AMERIHEALTH / INDEPENDENCE BLUE CROSS
|
|
|
- Alexia Watkins
- 6 years ago
- Views:
Transcription
1 AMERIHEALTH / INDEPENDENCE BLUE CROSS Urinary outlet obstruction is difficulty in the passage of urine from the bladder to the urethra caused by compression or resistance on the bladder outflow channel at any location from the bladder neck to the urethral meatus. In males, this can be caused by benign prostatic hyperplasia (BPH). BPH is a common age-related noncancerous condition in men that is characterized by an increase of epithelial and stromal cells in the periurethral area of the prostate. This increase in cells causes an enlargement of the prostate gland. This pathologic change is important because of the proximal anatomical relationship between the prostate and the bladder neck. The condition generally involves lower urinary tract symptoms (LUTS), which may include increased urinary frequency, urgency, incontinence, or straining; nocturia; decreased and intermittent force of the stream; hematuria; and the sensation of incomplete bladder emptying. Given the substantive symptomatic impact of urinary outlet obstruction, symptomatic appraisal of interference with activities of daily living is a crucial aspect of evaluation. In an effort to quantify the severity of symptomatic BPH, a urodynamic investigation (e.g., urine flow rate assessment) may be performed. Treatment for BPH includes watchful waiting (e.g., active surveillance), medical management with pharmacotherapy (e.g., alpha-blockers, 5-alpha-reductase inhibitors), minimally invasive treatments (e.g., transurethral needle ablation [TUNA], transurethral microwave thermotherapy [TUMT]), and surgery (e.g., TURP, laser treatments). If there is minimal bother (i.e., interference with activities of daily living) and no evidence of prostate enlargement, watchful waiting may be utilized. Medical management may be indicated for individuals with uncomplicated BPH or moderate to severe symptoms, and individuals who are waiting for surgery, unwilling to undergo surgery, or are poor surgical candidates. Individuals with BPH who have complications such as acute urinary retention, recurrent urinary tract infections, hematuria, bladder stones, or renal insufficiency/failure due to BPH may be treated surgically. Untreated BPH may worsen over time and increase the risk of stones, infection, or kidney failure. The choice of treatment for urinary outlet obstruction due to BPH should be based on the individual's presentation and anatomy, the surgeon's level of training and experience, and a discussion of the potential benefit and risks for complications. The primary goal of treatment is to alleviate bothersome symptoms (i.e., symptoms that interfere with activities of daily living) that result from prostatic enlargement. More recently, treatment has been focused on altering disease progression and preventing complications associated with BPH. Standard surgical treatments such as transurethral resection of the prostate (TURP), transurethral incision of the prostate (TUIP) (in which an incision is made where the prostate meets the bladder), and open prostatectomy may be accompanied by undesirable complications such as blood loss, need for transfusion, salt imbalances from fluid absorption, and side effects such as incontinence and retrograde ejaculation. Newer surgical techniques that use lasers, as well as minimally invasive techniques that use various sources of energy such as heat, microwaves, radiofrequency, and ultrasound, have been developed. SURGICAL TREATMENTS STANDARD SURGICAL TREATMENTS Transurethral resection of the prostate (TURP) is the standard treatment for BPH against which all treatments are measured. TURP involves removing the core of the prostate through the urethra using instruments and electrodissection. An electrified wire loop removes pieces of prostatic tissue and coagulated blood. TURP is performed under general or spinal anesthesia and requires a hospital stay. Other standard surgical options include TUIP and open prostatectomy. THERMAL TREATMENT Transurethral electrovaporization of the prostate (TUVP) vaporizes the enlarged prostate tissue, destroying it by coagulation and allowing it to slough away over several weeks. TUVP steams the tissue away using high heat, and dries out the tissue using lower heat. Advantages of TUVP have shown earlier post-treatment catheter removal and less bleeding-related complications when compared to TURP. Evidence in available published peer-reviewed literature demonstrates the safety and effectiveness of TUVP for the treatment of BPH (Poulakis 2004). LASER TREATMENTS
2 These procedures involve a laser fiber that is passed into the prostatic channel under telescopic guidance. The laser is then used, through vaporization or ablation techniques, to destroy the obstructing portions of the prostate with heat. With laser vaporization, high instantaneous heat is created to vaporize or steam away prostate tissue. Lower laser energy is applied with laser ablation, which heats the tissue enough to dry it out and allows it to shrink and slough away with time. Various types of laser treatments include: Visual laser ablation of the prostate (VLAP) VLAP delivers a laser energy that is focused, without direct contact with the prostate, on the enlarged prostatic tissue, and causes thermal injury or coagulation necrosis of the tissue. The primary mechanism of tissue destruction is coagulation rather than vaporization, and the coagulated tissue sloughs away over several weeks following VLAP. VLAP requires a post-treatment catheterization from several days to several weeks. Community practice suggests that VLAP is not commonly used for the treatment of urinary outlet obstruction due to benign prostatic hyperplasia (BPH), as laser vaporization is now used. Interstitial laser coagulation (ILC) ILC utilizes a fiber-optic laser probe that is inserted through a cystoscope into the prostate at fixed points. Laser energy is applied to coagulate each area of obstructing prostate tissue, producing coagulation necrosis. In contrast to other laser procedures, where coagulation necrosis occurs at the urethral surface, in interstitial laser coagulation, delivery of laser energy directly into the tissues produces coagulation necrosis inside the enlarged prostatic tissue. The treated tissue is absorbed over a period of several weeks. Community practice suggests that ILC is no longer considered a standard or an option for the treatment of urinary outlet obstruction due to benign prostatic hyperplasia (BPH). Transurethral ultrasound-guided laser-induced prostatectomy (TULIP) TULIP was one of the first laser treatments used for BPH. A laser probe is housed between two ultrasound transducers that are used for real-time scanning to position the laser while it is being used. Coagulation necrosis of the prostate tissue produces shrinking over several weeks following TULIP. TULIP has been replaced by other laser techniques that have fewer side effects, shorter post-treatment catheterization times, and fewer urinary symptoms. TULIP is not mentioned in any of the evidence-based BPH guidelines. Because this treatment appears to be outdated, results of controlled trials are no longer considered. Community practice suggests that TULIP is no longer considered a standard or an option for the treatment of urinary outlet obstruction due to benign prostatic hyperplasia (BPH). Holmium laser Holmium laser treatments of the prostate are treatments that use a holmium laser fiber and a specially adapted resectoscope to ablate, resect, or enucleate enlarged prostatic tissue. Relief of obstruction is immediate. Holmium lasers are among the most common laser technologies used to treat prostate disease. With the holmium laser, there is the ability to coagulate tissue simultaneously with tissue incision, ablation, resection or enucleation. This reduces intraoperative blood loss as well as post-operative bleeding. The American Urological Association (AUA 2010) states that holmium laser treatments are appropriate and effective treatment alternatives to TURP and open prostatectomy in individuals with moderate to severe LUTS due to BPH, and/or who are significantly bothered by these symptoms (i.e., interfere with activities of daily living). Additionally, according to AUA, these treatments have been associated with shorter post-treatment catheterization time and shorter length of hospital stay. Holmium laser ablation of the prostate (HoLAP) This technology delivers laser energy at a wavelength of infrared range which is primarily absorbed by water. HoLAP is intended to be comparable to TURP, in that the prostatic lobes may be vaporized down to a surgical capsule resulting in a TURP-like effect. HoLAP does not yield tissue for histologic analysis. A controlled trial reported that although HoLAP took longer to perform than TURP, LUTS due to BPH and physiological measures improved to a similar degree after HoLAP and TURP (Mottet 1999). Holmium laser resection of the prostate (HoLRP) This technology utilizes a specially adapted resectoscope to resect prostate tissue into pieces small enough to be removed with bladder irrigation and grasping forceps or a modified resectoscope loop. Improvements in LUTS due to BPH obtained by using HoLRP are comparable to TURP (Gilling 1999, Ruzat 2008). Holmium laser enucleation of the prostate (HoLEP) HoLEP is typically used for larger glands that previously would have been treated with an open prostatectomy. Here, an entire prostatic lobe can be
3 separated from connective tissue and deposited in the bladder. The tissue is then extracted from the bladder. HoLEP has been evaluated in clinical trials and compared favorably with TURP in meta-analyses and system reviews (Kuntz 2002, Elzayat 2007, Naspro 2009, Burke 2010). Photoselective vaporization (PVP) PVP uses a potasium-titanyl-phosphate (KTP) laser to vaporize prostate tissue. KTP laser wavelengths penetrate only 1 to 2 mm, and the vaporization process may help avoid the perioperative side effects such as tissue sloughing. Additional reported potential advantages of PVP include virtually bloodless tissue ablation, shorter length of hospital stay, and shorter post-treatment catheterization times. As compared with TURP, surgical treatment of high-risk populations such as individuals taking anticoagulants, may be possible with PVP (Burke 2010, Ruszat 2008). PVP is an appropriate and effective treatment alternative to TURP and open prostatectomy in men who have moderate to severe LUTS due to BPH and/or who are significantly bothered by the symptoms (i.e., interfere with activities of daily living). MINIMALLY INVASIVE TREATMENTS Although TURP is the most commonly used treatment option for BPH, minimally invasive treatments have been developed that utilize various sources of energy, such as heat, radiofrequency, ultrasound, and microwaves. Minimally invasive treatments available include the following: Water-induced thermotherapy (WIT) During this minimally invasive treatment, heated water is circulated through a proprietary closed-loop catheter system to produce coagulative necrosis and secondary ablation of obstructing prostatic tissue. Thermal insulation of the catheter shaft along the penile, bulbous, and membranous urethra, as well as in the sphincter region, prevents unwanted incidental damage of tissue along the urinary tract. According to the Urologic Clinics of North America, along with a review of the available published peer-reviewed literature and clinical guidelines, there is insufficient evidence to support the use of WIT for the treatment of urinary outlet obstruction due to BPH. Balloon dilation of the prostate This minimally invasive treatment utilizes a flexible balloon catheter, which is placed in the urethra at the level of the prostate above the external sphincter. The balloon is then inflated for a short time to distend the prostatic urethra. Currently, the AUA does not recommend the use of balloon dilation of the prostate. Furthermore, the safety and/or efficacy of this service cannot be established by review of the available published peer-reviewed literature. Transurethral ethanol ablation (chemoablation) of the prostate (TEAP) This minimally invasive treatment involves injecting absolute ethanol transurethrally into the prostate tissue. The injected ethanol causes cells of the prostate to burst, killing the cells. The prostate shrinks as the necrosed cells are absorbed. Currently, the AUA does not recommend the use of transurethral ethanol ablation of the prostate. Furthermore, the safety and/or efficacy of this service cannot be established by review of the available published peer-reviewed literature. High-intensity focused ultrasound (HIFU) This minimally invasive treatment uses targeted high-intensity ultrasound to create coagulation necrosis in the prostate tissue. In contrast to other treatments, the HIFU device is inserted rectally and does not contact the prostate or urethra. Post-treatment catheterization time ranges from a few days to over a week. The safety and/or efficacy of this service cannot be established by review of the available published peer-reviewed literature. Randomized controlled trials comparing HIFU to standard treatments for BPH have not been published. Furthermore, at this time, the AUA considers HIFU as investigational, with additional long-term studies being warranted. Transurethral needle ablation (TUNA) of the prostate (also called transurethral radiofrequency needle ablation [RFNA]) This minimally invasive treatment delivers selective thermal energy to the prostate using two 18-gauge needles at the end of a TUNA catheter. A lens inside the catheter is used to guide the placement of the catheter into the urethra, where the needles are advanced to cause heat-induced coagulation necrosis in the prostate parenchyma. The prostate shrinks as the necrosed cells are absorbed. AUA recommends the use of TUNA as an appropriate and effective treatment alternative for bothersome (i.e., interfere with activities of daily living), moderate, or severe LUTS due to BPH. TUNA has been compared favorably with TURP in clinical trials and meta-analysis (Bouza 2006, Boyle 2004, Hill 2004). Although the improvement of LUTS due to BPH does not
4 reach the same level as TURP; fewer adverse events (e.g., incontinence, retrograde ejaculation) are demonstrated. Transurethral microwave thermotherapy (TUMT) This minimally invasive treatment begins by introducing a coolant into the urethra through a transurethral probe, which cools the urethra, followed by a microwave emission that heats and ultimately ablates prostatic tissue. AUA recommends the use of TUMT as an appropriate and effective treatment alternative for bothersome (i.e., interfere with activities of daily living), moderate, or severe LUTS due to BPH (Hoffman 2007). Prostatic Urethral Lift (UroLift ) The UroLift system is a minimally invasive implant developed to treat LUTS related to urinary outflow obstruction secondary to BPH in men 50 years of age or older. In this procedure, permanent implants (made from common implantable materials: nitinol, stainless steel, and polyethylene terepthalate) are delivered trans-prostatically to retract the enlarged lateral lobes of the prostate. This procedure dilates the prostatic urethra in individuals leading to improvement in LUTS symptoms without the need for surgical resection or the application of thermal energy to the prostate. Current evidence for this intervention includes 1 randomized sham-controlled trial (n = 206) published by Roehrborn et al. (2013) which found that at 12-month follow-up, both objective and subjective outcomes were significantly improved in individuals undergoing the UroLift procedure with no adverse impact to sexual function reported among any of the participants. An RCT directly comparing UroLift to TURP is scheduled for completion in December Notification Policy Coverage is subject to the terms, conditions, and limitations of the members' contract. MEDICALLY NECESSARY The surgical and minimally invasive treatment of urinary outlet obstruction due to benign prostatic hyperplasia (BPH) is considered medically necessary and, therefore, covered when all of the following criteria are met: One of the following surgical or minimally invasive treatments is utilized: Transurethral Resection of the Prostate (TURP) Holmium laser ablation of the prostate [HoLAP]) Holmium laser enucleation of the prostate [HoLEP] Holmium laser resection of the prostate [(HoLRP] Photoselective vaporization (PVP) Transurethral electrovaporization of the prostate (TUVP) Transurethral needle ablation (TUNA) Transurethral microwave thermotherapy (TUMT) The individual has a diagnosis of lower urinary tract symptoms (LUTS) secondary to benign prostatic hyperplasia (BPH) (e.g., increased urinary frequency, urgency, incontinence, or straining; nocturia; decreased and intermittent force of the stream; hematuria; and the sensation of incomplete bladder emptying) that interfere with activities of daily living. The individual has a prostate-specific antigen (PSA) blood test that meets both of the following criteria: Given within 12 months of the procedure Resulted in a value of 2.5 ng/ml or less for individuals who are up to and including 60 years of age and 4.0 ng/ml or less for individuals who are over 60 years of age
5 The individual has a peak urine flow rate (Qmax) less than 15 cc/sec on a voided volume that is greater than 125 cc. The individual has failed a trial of satisfactory voiding with medication (alpha blocker and/or alpha-reductase inhibitor) or intolerance to medication (alpha blocker and/or 5-alpha-reductase inhibitor). In addition to the above criteria, if the individual has a diagnosis or history of prostate cancer and meets either of the following criteria: The individual is not a candidate for surgical resection of the prostate but will be treated by radiation therapy and has symptoms that are so severe that immediate relief is required. The individual is clinically in remission as evidenced by a PSA < 1.0 ng/ml. UroLift for the treatment of urinary outlet obstruction due to BPH is considered medically necessary and, therefore covered if the following criteria are met: The individual has a diagnosis of LUTS secondary to BPH (e.g., increased urinary frequency, urgency, incontinence, or straining; nocturia; decreased and intermittent force of the stream; hematuria; and the sensation of incomplete bladder emptying) that interfere with activities of daily living. The individual has a peak urine flow rate (Qmax) less than 15 cc/sec on a voided volume that is greater than 125 cc. The individual's symptoms are caused by enlargement of the lateral lobes of the prostate with no median lobe enlargement present. The individual has normal renal function. The individual has mild to moderate symptoms that are refractory to medication or the individual does not wish to take daily medication. The individual is a poor candidate for other surgical interventions for BPH, or the individual opts to undergo a minimally-invasive procedure. The individual has a PSA blood test that meets both of the following criteria: Given within 12 months of the procedure Resulted in a value of 2.5 ng/ml or less for individuals who are up to and including 60 years of age and 4.0 ng/ml or less for individuals who are over 60 years of age In addition to the above criteria, if the individual has a diagnosis or history of prostate cancer and meets either of the following criteria: The individual is not a candidate for surgical resection of the prostate but will be treated by radiation therapy and has symptoms that are so severe that immediate relief is required. The individual is clinically in remission as evidenced by a PSA < 1.0 ng/ml. NOT MEDICALLY NECESSARY The use of TUNA, TUMT, HoLAP, HoLEP, HoLRP, PVP,TUVP, and UroLift to treat conditions other than those described above is considered not medically necessary and, therefore, not covered because the available published peer-reviewed literature does not support their use in the diagnosis or treatment of other conditions. The following obsolete medical services are considered not medically necessary and, therefore, not covered because the available published peer-reviewed literature does not support their use in the treatment of illness or injury: Visual laser ablation of the prostate (VLAP) Interstitial laser coagulation (ILC) Transurethral ultrasound-guided laser-induced prostatectomy (TULIP) Water-induced thermotherapy (WIT) EXPERIMENTAL/INVESTIGATIONAL The following procedures are considered experimental/investigational and, therefore, not covered because their safety and/or effectiveness in the treatment of urinary outlet obstruction due to BPH has not been established by review of the available published peer-reviewed literature:
6 Balloon dilation of the prostate Transurethral ethanol ablation of the prostate (TEAP) High-intensity focused ultrasound (HIFU) REQUIRED DOCUMENTATION The individual's medical record must reflect the medical necessity for the care provided. These medical records may include, but are not limited to: records from the health care professional's office, hospital, nursing home, home health agencies, therapies, and test reports. The Company may conduct reviews and audits of services to our members, regardless of the participation status of the provider. All documentation is to be available to the Company upon request. Failure to produce the requested information may result in a denial for the service. Notification Guidelines Serum prostate-specific antigen (PSA) level and prostate size should not be used as the sole basis of treatment recommendations. BENEFIT APPLICATION Subject to the terms and conditions of the applicable benefit contract, surgical and minimally invasive treatments for urinary outlet obstruction due to BPH are covered under the medical benefits of the Company s products when medical necessity criteria listed in the medical policy are met. US FOOD AND DRUG ADMINISTRATION (FDA) STATUS The use of devices in the minimally invasive treatment of urinary outlet obstruction due to benign prostatic hyperplasia (BPH) should be in accordance with all of the FDA-approved labeling requirements and/or criteria. Notification References Agency for Healthcare Research and Quality (AHRQ). Guideline on the management of benign prostatic hyperplasia (BPH). [AHRQ Web site]. January Available at: Accessed November 06, Agency for Healthcare Research and Quality (AHRQ). Treatments for benign prostatic hyperplasia. [Centers for Medicare & Medicaid Services (CMS) Web site]. 08/02/200 Accessed November 06, American Urological Association (AUA). Clinical guidelines. Management of BPH. Chapter 1: Diagnosis and treatment recommendations. [AUA Web site] Available a Accessed November 06, 2014.
7 American Urological Association (AUA) Foundation. Management of benign prostatic hyperplasia (BPH). [AUA Foundation Urology Health Web site]. January Availab Accessed November 06, Breda G, Isgrò A. Treatment of benign prostatic hyperplasia with water-induced thermotherapy: experience of a single institution. J Endourol. 2002;16(2): Bouza C, Lopez T, Magro A, et al. Systematic review and meta-analysis of transurethral needle ablation in symptomatic Benign Prostatic Hyperplasia. BMC Urol.2006;6(1): Boyle P, Robertson C, Vaughan ED, et al. A meta-analysis of trials of transurethral needle ablation for treating symptomatic benign prostatic hyperplasia. BJU Int.2004; 94( Burke N, Whelan JP, Goeree L, et al. Systematic review and meta-analysis of trasnurethral resection of the prostate versus minimally invasive procedures for the treatment prostatic obstruction. Urology.2010;75(5): Cimentepe E, Unsal A, Saglam R. Randomized clinical trial comparing transurethral needle ablation with transurethral resection of the prostate for the treatment of benign p hyperplasia: results at 18 months. J Endourol. 2003;17(2): Cornell University, Department of Urology. BPH/Natural history. [Cornell University Web site] Available at: Accessed No Cornell University, Department of Urology. BPH treatment - surgical. [Cornell University Web site] Available at: Accessed November 06, de la Rosette JJ, Floratos DL, Severens JL, et al. Transurethral resection vs microwave thermotherapy of the prostate: a cost-consequences analysis. BJU Int. 2003;92(7):7 de la Rosette JJ, Gravas S. Fitzpatrick JM. Minimally invasive treatments of male lower urinary tract symptoms. Urol Clin North Am.2008;35(3): Djavan B, Eckersberger E, Handl MJ, et al. Durability and retreatment rates of minimal invasive treatments of benign prostatic hyperplasia: a cross-analysis of the literature 2010;17(4): Dmochowski RM. Bladder outlet obstruction: etiology and evaluation. [National Center for Biotechnology Information (NCBI) Web site] Available at: Accessed November 06, ECRI Institute. High-intensity focused ultrasound for benign prostateic hyperplasia and prostate cancer. Plymouth Meeting (PA): ECRI Institute; 2010 October 01. (ECRI ho Also available at: ECRI Institute. Photoselective vaporization of the prostate for benign prostatic hyperplasia. Plymouth Meeting (PA): ECRI Institute; 2010 September 20. (ECRI hotline respo available at: ECRI Institute. Transurethral microwave therapy (TUMT) for benign prostatic hypertrophy. Plymouth Meeting (PA): ECRI Institute; 2004 October 10. (ECRI hotline response at:
8 ECRI Institute. Water-induced thermotherapy for benign prostatic hyperplasia. Plymouth Meeting (PA): ECRI Institute; 2011 April 22. (ECRI hotline response). Also availabl Elzayat EA, Elhilali MN. Holmium laser enucleation of the prostate (HoLEP): long-term results, reoperation rate, and possible impact of the learning curve. Eur Urol. 2007;5 Fitzpatrick JM, et al. Minimally invasive and endoscopic management of benign prostatic hyperplasia. In: Wein AJ. Campbell-Walsh Urology. 9th ed. Philadelphia, PA: WB S Chapter 88. Gilling P, Mackey M, Cresswell M, et al. Holmium laser versus transurethral resection of the prostate: a randomized prospective trial with 1-year follow up. J Urol.1999;162 Hill B, Belville W, Bruskewitz R, et al. Transurethral needle ablation versus transurethral resection of the prostate for the treatment of symptomatic benign prostatic hyperpla results of a prospective, randomized, multicenter clinical trial. J Urol. 2004;171(6 Pt 1): Hoffman RM, MacDonald R, Wilt TJ. Laser prostatectomy for benign prostatic obstruction. Cochrane Database of Sys Rev. 2004;1:CD Hoffman RM, Monga M, Elliot SP, et al. Microwave thermotherapy for benign prostatic hyperplasia. Cochrane Database Sys Rev.2007;Oct 14;(4):CD Kuntz R, Lehrich K. Transurethral holmium laser enucleation versus transvesical open enucleation for prostate adenoma greater that 100 gm: a randomized prospective tria J Urol.2002;168(4 Pt 1): Kursh ED, Concepcion R, Chan S, et al. Interstitial laser coagulation versus transurethral prostate resection for treating benign prostatic obstruction: a randomized trial with up. Urology. 2003;61(3): Larson TR. Rationale and assessment of minimally invasive approaches to benign prostatic hyperplasia therapy. Urology. 2002;59(2 Suppl 1): Liedberg F, Adell L, Hagberg G, Palmqvist IB. Interstitial laser coagulation versus transurethral resection of the prostate for benign prostatic enlargement: a prospective ran Scand J Urol Nephrol. 2003;37(6): McVary KT. Clinical evaluation of benign prostatic hyperplasia. [National Center for Biotechnology Information (NCBI) Web site] Available at: Accessed November 06, Mottet N, Anidjar M, Bourdon O, et al. Randomized comparison of transurethral electroresection and Holmium:YAG laser vaporization for symptomatic benign prostatic hyp Endourol.1999;13(2): Montorsi F, Naspro R, Salonia A, et al. Holmium laser enucleation versus transurethral resection of the prostate: results from a 2-center, prospective, randomized trial in pa obstructive benign prostatic hyperplasia. J Urol. 2008;179(5 Suppl):S87-S90. Muruve NA, Steinbecker K, Willard TB. Transurethral needle ablation of the prostate (TUNA). [emedicine Web site]. 03/29/11. Available at: Accessed November 06, Muschter R, Schorsch I, Danielli L, et al. Transurethral water-induced thermotherapy for the treatment of benign prostatic hyperplasia: a prospective multicenter clinical trial
9 2000;164(5): Naspro R, Bachmann A, Gilling P, et al. A review of the recent evidence ( ) for 532-nm photoselective laser vaporization and holmium laser enucleation of the pro Urol.2009;56(6): Neotract Inc. Urolift--BPH Relief In Sight Available at: Accessed 10/2014 Novitas Solutions. Local Coverage Determination (LCD). L27534: Thermotherapies (minimally invasive surgical techniques [MISTs]) for benign prostatic hyperplasia (BPH) Solutions Web site]. Original: 07/11/08. (Revised: 04/02/2012). Available at: Accessed November 06, 2014 Planz B, Kalem T, Sprenger C, et al. A prospective randomized study of combined visual laser ablation and transurethral resection of the prostate versus transurethral pros Urol Int. 2003;71(1): Poulakis V, Dahm P, Witzsch U, et al. Transurethral electrovaporization vs. transurethral resection for symptomatic prostatic obstruction: a meta-analysis. BJU Int.2004;94( Ruszat R, Wler SF, Seitz M, et al. Comparison of potassium-titanyl-phosphate laser vaporization of the prostate and transurethral resection of the prostate: update of a pros randomized two-centre study. BJU Int.2008;102(10): Schorsch I, Muschter R, Danielli L, et al. Two year follow-up of a multi-center clinical study using water-induced thermotherapy for BPH. Paper presented at: American Urol Association Annual Meeting; May 2, 2000; Atlanta, GA. Notification Coding Inclusion of a code in this table does not imply reimbursement. Eligibility, benefits, limitations, exclusions, precertification/referral requirements, provider cont Company policies apply. The codes listed below are updated on a regular basis, in accordance with nationally accepted coding guidelines. Therefore, this policy applies to any and all fu coding changes, revisions, or updates. In order to ensure optimal reimbursement, all health care services, devices, and pharmaceuticals should be reported using the billing codes and modifiers that accurately represent the services rendered, unless otherwise directed by the Company. The Coding Table lists any CPT, ICD-9, ICD-10, and HCPCS billing codes related only to the specific policy in which they appear. Notification CPT Procedure Code Number(s)
10 MEDICALLY NECESSARY THE FOLLOWING CODES REPRESENT TRANSURETHRAL RESECTION OF THE PROSTATE (TURP) 52601, THE FOLLOWING CODES REPRESENT TRANSURETHRAL RESECTION OF THE PROSTATE (TURP) 52601, THE FOLLOWING CODE REPRESENTS HOLMIUM LASER ABLATION OF THE PROSTATE (HoLRP), PHOTOSELECTIVE VAPORIZATION (PVP), and TRANSURET ELECTROVAPORIZATION OF THE PROSTATE (TUVP) THE FOLLOWING CODE REPRESENTS HOLMIUM LASER ENUCLEATION OF THE PROSTATE (HoLEP) and HOLMIUM LASER RESECTION OF THE PROSTATE THE FOLLOWING CODE REPRESENTS TRANSURETHRAL NEEDLE ABLATION OF THE PROSTATE (TUNA) NOT MEDICALLY NECESSARY THE FOLLOWING CODE REPRESENTS VISUAL LASER ABLATION OF THE PROSTATE (VLAP) AND INTERSTITIAL LASER COAGULATION (ILC) THE FOLLOWING CODES REPRESENT TRANSURETHRAL ULTRASOUND-GUIDED LASER-INDUCED PROSTATECTOMY (TULIP) 52648, THE FOLLOWING CODE REPRESENTS WATER-INDUCED THERMOTHERAPY (WIT) THE FOLLOWING CODE REPRESENTS TRANSURETHRAL MICROWAVE THERMOTHERAPY (TUMT) THE FOLLOWING CODES REPRESENT PROSTATIC URETHRAL LIFT (UROLIFT ) 52441, EXPERIMENTAL/INVESTIGATIONAL THE FOLLOWING CODE REPRESENTS TRANSURETHRAL BALLOON DILATION 53899
11 THE FOLLOWING CODE REPRESENTS TRANSURETHRAL ETHANOL ABLATION OF THE PROSTATE (TEAP) THE FOLLOWING CODE REPRESENTS HIGH-INTENSITY FOCUSED ULTRASOUND (HIFU) ICD - 9 Procedure Code Number(s) N/A ICD - 10 Procedure Code Number(s) ICD-10-PCS codes will be in effect on the determined ICD-10 compliance date. However, they are being added to policy for informational purposes only. N/A N/A N/A ICD - 9 Diagnosis Code Number(s) 185 Malignant neoplasm of prostate Hypertrophy (benign) of prostate with urinary obstruction and other lower urinary tract symptoms (LUTS) Nodular prostate with urinary obstruction Benign localized hyperplasia of prostate with urinary obstruction and other lower urinary tract symptoms (LUTS) Hyperplasia of prostate, unspecified with urinary obstruction V10.46 Personal history of malignant neoplasm of prostate ICD -10 Diagnosis Code Number(s)
12 ICD-10-CM codes will be in effect on the determined ICD-10 compliance date. However, they are being added to policy for informational purposes only. C61 Malignant neoplasm of prostate N40.1 Enlarged prostate with lower urinary tract symptoms N40.3 Nodular prostate with lower urinary tract symptoms Z85.46 Personal history of malignant neoplasm of prostate HCPCS Level II Code Number(s) Healthcare Common Procedure Coding System (HCPCS) C Series Codes can only be reported for outpatient facility services. Professional providers should not report HCPCS C Series Codes for professional services regardless of where those services are performed: THE FOLLOWING CODES REPRESENT PROSTATIC URETHRAL LIFT (UROLIFT ) C9739 Cystourethroscopy, with insertion of transprostatic implant; 1 to 3 implants C9740 Cystourethroscopy, with insertion of transprostatic implant; 4 or more implants N/A Revenue Code Number(s)! Version Effective Date: 04/08/2015
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
POLICIES AND PROCEDURE MANUAL
 POLICIES AND PROCEDURE MANUAL Policy: MP048 Section: Medical Benefit Policy Subject: Surgical and Minimally Invasive Therapies for the Treatment of Benign Prostatic Hypertrophy I. Policy: Surgical and
POLICIES AND PROCEDURE MANUAL Policy: MP048 Section: Medical Benefit Policy Subject: Surgical and Minimally Invasive Therapies for the Treatment of Benign Prostatic Hypertrophy I. Policy: Surgical and
NOTE: This policy is not effective until April 1, Transurethral Water Vapor Thermal Therapy of the Prostate
 NOTE: This policy is not effective until April 1, 2019. Medical Policy Manual Surgery, Policy No. 210 Transurethral Water Vapor Thermal Therapy of the Prostate Next Review: December 2019 Last Review: December
NOTE: This policy is not effective until April 1, 2019. Medical Policy Manual Surgery, Policy No. 210 Transurethral Water Vapor Thermal Therapy of the Prostate Next Review: December 2019 Last Review: December
Treating BPH: Comparing Rezum UroLift and HoLEP
 Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
Benign Prostatic Hyperplasia (BPH)
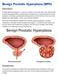 Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Name of Policy: Transurethral Microwave Thermotherapy
 Name of Policy: Transurethral Microwave Thermotherapy Policy #: 449 Latest Review Date: September 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable
Name of Policy: Transurethral Microwave Thermotherapy Policy #: 449 Latest Review Date: September 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable
What is Benign Prostatic Hyperplasia (BPH)?
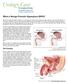 What is Benign Prostatic Hyperplasia (BPH)? Benign prostatic hyperplasia (BPH) is an enlarged prostate. The prostate goes through two main growth periods as a man ages. The first occurs early in puberty,
What is Benign Prostatic Hyperplasia (BPH)? Benign prostatic hyperplasia (BPH) is an enlarged prostate. The prostate goes through two main growth periods as a man ages. The first occurs early in puberty,
Subject: Temporary Prostatic Stent and Prostatic Urethral Lift
 02-54000-21 Original Effective Date: 03/15/05 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Temporary Prostatic Stent and Prostatic Urethral Lift THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
02-54000-21 Original Effective Date: 03/15/05 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Temporary Prostatic Stent and Prostatic Urethral Lift THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
MODULE 3: BENIGN PROSTATIC HYPERTROPHY
 MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
Rezūm procedure for the Prostate
 Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Executive Summary. Non-drug local procedures for treatment of benign prostatic hyperplasia 1. IQWiG Reports - Commission No.
 IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Surgical procedures for benign prostatic hyperplasia: A nationwide survey in Japan
 International Journal of Urology (2011) 18, 166 170 doi: 10.1111/j.1442-2042.2010.02687.x Short Communicationiju_2687 166..170 Surgical procedures for benign prostatic hyperplasia: A nationwide survey
International Journal of Urology (2011) 18, 166 170 doi: 10.1111/j.1442-2042.2010.02687.x Short Communicationiju_2687 166..170 Surgical procedures for benign prostatic hyperplasia: A nationwide survey
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
50% of men. 90% of men PATIENT FACTSHEET: BPH CONDITION AND TREATMENTS. Want more information? What are the symptoms?
 PATIENT FACTSHEET: BPH CONDITION AND TREATMENTS What is Benign Prostatic Hyperplasia (enlarged prostate)? Benign prostatic hyperplasia (BPH) is a noncancerous enlargement of the prostate, the gland that
PATIENT FACTSHEET: BPH CONDITION AND TREATMENTS What is Benign Prostatic Hyperplasia (enlarged prostate)? Benign prostatic hyperplasia (BPH) is a noncancerous enlargement of the prostate, the gland that
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Benign Prostatic Hyperplasia: Update on Innovative Current Treatments
 Benign Prostatic Hyperplasia: Update on Innovative Current Treatments Michael Ferrandino, MD As.soc Professor Director of Minimally Invasive Urologic Surgery Division of Urologic Surgery Duke University
Benign Prostatic Hyperplasia: Update on Innovative Current Treatments Michael Ferrandino, MD As.soc Professor Director of Minimally Invasive Urologic Surgery Division of Urologic Surgery Duke University
PATIENT INFORMATION 2017 NeoTract, Inc. All rights reserved. Printed in the USA. MAC Rev A
 PATIENT INFORMATION OVER 70% OF MEN IN THEIR 60s HAVE SYMPTOMS OF BPH 1 BPH affects more than 500 million men worldwide, with many men suffering from symptoms of enlarged prostate. 1 You no longer have
PATIENT INFORMATION OVER 70% OF MEN IN THEIR 60s HAVE SYMPTOMS OF BPH 1 BPH affects more than 500 million men worldwide, with many men suffering from symptoms of enlarged prostate. 1 You no longer have
OVER 70% OF MEN IN THEIR 60s HAVE SYMPTOMS OF BPH 1
 PATIENT INFORMATION BPH affects more than 500 million men worldwide, with many men suffering from symptoms of enlarged prostate. 1 You no longer have to be one of them! OVER 70% OF MEN IN THEIR 60s HAVE
PATIENT INFORMATION BPH affects more than 500 million men worldwide, with many men suffering from symptoms of enlarged prostate. 1 You no longer have to be one of them! OVER 70% OF MEN IN THEIR 60s HAVE
Benign Prostatic Hyperplasia (BPH):
 Benign Prostatic Hyperplasia (BPH): Evidence Based Guidelines for Primary Care Providers Jeanne Martin, DNP, ANP-BC Objectives 1. Understand the pathophysiology and prevalence of BPH 2. Select the appropriate
Benign Prostatic Hyperplasia (BPH): Evidence Based Guidelines for Primary Care Providers Jeanne Martin, DNP, ANP-BC Objectives 1. Understand the pathophysiology and prevalence of BPH 2. Select the appropriate
Medical Coverage Policy Prostatic Urethral Lifts
 Medical Coverage Policy Prostatic Urethral Lifts EFFECTIVE DATE:01 01 2017 POLICY LAST UPDATED: 10 03 2017 OVERVIEW Benign prostatic hyperplasia is a common condition in older men that can lead to increased
Medical Coverage Policy Prostatic Urethral Lifts EFFECTIVE DATE:01 01 2017 POLICY LAST UPDATED: 10 03 2017 OVERVIEW Benign prostatic hyperplasia is a common condition in older men that can lead to increased
Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj
 Original Article Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj Abstract Objectives: Prospective evaluation
Original Article Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj Abstract Objectives: Prospective evaluation
Surgical Treatment of LUTS in Men with BPE
 Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor
Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor
Overview. Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia. Iain McAuley September 15, 2014
 Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
Energy Delivery Systems for Treatment of Benign Prostatic Hyperplasia
 Ontario Health Technology Assessment Series 2006; Vol. 6, No. 17 Energy Delivery Systems for Treatment of Benign Prostatic Hyperplasia An Evidence-Based Analysis August 2006 Medical Advisory Secretariat
Ontario Health Technology Assessment Series 2006; Vol. 6, No. 17 Energy Delivery Systems for Treatment of Benign Prostatic Hyperplasia An Evidence-Based Analysis August 2006 Medical Advisory Secretariat
Transurethral Laser Technology: Treatments for BPH
 Transurethral Laser Technology: Treatments for BPH Richard Lee, MD Departments of Urology and Public Health The New York Presbyterian Hospital Weill Medical College of Cornell University Background Traditional
Transurethral Laser Technology: Treatments for BPH Richard Lee, MD Departments of Urology and Public Health The New York Presbyterian Hospital Weill Medical College of Cornell University Background Traditional
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
Chapter 2: Methodology
 Chapter 2: Methodology TABLE OF CONTENTS Introduction... 2 Study Selection and Data Abstraction... 2 Data Synthesis... 8 Guideline Development and Approvals... 9 Conflict of Interest... 10 Copyright 2010
Chapter 2: Methodology TABLE OF CONTENTS Introduction... 2 Study Selection and Data Abstraction... 2 Data Synthesis... 8 Guideline Development and Approvals... 9 Conflict of Interest... 10 Copyright 2010
Consensus Meeting for Asian-Pacific BPH Guideline
 Consensus Meeting for Asian-Pacific BPH Guideline Byung Ha Chung Yonsei University Health System S a t e l l i t e S y m p o s i u m I Contents Diagnosis and Treatment Guidelines for BPH Prostate Volume
Consensus Meeting for Asian-Pacific BPH Guideline Byung Ha Chung Yonsei University Health System S a t e l l i t e S y m p o s i u m I Contents Diagnosis and Treatment Guidelines for BPH Prostate Volume
Benign Prostatic Hyperplasia (BPH) Treatments
 Medical Coverage Policy Effective Date...10/15/2017 Next Review Date...10/15/2018 Coverage Policy Number... 0159 Benign Prostatic Hyperplasia (BPH) Treatments Table of Contents Related Coverage Resources
Medical Coverage Policy Effective Date...10/15/2017 Next Review Date...10/15/2018 Coverage Policy Number... 0159 Benign Prostatic Hyperplasia (BPH) Treatments Table of Contents Related Coverage Resources
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA
 St. Louis Hospital PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA INITIAL CLINICAL RESULTS Faculty of Medical Sciences New University of Lisbon JOÃO PISCO LUÍS CAMPOS PINHEIRO TIAGO BILHIM HUGO RIO TINTO
St. Louis Hospital PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA INITIAL CLINICAL RESULTS Faculty of Medical Sciences New University of Lisbon JOÃO PISCO LUÍS CAMPOS PINHEIRO TIAGO BILHIM HUGO RIO TINTO
Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP)
 JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
Original Article - Lasers in Urology. Min Ho Lee, Hee Jo Yang, Doo Sang Kim, Chang Ho Lee, Youn Soo Jeon
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Prostatic Urethral Lift Page 1 of 19 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Prostatic Urethral Lift Professional Institutional Original Effective Date:
Prostatic Urethral Lift Page 1 of 19 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Prostatic Urethral Lift Professional Institutional Original Effective Date:
Management of LUTS. Simon Woodhams February 2012
 Management of LUTS Simon Woodhams February 2012 The management of lower urinary tract symptoms (LUTS) in men Implementing NICE guidance May 2010 NICE clinical guideline 97 Background Lower urinary tract
Management of LUTS Simon Woodhams February 2012 The management of lower urinary tract symptoms (LUTS) in men Implementing NICE guidance May 2010 NICE clinical guideline 97 Background Lower urinary tract
EAU GUIDELINES POCKET EDITION 3
 EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
Prostate Artery Embolization
 Prostate Artery Embolization in the office interventional suite Robert J. Kennedy, M.D. Interventional & Vascular Center Melbourne, Florida The speaker has no financial conflicts of interest to disclose.
Prostate Artery Embolization in the office interventional suite Robert J. Kennedy, M.D. Interventional & Vascular Center Melbourne, Florida The speaker has no financial conflicts of interest to disclose.
Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH
 Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH The more you know, the better you ll feel. You ve likely had a discussion with your doctor about BPH 1. What follows are some
Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH The more you know, the better you ll feel. You ve likely had a discussion with your doctor about BPH 1. What follows are some
Control & confidence. You deserve both.
 Learn more about BPH and Plasma therapy Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH Your doctor is always happy to offer all the guidance you need so that you feel completely
Learn more about BPH and Plasma therapy Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH Your doctor is always happy to offer all the guidance you need so that you feel completely
Can men with prostates sized 80 ml or larger be managed conservatively?
 Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Prostatic Urethral Lift
 Prostatic Urethral Lift Policy Number: 7.01.151 Last Review: 10/2018 Origination: 10/2015 Next Review: 10/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Prostatic
Prostatic Urethral Lift Policy Number: 7.01.151 Last Review: 10/2018 Origination: 10/2015 Next Review: 10/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Prostatic
Management of Voiding Problems in Older Men. Dr. John Fenn Consultant, QEH 10 th October, 2005
 Management of Voiding Problems in Older Men Dr. John Fenn Consultant, QEH 10 th October, 2005 Voiding Problems Poor stream Hesitancy Straining Incomplete emptying Intermittent micturition Terminal dribbling
Management of Voiding Problems in Older Men Dr. John Fenn Consultant, QEH 10 th October, 2005 Voiding Problems Poor stream Hesitancy Straining Incomplete emptying Intermittent micturition Terminal dribbling
Submitted: August 15, Accepted: September 10, Published: October 15, 2018.
 Original Article doi: 10.22374/jeleu.v1i2.21 THULIUM LASER ENUCLEATION OF THE PROSTATE (THULEP) AS A TECHNIQUE FOR TREATMENT OF BPH: EVALUATION OF A SIX-YEAR EXPERIENCE AT A SINGLE INSTITUTION Mahmood
Original Article doi: 10.22374/jeleu.v1i2.21 THULIUM LASER ENUCLEATION OF THE PROSTATE (THULEP) AS A TECHNIQUE FOR TREATMENT OF BPH: EVALUATION OF A SIX-YEAR EXPERIENCE AT A SINGLE INSTITUTION Mahmood
Transurethral Hot Water Balloon Thermotherapy for Benign Prostatic Hyperplasia
 Transurethral Hot Water Balloon Thermotherapy for Benign Prostatic Hyperplasia Lance A. Mynderse, MD* and Thayne R. Larson, MD Address *Department of Urology, Mayo Foundation, 200 First Street, SW, Rochester,
Transurethral Hot Water Balloon Thermotherapy for Benign Prostatic Hyperplasia Lance A. Mynderse, MD* and Thayne R. Larson, MD Address *Department of Urology, Mayo Foundation, 200 First Street, SW, Rochester,
Prostatic Urethral Lift Corporate Medical Policy
 Prostatic Urethral Lift Corporate Medical Policy File Name: Prostatic Urethral Lift File Code: UM.SURG.19 Origination: 05/2018 Last Review: 01/2019 Next Review: 01/2020 Effective Date: 04/01/2019 Description/Summary
Prostatic Urethral Lift Corporate Medical Policy File Name: Prostatic Urethral Lift File Code: UM.SURG.19 Origination: 05/2018 Last Review: 01/2019 Next Review: 01/2020 Effective Date: 04/01/2019 Description/Summary
Policy #: 213 Latest Review Date: September 2012
 Name of Policy: Temporary Prostatic Stent Policy #: 213 Latest Review Date: September 2012 Category: Medicine Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates.
Name of Policy: Temporary Prostatic Stent Policy #: 213 Latest Review Date: September 2012 Category: Medicine Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates.
GUIDELINES ON NON-NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (BPO)
 GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (BPO) (Text update pril 2014) S. Gravas (chair),. Bachmann,. Descazeaud, M. Drake, C. Gratzke, S. Madersbacher, C. Mamoulakis,
GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (BPO) (Text update pril 2014) S. Gravas (chair),. Bachmann,. Descazeaud, M. Drake, C. Gratzke, S. Madersbacher, C. Mamoulakis,
BENIGN PROSTATIC HYPERPLASIA (BPH) affects 70%
 JOURNAL OF ENDOUROLOGY Volume 14, Number 2, March 2000 Mary Ann Liebert, Inc. Holmium Laser Enucleation of the Prostate With Tissue Morcellation: Initial United States Experience JEFFREY A. MOODY, M.D.,
JOURNAL OF ENDOUROLOGY Volume 14, Number 2, March 2000 Mary Ann Liebert, Inc. Holmium Laser Enucleation of the Prostate With Tissue Morcellation: Initial United States Experience JEFFREY A. MOODY, M.D.,
P ROLIEVE. Thermodilatation System. The Prolieve System Patient Information is Directed to You, the Patient. A Transurethral Microwave Therapy Device
 P ROLIEVE Thermodilatation System A Transurethral Microwave Therapy Device The Prolieve System Patient Information is Directed to You, the Patient. Contents Why am I being treated with the Prolieve Thermodilatation
P ROLIEVE Thermodilatation System A Transurethral Microwave Therapy Device The Prolieve System Patient Information is Directed to You, the Patient. Contents Why am I being treated with the Prolieve Thermodilatation
Medical Coverage Policy Prostatic Urethral Lifts
 Medical Coverage Policy Prostatic Urethral Lifts EFFECTIVE DATE:12 01 2018 POLICY LAST UPDATED: 10 03 2017 OVERVIEW Benign prostatic hyperplasia is a common condition in older men that can lead to increased
Medical Coverage Policy Prostatic Urethral Lifts EFFECTIVE DATE:12 01 2018 POLICY LAST UPDATED: 10 03 2017 OVERVIEW Benign prostatic hyperplasia is a common condition in older men that can lead to increased
HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION.
 IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT LASER AT YOUR SIDE IN YOUR HANDS is a high power holmium laser
IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT LASER AT YOUR SIDE IN YOUR HANDS is a high power holmium laser
Thulium Laser versus Standard Transurethral Resection of the Prostate: A Randomized Prospective Trial
 european urology 53 (2008) 382 390 available at www.sciencedirect.com journal homepage: www.europeanurology.com Benign Prostatic Obstruction Thulium Laser versus Standard Transurethral Resection of the
european urology 53 (2008) 382 390 available at www.sciencedirect.com journal homepage: www.europeanurology.com Benign Prostatic Obstruction Thulium Laser versus Standard Transurethral Resection of the
Cooled ThermoTherapy TM
 Are BPH Medications Weighing You Down? Think Outside the Pillbox Cooled ThermoTherapy TM A non-surgical, 30 minute in-office treatment that provides long-term relief from BPH symptoms and urinary obstruction
Are BPH Medications Weighing You Down? Think Outside the Pillbox Cooled ThermoTherapy TM A non-surgical, 30 minute in-office treatment that provides long-term relief from BPH symptoms and urinary obstruction
Benign prostatic hyperplasia (BPH)
 Diseases and Conditions Benign prostatic hyperplasia (BPH) By Mayo Clinic Staff Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate
Diseases and Conditions Benign prostatic hyperplasia (BPH) By Mayo Clinic Staff Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate
GUIDELINES ON NON-NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (Text update March 2015) S. Gravas (Chair), T. Bach,. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher, C. Mamoulakis,
GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (Text update March 2015) S. Gravas (Chair), T. Bach,. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher, C. Mamoulakis,
Last Review Status/Date: December Summary
 Section: Surgery Effective Date: January 15, 2016 Subject: Prostatic Urethral Lift Page: 1 of 9 Last Review Status/Date: December 2015 Summary Benign prostatic hyperplasia (BPH) is a common condition in
Section: Surgery Effective Date: January 15, 2016 Subject: Prostatic Urethral Lift Page: 1 of 9 Last Review Status/Date: December 2015 Summary Benign prostatic hyperplasia (BPH) is a common condition in
Review Article BPH Procedural Treatment: The Case for Value-Based Pay for Performance
 Advances in Urology Volume 2008, Article ID 954721, 6 pages doi:10.1155/2008/954721 Review Article BPH Procedural Treatment: The Case for Value-Based Pay for Performance Mark Stovsky and Irina Jaeger Department
Advances in Urology Volume 2008, Article ID 954721, 6 pages doi:10.1155/2008/954721 Review Article BPH Procedural Treatment: The Case for Value-Based Pay for Performance Mark Stovsky and Irina Jaeger Department
Chapter 4: Research and Future Directions
 Chapter 4: Research and Future Directions Introduction Many of the future research needs listed in the 1994 Agency for Health Care Policy and Research (AHCPR) clinical practice guideline Benign Prostatic
Chapter 4: Research and Future Directions Introduction Many of the future research needs listed in the 1994 Agency for Health Care Policy and Research (AHCPR) clinical practice guideline Benign Prostatic
Canada Medtronic of Canada Ltd Kitimat Road Mississauga, Ontario L5N 1W3 Canada Tel Fax
 What PATIENTS About TUNA Say Therapy TUNA THERAPY I would consider it to be a complete success. I have essentially no residual problems of any kind. I m back to the way I was before I ever had any symptoms
What PATIENTS About TUNA Say Therapy TUNA THERAPY I would consider it to be a complete success. I have essentially no residual problems of any kind. I m back to the way I was before I ever had any symptoms
Clinical Policy Title: Management of benign prostatic hyperplasia (BPH)
 Clinical Policy Title: Management of benign prostatic hyperplasia (BPH) Clinical Policy Number: 13.02.03 Effective Date: October 1, 2016 Initial Review Date: July 20, 2016 Most Recent Review Date: July
Clinical Policy Title: Management of benign prostatic hyperplasia (BPH) Clinical Policy Number: 13.02.03 Effective Date: October 1, 2016 Initial Review Date: July 20, 2016 Most Recent Review Date: July
The impact of minimally invasive surgeries for the treatment of symptomatic benign prostatic hyperplasia on male sexual function: a systematic review
 500 Review Asian Journal of Andrology (2010) 12: 500 508 2010 AJA, SIMM & SJTU All rights reserved 1008-682X/10 $ 32.00 www.nature.com/aja The impact of minimally invasive surgeries for the treatment of
500 Review Asian Journal of Andrology (2010) 12: 500 508 2010 AJA, SIMM & SJTU All rights reserved 1008-682X/10 $ 32.00 www.nature.com/aja The impact of minimally invasive surgeries for the treatment of
Medical technologies guidance Published: 16 September 2015 nice.org.uk/guidance/mtg26
 UroLift for treating lower urinary tract symptoms of benign prostatic hyperplasia Medical technologies guidance Published: 16 September 2015 nice.org.uk/guidance/mtg26 NICE 2018. All rights reserved. Subject
UroLift for treating lower urinary tract symptoms of benign prostatic hyperplasia Medical technologies guidance Published: 16 September 2015 nice.org.uk/guidance/mtg26 NICE 2018. All rights reserved. Subject
Chapter 3: Results of the Treatment Outcomes Analyses
 Chapter 3: Results of the Treatment Outcomes Analyses Introduction To determine the appropriateness of individual therapies, as well as to develop practice recommendations, the American Urological Association
Chapter 3: Results of the Treatment Outcomes Analyses Introduction To determine the appropriateness of individual therapies, as well as to develop practice recommendations, the American Urological Association
HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT
 IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT Manufactured by Asclepion Laser Technologies GmbH LASER AT
IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT Manufactured by Asclepion Laser Technologies GmbH LASER AT
APPENDIX CLINICAL INPUT RESPONSES
 CLINICAL INPUT RESPONSES AUA: American Urological Association; UCSF Med Ctr: University of California San Francisco Medical Center; PUL: prostatic urethral lift. * Indicates that information on conflicts
CLINICAL INPUT RESPONSES AUA: American Urological Association; UCSF Med Ctr: University of California San Francisco Medical Center; PUL: prostatic urethral lift. * Indicates that information on conflicts
Prostatic Urethral Lift. Summary
 Section: Surgery Effective Date: January 15, 2017 Subject: Prostatic Urethral Lift Page: 1 of 10 Last Review Status/Date: December 2016 Prostatic Urethral Lift Summary Benign prostatic hyperplasia (BPH)
Section: Surgery Effective Date: January 15, 2017 Subject: Prostatic Urethral Lift Page: 1 of 10 Last Review Status/Date: December 2016 Prostatic Urethral Lift Summary Benign prostatic hyperplasia (BPH)
Experience the Innovative Therapy for Benign Prostate Enlargement
 Experience the Innovative Therapy for Benign Prostate Enlargement A Guide to Treatment of Benign Prostatic Hyperplasia 1. 2. The Prostate The prostate gland is a part of the male reproductive system. A
Experience the Innovative Therapy for Benign Prostate Enlargement A Guide to Treatment of Benign Prostatic Hyperplasia 1. 2. The Prostate The prostate gland is a part of the male reproductive system. A
Long-term Follow-up of Transurethral Enucleation Resection of the Prostate for Symptomatic Benign Prostatic Hyperplasia
 Journal of Surgery 2016; 4(2): 40-44 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160402.18 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Long-term Follow-up of Transurethral Enucleation
Journal of Surgery 2016; 4(2): 40-44 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160402.18 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Long-term Follow-up of Transurethral Enucleation
Prostatic Urethral Lift
 Protocol Prostatic Urethral Lift (701151) Medical Benefit Effective Date: 04/01/18 Next Review Date: 01/19 Preauthorization No Review Dates: 05/17, 01/18 Preauthorization is not required. The following
Protocol Prostatic Urethral Lift (701151) Medical Benefit Effective Date: 04/01/18 Next Review Date: 01/19 Preauthorization No Review Dates: 05/17, 01/18 Preauthorization is not required. The following
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Prostatic Urethral Lift Page 1 of 17 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Prostatic Urethral Lift Professional Institutional Original Effective Date:
Prostatic Urethral Lift Page 1 of 17 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Prostatic Urethral Lift Professional Institutional Original Effective Date:
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Text update March 2017) S. Gravas (Chair), T. Bach, M. Drake, M. Gacci, C. Gratzke, T.R.W. Herrmann, S. Madersbacher,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Text update March 2017) S. Gravas (Chair), T. Bach, M. Drake, M. Gacci, C. Gratzke, T.R.W. Herrmann, S. Madersbacher,
Related Policies None
 Medical Policy MP 7.01.151 Original Policy Date: August 2015 Last Review: 12/27/2017 Effective Date: 03/01/2018 Section: Surgery Related Policies None DISCLAIMER Our medical policies are designed for informational
Medical Policy MP 7.01.151 Original Policy Date: August 2015 Last Review: 12/27/2017 Effective Date: 03/01/2018 Section: Surgery Related Policies None DISCLAIMER Our medical policies are designed for informational
Clinical guideline Published: 23 May 2010 nice.org.uk/guidance/cg97
 Lower urinary tract symptoms in men: management Clinical guideline Published: 23 May 2010 nice.org.uk/guidance/cg97 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Lower urinary tract symptoms in men: management Clinical guideline Published: 23 May 2010 nice.org.uk/guidance/cg97 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Related Policies None
 Medical Policy MP 7.01.151 BCBSA Ref. Policy: 7.01.151 Last Review: 12/27/2017 Effective Date: 03/01/2018 Section: Surgery End Date: 08/19/2018 Related Policies None DISCLAIMER Our medical policies are
Medical Policy MP 7.01.151 BCBSA Ref. Policy: 7.01.151 Last Review: 12/27/2017 Effective Date: 03/01/2018 Section: Surgery End Date: 08/19/2018 Related Policies None DISCLAIMER Our medical policies are
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: January 15, 2019 Related Policies: None Prostatic Urethral Lift Description Benign prostatic hyperplasia (BPH) is a common condition in older individuals that
FEP Medical Policy Manual Effective Date: January 15, 2019 Related Policies: None Prostatic Urethral Lift Description Benign prostatic hyperplasia (BPH) is a common condition in older individuals that
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of prostatic urethral lift implants to treat lower urinary tract symptoms
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of prostatic urethral lift implants to treat lower urinary tract symptoms
Surgical Management of Lower Urinary Tract Symptoms Attributed to Benign Prostatic Hyperplasia: AUA GUIDELINE
 1 Approved by the AUA Board of Directors May 2018 Authors disclosure of potential conflicts of interest and author/staff contributions appear at the end of the article. 2018 by the American Urological
1 Approved by the AUA Board of Directors May 2018 Authors disclosure of potential conflicts of interest and author/staff contributions appear at the end of the article. 2018 by the American Urological
Safety and efficacy of photoselective vaporization of the prostate using the 180-W GreenLight XPS laser system in patients taking oral anticoagulants
 Clinical Report Safety and efficacy of photoselective vaporization of the prostate using the 180-W GreenLight XPS laser system in patients taking oral anticoagulants Journal of International Medical Research
Clinical Report Safety and efficacy of photoselective vaporization of the prostate using the 180-W GreenLight XPS laser system in patients taking oral anticoagulants Journal of International Medical Research
PHOTOSELECTIVE POTASSIUM-TITANYL-PHOSPHATE LASER VAPORIZATION OF THE BENIGN OBSTRUCTIVE PROSTATE: OBSERVATIONS ON LONG-TERM OUTCOMES
 0022-5347/05/1744-1344/0 Vol. 174, 1344 1348, October 2005 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2005 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000173913.41401.67 PHOTOSELECTIVE
0022-5347/05/1744-1344/0 Vol. 174, 1344 1348, October 2005 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2005 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000173913.41401.67 PHOTOSELECTIVE
Lasers in Urology. An Evidence-Based Approach to Choosing the Right Tool
 Lasers in Urology An Evidence-Based Approach to Choosing the Right Tool Today medical lasers and specifically designed optical fibers offer benefits in a variety of surgical applications. Selecting the
Lasers in Urology An Evidence-Based Approach to Choosing the Right Tool Today medical lasers and specifically designed optical fibers offer benefits in a variety of surgical applications. Selecting the
GENDER HEALTH. Benign Prostatic Hyperplasia. Medical and Surgical Treatment Options
 GENDER HEALTH Benign Prostatic Hyperplasia Medical and Surgical Treatment Options ABSTRACT Benign prostatic hyperplasia (BPH) affects the aging male. Treatment options vary widely. Some men will elect
GENDER HEALTH Benign Prostatic Hyperplasia Medical and Surgical Treatment Options ABSTRACT Benign prostatic hyperplasia (BPH) affects the aging male. Treatment options vary widely. Some men will elect
Wednesday 25 June Poster Session 9: BPH 1 Chairmen: M. Speakman and D. Rosario
 Wednesday 25 June 14.30 15.30 Poster Session 9: BPH 1 Chairmen: M. Speakman and D. Rosario P080 Unreliable residual volume measurement after increased water load diuresis G. ALIVIZATOS, A. SKOLARIKOS,
Wednesday 25 June 14.30 15.30 Poster Session 9: BPH 1 Chairmen: M. Speakman and D. Rosario P080 Unreliable residual volume measurement after increased water load diuresis G. ALIVIZATOS, A. SKOLARIKOS,
PATIENT SELECTION GUIDE. finding the right fit
 PATIENT SELECTION GUIDE finding the right fit IDENTIFYING PATIENTS Rezūm, a new minimally invasive treatment, is now available to offer patients as a first-line BPH therapy. BPH TREATMENT OPTIONS Behavior
PATIENT SELECTION GUIDE finding the right fit IDENTIFYING PATIENTS Rezūm, a new minimally invasive treatment, is now available to offer patients as a first-line BPH therapy. BPH TREATMENT OPTIONS Behavior
Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate
 Singapore Med J 2016; 57(12): 676-680 doi: 10.11622/smedj.2016026 Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate Sundaram Palaniappan
Singapore Med J 2016; 57(12): 676-680 doi: 10.11622/smedj.2016026 Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate Sundaram Palaniappan
Comparison of outpatient versus inpatient transurethral prostate resection for benign prostatic hyperplasia: Comparative, prospective bi-centre study
 original research Comparison of outpatient versus inpatient transurethral prostate resection for benign prostatic hyperplasia: Comparative, prospective bi-centre study Jae Heon Kim, MD; * Jae Young Park,
original research Comparison of outpatient versus inpatient transurethral prostate resection for benign prostatic hyperplasia: Comparative, prospective bi-centre study Jae Heon Kim, MD; * Jae Young Park,
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: None Prostatic Urethral Lift Description Benign prostatic hyperplasia (BPH) is a common condition in older individuals that can
FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: None Prostatic Urethral Lift Description Benign prostatic hyperplasia (BPH) is a common condition in older individuals that can
Lasers in Urology. Laser Tissue Interaction, November 28 th, Qureshi, Muhammad Mohsin. Biomedical in vivo Opto-scopy Laboratory
 Laser Tissue Interaction, November 28 th, 2016 Lasers in Urology Qureshi, Muhammad Mohsin Gwangju Institute of Science and Technology Biomedical in vivo Opto-scopy Laboratory 2 Content Introduction to
Laser Tissue Interaction, November 28 th, 2016 Lasers in Urology Qureshi, Muhammad Mohsin Gwangju Institute of Science and Technology Biomedical in vivo Opto-scopy Laboratory 2 Content Introduction to
Number: Policy *Please see amendment for Pennsylvania Medicaid at the end of
 1 of 54 Number: 0079 Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB. I. Aetna considers the following approaches to the treatment of benign prostatic hypertrophy (BPH) medically
1 of 54 Number: 0079 Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB. I. Aetna considers the following approaches to the treatment of benign prostatic hypertrophy (BPH) medically
UroLift for treating lower urinary tract
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology consultation document UroLift for treating lower urinary tract The National Institute for Health and Care Excellence (NICE) is producing
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology consultation document UroLift for treating lower urinary tract The National Institute for Health and Care Excellence (NICE) is producing
All about the Prostate
 MEN S HEALTH Dr Nick Pendleton January 16 th 2018 All about the Prostate 1 What does it do? Functions of the Prostate 1. Secretes Prostatic Fluid slightly alkaline fluid, 30% of volume of seminal fluid,
MEN S HEALTH Dr Nick Pendleton January 16 th 2018 All about the Prostate 1 What does it do? Functions of the Prostate 1. Secretes Prostatic Fluid slightly alkaline fluid, 30% of volume of seminal fluid,
Benign enlargement of prostate (BEP), which is. Early Experiences with HoLEP. Original Article ABSTRACT INTRODUCTION. Bhandari BB*
 Original Article Early Experiences with HoLEP Bhandari BB* * Consultant Urologist, Shree Birendra Army Hospital, Norvic International Hospital, Alka Hospital ABSTRACT introduction: Holmium Laser Enucleation
Original Article Early Experiences with HoLEP Bhandari BB* * Consultant Urologist, Shree Birendra Army Hospital, Norvic International Hospital, Alka Hospital ABSTRACT introduction: Holmium Laser Enucleation
Holmium:YAG Transurethral Incision Versus Laser Photoselective Vaporization for Benign Prostatic Hyperplasia in a Small Prostate
 Holmium:YAG Transurethral Incision Versus Laser Photoselective Vaporization for Benign Prostatic Hyperplasia in a Small Prostate Ahmed M. Elshal, Mohamed A. Elkoushy, Hazem M. Elmansy, John Sampalis and
Holmium:YAG Transurethral Incision Versus Laser Photoselective Vaporization for Benign Prostatic Hyperplasia in a Small Prostate Ahmed M. Elshal, Mohamed A. Elkoushy, Hazem M. Elmansy, John Sampalis and
Lasers in Urology. Ju Hyun Park 1, Hwancheol Son 1,2, Jae-Seung Paick 1. DOI: /kju
 www.kjurology.org DOI:10.4111/kju.2010.51.2.115 Lasers in Urology Comparative Analysis of the Efficacy and Safety of Photoselective Vaporization of the Prostate for Treatment of Benign Prostatic Hyperplasia
www.kjurology.org DOI:10.4111/kju.2010.51.2.115 Lasers in Urology Comparative Analysis of the Efficacy and Safety of Photoselective Vaporization of the Prostate for Treatment of Benign Prostatic Hyperplasia
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Limited text update March 2016) S. Gravas (Chair), T. Bach, A. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Limited text update March 2016) S. Gravas (Chair), T. Bach, A. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher,
MEDICAL POLICY SUBJECT: TRANSRECTAL ULTRASOUND (TRUS)
 MEDICAL POLICY SUBJECT: TRANSRECTAL ULTRASOUND 06/16/05, 05/18/06, 03/15/07, 02/21/08 PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under
MEDICAL POLICY SUBJECT: TRANSRECTAL ULTRASOUND 06/16/05, 05/18/06, 03/15/07, 02/21/08 PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under
