Second Generation Antiarrhythmic Agents: Have We Reached Antiarrhythmic Nirvana?
|
|
|
- Kristina Simpson
- 5 years ago
- Views:
Transcription
1 JACC Vol. 9. NO S Second Generation Antiarrhythmic Agents: Have We Reached Antiarrhythmic Nirvana? LEONARD N. HOROWITZ, MD, FACC, JOEL MORGANROTH, MD, FACC Philadelphia, Pennsylvania During the first half of the 20th century, antiarrhythmic therapy was principally directed toward supraventricular arrhythmia; only relatively recently has therapy of ventricular arrhythmias been emphasized. In fact, significant pharmacologic treatment of ventricular arrhythmias was minimal until routine use of quinidine and procainamide began in the 1950s (1,2). The first generation oral antiarrhythmic drugs, quinidine, procainamide and disopyramide, previously constituted the principal antiarrhythmic agents for longterm treatment of ventricular arrhythmias in the United States. Compared with modem regulatory standards, the data on which the use of these drugs was based were modest at best and rudimentary at worst. However, because good clinical judgment compensates for a multitude of deficiencies, we have been able to provide effective antiarrhythmic therapy to many patients with this rather limited pharmacopoeia. Two beta-adrenergic blocking agents, propranolol and acebutolol, have been approved for the treatment of ventricular arrhythmias by the Food and Drug Administration. Unlike the first generation of antiarrhythmic drugs and the recently released agents which effect their antiarrhythmic action by direct alteration of electrophysiologic properties, the beta-blockers presumably act indirectly by blunting sympathetic tone. Although they are effective, either alone or as an adjunct to classic antiarrhythmic therapy, they will not be considered in this discussion of membrane-active antiarrhythmic agents. In slightly more than 12 months, four new antiarrhythmic drugs, tocainide, mexiletine, ftecainide and amiodarone, have been released for the treatment of ventricular arrhythmias. A fifth drug, encainide, is likely to be released within a year. These drugs are "second generation," not only because their electrophysiologic properties are new and in * Editorials published in Journal ofthe American College ofcardiology reflect the views of the authors and do not necessarily represent the views of JACC or the American College of Cardiology. From the Division of Clinical Cardiac Electrophysiology and Sudden Death Prevention Program of the Likoff Cardiovascular Institute, Hahnemann University and Hospital, Philadelphia, Pennsylvania. Manuscript received March 4, 1986; revised manuscript received July 1,1986, accepted July 21,1986. Address for reprints: Leonard N. Horowitz, MD. Philadelphia Heart Institute, Presbyterian-University of Pennsylvania Medical Center, 39th and Market Streets, Philadelphia, Pennsylvania by tbe American College of Cardiology some cases novel, but because their preapproval evaluations followed a more rigorous and circumspect path. More information is available to us so we can decide when and how these agents should be employed. Like all antiarrhythmic drugs of the first generation, the new agents have the potential to provoke or worsen ventricular arrhythmias. These proarrhythmic effects vary in incidence and may present a major problem in certain patient groups such as those with sustained ventricular tachyarrhythrnias, reduced left ventricular function and conduction disturbances. In common with other antiarrhythmic drugs, the second generation drugs have not been shown to prevent sudden death in patients with ventricular ectopic activity. These factors, along with efficacy and potential toxicity, must be considered in selecting antiarrhythmic regimens for an individual patient. Tocainide Efficacy. Tocainide hydrochloride, a class IB agent, has electrophysiologic and antiarrhythmic characteristics similar to those of lidocaine, of which it is a congener; however, it can be prescribed for oral administration. Tocainide is indicated for the "suppression of symptomatic ventricular arrhythmias, including frequent premature ventricular contractions, unifocal or multifocal, couplets and ventricular tachycardia" (3). It has been reported to significantly reduce (decrease by at least 70% in frequency) ventricular premature complexes in 20 to 50% of patients (4). When compared with quinidine or procainamide, tocainide has been less effective in suppressing ventricular premature complexes (5). In patients with malignant ventricular arrhythmias (ventricular tachycardia with hemodynamic compromise or ventricular fibrillation) tocainide has been shown to be effective in 10 to 15% of patients; however, notable exceptions with higher efficacy rates have been reported (6). These and other data provide support for the indications for tocainide. Adverse effects. Tocainide commonly produces minor, transient, gastrointestinal and neurologic adverse effects. These side effects have been reported in 30 to 40% of patients. Intolerable adverse reactions may require discontinuation of tocainide therapy in 10 to 20% of patients. The /87/$3.50
2 460 HOROWITZ AND MORGANROTH lacc Vol. 9. No.2 manufacturer has warned that blood dyscrasias, which are possibly drug related, have been reported in patients receiving tocainide, and frequent monitoring of hematologic variables is recommended. Pulmonary fibrosis has also been reported. Tocainide has produced minimal negative inotropic effects and most patients, even those with evidence of significant left ventricular dysfunction, can tolerate tocain ide without worsening of congestive heart failure. Moreover, tocainide can be administered with other cardioactive medications without significant interactions. Mexiletine Efficacy. Mexiletine hydrochloride, a class IB agent, is structurally similarto lidocaine and tocainide and has similar antiarrhythmic potency. Mexiletine is indicated for "suppression of symptomatic ventricular arrhythmias including premature ventricular contractions, unifocal or multifocal, couplets and ventricular tachycardia" (7). Mexiletine has been effective in reducing the frequency of ventricular premature complexes in 30 to 50% of patients (6-8). Comparisons with procainamide, quinidine and disopyramide have shown no significant difference in efficacy. In patients with more serious ventricular arrhythmias evaluated by noninvasive methods, the efficacy of mexiletine has been reported to be good (8). However, in patients with sustained ventricular tachycardia evaluated by electrophysiologic testing, mexiletine when used alone has generally been reported to have minimal efficacy (9). In this group of patients, however, the combination of mexiletine with procainamide or quinidine has been shown to be very effective (10). Adverse effects. Mexiletine commonly produces gastrointestinal and neurologic adverse reactions. Upper gastrointestinal distress has been reported in more than 40% of patients and light-headedness, tremor and coordination difficulties have been reported in 10 to 20% of patients (7). The manufacturer has noted that liver injury and elevation of certain hepatic enzymes have been noted in a small number of patients treated with mexiletine and may be related to it. Appropriate clinical follow-up is indicated. Flecainide F1ecainide acetate, a class IC agent, markedly depresses the sodium channel and is the first released agent of a group of agents with potent negative dromotropic effects which have been classified as IC agents. Efficacy. Flecainide is indicated for the "treatment of documented life-threatening ventricular arrhythmias, such as sustained ventricular tachycardia" and "symptomatic nonsustained ventricular tachycardia and frequent premature ventricular complexes" (11). More than 80% of patients will achieve greater than 75% suppression of ventricular premature complexes, or elimination of ventricular tachycardia, or both, during flecainide therapy, and the median reduction in ventricular premature complexes for all patients approximates 95% (12). F1ecainide has been shown to be more effective than quinidine in suppressing ventricularpremature complexes (12). In patients with refractory lifethreatening ventricular arrhythmias, it has been effective in 25% of patients evaluated by noninvasive or invasive techniques, or both (13,14). Although flecainide has not been directly compared with first generation antiarrhythmic drugs in this latter group of patients, in most of the patients treated with flecainide previous therapy with first generation agents had been unsuccessful. Adverse effects. The most common adverse effects noted with patients treated with flecainide have been central nervous system disturbances. These occur in 10 to 20% of patients. Discontinuation of treatment because of these effects has been reported in 5 to 10% of patients (11,15). The manufacturer has warned that flecainide can cause new or worsened arrhythmias. This proarrhythmic effect has been reported in 7O/c of the patients treated with flecainide and its frequency appears to be related to the dose, the method of dose titration and the underlying cardiac disease. The incidence of proarrhythrnic effect is highest among patients who have sustained ventricular tachycardia or whose dose is rapidly titrated upward, or both. When high initial doses and rapid upward titration were used in early studies of patients with sustained ventricular tachycardia, a proarrhythmic event occurred in 26% of patients, and in 10% of the patients treated, a proarrhythmic event resulted in death. With the current dosing recommendations, however, the incidence of proarrhythmic events resulting in death has decreased to 0.5%. Thus, it is extremely important to follow the recommended dosing schedule. In addition. flecainide has a negative inotropic effect and can cause or worsen congestive heart failure. This effect is particularly noted in patients with cardiomyopathy or preexisting severe heart failure. Because flecainide has potent depressant effects on cardiac conduction, patients with sinoatrial node and atrioventricular (AV) conduction disturbances must be carefully observed for the development of worsening of these abnormalities. Encainide Encainide hydrochloride also markedly slows intracardiac conduction and is classified as a class IC antiarrhythmic agent. Its antiarrhythmic effects are similar to those of flecainide. Encainide was recommended for approval by the Cardio-renal Advisory Committee in July 1985 and is in the latter stages of the Food and Drug Administration's review process. It will probably be released within a year. Efficacy. Encainide will be indicated for the treatment of ventricular arrhythmias similar to those for which flecainide is indicated. The efficacy of encainide in suppressing
3 JACC Vol. 9. NO.2 HOROWITZ AND MORGANROTH 461 both ventricular premature complexes and malignant ventricular arrhythmias is similar to that of flecainide. It produces adequate suppression of ventricular premature complexes in approximately 80% of patients and complete abolition in 30 to 40% of patients (16,17). Encainide is more effective than quinidine in suppressing ventricular premature complexes (18). When evaluated by electrophysiologic techniques. it has been reported to be effective in approximately 25% of patients with malignant ventricular arrhythmias (19). Adverse effects. The adverse effects produced by encainide during long-term oral use are predominantly neurologic. Blurred vision, dizziness and ataxia are reported in 10 to 20% of patients. Encainide will probably carry a proarrhythmia warning similar to that in the flecainide package insert. A proarrhythmic effect has been reported in 5 to 10% of patients receiving encainide, most commonly in patients with left ventricular dysfunction and malignant ventricular arrhythmia (20,21). This proarrhythmic effect may also be dose related (22). Like flecainide, encainide may depress sinus node function and AV conduction particularly in patients with preexisting disturbances. It is not expected that encainide will carry a warning relative to heart failure because minimal hemodynamic effects have been reported and heart failure uncommonly complicates the use of encainide even in patients with preexisting heart failure (23). Amiodarone Amiodarone, a benzofuran derivative, was initially introduced as a coronary vasodilator for treatment of angina pectoris but was found to have antiarrhythmic properties. Amiodarone increases the action potential duration and prolongs repolarization. In addition, it is a noncompetitive adrenergic antagonist. Efficacy. Because of its potentially life-threatening side effects and the substantial management difficulties associated with its use, amiodarone is indicated for the treatment of "documented, life-threatening recurrent ventricular arrhythmias [recurrent ventricular fibrillation and recurrent hemodynamically unstable ventricular tachycardia]. when these have not responded to documented adequate doses of other adequate available antiarrhythmics or when alternative agents could not be tolerated" (24). Because of its substantial toxicity, amiodarone should not be used for the treatment of ventricular premature complexes, even when these occur in repetitive forms. The efficacy of amiodarone in the treatment of sustained life-threatening ventricular arrhythmiasishighly variable, ranging from 30t080%(25-28). Controversy continues regarding the utility of electrophysiologic testing in evaluating amiodarone. Considerable recent evidence suggests that it may be useful in identifying patients who will not have recurrent arrhythmia and those patients who will have nonlife-threatening recurrent arrhythmia (27,28). Toxicity and adverse effects. Because its use is accompanied by substantial toxicity, amiodarone is indicated only for use in patients with life-threatening ventricular arrhythmias. Amiodarone has several potentially lethal toxicities, the most notable of which is pulmonary toxicity. Although the incidence of this adverse effect is debated, rates between 5 and 15% have been routinely reported and death may occur from this complication in as many as 10% of those with the adverse effect. It may cause a worsening of congestive heart failure and arrhythmias. Moreover, amiodarone poses major management problems because of its unusual pharmacokinetics and other less severe adverse effects. Amiodarone has been reported to cause hepatic injury, corneal microdeposits and uncommonly, impairment of vision, cutaneous photosensitivity, thyroid abnormalities and a number of drug interactions. It has significant interactions with other antiarrhythmic drugs. digitalis and warfarin anticoagulants. Antiarrhythmic Therapy in 1986 Clinical approach to antiarrhythmic therapy. Have we, therefore, entered antiarrhythmic nirvana? Can we and should we abandon the use of first generation antiarrhythmic agents because newer drugs are now available? What is the role of these new agents and where do they fit in the therapeutic algorithm for patients with ventricular arrhythmia? Clearly we have not attained perfection in antiarrhythmic therapy. All of the second generation agents have limitations and thus. none is the perfect antiarrhythmic agent. Such an "ideal" antiarrhythmic agent would have minimal adverse effects and be effective in the majority of patients, particularly those with malignant ventricular arrhythmias. Its metabolism and pharmacokinetics would be simple and unvarying in different patient populations. It would be nice if it were effective in treating supraventricular arrhythmias as well! We do not have and probably are not likely to have such an agent. The advantage of having twice as many agents available is that there is a greater variety from which to match an individual patient with a specific regimen and there are more choices from which to select an effective regimen that is well tolerated by the patient. It has recently been emphasized (29) that the selection of an antiarrhythmic regimen is more commonly based on consideration of toxicity profiles rather than on the relative efficacies of the various agents. It is now encumbent on us to develop rational and clinically useful approaches to the use of this larger number of antiarrhythmic agents (Table I). The use of first generation antiarrhythmic drugs should not be abandoned. Quinidine and procainarnide, in particular, are useful in the treatment of supraventricular arrhythmias. and all of these agents are useful in the treatment of
4 462 HOROWITZ AND MORGANROTH lacc Vol. 9. No.2 Table 1. Characteristics of Current Antiarrhythmic Agents* Efficacy Effect on Incidence of Proarrhythmia (%)t Incidence of Significant Drug VPCs MVA LV Function VPCs MVA Noncardiac Side Effects (%) Quinidine Procainamide t Disopyramide t t t Tocainide Mexiletine Flecainide t t <I Encainide <I Amiodarone NA +++ t NA 5 75 *This is a highly subjective summary of pertinent features of our current antiarrhythmic armamentarium. In the absence of controlled comparative trials. such estimates are based on personal experience and a review of available data. Efficacy and left ventricular function scales are 0 to 4. t lncludes an estimate of serious and potentially life-threatening proarrhythmic effects. LV = left ventricular; MVA = malignant ventricular arrhythmia; NA = not applicable; VPC = ventricular premature complexes. ventricular arrhythmias, both ventricular premature complexes and malignant or life-threatening ventricular arrhythmias. The addition of the new agents allows better tailoring of antiarrhythmic regimens for individual patients. Patients with benign ventricular premature complexes or potentially lethal ventricular arrhythmias (30). In these patients antiarrhythmic regimens should be selected after consideration of the goals of antiarrhythmic therapy, efficacy and toxicity of specific agents in this patient group and the individual patient's previous drug history and clinical status. In patients with few complicating factors, flecainide or encainide would be appropriate as a first choice because of their higher efficacy and lower incidence of toxicity. In patients with conduction disturbances, quinidine or procainamide might be betterinitial choices. In patients with severely depressed left ventricular function or severe congestive heart failure, the choice of an agent that has minimal or only modest negative inotropic potential, such as encainide, tocainide, mexiletine or quinidine, would be appropriate. Subsequent choices should be based on the patient's response, particularly side effects, to previously evaluated drugs. Thus, for patients with ventricular premature complexes, therapy should be guided by a consideration of the adverse effects of the available agents and the appropriate selection of initial therapy can be made by a knowledge of the patient's clinical status and the effects of the antiarrhythmic drugs. Patients with life-threatening or malignant ventricular arrhythmias. In these patients the complicating cardiovascular factors are usually many. Most of these patients have left ventricular dysfunction and conduction disturbances and the use of concomitant medications is common. Because of the severity of the arrhythmia, no argument exists regarding whether these patients should be treated. Whether they are evaluated by noninvasive or invasive techniques, it is critical that the antiarrhythmic regimens in such patients be quantitatively evaluated and the patients be followed closely. In this group of patients, the reported efficacy of class IA (quinidine-like) agents and class IC (flecainide-like) agents is similar; however, class IB agents (mexiletine or tocainide) are less often effective alone. The selection of which agent is the first choice for treatment requires weighing the risk and benefit of a specific regimen in an individual patient. The key is individualization of therapy. Quinidine or procainamide is effective in approximately 25% of these patients but each has frequent noncardiac toxic effects that may cause discontinuation of treatment in as many as onethird of patients. Flecainide and encainide, similarly, are effective in 25% of patients in this group but have a greater proarrhythmic potential, and flecainide can worsen left ventricular function. In patients with left ventriculardysfunction and congestive heart failure or severe conduction disturbance, quinidine and procainamide should be evaluated initially. Adjunctive use of mexiletine or tocainide augments efficacy with these agents and should also be considered. Even in patients with malignant ventricular arrhythmias without complicating heart failure or conduction abnormalities, ftecainide and encainide should not be considered initially because of their probably higher proarrhythmic potential. Particularly in patients with severe heart failure, encainide should be used before ftecainide. Clinical judgment is required in making the initial choice in therapy for these highest risk patients, and one must weigh the clinical toxicity of the quinidine-like and lidocaine-like drugs against the probably higher potential of proarrhythmia of encainide and ftecainide and heart failure of ftecainide. The approach in using this larger array of drugs should not be hierarchical. The choice of ftecainide for initial therapy does not mean that a first generation agent will not be effective if ftecainide proves unsuitable and vice versa. Before initiating amiodarone therapy in patients with ma-
5 lacc Vol. 9, No.2 February 1987:459~63 HOROWITZ ANDMORGANROTH 463 lignant ventricular arrhythmias, other less commonly used drugs or beta-adrenergic blockers can be tried. Treatment with amiodarone, alone or in combination with first generation or any of the newer agents, should always follow thorough evaluation of all other appropriate pharmacologic alternatives. It is also important to remember that in many patients alternative therapy with electrical devices or surgery is available and rational in patients in whom pharmacologic therapy is ineffective or not well tolerated. Although we have not reached a state of perfection in the treatment of ventricular arrhythmias, the advent of second generation antiarrhythmic drugs provides a significant advance in our ability to treat these disorders. Although much more remains to be learned about the mechanisms and treatment of ventricular arrhythmias, a significant advance in our ability to treat them has been made. References 1. Sokolow M. The present status of therapy of the cardiac arrhythmias with quinidine, Am Heart ;42: Mark LC, Kayden HJ, Steele JM, et al. The physiological disposition and cardiac effects of procaineamide. J Pharmacol Exp Ther 1951;102: Tonocard package insert, Merck, Sharp & Dohrne, West Point, PA. 4. Kutalek, SP, Morganroth 1, Horowitz LN. Tocainide: a new oral antiarrhythmic agent. Ann Intern Med 1985;103: Morganroth 1, Oshrain C, Steele PP. Comparative efficacy and safety of oral tocainide and quinidine for benign and potentially lethal ventricular arrhythmias. Am 1 Cardiol 1985;56: Podrid Pl, Lown B. Tocainide for refractory symptomatic ventricular arrhythmias. Am 1 Cardiol 1982;49: Mexitil package insert, Bochringer-Ingelheim Pharmaceuticals, Inc., Ridgefield, CN. 8. Podrid Pl, Lown a. Mexiletine for ventricular arrhythmias. Am 1 Cardiol 1981;47: Palileo EV. Welch W. Hoff 1, et al. Lack of effectiveness of oral mexiletine in patients with drug-refractory paroxysmal sustained ventricular tachycardia. A study utilizing programmed stimulation. Am 1 Cardiol 1982;50: Greenspan AM, Spielman SR, Webb CR, Sokoloff NM, Rae AP, Horowitz LN. Efficacy of combination therapy with mexiletine and a type IA agent for inducible ventricular tachyarrhythmias secondary to coronary artery disease. Am 1 Cardiol 1985;56: II. Tambocor package insert. Riker Laboratories. Inc/3M, St. Paul, MN. 12. The Flecaimde-Quinidine Research Group. Flecainide versus quinidine for treatment of chronic ventricular arrhythmias. A multicenter clinical trial. Circulation 1983;67: Lal R. Chapman PO, Naccarrelli GV, et al. Short- and long-term experience with flecainide acetate in the management of refractory life-threatening ventricular arrhythmias. 1 Am Coll Cardiol 1985;6: Flecainide Ventricular Tachycardia Study Group. Flecainide acetate treatment of resistant ventricular tachycardia. Am J Cardiol 19~6;57: Mueller RA, Baur HR. Flecainide: a new antiarrhythmic drug. Clin CardioI1986;9: Morganroth 1, Pool P, Miller R, et al. Dose-response range of encainide for benign and potentially lethal ventricular arrhythmias. Am 1 Cardiol 1986;57: Roden OM, Reele SB, Higgins SB, et al. Total suppression of ventricular arrhythmias by encainide. Pharmacokinetic and electrocardiographic characteristics. N Engll Med 1980;302: Morganroth 1, Somberg JC, Pool PE, et al. Comparative study of encainide and quinidine in the treatment of ventricular arrhythmias. 1 Am Coll Cardiol 1986;7: Horowitz LN. Encainide in lethal ventricular arrhythmias evaluated by electrophysiologic testing and reduction in symptoms. Am 1 Cardiol 1986;58:83C-6C. 20. Mason JW. Peters FA. Antiarrhythmic efficacy of encainide in patients with refractory recurrent ventricular tachycardia. Circulation 1981;63: DiBianco R, Fletcher RD, Cohen AL, et al. Treatment of frequent ventricular arrhythmia with encainide: assessment using serial ambulatory electrocardiograms, intracardiac electrophysiology studies, treadmill exercise tests, and radionuclide cineangiographic studies. Circulation 1982;65: Chesnie B, Podrid P, Lown B, Raeder E. Encainide for refractory ventricular tachyarrhythmia. Am 1 Cardiol 1983;52: Sami MH. Derbekyan VA. Lisbona R. Hemodynamic effects of encainide patients with ventricular arrhythmia and poor ventricular function. Am J Cardiol 1983;52: Cordarone package insert. Wyeth Laboratories, Inc. Philadelphia, PA. 25. Nademanee K. Singh BN, Hendrickson J, et al. Amiodarone in refractory life-threatening ventricular arrhythmias. Ann Intern Med 1983;98: Heger JJ. Prystowsky EN, Zipes DP. Clinical efficacy of amiodarone in treatment of recurrent ventricular tachycardia and ventricular fibrillation. Am Heart ;106: Winkle RA. Amiodarone and the American way. 1 Am Coll Cardiol 1985:6: Horowitz LN, Greenspan AM. Spielman SR, et al. Usefulness of electrophysiologic testing in evaluation of amiodarone therapy for sustained ventricular tachyarrhythmias associated with coronary heart disease. Am 1 Cardiol 1985;55: Zipes DL. A consideration of antiarrhythmic therapy. Circulation 1985;72: Morganroth J. Premature ventricular complexes: Diagnosis and indications for therapy. lama 1984;252:673-6.
Antiarrhythmic Drugs 1/31/2018 1
 Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
PHARMACOLOGY OF ARRHYTHMIAS
 PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Mr. Eknath Kole M.S. Pharm (NIPER Mohali)
 M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
Arrhythmias. Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium.
 Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification
 Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
DECLARATION OF CONFLICT OF INTEREST. Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical
 DECLARATION OF CONFLICT OF INTEREST Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical ESC Congress Paris, France August 27-31, 2011 Risk & Complications of AADs for Rhythm
DECLARATION OF CONFLICT OF INTEREST Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical ESC Congress Paris, France August 27-31, 2011 Risk & Complications of AADs for Rhythm
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
ARRHYTHMIAS IN THE ICU
 ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital
 Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital Content i. Rhythm versus Rate control ii. Anti-arrhythmic for Rhythm Control iii. Anti-arrhythmic for Rate
Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital Content i. Rhythm versus Rate control ii. Anti-arrhythmic for Rhythm Control iii. Anti-arrhythmic for Rate
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT
 ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
Chapter 14. Agents used in Cardiac Arrhythmias
 Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Propafenone for the Treatment of Refractory Complex Ventricular Ectopie Activity
 Propafenone for the Treatment of Refractory Complex Ventricular Ectopie Activity STEPHEN C. HAMMILL, M.D., F.A.C.C, PATRICIA B. SORENSON, R.N., DOUGLAS L. WOOD, M.D., F.A.C.C, Division of Cardiovascular
Propafenone for the Treatment of Refractory Complex Ventricular Ectopie Activity STEPHEN C. HAMMILL, M.D., F.A.C.C, PATRICIA B. SORENSON, R.N., DOUGLAS L. WOOD, M.D., F.A.C.C, Division of Cardiovascular
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation
 The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
B. 14 Antidysrhythmic drugs. a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification
 B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
the QT interval but without altering the JT interval and class lb drugs shorten both. Since both class la
 Postgraduate Medical Journal (1989) 65, 519-524 Combined anti-arrhythmic therapy with class 1 and class 3 drugs M.A. James,* P. Papouchado and J.V. Jones Department ofcardiology, Bristol Royal Infirmary,
Postgraduate Medical Journal (1989) 65, 519-524 Combined anti-arrhythmic therapy with class 1 and class 3 drugs M.A. James,* P. Papouchado and J.V. Jones Department ofcardiology, Bristol Royal Infirmary,
Cardiac Drugs: Chapter 9 Worksheet Cardiac Agents. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate.
 Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
National Coverage Determination (NCD) for Cardiac Pacemakers (20.8)
 Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Ventricular tachycardia Ventricular fibrillation and ICD
 EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ. ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C
 ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C Definitions of AF: A Simplified Scheme Term Definition Paroxysmal AF AF that terminates
ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C Definitions of AF: A Simplified Scheme Term Definition Paroxysmal AF AF that terminates
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ.
 «Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Amiodarone Prescribing and Monitoring: Back to the Future
 Amiodarone Prescribing and Monitoring: Back to the Future Subha L. Varahan, MD, FHRS, CCDS Electrophysiologist Oklahoma Heart Hospital Oklahoma City, OK Friday, February, 8 th, 2019 Iodinated benzofuran
Amiodarone Prescribing and Monitoring: Back to the Future Subha L. Varahan, MD, FHRS, CCDS Electrophysiologist Oklahoma Heart Hospital Oklahoma City, OK Friday, February, 8 th, 2019 Iodinated benzofuran
MEDICINAL PRODUCTS FOR THE TREATMENT OF ARRHYTHMIAS
 MEDICINAL PRODUCTS FOR THE TREATMENT OF ARRHYTHMIAS Guideline Title Medicinal Products for the Treatment of Arrhythmias Legislative basis Directive 75/318/EEC as amended Date of first adoption November
MEDICINAL PRODUCTS FOR THE TREATMENT OF ARRHYTHMIAS Guideline Title Medicinal Products for the Treatment of Arrhythmias Legislative basis Directive 75/318/EEC as amended Date of first adoption November
Antiarrhythmic Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017
 Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017 Types of Cardiac Arrhythmias Abnormalities of Impulse Formation: Rate disturbances. Triggered
Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017 Types of Cardiac Arrhythmias Abnormalities of Impulse Formation: Rate disturbances. Triggered
I have nothing to disclose.
 I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
Antiarrhythmic Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018
 Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 2 Ion Permeability Changes Potential Changes Genes and Proteins 3 Cardiac Na+ channels 5 6
Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 2 Ion Permeability Changes Potential Changes Genes and Proteins 3 Cardiac Na+ channels 5 6
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Anti arrhythmic drugs. Hilal Al Saffar College of medicine Baghdad University
 Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
Use of Electrophysiologic Testing in Patients With Nonsustained Ventricular Tachycardia Prognostic and Therapeutic Implications
 JACC Vol. 14, No. I July 1 8 1 5 5-61 155 ELECTROPHYSIOLOGIC STUDIES Use of Electrophysiologic Testing in Patients With Nonsustained Ventricular Tachycardia Prognostic and Therapeutic Implications RICHARD
JACC Vol. 14, No. I July 1 8 1 5 5-61 155 ELECTROPHYSIOLOGIC STUDIES Use of Electrophysiologic Testing in Patients With Nonsustained Ventricular Tachycardia Prognostic and Therapeutic Implications RICHARD
Chapter (9) Calcium Antagonists
 Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Atrial Fibrillation and Common Supraventricular Tachycardias. Sunil Kapur MD
 Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Prediction of Life-Threatening Arrhythmia in Patients after Myocardial Infarction by Late Potentials, Ejection Fraction and Holter Monitoring
 Prediction of Life-Threatening Arrhythmia in Patients after Myocardial Infarction by Late Potentials, Ejection Fraction and Holter Monitoring Yu-Zhen ZHANG, M.D.,* Shi-Wen WANG, M.D.,* Da-Yi Hu, M.D.,**
Prediction of Life-Threatening Arrhythmia in Patients after Myocardial Infarction by Late Potentials, Ejection Fraction and Holter Monitoring Yu-Zhen ZHANG, M.D.,* Shi-Wen WANG, M.D.,* Da-Yi Hu, M.D.,**
ANTI-ARRHYTHMICS AND WARFARIN. Dr Nithish Jayakumar
 ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
Atrial Fibrillation 10/2/2018. Depolarization & ECG. Atrial Fibrillation. Hemodynamic Consequences
 Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Fundamentals of Pharmacology for Veterinary Technicians Chapter 8
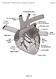 Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
There are future perspectives in the pharmacological treatment of arrhythmias
 There are future perspectives in the pharmacological treatment of arrhythmias George Andrikopoulos, MD, PhD, FESC, Cardiologist, Director, 1st Department of Cardiology/ Department of Electrophysiology
There are future perspectives in the pharmacological treatment of arrhythmias George Andrikopoulos, MD, PhD, FESC, Cardiologist, Director, 1st Department of Cardiology/ Department of Electrophysiology
Antiarrhythmic Pharmacology. The Electronics
 Antiarrhythmic Pharmacology Linking Pharmacological Treatment to the Patient and the Rhythm Presented By: Karen Marzlin BSN, RN,C, CCRN-CMC CNEA 2009 1 The Electronics Action Potential of Cardiac Cells
Antiarrhythmic Pharmacology Linking Pharmacological Treatment to the Patient and the Rhythm Presented By: Karen Marzlin BSN, RN,C, CCRN-CMC CNEA 2009 1 The Electronics Action Potential of Cardiac Cells
Synopsis of Management on Ventricular arrhythmias. M. Soni MD Interventional Cardiologist
 Synopsis of Management on Ventricular arrhythmias M. Soni MD Interventional Cardiologist No financial disclosure Premature Ventricular Contraction (PVC) Ventricular Bigeminy Ventricular Trigeminy Multifocal
Synopsis of Management on Ventricular arrhythmias M. Soni MD Interventional Cardiologist No financial disclosure Premature Ventricular Contraction (PVC) Ventricular Bigeminy Ventricular Trigeminy Multifocal
Prehospital Care Monograph
 Prehospital Care Monograph Amiodarone (Cordarone) City of Pittsburgh Bureau of Emergency Medical Services And Medical Direction Committee Center for Emergency Medicine Of Western Pennsylvania 1 This monograph
Prehospital Care Monograph Amiodarone (Cordarone) City of Pittsburgh Bureau of Emergency Medical Services And Medical Direction Committee Center for Emergency Medicine Of Western Pennsylvania 1 This monograph
Editorial TREATMENT OF SUDDEN CARDIAC DEATH SURVIVORS: DRUGS VERSUS DEVICE
 Editorial TREATMENT OF SUDDEN CARDIAC DEATH SURVIVORS: DRUGS VERSUS DEVICE Patients who survive an episode of sustained ventricular trachycardia (VT) or out-of-hospital ventricular fibrillation (VF) are
Editorial TREATMENT OF SUDDEN CARDIAC DEATH SURVIVORS: DRUGS VERSUS DEVICE Patients who survive an episode of sustained ventricular trachycardia (VT) or out-of-hospital ventricular fibrillation (VF) are
Electrocardiographic Recording
 Spontaneous Variability of Complex Ventricular Arrhythmias Detected by Long-term Electrocardiographic Recording ERIC L. MICHELSON, M.D., AND JOEL MORGANROTH, M.D. SUMMARY Variations in the frequency of
Spontaneous Variability of Complex Ventricular Arrhythmias Detected by Long-term Electrocardiographic Recording ERIC L. MICHELSON, M.D., AND JOEL MORGANROTH, M.D. SUMMARY Variations in the frequency of
Atrial Fibrillation: Rate vs. Rhythm. Michael Curley, MD Cardiac Electrophysiology
 Atrial Fibrillation: Rate vs. Rhythm Michael Curley, MD Cardiac Electrophysiology I have no relevant financial disclosures pertaining to this topic. A Fib Epidemiology #1 Most common heart rhythm disturbance
Atrial Fibrillation: Rate vs. Rhythm Michael Curley, MD Cardiac Electrophysiology I have no relevant financial disclosures pertaining to this topic. A Fib Epidemiology #1 Most common heart rhythm disturbance
Arrhythmias: Enhancement of Efficacy and
 Mexiletine in the Treatment of Resistant Ventricular Arrhythmias: Enhancement of Efficacy and Reduction of Dose-related Side Effects by Combination with Quinidine HENRY J. DUFF, M.D., DAN RODEN, M.D.,
Mexiletine in the Treatment of Resistant Ventricular Arrhythmias: Enhancement of Efficacy and Reduction of Dose-related Side Effects by Combination with Quinidine HENRY J. DUFF, M.D., DAN RODEN, M.D.,
Which Drugs Treat Ventricular Arrhythmias in Dogs & Cats?
 Rx SOLUTIONS PEER REVIEWED Which Drugs Treat Ventricular Arrhythmias in Dogs & Cats? Amara Estrada, DVM, DACVIM (Cardiology) University of Florida 2015 Kip Carter, MS, CMI Profile Most antiarrhythmic agents
Rx SOLUTIONS PEER REVIEWED Which Drugs Treat Ventricular Arrhythmias in Dogs & Cats? Amara Estrada, DVM, DACVIM (Cardiology) University of Florida 2015 Kip Carter, MS, CMI Profile Most antiarrhythmic agents
Controversies in Atrial Fibrillation and HF
 Controversies in Atrial Fibrillation and HF Dr.Yahya Al Hebaishi Cardiac electrophysiology division, PSCC, Riyadh Atrial Fibrillation: Rate or Rhythm? HF and AF: the twin epidemic of cardiovascular disease.
Controversies in Atrial Fibrillation and HF Dr.Yahya Al Hebaishi Cardiac electrophysiology division, PSCC, Riyadh Atrial Fibrillation: Rate or Rhythm? HF and AF: the twin epidemic of cardiovascular disease.
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Antidysrhythmics HST-151 1
 HST-151 1 Antidysrhythmics I. Ventricular muscle cell action potential a. Phase 0: Upstroke b. Phase 1: Early-fast repolarization c. Phase 2: Plateau d. Phase 3: Repolarization e. Phase 4: Diastole HST-151
HST-151 1 Antidysrhythmics I. Ventricular muscle cell action potential a. Phase 0: Upstroke b. Phase 1: Early-fast repolarization c. Phase 2: Plateau d. Phase 3: Repolarization e. Phase 4: Diastole HST-151
Catheter Ablation: Atrial fibrillation (AF) is the most common. Another Option for AF FAQ. Who performs ablation for treatment of AF?
 : Another Option for AF Atrial fibrillation (AF) is a highly common cardiac arrhythmia and a major risk factor for stroke. In this article, Dr. Khan and Dr. Skanes detail how catheter ablation significantly
: Another Option for AF Atrial fibrillation (AF) is a highly common cardiac arrhythmia and a major risk factor for stroke. In this article, Dr. Khan and Dr. Skanes detail how catheter ablation significantly
AF :RHYTHM CONTROL BY DR-MOHAMMED SALAH ASSISSTANT LECTURER CARDIOLOGY DEPARTMENT
 AF :RHYTHM CONTROL BY DR-MOHAMMED SALAH ASSISSTANT LECTURER CARDIOLOGY DEPARTMENT 5-2014 Atrial Fibrillation therapeutic Approach Rhythm Control Thromboembolism Prevention: Recommendations Direct-Current
AF :RHYTHM CONTROL BY DR-MOHAMMED SALAH ASSISSTANT LECTURER CARDIOLOGY DEPARTMENT 5-2014 Atrial Fibrillation therapeutic Approach Rhythm Control Thromboembolism Prevention: Recommendations Direct-Current
Antiarrhythmic agents in 2014
 7 AP-HRS Scientific Session, New Dehli, India - Oct 29 to Nov 1, 2014 Antiarrhythmic agents in 2014 Antonio Raviele, MD, FESC, FHRS President ALFA Alliance to Fight Atrial fibrillation - Venice, Italy
7 AP-HRS Scientific Session, New Dehli, India - Oct 29 to Nov 1, 2014 Antiarrhythmic agents in 2014 Antonio Raviele, MD, FESC, FHRS President ALFA Alliance to Fight Atrial fibrillation - Venice, Italy
dronedarone, 400mg, film-coated tablets (Multaq ) SMC No. (636/10) Sanofi-aventis Ltd
 dronedarone, 400mg, film-coated tablets (Multaq ) SMC No. (636/10) Sanofi-aventis Ltd 6 August 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
dronedarone, 400mg, film-coated tablets (Multaq ) SMC No. (636/10) Sanofi-aventis Ltd 6 August 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
How does the heart work? The heart is muscle whose main function is a pump; to push blood the rest of your body.
 1 You have a condition called atrial fibrillation. I would like you to learn more about this condition. You should read about it below, and can also watch an Internet program about it. After reading about
1 You have a condition called atrial fibrillation. I would like you to learn more about this condition. You should read about it below, and can also watch an Internet program about it. After reading about
My Patient Needs a Stress Test
 My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
Appraisal of mulfifocal atrial tachycardia
 British Heart Journal, 197I, 33, 500-504. Appraisal of mulfifocal atrial tachycardia Edward K. Chung From Division of Cardiology, Department of Medicine, West Virginia Uuiversity School of Medicine, Morgantown,
British Heart Journal, 197I, 33, 500-504. Appraisal of mulfifocal atrial tachycardia Edward K. Chung From Division of Cardiology, Department of Medicine, West Virginia Uuiversity School of Medicine, Morgantown,
Evidence for Lidocaine and Amiodarone in Cardiac Arrest Due to VF/Pulseless VT
 Evidence for Lidocaine and Amiodarone in Cardiac Arrest Due to VF/Pulseless VT Introduction Evidence supporting the use of lidocaine and amiodarone for advanced cardiac life support was considered by international
Evidence for Lidocaine and Amiodarone in Cardiac Arrest Due to VF/Pulseless VT Introduction Evidence supporting the use of lidocaine and amiodarone for advanced cardiac life support was considered by international
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Most antiarrhythmic drugs are potent compounds with a relatively narrow therapeutic
 Pharmacological Effects of Antiarrhythmic s Review and Update Peter R. Kowey, MD REVIEW ARTICLE Most antiarrhythmic drugs are potent compounds with a relatively narrow therapeutic index. When prescribed
Pharmacological Effects of Antiarrhythmic s Review and Update Peter R. Kowey, MD REVIEW ARTICLE Most antiarrhythmic drugs are potent compounds with a relatively narrow therapeutic index. When prescribed
Sotalol-Induced Coronary Spasm in a Patient with Dilated Cardiomyopathy Associated with Sustained Ventricular Tachycardia
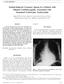 CASE REPORT Sotalol-Induced Coronary Spasm in a Patient with Dilated Cardiomyopathy Associated with Sustained Ventricular Tachycardia Shigenori MUTO, Naoto ASHIZAWA, Syuji ARAKAWA, Kyoei TANAKA, Norihiro
CASE REPORT Sotalol-Induced Coronary Spasm in a Patient with Dilated Cardiomyopathy Associated with Sustained Ventricular Tachycardia Shigenori MUTO, Naoto ASHIZAWA, Syuji ARAKAWA, Kyoei TANAKA, Norihiro
Rate and Rhythm Control of Atrial Fibrillation
 Rate and Rhythm Control of Atrial Fibrillation April 21, 2017 춘계심혈관통합학술대회 Jaemin Shim, MD, PhD Arrhythmia Center Korea University Anam Hospital Treatment of AF Goal Reducing symptoms Preventing complication
Rate and Rhythm Control of Atrial Fibrillation April 21, 2017 춘계심혈관통합학술대회 Jaemin Shim, MD, PhD Arrhythmia Center Korea University Anam Hospital Treatment of AF Goal Reducing symptoms Preventing complication
ARRHYTHMIA SINUS RHYTHM
 ARRHYTHMIA Dr. Ahmed A. Elberry, MBBCH, MSc, MD Assistant Professor of Clinical Pharmacy Faculty of pharmacy, KAU 1 SINUS RHYTHM SA node is cardiac pacemaker Normal sinus rhythm 60-100 beats/min Depolarisation
ARRHYTHMIA Dr. Ahmed A. Elberry, MBBCH, MSc, MD Assistant Professor of Clinical Pharmacy Faculty of pharmacy, KAU 1 SINUS RHYTHM SA node is cardiac pacemaker Normal sinus rhythm 60-100 beats/min Depolarisation
Ventricular Tachycardia Basics
 Ventricular Tachycardia Basics OVERVIEW Ventricular refers to the ventricles of the heart; tachycardia is the medical term for rapid heart rate The heart of the dog or cat is composed of four chambers;
Ventricular Tachycardia Basics OVERVIEW Ventricular refers to the ventricles of the heart; tachycardia is the medical term for rapid heart rate The heart of the dog or cat is composed of four chambers;
ANTI - ARRHYTHMIC DRUGS
 ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
Clinical and electrophysiological characteristics of patients having atrial flutter with 1:1 atrioventricular conduction
 Europace (2008) 10, 284 288 doi:10.1093/europace/eun012 of patients having atrial flutter with 1:1 atrioventricular conduction Mihoko Kawabata*, Kenzo Hirao, Kouji Higuchi, Takeshi Sasaki, Toshiyuki Furukawa,
Europace (2008) 10, 284 288 doi:10.1093/europace/eun012 of patients having atrial flutter with 1:1 atrioventricular conduction Mihoko Kawabata*, Kenzo Hirao, Kouji Higuchi, Takeshi Sasaki, Toshiyuki Furukawa,
Understanding Atrial Fibrillation Management. Roy Lin, MD
 Understanding Atrial Fibrillation Management Roy Lin, MD Disclosure None Definition of atrial fibrillation Atrial fibrillation is a supraventricular tachyarrhythmia characterized by uncoordinated atrial
Understanding Atrial Fibrillation Management Roy Lin, MD Disclosure None Definition of atrial fibrillation Atrial fibrillation is a supraventricular tachyarrhythmia characterized by uncoordinated atrial
Cardiac Arrhythmias. For Pharmacists
 Cardiac Arrhythmias For Pharmacists Agenda Overview of the normal Classification Management Therapy Conclusion Cardiac arrhythmias Overview of the normal Arrhythmia: definition From the Greek a-, loss
Cardiac Arrhythmias For Pharmacists Agenda Overview of the normal Classification Management Therapy Conclusion Cardiac arrhythmias Overview of the normal Arrhythmia: definition From the Greek a-, loss
Cibenzoline for Treatment of Ventricular Arrhythmias: A Double-Blind Placebo-Controlled Study
 372 lacc Vol. 4, No.2 August 1984:372-7 Cibenzoline for Treatment of Ventricular Arrhythmias: A Double-Blind Placebo-Controlled Study JOHN B, KOSTIS, MD, FACC, SUSAN KRIEGER, RN, ABEL MOREYRA, MD, FACC,
372 lacc Vol. 4, No.2 August 1984:372-7 Cibenzoline for Treatment of Ventricular Arrhythmias: A Double-Blind Placebo-Controlled Study JOHN B, KOSTIS, MD, FACC, SUSAN KRIEGER, RN, ABEL MOREYRA, MD, FACC,
Rate Control: What is the Goal and How to Achieve It? Steve Greer, MD, FHRS, FACC BHHI Primary Care Symposium February 28, 2014
 Rate Control: What is the Goal and How to Achieve It? Steve Greer, MD, FHRS, FACC BHHI Primary Care Symposium February 28, 2014 Financial Disclosures Boerhinger Ingelheim Research Support Boston Scientific
Rate Control: What is the Goal and How to Achieve It? Steve Greer, MD, FHRS, FACC BHHI Primary Care Symposium February 28, 2014 Financial Disclosures Boerhinger Ingelheim Research Support Boston Scientific
Asymptomatic WPW Syndrome; Observation or Ablation? 전남대학교병원순환기내과 박형욱
 Asymptomatic WPW Syndrome; Observation or Ablation? 전남대학교병원순환기내과 박형욱 Let It Be? Vs. Just Do It? Natural history of asymptomatic WPW Incidence of sudden cardiac death in natural history studies involving
Asymptomatic WPW Syndrome; Observation or Ablation? 전남대학교병원순환기내과 박형욱 Let It Be? Vs. Just Do It? Natural history of asymptomatic WPW Incidence of sudden cardiac death in natural history studies involving
Antiarrhythmics 17 I. OVERVIEW II. INTRODUCTION TO THE ARRHYTHMIAS
 Antiarrhythmics 17 I. OVERVIEW In contrast to skeletal muscle, which contracts only when it receives a stimulus, the heart contains specialized cells that exhibit automaticity. This means that they can
Antiarrhythmics 17 I. OVERVIEW In contrast to skeletal muscle, which contracts only when it receives a stimulus, the heart contains specialized cells that exhibit automaticity. This means that they can
Comparison of different proarrhythmia biomarkers in isolated rabbit hearts
 Comparison of different proarrhythmia biomarkers in isolated rabbit hearts Summary of PhD Thesis Szabolcs Orosz, MSc Supervisor: Attila Farkas MD, PhD 2nd Dept. of Internal Medicine and Cardiology Centre
Comparison of different proarrhythmia biomarkers in isolated rabbit hearts Summary of PhD Thesis Szabolcs Orosz, MSc Supervisor: Attila Farkas MD, PhD 2nd Dept. of Internal Medicine and Cardiology Centre
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
The ARREST Trial: Amiodarone for Resuscitation After Out-of-Hospital Cardiac Arrest Due to Ventricular Fibrillation
 The ARREST Trial: Amiodarone for Resuscitation After Out-of-Hospital Cardiac Arrest Due to Ventricular Fibrillation Introduction The ARREST (Amiodarone in out-of-hospital Resuscitation of REfractory Sustained
The ARREST Trial: Amiodarone for Resuscitation After Out-of-Hospital Cardiac Arrest Due to Ventricular Fibrillation Introduction The ARREST (Amiodarone in out-of-hospital Resuscitation of REfractory Sustained
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint
 CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
complicating myocardial infarction
 British Heart Journal, I970, 32, 21. Bretylium tosylate in treatment of refractory ventricular arrhythmias complicating myocardial infarction G. Terry,1 C. W. Vellani, M. R. Higgins, and A. Doig From the
British Heart Journal, I970, 32, 21. Bretylium tosylate in treatment of refractory ventricular arrhythmias complicating myocardial infarction G. Terry,1 C. W. Vellani, M. R. Higgins, and A. Doig From the
Atrial fibrillation (AF) is a disorder seen
 This Just In... An Update on Arrhythmia What do recent studies reveal about arrhythmia? In this article, the authors provide an update on atrial fibrillation and ventricular arrhythmia. Beth L. Abramson,
This Just In... An Update on Arrhythmia What do recent studies reveal about arrhythmia? In this article, the authors provide an update on atrial fibrillation and ventricular arrhythmia. Beth L. Abramson,
Chemically, MEXITIL is 1-methyl-2-(2, 6-xylyloxy) ethylamine hydrochloride and has the following structural formula:
 Mexitil (mexiletine hydrochloride, USP) Capsules of 150 mg, 200 mg and 250 mg Oral Antiarrhythmic Prescribing Information DESCRIPTION MEXITIL (mexiletine hydrochloride, USP) is an orally active antiarrhythmic
Mexitil (mexiletine hydrochloride, USP) Capsules of 150 mg, 200 mg and 250 mg Oral Antiarrhythmic Prescribing Information DESCRIPTION MEXITIL (mexiletine hydrochloride, USP) is an orally active antiarrhythmic
CORDARONE Sanofi-Aventis
 CORDARONE Sanofi-Aventis Composition Amiodarone 200 mg; tablets. Also AMPOULES 150 mg/3 ml. Indications Tablets Prevention of recurrence of the following: life-threatening ventricular tachycardias in which
CORDARONE Sanofi-Aventis Composition Amiodarone 200 mg; tablets. Also AMPOULES 150 mg/3 ml. Indications Tablets Prevention of recurrence of the following: life-threatening ventricular tachycardias in which
Journal of the American College of Cardiology Vol. 37, No. 2, by the American College of Cardiology ISSN /01/$20.
 Journal of the American College of Cardiology Vol. 37, No. 2, 2001 2001 by the American College of Cardiology ISSN 0735-1097/01/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)01133-5 Coronary
Journal of the American College of Cardiology Vol. 37, No. 2, 2001 2001 by the American College of Cardiology ISSN 0735-1097/01/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)01133-5 Coronary
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
The Response to Antiarrhythmia Therapy with Amiodarone in Diabetic Patients Undergoing Coronary Artery Bypass Grafting
 ISPUB.COM The Internet Journal of Cardiology Volume 1 Number 2 The Response to Antiarrhythmia Therapy with Amiodarone in Diabetic Patients Undergoing Coronary Artery Bypass Grafting M Tamim, N Erdil, U
ISPUB.COM The Internet Journal of Cardiology Volume 1 Number 2 The Response to Antiarrhythmia Therapy with Amiodarone in Diabetic Patients Undergoing Coronary Artery Bypass Grafting M Tamim, N Erdil, U
Flecainide Versus Quinidine for Treatment
 Flecainide Versus Quinidine for Treatment of Chronic Ventricular Arrhythmias A Multicenter Clinical Trial THE FLECAINIDE-QUINIDINE RESEARCH GROUP* SUMMARY The antiarrhythmic efficacy and safety of oral
Flecainide Versus Quinidine for Treatment of Chronic Ventricular Arrhythmias A Multicenter Clinical Trial THE FLECAINIDE-QUINIDINE RESEARCH GROUP* SUMMARY The antiarrhythmic efficacy and safety of oral
Mexiletine: An Effective Antiarrhythmic Drug for Treatment of Ventricular Arrhythmias in Congenital Heart Disease
 84 lacc Vol 10. No. 4 October 1987:S4-9 REPORTS ON THERAPY Mexiletine: An Effective Antiarrhythmic Drug for Treatment of Ventricular Arrhythmias in Congenital Heart Disease JEFFREY P. MOAK, MD, FACC, RICHARD
84 lacc Vol 10. No. 4 October 1987:S4-9 REPORTS ON THERAPY Mexiletine: An Effective Antiarrhythmic Drug for Treatment of Ventricular Arrhythmias in Congenital Heart Disease JEFFREY P. MOAK, MD, FACC, RICHARD
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS)
 DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
Dysrhythmias. Dysrythmias & Anti-Dysrhythmics. EKG Parameters. Dysrhythmias. Components of an ECG Wave. Dysrhythmias
 Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Treatment strategy decision tree
 strategy decision tree strategy decision tree Confirmed diagnosis of AF Further investigations and clinical assessment including risk stratification for stroke/thromboembolism Paroxysmal AF Persistent
strategy decision tree strategy decision tree Confirmed diagnosis of AF Further investigations and clinical assessment including risk stratification for stroke/thromboembolism Paroxysmal AF Persistent
Review guidance for patients on long-term amiodarone treatment
 Review guidance for patients on long-term amiodarone treatment This review guidance document has been produced in response to: 1. Current supply shortages of branded and generic versions of 100mg and 200mg
Review guidance for patients on long-term amiodarone treatment This review guidance document has been produced in response to: 1. Current supply shortages of branded and generic versions of 100mg and 200mg
Document 3 Summary of Data and Guidance for Medical Professionals
 Document 3 Summary of Data and Guidance for Medical Professionals Anvirzel Anvirzel is a novel antitumor compound extracted from the plant Nerium oleander, which belongs to the family Apocynaceae. Anvirzel
Document 3 Summary of Data and Guidance for Medical Professionals Anvirzel Anvirzel is a novel antitumor compound extracted from the plant Nerium oleander, which belongs to the family Apocynaceae. Anvirzel
National Horizon Scanning Centre. Dronedarone (Multaq) for atrial fibrillation and atrial flutter. December 2007
 Dronedarone (Multaq) for atrial fibrillation and atrial flutter December 2007 This technology summary is based on information available at the time of research and a limited literature search. It is not
Dronedarone (Multaq) for atrial fibrillation and atrial flutter December 2007 This technology summary is based on information available at the time of research and a limited literature search. It is not
Electrophysiologic and Clinical Effects of Oral Encainide in Paroxysmal Atrioventricular Node Reentrant Tachycardia
 992 JACC Vol. 14. No. 4 October 1989:992-8 Electrophysiologic and Clinical Effects of Oral Encainide in Paroxysmal Atrioventricular Node Reentrant Tachycardia MARCELLO CHIMIENTI, MD, MARIA LI BERGOLIS,
992 JACC Vol. 14. No. 4 October 1989:992-8 Electrophysiologic and Clinical Effects of Oral Encainide in Paroxysmal Atrioventricular Node Reentrant Tachycardia MARCELLO CHIMIENTI, MD, MARIA LI BERGOLIS,
Heart Failure Update John Coyle, M.D.
 Heart Failure Update 2011 John Coyle, M.D. Causes of Heart Failure Anderson,B.Am Heart J 1993;126:632-40 It It is now well-established that at least one-half of the patients presenting with symptoms and
Heart Failure Update 2011 John Coyle, M.D. Causes of Heart Failure Anderson,B.Am Heart J 1993;126:632-40 It It is now well-established that at least one-half of the patients presenting with symptoms and
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
How do arrhythmias occur?
 How do arrhythmias occur? An arrhythmia is an abnormal heart rhythm (= dysrhythmia). Can be fast (tachy) or slow (brady). Brady arrhythmias are usually due to conduc;on block, while tachyarrhythmias are
How do arrhythmias occur? An arrhythmia is an abnormal heart rhythm (= dysrhythmia). Can be fast (tachy) or slow (brady). Brady arrhythmias are usually due to conduc;on block, while tachyarrhythmias are
ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY
 ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY The heart beat begins when an electrical impulse from the sinoatrial node (SA node or sinus node) moves through it. The normal electrical sequence begins
ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY The heart beat begins when an electrical impulse from the sinoatrial node (SA node or sinus node) moves through it. The normal electrical sequence begins
