Management of Critical Burn Injuries: Recent Developments
|
|
|
- Mark Pope
- 6 years ago
- Views:
Transcription
1 Korean J Crit Care Med 2017 February 32(1):9-21 / ISSN (Print) ㆍ ISSN (Online) Review Management of Critical Burn Injuries: Recent Developments David J. Dries 1, and John J. Marini 2 1 Department of Surgery and Anesthesiology, 2 Department of Medicine, University of Minnesota, Minneapolis, MN, USA Background: Burn injury and its subsequent multisystem effects are commonly encountered by acute care practitioners. Resuscitation is the major component of initial burn care and must be managed to restore and preserve vital organ function. Later complications of burn injury are dominated by infection. Burn centers are often called to manage problems related to thermal injury, including lightning and electrical injuries. Methods: A selected review is provided of key management concepts as well as of recent reports published by the American Burn Association. Results: The burn-injured patient is easily and frequently over resuscitated, with ensuing complications that include delayed wound healing and respiratory compromise. A feedback protocol designed to limit the occurrence of excessive resuscitation has been proposed, but no new gold standard for resuscitation has replaced the venerated Parkland formula. While new medical therapies have been proposed for patients sustaining inhalation injury, a paradigm-shifting standard of medical therapy has not emerged. Renal failure as a specific contributor to adverse outcome in burns has been reinforced by recent data. Of special problems addressed in burn centers, electrical injuries pose multisystem physiologic challenges and do not fit typical scoring systems. Conclusion: Recent reports emphasize the dangers of over resuscitation in the setting of burn injury. No new medical therapy for inhalation injury has been generally adopted, but new standards for description of burn-related infections have been presented. The value of the burn center in care of the problems of electrical exposure, both manmade and natural, is demonstrated in recent reports. Key Words: burns; electrical injuries; infection; lightning; resuscitation; smoke inhalation injury. Introduction The burn-injured patient presents special challenges regarding resuscitation requirements, metabolic stress, pattern of complications and determinants of outcome [1]. This review highlights a selected group of papers focused on those aspects of care which are unique to burn centers and the burn-injured patient and contribute in important ways to outcome. This selective review of key principles, recent literature, and summary statements is directed toward the acute care physician or surgeon with an interest in such injuries who does not encounter such problems on a daily basis. Contemporary discussions of burn resuscitation often feature the Parkland formula proposed by Baxter and coworkers in the 1960s [1,2]. Reviews of recent experience with burn resuscitation suggest that treatment objectives and fluids administered in the approach originally recommended by the Parkland group should be re-examined [3]. What is contemporary thinking about initial fluid administration in the setting of burn injury? The American Burn Association Received on December 2, 2016 Accepted on December 25, 2016 Correspondence to: David J. Dries, Department of Surgery, Regions Hospital, 640 Jackson Street, St. Paul, MN 55101, USA Tel: , Fax: , david.j.dries@healthpartners.com *No potential conflict of interest relevant to this article was reported. cc This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Copyright c 2017 The Korean Society of Critical Care Medicine 9
2 10 The Korean Journal of Critical Care Medicine: Vol. 32, No. 1, February 2017 (ABA) has recently presented a statement to address this question [4]. The Parkland Burn Center of Dallas, Texas (USA) also published a report on the use of the Parkland formula in the institution where it originated [5]. Apart from understanding the special needs of fluid support, the practitioner should also recognize that sepsis also presents in non-traditional ways in the burn-injured patient [6]. In this paper, we summarize for the non-burn physician and surgeon some of the key aspects of a recent consensus statement produced by the ABA about organspecific infectious complications in the setting of burn injury. A number of outcome indicators related to burn unit practice are coming into clearer focus. Renal failure has a major impact on mortality in any critical care unit population [7]. We now have data indicating that similar concerns hold true regarding the extensively burned patient. Burn units are often selected to manage other problems of the integument and internal organs that bear resemblance to those of thermal exposure. Lifethreatening lightning strikes and other forms of electrical injury pose problems beyond the degree and pattern of skin exposure. In fact, outcome is generally determined by the degree of internal injury in patients victimized by damaging electrical energy [8]. Common to all varieties of extensive thermal injuries are the challenges to appropriately manage fluid balance and infection hazard. Resuscitation Fluid administration in the setting of burn injury and monitoring of efficacy are addressed by consensus recommendations presented in recent work published in the Journal of Burn Care & Research [4]. The University of Texas Southwestern group in Dallas also provides a 35 year retrospective and commentary on the present status of the Parkland formula often used to guide fluid therapy in this critical initial stage. This long venerated standard for burn resuscitation has recently been critiqued by multiple studies, and an insightful editorial review pointed out that burn patients frequently receive greater amounts of fluid than predicted [3]. In short, the accuracy and practicality of the original Parkland formula has been questioned. Resolution of these debates is important, in part because many burn centers have protocolized the implementation of the formula by highly trained and specialized nursing personnel (Figure 1). A valuable retrospective analysis has been conducted of the experience with burn patients treated at Parkland Memorial Hospital Burn Center during a 15 year period from 1991 to 2005 [5]. Included were burns in adults > 19% total body surface area (TBSA). In this adult group, adequate fluid resuscitation was defined by achieving a urine output of 0.5 to 1.0 ml/kg/hr. Over resuscitation was defined as a urine output > 1.0 ml/kg/hr. In a review of nearly 500 patients, 43% received adequate resuscitation based on urine output criteria. Forty-eight percent were over resuscitated. Using these adequacy criteria, however, there was no observed difference in complication rates or mortality incidence between resuscitation categories. Patients were evaluated for inhalation injury with bronchoscopy. Contrary to reports from other centers, the amount of fluid required for adequate resuscitation based on target urine output was not different in patients with inhalation injury as opposed to those without this insult. While other groups have reported [9] that intra-abdominal hypertension and abdominal compartment syndrome commonly occur in burn patients with volume resuscitation in excess of 250 ml/kg, the Parkland experience indicates only a 1% incidence of abdominal compartment syndrome, even in burns exceeding 40% TBSA, where administered resuscitation volumes exceeded 250 ml/kg. In summary, even in the home of the Parkland formula, actual burn resuscitation frequently does not meet the standard set forth by this clinical strategy. Patients commonly received higher fluid volumes than predicted by the Parkland formula. The Parkland team recommended placing emphasis on calculated formula volumes only as a guide to initial resuscitation, with subsequent fluids titrated to urine output. A consensus statement has been released from the
3 David J. Dries, et al. Burn Injury Developments 11 Protocol for Fluid Resuscitation of the Adult Burn Patient: Begin LR using burn center fluid resuscitation calculations STEP ONE Infuse at calculated rate as ordered by MD. Measure Urine Output after one hour Vitals Unstable: HR > 140/min, < 60/min BP < 90/60 mmhg SaO 2 < 90% Vitals Signs Stable: HR < 140/min, BP > 90/60 mmhg, SaO 2 > 90% CALL PHYSICIAN Urine Output < 15 ml Urine Output ml Urine Output ml Urine Output ml Urine Output > 200 ml Increase IV rate by 20% or 200 ml/hr (whichever is more) Increase IV rate by 10% or 100 ml/hr (whichever is more) Leave IV rate as is Decrease IV rate by 10% or 100 ml/hr (whichever is more) Decrease IV rate every 1/2 hour by 10% or 100 ml/hr, whichever is more. Measure blood sugar, lactate, hemoglobin. Call physician with questions. REPEAT STEP ONE EVERY HOUR UNTIL: Urine Output < 15 ml/hr for two or more hours despite increasing fluid rate CALL PHYSICIAN: Check urinary catheter, assess breath sounds, vital signs, bladder pressure. Consider albumin protocol. Calculated maintenance rate is reached and held for two hours AND patient is at least 24 hours post-burn Fluid resuscitation is complete: switch patient to maintenance IV of D5/0.45 NaCl + 20 meq KCI/liter at calculated maintenance rate If patient again develops oliguria or hemodynamic instability, CALL PHYSICIAN, Restart patient on LR at current rate and return to STEP ONE. Patient requires increasing fluids or more than twice current calculated rate for two or more hours. Patient may need colloid resuscitation: CALL PHYSICIAN to discuss. Check foley catheter, vital signs, bladder pressure Albumin protocol: begin a combination of 5% albumin at 1/3 of current IV rate, plus LR at 2/3 current rate. Repeat STEP ONE. Decrease IV as tolerated, maintaining the ratio of 1/3 albumin: 2/3 LR until maintenance rate is maintained for two hours. Switch IV fluid to plain LR and repeat STEP ONE Figure 1. Protocol for fluid resuscitation of adult burn patients. In response to requests from nurses, this protocol was developed to permit nursing staff to manage fluid resuscitation of acute burn patients. Initial fluid rates are calculated by the Parkland formula. Nurses begin hourly infusion, measure urine output, and adjust fluids according to patient response. Development of unstable vital signs, inadequate response to fluids, or persistently high fluid requirements prompt a call to the physician. A pathway to begin colloid replacement exists for patients who display increasing fluid requirements or develop symptoms of torso compartment syndrome. Adopted from references [3] with permission. LR: lactated Ringer s solution; D5: 5% dextrose. ABA regarding burn/shock resuscitation [4]. Notably, no standards for the approach to the resuscitation of burninjured patients have been derived from high quality contemporary studies. However, a number of guidelines are supported by evidence of lesser strength. Guidelines and Options from the ABA are listed in the Journal of Burn Care & Research [4]. Lacking unequivocal evidence, there currently is little agreement regarding optimal fluid composition, rate of fluid administration, and the role of colloids, such as albumin. No resuscitation parameters geared to regulating individual patient fluid needs by formula perform clearly better than routine hemodynamic endpoints and adequate urine output. Practitioners must be compulsive in providing adequate fluids but must also avoid excessive resuscitation. Many centers begin with the Parkland formula, which has now been renamed the Consensus formula for resucitation because it is the most widely used approach. This formula provides 4 ml/kg/% TBSA burned, describing the amount of lactated Ringers solution required
4 12 The Korean Journal of Critical Care Medicine: Vol. 32, No. 1, February 2017 in the first 24 hours after burn injury where kg represents initial patient weight, and % TBSA is the extent of 2nd and 3rd degree burn injury. Starting from the time of burn injury, half of the fluid is given in the first 8 hours and the remaining half is given over the next 16 hours. Unfortunately, rapid determination of % TBSA burn and calculation of fluid requirements can be difficult and is often incorrect when the clinician charged with treating burns is relatively inexperienced. Many centers are evolving resuscitation protocols such as that given in Figure 1 from the University of Utah. Fluid administration in this protocol begins with the Consensus formula, and fluids are titrated based on patient response [1]. Three additional points of clarification regarding burn resuscitation should be made. First, many patients, particularly those with burns < 20% TBSA, may be candidates for oral resuscitation as an intact gastrointestinal tract tolerates large amounts of administered fluid. Enteral resuscitation should be considered when resources are limited, an austere setting is encountered, and the patient is able to tolerate enteral intake. Second, invasive hemodynamic monitors including central venous catheters and pulmonary artery catheters have been employed to optimize burn resuscitation in a variety of prospective and retrospective studies. Patients with invasive central hemodynamic monitors tend to have far more fluid administered without commensurate improvement in outcome. While invasive monitoring may be indicated for patients with co-morbidities or patients who fail to respond to resuscitation prescriptions, a blanket endorsement of this approach cannot be made. Third, antioxidant therapies show promise in reduction of burn resuscitation fluid requirements and edema formation in a variety of preclinical trials. Unfortunately, patient data is limited and multicenter prospective validation has not been attempted. Sepsis and Infection in Burn-Injured Patients In an important action, the ABA convened a consensus conference addressing burn sepsis and infection using methodology recently employed by the Society of Critical Care Medicine and other critical care societies [6]. The conference and the documents produced from it applied consensus-driven definitions of organ dysfunction and infection as described in the general critical care population and modified these as appropriate to reflect the perturbations encountered in burn injury. This work is important, as the major cause of late death in the burn patient population is multiple organ dysfunction syndrome, which typically is driven by infection. Findings of this consensus conference process are highlighted below. The concept of Systemic Inflammatory Response Syndrome (SIRS) should not be applied to burn patients [10]. While the SIRS concept has been widely accepted and utilized in critical care practice and clinical trials, it has been widely criticized for being too inclusive and insufficiently specific to effectively identify a relevant inflammatory state. Burn patients frequently demonstrate characteristics of SIRS throughout the majority of hospitalization. Biochemical markers have also been evaluated but at present do not apply to the specific physiology of the burned patient. Sepsis should be redefined for the burn patient population [6]. Triggers in the burn-injured patient are different than those in other critical care populations. As in general critical care practice, sepsis is a condition warranting empiric antibiotics and a search for infection during that short course of empiric therapy. The concept of severe sepsis, the intervening state between sepsis and septic shock was dropped as the conference attendees felt that a distinctly separate state between sepsis and septic shock is not regularly seen. Septic shock definitions from consensus conferences including the Surviving Sepsis Campaign and consensus work of the major critical care societies are retained [11]. Of note, the ABA has not yet addressed the updated definition system reflected in the recent Sepsis-3 Consensus Statement [12]. Septic shock for the burned patient is defined as sepsisinduced hypotension that persists despite adequate fluid
5 David J. Dries, et al. Burn Injury Developments 13 resuscitation. Sepsis-induced hypotension is defined as a systolic blood pressure (SBP) < 90 mmhg or mean arterial pressure < 70 mmhg or a SBP decrease > 40 mmhg or > 2 SD below normal for age in the absence of other identified causes of hypotension. Sepsis-induced tissue hypoperfusion is defined as septic shock, an elevated lactate, or oliguria [6]. Smoke inhalation injury by anatomic definition is inflammation occurring below the glottis that results from exposure to the by-products of combustion. Diagnosis requires a relevant history of acute exposure and bronchoscopy that reveals carbonaceous material or signs of edema/ulceration. Smoke inhalation injury can occur with or without detection of products such as cyanide or carbon monoxide. Bronchoscopy demonstrating anatomic injury is the gold standard for diagnosis. Pneumonia, a common complication of inhalation injury, is defined in a fashion similar to those of previous consensus conferences conducted by critical care and respiratory societies [13,14]. The ABA Consensus Group did make statements regarding positive microbiology. Finding 10 5 organisms on a tracheal aspirate, bronchoalveolar lavage with 10 4 organisms, and protected bronchial brushings with > 10 3 organisms per ml are criteria for positive microbiology in the setting of burn injury. The burn literature supports discontinuation of antibiotics when these microbiologic thresholds are not met. The Clinical Pulmonary Infection Score was briefly discussed and felt to be insufficient to predict Ventilator- Associated Pneumonia (VAP) in the burn victim. Clinical suspicion of ventilator-associated pneumonia must be verified by quantitative culture results. VAP is an important complication in burn-injured patients. Burn patients are at high risk for developing VAP, particularly in the setting of inhalation injury. Prevention strategies are recommended, but relatively few are supported by strong evidence. Clinical diagnosis of VAP can be challenging in mechanically ventilated burn patients, a population in whom systemic inflammation, acute lung injury and non-infectious pulmonary infiltrates are prevalent. Quantitative strategies for identifying pathogens are the preferred method to confirm the diagnosis of VAP. Empiric antimicrobial therapy should cover resistant Staphylococcus aureus and gram-negative bacilli. In general, at least eight days of antibiotic therapy are recommended [15]. Several therapies are still under investigation to optimize outcome of VAP in burn-injured patients. Perhaps the most discussed is protocolized management of smoke inhalation. A variety of ventilation modes have been recommended. A recent survey of ventilator practice conducted by burn centers reveals a wide range of behavior. In addition, the role of early tracheostomy to facilitate secretion clearance remains unclear, along with the optimal means to deliver antimicrobials. While most centers use intravenous administration, several investigators are assessing the value of aerosolized antibiotics, which could enhance delivery to the lower respiratory tract. An encouraging development comes from the Division of Burn Surgery at the University of California-Davis, who introduced a VAP prevention bundle including elevation of the head-of-the-bed to 30 degrees, daily oral care with chlorhexidine, daily sedation interruption with assessment of readiness to wean from mechanical ventilation, and prophylaxis against stress ulceration and deep venous thrombosis. Compliance with the bundle was facilitated by a nurse advocate dedicated to the intensive care unit. Not surprisingly, TBSA burn extent and number of ventilator days were independent predictors of development of VAP. However, data obtained after implementation of the management bundle revealed a significantly reduced development of VAP, independent of TBSA burn extent and number of ventilator days [16,17]. Definitions for bloodstream and catheter-related bloodstream infections are accepted as defined in previous reports [6]. Catheter colonization is indicated by growth of organisms from a catheter segment, as identified by semiquantitative or quantitative culture. A catheterrelated bloodstream infection reflects identification of the identical organism from blood culture and semiquantitative or quantitative culture from a catheter segment. Clinical symptoms of bloodstream infection should also
6 14 The Korean Journal of Critical Care Medicine: Vol. 32, No. 1, February 2017 be present without any other apparent source of infection. Finally, exit site infection is defined as erythema, tenderness, induration, or purulence within 2 cm of the exit site of a catheter. Blood cultures should ideally include quantitative techniques with a specimen of 10 ml. Blood cultures must also reflect recognized pathogens not usually regarded as skin contaminants. Definitions of wound-related complications were also assembled [6,18]. Wound colonization is present with bacteria on the wound surface at low concentrations. Wound infection is present with high concentrations of bacteria in the wound and wound eschar (> 10 5 bacteria/ gram tissue). Invasive infection occurs with high concentrations of pathogens (> 10 5 bacteria/gram tissue) and changes such as separation of eschar or skin grafts, invasion of adjacent unburned tissue or development of sepsis, as defined above. A diagnosis of cellulitis requires bacteria recovered from the wound or wound eschar in high concentrations and advancing erythema, induration, warmth, and tenderness of surrounding tissues. Sepsis, as defined above, must be present. Necrotizing fasciitis is an aggressive, invasive infection with necrosis of tissues beneath the skin. Objective diagnostic criteria include biopsy and swab culture techniques, but none of these is ideal. Clinical correlates include systemic changes compatible with serious infection, premature separation of eschar, and unexplained tissue loss or change in the depth of wounds. Pseudomonas aeruginosa is a frequent colonizing organism in burn and other soft tissue wounds. The yellow/green exudate of Pseudomonas does not necessarily indicate invasive infection. When changes consistent with deep tissue injury and systemic changes including organ dysfunction are seen, aggressive antibiotic therapy and surgical debridement are urgently warranted. Electrical and Lightning Injury An electrical injury occurs when a person comes in contact with the current produced by an electrical energy source. This source may be manmade, such as a power line, or a natural one, such as a lightning strike. Electrical injury that emanates from a manmade source is typically transmitted after its generation at very high voltage, but transformers reduce voltage gradually and power lines distributing electricity for homes, buildings, and most industries carry low voltage (typically less than 600 volts). Homes and buildings generally have a system providing < 240 volts for general use. Therefore, relatively low voltage sources account for the majority of accidental injuries secondary to electricity [8]. Electric current exists in two forms, alternating current (AC) and direct current (DC). In AC, electrons flow back and forth through a conductor in cyclic fashion. This type of current is most commonly used in households and offices and is standardized to a frequency of 50 or 60 cycles per second, depending on country. When current is direct, the electrons flow in only one direction. This type of current is produced by various batteries and is used in medical equipment such as defibrillators, pacemakers, and electric scalpels. Although AC is considered to be a far more efficient way of generating and distributing electricity, it is more dangerous than DC because it causes tetanic muscle contractions that often prolong contact of the victim with the source [8,19]. Lightning is a form of direct current generated when an electrical potential difference between a thunder cloud and the ground overcomes the insulating properties of the surrounding air. The current flow of a lightning strike rises to a peak in approximately 2 microseconds and it lasts only 1 to 2 milliseconds. Voltage of a lightning strike may exceed 1,000,000 volts with greater than 200,000 amperes of current flow. Transformation of the electrical energy to heat can generate temperatures as high as 50,000 F. However, the extremely short duration of lightning strikes prevents the struck object from melting in most cases [20]. In general, the type and extent of an electrical injury depends on the intensity of the electric current. According to Ohm s Law, electric current is proportional to the voltage of the source and inversely proportional to the
7 David J. Dries, et al. Burn Injury Developments 15 resistance of the conductor. Because resistance varies significantly between tissues, exposure of different parts of the body to the same current will produce different conduction paths and result in different degrees of injury. The least resistance is found in the nervous system, blood, mucus membranes, and muscles; the highest resistance is found in bones, fat, and tendons. Skin has intermediate resistance. The skin is the primary resistor against electrical current with a resistance ranging in adults between 40,000 and 100,000 ohms depending on its thickness (thicker skin means higher resistance). Even more important than thickness of the skin in determining injury is the presence or absence of moisture on the skin. The presence of simple perspiration may decrease the resistance of the skin to less than 1,000 ohms. Wet skin in a bathtub or swimming pool may facilitate electrocution as it offers almost no resistance at all, generating the maximum intensity of current that the applied voltage can drive [8]. Duration of contact with electrical current is another important determinant of injury. An electric shock caused by alternating current will produce greater injury than a shock caused by direct current of the same amperage because direct current causes a single muscle contraction that tends to throw the victim away from the power source, whereas alternating current repeatedly stimulates muscle contraction, often trapping the victim into sustained contact with the energy source. The pathway of current through the body from entry to exit point determines the number of organs that are affected, and as a result, the type and severity of injury. Determination of the electrical pathway is important for acute management and for overall prognosis. For example, a vertical pathway parallel to the axis of the body is the most dangerous because it involves virtually all vital organs including the central nervous system, heart, respiratory muscles, and in the pregnant patient, the uterus, and fetus. Electrical injury affects the cardiovascular system by directly causing necrosis of the cardiac muscle and by inciting dysrhythmias. The degree of myocardial injury depends on the voltage and type of current. Predisposition to injury of the vascular bed reflects its high water content and excellent conductivity. Electric current affects vessels of different size in different ways. Large arteries are not immediately affected because their rapid blood flow allows for rapid heat dissipation. However these same large vessels are susceptible to medial necrosis and later sequelae such as aneurysm formation and the potential for delayed rupture. Smaller vessels are acutely affected due to coagulation necrosis, which may lead to ischemia and compartment syndromes. The most frequently encountered rhythm disturbance is sinus tachycardia, often accompanied by non-specific ST- and T-wave changes. Conduction defects such as heart blocks are also common [8,19-21]. Cardiac standstill and ventricular fibrillation are the most serious cardiac complications of electrical injury and are invariably fatal unless the victim is immediately resuscitated from them. No pathognomonic change characterizes passage of electrical current through the nervous system. Acute cranial nerve deficits and seizures may occur after electrical injury to the brain. Direct injury to the spinal cord at the lower cervical level has also been reported. Loss of consciousness, confusion, and impaired recall are common among victims of electrical injury. If there is no associated tissue damage, these patients tend to recover well. Dysfunction of peripheral motor and sensory nerves may cause a variety of deficits. The most serious consequence of neural electrical injury is malfunction of the respiratory control center that culminates in sustained respiratory arrest. Other patients may exhibit a variety of additional non-specific abnormal respiratory patterns after electrical encounters [8,22]. There are no specific injuries to the lungs or airways directly associated with electric current. Exposure to current generated by low voltage sources may cause cutaneous injury by transformation of electrical to thermal energy. Injuries can range from local erythema to full-thickness burns. As with other organs, the severity of a surface burn depends on the intensity of the current, surface involved, and duration of exposure. More serious burns are caused by exposure to arcs that are created in accidents with high voltage currents
8 16 The Korean Journal of Critical Care Medicine: Vol. 32, No. 1, February 2017 (> 1,000 volts). In such cases, the severity of the burn depends not only on the temperature but also the energy within the arc. Burns due to lightning are common but typically quite superficial due to the short duration of contact between the energy source and the victim [19]. Management of electrical injury requires cardiopulmonary resuscitation and multiple organ system trauma care. Thorough evaluation for hidden injury, particularly to the spinal cord, should take place, including assessment for event-associated blunt thoracic or abdominal trauma. Imaging of the head, neck, chest, abdomen, and pelvis may be appropriate to rule out internal injury along with serial evaluation of liver, pancreatic, and renal function for traumatic and ischemic injury. Patients with high voltage injuries should be evaluated for rhabdomyolysis and heme-derived pigments in the urine. Limbs must be assessed for compartment syndromes that may require fasciotomy. Ophthalmologic and otoscopic evaluation may also be important [8]. It is not uncommon for electrical injuries, particularly those associated with lightning, to cause multiple casualties. In other instances of trauma that involve several simultaneously injured people, efforts are logically focused on those who show signs of life. Lightning victims are an exception to this general rule because patients struck by lightning may become acutely apneic due to paralysis of respiratory centers and have dilated nonreactive pupils due to autonomic dysfunction. However, it is possible for the heart to recover spontaneously. Thus, administration of oxygen and supplemental ventilation should be applied immediately to the apneic lightning victim as efforts are made for cardiac resuscitation. Airway control should be established as rapidly as possible to minimize the effects of anoxia, a major cause of mortality [20]. The combination of extensive burns and significant internal visceral injury that can accompany high voltage electrical exposures increases fluid requirements, due to extravasation into extra vascular compartments and ongoing fluid losses. Because muscle destruction that usually accompanies these injuries may cause myoglobinuria and lead to renal failure, aggressive fluid resuscitation is important. Whereas the appropriate fluid prescription for most burn patients can be determined by the extent of cutaneous injury, electrical and lightning injuries do not follow such rules, due to their higher incidence of internal injuries. Where any risk of cardiac injury is possible based on mechanism or energy source, cardiac monitoring with echocardiography to determine pump function is prudent. Enzyme markers of cardiac injury may be misleading, as normal enzyme concentrations in the circulating blood do not exclude the possibly of conducting system injury with consequent rhythm disturbances. This observation serves to emphasize the value of an interval monitoring [8,19]. Pulmonary Issues Respiratory failure in the burn victim is often characterized by hypoxemia with evolution to acute lung injury or acute respiratory distress syndrome (ARDS) [23]. Even in patients without defined inhalation injury, the presence of ARDS is associated with poorer outcome. Management of inhalation injury consists primarily of time-honored supportive care. This may include mechanical ventilation with supplemental oxygen therapy and effective pulmonary toilet aided by catheter means or bronchoscopic interventions. Inhalation injury describes pulmonary trauma caused by inhalation of thermal or chemical irritants. Such injuries are classified into categories of heat injury (which is usually restricted to upper airway structures except in the case of steam jet exposure), of local chemical irritation to the respiratory tract, and of systemic toxicity that may occur with exposure to carbon monoxide or cyanide [24]. The classic description of the effects of inhalation injury and its principle complication, pneumonia, was produced in the 1980s from the U.S. Army Institute of Surgical Research. In a review of over 1,000 patients, subjects at risk for inhalation injury were investigated by bronchoscopy, Xenon lung scans, or both. Diagnosis of inhalation injury was made in 373 patients. With increas-
9 David J. Dries, et al. Burn Injury Developments 17 ing burn size, there was a corresponding rise in incidence of inhalation injury. The diagnosis of pneumonia was made at approximately 10 days for patients with inhalation injury. Expected mortality rate was reported to rise from 20% in the presence of inhalation injury alone to 60% when both inhalation injury and pneumonia were present. Contributions of inhalation injury and pneumonia to mortality were found to be independent and additive. Expected mortality in patients with very small or very large burns was not affected by these pulmonary complications, except at the extremes of age. While many techniques have been developed to manage cutaneous injury, relatively few diagnosis-specific therapies have been identified for the patient with inhalation injury. Improvements in mortality from inhalation injury are mainly attributed to general improvements in critical care rather than to focused interventions for smoke inhalation. A variety of factors explain slower progress for improvement in management of inhalation injury. Cutaneous burn injury may be excised and replaced with skin grafts, but injury to pulmonary tissue must merely be supported and protected from secondary injury. In addition to smoke inhalation, the critically ill burn patient often has multiple mechanisms contributing to lung injury, such as sepsis, ventilator-induced lung injury, or systemic inflammation in response to burns. Thus, inhalation injury impacts burn patient outcome but its role is difficult to separate from the contributions of other injury drivers which affect the lungs. Another significant limitation for clinicians treating smoke inhalation has been the lack of uniform criteria for diagnosis and scaling of outcome severity. As a result, multicenter trials are confounded by differing local definitions of inhalation injury. The need for widely accepted diagnostic criteria and for a quantifying system for inhalation injury has been acknowledged in the burn literature [24]. A large survey regarding mechanical ventilation practices was recently conducted in North American burn centers. Pressure support and volume assist control were most common initial mechanical ventilation modes used, regardless of the presence of smoke inhalation. Using the recent Berlin definition for ARDS, the ARDSNet protocols for patients treated positive end-expiratory pressure were the most popular ventilation choices along with fluid restriction and diuresis. For severe ARDS, airway pressure release ventilation (APRV) and neuromuscular blockade were commonly used. The most frequently reported timeframe for placement of tracheostomy was two weeks. In general, wide variation in clinical practice was noted among North American burn centers, with no single ventilator mode or treatment adjunct pre-eminent in the management of burn patients, regardless of pulmonary insult [17]. Outcomes For over half a century, investigators have sought reliable predictive indices for outcomes from burn injury. Perhaps the best known is the Baux rule, a simple sum of patient age and total body surface area in those suffering 2nd and 3rd degree burns. This index continues to receive attention; in fact, the Baux rule was recently addressed using patient registry data from the ABA [25]. The most recent summary of outcomes in burn care comes from the 2016 National Burn Repository Annual Report produced by the ABA [26]. Relevant data is drawn from burn admissions during the time interval spanning 2006 to A number of important observations can be made. First, over 200,000 records are reviewed from a representative cross-section of U.S. burn centers. In all age categories, except age > 80 years old, males outnumber females. Pediatric patients ranging in age from 1-15 years comprised 30% of the total sample while patients 60 years or older represented 14% of burn cases reported. More than 75% of all burns were < 10% TBSA, and these cases had a mortality rate of only 0.6%. The mortality rates for all burns and for fire/flame injuries were 3.3% and 5.8%, respectively. The two most common etiologies of burn injury were fire/flame and scalds, accounting for 75% of cases reported. Scald injuries were
10 18 The Korean Journal of Critical Care Medicine: Vol. 32, No. 1, February 2017 most prevalent in children under the age of 5 years while fire/flame injuries dominated in the remaining age categories. Seventy-three percent of burn injuries with a known place of event were reported to have occurred in the home. Nearly 95% of cases with known circumstances of injury were identified as accidents, with nearly 14% of burns reported as work-related. Just over 2% of cases were suspected abuse and 1% of burn injuries were selfinflicted. During the 10 year period from 2006 to 2015, the average length of stay for females declined from 9.3 days to 7.9 days while that for males declined less significantly, from 9.1 to 8.8 days. The mortality rate for females declined from 4.1% to 2.9% compared with 3.9% to 3% for males. Deaths from burn injury increased with advancing age, increasing burn size, and the presence of inhalation injury. Pneumonia was the most frequent complication reported and occurred in 5.4% of fire/flame-injured patients. The frequency of pneumonia and respiratory failure was much greater in patients treated 4 days or more with mechanical ventilation. As age advances, the rate of complications increases (with the exception of infants who have a higher rate than other children). Extensive burn wounds heal slowly and the period of critical illness tends to be protracted. For burn survivors, the average length of hospital stay was slightly greater than 1 day per % TBSA burned. For patients who died, the total hospital days were nearly two times that of survivors on average; however, this trend was reversed in patients with > 20% TBSA burns. Eight-seven percent of patients were discharged to home and 3% of patients were transferred to rehabilitation facilities. Overall, the charges for patients who died were more than three times greater than those for patients who survived; however, this was skewed by the relatively high proportion of the patient sample with burns < 10% TBSA. For burns > 10% TBSA treated in American hospitals, total charges for surviving patients averaged over $250,000 U.S. and charges for non-survivors averaged $340,000 U.S. [26]. A classic single center outcome review of over 1,600 patients admitted to the Massachusetts General Hospital and the Schriners Burn Institute in Boston was published in early 1998 [27]. Logistic regression analysis was employed to develop probability estimates for mortality based on a small set of well-defined variables. Three risk factors for death were identified: age > 60 years; TBSA burns > 40% and inhalation injury. The mortality formula developed from this report predicts 0.3%, 3%, 33% or 90% mortality depending on whether 0, 1, 2 or 3 risk factors are present respectively. Early recognition of organ dysfunction and sepsis may prevent further complications in the critically ill burned patient. Markers for renal injury have been investigated as a means to provide earlier recognition of acute renal failure [28]. Cystatin C, plasma neutrophil gelatinaseassociated lipocalin (NGAL), and urine NGAL were evaluated in patients demonstrating acute kidney injury within five days of burn injury. Mortality was high in both the early acute kidney injury patients (77%) and patients with late presentation of acute kidney injury (58%). NGAL was elevated within hours after injury in patients with early acute kidney injury and early death. Cystatin C and serum creatinine did not rise until 12 hours after injury. Many severely injured patients are vulnerable to sepsis from many sources. Early diagnosis and treatment of such infections may reduce the incidence of complications and improve survival. Burn patients have been evaluated for effectiveness of N-terminal pro B-type natriuretic peptide (pro-bnp), procalcitonin, and hemodynamic monitors using arterial pressure waveform analysis to identify the presentation of sepsis [29]. Pro- BNP, systemic vascular resistance, and stroke volume variation appeared to have good predictive quality for identification of sepsis in burn patients. The combination of elevated pro-bnp and stroke volume variation with low systemic vascular resistance may help provide early identification of infectious complications. Development of burn centers in the United States has been associated with a verification process to standardize
11 David J. Dries, et al. Burn Injury Developments 19 and optimize overall quality of care delivered [30,31]. Perhaps as a direct beneficial consequence, burn centers have been demonstrated to improve survival and decrease resource consumption. Using the discharge database from the state of California, five burn centers verified by the ABA and the American College of Surgeons were compared with 12 non-verified burn centers. In 2003, 2,867 patients were admitted to burn centers; over 1,600 of these patients were admitted to non-verified centers. Verified centers admitted more patients with large burns, burns requiring complex reconstruction, and more patients requiring critical care support including mechanical ventilation. Verified burn centers also performed fewer operations than non-verified centers. More patients from verified centers were able to return home while additional rehabilitation care was required in patients from non-verified centers. Mortality, however, was 3% in non-verified burn centers and 4% in verified burn centers, perhaps in part reflecting the severity mix. Differences in resource consumption including operative procedures, post-discharge destination, and median hospital charge support the use of verified burn centers in the management of burn-injured patients. Clearly, the population seen in verified and non-verified burn centers is different and this report details resource consumption issues which may be better addressed in a regionalized burn care system [32]. which have been better defined. Inhalation injury that requires respiratory assistance should be provided in accordance with the same principles of lung protective mechanical ventilation used in other patients with ARDS. Upper airway damage and smoke inhalation injury can occur with or without detection of oropharyngeal change or detection of combustion products in the blood such as cyanide or carbon monoxide. Bronchoscopy demonstrating anatomic injury represents the gold standard for diagnosis. A number of factors predict mortality in burn injury. Burn size, presence or absence of inhalation injury, and extremes of age have been widely reported to be influential. Renal failure and insufficiency are strongly associated with poor outcome following extensive burns. Among the special problems addressed in burn centers, electrical injuries pose multisystem physiologic challenges and do not fit typical scoring systems based on abnormalities observed at the skin surface. Management by verified burn centers reduces cost of therapy for burn injury. Acknowledgements The authors gratefully recognize the technical assistance of Mrs. Sherry Willett in the preparation of this manuscript. Conclusions The burn patient is easily over resuscitated. Practitioners must be willing to reduce fluid prescriptions when signs of adequate perfusion are present. Currently, adequate vital signs and urine output are the gold standard for perfusion assessment. In the burn-injured patient traditional definitions of systemic inflammatory response syndrome (SIRS) and sepsis must be redefined based on the physiologic characteristics of burn injury. In addition, the burn patient is at risk for soft tissue infections and burn wound infection ORCID David J. Dries References 1. Latenser BA. Critical care of the burn patient: the first 48 hours. Crit Care Med 2009; 37: Baxter CR. Fluid volume and electrolyte changes of the early postburn period. Clin Plast Surg 1974; 1:
12 20 The Korean Journal of Critical Care Medicine: Vol. 32, No. 1, February Saffle JR. The phenomenon of fluid creep in acute burn resuscitation. J Burn Care Res 2007; 28: Pham TN, Cancio LC, Gibran NS; American Burn Association. American Burn Association practice guidelines burn shock resuscitation. J Burn Care Res 2008; 29: Blumetti J, Hunt JL, Arnoldo BD, Parks JK, Purdue GF. The Parkland formula under fire: is the criticism justified? J Burn Care Res 2008; 29: Greenhalgh DG, Saffle JR, Holmes JH 4th, Gamelli RL, Palmieri TL, Horton JW, et al. American Burn Association consensus conference to define sepsis and infection in burns. J Burn Care Res 2007; 28: Uchino S, Kellum JA, Bellomo R, Doig GS, Morimatsu H, Morgera S, et al. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA 2005; 294; Koumbourlis AC. Electrical injuries. Crit Care Med 2002; 30(11 Suppl): S Ivy ME, Atweh NA, Palmer J, Possenti PP, Pineau M, D Aiuto M. Intra-abdominal hypertension and abdominal compartment syndrome in burn patients. J Trauma 2000; 49: Bone RC, Balk RA, Cerra FB, Dellinger RP, Fein AM, Knaus WA, et al. Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest 1992; 101: Dellinger RP, Levy MM, Rhodes A, Annane D, Gerlach H, Opal SM, et al. Surviving sepsis guidelines: international guidelines for management of severe sepsis and septic shock: Crit Care Med 2013; 41: Singer M, Deutschman CS, Seymour CW, Shankar- Hari M, Annane D, Bauer M, et al. The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA 2016; 315: Hubmayr RD, Burchardi H, Elliot M, Fessler H, Georgopoulos D, Jubran A, et al. Statement of the 4th international consensus conference in critical care on ICU-acquired pneumonia--chicago, Illinois, May Intensive Care Med 2002; 28: Rello J, Paiva JA, Baraibar J, Barcenilla F, Bodi M, Castander D, et al. International conference for the development of consensus on the diagnosis and treatment of ventilator-associated pneumonia. Chest 2001; 120: Mosier MJ, Pham TN. American Burn Association practice guidelines for prevention, diagnosis, and treatment of ventilator-associated pneumonia (VAP) in burn patients. J Burn Care Res 2009; 30: Sen S, Johnston C, Greenhalgh D, Palmieri T. Ventilator-associated pneumonia prevention bundle significantly reduces the risk of ventilator-associated pneumonia in critically ill burn patients. J Burn Care Res 2016; 37: Chung KK, Rhie RY, Lundy JB, Cartotto R, Henderson E, Pressman MA, et al. A survey of mechanical ventilator practices across burn centes in North America. J Burn Care Res 2016; 37: e Peck MD, Weber J, McManus A, Sheridan R, Heimbach D. Surveillance of burn wound infections: a proposal for definitions. J Burn Care Rehabil 1998; 19: Arnoldo BD, Purdue GF, Kowalske K, Helm PA, Burris A, Hunt JL. Electrical injuries: a 20-year review. J Burn Care Rehabil 2004; 25: Lichtenberg R, Dries D, Ward K, Marshall W, Scanlon P. Cardiovascular effects of lightning strikes. J Am Coll Cardiol 1993; 21: Arnoldo B, Klein M, Gibran NS. Practice guidelines for the management of electrical injuries. J Burn Care Res 2006; 27: Singerman J, Gomez M, Fish JS. Long-term sequelae of low-voltage electrical injury. J Burn Care Res 2008; 29: ARDS Definition Task Force, Ranieri VM, Rubenfeld GD, Thompson BT, Ferguson ND, Caldwell E,
The Parkland Formula Under Fire: Is the Criticism Justified?
 The Parkland Formula Under Fire: Is the Criticism Justified? Jennifer Blumetti, MD, John L. Hunt, MD, Brett D. Arnoldo, MD, Jennifer K. Parks, MPH, Gary F. Purdue, MD Controversy has continued regarding
The Parkland Formula Under Fire: Is the Criticism Justified? Jennifer Blumetti, MD, John L. Hunt, MD, Brett D. Arnoldo, MD, Jennifer K. Parks, MPH, Gary F. Purdue, MD Controversy has continued regarding
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
ELECTRICAL INJURY 9/21/2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
 ELECTRICAL INJURY SAMUEL P. MANDELL, MD, MPH ASSISTANT PROFESSOR OF SURGERY UNIVERSITY OF WASHINGTON SEPTEMBER 28, 2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
ELECTRICAL INJURY SAMUEL P. MANDELL, MD, MPH ASSISTANT PROFESSOR OF SURGERY UNIVERSITY OF WASHINGTON SEPTEMBER 28, 2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
CEDR 2018 QCDR Measures for CMS 2018 MIPS Performance Year Reporting
 ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
High Voltage Safety. Dangers of Electricity. W. Maes. Department of Marine Engineering Antwerp Maritime Academy HV, 2015
 Dangers of Electricity W. Maes Department of Marine Engineering Antwerp Maritime Academy HV, 2015 Outline 1 The physical effect of an electric current on the human body Heating Source of power Electro-magnetical
Dangers of Electricity W. Maes Department of Marine Engineering Antwerp Maritime Academy HV, 2015 Outline 1 The physical effect of an electric current on the human body Heating Source of power Electro-magnetical
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline
 TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
Basics from anatomy and physiology classes Local tissue reactions
 Septicaemia & SIRS Septicaemia is a life-threatening condition that arises when the physical reaction to an infection, causes damage to tissue and organs Basics from anatomy and physiology classes Local
Septicaemia & SIRS Septicaemia is a life-threatening condition that arises when the physical reaction to an infection, causes damage to tissue and organs Basics from anatomy and physiology classes Local
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Understand the scope of sepsis morbidity and mortality Identify risk factors that predispose a patient to development of sepsis Define and know the
 Understand the scope of sepsis morbidity and mortality Identify risk factors that predispose a patient to development of sepsis Define and know the differences between sepsis, severe sepsis and septic
Understand the scope of sepsis morbidity and mortality Identify risk factors that predispose a patient to development of sepsis Define and know the differences between sepsis, severe sepsis and septic
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test
 Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Staging Sepsis for the Emergency Department: Physician
 Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Presented by: Indah Dwi Pratiwi
 Presented by: Indah Dwi Pratiwi Normal Fluid Requirements Resuscitation Fluids Goals of Resuscitation Maintain normal body temperature In most cases, elevate the feet and legs above the level of the heart
Presented by: Indah Dwi Pratiwi Normal Fluid Requirements Resuscitation Fluids Goals of Resuscitation Maintain normal body temperature In most cases, elevate the feet and legs above the level of the heart
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
Tailored Volume Resuscitation in the Critically Ill is Achievable. Objectives. Clinical Case 2/16/2018
 Tailored Volume Resuscitation in the Critically Ill is Achievable Heath E Latham, MD Associate Professor Fellowship Program Director Pulmonary and Critical Care Objectives Describe the goal of resuscitation
Tailored Volume Resuscitation in the Critically Ill is Achievable Heath E Latham, MD Associate Professor Fellowship Program Director Pulmonary and Critical Care Objectives Describe the goal of resuscitation
Septic Shock. Rontgene M. Solante, MD, FPCP,FPSMID
 Septic Shock Rontgene M. Solante, MD, FPCP,FPSMID Learning Objectives Identify situations wherein high or low BP are hemodynamically significant Recognize complications arising from BP emergencies Manage
Septic Shock Rontgene M. Solante, MD, FPCP,FPSMID Learning Objectives Identify situations wherein high or low BP are hemodynamically significant Recognize complications arising from BP emergencies Manage
BURNS MODULE. In the paediatric population consider non-accidental injury as a mechanism for burn injuries.
 BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
TITLE OF CASE: Burn Injuries and Management
 TITLE OF CASE: Burn Injuries and Management AUTHOR OF CASE: Magdalena Malinowska SUMMARY: Patient is a 23 year old female who was brought in by EMS to the Emergency Room post a motor vehicle accident in
TITLE OF CASE: Burn Injuries and Management AUTHOR OF CASE: Magdalena Malinowska SUMMARY: Patient is a 23 year old female who was brought in by EMS to the Emergency Room post a motor vehicle accident in
EmergencyKT: Management of Thermal Injury in Adult Patients
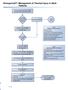 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Sepsis Update: Focus on Early Recognition and Intervention. Disclosures
 Sepsis Update: Focus on Early Recognition and Intervention Jessie Roske, MD October 2017 Disclosures I have no actual or potential conflict of interest in relation to this program/presentation. I will
Sepsis Update: Focus on Early Recognition and Intervention Jessie Roske, MD October 2017 Disclosures I have no actual or potential conflict of interest in relation to this program/presentation. I will
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Initial Resuscitation of Sepsis & Septic Shock
 Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
R2R: Severe sepsis/septic shock. Surat Tongyoo Critical care medicine Siriraj Hospital
 R2R: Severe sepsis/septic shock Surat Tongyoo Critical care medicine Siriraj Hospital Diagnostic criteria ACCP/SCCM consensus conference 1991 SCCM/ESICM/ACCP/ATS/SIS International Sepsis Definitions Conference
R2R: Severe sepsis/septic shock Surat Tongyoo Critical care medicine Siriraj Hospital Diagnostic criteria ACCP/SCCM consensus conference 1991 SCCM/ESICM/ACCP/ATS/SIS International Sepsis Definitions Conference
Clinical Evidence Summary ACCURYN ADVANCED CRITICAL CARE MONITORING
 Clinical Evidence Summary ACCURYN ADVANCED CRITICAL CARE MONITORING Table of Contents Introduction: Urine Output 3 Intensive monitoring of urine output is associated with increased detection 4 of acute
Clinical Evidence Summary ACCURYN ADVANCED CRITICAL CARE MONITORING Table of Contents Introduction: Urine Output 3 Intensive monitoring of urine output is associated with increased detection 4 of acute
Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016
 Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016 Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care
Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016 Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
SEPSIS: IT ALL BEGINS WITH INFECTION. Theresa Posani, MS, RN, ACNS-BC, CCRN M/S CNS/Sepsis Coordinator Texas Health Harris Methodist Ft.
 SEPSIS: IT ALL BEGINS WITH INFECTION Theresa Posani, MS, RN, ACNS-BC, CCRN M/S CNS/Sepsis Coordinator Texas Health Harris Methodist Ft. Worth 1 2 3 OBJECTIVES Review the new Sepsis 3 definitions of sepsis
SEPSIS: IT ALL BEGINS WITH INFECTION Theresa Posani, MS, RN, ACNS-BC, CCRN M/S CNS/Sepsis Coordinator Texas Health Harris Methodist Ft. Worth 1 2 3 OBJECTIVES Review the new Sepsis 3 definitions of sepsis
COBIS. Fluid Resuscitation in Adults ADULT GUIDELINE
 COBIS Fluid Resuscitation in Adults ADULT GUIDELINE Page 1 of 6 Fluid resuscitation in adults Summary Fluid resuscitation for adults with burns is indicated for patients with greater than 15% burns. Patients
COBIS Fluid Resuscitation in Adults ADULT GUIDELINE Page 1 of 6 Fluid resuscitation in adults Summary Fluid resuscitation for adults with burns is indicated for patients with greater than 15% burns. Patients
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE
 Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Using Big Data to Prevent Infections
 Using Big Data to Prevent Infections A thought paper by Scalable Health Big Data Analytics Reduces Infections in Hospitals Healthcare Associated Infections (HAIs) are developed while patients are receiving
Using Big Data to Prevent Infections A thought paper by Scalable Health Big Data Analytics Reduces Infections in Hospitals Healthcare Associated Infections (HAIs) are developed while patients are receiving
Support Funding for the Military Burn Research Program in FY19
 Support Funding for the Military Burn Research Program in FY19 Burns are one of the most painful and devastating battlefield injuries: 95 percent of those with burn injuries generally survive but must
Support Funding for the Military Burn Research Program in FY19 Burns are one of the most painful and devastating battlefield injuries: 95 percent of those with burn injuries generally survive but must
Burn Resuscitation Formulas. John P. Sabra, MD Seton Surgical Group Department of Surgery Dell Medical School Austin, TX
 Burn Resuscitation Formulas John P. Sabra, MD Seton Surgical Group Department of Surgery Dell Medical School Austin, TX BURN INJURY % Physiologic Change % TBSA burn Stasis BURN VASCULAR PERMEABILITY
Burn Resuscitation Formulas John P. Sabra, MD Seton Surgical Group Department of Surgery Dell Medical School Austin, TX BURN INJURY % Physiologic Change % TBSA burn Stasis BURN VASCULAR PERMEABILITY
ISF criteria (International sepsis forum consensus conference of infection in the ICU) Secondary peritonitis
 Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
No conflicts of interest to disclose
 No conflicts of interest to disclose Introduction Epidemiology Surviving sepsis guidelines 2012 Updates Resuscitation protocols Map Goals Transfusion Sepsis-3 Bundle Management Questions Sepsis is a systemic,
No conflicts of interest to disclose Introduction Epidemiology Surviving sepsis guidelines 2012 Updates Resuscitation protocols Map Goals Transfusion Sepsis-3 Bundle Management Questions Sepsis is a systemic,
Fluid Resuscitation and Monitoring in Sepsis. Deepa Gotur, MD, FCCP Anne Rain T. Brown, PharmD, BCPS
 Fluid Resuscitation and Monitoring in Sepsis Deepa Gotur, MD, FCCP Anne Rain T. Brown, PharmD, BCPS Learning Objectives Compare and contrast fluid resuscitation strategies in septic shock Discuss available
Fluid Resuscitation and Monitoring in Sepsis Deepa Gotur, MD, FCCP Anne Rain T. Brown, PharmD, BCPS Learning Objectives Compare and contrast fluid resuscitation strategies in septic shock Discuss available
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Update in Critical Care Medicine
 Update in Critical Care Medicine Michael A. Gropper, MD, PhD Professor and Executive Vice Chair Department of Anesthesia and Perioperative Care Director, Critical Care Medicine UCSF Disclosure None Update
Update in Critical Care Medicine Michael A. Gropper, MD, PhD Professor and Executive Vice Chair Department of Anesthesia and Perioperative Care Director, Critical Care Medicine UCSF Disclosure None Update
Sepsis is an important issue. Clinician s decision-making capability. Guideline recommendations
 Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012 Clinicians decision-making capability Guideline recommendations Sepsis is an important issue 8.7%
Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012 Clinicians decision-making capability Guideline recommendations Sepsis is an important issue 8.7%
HAP/VAP care bundle interventions - a UK approach. Dr R G Masterton NHS Ayrshire & Arran
 HAP/VAP care bundle interventions - a UK approach Dr R G Masterton NHS Ayrshire & Arran How Hazardous Is Health Care? (Leape and Amalberti) Total lives lost per year 100,000 10,000 1,000 100 10 1 HAZARDOUS
HAP/VAP care bundle interventions - a UK approach Dr R G Masterton NHS Ayrshire & Arran How Hazardous Is Health Care? (Leape and Amalberti) Total lives lost per year 100,000 10,000 1,000 100 10 1 HAZARDOUS
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
CURRICULUM FOR FELLOWSHIP IN CRITICAL CARE MEDICINE
 CURRICULUM FOR FELLOWSHIP IN CRITICAL CARE MEDICINE AIM: The course has been designed to train candidates by the anesthesiologists in the principles and practice of intensive care & artificial ventilation
CURRICULUM FOR FELLOWSHIP IN CRITICAL CARE MEDICINE AIM: The course has been designed to train candidates by the anesthesiologists in the principles and practice of intensive care & artificial ventilation
Sepsis Early Recognition and Management. Therese Hughes, PhD, MPA, RN
 Sepsis Early Recognition and Management Therese Hughes, PhD, MPA, RN 1 Sepsis a Deadly Progression Affects millions around the world each year, killing one in four Contributes to approximately 50% of all
Sepsis Early Recognition and Management Therese Hughes, PhD, MPA, RN 1 Sepsis a Deadly Progression Affects millions around the world each year, killing one in four Contributes to approximately 50% of all
Sepsis clinical evolution: Understand essential challenges to developing effective queries
 Understand essential challenges to developing effective queries ADVICE FROM THE ACDIS REGULATORY COMMITTEE Summary: This paper provides a timeline of the various sepsis definitions and their implications
Understand essential challenges to developing effective queries ADVICE FROM THE ACDIS REGULATORY COMMITTEE Summary: This paper provides a timeline of the various sepsis definitions and their implications
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
Surviving Sepsis Campaign. Guidelines for Management of Severe Sepsis/Septic Shock. An Overview
 Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Dry body skin has a ( higher / lower ) resistance to the flow of the electric current than the internal organs of the body.
 RESISTANCE OF INTERNAL ORGANS (SUCH AS HEART, LUNGS, LIVER, ETC.) Dry body skin has a ( higher / lower ) resistance to the flow of the electric current than the internal organs of the body. 19. Electricity
RESISTANCE OF INTERNAL ORGANS (SUCH AS HEART, LUNGS, LIVER, ETC.) Dry body skin has a ( higher / lower ) resistance to the flow of the electric current than the internal organs of the body. 19. Electricity
Nurse Driven Fluid Optimization Using Dynamic Assessments
 Nurse Driven Fluid Optimization Using Dynamic Assessments 2016 1 WHAT WE BELIEVE We believe that clinicians make vital fluid and drug decisions every day with limited and inconclusive information Cheetah
Nurse Driven Fluid Optimization Using Dynamic Assessments 2016 1 WHAT WE BELIEVE We believe that clinicians make vital fluid and drug decisions every day with limited and inconclusive information Cheetah
Pediatric Code Blue. Goals of Resuscitation. Focus Conference November Ensure organ perfusion
 Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
How can the PiCCO improve protocolized care?
 How can the PiCCO improve protocolized care? Azriel Perel Professor and Chairman Department of Anesthesiology and Intensive Care Sheba Medical Center, Tel Aviv University, Israel ESICM, Vienna 2009 Disclosure
How can the PiCCO improve protocolized care? Azriel Perel Professor and Chairman Department of Anesthesiology and Intensive Care Sheba Medical Center, Tel Aviv University, Israel ESICM, Vienna 2009 Disclosure
Disclosures. Objectives. Procalcitonin: Pearls and Pitfalls in Daily Practice
 Procalcitonin: Pearls and Pitfalls in Daily Practice Sarah K Harrison, PharmD, BCCCP Clinical Pearl Disclosures The author of this presentation has no disclosures concerning possible financial or personal
Procalcitonin: Pearls and Pitfalls in Daily Practice Sarah K Harrison, PharmD, BCCCP Clinical Pearl Disclosures The author of this presentation has no disclosures concerning possible financial or personal
SEPSIS & SEPTIC SHOCK
 SEPSIS & SEPTIC SHOCK DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential bias
SEPSIS & SEPTIC SHOCK DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential bias
OHSU. Update in Sepsis
 Update in Sepsis Jonathan Pak, MD June 1, 2017 Structure of Talk 1. Sepsis-3: The latest definition 2. Clinical Management - Is EGDT dead? - Surviving Sepsis Campaign Guidelines 3. A novel therapy: Vitamin
Update in Sepsis Jonathan Pak, MD June 1, 2017 Structure of Talk 1. Sepsis-3: The latest definition 2. Clinical Management - Is EGDT dead? - Surviving Sepsis Campaign Guidelines 3. A novel therapy: Vitamin
EFFECT OF EARLY VASOPRESSIN VS NOREPINEPHRINE ON KIDNEY FAILURE IN PATIENTS WITH SEPTIC SHOCK. Alexandria Rydz
 EFFECT OF EARLY VASOPRESSIN VS NOREPINEPHRINE ON KIDNEY FAILURE IN PATIENTS WITH SEPTIC SHOCK Alexandria Rydz BACKGROUND- SEPSIS Sepsis is defined as life-threatening organ dysfunction caused by a dysregulated
EFFECT OF EARLY VASOPRESSIN VS NOREPINEPHRINE ON KIDNEY FAILURE IN PATIENTS WITH SEPTIC SHOCK Alexandria Rydz BACKGROUND- SEPSIS Sepsis is defined as life-threatening organ dysfunction caused by a dysregulated
Sepsi: nuove definizioni, approccio diagnostico e terapia
 GIORNATA MONDIALE DELLA SEPSI DIAGNOSI E GESTIONE CLINICA DELLA SEPSI Giovedì, 13 settembre 2018 Sepsi: nuove definizioni, approccio diagnostico e terapia Nicola Petrosillo Società Italiana Terapia Antiinfettiva
GIORNATA MONDIALE DELLA SEPSI DIAGNOSI E GESTIONE CLINICA DELLA SEPSI Giovedì, 13 settembre 2018 Sepsi: nuove definizioni, approccio diagnostico e terapia Nicola Petrosillo Società Italiana Terapia Antiinfettiva
Sepsis. From EMS to ER to ICU. What we need to be doing
 Sepsis From EMS to ER to ICU What we need to be doing NEHAL BHATT, MD ATHENS PULMONARY, CRITICAL CARE AND SLEEP Objectives 1. Define the changes to the definition of Sepsis 2. Describe the assessment,
Sepsis From EMS to ER to ICU What we need to be doing NEHAL BHATT, MD ATHENS PULMONARY, CRITICAL CARE AND SLEEP Objectives 1. Define the changes to the definition of Sepsis 2. Describe the assessment,
CHAPTER 3. The Human Body National Safety Council
 CHAPTER 3 The Human Body The Human Body Composed of many different organs and tissues All parts work together: To sustain life Allow activity Injury or illness impairs functions 3-3 Cranial located in
CHAPTER 3 The Human Body The Human Body Composed of many different organs and tissues All parts work together: To sustain life Allow activity Injury or illness impairs functions 3-3 Cranial located in
How Well Does The Parkland Formula Estimate Actual Fluid Resuscitation Volumes?
 How Well Does The Parkland Formula Estimate Actual Fluid Resuscitation Volumes? Robert C. Cartotto, MD, FRCS(C), Marilyn Innes, BA, Melinda A. Musgrave, PhD, MD, Manuel Gomez, MD, Andrew B. Cooper, MD,
How Well Does The Parkland Formula Estimate Actual Fluid Resuscitation Volumes? Robert C. Cartotto, MD, FRCS(C), Marilyn Innes, BA, Melinda A. Musgrave, PhD, MD, Manuel Gomez, MD, Andrew B. Cooper, MD,
New Strategies in the Management of Patients with Severe Sepsis
 New Strategies in the Management of Patients with Severe Sepsis Michael Zgoda, MD, MBA President, Medical Staff Medical Director, ICU CMC-University, Charlotte, NC Factors of increases in the dx. of severe
New Strategies in the Management of Patients with Severe Sepsis Michael Zgoda, MD, MBA President, Medical Staff Medical Director, ICU CMC-University, Charlotte, NC Factors of increases in the dx. of severe
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
Online Supplement for:
 Online Supplement for: INFLUENCE OF COMBINED INTRAVENOUS AND TOPICAL ANTIBIOTIC PROPHYLAXIS ON THE INCIDENCE OF INFECTIONS, ORGAN DYSFUNCTIONS, AND MORTALITY IN CRITICALLY ILL SURGICAL PATIENTS A PROSPECTIVE,
Online Supplement for: INFLUENCE OF COMBINED INTRAVENOUS AND TOPICAL ANTIBIOTIC PROPHYLAXIS ON THE INCIDENCE OF INFECTIONS, ORGAN DYSFUNCTIONS, AND MORTALITY IN CRITICALLY ILL SURGICAL PATIENTS A PROSPECTIVE,
4/5/2018. Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY. I have no financial disclosures
 Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY I have no financial disclosures 1 Objectives Why do we care about sepsis Understanding the core measures by Centers for Medicare
Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY I have no financial disclosures 1 Objectives Why do we care about sepsis Understanding the core measures by Centers for Medicare
Critical Care Medicine: Landmarks and Legends 1305 Matthew R. Rosengart
 CRITICAL CARE FOR THE GENERAL SURGEON Foreword Ronald F. Martin xiii Preface Juan Carlos Puyana and Matthew R. Rosengart xvii Critical Care Medicine: Landmarks and Legends 1305 Matthew R. Rosengart Critical
CRITICAL CARE FOR THE GENERAL SURGEON Foreword Ronald F. Martin xiii Preface Juan Carlos Puyana and Matthew R. Rosengart xvii Critical Care Medicine: Landmarks and Legends 1305 Matthew R. Rosengart Critical
Text-based Document. Implications of the Sepsis-3 Definition on Nursing Research and Practice. Authors Peach, Brian C. Downloaded 5-Jul :03:48
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1070 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: CARDIOVASCULAR INTENSIVE Job Title of Reviewer: Director, CVICU EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY
PS1070 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: CARDIOVASCULAR INTENSIVE Job Title of Reviewer: Director, CVICU EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY
Titrating Critical Care Medications
 Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
RESPIRATORY COMPLICATIONS AFTER SCI
 SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
High-Acuity Nursing. Global edition. Global edition. Kathleen Dorman Wagner Melanie G. Hardin-Pierce
 High-Acuity Nursing For these Global Editions, the editorial team at Pearson has collaborated with educators across the world to address a wide range of subjects and requirements, equipping students with
High-Acuity Nursing For these Global Editions, the editorial team at Pearson has collaborated with educators across the world to address a wide range of subjects and requirements, equipping students with
Diagnosis Coding Problematic Areas: Coding & Sequencing
 Diagnosis Coding Problematic Areas: Coding & Sequencing OBJECTIVES Guideline information Sepsis, Severe Sepsis, Septic Shock HIV Diabetes Under/Over-dosing Hypertension Ulcers Burns INCLUDES, USE ADDITIONAL
Diagnosis Coding Problematic Areas: Coding & Sequencing OBJECTIVES Guideline information Sepsis, Severe Sepsis, Septic Shock HIV Diabetes Under/Over-dosing Hypertension Ulcers Burns INCLUDES, USE ADDITIONAL
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Current State of Pediatric Sepsis. Jason Clayton, MD PhD Pediatric Critical Care 9/19/2018
 Current State of Pediatric Sepsis Jason Clayton, MD PhD Pediatric Critical Care 9/19/2018 Objectives Review the history of pediatric sepsis Review the current definition of pediatric sepsis Review triage
Current State of Pediatric Sepsis Jason Clayton, MD PhD Pediatric Critical Care 9/19/2018 Objectives Review the history of pediatric sepsis Review the current definition of pediatric sepsis Review triage
Sepsis 3.0: The Impact on Quality Improvement Programs
 Sepsis 3.0: The Impact on Quality Improvement Programs Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care Warren Alpert Medical School of Brown University
Sepsis 3.0: The Impact on Quality Improvement Programs Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care Warren Alpert Medical School of Brown University
Advanced Cardiac Life Support (ACLS) Science Update 2015
 1 2 3 4 5 6 7 8 9 Advanced Cardiac Life Support (ACLS) Science Update 2015 What s New in ACLS for 2015? Adult CPR CPR remains (Compressions, Airway, Breathing Chest compressions has priority over all other
1 2 3 4 5 6 7 8 9 Advanced Cardiac Life Support (ACLS) Science Update 2015 What s New in ACLS for 2015? Adult CPR CPR remains (Compressions, Airway, Breathing Chest compressions has priority over all other
Evidence-Based. Management of Severe Sepsis. What is the BP Target?
 Evidence-Based Management of Severe Sepsis Michael A. Gropper, MD, PhD Professor and Vice Chair of Anesthesia Director, Critical Care Medicine Chair, Quality Improvment University of California San Francisco
Evidence-Based Management of Severe Sepsis Michael A. Gropper, MD, PhD Professor and Vice Chair of Anesthesia Director, Critical Care Medicine Chair, Quality Improvment University of California San Francisco
SEP-1 CHALLENGING CASES WITH DR. TOWNSEND
 UW MEDICINE PATIENTS ARE FIRST SEP-1 CHALLENGING CASES WITH DR. TOWNSEND AMADAE AREVALO RN, MSN, CCRN KATIE MEHRING RN, BSN, CCDS AMANDA SIGALA, RN, BSN, MPH, CPHQ JUNE 12, 2018 OBJECTIVES 1. Summarize
UW MEDICINE PATIENTS ARE FIRST SEP-1 CHALLENGING CASES WITH DR. TOWNSEND AMADAE AREVALO RN, MSN, CCRN KATIE MEHRING RN, BSN, CCDS AMANDA SIGALA, RN, BSN, MPH, CPHQ JUNE 12, 2018 OBJECTIVES 1. Summarize
Product Catalog. Pediatric Learning Solutions. Listing of all current products (as of May, 2013) offered by Children's Hospital Association.
 Product Catalog Pediatric Learning Solutions Listing of all current products (as of May, 2013) offered by Children's Hospital Association. Acquired Heart Disease in Children WBT Acute Respiratory Distress
Product Catalog Pediatric Learning Solutions Listing of all current products (as of May, 2013) offered by Children's Hospital Association. Acquired Heart Disease in Children WBT Acute Respiratory Distress
Surviving Sepsis Campaign Guidelines 2012 & Update for David E. Tannehill, DO Critical Care Medicine Mercy Hospital St.
 Surviving Sepsis Campaign Guidelines 2012 & Update for 2015 David E. Tannehill, DO Critical Care Medicine Mercy Hospital St. Louis Be appropriately aggressive the longer one delays aggressive metabolic
Surviving Sepsis Campaign Guidelines 2012 & Update for 2015 David E. Tannehill, DO Critical Care Medicine Mercy Hospital St. Louis Be appropriately aggressive the longer one delays aggressive metabolic
MAKING SENSE OF IT ALL AUGUST 17
 MAKING SENSE OF IT ALL AUGUST 17 @SepsisUK Dr Ron Daniels B.E.M. CEO, UK Sepsis Trust CEO, Global Sepsis Alliance Special Adviser to WHO SCALE AND BURDEN @sepsisuk Dr Ron Daniels B.E.M. CEO, UK Sepsis
MAKING SENSE OF IT ALL AUGUST 17 @SepsisUK Dr Ron Daniels B.E.M. CEO, UK Sepsis Trust CEO, Global Sepsis Alliance Special Adviser to WHO SCALE AND BURDEN @sepsisuk Dr Ron Daniels B.E.M. CEO, UK Sepsis
VAP Prevention bundles
 VAP Prevention bundles Dr. Shafiq A.Alimad MD Head of medical department at USTH YICID workshop, 15-12-2014 Care Bundles What are they & why use them? What are Care Bundles? Types of Care Bundles available
VAP Prevention bundles Dr. Shafiq A.Alimad MD Head of medical department at USTH YICID workshop, 15-12-2014 Care Bundles What are they & why use them? What are Care Bundles? Types of Care Bundles available
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2)
 Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
CHAPTER 3. The Human Body National Safety Council
 CHAPTER 3 The Human Body Lesson Objectives 1. Describe the primary areas of the body. 2. List the 10 body systems and explain a key function of each. 3. For each body system, describe at least 1 injury
CHAPTER 3 The Human Body Lesson Objectives 1. Describe the primary areas of the body. 2. List the 10 body systems and explain a key function of each. 3. For each body system, describe at least 1 injury
ANWICU knowledge
 ANWICU knowledge www.anwicu.org.uk This presenta=on is provided by ANWICU We are a collabora=ve associa=on of ICUs in the North West of England. Permission to provide this presenta=on has been granted
ANWICU knowledge www.anwicu.org.uk This presenta=on is provided by ANWICU We are a collabora=ve associa=on of ICUs in the North West of England. Permission to provide this presenta=on has been granted
The changing face of
 The changing face of sepsis. @SepsisUK Dr Ron Daniels B.E.M. CEO, UK Sepsis Trust CEO, Global Sepsis Alliance Special Adviser (maternal sepsis) to WHO Breast cancer Cognitive impairment Mild 3.8 7.1
The changing face of sepsis. @SepsisUK Dr Ron Daniels B.E.M. CEO, UK Sepsis Trust CEO, Global Sepsis Alliance Special Adviser (maternal sepsis) to WHO Breast cancer Cognitive impairment Mild 3.8 7.1
EMERGENCY MEDICAL SERVICES ONLINE COURSE CATALOG. TargetSolutions. Technology with a Purpose
 EMERGENCY MEDICAL SERVICES ONLINE COURSE CATALOG 1 Technology with a Purpose TargetSolutions delivers employee training that helps organizations achieve compliance, mitigate We risk, believe reduce a well-trained
EMERGENCY MEDICAL SERVICES ONLINE COURSE CATALOG 1 Technology with a Purpose TargetSolutions delivers employee training that helps organizations achieve compliance, mitigate We risk, believe reduce a well-trained
Case Scenario 3: Shock and Sepsis
 Name: Molly Boyle 1. Define the term shock (Lewis textbook): Shock is a syndrome characterized by decreased perfusion and impaired metabolism. Shock can have a number of causes that result in damage to
Name: Molly Boyle 1. Define the term shock (Lewis textbook): Shock is a syndrome characterized by decreased perfusion and impaired metabolism. Shock can have a number of causes that result in damage to
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen
 Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
DESIGNER RESUSCITATION: TITRATING TO TISSUE NEEDS
 DESIGNER RESUSCITATION: TITRATING TO TISSUE NEEDS R. Phillip Dellinger MD, MSc, MCCM Professor and Chair of Medicine Cooper Medical School of Rowan University Chief of Medicine Cooper University Hospital
DESIGNER RESUSCITATION: TITRATING TO TISSUE NEEDS R. Phillip Dellinger MD, MSc, MCCM Professor and Chair of Medicine Cooper Medical School of Rowan University Chief of Medicine Cooper University Hospital
SHOCK Susanna Hilda Hutajulu, MD, PhD
 SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
Prescribe appropriate immunizations for. Prescribe childhood immunization as per. Prescribe influenza vaccinations in high-risk
 Supplemental Digital Appendix 1 46 Health Care Problems and the Corresponding 59 Practice Indicators Expected of All Physicians Entering or in Practice Infectious and parasitic diseases Avoidable complications/death
Supplemental Digital Appendix 1 46 Health Care Problems and the Corresponding 59 Practice Indicators Expected of All Physicians Entering or in Practice Infectious and parasitic diseases Avoidable complications/death
Sepsis Management: Past, Present, and Future
 Sepsis Management: Past, Present, and Future Benjamin Ferrell, MD Tennessee ACP Meeting October 28, 2017 Learning Objectives Identify the most updated definition and clinical criteria for sepsis Describe
Sepsis Management: Past, Present, and Future Benjamin Ferrell, MD Tennessee ACP Meeting October 28, 2017 Learning Objectives Identify the most updated definition and clinical criteria for sepsis Describe
Sepsis: Identification and Management in an Acute Care Setting
 Sepsis: Identification and Management in an Acute Care Setting Dr. Barbara M. Mills DNP Director Rapid Response Team/ Code Resuscitation Stony Brook University Medical Center SEPSIS LECTURE NPA 2018 OBJECTIVES
Sepsis: Identification and Management in an Acute Care Setting Dr. Barbara M. Mills DNP Director Rapid Response Team/ Code Resuscitation Stony Brook University Medical Center SEPSIS LECTURE NPA 2018 OBJECTIVES
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
The Septic Patient. Dr Arunraj Navaratnarajah. Renal SpR Imperial College NHS Healthcare Trust
 The Septic Patient Dr Arunraj Navaratnarajah Renal SpR Imperial College NHS Healthcare Trust Objectives of this session Define SIRS / sepsis / severe sepsis / septic shock Early recognition of Sepsis The
The Septic Patient Dr Arunraj Navaratnarajah Renal SpR Imperial College NHS Healthcare Trust Objectives of this session Define SIRS / sepsis / severe sepsis / septic shock Early recognition of Sepsis The
