Antidysrhythmics HST-151 1
|
|
|
- Clinton Brooks
- 6 years ago
- Views:
Transcription
1 HST Antidysrhythmics I. Ventricular muscle cell action potential a. Phase 0: Upstroke b. Phase 1: Early-fast repolarization c. Phase 2: Plateau d. Phase 3: Repolarization e. Phase 4: Diastole
2 HST II. Cardiac arrhythmia: a. Abnormal impulse formation i. Early afterdepolarizations (EADs): interrupts phase 3 - exacerbated at slow heart rates and may contribute to development of long QT-related arrhythmias ii. Delayed afterdepolarizations (DADs): interrupts phase 4 - occurs when intracellular calcium is increased; is exacerbated by fast heart rates, may relate to digitalis excess, catecholamines, and myocardial ischemia b. Abnormal impulse propagation: i. Abnormal depolarization (QRS) ii. Abnormal repolarization (QT c ) III. Cellular mechanism of arrhythmia: a. Enhanced automaticity: sinus and AV node, His-Purkinje system i. Beta-adrenergic stimulation, hypokalemia, mechanical stretch increase phase 4 slope & pacemaker rate b. Reentry: impulse reenters and excites areas of the heart more than once i. Obstacle for homogeneous conduction (anatomic, physiologic) ii. Unidirectional block in conduction circuit iii. Path length X conduction velocity > refractory period
3 HST c. Polymorphic ventricular tachycardia (Torsades de Pointes): ("twisting of the points") or drug-induced long QT syndrome (DILQTS) IV. Polymorphic arrhythmia that can rapidly develop into ventricular fibrillation Associated with drugs that have Class III actions (potassium channel blockers) Also seen with other drugs such as terfenadine, cisapride, under certain circumstances Usually occurs within the first week of therapy Preexisting prolonged QTc intervals may be indicator of susceptibility Potentiated by bradycardia Often associated with concurrent electrolyte disturbances (hypokalemia, hypomagnesemia) Classification of Antiarrhythmic drugs: Although several of the drugs used to treat cardiac arrhythmias have been used for many years (e.g.- quinidine and digitalis since the early 1900s), most of the agents approved for use today have only been available for a decade or less. Research in recent years has provided much information regarding the cellular mechanisms of arrhythmias and the mechanisms by which some of the antiarrhythmic drugs act, but the general approach to antiarrhythmic therapy remains largely empirical. The recent results of several clinical trials, including the Cardiac Arrhythmia Suppression Trial (CAST), have indicated that many antiarrhythmic drugs may significantly increase mortality compared to placebo. All of the antiarrhythmic drugs act by altering ion fluxes within excitable tissues in the myocardium. The three ions of primary importance are Na +, Ca ++, and K +. Antiarrhythmic drugs can be classified by their ability to directly or indirectly block flux of one or
4 HST more of these ions across the membranes of excitable cardiac muscle cells. Class I drugs, those that act by blocking the sodium channel, are subdivided into 3 subgroups, IA, IB, and IC based on their effects on repolarization and potency towards blocking the sodium channel o Subclass IA drugs have high potency as sodium channel blockers (prolong QRS interval), and also usually prolong repolarization (prolong QT interval) through blockade of potassium channels o Subclass IB drugs have the lowest potency as sodium channel blockers, produce little if any change in action potential duration (no effect on QRS interval) in normal tissue, and shorten repolarization (decrease QT interval) o Subclass IC drugs are the most potent sodium channel blocking agents (prolong QRS interval), and have little effect on repolarization (no effect on QT interval) Class II drugs act indirectly on electrophysiological parameters by blocking betaadrenergic receptors (slow sinus rhythm, prolong PR interval, little effect on QRS or QT intervals) Class III drugs prolong repolarization (increase refractoriness) by blocking outward potassium conductance (prolong QT interval), with typically little effect on the rate of depolarization (no effect on QRS interval) Class IV drugs are relatively selective AV nodal L-type calcium-channel blockers (slow sinus rhythm, prolong PR interval, no effect on QRS interval) Miscellaneous In addition to the standard classes, IA-C, II, III, and IV, there is also a miscellaneous group of drugs that includes digoxin, adenosine, magnesium, alinidine (a chloride channel blocker) and other compounds whose actions don't fit the standard four classes
5 HST Ventricular Action Potential Ca ++ Class I Class I & III* Depolarization Na + IKr IKs Table 1. Vaughan Williams Classification of Antiarrhythmic Drugs Class Action Drugs I Sodium Channel Blockade IA IB IC Prolong repolarization Shorten repolarization Little effect on repolarization Quinidine, procainamide, disopyramide Lidocaine, mexiletine, tocainide, phenytoin Encainide, flecainide, propafenone, moricizine(?) II Beta-Adrenergic Blockade Propanolol, esmolol, acebutolol, l-sotalol III Prolong Repolarization (Potassium Channel Blockade; Other) Ibutilide, dofetilide, sotalol (d,l), amiodarone, bretylium IV Calcium Channel Blockade Verapamil, diltiazem, bepridil Miscellaneous Miscellaneous Actions Adenosine, digitalis, magnesium
6 HST Table 2. Class Toxicities of Antiarrhythmic Drugs (Adapted from Woosley, 1991) Class I Class II Class III Class IV Proarrhythmic effects: Sinus bradycardia Sinus bradycardia Sinus bradycardia IA- Torsades de pointes IC- CAST proarrhythmia Negative inotropic effect AV block Depression of LV function (adrenergicdependent) Torsades de pointes AV block Negative inotropic effect Infranodal conduction block V. Mechanism of antiarrhythmic drugs: Antiarrhythmic drugs act by altering the flux of ions across the membranes of excitable cells in the heart. The primary mechanisms of action correspond to the mechanisms used in developing the Vaughan Williams classification system, and include inhibition of sodium channels (Class I drugs), inhibition of calcium channels (Class IV drugs), inhibition of potassium channels (Class III drugs), and blockade of beta-adrenergic receptors in the heart (Class II drugs). a. Sodium Channel Blockade Sodium channels are responsible for the initial rapid (Phase 0) depolarization of atrial, Purkinje, and ventricular cells. Sodium channel activation (opening) is voltage-dependent The sodium current entering the cell during phase 0 depolarization is very intense, but brief Activation (opening) and inactivation (closing) of cardiac sodium channels is very rapid Blockade of sodium channels: o Slows the rate and amplitude of phase 0 depolarization o Reduces cell excitability o Reduces conduction velocity SA and AV nodal cells have relatively few sodium channels and therefore lack a rapid phase 0 depolarization.
7 HST b. Calcium Channel (L-type) Blockade Calcium channels (L-type) are responsible for the prolonged plateau phase (Phase 2) seen in the action potential of atrial, Purkinje, and ventricular cells. L-type calcium channel opening is voltage-dependent, but requires a more positive membrane potential than cardiac sodium channels The calcium current entering the cell during phase 2 is intense and prolonged L-type calcium channels are slow to activate (open) and slow to inactivate (close) Blockade of calcium channels reduces the amplitude and length (time) of phase 2 in atrial, Purkinje, and ventricular cells In SA and AV nodal cells, calcium entry through L-type channels represents the major ion flux during depolarization. c. Potassium Channel Blockade Potassium channels, particularly the channel giving rise to the "delayed rectifier current", are activated during the repolarization (Phase 3) of the action potential. Blockade of potassium channels prolongs action potential duration. o Prolongation of action potential duration usually results in an increase in effective refractory period d. Use (Rate)-Dependent Blockade by Channel Blockers An ideal antiarrhythmic drug should target ectopic pacemakers and rapidly depolarizing tissue to a greater extent than normal tissues of the heart Many of the sodium (Class I) and calcium (Class IV) channel blockers have this property because they preferentially block sodium and calcium channels in depolarized tissues (cf, Modulated Receptor Hypothesis in preceding lecture). Enhanced sodium or calcium channel blockade in rapidly depolarizing tissue has been termed "use-dependent blockade" and is thought to be responsible for increased efficacy in slowing and converting tachycardias with minimal effects on tissues depolarizing at normal (sinus) rates Many of the drugs that prolong repolarization (Class III drugs, potassium channel blockers) exhibit negative or reverse rate-dependence o These drugs have little effect on prolonging repolarization in rapidly depolarizing tissue o These drugs can cause prolongation of repolarization in slowly depolarizing tissue or following a long compensatory pause, leading to repolarization disturbances and torsades de pointes
8 HST IA III IC II & IV VI. Acute Treatement of VT: a. Lidocaine (50-75 mg bolus, 1-3 mg/min) b. Procainamide ( 500 mg 1 g over min, 1-4mg/min) c. Amidodarone (100 mg over 10 min, 1mg/min) d. Bretylium (300 mg over 1 hr, 1 mg/min) e. Magnesium sulfate f. DC cardioversion/defibrillation VII. Classification of SVT: a. Sinus tachycardia: i. Physiologic ii. Nonphysiologic: 1. Inappropriate sinus tachycardia (IST) 2. Sinus node reentry (SNR) b. AV Node independent (Atrial) i. PACs ii. Atrial tachycardia iii. Atrial flutter iv. Atrial fibrillation c. AV node dependent (junctional) i. AV node reentry ii. AV reentry d. Junctional ectopic tachycardia (JET) VIII. SVT : ECG correlation:
9 HST AVNRT AVRT V 1 V 1 AVN Atrium His AP RBB LBB Ventricle IX. Antiarrhythmic drug effects in SVT: a. AVN independent: i. Prevent/terminate tachycardia ii. Slow ventricular rate b. AVN depedendent: i. Prevent/terminate tachycardia X. Radiofrequency (RF) catheter ablation of left free wall accessory AV connection a. Radiofrequency (RF) catheter ablation has recently replaced surgical ablation in nearly all cases of ablation for cardiac arrhythmias. It is now a first-line therapy and highly effective in treating:
10 HST i. Wolff-Parkinson-White syndrome ii. AV nodal reentry iii. Atrial ectopic tachycardia b. RF ablation is also useful in treating: i. Atrial fibrillation ii. Several types of monomorphic ventricular tachycardias XI. Clinical studies: a. Cardiac Arrhythmia Suppression Trial (CAST): encainide or flecainide vs placebo
11 HST XII. Antiarrhythmic in structural HD (VT) a. Beta blocker b. Sotalol c. Amiodarone XIII. Non-pharmacological Therapy a. Surgery b. Catheter ablation c. Implantable cardioverter-defibrillator (ICD) XIV. Automatic implatable cardioverter/defibrillator devices (ICDs) therapy circa 1980: Large devices, abdominal site a. Thoracotomy, multiple incisions b. Long hospital stay c. General anesthesia d. Complication from major surgery e. Perioperative mortality up to 5% f. Nonprogrammable therapy g. High energy shock only h. Device longevity ~ 1.5 years i. Fewer than 1000 implants/year XV. ICD therapy present: a. Can now be implanted without thoracotomy b. Current generation devices terminate arrhythmias by anticardiac pacing, cardioversion, and defibrillation c. Considered by some experts to be the therapy of first choice in patients with ventricular tachycardias based on a number of recent clinical trials comparing ICD therapy to antiarrhythmic drug therapy (both Class I and Class III drugs) d. A significant fraction of patients receiving an ICD may still require antiarrhythmic drug therapy to decrease the frequency of arrhythmic episodes (to prolong battery life) and to reduce the number of inappropriate (energy-consuming and painful) shocks. Improvements in ICD design may reduce or eliminate the need for concurrent drug therapy. XVI. Conclusions: a. Antiarrhythmic drugs are first line therapy for the acute management of most supraventricular and ventricular arrhythmias b. Catheter ablation is curative for most forms of recurrent SVTs
12 HST c. Life threatening ventricular arrhythmias are best managed with ICDs and adjunctive drug therapy when necessary APPENDIX: Therapeutics It is often problematic to determine the best drug for a given patient due to the unknown etiology of many arrhythmias, patient-to-patient variability, and the multiple actions of many antiarrhythmic drugs. Three trial-and-error approaches are widely used: o Empiric. That is, based upon the clinician's past experience. o Serial drug testing guided by electrophysiological study (EPS). This invasive technique requires cardiac catheterization and induction of arrhythmias by programmed electrical stimulation of the heart, followed by a delivery of drugs to predict the most efficacious drug(s) to use for a given patient. o Drug testing guided by electrocardiographic monitoring (Holter monitoring). This noninvasive technique involves 24-hour recording of a patient's ECG before and during each drug treatment to predict optimal efficacy. The recent Electrophysiologic versus Electrocardiographic Monitoring (ESVEM) study concluded that there may not be any significant difference between the predictive value of this technique compared to programmed electrical stimulation. Before beginning therapy: o Any factor that might predispose a patient to arrhythmias (electrolyte abnormalities, hypoxia, proarrhythmic drugs, underlying disease states) should be eliminated o A firm diagnosis should be made before beginning therapy and a baseline ECG should be established to monitor the efficacy of treatment Monitoring during therapy should include: o Continuous and careful monitoring for efficacy and adverse effects o Monitoring plasma concentrations of drug, including free vs. proteinbound because of the narrow therapeutic index of most antiarrhythmic drugs
13 HST Table 3. Drugs of Choice for Cardiac Arrhythmias (Adapted from The Medical Letter (1996) 38, 75-82) Arrhythmia (Links point to ECGs) Atrial fibrillation/flutter Other supraventricular tachycardias PVCs or nonsustained ventricular tachycardia Sustained ventricular tachycardia Ventricular fibrillation Drug of Choice (Non-drug therapy) (Cardioversion) Verapamil, diltiazem, or beta-blocker to slow ventricular response Adenosine, verapamil, or diltiazem for termination (RF ablation) No drug therapy for asymptomatic patients (Cardioversion or chest thump is the safest and most effective treatment) Lidocaine for acute treatment (Defibrillation is treatment of choice) Alternatives (Non-drug therapy) Digoxin to slow ventricular response Class IA, IC drugs for long-term suppression Ibutilide for termination Low dose amiodarone for prevention Dofetilide for prevention (RF ablation) Class II drugs or digoxin for termination (Cardioversion or atrial pacing) Class IA, IC, II, or IV drugs or digoxin for longterm suppression Class II drugs for symptomatic patients Procainamide, bretylium or amiodarone for acute treatment Sotalol, amiodarone, Class IA, IB, II, III can be used for long-term suppression (RF ablation or ICD) Amiodarone, procainamide or bretylium
14 HST Lidocaine to prevent recurrence to prevent recurrence (RF ablation or ICD) Digitalis-induced ventricular tachyarrhythmia Digibind for lifethreatening toxicity Lidocaine Phenytoin Avoid cardioversion except for ventricular fibrillation Potassium (if hypokalemic) Remove causative agents Torsades de pointes Magnesium sulfate Isoproterenol Potassium (if hypokalemic) (Cardiac pacing) Table 4. Relative Efficacies of Antiarrhythmic Drugs by Class (Adapted from Melmon and Morelli, 3rd ed.) Drug Class Efficacy IA IB IC II III IV Atrial fibrillation Ventricular arrhythmias Ventricular arrhythmias AV nodal reentry WPW-related arrhythmias Ventricular arrhythmias (can increase mortality despite suppressing PVCs) Atrial fibrillation/flutter (Ventricular arrhythmias) Atrial fibrillation/flutter Ventricular arrhythmias Atrial fibrillation/flutter Atrial automaticities
15 HST AV nodal reentry Adenosine Digitalis AV nodal reentry Orthodromic tachycardia AV nodal reentry Atrial fibrillation/flutter Magnesium Torsades de pointes Table 5. Adverse Extra-Cardiac Effects of Selected Antiarrhythmic Drugs (Adapted from The Medical Letter 33:55-60 and Katzung, 8th ed.) Drug (Class) Adverse Extra-Cardiac Effects and Toxicities GI disturbances in 30-50% of patients: diarrhea, nausea, vomiting Cinchonism Quinidine (IA) Hypotension (due to alpha-adrenergic blocking activities) Can elevate serum digoxin concentrations, resulting in digitalis toxicity Hypersensitivity reactions: rashes, fever, angioneurotic edema, hepatitis Reversible thrombocytopenia Hypotension (due to ganglionic blocking activity) Procainamide (IA) Long-term use results in a lupus-like syndrome in 15-30% of patients consisting of arthralgia and arthritis (pleuritis, pericarditis, parenchymal pulmonary disease also occur in some patients) GI symptoms in 10% of patients Adverse CNS effects: giddiness, psychosis, depression, hallucinations Hypersensitivity reactions: fever, agranulocytosis (can lead to fatal infections), Raynaud's syndrome, myalgias, skin rashes, digital vasculitis Lidocaine (IB) Lowest incidence of toxicity of currently used antiarrhythmic
16 HST drugs CNS depression: drowsiness, disorientation, slurred speech, respiratory depression, nausea CNS stimulation: tinnitus, muscle twitching, psychosis, seizures Concurrent use of tocainide or mexiletine can cause additive CNS toxicity, including seizures (seizures respond to i.v. diazepam) GI effects: nausea, vomiting Tocainide (IB) Mexiletine (IB) Flecainide (IC) CNS effects: dizziness, disorientation, tremor Hematological effects (0.2%) with tocainide: agranulocytosis, bone marrow suppression, thrombocytopenia; can lead to death Concurrent use of either of these drugs and quinidine in combination may be effective at lower doses than either drug alone and thereby minimize adverse effects of both drugs CNS effects in 10-15% of patients: dizziness, tremor, agitation, headache, visual disturbances GI upset Although this drug is highly effective in treating many arrhythmias, its large number adverse effects limits its clinical use Adverse effects are common (more than 75% of patients receiving drug) and increase after a year of treatment; some toxicities result in death Half-life of days can prolong toxicity Amiodarone (III) Pulmonary toxicity and fibrosis (10-15%, can cause death in 10% of those affected); can be irreversible Constipation in 20% of patients) Hepatic dysfunction; can be irreversible Asymptomatic corneal deposits occur in all patients CNS effects (ataxia, dizziness, depression, nightmares, hallucinations) Hypothyroidism or hyperthyroidism (5% of patients)
17 HST Cutaneous photosensitivity (25% of patients) and blue-grey discoloration of skin (less than 5% of patients) Peripheral neuropathy Substantial increases in LDL-cholesterol concentrations often seen; phospholipidosis Enhances the effect of warfarin and increases the serum concentrations of digoxin, quinidine, procainamide, flecainide, theophylline and other drugs Digitalis (Misc.) Many adverse non-cardiac effects (anorexia, nausea, vomiting, diarrhea, abdominal pain, headache, confusion, abnormal vision) Adverse effects may indicate digitalis toxicity Short half-life in blood (less than 10 seconds) Adenosine (Misc.) Causes hypotension, flushing in 20% of patients Transient dyspnea, chest discomfort (non-myocardial) in > 10% Metallic taste Headache, hypotension, nausea, paresthesias are less common Recommended Reading Katzung (8th ed.) Chapt. 14 or Goodman & Gilman (9th ed.), Chapt. 35 Supplemental Reading o "Antiarrhythmics-from cell to clinic: past, present, and future," Heart 84:14-24 (2000) o Symposium Proceedings: "Changing Trends in Antiarrhythmic Therapy," Am. J. Cardiol. (1997) 80(8A):1G-104G "Controlling cardiac arrhythmias: an overview with a historical perspective," Am J Cardiol. (1997) 80(8A): 4G-15G. Review. o "Drugs for cardiac arrhythmias," The Medical Letter (1996), 38: o Clinical Pharmacology (Melmon & Morrelli) (3rd ed.) Chapt. 6
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Mr. Eknath Kole M.S. Pharm (NIPER Mohali)
 M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
PHARMACOLOGY OF ARRHYTHMIAS
 PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
Antiarrhythmic Drugs 1/31/2018 1
 Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018
 Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 2 Ion Permeability Changes Potential Changes Genes and Proteins 3 Cardiac Na+ channels 5 6
Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 2 Ion Permeability Changes Potential Changes Genes and Proteins 3 Cardiac Na+ channels 5 6
Antiarrhythmic Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017
 Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017 Types of Cardiac Arrhythmias Abnormalities of Impulse Formation: Rate disturbances. Triggered
Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017 Types of Cardiac Arrhythmias Abnormalities of Impulse Formation: Rate disturbances. Triggered
Arrhythmias. Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium.
 Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
B. 14 Antidysrhythmic drugs. a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification
 B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
Chapter 14. Agents used in Cardiac Arrhythmias
 Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.01.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.01.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
ARRHYTHMIA SINUS RHYTHM
 ARRHYTHMIA Dr. Ahmed A. Elberry, MBBCH, MSc, MD Assistant Professor of Clinical Pharmacy Faculty of pharmacy, KAU 1 SINUS RHYTHM SA node is cardiac pacemaker Normal sinus rhythm 60-100 beats/min Depolarisation
ARRHYTHMIA Dr. Ahmed A. Elberry, MBBCH, MSc, MD Assistant Professor of Clinical Pharmacy Faculty of pharmacy, KAU 1 SINUS RHYTHM SA node is cardiac pacemaker Normal sinus rhythm 60-100 beats/min Depolarisation
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification
 Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
Atrial Fibrillation 10/2/2018. Depolarization & ECG. Atrial Fibrillation. Hemodynamic Consequences
 Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
ANTI-ARRHYTHMICS AND WARFARIN. Dr Nithish Jayakumar
 ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital
 Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital Content i. Rhythm versus Rate control ii. Anti-arrhythmic for Rhythm Control iii. Anti-arrhythmic for Rate
Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital Content i. Rhythm versus Rate control ii. Anti-arrhythmic for Rhythm Control iii. Anti-arrhythmic for Rate
Dysrhythmias. Dysrythmias & Anti-Dysrhythmics. EKG Parameters. Dysrhythmias. Components of an ECG Wave. Dysrhythmias
 Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
ARRHYTHMIAS IN THE ICU
 ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT
 ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
Cardiac Arrhythmias. For Pharmacists
 Cardiac Arrhythmias For Pharmacists Agenda Overview of the normal Classification Management Therapy Conclusion Cardiac arrhythmias Overview of the normal Arrhythmia: definition From the Greek a-, loss
Cardiac Arrhythmias For Pharmacists Agenda Overview of the normal Classification Management Therapy Conclusion Cardiac arrhythmias Overview of the normal Arrhythmia: definition From the Greek a-, loss
Antiarrhythmic Pharmacology. The Electronics
 Antiarrhythmic Pharmacology Linking Pharmacological Treatment to the Patient and the Rhythm Presented By: Karen Marzlin BSN, RN,C, CCRN-CMC CNEA 2009 1 The Electronics Action Potential of Cardiac Cells
Antiarrhythmic Pharmacology Linking Pharmacological Treatment to the Patient and the Rhythm Presented By: Karen Marzlin BSN, RN,C, CCRN-CMC CNEA 2009 1 The Electronics Action Potential of Cardiac Cells
Anti arrhythmic drugs. Hilal Al Saffar College of medicine Baghdad University
 Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
DECLARATION OF CONFLICT OF INTEREST. Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical
 DECLARATION OF CONFLICT OF INTEREST Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical ESC Congress Paris, France August 27-31, 2011 Risk & Complications of AADs for Rhythm
DECLARATION OF CONFLICT OF INTEREST Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical ESC Congress Paris, France August 27-31, 2011 Risk & Complications of AADs for Rhythm
Antiarrhythmias. Edward JN Ishac, Ph.D. Smith Building, Room
 Antiarrhythmias Edward JN Ishac, Ph.D. Smith Building, Room 72 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University Richmond,
Antiarrhythmias Edward JN Ishac, Ph.D. Smith Building, Room 72 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University Richmond,
ANTI - ARRHYTHMIC DRUGS
 ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY
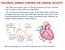 ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY The heart beat begins when an electrical impulse from the sinoatrial node (SA node or sinus node) moves through it. The normal electrical sequence begins
ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY The heart beat begins when an electrical impulse from the sinoatrial node (SA node or sinus node) moves through it. The normal electrical sequence begins
I have nothing to disclose.
 I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
Amiodarone Prescribing and Monitoring: Back to the Future
 Amiodarone Prescribing and Monitoring: Back to the Future Subha L. Varahan, MD, FHRS, CCDS Electrophysiologist Oklahoma Heart Hospital Oklahoma City, OK Friday, February, 8 th, 2019 Iodinated benzofuran
Amiodarone Prescribing and Monitoring: Back to the Future Subha L. Varahan, MD, FHRS, CCDS Electrophysiologist Oklahoma Heart Hospital Oklahoma City, OK Friday, February, 8 th, 2019 Iodinated benzofuran
Alaska Nurse Practitioner Annual Conference 2009
 Alaska Nurse Practitioner Annual Conference 2009 LAURIE RACENET, RN, MSN, ANP, CEPS, CCDS Alaska Heart Institute Member: Boston Scientific Allied Professional Advisory Board Participant in Industry Sponsored
Alaska Nurse Practitioner Annual Conference 2009 LAURIE RACENET, RN, MSN, ANP, CEPS, CCDS Alaska Heart Institute Member: Boston Scientific Allied Professional Advisory Board Participant in Industry Sponsored
This document does not consider management of individual arrhythmias look elsewhere, e.g. OHCM.
 Cardiac arrhythmias This document does not consider management of individual arrhythmias look elsewhere, e.g. OHCM. Physiology Automaticity = ability of specialised cardiac conducting tissue to spontaneously
Cardiac arrhythmias This document does not consider management of individual arrhythmias look elsewhere, e.g. OHCM. Physiology Automaticity = ability of specialised cardiac conducting tissue to spontaneously
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Core Content In Urgent Care Medicine
 Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Management of acute Cardiac Arrhythmias
 Management of acute Cardiac Arrhythmias Dr. Zulkeflee Muhammad MBChB (New Zealand), MRCP (United Kingdom) Cardiologist Electrophysiology Unit Istitut Jantung Negara Objectives Review the etiology and recognition
Management of acute Cardiac Arrhythmias Dr. Zulkeflee Muhammad MBChB (New Zealand), MRCP (United Kingdom) Cardiologist Electrophysiology Unit Istitut Jantung Negara Objectives Review the etiology and recognition
Atrial fibrillation in the ICU
 Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
CVD: Cardiac Arrhythmias. 1. Final Cardiac Arrhythmias_BMP. 1.1 Cardiovascular Disease. Notes:
 CVD: Cardiac Arrhythmias 1. Final Cardiac Arrhythmias_BMP 1.1 Cardiovascular Disease 1.2 Directions for taking this course 1.3 Content Experts 1.4 Disclosures 1.5 Accreditation Information 1.6 Learning
CVD: Cardiac Arrhythmias 1. Final Cardiac Arrhythmias_BMP 1.1 Cardiovascular Disease 1.2 Directions for taking this course 1.3 Content Experts 1.4 Disclosures 1.5 Accreditation Information 1.6 Learning
APPROACH TO TACHYARRYTHMIAS
 APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
Pharmacotherapy of Antiarrhythmias
 Pharmacotherapy of Antiarrhythmias Edward JN Ishac, Ph.D. Smith Building, Room 72 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Pharmacotherapy of Antiarrhythmias Edward JN Ishac, Ph.D. Smith Building, Room 72 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
3. AV Block 1. First-degree AV block 1. Delay in AV node 2. Long PR interval 3. QRS complex follows each P wave 4. Benign, no tx
 1. Rhythms & arrhythmias SA nodal rhythms Sinus rhythm Sinus tachycardia Sinus bradycardia Sinus arrhythmia Sick sinus syndrome SA block Sinus arrest AV blocks First-degree Second-degree Mobitz Type I
1. Rhythms & arrhythmias SA nodal rhythms Sinus rhythm Sinus tachycardia Sinus bradycardia Sinus arrhythmia Sick sinus syndrome SA block Sinus arrest AV blocks First-degree Second-degree Mobitz Type I
ARRHYTHMIAS. REENTERY occurs when propagating impulse fails to die out after normal activation of heart and persist to re excite the heart.
 ARRHYTHMIAS Arrhythmia is defined as loss of cardiac rhythm, especially irregularity of heartbeat. PATHOPHYSIOLOGY Ectopic complexes (ectopic beats) 1. By definition, arise from a site other than the sinus
ARRHYTHMIAS Arrhythmia is defined as loss of cardiac rhythm, especially irregularity of heartbeat. PATHOPHYSIOLOGY Ectopic complexes (ectopic beats) 1. By definition, arise from a site other than the sinus
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Treatment of Arrhythmias in the Emergency Setting
 Treatment of Arrhythmias in the Emergency Setting Zian H. Tseng, M.D. Assistant Professor of Medicine Cardiac Electrophysiology Section Cardiology Division University of California, San Francisco There
Treatment of Arrhythmias in the Emergency Setting Zian H. Tseng, M.D. Assistant Professor of Medicine Cardiac Electrophysiology Section Cardiology Division University of California, San Francisco There
! YOU NEED TO MONITOR QT INTERVALS IN THESE PATIENTS.
 Antiarrhythmic Pharmacopoeia Powerful drugs, split into 4 major classes, according to the predominant receptor they effect. Some fit into several classes at once, like sotolol. Some don t fit at all, owing
Antiarrhythmic Pharmacopoeia Powerful drugs, split into 4 major classes, according to the predominant receptor they effect. Some fit into several classes at once, like sotolol. Some don t fit at all, owing
Case #1. 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136
 Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
How do arrhythmias occur?
 How do arrhythmias occur? An arrhythmia is an abnormal heart rhythm (= dysrhythmia). Can be fast (tachy) or slow (brady). Brady arrhythmias are usually due to conduc;on block, while tachyarrhythmias are
How do arrhythmias occur? An arrhythmia is an abnormal heart rhythm (= dysrhythmia). Can be fast (tachy) or slow (brady). Brady arrhythmias are usually due to conduc;on block, while tachyarrhythmias are
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
ECGs and Arrhythmias: Family Medicine Board Review 2009
 Rate Rhythm Intervals Hypertrophy ECGs and Arrhythmias: Family Medicine Board Review 2009 Axis Jess (Fogler) Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Ischemia Overview
Rate Rhythm Intervals Hypertrophy ECGs and Arrhythmias: Family Medicine Board Review 2009 Axis Jess (Fogler) Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Ischemia Overview
Supraventricular Tachycardia: From Fetus to Adult. Mohamed Hamdan, MD
 Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Paramedic Rounds. Tachyarrhythmia's. Sean Sutton Dallas Wood
 Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ. ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C
 ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C Definitions of AF: A Simplified Scheme Term Definition Paroxysmal AF AF that terminates
ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C Definitions of AF: A Simplified Scheme Term Definition Paroxysmal AF AF that terminates
Arrhythmic Complications of MI. Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine
 Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
SHOCK THE PATIENT. Disclosures. Goals of the Talk. Tachyarrhythmias- Unstable 11/7/2017
 Disclosures Common Heart Rhythms in the Hospital Research Support: NIH, PCORI, Medtronic, Cardiogram Consulting: InCarda, Johnson & Johnson, Lifewatch Equity: InCarda Gregory M Marcus, MD, MAS Associate
Disclosures Common Heart Rhythms in the Hospital Research Support: NIH, PCORI, Medtronic, Cardiogram Consulting: InCarda, Johnson & Johnson, Lifewatch Equity: InCarda Gregory M Marcus, MD, MAS Associate
V. TACHYCARDIAS Rapid rhythm abnormalities
 V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
Atrial Fibrillation and Common Supraventricular Tachycardias. Sunil Kapur MD
 Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Rate and Rhythm Control of Atrial Fibrillation
 Rate and Rhythm Control of Atrial Fibrillation April 21, 2017 춘계심혈관통합학술대회 Jaemin Shim, MD, PhD Arrhythmia Center Korea University Anam Hospital Treatment of AF Goal Reducing symptoms Preventing complication
Rate and Rhythm Control of Atrial Fibrillation April 21, 2017 춘계심혈관통합학술대회 Jaemin Shim, MD, PhD Arrhythmia Center Korea University Anam Hospital Treatment of AF Goal Reducing symptoms Preventing complication
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Ventricular tachycardia Ventricular fibrillation and ICD
 EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation
 The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
Arrhythmias (I) Supraventricular Tachycardias. Disclosures
 Arrhythmias (I) Supraventricular Tachycardias Amy Leigh Miller, MD, PhD Cardiovascular Electrophysiology, Brigham & Women s Hospital Disclosures None Short R-P Tachycardia REGULAR with 1:1 P/R relationship
Arrhythmias (I) Supraventricular Tachycardias Amy Leigh Miller, MD, PhD Cardiovascular Electrophysiology, Brigham & Women s Hospital Disclosures None Short R-P Tachycardia REGULAR with 1:1 P/R relationship
a lecture series by SWESEMJR
 Electrolyte disturbances Hypokalaemia Decreased extracellular potassium increases excitability in the myocardial cells and consequently the effect of very severe hypokalaemia is ventricular arrhythmia.
Electrolyte disturbances Hypokalaemia Decreased extracellular potassium increases excitability in the myocardial cells and consequently the effect of very severe hypokalaemia is ventricular arrhythmia.
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint
 CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
Antiarrhythmics 17 I. OVERVIEW II. INTRODUCTION TO THE ARRHYTHMIAS
 Antiarrhythmics 17 I. OVERVIEW In contrast to skeletal muscle, which contracts only when it receives a stimulus, the heart contains specialized cells that exhibit automaticity. This means that they can
Antiarrhythmics 17 I. OVERVIEW In contrast to skeletal muscle, which contracts only when it receives a stimulus, the heart contains specialized cells that exhibit automaticity. This means that they can
Current Guideline for AF Treatment. Young Keun On, MD, PhD, FHRS Samsung Medical Center Sungkyunkwan University School of Medicine
 Current Guideline for AF Treatment Young Keun On, MD, PhD, FHRS Samsung Medical Center Sungkyunkwan University School of Medicine Case 1 59 year-old lady Sudden palpitation and breathlessness for 12 hours
Current Guideline for AF Treatment Young Keun On, MD, PhD, FHRS Samsung Medical Center Sungkyunkwan University School of Medicine Case 1 59 year-old lady Sudden palpitation and breathlessness for 12 hours
Atrial Fibrillation: Rate vs. Rhythm. Michael Curley, MD Cardiac Electrophysiology
 Atrial Fibrillation: Rate vs. Rhythm Michael Curley, MD Cardiac Electrophysiology I have no relevant financial disclosures pertaining to this topic. A Fib Epidemiology #1 Most common heart rhythm disturbance
Atrial Fibrillation: Rate vs. Rhythm Michael Curley, MD Cardiac Electrophysiology I have no relevant financial disclosures pertaining to this topic. A Fib Epidemiology #1 Most common heart rhythm disturbance
Ablation Update and Case Studies. Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group
 Ablation Update and Case Studies Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group Disclosures No financial relationships to disclose Objectives At the conclusion of this activity,
Ablation Update and Case Studies Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group Disclosures No financial relationships to disclose Objectives At the conclusion of this activity,
Acute Arrhythmias in the Hospitalized Patient
 Acute Arrhythmias in the Hospitalized Patient Gregory M Marcus, MD, MAS Associate Professor of Medicine Division of Cardiology University of California, San Francisc Disclosures Medtronic: Research Support
Acute Arrhythmias in the Hospitalized Patient Gregory M Marcus, MD, MAS Associate Professor of Medicine Division of Cardiology University of California, San Francisc Disclosures Medtronic: Research Support
VENTRICULAR ARRHYTHMIAS
 VI VENTRICULAR ARRHYTHMIAS Jonathan J. Langberg, m.d. David B. DeLurgio, m.d. Assessment and treatment of ventricular tachyarrhythmias present extraordinary challenges to the clinician. Moreover, the prognosis
VI VENTRICULAR ARRHYTHMIAS Jonathan J. Langberg, m.d. David B. DeLurgio, m.d. Assessment and treatment of ventricular tachyarrhythmias present extraordinary challenges to the clinician. Moreover, the prognosis
WHAT DO YOU SEE WHEN YOU STIMULATE BETA
 CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
TACHYARRHYTHMIAs. Pawel Balsam, MD, PhD
 TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
CORDARONE Sanofi-Aventis
 CORDARONE Sanofi-Aventis Composition Amiodarone 200 mg; tablets. Also AMPOULES 150 mg/3 ml. Indications Tablets Prevention of recurrence of the following: life-threatening ventricular tachycardias in which
CORDARONE Sanofi-Aventis Composition Amiodarone 200 mg; tablets. Also AMPOULES 150 mg/3 ml. Indications Tablets Prevention of recurrence of the following: life-threatening ventricular tachycardias in which
Ventricular arrhythmias in acute coronary syndromes. Dimitrios Manolatos, MD, PhD, FESC Electrophysiology Lab Evaggelismos General Hospital
 Ventricular arrhythmias in acute coronary syndromes Dimitrios Manolatos, MD, PhD, FESC Electrophysiology Lab Evaggelismos General Hospital introduction myocardial ischaemia and infarction leads to severe
Ventricular arrhythmias in acute coronary syndromes Dimitrios Manolatos, MD, PhD, FESC Electrophysiology Lab Evaggelismos General Hospital introduction myocardial ischaemia and infarction leads to severe
CARDIAC ARRHYTHMIAS IN NEONATE
 Introduction: CARDIAC ARRHYTHMIAS IN NEONATE DR. PANKAJ SAKHUJA Neonatologist Average heart rate in a healthy newborn is 120-160 beats/min and the range is from 80-230 beats/min. A normal (sinus) rhythm
Introduction: CARDIAC ARRHYTHMIAS IN NEONATE DR. PANKAJ SAKHUJA Neonatologist Average heart rate in a healthy newborn is 120-160 beats/min and the range is from 80-230 beats/min. A normal (sinus) rhythm
Lecture outline. Electrical properties of the heart. Automaticity. Excitability. Refractoriness. The ABCs of ECGs Back to Basics Part I
 Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
Cardiac Arrhythmias. Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company
 Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
4/14/15 HTEC 91. Topics for Today. Guess That Rhythm. Premature Ventricular Contractions (PVCs) Ventricular Rhythms
 4/14/15 Topics for Today HTEC 91 Medical Office Diagnostic Tests Week 5 Ventricular Rhythms PVCs: Premature Ventricular Contractions VT: Ventricular Tachycardia VF: Ventricular Fibrillation Asystole Study
4/14/15 Topics for Today HTEC 91 Medical Office Diagnostic Tests Week 5 Ventricular Rhythms PVCs: Premature Ventricular Contractions VT: Ventricular Tachycardia VF: Ventricular Fibrillation Asystole Study
ALS MODULE 7 Pharmacology
 ALS MODULE 7 Pharmacology Relates to HLT404C Apply Advanced Resuscitation Techniques Introduction There are no studies that addressed the order of drug administration. There is inadequate evidence to define
ALS MODULE 7 Pharmacology Relates to HLT404C Apply Advanced Resuscitation Techniques Introduction There are no studies that addressed the order of drug administration. There is inadequate evidence to define
Pharmacology: Arrhythmias PC PHPP 515 (IT I) Fall JACOBS Wed, Dec. 03 4:00 5:50 PM
 Pharmacology: Arrhythmias PC PHPP 515 (IT I) Fall 2014 JACOBS Wed, Dec. 03 4:00 5:50 PM Required Reading (via Access Pharmacy) Katzung: Chapters 14 Recommended Reading (via Access Pharmacy) Goodman and
Pharmacology: Arrhythmias PC PHPP 515 (IT I) Fall 2014 JACOBS Wed, Dec. 03 4:00 5:50 PM Required Reading (via Access Pharmacy) Katzung: Chapters 14 Recommended Reading (via Access Pharmacy) Goodman and
Adenosine. poison/drug induced. flushing, chest pain, transient asystole. Precautions: tachycardia. fibrillation, atrial flutter. Indications: or VT
 Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Practical Approach to Arrhythmias
 Outline Practical Approach to Arrhythmias Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Conduction System ECG Acquisition ECG Interpretation Heart rate Rhythm Arrhythmias Tachyarrhythmias Supraventricular
Outline Practical Approach to Arrhythmias Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Conduction System ECG Acquisition ECG Interpretation Heart rate Rhythm Arrhythmias Tachyarrhythmias Supraventricular
Implantable Cardioverter-Defibril. Defibrillators. Ratko Magjarević
 Implantable Cardioverter-Defibril Defibrillators Ratko Magjarević University of Zagreb Faculty of Electrical Engineering and Computing Croatia ratko.magjarevic@fer.hr Ventricular Fibrillation Ventricular
Implantable Cardioverter-Defibril Defibrillators Ratko Magjarević University of Zagreb Faculty of Electrical Engineering and Computing Croatia ratko.magjarevic@fer.hr Ventricular Fibrillation Ventricular
Prehospital Care Monograph
 Prehospital Care Monograph Amiodarone (Cordarone) City of Pittsburgh Bureau of Emergency Medical Services And Medical Direction Committee Center for Emergency Medicine Of Western Pennsylvania 1 This monograph
Prehospital Care Monograph Amiodarone (Cordarone) City of Pittsburgh Bureau of Emergency Medical Services And Medical Direction Committee Center for Emergency Medicine Of Western Pennsylvania 1 This monograph
ECGs and Arrhythmias: Family Medicine Board Review 2012
 Overview ECGs and Arrhythmias: Family Medicine Board Review 2012 Jess Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Bundle branch blocks Quick review of ischemia Arrhythmias
Overview ECGs and Arrhythmias: Family Medicine Board Review 2012 Jess Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Bundle branch blocks Quick review of ischemia Arrhythmias
Sustained tachycardia with wide QRS
 Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Document 3 Summary of Data and Guidance for Medical Professionals
 Document 3 Summary of Data and Guidance for Medical Professionals Anvirzel Anvirzel is a novel antitumor compound extracted from the plant Nerium oleander, which belongs to the family Apocynaceae. Anvirzel
Document 3 Summary of Data and Guidance for Medical Professionals Anvirzel Anvirzel is a novel antitumor compound extracted from the plant Nerium oleander, which belongs to the family Apocynaceae. Anvirzel
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ.
 «Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC
 Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
