Syncope: Ockham s Razor
|
|
|
- Gilbert Dawson
- 6 years ago
- Views:
Transcription
1 Syncope: Ockham s Razor Time/Place Wednesday, 25 th January am-12pm Room 210, Wallace Wurth Building Facilitators Michael Grimm & Tony Grabs Aims Illustrate multiple possible causes for a common presenting symptom. Illustrate the way tests can turn up pathology which may not be relevant to the symptomatology but nonetheless needs to be dealt with. Illustrate the frequent co-existence of multiple pathology especially in older patients. Abstract Mr Smith is a 73 year old male who presents to the Emergency Department following a collapse. Clinical assessment and several investigations reveal multiple abnormalities, some of which may explain his presenting problem. Readings Preparation Read the case thoroughly before the case method tutorial and come prepared to discuss your perceptions and reflections. Consider the following questions: 1. What features of this case did not add up to a simple diagnosis and why? How reliable is history from a relative? 2. Were all the investigations performed appropriate and necessary? 3. Mr Smith was admitted under the care of the Cardiology team. Why do you think this was done and would it have been more appropriate to admit under Neurology? 4. Coronary disease is very common. Syncope is also common. Why did you conclude that the two were unlikely to be causally related in Mr Smith? 5. What would your approach to Mr Smith have been had he not suffered the syncopal episode at all but came to see you in a preoperative clinic prior to admission for hernia repair, and you found the ECG and clinical findings outlined on his presentation above (trifascicular block; systolic aortic murmur)? Would you have ordered further tests and would you have recommended it was safe for him to go to surgery? 6. What tools are available for assessing severity of valvular heart disease and how do these differ from other cardiac investigations? 7. How will you assess the relevance of the tachycardia discovered on the ECG monitor in hospital? Page 1
2 8. Where should you go from here in terms of managing Mr Smith? 9. What is Ockham s razor and what is its relevance to medicine and in particular, the making of diagnoses? Page 2
3 OCKHAM S RAZOR Presenting Complaint Mr William Smith, aged 73, presented to the Emergency Department via ambulance on a Sunday afternoon when you are working a day shift as an intern (it s in fact your first weekend shift but luckily you were an excellent student so you feel reasonably confident! So far you have sutured a few lacerations but now it seems there is a patient with a more complex and challenging problem). On arrival, Mr Smith is confused and agitated and a little uncertain as to why he is there at all. Fortunately his wife accompanied him in the ambulance and you are able to talk to her. She tells you that he was just about to set off for a regular walk to the park when he put his hand to his chest, became a little pale and sweaty and looked quite unwell and collapsed to the floor in front of her, hitting his head on the wall on the way down but not doing any major injury. Initial Assessment in the Emergency Department Your initial assessment of Mr Smith reveals that he is haemodynamically stable with a blood pressure of 120/80 and a heart rate of 75 and while the ED nurse is doing an ECG, you take the opportunity of talking further to his wife. You ask her more about what happened today. She is adamant that he was in fact unconscious but only for seconds. She says he became quite pale but she did not think to check whether or not he had a pulse. After this fairly brief period he became awake again and reasonably lucid, although somewhat confused and agitated, and had no real recollection of what had happened. His state had remained much the same over the following thirty minutes or so, which was the time that it took for the ambulance to arrive and for him to reach the Emergency Department. Mrs Smith tells you that he has been generally fit and well but has complained occasionally of a tight feeling in the chest on his regular walks over the last year or two. He has also complained to her on a couple of occasions of rapid flutters in his chest lasting only a few seconds, which he has ignored. He has never lost consciousness before like this. He has a history of hypertension going back some twenty years or so she thinks, and for which he currently takes perindopril 4mg daily. He also takes aspirin daily (on his GP s advice). His wife does not know what his cholesterol is but believes that it has been normal and has not required treatment. Mr Smith smoked 20 cigarettes a day from the age of twenty to about the age of fifty when he gave them up with some difficulty but has not smoked since. He drinks one or two light beers a day and has never been a heavy drinker. He is a retired businessman who has no financial worries. Page 3
4 On examination The blood pressure and heart rate noted on admission have not changed significantly. You find no signs of cardiac failure but do notice on auscultation that he has relatively normal heart sounds but a moderately loud mid-systolic ejection murmur which fills most of systole and is audible all over the precordium and radiates into the carotid arteries. Neurological examination is completely normal and Mr Smith is now fully oriented to time and place but still has no recollection at all of his actual collapse. The remainder of his physical examination is unremarkable, apart from him being overweight. His ECG is provided (see figure 1). This shows a prolonged PR interval (first degree heart block), a right bundle branch block and marked left axis deviation due to left anterior hemi-block. This combination is commonly referred to as trifascicular block. As a conscientious intern, you form your own provisional diagnosis and suggest investigations and management, but then of course discuss these with your team members (registrar and consultant). Progress You discuss the case with the medical registrar and admit Mr Smith under what turns out to be the cardiology team that you are commencing work with the following day (Monday). The blood tests you carried out in the Emergency Department show no evidence of myocardial infarction (troponin was normal on both Sunday afternoon and Sunday evening); cholesterol is 5.8 mmol/l (normal < 5.5 mmol/l) and his urea, electrolytes and creatinine are all normal. He is HIV negative and his liver function and thyroid function are normal. A chest x-ray is normal except for some calcification in the area of the aortic valve. Subsequent investigations You are concerned about the possibility that Mr Smith may have suffered an episode of complete heart block related to his trifascicular block and so you monitor his ECG and organise for him to have a Holter monitor carried out in the next couple of days. This is 24 hour recording of the ECG, which is recorded and subsequently analysed by computer. The patient is able to press a button and make notes at the time of any symptoms or event such as chest pain or palpitations, so that the test can correlate changes in the ECG with clinical events. However, rhythm disturbances can be detected even in the absence of the patient highlighting an event. You are keen also to document whether or not your provisional clinical diagnosis of aortic stenosis is accurate and you arrange for him to have an echocardiogram. This Page 4
5 shows normal left ventricular function with borderline hypertrophy of the left ventricular wall. The aortic valve is thickened, disorganised and calcified and there is a peak gradient across the aortic valve of 60mmHg, (normally of course, there is no gradient across an open aortic valve). Cardiac catheterisation Both in order to confirm your diagnosis and also to check for possible co-existent coronary artery disease (a very important piece of information for a surgeon contemplating operating on this man s aortic valve), you suggest (and your team agrees) that he should have coronary angiography in the cardiac catheter laboratory. The cardiac catheter report is attached (figure 2). As you can see, it confirms moderate aortic stenosis and some co-existent coronary disease, which may well need to be dealt with at the time of any contemplated surgery. Assessment You are still a little uncertain as to the pathogenesis of the event that occurred on the previous weekend. You know from your reading around this case by now, that aortic stenosis can present with syncope due to an inappropriate haemodynamic response to a pressure overload. You also know that this is not terribly common as a first presentation and nor is it very common in moderate aortic stenosis which is what Mr Smith appears to be suffering from. You are also still drawn to your initial diagnosis, which was that of intermittent complete heart block associated with trifascicular block. You know that this can occur in association with or quite separate from aortic valve disease. Your training has warned you against unnecessarily multiplying diagnoses (Ockham s razor), and you are very keen to combine all or most of your findings into one or as few as diagnoses as possible. You know that aortic valve disease is commonly associated with abnormalities of the ventricular conduction system and this may well provide a link between several of Mr Smith s problems. Coronary artery disease is common but it seems unlikely to you from your experience and reading, that Mr Smith s coronary disease is the cause of his presentation, although this is not impossible. While contemplating all of this, you are called to the ward by the nursing staff who have noticed an intermittent tachyarrhythmia on Mr Smith s ECG, (figure 3). This long rhythm strip is from a single lead (V1), showing underlying sinus rhythm (you note that the PR interval is normal at this stage but are also conscious of the fact that PR intervals can vary). The patient is suffering from runs of a broad- complex, slightly irregular tachycardia, which you consider possibly to be ventricular tachycardia or alternately atrial fibrillation with aberrant intraventricular conduction due to the rapid rate. Page 5
6 You are interested in whether or not Mr Smith is symptomatic while this is happening and you find that he is completely unaware of his arrhythmia at present, although he does tell you that he has noticed occasional palpitations overnight, similar to those he had mentioned to his wife in the past. Summary and Issues Mr Smith is a 73 year old male who has presented following a collapse. You have identified several potential diagnoses (and corresponding potential treatments) for Mr Smith s presenting symptom. Page 6
ECG Workshop. Nezar Amir
 ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
5AB Dysrhythmia Interpretation and Management 2016
 5AB Dysrhythmia Interpretation and Management 2016 How to complete your biennial ECG review: A website has been created that contains the basic review information. Use this as a reference during your review.
5AB Dysrhythmia Interpretation and Management 2016 How to complete your biennial ECG review: A website has been created that contains the basic review information. Use this as a reference during your review.
Appendix D Output Code and Interpretation of Analysis
 Appendix D Output Code and Interpretation of Analysis 8 Arrhythmia Code No. Description 8002 Marked rhythm irregularity 8110 Sinus rhythm 8102 Sinus arrhythmia 8108 Marked sinus arrhythmia 8120 Sinus tachycardia
Appendix D Output Code and Interpretation of Analysis 8 Arrhythmia Code No. Description 8002 Marked rhythm irregularity 8110 Sinus rhythm 8102 Sinus arrhythmia 8108 Marked sinus arrhythmia 8120 Sinus tachycardia
HEART CONDITIONS IN SPORT
 HEART CONDITIONS IN SPORT Dr. Anita Green CHD Risk Factors Smoking Hyperlipidaemia Hypertension Obesity Physical Inactivity Diabetes Risks are cumulative (multiplicative) Lifestyles predispose to RF One
HEART CONDITIONS IN SPORT Dr. Anita Green CHD Risk Factors Smoking Hyperlipidaemia Hypertension Obesity Physical Inactivity Diabetes Risks are cumulative (multiplicative) Lifestyles predispose to RF One
What is the next best step in management?
 MQs Syncope Question 1 60- year- old man was admitted after an episode of transient loss of consciousness. He and his wife described walking down the street and then him just going down with a minimal
MQs Syncope Question 1 60- year- old man was admitted after an episode of transient loss of consciousness. He and his wife described walking down the street and then him just going down with a minimal
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
A walk through a STEMI
 A walk through a STEMI M.M. s Story Kim Robison Ashley Corcoran Situation M.M. is an 82 year old male brought in by private vehicle on 10/22/17 to the Emergency Department Pt. c/o left arm numbness, pain
A walk through a STEMI M.M. s Story Kim Robison Ashley Corcoran Situation M.M. is an 82 year old male brought in by private vehicle on 10/22/17 to the Emergency Department Pt. c/o left arm numbness, pain
SAUDI FELLOWSHIP TRAINING PROGRAM. Adult Cardiology. Final Written Examination 2019
 SAUDI FELLOWSHIP TRAINING PROGRAM Adult Cardiology Final Written Examination 2019 Objectives 1. Determine the trainee has sufficient competency related to the required specialty. 2. Determine the eligibility
SAUDI FELLOWSHIP TRAINING PROGRAM Adult Cardiology Final Written Examination 2019 Objectives 1. Determine the trainee has sufficient competency related to the required specialty. 2. Determine the eligibility
AF in the ER: Common Scenarios CASE 1. Fast facts. Diagnosis. Management
 AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
Lynne-Supraventricular Tachycardia-Pacemaker
 Lynne-Supraventricular Tachycardia-Pacemaker A mother s perspective Amy started fainting unexpectedly as a child. When she was checked by a doctor, her heart rhythm was always normal so she was told she
Lynne-Supraventricular Tachycardia-Pacemaker A mother s perspective Amy started fainting unexpectedly as a child. When she was checked by a doctor, her heart rhythm was always normal so she was told she
physiology 6 Mohammed Jaafer Turquoise team
 15 physiology 6 Mohammed Jaafer 22-3-2016 Turquoise team Cardiac Arrhythmias and Their Electrocardiographic Interpretation Today, we are going to talk about the abnormal excitation. As we said before,
15 physiology 6 Mohammed Jaafer 22-3-2016 Turquoise team Cardiac Arrhythmias and Their Electrocardiographic Interpretation Today, we are going to talk about the abnormal excitation. As we said before,
Hatim Al Lawati. MD, FRCPC, DABIM(CV), FACC
 Hatim Al Lawati. MD, FRCPC, DABIM(CV), FACC Consultant Interventional Cardiology & Structural Heart Disease Department of Medicine Sultan Qaboos University Hospital hatim.al.lawati@gmail.com April 2017
Hatim Al Lawati. MD, FRCPC, DABIM(CV), FACC Consultant Interventional Cardiology & Structural Heart Disease Department of Medicine Sultan Qaboos University Hospital hatim.al.lawati@gmail.com April 2017
Syncope Due to Intracavitary Left Ventricular Obstruction Secondary to Giant Esophageal Hiatus Hernia
 American Journal of Medical Case Reports, 2017, Vol. 5, No. 4, 89-93 Available online at http://pubs.sciepub.com/ajmcr/5/4/4 Science and Education Publishing DOI:10.12691/ajmcr-5-4-4 Syncope Due to Intracavitary
American Journal of Medical Case Reports, 2017, Vol. 5, No. 4, 89-93 Available online at http://pubs.sciepub.com/ajmcr/5/4/4 Science and Education Publishing DOI:10.12691/ajmcr-5-4-4 Syncope Due to Intracavitary
Pathological Arrhythmias/ Tachyarrhythmias
 Pathological Arrhythmias/ Tachyarrhythmias caused by: 1.Ectopic focus: Extrasystole or premature beat. If discharge is occasional. Can be: Atrial Extrasystole Vevtricular Extrasystole 2.Cardiac Arrhythmia
Pathological Arrhythmias/ Tachyarrhythmias caused by: 1.Ectopic focus: Extrasystole or premature beat. If discharge is occasional. Can be: Atrial Extrasystole Vevtricular Extrasystole 2.Cardiac Arrhythmia
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
2018 HPN Provider Summary Guide. Adult Cardiology Patients (18 Years and Older) Referral Guidelines
 12.2 CARDIOLOGY REFERRAL GUIDELINES Contracted Group: Southwest Medical Associates For Appointments: 888 S. Rancho Las Vegas, NV 89109 Phone: (702) 877-8654 Fax: (702) 242-7998 Adult Cardiology Patients
12.2 CARDIOLOGY REFERRAL GUIDELINES Contracted Group: Southwest Medical Associates For Appointments: 888 S. Rancho Las Vegas, NV 89109 Phone: (702) 877-8654 Fax: (702) 242-7998 Adult Cardiology Patients
Skin supplied by T1-4 (medial upper arm and neck) T5-9- epigastrium Visceral afferents from skin and heart are the same dorsal root ganglio
 Cardio 2 ECG... 3 Cardiac Remodelling... 11 Valvular Diseases... 13 Hypertension... 18 Aortic Coarctation... 24 Erythropoiesis... 27 Haemostasis... 30 Anaemia... 36 Atherosclerosis... 44 Angina... 48 Myocardial
Cardio 2 ECG... 3 Cardiac Remodelling... 11 Valvular Diseases... 13 Hypertension... 18 Aortic Coarctation... 24 Erythropoiesis... 27 Haemostasis... 30 Anaemia... 36 Atherosclerosis... 44 Angina... 48 Myocardial
Management of ATRIAL FIBRILLATION. in general practice. 22 BPJ Issue 39
 Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Congestive Heart Failure or Heart Failure
 Congestive Heart Failure or Heart Failure Dr Hitesh Patel Ascot Cardiology Group Heart Failure Workshop April, 2014 Question One What is the difference between congestive heart failure and heart failure?
Congestive Heart Failure or Heart Failure Dr Hitesh Patel Ascot Cardiology Group Heart Failure Workshop April, 2014 Question One What is the difference between congestive heart failure and heart failure?
15 16 September Seminar W10O. ECG for General Practice
 15 16 September 2012 Seminar W10O ECG for General Practice Speaker: Ms Natasha Eaton ECG for General Practice Speaker: Natasha Eaton Cardiac CNC Executive Representative Electrocardiography The graphic
15 16 September 2012 Seminar W10O ECG for General Practice Speaker: Ms Natasha Eaton ECG for General Practice Speaker: Natasha Eaton Cardiac CNC Executive Representative Electrocardiography The graphic
BOXER CARDIOMYOPATHY
 BOXER CARDIOMYOPATHY by: Wendy Wallner, DVM What is Boxer cardiomyopathy? Boxer cardiomyopathy as we know it consists primarily of an electrical conduction disorder which causes the heart to beat erratically
BOXER CARDIOMYOPATHY by: Wendy Wallner, DVM What is Boxer cardiomyopathy? Boxer cardiomyopathy as we know it consists primarily of an electrical conduction disorder which causes the heart to beat erratically
HISTORY. Question: How do you interpret the patient s history? CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: 45-year-old man.
 HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
Ambulatory Electrocardiography. Holter Monitor Electrocardiography
 Ambulatory Electrocardiography Holter Monitor Electrocardiography Edward K. Chung Ambulatory Electrocardiography Holter Monitor Electrocardiography With 152 Electrocardiograms Springer-Verlag New York
Ambulatory Electrocardiography Holter Monitor Electrocardiography Edward K. Chung Ambulatory Electrocardiography Holter Monitor Electrocardiography With 152 Electrocardiograms Springer-Verlag New York
Heart Valve disease: MR. AS tough patient When to echo, When to refer, What s new
 Heart Valve disease: MR. AS tough patient When to echo, When to refer, What s new B. Sonnenberg UAH Cardiology CME Day 5 May 2015 Disclosures Speaker s or Advisory Boards: none Research grants: none (co-investigator
Heart Valve disease: MR. AS tough patient When to echo, When to refer, What s new B. Sonnenberg UAH Cardiology CME Day 5 May 2015 Disclosures Speaker s or Advisory Boards: none Research grants: none (co-investigator
HISTORY. Question: What category of heart disease is suggested by the fact that a murmur was heard at birth?
 HISTORY 23-year-old man. CHIEF COMPLAINT: Decreasing exercise tolerance of several years duration. PRESENT ILLNESS: The patient is the product of an uncomplicated term pregnancy. A heart murmur was discovered
HISTORY 23-year-old man. CHIEF COMPLAINT: Decreasing exercise tolerance of several years duration. PRESENT ILLNESS: The patient is the product of an uncomplicated term pregnancy. A heart murmur was discovered
Severe Hypertension. Pre-referral considerations: 1. BP of arm and Leg 2. Ambulatory BP 3. Renal causes
 Severe Hypertension *Prior to making a referral, call office or Doc Halo, to speak with a Cardiologist or APP to discuss patient and possible treatment options. Please only contact the patient's cardiologist.
Severe Hypertension *Prior to making a referral, call office or Doc Halo, to speak with a Cardiologist or APP to discuss patient and possible treatment options. Please only contact the patient's cardiologist.
ECG Cases and Questions. Ashish Sadhu, MD, FHRS, FACC Electrophysiology/Cardiology
 ECG Cases and Questions Ashish Sadhu, MD, FHRS, FACC Electrophysiology/Cardiology 32 yo female Life Insurance Physical 56 yo male with chest pain Terminology Injury ST elevation Ischemia T wave inversion
ECG Cases and Questions Ashish Sadhu, MD, FHRS, FACC Electrophysiology/Cardiology 32 yo female Life Insurance Physical 56 yo male with chest pain Terminology Injury ST elevation Ischemia T wave inversion
Detection Of Heart. By Dr Gary Mo
 Detection Of Heart Disease By Dr Gary Mo Types Of Heart Disease A. Coronary Heart Disease B. Valvular Heart Disease C. Cardiac Arrhythmia ( Rhythm disturbance ) D. Heart Blocks ( Conduction Abnormalities
Detection Of Heart Disease By Dr Gary Mo Types Of Heart Disease A. Coronary Heart Disease B. Valvular Heart Disease C. Cardiac Arrhythmia ( Rhythm disturbance ) D. Heart Blocks ( Conduction Abnormalities
REtrive. REpeat. RElearn Design by. Test-Enhanced Learning based ECG practice E-book
 Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Update on Palpitations and AF February 28 th 2018
 Update on Palpitations and AF February 28 th 2018 Dr Mrinal Andrew Saha MA(Cantab) MBBS FRCP PhD Consultant Interventional Cardiologist GHNHSFT Dr Mrinal Saha Appointed 2010 Special interests: Angioplasty,
Update on Palpitations and AF February 28 th 2018 Dr Mrinal Andrew Saha MA(Cantab) MBBS FRCP PhD Consultant Interventional Cardiologist GHNHSFT Dr Mrinal Saha Appointed 2010 Special interests: Angioplasty,
Richard Grocott Mason
 Richard Grocott Mason What to do with a 50 year old man with chest pain? Does the pain sound cardiac? Is this a possible acute coronary syndrome? Does patient have a previous cardiac history? Natural history
Richard Grocott Mason What to do with a 50 year old man with chest pain? Does the pain sound cardiac? Is this a possible acute coronary syndrome? Does patient have a previous cardiac history? Natural history
Arrhythmias and congenital heart disease
 Arrhythmias and congenital heart disease Jolien Roos-Hesselink ErasmusMC Rotterdam Netherlands Patient W, born in 1969 Tetralogy of Fallot 1975 at the age of 6 years surgical correction 2002 Patient W:
Arrhythmias and congenital heart disease Jolien Roos-Hesselink ErasmusMC Rotterdam Netherlands Patient W, born in 1969 Tetralogy of Fallot 1975 at the age of 6 years surgical correction 2002 Patient W:
Study methodology for screening candidates to athletes risk
 1. Periodical Evaluations: each 2 years. Study methodology for screening candidates to athletes risk 2. Personal history: Personal history of murmur in childhood; dizziness, syncope, palpitations, intolerance
1. Periodical Evaluations: each 2 years. Study methodology for screening candidates to athletes risk 2. Personal history: Personal history of murmur in childhood; dizziness, syncope, palpitations, intolerance
Exercise Test: Practice and Interpretation. Jidong Sung Division of Cardiology Samsung Medical Center Sungkyunkwan University School of Medicine
 Exercise Test: Practice and Interpretation Jidong Sung Division of Cardiology Samsung Medical Center Sungkyunkwan University School of Medicine 2 Aerobic capacity and survival Circulation 117:614, 2008
Exercise Test: Practice and Interpretation Jidong Sung Division of Cardiology Samsung Medical Center Sungkyunkwan University School of Medicine 2 Aerobic capacity and survival Circulation 117:614, 2008
Circulation and Cardiac Emergencies. Emergency Medical Response
 Circulation and Cardiac Emergencies Lesson 19: The Circulatory System and Cardiac Emergencies You Are the Emergency Medical Responder You are called to the home of a 50-year-old man whose wife called 9-1-1
Circulation and Cardiac Emergencies Lesson 19: The Circulatory System and Cardiac Emergencies You Are the Emergency Medical Responder You are called to the home of a 50-year-old man whose wife called 9-1-1
HR: 50 bpm (Sinus) PR: 280 ms QRS: 120 ms QT: 490 ms Axis: -70. Sinus bradycardia with one ventricular escape (*)
 1? HR: 50 bpm (Sinus) PR: 280 ms QRS: 120 ms QT: 490 ms Axis: -70 1 Sinus P waves? 2 sinus cycles The pause (2 sinus cycles) suggests that the sinus fired (?) but did not conduct to the atria (i.e., missing
1? HR: 50 bpm (Sinus) PR: 280 ms QRS: 120 ms QT: 490 ms Axis: -70 1 Sinus P waves? 2 sinus cycles The pause (2 sinus cycles) suggests that the sinus fired (?) but did not conduct to the atria (i.e., missing
URN: Family name: Given name(s): Address: Initial Signature Print Name Role
 Do Not Write in this binding margin v5.00-02/2012 Mat. No.: 10206019 SW030b The State of Queensland (Queensland Health) 2012 Contact CIM@health.qld.gov.au ÌSW030bIÎ Facility: s Never Replace Clinical Judgement
Do Not Write in this binding margin v5.00-02/2012 Mat. No.: 10206019 SW030b The State of Queensland (Queensland Health) 2012 Contact CIM@health.qld.gov.au ÌSW030bIÎ Facility: s Never Replace Clinical Judgement
National Coverage Determination (NCD) for Cardiac Pacemakers (20.8)
 Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Cardiology Services Bon Secours Hospital. Mary Buckley Staff Nurse Cardiology
 Cardiology Services Bon Secours Hospital Mary Buckley Staff Nurse Cardiology Overview Philosophy Cardiology Team Referral Criteria Electrocardiograph (ECG) 24/48 Hour Holter Monitor Event Monitors 24 Hour
Cardiology Services Bon Secours Hospital Mary Buckley Staff Nurse Cardiology Overview Philosophy Cardiology Team Referral Criteria Electrocardiograph (ECG) 24/48 Hour Holter Monitor Event Monitors 24 Hour
TAVR : Caring for your patients before and after TAVR
 TAVR : Caring for your patients before and after TAVR Zubair Ahmed MD FSCAI Interventional Cardiologist Washington Regional Medical Center / Walker Heart Institute What is Aortic Valve Stenosis? AVA ~4
TAVR : Caring for your patients before and after TAVR Zubair Ahmed MD FSCAI Interventional Cardiologist Washington Regional Medical Center / Walker Heart Institute What is Aortic Valve Stenosis? AVA ~4
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM. General Instructions: ID NUMBER: FORM NAME: H F A DATE: 10/13/2017 VERSION: CONTACT YEAR NUMBER:
 ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
Clinical Case 1 A patient with a syncope Panos E. Vardas President Elect of the ESC, Prof of Cardiology, University Hospital of Crete
 Clinical Case 1 A patient with a syncope Panos E. Vardas President Elect of the ESC, Prof. of Cardiology, University Hospital of Crete Case presentation A 64-year-old male smoker, with arterial hypertension
Clinical Case 1 A patient with a syncope Panos E. Vardas President Elect of the ESC, Prof. of Cardiology, University Hospital of Crete Case presentation A 64-year-old male smoker, with arterial hypertension
Myocardial Infarction. Reading Assignment (p66-78 in Outline )
 Myocardial Infarction Reading Assignment (p66-78 in Outline ) Objectives 1. Why do ST segments go up or down in ischemia? 2. STEMI locations and culprit vessels 3. Why 15-lead ECGs? 4. What s up with avr?
Myocardial Infarction Reading Assignment (p66-78 in Outline ) Objectives 1. Why do ST segments go up or down in ischemia? 2. STEMI locations and culprit vessels 3. Why 15-lead ECGs? 4. What s up with avr?
ACEM Fellowship Examination Emergency Medicine Practice Questions VAQ (Part C)
 ACEM Fellowship Examination Emergency Medicine 2013-14 Practice Questions VAQ (Part C) Question 1 A 67- year- old lady presents to the Emergency Department (ED) with a history of increasing Shortness of
ACEM Fellowship Examination Emergency Medicine 2013-14 Practice Questions VAQ (Part C) Question 1 A 67- year- old lady presents to the Emergency Department (ED) with a history of increasing Shortness of
QUESTION EXAMPLES ECG
 ACEM Fellowship VAQ Examination QUESTION EXAMPLES ECG ECG 1: A 16 year old boy with a congenital heart problem presents to your ED with syncopal episodes. An ECG is taken. Describe and interpret his ECG
ACEM Fellowship VAQ Examination QUESTION EXAMPLES ECG ECG 1: A 16 year old boy with a congenital heart problem presents to your ED with syncopal episodes. An ECG is taken. Describe and interpret his ECG
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Mitral Regurgitation
 UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
Cardiac Conditions in Sport & Exercise. Cardiac Conditions in Sport. USA - Sudden Cardiac Death (SCD) Dr Anita Green. Sudden Cardiac Death
 Cardiac Conditions in Sport & Exercise Dr Anita Green Cardiac Conditions in Sport Sudden Cardiac Death USA - Sudden Cardiac Death (SCD)
Cardiac Conditions in Sport & Exercise Dr Anita Green Cardiac Conditions in Sport Sudden Cardiac Death USA - Sudden Cardiac Death (SCD)
Anomalous muscle bundle of the right ventricle
 British Heart Journal, 1978, 40, 1040-1045 Anomalous muscle bundle of the right ventricle Its recognition and surgical treatment M. D. LI, J. C. COLES, AND A. C. McDONALD From the Department of Paediatrics,
British Heart Journal, 1978, 40, 1040-1045 Anomalous muscle bundle of the right ventricle Its recognition and surgical treatment M. D. LI, J. C. COLES, AND A. C. McDONALD From the Department of Paediatrics,
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
A Cardiologist s Guide to Love
 A Cardiologist s Guide to Love A brief overview of what everyone should know about Palpitations, Heartache and Heartbreak! Eric J Dueweke, MD FACC Disclosure No one has yet to offer to pay me for my opinion.
A Cardiologist s Guide to Love A brief overview of what everyone should know about Palpitations, Heartache and Heartbreak! Eric J Dueweke, MD FACC Disclosure No one has yet to offer to pay me for my opinion.
The Electrocardiogram part II. Dr. Adelina Vlad, MD PhD
 The Electrocardiogram part II Dr. Adelina Vlad, MD PhD Basic Interpretation of the ECG 1) Evaluate calibration 2) Calculate rate 3) Determine rhythm 4) Determine QRS axis 5) Measure intervals 6) Analyze
The Electrocardiogram part II Dr. Adelina Vlad, MD PhD Basic Interpretation of the ECG 1) Evaluate calibration 2) Calculate rate 3) Determine rhythm 4) Determine QRS axis 5) Measure intervals 6) Analyze
Perioperative Cardiac Management. Emma Sargsyan, MD, FACP
 Perioperative Cardiac Management Emma Sargsyan, MD, FACP March 22-24, 2018 Outline Evaluation of cardiac risk prior to non-cardiac surgery Management of cardiac risk for non-cardiac surgery 2 Preop medical
Perioperative Cardiac Management Emma Sargsyan, MD, FACP March 22-24, 2018 Outline Evaluation of cardiac risk prior to non-cardiac surgery Management of cardiac risk for non-cardiac surgery 2 Preop medical
CARDIAC EXAMINATION MINI-QUIZ
 CARDIAC EXAMINATION MINI-QUIZ 1. Sitting bolt upright, your dyspneic (short of breath) patient has visible jugular venous pulsations to the angle of his jaw, which is 12 cm above his sternal angle. What
CARDIAC EXAMINATION MINI-QUIZ 1. Sitting bolt upright, your dyspneic (short of breath) patient has visible jugular venous pulsations to the angle of his jaw, which is 12 cm above his sternal angle. What
HISTORY. Question: What type of heart disease is suggested by this history? CHIEF COMPLAINT: Decreasing exercise tolerance.
 HISTORY 15-year-old male. CHIEF COMPLAINT: Decreasing exercise tolerance. PRESENT ILLNESS: A heart murmur was noted in childhood, but subsequent medical care was sporadic. Easy fatigability and slight
HISTORY 15-year-old male. CHIEF COMPLAINT: Decreasing exercise tolerance. PRESENT ILLNESS: A heart murmur was noted in childhood, but subsequent medical care was sporadic. Easy fatigability and slight
Supraventricular Tachycardia (SVT) patient information
 Supraventricular Tachycardia (SVT) patient information Working together to improve the diagnosis, treatment and quality of life for all those affected by arrhythmias www.heartrhythmalliance.org Registered
Supraventricular Tachycardia (SVT) patient information Working together to improve the diagnosis, treatment and quality of life for all those affected by arrhythmias www.heartrhythmalliance.org Registered
Electrocardiography Abnormalities (Arrhythmias) 7. Faisal I. Mohammed, MD, PhD
 Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction
 Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Recommended Evaluation Data Excerpt from NVIC 04-08
 Recommended Evaluation Data Excerpt from NVIC 04-08 Purpose: This document is an excerpt from the Medical and Physical Evaluations Guidelines for Merchant Mariner Credentials, contained in enclosure 3
Recommended Evaluation Data Excerpt from NVIC 04-08 Purpose: This document is an excerpt from the Medical and Physical Evaluations Guidelines for Merchant Mariner Credentials, contained in enclosure 3
Valvular Heart Disease: Assessment and Timing of Intervention. Graham Cole Consultant Cardiologist Imperial College Healthcare NHS Trust
 Valvular Heart Disease: Assessment and Timing of Intervention Graham Cole Consultant Cardiologist Imperial College Healthcare NHS Trust Disclosures: Speaker fee: Bayer Acknowledgements: Matt Shun-Shin
Valvular Heart Disease: Assessment and Timing of Intervention Graham Cole Consultant Cardiologist Imperial College Healthcare NHS Trust Disclosures: Speaker fee: Bayer Acknowledgements: Matt Shun-Shin
CMS Limitations Guide - Cardiovascular Services
 CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
Dos and Don t in Cardiac Arrhythmia. Case 1 -ECG. Case 1. Management. Emergency Admissions. Reduction of TE risk -CHADS 2 score. Hospital Admissions
 Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
DVLA Medical Questionnaire
 DVLA Medical Questionnaire Your Name: DOB: Today s Date: 2016 - www.countryhealth.co.uk Contents Introduction Key Client Information Important notes Vision assessment Health questionnaire Nervous system
DVLA Medical Questionnaire Your Name: DOB: Today s Date: 2016 - www.countryhealth.co.uk Contents Introduction Key Client Information Important notes Vision assessment Health questionnaire Nervous system
12 Lead ECG Interpretation
 12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
Management of Arrhythmias The General Practitioners role
 Management of Arrhythmias The General Practitioners role Rohan Gunawardena MD, FRCP, FCCP, FACC Consultant Cardiac Electrophysiologist National Hospital of Sri Lanka Arrhythmias not common Palpitations
Management of Arrhythmias The General Practitioners role Rohan Gunawardena MD, FRCP, FCCP, FACC Consultant Cardiac Electrophysiologist National Hospital of Sri Lanka Arrhythmias not common Palpitations
AORTIC STENOSIS HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE
 AORTIC STENOSIS HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE WHAT IS AORTIC STENOSIS? THE AORTIC VALVE The aorta is the major vessel that carries oxygenated blood out of the left side of the
AORTIC STENOSIS HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE WHAT IS AORTIC STENOSIS? THE AORTIC VALVE The aorta is the major vessel that carries oxygenated blood out of the left side of the
ECG Tutorial Series. Case 1. Case 2. Case 3. Prof. Wang, Tzong-Luen
 ECG Tutorial Series Prof. Wang, Tzong-Luen MD, PhD, JM, FESC, FACC, FCAPSC Chief, ED, Shin-Kong Wu Ho-Su Memorial Hospital Case 1 A 38-year-old male is visiting a family member in the hospital, but collapes
ECG Tutorial Series Prof. Wang, Tzong-Luen MD, PhD, JM, FESC, FACC, FCAPSC Chief, ED, Shin-Kong Wu Ho-Su Memorial Hospital Case 1 A 38-year-old male is visiting a family member in the hospital, but collapes
, David Stultz, MD.
 http://www.dilbert.com EKG Rounds Handouts available at http://www.drstultz.com January 5, 2004 David Stultz, MD Cardiology Fellow, PGY 4 Overview of Topics How to read an EKG Normal EKG Determination
http://www.dilbert.com EKG Rounds Handouts available at http://www.drstultz.com January 5, 2004 David Stultz, MD Cardiology Fellow, PGY 4 Overview of Topics How to read an EKG Normal EKG Determination
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Family Medicine for English language students of Medical University of Lodz ECG. Jakub Dorożyński
 Family Medicine for English language students of Medical University of Lodz ECG Jakub Dorożyński Parts of an ECG The standard ECG has 12 leads: six of them are considered limb leads because they are placed
Family Medicine for English language students of Medical University of Lodz ECG Jakub Dorożyński Parts of an ECG The standard ECG has 12 leads: six of them are considered limb leads because they are placed
ACC/AHA Guidelines for Ambulatory Electrocardiography: Executive Summary and Recommendations
 (Circulation. 1999;100:886-893.) 1999 American Heart Association, Inc. ACC/AHA Practice Guidelines ACC/AHA Guidelines for Ambulatory Electrocardiography: Executive Summary and Recommendations A Report
(Circulation. 1999;100:886-893.) 1999 American Heart Association, Inc. ACC/AHA Practice Guidelines ACC/AHA Guidelines for Ambulatory Electrocardiography: Executive Summary and Recommendations A Report
Study of rhythm disturbances in acute myocardial infarction in Government Dharmapuri Medical College Hospital, Dharmapuri
 Original Research Article Study of rhythm disturbances in acute myocardial infarction in Government Dharmapuri Medical College Hospital, Dharmapuri P. Sasikumar * Department of General Medicine, Govt.
Original Research Article Study of rhythm disturbances in acute myocardial infarction in Government Dharmapuri Medical College Hospital, Dharmapuri P. Sasikumar * Department of General Medicine, Govt.
WESTMEAD Cardiac QUESTIONS PRACTICE SAQ
 QUESTION 1 A 65-year-old man presents to the emergency department with a history of palpitations. His vital signs are: BP 105/60 mmhg HR 156 beats/min RR 26 /min Temperature 36.2 o C His ECG is on the
QUESTION 1 A 65-year-old man presents to the emergency department with a history of palpitations. His vital signs are: BP 105/60 mmhg HR 156 beats/min RR 26 /min Temperature 36.2 o C His ECG is on the
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
The production of murmurs is due to 3 main factors:
 Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
The more we listen, the more lives we save. Heart Valve V O I C E. Heart Valve Disease. A Practical Guide for Primary Care
 Heart Valve V O I C E The more we listen, the more lives we save. Heart Valve Disease A Practical Guide for Primary Care About Heart Valve Voice Heart Valve Voice is a charity run by a group of multi-disciplinary
Heart Valve V O I C E The more we listen, the more lives we save. Heart Valve Disease A Practical Guide for Primary Care About Heart Valve Voice Heart Valve Voice is a charity run by a group of multi-disciplinary
A Case Showing Atrial Dissociation and Other Various Kinds of Arrhythmias
 A Case Showing Atrial Dissociation and Other Various Kinds of Arrhythmias Shigeru KAWAGOE, M.D., Keiichi HASHIMOTO, M.D., Hirokazu HAYAKAWA, M.D., and Eiichi KIMURA, M.D. SUMMARY A case is reported in
A Case Showing Atrial Dissociation and Other Various Kinds of Arrhythmias Shigeru KAWAGOE, M.D., Keiichi HASHIMOTO, M.D., Hirokazu HAYAKAWA, M.D., and Eiichi KIMURA, M.D. SUMMARY A case is reported in
General Cardiovascular Magnetic Resonance Imaging
 2 General Cardiovascular Magnetic Resonance Imaging 19 Peter G. Danias, Cardiovascular MRI: 150 Multiple-Choice Questions and Answers Humana Press 2008 20 Cardiovascular MRI: 150 Multiple-Choice Questions
2 General Cardiovascular Magnetic Resonance Imaging 19 Peter G. Danias, Cardiovascular MRI: 150 Multiple-Choice Questions and Answers Humana Press 2008 20 Cardiovascular MRI: 150 Multiple-Choice Questions
Atrial Fibrillation. A guide for Southwark General Practice. Key Messages. Always work within your knowledge and competency
 Atrial Fibrillation A guide for Southwark General Practice Key Messages 1. Routinely offer pulse checks to patients at high risk of AF 2. Use the CHA 2 DS 2 VASc score to identify patients for anticoagulation
Atrial Fibrillation A guide for Southwark General Practice Key Messages 1. Routinely offer pulse checks to patients at high risk of AF 2. Use the CHA 2 DS 2 VASc score to identify patients for anticoagulation
December 2018 Tracings
 Tracings Tracing 1 Tracing 4 Tracing 1 Answer Tracing 4 Answer Tracing 2 Tracing 5 Tracing 2 Answer Tracing 5 Answer Tracing 3 Tracing 6 Tracing 3 Answer Tracing 6 Answer Questions? Contact Dr. Nelson
Tracings Tracing 1 Tracing 4 Tracing 1 Answer Tracing 4 Answer Tracing 2 Tracing 5 Tracing 2 Answer Tracing 5 Answer Tracing 3 Tracing 6 Tracing 3 Answer Tracing 6 Answer Questions? Contact Dr. Nelson
TGA atrial vs arterial switch what do we need to look for and how to react
 TGA atrial vs arterial switch what do we need to look for and how to react Folkert Meijboom, MD, PhD, FES Dept ardiology University Medical entre Utrecht The Netherlands TGA + atrial switch: Follow-up
TGA atrial vs arterial switch what do we need to look for and how to react Folkert Meijboom, MD, PhD, FES Dept ardiology University Medical entre Utrecht The Netherlands TGA + atrial switch: Follow-up
Electrocardiography. Hilal Al Saffar College of Medicine,Baghdad University
 Electrocardiography Hilal Al Saffar College of Medicine,Baghdad University Which of the following is True 1. PR interval, represent the time taken for the impulse to travel from SA node to AV nose. 2.
Electrocardiography Hilal Al Saffar College of Medicine,Baghdad University Which of the following is True 1. PR interval, represent the time taken for the impulse to travel from SA node to AV nose. 2.
Lecture outline. Electrical properties of the heart. Automaticity. Excitability. Refractoriness. The ABCs of ECGs Back to Basics Part I
 Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
Direct Current (DC) Cardioversion
 Page 1 of 10 Direct Current (DC) Cardioversion Introduction This leaflet is to inform you about your planned Direct Current (DC) electrical cardioversion. A cardioversion is an electrical treatment which
Page 1 of 10 Direct Current (DC) Cardioversion Introduction This leaflet is to inform you about your planned Direct Current (DC) electrical cardioversion. A cardioversion is an electrical treatment which
Arrhythmias. A/Prof Drew Richardson. The Canberra Hospital May MB BS (Hons) FACEM Grad CertHE MD
 Arrhythmias A/Prof Drew Richardson MB BS (Hons) FACEM Grad CertHE MD The Canberra Hospital May 2013 Objectives Recognise the features of the common nonlethal arrhythmias Describe the emergency treatment
Arrhythmias A/Prof Drew Richardson MB BS (Hons) FACEM Grad CertHE MD The Canberra Hospital May 2013 Objectives Recognise the features of the common nonlethal arrhythmias Describe the emergency treatment
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to
 Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Cardiology and Nuclear Medicine Patient Information Leaflet
 Myocardial Perfusion Scan Cardiology and Nuclear Medicine Patient Information Leaflet What is a myocardial perfusion scan? A myocardial perfusion scan uses a small amount of a radioactive chemical to see
Myocardial Perfusion Scan Cardiology and Nuclear Medicine Patient Information Leaflet What is a myocardial perfusion scan? A myocardial perfusion scan uses a small amount of a radioactive chemical to see
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
EKG of the WEEK Questions
 EKG of the WEEK Questions ECG 1 EKG 2 A one month old with some symptoms and physical signs compatible with cardiac disease (tachypnea, FTT and loud P2). The child was born to a 42 years old mother and
EKG of the WEEK Questions ECG 1 EKG 2 A one month old with some symptoms and physical signs compatible with cardiac disease (tachypnea, FTT and loud P2). The child was born to a 42 years old mother and
Valvular Heart Disease Mitral Stenosis
 Valvular Heart Disease Mitral Stenosis A 75 year old woman with loud first heart sound and mid-diastolic murmur Chronic dyspnea Class 2/4 Fatigue Recent orthopnea/pnd Nocturnal palpitation Pedal edema
Valvular Heart Disease Mitral Stenosis A 75 year old woman with loud first heart sound and mid-diastolic murmur Chronic dyspnea Class 2/4 Fatigue Recent orthopnea/pnd Nocturnal palpitation Pedal edema
You Don t Want to Miss This One! Focus on can t miss EKG tracings
 You Don t Want to Miss This One! Focus on can t miss EKG tracings Renaissance St. Louis Grand Hotel Convention Center October 23, 2014 David K. Tan, M.D., EMT-T, FAAEM EMS Section Chief, Division of Emergency
You Don t Want to Miss This One! Focus on can t miss EKG tracings Renaissance St. Louis Grand Hotel Convention Center October 23, 2014 David K. Tan, M.D., EMT-T, FAAEM EMS Section Chief, Division of Emergency
Patient Resources: Arrhythmias and Congenital Heart Disease
 Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Case submission for CSI Asia-Pacific Case 2
 Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
Electrophysiology Studies and Catheter Ablation. Electrophysiology Studies and Catheter Ablation
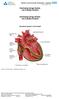 Electrophysiology Studies Cardiac Conduction System. Mdmedicine.wordpress.com Patient Information Leaflet for: Electrophysiology Studies Available via Trust Docs Version: 6 Trust Docs ID: 10 Page 1 of
Electrophysiology Studies Cardiac Conduction System. Mdmedicine.wordpress.com Patient Information Leaflet for: Electrophysiology Studies Available via Trust Docs Version: 6 Trust Docs ID: 10 Page 1 of
Uptofate Study Summary
 CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
Patient Resources: Syncope
 Patient Resources: Syncope Overview Syncope is the medical term for fainting or loss of consciousness. Fainting can occur for a few different reasons. The autonomic (involuntary) nervous system helps to
Patient Resources: Syncope Overview Syncope is the medical term for fainting or loss of consciousness. Fainting can occur for a few different reasons. The autonomic (involuntary) nervous system helps to
Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC
 Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC Who am I? Class Outline Gross anatomy of the heart Trip around the heart Micro anatomy: cellular and tissue level Introduction
Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC Who am I? Class Outline Gross anatomy of the heart Trip around the heart Micro anatomy: cellular and tissue level Introduction
Chest Pain. Dr. Amitesh Aggarwal. Department of Medicine
 Chest Pain Dr. Amitesh Aggarwal Department of Medicine BACKGROUND Approx 5% of all ED visits 15 % - AMI 25-30 % - Unstable angina 50-55 % - Other conditions Atypical presentations common 2% of patients
Chest Pain Dr. Amitesh Aggarwal Department of Medicine BACKGROUND Approx 5% of all ED visits 15 % - AMI 25-30 % - Unstable angina 50-55 % - Other conditions Atypical presentations common 2% of patients
Cardiology. the Sounds: #7 HCM. LV Outflow Obstruction: Aortic Stenosis. (Coming Soon - HCM)
 A Cardiology HCM LV Outflow Obstruction: Aortic Stenosis (Coming Soon - HCM) the Sounds: #7 Howard J. Sachs, MD www.12daysinmarch.com E-mail: Howard@12daysinmarch.com Aortic Valve Disorders Stenosis Regurgitation
A Cardiology HCM LV Outflow Obstruction: Aortic Stenosis (Coming Soon - HCM) the Sounds: #7 Howard J. Sachs, MD www.12daysinmarch.com E-mail: Howard@12daysinmarch.com Aortic Valve Disorders Stenosis Regurgitation
