ACUTE RENAL FAILURE oliguria anuria
|
|
|
- Albert Sharp
- 5 years ago
- Views:
Transcription
1 ACUTE RENAL FAILURE acute inability of kidneys to regulate water and solutes balance oliguria decrease in urine flow (less than 20ml/h) ml/day anuria urine output <50 ml/day
2 ACUTE PRERENAL FAILURE About 70% of all ARF cases Patomechanisms intravascular depletion cardiac failure systemic vasodilatation (sepsis, anesthesia, anaphylaxis) preglomerular vasoconstriction nonsteroidal antiinflammatory drugs vasoconstrictors
3 Hypovolemia Afferent Glomerular Arteriole CONSTRICTION VASODILATION GFR Mild Hypovolemia Angiotensin II Sympathethic system ADH < Myogenic reaction TG feedback NO Prostaglandins Unchanged Moderate hypovolemia Angiotensin II Sympathethic system ADH = Myogenic reaction TG feedback NO Prostaglandins Unchanged or slightly decreased Severe hypovolemia Angiotensin II Sympathethic system ADH > Myogenic reaction TG feedback NO Prostaglandins Decreased Acute Prerenal Failure
4 TOXIC NEPHROPATHY 1. Aminoglycosides - aminoglycosides are filtered - part of the filtered load is reabsorpbed in proximal tubule and accumulates within cells => toxicity 2. Cephalosporins - synergistic toxicity with aminoglycosides 3. Radiocontrast agents - induce osmotic diuresis => volume depletion - direct tubular toxicity (proximal tubules) - renal vasocontriction due to tubuloglomerular feedback - population with increased risk: - aged people - heart failure - volume depletion
5 TOXIC NEPHROPATHY 4. Organic solvents: - carbon tetrachloride (proximal tubules) - ethylene glycol: direct toxicity to epithelial cells + oxalic acid crystals 5. Pigment induced ATN - myoglobin (ATN occurs in 30% of pts with rhabdomyolysis) - hemoglobin: intravascular hemolysis hemoglobinuria - cytotoxicity towards proximal tubules - precipitation of protein within the tubules - heme proteins scavenge NO vasocontriction 6. Heavy metals - mercury, bismuth,arsen rare nowadays
6 PATHOMECHANISM OF OLIGURIA - ANURIA 1. Intrarenal vasoconstriction - in humans RBF by 30-50% - loss of autoregulation - endothelin > NO 2. Decreased permeability coefficient in glomerulus - reduction in size and density of the endothelial fenestrae - epithelial swelling - constriction of mesangial cells (ANG II, ADH, endothelins) 3. Damage to tubular epithelium - back leakage of filtrate - tubular obstruction
7 ACUTE OBSTRUCTIVE UROPATHY 1. Types of obstructive uropathy Partial or complete Unilateral or bilateral Acute or chronic 2. Changes in GFR Intitially unchanged Decreased ( after few hours) 3. Tubular function Partial obstruction Decreased ability to concentrate urine Decreased ability to acidify urine After relief of obstruction postobstructive diuresis: Volume overload Osmotic diuresis Decreased tubular Na + reabsorption (TALH) Reduced rersponsiveness to ADH
8 ACUTE OBSTRUCTIVE UROPATHY James M. Gloor & Vicente E. Torres
9 CLINICAL COURSE OF ATN 1. The initiation phase - hours days - no morphological changes - time for prevention of ATN 2. The maintenance phase - GFR is low < 5mL/min - lasts 1-2 weeks up to 6-8 weeks - patient is oliguric (<400mL/day) or non-oliguric (>400 ml/day) 3. The recovery phase - progressive rise in urine volume (up to ml/h) - dysfunction of tubules (polyuria + osmotic diuresis) - renal function improves within weeks up to 1 year - in 1/3 of pts GFR remains 20-30% below normal - minor but persistent defect in maximum urine concentration ability and in urine acidification
10 METABOLIC COMPLICATIONS OF ATN 1. Progressive rise in metabolites which are not excreted via kidney: - BUN of mg/dl per day (more in catabolic pts) - creatinine mg/dl per day 2. Water and sodium retention 3. Hyperkalemia - serum K + rises <0.5 meq/l/day 4. Acidosis - plasma HCO 3- falls 1-2 meq/l/day (more in catabolic pts) 5. Hypocalcemia due to: - hyperphosphatemia - resistance to PTH - lack of viatmin D hydroxylation in kidney - malabsorption
11 CHRONIC RENAL FAILURE CAUSES 1. Diabetic nephropathy 2. Hypertension 3. Glomerulonephritis 4. Other interstitial nephritis obstructive uropathy polycystic kidney disease
12 DIABETIC NEPHROPATHY
13 DIABETIC NEPHROPATHY- HYPERFILTRATION Increased filtered glucose load Increased proximal glucose-sodium rebasorption Decreased amount of sodium in distal nephron Decreased amount of sodium reabsorbed at macula densa Reduced release of adenosine from macula densa Reduced resistance of the glomerular afferent arteriole HYPERFILTRAFION
14 HYPERFILTRATION => GLOMERULOSCLEROSIS
15 DECREASE OF GFR vs. PLASMA CREATININE
16 STAGES OF RENAL FAILURE 1. GFR>50 ml/min no disorders 2. 50ml/min> GFR >25ml/min decreased functional kidneys reserve; polyuria 3. 25ml/min> GFR > 5 ml/min renal insufficiency; metabolic & systemic disorders 4. GFR< 5 ml/min - uremia
17 CRF - METABOLIC & SYSTEMIC DISORDERS Accumulation of toxic compounds organic (urea, guanidine, guanidinosuccinic acid, methylguanidine... β2-microglobulin deposition in connective tissue, joints middle molecules Advanced Glycation End Products inorganic compounds (phosphate) Hormonal alterations Impaired renal degradation Prolactin => lactation LH => gynecomastia Gastrin => gastritis Glucagon => glucose intolerance Insulin => hyperinsulinism PTH => osteitis fibrosa Decreased synthesis or activation Erythropoietin 1,25-dihydroxyvitamin D3 Trade-off hypothesis Excessive activation of compensatory mechanisms leads to pathology
18 CRF - METABOLIC & SYSTEMIC DISORDERS (I) Acid-base and water balance metabolic acidosis ( muscle degradation) hypervolemia hyperkalemia (rare) Anemia shortened lifespan of red blood cells reduced synthesis of erythropoetin inhibition of the erythropoetin effect on bone marrow excessive blood loses Lipids metabolism hipertriglyceridemia impaired lipolytic activity of plasma Cardiovascular system hypervolemia => increased afterload => left ventricle failure hypertension pericarditis
19 CRF - METABOLIC & SYSTEMIC DISORDERS (II) Nervous system peripheral polyneuropathy (organic toxic compounds and middle molecules) reduced activity of baroreceptors impaired motility of GI tract arrhytmias lack or excessive stimulation of muscles ( paralysis; restless legs syndrome) Gastrointestinal tract diffusion of toxic compounds into GI lumen inflammation bleeding malabsorption Bone demineralisation due to metabolic acidosis demineralisation ( hyperparathyroidism, lack of vitamin D 3 )
20 PROTEINURIA NEPHROTIC SYNDROME
21 GLOMERULAR PERMEABILITY proteins with a radius <20 A and neutral electric charge are filtered without hindrance proteins with a radius > 50A and neutral electric charge are not filtered
22 PROTEINURIA 1. Overflow proteinuria Excessive filtration of proteins which cannot be reabsorbed (myeloma, hemoglobinuria, myoglobinuria) 2. Tubular proteinuria inability of proximal tubules to reabsorb proteins filtered in normal amounts Fanconi syndrome, aminoglycosides nephropathy, heavy metal toxicity 3. Glomerular proteinuria glomerular hemodynamics glomerular endothelial cells glomerular basement membrane podocytes
23 NEPHROTIC SYNDROME Proteinuria > 3.5 g/day Hypoalbuminemia Hyperlipidemia Edema
24 REGULATION OF BLOOD PRESSURE BLOOD PRESSURE = CARDIAC OUTPUT x VASCULAR RESISTANCE A. Acute mechanisms fast, not precise,adaptation after hours-days B. Long term mechanism slow, precise, steady correction pressure diuresis adaptation of water & sodium excretion via kidney to maintain steady ECF volume => blood volume => BP
25 HYPERTENSION BLOOD PRESSURE BP systolic [mm Hg] BP diastolis [mm Hg] Normal <120 <80 Prehypertension Hypertension I o Hypertension II o > >100 95% of hypertension = primary, essential hypertension 5% of hypertension = secondary hypertension
26 PATHOGENESIS OF HYPERTENSION 1. Hypertension due to excessive ECF volume Initially hypervolemic hypertension which changes into vasoconstrictive hypertension 2. Vasoconstrictive hypertension The primary defect: increased peripheral ( renal) arterial resistance 3. Mixed hypertension
27 INHIBITORS of Na + -K + -ATPase SODIUM RETENTION Endogenous inhibitors of Na + -K + -ATPase Inhibition of Na + -K + -ATPase in renal tubules Inhibition of Na + -K + -ATPase in other cells Increased urinary Na + excretion Increased Ca ++ in cytosol Contraction of vascular smooth muscles Increased release of cathecholamines from presynaptic bulb Endothelium increased endothelins decreased NO INCREASED PERIPHERAL RESISTANCE
28 Renal failure Retention of sodium Hypervolemia Formation of natriuretic hormones (Inhibitors of Na + -K + ATPase) Hypertension Increased sodium excretion via surviving nephrons PATHOLOGY COMPENSATION
29 SODIUM & POTASSIUM DIET RECOMENDATIONS GENERAL: reduction of Na + intake and supplemetation of K + Na + intake of 65 mmol/day for 50 year old or younger Na + intake of 55 mmol/day for 50years< adult <70 years Na + intake of 50 mmol/day for older than 70 years K + intake higher than 120 mmol/day Dietary K + /Na + ratio should be increased from to approx. 2.0
30 SODIUM & POTASSIUM - DIET Sodium [ mmoll] Potassium [mmol] Two slices of ham Cup of canned chicken noodle soup Orange Cup of boiled pea Natural food 20-40/day >150/day Western civilisation /day 30-70/day Natural food K + /Na + ratio >3 => hypertension in less than 1% Western civilisation - K + /Na + ratio <0.4 => hypertension in 30% Only 12-15% of Na+ originates from natural food and about 80% is the result of food processing
31 ESSENTIAL PRIMARY HYPERTENSION 1. Abnormalities in CNS Increased basal sympathetic activity Abnormal stress response 2. Abnormalities in kidney Increased RAA activity Deficiency of vasodilators Excessive Na + reabsorption Age dependent decrease of the kidneys ability to excrete sodium 3. Abnormalities in blood vessels Decreased NO and/or increased endothelins production Excessive sensitivity to catecholamines
32 SECONDARY HYPERTENSION 1. Renal failure (2-4%) Hypervolemic mechanism 2. Stenosis of the renal artery (1%) Vasoconstrictive and hypervolemic mechanism 3. Pheochromocytoma Excessive synthesis of catecholamines => increased sympathetic activity Positive inotropic and chronotropic effect on the heart=> increased cardiac output Constriction of large veins =>increased preload=>increased cardiac output Stimulation of RAA &stimulation of Na + reabsorption in kidney=> ECF volume Constriction of arteries => increased BP
33 SECONDARY HYPERTENSION 4. Glucocorticoids Hypervolemic mechanism Stimulation of angiotensinogen synthesis in liver Sensitization of the vascular wall to catecholamines 5. Hyperthyroidism ( Systolic BP and Diastolic BP) reduced peripheral resistance increased sensitivity of the cardiovascular system to catecholamines cardiac hypertrophy ( thyroid hormones & hyperdynamic circulation) stimulation of angiotensinogen synthesis in liver stimulation of sympathetic system => increased release of renin increase in blood volume & erythrocyte mass)
34 SECONDARY HYPERTENSION 6. Obesity More frequent in abdominal obesity Release of FFA from adipocytes (catecholamines)=> FFA inhibit insulin uptake into hepatocytes=> peripheral hyperinsulinism Adipocytes produce: Leptin => stimulation of sympathetic system Angiotensin II Hormones decreasing tissue sensitivity to insulin => hyperinsulinism Increased intraabdominal pressure => increased pressure applied to renal veins=> reduced renal blood flow => reduced pressure natriuresis
35 HYPERTENSION SYSTEMIC CONSEQUENCES 1. Heart Increased afterload => concentric hypertrophy of the left ventricle Hypertrophy of the ventricle => decreased compliance of the ventricle => diastolic failure of heart Acceleration of atherosclerosis=>ischemic heart disease => systolic and diastolic heart failure 2. Arteries & microvessels Eccentric hypertrophy of the large arteries Concentric hypertrophy of the medium and small vessels Reduction of the microvascular network 3. Cerebral circulation Impaired autoregulation of the cerebral blood flow Shift of physiological autoregulation range (60 150mm Hg) towards higher values High blood pressure is better tolerated than lowered blood pressure
Renal diseases. Acute renal failure Chronic renal failure Nephrotic syndrome
 Renal diseases Acute renal failure Chronic renal failure Nephrotic syndrome Acute renal failure Acute renal failure (ARF) is characterized by sudden loss of the ability of the kidneys: to excrete wastes
Renal diseases Acute renal failure Chronic renal failure Nephrotic syndrome Acute renal failure Acute renal failure (ARF) is characterized by sudden loss of the ability of the kidneys: to excrete wastes
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
MAJOR FUNCTIONS OF THE KIDNEY
 MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
Glomerular filtration rate (GFR)
 LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
BUFFERING OF HYDROGEN LOAD
 BUFFERING OF HYDROGEN LOAD 1. Extracellular space minutes 2. Intracellular space minutes to hours 3. Respiratory compensation 6 to 12 hours 4. Renal compensation hours, up to 2-3 days RENAL HYDROGEN SECRETION
BUFFERING OF HYDROGEN LOAD 1. Extracellular space minutes 2. Intracellular space minutes to hours 3. Respiratory compensation 6 to 12 hours 4. Renal compensation hours, up to 2-3 days RENAL HYDROGEN SECRETION
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
** Accordingly GFR can be estimated by using one urine sample and do creatinine testing.
 This sheet includes the lecture and last year s exam. When a patient goes to a clinic, we order 2 tests: 1) kidney function test: in which we measure UREA and CREATININE levels, and electrolytes (Na+,
This sheet includes the lecture and last year s exam. When a patient goes to a clinic, we order 2 tests: 1) kidney function test: in which we measure UREA and CREATININE levels, and electrolytes (Na+,
RENAL PHYSIOLOGY. Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM
 RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte,
RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte,
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
RENAL PHYSIOLOGY. Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM
 RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte, H
RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte, H
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Introduction to the kidney: regulation of sodium & glucose. Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health
 Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Renal physiology II. Basic renal processes. Dr Alida Koorts BMS
 Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Alterations of Renal and Urinary Tract Function
 Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
1. Disorders of glomerular filtration
 RENAL DISEASES 1. Disorders of glomerular filtration 2. Nephrotic syndrome 3. Disorders of tubular transport 4. Oliguria and polyuria 5. Nephrolithiasis 6. Disturbances of renal blood flow 7. Acute renal
RENAL DISEASES 1. Disorders of glomerular filtration 2. Nephrotic syndrome 3. Disorders of tubular transport 4. Oliguria and polyuria 5. Nephrolithiasis 6. Disturbances of renal blood flow 7. Acute renal
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Functions of the kidney
 Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
THE CLINICAL BIOCHEMISTRY OF KIDNEY FUNCTIONS. Dr Boldizsár CZÉH
 THE CLINICAL BIOCHEMISTRY OF KIDNEY FUNCTIONS Dr Boldizsár CZÉH The kidneys are vital organs Functional unit: Nephron RENAL FUNCTIONS Electrolyte & Fluid Balances Acid-Base Balances Elimination of Metabolic
THE CLINICAL BIOCHEMISTRY OF KIDNEY FUNCTIONS Dr Boldizsár CZÉH The kidneys are vital organs Functional unit: Nephron RENAL FUNCTIONS Electrolyte & Fluid Balances Acid-Base Balances Elimination of Metabolic
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
HIHIM 409 7/26/2009. Kidney and Nephron. Fermamdo Vega, M.D. 1
 Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Basic Functions of the Kidneys
 Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Chapter 15 Fluid and Acid-Base Balance
 Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
renoprotection therapy goals 208, 209
 Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Acute Kidney Injury. APSN JSN CME for Nephrology Trainees May Professor Robert Walker
 Acute Kidney Injury APSN JSN CME for Nephrology Trainees May 2017 Professor Robert Walker Kidney International (2017) 91, 1033 1046; http://dx.doi.org/10.1016/ j.kint.2016.09.051 Case for discussion 55year
Acute Kidney Injury APSN JSN CME for Nephrology Trainees May 2017 Professor Robert Walker Kidney International (2017) 91, 1033 1046; http://dx.doi.org/10.1016/ j.kint.2016.09.051 Case for discussion 55year
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
General introduction of nephrology. Xiaoqiang Ding M.D., Ph.D. Department of nephrology Zhongshan Hospital, Fudan University
 General introduction of nephrology Xiaoqiang Ding M.D., Ph.D. Department of nephrology Zhongshan Hospital, Fudan University Terminology Kidney,renal Nephrology Scope of nephrology Kidney diseases and
General introduction of nephrology Xiaoqiang Ding M.D., Ph.D. Department of nephrology Zhongshan Hospital, Fudan University Terminology Kidney,renal Nephrology Scope of nephrology Kidney diseases and
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
Chapter 20 Diseases of the kidney:
 Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
Renal Blood flow; Renal Clearance. Dr Sitelbanat
 Renal Blood flow; Renal Clearance Dr Sitelbanat Objectives At the end of this lecture student should be able to describe: Renal blood flow Autoregulation of GFR and RBF Regulation of GFR The Calcuation
Renal Blood flow; Renal Clearance Dr Sitelbanat Objectives At the end of this lecture student should be able to describe: Renal blood flow Autoregulation of GFR and RBF Regulation of GFR The Calcuation
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION
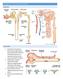 LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Acute Kidney Injury. I. David Weiner, M.D. Division of Nephrology, Hypertension and Transplantation University of Florida and NF/SGVHS
 Acute Kidney Injury I. David Weiner, M.D. Division of Nephrology, Hypertension and Transplantation University of Florida and NF/SGVHS 374-6102 David.Weiner@medicine.ufl.edu www.renallectures.com Concentration
Acute Kidney Injury I. David Weiner, M.D. Division of Nephrology, Hypertension and Transplantation University of Florida and NF/SGVHS 374-6102 David.Weiner@medicine.ufl.edu www.renallectures.com Concentration
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
HTN, retenopathy, edema, encephalopathy
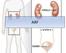 ARF Uremic syndrom Uremic syndrome (uremia) is a serious complication of CRF & ARF. It occurs when urea and other waste products build up in the body because the kidneys are unable to eliminate them. These
ARF Uremic syndrom Uremic syndrome (uremia) is a serious complication of CRF & ARF. It occurs when urea and other waste products build up in the body because the kidneys are unable to eliminate them. These
By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences. Body fluids and.
 By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences Body fluids and Renal physiology 25 Volume and Osmolality of Extracellular and Intracellular Fluids
By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences Body fluids and Renal physiology 25 Volume and Osmolality of Extracellular and Intracellular Fluids
Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION
 3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Water, Electrolytes, and Acid-Base Balance
 Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Renal pathophysiology.
 Renal pathophysiology basa.konecna@gmail.com Outline Intro basic structure & physiology Nephrotic syndrome Nephritic syndrome Acute renal failure Chronic kidney disease Gross structure and location Kidney
Renal pathophysiology basa.konecna@gmail.com Outline Intro basic structure & physiology Nephrotic syndrome Nephritic syndrome Acute renal failure Chronic kidney disease Gross structure and location Kidney
CCRN Review - Renal. CCRN Review - Renal 10/16/2014. CCRN Review Renal. Sodium Critical Value < 120 meq/l > 160 meq/l
 CCRN Review Renal Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Sodium 136-145 Critical Value < 120 meq/l > 160 meq/l Sodium Etiology
CCRN Review Renal Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Sodium 136-145 Critical Value < 120 meq/l > 160 meq/l Sodium Etiology
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note
![Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note](/thumbs/77/75431210.jpg) Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University
 RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Excretory System-Training Handout
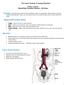 Excretory System-Training Handout Karen L. Lancour National Rules Committee Chairman Life Science Excretion - Excretion is the removal of the metabolic wastes of an organism. Wastes that are removed include
Excretory System-Training Handout Karen L. Lancour National Rules Committee Chairman Life Science Excretion - Excretion is the removal of the metabolic wastes of an organism. Wastes that are removed include
Introduction to Clinical Diagnosis Nephrology
 Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Functions of the kidney:
 Diseases of renal system : Normal anatomy of renal system : Each human adult kidney weighs about 150 gm, the ureter enters the kidney at the hilum, it dilates into a funnel-shaped cavity, the pelvis, from
Diseases of renal system : Normal anatomy of renal system : Each human adult kidney weighs about 150 gm, the ureter enters the kidney at the hilum, it dilates into a funnel-shaped cavity, the pelvis, from
Renal Reabsorption & Secretion
 Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
BLOCK REVIEW Renal Physiology. May 9, 2011 Koeppen & Stanton. EXAM May 12, Tubular Epithelium
 BLOCK REVIEW Renal Physiology Lisa M. HarrisonBernard, Ph.D. May 9, 2011 Koeppen & Stanton EXAM May 12, 2011 Tubular Epithelium Reabsorption Secretion 1 1. 20, 40, 60 rule for body fluid volumes 2. ECF
BLOCK REVIEW Renal Physiology Lisa M. HarrisonBernard, Ph.D. May 9, 2011 Koeppen & Stanton EXAM May 12, 2011 Tubular Epithelium Reabsorption Secretion 1 1. 20, 40, 60 rule for body fluid volumes 2. ECF
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Diuretic Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome.
 Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
5/10/2014. Observation, control of blood pressure. Observation, control of blood pressure and risk factors.
 Overview The Kidneys Nicola Barlow Clinical Biochemistry Department City Hospital Renal physiology Renal pathophysiology Acute kidney injury Chronic kidney disease Assessing renal function GFR Proteinuria
Overview The Kidneys Nicola Barlow Clinical Biochemistry Department City Hospital Renal physiology Renal pathophysiology Acute kidney injury Chronic kidney disease Assessing renal function GFR Proteinuria
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Chapter 10: Urinary System & Excretion
 Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
RENAL. 6. Renal acid secretion is affected by all of the following except a. pco 2 b. K c. Carbonic anhydrase d. Aldosterone e. Ca
 RENAL 1. The reabsorption of Na in the proximal tubules a. Reabsorbs 80% of the filtered sodium load b. Causes increased hypertonicity c. Is powered by N/H ATPase d. Shares a common carrier with glucose
RENAL 1. The reabsorption of Na in the proximal tubules a. Reabsorbs 80% of the filtered sodium load b. Causes increased hypertonicity c. Is powered by N/H ATPase d. Shares a common carrier with glucose
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Counter-Current System Regulation of Renal Functions
 Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
A&P of the Urinary System
 A&P of the Urinary System Week 44 1 Objectives Identify the organs of the urinary system, from a Identify the parts of the nephron (the functional unit List the characteristics of a normal urine specimen.
A&P of the Urinary System Week 44 1 Objectives Identify the organs of the urinary system, from a Identify the parts of the nephron (the functional unit List the characteristics of a normal urine specimen.
Chapter 23. Composition and Properties of Urine
 Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
RENAL PHYSIOLOGY. Danil Hammoudi.MD
 RENAL PHYSIOLOGY Danil Hammoudi.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood
RENAL PHYSIOLOGY Danil Hammoudi.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
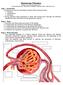 Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Urinary System (Anatomy & Physiology)
 Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Advanced Pathophysiology Unit 7: Renal-Urologic Page 1 of 18
 Advanced Pathophysiology Unit 7: Renal-Urologic Page 1 of 18 Learning Objectives for this File: 1. Learn how the macula densa monitors physiologic state and its connection with renin production based on
Advanced Pathophysiology Unit 7: Renal-Urologic Page 1 of 18 Learning Objectives for this File: 1. Learn how the macula densa monitors physiologic state and its connection with renin production based on
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (1)
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (1) Dr. Attila Nagy 2017 Functional roles of the kidney 1.Homeostasis of fluid compartments (isosmia, isovolemia, isoionia, isohydria,) 2. Elimination
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (1) Dr. Attila Nagy 2017 Functional roles of the kidney 1.Homeostasis of fluid compartments (isosmia, isovolemia, isoionia, isohydria,) 2. Elimination
II.Tubulointerstitial diseases
 II.Tubulointerstitial diseases two major groups of processes (1) ischemic or toxic tubular injury, leading to acute kidney injury (AKI) and acute renal failure, and (2) inflammatory reactions of the tubules
II.Tubulointerstitial diseases two major groups of processes (1) ischemic or toxic tubular injury, leading to acute kidney injury (AKI) and acute renal failure, and (2) inflammatory reactions of the tubules
Cardiorenal and Renocardiac Syndrome
 And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
RENAL FUNCTION An Overview
 RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
