the best medical therapy received by patients in past clinical trials did not include widespread use of these current thera n engl j med 358;15 april 10, 2008
5 Clinical Decisions pies that have been shown to reduce the risk of stroke. Would intensive medical therapy erase the benefit of carotid endarterectomy in asymptomatic patients and therefore make it unnecessary? This important question can be answered only by a proper clinical trial comparing the two treatments. Until this is accomplished, any claim regarding a benefit of intensive medical therapy as compared with carotid endarterectomy remains conjectural. The other therapy that might be considered is carotid angioplasty and stenting. Although this intervention has a role in patients considered for carotid endarterectomy who are deemed to be at high surgical risk, the role of angioplasty and stenting in low-risk, asymptomatic patients is unknown. Ultimately, the patient will decide whether he wants to undergo carotid endarterectomy, after a thorough, unbiased presentation of the risks and potential benefits of the procedure. If he elects not to have the operation, intensive medical therapy, counseling of the patient and his family about the warning symptoms of transient ischemic attacks, and careful follow-up are indicated. Before surgery is scheduled, it may be important to confirm the results of duplex ultrasonography by performing magnetic resonance or computed tomographic arteriography, although this is unnecessary if the duplex images came from an appropriately accredited and reliable vascular laboratory. Finally, the surgeon s level of experience is extremely important in realizing a beneficial outcome from carotid endarterectomy. 9 The chosen surgeon should be well trained and have documentation of good outcomes (overall rate of stroke or death, <3%). No potential conflict of interest relevant to this article was reported. From the Department of Surgery, Division of Vascular and Endovascular Surgery, University of Texas Southwestern Medical Center, Dallas. 1. Executive Committee for the Asymptomatic Carotid Atherosclerosis Study. Endarterectomy for asymptomatic carotid artery stenosis. JAMA 1995;273: Halliday A, Mansfield A, Marro J, et al. Prevention of disabling and fatal strokes by successful carotid endarterectomy in patients without recent neurological symptoms: randomised controlled trial. Lancet 2004;363: [Erratum, Lancet 2004; 364:416.] 3. Wolff T, Guirguis-Blake J, Miller T, Gillespie M, Harris R. Screening for carotid artery stenosis: an update of the evidence for the U.S. Preventive Services Task Force. Ann Intern Med 2007; 147: Cohen SN, Hobson RW II, Weiss DG, Chimowitz MI, VA Cooperative Study 167 Group. Death associated with asymptomatic carotid stenosis: long-term clinical evaluation. J Vasc Surg 1993;18: Adams RJ, Chimowitz MI, Alpert JS, et al. Coronary risk evaluation in patients with transient ischemic attack and ischemic stroke: a scientific statement for healthcare professionals from the Stroke Council and the Council on Clinical Cardiology of the American Heart Association/American Stroke Association. Circulation 2003;108: Yadav JS, Wholey MH, Kuntz RE, et al. Protected carotid-artery stenting versus endarterectomy in high-risk patients. N Engl J Med 2004;351: Coward LJ, Featherston RL, Brown MM. Safety and efficacy of endovascular treatment of carotid artery stenosis compared with carotid endarterectomy: a Cochrane systematic review of the randomized evidence. Stroke 2005;36: Medicare covers percutaneous transluminal angioplasty of the carotid artery concurrent with the placement of an FDAapproved carotid stent with embolic protection device. Medicare bulletin Baltimore: Centers for Medicare & Medicaid Services. (Accessed March 21, 2008, at transmittals/downloads/r53ncd.pdf.) 9. Matsen SL, Chang DC, Perler BA, Roseborough GS, Williams GM. Trends in the in-hospital stroke rate following carotid endarterectomy in California and Maryland. J Vasc Surg 2006;44: Feasby TE, Kennedy J, Quan H, Girard L, Ghali WA. Realworld replication of randomized controlled trial results for carotid endarterectomy. Arch Neurol 2007;64: Abbott AL, Bladin CF, Levi CR, Chambers BR. What should we do with asymptomatic carotid stenosis? Int J Stroke 2007;2: Copyright 2008 Massachusetts Medical Society. n engl j med 358;15 april 10,
Disclosures. State of the Art Management of Carotid Stenosis. NIH funding for clinical trials Consultant for Scientia Vascular and Medtronic
 State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
03/30/2016 DISCLOSURES TO OPERATE OR NOT THAT IS THE QUESTION CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE
 CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
CAROTID STENTING A 2009 UPDATE. Hoang Duong, MD Director of Interventional Neuroradiology Memorial Regional Hospital
 CAROTID STENTING A 2009 UPDATE Hoang Duong, MD Director of Interventional Neuroradiology Memorial Regional Hospital TREATMENT FOR CAROTID STENOSIS Best medical management Antiplatelet therapy Antihypertensive
CAROTID STENTING A 2009 UPDATE Hoang Duong, MD Director of Interventional Neuroradiology Memorial Regional Hospital TREATMENT FOR CAROTID STENOSIS Best medical management Antiplatelet therapy Antihypertensive
Carotid Artery Stenosis
 Evidence-Based Approach to Carotid Artery Stenosis Seong-Wook Park, MD Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine, Seoul, Korea Carotid Artery Stenosis Carotid
Evidence-Based Approach to Carotid Artery Stenosis Seong-Wook Park, MD Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine, Seoul, Korea Carotid Artery Stenosis Carotid
How to Choose Between Carotid Stenting and Carotid Endarterectomy for Stroke Prevention
 How to Choose Between Carotid Stenting and Carotid Endarterectomy for Stroke Prevention Christopher J. White MD, MSCAI Chief of Medical Services, Professor and Chairman of Medicine Ochsner Medical Center
How to Choose Between Carotid Stenting and Carotid Endarterectomy for Stroke Prevention Christopher J. White MD, MSCAI Chief of Medical Services, Professor and Chairman of Medicine Ochsner Medical Center
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million life insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million Life Insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
Treatment Considerations for Carotid Artery Stenosis. Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery
 Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
New Trials in Progress: ACT 1. Jon Matsumura, MD Cannes, France June 28, 2008
 New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
AN ASSESSMENT OF INTER-RATER RELIABILITY IN THE TREATMENT OF CAROTID ARTERY STENOSIS
 Pak Heart J ORIGINAL ARTICLE AN ASSESSMENT OF INTER-RATER RELIABILITY IN THE TREATMENT OF CAROTID ARTERY STENOSIS 1 2 3 4 5 Abhishek Nemani, Arshad Ali, Arshad Rehan, Ali Aboufaris, Jabar Ali 1-4 Guthrie
Pak Heart J ORIGINAL ARTICLE AN ASSESSMENT OF INTER-RATER RELIABILITY IN THE TREATMENT OF CAROTID ARTERY STENOSIS 1 2 3 4 5 Abhishek Nemani, Arshad Ali, Arshad Rehan, Ali Aboufaris, Jabar Ali 1-4 Guthrie
Contemporary Management of Carotid Disease What We Know So Far
 Contemporary Management of Carotid Disease What We Know So Far Ammar Safar, MD, FSCAI, FACC, FACP, RPVI Interventional Cardiology & Endovascular Medicine Disclosers NONE Epidemiology 80 % of stroke are
Contemporary Management of Carotid Disease What We Know So Far Ammar Safar, MD, FSCAI, FACC, FACP, RPVI Interventional Cardiology & Endovascular Medicine Disclosers NONE Epidemiology 80 % of stroke are
Carotid Artery Stenting Today: A Few Updating Remarks
 Carotid Artery Stenting Today: A Few Updating Remarks Camilo R. Gomez, MD, MBA Director, Alabama Neurological Institute Birmingham, Alabama Disclaimer & Warning Company Pharmaceutical BMS-Sanofi-Aventis
Carotid Artery Stenting Today: A Few Updating Remarks Camilo R. Gomez, MD, MBA Director, Alabama Neurological Institute Birmingham, Alabama Disclaimer & Warning Company Pharmaceutical BMS-Sanofi-Aventis
Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary
 SOCIETY FOR VASCULAR SURGERY DOCUMENT Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary John J. Ricotta, MD, a Ali AbuRahma, MD, FACS, b
SOCIETY FOR VASCULAR SURGERY DOCUMENT Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary John J. Ricotta, MD, a Ali AbuRahma, MD, FACS, b
Carotid Artery Stenting Versus
 Carotid Artery Stenting Versus Carotid Endarterectomy Seong-Wook Park, MD, PhD, FACC,, Seoul, Korea Stroke & Carotid artery stenosis Stroke & Carotid artery stenosis Cerebrovascular disease is one of the
Carotid Artery Stenting Versus Carotid Endarterectomy Seong-Wook Park, MD, PhD, FACC,, Seoul, Korea Stroke & Carotid artery stenosis Stroke & Carotid artery stenosis Cerebrovascular disease is one of the
CLINICAL TIMELINE EVA-3S CREST ICSS SPACE SAPPHIRE
 Normal Risk Symptomatic Patients: Ongoing Debate CAS vs CEA John R. Laird, MD Professor of Medicine Medical Director of the Vascular Center University of California, Davis CLINICAL TIMELINE Randomized
Normal Risk Symptomatic Patients: Ongoing Debate CAS vs CEA John R. Laird, MD Professor of Medicine Medical Director of the Vascular Center University of California, Davis CLINICAL TIMELINE Randomized
Carotid Artery Stenting
 Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Carotid Artery Revascularization: Current Strategies. Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014
 Carotid Artery Revascularization: Current Strategies Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014 Disclosures None 1 Stroke in 2014 Stroke kills almost
Carotid Artery Revascularization: Current Strategies Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014 Disclosures None 1 Stroke in 2014 Stroke kills almost
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO
 Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE?
 UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE? Richard W. Petrella M.D. FACP,FACC,FASCI DEPARTMENT CHAIRMAN CVM&S UPMC HAMOT MEDICAL CENTER 1 LEARNING OBJECTIVES REVIEW THE RISK FACTORS FOR
UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE? Richard W. Petrella M.D. FACP,FACC,FASCI DEPARTMENT CHAIRMAN CVM&S UPMC HAMOT MEDICAL CENTER 1 LEARNING OBJECTIVES REVIEW THE RISK FACTORS FOR
TCAR: TransCarotid Artery Revascularization Angela A. Kokkosis, MD, RPVI, FACS
 TCAR: TransCarotid Artery Revascularization Angela A. Kokkosis, MD, RPVI, FACS Assistant Professor of Surgery Director of Carotid Interventions Division of Vascular & Endovascular Surgery Stony Brook University
TCAR: TransCarotid Artery Revascularization Angela A. Kokkosis, MD, RPVI, FACS Assistant Professor of Surgery Director of Carotid Interventions Division of Vascular & Endovascular Surgery Stony Brook University
Carotid Endarterectomy vs. Carotid artery Stenting (Surgeon Perspective)
 Carotid Endarterectomy vs. Carotid artery Stenting (Surgeon Perspective) T-Woei Tan, MD, FACS, RPVI Assistant Professor of Surgery Vascular and Endovascular Surgery Louisiana State University Health -
Carotid Endarterectomy vs. Carotid artery Stenting (Surgeon Perspective) T-Woei Tan, MD, FACS, RPVI Assistant Professor of Surgery Vascular and Endovascular Surgery Louisiana State University Health -
Carotid Artery Disease How the Data Will Influence Management The Symptomatic vs. the Asymptomatic Patient
 Carotid Artery Disease How the 2014-2015 Data Will Influence Management The Symptomatic vs. the Asymptomatic Patient Christopher J. White, MD, MSCAI, FACC, FAHA, FESC Professor and Chair of Medicine Ochsner
Carotid Artery Disease How the 2014-2015 Data Will Influence Management The Symptomatic vs. the Asymptomatic Patient Christopher J. White, MD, MSCAI, FACC, FAHA, FESC Professor and Chair of Medicine Ochsner
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACAS (Asymptomatic Carotid Atherosclerosis Study), 65 66 ACST (Asymptomatic Carotid Surgery Trial), 6 7, 65, 75 Age factors, in carotid
Index Note: Page numbers of article titles are in boldface type. A ACAS (Asymptomatic Carotid Atherosclerosis Study), 65 66 ACST (Asymptomatic Carotid Surgery Trial), 6 7, 65, 75 Age factors, in carotid
Carotid Artery Stenting (CAS) Pathophysiology. Technical Considerations. Plaque characteristics: relevant concepts. CAS and CEA
 Carotid Artery Stenting (CAS) Carotid Artery Stenting for Stroke Risk Reduction Matthew A. Corriere MD, MS, RPVI Assistant Professor of Surgery Department of Vascular and Endovascular Surgery Rationale:
Carotid Artery Stenting (CAS) Carotid Artery Stenting for Stroke Risk Reduction Matthew A. Corriere MD, MS, RPVI Assistant Professor of Surgery Department of Vascular and Endovascular Surgery Rationale:
BULgarian Carotid Artery Stenting versus Surgery Study (BULCASSS): Randomized single center trial
 BULgarian Carotid Artery Stenting versus Surgery Study (): Randomized single center trial Ivo Petrov, M. Konteva, H. Dimitrov, K. Kichukov Tokuda Hospital Sofia Cardiology Department Background Carotid
BULgarian Carotid Artery Stenting versus Surgery Study (): Randomized single center trial Ivo Petrov, M. Konteva, H. Dimitrov, K. Kichukov Tokuda Hospital Sofia Cardiology Department Background Carotid
Surgical Treatment of Carotid Disease
 Department of Cardiothoracic & Vascular Surgery McGovern Medical School / The University of Texas Health Science Center at Houston Surgical Treatment of Carotid Disease The Old, the New, and the Future
Department of Cardiothoracic & Vascular Surgery McGovern Medical School / The University of Texas Health Science Center at Houston Surgical Treatment of Carotid Disease The Old, the New, and the Future
Slide 1. Slide 2 Conflict of Interest Disclosure. Slide 3 Stroke Facts. The Treatment of Intracranial Stenosis. Disclosure
 Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
More than strokes occur
 Surgery vs Stent: Treatment for Carotid Artery Disease Imad A. Alhaddad, MD ABSTRACT PURPOSE: This article summarizes and compares the roles of surgery and stent in the management of carotid artery disease.
Surgery vs Stent: Treatment for Carotid Artery Disease Imad A. Alhaddad, MD ABSTRACT PURPOSE: This article summarizes and compares the roles of surgery and stent in the management of carotid artery disease.
Assessment of the procedural etiology of stroke resulting from carotid artery stenting
 Assessment of the procedural etiology of stroke resulting from carotid artery stenting 1. Study Purpose and Rationale: A. Background Stroke is the 3 rd leading cause of death in the United States and carries
Assessment of the procedural etiology of stroke resulting from carotid artery stenting 1. Study Purpose and Rationale: A. Background Stroke is the 3 rd leading cause of death in the United States and carries
Which Patients Are Good Candidates for Carotid Artery Stenting or Carotid Endarterectomy
 13 th Annual Angioplasty Summit TCT Asia Pacific Seoul, Korea April 24, 2008 Which Patients Are Good Candidates for Carotid Artery Stenting or Carotid Endarterectomy Michael R. Jaff, DO, FACP, FACC Associate
13 th Annual Angioplasty Summit TCT Asia Pacific Seoul, Korea April 24, 2008 Which Patients Are Good Candidates for Carotid Artery Stenting or Carotid Endarterectomy Michael R. Jaff, DO, FACP, FACC Associate
Stroke prevention in asymptomatic carotid stenosis. ΛΙΛΛΗΣ ΛΕΩΝΙΔΑΣ Καρδιολόγος Επιστημονικός Συνεργάτης Α Καρδιολογικής Κλινικής ΑΠΘ ΠΓΝΘ ΑΧΕΠΑ
 Stroke prevention in asymptomatic carotid stenosis ΛΙΛΛΗΣ ΛΕΩΝΙΔΑΣ Καρδιολόγος Επιστημονικός Συνεργάτης Α Καρδιολογικής Κλινικής ΑΠΘ ΠΓΝΘ ΑΧΕΠΑ Σεμινάρια Ομάδων Εργασίας Ελληνικής Καρδιολογικής Εταιρείας
Stroke prevention in asymptomatic carotid stenosis ΛΙΛΛΗΣ ΛΕΩΝΙΔΑΣ Καρδιολόγος Επιστημονικός Συνεργάτης Α Καρδιολογικής Κλινικής ΑΠΘ ΠΓΝΘ ΑΧΕΠΑ Σεμινάρια Ομάδων Εργασίας Ελληνικής Καρδιολογικής Εταιρείας
Carotid Artery Stenting
 Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid. The. Issue. Now approved by the FDA, carotid stenting moves into the spotlight in endovascular care.
 The Carotid Issue 33 Carotid Revascularization in 2004 By Thomas G. Brott, MD; Jamie Roberts, LPN, CRC; Robert W. Hobson II, MD; and Susan Hughes, BSN Now approved by the FDA, carotid stenting moves into
The Carotid Issue 33 Carotid Revascularization in 2004 By Thomas G. Brott, MD; Jamie Roberts, LPN, CRC; Robert W. Hobson II, MD; and Susan Hughes, BSN Now approved by the FDA, carotid stenting moves into
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for
 Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
The Struggle to Manage Stroke, Aneurysm and PAD
 The Struggle to Manage Stroke, Aneurysm and PAD In this article, Dr. Salvian examines the management of peripheral arterial disease, aortic aneurysmal disease and cerebrovascular disease from symptomatology
The Struggle to Manage Stroke, Aneurysm and PAD In this article, Dr. Salvian examines the management of peripheral arterial disease, aortic aneurysmal disease and cerebrovascular disease from symptomatology
SAMIR R. KAPADIA, MD Department of Cardiovascular Medicine, Cleveland Clinic
 INTERPRETING KEY TRIALS CME CREDIT EDUCATIONAL OBJECTIVE: Readers will discuss the risks and benefits of carotid artery stenting vs endarterectomy with prospective candidates for these procedures OLCAY
INTERPRETING KEY TRIALS CME CREDIT EDUCATIONAL OBJECTIVE: Readers will discuss the risks and benefits of carotid artery stenting vs endarterectomy with prospective candidates for these procedures OLCAY
Approach to the Patient with Carotid Artery Disease
 Approach to the Patient with Carotid Artery Disease Michael R. Jaff, DO, FACP, FACC Director, Vascular Medicine Massachusetts General Hospital Boston, Massachusetts Conflict of Interest Statement Within
Approach to the Patient with Carotid Artery Disease Michael R. Jaff, DO, FACP, FACC Director, Vascular Medicine Massachusetts General Hospital Boston, Massachusetts Conflict of Interest Statement Within
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH
 ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Outcome
 Measure #344: Rate of Carotid Artery Stenting (CAS) for Asymptomatic Patients, Without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Effective Clinical
Measure #344: Rate of Carotid Artery Stenting (CAS) for Asymptomatic Patients, Without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Effective Clinical
ESC Heart & Brain Workshop
 ESC Heart & Brain Workshop The role of vascular surgeon in stroke prevention Barbara Rantner, MD, PhD, Department of Vascular Surgery, Medical University Innsbruck, Innsbruck, Austria Supported by Bayer,
ESC Heart & Brain Workshop The role of vascular surgeon in stroke prevention Barbara Rantner, MD, PhD, Department of Vascular Surgery, Medical University Innsbruck, Innsbruck, Austria Supported by Bayer,
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
APPENDIX A NORTH AMERICAN SYMPTOMATIC CAROTID ENDARTERECTOMY TRIAL
 APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
Open heart surgery or carotid endarterectomy. Which procedure should be done first?
 Open heart surgery or carotid endarterectomy. Which procedure should be done first? Pedro Pinto Sousa 1, Gabriela Teixeira 2, João Gonçalves 2 ; Luís Vouga 1, Rui Almeida 2 ; Pedro Sá Pinto 2 1 Centro
Open heart surgery or carotid endarterectomy. Which procedure should be done first? Pedro Pinto Sousa 1, Gabriela Teixeira 2, João Gonçalves 2 ; Luís Vouga 1, Rui Almeida 2 ; Pedro Sá Pinto 2 1 Centro
Introduction. Risk factors of PVD 5/8/2017
 PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
The Effectiveness of Medical Therapy for Severe Carotid Stenosis in Reducing Large-Vessel Embolic Stroke: Open Question or Question Answered?
 TCT 2009 San Francisco, California September 22, 2009 The Effectiveness of Medical Therapy for Severe Carotid Stenosis in Reducing Large-Vessel Embolic Stroke: Open Question or Question Answered? Michael
TCT 2009 San Francisco, California September 22, 2009 The Effectiveness of Medical Therapy for Severe Carotid Stenosis in Reducing Large-Vessel Embolic Stroke: Open Question or Question Answered? Michael
Quality Measures MIPS CV Specific
 Quality Measures MIPS CV Specific MEASURE NAME Atrial Fibrillation and Atrial Flutter: Chronic Anticoagulation Therapy CAHPS for MIPS Clinician/Group Survey Cardiac Rehabilitation Patient Referral from
Quality Measures MIPS CV Specific MEASURE NAME Atrial Fibrillation and Atrial Flutter: Chronic Anticoagulation Therapy CAHPS for MIPS Clinician/Group Survey Cardiac Rehabilitation Patient Referral from
Original Contributions. Prospective Comparison of a Cohort With Asymptomatic Carotid Bruit and a Population-Based Cohort Without Carotid Bruit
 98 Original Contributions Prospective Comparison of a Cohort With Carotid Bruit and a Population-Based Cohort Without Carotid Bruit David O. Wiebers, MD, Jack P. Whisnant, MD, Burton A. Sandok, MD, and
98 Original Contributions Prospective Comparison of a Cohort With Carotid Bruit and a Population-Based Cohort Without Carotid Bruit David O. Wiebers, MD, Jack P. Whisnant, MD, Burton A. Sandok, MD, and
Carotid Artery Stenting
 Carotid Artery Stenting Natural history of the carotid stenosis Asymptomatic 80% carotid stenosis - 6% risk of stroke / year Symptomatic carotid stenosis have 10% risk of CVA at one year and 40% at 5 years
Carotid Artery Stenting Natural history of the carotid stenosis Asymptomatic 80% carotid stenosis - 6% risk of stroke / year Symptomatic carotid stenosis have 10% risk of CVA at one year and 40% at 5 years
Peter A. Soukas, M.D., FACC, FSVM, FSCAI, RPVI
 Peter A. Soukas, M.D., FACC, FSVM, FSCAI, RPVI Director, Peripheral Vascular Interventional Laboratory Director, Vascular & Endovascular Medicine Fellowship Program Assistant Professor of Medicine The
Peter A. Soukas, M.D., FACC, FSVM, FSCAI, RPVI Director, Peripheral Vascular Interventional Laboratory Director, Vascular & Endovascular Medicine Fellowship Program Assistant Professor of Medicine The
Carotid artery stenting in the elderly: the time has come
 88 Journal of Geriatric Cardiology June 2007 Vol 4 No 2 Symposium: Review Article Carotid artery stenting in the elderly: the time has come Dipsu Patel, Neil E Strickman St. Luke s Episcopal Hospital/Texas
88 Journal of Geriatric Cardiology June 2007 Vol 4 No 2 Symposium: Review Article Carotid artery stenting in the elderly: the time has come Dipsu Patel, Neil E Strickman St. Luke s Episcopal Hospital/Texas
Management of Carotid Disease CHRISTOPHER LAU PGY-3 BROOKLYN VA
 Management of Carotid Disease CHRISTOPHER LAU PGY-3 BROOKLYN VA SUNY DOWNSTATE MEDICAL CENTER Case 61 year old male referred to Vascular Surgery for left internal carotid stenosis Presented with transient
Management of Carotid Disease CHRISTOPHER LAU PGY-3 BROOKLYN VA SUNY DOWNSTATE MEDICAL CENTER Case 61 year old male referred to Vascular Surgery for left internal carotid stenosis Presented with transient
CANADIAN STROKE BEST PRACTICE RECOMMENDATIONS
 CANADIAN STROKE BEST PRACTICE RECOMMENDATIONS Management of Extracranial Carotid Disease and Intracranial Atherosclerosis Coutts S, Wein T (Writing Group Chairs) on Behalf of the PREVENTION of STROKE Writing
CANADIAN STROKE BEST PRACTICE RECOMMENDATIONS Management of Extracranial Carotid Disease and Intracranial Atherosclerosis Coutts S, Wein T (Writing Group Chairs) on Behalf of the PREVENTION of STROKE Writing
Carotid Endarterectomy versus Carotid Angioplasty Cui Bono *
 Eur J Vasc Endovasc Surg (2010) 39, S44eS48 Carotid Endarterectomy versus Carotid Angioplasty Cui Bono * W.S. Moore* Division of Vascular Surgery, David Geffen School of Medicine at UCLA, 200 UCLA Medical
Eur J Vasc Endovasc Surg (2010) 39, S44eS48 Carotid Endarterectomy versus Carotid Angioplasty Cui Bono * W.S. Moore* Division of Vascular Surgery, David Geffen School of Medicine at UCLA, 200 UCLA Medical
Joshua A. Beckman, MD. Brigham and Women s Hospital
 Peripheral Vascular Disease: Overview, Peripheral Arterial Obstructive Disease, Carotid Artery Disease, and Renovascular Disease as a Surrogate for Coronary Artery Disease Joshua A. Beckman, MD Brigham
Peripheral Vascular Disease: Overview, Peripheral Arterial Obstructive Disease, Carotid Artery Disease, and Renovascular Disease as a Surrogate for Coronary Artery Disease Joshua A. Beckman, MD Brigham
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Peripheral Vascular Disease
 Peripheral artery disease (PAD) results from the buildup of plaque (atherosclerosis) in the arteries of the legs. For people with PAD, symptoms may be mild, requiring no treatment except modification of
Peripheral artery disease (PAD) results from the buildup of plaque (atherosclerosis) in the arteries of the legs. For people with PAD, symptoms may be mild, requiring no treatment except modification of
Clinical Trial Synopsis TL-OPI-516, NCT#
 Clinical Trial Synopsis, NCT#00225277 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl Versus
Clinical Trial Synopsis, NCT#00225277 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl Versus
Carotid Artery Stent: Is it ready for prime time?
 2010 CATH LAB SYMPOSIUM Carotid Artery Stent: Is it ready for prime time? Luis F. Tami, MD, FACC, FSCAI Interventional Cardiology and Vascular Medicine Memorial Regional Hospital August 2010 CAE and CAS
2010 CATH LAB SYMPOSIUM Carotid Artery Stent: Is it ready for prime time? Luis F. Tami, MD, FACC, FSCAI Interventional Cardiology and Vascular Medicine Memorial Regional Hospital August 2010 CAE and CAS
Asymptomatic Carotid Stenosis To Do or Not To Do
 Asymptomatic Carotid Stenosis To Do or Not To Do October 22, 2016 Neurosciences: Updates and Controversies Andrew C. MacDougall, MD Advocate Medical Group Advocate Lutheran General Hospital Principle
Asymptomatic Carotid Stenosis To Do or Not To Do October 22, 2016 Neurosciences: Updates and Controversies Andrew C. MacDougall, MD Advocate Medical Group Advocate Lutheran General Hospital Principle
Peripheral Arterial Occlusive Disease- The Challenge in patients with diabetes
 Peripheral Arterial Occlusive Disease- The Challenge in patients with diabetes Ashok Handa Reader in Surgery and Consultant Surgeon Nuffield Department of Surgery University of Oxford Introduction Vascular
Peripheral Arterial Occlusive Disease- The Challenge in patients with diabetes Ashok Handa Reader in Surgery and Consultant Surgeon Nuffield Department of Surgery University of Oxford Introduction Vascular
THE incidence of stroke after noncardiac surgery
 Lack of Association between Carotid Artery Stenosis and Stroke or Myocardial Injury after Noncardiac Surgery in High-risk Patients ABSTRACT Background: Whether carotid artery stenosis predicts stroke after
Lack of Association between Carotid Artery Stenosis and Stroke or Myocardial Injury after Noncardiac Surgery in High-risk Patients ABSTRACT Background: Whether carotid artery stenosis predicts stroke after
The U.S. Preventive Services Task Force (USPSTF)
 Clinical Guidelines Annals of Internal Medicine Screening for Carotid Artery Stenosis: U.S. Preventive Services Task Force Recommendation Statement U.S. Preventive Services Task Force* Description: Update
Clinical Guidelines Annals of Internal Medicine Screening for Carotid Artery Stenosis: U.S. Preventive Services Task Force Recommendation Statement U.S. Preventive Services Task Force* Description: Update
Hypothesis: When compared to conventional balloon angioplasty, cryoplasty post-dilation decreases the risk of SFA nses in-stent restenosis
 Cryoplasty or Conventional Balloon Post-dilation of Nitinol Stents For Revascularization of Peripheral Arterial Segments Background: Diabetes mellitus is associated with increased risk of in-stent restenosis
Cryoplasty or Conventional Balloon Post-dilation of Nitinol Stents For Revascularization of Peripheral Arterial Segments Background: Diabetes mellitus is associated with increased risk of in-stent restenosis
Guidelines for Ultrasound Surveillance
 Guidelines for Ultrasound Surveillance Carotid & Lower Extremity by Ian Hamilton, Jr, MD, MBA, RPVI, FACS Corporate Medical Director BlueCross BlueShield of Tennessee guidelines for ultrasound surveillance
Guidelines for Ultrasound Surveillance Carotid & Lower Extremity by Ian Hamilton, Jr, MD, MBA, RPVI, FACS Corporate Medical Director BlueCross BlueShield of Tennessee guidelines for ultrasound surveillance
Carotid Stenosis (carotid artery disease)
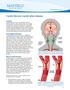 1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
Will guidelines and clinical practice for asymptomatic stenosis change in the near future?
 Will guidelines and clinical practice for asymptomatic stenosis change in the near future? M Storck, MD, PhD Director Dept. Vascular and Thoracic Surgery Klinikum Karlsruhe Academic Teaching Hospital,
Will guidelines and clinical practice for asymptomatic stenosis change in the near future? M Storck, MD, PhD Director Dept. Vascular and Thoracic Surgery Klinikum Karlsruhe Academic Teaching Hospital,
The argument against revascularization for asymptomatic carotid stenosis
 The argument against revascularization for asymptomatic carotid stenosis Seemant Chaturvedi, MD, FAHA, FAAN Professor of Clinical Neurology Vice-Chair for VA Programs Univ. of Miami Miller School of Medicine
The argument against revascularization for asymptomatic carotid stenosis Seemant Chaturvedi, MD, FAHA, FAAN Professor of Clinical Neurology Vice-Chair for VA Programs Univ. of Miami Miller School of Medicine
Cardiac evaluation for the noncardiac. Nathaen Weitzel MD University of Colorado Denver Dept of Anesthesiology
 Cardiac evaluation for the noncardiac patient Nathaen Weitzel MD University of Colorado Denver Dept of Anesthesiology Objectives! Review ACC / AHA guidelines as updated for 2009! Discuss new recommendations
Cardiac evaluation for the noncardiac patient Nathaen Weitzel MD University of Colorado Denver Dept of Anesthesiology Objectives! Review ACC / AHA guidelines as updated for 2009! Discuss new recommendations
Advances in the treatment of posterior cerebral circulation symptomatic disease
 Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Andrew Cohen, MD and Neil S. Skolnik, MD INTRODUCTION
 2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
My Latest Take on RCT Data: When is CEA or CAS the Best Option? The Interventional Position
 LINC 2016 Leipzig, Jan 26-29, 2016 My Latest Take on RCT Data: When is CEA or CAS the Best Option? The Interventional Position Horst Sievert, Iris Grunwald CardioVasculäres Centrum Frankfurt - CVC, Frankfurt
LINC 2016 Leipzig, Jan 26-29, 2016 My Latest Take on RCT Data: When is CEA or CAS the Best Option? The Interventional Position Horst Sievert, Iris Grunwald CardioVasculäres Centrum Frankfurt - CVC, Frankfurt
Extracranial Carotid Artery/Stenting
 Extracranial Carotid Artery/Stenting Policy Number: 7.01.68 Last Review: 6/2017 Origination: 4/2005 Next Review: 6/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Extracranial Carotid Artery/Stenting Policy Number: 7.01.68 Last Review: 6/2017 Origination: 4/2005 Next Review: 6/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Debata II: Carotidal stenting v.s. carotidal endatherectomy- surgical side
 Debata II: Carotidal stenting v.s. carotidal endatherectomy- surgical side Academician Mitrev Z, Special hospital for surgery Filip Vtori Skopje - Macedonija Oktomvri, 2008 History Hippocrates, 400 B.C.
Debata II: Carotidal stenting v.s. carotidal endatherectomy- surgical side Academician Mitrev Z, Special hospital for surgery Filip Vtori Skopje - Macedonija Oktomvri, 2008 History Hippocrates, 400 B.C.
MEET Θ symptomatic patients. K. Mathias Department of Radiology Teaching Hospital of Dortmund - Germany
 MEET Θ 2006 Why I stent asymptomatic and symptomatic patients K. Mathias Department of Radiology Teaching Hospital of Dortmund - Germany Evidence for treating symptomatic patients symptomatic patients
MEET Θ 2006 Why I stent asymptomatic and symptomatic patients K. Mathias Department of Radiology Teaching Hospital of Dortmund - Germany Evidence for treating symptomatic patients symptomatic patients
Effective Health Care
 Number 5 Effective Health Care Comparative Effectiveness of Management Strategies for Renal Artery Stenosis Executive Summary Background Renal artery stenosis (RAS) is defined as the narrowing of the lumen
Number 5 Effective Health Care Comparative Effectiveness of Management Strategies for Renal Artery Stenosis Executive Summary Background Renal artery stenosis (RAS) is defined as the narrowing of the lumen
Accumulating evidence from randomized, controlled trials shows that carotid. Efficacy versus Effectiveness of Carotid Endarterectomy
 BACK OF THE ENVELOPE DAVID A. GOULD, MD Research Fellow VA Outcomes Group Department of Veterans Affairs Medical Center White River Junction, Vt Resident Department of Dartmouth Medical School Hanover,
BACK OF THE ENVELOPE DAVID A. GOULD, MD Research Fellow VA Outcomes Group Department of Veterans Affairs Medical Center White River Junction, Vt Resident Department of Dartmouth Medical School Hanover,
Management of combined coronary & carotid disease
 Management of combined coronary & carotid disease Combined Carotid and coronary artery diseases Frequent combination Fear of imminent death psychologically traumatic for the patients and their families
Management of combined coronary & carotid disease Combined Carotid and coronary artery diseases Frequent combination Fear of imminent death psychologically traumatic for the patients and their families
Randomized comparison of single versus double mammary coronary artery bypass grafting: 5 year outcomes of the Arterial Revascularization Trial
 Randomized comparison of single versus double mammary coronary artery bypass grafting: 5 year outcomes of the Arterial Revascularization Trial Embargoed until 10:45 a.m. CT, Monday, Nov. 14, 2016 David
Randomized comparison of single versus double mammary coronary artery bypass grafting: 5 year outcomes of the Arterial Revascularization Trial Embargoed until 10:45 a.m. CT, Monday, Nov. 14, 2016 David
The Great Swedish Debate. Håkan Pärsson Department Vascular Surgery Helsingborgs Lasarett, University Lund
 The Great Swedish Debate Håkan Pärsson Department Vascular Surgery Helsingborgs Lasarett, University Lund My Disclosures Trying to bribe the moderators What do my patients expect? Balanced information
The Great Swedish Debate Håkan Pärsson Department Vascular Surgery Helsingborgs Lasarett, University Lund My Disclosures Trying to bribe the moderators What do my patients expect? Balanced information
Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk
 Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk Amy B. Reed, MD, a Peter Gaccione, MA, b Michael Belkin, MD, b Magruder C. Donaldson, MD, b John A. Mannick, MD,
Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk Amy B. Reed, MD, a Peter Gaccione, MA, b Michael Belkin, MD, b Magruder C. Donaldson, MD, b John A. Mannick, MD,
PAPER. Carotid Angioplasty and Stenting vs Carotid Endarterectomy for Treatment of Asymptomatic Disease
 PAPER Carotid Angioplasty and Stenting vs Carotid Endarterectomy for Treatment of Asymptomatic Disease Single-Center Experience Gale L. Tang, MD; Jon S. Matsumura, MD; Mark D. Morasch, MD; William H. Pearce,
PAPER Carotid Angioplasty and Stenting vs Carotid Endarterectomy for Treatment of Asymptomatic Disease Single-Center Experience Gale L. Tang, MD; Jon S. Matsumura, MD; Mark D. Morasch, MD; William H. Pearce,
Extracranial Carotid Artery/Stenting
 Extracranial Carotid Artery/Stenting Policy Number: 7.01.68 Last Review: 6/2018 Origination: 4/2005 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Extracranial Carotid Artery/Stenting Policy Number: 7.01.68 Last Review: 6/2018 Origination: 4/2005 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Update on the only remaining Carotid Multicenter Randomised International Trial in the World:ACST-2
 Update on the only remaining Carotid Multicenter Randomised International Trial in the World:ACST-2 Alison Halliday MD Professor of Vascular Surgery University of Oxford Disclosure Statement of Financial
Update on the only remaining Carotid Multicenter Randomised International Trial in the World:ACST-2 Alison Halliday MD Professor of Vascular Surgery University of Oxford Disclosure Statement of Financial
The MAIN-COMPARE Study
 Long-Term Outcomes of Coronary Stent Implantation versus Bypass Surgery for the Treatment of Unprotected Left Main Coronary Artery Disease Revascularization for Unprotected Left MAIN Coronary Artery Stenosis:
Long-Term Outcomes of Coronary Stent Implantation versus Bypass Surgery for the Treatment of Unprotected Left Main Coronary Artery Disease Revascularization for Unprotected Left MAIN Coronary Artery Stenosis:
Why I do not believe the
 Why I do not believe the EVA-3S Trial J Mocco,, MD Ken Snyder, MD,PhD LN Hopkins, MD University at Buffalo Neurosurgery LN Hopkins, MD Potential Conflicts Consultant & research support: Boston Scientific,
Why I do not believe the EVA-3S Trial J Mocco,, MD Ken Snyder, MD,PhD LN Hopkins, MD University at Buffalo Neurosurgery LN Hopkins, MD Potential Conflicts Consultant & research support: Boston Scientific,
Coronary Artery Disease: Revascularization (Teacher s Guide)
 Stephanie Chan, M.D. Updated 3/15/13 2008-2013, SCVMC (40 minutes) I. Objectives Coronary Artery Disease: Revascularization (Teacher s Guide) To review the evidence on whether percutaneous coronary intervention
Stephanie Chan, M.D. Updated 3/15/13 2008-2013, SCVMC (40 minutes) I. Objectives Coronary Artery Disease: Revascularization (Teacher s Guide) To review the evidence on whether percutaneous coronary intervention
IS CAROTID ULTRASOUND NECESSARY IN THE CLINICAL EVALUATION OF THE ASYMPTOMATIC HOLLENHORST PLAQUE? (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS)
 IS CAROTID ULTRASOUND NECESSARY IN THE CLINICAL EVALUATION OF THE ASYMPTOMATIC HOLLENHORST PLAQUE? (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) By Sophie J. Bakri MD, Ashraf Luqman MD, Bhupesh Pathik
IS CAROTID ULTRASOUND NECESSARY IN THE CLINICAL EVALUATION OF THE ASYMPTOMATIC HOLLENHORST PLAQUE? (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) By Sophie J. Bakri MD, Ashraf Luqman MD, Bhupesh Pathik
Antiplatelet Therapy in Primary CVD Prevention and Stable Coronary Artery Disease. Καρακώστας Γεώργιος Διευθυντής Καρδιολογικής Κλινικής, Γ.Ν.
 Antiplatelet Therapy in Primary CVD Prevention and Stable Coronary Artery Disease Καρακώστας Γεώργιος Διευθυντής Καρδιολογικής Κλινικής, Γ.Ν.Κιλκίς Primary CVD Prevention A co-ordinated set of actions,
Antiplatelet Therapy in Primary CVD Prevention and Stable Coronary Artery Disease Καρακώστας Γεώργιος Διευθυντής Καρδιολογικής Κλινικής, Γ.Ν.Κιλκίς Primary CVD Prevention A co-ordinated set of actions,
THE NATIONAL QUALITY FORUM
 THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
ACC NY Cardiovascular Symposium
 ACC NY Cardiovascular Symposium Peripheral Vascular Disease: Watch the Heart and the Brain Evolving Role of Exercise, ACE-Inhibitors, Interventional and Surgical Options Mark A. Creager, M.D President,
ACC NY Cardiovascular Symposium Peripheral Vascular Disease: Watch the Heart and the Brain Evolving Role of Exercise, ACE-Inhibitors, Interventional and Surgical Options Mark A. Creager, M.D President,
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Dr Julia Hopyan Stroke Neurologist Sunnybrook Health Sciences Centre
 Dr Julia Hopyan Stroke Neurologist Sunnybrook Health Sciences Centre Objectives To learn what s new in stroke care 2010-11 1) Acute stroke management Carotid artery stenting versus surgery for symptomatic
Dr Julia Hopyan Stroke Neurologist Sunnybrook Health Sciences Centre Objectives To learn what s new in stroke care 2010-11 1) Acute stroke management Carotid artery stenting versus surgery for symptomatic
Module 2. Global Cardiovascular Risk Assessment and Reduction in Women with Hypertension
 Module 2 Global Cardiovascular Risk Assessment and Reduction in Women with Hypertension 1 Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored,
Module 2 Global Cardiovascular Risk Assessment and Reduction in Women with Hypertension 1 Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored,
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Special Topic Section
 Special Topic Section Cerebrovasc Dis 2004;18:69 74 DOI: 10.1159/000078753 Received: March 8, 2004 Accepted: March 8, 2004 Published online: June 1, 2004 International Carotid Stenting Study: Protocol
Special Topic Section Cerebrovasc Dis 2004;18:69 74 DOI: 10.1159/000078753 Received: March 8, 2004 Accepted: March 8, 2004 Published online: June 1, 2004 International Carotid Stenting Study: Protocol
a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers
 The study a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers Conflict of interest have the following potential conflicts of interest to report: Consulting
The study a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers Conflict of interest have the following potential conflicts of interest to report: Consulting
Registry Assessment of Peripheral Interventional Devices (RAPID)
 Registry Assessment of Peripheral Interventional Devices (RAPID) Adding Data Sources May 2, 2018 W. Schuyler Jones, MD Duke Clinical Research Institute Duke Heart Center Disclosures Research Grants: Agency
Registry Assessment of Peripheral Interventional Devices (RAPID) Adding Data Sources May 2, 2018 W. Schuyler Jones, MD Duke Clinical Research Institute Duke Heart Center Disclosures Research Grants: Agency
