Effect of Biofeedback Training on Fecal Incontinence in Children with Myelomeningocele
|
|
|
- Ralph Summers
- 6 years ago
- Views:
Transcription
1 Med. J. Cairo Univ., Vol. 77, No. 1, March: , 29 Effect of Biofeedback Training on Fecal Incontinence in Children with Myelomeningocele REDA S.M. SARHAN, P.T.D.* and ENAS EL-SAYED, P.T.D.** The Department of Physical Therapy, Faculty of Medicine, Al-Azhar University*and the Department of Physical Therapy for Neuromuscular Disorders & its Surgery, Faculty of Physical Therapy, Cairo University. Abstract Purpose: This study aimed at evaluating the effects of biofeedback training on children with fecal incontinence. Subjects: Twenty children (12 males and 8 females), diagnosed as spina-pifida (myelomeningocele), were recruited from pediatrics outpatient clinic, King Abdul-Aziz university hospital, Jeddah, Saudi Arabia. Their age ranged from ten to fifteen years. Methods: Anorectal manometric functions were assessed for all children before and after treatment. The children were randomly divided into two groups of equal number (control and study). Both groups received physical therapy program (daily rectal evacuation program, diet control and pelvic floor muscle exercises). In addition, the study group received biofeedback training program. Treatment for all patients continued for three months (one hour/session, three times/ week). Results: The results revealed statistically significant improvement in the outcome measures in the study group. Biofeedback training improved anal squeeze as well as rectal sensation. Conclusion: Biofeedback training in conjunction with conventional therapy program was effective in improving fecal incontinence in children with myelomeningocele. Key Words: Spina bifida Myelomeningocele Neurogenic fecal incontinence Urodynamic biofeedback. Introduction NEURAL tube defects are complex congenital malformations involving the spine (spina bifida) or the cranium (anencephaly, encephaloceles) [1,2]. These defects occur before the end of the 4 th week of gestation and are characterized by a midline vertebral defect (spina bifida), most often in the dorsal portion of the lumbosacral vertebrae. When only a meningeal sac protrudes through the defect, it is called a meningocele; if the spinal cord also protrudes, it is called a myelomeningocele (MMC) [3]. Myelomeningocele accounts for about 75% of all cases of spina bifida and may affect as many as one out of every 8 infants. The cause is unknown; however, folic acid deficiency is thought to play a part in neural tube defects. conception folic acid supplementation may prevent spina bifida. The disorder appears to be more common in families. Research also indicates possible environmental factors such as radiation. Protrusion of the spinal cord and meninges damages the spinal cord and nerve roots, causing a decrease or lack of function of body areas controlled at or below the defect. Symptoms are related to the anatomic level of the defect [4,5,6]. Recent spinal hemorrhages may be superimposed upon pre-existing defects. If early therapeutic strategies can prevent these superimposed secondary spinal hemorrhages, motor outcome may improve [7]. Rectal sensation, peristalsis and adequate anorectal function are of major importance for normal continence and defecation. Neurological defects in patients with spinal lesions may affect one or more of these components and are manifested as inadequate sensation of rectal fullness, poor peristalsis, inappropriate tone or activity of the anorectal sphincter mechanism or a combination of these, resulting in fecal incontinence or chronic constipation or both [8]. Fecal incontinence is the inability to control bowel movements, causing stool to leak from rectum it ranges from an occasional leakage of stool while passing gas to a complete loss of bowel control [9]. In childhood and adolescence, fecal soiling represents a psychologically devastating problem. The medical management of those patients is usually combined with behavioral techniques (toilet training) and cognitive exercises (psychotherapy and family therapy). In patients who cannot 121
2 122 Effect of Biofeedback Training on Fecal Incontinence achieve the main elements for bowel continence (anorectal sensation, functioning sphincters and rectal motility), these methods of treatment often fail to achieve satisfactory results [,11]. Biofeedback is a conditioning treatment in which information about a physiologic process is converted into a simple visual or auditory signal to enable the patient to learn to control a disordered function [12]. Anal sphincter exercises and biofeedback therapy have been used to treat the symptoms of people with fecal incontinence. However, standards of treatment are still lacking and the magnitude of alleged benefits has yet to be established [13]. Aim of the study: The aim of the present study was to evaluate quantitatively the effectiveness of biofeedback training as a primary tool designed to control fecal incontinence in children with myelomeningocele. Subjects Materials and Methods Subjects: The present study included twenty children of both sexes (12 males and 8 females) diagnosed as MMC. They were recruited from pediatrics out - patient clinic, King Abdul-Aziz university hospital, Jeddah, Saudi Arabia. Inclusion criteria: Patient's age ranged from ten to fifteen years (mean = 11.6±2.8). They were the same as regard the socioeconomic status and the educational level, they were ambulant and their IQ varied from 73 to 96 (mean = 88.4) estimated by psychiatrist. The patients' level of incontinence ranged from grade zero to grade one according to Kelly's score for continence [14]. Exclusion criteria: Ano-rectal surgical interference e.g. sphinctreric repair or muscle transplantation. Children were randomly assigned into two equal groups: and control groups. Materials: Evaluation instruments: Electromyograph: Danetee Key point M, made in Denmark. Sandhill's anorectal manometry kit: It includes syringes, pressure transducers, stopcocks, extension lines and recorder. Treatment instruments: Aanorectal manometry: It includes: Schuster probe, model PIN, A86-55, Sandhill's Scientific, Inc., Littleton, Colorado USA, which is a flexible, silicone, rubber tubes, pediatric size. Manometry kit (Sandhill's): Computer accessories: Colored monitor, loudspeaker, keyboard, mouth and multi-channel recorder. Computer programs with two different soft wares, one for anorectal manometry and the other for biofeedback training called biofeedback meter which has audible tones and visual bar graph for reinforcing the level of effort. Methods: Evaluation methods: All children were evaluated clinically through detailed history taking and general and local examination. Anorectal manometry: It was performed by using the Sandhill anorectal kits. The following measurements were recorded: Maximal resting anal pressure (MRAP): It is the highest pressure in the anal canal with the patient at rest, located at 1.5 cm from the anal verge for both males and females. The normal MRAP ranges from 7-12 cm water for males and 6- cm. water for females [15]. Maximal voluntary contraction pressure (MSAP): It is the maximal increase above the resting pressure [16]. Voluntary contraction time: It is the time from the beginning of contraction until half decrease of the rectal pressure amplitude. Threshold of rectal sensation: The upper balloon was gradually inflated by water until the patient felt desire to defecate. The smallest volume to which the patient responds was recorded as the minimum sensory threshold. Maximal tolerable rectal volume: A balloon catheter with a 5cc capacity was inserted in the rectum and gradually inflated with air. The volume at which the patient perceives additional inflation would be intolerable or at which the balloon in involuntarily expelled is considered the maximal tolerable volume. This volume constitutes a rough measure of rectal capacity.
3 Reda S.M. Sarhan & Enas El-Sayed 123 Treatment methods: group: Patients belonging to control group received conventional therapy program in the form of: Daily rectal evacuation program: After complete initial rectal evacuation, the rectum was maintained empty through a pediatrician through giving daily anal laxative suppository given twice daily for the first 2 days, then once daily for days to three weeks. The child was asked to go to the toilet every 6 hours during the daytime. This fixed dose might stimulate a conditional reflex for daily rectal evacuation. When complete control was reached, the suppository program was stopped and the child was encouraged to go to the toilet for regular rectal evaluation. Diet control: The diet was given in the form of bulk forming diet, fruits, vegetables, cereals and bran. The usual daily dose for children was two table spoonful twice/day. Pelvic floor muscle exercises (Kegel's exercises) [17] : The patient was instructed to lie side lying position with knees bent towards the chest. He or she was instructed to pull his/her pelvic muscles upward and inward and hold the contraction for 6 seconds, as if to hold back a defecation movement, followed by relaxion for 6 seconds. The exercise was repeated 25 times. Gradually increase the time until reaching seconds of contraction and relaxation for each with repetition up to 3 times. To avoid substitution of hip adductor muscles for pelvic-floor muscle contractions, the patient's knees were manually supported. During the performance of pelvic muscle contractions, the patient was instructed to perform pursed-lip breathing to avoid valsalva response. group: Patients belonging to the study group were subjected to the same conventional therapy program in addition to biofeedback training. Technique for biofeedback training: The patient was instructed to lie on the left side lying position with flexed knees towards chest and facing the monitor in order to see the changes that occur during the procedure on the screen. A schuster balloon tri-luminal catheter pediatric size (Sandhill) was used as follow [18] : The lower (distal) balloon was adjusted to lie opposite to the anal verge. The middle balloon was adjusted opposite to the internal anal sphincter located at 1.5 cm from the anal verge for both males and females. The upper (proximal) balloon was adjusted 4-12 cm above the anal verge. The part of the probe that remains extra - anal was fixed to the perineum by adhesive tapes to prevent its sliding out. Steps for biofeedback training: The middle balloon was inflated by air first to stimulate the internal anal sphincter thus avoiding slipping of the catheter, followed by inflation of the lower balloon to stimulate the external anal sphincter (anal resting pressure). The rectum was stimulated by inflation of the upper balloon gradually by air until the patient feels desire to defecate (threshold of rectal sensation). Immediately after onset of feeling rectal distension, the patient was asked to pull his/her pelvic muscles upward and inward (strain), as much as he can for of 6 seconds, as if to defecate and then asked to relax the muscles for 6 seconds with repetition for 25 times, to increase and decrease the pressure of the anal canal at the same time. In order to reinforce controlling the anal sphincter by will, the patient was shown that the pressure diagram on the monitor of the computer screen increases during contraction and decreases during relaxation. The rectal distention was stopped when the rectal pressure amplitudes reached to its half value due to sphincteric fatigue. Patients were encouraged verbally to practice pelvic floor contraction between biofeedback sessions and to take bulk-forming agents. After each session, the patient was requested to practice the same procedure at home, twice daily. The procedure was repeated each session and the patient was encouraged to increase the time of contraction gradually until reaching seconds contraction followed by seconds relaxation and to repeat the contractions up to 3 times/ session.
4 124 Effect of Biofeedback Training on Fecal Incontinence When the patient linked psychologically the sensation of rectal distension with voluntary contraction of the pelvic floor muscle and external anal sphincter, the patient was asked to repeat these procedures and relax the anal sphincter without visualizing the monitor. When the patient had acquired the capability of contracting and relaxing the sphincter without looking at the monitor on every single attempt, the patient has been encouraged to practice regularly these exercises at home. The study continued for three months, three times per week and each session lasted for 6 min. **: Highly significant. ***: Very highly significant. Anal resting pressure (cc water) Results Maximal resting anal pressure: Before treatment, there was no significant difference in the mean value of the anal resting pressure between the study and control groups ( p=.831). After treatment, a very highly significant improvement was found in the study group compared to that of the control group ( p=.1). Also the results revealed a highly significant increase in the anal resting pressure mean value within the study group after treatment compared to that before treatment (p=.3) [Table (1) and Fig. (1)]. Table (1): Comparison between study and control groups as regard maximal anal resting pressure before and after treatment. Maximal anal resting pressure (cm water) group group t p Mean±SD Mean±SD 44.75± ± ± ± *** t p.3**.168 Fig. (1): Mean values of maximal anal resting pressure before and after treatment in the study and control groups. Maximal voluntary contraction pressure: Before treatment, there was no significant difference in the mean value of the voluntary contraction pressure between the study and control groups (p=.871). After treatment, a very highly significant improvement was found in the study group compared to that of the control group (p=.1). Also the results revealed a very highly significant increase in the voluntary contraction pressure mean value within the study group after treatment compared to that before treatment ( p=.1) [Table (2) and Fig. (2)]. Table (2): Comparison between study and control groups as regard maximal voluntary contraction pressure before and after treatment. Maximal voluntary contraction group group t p pressure Mean±SD Mean±SD (cm water) 71.88± ± ± ± *** t p.1***.51 ***: Very highly significant. Voluntary contraction pressure (cc water) Fig. (2): Mean values of maximal voluntary contraction pressure before and after treatment in the study and control groups. Voluntary contraction time: Before intervention, there was no significant difference in the mean value of the voluntary contraction time between the study and control groups (p=.94). After treatment, a very highly significant improvement was found in the study group compared to that of the control group ( p=.1). Also the results revealed a very highly significant increase in the voluntary contraction time mean value within the study group after treatment compared to that before treatment ( p=.1) [Table (3) and Fig. (3)].
5 Reda S.M. Sarhan & Enas El-Sayed 125 Table (3): Comparison between study and control groups as regard voluntary contraction pressure before and after treatment. Voluntary contraction group group t p time (sec.) Mean±SD Mean±SD 42.13± ± ± ± * ** t p.1 ***.62 Threshold rectal sensation (cc air) ***: Very highly significant. Voluntary contraction time (sec.) Fig. (3): Mean values of voluntary contraction time before and after treatment in the study and control groups. Threshold of rectal sensation: Before intervention, there was no significant difference in the mean value of the rectal sensation threshold between the study and control groups (p=.61). After treatment, a highly significant decrease was found in the study group compared to that of the control group (p=.2). Also the results revealed a very highly significant decrease in the rectal sensation threshold mean value within the study group and a significant decrease within the control group after treatment compared to that before treatment (p=.1 and.19 respectively) [Table (4) and Fig.(4)]. Table (4): Comparison between study and control groups as regard threshold of rectal sensation before and after treatment. Threshold of rectal sensation (cc air) group group t p Mean±SD Mean±SD 65.63± ± ± ± ** t p.1 ***.19* *: Significant. **: Highly significant. ***: Very highly significant. Fig. (4): Mean values of threshold of rectal sensation before and after treatment in the study and control groups. Maximal tolerable rectal volume: Before intervention, there was no significant difference in the mean value of the maximal tolerable rectal volume between the study and control groups (p=.898). After treatment, a very highly significant decrease was shown in the study group compared to that of the control group ( p=.1). Moreover, a highly significant decrease was obtained in the maximal tolerable rectal volume mean value within the study group after treatment compared to that before treatment ( p=.1) [Table (5) and Fig. (5)]. Table (5): Comparison between study and control groups as regard maximum tolerable rectal volume before and after treatment. Maximal tolerable rectal volume (cc air) ± ± ± ± *** t p.1 **.87 **: Highly significant. ***: Very highly significant. Maximum tolerable rectal volume (cc air) group group t p Mean±SD Mean±SD Fig. (5): Mean values of maximal tolerable rectal volume before and after treatment in the study and control groups.
6 126 Effect of Biofeedback Training on Fecal Incontinence Discussion The management of the fecal incontinence in children is difficult and its social consequences are usually devastating. The general objectives of any bowel program are to produce social continence, predictability and independence. Achievement of those goals depends in part on the underlying cause. In children, fecal incontinence can occur from a variety of causes. The most common is overflow incontinence from functional fecal retention, but it can also occur in otherwise healthy children with functional non-retentive fecal soiling or in children with organic causes such as congenital malformations in children with myelomeningocele or any other condition affecting the anorectum, anal sphincters or the spinal cord. The results of the present study showed clearly the beneficial effects of using biofeedback training on increasing the anal resting pressure, increasing the voluntary contraction pressure, decreasing the rectal sensation threshold and improving anal squeeze. The findings of the current study are supported by Dobben et al. [9] who indicated that physiotherapy is a common treatment option in patients with fecal incontinence. Although physiotherapy may result in relief of symptoms, changes in the anorectal function is still unclear. Physiotherapy improves squeeze pressure and urges sensation, however, improved anorectal function does not always result in a decrease in fecal incontinence complaints. Moreover, our results are supported by those of Jensen [19] who attributed the effect of biofeedback training to the increased sensory feedback mechanism resulting in enhancement of voluntary motor control. He concluded that a multidisciplinary approach to treatment has the potential to improve the outcome for patients with fecal incontinence. The improvement of the outcomes in patients with fecal incontinence also came in agreement with the findings of Terra et al. [2] who found that pelvic floor rehabilitation with biofeedback leads to a modest improvement in severity of fecal incontinence, squeeze pressure and maximal tolerated volume. They reported that the improvement might be due to an improved pattern of recognition areas of both sensory and cerebellar cortexes. This leads to development of pattern anagrams in the sensorymotor cortex that is related to the anorectal function. Also, the findings of the current work coincide with that of Whitehead et al. [21] who observed that approximately six hours of biofeedback training given to eight fecally incontinent children with MMC were enough to learn children to evacuate normally or to reduce soiling. The patients were shown a polygraph tracing of the external anal sphincter while they were being encouraged voluntarily to contract the sphincter when the rectum was distended with progressively larger volumes of air in a balloon. The results Norton and Kamm [22] are also consistent with that of the current research. They reported that application of biofeedback training in addation to traditional physical therapy program, played an important role for those patients with congenital/neuropathic incontinence. Combination of those maneuvers can be used to change stool consistency, anorectal function and rectal evacuation. Sphincter pressure can be altered and bowel movement can be induced. The results of the present study are also confirmed by those of Norton et al. [13] who postulated that anorectal biofeedback is a treatment program that utilizes neuromuscular conditioning techniques to treat patients with fecal incontinence or chronic constipation that is associated with dysynergic defecation. Dysynergic defecation, also known as anismus or pelvic floor dysynergia, is characterized by failure of the abdominal, rectal, pelvic floor and anal sphincter muscles to coordinate and complete the act of defecation. It is characterized by impaired propulsion of stool from the rectum, paradoxical anal contraction, or inadequate anal relaxation or a combination of these mechanisms. Moreover, the results of the present piece of work coincide with the findings of Solomon et al. [23] who performed a prospective, randomized, controlled trial to assess whether pelvic floor exercises with biofeedback using anal manometry or transanal ultrasound are superior to pelvic floor exercises with feedback from digital examination alone in terms of continence, quality of life, physiologic sphincter strength and compliance. They concluded that patients who completed pelvic floor exercises with feedback from digital examination achieved benefit from biofeedback and measurement with transanal ultrasound or manometry. Their study has confirmed that pelvic floor retraining programs are effective treatment for improving physiologic, clinical and quality of life parameters in those patients. In contrast, Van Tets et al. [24] concluded that external sphincter contraction exercises under direct electromyographic vision were not effective in neurogenic fecal incontinence. The degree of continence did not improve and the external sphincter function did not increase significantly. Their results can be attributed to the age range they included
7 Reda S.M. Sarhan & Enas El-Sayed 127 which was very wide being years. Also, they studied the effect of biofeedback on neurogenic fecal incontinence in general whatever the cause which may include aging causes. The results of the present study were not also in agreement with those of Brazelli and Griffiths [25] who reported that, in a randomized controlled study, bio-feedback plus behavioral management was compared to behavioral management alone in children with fecal incontinence due to MMC. Both study and control groups displayed significant improvement, suggesting that bio-feedback has the same effects as behavioral management for most children with MMC. However, it must be stressed that patients with spinal cord defects show commonly worst responses to bio-feedback than patients with incontinence due to other causes. Conculosin: This study demonstrated that biofeedback training program is an effective tool in improving bowel continence parameters in children with MMC. It is recommended that biofeedback therapy in combination with conventional physical therapy are essential treatment for patients with fecal incontinence. References 1- ALATISE O., ADEOLU A. and KOMOLAFE E.: Pattern and factors affecting management outcome of spina bifida cystica in ile-life. Nigeria Pediatr Neurosurg, 42 (5): , COURTNEY A., ROWLAND A., CRAGAN J. and CLIN- TON A.: Are Encephalocede Neural Tube Defects?. Off. J. Am. Acad Paediatr., 13: 1-, MAIN D. and MENNUTI M.: Neural tube defects: Issues in prenatal diagnosis and counseling. Obstet. Gynecol., 67: 1-16, EMAS T.: Spina Bifida. In: Tecklin J, editor. Pediatric Physical Therapy. 4 th ed, NewYork, Lippoincott Williams & Wilkins, pp 231, NJAMNSHI A., DJIENTCHEU V., LEKOUBOU A., GUEMSE M., OBAMA M., MBU R., TAKONGMO S. and KAGO I.: Neural Tube Defects are Rare Among Black Americans but not in Sub-Saharan Black Africans: The case of Yaounde-Cameroon. J. Neurological Sciences, 27 (1-2): 13-17, TANNE J.: US study shows that folic acid fortification decreases neural tube defects. BMJ, 331: 594, SIVAL D., VERBEEK R., BROUWER O., SOLLIE K., BOS A. and DUNNEN W.: Spinal hemorrhages are associated with early neonatal motor function loss in human spina bifida aperta. Early Human Development, 84 (7): , PONTICELLI A., IACOBELLI B., SILVERI M., BROGGI G., RIVOSECCHI M. and Gennaro M.: Colorectal dysfunction and fecal incontinence in children with spina bifida. BJUI, 81 (3): 117-9, DOBBEN A., TERRA M., BERGHMANS B., DEU- TEKOM M., BOECKXSTAENS G., JANSSEN L., BOSSUYT P. and STOKER J.: Functional changes after physiotherapy in fecal incontinence. International J. Colorectal Dis., 21 (6): , SEONG M.: Diagnosis and Management of Fecal Incontinence. J. Korean Soc. Coloproctol., 23 (5): , WONG A., KRAVARUSIC D. and WONG S.: Impact of cecostomy and antegrade colonic enemas on management of fecal incontinence and constipation ten years of experience in pediatric population. J. Ped. Sur., 43 (8): , CHIARIONI G. and WHITEHEAD W.: The role of biofeedback in the treatment of gastrointestinal disorders. NCP Gastroenterology & Hepatology, 5: , NORTON C., CODY J. and HOSKER G.: Biofeedback and/or sphincter exercises for the treatment of fecal incontinence in adults. Cochrane Database of Systematic Reviews, 3:.2/ CD2111, KELLY J.: The clinical and radiological assessment of anal continence in childhood. ANZ Journal of Surgery, 42 (1): 62-3, HENRY M. and SWASH M.: Coloproctology and the Pelvic Floor. London, Butterworth, pp 46, SULTAN A., KAMM M., HUDSON C., THOMAS J., and BARTRAM C.: Anal-Sphincter Disruption during Vaginal Delivery. N. Engl. J. Med., 329 (26): , MØRKVED S., BØ K., SCHEI B. and SALVESEN K.: Pelvic floor muscle training during pregnancy to prevent urinary incontinence: A single-blind randomized controlled trial. Obstet. Gynecol., 1 (2): , MARQUES G., MARTINS J. and Nobre V.: Comparison between perfusion and balloon techniques for performing anorectal manometry in children with intestinal constipation. Acta Cir. Bras., 23 (5): 45-11, JENSEN L.: Fecal Incontinence: Evaluation and treatment. JWOCN, 24 (5): , TERRA M., DOBBEN A., BERGHMANS B., DEU- TEKOM M., BAETEN C., JANSSEN L., BOECKXS- TAENS G., ENGEL A., FELT-BERSMA R. and SLORS J.: Electrical stimulation and pelvic floor muscle training with biofeedback in patients with fecal incontinence: A Cohort of 281 Patients. Dis. Colon Rectum, 49 (8): , WHITEHEAD W.: Biofeedback treatment of fecal incontinence. South Med. J., 85: , NORTON C. and KAMM M.: Anal sphincter biofeedback and pelvic floor exercises for fecal incontinence in adults a systematic review. Aliment Pharmacol. Ther., 15 (8): , SOLOMON M., PAGER C., REX J., ROBERTS R. and MANNING J.: Randomized controlled trial of biofeedback with anal manometry, transanal ultrasound, or pelvic floor retraining with digital guidance alone in the treatment of mild to moderate fecal incontinence. Dis. Colon Rectum, 46: 73-, VAN TETS W., KUIJPERS J. and BLEIJENBER G.: Biofeedback treatment is ineffective in neurogenic fecal incontinence. Dis. Colon Rectum, 39 (9): 992-4, BRAZELLI M. and GRIFFITHS P.: Behavioural and cognitive interventions with or without other treatments for the management of fecal incontinence in children. Cochrane Database of Systematic Reviews, 19 (2): Art. No., CD224, 26.
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Anorectal Diagnostic Overview
 Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
PREPARING FOR ANORECTOAL MANOMETRY. ManoScan Anorectal Manometry System
 PREPARING FOR ANORECTOAL MANOMETRY ManoScan Anorectal Manometry System WHAT IS ANORECTAL MANOMETRY? Anorectal manometry is a test used to evaluate the function and coordination of the sphincter and pelvic
PREPARING FOR ANORECTOAL MANOMETRY ManoScan Anorectal Manometry System WHAT IS ANORECTAL MANOMETRY? Anorectal manometry is a test used to evaluate the function and coordination of the sphincter and pelvic
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function
 Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Populations Interventions Comparators Outcomes Individuals: With fecal incontinence
 Protocol Biofeedback as a Treatment of Fecal Incontinence or Constipation (20164) Medical Benefit Effective Date: 07/01/13 Next Review Date: 03/19 Preauthorization No Review Dates: 09/07, 09/08, 09/09,
Protocol Biofeedback as a Treatment of Fecal Incontinence or Constipation (20164) Medical Benefit Effective Date: 07/01/13 Next Review Date: 03/19 Preauthorization No Review Dates: 09/07, 09/08, 09/09,
Biofeedback for Pelvic Floor Disorders and Incontinence
 The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
Biofeedback as a Treatment of Fecal Incontinence or Constipation
 Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: 2.01.64 Last Review: 7/2014 Origination: 7/2008 Next Review: 7/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue
Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: 2.01.64 Last Review: 7/2014 Origination: 7/2008 Next Review: 7/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue
Langley Catheter Protocols
 Langley Catheter Protocols Stericom Ltd Units 1&2 Higham Mead Chesham HP5 2AH England Tel: +44 (0)1494 794315 Fax: +44 (0)1494 772759 info@stericom.com www.stericom.com Instructions for use The 2-balloon
Langley Catheter Protocols Stericom Ltd Units 1&2 Higham Mead Chesham HP5 2AH England Tel: +44 (0)1494 794315 Fax: +44 (0)1494 772759 info@stericom.com www.stericom.com Instructions for use The 2-balloon
MEDICAL POLICY SUBJECT: BIOFEEDBACK
 MEDICAL POLICY PAGE: 1 OF: 6 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 6 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
Biofeedback as a Treatment of Fecal Incontinence or Constipation
 Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: 2.01.64 Last Review: 7/2018 Origination: 7/2008 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: 2.01.64 Last Review: 7/2018 Origination: 7/2008 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
A Case of Fecal Incontinence: Medical and Interventional Treatment Options
 A Case of Fecal Incontinence: Medical and Interventional Treatment Options HPI JP is a 69 year-old F with a 12-month history of FI. Her symptoms began after a colonoscopy She has been experiencing passive
A Case of Fecal Incontinence: Medical and Interventional Treatment Options HPI JP is a 69 year-old F with a 12-month history of FI. Her symptoms began after a colonoscopy She has been experiencing passive
MCOMPASS ANAL MANOMETRY AN OVERVIEW
 MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
REF PERINEOMETER (BIOFEEDBACK MONITOR) FOR FECAL INCONTINENCE AND KEGEL EXERCISES SEE INSTRUCTIONS FOR USE INSTRUCTION MANUAL
 REF 18-1005 PERINEOMETER (BIOFEEDBACK MONITOR) FOR FECAL INCONTINENCE AND KEGEL EXERCISES SEE INSTRUCTIONS FOR USE INSTRUCTION MANUAL TABLE OF CONTENTS Introduction...................... 1 Monitor 5 Device
REF 18-1005 PERINEOMETER (BIOFEEDBACK MONITOR) FOR FECAL INCONTINENCE AND KEGEL EXERCISES SEE INSTRUCTIONS FOR USE INSTRUCTION MANUAL TABLE OF CONTENTS Introduction...................... 1 Monitor 5 Device
Function of the anal sphincters in patients with
 Function of the anal sphincters in patients with intussusception of the rectum B. FRENCKNER AND T. IHRE Gut, 1976,17, 147-151 From the Department of Clinical Physiology and the Department of Surgery, Serafimer
Function of the anal sphincters in patients with intussusception of the rectum B. FRENCKNER AND T. IHRE Gut, 1976,17, 147-151 From the Department of Clinical Physiology and the Department of Surgery, Serafimer
Human Anatomy rectum
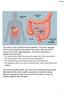 rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
mcompass Interpretation Quick Reference Guide
 mcompass Interpretation Quick Reference Guide This document is designed to give you a starting point for reviewing of the mcompass anorectal manometry results. By no means are these the only questions
mcompass Interpretation Quick Reference Guide This document is designed to give you a starting point for reviewing of the mcompass anorectal manometry results. By no means are these the only questions
Bowel Management for Children with Anorectal Malformations by Kathleen Guardino, RN, MSN
 Bowel Management for Children with Anorectal Malformations by Kathleen Guardino, RN, MSN Dr. Alberto Peña, Chief of Surgery at Schneider Children's Hospital created the posterior sagittal anorectoplasty
Bowel Management for Children with Anorectal Malformations by Kathleen Guardino, RN, MSN Dr. Alberto Peña, Chief of Surgery at Schneider Children's Hospital created the posterior sagittal anorectoplasty
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
Saint-Petersburg State Pediatric Medical University, Saint-Petersburg, Russia
 Saint-Petersburg State Pediatric Medical University, Saint-Petersburg, Russia Modern technologies in treatment of fecal incontinence in children Komissarov Igor Alexeevich- Ph.D, M.D, Prof. Kolesnikova
Saint-Petersburg State Pediatric Medical University, Saint-Petersburg, Russia Modern technologies in treatment of fecal incontinence in children Komissarov Igor Alexeevich- Ph.D, M.D, Prof. Kolesnikova
Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests
 Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Biofeedback as a Treatment of Fecal Incontinence or Constipation
 2.01.64 Biofeedback as a Treatment of Fecal Incontinence or Constipation Section 2.0 Medicine Subsection Effective Date February 15, 2015 Original Policy Date December 15, 2014 Next Review Date December
2.01.64 Biofeedback as a Treatment of Fecal Incontinence or Constipation Section 2.0 Medicine Subsection Effective Date February 15, 2015 Original Policy Date December 15, 2014 Next Review Date December
Sphincter exercises for people with bowel control problems. Information for patients. Physiotherapy Department
 Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Duc M. Vo, MD, FACS Northwest Surgical Specialists
 Duc M. Vo, MD, FACS Northwest Surgical Specialists Disclosures none Outline Definition Etiologies Exam findings Additional testing Medical management Surgical options What is fecal incontinence? Recurrent
Duc M. Vo, MD, FACS Northwest Surgical Specialists Disclosures none Outline Definition Etiologies Exam findings Additional testing Medical management Surgical options What is fecal incontinence? Recurrent
CONSTIPATION. Atan Baas Sinuhaji
 CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
3D Dynamic Ultrasound In Obstructed Defecation
 3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
Neurogenic Bowel: What You Should Know. A Guide for People with Spinal Cord Injury
 Neurogenic Bowel: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about bowel movements After SCI, you may need more
Neurogenic Bowel: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about bowel movements After SCI, you may need more
Biofeedback provides long term benefit for patients with intractable, slow and normal transit constipation
 Gut 1998;42:517 521 517 St Mark s Hospital, London, UK E Chiotakakou-Faliakou M A Kamm AJRoy J B Storrie I C Turner Correspondence to: Dr M A Kamm, St Mark s Hospital, Northwick Park, Watford Road, Harrow,
Gut 1998;42:517 521 517 St Mark s Hospital, London, UK E Chiotakakou-Faliakou M A Kamm AJRoy J B Storrie I C Turner Correspondence to: Dr M A Kamm, St Mark s Hospital, Northwick Park, Watford Road, Harrow,
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 4 October, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.4.532 How to Interpret
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 4 October, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.4.532 How to Interpret
MCOMPASS ANAL MANOMETRY AN OVERVIEW
 MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
Peristeen and the Neurogenic Bowel Dysfunction Score (NBD) for pediatric patients with spina bifida
 Peristeen and the Neurogenic Bowel Dysfunction Score (NBD) for pediatric patients with spina bifida Coloplast develops products and services that make life easier for people with very personal and private
Peristeen and the Neurogenic Bowel Dysfunction Score (NBD) for pediatric patients with spina bifida Coloplast develops products and services that make life easier for people with very personal and private
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
1. What evidence exists that prevention of constipation in the first year of life improves outcome of bowel management in later childhood?
 BOWEL FUNCTION AND CARE Overall Outcomes Primary Outcomes o Maintenance of social continence as appropriate for age level Secondary Outcomes o Maximization of independence with managing bowel program o
BOWEL FUNCTION AND CARE Overall Outcomes Primary Outcomes o Maintenance of social continence as appropriate for age level Secondary Outcomes o Maximization of independence with managing bowel program o
encathopedia Volume 8 NEUROGENIC BOWEL DYSFUNCTION AND TAI
 encathopedia Volume 8 NEUROGENIC BOWEL DYSFUNCTION AND TAI Neurogenic Bowel Dysfunction Neurogenic Bowel Dysfunction (NBD) is when the bowel does not work properly due to loss of normal sensory or motor
encathopedia Volume 8 NEUROGENIC BOWEL DYSFUNCTION AND TAI Neurogenic Bowel Dysfunction Neurogenic Bowel Dysfunction (NBD) is when the bowel does not work properly due to loss of normal sensory or motor
Medical Policy. MP Biofeedback as a Treatment of Fecal Incontinence or Constipation
 Medical Policy MP 2.01.64 BCBSA Ref. Policy: 2.01.64 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.27 Biofeedback as a Treatment of Urinary Incontinence in
Medical Policy MP 2.01.64 BCBSA Ref. Policy: 2.01.64 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.27 Biofeedback as a Treatment of Urinary Incontinence in
Biofeedback has been reported to be an effective treatment
 ORIGINAL CONTRIBUTION Randomized Controlled Trial Shows Biofeedback to be Superior to Pelvic Floor Exercises for Fecal Incontinence Steve Heymen, Ph.D. Yolanda Scarlett, M.D. Kenneth Jones, Ph.D. Yehuda
ORIGINAL CONTRIBUTION Randomized Controlled Trial Shows Biofeedback to be Superior to Pelvic Floor Exercises for Fecal Incontinence Steve Heymen, Ph.D. Yolanda Scarlett, M.D. Kenneth Jones, Ph.D. Yehuda
Lets talk about Faecal incontinence (FI) in Scleroderma
 Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
SACRAL NERVE STIMULATION FOR EXPERIENCE IN CHILDREN
 SACRAL NERVE STIMULATION FOR COLORECTAL DISEASES: EXPERIENCE IN CHILDREN C. LOUIS-BORRIONE - JM. GUYS TIMONE-ENFANTS MARSEILLE SACRAL NEUROMODULATION IN CHILDREN 26 : Humphreys et al - 23 children with
SACRAL NERVE STIMULATION FOR COLORECTAL DISEASES: EXPERIENCE IN CHILDREN C. LOUIS-BORRIONE - JM. GUYS TIMONE-ENFANTS MARSEILLE SACRAL NEUROMODULATION IN CHILDREN 26 : Humphreys et al - 23 children with
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
Chapter 31 Bowel Elimination
 Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Controlled randomised trial of visual biofeedback
 Gut 1995; 37: 95-99 Service de Medecine C, CHG de F6camp, 764 F6camp, France D Koutsomanis St Mark's Hospital, London EC1V 2PS J E Lennard-Jones A J Roy M A Kamm Correspondence to: Professor J E Lennard-Jones,
Gut 1995; 37: 95-99 Service de Medecine C, CHG de F6camp, 764 F6camp, France D Koutsomanis St Mark's Hospital, London EC1V 2PS J E Lennard-Jones A J Roy M A Kamm Correspondence to: Professor J E Lennard-Jones,
Bowel Function and Care. Pat Beierwaltes, Chair Paige Church Lusine Ambartsumyan Sharon Braille Julie Dicker Tiffany Gordon Sue Liebold
 Bowel Function and Care Pat Beierwaltes, Chair Paige Church Lusine Ambartsumyan Sharon Braille Julie Dicker Tiffany Gordon Sue Liebold Outcomes Primary Outcomes Maintenance of social continence as appropriate
Bowel Function and Care Pat Beierwaltes, Chair Paige Church Lusine Ambartsumyan Sharon Braille Julie Dicker Tiffany Gordon Sue Liebold Outcomes Primary Outcomes Maintenance of social continence as appropriate
Faecal Incontinence Information Leaflet THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P.
 UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
Research Article Pelvic Muscle Rehabilitation: A Standardized Protocol for Pelvic Floor Dysfunction
 Advances in Urology, Article ID 487436, 7 pages http://dx.doi.org/1155/2014/487436 Research Article Pelvic Muscle Rehabilitation: A Standardized Protocol for Pelvic Floor Dysfunction Rodrigo Pedraza, 1,2
Advances in Urology, Article ID 487436, 7 pages http://dx.doi.org/1155/2014/487436 Research Article Pelvic Muscle Rehabilitation: A Standardized Protocol for Pelvic Floor Dysfunction Rodrigo Pedraza, 1,2
Application of Anorectal Dynamics in the Treatment of Colon Disease Packing
 Application of Anorectal Dynamics in the Treatment of Colon Disease Packing Zongyue Gao 1, 2, a, Yuyan Liu 1, 2, b, Chunxia Wan 1, 2, c 3, d* and Xiaoli Zhou 1 Henan Province Hospital of TCM, 450000, Henan,
Application of Anorectal Dynamics in the Treatment of Colon Disease Packing Zongyue Gao 1, 2, a, Yuyan Liu 1, 2, b, Chunxia Wan 1, 2, c 3, d* and Xiaoli Zhou 1 Henan Province Hospital of TCM, 450000, Henan,
Constipation. Information for adults. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
 Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Efficacy of Peristeen transanal irrigation system for neurogenic bowel in the pediatric population: Preliminary findings
 Efficacy of Peristeen transanal irrigation system for neurogenic bowel in the pediatric population: Preliminary findings Tiffany Gordon, MSN, RN, CRRN, CPN David Vandersteen, MD John Belew RN, PhD Gillette
Efficacy of Peristeen transanal irrigation system for neurogenic bowel in the pediatric population: Preliminary findings Tiffany Gordon, MSN, RN, CRRN, CPN David Vandersteen, MD John Belew RN, PhD Gillette
A Nursing Assessment Tool for Adults With Fecal Incontinence
 Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
A guide to Anoplasty (anal surgery)
 Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
ACG Clinical Guideline: Management of Benign Anorectal Disorders
 ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
Female Urinary Incontinence: What It Is and What You Can Do About It
 Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Accidental Bowel Leakage (Fecal Incontinence)
 Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Bowel dysfunctions following hysterectomy
 Bowel dysfunctions following hysterectomy Marco Scaglia Retrospective studies Retrospective studies 6% of patients developed new symptoms (Carlson 1994) Constipation is more common in women after hysterectomy
Bowel dysfunctions following hysterectomy Marco Scaglia Retrospective studies Retrospective studies 6% of patients developed new symptoms (Carlson 1994) Constipation is more common in women after hysterectomy
Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands
 Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands Constipation 0-10% >10-20% >20-30% >30-40% Mugie SM, et al. Best Pract & Res Clin Gastroenterol
Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands Constipation 0-10% >10-20% >20-30% >30-40% Mugie SM, et al. Best Pract & Res Clin Gastroenterol
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National
 Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National What is Bowel and Bladder Dysfunction? Lower urinary tract symptoms (LUTS) and bowel movement disorders Majority
Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National What is Bowel and Bladder Dysfunction? Lower urinary tract symptoms (LUTS) and bowel movement disorders Majority
Physical Therapy. Pelvic Floor Physical Therapy for Gastrointestinal Conditions. Objectives: Upon completion, participants will be able to:
 Pelvic Floor Physical Therapy for Gastrointestinal Conditions By Meghan Z. Markowski, PT, DPT, WCS, BCB-PMD Brigham and Women s s Hospital Department of Rehabilitation Services 850 Boylston Street, Suite
Pelvic Floor Physical Therapy for Gastrointestinal Conditions By Meghan Z. Markowski, PT, DPT, WCS, BCB-PMD Brigham and Women s s Hospital Department of Rehabilitation Services 850 Boylston Street, Suite
Fecal Incontinence. Inability to retain feces or bowel movements, resulting in involuntary passage of feces or bowel movements
 Fecal Incontinence (Involuntary Passage of Feces or Bowel Movements) Basics OVERVIEW Inability to retain feces or bowel movements, resulting in involuntary passage of feces or bowel movements GENETICS
Fecal Incontinence (Involuntary Passage of Feces or Bowel Movements) Basics OVERVIEW Inability to retain feces or bowel movements, resulting in involuntary passage of feces or bowel movements GENETICS
11/04/2011 OVERVIEW. Neurogenic Bowel Management. in adults with Spinal Cord Injury (S.C.I.) Sequence of events in normal Defecation
 Neurogenic Bowel Management in adults with Spinal Cord Injury (S.C.I.) Dimitrios D. Ergeletzis MD Physiatrist Director of Physical Medicine & Rehabilitation Dept.- GIROKOMEION ATHENS, Greece OVERVIEW Anatomy
Neurogenic Bowel Management in adults with Spinal Cord Injury (S.C.I.) Dimitrios D. Ergeletzis MD Physiatrist Director of Physical Medicine & Rehabilitation Dept.- GIROKOMEION ATHENS, Greece OVERVIEW Anatomy
Physiotherapy Management for Faecal Incontinence in Children. Amy Chung MSSc, Dip. (Acupuncture), P.D.PT 19 Sept 2009
 Physiotherapy Management for Faecal Incontinence in Children Amy Chung MSSc, Dip. (Acupuncture), P.D.PT 19 Sept 2009 Contents Introduction Overview of physiotherapy management Local experience - Continence
Physiotherapy Management for Faecal Incontinence in Children Amy Chung MSSc, Dip. (Acupuncture), P.D.PT 19 Sept 2009 Contents Introduction Overview of physiotherapy management Local experience - Continence
Progress in Biofeedback Conditioning for
 GASTROENTEROLOGY 76:742-746, 1979 Progress in Biofeedback Conditioning for Fecal Incontinence M. A. CERULLI, P. NIKOOMANESH, and M. M. SCHUSTER Department of Medicine, Division of Gastroenterology, Baltimore
GASTROENTEROLOGY 76:742-746, 1979 Progress in Biofeedback Conditioning for Fecal Incontinence M. A. CERULLI, P. NIKOOMANESH, and M. M. SCHUSTER Department of Medicine, Division of Gastroenterology, Baltimore
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury
 The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
Randomised controlled trial of biofeedback training in persistent encopresis with anismus
 Arch Dis Child 1998;79:131 135 131 Clinical Epidemiology and Biostatistics Unit, Melbourne University Department of Paediatrics, Royal Children s Hospital, Parkville Victoria, Australia 3052 T Nolan Department
Arch Dis Child 1998;79:131 135 131 Clinical Epidemiology and Biostatistics Unit, Melbourne University Department of Paediatrics, Royal Children s Hospital, Parkville Victoria, Australia 3052 T Nolan Department
Novel Options for the Management of Fecal Incontinence
 Novel Options for the Management of Fecal Incontinence Arnold Wald, MD, MACG University of Wisconsin School of Medicine and Public Health, Madison WI ANORECTAL CONTINENCE MECHANISMS Reservoir Elements
Novel Options for the Management of Fecal Incontinence Arnold Wald, MD, MACG University of Wisconsin School of Medicine and Public Health, Madison WI ANORECTAL CONTINENCE MECHANISMS Reservoir Elements
Common Gastrointestinal Problems in the Elderly
 Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
NIH Public Access Author Manuscript Best Pract Res Clin Gastroenterol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: Best Pract Res Clin Gastroenterol. 2011 February ; 25(1): 159 166. doi:10.1016/j.bpg.2011.01.004. BIOFEEDBACK THERAPY FOR CONSTIPATION
NIH Public Access Author Manuscript Published in final edited form as: Best Pract Res Clin Gastroenterol. 2011 February ; 25(1): 159 166. doi:10.1016/j.bpg.2011.01.004. BIOFEEDBACK THERAPY FOR CONSTIPATION
Anorectal physiology test
 Anorectal physiology test We hope this factsheet will help to answer some of your questions about having an anorectal physiology test. If you have any further questions or concerns, please don t hesitate
Anorectal physiology test We hope this factsheet will help to answer some of your questions about having an anorectal physiology test. If you have any further questions or concerns, please don t hesitate
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
B l a d d e r & B o w e l C a r e. For Patients with Spinal Cord Injuries
 B l a d d e r & B o w e l C a r e For Patients with Spinal Cord Injuries 1 Bladder Specific Care Intermittent Catheterization (IC) is used to empty the bladder with a catheter. A catheter is a tube that
B l a d d e r & B o w e l C a r e For Patients with Spinal Cord Injuries 1 Bladder Specific Care Intermittent Catheterization (IC) is used to empty the bladder with a catheter. A catheter is a tube that
Increased motor unit fibre density in the external
 Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 343-347 Increased motor unit fibre density in the external anal sphincter muscle in ano-rectal incontinence: a single fibre EMG study M E NEILL
Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 343-347 Increased motor unit fibre density in the external anal sphincter muscle in ano-rectal incontinence: a single fibre EMG study M E NEILL
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
ANMS-ESNM position paper and consensus guidelines on biofeedback therapy for anorectal disorders
 Neurogastroenterology & Motility Neurogastroenterol Motil (2015) 27, 594 609 doi: 10.1111/nmo.12520 POSITION PAPER ANMS-ESNM position paper and consensus guidelines on therapy for anorectal disorders S.
Neurogastroenterology & Motility Neurogastroenterol Motil (2015) 27, 594 609 doi: 10.1111/nmo.12520 POSITION PAPER ANMS-ESNM position paper and consensus guidelines on therapy for anorectal disorders S.
Measurement of anal pressure and motility
 Measurement of anal pressure and motility B. D. HANCOCK' From the University Hospital of South Manchester Gut, 1976, 17, 645-651 SUMMARY A fine open perfused system and a closed balloon system for the
Measurement of anal pressure and motility B. D. HANCOCK' From the University Hospital of South Manchester Gut, 1976, 17, 645-651 SUMMARY A fine open perfused system and a closed balloon system for the
Chapter 8. Pediatric Surgery
 Chapter 8 Pediatric Surgery 8.1 Hydrocephalus Hydrocephalus is a congenital disorder. There may be difficulties during normal vaginal delivery due large size of the head. In 1970s, when these pictures
Chapter 8 Pediatric Surgery 8.1 Hydrocephalus Hydrocephalus is a congenital disorder. There may be difficulties during normal vaginal delivery due large size of the head. In 1970s, when these pictures
Hemorrhoids. Carlos R. Alvarez-Allende PGY-III Colorectal Surgery
 Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
Anorectal manometry results in defecation disorders
 Archives of Disease in Childhood, 1983, 58, 257-261 Anorectal manometry results in defecation disorders D MOLNAR, L S TAITZ, 0 M URWIN, AND J K H WALES Department of Paediatrics, University of Sheffield,
Archives of Disease in Childhood, 1983, 58, 257-261 Anorectal manometry results in defecation disorders D MOLNAR, L S TAITZ, 0 M URWIN, AND J K H WALES Department of Paediatrics, University of Sheffield,
The Digestive System or tract extends from the mouth to the anus.
 The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
Bowel Function After Spinal Cord Injury
 Bowel Function After Spinal Cord Injury A resource for individuals with SCI and their supporters This presentation is based on SCI Model Systems research and was developed with support from the National
Bowel Function After Spinal Cord Injury A resource for individuals with SCI and their supporters This presentation is based on SCI Model Systems research and was developed with support from the National
Minimum standards of anorectal manometry
 Neurogastroenterol. Mot. (22) 14, 553 559 Minimum standards of anorectal manometry S. S. C. RAO, F. AZPIROZ,* N. DIAMANT, P. ENCK,à G. TOUGAS & A. WALD University of Iowa, Iowa City, USA; *Hospital General
Neurogastroenterol. Mot. (22) 14, 553 559 Minimum standards of anorectal manometry S. S. C. RAO, F. AZPIROZ,* N. DIAMANT, P. ENCK,à G. TOUGAS & A. WALD University of Iowa, Iowa City, USA; *Hospital General
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Crucial Role of Rectoanal Inhibitory Reflex in Emptying Function After Anoplasty in Infants with Anorectal Malformations
 Original Article Crucial Role of Rectoanal Inhibitory Reflex in Emptying Function After Anoplasty in Infants with Anorectal Malformations Surasak Sangkhathat, Sakda Patrapinyokul and Noppawan Osatakul,
Original Article Crucial Role of Rectoanal Inhibitory Reflex in Emptying Function After Anoplasty in Infants with Anorectal Malformations Surasak Sangkhathat, Sakda Patrapinyokul and Noppawan Osatakul,
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION. Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital
 ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
Long-Term Bowel Symptoms Following Corrective Surgery
 HIRSCHSPRUNG'S DISEASE Samuel Nurko MD MPH Center for Motility and Functional Gastrointestinal Disorders Children s Hospital Medical Center, Boston Ma Long-Term Bowel Symptoms Following Corrective Surgery
HIRSCHSPRUNG'S DISEASE Samuel Nurko MD MPH Center for Motility and Functional Gastrointestinal Disorders Children s Hospital Medical Center, Boston Ma Long-Term Bowel Symptoms Following Corrective Surgery
Bowel Dysfunction in Neurological Disease Best Practice in an Evolving Disorder
 Bowel Dysfunction in Neurological Disease Best Practice in an Evolving Disorder Anton Emmanuel October 2016 National Hospital for Neurology & Neurosurgery Regulation of colonic function Brain gut axis
Bowel Dysfunction in Neurological Disease Best Practice in an Evolving Disorder Anton Emmanuel October 2016 National Hospital for Neurology & Neurosurgery Regulation of colonic function Brain gut axis
Prescribing Guidance for the Treatment of Constipation in Children
 Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
New Advances in Biofeedback. Brigitte Fung Physiotherapist Kwong Wah Hospital
 New Advances in Biofeedback Brigitte Fung Physiotherapist Kwong Wah Hospital Content What is biofeedback Types of biofeedback Uses of biofeedback in UI Uses of Biofeedback in FI & Constipation What is
New Advances in Biofeedback Brigitte Fung Physiotherapist Kwong Wah Hospital Content What is biofeedback Types of biofeedback Uses of biofeedback in UI Uses of Biofeedback in FI & Constipation What is
Developing spinal cord compression care guidelines at WPH
 Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Bernie Foran, Suzanne Hodson, Jane Mason, Rebecca Mills, Jan Siddall, Rebecca Walsh, Clare
Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Bernie Foran, Suzanne Hodson, Jane Mason, Rebecca Mills, Jan Siddall, Rebecca Walsh, Clare
Patient Information Leaflet
 Patient Information Leaflet Background Faecal incontinence is a common health problem, affecting over 1% of community-dwelling adults (1;2). Chronic constipation may affect 3-5% of the population depending
Patient Information Leaflet Background Faecal incontinence is a common health problem, affecting over 1% of community-dwelling adults (1;2). Chronic constipation may affect 3-5% of the population depending
The pelvic floor is a system of muscles, ligaments, and tissues that keep your pelvic organs firmly in place.
 The pelvic floor is a system of muscles, ligaments, and tissues that keep your pelvic organs firmly in place. Think of it as the hammock of muscle that holds up your uterus, vagina, bladder, small intestine,
The pelvic floor is a system of muscles, ligaments, and tissues that keep your pelvic organs firmly in place. Think of it as the hammock of muscle that holds up your uterus, vagina, bladder, small intestine,
from Bowel Control Problems twitter.com/voicesforpfd
 BREAK FREE from Bowel Control Problems POP Quiz THE NUMBER OF PEOPLE IN THE UNITED STATES WITH BOWEL CONTROL PROBLEMS: A. 6 million B. 12 million C. 18 million BOWEL CONTROL PROBLEMS Nearly 18 million
BREAK FREE from Bowel Control Problems POP Quiz THE NUMBER OF PEOPLE IN THE UNITED STATES WITH BOWEL CONTROL PROBLEMS: A. 6 million B. 12 million C. 18 million BOWEL CONTROL PROBLEMS Nearly 18 million
ANAL SPHINCTER PRESSURE CHARACTERISTICS
 GASTROENTEROLOGY Copyright 1967 by The Williams & Wilkins Co. Vol. 52, No.3 Printed in U.S.A. ANAL SPHINCTER PRESSURE CHARACTERISTICS LEONARD A. KATZ, M.D., HERBERT J. KAUFMANN, M.D., AND HOWARD M. SPIRO,
GASTROENTEROLOGY Copyright 1967 by The Williams & Wilkins Co. Vol. 52, No.3 Printed in U.S.A. ANAL SPHINCTER PRESSURE CHARACTERISTICS LEONARD A. KATZ, M.D., HERBERT J. KAUFMANN, M.D., AND HOWARD M. SPIRO,
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 24 The Digestive System Introduction The purpose of this chapter is to Identify the anatomical components of the digestive system as well as their
Principles of Anatomy and Physiology 14 th Edition CHAPTER 24 The Digestive System Introduction The purpose of this chapter is to Identify the anatomical components of the digestive system as well as their
UNDERSTANDING IBS AND CC Implications for diagnosis and management
 UNDERSTANDING IBS AND CC Implications for diagnosis and management J. TACK, M.D., Ph.D. Department of Gastroenterology University Hospitals, K.U. Leuven Leuven, Belgium TYPES OF GASTROINTESTINAL DISORDERS
UNDERSTANDING IBS AND CC Implications for diagnosis and management J. TACK, M.D., Ph.D. Department of Gastroenterology University Hospitals, K.U. Leuven Leuven, Belgium TYPES OF GASTROINTESTINAL DISORDERS
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Continence/Constipation Workshop for RNs in Long-Term Care
 Continence/Constipation Workshop for RNs in Long-Term Care Slide Presentation Supporting Implementation of the RNAO BPGs: Promoting Continence Using Prompted Voiding and Prevention of Constipation in the
Continence/Constipation Workshop for RNs in Long-Term Care Slide Presentation Supporting Implementation of the RNAO BPGs: Promoting Continence Using Prompted Voiding and Prevention of Constipation in the
