ANTIHYPERTENSIVE AGENTS AND VASODILATORS. Lecture 5
|
|
|
- Phillip Dorsey
- 6 years ago
- Views:
Transcription
1 ANTIHYPERTENSIVE AGENTS AND VASODILATORS Lecture 5
2 Hypertension Blood pressure BP = CO x PVR n Interaction between autonomic nervous system, cardiovascular system and renal system Normal: 110/70 Prehypertension <130/90 Hypertension 130/90 Taken in 3 different office visits
3
4 Hypertension Etiology of HPN Primary or essential = no specific cause n Genetic risk Secondary n Hyperthyroidism n Pheochromocytoma n Renal disease n Diabetes n Obesity and dyslipidemia
5 Hypertension Hypertensive urgency BP 180/110 Hypertensive emergency Hypertensive urgency with end organ damage Ex. Hypertensive encephalopathy, angina, stroke, etc. Goal Decrease blood pressure to /90 Do not decrease more than 20% of MAP every hour n Proper brain perfusion
6 Hypertension Treatment Pharmacologic n Dependent on level of BP, presence of end-organ damage and presence of co-morbidities n Single/Mono-therapy vs combination therapy Non-pharmacologic n Diet and exercise n Salt restriction n Control co-morbidities (ex. DM) n Avoid other substances which may increase BP n Ex. cold remedies, caffeine, smoking, alcohol, contraceptives n Patient education
7 Introduction to antihypertensive agents 4 general mechanisms: 1. Decrease blood volume Decrease sodium = Diuretics 2. Sympathoplegic agents (sympatholytic) By vasodilation, ê cardiac function, é venous pooling 4 groups 3. Decrease PVR Direct vasodilators 4 groups 4. Inhibit RAAS Block production or action of angiotensin à ê PVR by vasodilation and decrease aldosterone effect
8 Diuretics Review of the renal system and urine formation RAAS system RAAS system through the juxtaglomerular apparatus Renin: increases aldosterone secretion via production of angiotensin. Angiotensin: increases aldosterone, anti-diuretic hormone, blood pressure and thirst. Aldosterone: increases active reabsorption of Na+ and secretion of K+ by the distal tubules
9
10
11 Diuretics Increase urine volume = depletes blood volume Basic MOA Inhibits NaCl transporter = ê reabsorption in the renal tubules = ê water reabsorption n Ex. furosemide (loop of Henle), hydrochlorthiazide (DCT) Aldosterone antagonism n Inhibits Na reabsorption from the DCT and collecting tubule n Ex. spironolactone Osmotic diuretic n Increase osmolarity of urine = ê water reabsorption n Ex. mannitol = only thru IV infusion Effect Can decrease BP by 10-15mmHg
12 Diuretics Side effects Hyponatremia Hypokalemia n Except for spironolactone (potassium sparing diuretic) Increases uric acid reabsorption n May precipitate gout May increase blood lipid levels
13 Sympathoplegic agents Drugs that act on the CNS Drugs that act on autonomic ganglia Drugs that reduce release of norepinephrine Drugs that block postsynaptic adrenoceptors
14 Centrally acting sympathoplegics Basic MOA: reduce sympathetic outflow from the brainstem à vasodilation Methyldopa Converted to α-methyldopamine and α- methylnorepinephrine n Replaces norepinephrine in the vesicles of the axon n A false sympathetic transmitter n Stimulates central alpha receptors = vasodilation n Safe for pregnant patients Side effect n Sedation and lactation
15 Centrally acting sympathoplegics Clonidine Stimulates central alpha receptors and arterial alpha receptors n Produces a brief rise in blood pressure followed by a more prolonged hypotension by inhibiting sympathetic stimulation from the medulla n Reduces heart rate and promotes vasodilation Side effects n Highly lipid soluble = easily enters the brain n Sedation and dry mouth (ê salivation)
16 Ganglion blocking agents Blocks ganglions of both sympathetic and parasympathetic nerves Too many side effects Not used anymore
17 Inhibit Norepinephrine release MOA: Inhibit release of NE from the axon Guanethidine Significant anti-sympathetic effect Inhibits release of NE as well as replaces NE in the vesicles = depleting NE stores Polar chemical = does not enter the CNS Side effects n Hypotension, diarrhea, impaired ejaculation or retrograde ejaculation
18
19 Inhibit Norepinephrine release Reserpine Decreases norepinephrine production by inhibiting VMAT (vesicular membrane associated transporter) Decreases sympathetic activity Side effects n Affects brain and peripheral nerves n Sedation, lassitude, nightmares and mental depression
20 Adrenoceptor Antagonists Alpha and beta blockers α1 blockers (-zosin) Prazosin, terazosin, doxazosin Dilates arterioles and venules Concomitant salt and water retention Also useful for men with urinary bladder obstruction such as BPH n Relaxes prostate muscle Side effect n 1 st dose phenomenon = sudden drop in BP after the 1 st dose n 1 st dose should be a small dose, succeeding doses may be increased.
21 Adrenoceptor Antagonists = Opposite effect Type Tissue location Action α1 Most vascular smooth muscle Contraction Pupillary dilator muscle Pilomotor smooth muscle Prostate Heart Contraction (dilates pupil) Erects hair Contraction é inotropy α2 Post synaptic CNS neurons Probably multiple (ê BP) Platelets Adrenergic and cholinergic nerve terminals Some vascular smooth muscle Fat cells Aggregation Inhibits transmitter release Contraction Inhibits lipolysis
22 Adrenoceptor Antagonists = Opposite effect Type Tissue location Action β1 Heart, juxtaglomerular cells é chronotropy and inotropy é renin release β2 Respiratory, uterine and vascular smooth muscle Skeletal muscle Human liver Smooth muscle relaxation β3 Fat cells lipolysis é Potassium uptake Activates glycogenolysis D1 Smooth muscle Dilates renal blood vessels D2 Nerve endings Modulates transmitter release
23 Adrenoceptor Antagonists β blockers Propanolol Non-selective beta blocker Decreases HR Inhibits stimulation renin production Decreased sympathetic activity à decreased BP Side effect n Bradycardia n Asthma (promote bronchoconstriction) n Diabetes (inc. blood glucose)
24 Adrenoceptor Antagonists β blockers Metoprolol and atenolol Selective β1 antagonist = ê HR Extensively metabolized by liver enzymes (Cyt P450) Better for asthmatic and diabetic patients Other beta1 blockers Nadolol, carteolol, pindolol, acebutolol, labetalol, carvedilol, esmolol.
25 Direct Vasodilators Mechanism Release of nitric oxide from endothelium Reduction of calcium influx Hyperpolarization of smooth muscle membrane through opening of potassium channels Activation of dopamine receptors Examples Nitroprusside, hryalazine, nitrates Calcium channel blockers Minoxidil, diazoxide Fenoldopam
26
27
28
29 Direct Vasodilators Arteriodilators Venodilators Both Hydralazine Minoxidil Diazoxide Fenoldopam CCB s Nitrates Na nitroprusside ACEI and ARB Centrally acting alpha1 blockers
30 Direct Vasodilators Sodium nitroprusside MOA: release of NO to endothelium n By activation of guanylyl cyclase à vessel relaxation Only parenterally administered (no oral preparation) Used for hypertensive emergencies n Rapidly lowers blood pressure within minutes n Effects disappear rapidly as well. Side effects n Metabolized to cyanide, which is then metabolized to thiocyanate (less toxic form) n Cyanide poisoning (metabolic acidosis, arrythmias, hypotension) n Take hydroxycobalamin (Vit B12) to combine with cyanide to create an inert compound (cyanocobalamin)
31 Direct Vasodilators Hydralazine Arteriodilator MOA: release of nitric oxide For initial therapy of severe hypertension Side effects n Tachyphylaxis = cannot be used over long periods n Headache, nausea, anorexia n Lupus like syndrome = arthralgia, myalgia, skin rash, fever n Disappears after discontinuation of drug
32 Direct Vasodilators Nitrates or nitrites Nitroglycerin, isosorbide dinitrate, isosorbide mononitrate, nitric oxide Vasodilator (both arteries and veins) n Relaxes all smooth muscles (no effect on cardiac or skeletal muscles) MOA: releases nitric oxide in endothelium which relaxes blood vessels Rapidly metaboized by the liver into inactive substances n Preferred route is sublingual, which bypasses the liver n Except isosorbide mononitrate (good for oral route)
33 Direct Vasodilators Nitrates or nitrites Effect n Rapid onset of action and short duration n Decreases preload (venodilation) n Not good for normal hearts n Good for heart failure and heart overload n Dilates coronary blood vessels = increase flow n Slight decrease in platelet aggregation n Decreases afterload (arteriodilation)
34 Direct Vasodilators Nitrates or nitrites Side effects n Tolerance = cannot be used over several days n Reflex sympathetic response n Headache = dilation of cerebral arteries = throbbing or pulsating headache
35 Direct Vasodilators Calcium Channel Blockers (CCB) 2 groups Dihydropyridines n -dipine Non-dihydropyridines n Verapamil n Diltiazem MOA: inhibits calcium influx into vascular smooth muscles, thus decreasing muscle contractility of the blood vessels Vasodilator: Arteries > veins
36 Direct Vasodilators Calcium Channel Blockers (CCB) Dihydropyridines n Amlodipine, nifedipine, nicardipine, felodipine n Blocks calcium channels in blood vessels = vasodilation n Side effects n Headache n Reflex tachycardia
37 Direct Vasodilators Calcium Channel Blockers (CCB) Non-dihydropyridines n Verapamil n Modest vasodilation n Blocks cardiac contractility and significant SA and AV node conduction n Decreases HR = ê workload of heart n Diltiazem n Modest vasodilation n Blocks cardiac contractility and moderate SA and AV node conduction n Decreases HR = ê workload of heart
38 Direct Vasodilators Minoxidil MOA: hyperpolarization of smooth muscle (K channels) Arteriodilator Side effect n Hypertrichosis = used as a topical agent
39 Direct Vasodilators Diazoxide MOA: hyperpolarization of resting membrane potential by opening K channels Arteriodilator Side effect n Excessive hypotension n Inhibits insulin release
40 Direct Vasodilators Fenoldopam MOA: dopamine1 (D1) receptor agonist Arteriodilator Side effect n Increases intraocular pressure (not good for glaucoma patients)
41 Angiotensin blockers Review of the renal system and urine formation RAAS system RAAS system through the juxtaglomerular apparatus Aldosterone: increases active reabsorption of Na+ and secretion of K+ by the distal tubules Renin: increases aldosterone secretion via production of angiotensin. Angiotensin: increases aldosterone, anti-diuretic hormone, blood pressure and thirst. n Angiotensin II = vasoconstrictor
42
43 Angiotensin blockers RAAS system Renin is released from the kidneys (JG-App) Renin acts upon angiotensinogen to form Angiotensin I Angiotensin I is converted to Angiotensin II by ACE (Angiotensin converting enzyme) in the lungs Angiotensin II is converted to Antiogensin III in the adrenal gland n Angiotensin II and III stimulate aldosterone release à sodium and water reabsorption
44
45 Angiotensin blockers ACE inhibtors -pril ARB s (Antiogensin receptor blockers -sartan Aldosterone antagonists (diuretic) Renin antagonist aliskiren
46 Angiotensin blockers ACE inhibitors Captopril, enalapril, perindopril, quinapril, etc. Inhibits conversion of angiotensin I to angiotensin II n Prevents vasoconstriction and aldosterone secretion Prevents inactivation of bradykinin n Stimulates release of NO à vasodilation No reflex sympathetic activation à good for patients with heart failure Diminishes proteinuria and stabilizes renal function n Especially good for patients with kidney problems or diabetes
47 Angiotensin blockers ACE inhibitors Side effects n Hyperkalemia (potassium sparing effect) n Possible drug interactions with diuretics n Dry cough (due to accumulation of bradykinin) n Angioedema n Contraindicated during pregnancy
48 Angiotensin blockers Angiotensin receptor blockers (ARB) Losartan, valsartan, candesartan, telmisartan Similar effect with ACE inhibitors n Except no accumulation of bradykinin = less cough side effect n Decreased proteinuria and improved renal function n No sympathetic reflex response to vasodilation Contraindicated in pregnancy
49 Angina pectoris Chest pain from myocardial ischemia Due to lack of blood flow to heart muscles Blockage of coronary arteries (CAD or coronary artery disease) n 2 types n Stable angina n Classic angina (effort angina) = atheromatous obstruction of coronaries, manifesting during effort or exercise n Unstable angina
50 Angina pectoris Unstable angina or acute coronary syndrome n When episodes of angina occur at rest, or when there is an increase in severity, frequency and duration of chest pain in patients with previously stable angina n Progressive blockage of the coronaries due to platelet plug or other occlusive thrombi Special type of angina Prinzmetal angina (vasospastic angina) = transient spasm of localized portions of the coronaries (also due to atheromatous obstruction) May be stable or unstable
51 Angina pectoris Coronary blood flow Due to perfusion pressure (aortic diastolic pressure) and duration of diastole n Blood flows to coronary arteries only during diastole Inversely proportional to coronary vascular resistance
52 Angina pectoris Treatment Decrease oxygen demand (decrease workload of heart) n Increase contractility n Decrease heart rate = beta blockers n Decrease blood pressure or peripheral vascular resistance Increase delivery (increase coronary blood flow) n Dilate vessels and prolong diastolic time n Vasodilators and beta blockers n Remove blockage or atherosclerosis n Anti hyperlipidemics, anti-platelets
53 Angina pectoris Treatment Nitrates Potential benefits Effect of Nitrates ê ventricular volume ê arterial pressure ê ejection time vasodilation of coronary arteries é collateral flow ê LV diastolic pressure Result ê Myocardial O2 requirement Relief of coronary artery spasm é Perfusion to ischemic myocardium é Subendocardial perfusion
54 Angina pectoris Effect of Nitrates Potential deletirious effects Reflex tachycardia Reflex é in contractility ê diastolic perfusion time due to tachycardia Result é Myocardial O2 demand ê Coronary perfusion
55 Erectile dysfunction Due to atherosclerosis of vascular bed in penis Promote vasodilation to increase blood flow to penis and erectile tissue Deadly interaction with nitrates Severe hypotension 6 hour interval between nitrates and sildenafil
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs
 Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Antihypertensive Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
sympatholytics sympatholytics sympatholytics
 sympatholytics sympatholytics sympatholytics CNS-ACTING SYMPATHOPLEGICS Sympathetic brain signals Doesn t affect baroreceptor reflex (no orthostatic hypotension) Methyldopa α-methylne crosses BBB (+) α-adrenoreceptors
sympatholytics sympatholytics sympatholytics CNS-ACTING SYMPATHOPLEGICS Sympathetic brain signals Doesn t affect baroreceptor reflex (no orthostatic hypotension) Methyldopa α-methylne crosses BBB (+) α-adrenoreceptors
HYPERTENSION: Sustained elevation of arterial blood pressure above normal o Systolic 140 mm Hg and/or o Diastolic 90 mm Hg
 Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Antihypertensives. Antihypertensive Classes. RAAS Inhibitors. Renin-Angiotensin Cascade. Angiotensin Receptors. Approaches to Hypertension Treatment
 Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
Section 3, Lecture 2
 59-291 Section 3, Lecture 2 Diuretics: -increase in Na + excretion (naturesis) Thiazide and Related diuretics -decreased PVR due to decreases muscle contraction -an economical and effective treatment -protect
59-291 Section 3, Lecture 2 Diuretics: -increase in Na + excretion (naturesis) Thiazide and Related diuretics -decreased PVR due to decreases muscle contraction -an economical and effective treatment -protect
AUTONOMIC DRUGS: ADRENOCEPTOR AGONISTS AND SYMPATHOMIMETICS. Lecture 4
 AUTONOMIC DRUGS: ADRENOCEPTOR AGONISTS AND SYMPATHOMIMETICS Lecture 4 Introduction (review) 5 key features of neurotransmitter function, which can be targets for pharmacotherapy Synthesis Storage Release
AUTONOMIC DRUGS: ADRENOCEPTOR AGONISTS AND SYMPATHOMIMETICS Lecture 4 Introduction (review) 5 key features of neurotransmitter function, which can be targets for pharmacotherapy Synthesis Storage Release
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias
 1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
Beta 1 Beta blockers A - Propranolol,
 Pharma Lecture 3 Beta blockers that we are most interested in are the ones that target Beta 1 receptors. Beta blockers A - Propranolol, it s a non-selective competitive antagonist of beta 1 and beta 2
Pharma Lecture 3 Beta blockers that we are most interested in are the ones that target Beta 1 receptors. Beta blockers A - Propranolol, it s a non-selective competitive antagonist of beta 1 and beta 2
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood:
 Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
7/7/ CHD/MI LVH and LV dysfunction Dysrrhythmias Stroke PVD Renal insufficiency and failure Retinopathy. Normal <120 Prehypertension
 Prevalence of Hypertension Hypertension: Diagnosis and Management T. Villela, M.D. Program Director University of California, San Francisco-San Francisco General Hospital Family and Community Medicine
Prevalence of Hypertension Hypertension: Diagnosis and Management T. Villela, M.D. Program Director University of California, San Francisco-San Francisco General Hospital Family and Community Medicine
Antihypertensive drugs SUMMARY Made by: Lama Shatat
 Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Antihypertensive Agents
 Antihypertensive Agents Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Süzer Farmakoloji 3. Baskı 2005
Antihypertensive Agents Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Süzer Farmakoloji 3. Baskı 2005
Hypertension (JNC-8)
 Hypertension (JNC-8) Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 17, 2018, presented by Ezra Levy, Pharm.D.! The 8 th Joint
Hypertension (JNC-8) Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 17, 2018, presented by Ezra Levy, Pharm.D.! The 8 th Joint
Introduction. Factors affecting blood pressure: 1-COP = HR X SV mainly affect SBP. 2-TPR = diameter of arterioles X viscosity of blood affect DBP
 Introduction Hypertension is a persistent elevation of blood pressure above 140 / 90 mmhg for more than three sitting. (0ptimal level
Introduction Hypertension is a persistent elevation of blood pressure above 140 / 90 mmhg for more than three sitting. (0ptimal level
Chapter 23. Media Directory. Cardiovascular Disease (CVD) Hypertension: Classified into Three Categories
 Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Management of Hypertension
 Clinical Practice Guidelines Management of Hypertension Definition and classification of blood pressure levels (mmhg) Category Systolic Diastolic Normal
Clinical Practice Guidelines Management of Hypertension Definition and classification of blood pressure levels (mmhg) Category Systolic Diastolic Normal
Angina Pectoris. Edward JN Ishac, Ph.D. Smith Building, Room
 Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University
Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University
HYPERTENSION IN EMERGENCY MEDICINE Michael Jay Bresler, M.D., FACEP
 HYPERTENSION IN EMERGENCY MEDICINE Michael Jay Bresler, M.D., FACEP What is normal blood pressure? Prehypertension 130-139/80-90 Compared with normal BP Double the risk for developing hypertension. Lifestyle
HYPERTENSION IN EMERGENCY MEDICINE Michael Jay Bresler, M.D., FACEP What is normal blood pressure? Prehypertension 130-139/80-90 Compared with normal BP Double the risk for developing hypertension. Lifestyle
Pharmacology. Drugs affecting the Cardiovascular system (Antianginal Drugs)
 Lecture 7 (year3) Dr Noor Al-Hasani Pharmacology University of Baghdad College of dentistry Drugs affecting the Cardiovascular system (Antianginal Drugs) Atherosclerotic disease of the coronary arteries,
Lecture 7 (year3) Dr Noor Al-Hasani Pharmacology University of Baghdad College of dentistry Drugs affecting the Cardiovascular system (Antianginal Drugs) Atherosclerotic disease of the coronary arteries,
ANTIHYPERTENSIVE DRUGS
 ANTIHYPERTENSIVE DRUGS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: September 28, 2010 Materials on: Exam #3 Required reading: Katzung, Chapter 11 1 1 in 3 adults HYPERTENSION 64% of
ANTIHYPERTENSIVE DRUGS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: September 28, 2010 Materials on: Exam #3 Required reading: Katzung, Chapter 11 1 1 in 3 adults HYPERTENSION 64% of
Antihypertensive Agents
 Antihypertensive Agents Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 7, 08, presented by Ezra Levy, Pharm.D! Usual Dose,
Antihypertensive Agents Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 7, 08, presented by Ezra Levy, Pharm.D! Usual Dose,
University of Al Qadisiyah College of Pharmacy Dr. Bassim I Mohammad, MBChB, MSc, Ph.D
 University of Al Qadisiyah College of Pharmacy Dr. Bassim I Mohammad, MBChB, MSc, Ph.D Cardiovascular Pharmacology 1. Antihypertensives 2. Antianginal 3. Drugs for HF 4. Antiarrythemics 5. Drugs for Hyperlipoproteniemia
University of Al Qadisiyah College of Pharmacy Dr. Bassim I Mohammad, MBChB, MSc, Ph.D Cardiovascular Pharmacology 1. Antihypertensives 2. Antianginal 3. Drugs for HF 4. Antiarrythemics 5. Drugs for Hyperlipoproteniemia
DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI
 DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI 3. Vasodilators Drugs which dilate blood vessels ( decrease peripheral vascular resistance) by acting on smooth muscle cells through non-autonomic mechanisms:
DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI 3. Vasodilators Drugs which dilate blood vessels ( decrease peripheral vascular resistance) by acting on smooth muscle cells through non-autonomic mechanisms:
Treatment of Essential Hypertension
 2016 edition by Mark A. Simmons, PhD Department of Pharmaceutical Sciences School of Pharmacy University of Maryland Eastern Shore Originally developed by Hugh J. Burford, PhD, FCP Department of Pharmacology
2016 edition by Mark A. Simmons, PhD Department of Pharmaceutical Sciences School of Pharmacy University of Maryland Eastern Shore Originally developed by Hugh J. Burford, PhD, FCP Department of Pharmacology
Angina Pectoris Dr. Shariq Syed
 Angina Pectoris Dr. Syed 1 What is Angina Pectoris (AP)? Commonly known as angina is chest pain often due to ischemia of the heart muscle, Because of obstruction or spasm of the coronary arteries 2 What
Angina Pectoris Dr. Syed 1 What is Angina Pectoris (AP)? Commonly known as angina is chest pain often due to ischemia of the heart muscle, Because of obstruction or spasm of the coronary arteries 2 What
Antihypertensive Agents
 1. Blood Pressure Regulation Antihypertensive Agents - 2007 Edward JN Ishac. Ph.D. Associate Professor, Dept. Pharmacology & Toxicology Office: Smith 742; Tel: 828 2127 eishac@hsc.vcu.edu Frank's formula,
1. Blood Pressure Regulation Antihypertensive Agents - 2007 Edward JN Ishac. Ph.D. Associate Professor, Dept. Pharmacology & Toxicology Office: Smith 742; Tel: 828 2127 eishac@hsc.vcu.edu Frank's formula,
Hypertension Update. Objectives 4/28/2015. Beverly J. Mathis, D.O. OOA May 2015
 Hypertension Update Beverly J. Mathis, D.O. OOA May 2015 Objectives Learn new recommendations for BP treatment goals Approach to hypertension in the office Use of hypertensive drugs, and how to tailor
Hypertension Update Beverly J. Mathis, D.O. OOA May 2015 Objectives Learn new recommendations for BP treatment goals Approach to hypertension in the office Use of hypertensive drugs, and how to tailor
Antihypertensive Drugs. Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014
 Antihypertensive Drugs Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Antihypertensive Drugs What is Hypertension: A common, incurable, persistent, but usually
Antihypertensive Drugs Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Antihypertensive Drugs What is Hypertension: A common, incurable, persistent, but usually
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Antihypertensives. Diagnostic category
 Measurement of blood pressure At first assessment, take both arms then choose the one with the higher reading. Beware of orthostatic hypotension. Measure BP in sitting position, and repeat after patient
Measurement of blood pressure At first assessment, take both arms then choose the one with the higher reading. Beware of orthostatic hypotension. Measure BP in sitting position, and repeat after patient
Prof dr Aleksandar Raskovic DIRECT VASODILATORS
 Prof dr Aleksandar Raskovic DIRECT VASODILATORS Direct vasodilators Minoxidil (one of the most powerful peripheral arterial dilators) Opening of KATP channels, efflux of K, lose of Ca and smooth muscle
Prof dr Aleksandar Raskovic DIRECT VASODILATORS Direct vasodilators Minoxidil (one of the most powerful peripheral arterial dilators) Opening of KATP channels, efflux of K, lose of Ca and smooth muscle
Pharmacotherapy of Angina Pectoris
 Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Pharmacotherapy of Angina Pectoris
 Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Hypertension. Penny Mosley MRPharmS
 Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Treatment of Essential Hypertension
 2016 edition by Mark A. Simmons, PhD Department of Pharmaceutical Sciences School of Pharmacy University of Maryland Eastern Shore Originally developed by Hugh J. Burford, PhD, FCP Department of Pharmacology
2016 edition by Mark A. Simmons, PhD Department of Pharmaceutical Sciences School of Pharmacy University of Maryland Eastern Shore Originally developed by Hugh J. Burford, PhD, FCP Department of Pharmacology
Categories of HTN. Overview of Hypertension. Types of Hypertension
 Categories of HTN Overview of Hypertension Normal SBP 100 Quick review of the Basics: What is
Categories of HTN Overview of Hypertension Normal SBP 100 Quick review of the Basics: What is
Antihypertensive Drugs. Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan October, 2017
 Antihypertensive Drugs Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan October, 2017 Antihypertensive Drugs What is Hypertension? A common, incurable, persistent, but usually
Antihypertensive Drugs Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan October, 2017 Antihypertensive Drugs What is Hypertension? A common, incurable, persistent, but usually
ANTIHYPERTENSIVES. Assoc. Prof. Bilgen Başgut
 ANTIHYPERTENSIVES Assoc. Prof. Bilgen Başgut Hypertension Hypertension is a condition in which the blood pressure is persistently higher than normal Hypertension > 140 mmhg > 90 mmhg Systolic Blood Pressure
ANTIHYPERTENSIVES Assoc. Prof. Bilgen Başgut Hypertension Hypertension is a condition in which the blood pressure is persistently higher than normal Hypertension > 140 mmhg > 90 mmhg Systolic Blood Pressure
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS)
 DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
Chapter 10 Worksheet Blood Pressure and Antithrombotic Agents
 Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Autonomic Nervous System. Introduction
 Autonomic Nervous System Introduction 1 The nervous system is divided into: 1- the central nervous system (CNS; the brain and spinal cord) 2- the peripheral nervous system (PNS; neuronal tissues outside
Autonomic Nervous System Introduction 1 The nervous system is divided into: 1- the central nervous system (CNS; the brain and spinal cord) 2- the peripheral nervous system (PNS; neuronal tissues outside
Drug Treatment of Ischemic Heart Disease
 Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Antihypertensive drugs: I. Thiazide and other diuretics:
 Clinical assessment of hypertensive patient: You have to take history regarding the presence of other risk factors for CAb like diabetes mellitus, smoking, etc. Take history whether the patient takes medications
Clinical assessment of hypertensive patient: You have to take history regarding the presence of other risk factors for CAb like diabetes mellitus, smoking, etc. Take history whether the patient takes medications
Treatment of T Angina reatment of By Ali Alalawi
 Treatment of Angina By Ali Alalawi Determinants of Oxygen Demand Need to improve ratio of: Coronary blood flow / cardiac work Or Cardiac O2 Supply / Cardiac Requirement Coronary Circulation vs Other Circulation
Treatment of Angina By Ali Alalawi Determinants of Oxygen Demand Need to improve ratio of: Coronary blood flow / cardiac work Or Cardiac O2 Supply / Cardiac Requirement Coronary Circulation vs Other Circulation
Cardiac Drugs: Chapter 9 Worksheet Cardiac Agents. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate.
 Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Hypertension Management - Summary
 Who should have blood pressure assessed? Hypertension Management - Summary All patients over the age of 40 years, every 1-3 years in order to determine their cardiovascular risk (ie. Framingham Risk Score)
Who should have blood pressure assessed? Hypertension Management - Summary All patients over the age of 40 years, every 1-3 years in order to determine their cardiovascular risk (ie. Framingham Risk Score)
Cardiovascular drugs
 chapter 13 Cardiovascular drugs Cardiovascular drugs act on the heart or blood vessels to control the cardiovascular system. They are used to treat a variety of conditions from hypertension to chronic
chapter 13 Cardiovascular drugs Cardiovascular drugs act on the heart or blood vessels to control the cardiovascular system. They are used to treat a variety of conditions from hypertension to chronic
Dr. Vishaal Bhat. anti-adrenergic drugs
 Dr. Vishaal Bhat anti-adrenergic drugs Divisions of human nervous system Human Nervous system Central Nervous System Peripheral Nervous System Autonomic Nervous System Nervous system Includes neurons and
Dr. Vishaal Bhat anti-adrenergic drugs Divisions of human nervous system Human Nervous system Central Nervous System Peripheral Nervous System Autonomic Nervous System Nervous system Includes neurons and
Drug Treatment of Ischemic Heart Disease
 Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan November, 2017 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan November, 2017 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Heart failure. Failure? blood supply insufficient for body needs. CHF = congestive heart failure. increased blood volume, interstitial fluid
 Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
Hypertensives Emergency and Urgency
 Hypertensives Emergency and Urgency Budi Yuli Setianto Cardiology Divisision Department of Internal Medicine Faculty of Medicine UGM Sardjito Hospital Yogyakarta Background USA: Hypertension is 30% of
Hypertensives Emergency and Urgency Budi Yuli Setianto Cardiology Divisision Department of Internal Medicine Faculty of Medicine UGM Sardjito Hospital Yogyakarta Background USA: Hypertension is 30% of
Antianginal Drugs 18 I. OVERVIEW II. TYPES OF ANGINA
 Antianginal Drugs 18 I. OVERVIEW Atherosclerotic disease of the coronary arteries, also known as coronary artery disease or ischemic heart disease, is the most common cause of mortality around the world.
Antianginal Drugs 18 I. OVERVIEW Atherosclerotic disease of the coronary arteries, also known as coronary artery disease or ischemic heart disease, is the most common cause of mortality around the world.
DRUGS USED IN ANGINA PECTORIS
 DRUGS USED IN ANGINA PECTORIS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 16, 2010 Materials on: Exam #7 Required reading: Katzung, Chapter 12 1 TYPES OF ISCHEMIC HEART DISEASE
DRUGS USED IN ANGINA PECTORIS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 16, 2010 Materials on: Exam #7 Required reading: Katzung, Chapter 12 1 TYPES OF ISCHEMIC HEART DISEASE
HypertensionTreatment Guidelines. Michaelene Urban APRN, MSN, ACNS-BC, ANP-BC
 HypertensionTreatment Guidelines Michaelene Urban APRN, MSN, ACNS-BC, ANP-BC Objectives: Review the definition of the different stages of HTN. Review the current guidelines for treatment of HTN. Provided
HypertensionTreatment Guidelines Michaelene Urban APRN, MSN, ACNS-BC, ANP-BC Objectives: Review the definition of the different stages of HTN. Review the current guidelines for treatment of HTN. Provided
ANGINA PECTORIS. angina pectoris is a symptom of myocardial ischemia in the absence of infarction
 Pharmacology Ezra Levy, Pharm.D. ANGINA PECTORIS A. Definition angina pectoris is a symptom of myocardial ischemia in the absence of infarction angina usually implies severe chest pain or discomfort during
Pharmacology Ezra Levy, Pharm.D. ANGINA PECTORIS A. Definition angina pectoris is a symptom of myocardial ischemia in the absence of infarction angina usually implies severe chest pain or discomfort during
Byvalson. (nebivolol, valsartan) New Product Slideshow
 Byvalson (nebivolol, valsartan) New Product Slideshow Introduction Brand name: Byvalson Generic name: Nebivolol, valsartan Pharmacological class: Beta-blocker + angiotensin II receptor blocker (ARB) Strength
Byvalson (nebivolol, valsartan) New Product Slideshow Introduction Brand name: Byvalson Generic name: Nebivolol, valsartan Pharmacological class: Beta-blocker + angiotensin II receptor blocker (ARB) Strength
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina
 Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Heart Failure. Subjective SOB (shortness of breath) Peripheral edema. Orthopnea (2-3 pillows) PND (paroxysmal nocturnal dyspnea)
 Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Antihypertensive Drugs. Nafrialdi
 Antihypertensive Drugs Nafrialdi 1 Mechanisms of Blood Pressure Regulation Blood Presure Cardiac Output Peripheral Resistance Heart Rate Stroke volume Vascular tone Vessel elasticity Myocardial contractility
Antihypertensive Drugs Nafrialdi 1 Mechanisms of Blood Pressure Regulation Blood Presure Cardiac Output Peripheral Resistance Heart Rate Stroke volume Vascular tone Vessel elasticity Myocardial contractility
M2 TEACHING UNDERSTANDING PHARMACOLOGY
 M2 TEACHING UNDERSTANDING PHARMACOLOGY USING CVS SYSTEM AS AN EXAMPLE NIGEL FONG 2 JAN 2014 TODAY S OBJECTIVE Pharmacology often seems like an endless list of mechanisms and side effects to memorize. To
M2 TEACHING UNDERSTANDING PHARMACOLOGY USING CVS SYSTEM AS AN EXAMPLE NIGEL FONG 2 JAN 2014 TODAY S OBJECTIVE Pharmacology often seems like an endless list of mechanisms and side effects to memorize. To
What in the World is Functional Medicine?
 What in the World is Functional Medicine? An Introduction to a Systems Based Approach of Chronic Disease Meneah R Haworth, FNP-C Disclosure v I am a student of the Institute for Functional Medicine. They
What in the World is Functional Medicine? An Introduction to a Systems Based Approach of Chronic Disease Meneah R Haworth, FNP-C Disclosure v I am a student of the Institute for Functional Medicine. They
Angiotensin-converting enzyme inhibitor (ACEI)
 Aldosterone Alpha1 blockers Alpha 2 blockers Angina pectoris Week Four Terms and Meds to Know In the renin-angiotensin-aldosterone system. Helps regulate sodium, wherever this goes sodium goes in turn
Aldosterone Alpha1 blockers Alpha 2 blockers Angina pectoris Week Four Terms and Meds to Know In the renin-angiotensin-aldosterone system. Helps regulate sodium, wherever this goes sodium goes in turn
Top 200 Section 4. Cardiovascular Drugs
 Top 200 Section 4 Cardiovascular Drugs Objectives After finishing this presentation the audience should be able to: Describe conditions/disease states that would make a person a candidate for drug therapy.
Top 200 Section 4 Cardiovascular Drugs Objectives After finishing this presentation the audience should be able to: Describe conditions/disease states that would make a person a candidate for drug therapy.
Pharmacology of the Sympathetic Nervous System II
 Pharmacology of the Sympathetic Nervous System II Edward JN Ishac, Ph.D. Professor Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Pharmacology of the Sympathetic Nervous System II Edward JN Ishac, Ph.D. Professor Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
HEART FAILURE PHARMACOLOGY. University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
Heart Failure Clinician Guide JANUARY 2018
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2018 Introduction This evidence-based guideline summary is based on the 2018 National Heart Failure Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2018 Introduction This evidence-based guideline summary is based on the 2018 National Heart Failure Guideline.
Chapter 2 ~ Cardiovascular system
 Chapter 2 ~ Cardiovascular System: General Section 1 of 6 Chapter 2 ~ Cardiovascular system 2.1 Positive inotropic drugs 2.1.1 Cardiac glycosides DIGOXIN 2.2 Diuretics Elixir 50micrograms in 1ml Injection
Chapter 2 ~ Cardiovascular System: General Section 1 of 6 Chapter 2 ~ Cardiovascular system 2.1 Positive inotropic drugs 2.1.1 Cardiac glycosides DIGOXIN 2.2 Diuretics Elixir 50micrograms in 1ml Injection
Autonomic Nervous System
 Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
New classification of HT Systolic Diastolic Normal <120 <80 Prehypertension Stage1HT Stage 2 HT >160 or >100
 Hypertension 1 Definition Hypertension can be defined as a condition where blood pressure is elevated to an extent that clinical benefit is obtained from blood pressure lowering. it is an important risk
Hypertension 1 Definition Hypertension can be defined as a condition where blood pressure is elevated to an extent that clinical benefit is obtained from blood pressure lowering. it is an important risk
Hypertension Update Warwick Jaffe Interventional Cardiologist Ascot Hospital
 Hypertension Update 2008 Warwick Jaffe Interventional Cardiologist Ascot Hospital Definition of Hypertension Continuous variable At some point the risk becomes high enough to justify treatment Treatment
Hypertension Update 2008 Warwick Jaffe Interventional Cardiologist Ascot Hospital Definition of Hypertension Continuous variable At some point the risk becomes high enough to justify treatment Treatment
Angina pectoris due to coronary atherosclerosis : Atenolol is indicated for the long term management of patients with angina pectoris.
 Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
Chapter (9) Calcium Antagonists
 Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Beta-blockers. Atenolol. Propranolol. Bisoprolol. Metoprolol. Labetalol. Carvedilol.
 Drugs of CVS Beta-blockers Atenolol. Propranolol. Bisoprolol. Metoprolol. Labetalol. Carvedilol. Atenolol.cardioselective Propranolol, nonselective Bisoprolol, cardioselective Metoprolol Carvedilol, alpha
Drugs of CVS Beta-blockers Atenolol. Propranolol. Bisoprolol. Metoprolol. Labetalol. Carvedilol. Atenolol.cardioselective Propranolol, nonselective Bisoprolol, cardioselective Metoprolol Carvedilol, alpha
Difficult to Treat Hypertension
 Difficult to Treat Hypertension According to Goldilocks JNC 8 Blood Pressure Goals (2014) BP Goal 60 years old and greater*- systolic < 150 and diastolic < 90. (Grade A)** BP Goal 18-59 years old* diastolic
Difficult to Treat Hypertension According to Goldilocks JNC 8 Blood Pressure Goals (2014) BP Goal 60 years old and greater*- systolic < 150 and diastolic < 90. (Grade A)** BP Goal 18-59 years old* diastolic
Heart Failure. Dr. Alia Shatanawi
 Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Heart Failure Clinician Guide JANUARY 2016
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2016 Introduction This evidence-based guideline summary is based on the 2016 National Heart Failure Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2016 Introduction This evidence-based guideline summary is based on the 2016 National Heart Failure Guideline.
Cardiac Pathophysiology
 Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Hypertension diagnosis (see detail document) Diabetic. Target less than 130/80mmHg
 Hypertension diagnosis (see detail document) Non-diabetic Diabetic Very elderly (older than 80 years) Target less than 140/90mmHg Target less than 130/80mmHg Consider SBP target less than 150mmHg Non-diabetic
Hypertension diagnosis (see detail document) Non-diabetic Diabetic Very elderly (older than 80 years) Target less than 140/90mmHg Target less than 130/80mmHg Consider SBP target less than 150mmHg Non-diabetic
Hypertension is also an important risk factor in the development of chronic kidney disease and heart failure.
 Hypertension Hypertension Hypertension is defined as either a sustained systolic blood pressure of greater than 140 mm Hg or a sustained diastolic blood pressure of greater than 90 mm Hg. Hypertension
Hypertension Hypertension Hypertension is defined as either a sustained systolic blood pressure of greater than 140 mm Hg or a sustained diastolic blood pressure of greater than 90 mm Hg. Hypertension
Adrenergic agonists Sympathomimetic drugs. ANS Pharmacology Lecture 4 Dr. Hiwa K. Saaed College of Pharmacy/University of Sulaimani
 Adrenergic agonists Sympathomimetic drugs ANS Pharmacology Lecture 4 Dr. Hiwa K. Saaed College of Pharmacy/University of Sulaimani 2017-2018 Adrenergic agonists The adrenergic drugs affect receptors that
Adrenergic agonists Sympathomimetic drugs ANS Pharmacology Lecture 4 Dr. Hiwa K. Saaed College of Pharmacy/University of Sulaimani 2017-2018 Adrenergic agonists The adrenergic drugs affect receptors that
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
HYPERTENSION IN CKD. LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL
 HYPERTENSION IN CKD LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL Stages in Progression of Chronic Kidney Disease and Therapeutic Strategies Complications Normal Increased risk Damage GFR
HYPERTENSION IN CKD LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL Stages in Progression of Chronic Kidney Disease and Therapeutic Strategies Complications Normal Increased risk Damage GFR
Lujain Hamdan. Ayman Musleh & Yahya Salem. Mohammed khatatbeh
 12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
Dr Narender Goel MD (Internal Medicine and Nephrology) Financial Disclosure: None, Conflict of Interest: None
 Dr Narender Goel MD (Internal Medicine and Nephrology) drnarendergoel@gmail.com Financial Disclosure: None, Conflict of Interest: None 12 th December 2013, New York Visit us at: http://kidneyscience.info/
Dr Narender Goel MD (Internal Medicine and Nephrology) drnarendergoel@gmail.com Financial Disclosure: None, Conflict of Interest: None 12 th December 2013, New York Visit us at: http://kidneyscience.info/
Autonomic Pharmacology
 Autonomic Pharmacology ADRENERGIC RECEPTOR BLOCKERS Adrenergic-receptor antagonists block the effects of sympathetic stimulation and adrenergic agonists mediated through - and -receptors. Adrenergic receptor
Autonomic Pharmacology ADRENERGIC RECEPTOR BLOCKERS Adrenergic-receptor antagonists block the effects of sympathetic stimulation and adrenergic agonists mediated through - and -receptors. Adrenergic receptor
5 4_part2. Aya Alomoush. Alia Shatanawi
 5 4_part2 Aya Alomoush Alia Shatanawi 1 P a g e This sheet will talk about vasodilators and an introduction of Ischemic Heart Disease(IHD) which is the topic of lecture 7 and half of lecture 6(starting
5 4_part2 Aya Alomoush Alia Shatanawi 1 P a g e This sheet will talk about vasodilators and an introduction of Ischemic Heart Disease(IHD) which is the topic of lecture 7 and half of lecture 6(starting
Management of Hypertension. M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine
 Management of Hypertension M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine Disturbing Trends in Hypertension HTN awareness, treatment and control rates are decreasing
Management of Hypertension M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine Disturbing Trends in Hypertension HTN awareness, treatment and control rates are decreasing
8/20/2018. Objectives. What is hypertension? cont. What is hypertension? Epidemiology cont. Epidemiology
 Objectives Hypertension (high blood pressure): Clinical Pearls for the Pharmacy Technician Tanya Schmidt PharmD, RPh Director of Central Operations at Thrifty White Pharmacy North Dakota Board of Pharmacy
Objectives Hypertension (high blood pressure): Clinical Pearls for the Pharmacy Technician Tanya Schmidt PharmD, RPh Director of Central Operations at Thrifty White Pharmacy North Dakota Board of Pharmacy
ANTI - ARRHYTHMIC DRUGS
 ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
Fundamentals of Pharmacology for Veterinary Technicians Chapter 8
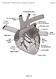 Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Systemic Pharmacology Lecture 7: Neuropharmacology
 Systemic Pharmacology Lecture 7: Neuropharmacology Drugs act on Sympathetic NS (adrenergic system) Adrenergic Drugs (Sympathomimetics), adrenergic agonists, or alpha- and beta-adrenergic agonists Antiadrenergic
Systemic Pharmacology Lecture 7: Neuropharmacology Drugs act on Sympathetic NS (adrenergic system) Adrenergic Drugs (Sympathomimetics), adrenergic agonists, or alpha- and beta-adrenergic agonists Antiadrenergic
Management of Hypertension. Ahmed El Hawary MD Suez Canal University
 Management of Hypertension Ahmed El Hawary MD Suez Canal University Minimal vs. Optimal Care Resources more than science affect type of care and level of management. what is possible (minimal care) and
Management of Hypertension Ahmed El Hawary MD Suez Canal University Minimal vs. Optimal Care Resources more than science affect type of care and level of management. what is possible (minimal care) and
TREATMENT OF HYPERTENSION
 TREATMENT OF HYPERTENSION Aim of treatment BP Goals Main items of treatment Lifestyle modification When to start drug Rx Pharmacological therapy 1. Relief of symptoms 2. Prevention of complications and
TREATMENT OF HYPERTENSION Aim of treatment BP Goals Main items of treatment Lifestyle modification When to start drug Rx Pharmacological therapy 1. Relief of symptoms 2. Prevention of complications and
Hypertension and the Dental Patient
 Course Number: 205 Hypertension and the Dental Patient John H. Hardeman, MD, DDS Upon successful completion of this CE activity, 2 CE credit hours may be awarded. A Peer-Reviewed CE Activity by Dentistry
Course Number: 205 Hypertension and the Dental Patient John H. Hardeman, MD, DDS Upon successful completion of this CE activity, 2 CE credit hours may be awarded. A Peer-Reviewed CE Activity by Dentistry
Drug Treatment of Ischemic Heart Disease
 Drug Treatment of Ischemic Heart Disease 1 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant Angina Primary Angina Unstable Angina Myocardial Infarction 2 3 Secondary Angina Primary
Drug Treatment of Ischemic Heart Disease 1 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant Angina Primary Angina Unstable Angina Myocardial Infarction 2 3 Secondary Angina Primary
Chapter 10. Learning Objectives. Learning Objectives 9/11/2012. Congestive Heart Failure
 Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
