This protocol aims to offer patients an option for parenteral diuretics via two routes of administration
|
|
|
- Bertina Bailey
- 5 years ago
- Views:
Transcription
1
2 Background Heart Failure (HF) is a growing problem and incurs high cost to both patient and the NHS. It is known to be associated with increasing hospitalisations costing approx. 2% of the overall NHS budget (70% of this from hospitalisation), 1 million hospital bed days and 5% of all emergency medical admissions (National Heart Failure Audit 2013; NICE CG108, 2010). The prevalence of HF is expected to continue to rise, through a combination of improved survival of patients with ischaemic heart disease and acute coronary syndromes, more efficacious therapy for heart failure and the effects of an ageing population. Heart failure is characterised by episodes of decompensation often requiring hospitalisation. A proportion of admissions are due to rapid deterioration resulting in shortness of breath and pulmonary oedema which inevitably results in hospitalisation. However, many are due to a more steady deterioration with increasing peripheral oedema. Use of intravenous (IV) and subcutaneous (SC) diuretics has been piloted in several areas of the UK and found to be effective in treating fluid overload and symptoms in HF patients and resulted in reduced hospitalisations, the largest being the British Heart Foundation (2014). The programme was led by heart failure specialist nurses (HFSNs) working within existing HF teams. This builds on existing evidence that HF patients under the care of an HFSN are five times less likely to be hospitalised compared to all HF patients. It collected evidence showing both cost-saving and improvement in quality of life in heart failure patients who were treated with parenteral diuretics in the community. The main outcomes for patients included: Reduced hospital admissions Supported early discharge Provided a better experience for patients and carers Supporting people when their condition becomes more advanced Enable people to have choice to remain at home during end of life care Purpose of Guidelines These guidelines have been developed to provide a template in the Mersey and Cheshire region to facilitate the administration of parenteral diuretics in an out of hospital setting or as a day case. The guidelines are intended to be adapted locally to reflect local services and resources available. This protocol aims to offer patients an option for parenteral diuretics via two routes of administration Section 1: Guidelines for the administration of community intravenous (IV) diuretics for patients with heart failure: Prevention of hospital admission, facilitation of early discharge and for symptomatic management of palliative patients. Section 2: Guidelines for the administration of subcutaneous (SC) diuretics to patients with heart failure who are approaching the end of life: when a person is judged by the multi professional clinical team to be approaching the end of life they may be considered for SC diuretics at home or within the Hospice setting to aid symptom control. 1
3 SECTION 1: Guidelines for the administration of community intravenous (IV) diuretics for patients with Heart Failure 1.1 Guidelines for provision of community IV diuretics in advanced heart failure Two patient groups may be suitable for community IV diuretics: Prevention of acute hospital admission To facilitate early discharge 1.2 Patient Selection 1. Suitable patients should be identified following assessment by an appropriate Heart Failure Specialist. 2. The Heart Failure team will assess the patient and ensure oral medication has been optimised. Where this has been exhausted, a referral will be made to your local service. 3. The Community Heart Failure team will assess and organise IV administration. This may involve liaising with other health care professionals including active case managers, district nurses or the palliative care team as appropriate. 4. Patients treated in the community to prevent admission to hospital would receive IV diuretics if they meet the appropriate criteria. These groups of patients are likely to have had previous episodes of decompensating heart failure and be known to the Heart Failure service. 1.3 Route of Administration Patients requiring administration of IV furosemide should have long term venous access considered. Consideration should be given to: Device availability (requires an appropriate device to deliver a one hour metered dose). Availability of frequent cannulation. Patient s condition/age/diagnosis/vascular condition. Type and duration of therapy ( including frequency of administration, volume and other concomitant IV therapy). Potential complications. Patient preference. 2
4 1.4 Patient Review and administration Inclusion criteria 1. Established, fully investigated heart failure as defined by the local Heart Failure Service. 2. Patient known to or discussed with and/or under supervision of Consultant Cardiologist. 3. Heart failure confirmed as cause of symptoms (no reversible causes identified). 4. Failure to relieve fluid overload by: a. Life-style measures including fluid restriction. b. Patients on Furosemide could be considered to be switched to Bumetanide whilst considering intravenous diuretics (Bumetanide 1mg is considered to be equivalent to Furosemide 40mg). c. After consideration of a thiazide. d. If evidence of symptomatic hypotension, consider stopping non-heart failure antihypertensives (e.g. amlodipine) avoided abrupt withdrawal of beta-blockers due to the risk of rebound tachycardia. e. Consider temporary reduction/withdrawal of ACEi/ARB/sacubitril valsartan/mra s if necessary for hypotension. 5. Fluid retention as evidence by peripheral oedema extending above the knee and /or weight gain of > 3kg above dry weight. 6. Renal stability (CrCl 30ml/l/min) and stable for the preceding 2 months, though this may not necessarily be a deterrent to use, providing the dose is carefully titrated and monitored after discussion and agreement with a Cardiologist. 7. To facilitate early discharge patients must be established, stable and responding to IV furosemide but where on-going treatment is anticipated in an ambulatory patient who wishes to be discharged from hospital. Renal function must be considered as per point Patient has sufficient and appropriate social/family /carer support. 9. Patient able to give informed consent to IV diuretic therapy at home. 10. Patient able to weigh themselves / be weighed daily. 11. Patients with pulmonary oedema or effusions can be considered for IV administration in the community only after discussion and agreement with a cardiologist/specialist team. Exclusion criteria 1. Difficult IV access (unless long term IV line in place or being considered). 2. Symptomatic hypotension (consider reduction or withdrawal of antihypertensive medication as per 4d and 4e of the inclusion criteria before excluding). 3. Insufficient carer support. 4. Pulmonary oedema with signs of uncontrolled respiratory distress and still for active HF management. If this is an expected result of on-going treatment then consideration of palliative medication to control symptoms should be considered eg opioids. 3
5 1.5 Assessment, administration and monitoring Patient assessed as per inclusion/exclusion criteria and agreed to start IV furosemide. Initial Assessment: Check BP, HR, weight and advise patient guided in/output and symptoms diary. If symptomatic hypotension reduce/stop other antihypertensives (avoid stopping beta-blockers). Check U+E s see table 2. Infusion site (if already in-situ), if evidence of systemic infection, admission will be required. If localised infection at puncture site, the GP/practitioner will review and treat or refer accordingly. Advise patient not to take oral diuretics on the day of IV administration. Commence at the equivalent dose or increase by one dose increment if clinically appropriate, no later than 4pm (see table 1). Maximum rate of IV furosemide administration is 4mg/min. Dilute if necessary in sodium chloride 0.9%. Glucose solutions are unsuitable. PO diuretics have approximately 50-60% bioavailability with wide interpatient variability vs. IV diuretics which has 100% bioavailability. Table 1: Diuretic Equivalent doses PO furosemide PO bumetanide IV furosemide Infusion time 40mg 1mg 40mg N/A 80mg 2mg 80mg N/A 120mg 3mg 120mg 30 mins 160mg 4mg 160mg 40 mins 200mg 5mg 200mg 50 mins 240mg 6mg 240mg 60 mins Ongoing monitoring HR, BP, weight, fluid balance and symptoms. If symptomatic low BP, stop or reduce other antihypertensives. Infusion site: if evidence of systemic infection, admission will be required. If localised infection at puncture site, the GP/practitioner will need to review and treat, or refer accordingly. Renal function and electrolytes see table 2. Failure to respond to IV diuretic regime Increase loop diuretic by 40mg increments of furosemide (to a maximum of 240mg Furosemide). Consider addition of thiazides orally (if not already prescribed), either daily or on alternate days. If no response i.e. improvement of symptoms and weight loss within 72 hours or locally agreed timeframe, then consideration if hospital admission may be appropriate or to discuss with the GP and/or Consultant and Palliative Care Team for consideration for end of life care measures. If the patient gains weight following 2 administrations of IV furosemide, then Heart Failure Specialist opinion should be sought promptly as admission to hospital may be required. 4
6 Monitoring and follow up after completion of IV diuretics Patients should have IV diuretics converted to an appropriate oral dose when clinically appropriate. Careful monitoring of electrolytes and weight should continue once oral diuretics are restarted (initial U+E within a week). The oral dose of diuretic should be determined with the Heart Failure team considering the IV diuretic dose given and the clinical response of the patient. In addition, the oral dose prior to IV administration and the patients renal function should be considered when determining the oral dose of diuretics to restart. Once IV diuretics are no longer required the Heart Failure Team will communicate with the patients GP to arrange ongoing follow up within a week. A transfer of care letter should be completed following completion of the IV diuretics. Table 2: Monitoring of Renal Function and Electrolytes U+E Levels Initial assessment and monitoring of renal function during IV administration Potassium < 3.5mmol/l Short course of oral potassium supplements and dietary advice. If continues to fall, consider an MRA and discuss with HF team/cardiology team/on-call team > < 6.0mmol/l Stop K+ supplements, K+ sparing diuretics and consider reducing / stopping ACEi /ARBs MRA s or sacubitril/valsartan. Consider haemolysis if other results stable and repeat. > 6.0mmol/l As above and arrange ECG, discuss with on call medical/ cardiology team and consider admission Sodium mmol/l With no symptoms of hyponatremia, consider stopping medication known to reduce sodium including MRAs/ACE inhibitors/antidepressants/ppi s. < 125mmol/l As above or if symptomatic hyponatremia, discuss with on call medical/ cardiology team and admit to hospital. Creatinine Increases by > 50% of baseline or > 300µmol/l Reduce / stop nephrotoxic medications. If creatinine continues to increase then discuss with cardiologist. 1.7 CONSENT Prior to commencing community IV diuretics, a verbal explanation and information leaflet will be provided to the patient (Appendix B) and verbal consent obtained. 1.8 LOCATION Ideally, administered in the patients home, as this is more comfortable and convenient. Where there are safety concerns or clinical need, day-case administration under the above guidelines could be provided in the hospital, contact the hospital heart failure team. 1.9 OUTCOME MEASURES At the end of each episode, audit data should be completed to assess this service see appendix C 5
7 SECTION 2: Guidelines for the administration of subcutaneous (SC) diuretics for heart failure patients approaching end of life. 2.1 Background Subcutaneous (SC) administration of furosemide is unlicensed in the UK but has been used with success (Dickman & Schneider 2016). Subcutaneous furosemide could be considered in end-stage heart failure patients requiring parenteral diuresis for symptom control within the hospice or community setting. Symptomatic management of dyspnoea using opiates and/ or benzodiazepines and non-pharmaceutical measures should be initiated as necessary alongside parenteral diuretic therapy. 2.2 Patient Selection 1. Suitable patients should be identified following assessment by an appropriate Heart Failure or Palliative Care specialist, in agreement with the patient s GP. 2. The Community Heart Failure or Palliative Care team will assess and organise subcutaneous administration via a syringe driver. This will involve liaising with other health care professionals including GP, district nurses or community matrons as appropriate. 3. Consideration should be given to the practicalities of administering a diuretic for patients whom cannot transfer to a toilet or commode and do not have a catheter in situ. Inclusion Criteria End stage heart failure patients who are unresponsive to high dose oral diuretics with poor or no venous access. End stage heart failure patients who wish to avoid hospital admission/ attendance for whom administration with IV diuretics in the community cannot be facilitated. End stage heart failure patients who decline/can not tolerate IV diuretic therapy. End stage heart failure patients in the last days of life who require ongoing administration of diuretics for symptomatic relief. Exclusion Criteria No identifiable symptomatic benefit from high dose IV or SC diuretic therapy. Severe site reaction to SC administration of furosemide. 2.3 Prescribing and Administration Furosemide ampoules have a concentration of 10mg/ml and are available in 2ml, 5ml or 25ml ampoules. Use the previous oral 24 hour requirement as a continuous SC infusion over 24 hours, as a starting dose and titrate up or down according to response. Convert the bumetanide dose to furosemide as per table 1 in section 1. Furosemide should be used as a solitary agent in a syringe driver and should not be mixed with other medication. A maximum dose of 200mg in 24 hours may be administered via a single 30ml syringe driver. Smaller doses may be administered using smaller syringe sizes where necessary. Furosemide may be used undiluted in a syringe driver. If a diluent is required, sodium chloride 0.9% should be used. The injection is alkaline and must not be mixed or diluted with glucose solutions or other acidic fluids due to risk of precipitation. Exposure to light may cause degradation and discolouration, the solution should not be used if a yellow colour is present. Furosemide 10mg/ml in polypropylene syringes is stable at 25oC in normal light for 24 hours. Ensure that the driver is not exposed to light, by covering or using a holder. Reference should be made to local instructions and guidance on the general use of syringe drivers. 6
8 2.4 Recommended infusion sites for SC administration Upper chest. Upper anterior aspect of arms. Sites are restricted in heart failure patients because of probable oedema. Sites to be avoided are bony prominences and areas where tissue is damaged, thus decreasing absorption. If possible, use a site away from areas where tattoos are present as these may mask site reactions. If there is very poor peripheral perfusion in the terminal stage, subcutaneous absorption may be limited. 2.5 Monitoring Usually, careful monitoring of renal function and U+Es is required for parenteral administration of diuretics, but this may be less important when diuretics are administered for symptom control. The heart failure or palliative care team will advise regarding the appropriate frequency of blood tests and monitoring. However, during the last few days of life it is not appropriate to monitor weight or renal function. SC administration can be associated with pain and itching at the site of injection. This may necessitate cessation of treatment. 2.6 Contraindication and Precautions For patients in the final days of life, while the prescriber must consider these contraindications and precautions, they may not necessarily be a deterrent to use, providing the dose is carefully titrated. The conditions include: Anuria Comatose or pre-comatose states associated with hepatic cirrhosis CrCl<30ml/min per 1.73m 2 Dehydration Drug-induced renal failure Hypersensitivity to sulphonamides Hypovolaemia or hyponatraemia 2.7 Definitions Palliative Palliative care is an approach that improves the quality of life of patients and their families facing life-threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual It may be done alongside treatment intended to reverse particular conditions. WHO (2002) End of Life Patients are approaching the end of life when they are likely to die within the next 12 months. This includes patients whose death is imminent (expected within a few hours or days). Leadership Alliance for Care of Dying People. One chance to get it right (2014) Care of the dying Care needed when a person is judged by the multi professional clinical team to be within a few (2-3) days of death. NICE Guidance on care of dying adults in the last days of life (2015) Verma AK, da Silva JH, Kuhl DR. Diuretic effects of subcutaneous furosemide in human volunteers: a randomized pilot study. Ann Pharmacother 2004;38: Zacharias H, Raw J, Nunn A, et al. Is there a role for subcutaneous furosemide in the community and hospice management of end-stage heart failure? Palliat Med 2011;25:
9 APPENDICES APPENDIX A Community referral form for community IV diuretics IV SERVICE REFERRAL FORM A completed prescription chart MUST be received prior to acceptance Patient Name D.O.B NHS Number Address: Telephone no: Hospital/Ward if applicable Tel No Cardiologist Heart Failure Nurse Patients GP practice Tel No Patients NOK Name Relationship Address Tel No Religion Ethnicity Diagnosis PMH Allergies Drug Name: Furosemide Dosage Frequency Infusion time Type of IV line Type of Flush required Observations U&E Is patient known to other agencies? Monitoring and other needs Date of insertion. Date of removal.. BP HR Weight NYHA Oedema score Na K Urea creatinine e-gfr Y/N Details Any other special instructions 8
10 APPENDIX B Patient information leaflet Home diuretic service - Patient Information Sheet Background People with heart failure are often admitted to hospital because of problems with fluid retention which happens because the heart is not pumping properly. This fluid can build up in the lungs which makes you feel short of breath and in your legs or abdomen which causes swelling and can be uncomfortable. Diuretics (often known as water tablets) work on the kidneys causing you to pass more urine so your body can get rid of this extra fluid. The most common diuretics are furosemide and bumetanide Sometimes the tablets, despite increasing the dose are not effective in getting rid of the extra fluid so diuretics are then given by injection to relieve this fluid overload. Intravenously: A cannula is inserted into a vein and the diuretic is given by infusion over a few hours. You may have already received this treatment on previous admissions to hospital with your heart failure condition. It is now possible to have this treatment at home. A healthcare professional will come to your home to start the infusion and take you off the infusion when it has finished. Blood tests will be done as needed. Subcutaneously: this is where a cannula is placed under the skin (can be inserted in different places such as the abdomen, arm or leg) and the diuretic is given by a small machine over 24 hours. Blood tests will be done as needed and a healthcare professional will monitor you at home. What are the advantages of having this treatment at home? The main advantage of this treatment is that it can be given to try and avoid you having to be admitted to hospital due to your heart failure or sometimes if you are in hospital you can be discharged earlier. What are the disadvantages of having this treatment at home? When you are in hospital there are doctors and nurses available 24 hours a day. At home you will not be as closely monitored and your family member or carer may need to be at home to help look after you. What are the side effects? These are the same whether diuretics are given intravenously or subcutaneously. The most common problems are: 1) Dizziness on standing due a drop in blood pressure (postural hypotension). If this does happen then the dose may need to be reduced and your other tablets altered. 2) Passing more urine. If the diuretics work you may need go to the toilet more frequently than usual. You need to be able to get to the toilet/commode easily or have a urine bottle close to hand. If you find it difficult to get out of bed then a catheter may be needed (a tube inserted into the bladder) to make it easier for you. 3) Changes in your kidney function. Diuretics can affect your kidneys so regular blood tests may be needed so that we can monitor for any changes and alter your treatment if needed. 4) Soreness or inflammation where the cannula is inserted. The site where the cannula is inserted will be checked by the nurse every time the infusion is set up and when it has finished. If any soreness develops at the site then it can be changed to a different area. If any infection has developed you may need antibiotic treatment. 5) Gout may occur with higher doses of any diuretics. 6) There is a small risk of hearing disorders and tinnitus (ringing in the ear). Although uncommon, deafness may occur which may not always be reversible. What if it does not work? If that happens then the team will discuss with you what your wishes are and what other options can be tried, they will liaise with your heart failure nurse and GP. You may need to go into hospital for more 9
11 treatment or you may decide to stay at home. You may have already completed an advance care plan stating what your preferences for care are and the team can discuss this further with you. Who provides this service? This service will be provided by the hospital at home team. This is a group of health care professionals comprising of doctors and advanced nurse practitioners who specialize in providing care in the home. What if there is a problem (harm, risks, complaints procedure)? If you suffer from any adverse effect then the treatment will be reviewed and stopped following discussion with yourself and the members of the healthcare team. The treatment can also be stopped at any time at your request. You will be given the contact numbers for the team members involved in your care and out of hours contact numbers. If you have questions or concerns regarding your treatment and care you should ask to speak to the heart failure nurse who will do their best to answer your questions You can also contact the following people for further information and advice - Local numbers would need to be included when adapted locally 10
12 APPENDIX C Audit/Outcome data Community Intravenous Diuretic Outcome Measures Patients Name : Hospital Number/ NHS Number : Treatment start date: Aim of Treatment (Please tick one box) Treatment finish date: Admission avoidance Duration of treatment: Early discharge Max dose of diuretic dosage: End of life care at home Route of administration: IV Measures Start Date Finish Date Outcome (Please tick one box) NYHA Clinic/Home visit FU Hospital admission Weight (kg) Hospice admission Oedema level Death PERIPHERAL OEDEMA SCORE None Ankle only Below knee Above knee Sacral /abdomen NYHA CLASSIFICATION Class 1 Asymptomatic, no limitation, can perform all activities without any breathlessness or fatigue despite the presence of heart disease Class 2 Mild, slight limitation of physical activity Class 3 Moderate, marked limitation of physical activity, comfortable at rest, but activity results in breathlessness and fatigue Class 4 Severe, unable to carryout physical activity without discomfort. Symptoms present even at rest 11
13 Acknowledgements These guidelines were developed by disease experts and commissioners (listed below) from across the Cheshire and Merseyside area. The development of the guidelines supported by the Cheshire and Merseyside Cardiac Network, and led by Jo Bateman, Lead Cardiology Pharmacist/Deputy Clinical Services Manager, The Countess of Chester Hospital NHS Foundation Trust. The development of these guidelines would not have been possible without the expertise and commitment of: Karen Ashton - Bridgewater Community Healthcare Carolyn Barton St Helens CCG/MMT Alison Bethel - The Countess of Chester Hospital NHS Foundation Trust/ CWP Amanda Brookes Liverpool CCG Joanne Charles Merseycare NHS Foundation Trust Karen Dickman Knowsley CVD Service, LHCH Suzanne Doolan Merseycare NHS Foundation Trust Dr Homeyra Douglas Aintree Hospital Sandra Dunne Warrington and Halton NHS Trust Julie Gaskill Bridgewater Community Healthcare Dr Clare Hammond LHCH Jessica Jones - LCH Lisa Knights - Wirral Community Foundation Trust Amanda Leyland - Bridgewater Community Healthcare Julie Norman Wirral Community Foundation Trust Diane Taylor Wirral Community Foundation Trust Nicky Trotter West Lancashire Heart Failure Nurse Nicole Williams - Wirral Community Foundation Trust Dr Julie Raj AUHFT/Woodlands Hospice Dr Rajiv Sankaranarayanan - Aintree Hospital Elcy Varughese Community Cardiac Team, Mersey Care NHS Foundation Trust 12
Guidance for the Use of Subcutaneous Furosemide by Continuous Infusion for Heart Failure in Community Settings
 Guidance for the Use of Subcutaneous Furosemide by Continuous Infusion for Heart Failure in Community Settings NHS Highland Authorised by: Planning For Fairness: Yes/No (Formerly EQIA) Distribution Consultant
Guidance for the Use of Subcutaneous Furosemide by Continuous Infusion for Heart Failure in Community Settings NHS Highland Authorised by: Planning For Fairness: Yes/No (Formerly EQIA) Distribution Consultant
Specialist Palliative Care Audit and Guidelines Group (SPAGG)
 Specialist Palliative Care Audit and Guidelines Group (SPAGG) Clinical Guideline for the Prescribing and Administration of Furosemide via continuous subcutaneous infusion (CSCI) for Heart Failure Patients
Specialist Palliative Care Audit and Guidelines Group (SPAGG) Clinical Guideline for the Prescribing and Administration of Furosemide via continuous subcutaneous infusion (CSCI) for Heart Failure Patients
Frimley Health Area Prescribing Committee
 Frimley Health Area Prescribing Committee Frimley Health NHS Foundation Trust North East Hampshire and Farnham CCG East Berkshire CCG Surrey Heath CCG Buckinghamshire CCG SHARED CARE Guideline Amber Traffic
Frimley Health Area Prescribing Committee Frimley Health NHS Foundation Trust North East Hampshire and Farnham CCG East Berkshire CCG Surrey Heath CCG Buckinghamshire CCG SHARED CARE Guideline Amber Traffic
Shared Care Guideline Metolazone for fluid management in CKD (Adults)
 Shared Care Guideline Metolazone for fluid management in CKD (Adults) It is vital for safe and appropriate patient care that there is a clear understanding of where clinical and prescribing responsibility
Shared Care Guideline Metolazone for fluid management in CKD (Adults) It is vital for safe and appropriate patient care that there is a clear understanding of where clinical and prescribing responsibility
CONTROLLED DOCUMENT. Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) Controlled Document Number: CG259
 Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor:
Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor:
REVIEW OF HEART FAILURE INDICATORS IN CHESHIRE AND MERSEYSIDE
 REVIEW OF HEART FAILURE INDICATORS IN CHESHIRE AND MERSEYSIDE DEVELOPING BASELINES TO MEASURE IMPROVEMENTS OCTOBER 2012 SAM JAMES SAM.JAMES@NORTHWEST.NHS.UK RUTH GRAINGER RUTH.GRAINGER@CISSU.NHS.UK ANNE
REVIEW OF HEART FAILURE INDICATORS IN CHESHIRE AND MERSEYSIDE DEVELOPING BASELINES TO MEASURE IMPROVEMENTS OCTOBER 2012 SAM JAMES SAM.JAMES@NORTHWEST.NHS.UK RUTH GRAINGER RUTH.GRAINGER@CISSU.NHS.UK ANNE
Community and Mental Health Services. Palliative Care. Criteria and
 Community and Mental Health Services Specialist Palliative Care Service Referral Criteria and Guidance November 2018 Specialist Palliative Care Service Referrals These guidelines cover referrals for patients
Community and Mental Health Services Specialist Palliative Care Service Referral Criteria and Guidance November 2018 Specialist Palliative Care Service Referrals These guidelines cover referrals for patients
Chronic heart failure: management of chronic heart failure in adults in primary and secondary care (partial update)
 Chronic heart failure: management of chronic heart failure in adults in primary and secondary care (partial update) NICE guideline Apendix C The algorithms Draft for consultation, January 2010 Chronic
Chronic heart failure: management of chronic heart failure in adults in primary and secondary care (partial update) NICE guideline Apendix C The algorithms Draft for consultation, January 2010 Chronic
Specialist Palliative Care Service Referral Criteria and Guidance
 Specialist Palliative Care Service Referral Criteria and Guidance Specialist Palliative Care Service Referrals These guidelines cover referrals for patients with progressive terminal illness, whether
Specialist Palliative Care Service Referral Criteria and Guidance Specialist Palliative Care Service Referrals These guidelines cover referrals for patients with progressive terminal illness, whether
Effective Shared Care Agreement for the treatment of severe motor complications in people with Parkinson Disease with apomorphine (APO-go )
 Effective Shared Care Agreement for the treatment of severe motor complications in people with Parkinson Disease with apomorphine (APO-go ) This shared care agreement outlines the ways in which the responsibilities
Effective Shared Care Agreement for the treatment of severe motor complications in people with Parkinson Disease with apomorphine (APO-go ) This shared care agreement outlines the ways in which the responsibilities
PRESCRIBING GUIDELINES FOR SYMPTOM MANAGEMENT IN THE DYING PATIENT
 PRESCRIBING GUIDELINES FOR SYMPTOM MANAGEMENT IN THE DYING PATIENT A collaboration between: St. Rocco s Hospice, Bridgewater Community Healthcare NHS Trust, NHS Warrington Clinical Commissioning Group,
PRESCRIBING GUIDELINES FOR SYMPTOM MANAGEMENT IN THE DYING PATIENT A collaboration between: St. Rocco s Hospice, Bridgewater Community Healthcare NHS Trust, NHS Warrington Clinical Commissioning Group,
Heart Failure (HF) - Primary Care Flow Charts. Pre diagnosis Symptoms or signs suggestive of HF
 Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts. Symptoms or signs suggestive of HF. Pre diagnosis. Refer to the Heart Failure Clinic at VHK for
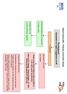 Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Specialist Palliative Care Referral for Patients
 Specialist Palliative Care Referral for Patients This guideline covers referrals for patients with progressive terminal illness, whether due to cancer or other disease. For many patients in the late stages
Specialist Palliative Care Referral for Patients This guideline covers referrals for patients with progressive terminal illness, whether due to cancer or other disease. For many patients in the late stages
Ultrafiltration. A guide for patients undergoing ultrafiltration for the treatment of heart failure
 Ultrafiltration A guide for patients undergoing ultrafiltration for the treatment of heart failure Dr Sue Ellery Consultant Cardiologist Patient Information What is heart failure? 3 What is the treatment
Ultrafiltration A guide for patients undergoing ultrafiltration for the treatment of heart failure Dr Sue Ellery Consultant Cardiologist Patient Information What is heart failure? 3 What is the treatment
Essential Shared Care Agreement: Lithium
 Ref No. E042 Essential Shared Care Agreement: Lithium Please complete the following details: Patient s name, address, date of birth Treatment (indication, dose regimen, brand name) Monitoring (proposed
Ref No. E042 Essential Shared Care Agreement: Lithium Please complete the following details: Patient s name, address, date of birth Treatment (indication, dose regimen, brand name) Monitoring (proposed
Please inform the Diabetes Nurse Specialist that this patient has been admitted within 24hrs of admission.
 Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
PACKAGE LEAFLET: INFORMATION FOR THE USER. Active substance: enoximone
 PACKAGE LEAFLET 1 PACKAGE LEAFLET: INFORMATION FOR THE USER Perfan Injection 100 mg/20 ml Concentrate for Solution for Injection Active substance: enoximone Read all of this leaflet carefully before you
PACKAGE LEAFLET 1 PACKAGE LEAFLET: INFORMATION FOR THE USER Perfan Injection 100 mg/20 ml Concentrate for Solution for Injection Active substance: enoximone Read all of this leaflet carefully before you
Patient details GP details Specialist details Name GP Name Dr Specialist Name Dr R. Horton
 Rationale for Initiation, Continuation and Discontinuation (RICaD) Sacubitril/Valsartan (Entresto) For the treatment of symptomatic heart failure with reduced ejection fraction (NICE TA388) This document
Rationale for Initiation, Continuation and Discontinuation (RICaD) Sacubitril/Valsartan (Entresto) For the treatment of symptomatic heart failure with reduced ejection fraction (NICE TA388) This document
PACKAGE LEAFLET: Information for the patient FUROSEMID Tablets - 40 mg Solution for injection - 20 mg / 2 ml (Furosemide)
 PACKAGE LEAFLET: Information for the patient FUROSEMID Tablets - 40 mg Solution for injection - 20 mg / 2 ml (Furosemide) Read this leaflet carefully before you start taking this medicine. - Keep this
PACKAGE LEAFLET: Information for the patient FUROSEMID Tablets - 40 mg Solution for injection - 20 mg / 2 ml (Furosemide) Read this leaflet carefully before you start taking this medicine. - Keep this
PALLIATIVE CARE PRESCRIBING FOR PATIENTS WHO ARE SUBSTANCE MISUSERS
 PALLIATIVE CARE PRESCRIBING FOR PATIENTS WHO ARE SUBSTANCE MISUSERS Background information Substance misusers who develop palliative care needs are likely to have psychological, social and existential
PALLIATIVE CARE PRESCRIBING FOR PATIENTS WHO ARE SUBSTANCE MISUSERS Background information Substance misusers who develop palliative care needs are likely to have psychological, social and existential
Factsheet Sacubitril valsartan (Entresto ) for chronic heart failure with reduced ejection fraction
 North Central London Joint Formulary Committee Factsheet Sacubitril valsartan (Entresto ) for chronic heart failure with reduced ejection fraction Start date: July 2016 Review date: July 2019 Document
North Central London Joint Formulary Committee Factsheet Sacubitril valsartan (Entresto ) for chronic heart failure with reduced ejection fraction Start date: July 2016 Review date: July 2019 Document
Guidelines for the Prescribing of Sacubitril / Valsartan
 Hull & East Riding Prescribing Committee Guidelines for the Prescribing of Sacubitril / Valsartan 1. BACKGROUND Sacubitril valsartan is an angiotensin receptor neprilysin inhibitor, including both a neprilysin
Hull & East Riding Prescribing Committee Guidelines for the Prescribing of Sacubitril / Valsartan 1. BACKGROUND Sacubitril valsartan is an angiotensin receptor neprilysin inhibitor, including both a neprilysin
Hypertension Clinical case scenarios for primary care
 Hypertension Clinical case scenarios for primary care Implementing NICE guidance August 2011 NICE clinical guideline 127 What this presentation covers Five clinical case scenarios, including: presentation
Hypertension Clinical case scenarios for primary care Implementing NICE guidance August 2011 NICE clinical guideline 127 What this presentation covers Five clinical case scenarios, including: presentation
NICE Chronic Heart Failure Guidelines in Adults 2018
 NICE Chronic Heart Failure Guidelines in Adults 2018 The Whys, Whats and Hows of the importance of effectively managing heart failure in Primary Care and the community. Foreword Dr Clare J Taylor, General
NICE Chronic Heart Failure Guidelines in Adults 2018 The Whys, Whats and Hows of the importance of effectively managing heart failure in Primary Care and the community. Foreword Dr Clare J Taylor, General
Care in the Last Days of Life
 Care in the Last Days of Life Introduction This guideline is an aid to clinical decision making and good practice in person-centred care for patients who are deteriorating and at risk of dying. The patient
Care in the Last Days of Life Introduction This guideline is an aid to clinical decision making and good practice in person-centred care for patients who are deteriorating and at risk of dying. The patient
Formulary and Clinical Guideline Document Pharmacy Department Medicines Management Services
 Formulary and Clinical Guideline Document Pharmacy Department Medicines Management Services VIOLENCE, AGGRESSION OR SEVERE BEHAVIOURAL DISTURBANCE Introduction During an acute episode or illness, some
Formulary and Clinical Guideline Document Pharmacy Department Medicines Management Services VIOLENCE, AGGRESSION OR SEVERE BEHAVIOURAL DISTURBANCE Introduction During an acute episode or illness, some
Renal Palliative Care Last Days of Life
 Renal Palliative Care Last Days of Life Introduction This guideline is an aid to clinical decision-making and good practice for patients with stage 4-5 chronic kidney disease (egfr
Renal Palliative Care Last Days of Life Introduction This guideline is an aid to clinical decision-making and good practice for patients with stage 4-5 chronic kidney disease (egfr
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Proposed Health Technology Appraisal. Serelaxin for treating acute decompensation of heart failure
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Health Technology Appraisal Serelaxin for treating acute decompensation of heart Draft scope (pre-referral) Draft remit/appraisal objective To
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Health Technology Appraisal Serelaxin for treating acute decompensation of heart Draft scope (pre-referral) Draft remit/appraisal objective To
How to prevent blood clots whilst in hospital and after your return home
 How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
Specialist palliative care for patients with heart failure. Dr Katie Taylor Consultant in Palliative Medicine
 Specialist palliative care for patients with heart failure Dr Katie Taylor Consultant in Palliative Medicine Objectives Identify which patients to refer to hospice Review symptom management Think about
Specialist palliative care for patients with heart failure Dr Katie Taylor Consultant in Palliative Medicine Objectives Identify which patients to refer to hospice Review symptom management Think about
Palliative care for heart failure patients. Susan Addie
 Palliative care for heart failure patients Susan Addie Treatments The most common limiting and distressing complaint is of fatigue and breathlessness. Optimal treatment strategies relieve symptoms, improves
Palliative care for heart failure patients Susan Addie Treatments The most common limiting and distressing complaint is of fatigue and breathlessness. Optimal treatment strategies relieve symptoms, improves
Pain relief after surgery. Patient Information
 Pain relief after surgery Patient Information Author ID: JT Leaflet Number: Pain 003 Version: 5 Name of Leaflet: Pain after surgery Date Produced: April 2017 Review Date: April 2019 This leaflet describes
Pain relief after surgery Patient Information Author ID: JT Leaflet Number: Pain 003 Version: 5 Name of Leaflet: Pain after surgery Date Produced: April 2017 Review Date: April 2019 This leaflet describes
9 Diabetes care. Back to contents
 Back to contents Diabetes is a major risk factor for the development of peripheral vascular disease and 349/628 (55.6%) of the patients in this study had diabetes. Hospital inpatients with diabetes are
Back to contents Diabetes is a major risk factor for the development of peripheral vascular disease and 349/628 (55.6%) of the patients in this study had diabetes. Hospital inpatients with diabetes are
Drug Name: Lithium Clinical Indications: Treatment and prophylaxis of mania; bipolar disorder; augmentation therapy in treatment resistant depression
 SHARED CARE PROTOCOL AND INFORMATION FOR GPS Drug Name: Lithium Clinical Indications: Treatment and prophylaxis of mania; bipolar disorder; augmentation therapy in treatment resistant depression Version:
SHARED CARE PROTOCOL AND INFORMATION FOR GPS Drug Name: Lithium Clinical Indications: Treatment and prophylaxis of mania; bipolar disorder; augmentation therapy in treatment resistant depression Version:
Oxford Kidney Unit A guide to conservative kidney management. Information for Healthcare Professionals
 Oxford Kidney Unit A guide to conservative kidney management Information for Healthcare Professionals What is conservative kidney management? Some people with advanced kidney disease (chronic kidney disease
Oxford Kidney Unit A guide to conservative kidney management Information for Healthcare Professionals What is conservative kidney management? Some people with advanced kidney disease (chronic kidney disease
Treating the symptoms of kidney failure
 Treating the symptoms of kidney failure Information for patients, relatives and carers Renal Department The York Hospital and Scarborough Hospital Tel: 01904 725370 For more information, please contact:
Treating the symptoms of kidney failure Information for patients, relatives and carers Renal Department The York Hospital and Scarborough Hospital Tel: 01904 725370 For more information, please contact:
CHEMOTHERAPY NETWORK GROUP POLICY FOR ADMINISTRATION OF CYTOTOXIC CHEMOTHERAPY
 CHEMOTHERAPY NETWORK GROUP POLICY FOR ADMINISTRATION OF CYTOTOXIC CHEMOTHERAPY Version 4.0 March 2016 Review date March 2018 Introduction It is the purpose of this policy to provide clear guidelines that
CHEMOTHERAPY NETWORK GROUP POLICY FOR ADMINISTRATION OF CYTOTOXIC CHEMOTHERAPY Version 4.0 March 2016 Review date March 2018 Introduction It is the purpose of this policy to provide clear guidelines that
PAIN MANAGEMENT Person established taking oral morphine or opioid naive.
 PAIN MANAGEMENT Person established taking oral morphine or opioid naive. Important; it is the responsibility of the prescriber to ensure that guidelines are followed when prescribing opioids. Every member
PAIN MANAGEMENT Person established taking oral morphine or opioid naive. Important; it is the responsibility of the prescriber to ensure that guidelines are followed when prescribing opioids. Every member
Southern Derbyshire Shared Care Pathology Guidelines. AKI guidelines for primary care
 Southern Derbyshire Shared Care Pathology Guidelines AKI guidelines for primary care Contents: Flow Diagram: Recommended response time to AKI warning stage test results for adults in primary care 2 Table
Southern Derbyshire Shared Care Pathology Guidelines AKI guidelines for primary care Contents: Flow Diagram: Recommended response time to AKI warning stage test results for adults in primary care 2 Table
ADVANCE PREPARATION OF INSULIN FOR PATIENTS TO ADMINISTER AT HOME
 STANDARD OPERATING PROCEDURE ADVANCE PREPARATION OF INSULIN FOR PATIENTS TO ADMINISTER AT HOME First Issued July 08 Issue Version Two Purpose of Issue/Description of Change Planned Review Date To promote
STANDARD OPERATING PROCEDURE ADVANCE PREPARATION OF INSULIN FOR PATIENTS TO ADMINISTER AT HOME First Issued July 08 Issue Version Two Purpose of Issue/Description of Change Planned Review Date To promote
Deactivating the shock function of an implantable cardioverter defibrillator (ICD) towards the end of life
 Deactivating the shock function of an implantable cardioverter defibrillator (ICD) towards the end of life A guide for patients and carers This leaflet is for people who have an implantable cardiac defibrillator
Deactivating the shock function of an implantable cardioverter defibrillator (ICD) towards the end of life A guide for patients and carers This leaflet is for people who have an implantable cardiac defibrillator
Heart Failure Vital steps for palliative care. Dr Karen J Hogg Glasgow Royal Infirmary
 Heart Failure Vital steps for palliative care Dr Karen J Hogg Glasgow Royal Infirmary Overview Why is heart failure a problem? Why do we need integrated cardiology and palliative care services? Cardiology
Heart Failure Vital steps for palliative care Dr Karen J Hogg Glasgow Royal Infirmary Overview Why is heart failure a problem? Why do we need integrated cardiology and palliative care services? Cardiology
APOMORPHINE (Adults) Shared Care Guidelines DRUG:
 Shared Care Guidelines DRUG: APOMORPHINE (Adults) Indication: Treatment of motor fluctuations in patients with Parkinson's disease which is not sufficiently controlled by oral anti-parkinson medication.
Shared Care Guidelines DRUG: APOMORPHINE (Adults) Indication: Treatment of motor fluctuations in patients with Parkinson's disease which is not sufficiently controlled by oral anti-parkinson medication.
Controlled Document Number: Version Number: 1. Controlled Document Sponsor: Controlled Document Lead (Author): On: July Review Date: July 2020
 Guidelines for the Use of Naloxone in Palliative Care in Adult Patients CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor: Controlled
Guidelines for the Use of Naloxone in Palliative Care in Adult Patients CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor: Controlled
GUIDELINES FOR THE MANAGEMENT OF PALLIATIVE CARE PATIENTS WITH A HISTORY OF SUBSTANCE MISUSE
 GUIDELINES FOR THE MANAGEMENT OF PALLIATIVE CARE PATIENTS WITH A HISTORY OF SUBSTANCE MISUSE 41.1 GENERAL PRINCIPLES The ICD 10 diagnostic criteria for dependency syndrome are listed in Table 41.1 below.
GUIDELINES FOR THE MANAGEMENT OF PALLIATIVE CARE PATIENTS WITH A HISTORY OF SUBSTANCE MISUSE 41.1 GENERAL PRINCIPLES The ICD 10 diagnostic criteria for dependency syndrome are listed in Table 41.1 below.
End of life prescribing guidance
 End of life prescribing guidance Introduction This guidance has been prepared to ASSIST IN DECISION MAKING for the prescribing and monitoring of medicines useful in the management of symptoms commonly
End of life prescribing guidance Introduction This guidance has been prepared to ASSIST IN DECISION MAKING for the prescribing and monitoring of medicines useful in the management of symptoms commonly
EXTRACT FOR USE BY NORTH WEST AMBULANCE SERVICE PARAMEDICS
 PRIMARY PERCUTANEOUS CORONARY INTERVENTION (PPCI) PROTOCOL EXTRACT FOR USE BY NORTH WEST AMBULANCE SERVICE PARAMEDICS ** Final Implementation** 9.00am 1 st June 2010 Liverpool Heart and Chest Hospital
PRIMARY PERCUTANEOUS CORONARY INTERVENTION (PPCI) PROTOCOL EXTRACT FOR USE BY NORTH WEST AMBULANCE SERVICE PARAMEDICS ** Final Implementation** 9.00am 1 st June 2010 Liverpool Heart and Chest Hospital
Simple removal of the kidney (simple nephrectomy): procedure-specific information
 PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical POOLE HOSPITAL NHS FOUNDATION TRUST
 Service Specification No. Service Commissioner Leads 02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical Provider Lead POOLE HOSPITAL NHS FOUNDATION TRUST Period 1 April 2013 to 31
Service Specification No. Service Commissioner Leads 02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical Provider Lead POOLE HOSPITAL NHS FOUNDATION TRUST Period 1 April 2013 to 31
Indwelling Pleural Catheter
 Indwelling Pleural Catheter Exceptional healthcare, personally delivered What is an ambulatory indwelling pleural catheter? An ambulatory indwelling pleural catheter is a specially designed small tube
Indwelling Pleural Catheter Exceptional healthcare, personally delivered What is an ambulatory indwelling pleural catheter? An ambulatory indwelling pleural catheter is a specially designed small tube
SPAGG. Coversheet for Specialist Palliative Audit and Guideline Group Agreed Documentation
 SPAGG Coversheet for Specialist Palliative Audit and Guideline Group Agreed Documentation This sheet is to accompany all documentation agreed by SPAGG. This will assist maintenance of the guidelines as
SPAGG Coversheet for Specialist Palliative Audit and Guideline Group Agreed Documentation This sheet is to accompany all documentation agreed by SPAGG. This will assist maintenance of the guidelines as
Cardiology. Heart Failure. Information
 Cardiology Heart Failure Information Heart Failure Service This leaflet is for patients who have heart failure. It explains what it is, what the symptoms are and what treatment to expect. What is Heart
Cardiology Heart Failure Information Heart Failure Service This leaflet is for patients who have heart failure. It explains what it is, what the symptoms are and what treatment to expect. What is Heart
Summary/Key Points Introduction
 Summary/Key Points Introduction Scope of Heart Failure (HF) o 6.5 million Americans 20 years of age have HF o 960,000 new cases of HF diagnosed annually o 5-year survival rate for HF is ~50% Classification
Summary/Key Points Introduction Scope of Heart Failure (HF) o 6.5 million Americans 20 years of age have HF o 960,000 new cases of HF diagnosed annually o 5-year survival rate for HF is ~50% Classification
National Horizon Scanning Centre. Irbesartan (Aprovel) for heart failure with preserved systolic function. August 2008
 Irbesartan (Aprovel) for heart failure with preserved systolic function August 2008 This technology summary is based on information available at the time of research and a limited literature search. It
Irbesartan (Aprovel) for heart failure with preserved systolic function August 2008 This technology summary is based on information available at the time of research and a limited literature search. It
Acute Kidney Injury 2
 South West Cardiovascular Strategic Clinical Network Acute Kidney Injury 2 Audit review meeting 18/07/2014 Redwood Education Centre Author: Summary of results: Dr Preetham Boddana Consultant Nephrologist
South West Cardiovascular Strategic Clinical Network Acute Kidney Injury 2 Audit review meeting 18/07/2014 Redwood Education Centre Author: Summary of results: Dr Preetham Boddana Consultant Nephrologist
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a)
 Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
keyword: diuretics Drug monitoring Monitoring diuretics in primary care 2 March 2009 best tests
 www.bpac.org.nz keyword: diuretics Drug monitoring Monitoring diuretics in primary care 2 March 2009 best tests Why do we monitor patients taking diuretics and what do we monitor? Monitoring a person on
www.bpac.org.nz keyword: diuretics Drug monitoring Monitoring diuretics in primary care 2 March 2009 best tests Why do we monitor patients taking diuretics and what do we monitor? Monitoring a person on
DRUG GUIDELINE. HYDRALAZINE (Intravenous severe hypertension in pregnancy)
 DRUG GUIDELINE HYDRALAZINE (Intravenous severe hypertension SCOPE (Area): FOR USE IN: Labour Ward, HDU, Theatre and ED EXCLUSIONS: Paediatrics (seek Paediatrician advice) and other general wards. SCOPE
DRUG GUIDELINE HYDRALAZINE (Intravenous severe hypertension SCOPE (Area): FOR USE IN: Labour Ward, HDU, Theatre and ED EXCLUSIONS: Paediatrics (seek Paediatrician advice) and other general wards. SCOPE
AN INFORMATION LEAFLET
 LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
Bronchodilator Delivery and Nebuliser Trials in Adults
 Bronchodilator Delivery and Nebuliser Trials in Adults Acute Management Favour the use of MDI (+/- Spacer) If considering nebuliser Short term treatment Approx. < 3 weeks See optimisation of inhaled bronchodilators
Bronchodilator Delivery and Nebuliser Trials in Adults Acute Management Favour the use of MDI (+/- Spacer) If considering nebuliser Short term treatment Approx. < 3 weeks See optimisation of inhaled bronchodilators
Ketorolac injection. Supportive care
 Supportive care Ketorolac injection Supportive care: specialist medicines This leaflet provides information on a medicine called ketorolac which is used to treat pain that is difficult to control. It is
Supportive care Ketorolac injection Supportive care: specialist medicines This leaflet provides information on a medicine called ketorolac which is used to treat pain that is difficult to control. It is
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care
 SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
Charles Spencer MD, FRCP Consultant Cardiologist Mid Staffs NHSFT
 Charles Spencer MD, FRCP Consultant Cardiologist Mid Staffs NHSFT Key Messages Heart Failure is Common Heart failure is complex Heart Failure is a major issue for the NHS Heart Failure has a worse prognosis
Charles Spencer MD, FRCP Consultant Cardiologist Mid Staffs NHSFT Key Messages Heart Failure is Common Heart failure is complex Heart Failure is a major issue for the NHS Heart Failure has a worse prognosis
PREOPERATIVE ANAEMIA PATHWAY
 PREOPERATIVE ANAEMIA PATHWAY Surname: Patient ID No. Forename: DOB: / / Age: NHS Number: Likes to be called: Address: Tel. No. Religion/Spirituality: Next of Kin: Name GP Name: GP Practice: Planned Operation:
PREOPERATIVE ANAEMIA PATHWAY Surname: Patient ID No. Forename: DOB: / / Age: NHS Number: Likes to be called: Address: Tel. No. Religion/Spirituality: Next of Kin: Name GP Name: GP Practice: Planned Operation:
Shared Care Guideline
 Shared Care Guideline Gentamicin for Nebulisation For the long term prophylaxis of chronic lung infections in non CF bronchiectasis Executive Summary Indication Nebulised gentamicin is indicated in patients
Shared Care Guideline Gentamicin for Nebulisation For the long term prophylaxis of chronic lung infections in non CF bronchiectasis Executive Summary Indication Nebulised gentamicin is indicated in patients
Doncaster & Bassetlaw. AKI guidelines for primary care
 Doncaster & Bassetlaw AKI guidelines for primary care Contents: FLOW DIAGRAM: MANAGEMENT OF PATIENTS WITH AKI DETECTED IN PRIMARY CARE... 2 FLOW DIAGRAM: MANAGEMENT OF HYPERKALAEMIA.... 3 FLOW DIAGRAM:
Doncaster & Bassetlaw AKI guidelines for primary care Contents: FLOW DIAGRAM: MANAGEMENT OF PATIENTS WITH AKI DETECTED IN PRIMARY CARE... 2 FLOW DIAGRAM: MANAGEMENT OF HYPERKALAEMIA.... 3 FLOW DIAGRAM:
Prescribing Framework for Rivastigmine in the Treatment and Management of Dementia
 Hull & East Riding Prescribing Committee Prescribing Framework for Rivastigmine in the Treatment and Management of Dementia Patients Name:.. NHS Number: Patients Address:... (Use addressograph sticker)
Hull & East Riding Prescribing Committee Prescribing Framework for Rivastigmine in the Treatment and Management of Dementia Patients Name:.. NHS Number: Patients Address:... (Use addressograph sticker)
Red blood cell transfusion
 Red blood cell transfusion This leaflet explains more about red blood cell transfusion, including the benefits, risks and any alternatives and what you can expect when you come to hospital. If you have
Red blood cell transfusion This leaflet explains more about red blood cell transfusion, including the benefits, risks and any alternatives and what you can expect when you come to hospital. If you have
GOVERNING BODY REPORT
 GOVERNING BODY REPORT DATE OF MEETING: 20th September 2012 TITLE OF REPORT: KEY MESSAGES: NHS West Cheshire Clinical Commissioning Group has identified heart disease as one of its six strategic clinical
GOVERNING BODY REPORT DATE OF MEETING: 20th September 2012 TITLE OF REPORT: KEY MESSAGES: NHS West Cheshire Clinical Commissioning Group has identified heart disease as one of its six strategic clinical
PATIENT GROUP DIRECTION (PGD)
 PATIENT GROUP DIRECTION (PGD) SUPPLY OF NALOXONE HYDROCHLORIDE INJECTION BY REGISTERED NURSES TO CLIENTS BEING RELEASED FROM HMP FORD Version Number: 01HMP Patient Group Direction originally drawn up by:
PATIENT GROUP DIRECTION (PGD) SUPPLY OF NALOXONE HYDROCHLORIDE INJECTION BY REGISTERED NURSES TO CLIENTS BEING RELEASED FROM HMP FORD Version Number: 01HMP Patient Group Direction originally drawn up by:
NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT
 NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT CONTENTS PATIENTS ADMITTED WITH HEART FAILURE...4 Demographics... 4 Trends in Symptoms... 4 Causes and Comorbidities
NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT CONTENTS PATIENTS ADMITTED WITH HEART FAILURE...4 Demographics... 4 Trends in Symptoms... 4 Causes and Comorbidities
A Clinical Guideline for the use of Intravenous Aminophylline in Acute Severe Asthma in Children
 For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Assessed and approved by the:
For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Assessed and approved by the:
Palliative Care Out-of-hours. A resource pack for West Dorset. Contents:
 Palliative Care Out-of-hours. A resource pack for West Dorset Contents: Section 1 Supply of drugs DCH Pharmacy hours and arrangements How to contact a community pharmacist out of hours Palliative care
Palliative Care Out-of-hours. A resource pack for West Dorset Contents: Section 1 Supply of drugs DCH Pharmacy hours and arrangements How to contact a community pharmacist out of hours Palliative care
PAIN AND SYMPTOM MANAGEMENT GUIDANCE IN THE LAST DAYS OF LIFE
 PAIN AND SYMPTOM MANAGEMENT GUIDANCE IN THE LAST DAYS OF LIFE Reference: DCM029 Version: 1.1 This version issued: 07/06/18 Result of last review: Minor changes Date approved by owner (if applicable): N/A
PAIN AND SYMPTOM MANAGEMENT GUIDANCE IN THE LAST DAYS OF LIFE Reference: DCM029 Version: 1.1 This version issued: 07/06/18 Result of last review: Minor changes Date approved by owner (if applicable): N/A
Sirolimus 1mg/1ml oral solution
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Sirolimus 1mg/1ml oral solution You should read this information sheet in conjunction with any patient information
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Sirolimus 1mg/1ml oral solution You should read this information sheet in conjunction with any patient information
LIVING WITH HEART FAILURE
 1 PERSONAL RECORD An everyday guide to LIVING WITH HEART FAILURE Personal record HOW TO USE THIS RECORD This personal record accompanies our publication An everyday guide to living with heart failure.
1 PERSONAL RECORD An everyday guide to LIVING WITH HEART FAILURE Personal record HOW TO USE THIS RECORD This personal record accompanies our publication An everyday guide to living with heart failure.
Prescribing Framework for Galantamine in the Treatment and Management of Dementia
 Hull & East Riding Prescribing Committee Prescribing Framework for Galantamine in the Treatment and Management of Dementia Patients Name:.. NHS Number: Patients Address:... (Use addressograph sticker)
Hull & East Riding Prescribing Committee Prescribing Framework for Galantamine in the Treatment and Management of Dementia Patients Name:.. NHS Number: Patients Address:... (Use addressograph sticker)
Medicines Protocol RECTAL DIAZEPAM
 Medicines Protocol RECTAL DIAZEPAM RECTAL DIAZEPAM v2.0 1/6 Protocol Details Version 2.0 Legal category Staff grades POM Registered Paramedic Registered Nurse Specialist Paramedic (Urgent and Emergency
Medicines Protocol RECTAL DIAZEPAM RECTAL DIAZEPAM v2.0 1/6 Protocol Details Version 2.0 Legal category Staff grades POM Registered Paramedic Registered Nurse Specialist Paramedic (Urgent and Emergency
SHARED CARE GUIDELINE FOR THE MANAGEMENT OF PATIENTS ON NALTREXONE FOR ALCOHOL DEPENDENCE INDICATION
 SHARED CARE GUIDELINE FOR THE MANAGEMENT OF PATIENTS ON NALTREXONE FOR ALCOHOL DEPENDENCE INDICATION Naltrexone is used as part of a comprehensive programme of treatment against alcoholism to reduce the
SHARED CARE GUIDELINE FOR THE MANAGEMENT OF PATIENTS ON NALTREXONE FOR ALCOHOL DEPENDENCE INDICATION Naltrexone is used as part of a comprehensive programme of treatment against alcoholism to reduce the
Patient Group Direction for SALBUTAMOL INHALER (Version 02) Valid From 1 October September 2019
 Version Control This PGD has been agreed by the following organisations FCMS PDS Medical Doncaster CCG Lancashire CCGs including East Lancashire, Fylde and Wyre and North Lancashire CCGs Change history
Version Control This PGD has been agreed by the following organisations FCMS PDS Medical Doncaster CCG Lancashire CCGs including East Lancashire, Fylde and Wyre and North Lancashire CCGs Change history
Clinical guideline for the introduction of Sacubitril Valsartan in primary and secondary care in Cornwall
 Clinical guideline for the introduction of Sacubitril Valsartan in primary and secondary care in Cornwall Page 1 of 15 Summary Patient clinically assessed and reviewed by a Consultant Cardiologist, Cardiology
Clinical guideline for the introduction of Sacubitril Valsartan in primary and secondary care in Cornwall Page 1 of 15 Summary Patient clinically assessed and reviewed by a Consultant Cardiologist, Cardiology
Clinical. High Dose Antipsychotic Prescribing Procedures. Document Control Summary. Contents
 Clinical High Dose Antipsychotic Prescribing Procedures Document Control Summary Status: Version: Author/Owner/Title: Approved by: Ratified: Related Trust Strategy and/or Strategic Aims Implementation
Clinical High Dose Antipsychotic Prescribing Procedures Document Control Summary Status: Version: Author/Owner/Title: Approved by: Ratified: Related Trust Strategy and/or Strategic Aims Implementation
PACKAGE LEAFLET: INFORMATION FOR THE USER. Glucose Intravenous Infusion BP 10% w/v solution for infusion Glucose (as glucose monohydrate)
 PACKAGE LEAFLET: INFORMATION FOR THE USER Glucose Intravenous Infusion BP 10% w/v solution for infusion Glucose (as glucose monohydrate) Read all of this leaflet carefully before you start using this medicine
PACKAGE LEAFLET: INFORMATION FOR THE USER Glucose Intravenous Infusion BP 10% w/v solution for infusion Glucose (as glucose monohydrate) Read all of this leaflet carefully before you start using this medicine
Acute Kidney Injury. Patient Information Leaflet
 Acute Kidney Injury Patient Information Leaflet What is Acute Kidney Injury (AKI)? Acute Kidney injury is a rapid fall in kidney function in a person who has become unwell. It can happen over hours or
Acute Kidney Injury Patient Information Leaflet What is Acute Kidney Injury (AKI)? Acute Kidney injury is a rapid fall in kidney function in a person who has become unwell. It can happen over hours or
Shared Care Agreement Apomorphine For use in Parkinson s Disease
 Shared Care Agreement Apomorphine For use in Parkinson s Disease This shared care agreement outlines suggested ways in which the prescribing responsibilities can be shared between the specialist and GP.
Shared Care Agreement Apomorphine For use in Parkinson s Disease This shared care agreement outlines suggested ways in which the prescribing responsibilities can be shared between the specialist and GP.
Diabetes in the Last Hours and Days of Life. November 2016
 Diabetes in the Last Hours and Days of Life November 2016 Guideline Development Group Members Dr Julie Raj Consultant in Palliative Medicine, Aintree University Hospital NHS Foundation Trust Mrs Sue Howarth
Diabetes in the Last Hours and Days of Life November 2016 Guideline Development Group Members Dr Julie Raj Consultant in Palliative Medicine, Aintree University Hospital NHS Foundation Trust Mrs Sue Howarth
Acute Kidney Injury (AKI) Undergraduate nurse education
 Acute Kidney Injury (AKI) Undergraduate nurse education Year Three Developed Summer 2017 Objectives Understand Acute Kidney Injury and its relevance to patient care. Brief revision of the Anatomy and physiology
Acute Kidney Injury (AKI) Undergraduate nurse education Year Three Developed Summer 2017 Objectives Understand Acute Kidney Injury and its relevance to patient care. Brief revision of the Anatomy and physiology
Percutaneous removal of kidney stone(s): procedurespecific information
 PATIENT INFORMATION Percutaneous removal of kidney stone(s): procedurespecific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British
PATIENT INFORMATION Percutaneous removal of kidney stone(s): procedurespecific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British
London Strategic Clinical Networks. My AKI. Guidance for patients with, or recovering from, acute kidney injury
 London Strategic Clinical Networks My AKI Guidance for patients with, or recovering from, acute kidney injury Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net
London Strategic Clinical Networks My AKI Guidance for patients with, or recovering from, acute kidney injury Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net
Western Locality Shared care Information ~ Penicillamine, Rheumatology April 2013
 Western Locality Shared care Information ~ Penicillamine, Rheumatology April 2013 Penicillamine Treatment of: Rheumatoid arthritis Specialist: Please complete the Shared Care letter sending a request to
Western Locality Shared care Information ~ Penicillamine, Rheumatology April 2013 Penicillamine Treatment of: Rheumatoid arthritis Specialist: Please complete the Shared Care letter sending a request to
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life
 MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life The following pages are guidelines for the management of common symptoms for a person thought to be
MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life The following pages are guidelines for the management of common symptoms for a person thought to be
GUIDELINES FOR CONVERSION FROM A STRONG OPIOID TO METHADONE
 GUIDELINES FOR CONVERSION FROM A STRONG OPIOID TO METHADONE GENERAL PRINCIPLES Methadone may be used as a strong opioid alternative when severe cancer-related pain responds poorly to other opioids, or
GUIDELINES FOR CONVERSION FROM A STRONG OPIOID TO METHADONE GENERAL PRINCIPLES Methadone may be used as a strong opioid alternative when severe cancer-related pain responds poorly to other opioids, or
Having an Anaesthetic Your Questions Answered
 PATIENT INFORMATION Having an Anaesthetic Your Questions Answered This leaflet explains what you can expect when having an anaesthetic for a planned operation. What is anaesthesia? Anaesthesia means loss
PATIENT INFORMATION Having an Anaesthetic Your Questions Answered This leaflet explains what you can expect when having an anaesthetic for a planned operation. What is anaesthesia? Anaesthesia means loss
Atrial fibrillation. Understanding NICE guidance
 Understanding NICE guidance Information for people who use NHS services Atrial fibrillation NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Understanding NICE guidance Information for people who use NHS services Atrial fibrillation NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Kidney Patients with Chronic Kidney Disease
 Cheshire and Merseyside Kidney Care Services Renal Replacement Therapy Options for Kidney Patients with Chronic Kidney Disease Stage 5 Renal Replacement Therapy Options for Kidney Patients with Chronic
Cheshire and Merseyside Kidney Care Services Renal Replacement Therapy Options for Kidney Patients with Chronic Kidney Disease Stage 5 Renal Replacement Therapy Options for Kidney Patients with Chronic
Cardiac Catheter Labs Intravenous Drug Therapy Guide
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Cardiac Catheter Lab IV Medicines Guideline Helen Buxton ( Senior Cath Lab
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Cardiac Catheter Lab IV Medicines Guideline Helen Buxton ( Senior Cath Lab
