Papers. Abstract. Introduction. Methods
|
|
|
- Jayson Griffin
- 5 years ago
- Views:
Transcription
1 Conservative management of persistent postnatal urinary and faecal incontinence: randomised controlled trial Topic: 66;68;159;161 Cathryn M A Glazener, G Peter Herbison, P Don Wilson, Christine MacArthur, Gordon D Lang, Harry Gee, Adrian M Grant Abstract Objectives To assess the effect of nurse assessment with reinforcement of pelvic floor muscle training exercises and bladder training compared with standard management among women with persistent incontinence three months postnatally. Design Randomised controlled trial with nine months follow up. Setting Community intervention in three centres (Dunedin, New Zealand; Birmingham; Aberdeen). Participants 747 women with urinary incontinence three months postnatally, allocated at random to intervention (371) or control (376) groups. Intervention Assessment by nurses of urinary incontinence with conservative advice on pelvic floor exercises at five, seven, and nine months after delivery supplemented with bladder training if appropriate at seven and nine months. Main outcome measures Primary: persistence and severity of urinary incontinence 12 months after delivery. Secondary: performance of pelvic floor exercises, change in coexisting faecal incontinence, wellbeing, anxiety, and depression. Results Women in the intervention group had significantly less urinary incontinence: 167/279 (59.9%) v 169/245 (69.0%), difference 9.1% (95% confidence interval 1.0% to 17.3%, P = 0.037) for any incontinence and 55/279 (19.7%) v 78/245 (31.8%), difference 12.1% (4.7% to 19.6%, P = 0.002) for severe incontinence. Faecal incontinence was also less common: 12/273 (4.4%) v 25/237 (10.5%), difference 6.1% (1.6% to 10.8%, P = 0.012). At 12 months women in the intervention group were more likely to be performing pelvic floor exercises (218/278 (79%) v 118/244 (48%), P < 0.001). Conclusions A third of women may have some urinary incontinence three months after childbirth. Conservative management provided by nurses seems to reduce the likelihood of urinary and coexisting faecal incontinence persisting 12 months postpartum. Further trials for faecal incontinence are needed. Introduction Incontinence is a common and distressing problem after childbirth. Three months after delivery 20-30% of women have urinary incontinence 1 3 and about 4% have faecal incontinence. 45 Despite the extent of the problem, there is little evidence on which to base best management. Conservative treatments, centring on retraining the pelvic floor musculature, have been shown to be effective among older women with stress incontinence. 67 However, in one of the few trials that included postpartum women, Sleep and Grant found no reduction three months after delivery for women in whom the use of postnatal pelvic floor exercises was reinforced compared with standard management given to all women who have recently given birth. 8 This finding, together with electrophysiological evidence of spontaneous nerve recovery during this period, 9 suggested that targeting women with persistent incontinence would be more effective. 10 We developed an assessment and management intervention with nurses, based on the model successfully tested by O Brien and colleagues in a mixed community based population of older women. 11 We tested its use in a pilot study. 10 We then carried out a randomised controlled trial to examine the effect on incontinence at 12 months in women who had urinary incontinence three months after childbirth. Methods Approval was obtained from the research ethics committees in each of the three centres. Women living within a 50 km (30 mile) radius and who delivered in these units during a 12 month recruitment period were contacted by post three months after delivery (October 1993 to September 1994). They were asked to complete a questionnaire about urinary and faecal incontinence, associated symptoms, and other health issues. We did not approach women whose babies were stillborn or died as neonates. We used a slightly modified version of the questionnaire tested in the preceding pilot study. 10 We invited women who had urinary incontinence in the preceding month (defined as any involuntary Health Services Research Unit, Aberdeen, Polwarth Building, Foresterhill, Aberdeen, AB25 2ZD CathrynMA Glazener senior clinical research fellow Adrian M Grant director Preventive and Social Dunedin School of Otago, PO Box 913, Dunedin, New Zealand G Peter Herbison statistician Women s and Children s Health, Dunedin School of Otago P Don Wilson urogynaecologist Public Health and Epidemiology, Birmingham, Birmingham B15 2TT Christine MacArthur professor of maternal and child epidemiology Obstetrics and Gynaecology, Aberdeen Royal Hospitals Trust, Aberdeen AB25 2ZL Gordon D Lang obstetrician continued over BMJ 2001;323:1 5 BMJ VOLUME SEPTEMBER 2001 bmj.com 1
2 Fetal Birmingham, Birmingham B15 2TG Harry Gee obstetrician Correspondence to: C M A Glazener c.glazener@ abdn.ac.uk loss of urine) to participate in the trial. After signed consent, they were randomly allocated to receive the nurse assessment and treatment programme or to a control group. Women were followed up by repeat questionnaire at 12 months after delivery, equivalent to around seven months after the first visit of the nurse to the intervention group. Intervention The nurses (a midwife, a health visitor, and a continence advisor) received a short course of specialised training in conservative management from local physiotherapists. The intervention comprised a structured home interview designed to identify different types of incontinence at five months after delivery. The nurse identified women whose symptoms were not typical of stress or urge incontinence or who had evidence of urinary tract infection; these women were referred to their primary care physician but remained enrolled in the trial for follow up and analysis. The nurse used a standard set of diagrams and instructions to teach the women in the intervention group about the anatomy of the pelvic floor and muscle contraction regimens. After preparatory exer cises to identify the pelvic floor musculature, the women were asked to follow a basic exercise programme of eight to ten sessions each day of fast and slow contractions with the aim of contractions daily. The nurse visited again and reinforced the instructions at seven and nine months after delivery. Women with symptoms of frequency or urgency also received instruction on bladder training at these later sessions. This aimed to increase bladder capacity by deferring voiding for progressively longer periods of time; the women were also advised to avoid drinks that contain caffeine. The control group did not receive any visits from research nurses. Like the intervention group, they had received peripartum preparation, which sometimes included pelvic floor exercises, 14 and could seek medical advice. Outcomes The primary outcome measure was persistence of any urinary incontinence. Secondary outcomes included severe urinary incontinence (defined as at least once a week) and faecal incontinence (see box). Women who reported faecal incontinence sometimes, often, or always were classified as having severe incontinence. Other variables measured were the use and frequency of pelvic floor exercises, use of pads, an overall rating of severity of urinary incontinence with a visual analogue scale, a measure of general wellbeing (see box), and anxiety and depression measured by the hospital anxiety and depression scale. 15 Power calculation We aimed to recruit 660 women, giving 80% power to detect a 10% difference in persistence of urinary incontinence between the two groups, assuming that 75% of the control group would still be incontinent at one year after delivery. These figures were conservatively based on findings in the pilot study. 10 Randomisation Randomisation was achieved with remote access to a computer program in Dunedin. It registered each woman before presenting the allocation by using stratification by parity (four versus fewer), method of Phrasing of questions Urinary incontinence At present, do you ever lose any urine when you don t mean to? (yes/no) In the past month, how often has this happened on average? (less than twice a month/twice a month/once a week/a few times a week/once a day/twice a day/three or more times a day) (severe = once a week or more often) Faecal incontinence Do you ever lose control of wind or bowel motions from your back passage between visits to the toilet? (no/rarely/sometimes/often/always) (severe = sometimes or more often) General wellbeing How are you feeling generally? (very well/well/not very well/not at all well) Type of urinary incontinence Do you lose urine when you: (yes/no) Stress: cough, laugh, sneeze, run, jump, or play sport (if not also urge or mixed) Urge: feel an urgent desire to pass water and are unable to reach the toilet in time (if not also stress or mixed) Mixed: At some other time (including women who ticked both stress and urge) delivery (caesarean versus other), and frequency of incontinence (at least once a week versus less). The intervention could not be performed blind, but the collection of outcome data was by anonymised questionnaire, which was identified only by a study number and which could not be related back to trial allocation at the time of data entry. Analysis Groups were compared with χ 2 test or t tests as appropriate, with results expressed as absolute or relative differences with 95% confidence intervals. Analysis was by intention to treat. Prespecified secondary analyses were stratified by initial severity of incontinence (at least once a week versus less) and by type of incontinence (stress, urge, or mixed, see box). We explored the impact of differential loss to follow up with analyses stratified by centre. Results Of questionnaires sent to women three months postnatally, 7879 (72%) were returned. Among the respondents, 2632 (33%) had urinary incontinence in the previous month, and 747 (28%) of these consented to participate in the trial (figure 1). The trial groups were comparable at baseline (table 1). However, the women who had incontinence but who did not participate were younger, had fewer spontaneous vaginal deliveries, more intact perineums, lighter babies, and were less likely to have severe incontinence (table 1). In the intervention group, 316/371 received the intervention as allocated, but all women were included in the intention to treat comparison with the 376 in the control group. At follow up, women in the intervention group were more likely to report performing some pelvic floor exercises in the previous month (218/278 (79%) v 118/244 (48%), 95% confidence interval for 2 BMJ VOLUME SEPTEMBER 2001 bmj.com
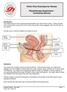
3 Women with live baby at 3 months after delivery (n= ) Respondents to questionnaire (n= 7879, 71.7%) Incontinent (n=2632, 33.4%) Continent (n=5247, 66.6%) Participants (n=747) Intervention (n=371) Received intervention as allocated (n=316) Followed up at 12 months (n=279, 75%) (lost to follow up, n=92) Non-participants (n=1885) (n=376) Received control intervention(n=376) Followed up at 12 months (n=245, 65%) (lost to follow up, n=131) Respondents to questionnaire (n= 7879, 71.7%) Fig 1 Population studied. Reasons for not receiving active intervention as allocated include new pregnancy, too busy, moved away, family problems, incontinence resolved, non-stress or urge incontinence difference 22% to 38%, P < 0.001) and to be performing more contractions (mean (SD) number per day 20 (29) v 5 (15), 11 to 19, P < 0.001). These women were also significantly less likely to have any incontinence, which was reflected in a difference in severe incontinence (table 2). Overall ratings of severity, use of pads, and number of pad changes were lower in the intervention group, which also reported less faecal incontinence to motions and less severe faecal incontinence (table 2). Although there were no significant differences in general wellbeing or depression, women in the intervention group were less anxious than those in the control group (table 2). The results of the stratified analyses were consistent with the overall results in favouring the intervention group. The absence of significant heterogeneity suggested that the intervention was effective irrespective of type or severity of incontinence (figs 2 and 3). More women in the intervention group returned a completed follow up questionnaire (75% v 65%). Table 3 shows that the women who did not respond at follow up were more likely to have had severe incontinence at baseline (65% v 52%), though this was not affected by Table 1 Baseline characteristics of intervention, control, and non-participant groups. Figures are number (percentage) of women unless stated otherwise. Not all data were available for all women trial allocation among non-responders (69% v 63%). The differential loss to follow up was confined to participants in one centre (Birmingham). Stratified analyses restricted to the two other centres, which did not have such losses, suggested larger rather than smaller effects (51% still incontinent in the intervention group v 67% in the controls, P = 0.004). Discussion Intervention (n=371) (n=376) Nurse assessment and conservative treatment targeted at women with incontinence three months postnatally moderately reduces the risk of incontinence a year later. The difference in the primary outcome measure, Non-participants (n=1885) Centre: Dunedin Birmingham Aberdeen Mean (SD) age (years) 29.6 (5.2) 29.4 (5.1) 28.4 (5.4) Primiparous 134 (36.7) 139 (37.6) 735 (39.4) Incontinence before index pregnancy: Primiparas 14 (10.4) 10 (7.2) 81 (11.0) Multiparas 121 (52.4) 112 (48.5) 455 (40.3) Method of delivery: Spontaneous vaginal 285 (78.3) 291 (78.6) 1347 (72.3) Assisted vaginal* 50 (13.7) 51 (13.8) 291 (15.6) Caesarean section 29 (8.0) 28 (7.6) 226 (12.1) Perineum: Intact 124 (34.4) 128 (35.9) 754 (42.1) Tear 154 (42.8) 160 (44.8) 640 (35.8) Episiotomy (with or without tear) 82 (22.8) 69 (19.3) 395 (22.1) Mean (SD) birthweight (g) 3478 (505) 3416 (523) 3389 (584) Severe incontinence (at least once a week) 212 (57.1) 204 (54.3) 882 (46.8) Type of incontinence: Stress only 199 (54.1) 187 (51.3) 1003 (54.6) Urge only 53 (14.4) 61 (16.8) 308 (16.8) Mixed 116 (31.5) 116 (31.9) 526 (28.6) Faecal incontinence (motions) 57 (16.3) 54 (15.1) 259 (14.8) Mean (SD) anxiety score 6.9 (3.78) 7.0 (3.76) 7.25 (3.76) Mean (SD) depression score 6.18 (3.89) 5.84 (3.66) 6.69 (3.97) *Breech, vacuum/ventouse, forceps. Of these 12, 13, and 103, respectively, were elective. Derived from hospital anxiety and depression scale. 14 Table 2 Incontinence and other outcome measures at 12 months. Figures are numbers (percentage) of women and means (95% confidence interval) Intervention (279) (245) Absolute difference (95% CI for difference) Significance Urinary incontinence (any) 167 (59.9) 169 (69.0) 9.1 (1.0 to 17.3) χ 2 =4.33, P=0.037 Urinary incontinence (severe*) 55 (19.7) 78 (31.8) 12.1 (4.7 to 19.6) χ 2 =9.49, P=0.002 Mean overall rating of severity (n=142 and 142) 2.8 (2.4 to 3.1) 3.6 (3.1 to 4.0) 0.8 (0.22 to 1.36) t= 2.73, P=0.007 Any pad use 41/276 (14.9) 55/245 (22.4) 7.5 (0.9 to 14.3) χ 2 =4.49, P=0.034 Mean No of pad changes (n=275 and 244) 0.19 (0.13 to 0.25) 0.34 (0.25 to 0.43) 0.15 (0.04 to 0.26) t= 2.65, P=0.008 Any faecal incontinence (to motions) 12/273 (4.4) 25/237 (10.5) 6.1 (1.6 to 10.8) χ 2 =6.25, P=0.012 Severe faecal incontinence (to motions ) 5/273 (1.8) 12/237 (5.1) 3.3 (0.02 to 6.4) χ 2 =3.17, P=0.075 General feeling of wellbeing (very well) 130/276 (47.1) 110/244 (45.1) 2.0 ( 6.5 to 10.6) χ 2 =0.139, P=0.709 Mean HAD anxiety score (n=238 and 219) 6.1 (5.6 to 6.5) 6.8 (6.3 to 7.3) 0.7 (0.05 to 1.43) t= 2.08, P=0.038 Mean HAD depression score (n=238 and 219) 4.8 (4.4 to 5.3) 5.2 (4.7 to 5.7) 0.4 ( 0.28 to 1.02) t= 1.13, P=0.260 *Severe urinary incontinence defined as at least once a week. Analogue scale range: 0=no problem at all to 10=can t think of anything worse. Incontinent women only. Severe faecal incontinence defined as sometimes, often, or always. Hospital anxiety and depression score range: 0 (no anxiety or depression) to 21 (maximum score). BMJ VOLUME SEPTEMBER 2001 bmj.com 3
4 All women Low initial severity (<1/week) High initial severity (>1/week) Stress incontinence initially Urge incontinence initially Mixed incontinence initially Treatment 167/279 68/130 99/149 91/156 18/41 57/79 169/245 75/123 94/122 87/124 25/43 54/67 Relative risk (95% CI fixed) conservative treatment 1 2 control any urinary incontinence 12 months after delivery, is unlikely to reflect chance. It suggests that about 11 women would have to be treated to prevent one case of persistent incontinence, with the benefit concentrated among those with severe incontinence. Furthermore, women in the intervention group were significantly less likely to have persistence of faecal incontinence and had lower anxiety scores. There was no evidence of any differential effects among subgroups of women characterised by initial type of urinary incontinence (stress, urge, or mixed). Although the relative risk reduction for any incontinence was similar in the analyses stratified by initial severity, the risk of eventually having severe incontinence was principally reduced among women whose initial incontinence was severe. This finding should be interpreted cautiously and as hypothesis generating rather than testing, but it does provide some basis for limiting the intervention to women with more severe incontinence. 5 Relative risk (95% CI fixed) 0.87 (0.76 to 0.99) 0.86 (0.69 to 1.07) 0.86 (0.74 to 1.00) 0.83 (0.70 to 0.99) 0.76 (0.49 to 1.16) 0.90 (0.75 to 1.07) Fig 2 Relative risk of any incontinence at 12 months postpartum according to initial severity of incontinence and initial type of incontinence with conservative treatment compared with control All women Low initial severity (<1/week) High initial severity (>1/week) Stress incontinence initially Urge incontinence initially Mixed incontinence initially Treatment 55/279 12/130 43/149 29/156 4/41 21/79 78/245 13/123 65/122 37/124 8/43 31/67 Relative risk (95% CI fixed) conservative treatment 1 5 control 10 Relative risk (95% CI fixed) 0.62 (0.46 to 0.84) 0.87 (0.41 to 1.84) 0.54 (0.40 to 0.73) 0.62 (0.41 to 0.95) 0.52 (0.17 to 1.61) 0.57 (0.37 to 0.90) Fig 3 Relative risk of severe incontinence (at least once a week) at 12 months postpartum according to initial severity of incontinence and initial type of incontinence with conservative treatment compared with control Table 3 Differential response rates and incontinence at baseline and outcome at 12 months. Figures are numbers (percentage) of women Up to twice a month According to return of second questionnaire: Incontinence At least once a week Returned (n=524) 253 (48) 271 (52) Not returned (n=223) 78 (35) 145 (65) In women who did not return second questionnaire: Intervention (n=92) 29 (32) 63 (69) (n=131) 49 (37) 82 (63) Significance χ 2 =10.69, P=0.001 χ 2 =0.584, P=0.444 Strengths and weaknesses Randomisation stratified by parity, method of delivery, and frequency of incontinence ensured that smaller subgroups were evenly distributed between the trial arms. We chose to stratify at para 4 because previous work has shown that the likelihood of urinary incontinence increases considerably after four children (compared with primiparous women). 2 There was a higher response rate to the 12 month questionnaire in the intervention group, which needs to be taken into account in the interpretation. This would introduce bias if the non-responders in the control group were less likely to be incontinent than those who responded. However, further analysis showed that non-responders had more rather than less severe incontinence initially, suggesting that severity of incontinence was not the factor contributing to their differential response rate. If anything, those lost from the intervention group had more severe incontinence at baseline, and yet it was the women in this group who seemed to benefit most. Furthermore, the difference in response rates was seen in only one of the centres (Birmingham). Secondary analyses restricted to the two other centres indicated a larger rather than smaller effect compared with the overall trial result. Implications The reduction in incontinence contrasts with the findings of a comparable trial, which indicated that providing enhanced instruction on pelvic floor exercises to all postnatal women immediately after delivery was not effective. 8 However, two thirds of these women would be unlikely to suffer from incontinence in the long term, the active intervention occurred briefly in hospital and was supplemented by diaries and telephone reminders at home for a month, and the intervention was given during the period when spontaneous recovery of nerve damage might be occurring. 9 Our policy of targeting women who had persistent incontinence was therefore likely to reach a more receptive population at a period when they had more time to devote to their own health. The intervention resulted in a greater reported use of pelvic floor exercises, consistent with a causal link with the lower rates of incontinence. Another possible mediator is the social support provided by repeated contact with the research nurses. In addition to reduced anxiety there was a proportional improvement in general wellbeing and reduction in depression, although these differences did not reach significance. Similar changes in wellbeing and depression among women in the intervention group (albeit without any detectable effect on incontinence) were also seen in the trial of nurse led reinforcement of pelvic floor exercises immediately after delivery. 8 Our results may be particularly important in guiding the management of persistent faecal incontinence. Recent systematic reviews of all trials of conservative treatment of faecal incontinence found no other trials of pelvic floor exercises versus no treatment and only limited evidence to favour biofeedback and electrical stimulation. In our trial the women with faecal incontinence also had urinary incontinence. In the baseline survey there were 329/4814 (7%) more women continent to urine but incontinent to faeces who were not invited to participate in the trial. Our 4 BMJ VOLUME SEPTEMBER 2001 bmj.com
5 What is already known on this topic Vaginal delivery is a risk factor for urinary incontinence Three months after childbirth 20-30% of women still experience urinary incontinence Most women do not seek treatment What this study adds Women will use conservative treatments such as pelvic floor exercises or bladder training Conservative management prevents persistent urinary incontinence in about one in 10 women who have postnatal incontinence Coexisting persistent faecal incontinence is also improved findings regarding faecal incontinence should be interpreted cautiously in view of the scarcity of other information on the management of faecal incontinence and the fact that this was not our primary outcome measure. Can these results be generalised to an unselected postnatal population? The initial questionnaire to postnatal women had a 72% response rate, which is high for postal surveys. The demographic characteristics of non-respondents were typical of other non-responders to such surveys, 18 and their obstetric characteristics suggested that they would be likely to have less incontinence than responders (data not shown). Similarly, the women who were incontinent but did not participate in the study were more normal than the trial women in obstetric terms, and they were less likely to have severe incontinence. This might have reduced their motivation to enter the trial. Conclusion Incontinence to urine and faeces commonly dates from pregnancy and childbirth. Conservative management by nurses of postnatal women with persistent incontinence seems to be effective in reducing both urinary and faecal incontinence. The benefit for women with urinary incontinence is greater among those with more severe initial symptoms, which could provide a basis for a more restrictive approach to this form of management. Further randomised trials for faecal incontinence are needed. Further research would also identify the most effective and efficient ways to deliver an intervention of the kind tested in this trial and to assess whether the benefits observed in this study are sustained, particularly among women who have more children by vaginal delivery. We thank the women who took part and Alison MacDonald, Anne-Marie Rennie, Jane Cook, and Jane Harvey, who provided nursing and administrative support. The Health Services Research Unit receives core support from the Chief Scientist Office of the Scottish Executive Health Department. The views expressed are those of the authors. Contributors: All authors contributed to the design of the study, adapted from a pilot study conceived by PDW, GPH, and AMG. CMAG, GPH, PDW, CMcA, HG, and GDL supervised the execution of the study and data collection. CMAG and GPH analysed the data. The paper was written jointly by all authors. CMAG and GPH are guarantors for this paper. Funding: WellBeing (grant sponsored by GlaxoWellcome) and Health Research Council of New Zealand. Competing interests: None declared. 1 MacArthur C, Lewis M, Knox EG. Health after childbirth. London: HMSO, Wilson PD, Herbison RM, Herbison GP. Obstetric practice and the prevalence of urinary incontinence three months after delivery. Br J Obstet Gynaecol 1996;103: MacArthur C, Lewis M, Bick D. Stress incontinence after childbirth.brj Midwifery 1993;1: MacArthur C, Bick DE, Keighley MRB. Faecal incontinence after childbirth. Br J Obstet Gynaecol 1997;104: Sultan AH, Kamm MA, Hudson CN, Thomas JM, Bartram CI. Anal-sphincter disruption during vaginal delivery. N Engl J Med 1993;329: Berghmans LC, Hendriks HJ, Bo K, Hay-Smith EJ, de Bie RA, van Waalwijk van Doorn ES, et al. Conservative treatment of stress urinary incontinence in women: a systematic review of randomized clinical trials. Br J Urol 1998;82: Hay-Smith EJ, Bo K, Berghmans LC, Hendriks HJ, De Bie RA, van Waalwijk van Doorn ES. Pelvic floor muscle training for urinary incontinence in women. Cochrane Database Syst Rev 2001;(1):CD Sleep J, Grant A. Pelvic floor exercises in postnatal care. Midwifery 1987;3: Snooks SJ, Badenoch DF, Tiptaft RC, Swash M. Perineal damage in genuine stress incontinence. An electrophysiological study. Br J Urol 1985;57: Wilson PD, Herbison GP. A randomized controlled trial of pelvic floor muscle exercises to treat postnatal urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 1998;9: O Brien J, Austin M, Sethi P, O Boyle P. Urinary incontinence: prevalence, need for treatment, and effectiveness of intervention by nurse. BMJ 1991;303: Jozwik M, Jozwik M. The physiological basis of pelvic floor exercises in the treatment of stress urinary incontinence [review]. Br J Obstet Gynaecol 1998;105: Millard RJ. Bladder control a simple self-help guide. Sydney: MacLennan and Petty, Mason L, Glenn S, Walton I, Hughes C. The instruction in pelvic floor exercises provided to women during pregnancy or following delivery. Midwifery 2001;17: Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand 1983;67: Norton C, Hosker G, Brazzelli M. Biofeedback and/or sphincter exercises for the treatment of faecal incontinence in adults. Cochrane Database Syst Rev 2000;(4):CD Hosker G, Norton C, Brazzelli M. Electrical stimulation for faecal incontinence in adults. Cochrane Database Syst Rev 2000;(4):CD Cartwright A. Who responds to postal questionnaires? J Epidemiol Community Health 1986;3: (Accepted 5 July 2001) BMJ VOLUME SEPTEMBER 2001 bmj.com 5
This is the author's version of the work. It is posted here for personal use, not for
 1 This is the author's version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obsterics and Gynaecology 2013; DOI: 10.1111/1471-0528.12473
1 This is the author's version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obsterics and Gynaecology 2013; DOI: 10.1111/1471-0528.12473
NEW POSTNATAL URINARY INCONTINENCE : OBSTETRIC AND OTHER RISK FACTORS IN PRIMIPARAE. New postnatal urinary incontinence in primiparae
 Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Faecal incontinence persisting after childbirth: a 12 year longitudinal
 Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse
 DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
Pelvic floor muscle training for prevention and treatment of urinary and faecal incontinence in antenatal and postnatal women (Review)
 Pelvic floor muscle training for prevention and treatment of urinary and faecal incontinence in antenatal and postnatal women (Review) Boyle R, Hay-Smith EJC, Cody JD, Mørkved S This is a reprint of a
Pelvic floor muscle training for prevention and treatment of urinary and faecal incontinence in antenatal and postnatal women (Review) Boyle R, Hay-Smith EJC, Cody JD, Mørkved S This is a reprint of a
The Effectiveness of a Pelvic Floor Muscle Exercise Program on Urinary Incontinence Following Childbirth: A Systematic Review
 The Effectiveness of a Pelvic Floor Muscle Exercise Program on Urinary Incontinence Following Childbirth: A Systematic Review Robin Watts, RN BA MHSc PhD FRCNA 1 Gaby Haddow, PhD BAppSci(Hons) 2 Jeanette
The Effectiveness of a Pelvic Floor Muscle Exercise Program on Urinary Incontinence Following Childbirth: A Systematic Review Robin Watts, RN BA MHSc PhD FRCNA 1 Gaby Haddow, PhD BAppSci(Hons) 2 Jeanette
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider.
 Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Lets talk about Faecal incontinence (FI) in Scleroderma
 Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Impact of Delivery Types on Women s Postpartum Sexual Health
 Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Midline episiotomy and anal incontinence: retrospective cohort study
 Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Dr. Najwa Alfarra Department of physical therapy, King Faisal Specialist Hospital and Research Center, Kingdom of Saudi Arabia
 IOSR Journal of Nursing and Health Science (IOSR-JNHS) e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 6, Issue 6 Ver. III. (Nov.- Dec.2017), PP 38-56 www.iosrjournals.org Comparison between the significant
IOSR Journal of Nursing and Health Science (IOSR-JNHS) e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 6, Issue 6 Ver. III. (Nov.- Dec.2017), PP 38-56 www.iosrjournals.org Comparison between the significant
A non-invasive, safe and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1
 A non-invasive, safe and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 INNOVO INNOVO has changed my life for the better. I no longer
A non-invasive, safe and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 INNOVO INNOVO has changed my life for the better. I no longer
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Natural progression of anal incontinence after childbirth
 Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
restore the pelvic floor
 restore the pelvic floor A non-invasive, safe, and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 has changed my life for the better.
restore the pelvic floor A non-invasive, safe, and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 has changed my life for the better.
EXPECTING A BABY? SOME PREGNANT WOMEN CAN HAVE BLADDER AND BOWEL CONTROL PROBLEMS. YOU CAN GET HELP. HOW DO I KNOW IF I HAVE A PROBLEM?
 11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship?
 DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
Anal incontinence after childbirth is more common than was previously believed. Anal incontinence after childbirth. Methods
 Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Telford and Wrekin Clinical Commissioning Group
 Telford and Wrekin Clinical Commissioning Group Agenda Item 9.2 CLINICAL COMMISSIONING GROUP GOVERNANCE BOARD EXECUTIVE SUMMARY DATE: 9 th April 2013 TITLE OF PAPER: Continence pathway and Referral letter
Telford and Wrekin Clinical Commissioning Group Agenda Item 9.2 CLINICAL COMMISSIONING GROUP GOVERNANCE BOARD EXECUTIVE SUMMARY DATE: 9 th April 2013 TITLE OF PAPER: Continence pathway and Referral letter
The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth
 Int Urogynecol J (8) 19:525 53 DOI.7/s192-7-472-z ORIGINAL ARTICLE The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth Jacobus
Int Urogynecol J (8) 19:525 53 DOI.7/s192-7-472-z ORIGINAL ARTICLE The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth Jacobus
DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?
 DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?.* Mohamed El-Negeri', Mohamed Eltotongy \ Maged Elshamy AbdA. Yasser Abdel Dayem'", waleed Omar \ Waleed Thabet Elrefaei, Department
DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?.* Mohamed El-Negeri', Mohamed Eltotongy \ Maged Elshamy AbdA. Yasser Abdel Dayem'", waleed Omar \ Waleed Thabet Elrefaei, Department
Effect of postpartum pelvic floor muscle training in prevention and treatment of urinary incontinence: a one-year follow up
 British Journal of Obstetrics and Gynaecology August 2000, V01107, pp. 1022-1028 Effect of postpartum pelvic floor muscle training in prevention and treatment of urinary incontinence: a one-year follow
British Journal of Obstetrics and Gynaecology August 2000, V01107, pp. 1022-1028 Effect of postpartum pelvic floor muscle training in prevention and treatment of urinary incontinence: a one-year follow
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Screening of Immediate Post Partum Females for Urinary Incontinence Ami Vishal Mehta 1, Zarna
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Screening of Immediate Post Partum Females for Urinary Incontinence Ami Vishal Mehta 1, Zarna
Urinary dysfunction assessment tool (community)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence
 MACROJOURNALS The Journal of MacroTrends in Health and Medicine Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence Vjollca Ndreu*, Fatjona Kamberi*, Enkeleda Sinaj*,
MACROJOURNALS The Journal of MacroTrends in Health and Medicine Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence Vjollca Ndreu*, Fatjona Kamberi*, Enkeleda Sinaj*,
Guidelines for referring patients to Physiotherapy for the treatment of Pelvic Floor Dysfunction
 Guidelines for referring patients to Physiotherapy for the treatment of Pelvic Floor Dysfunction N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed
Guidelines for referring patients to Physiotherapy for the treatment of Pelvic Floor Dysfunction N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed
Pelvic floor exercises for women. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic floor exercises for women This leaflet will provide you with information about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic floor exercises for women This leaflet will provide you with information about
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Pelvic Floor Muscle Exercises
 INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
The development of a questionnaire to measure the severity of symptoms and the quality of life before and after surgery for stress incontinence
 BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
Women's physiotherapy
 The women s health physiotherapy outpatient team treats a variety of conditions affecting women: chronic pelvic pain urinary incontinence birth-related perineal trauma antenatal and postnatal musculoskeletal
The women s health physiotherapy outpatient team treats a variety of conditions affecting women: chronic pelvic pain urinary incontinence birth-related perineal trauma antenatal and postnatal musculoskeletal
Physiotherapy advice following your third or fourth degree perineal tear
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Women s & Children s Directorate The TVT Operation - a guide for patients
 Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Continence Worksheet Name: Date: Name of Trainer: Name of Company: Clinical Update (NZ) Ltd
 Continence Worksheet Name: Date: Name of Trainer: Name of Company: Clinical Update (NZ) Ltd Segment 1 What is continence? Incontinence is not a but a sign of What organs are involved? and Urine incontinence
Continence Worksheet Name: Date: Name of Trainer: Name of Company: Clinical Update (NZ) Ltd Segment 1 What is continence? Incontinence is not a but a sign of What organs are involved? and Urine incontinence
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
The UNIVERSITY of NEWCASTLE
 The UNIVERSITY of NEWCASTLE R esearch C entre for G ender and H ealth Characteristics of Australian women with incontinence according to incontinence severity and treatment-seeking behaviour Results from
The UNIVERSITY of NEWCASTLE R esearch C entre for G ender and H ealth Characteristics of Australian women with incontinence according to incontinence severity and treatment-seeking behaviour Results from
Keeping control What you should expect from your NHS bladder and bowel service
 Keeping control What you should expect from your NHS bladder and bowel service Based on findings from the national audit of continence care 2010 National audit funded by: Report authors Dr Danielle Harari
Keeping control What you should expect from your NHS bladder and bowel service Based on findings from the national audit of continence care 2010 National audit funded by: Report authors Dr Danielle Harari
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
ONE IN THREE WOMEN WHO EVER HAD A BABY WET THEMSELVES EVERY WOMAN WHO HAS HAD A BABY SHOULD DO PELVIC FLOOR MUSCLE TRAINING.
 08 EVERY WOMAN WHO HAS HAD A BABY SHOULD Women who have even just one baby are nearly three times more likely to leak urine and wet themselves, than women who have not had a baby. The more babies you have,
08 EVERY WOMAN WHO HAS HAD A BABY SHOULD Women who have even just one baby are nearly three times more likely to leak urine and wet themselves, than women who have not had a baby. The more babies you have,
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
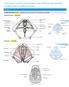 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
The urethral support system during pregnancy and after childbirth Wijma, Jacobus
 University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
Bladder retraining - treatment for urgency and urge incontinence
 Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
IMPROVING URINARY INCONTINENCE
 IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
Patient Advice for Third & Fourth Degree Tears
 Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Module 5 Management Of Urinary Incontinence
 Management Of Urinary Incontinence V3: Last Reviewed September 2017 Learning Outcomes Outline conservative management options Discover the options available to manage the different types of incontinence
Management Of Urinary Incontinence V3: Last Reviewed September 2017 Learning Outcomes Outline conservative management options Discover the options available to manage the different types of incontinence
Sphincter exercises for people with bowel control problems. Information for patients. Physiotherapy Department
 Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Your pelvic floor muscles
 Continence office Ballochmyle Suite, University Hospital Ayr Telephone 019 177 Your pelvic floor muscles Advice and exercise for women Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa
Continence office Ballochmyle Suite, University Hospital Ayr Telephone 019 177 Your pelvic floor muscles Advice and exercise for women Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Care of your Perineum following 3 rd and 4 th degree tears
 Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Pelvic floor education for new mothers: timing the message for best effect
 Commonwealth Department of Health and Aged Care National Continence Management Strategy Innovative Grants Program Pelvic floor education for new mothers: timing the message for best effect Nicole Tweddle
Commonwealth Department of Health and Aged Care National Continence Management Strategy Innovative Grants Program Pelvic floor education for new mothers: timing the message for best effect Nicole Tweddle
Initial management of stress urinary incontinence: pelvic floor muscle training and duloxetine
 DOI: 1.1111/j.1471-528.6.878.x www.blackwellpublishing.com/bjog Review article Initial management of stress urinary incontinence: pelvic floor muscle training and duloxetine RM Freeman Urogynaecology Unit,
DOI: 1.1111/j.1471-528.6.878.x www.blackwellpublishing.com/bjog Review article Initial management of stress urinary incontinence: pelvic floor muscle training and duloxetine RM Freeman Urogynaecology Unit,
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION What is the effect of retraining diaphragmatic, deep abdominal, and pelvic floor muscle (PFM) coordinated function in a graded, multi-stage, supervised
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION What is the effect of retraining diaphragmatic, deep abdominal, and pelvic floor muscle (PFM) coordinated function in a graded, multi-stage, supervised
Pelvic floor exercises for women. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic Floor Exercises for Women This leaflet will provide you with information about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic Floor Exercises for Women This leaflet will provide you with information about
A Stress Urinary Incontinence fact sheet for
 A Stress Urinary Incontinence fact sheet for women and teenagers What is Stress Urinary Incontinence? Get to know your gusset - the science bit Stress urinary incontinence (SUI) is defined as a sudden
A Stress Urinary Incontinence fact sheet for women and teenagers What is Stress Urinary Incontinence? Get to know your gusset - the science bit Stress urinary incontinence (SUI) is defined as a sudden
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men Why are my pelvic floor muscles important? Your pelvic floor muscles are important for bladder and bowel control. These muscles help to keep the bladder
Pelvic Floor Muscle Exercises and Advice for Men Why are my pelvic floor muscles important? Your pelvic floor muscles are important for bladder and bowel control. These muscles help to keep the bladder
Physiotherapy advice following your vaginal birth
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Pelvic floor muscle exercises (long)
 Pelvic floor muscle exercises (long) This leaflet aims to give an overview of pelvic floor muscles, their function, how they can be exercised and why this is so important. What are pelvic floor muscles
Pelvic floor muscle exercises (long) This leaflet aims to give an overview of pelvic floor muscles, their function, how they can be exercised and why this is so important. What are pelvic floor muscles
Urinary dysfunction assessment tool (care home)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Pregnancy and delivery: a urodynamic viewpoint
 British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
Faecal Incontinence Information Leaflet THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
Occult anal sphincter injuries myth or reality?
 DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
SELF CARE IN URINARY INCONTINENCE
 O P I N I O N SelfCare 2011;2(6):160-166 Advancing the study&understanding of self-care JULIAN SPINKS General Practitioner, Medway Primary Care Trust ABSTRACT Urinary incontinence and its associated urinary
O P I N I O N SelfCare 2011;2(6):160-166 Advancing the study&understanding of self-care JULIAN SPINKS General Practitioner, Medway Primary Care Trust ABSTRACT Urinary incontinence and its associated urinary
Repair of vaginal tears and episiotomy guidelines
 Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
(UI Urine incontinence)! " # $% &'! ( ) * " " +, -. &/ !!" # $%& /'0 = ='' &!( )'*(" &%: "## $ "% % &' ( )* .!
 39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
Posterior Tibial Nerve Stimulation for Voiding Dysfunction
 Posterior Tibial Nerve Stimulation for Voiding Dysfunction Corporate Medical Policy File name: Posterior Tibial Nerve Stimulation for Voiding Dysfunction File code: UM.NS.05 Origination: 8/2011 Last Review:
Posterior Tibial Nerve Stimulation for Voiding Dysfunction Corporate Medical Policy File name: Posterior Tibial Nerve Stimulation for Voiding Dysfunction File code: UM.NS.05 Origination: 8/2011 Last Review:
Urodynamics Clinic. Patient Information
 Patient Information Urodynamics Clinic Author: Gynaecology Produced and designed by the Communications Team Issue date May 2017 - Review date May 2020 Version 3 Ref no. PILCOM1433 Urodynamics Clinic An
Patient Information Urodynamics Clinic Author: Gynaecology Produced and designed by the Communications Team Issue date May 2017 - Review date May 2020 Version 3 Ref no. PILCOM1433 Urodynamics Clinic An
Pelvic Floor and More.. Urinary Continence. Urinary Incontinence. Normal Bladder Function
 Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
Tension-free Vaginal Tape (TVT)
 Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Disease Management. Incontinence Care. Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09
 Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
Randomised Mixed Methods Pilot Trial of Sacral and Percutaneous Tibial Nerve Stimulation for Faecal Incontinence
 Research for Patient Benefit Randomised Mixed Methods Pilot Trial of Sacral and Percutaneous Tibial Nerve Stimulation for Faecal Incontinence Thin NN 1, Taylor SJC 2, Bremner SA 2, Hounsome N 2, Alam A
Research for Patient Benefit Randomised Mixed Methods Pilot Trial of Sacral and Percutaneous Tibial Nerve Stimulation for Faecal Incontinence Thin NN 1, Taylor SJC 2, Bremner SA 2, Hounsome N 2, Alam A
PELVIC FLOOR MUSCLE TRAINING FOR WOMEN STRONG PELVIC FLOOR MUSCLES MEAN GOOD BLADDER AND BOWEL CONTROL WHAT ARE THE PELVIC FLOOR MUSCLES?
 06 STRONG S MEAN WHAT ARE THE S? The floor of the pelvis is made up of layers of muscle and other tissues. These layers stretch like a hammock from the tailbone at the back, to the pubic bone at the front.
06 STRONG S MEAN WHAT ARE THE S? The floor of the pelvis is made up of layers of muscle and other tissues. These layers stretch like a hammock from the tailbone at the back, to the pubic bone at the front.
URINARY INCONTINENCE FOR FALLS PREVENTION. by Susan Elms P.T. Elms Physiotherapy
 URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
Y0028_2726_0 File&Use Bladder Control Does Matter
 Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
