International Spinal Cord Injury Cardiovascular Function Basic Data Set - Version 1.0 and Training cases
|
|
|
- Daisy Craig
- 5 years ago
- Views:
Transcription
1 1 TRAINING CASES FOR THE INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET The 5 cases included were prepared by Drs.Fin Biering-Sørensen, William Donovan, Ann- Katrin Karlsson and Andrei Krassioukov. The cases were reviewed and adjusted for inconsistencies by the others in the working group for the International Spinal Cord Injury Cardiovascular Function Basic Data Set, and by the external reviewer Dr. Clive Inman, to whom we are indebted for his careful review and expert comments. If the readers find specific issues requiring clarification, or any other issues related to the International Spinal Cord Injury Cardiovascular Function Basic Data Set that may be improved, please inform the working group for this Data Set. Contact: Andrei Krassioukov, Krassioukov@icord.org CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET VERSION 1.0. Case 1 This 47 years old woman sustained a C5 tetraplegia in a road traffic accident 1 st of December She also got intrathoracic injuries and was admitted to intensive care unit. She received a tracheostomy and was treated with invasive ventilation. Both parents had died from myocardial infarction. She was healthy except a history of hypertension and was treated with betablockers before injury. On admission to the hospital, her blood pressure was 90/60 mmhg, heart rate 55 and her betablockers were not given. She suffered from dependent oedema in the legs and was treated with pressure stockings. Three days post injury when still being in bed her oxygenation suddenly dropped to 80 %. There were signs of mucus in her trachea and suction of the tracehostomy was performed. During the suctioning she developed significant bradycardia with heart rate of 35 bpm. After tracheal suction her heart rate increased to 45 but decreased again when suction was initiated again. Pulse and blood pressure was monitored every 6 th hour and her pulse was found to be between bpm and systolic blood pressure was , diastolic blood pressure mmhg. A 24 h Holter ECG recording showed sinus bradycardia and a pacemaker was implanted on the 15 th of December. On the day of examination (January 5, 2010) at 10:00 am she was in bed in the supine position and her blood pressure was measured as 90/60 mmhg with regular pulse of 55 bpm. She used laxatives for bowel emptying, IE low molecular weight heparin for DVT prophylaxis and paracetamol for pain management.
2 2 INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET Version 1.0 DATA FORM Date performed: CASE 1 Cardiovascular history before spinal cord lesion (collected once): date last inserted YYYYMMDD, date last performed YYYYMMDD X Hypertension ropathy (alcoholic, diabetic, and others) Myocardial infarction Stroke X Family history of cardiovascular disease myocardial infarction Events related to cardiovascular function after spinal cord lesion: X Cardiac pacemaker, date , Cardiovascular function after spinal cord lesion within the last three months: X Cardiac conditions, specify sinus bradycardia X Dependent oedema mic dysreflexia Any medication affecting cardiovascular function on the day of examination: XNo Yes, anticholinergics Yes, antihypertensives (beta-blocker, antiarhythmics, ACE etc) Yes, antihypotensives
3 3 Yes, cardiac (digitalis etc) Yes, other, specify Objective measures: Time performed: 10:00 Position during testing: X Supine Devices in use during testing: None X Unknown Pulse: _55_beats per minute (bpm) X Regular Blood pressure: _90_/_60_mmHg
4 4 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET VERSION 1.0. Case 2 Mr Smith is a 20 years old man (Date of birth March 15, 1989) that was involved in a ski accident on February 15, He was admitted to the local hospital and diagnosed with a C6/7 fracture dislocation injury resulting in C6 AIS B tetraplegia. He was a healthy young man prior the accident and denied use of any medications or recreational drugs. On admission to the emergency department, he was alert and oriented and did not require ventilator support; his arterial blood pressure was measured at 80/60 mmhg with HR of 58 bpm. He was started on intravenous fluid and Dopamine drip. Following evaluation by the trauma team and MRI evaluation, he underwent decompression and bone graft fixation at C5-C7 using posterior approach. His postoperative recovery was uneventful. However, the first attempt with mobilization in the bed and transfer to the wheelchair resulted in significant episodes of dizziness and light-headedness. He required an abdominal binder and midodrine in the morning hours for management of orthostatic hypotension. Despite the initiation of the DVT prophylaxis protocol with enoxoparine, one month following injury (March 19, 2010) he developed a sudden onset of shortness of breath. On examination, swelling of the right calf was established and the patient also had tachycardia of 135 bpm. Following Spiral CT a right pulmonary embolism with plural effusion was diagnosed and consequently right popletal vein DVT was also established by ultrasound. Following one month s admission to the Spine Surgical Unit, the patient was transferred to the inpatient rehabilitation at the local rehabilitation centre. Presently, it is three months post his injury (May 20, 2010), he has continued with his rehabilitation at the rehabilitation centre. He is using a manual wheelchair for mobility. He continued to use an abdominal binder and pressure stockings to manage his lower arterial blood pressure; however, midodrin was discontinued approximately three weeks ago. He recently was switched from a Foley catheter to the intermittent catheterisation for the management of his bladder. Since admission to the rehabilitation centre he had one urinary tract infection that required oral antibiotics and was associated with episodes of autonomic dysreflexia. His bowel routine is occurring every other day on the commode and he requires digital stimulation. His present medications include baclofen 10 mg three times per day; warfarin 5 mg once per day (with INR ranging between 2-3 international units). Today during the morning examination (9:30 am) his supine arterial blood pressure was measured at 100/80 mmhg with regular HR of 68 bpm. Following transfer to the sitting position in the wheelchair his arterial blood pressure was measured at 80/65 mmhg with regular HR of 85 bpm and the subject complained on light-headedness. Neither abdominal binder or stockings were used during the testing today.
5 5 INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET - Version 1.0 DATA FORM CASE 2 Date performed: 2010/05/20 Cardiovascular history before spinal cord lesion (collected once): Cardiac pacemaker, date last inserted YYYYMMDD Cardiac surgery, specify, date last performed YYYYMMDD Other cardiac disorders, specify Hypertension Hypotension Orthostatic hypotension Deep vein thrombosis Neuropathy (alcoholic, diabetic, and others) Diabetes Hyperlipidemia Myocardial infarction Stroke Family history of cardiovascular disease Other, specify X None of the above Events related to cardiovascular function after spinal cord lesion: Cardiac pacemaker X Pulmonary embolism 2010/03/19 Myocardial infarction, Stroke, date X Deep vein thrombosis 2010/03/19 Other, specify, None of the above Cardiovascular function after spinal cord lesion within the last three months: Cardiac conditions, specify X Orthostatic hypotension Dependent oedema Hypertension X Autonomic dysreflexia Other, specify None of the above
6 6 Any medication affecting cardiovascular function on the day of examination: No Yes, anticholinergics Yes, antihypertensives (beta-blocker, antiarhythmics, ACE etc) Yes, antihypotensives Yes, cardiac (digitalis etc) Yes, other, specify X None of the above Objective measures: Time performed: 09:30 am Position during testing: Devices in use during testing: X X None Pulse: _85_beats per minute (bpm) X Regular Blood pressure: 80/65 mmhg
7 7 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET VERSION 1.0. Case 3 Mr. Elm is a 54 years old man (date of birth July 27, 1955) who was involved in a motor vehicle accident on January 20, He was extracted from the vehicle by the fire department crew and required resuscitation on the scene of the accident. He was admitted to the local hospital unconscious with ventilator support. His arterial blood pressure on admission was 90/60 mmhg. He regained consciousness a few hours following admission. Evaluation by the trauma team and following MRI evaluation established that the subject had a C2 odontoid fracture with complete C2 spinal cord injury. Five years ago he was diagnosed with diabetes mellitus type 2 and hyperlipidemia. He also had a history of hypertension and obesity. In addition to Insulin he was also taking ramipril, hydrochlorothiazide and atorvastatin on a regular basis. His postoperative recovery was complicated with atelectasis and pneumonia that required antibiotic therapy. Furthermore, the first attempt with mobilization in the bed resulted in significant episodes of dizziness and light-headedness. His supine blood pressure was usually within 135/85 mmhg but with transfer to the sit up position he demonstrated a significant drop to 70/50 mmhg despite the use of an abdominal binder. The initiation of midodrine 10 mg per mouth 60 min before the transfer to the wheelchair in the morning and an additional dose in the afternoon resulted in stabilization of blood pressure and resolution of light-headedness and dizziness. Despite the initiation of the DVT prophylaxis protocol with enoxoparine, one month following injury (February 15, 2010) he developed a right leg swelling and redness. Ultrasound confirmed the right popliteal vein DVT. Presently, it is five months post his injury (June 20, 2010), he has continued with his rehabilitation at the inpatient Rehabilitation Unit. He requires a power wheel chair for mobility that also has a ventilator for respiratory support. He continued to use an abdominal binder and midodrine for management of his lower arterial blood pressure and orthostatic hypotension. He has a Foley catheter and since admission to the rehabilitation centre he had numerous urinary tract infections complicated with significant episodes of autonomic dysreflexia (AD). His bowel routine is occurring every other day in the bed and also accompanied with mild episodes of AD during the digital stimulation. There is also persistent oedema present in his legs (right>left) from the knee down, and patient required pressure stockings during the day time. His present medications include baclofen 10 mg three times per day; warfarin 5 mg once per day (with INR ranging between 2-3 international units); atorvastatin, insulin sliding scale. Today during the morning examination (8:30 am) while seated in his wheelchair his arterial blood pressure was measured at 95/70 mmhg with regular HR of 68 bpm. Neither abdominal binder or stockings were used during the testing today.
8 8 INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET Version 1.0 DATA FORM Date performed: 2010/06/20 CASE 3 Cardiovascular history before spinal cord lesion (collected once): date last inserted YYYYMMDD, date last performed YYYYMMDD X Hypertension pathy (alcoholic, diabetic, and others) XDiabetes X Hyperlipidemia Myocardial infarction Stroke Family history of cardiovascular disease Events related to cardiovascular function after spinal cord lesion: date X Deep vein thrombosis 2010/02/15, Cardiovascular function after spinal cord lesion within the last three months: X Orthostatic hypotension X Dependent oedema X Autonomic dysreflexia e Any medication affecting cardiovascular function on the day of examination: No Yes, anticholinergics Yes, antihypertensives (beta-blocker, antiarhythmics, ACE etc)
9 9 X Yes, antihypotensives Yes, cardiac (digitalis etc) Yes, other, specify Objective measures: Time performed: 08:30 am Position during testing: Devices in use during testing: X X None stockings Pulse: _68_beats per minute (bpm) X Regular Blood pressure: 95/70 mmhg
10 10 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET VERSION 1.0. Case 4 Mr. Oak is a 49-year-old man with a history of alcoholism and peripheral neuropathy who fell off a bar stool, striking his chin against the floor when preparing to leave the pub on March 5, He was unable to get up. Ambulance was called and he was taken to a trauma center where he was noted to be oriented to person and place but not to time, and in no respiratory distress. Vital signs at admission were following: blood pressure (BP) - 100/75 mmhg, pulse (P) - 48 bpm, irregular, respiration (R) 14 per minute. Abdominal exam revealed hepatomegally 3 finger breaths below the right costal margin. International Standards exam revealed a C6 AIS D central cord syndrome. C-spine plain films were unremarkable except for the degenerative joint disease and cervical stenosis at C 4/5 and 5/6. MRI showed cord swelling and edema from C4 to C7 with a small central hemorrhage at C5, 6 levels. He was noted to have a past history of atrial fibrillation. Medications included warfarin and digoxin. The latter was held due to bradycardia. No surgery was deemed warranted. He was placed in a cervical orthosis. During the rehabilitation he remained hypotensive and required midodrine 10 mg, 1 hour before rising in the morning. At discharge, he was able to walk with a spastic gait, using a rolling walker, he had hand intrinsic atrophy and could void voluntarily to completion but with urgency. He required oxybutinin 5 mg twice daily. He also had sensation of bowel fullness but required a suppository each evening to completely evacuate. Following inpatient rehabilitation he was discharge home. Today, during his first clinic visit (June , 9:30 AM), his vital signs taken in the morning, while seated, without abdominal binder were as following BP - 108/76 mmhg, P - 69 bpm (irregular); R -12 per minute. He admitted that he had numerous falls during the last few weeks but did not seek medical attention. He stated that falls commonly associated with episodes of lightheadedness and dizziness. Exam shows a bruise over the right trochanter but no evidence of bone injury. Exam was noted for 2 finger breath hepatomegally, safe but still spastic gait with 1 forearm crutch. X-rays of the right hip were negative for fracture. His present medication includes following: warfarin with weekly INR (his INR today was 2.1), oxybutinin; and digoxin.
11 11 INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET Version 1.0 DATA FORM CASE 4 Date performed: 2010/06/12 Cardiovascular history before spinal cord lesion (collected once): Cardiac pacemaker, date last inserted Cardiac surgery, specify, date last performed X Other cardiac disorders, specify atrial fibrillation Hypertension Hypotension Orthostatic hypotension Deep vein thrombosis X Neuropathy alcoholic None of the above Events related to cardiovascular function after spinal cord lesion: Cardiac pacemaker, Myocardial infarction, Stroke, Pulmonary embolism, Deep vein thrombosis, Other, specify, X None of the above Cardiovascular function after spinal cord lesion within the last three months: Cardiac conditions, specify X Orthostatic hypotension Dependent oedema Hypertension Autonomic dysreflexia Deep vein thrombosis, X Other, specify: atrial fibrillation None of the above Any medication affecting cardiovascular function on the day of examination: No Yes, anticholinergics
12 12 Objective measures: Yes, antihypertensives (beta-blocker, antiarhythmics, ACE etc) ves X Yes, cardiac (digitalis etc) digoxin X Yes, other, specify oxybutinin, warfarin None of the above Time performed: 09:30 AM Position during testing: X Sitting Supine Devices in use during testing: Abdominal binder Pressure stockings Unknown X None Pulse: 69 beats per minute (bpm) Regular X Irregular Blood pressure: 108/76 mmhg
13 13 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET VERSION 1.0. Case 5 This 48 years old previously healthy man without any medicine intake crashed with his mountain bike on June 17, He was unconscious and initially without pulse or respiration. Witnesses started resuscitation. He was not seen to move any of the extremities. When the ambulance arrived he had pulse and difficult respiration and Glasgow Coma Scale (GCS) of 3. He was intubated at the site of accident and during this procedure he woke up to GCS 8-9. Afterwards he was transferred to the Trauma centre, still without any movement or reflexes and with flaccid anal sphincter. His head CT scan showed no fractures other intracranial pathologies. The cervical spine CT showed a type II C2 fracture with a little posterior subluxation and fracture of C4 right lamina and facet joint. His chest and abdominal CT was without trauma signs. Initially the blood pressure (BP) was labile and infusion with noradrenalin was started. His BP stabilized to 105/53 mmhg with a regular heart rate (HR). On June 19, 2010 he was surgically stabilised with a screw in C2 and on the same time he had a tracheostomy performed. Following recovery from anaesthesia, he was found to have an AIS A, C1 lesion. Within the first week after injury there was tendency to bradycardia, including four incidences of asystole, usually caused by tracheal suction or turning in the bed. The latest incidence was a 30 second sinus arrest followed by ventricular escapade rhythm. With initiation of isoprenalin his cardiovascular parameters were measured at 159/92 mmhg with regular HR of 90 bpm. On June 24, 2010 he was instrumented with a permanent pacemaker. During the hospitalisation to the ICU he also developed orthostatic hypotension that required midodrine for management and episodes of autonomic dysreflexia that required administration of captopril. On August 2, 2010 he was transferred from the ICU to the Centre for Respiratory Disabled to have instituted home ventilation with 24 hours team support. On November 1, 2010 he was transferred to the Spinal Injures Centre for final adaptation of his aids including the electric wheelchair, which he learned to drive with the chin. When he was discharged to his adapted home on November 29, 2010 his neurological lesion was unchanged AIS A C1, he used various pharmacological agents for the bowel management and midodrine mg for his orthostatic hypotension. During the last few months he has been experiencing episodes of orthostatic hypotension and autonomic dysreflexia that required pharmacological management. On examination at 1:00 PM on the day of discharge his BP was 110/65 mmhg, with regular HR of 60 bpm, measured sitting in the wheelchair without use of pressure stockings or abdominal binder.
14 14 INTERNATIONAL SPINAL CORD INJURY CARDIOVASCULAR FUNCTION BASIC DATA SET Version 1.0 DATA FORM Date performed: CASE 5 Cardiovascular history before spinal cord lesion (collected once): date last inserted YYYYMMDD, date last performed YYYYMMDD ropathy (alcoholic, diabetic, and others) Myocardial infarction Stroke Family history of cardiovascular disease X None of the above Events related to cardiovascular function after spinal cord lesion: X Cardiac pacemaker, date , the above Cardiovascular function after spinal cord lesion within the last three months: X Orthostatic hypotension Dependent oedema X Autonomic dysreflexia Any medication affecting cardiovascular function on the day of examination: No Yes, anticholinergics Yes, antihypertensives (beta-blocker, antiarhythmics, ACE etc) X Yes, antihypotensives (Midodrine)
15 15 Yes, cardiac (digitalis etc) Yes, other, specify Objective measures: Time performed: 13:00 Position during testing: Devices in use during testing: X Sitting X None Pulse: 60 beats per minute (bpm) X Regular Blood pressure: _110/65_mmHg
ADULT TRANSCATHETER AORTIC VALVE REPLACEMENT (TAVR) TELEMETRY BED TRANSFER ORDERS 1 of 4
 TELEMETRY BED TRANSFER 1 of 4 9 Actual 9 Estimated Patient ID Area Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Transfer to: 10 South Attending Physician: Diagnosis:
TELEMETRY BED TRANSFER 1 of 4 9 Actual 9 Estimated Patient ID Area Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Transfer to: 10 South Attending Physician: Diagnosis:
AUTONOMIC FUNCTION IS A HIGH PRIORITY
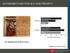 AUTONOMIC FUNCTION IS A HIGH PRIORITY 1 Bladder-Bowel-AD Tetraplegia Sexual function Walking Bladder-Bowel-AD Paraplegia Sexual function Walking 0 10 20 30 40 50 Percentage of respondents an ailment not
AUTONOMIC FUNCTION IS A HIGH PRIORITY 1 Bladder-Bowel-AD Tetraplegia Sexual function Walking Bladder-Bowel-AD Paraplegia Sexual function Walking 0 10 20 30 40 50 Percentage of respondents an ailment not
bilateral, both before below elbow twice a day below knee bedrest
 Abbreviations Student Name: A approximately assessment assist active active assist abdominal aortic aneurysm active assistive range of motion abduction/adduction acromioclavicular joint anterior cruciate
Abbreviations Student Name: A approximately assessment assist active active assist abdominal aortic aneurysm active assistive range of motion abduction/adduction acromioclavicular joint anterior cruciate
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
SPINAL CORD INJURIES DR. F. DE V. THERON MUELMED/PAH HOSPITAL SPINAL UNIT 2012
 SPINAL CORD INJURIES DR. F. DE V. THERON MUELMED/PAH HOSPITAL SPINAL UNIT 2012 INTRODUCTION Mortal condition recognised since antiquity First described in the Edwin Smith papyrus 2500BC An ailment not
SPINAL CORD INJURIES DR. F. DE V. THERON MUELMED/PAH HOSPITAL SPINAL UNIT 2012 INTRODUCTION Mortal condition recognised since antiquity First described in the Edwin Smith papyrus 2500BC An ailment not
convey the clinical quality measure's title, number, owner/developer and contact
 CMS-0033-P 153 convey the clinical quality measure's title, number, owner/developer and contact information, and a link to existing electronic specifications where applicable. TABLE 20: Proposed Clinical
CMS-0033-P 153 convey the clinical quality measure's title, number, owner/developer and contact information, and a link to existing electronic specifications where applicable. TABLE 20: Proposed Clinical
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Nitroglycerin and Heparin Drip Interfacility Protocols
 Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
ADULT CARDIAC SURGERY TELEMETRY BED TRANSFER ORDERS 1 of 4
 ADULT CARDIAC SURGERY TELEMETRY BED TRANSFER 1 of 4 9 Actual 9 Estimated Attending Surgeon: Medical Record Number Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART
ADULT CARDIAC SURGERY TELEMETRY BED TRANSFER 1 of 4 9 Actual 9 Estimated Attending Surgeon: Medical Record Number Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine
 Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
HTEC 91. Performing ECGs: Procedure. Normal Sinus Rhythm (NSR) Topic for Today: Sinus Rhythms. Characteristics of NSR. Conduction Pathway
 HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
4. Which survey program does your facility use to get your program designated by the state?
 TRAUMA SURVEY Please complete one survey for each TCD designation you have in your facility. There would be a maximum of three surveys completed if your facility was designated as a trauma, stroke and
TRAUMA SURVEY Please complete one survey for each TCD designation you have in your facility. There would be a maximum of three surveys completed if your facility was designated as a trauma, stroke and
Basic Assessment and Treatment of Trauma
 Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
5AB Dysrhythmia Interpretation and Management 2016
 5AB Dysrhythmia Interpretation and Management 2016 How to complete your biennial ECG review: A website has been created that contains the basic review information. Use this as a reference during your review.
5AB Dysrhythmia Interpretation and Management 2016 How to complete your biennial ECG review: A website has been created that contains the basic review information. Use this as a reference during your review.
Life Care Plan. Eric Henderson Potential Complications For Information Purposes Only. No Prediction of Frequency of Occurrence Available.
 Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
Acute Stroke with Alteplase Administration Order Set
 Review Due Date: 2017 October PATIENT CARE DERS Weight: Adverse Reactions or Intolerances Drug No Yes (list) Food No Yes (list) _ Latex No Yes Admission Admit to Neurology service: Dr. Critical Care Diagnosis:
Review Due Date: 2017 October PATIENT CARE DERS Weight: Adverse Reactions or Intolerances Drug No Yes (list) Food No Yes (list) _ Latex No Yes Admission Admit to Neurology service: Dr. Critical Care Diagnosis:
B. high blood pressure. D. hearing impairment. 2. Of the following, the LEAST likely reason for an EMS unit to be called
 CHAPTER 36 Geriatrics HANDOUT 36-2: Evaluating Content Mastery Student s Name EVALUATION CHAPTER 36 QUIZ Write the letter of the best answer in the space provided. 1. Among patients over age 65, almost
CHAPTER 36 Geriatrics HANDOUT 36-2: Evaluating Content Mastery Student s Name EVALUATION CHAPTER 36 QUIZ Write the letter of the best answer in the space provided. 1. Among patients over age 65, almost
North West London Trauma Network Spinal Pathway and Protocols
 North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
QUESTION EXAMPLES ECG
 ACEM Fellowship VAQ Examination QUESTION EXAMPLES ECG ECG 1: A 16 year old boy with a congenital heart problem presents to your ED with syncopal episodes. An ECG is taken. Describe and interpret his ECG
ACEM Fellowship VAQ Examination QUESTION EXAMPLES ECG ECG 1: A 16 year old boy with a congenital heart problem presents to your ED with syncopal episodes. An ECG is taken. Describe and interpret his ECG
Chapter 32. Objectives. Objectives 01/09/2013. Spinal Column and Spinal Cord Trauma
 Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
AF in the ER: Common Scenarios CASE 1. Fast facts. Diagnosis. Management
 AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
Appendix to Gibson et al. Application of a decision rule and a D-dimer assay in the
 Appendix to Gibson et al. Application of a decision rule and a D-dimer assay in the diagnosis of pulmonary embolism (Thromb Haemost 2010; 103.4) Case 1 You are paged by an emergency room physician, who
Appendix to Gibson et al. Application of a decision rule and a D-dimer assay in the diagnosis of pulmonary embolism (Thromb Haemost 2010; 103.4) Case 1 You are paged by an emergency room physician, who
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Life Care Plan. Hannah Sayne Potential Complications For Information Purposes Only. No Prediction of Frequency of Occurrence Available.
 Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
Venous Thromboembolism Prophylaxis
 Approved by: Venous Thromboembolism Prophylaxis Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: Date Approved January
Approved by: Venous Thromboembolism Prophylaxis Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: Date Approved January
Quality & Hospital Acquired Conditions
 Quality & Hospital Acquired Conditions Rebecca Armbruster, DO, MS, FACOI Medical Director Resource Management Patricia Heys, BS Director of Infection Prevention & Control Sally Hinkle, DNP, MPA, RN Director
Quality & Hospital Acquired Conditions Rebecca Armbruster, DO, MS, FACOI Medical Director Resource Management Patricia Heys, BS Director of Infection Prevention & Control Sally Hinkle, DNP, MPA, RN Director
WESTMEAD Cardiac QUESTIONS PRACTICE SAQ
 QUESTION 1 A 65-year-old man presents to the emergency department with a history of palpitations. His vital signs are: BP 105/60 mmhg HR 156 beats/min RR 26 /min Temperature 36.2 o C His ECG is on the
QUESTION 1 A 65-year-old man presents to the emergency department with a history of palpitations. His vital signs are: BP 105/60 mmhg HR 156 beats/min RR 26 /min Temperature 36.2 o C His ECG is on the
autonomic dysreflexia
 ! autonomic dysreflexia AUTONOMIC DYSREFLEXIA & YOU Recognize and act WHAT IS AUTONOMIC DYSREFLEXIA (AD)? It is a dangerous rise in your blood pressure that is triggered by a painful or non-painful stimulation
! autonomic dysreflexia AUTONOMIC DYSREFLEXIA & YOU Recognize and act WHAT IS AUTONOMIC DYSREFLEXIA (AD)? It is a dangerous rise in your blood pressure that is triggered by a painful or non-painful stimulation
Critical Incidents Reported to Manitoba Health
 Critical Incidents Reported to Manitoba Health April 1, 2013 - June 30, 2013 Degree of PCH resident had unwitnessed fall resulting in fractured hip. Found on floor with walker by feet. Surgical repair
Critical Incidents Reported to Manitoba Health April 1, 2013 - June 30, 2013 Degree of PCH resident had unwitnessed fall resulting in fractured hip. Found on floor with walker by feet. Surgical repair
ACLS Prep. Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep.
 November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
Our Commitment to Quality and Patient Safety Core Measures
 Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
SCORES FOR 4 TH QUARTER, RD QUARTER, 2014
 SCORES FOR 4 TH QUARTER, 2013 3 RD QUARTER, 2014 PATIENT SATISFACTION SCORES (HCAHPS): 4 STARS OUT OF 5 (ONLY 4 AREA ACUTE CARE HOSPITALS RECEIVED A 4-STAR RATING. NONE ACHIEVED 5-STARS). STRUCTURAL MEASURES:
SCORES FOR 4 TH QUARTER, 2013 3 RD QUARTER, 2014 PATIENT SATISFACTION SCORES (HCAHPS): 4 STARS OUT OF 5 (ONLY 4 AREA ACUTE CARE HOSPITALS RECEIVED A 4-STAR RATING. NONE ACHIEVED 5-STARS). STRUCTURAL MEASURES:
GENERAL SURGICAL ADULT POST-OPERATIVE ORDERS 1 of 4
 down ADULT POST-OPERATIVE 1 of 4 9 Actual 9 Estimated Patient ID Area Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Admit to: Post Anesthesia Care Unit (PACU),
down ADULT POST-OPERATIVE 1 of 4 9 Actual 9 Estimated Patient ID Area Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Admit to: Post Anesthesia Care Unit (PACU),
2:39 2: Dizziness and nausea Cerebral. 2:57 1: Vomiting Gastro-intestinal
 Supplemental: Table B: Detailed description of adverse events by time, treatment group and procedure T-spinal to incident T-spinal to PACU discharge Group THA/TKA Adverse event description Adverse event
Supplemental: Table B: Detailed description of adverse events by time, treatment group and procedure T-spinal to incident T-spinal to PACU discharge Group THA/TKA Adverse event description Adverse event
Diagnosis: Allergies with reaction type:
 Patient Name: Diagnosis: Allergies with reaction type: ICU Stroke-Ischemic S/P tpa Version 2 5/29/14 This order set is designed to be used with an admission set or for a patient already admitted Nursing
Patient Name: Diagnosis: Allergies with reaction type: ICU Stroke-Ischemic S/P tpa Version 2 5/29/14 This order set is designed to be used with an admission set or for a patient already admitted Nursing
Hip Surgery and Mobility
 Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
How to prevent blood clots whilst in hospital and after your return home
 How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
Canadian Trauma Trials Collaborative. Occult Pneumothorax in Critical Care (OPTICC): Standardized Data Collection Sheet
 Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
A walk through a STEMI
 A walk through a STEMI M.M. s Story Kim Robison Ashley Corcoran Situation M.M. is an 82 year old male brought in by private vehicle on 10/22/17 to the Emergency Department Pt. c/o left arm numbness, pain
A walk through a STEMI M.M. s Story Kim Robison Ashley Corcoran Situation M.M. is an 82 year old male brought in by private vehicle on 10/22/17 to the Emergency Department Pt. c/o left arm numbness, pain
11. Spinal cord injury
 11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
Admission of patient CVICU and hemodynamic monitoring
 Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
SPINE EVALUATION AND CLEARANCE Basic Principles
 SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
Mr B M Soni Consultant in Spinal Injuries
 Mr B M Soni Consultant in Spinal Injuries Autonomic Dysreflexia in Spinal Cord Injury Patients 1 What is autonomic dysreflexia? Autonomic dysreflexia is a condition that develops after spinal cord injury
Mr B M Soni Consultant in Spinal Injuries Autonomic Dysreflexia in Spinal Cord Injury Patients 1 What is autonomic dysreflexia? Autonomic dysreflexia is a condition that develops after spinal cord injury
CEU Final Exam for Code It! Sixth Edition
 CEU Final Exam for 3-2-1 Code It! Sixth Edition Note to CEU applicant In order to receive CEU credit for taking this exam, the following criteria must be met: You must be certified by AAPC prior to purchasing
CEU Final Exam for 3-2-1 Code It! Sixth Edition Note to CEU applicant In order to receive CEU credit for taking this exam, the following criteria must be met: You must be certified by AAPC prior to purchasing
Nursing Management Pre /Post Thrombolysis in Stroke
 Craigavon Area Hospital Guidelines for Nursing Management Pre /Post Thrombolysis in Stroke 1. A senior nurse in the stroke unit will be required to monitor the patients condition post Thrombolysis on a
Craigavon Area Hospital Guidelines for Nursing Management Pre /Post Thrombolysis in Stroke 1. A senior nurse in the stroke unit will be required to monitor the patients condition post Thrombolysis on a
Resident At Risk. The National Early Warning Score (NEWS) and Monitoring Vital Signs
 Resident At Risk The National Early Warning Score (NEWS) and Monitoring Vital Signs Schein et al 64 consecutive ward patients requiring CPR 84% clinical deterioration 8 hours before arrest Pathophysiology
Resident At Risk The National Early Warning Score (NEWS) and Monitoring Vital Signs Schein et al 64 consecutive ward patients requiring CPR 84% clinical deterioration 8 hours before arrest Pathophysiology
Stroke Transfer Checklist
 Stroke Transfer Checklist When preparing to transfer an acute stroke patient to the UF Health Shands Comprehensive Stroke Center, please make every attempt to include the following information: Results
Stroke Transfer Checklist When preparing to transfer an acute stroke patient to the UF Health Shands Comprehensive Stroke Center, please make every attempt to include the following information: Results
URN: Family name: Given name(s): Address: Initial Signature Print Name Role
 Do Not Write in this binding margin v5.00-02/2012 Mat. No.: 10206019 SW030b The State of Queensland (Queensland Health) 2012 Contact CIM@health.qld.gov.au ÌSW030bIÎ Facility: s Never Replace Clinical Judgement
Do Not Write in this binding margin v5.00-02/2012 Mat. No.: 10206019 SW030b The State of Queensland (Queensland Health) 2012 Contact CIM@health.qld.gov.au ÌSW030bIÎ Facility: s Never Replace Clinical Judgement
Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc. Copyright 2014, 2011, 2006 by Saunders, an imprint of Elsevier, Inc.
 Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc 1 Spinal Cord Injury Results from fracture and/or dislocation of vertebrae // Compresses, stretches, or tears spinal cord Cervical
Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc 1 Spinal Cord Injury Results from fracture and/or dislocation of vertebrae // Compresses, stretches, or tears spinal cord Cervical
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Chapter 18. Objectives. Objectives 01/09/2013. Altered Mental Status, Stroke, and Headache
 Chapter 18 Altered Mental Status, Stroke, and Headache Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives
Chapter 18 Altered Mental Status, Stroke, and Headache Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives
Thrombolysis Delivery, Care, and Monitoring. 5 Acute Trusts - 6 Primary Care Trusts Ambulance Trust 4 Local Authorities
 Thrombolysis Delivery, Care, and Monitoring Documentation & Pathways Need to follow locally agreed policies and procedures Follow thrombolysis pathway? Need to complete Sits database Weight Dose matters!
Thrombolysis Delivery, Care, and Monitoring Documentation & Pathways Need to follow locally agreed policies and procedures Follow thrombolysis pathway? Need to complete Sits database Weight Dose matters!
Primary Stroke Center Quality & Performance Measures
 Primary Stroke Center Quality & Performance Measures This section of the manual contains information related to the quality performance of Primary Stroke Centers. Brain Attack Coalition Definitions Recognition
Primary Stroke Center Quality & Performance Measures This section of the manual contains information related to the quality performance of Primary Stroke Centers. Brain Attack Coalition Definitions Recognition
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship
 Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Cardiovascular Emergencies. Chapter 12
 Cardiovascular Emergencies Chapter 12 Cardiovascular Emergencies Cardiovascular disease (CVD) claimed 931,108 lives in the US during 2001. 2,551 per day Almost two people per minute! CVD accounts for 38.5%
Cardiovascular Emergencies Chapter 12 Cardiovascular Emergencies Cardiovascular disease (CVD) claimed 931,108 lives in the US during 2001. 2,551 per day Almost two people per minute! CVD accounts for 38.5%
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM. Gordon Lowe Professor of Vascular Medicine University of Glasgow
 CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
Pathophysiology. Tutorial 3 Hemodynamic Disorders
 Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
CHEST INJURY PULMONARY CONTUSION
 CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
ACUTE KIDNEY INJURY (AKI) ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) ADVANCED DIRECTIVE LIMITING CARE...91 AGE...9 AGE UNITS...
 ACUTE KIDNEY INJURY (AKI)...122 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS)...124 ADVANCED DIRECTIVE LIMITING CARE...91 AGE...9 AGE UNITS...10 AIRBAG DEPLOYMENT...30 AIS PREDOT CODE...118 AIS SEVERITY...119
ACUTE KIDNEY INJURY (AKI)...122 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS)...124 ADVANCED DIRECTIVE LIMITING CARE...91 AGE...9 AGE UNITS...10 AIRBAG DEPLOYMENT...30 AIS PREDOT CODE...118 AIS SEVERITY...119
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
MSCC CARE PATHWAYS & CASE STUDIES. By Michael Balloch Spine CNS
 MSCC CARE PATHWAYS & CASE STUDIES By Michael Balloch Spine CNS Aims To be familiar with the routes of MSCC prentaion How the guidelines work in practice Routes of presentation Generic intervention Managing
MSCC CARE PATHWAYS & CASE STUDIES By Michael Balloch Spine CNS Aims To be familiar with the routes of MSCC prentaion How the guidelines work in practice Routes of presentation Generic intervention Managing
1. What additional information needs to be collected to properly treat this client?
 CASE 1 A 45-year-old male presents to the emergency department with a complaint of chest pain for the past two hours. 1. What additional information needs to be collected to properly treat this client?
CASE 1 A 45-year-old male presents to the emergency department with a complaint of chest pain for the past two hours. 1. What additional information needs to be collected to properly treat this client?
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Adamec I., Klepac N., Milivojević I., Radić B., Habek M. (2012) Sick sinus syndrome and orthostatic hypotension in Parkinson's disease. Acta Neurologica Belgica, 112 (3).
Središnja medicinska knjižnica Adamec I., Klepac N., Milivojević I., Radić B., Habek M. (2012) Sick sinus syndrome and orthostatic hypotension in Parkinson's disease. Acta Neurologica Belgica, 112 (3).
Chapter 11. Objectives. Objectives 01/09/2013. Baseline Vital Signs, Monitoring Devices, and History Taking
 Chapter 11 Baseline Vital Signs, Monitoring Devices, and History Taking Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights
Chapter 11 Baseline Vital Signs, Monitoring Devices, and History Taking Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights
Q1 Contact Information
 Q1 Contact Information Answered: 7 Skipped: 0 ANSWER CHOICES Hospital Name of Person Completing Survey Email RESPONSES 100.00% 7 100.00% 7 100.00% 7 # HOSPITAL DATE 1 Saint Luke's Hospital of Kansas City
Q1 Contact Information Answered: 7 Skipped: 0 ANSWER CHOICES Hospital Name of Person Completing Survey Email RESPONSES 100.00% 7 100.00% 7 100.00% 7 # HOSPITAL DATE 1 Saint Luke's Hospital of Kansas City
Pharmaceutical Care of People with Atrial Fibrillation. Course activities
 Pharmaceutical Care of People with Atrial Fibrillation Course activities Pharmaceutical Care of People with Atrial Fibrillation Course activities page 3 Case Study 1 5 Case Study 2 7 Case Study 3 9 Case
Pharmaceutical Care of People with Atrial Fibrillation Course activities Pharmaceutical Care of People with Atrial Fibrillation Course activities page 3 Case Study 1 5 Case Study 2 7 Case Study 3 9 Case
Z19.2 Cross Reference to Patient Care Maps & Clinical Care Procedures
 2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
Pulmonary Rehabilitation in Acute Spinal Cord Injury. Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university
 Pulmonary Rehabilitation in Acute Spinal Cord Injury Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university Causes of spinal cord injury Traumatic injury Motor vehicle
Pulmonary Rehabilitation in Acute Spinal Cord Injury Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university Causes of spinal cord injury Traumatic injury Motor vehicle
Management strategies for atrial fibrillation Thursday, 20 October :27
 ALTHOUGH anyone who has had to run up a flight of steps or has had a frightening experience is quite familiar with a racing heartbeat, for the more than 2 million Americans who suffer from atrial fibrillation
ALTHOUGH anyone who has had to run up a flight of steps or has had a frightening experience is quite familiar with a racing heartbeat, for the more than 2 million Americans who suffer from atrial fibrillation
Data Collection Tool. Standard Study Questions: Admission Date: Admission Time: Age: Gender:
 Data Collection Tool Standard Study Questions: Admission Date: Admission Time: Age: Gender: Specifics of Injury: Time of Injury: Mechanism of Injury Blunt vs Penetrating? Injury Severity Score? Injuries:
Data Collection Tool Standard Study Questions: Admission Date: Admission Time: Age: Gender: Specifics of Injury: Time of Injury: Mechanism of Injury Blunt vs Penetrating? Injury Severity Score? Injuries:
Operation Stroke. How to Reduce the Risk of Stroke Complications
 Operation Stroke How to Reduce the Risk of Stroke Complications Objectives Focus on Acute Stroke as an active disease Discuss the most common stroke complications Describe how first 72 hours sets the stage
Operation Stroke How to Reduce the Risk of Stroke Complications Objectives Focus on Acute Stroke as an active disease Discuss the most common stroke complications Describe how first 72 hours sets the stage
Prehospital Resuscitation for the 21 st Century Simulation Case. VF/Asystole
 Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist
 Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist Introduction. Basic Life Support (BLS). Advanced Cardiac Life Support (ACLS). Cardiovascular diseases (CVDs) are the number one cause of death
Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist Introduction. Basic Life Support (BLS). Advanced Cardiac Life Support (ACLS). Cardiovascular diseases (CVDs) are the number one cause of death
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Personal Training Program Health History Questionnaire
 Personal Training Program Health History Questionnaire PERSONAL Name: Today s Date: Address: Date of Birth: City: State: Zip Code: Home Phone: Cell Phone: Email: EMERGENCY CONTACT INFORMATION Name: Address:
Personal Training Program Health History Questionnaire PERSONAL Name: Today s Date: Address: Date of Birth: City: State: Zip Code: Home Phone: Cell Phone: Email: EMERGENCY CONTACT INFORMATION Name: Address:
SAUDI FELLOWSHIP TRAINING PROGRAM. Adult Cardiology. Final Written Examination 2019
 SAUDI FELLOWSHIP TRAINING PROGRAM Adult Cardiology Final Written Examination 2019 Objectives 1. Determine the trainee has sufficient competency related to the required specialty. 2. Determine the eligibility
SAUDI FELLOWSHIP TRAINING PROGRAM Adult Cardiology Final Written Examination 2019 Objectives 1. Determine the trainee has sufficient competency related to the required specialty. 2. Determine the eligibility
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 26 Caring for Clients with Coronary Heart Disease and Dysrhythmias Coronary Heart Disease (CHD) Leading
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 26 Caring for Clients with Coronary Heart Disease and Dysrhythmias Coronary Heart Disease (CHD) Leading
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to
 Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
42 y/o woman with unwitnessed episode of loss of consciousness and urinary incontinence
 Top Five Neurological Emergencies: When To Refer February 23, 2011 Jinny Tavee, MD Associate Professor Neurological Institute Cleveland Clinic Foundation 1 CASE 1 42 y/o woman with unwitnessed episode
Top Five Neurological Emergencies: When To Refer February 23, 2011 Jinny Tavee, MD Associate Professor Neurological Institute Cleveland Clinic Foundation 1 CASE 1 42 y/o woman with unwitnessed episode
Cardiac Pathophysiology
 Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
CVICU EXAM. Mrs. Jennings is a 71-year-old post-op CABG x5 with an IABP in her left femoral artery
 CVICU EXAM 1111 North 3rd Street Mrs. Jennings is a 71-year-old post-op CABG x5 with an IABP in her left femoral artery 1. Nursing standards for a patient on an IABP device include: a. Know results of
CVICU EXAM 1111 North 3rd Street Mrs. Jennings is a 71-year-old post-op CABG x5 with an IABP in her left femoral artery 1. Nursing standards for a patient on an IABP device include: a. Know results of
1. Spinal cord injury mild flexion-extension whiplash ~ complete transection with permanent quadriplegia
 Wk 5. Management of Clients with Neurologic Trauma 1. Spinal cord injury mild flexion-extension whiplash ~ complete transection with permanent quadriplegia most common in cervical, lower thoracic-upper
Wk 5. Management of Clients with Neurologic Trauma 1. Spinal cord injury mild flexion-extension whiplash ~ complete transection with permanent quadriplegia most common in cervical, lower thoracic-upper
Prescribe appropriate immunizations for. Prescribe childhood immunization as per. Prescribe influenza vaccinations in high-risk
 Supplemental Digital Appendix 1 46 Health Care Problems and the Corresponding 59 Practice Indicators Expected of All Physicians Entering or in Practice Infectious and parasitic diseases Avoidable complications/death
Supplemental Digital Appendix 1 46 Health Care Problems and the Corresponding 59 Practice Indicators Expected of All Physicians Entering or in Practice Infectious and parasitic diseases Avoidable complications/death
The in-hospital management of COPD-exacerbation includes three core processes:
 Appendix 1A. Process flow for in-hospital management of COPDexacerbation The in-hospital management of COPD-exacerbation includes three core processes: 1. Diagnostic assessment 2. Pharmacological management
Appendix 1A. Process flow for in-hospital management of COPDexacerbation The in-hospital management of COPD-exacerbation includes three core processes: 1. Diagnostic assessment 2. Pharmacological management
Reducing the risk of venous thrombo-embolism (VTE) in hospital and after discharge
 Reducing the risk of venous thrombo-embolism (VTE) in hospital and after discharge What is a venous thromboembolism (VTE)? This is a medical term that describes a blood clot that develops in a deep vein
Reducing the risk of venous thrombo-embolism (VTE) in hospital and after discharge What is a venous thromboembolism (VTE)? This is a medical term that describes a blood clot that develops in a deep vein
County of Santa Clara Emergency Medical Services System
 County of Santa Clara Emergency Medical Services System Policy #700-M12: Continuous Positive Airway Pressure CONTINUOUS POSITIVE AIRWAY PRESSURE Effective: February 8, 2013TBD Replaces: NewFebruary 8,
County of Santa Clara Emergency Medical Services System Policy #700-M12: Continuous Positive Airway Pressure CONTINUOUS POSITIVE AIRWAY PRESSURE Effective: February 8, 2013TBD Replaces: NewFebruary 8,
Chapter 03: Sinus Mechanisms Test Bank MULTIPLE CHOICE
 Instant download and all chapters Tesst Bank ECGs Made Easy 5th Edition Barbara J Aehlert https://testbanklab.com/download/tesst-bank-ecgs-made-easy-5th-edition-barbara-jaehlert/ Chapter 03: Sinus Mechanisms
Instant download and all chapters Tesst Bank ECGs Made Easy 5th Edition Barbara J Aehlert https://testbanklab.com/download/tesst-bank-ecgs-made-easy-5th-edition-barbara-jaehlert/ Chapter 03: Sinus Mechanisms
What are you trying to achieve? Falls Prevention, Assessment and Management Strategies. Falls can be classified into four main groups:
 What are you trying to achieve? Falls Prevention, Assessment and Management Strategies Dr Adam Darowski Community: Falls risk assessment: Falls risk is 50% per year in 80yr population and higher in those
What are you trying to achieve? Falls Prevention, Assessment and Management Strategies Dr Adam Darowski Community: Falls risk assessment: Falls risk is 50% per year in 80yr population and higher in those
Trauma resuscitation in the Elderlyfrom a physiological perspective
 6 November 2017 Trauma resuscitation in the Elderlyfrom a physiological perspective Joseph Mathew Consultant, Emergency/ 6 November 2017 2 http://www.who.int/ageing/publications/global_health.pdf 6 November
6 November 2017 Trauma resuscitation in the Elderlyfrom a physiological perspective Joseph Mathew Consultant, Emergency/ 6 November 2017 2 http://www.who.int/ageing/publications/global_health.pdf 6 November
Appendix. Potentially Preventable Complications (PPCs) identify. complications that can occur during an admission. There are 64
 Calikoglu S, Murray R, Feeney D. Hospital pay-for-performance programs in Maryland produced strong results, including reduced hospital-acquired infections. Health Aff (Millwood). 2012;31(12). Appendix
Calikoglu S, Murray R, Feeney D. Hospital pay-for-performance programs in Maryland produced strong results, including reduced hospital-acquired infections. Health Aff (Millwood). 2012;31(12). Appendix
Developing spinal cord compression care guidelines at WPH
 Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Bernie Foran, Suzanne Hodson, Jane Mason, Rebecca Mills, Jan Siddall, Rebecca Walsh, Clare
Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Bernie Foran, Suzanne Hodson, Jane Mason, Rebecca Mills, Jan Siddall, Rebecca Walsh, Clare
Appendix G Explanation/Clarification Summary
 Appendix G Explanation/Clarification Summary Summary of Changes for Recommendations Alignment of measures with VBP by fiscal year Measures and service dates were adjusted to be consistent with the FY2016
Appendix G Explanation/Clarification Summary Summary of Changes for Recommendations Alignment of measures with VBP by fiscal year Measures and service dates were adjusted to be consistent with the FY2016
Present-on-Admission (POA) Coding
 1 Present-on-Admission (POA) Coding Michael Pine, MD, MBA Michael Pine and Associates, Inc 2 POA and Coding Guidelines (1) Unless otherwise specified, a POA modifier must be assigned to each principal
1 Present-on-Admission (POA) Coding Michael Pine, MD, MBA Michael Pine and Associates, Inc 2 POA and Coding Guidelines (1) Unless otherwise specified, a POA modifier must be assigned to each principal
