Clinical Policy Title: Management of benign prostatic hyperplasia (BPH)
|
|
|
- Thomas Dixon
- 5 years ago
- Views:
Transcription
1 Clinical Policy Title: Management of benign prostatic hyperplasia (BPH) Clinical Policy Number: Effective Date: October 1, 2016 Initial Review Date: July 20, 2016 Most Recent Review Date: July 19, 2017 Next Review Date: July 2018 Related policies: Policy contains: Benign prostatic hyperplasia(bph) Benign prostatic hypertrophy (BPH) Transurethral resection of the prostate None. ABOUT THIS POLICY: AmeriHealth Caritas Pennsylvania has developed clinical policies to assist with making coverage determinations. AmeriHealth Caritas Pennsylvania s clinical policies are based on guidelines from established industry sources, such as the Centers for Medicare & Medicaid Services (CMS), state regulatory agencies, the American Medical Association (AMA), medical specialty professional societies, and peer-reviewed professional literature. These clinical policies along with other sources, such as plan benefits and state and federal laws and regulatory requirements, including any state- or plan-specific definition of medically necessary, and the specific facts of the particular situation are considered by AmeriHealth Caritas Pennsylvania when making coverage determinations. In the event of conflict between this clinical policy and plan benefits and/or state or federal laws and/or regulatory requirements, the plan benefits and/or state and federal laws and/or regulatory requirements shall control. AmeriHealth Caritas Pennsylvania s clinical policies are for informational purposes only and not intended as medical advice or to direct treatment. Physicians and other health care providers are solely responsible for the treatment decisions for their patients. AmeriHealth Caritas Pennsylvania s clinical policies are reflective of evidence-based medicine at the time of review. As medical science evolves, AmeriHealth Caritas Pennsylvania will update its clinical policies as necessary. AmeriHealth Caritas Pennsylvania s clinical policies are not guarantees of payment. Coverage policy AmeriHealth Caritas Pennsylvania considers the management of benign prostatic hyperplasia (BPH) to be clinically proven and, therefore, medically necessary when the following criteria are met: A. Indications: 1. Members age 45 years or older who present with obstructive and/ or irritative voiding symptoms (i.e. frequent urination and nocturia). 2. Acute urinary retention (i.e., the sudden inability to urinate). 3. Common obstructive symptoms: a. Hesitancy (difficulty initiating the urinary stream; interrupted, weak stream). b. Straining to void. c. Dribbling, (loss of small amounts of urine due to a poor urinary stream). d. Sensation of incomplete voiding. 1
2 B. Pharmacotherapy is considered first-line treatment for moderate to severe symptomatic BPH in members who do not have concomitant renal insufficiency, refractory urinary retention, persistent hematuria, recurrent bladder stones, or recurrent urinary tract infections (UTIs). C. When nonsurgical management has failed the following procedures are clinically proven and, therefore, medically necessary: 1. Minimally Invasive Therapies Limitations: Transurethral electrical vaporization of the prostate (TUEVP, TUVP, TVP), transurethral vapor resection (TUVRP). Transurethral microwave thermotherapy (TUMT). Transurethral needle ablation (TUNA) or radiofrequency needle ablation (RFNA). 2. Surgical Treatments Open or laparoscopic prostatectomy. Transurethral incision of the prostate (TUIP). Transurethral resection of the prostate (TURP). 3. Laser Therapy: Contact laser ablation of the prostate (CLAP). Holmium laser ablation/enucleation/resection (HoLAP, HoLEP, HoLRP). Noncontact visual ablation (VLAP). Photoselective vaporization of the prostate (PVP). Laser vaporization and laser ablation/coagulation). All other treatments for BPH are not medically necessary because each is considered experimental, investigational or unproven. There is limited data to demonstrate improved health outcomes for members with BPH treated with the following therapies. The treatments are (this list may not be allinclusive): 1. Absolute ethanol injection. 2. Cryosurgical ablation. 3. High-intensity focused ultrasound (HIFU). 4. Histotripsy. 5. Interstitial laser coagulation (ILC). 6. Plasma kinetic vaporization (e.g., PlasmaKinetic Tissue Management System). 7. Prostate artery embolization. 8. Prostatic urethral lift. 9. Transrectal thermal therapy. 10. Transurethral balloon dilation of the prostatic urethra. 11. Transurethral ultrasound-guided laser incision of the prostate (TULIP). 12. Direct injection of botulinum toxin in to the prostate gland. 13. Water-induced thermotherapy (WIT). 2
3 Note: Transurethral water-induced thermotherapy (WIT), performed in the physician s office, is a new procedure that has been shown in a large clinical study to significantly relieve lower urinary tract symptoms (LUTS) due to BPH; however, its long-term effectiveness has not been determined. Alternative covered services: For members with moderate to severe symptoms of BPH, watchful waiting (active surveillance).with a participating provider. Note: Watchful waiting (active surveillance) is the preferred management strategy for patients with mild symptoms. It is also an appropriate option for men with moderate-to-severe symptoms who have not yet developed complications of LUTS and BOO (e.g., renal insufficiency, urinary retention or recurrent infection). Watchful waiting patients usually are reexamined yearly, repeating the initial evaluation. Background Benign prostatic hyperplasia (BPH), also known as benign prostatic hypertrophy, is a histologic diagnosis characterized by proliferation of the cellular elements of the prostate. Chronic bladder outlet obstruction (BOO) secondary to BPH may lead to urinary retention, renal insufficiency, recurrent urinary tract infections, gross hematuria, and bladder calculi. The digital rectal examination (DRE) is an integral part of the evaluation in men with presumed BPH. During this portion of the examination, prostate size and contour can be assessed, nodules can be evaluated, and areas suggestive of malignancy can be detected. The normal prostate volume in a young man is approximately 20 grams. The prevalence and the severity of lower urinary tract symptoms (LUTS) in the aging male can be progressive, and is an important diagnosis in the healthcare of our patients and the welfare of society. In assessing the burden of disease, the Urologic Diseases in America BPH Project examined the prevalence of moderate to-severe LUTS reported in U.S. population-based studies that used the definition of an American Urological Association (AUA) Symptom Index (SI) score of 7 (Wei, 2008). Results from the Olmsted County Study showed a progressive increase in the prevalence of moderate-to-severe LUTS, rising to nearly 50 percent by the eighth decade of life (Lepor, 2003). A multinational study estimates that the prevalence of men with at least one LUTS symptom is 72.3 percent (Coyne, 2009). Two scores are widely used to evaluate BPH-related symptoms. The American Urological Association Symptom Index (AUASI) is a self-administered 7-item questionnaire assessing the severity of various urinary symptoms. Total AUASI scores range from 0 to 35 with overall severity categorized as mild (<7), moderate (8-19), or severe (20-35) (Barry, 2017). The International Prostate Symptoms Score (IPSS) incorporates the questions from the AUASI and a quality of life question or bother score (I-PSS, 2017). 3
4 The IPSS is based on the answers to seven questions concerning urinary symptoms and one question concerning quality of life, namely incomplete emptying, frequency, intermittency, urgency, weak stream, straining, and nocturia. Question eight refers to the patient s perceived quality of life. The International Scientific Committee (SCI), under the patronage of the World Health Organization (WHO) and the International Union against Cancer (UICC), recommends the use of only a single question to assess the quality of life. The answers to this question range from delighted to terrible or 0 to 6. Although this single question may or may not capture the global impact of BPH symptoms or quality of life, it may serve as a valuable starting point for a doctor-patient conversation. The SCI has agreed to use the symptom index for BPH, which has been developed by the AUA Measurement Committee, as the official worldwide symptoms assessment tool for patients suffering from prostatism. The SCI recommends that physicians consider the following components for a basic diagnostic workup: history, physical exam, appropriate labs, such as U/A, creatine, etc., and DRE or other evaluation to rule out prostate cancer. Treatment options: A discussion about medical therapy is generally indicated for patients with moderate-to-severe symptoms (e.g., AUASI score, 8), bothersome symptoms, or both. Available medical therapies for BPHrelated lower urinary tract dysfunction include alpha-adrenergic blockers (e.g., alfuzosin, doxazosin, tamsulosin, terazosin, and silodosin), 5-alpha-reductase inhibitors (e.g., finasteride, dutasteride), combination alpha-adrenergic blockers and 5-alpha-reductase inhibitors, anti-muscarinic agents (e.g., darifenacin, solifenacin, oxybutynin), and phosphodiesterase-5 inhibitors (e.g., tadalafil). The gold standard for treating BPH is transurethral resection of the prostate (TURP). Treatment of BPH should be individualized to the patient and involves evaluation of symptoms along with objective findings from examination and laboratory results. Initial treatment for BPH is usually drug therapy designed to relieve obstruction, but this often provides only modest relief and up to 30 percent of patients require surgical intervention (Roehrborn, 2011). There are several surgical treatments for BPH that involve burning, cutting, or removal of prostatic tissue (Hayes, 2015; Moul, 2015). Traditionally, the primary goal of treatment has been to alleviate bothersome LUTS that result from prostatic enlargement. More recently, treatment has additionally been focused on the alteration of disease progression and prevention of complications that can be associated with BPH/LUTS. A variety of pharmacologic classes are employed including alpha-adrenergic antagonists (alpha-blockers), 5-alphareductase inhibitors (5-ARIs), anticholinergics and phytotherapeutics. Choosing the correct medical treatment for BPH is truly complex and ever-changing. Surgery options: Surgical intervention is an appropriate treatment alternative for patients with moderate-to- severe LUTS and for patients who have developed AUR or other BPH-related complications. By definition, surgery is 4
5 the most invasive option for BPH management and generally, patients will have failed medical therapy before proceeding with surgery. However, medical therapy may not be viewed as a requirement because some patients may wish to pursue the most effective therapy as a primary treatment if their symptoms are particularly bothersome. As with other medical treatment alternatives, the decision to elect surgery as the treatment alternative is based upon the patient's own views of treatment risks vs. benefits. The 2003 AUA Guideline recognized that TURP remained the benchmark for therapy. Alternative technologies such as laser-assisted TURP were reported to offer lower morbidities but were typically still performed in the operating room setting and require anesthesia. Surgery is recommended for patients who have renal insufficiency secondary to BPH, who have recurrent UTIs, bladder stones or gross hematuria due to BPH, and those who have LUTS refractory to other therapies. The presence of a bladder diverticulum is not an absolute indication for surgery unless associated with recurrent UTI or progressive bladder dysfunction. Open prostatectomy: Open prostatectomy is an appropriate and effective treatment alternative for men with moderate to severe LUTS and/or who are significantly bothered by these symptoms. The choice of approach should be based on the patient's individual presentation including anatomy, the surgeon's experience, and discussion of the potential benefit and risks for complications. The AUA 2014 guideline (McVary, 2014) noted that there is usually a longer hospital stay and a larger loss of blood associated with open procedures. Laser therapies: Transurethral laser enucleation (holmium laser resection of the prostate [HoLRP], holmium laser enucleation of the prostate [HoLEP]), transurethral side firing laser ablation (holmium laser ablation of the prostate [HoLAP], and photoselective vaporization [PVP]) are appropriate and effective treatment alternatives to transurethral resection of the prostate and open prostatectomy in men with moderate to severe LUTS and/or those who are significantly bothered by these symptoms. The choice of approach should be based on the patient's presentation, anatomy, the surgeon's level of training and experience, and a discussion of the potential benefit and risks for complications. Generally, transurethral laser approaches have been associated with shorter catheterization time and length of stay, with comparable improvements in LUTS. There is a decreased risk of the perioperative complication of transurethral resection syndrome. Information concerning certain outcomes, including retreatment and urethral strictures, is limited due to short follow-up. As with all new devices, comparison of outcomes between studies should be considered cautiously given the rapid evolution in technologies and power levels. Emerging evidence suggests a possible role of transurethral enucleation and laser vaporization as options for men with very large prostates (> 100 g). 5
6 In general, laser energy can be used to produce a variety of effects within prostate tissue including coagulation necrosis or vaporization and resection of tissue. Today, the holmium and variants of the PVP laser are the most common laser technologies used to treat prostate disorders. Transurethral Holmium Laser Ablation of the Prostate (HoLAP): The holmium:yag laser may be used to treat prostatic tissue transurethrally using a 550 micron sidefiring laser fiber in a noncontact mode. This technology delivers laser energy at a wavelength of 2120 nm (infrared range) which is absorbed primarily by water and results in an optical penetration depth of 0.4 mm. The HoLAP procedure is intended to be comparable to TURP in that the prostatic lobes may be vaporized down to the surgical capsule resulting in a TURP-like effect. Transurethral Holmium Laser Enucleation of the Prostate (HoLEP): The holmium laser has been used to enucleate the prostate adenoma, separating the adenoma from the surgical capsule, from apex to base, after any median lobe has been freed from the bladder neck. Typically, the technology is utilized for larger glands that previously would have been treated surgically with an open prostatectomy. Generally, the results compare favorably to open prostatectomy in the hands of an experienced surgeon. In other trials, improvements in symptom scores, quality of life (QoL) indices, and flow rate, approach those obtained after TURP. Nonetheless, long-term data beyond two years are still lacking, and the procedure requires specialized training and equipment. The AUA guideline authors believe that the learning curve for holmium laser enucleation of the prostate appears to be greater than that of other technologies. Photoselective Vaporization of the Prostate (PVP): PVP of the prostate is a form of transurethral prostatectomy performed using a 600 micron side- firing fiber in a noncontact mode. The primary difference from HoLAP is its wavelength of 532 nm (in the green visible spectrum) which is absorbed by both the water irrigation and hemoglobin resulting in an optical penetration depth of 0.8 mm. The other acronyms for this procedure, KTP (potassium tintanyl phosphate) and LBO (lithium borate), identify the crystal used in the laser generator. Typically performed using normal saline irrigation and a continuous flow scope, the goal of PVP is to create a TURP-like cavity after ablating the various prostatic lobes down to the surgical capsule. Symptom scores improved consistently in all studies, as did Qi scores and maximum urinary flow rates. Transurethral Needle Ablation (TUNA) of the Prostate: TUNA of the prostate is an appropriate and effective treatment alternative for bothersome moderate or severe LUTS secondary to BPH. Transurethral Microwave Thermotherapy (TUMT) 6
7 TUMT is effective in partially relieving LUTS secondary to BPH and may be considered in men with moderate or severe symptoms. It heats the prostate using a microwave antennae mounted on a urethral catheter. This interventional therapy is effective in partially relieving the symptoms and bother believed secondary to BPH. TUMT is the least operator-dependent of the BPH interventions and predicting responders is difficult and inconsistent. Transurethral Incision of the Prostate (TUIP) TUIP is an appropriate and effective treatment alternative in men with moderate to severe LUTS and/or who are significantly bothered by these symptoms when prostate size is less than 30 cc. The choice of approach should be based on the patient's individual presentation including anatomy, the surgeon's experience and discussion of the potential benefits and risks for complications. The Diagnosis Improvement in Primary Care Trial (D-IMPACT), a prospective, multicenter study in three European countries, identified simple tests for primary care practitioners to diagnose BPH in men who present with LUTS. D-IMPACT found that a diagnostic algorithm including only the objective variables of age, International Prostate Symptom Score (IPSS) and prostate-specific antigen level (PSA), allows accurate diagnosis of BPH in approximately three-quarters of patients who report LUTS (Carballido, 2011). Searches AmeriHealth Caritas Pennsylvania searched PubMed and the databases of: UK National Health Services Centre for Reviews and Dissemination. Agency for Healthcare Research and Quality s National Guideline Clearinghouse and other evidence-based practice centers. The Centers for Medicare & Medicaid Services (CMS). We conducted searches on May 26, Search terms were: benign prostatic hypertrophy, and benign prostatic hyperplasia. We included: Systematic reviews, which pool results from multiple studies to achieve larger sample sizes and greater precision of effect estimation than in smaller primary studies. Systematic reviews use predetermined transparent methods to minimize bias, effectively treating the review as a scientific endeavor, and are thus rated highest in evidence-grading hierarchies. Guidelines based on systematic reviews. Economic analyses, such as cost-effectiveness, and benefit or utility studies (but not simple cost studies), reporting both costs and outcomes sometimes referred to as efficiency studies which also rank near the top of evidence hierarchies. 7
8 Findings Numerous literature reviews have been published on treatments for benign prostatic hyperplasia. TURP, the traditional standard surgical treatment for BPH, is now used less with the development of other methods, and is generally used in cases of moderate-to-severe refractory LUTS or when complications in other procedures occur. One analysis of 67 studies (n=3470) documented that over the past three decades, patients undergoing TURP have greater average prostate tissue volume and lower morbidity rates, require fewer transfusions, experience more urinary tract infections rates, and have higher reported rates of failure to void (Mayer, 2012). The trend to substitute minimally invasive procedures for open procedures has continued for decades. One review of 27 observational studies (n=764) documented shorter hospital stays, reduced length of catheter use, shorter duration of operations, and less estimated blood loss in minimally invasive prostatectomy versus open prostatectomy. No differences were observed in Qmax, I-PSS, and perioperative complications, leading authors to conclude that minimally invasive procedures compare favorably with open procedures (Lucca, 2015). Laser therapies are one treatment mode increasingly used to treat BPH. A meta-analysis of six studies (n=640) compared outcomes for thulium laser prostatectomy (TmLRP) with TURP for one year after surgery. TmLRP was associated with less decrease of serum sodium salt, less blood transfused, shorter catheterization time, shorter hospital time and more operation time, while no differences between groups were noted in incidence of the TUR syndrome, recatheterization rate, transitory urge incontinence, stress incontinence, urethral stricture, and retrograde ejaculation (Jiang, 2016). A Hayes review of laser therapy used in men with BPH reviewed evidence and found support for several types of lasers. Holmium laser resection for BPH can be used for prostate glands <100 ml in volume that cannot be controlled by medicine; noncontact/contact/hybrid laser ablation techniques were found to be effective for prostate glands <70 ml in volume with bleeding or other disorders; and photoselective vaporization have good outcomes for BPH patients who cannot be effectively managed using medicinal therapy and who wish to avoid complications more often associated with TURP (Hayes, 2014). An analysis of nine trials (n=889) comparing the increasingly popular photoselective vaporization (PVP) with TURP found significantly lower catheterization time, length of stay, and blood transfusion rates for the PVP group, which took longer than TURP (average operating time 20 minutes greater). No significant differences were identified in complication rates (Thangasamy, 2012). Another analysis of 11 RCTs and case-controlled studies (n=1398) of men with prostate volume <70ml found PVP patients had fewer transfusions, capsular perforations, cases of TUR syndrome, and clot retentions than TURP patients (Ding, 2012). Another study of five trials comparing PVP with TURP showed fewer complications for those undergoing PVP (Zhang, 2012). A meta-analysis of 18 randomized controlled trials (n=2433) evaluated changes in erectile function for nine approaches to BPH. Of these treatments, only photoselective vaporization of the prostate resulted 8
9 in a decrease in erectile function, and a significant increase was observed post-operatively for Holmium laser enucleation of the prostate, plasmakinetic enucleation of the prostate, Thulium laser, and TURP (Li, 2016). These findings support those from a 2010 review of 33 studies on effects of minimally invasive surgery for BPH (Frieben, 2010). An analysis of 14 RCTs documented a 27 percent reductions in average AUA symptom score and a 13 percent increase in maximum urinary flow both statistically significant - three months after sham endoscopic procedure for BPH, with similar results for prostate based endoscopic studies. Authors warned that future trials would be strengthened with the inclusion of a placebo group in the form of sham surgery (Welliver, 2015). Policy updates: A total of 6 guidelines/other and 17 peer-reviewed references were added to this policy in Summary of clinical evidence: Citation Li (2016) Content, Methods, Recommendations Key points: Impact on erectile function for various BPH treatments Review of 18 articles (n=2433) on impact on erectile function of nine treatments for BPH Treatments included transurethral resection of the prostate (TURP), plasmakinetic resection of the prostate (PKRP), plasmakinetic enucleation of the prostate (PKEP), Holmium laser enucleation of the prostate (HoLEP), Holmium laser resection of the prostate (HoLRP), photoselective vaporization of the prostate (PV), Thulium laser, open prostatectomy (OP), and laparoscopic simple prostatectomy (LSP). None of the nine treatments reduced erectile function, except for PVP Postoperative erectile function significantly increased for those undergoing HoLEP, PKEP, Thulium laser, and TURP Lucca (2015) Key points: Minimally invasive simple prostatectomy for BPH Review of 27 studies (n=764) comparing outcomes for men undergoing minimally invasive simple prostatectomy with open simple prostatectomy The minimally invasive group had lower length of hospital stay, lower length of catheter use, less estimated blood loss, but average operating time was significantly higher Authors conclude that minimally invasive procedures offer an effective, safe option Hayes (2014) Key points: Laser therapy for benign prostatic hyperplasia Literature review of studies from 1985 to 2010, that included at least six months of follow up, included at least 50 patients with symptomatic BPH, and measured symptoms and/or objective urinary outcomes Holmium laser resection of the prostate had favorable outcomes for patients with prostate sizes <100 g, who cannot be managed with medical therapy, and who wish to avoid certain complications associated with TURP Non-contact, contact, and laser ablation techniques had favorable outcomes in BPH patients whose prostate sizes are less than grams and who have conditions such as bleeding disorders, and who wish to avoid TURP complications 9
10 Citation Thangasamy (2012) Content, Methods, Recommendations Photoselective vaporization of the prostate had favorable outcomes for BPH patients who cannot be managed with medicine and who wish to avoid TURP complications Key points: Outcomes of photoselective vaporization compared to TURP Review of nine trials; 448 patients underwent PVP, 441 underwent TURP In the PVP group, catheterization time and length of stay were significantly shorter, blood transfusion was less likely In the TURP group, average operating time was 20 minutes less No differences found for all other complications References Professional society guidelines/other: American Cancer Society recommendations for prostate cancer early detection (ACS). Last revised April, Accessed: May 25, Cunningham GR, O Leary MP, Libman H. Medical treatment of benign prostate hyperplasia. UptoDate. Last updated November, Accessed May 25, International Prostate Symptom Score (I-PSS) Accessed May 26, McVary KT, Roehrborn CG, Avins AL, et al. Management of benign prostatic hyperplasia (BPH). American Urological Association (AUA). Last confirmed Accessed May 25, National Institute for Health and Care Excellence (NICE). Greenlight XPS for treating benign prostatic hyperplasia. June Accessed May 25, Nickel JC, Mandez-Prost CE, Whelan TF, Paterson FR, Razvi H, and the Canadian Prostate Health Council and the CUA Guidelines Committee. Can Urol Assoc J. 2010;4(5): Pearson R, Williams PM. Common questions about the diagnosis and management of benign prostatic hypertrophy. Am Fam Phys. 2014;90(11): Peer-reviewed references: 10
11 Azoulay L, Eberg M, Benayoun S, Pollak M. 5α-reductase inhibitors and the risk of cancer-related mortality in men with prostate cancer. JAMA Oncol. 2015;1(3): Barry, MJ, Fowler, FJ, Jr., O'Leary, MP, et al. The American Urological Association symptom index for benign prostatic hyperplasia. The Measurement Committee of the American Urological Association. J Urol. 2017;197(2S):S189 S197. Carballido J, Fourcade R, Pagliarulo A, et al. Can benign prostatic hyperplasia be identified in the primary care setting using only simple tests? Results of the Diagnosis Improvement in Primary Care Trial. Int J Clin Pract. 2011;65(9): Coyne KS, Sexton CC, Thompson CL, et al. The prevalence of lower urinary tract symptoms (LUTS) in the USA, the UK, and Sweden: results from the Epidemiology of LUTS (EpiLUTS) study. BJU Int. 2009;104(3): Ding H, Du W, Lu ZP, Zhai ZX, Wang HZ, Wang ZP. Photoselective green-light laser vaporization vs. TURP for BPH: meta-analysis. Asian J Androl. 2012;14(5): D'Silva KA, Dahm P, Wong CL. Does this man with lower urinary tract symptoms have bladder outlet obstruction? The Rational Clinical Examination: a systematic review. JAMA. 2014;312(5): Emberton M, Cornel EB, Bassi PF, Fourcade RO, Gómez JM, Castro R. Benign prostatic hyperplasia as a progressive disease: a guide to the risk factors and options for medical management. Int J Clin Pract. 2008;62(7): Frieben RW, Lin HC, Hinh PP, Berardinelli F, Canfield SE, Wang R. The impact of minimally invasive surgeries for the treatment of symptomatic benign prostatic hyperplasia on male sexual function: a systematic review. Asian J Androl. 2010;12(4): Hayes Inc., Hayes Medical Technology Report. UroLift System for treatment of benign prostatic hypertrophy/hyperplasia (BPH). Lansdale, PA: Hayes Inc., February Hayes Inc. Medical Technology Directory. Laser Therapy for Benign Prostate Hyperplasia. Lansdale PA: Hayes Inc., April Jiang H, Zhou Y. Safety and efficacy of thulium laser prostatectomy versus transurethral resection of prostate for treatment of benign prostate hyperplasia: a meta-analysis. Low Urin Tract Symptoms. 2016;8(3): Lepor H. Landmark studies impacting the medical management of benign prostatic hyperplasia. Rev Urol. 2003; 5(Suppl 5): S
12 Li Z, Chen P, Wang J, et al. The impact of surgical treatments for lower urinary tract symptoms/benign prostatic hyperplasia on male erectile function: a systematic review and network meta-analysis. Medicine (Baltimore). 2016;95(24):e3862. Lucca I, Shariat SF, Hofbauer SL, Klatte T. Outcomes of minimally invasive simple prostatectomy for benign prostatic hyperplasia: a systematic review and meta-analysis. World J Urol. 2015;33(4): Mayer EK, Rroeze SG, Chopra S, Bottle A, Patel A. Examining the gold standard : a comparative critical analysis of three consecutive decades of monopolar transurethral resection of the prostate (TURP) outcomes. BJU Int. 2012;110(11): Moul JW. High-risk prostate cancer and radical prostatectomy in the setting and context of multidisciplinary care. Urol Oncol. 2015;33(5): Nickel JC, Gilling P, Tammela TL, Morrill B, Wilson TH, Rittmaster RS. Comparison of dutasteride and finasteride for treating benign prostatic hyperplasia: the Enlarged Prostate International Comparator Study (EPICS). BJU Int. 2011;108(3): Perera M, Roberts MJ, Doi SA, Bolton D. Prostatic urethral lift improves urinary symptoms and flow while preserving sexual function for men with benign prostatic hyperplasia: a systematic review and meta-analysis. Eur Urol. 2015;67(4): Roehrborn CG. Male lower urinary tract symptoms (LUTS) and benign prostatic hyperplasia (BPH). Med Clin N Am. 2011;95; Seftel AD, Rosen RC, Rosenberg MT, Sadovsky R. Benign prostatic hyperplasia evaluation, treatment and association with sexual dysfunction: practice patterns according to physician specialty. Int J Clin Pract. 2008;62(4): Sonksen J, Barber NJ, Speakman MJ, et al. Prospective, randomized, multinational study of prostatic urethral lift versus transurethral resection of the prostate: 12-month results from the BPH6 study. Eur Urol. 2015;68(4): Thangasamy IA, Chalasani V, Bachmann A, Woo HH. Photoselective vaporization of the prostate using 80-W and 120-W laser versus transurethral resection of the prostate for benign prostatic hyperplasia: a systematic review with meta-analysis from 2001 to Eur Urol. 2012;62(2): Wei JT, Calhoun E, Jacosen SJ. Urologic diseases in America project: benign prostatic hyperplasia. J Urol. 2008;179(5 Suppl):S
13 Welliver C, Kottwitz M, Feustel P, McVary K. Clinically and statistically significant changes seen in sham surgery arms of randomized, controlled benign prostatic hyperplasia surgery trials. J Urol. 2015;194(6): Zhang X, Geng J, Zheng J, Peng B, Che J, Liang C. Photoselective vaporization versus transurethral resection of the prostate for benign prostatic hyperplasia: a meta-analysis. J Endourol. 2012;26(9): CMS National Coverage Determinations (NCDs): No NCDs identified as of the writing of this policy. Local Coverage Determinations (LCDs): L36109 Minimally Invasive Treatment for Benign Prostatic Hyperplasia Involving Prostatic Urethral Lift (Urolift ). Effective date October 1, KeyWord=benign+prostatic+hyperplasia&KeyWordLookUp=Title&KeyWordSearchType=And&bc=gAAAA CAAAAAAAA%3d%3d&. Accessed May 26, Commonly submitted codes Below are the most commonly submitted codes for the service(s)/item(s) subject to this policy. This is not an exhaustive list of codes. Providers are expected to consult the appropriate coding manuals and bill accordingly. CPT Code Description Comments Transurethral incision of prostate Transurethral electrosurgical resection of prostate, including control of postoperative bleeding; complete Transurethral resection; residual or regrowth of prostatic tissue including control of postoperative bleeding; complete Laser coagulation of prostate; including control of postoperative bleeding; complete Laser vaporization of prostate; including control of postoperative bleeding; complete Laser enucleation of prostate with morcellation including control of postoperative bleeding; complete ICD-10 Code Description Comments N40.1 Enlarged prostate with lower urinary tract symptoms N13.8 Urinary obstruction R33.8 Urinary retention R35.0 Urinary frequency Requires additional code for symptoms 13
14 ICD-10 Code Description Comments R35.1 Nocturia R39.11 Urinary hesitancy R39.12 Weak urinary stream R39.14 Incomplete bladder emptying R39.16 Straining on urination HCPCS Level II Code N/A Appendix Description Comments The American Urological Association (AUA) has issued a Guideline on the Management of Benign Prostatic Hyperplasia (BPH), which the AUA validated in The guideline includes an algorithm for the diagnosis and basic treatment of lower urinary tract symptoms (LUTS), which is presented below: 14
Clinical Policy Title: Management of benign prostatic hyperplasia
 Clinical Policy Title: Management of benign prostatic hyperplasia Clinical Policy Number: 13.02.03 Effective Date: October 1, 2016 Initial Review Date: July 20, 2016 Most Recent Review Date: June 5, 2018
Clinical Policy Title: Management of benign prostatic hyperplasia Clinical Policy Number: 13.02.03 Effective Date: October 1, 2016 Initial Review Date: July 20, 2016 Most Recent Review Date: June 5, 2018
NOTE: This policy is not effective until April 1, Transurethral Water Vapor Thermal Therapy of the Prostate
 NOTE: This policy is not effective until April 1, 2019. Medical Policy Manual Surgery, Policy No. 210 Transurethral Water Vapor Thermal Therapy of the Prostate Next Review: December 2019 Last Review: December
NOTE: This policy is not effective until April 1, 2019. Medical Policy Manual Surgery, Policy No. 210 Transurethral Water Vapor Thermal Therapy of the Prostate Next Review: December 2019 Last Review: December
Benign Prostatic Hyperplasia (BPH)
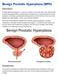 Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Benign Prostatic Hyperplasia (BPH):
 Benign Prostatic Hyperplasia (BPH): Evidence Based Guidelines for Primary Care Providers Jeanne Martin, DNP, ANP-BC Objectives 1. Understand the pathophysiology and prevalence of BPH 2. Select the appropriate
Benign Prostatic Hyperplasia (BPH): Evidence Based Guidelines for Primary Care Providers Jeanne Martin, DNP, ANP-BC Objectives 1. Understand the pathophysiology and prevalence of BPH 2. Select the appropriate
Treating BPH: Comparing Rezum UroLift and HoLEP
 Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
50% of men. 90% of men PATIENT FACTSHEET: BPH CONDITION AND TREATMENTS. Want more information? What are the symptoms?
 PATIENT FACTSHEET: BPH CONDITION AND TREATMENTS What is Benign Prostatic Hyperplasia (enlarged prostate)? Benign prostatic hyperplasia (BPH) is a noncancerous enlargement of the prostate, the gland that
PATIENT FACTSHEET: BPH CONDITION AND TREATMENTS What is Benign Prostatic Hyperplasia (enlarged prostate)? Benign prostatic hyperplasia (BPH) is a noncancerous enlargement of the prostate, the gland that
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
POLICIES AND PROCEDURE MANUAL
 POLICIES AND PROCEDURE MANUAL Policy: MP048 Section: Medical Benefit Policy Subject: Surgical and Minimally Invasive Therapies for the Treatment of Benign Prostatic Hypertrophy I. Policy: Surgical and
POLICIES AND PROCEDURE MANUAL Policy: MP048 Section: Medical Benefit Policy Subject: Surgical and Minimally Invasive Therapies for the Treatment of Benign Prostatic Hypertrophy I. Policy: Surgical and
MODULE 3: BENIGN PROSTATIC HYPERTROPHY
 MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
Last Review Status/Date: December Summary
 Section: Surgery Effective Date: January 15, 2016 Subject: Prostatic Urethral Lift Page: 1 of 9 Last Review Status/Date: December 2015 Summary Benign prostatic hyperplasia (BPH) is a common condition in
Section: Surgery Effective Date: January 15, 2016 Subject: Prostatic Urethral Lift Page: 1 of 9 Last Review Status/Date: December 2015 Summary Benign prostatic hyperplasia (BPH) is a common condition in
Overview. Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia. Iain McAuley September 15, 2014
 Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
What is Benign Prostatic Hyperplasia (BPH)?
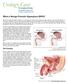 What is Benign Prostatic Hyperplasia (BPH)? Benign prostatic hyperplasia (BPH) is an enlarged prostate. The prostate goes through two main growth periods as a man ages. The first occurs early in puberty,
What is Benign Prostatic Hyperplasia (BPH)? Benign prostatic hyperplasia (BPH) is an enlarged prostate. The prostate goes through two main growth periods as a man ages. The first occurs early in puberty,
Management of LUTS. Simon Woodhams February 2012
 Management of LUTS Simon Woodhams February 2012 The management of lower urinary tract symptoms (LUTS) in men Implementing NICE guidance May 2010 NICE clinical guideline 97 Background Lower urinary tract
Management of LUTS Simon Woodhams February 2012 The management of lower urinary tract symptoms (LUTS) in men Implementing NICE guidance May 2010 NICE clinical guideline 97 Background Lower urinary tract
Benign Prostatic Hyperplasia: Update on Innovative Current Treatments
 Benign Prostatic Hyperplasia: Update on Innovative Current Treatments Michael Ferrandino, MD As.soc Professor Director of Minimally Invasive Urologic Surgery Division of Urologic Surgery Duke University
Benign Prostatic Hyperplasia: Update on Innovative Current Treatments Michael Ferrandino, MD As.soc Professor Director of Minimally Invasive Urologic Surgery Division of Urologic Surgery Duke University
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
Rezūm procedure for the Prostate
 Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Chapter 2: Methodology
 Chapter 2: Methodology TABLE OF CONTENTS Introduction... 2 Study Selection and Data Abstraction... 2 Data Synthesis... 8 Guideline Development and Approvals... 9 Conflict of Interest... 10 Copyright 2010
Chapter 2: Methodology TABLE OF CONTENTS Introduction... 2 Study Selection and Data Abstraction... 2 Data Synthesis... 8 Guideline Development and Approvals... 9 Conflict of Interest... 10 Copyright 2010
Subject: Temporary Prostatic Stent and Prostatic Urethral Lift
 02-54000-21 Original Effective Date: 03/15/05 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Temporary Prostatic Stent and Prostatic Urethral Lift THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
02-54000-21 Original Effective Date: 03/15/05 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Temporary Prostatic Stent and Prostatic Urethral Lift THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
Prostatic Urethral Lift
 Protocol Prostatic Urethral Lift (701151) Medical Benefit Effective Date: 04/01/18 Next Review Date: 01/19 Preauthorization No Review Dates: 05/17, 01/18 Preauthorization is not required. The following
Protocol Prostatic Urethral Lift (701151) Medical Benefit Effective Date: 04/01/18 Next Review Date: 01/19 Preauthorization No Review Dates: 05/17, 01/18 Preauthorization is not required. The following
Prostatic Urethral Lift. Summary
 Section: Surgery Effective Date: January 15, 2017 Subject: Prostatic Urethral Lift Page: 1 of 10 Last Review Status/Date: December 2016 Prostatic Urethral Lift Summary Benign prostatic hyperplasia (BPH)
Section: Surgery Effective Date: January 15, 2017 Subject: Prostatic Urethral Lift Page: 1 of 10 Last Review Status/Date: December 2016 Prostatic Urethral Lift Summary Benign prostatic hyperplasia (BPH)
Surgical procedures for benign prostatic hyperplasia: A nationwide survey in Japan
 International Journal of Urology (2011) 18, 166 170 doi: 10.1111/j.1442-2042.2010.02687.x Short Communicationiju_2687 166..170 Surgical procedures for benign prostatic hyperplasia: A nationwide survey
International Journal of Urology (2011) 18, 166 170 doi: 10.1111/j.1442-2042.2010.02687.x Short Communicationiju_2687 166..170 Surgical procedures for benign prostatic hyperplasia: A nationwide survey
Medical Coverage Policy Prostatic Urethral Lifts
 Medical Coverage Policy Prostatic Urethral Lifts EFFECTIVE DATE:12 01 2018 POLICY LAST UPDATED: 10 03 2017 OVERVIEW Benign prostatic hyperplasia is a common condition in older men that can lead to increased
Medical Coverage Policy Prostatic Urethral Lifts EFFECTIVE DATE:12 01 2018 POLICY LAST UPDATED: 10 03 2017 OVERVIEW Benign prostatic hyperplasia is a common condition in older men that can lead to increased
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
Executive Summary. Non-drug local procedures for treatment of benign prostatic hyperplasia 1. IQWiG Reports - Commission No.
 IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
Prostatic Urethral Lift
 Prostatic Urethral Lift Policy Number: 7.01.151 Last Review: 10/2018 Origination: 10/2015 Next Review: 10/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Prostatic
Prostatic Urethral Lift Policy Number: 7.01.151 Last Review: 10/2018 Origination: 10/2015 Next Review: 10/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Prostatic
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
Increasing Awareness, Diagnosis, and Treatment of BPH, LUTS, and EP
 Introduction to Enlarged Prostate E. David Crawford, MD Professor of Surgery (Urology) and Radiation Oncology Head, Urologic Oncology E. David Crawford Endowed Chair in Urologic Oncology University of
Introduction to Enlarged Prostate E. David Crawford, MD Professor of Surgery (Urology) and Radiation Oncology Head, Urologic Oncology E. David Crawford Endowed Chair in Urologic Oncology University of
EAU GUIDELINES POCKET EDITION 3
 EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
GUIDELINES ON NON-NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (Text update March 2015) S. Gravas (Chair), T. Bach,. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher, C. Mamoulakis,
GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (Text update March 2015) S. Gravas (Chair), T. Bach,. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher, C. Mamoulakis,
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Prostatic Urethral Lift Page 1 of 19 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Prostatic Urethral Lift Professional Institutional Original Effective Date:
Prostatic Urethral Lift Page 1 of 19 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Prostatic Urethral Lift Professional Institutional Original Effective Date:
GUIDELINES ON NON-NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (BPO)
 GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (BPO) (Text update pril 2014) S. Gravas (chair),. Bachmann,. Descazeaud, M. Drake, C. Gratzke, S. Madersbacher, C. Mamoulakis,
GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (BPO) (Text update pril 2014) S. Gravas (chair),. Bachmann,. Descazeaud, M. Drake, C. Gratzke, S. Madersbacher, C. Mamoulakis,
Victoria Sharp, MD, MBA, FAAFP. Clinical Professor of Urology and Family Medicine
 Victoria Sharp, MD, MBA, FAAFP Clinical Professor of Urology and Family Medicine Victoria Sharp, MD, MBA, FAAFP Market Chief Medial Officer AmeriHealth Caritas Family of Companies Office phone: (515) 330-3740
Victoria Sharp, MD, MBA, FAAFP Clinical Professor of Urology and Family Medicine Victoria Sharp, MD, MBA, FAAFP Market Chief Medial Officer AmeriHealth Caritas Family of Companies Office phone: (515) 330-3740
Consensus Meeting for Asian-Pacific BPH Guideline
 Consensus Meeting for Asian-Pacific BPH Guideline Byung Ha Chung Yonsei University Health System S a t e l l i t e S y m p o s i u m I Contents Diagnosis and Treatment Guidelines for BPH Prostate Volume
Consensus Meeting for Asian-Pacific BPH Guideline Byung Ha Chung Yonsei University Health System S a t e l l i t e S y m p o s i u m I Contents Diagnosis and Treatment Guidelines for BPH Prostate Volume
Related Policies None
 Medical Policy MP 7.01.151 Original Policy Date: August 2015 Last Review: 12/27/2017 Effective Date: 03/01/2018 Section: Surgery Related Policies None DISCLAIMER Our medical policies are designed for informational
Medical Policy MP 7.01.151 Original Policy Date: August 2015 Last Review: 12/27/2017 Effective Date: 03/01/2018 Section: Surgery Related Policies None DISCLAIMER Our medical policies are designed for informational
Transurethral Laser Technology: Treatments for BPH
 Transurethral Laser Technology: Treatments for BPH Richard Lee, MD Departments of Urology and Public Health The New York Presbyterian Hospital Weill Medical College of Cornell University Background Traditional
Transurethral Laser Technology: Treatments for BPH Richard Lee, MD Departments of Urology and Public Health The New York Presbyterian Hospital Weill Medical College of Cornell University Background Traditional
Related Policies None
 Medical Policy MP 7.01.151 BCBSA Ref. Policy: 7.01.151 Last Review: 12/27/2017 Effective Date: 03/01/2018 Section: Surgery End Date: 08/19/2018 Related Policies None DISCLAIMER Our medical policies are
Medical Policy MP 7.01.151 BCBSA Ref. Policy: 7.01.151 Last Review: 12/27/2017 Effective Date: 03/01/2018 Section: Surgery End Date: 08/19/2018 Related Policies None DISCLAIMER Our medical policies are
Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP)
 JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA
 St. Louis Hospital PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA INITIAL CLINICAL RESULTS Faculty of Medical Sciences New University of Lisbon JOÃO PISCO LUÍS CAMPOS PINHEIRO TIAGO BILHIM HUGO RIO TINTO
St. Louis Hospital PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA INITIAL CLINICAL RESULTS Faculty of Medical Sciences New University of Lisbon JOÃO PISCO LUÍS CAMPOS PINHEIRO TIAGO BILHIM HUGO RIO TINTO
Management of Voiding Problems in Older Men. Dr. John Fenn Consultant, QEH 10 th October, 2005
 Management of Voiding Problems in Older Men Dr. John Fenn Consultant, QEH 10 th October, 2005 Voiding Problems Poor stream Hesitancy Straining Incomplete emptying Intermittent micturition Terminal dribbling
Management of Voiding Problems in Older Men Dr. John Fenn Consultant, QEH 10 th October, 2005 Voiding Problems Poor stream Hesitancy Straining Incomplete emptying Intermittent micturition Terminal dribbling
All about the Prostate
 MEN S HEALTH Dr Nick Pendleton January 16 th 2018 All about the Prostate 1 What does it do? Functions of the Prostate 1. Secretes Prostatic Fluid slightly alkaline fluid, 30% of volume of seminal fluid,
MEN S HEALTH Dr Nick Pendleton January 16 th 2018 All about the Prostate 1 What does it do? Functions of the Prostate 1. Secretes Prostatic Fluid slightly alkaline fluid, 30% of volume of seminal fluid,
Can men with prostates sized 80 ml or larger be managed conservatively?
 Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Prostate Artery Embolization
 Prostate Artery Embolization in the office interventional suite Robert J. Kennedy, M.D. Interventional & Vascular Center Melbourne, Florida The speaker has no financial conflicts of interest to disclose.
Prostate Artery Embolization in the office interventional suite Robert J. Kennedy, M.D. Interventional & Vascular Center Melbourne, Florida The speaker has no financial conflicts of interest to disclose.
AMERIHEALTH / INDEPENDENCE BLUE CROSS
 AMERIHEALTH / INDEPENDENCE BLUE CROSS Urinary outlet obstruction is difficulty in the passage of urine from the bladder to the urethra caused by compression or resistance on the bladder outflow channel
AMERIHEALTH / INDEPENDENCE BLUE CROSS Urinary outlet obstruction is difficulty in the passage of urine from the bladder to the urethra caused by compression or resistance on the bladder outflow channel
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Prostatic Urethral Lift Page 1 of 17 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Prostatic Urethral Lift Professional Institutional Original Effective Date:
Prostatic Urethral Lift Page 1 of 17 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Prostatic Urethral Lift Professional Institutional Original Effective Date:
GENDER HEALTH. Benign Prostatic Hyperplasia. Medical and Surgical Treatment Options
 GENDER HEALTH Benign Prostatic Hyperplasia Medical and Surgical Treatment Options ABSTRACT Benign prostatic hyperplasia (BPH) affects the aging male. Treatment options vary widely. Some men will elect
GENDER HEALTH Benign Prostatic Hyperplasia Medical and Surgical Treatment Options ABSTRACT Benign prostatic hyperplasia (BPH) affects the aging male. Treatment options vary widely. Some men will elect
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: January 15, 2019 Related Policies: None Prostatic Urethral Lift Description Benign prostatic hyperplasia (BPH) is a common condition in older individuals that
FEP Medical Policy Manual Effective Date: January 15, 2019 Related Policies: None Prostatic Urethral Lift Description Benign prostatic hyperplasia (BPH) is a common condition in older individuals that
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: None Prostatic Urethral Lift Description Benign prostatic hyperplasia (BPH) is a common condition in older individuals that can
FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: None Prostatic Urethral Lift Description Benign prostatic hyperplasia (BPH) is a common condition in older individuals that can
Benign Prostatic Hyperplasia. Jay Lee, MD, FRCSC Clinical Associate Professor University of Calgary
 Benign Prostatic Hyperplasia Jay Lee, MD, FRCSC Clinical Associate Professor University of Calgary Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Benign Prostatic Hyperplasia Jay Lee, MD, FRCSC Clinical Associate Professor University of Calgary Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Name of Policy: Transurethral Microwave Thermotherapy
 Name of Policy: Transurethral Microwave Thermotherapy Policy #: 449 Latest Review Date: September 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable
Name of Policy: Transurethral Microwave Thermotherapy Policy #: 449 Latest Review Date: September 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable
PATIENT INFORMATION 2017 NeoTract, Inc. All rights reserved. Printed in the USA. MAC Rev A
 PATIENT INFORMATION OVER 70% OF MEN IN THEIR 60s HAVE SYMPTOMS OF BPH 1 BPH affects more than 500 million men worldwide, with many men suffering from symptoms of enlarged prostate. 1 You no longer have
PATIENT INFORMATION OVER 70% OF MEN IN THEIR 60s HAVE SYMPTOMS OF BPH 1 BPH affects more than 500 million men worldwide, with many men suffering from symptoms of enlarged prostate. 1 You no longer have
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Text update March 2017) S. Gravas (Chair), T. Bach, M. Drake, M. Gacci, C. Gratzke, T.R.W. Herrmann, S. Madersbacher,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Text update March 2017) S. Gravas (Chair), T. Bach, M. Drake, M. Gacci, C. Gratzke, T.R.W. Herrmann, S. Madersbacher,
Chapter 4: Research and Future Directions
 Chapter 4: Research and Future Directions Introduction Many of the future research needs listed in the 1994 Agency for Health Care Policy and Research (AHCPR) clinical practice guideline Benign Prostatic
Chapter 4: Research and Future Directions Introduction Many of the future research needs listed in the 1994 Agency for Health Care Policy and Research (AHCPR) clinical practice guideline Benign Prostatic
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Limited text update March 2016) S. Gravas (Chair), T. Bach, A. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Limited text update March 2016) S. Gravas (Chair), T. Bach, A. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher,
Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano
 Dipartimento di Urologia Direttore Prof. Giorgio Guazzoni Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano alberto.saita@humanitas.it
Dipartimento di Urologia Direttore Prof. Giorgio Guazzoni Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano alberto.saita@humanitas.it
Chapter 3: Results of the Treatment Outcomes Analyses
 Chapter 3: Results of the Treatment Outcomes Analyses Introduction To determine the appropriateness of individual therapies, as well as to develop practice recommendations, the American Urological Association
Chapter 3: Results of the Treatment Outcomes Analyses Introduction To determine the appropriateness of individual therapies, as well as to develop practice recommendations, the American Urological Association
Chapter 3: Results of the Treatment Outcomes Analyses
 Chapter 3: Results of the Treatment Outcomes Analyses TABLE OF CONTENTS INTRODUCTION... 3 WATCHFUL WAITING... 11 STUDY OUTCOMES... 11 MEDICAL THERAPIES... 13 ALPHA-ADRENERGIC ANTAGONISTS (ALPHA-BLOCKERS)...
Chapter 3: Results of the Treatment Outcomes Analyses TABLE OF CONTENTS INTRODUCTION... 3 WATCHFUL WAITING... 11 STUDY OUTCOMES... 11 MEDICAL THERAPIES... 13 ALPHA-ADRENERGIC ANTAGONISTS (ALPHA-BLOCKERS)...
Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj
 Original Article Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj Abstract Objectives: Prospective evaluation
Original Article Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj Abstract Objectives: Prospective evaluation
Benign prostatic hyperplasia (BPH)
 Diseases and Conditions Benign prostatic hyperplasia (BPH) By Mayo Clinic Staff Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate
Diseases and Conditions Benign prostatic hyperplasia (BPH) By Mayo Clinic Staff Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate
EVALUATION OF THE EFFICACY OF TADALAFIL IN IMPROVING LOWER URINARY TRACT SYMPTOMS IN PATIENTS WITH SYMPTOMATIC BENIGN PROSTATIC ENLARGEMENT
 Basrah Journal Of Surgery EVALUATION OF THE EFFICACY OF TADALAFIL IN IMPROVING LOWER URINARY TRACT SYMPTOMS IN PATIENTS WITH SYMPTOMATIC BENIGN PROSTATIC ENLARGEMENT MB, ChB, FIBMS, Assistant Professor
Basrah Journal Of Surgery EVALUATION OF THE EFFICACY OF TADALAFIL IN IMPROVING LOWER URINARY TRACT SYMPTOMS IN PATIENTS WITH SYMPTOMATIC BENIGN PROSTATIC ENLARGEMENT MB, ChB, FIBMS, Assistant Professor
Male Lower Urinary Tract Symptoms: Management in primary care and beyond. Daniel Cohen PhD FRCS(Urol) Consultant Urological Surgeon
 Male Lower Urinary Tract Symptoms: Management in primary care and beyond Daniel Cohen PhD FRCS(Urol) Consultant Urological Surgeon 1 LUTS Very common: 1/3 men over age of 50 have moderate to severe LUTS
Male Lower Urinary Tract Symptoms: Management in primary care and beyond Daniel Cohen PhD FRCS(Urol) Consultant Urological Surgeon 1 LUTS Very common: 1/3 men over age of 50 have moderate to severe LUTS
Submitted: August 15, Accepted: September 10, Published: October 15, 2018.
 Original Article doi: 10.22374/jeleu.v1i2.21 THULIUM LASER ENUCLEATION OF THE PROSTATE (THULEP) AS A TECHNIQUE FOR TREATMENT OF BPH: EVALUATION OF A SIX-YEAR EXPERIENCE AT A SINGLE INSTITUTION Mahmood
Original Article doi: 10.22374/jeleu.v1i2.21 THULIUM LASER ENUCLEATION OF THE PROSTATE (THULEP) AS A TECHNIQUE FOR TREATMENT OF BPH: EVALUATION OF A SIX-YEAR EXPERIENCE AT A SINGLE INSTITUTION Mahmood
Medical Coverage Policy Prostatic Urethral Lifts
 Medical Coverage Policy Prostatic Urethral Lifts EFFECTIVE DATE:01 01 2017 POLICY LAST UPDATED: 10 03 2017 OVERVIEW Benign prostatic hyperplasia is a common condition in older men that can lead to increased
Medical Coverage Policy Prostatic Urethral Lifts EFFECTIVE DATE:01 01 2017 POLICY LAST UPDATED: 10 03 2017 OVERVIEW Benign prostatic hyperplasia is a common condition in older men that can lead to increased
Benign Prostatic Hyperplasia (BPH) Treatments
 Medical Coverage Policy Effective Date...10/15/2017 Next Review Date...10/15/2018 Coverage Policy Number... 0159 Benign Prostatic Hyperplasia (BPH) Treatments Table of Contents Related Coverage Resources
Medical Coverage Policy Effective Date...10/15/2017 Next Review Date...10/15/2018 Coverage Policy Number... 0159 Benign Prostatic Hyperplasia (BPH) Treatments Table of Contents Related Coverage Resources
Key words: Lower Urinary Tract Symptoms (LUTS), Prostatic Hyperplasia, Alpha-1 Adrenoceptor Antagonists, Tamsulosin, Terazosin.
 The Professional Medical Journal DOI: 10.17957/TPMJ/17.4102 ORIGINAL PROF-4102 PROSTATIC HYPERPLASIA; COMPARISON BETWEEN TAMSULOSIN AND TERAZOSIN FOR EFFICACY IN MEDICAL MANAGEMENT OF LOWER URINARY TRACT
The Professional Medical Journal DOI: 10.17957/TPMJ/17.4102 ORIGINAL PROF-4102 PROSTATIC HYPERPLASIA; COMPARISON BETWEEN TAMSULOSIN AND TERAZOSIN FOR EFFICACY IN MEDICAL MANAGEMENT OF LOWER URINARY TRACT
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of prostatic urethral lift implants to treat lower urinary tract symptoms
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of prostatic urethral lift implants to treat lower urinary tract symptoms
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
EFFICACY OF LASER SURGERY FOR BENIGN PROSTATIC HYPERPLASIA TREATMENT
 EFFICACY OF LASER SURGERY FOR BENIGN PROSTATIC HYPERPLASIA TREATMENT Hasmeinda Medical faculty of Universitas Muhammadiyah Surakarta ABSTRACT Benign prostatic hyperplasia (BPH) is the most important cases
EFFICACY OF LASER SURGERY FOR BENIGN PROSTATIC HYPERPLASIA TREATMENT Hasmeinda Medical faculty of Universitas Muhammadiyah Surakarta ABSTRACT Benign prostatic hyperplasia (BPH) is the most important cases
OVER 70% OF MEN IN THEIR 60s HAVE SYMPTOMS OF BPH 1
 PATIENT INFORMATION BPH affects more than 500 million men worldwide, with many men suffering from symptoms of enlarged prostate. 1 You no longer have to be one of them! OVER 70% OF MEN IN THEIR 60s HAVE
PATIENT INFORMATION BPH affects more than 500 million men worldwide, with many men suffering from symptoms of enlarged prostate. 1 You no longer have to be one of them! OVER 70% OF MEN IN THEIR 60s HAVE
Energy Delivery Systems for Treatment of Benign Prostatic Hyperplasia
 Ontario Health Technology Assessment Series 2006; Vol. 6, No. 17 Energy Delivery Systems for Treatment of Benign Prostatic Hyperplasia An Evidence-Based Analysis August 2006 Medical Advisory Secretariat
Ontario Health Technology Assessment Series 2006; Vol. 6, No. 17 Energy Delivery Systems for Treatment of Benign Prostatic Hyperplasia An Evidence-Based Analysis August 2006 Medical Advisory Secretariat
Prostate Disease. Chad Baxter, MD
 Prostate Disease Chad Baxter, MD Managing BPH and LUTS Chad Baxter, MD Department of Urology cbaxter@mednet.ucla.edu 33 nd Annual UCLA Intensive Course in Geriatric Medicine & Board Review Prevalence of
Prostate Disease Chad Baxter, MD Managing BPH and LUTS Chad Baxter, MD Department of Urology cbaxter@mednet.ucla.edu 33 nd Annual UCLA Intensive Course in Geriatric Medicine & Board Review Prevalence of
Service Line: Rapid Response Service Version: 1.0 Publication Date: March 01, 2017 Report Length: 16 Pages
 CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Bipolar versus Monopolar Transurethral Resection of the Prostate or GreenLight Laser Treatment: A Review of Clinical and Cost-Effectiveness
CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Bipolar versus Monopolar Transurethral Resection of the Prostate or GreenLight Laser Treatment: A Review of Clinical and Cost-Effectiveness
Clinical guideline Published: 23 May 2010 nice.org.uk/guidance/cg97
 Lower urinary tract symptoms in men: management Clinical guideline Published: 23 May 2010 nice.org.uk/guidance/cg97 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Lower urinary tract symptoms in men: management Clinical guideline Published: 23 May 2010 nice.org.uk/guidance/cg97 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
REPORTS. Clinical and Economic Outcomes in Patients Treated for Enlarged Prostate
 Clinical and Economic Outcomes in Patients Treated for Enlarged Prostate Michael James Naslund, MD, MBA; Muta M. Issa, MD, MBA; Amy L. Grogg, PharmD; Michael T. Eaddy, PharmD, PhD; and Libby Black, PharmD
Clinical and Economic Outcomes in Patients Treated for Enlarged Prostate Michael James Naslund, MD, MBA; Muta M. Issa, MD, MBA; Amy L. Grogg, PharmD; Michael T. Eaddy, PharmD, PhD; and Libby Black, PharmD
Surgical Treatment of LUTS in Men with BPE
 Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor
Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor
Korean Urologist s View of Practice Patterns in Diagnosis and Management of Benign Prostatic Hyperplasia: A Nationwide Survey
 Original Article DOI 10.3349/ymj.2010.51.2.248 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(2):248-252, 2010 Korean Urologist s View of Practice Patterns in Diagnosis and Management of Benign Prostatic
Original Article DOI 10.3349/ymj.2010.51.2.248 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(2):248-252, 2010 Korean Urologist s View of Practice Patterns in Diagnosis and Management of Benign Prostatic
The Evolution of Combination Therapy. US men eligible for BPH treatment * with projected population changes
 The Management of BPH & The Impact of Combination Therapy Results Combination of Avodart and Tamsulosin (CombAT) Medical Therapy of Prostate Symptoms (MTOPS) Dr. Jack Barkin, md, fics, facs, dabu, Mcert
The Management of BPH & The Impact of Combination Therapy Results Combination of Avodart and Tamsulosin (CombAT) Medical Therapy of Prostate Symptoms (MTOPS) Dr. Jack Barkin, md, fics, facs, dabu, Mcert
Safety and efficacy of photoselective vaporization of the prostate using the 180-W GreenLight XPS laser system in patients taking oral anticoagulants
 Clinical Report Safety and efficacy of photoselective vaporization of the prostate using the 180-W GreenLight XPS laser system in patients taking oral anticoagulants Journal of International Medical Research
Clinical Report Safety and efficacy of photoselective vaporization of the prostate using the 180-W GreenLight XPS laser system in patients taking oral anticoagulants Journal of International Medical Research
TITLE: Plasma Vaporization of the Prostate for Treatment of Benign Prostatic Hypertrophy: A Review of Clinical and Cost-Effectiveness, and Safety
 TITLE: Plasma Vaporization of the Prostate for Treatment of Benign Prostatic Hypertrophy: A Review of Clinical and Cost-Effectiveness, and Safety DATE: 05 March 2014 CONTEXT AND POLICY ISSUES Benign prostatic
TITLE: Plasma Vaporization of the Prostate for Treatment of Benign Prostatic Hypertrophy: A Review of Clinical and Cost-Effectiveness, and Safety DATE: 05 March 2014 CONTEXT AND POLICY ISSUES Benign prostatic
Surgical Management of Lower Urinary Tract Symptoms Attributed to Benign Prostatic Hyperplasia: AUA GUIDELINE
 1 Approved by the AUA Board of Directors May 2018 Authors disclosure of potential conflicts of interest and author/staff contributions appear at the end of the article. 2018 by the American Urological
1 Approved by the AUA Board of Directors May 2018 Authors disclosure of potential conflicts of interest and author/staff contributions appear at the end of the article. 2018 by the American Urological
APPENDIX CLINICAL INPUT RESPONSES
 CLINICAL INPUT RESPONSES AUA: American Urological Association; UCSF Med Ctr: University of California San Francisco Medical Center; PUL: prostatic urethral lift. * Indicates that information on conflicts
CLINICAL INPUT RESPONSES AUA: American Urological Association; UCSF Med Ctr: University of California San Francisco Medical Center; PUL: prostatic urethral lift. * Indicates that information on conflicts
Clinical Policy Title: Abdominal aortic aneurysm screening
 Clinical Policy Title: Abdominal aortic aneurysm screening Clinical Policy Number: 08.01.10 Effective Date: August 1, 2017 Initial Review Date: June 22, 2017 Most Recent Review Date: July 20, 2017 Next
Clinical Policy Title: Abdominal aortic aneurysm screening Clinical Policy Number: 08.01.10 Effective Date: August 1, 2017 Initial Review Date: June 22, 2017 Most Recent Review Date: July 20, 2017 Next
BENIGN PROSTATIC HYPERPLASIA (BPH) affects 70%
 JOURNAL OF ENDOUROLOGY Volume 14, Number 2, March 2000 Mary Ann Liebert, Inc. Holmium Laser Enucleation of the Prostate With Tissue Morcellation: Initial United States Experience JEFFREY A. MOODY, M.D.,
JOURNAL OF ENDOUROLOGY Volume 14, Number 2, March 2000 Mary Ann Liebert, Inc. Holmium Laser Enucleation of the Prostate With Tissue Morcellation: Initial United States Experience JEFFREY A. MOODY, M.D.,
Number: Policy *Please see amendment for Pennsylvania Medicaid at the end of
 1 of 54 Number: 0079 Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB. I. Aetna considers the following approaches to the treatment of benign prostatic hypertrophy (BPH) medically
1 of 54 Number: 0079 Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB. I. Aetna considers the following approaches to the treatment of benign prostatic hypertrophy (BPH) medically
Prostatic Urethral Lift Corporate Medical Policy
 Prostatic Urethral Lift Corporate Medical Policy File Name: Prostatic Urethral Lift File Code: UM.SURG.19 Origination: 05/2018 Last Review: 01/2019 Next Review: 01/2020 Effective Date: 04/01/2019 Description/Summary
Prostatic Urethral Lift Corporate Medical Policy File Name: Prostatic Urethral Lift File Code: UM.SURG.19 Origination: 05/2018 Last Review: 01/2019 Next Review: 01/2020 Effective Date: 04/01/2019 Description/Summary
Cooled ThermoTherapy TM
 Are BPH Medications Weighing You Down? Think Outside the Pillbox Cooled ThermoTherapy TM A non-surgical, 30 minute in-office treatment that provides long-term relief from BPH symptoms and urinary obstruction
Are BPH Medications Weighing You Down? Think Outside the Pillbox Cooled ThermoTherapy TM A non-surgical, 30 minute in-office treatment that provides long-term relief from BPH symptoms and urinary obstruction
Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate
 Singapore Med J 2016; 57(12): 676-680 doi: 10.11622/smedj.2016026 Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate Sundaram Palaniappan
Singapore Med J 2016; 57(12): 676-680 doi: 10.11622/smedj.2016026 Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate Sundaram Palaniappan
Long-term Follow-up of Transurethral Enucleation Resection of the Prostate for Symptomatic Benign Prostatic Hyperplasia
 Journal of Surgery 2016; 4(2): 40-44 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160402.18 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Long-term Follow-up of Transurethral Enucleation
Journal of Surgery 2016; 4(2): 40-44 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160402.18 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Long-term Follow-up of Transurethral Enucleation
Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH
 Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH The more you know, the better you ll feel. You ve likely had a discussion with your doctor about BPH 1. What follows are some
Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH The more you know, the better you ll feel. You ve likely had a discussion with your doctor about BPH 1. What follows are some
Control & confidence. You deserve both.
 Learn more about BPH and Plasma therapy Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH Your doctor is always happy to offer all the guidance you need so that you feel completely
Learn more about BPH and Plasma therapy Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH Your doctor is always happy to offer all the guidance you need so that you feel completely
Comparison of outpatient versus inpatient transurethral prostate resection for benign prostatic hyperplasia: Comparative, prospective bi-centre study
 original research Comparison of outpatient versus inpatient transurethral prostate resection for benign prostatic hyperplasia: Comparative, prospective bi-centre study Jae Heon Kim, MD; * Jae Young Park,
original research Comparison of outpatient versus inpatient transurethral prostate resection for benign prostatic hyperplasia: Comparative, prospective bi-centre study Jae Heon Kim, MD; * Jae Young Park,
Policy for Prostatism/Lower Urinary Tract Symptoms in men
 NHS Halton Clinical Commissioning Group NHS Liverpool Clinical Commissioning Group NHS St Helens Clinical Commissioning Group NHS South Sefton Clinical Commissioning Group NHS Southport and Formby Clinical
NHS Halton Clinical Commissioning Group NHS Liverpool Clinical Commissioning Group NHS St Helens Clinical Commissioning Group NHS South Sefton Clinical Commissioning Group NHS Southport and Formby Clinical
Combination of Thulium Laser Incision and Bipolar Resection Offers Higher Resection. Velocity than Bipolar Resection Alone in Large Prostates
 Running Head: combination of thulium laser and bipolar in endoscopic prostatectomy-huang et al. Combination of Thulium Laser Incision and Bipolar Resection Offers Higher Resection Velocity than Bipolar
Running Head: combination of thulium laser and bipolar in endoscopic prostatectomy-huang et al. Combination of Thulium Laser Incision and Bipolar Resection Offers Higher Resection Velocity than Bipolar
