Management of Aortic Valve Disease: Review Questions
|
|
|
- Geraldine Gallagher
- 6 years ago
- Views:
Transcription
1 S e l f - A s s e s s m e n t i n C a r d i o l o g y Management of Aortic Valve Disease: Review Questions Josh Leitner, MD Wen-Chih Wu, MD QUESTIONS Choose the single best answer for each question. Questions 1 and 2 refer to the following case. A 72-year-old man with a past medical history noteworthy only for hypertension controlled on hydrochlorothiazide and a described heart murmur with a tight valve presents to the emergency department (ED) complaining of weeks of progressive exertional dyspnea and an episode of dyspnea awakening him from sleep. The patient reports no chest pain. Upon presentation, his blood pressure is 102/68 mm Hg, heart rate is 98 bpm and regular, respiratory rate is 18 breaths/min, and oxygen saturation is 90% on room air, which improves to 99% following oxygen supplementation at a rate of 4 L/min via nasal cannula. Physical examination reveals a diminished A 2, late-peaking systolic crescendo-decrescendo murmur, delayed and diminished carotid upstroke, an audible S 3, dilated jugular veins, and bibasilar rales. Chest radiograph shows pulmonary edema. An electrocardiogram (ECG) shows sinus tachycardia, left ventricular (LV) hypertrophy, left atrial enlargement, and 0.5-mm ST depressions in the anterior and lateral leads, with T-wave inversions in the lateral precordial leads. 1. What is the next most appropriate step in the management of this patient? (A) Immediate cardiothoracic surgery consultation for emergent aortic valve replacement surgery (B) Immediate measurement of brain natriuretic peptide (BNP) level and bedside echocardiogram to assess ejection fraction and valve function; initiate intravenous (IV) furosemide only if either of the tests is abnormal (C) Initiation of IV furosemide accompanied by IV nitroglycerine drip (D) Initiation of IV furosemide without nitroglycerine, with accurate monitoring of weight and urine output; readminister diuretic only if there are persistent findings of volume overload 2. The following morning, the patient s clinical status is improved, with normal oxygen saturation on room air. Serial ECGs show sinus rhythm with normalization of the T-wave inversions noted previously. Troponin levels are undetectable. An echocardiogram shows normal LV size, moderate LV hypertrophy, a LV ejection fraction (LVEF) of 40%, and a calcified aortic valve with severe stenosis (aortic valve area = 0.8 cm 2 ). Which of the following is indicated in the workup and management of the patient at this time? (A) Cardiology consultation for invasive coronary angiography prior to planned aortic valve replacement (B) Exercise stress test with nuclear myocardial perfusion imaging to assess for ischemia and exercise tolerance (C) High-dose statin therapy for reduction of aortic valve calcification (D) Initiation of a β-blocker, an angiotensinconverting enzyme (ACE) inhibitor, oral furosemide, and long-acting nitrates to reduce further hospitalizations and consideration of valve surgery if symptoms recur 3. A 71-year-old woman with medication-controlled hypertension, hypercholesterolemia, and osteoarthritis presents in the outpatient setting for routine care. Physical examination reveals a harsh, midpeaking systolic murmur radiating to the neck, a slightly diminished carotid upstroke, no jugular venous distension, clear lungs, and no peripheral edema. She notes that her ambulation is at times limited by knee pain, but generally she is able to complete her Dr. Leitner is a clinical fellow in cardiology, Warren Alpert Medical School of Brown University, Providence, RI. Dr. Wu is an assistant professor of medicine, Providence VA Medical Center and Warren Alpert Medical School at Brown University. Hospital Physician November/December
2 activities of daily living, including walking through the supermarket, with no limiting dyspnea or chest discomfort. She denies any history of syncope. An echocardiogram performed 2 weeks prior demonstrates normal biventricular systolic function, moderate LV hypertrophy, normal LV dimensions, mild mitral regurgitation with mitral annular calcification, and a heavily calcified aortic valve with severe aortic stenosis. Which of the following interventions is indicated at this time? (A) Hospitalization for further workup and management of severe aortic valve disease (B) Initiation of oral furosemide and a statin (C) Repeat clinical assessment in 3 to 6 months and repeat echocardiographic assessment within 1 year or sooner if symptoms develop (D) Treadmill exercise stress testing with nuclear myocardial perfusion imaging to assess for the presence of coronary artery disease 4. A 64-year-old man with hypertension requiring 3 medications for control presents in the outpatient setting for routine care, having recently moved to the area. He denies any limiting dyspnea, orthopnea, or chest discomfort and notes that he can complete his activities of daily living effortlessly. He denies recent illness, hospitalization, or fevers. Physical examination reveals a symmetric blood pressure of 138/52 mm Hg, heart rate of 92 bpm, no jugular venous distension, markedly bounding pulses, and a decrescendo pandiastolic murmur at the left upper sternal border. The patient has a copy of an echocardiogram report from his prior assessment showing a moderately dilated left ventricle (internal dimension in diastole: 6.3 cm), an LVEF of 60%, a dilated aortic root (4.8 cm) with moderate to severe aortic insufficiency, and a bicuspid aortic valve. A repeat echocardiogram confirms the bicuspid aortic valves with the same left ventricle internal dimensions, but also shows an LVEF of 50%, an aortic root diameter of 4.9 cm, and severe aortic insufficiency. The patient is seen the following week, still without any limiting symptoms. Which of the following interventions is indicated at this time? (A) Cardiology consultation for coronary angiography and referral for aortic valve replacement with or without aortic graft (B) Initiation of ACE inhibitor and furosemide and repeat echocardiogram in 6 months or sooner if symptoms develop (C) Initiation of β-blocker and diuretic and reassessment in 6 months (D) Transfer to emergency department for urgent contrast computed tomography (CT) of the aorta to assess for dissection 5. A 73-year-old woman with known mild to moderate aortic insufficiency and normal LV systolic function returns for follow-up after a repeat echocardiogram, which is of good quality, demonstrating mildly dilated left ventricle with internal dimensions of 5.9 cm in diastole and 4.0 cm in systole, an LVEF of 65%, and moderate aortic insufficiency. Although she feels generally able to meet her activities of daily living, she notes having slightly less energy compared to 6 months prior. She denies any marked exertional or nocturnal dyspnea, orthopnea, or chest discomfort, and denies any recent fevers, illnesses, or hospitalizations. Her blood pressure and cholesterol are normal without the need of medications. According to recent ACC/AHA guidelines, which of the following is routinely recommended for further assessment and management of this patient? (A) Recommendation of antibiotic prophylaxis for all surgical and dental procedures (B) Referral for cardiac catheterization and aortography to accurately quantify the grade of aortic regurgitation (C) Referral for elective aortic valve replacement (D) Repeat clinical assessment in 6 to 12 months with repeat transthoracic echocardiogram in 1 year, or sooner if symptoms develop 6. A 51-year-old man who has been hospitalized for delayed presentation of a pneumococcal pneumonia complicated by bacteremia and hypotension has clinical improvement after initiation of antibiotics and aggressive hydration but has persistent lowgrade fevers. Two days later, he develops increasing sinus tachycardia, dyspnea without chest or back pain, and diaphoresis. Physical examination reveals a blood pressure of 98/68 mm Hg, heart rate of 122 bpm, oxygen saturation of 90% on room air, a faint early diastolic murmur, bibasilar rales, and cool distal extremities. ECG reveals sinus tachycardia without other abnormality. Chest radiograph shows normal heart size, pulmonary vascular congestion, and mild pulmonary edema. Bedside transesophageal echocardiography reveals severe destruction of the aortic valve with severe aortic insufficiency. Which of the following interventions are indicated at this time? (A) Aggressive intravenous hydration, repeat blood cultures, addition of broad-spectrum antibiotics, 34 Hospital Physician November/December
3 and repeat transesophageal echocardiogram after 3 days of therapy (B) Aspirin, nitroglycerine, IV heparin, and evaluation of serial troponin levels every 8 hours (C) Cautious administration of IV nitroprusside drip, intensive blood pressure monitoring, and referral for emergent valve replacement surgery (D) IV β-blockers for improved heart rate control and urgent interventional cardiology consultation for intra-aortic balloon pump placement for his cardiogenic shock ANSWERS AND EXPLANATIONS 1. (D) Initiation of IV furosemide without nitroglycerine, with accurate monitoring of weight and urine output; readminister diuretic only if there are persistent findings of volume overload. The patient has acute decompensated heart failure related to severe aortic stenosis. This condition requires careful diuresis to relieve pulmonary edema and volume overload with close attention to the patient s volume status. Overaggressive reduction of preload (through aggressive diuresis and/or nitrates) can result in marked hemodynamic instability given the limited capacity of the heart to augment cardiac output due to the stenotic valve. 1 Given the clinical picture, neither a BNP level nor an urgent echocardiogram is likely to alter the clinical management of the patient at this point. Small ST-segment and T-wave changes are nonspecific in the setting of LV hypertrophy and tachycardia and must be interpreted in the larger clinical context. 2. (A) Cardiology consultation for invasive coronary angiography prior to planned aortic valve replacement. The development of symptoms attributable to aortic stenosis angina, syncope, or heart failure is a significant prognostic turning point in the disease course and warrants assessment for surgery. Medical therapy has not been demonstrated to alter the natural history of severe aortic stenosis. In the absence of surgical aortic valve replacement, the presence of angina, syncope, or heart failure is associated with a 50% mortality at 5, 3, and 2 years, respectively. 2 Exercise stress testing is contraindicated in patients with symptomatic severe aortic stenosis due to a high rate of complications and low diagnostic accuracy. Given the overlap of risk factors with coronary artery disease, invasive coronary angiography should be performed prior to aortic valve replacement to assess whether concomitant coronary artery bypass grafting is necessary. Statin therapy has demonstrated no benefit for prevention of progression of severe aortic valve calcification and should not be initiated for this purpose (C) Repeat clinical assessment in 3 to 6 months and repeat echocardiographic assessment within 1 year or sooner if symptoms develop. Even with severe aortic stenosis, asymptomatic patients enjoy a natural history similar to normal patients until the development of symptoms. 3 These patients are best monitored by serial clinical assessment with a thorough evaluation for exertional symptoms, as well as annual echocardiogram for development of LV systolic dysfunction. The American College of Cardiology/ American Heart Association (ACC/AHA) guidelines suggest serial echocardiography annually for severe aortic stenosis (or with change in clinical status, especially development of dyspnea, angina, or syncope) every 1 to 2 years for moderate stenosis and every 3 to 5 years for mild stenosis. 3 Given this patient s absence of symptoms and reassuring physical examination, there is no role for hospitalization at this time. Exercise testing in asymptomatic severe aortic stenosis is controversial and may be helpful in some patients with nonspecific symptoms to assess exercise capacity, development of exertional symptoms, or abnormal hemodynamic response to exercise. Stress testing in asymptomatic patients with severe aortic stenosis carries risk and is ideally performed with direct communication with the testing facility staff and cardiology consultation. Exercise stress testing is unlikely to be useful for the assessment of coronary artery disease in the setting of severe aortic stenosis. Exercise stress testing is contraindicated in patients with symptomatic aortic stenosis. Since volume overload or history of heart failure was not demonstrated, there is no role for diuresis in this patient. Statin therapy has not been demonstrated to alter the course of severe calcific aortic stenosis and should not be initiated for this purpose. Cardiology consultation in the future would be warranted when aortic valve replacement is contemplated and preoperative cardiac catheterization is needed, which is routinely performed prior to surgical valve replacement for evaluation of coronary artery disease. 4. (A) Cardiology consultation for coronary angiography and referral for aortic valve replacement with or without aortic graft. In contrast to stenotic aortic valve disease, surgery is indicated for chronic Hospital Physician November/December
4 regurgitant aortic valve disease prior to the development of symptoms. The indications for aortic valve replacement with asymptomatic chronic severe aortic insufficiency include new LV systolic dysfunction (defined by the ACC/AHA valve disease guidelines as LVEF 50%) or severe LV dilatation (LV enddiastolic dimension > 75 mm or LV end- systolic dimension > 55 mm). 3 This patient has demonstrated an interval decrease in LV systolic function into the abnormal range of 50% or less, which is a class 1 indication for aortic valve replacement, regardless of LV dimensions. 3 As with other valve lesions, patients at risk should be assessed for coronary disease prior to valve surgery. In this case, the patient is also at risk for both aortic dissection and rupture given the presence of a bicuspid aortic valve and a dilated aortic root; therefore, he should also be considered for aortic root replacement with a valved conduit for maximal likelihood of surgical success and recovery of LV systolic function. An increase in pulse pressure (the difference between systolic and diastolic blood pressure) with an increased systolic blood pressure is a hallmark of chronic aortic insufficiency due to increased LV preload and may not be controlled on multiple medications. Therefore, medical therapy with a diuretic or β-blocker is not indicated, and in fact, rate-slowing with β-blockade poses theoretical harm because it would prolong diastole, exacerbating the time of insufficiency. Medical therapy with vasodilators such as an ACE inhibitors can be considered but should not delay or be considered a replacement for surgery in patients with chronic severe aortic insufficiency that has already met surgical criteria. 5. (D) Repeat clinical assessment in 6 to 12 months with repeat transthoracic echocardiogram in 1 year, or sooner if symptoms develop. This patient has asymptomatic moderate aortic insufficiency without evidence of LV dysfunction or dilatation; one could generally expect a long period without symptoms or development of LV dysfunction and an average mortality rate of less than 0.2% per year. 3,4 Therefore, the risks of aortic valve replacement and postoperative complications outweigh its benefits, and valve surgery is not yet indicated. 3 However, given the progressive nature of the disease, these patients should be followed closely, ideally with a multidisciplinary team including primary care physicians, cardiologists, and cardiothoracic surgeons. Although most patients with chronic aortic insufficiency develop symptoms prior to development of LV dysfunction, more than one quarter who die or develop systolic dysfunction do so before the onset of warning symptoms. Therefore, noninvasive assessment, generally with transthoracic echocardiography, is indicated, with particular attention to LV dimensions and LV systolic function. 3 Moreover, if the transthoracic echocardiography is of good quality, which is the case in this patient, there is no indication for invasive aortography. The 2008 AHA focused update on infectious endocarditis suggests that antibiotic prophylaxis is only recommended for patients with a high risk of endocarditis defined as (1) patients with prosthetic heart valves, (2) patients with complex congenital heart disease, (3) patients with valvulopathy in a transplanted heart, and (4) patients with a prior history of endocarditis. 4 The presence of aortic insufficiency alone, as seen in this patient, is no longer a recommendation for antibiotic prophylaxis (C) Cautious administration of IV nitroprusside drip, intensive blood pressure monitoring, and referral for emergent valve replacement surgery. This patient has acute severe aortic insufficiency from acute infective endocarditis. Acute severe aortic insufficiency is a clinical emergency that requires a high index of suspicion in the appropriate clinical setting (chest trauma, aortic dissection, or acute infective endocarditis), and generally requires emergent surgical valve replacement. Many of the classic physical examination manifestations of chronic aortic insufficiency are not evident in acute aortic insufficiency, including normal or only minimally increased pulse pressure. Emergent echocardiography is invaluable in quickly establishing the diagnosis, etiology, and severity. Cautious afterload reduction with nitroprusside and intensive blood pressure monitoring are useful to stabilize the patient s symptoms and serve as a bridge to emergent surgery in patients with acute severe aortic insufficiency, especially in the setting of heart failure. 3 Given the hemodynamic instability of the patient and the fact that aortic insufficiency occurs during diastole, β-blockers are contraindicated as they can prolong diastole. Similarly, an intra-aortic balloon pump exerts its actions by inflating during cardiac diastole, exacerbating aortic insufficiency, and it is also contraindicated. There is no evidence to suggest that this patient has an acute coronary syndrome, and thus there is no role for aspirin, nitroglycerine, IV heparin, and evaluation of serial troponin levels every 8 hours. 36 Hospital Physician November/December
5 The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veteran Affairs. This work is supported by the Research Enhancement Award Program, Providence Veterans Affairs Medical Center, providing research time for Dr. Wu, and the Brown Fellowship Program in Cardiology providing research time for Dr. Leitner. REFERENCES 1. Hunt SA, Abraham WT, Chin MH, et al focused update incorporated into the ACC/AHA 2005 guidelines for the diagnosis and management of heart failure in adults: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol ;53:e Otto C, Bonow R. Valvular heart disease. In: Libby P, Bonow R, Zipes DP, Mann DL, editors. Braunwald s heart disease: a textbook of cardiovascular medicine, 8th ed. New York: Saunders; 2008: Bonow RO, Carabello BA, Chatterjee K, et al focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease. A report of the American College of Cardiology/ American Heart Association Task Force on Practice Guidelines (Writing committee to revise the 1998 guidelines for the management of patients with valvular heart disease). J Am Coll Cardiol 2008;52(13):e Nishimura RA, Carabello BA, Faxon DP, et al. ACC/AHA 2008 Guideline update on valvular heart disease: focused update on infective endocarditis: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J Am Coll Cardiol 2008;52: Copyright 2009 by Turner White Communications Inc., Wayne, PA. All rights reserved. self-assessment questions on the web Now you can access the entire self-assessment series on the Web. Go to click on the Hospital Physician link, and then click on the Self-Assessment Questions option. Cardiology A current list of certification and recertification exam dates and registration information is maintained on the American Board of Internal Medicine Web site, at Hospital Physician November/December
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA
 Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA Case History A 50-year-old man with type 1 diabetes mellitus and hypertension presents after experiencing 1 hour of midsternal chest pain that began after
Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA Case History A 50-year-old man with type 1 diabetes mellitus and hypertension presents after experiencing 1 hour of midsternal chest pain that began after
MITRAL VALVE DISEASE- ASSESSMENT AND MANAGEMENT. Irene Frantzis P year, SGUL Sheba Medical Center
 MITRAL VALVE DISEASE- ASSESSMENT AND MANAGEMENT Irene Frantzis P year, SGUL Sheba Medical Center MITRAL VALVE DISEASE Mitral Valve Regurgitation Mitral Valve Stenosis Mitral Valve Prolapse MITRAL REGURGITATION
MITRAL VALVE DISEASE- ASSESSMENT AND MANAGEMENT Irene Frantzis P year, SGUL Sheba Medical Center MITRAL VALVE DISEASE Mitral Valve Regurgitation Mitral Valve Stenosis Mitral Valve Prolapse MITRAL REGURGITATION
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Valvular Heart Disease
 Valvular Heart Disease Roman M. Sniecinski, MD, FASE Associate Professor of Anesthesiology Emory University School of Medicine Learning Objectives Review the major pathophysiology of the most common heart
Valvular Heart Disease Roman M. Sniecinski, MD, FASE Associate Professor of Anesthesiology Emory University School of Medicine Learning Objectives Review the major pathophysiology of the most common heart
HISTORY. Question: How do you interpret the patient s history? CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: 45-year-old man.
 HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
The production of murmurs is due to 3 main factors:
 Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
Cardiovascular Images
 Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Diagnosis & Management of Heart Failure. Abena A. Osei-Wusu, M.D. Medical Fiesta
 Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Clinicians and Facilities: RESOURCES WHEN CARING FOR WOMEN WITH ADULT CONGENITAL HEART DISEASE OR OTHER FORMS OF CARDIOVASCULAR DISEASE!!
 Clinicians and Facilities: RESOURCES WHEN CARING FOR WOMEN WITH ADULT CONGENITAL HEART DISEASE OR OTHER FORMS OF CARDIOVASCULAR DISEASE!! Abha'Khandelwal,'MD,'MS' 'Stanford'University'School'of'Medicine'
Clinicians and Facilities: RESOURCES WHEN CARING FOR WOMEN WITH ADULT CONGENITAL HEART DISEASE OR OTHER FORMS OF CARDIOVASCULAR DISEASE!! Abha'Khandelwal,'MD,'MS' 'Stanford'University'School'of'Medicine'
General Cardiovascular Magnetic Resonance Imaging
 2 General Cardiovascular Magnetic Resonance Imaging 19 Peter G. Danias, Cardiovascular MRI: 150 Multiple-Choice Questions and Answers Humana Press 2008 20 Cardiovascular MRI: 150 Multiple-Choice Questions
2 General Cardiovascular Magnetic Resonance Imaging 19 Peter G. Danias, Cardiovascular MRI: 150 Multiple-Choice Questions and Answers Humana Press 2008 20 Cardiovascular MRI: 150 Multiple-Choice Questions
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
AF in the ER: Common Scenarios CASE 1. Fast facts. Diagnosis. Management
 AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
Lnformation Coverage Guidance
 Lnformation Coverage Guidance Coverage Indications, Limitations, and/or Medical Necessity Abstract: B-type natriuretic peptide (BNP) is a cardiac neurohormone produced mainly in the left ventricle. It
Lnformation Coverage Guidance Coverage Indications, Limitations, and/or Medical Necessity Abstract: B-type natriuretic peptide (BNP) is a cardiac neurohormone produced mainly in the left ventricle. It
The production of murmurs is due to 3 main factors:
 Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
A Health Care Professional s Guide Aortic Stenosis in Seniors
 A Health Care Professional s Guide Aortic Stenosis in Seniors With highlights from the 2014 ACC/AHA practice guidelines for valve disease Aortic stenosis (AS) is primarily caused by calcification of the
A Health Care Professional s Guide Aortic Stenosis in Seniors With highlights from the 2014 ACC/AHA practice guidelines for valve disease Aortic stenosis (AS) is primarily caused by calcification of the
Tricuspid and Pulmonic Valve Disease
 Chapter 31 Tricuspid and Pulmonic Valve Disease David A. Tate Acquired disease of the right-sided cardiac valves is much less common than disease of the leftsided counterparts, possibly because of the
Chapter 31 Tricuspid and Pulmonic Valve Disease David A. Tate Acquired disease of the right-sided cardiac valves is much less common than disease of the leftsided counterparts, possibly because of the
Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year
![Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year](/thumbs/76/74263761.jpg) PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
Topic Page: congestive heart failure
 Topic Page: congestive heart failure Definition: congestive heart f ailure from Merriam-Webster's Collegiate(R) Dictionary (1930) : heart failure in which the heart is unable to maintain an adequate circulation
Topic Page: congestive heart failure Definition: congestive heart f ailure from Merriam-Webster's Collegiate(R) Dictionary (1930) : heart failure in which the heart is unable to maintain an adequate circulation
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM. General Instructions: ID NUMBER: FORM NAME: H F A DATE: 10/13/2017 VERSION: CONTACT YEAR NUMBER:
 ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
7. Echocardiography Appropriate Use Criteria (by Indication)
 Criteria for Echocardiography 1133 7. Echocardiography Criteria (by ) Table 1. TTE for General Evaluation of Cardiac Structure and Function Suspected Cardiac Etiology General With TTE 1. Symptoms or conditions
Criteria for Echocardiography 1133 7. Echocardiography Criteria (by ) Table 1. TTE for General Evaluation of Cardiac Structure and Function Suspected Cardiac Etiology General With TTE 1. Symptoms or conditions
Medical Management of Acute Heart Failure
 Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Aortic Stenosis: UPDATE Anjan Sinha, MD Krannert Institute of Cardiology
 Aortic Stenosis: UPDATE 2010 Anjan Sinha, MD Krannert Institute of Cardiology None Disclosures 67-Year-Old Male Dyspnea and angina Class III heart failure No PND or orthopnea 3/6 late peak SEM Diminished
Aortic Stenosis: UPDATE 2010 Anjan Sinha, MD Krannert Institute of Cardiology None Disclosures 67-Year-Old Male Dyspnea and angina Class III heart failure No PND or orthopnea 3/6 late peak SEM Diminished
Cor pulmonale. Dr hamid reza javadi
 1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
Which one of the following echocardiographic profiles most strongly indicates the need for aortic valve replacement? FS [
 Question 46 A 45-year-old asymptomatic man returns for follow-up. He was diagnosed 10 years ago with aortic regurgitation due to a congentia lbicuspid aortic valve, He has never had endocarditis Which
Question 46 A 45-year-old asymptomatic man returns for follow-up. He was diagnosed 10 years ago with aortic regurgitation due to a congentia lbicuspid aortic valve, He has never had endocarditis Which
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
TSDA Boot Camp September 13-16, Introduction to Aortic Valve Surgery. George L. Hicks, Jr., MD
 TSDA Boot Camp September 13-16, 2018 Introduction to Aortic Valve Surgery George L. Hicks, Jr., MD Aortic Valve Pathology and Treatment Valvular Aortic Stenosis in Adults Average Course (Post mortem data)
TSDA Boot Camp September 13-16, 2018 Introduction to Aortic Valve Surgery George L. Hicks, Jr., MD Aortic Valve Pathology and Treatment Valvular Aortic Stenosis in Adults Average Course (Post mortem data)
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
CASE DISCUSSION. Dr JAYASREE VEERABOINA 2nd yr PG MS OBG
 CASE DISCUSSION Dr JAYASREE VEERABOINA 2nd yr PG MS OBG Normal Cardiovascular changes in Pregnancy CARDIAC OUTPUT 5 th wk -- starts 12 wks -- 30-35% 30-32 wks -- 40% During labour -- 50% After delivery
CASE DISCUSSION Dr JAYASREE VEERABOINA 2nd yr PG MS OBG Normal Cardiovascular changes in Pregnancy CARDIAC OUTPUT 5 th wk -- starts 12 wks -- 30-35% 30-32 wks -- 40% During labour -- 50% After delivery
Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know
 Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know James F. Burke, MD Program Director Cardiovascular Disease Fellowship Lankenau Medical Center Disclosure Dr. Burke has no conflicts
Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know James F. Burke, MD Program Director Cardiovascular Disease Fellowship Lankenau Medical Center Disclosure Dr. Burke has no conflicts
DAY1_CARDIOVASCULAR PRACTICE QUESTIONS
 DAY1_CARDIOVASCULAR PRACTICE QUESTIONS 1 P age 1. A 59-year-old male is admitted complaining of chest pain and dyspnea. ST elevation and T-wave inversion were seen on the ECG in V2, V3, and V4. IV thrombolytic
DAY1_CARDIOVASCULAR PRACTICE QUESTIONS 1 P age 1. A 59-year-old male is admitted complaining of chest pain and dyspnea. ST elevation and T-wave inversion were seen on the ECG in V2, V3, and V4. IV thrombolytic
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
Percutaneous Coronary Intervention and Pulmonary Balloon Valvuloplasty in a Patient With Severe Valvular Pulmonary Stenosis
 Case Report Percutaneous Coronary Intervention and Pulmonary Balloon Valvuloplasty in a 56-Year-Old Woman With Severe Valvular Pulmonary Stenosis: A Case Report Ata Firouzi 1, MD; Omid Shafe* 1, MD; Farzad
Case Report Percutaneous Coronary Intervention and Pulmonary Balloon Valvuloplasty in a 56-Year-Old Woman With Severe Valvular Pulmonary Stenosis: A Case Report Ata Firouzi 1, MD; Omid Shafe* 1, MD; Farzad
Congestive Heart Failure Patient Profile. Patient Identity - Mr. Douglas - 72 year old man - No drugs, smokes, moderate social alcohol consumption
 Congestive Heart Failure Patient Profile Patient Identity - Mr. Douglas - 72 year old man - No drugs, smokes, moderate social alcohol consumption Chief Complaint - SOB - When asked: Increasing difficulty
Congestive Heart Failure Patient Profile Patient Identity - Mr. Douglas - 72 year old man - No drugs, smokes, moderate social alcohol consumption Chief Complaint - SOB - When asked: Increasing difficulty
ASE 2011 Appropriate Use Criteria for Echocardiography
 ASE 2011 Appropriate Use Criteria for Echocardiography Table 1. TTE for General Evaluation of Cardiac Structure and Function 1 2 Suspected Cardiac Etiology General With TTE Symptoms or conditions potentially
ASE 2011 Appropriate Use Criteria for Echocardiography Table 1. TTE for General Evaluation of Cardiac Structure and Function 1 2 Suspected Cardiac Etiology General With TTE Symptoms or conditions potentially
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
CCRN Review Cardiovascular
 CCRN Review Cardiovascular Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Angina Definition discomfort that occurs when oxygen demand
CCRN Review Cardiovascular Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Angina Definition discomfort that occurs when oxygen demand
Comprehensive Cardiology: Matters of the Heart Class III SARAH BEANLANDS RN BSCN MSC
 Comprehensive Cardiology: Matters of the Heart Class III SARAH BEANLANDS RN BSCN MSC Overview ACS continued Heart Failure Valvular Disorders and Endocarditis Diagnosis Nuclear stress test- stable angina
Comprehensive Cardiology: Matters of the Heart Class III SARAH BEANLANDS RN BSCN MSC Overview ACS continued Heart Failure Valvular Disorders and Endocarditis Diagnosis Nuclear stress test- stable angina
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Cardiology. the Sounds: #7 HCM. LV Outflow Obstruction: Aortic Stenosis. (Coming Soon - HCM)
 A Cardiology HCM LV Outflow Obstruction: Aortic Stenosis (Coming Soon - HCM) the Sounds: #7 Howard J. Sachs, MD www.12daysinmarch.com E-mail: Howard@12daysinmarch.com Aortic Valve Disorders Stenosis Regurgitation
A Cardiology HCM LV Outflow Obstruction: Aortic Stenosis (Coming Soon - HCM) the Sounds: #7 Howard J. Sachs, MD www.12daysinmarch.com E-mail: Howard@12daysinmarch.com Aortic Valve Disorders Stenosis Regurgitation
Acute Mitral Regurgitation- An Easy-to-Miss but Critical-to-Diagnose. Condition
 Acute Mitral Regurgitation- An Easy-to-Miss but Criticalto-Diagnose Condition CLINICAL VIGNETTE Acute Mitral Regurgitation- An Easy-to-Miss but Critical-to-Diagnose Condition Janki Shah, MD; Samuel Daneshvar,
Acute Mitral Regurgitation- An Easy-to-Miss but Criticalto-Diagnose Condition CLINICAL VIGNETTE Acute Mitral Regurgitation- An Easy-to-Miss but Critical-to-Diagnose Condition Janki Shah, MD; Samuel Daneshvar,
Results of Ischemic Heart Disease
 Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Detailed Order Request Checklists for Cardiology
 Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
Medical Treatment for acute Decompensated Heart Failure. Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011
 Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
2018 HPN Provider Summary Guide. Adult Cardiology Patients (18 Years and Older) Referral Guidelines
 12.2 CARDIOLOGY REFERRAL GUIDELINES Contracted Group: Southwest Medical Associates For Appointments: 888 S. Rancho Las Vegas, NV 89109 Phone: (702) 877-8654 Fax: (702) 242-7998 Adult Cardiology Patients
12.2 CARDIOLOGY REFERRAL GUIDELINES Contracted Group: Southwest Medical Associates For Appointments: 888 S. Rancho Las Vegas, NV 89109 Phone: (702) 877-8654 Fax: (702) 242-7998 Adult Cardiology Patients
SAUDI FELLOWSHIP TRAINING PROGRAM. Adult Cardiology. Final Written Examination 2019
 SAUDI FELLOWSHIP TRAINING PROGRAM Adult Cardiology Final Written Examination 2019 Objectives 1. Determine the trainee has sufficient competency related to the required specialty. 2. Determine the eligibility
SAUDI FELLOWSHIP TRAINING PROGRAM Adult Cardiology Final Written Examination 2019 Objectives 1. Determine the trainee has sufficient competency related to the required specialty. 2. Determine the eligibility
Valvular Heart Disease Mitral Stenosis
 Valvular Heart Disease Mitral Stenosis A 75 year old woman with loud first heart sound and mid-diastolic murmur Chronic dyspnea Class 2/4 Fatigue Recent orthopnea/pnd Nocturnal palpitation Pedal edema
Valvular Heart Disease Mitral Stenosis A 75 year old woman with loud first heart sound and mid-diastolic murmur Chronic dyspnea Class 2/4 Fatigue Recent orthopnea/pnd Nocturnal palpitation Pedal edema
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM
 ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM ID NUMBER: FORM NAME: H F A DATE: 10/01/2015 VERSION: D CONTACT YEAR NUMBER: FORM SEQUENCE NUMBER: General Instructions: The Heart Failure Hospital Record
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM ID NUMBER: FORM NAME: H F A DATE: 10/01/2015 VERSION: D CONTACT YEAR NUMBER: FORM SEQUENCE NUMBER: General Instructions: The Heart Failure Hospital Record
Valvular Heart Disease
 Valvular Heart Disease MITRAL STENOSIS Pathophysiology rheumatic fever. calcific degeneration, malignant carcinoid disease, congenital mitral stenosis. SLE. The increased pressure gradient across the mitral
Valvular Heart Disease MITRAL STENOSIS Pathophysiology rheumatic fever. calcific degeneration, malignant carcinoid disease, congenital mitral stenosis. SLE. The increased pressure gradient across the mitral
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
HISTORY. Question: What category of heart disease is suggested by the fact that a murmur was heard at birth?
 HISTORY 23-year-old man. CHIEF COMPLAINT: Decreasing exercise tolerance of several years duration. PRESENT ILLNESS: The patient is the product of an uncomplicated term pregnancy. A heart murmur was discovered
HISTORY 23-year-old man. CHIEF COMPLAINT: Decreasing exercise tolerance of several years duration. PRESENT ILLNESS: The patient is the product of an uncomplicated term pregnancy. A heart murmur was discovered
Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg
 Rotation: or: Faculty: Coronary Care Unit (CVICU) Dr. Jeff Rottman Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg Duty Hours: Mon Fri, 7 AM to 7 PM, weekend call shared with consult
Rotation: or: Faculty: Coronary Care Unit (CVICU) Dr. Jeff Rottman Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg Duty Hours: Mon Fri, 7 AM to 7 PM, weekend call shared with consult
Heart Failure. Cardiac Anatomy. Functions of the Heart. Cardiac Cycle/Hemodynamics. Determinants of Cardiac Output. Cardiac Output
 Cardiac Anatomy Heart Failure Professor Qing ZHANG Department of Cardiology, West China Hospital www.blaufuss.org Cardiac Cycle/Hemodynamics Functions of the Heart Essential functions of the heart to cover
Cardiac Anatomy Heart Failure Professor Qing ZHANG Department of Cardiology, West China Hospital www.blaufuss.org Cardiac Cycle/Hemodynamics Functions of the Heart Essential functions of the heart to cover
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United
 Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Peripartum Cardiomyopathy. Lavanya Rai Manipal
 Peripartum Cardiomyopathy Lavanya Rai Manipal Definition - PPCM - Dilated cardiomyopathy of unknown cause resulting in cardiac failure that occurs in the peripartum period in women without any preexisting
Peripartum Cardiomyopathy Lavanya Rai Manipal Definition - PPCM - Dilated cardiomyopathy of unknown cause resulting in cardiac failure that occurs in the peripartum period in women without any preexisting
Ejection across stenotic aortic valve requires a systolic pressure gradient between the LV and aorta. This places a pressure load on the LV.
 Valvular Heart Disease Etiology General Principles Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Valvular Heart Disease Etiology General Principles Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Acute Valve Regurgitation Catherine M. Otto, MD J. Ward Kennedy-Hamilton Endowed Chair in Cardiology University of Washington, Seattle
 Acute Valve Regurgitation Catherine M. Otto, MD J. Ward Kennedy-Hamilton Endowed Chair in Cardiology University of Washington, Seattle No conflicts of interest Acute Aortic Regurgitation Causes aortic
Acute Valve Regurgitation Catherine M. Otto, MD J. Ward Kennedy-Hamilton Endowed Chair in Cardiology University of Washington, Seattle No conflicts of interest Acute Aortic Regurgitation Causes aortic
HEART CONDITIONS IN SPORT
 HEART CONDITIONS IN SPORT Dr. Anita Green CHD Risk Factors Smoking Hyperlipidaemia Hypertension Obesity Physical Inactivity Diabetes Risks are cumulative (multiplicative) Lifestyles predispose to RF One
HEART CONDITIONS IN SPORT Dr. Anita Green CHD Risk Factors Smoking Hyperlipidaemia Hypertension Obesity Physical Inactivity Diabetes Risks are cumulative (multiplicative) Lifestyles predispose to RF One
Mitral Valve Disease. Prof. Sirchak Yelizaveta Stepanovna
 Mitral Valve Disease Prof. Sirchak Yelizaveta Stepanovna Fall 2008 Mitral Valve Stenosis Lecture Outline Mitral Stenosis Mitral Regurgitation Etiology Pathophysiology Clinical features Diagnostic testing
Mitral Valve Disease Prof. Sirchak Yelizaveta Stepanovna Fall 2008 Mitral Valve Stenosis Lecture Outline Mitral Stenosis Mitral Regurgitation Etiology Pathophysiology Clinical features Diagnostic testing
Degenerative Mitral Regurgitation: Etiology and Natural History of Disease and Triggers for Intervention
 Degenerative Mitral Regurgitation: Etiology and Natural History of Disease and Triggers for Intervention John N. Hamaty D.O. FACC, FACOI November 17 th 2017 I have no financial disclosures Primary Mitral
Degenerative Mitral Regurgitation: Etiology and Natural History of Disease and Triggers for Intervention John N. Hamaty D.O. FACC, FACOI November 17 th 2017 I have no financial disclosures Primary Mitral
MATRIX VHD FORM. State the name of the patient ( Product Recipient ) for whom you are providing the information contained in this form.
 MATRIX VHD FORM A. Patient Information State the name of the patient ( Product Recipient ) for whom you are providing the information contained in this form. (First Name) (Middle Initial) (Last Name) (Date
MATRIX VHD FORM A. Patient Information State the name of the patient ( Product Recipient ) for whom you are providing the information contained in this form. (First Name) (Middle Initial) (Last Name) (Date
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Mitral Regurgitation
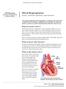 UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
Hypertension in Aortic Valve Disease
 Hypertension in Aortic Valve Disease Hanna M. Nosseir MRCP, FRCP Head of Cardiology department Galaa Military Medical Complex Aortic stenosis: Introduction Arterial hypertension and aortic stenosis are
Hypertension in Aortic Valve Disease Hanna M. Nosseir MRCP, FRCP Head of Cardiology department Galaa Military Medical Complex Aortic stenosis: Introduction Arterial hypertension and aortic stenosis are
Educational Goals & Objectives
 Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
Aortic valve disease. Acknowledgement for slides. Heart Valves 4/28/2018. Adopted from
 Aortic valve disease Senthil Kumar, MD 4.26.2018 28 th Annual Coming Together in Advanced Practice Conference Acknowledgement for slides Adopted from http://www.slideshare.net/ Dr. Anand Chockalingam Dr.
Aortic valve disease Senthil Kumar, MD 4.26.2018 28 th Annual Coming Together in Advanced Practice Conference Acknowledgement for slides Adopted from http://www.slideshare.net/ Dr. Anand Chockalingam Dr.
Disclosures Nothing to disclose
 Aortic Valve Disease Illustrative Cases December 8, 2009 David Stultz, MD, FACC Southwest Cardiology, Inc Handout available at http://www.drstultz.com Disclosures Nothing to disclose Objectives Understand
Aortic Valve Disease Illustrative Cases December 8, 2009 David Stultz, MD, FACC Southwest Cardiology, Inc Handout available at http://www.drstultz.com Disclosures Nothing to disclose Objectives Understand
Listing Form: Heart or Cardiovascular Impairments. Medical Provider:
 Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction
 Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Non-cardiac Surgery in Valvular Heart Disease
 Jafar Golshahi, MD; Shahnaz Aram, MD Abstract Background- Valvular heart disease is one of the common complications of acute rheumatic fever, which manifests its clinical complications one or two decades
Jafar Golshahi, MD; Shahnaz Aram, MD Abstract Background- Valvular heart disease is one of the common complications of acute rheumatic fever, which manifests its clinical complications one or two decades
Ejection across stenotic aortic valve requires a systolic pressure gradient between the LV and aorta. This places a pressure load on the LV.
 Valvular Heart Disease General Principles Etiology Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Valvular Heart Disease General Principles Etiology Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology
 Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Perioperative Cardiac Management. Emma Sargsyan, MD, FACP
 Perioperative Cardiac Management Emma Sargsyan, MD, FACP March 22-24, 2018 Outline Evaluation of cardiac risk prior to non-cardiac surgery Management of cardiac risk for non-cardiac surgery 2 Preop medical
Perioperative Cardiac Management Emma Sargsyan, MD, FACP March 22-24, 2018 Outline Evaluation of cardiac risk prior to non-cardiac surgery Management of cardiac risk for non-cardiac surgery 2 Preop medical
New murmur: acute valvular regurgitations. A.Pasquet, MD,PhD. UCL -Cliniques Saint Luc
 New murmur: acute valvular regurgitations. A.Pasquet, MD,PhD UCL -Cliniques Saint Luc Acute valvular regurgitation Clinical case Mr Dupont, a 53 y old men, without any particular medical history On Thursday
New murmur: acute valvular regurgitations. A.Pasquet, MD,PhD UCL -Cliniques Saint Luc Acute valvular regurgitation Clinical case Mr Dupont, a 53 y old men, without any particular medical history On Thursday
By the end of this session, the student should be able to:
 Valvular Heart disease HVD By Dr. Ashraf Abdelfatah Deyab VHD- Objectives By the end of this session, the student should be able to: Define and classify valvular heart disease. Enlist the causes of acquired
Valvular Heart disease HVD By Dr. Ashraf Abdelfatah Deyab VHD- Objectives By the end of this session, the student should be able to: Define and classify valvular heart disease. Enlist the causes of acquired
Valvular Heart Disease: Assessment and Timing of Intervention. Graham Cole Consultant Cardiologist Imperial College Healthcare NHS Trust
 Valvular Heart Disease: Assessment and Timing of Intervention Graham Cole Consultant Cardiologist Imperial College Healthcare NHS Trust Disclosures: Speaker fee: Bayer Acknowledgements: Matt Shun-Shin
Valvular Heart Disease: Assessment and Timing of Intervention Graham Cole Consultant Cardiologist Imperial College Healthcare NHS Trust Disclosures: Speaker fee: Bayer Acknowledgements: Matt Shun-Shin
Acute Coronary Syndrome. Sonny Achtchi, DO
 Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
CARDIOLOGY SAUDI BOARD PROGRAM
 CARDIOLOGY SAUDI BOARD PROGRAM Objectives: Saudi Board Third Year-F3 Final Written Examination of Cardiology- 2016 Provide an objective assessment instrument for the medical knowledge competency of The
CARDIOLOGY SAUDI BOARD PROGRAM Objectives: Saudi Board Third Year-F3 Final Written Examination of Cardiology- 2016 Provide an objective assessment instrument for the medical knowledge competency of The
My Patient Needs a Stress Test
 My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
Local Coverage Determination (LCD) for Cardiac Catheterization (L29090)
 Local Coverage Determination (LCD) for Cardiac Catheterization (L29090) Contractor Information Contractor Name First Coast Service Options, Inc. Contractor Number 09102 Contractor Type MAC - Part B LCD
Local Coverage Determination (LCD) for Cardiac Catheterization (L29090) Contractor Information Contractor Name First Coast Service Options, Inc. Contractor Number 09102 Contractor Type MAC - Part B LCD
Complications of Acute Myocardial Infarction
 Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
Perioperative Cardiovascular Evaluation and Care for Noncardiac. Dr Mahmoud Ebrahimi Interventional cardiologist 91/9/30
 Perioperative Cardiovascular Evaluation and Care for Noncardiac Surgery Dr Mahmoud Ebrahimi Interventional cardiologist 91/9/30 Active Cardiac Conditions for Which the Patient Should Undergo Evaluation
Perioperative Cardiovascular Evaluation and Care for Noncardiac Surgery Dr Mahmoud Ebrahimi Interventional cardiologist 91/9/30 Active Cardiac Conditions for Which the Patient Should Undergo Evaluation
Clinical Appropriateness Guidelines: Diagnostic Coronary Angiography
 Clinical Appropriateness Guidelines: Diagnostic Coronary Angiography Appropriate Use Criteria Effective Date: January 2, 2018 Proprietary Date of Origin: 08/27/2015 Last revised: 02/23/2017 Last reviewed:
Clinical Appropriateness Guidelines: Diagnostic Coronary Angiography Appropriate Use Criteria Effective Date: January 2, 2018 Proprietary Date of Origin: 08/27/2015 Last revised: 02/23/2017 Last reviewed:
Pulmonary Hypertension: Another Use for Viagra
 Pulmonary Hypertension: Another Use for Viagra Kathleen Tong, MD Director, Heart Failure Program Assistant Clinical Professor University of California, Davis Disclosures I have no financial conflicts A
Pulmonary Hypertension: Another Use for Viagra Kathleen Tong, MD Director, Heart Failure Program Assistant Clinical Professor University of California, Davis Disclosures I have no financial conflicts A
Disclosures. Objectives 10/11/17. Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock. I have no disclosures to report
 Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock Christopher K. Gordon MSN, ACNP-BC Disclosures I have no disclosures to report 1. Pathophysiology 2. Epidemiology 3. Assessment
Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock Christopher K. Gordon MSN, ACNP-BC Disclosures I have no disclosures to report 1. Pathophysiology 2. Epidemiology 3. Assessment
The PAIN Pathway for the Management of Acute Coronary Syndrome
 2 The PAIN Pathway for the Management of Acute Coronary Syndrome Eyal Herzog, Emad Aziz, and Mun K. Hong Acute coronary syndrome (ACS) subsumes a spectrum of clinical entities, ranging from unstable angina
2 The PAIN Pathway for the Management of Acute Coronary Syndrome Eyal Herzog, Emad Aziz, and Mun K. Hong Acute coronary syndrome (ACS) subsumes a spectrum of clinical entities, ranging from unstable angina
Mitral Stenosis: A Review
 Cardiovascular Innovations and Applications Vol. x No. x (2016) x x ISSN 2009-8618 DOI 10.15212/CVIA.2016.0041 REVIEW Mitral Stenosis: A Review By C. Richard Conti, MD, MACC 1 1 Department of Medicine,
Cardiovascular Innovations and Applications Vol. x No. x (2016) x x ISSN 2009-8618 DOI 10.15212/CVIA.2016.0041 REVIEW Mitral Stenosis: A Review By C. Richard Conti, MD, MACC 1 1 Department of Medicine,
HISTORY. Question: What type of heart disease is suggested by this history? CHIEF COMPLAINT: Decreasing exercise tolerance.
 HISTORY 15-year-old male. CHIEF COMPLAINT: Decreasing exercise tolerance. PRESENT ILLNESS: A heart murmur was noted in childhood, but subsequent medical care was sporadic. Easy fatigability and slight
HISTORY 15-year-old male. CHIEF COMPLAINT: Decreasing exercise tolerance. PRESENT ILLNESS: A heart murmur was noted in childhood, but subsequent medical care was sporadic. Easy fatigability and slight
Assessment and Diagnosis of Heart Failure
 Assessment and Diagnosis of Heart Failure Heart failure (HF) is a complex clinical syndrome resulting from any structural or functional impairment of ventricular filling or ejection of blood and is characterized
Assessment and Diagnosis of Heart Failure Heart failure (HF) is a complex clinical syndrome resulting from any structural or functional impairment of ventricular filling or ejection of blood and is characterized
ECG Workshop. Nezar Amir
 ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
Is it HF secondary to rheumatic heart disease???
 Is it HF secondary to rheumatic heart disease??? Is mitral regurg. Is complication of CHF??? Cardiomyopathy Definition The term cardiomyopathy is purely descriptive, meaning disease of the heart muscle
Is it HF secondary to rheumatic heart disease??? Is mitral regurg. Is complication of CHF??? Cardiomyopathy Definition The term cardiomyopathy is purely descriptive, meaning disease of the heart muscle
Stress Testing in Valvular Disease
 2017 ASE Florida Orlando, FL October 10, 2017 2:40 2:50 PM 10 min Grand Harbor Ballroom South Stress Testing in Valvular Disease Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology Echo Lab Associate
2017 ASE Florida Orlando, FL October 10, 2017 2:40 2:50 PM 10 min Grand Harbor Ballroom South Stress Testing in Valvular Disease Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology Echo Lab Associate
Pathophysiology: Heart Failure
 Pathophysiology: Heart Failure Mat Maurer, MD Irving Assistant Professor of Medicine Outline Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology Heart Failure: Definitions
Pathophysiology: Heart Failure Mat Maurer, MD Irving Assistant Professor of Medicine Outline Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology Heart Failure: Definitions
Heart Valve disease: MR. AS tough patient When to echo, When to refer, What s new
 Heart Valve disease: MR. AS tough patient When to echo, When to refer, What s new B. Sonnenberg UAH Cardiology CME Day 5 May 2015 Disclosures Speaker s or Advisory Boards: none Research grants: none (co-investigator
Heart Valve disease: MR. AS tough patient When to echo, When to refer, What s new B. Sonnenberg UAH Cardiology CME Day 5 May 2015 Disclosures Speaker s or Advisory Boards: none Research grants: none (co-investigator
Ischaemic heart disease. IInd Chair and Clinic of Cardiology
 Ischaemic heart disease IInd Chair and Clinic of Cardiology Definition Syndrome due to chronic insufficient oxygen supply to myocardial cells Nomenclature: ischaemic heart disease (IHD), coronary artery
Ischaemic heart disease IInd Chair and Clinic of Cardiology Definition Syndrome due to chronic insufficient oxygen supply to myocardial cells Nomenclature: ischaemic heart disease (IHD), coronary artery
Images in Cardiovascular Medicine
 Images in Cardiovascular Medicine Management of Severe Mitral Stenosis During Pregnancy Rebecca S. Norrad, MBBS; Omid Salehian, MSc, MD, FRCPC, FACC, FAHA A 37-year-old woman originally from Iraq was referred
Images in Cardiovascular Medicine Management of Severe Mitral Stenosis During Pregnancy Rebecca S. Norrad, MBBS; Omid Salehian, MSc, MD, FRCPC, FACC, FAHA A 37-year-old woman originally from Iraq was referred
The Ins and Outs of Cardiac Surgery. Stephanie Wold RN MN NP
 The Ins and Outs of Cardiac Surgery Stephanie Wold RN MN NP 1 The Ins and Outs of Cardiac Surgery Cardiac Surgery in a Nutshell 2 Outline Wait Times and Referral Process for Cardiac Surgery Getting Ready
The Ins and Outs of Cardiac Surgery Stephanie Wold RN MN NP 1 The Ins and Outs of Cardiac Surgery Cardiac Surgery in a Nutshell 2 Outline Wait Times and Referral Process for Cardiac Surgery Getting Ready
