Penile Tumors: Their Management by Mohs Micrographic Surgery
|
|
|
- Jacob Crawford
- 5 years ago
- Views:
Transcription
1 ' Penile Tumors: Their Management by Mohs Micrographic Surgery MARC D. BROWN, M.D. CHRISTOPHER B. ZACHARY, M.D. ROY C. GREKIN, M.D. NEIL A. SWANSON, M.D. FIRST PRIZE Abstract. Penile tumors represent a difficult group of neoplasms requiring effective and curative treatment while minimizing tissue loss to prevent cosmetic and functional deformity. Over the past 6 years, we have treated 20 patients with penile cancer utilizing the fresh tissue technique of Mohs micrographic surgery. Tumors were excised with an average of 2.25 stages. Most defects (80%) were allowed to heal by second intention. Since surgery, four patients have developed metastatic disease in their regional lymphatic system, and one patient has died from metastatic spread. One patient has developed local recurrence. Micrographic surgery is a very useful treatment modality for patients with penile tumors. Patients with SCC of the penis should be considered for. elective regional lymph node biopsy and/or dissection in conjunction with micrographically controlled excision of the primary tumor. Marc D. Brown, M.D., Surgical Fellow, Department of Dermatology, and Neil A. Swanson, M.D., Associate Professor of Dermatology and Otolaryngology, are from the University of Michigan Medical School, Ann Arbor, Michigan. Christopher B. Zachary, M.D., is Assistant Professor, Department of Dermatology, University of Minnesota Medical School, Minneapolis, Minnesota. Roy C. Grekin, M.D., is Assistant Clinical Professor, Department of Dermatology, University of California, San Francisco. Address reprint requests to Marc D. Brown, M.D., Taubman Center 1910/0314, 1500 East Medical Center Drive, Ann Arbor, MI 48109/ Dermatol. Surg. Oncol. 13:11 November 1987 INTRODUCTION Surgical treatment of penile carcinoma has primarily been the domain of the urologist. The traditional surgical approach for penile malignancies (most commonly squamous in origin) has been partial or total penectomy, either with or without ilioinguinal lymphoadenectomy. ' r2 This surgical approach often results in marked cosmetic deformity of the penis, with impaired sexual function and body image. As the benefits of Mohs micrographic surgery become established, there is an increasing tendency for patients with penile tumors to be referred for treatment by this technique. Mohs surgery offers the unique advantages of effective surgical treatment with microscopically controlled tumor-free borders while maintaining cosmetic and functional demands by maximal preservation of normal tissue. The purpose of this paper is to present our experience over the past 6 years in treating penile neoplasms with the Mohs technique. In doing so, we hope to emphasize the advantages of this surgical approach as the preferred treatment modality for localized penile carcinomas. MATERIALS AND METHODS Twenty patients with penile cancers were treated by the fresh-tissue technique of Mohs micrographic surgery at the University of Michigan's Department of Cutaneous Surgery and Oncology between 1981 and Preoperative evaluation included the size and location of the penile tumor, bilateral palpation of femoral and inguinal lymph nodes, and careful inspection of the scrotum and base of the penis to 1163
2 PENILE TUMORS FIGURE 1. SCC on the glans penis, preoperatively. FIGURE 2. Healing by second intention 2 weeks post- operatively. rule out local extension. All patients were evaluated concurrently by a urologist. The patients were clinically examined during the early postoperative period, and subsequently followed by us or their referring physician. Their progress and clinical outcome was reviewed by examination of inpatient and outpatient hospital records, as well as by telephone survey. Mean follow-up was approximately 3 years for 17 patients; three patients were lost to follow-up. Mohs surgery was performed in an outpatient setting in the standard fashion. Local anesthesia was achieved with a Carbocaine block. A tourniquet was placed at the base of the penis to minimize bleeding. A foley catheter was inserted for patient comfort and to serve as an anatomic landmark for the urethra and meatus (Fig. 1). Due to the contractile nature of the penile tissue, marking sutures were used to identify the margins of the sections instead of the conventional method of scoring the tissue with a scalpel blade. Hemostasis was obtained with several modalities, including use of a Bovie, spot electrocautery, pressure, and gelfoam. The average age of our patient population was 55 years, with a range of 35 to 80 years. Histologically, eleven patients had squamous cell carcinoma (SCC), seven patients had Bowen s squamous intraepidermal neoplasia, one patient had a verrucous carcinoma, and one patient had a leiomyosarcoma. Sixteen tumors were confined to the glans penis, and four were located on the distal shaft. There were no palpable nodes at the time of surgery, and there was no clinical extention to the 1164 scrotum or base of the penis. Four of these referral cases were recurrent tumors, having been treated elsewhere by non-mohs therapy. Preexisting conditions were seen in four patients; three patients with SCC had a previous diagnosis of balanitis xerotica obliterans (BXO), and the one patient with a leiomyosarcoma had sustained a previous traumatic event to the penis. Tumor size ranged from 0.5 x 0.5 to 6.0 x 5.0 cm with an average size of 2.3 x 1.8 cm. RESULTS All patients tolerated the surgery well in an outpatient setting with no significant perioperative or postoperative complications. Tumor excision was complete in nineteen patients with an average of 2.25 stages. The average postoperative defect size was 3.6 x 3.0 cm, with the largest defect being 6.0 x 7.0 cm. Most defects (16 patients) were allowed to heal by second intention (Fig. 2), three were closed primarily, and one was referred to the urology service for closure and repair. Of the seventeen patients reviewed, only one has possibly developed local recurrence. Four patients with SCC were subsequently found to have positive regional nodes, despite being clinically negative at the time of surgery. One patient has died of metastatic disease, and one patient has died from unrelated medical causes. Two of the four patients with metastatic disease and the one patient with local recurrence had a preexisting diagnosis of J. Dermatol. Surg. Oncol. 13:11 November 1987
3 BROWN ET AL BXO. Although the number of patients is small, BXO appeared to be a poor prognostic indicator. DISCUSSION Penile malignancies account for less than 1% of male cancers in the U.S.3*4 There is an estimated 1 to 2 new cases per 10,000 population per year.4 Early circumcision and proper hygiene probably account for this low U.S. incidence, especially when compared to underdeveloped countries. In certain African and Asian populations, where circumcision is uncommon, penile carcinoma accounts for 10 to 20% of all malignancies in males.4 The development of penile cancer among uncircumcised males has been associated with the chronic, irritative effects of smegma, the by-product of bacterial action on desquamated cells that is retained within the preputial sac. Although smegma has been identified as a carcinogen in animal models, the specific component responsible for malignant degeneration in human males has not been identified.3 Adult cirumcision appears to offer little or no protection against the future appearance of penile tumors. Penile cancers rarely develop in males circumcised in the neonatal period, but becomes more frequent when circumcision is delayed until puberty. No consistent etiologic relationship has been established for antecedent trauma and/or venereal disease. Precancerous lesions include leukoplakia, BXO, and the Buschke-Lowenstein tumor. Erythoplasia of Querat and Bowen's disease are considered to be carcinomas in situ, and are histologically identical. Penile carcinoma is usually seen in the 6th to 7th decade, but is not uncommon in the 4th to 5th. In our population, the mean age was 55 years. The tumor is most common on the glans, prepuce, or coronal sulcus, and much less common on the shaft or meatus. Common presenting symptoms include the presence of a tumor mass or phimosis of recent onset. The cancer may appear indurated and erythematous, warty and exophytic, or flat and ulcerated. All these tumors appear to have a similar rate of growth, but the ulcerative lesion has a tendency towards earlier nodal metastases. Initially, the phimosis may obscure the tumor mass and result in a delayed diagnosis. Eventually, a foul odor, discharge, and bleeding may occur. At times, inguinal adenopathy may be the presenting symptom. Pain is not a common symptom, even with extensive local destruction. Likewise, urinary symptoms are uncommon unless the tumor is far advanced with resultant autoamputation. 1. Dermatol. Surg. Oncol. 13:11 November 1987 Unfortunately, many lesions are quite advanced at the time of diagnosis. Possibly due to fear of penile surgery, as high as 50% of patients delay medical care for greater than 1 year.3 Penile cancer has a relentless progressive course with death in approximately 2 years if untreated. Death usually results from uncontrolled regional lymphatic spread leading to skin necrosis, chronic infection, debilitation, and sepsis. Because carcinoma of the penis is uncommon in the U.S., there has been a relative scarcity of wellcontrolled, prospective studies concerning the proper treatment of this cancer. Controversy in disease management includes the appropriate surgical treatment of the primary lesion and the subsequent evaluation and treatment of nodal disease. Selected small tumors that are limited to the prepuce have been treated by circumcision alone. However, tumor recurrence can be unacceptably high, with reports of a 40 to 50% recurrence rate.3,4 For tumors on the glans and distal shaft, partial amputation with a 2-cm proximal margin is recommended. For more extensive lesions or those located on the proximal shaft, total penectomy is performed. The desired goal in the treatment of the primary tumor is complete excision with adequate tumorfree margins. Mohs micrographic surgery allows the precise identification of these tumor-free margins, while minimizing tissue loss. It is an excellent alternative to the traditional surgical approach of partial or total penectomy. Microscopically controlled chemosurgery was introduced in 1941 by Frederic M~hs.~ A fixation process with zinc chloride paste was utilized to remove thin layers of tissue which were sequentially examined microscopically for evidence of tumor. This procedure was continued, sometimes over a period of days, until tumor-free margins were defined. In 1985, Mohs summarized his results with the fixed tissue technique in the treatment of SCC of the penise6 He treated 29 patients with a followup of at least 5 years in 25 cases. The primary carcinoma was eradicated in 23 patients (92%) with a 5-year cure rate of 68%. The cure rate was highest for the more distally located carcinomas. There was an 81% cure rate when the tumor was localized to the glans and/or prepuce, but only a 57% cure rate when the penile shaft was involved. The size of the penile lesion also affected prognosis, with a 100% cure rate if less than 1.0 cm, but only a 50% cure if greater than 3.0 cm. Other poor prognostic indicators included nodal metastases at the time of surgery and previous treatment of the primary tumor by conventional 1165
4 PENILE TUMORS surgery or radiation therapy. None of the patients treated by Mohs reported a functional deficit, either sexual or urinary. Mohs concluded that except for large and highly anaplastic tumors, which would preclude preservation of a functional penis, and those on the foreskin, which could be excised completely by circumcision, microscopically controlled surgery was the preferred surgical technique for treatment of localized penile carcinomas. The fresh tissue technique of micrographic surgery was popularized in the 1970s by Stegman and Trom~vich.~ This approach required the surgical excision of fresh, unfixed tissue with subsequent analysis of cryostat sections. The fresh tissue technique is far more rapid and precise and has largely replaced the fixed tissue technique. All of our patients were treated with the fresh tissue technique. Although we cannot yet quote a 5-year survival rate, our results to date have been very satisfactory and encouraging. Only one patient has developed a local recurrence, and it is possible that this represents a second primary lesion. Five to fifteen percent of patients with penile cancer develop a second primary tumor.4 Our patient had a long standing history of extensive BXO, with a second tumor developing 4 years after the primary surgery. With the preexisting condition of BXO and the relatively long period of time elapsed between tumors, it is likely that this tumor may be a second primary SCC of the penis. Four of our patients have developed metastatic spread to the inguinal nodes, and one of these patients has died from his metastatic disease. This was 20% of our total population and 35% of the patients with SCC (including the three patients lost to follow-up). Metastatic spread was not suspected clinically at the time of surgery, which was a surprising finding in that an estimated 50% of patients present with inguinal adenopathy at the time of diagnosis. In all cases, metastatic involvement was diagnosed within 1 year postsurgery. The earliest route of spread of penile cancer is metastases to the regional femoral and iliac lymph nodes. There are multiple cross communications throughout all levels of penile lymphatic drainage such that drainage is bilateral to both inguinal areas. In spite of the rich blood supply of the penis and possible spread through the pelvic vasculature, visceral metastases are rare. Clinically detectable distant metastases to lung, liver, bone, and brain occur in less than 10% of patients, usually late in the course of the disease. Our 20% incidence of metastatic disease raises the controversy of proper management of regional lymph nodes with penile cancer. Approximately 1/3 of patients presenting with penile carcinoma have 1166 metastatic spread to the regional inguinal lymph nodes.' Because 40 to 50% of patients with positive nodes can be cured by node dissection, it is important to diagnose and treat this metastatic spread in a timely fashion. Unfortunately, clinical evaluation is imprecise and inaccurate with unacceptable false positive and false negative rates. It has been estimated that as high as 50% of patients with clinically positive nodes have no metastatic disease on histologic examination while 20% of patients with clinically negative nodes have occult To further complicate the issue, approximately 10% of patients with clinically positive nodes that are negative on node biopsy subsequently will demonstrate regional disea~e.~ Although bilateral prophylactic inguinal lymphadenectomy is potentially curative and is the most accurate diagnostic staging procedure, it carries a significant incidence of morbidity, including wound infection, skin flap necrosis, pulmonary emboli, and chronic lymphedema.3,'3 Johnson and Lol4 compared patients who had late versus early node dissection and found a significant difference in mortality (57 vs. 13% 5-year survival). Therefore, the diagnostic challenge is to identify which patients have metastatic spread and to therapeutically dissect the involved nodes as early as possible. Some authors recommend "watchful waiting" if the regional nodes are clinically negative, especially if the primary tumor is small and located distally on the glans or prep~ce.~,'~ Others have strongly recommended bilateral sentinel node biopsies, regardless of whether the nodes are clinically in~olved.'~'~~'~ This recommendation is based on lymphangiographic evidence that a sentinel node located near the junction of the saphenous and femoral veins is the first site of metastatic spread from a penile cancer.15 The sensitivity of this diagnostic procedure has been estimated to be 88%.' If the sentinel node is positive, then a bilateral deep and superficial ilioinguinal node dissection is warranted. If the sentinel node is negative, no further surgery is recommended. However, close clinical follow-up and observation (preferably by the same physician) for the appearance of unrecognized inguinal metastases in biopsy negative patients is mandatory. There have been several reports of patients with false negative sentinel node biopsies who subsequently developed metastatic spread.',12 Nonetheless, the sentinel node biopsy, because of its simplicity and low morbidity, is an attractive method for staging apparently localized penile cancer. The role of the sentinel node biopsy requires continued assessment, as well as establishment of its true sensitivity and specificity. I. Dermatol. Surg. Oncol. 13:ll November 1987
5 BROWN ET AL An alternate proposal is that of a bilateral superficial node dissection. This involves removal of those nodes superficial to the fascia lata with progression to total lymphadenectomy (including nodes deep to the fascia lata contained within the femoral triangle) if the superficial nodes are positi~e.~ This approach is based on the fact that iliac lymph nodes rarely become involved unless metastases have first reached the superficial inguinal nodes. Finally, some urologists recommend bilateral prophylactic and therapeutic ilioinguinal node dissections for penile cancers.',i6 This approach offers the best chance of cure, but its usefulness is limited by the morbidity of the procedure and the lack of controlled prospective studies to substantiate its benefit.i4 Its best indication may be for large tumors located more proximally on the penile shaft in association with convincing clinical evidence of lymphatic involvement.' Our experience of nodal metastases with clinically negative nodes at the time of primary surgery in 36% patients with SCC of the penis would suggest a more aggressive diagnostic approach than a "watch and wait" policy. In view of the high incidence of lymph node metastases and the probable need for sentinel node biopsy, superficial node dissection or complete ilioinguinal node dissection, it is imperative that a urologist be a member of the treatment team. SUMMARY Our experience with 20 patients with penile cancer treated by micrographic surgery has been encouraging. Mohs surgery has several distinct advantages. First and foremost, it is a pricise surgical approach for the removal of the primary penile tumor, with a surgical field microscopically free of invasive tumor or marked dysplastic changes. It offers comparable survival rates with a less radical procedure and may often be curative. Through preservation of penile tissue, there is considerable cosmetic benefit and maintenance of normal sexual function. Surgery is well tolerated with the use of local anesthesia in an outpatient setting with negligible mor- bidity and high patient acceptance. Follow-up over ensuing years is necessary to define the 5-year survival rate. In the future, closer attention to the depth of invasion, histologic differentiation and intravascular involvement may help to better define prognosis. Our experience and that of others indicates the potential need for sentinel node biopsy and/or lymphadenectomy at the time of primary surgery for prognostic and therapeutic reasons. REFERENCES 1. Fraley E, Zharg G, Sazoma R, Lange PH. Cancer of the penis: Prognosis and treatment plans. Cancer 55: , Kossow JH, Hotchkiss RS, Morales PA. Carcinoma of the penis treated surgically: Analysis of 100 cases. Urology 2~ , Paulson DF, Perez CA, Anderson T. Cancer of the urethra and penis. In: Cancer: Principles and practice of oncology, 2nd ed. Philadelphia, JB Lippincott, Co, 1985, pp Schellhammer PF, Grabstald H. Tumors of the penis. In: Campbell's Urology, 5th ed. Philadelphia, WB Saunders, 1986, pp Mohs FE. Chemosurgery: Microscopically controlled surgery for skin cancer. Springfield, Illinois, Charles C Thomas, Publisher, Mohs FE, Snow SN, Messing E, Kuglitsch ME. Microscopically controlled surgery in the treatment of carcinoma of the penis. J Urol 133: , Tromovitch TA, Stegman SJ. Microscopically controlled excision of skin tumors. Arch Dermatol 110:231, Fowler JE. Sentinel lymph node biopsy for staging penile cancer. Urology 23: , Persky LL, DeKernion J. Carcinoma of the penis. Cancer 36~ , Grabstald H. Controversies concerning lymph node dissection for cancer of the penis. Urol Clin N Am 7: , Catalona WJ. Role of lymphadenectomy iii carcinoma of the penis. Urol Clin N Am , Wespes E, Simon J, Shulman C. Cabanas approach: Is sentinel node biopsy reliable for staging penile carcinoma? Urol- O ~ Y 28~ , Droller MI. Carcinoma of the penis: An overview. Urol Clin N Am 7: , Johnson DE, Lo RK. Management of regional lymph nodes in penile carcinoma. Urology 24: , Cabanas RM. An approach for the treatment of penile carcinoma. Cancer 39:456, Hardner G, Bhanalaph T, Murphy G, et al. Carcinoma of the penis: Analysis of therapy in 100 consecutive cases. J Urol 108: , Dermatol. Surg. Oncol. 13:11 November
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
Carcinoma of the penis. Report of three cases and review of literature.
 ISPUB.COM The Internet Journal of Surgery Volume 20 Number 2 Carcinoma of the penis. Report of three cases and review of literature. V Yagnik Citation V Yagnik. Carcinoma of the penis. Report of three
ISPUB.COM The Internet Journal of Surgery Volume 20 Number 2 Carcinoma of the penis. Report of three cases and review of literature. V Yagnik Citation V Yagnik. Carcinoma of the penis. Report of three
GUIDELINES ON PENILE CANCER
 46 E. Solsona (chairman), F. Algaba, S. Horenblas, G. Pizzocaro, T. Windahl Eur Urol 2002;42(3):199-203 Introduction Penile carcinoma is an uncommon malignant disease with an incidence ranging from 0.1
46 E. Solsona (chairman), F. Algaba, S. Horenblas, G. Pizzocaro, T. Windahl Eur Urol 2002;42(3):199-203 Introduction Penile carcinoma is an uncommon malignant disease with an incidence ranging from 0.1
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
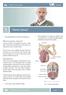 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
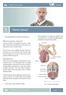 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
Choe s Urology Oral Board Self-Assessment, 4th ed. Anadem Publishing, Inc
 Choe s Urology Oral Board Self-Assessment, 4th ed. Anadem Publishing, Inc. anadem@anadem.com 800-633-0055 CASE (1 of 95 new or revised cases/450+ pages) HPI: PMH: PSH: 65-year-old African-American male
Choe s Urology Oral Board Self-Assessment, 4th ed. Anadem Publishing, Inc. anadem@anadem.com 800-633-0055 CASE (1 of 95 new or revised cases/450+ pages) HPI: PMH: PSH: 65-year-old African-American male
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW
 MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
A five year study on differential diagnosis of verruciform penile lesions
 Original Research Article A five year study on differential diagnosis of verruciform penile lesions S. Sujatha 1, V. Srinivas Kumar 2*, K. Durga 3 1 Associate Professor, 2 Assistant Professor, 3 Professor
Original Research Article A five year study on differential diagnosis of verruciform penile lesions S. Sujatha 1, V. Srinivas Kumar 2*, K. Durga 3 1 Associate Professor, 2 Assistant Professor, 3 Professor
GUIDELINEs ON PENILE CANCER
 GUIDELINEs ON PENILE CANCER (update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin Eur Urol 2010, doi:10.1016/j.eururo.2010.01.039 Introduction Over
GUIDELINEs ON PENILE CANCER (update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin Eur Urol 2010, doi:10.1016/j.eururo.2010.01.039 Introduction Over
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter.
 Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Penile cancer teams in UK. Common variants. Penile cancer teams. Basaloid squamous carcinoma. The Pathology of Penile Tumours
 The Pathology of Penile Tumours Dr Jonathan H Shanks The Christie NHS Foundation Trust, Manchester, UK Penile cancer teams in UK 12 centres for penile cancer work (10 in England and Wales, 2 in Scotland)
The Pathology of Penile Tumours Dr Jonathan H Shanks The Christie NHS Foundation Trust, Manchester, UK Penile cancer teams in UK 12 centres for penile cancer work (10 in England and Wales, 2 in Scotland)
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
A study of incidence and management of carcinoma of penis
 Research Article A study of incidence and management of carcinoma of penis K C T Naik 1*, A Setu Madhavi 2 1 Associate Professor, 2 Assistant Professor, Department of Surgery, RIMS Medical College, Ongole
Research Article A study of incidence and management of carcinoma of penis K C T Naik 1*, A Setu Madhavi 2 1 Associate Professor, 2 Assistant Professor, Department of Surgery, RIMS Medical College, Ongole
Comparative Study Between Video Endoscopic Inguinal Lymphadenectomy and Open Inguinal Lymphadenectomy Of Carcinoma of Penis
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 6 Ver. VIII (June. 2016), PP 23-28 www.iosrjournals.org Comparative Study Between Video Endoscopic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 6 Ver. VIII (June. 2016), PP 23-28 www.iosrjournals.org Comparative Study Between Video Endoscopic
ACCME/Disclosures. 52 year old man who consulted for a long-standing mass on the distal penis 4/13/2016
 ACCME/Disclosures United States and Canadian Academy of Pathology Seattle, WA 2016 Elsa F Velazquez, MD Director of Dermatopathology, V.P. Clinical Assistant Professor of Dermatology Tufts University,
ACCME/Disclosures United States and Canadian Academy of Pathology Seattle, WA 2016 Elsa F Velazquez, MD Director of Dermatopathology, V.P. Clinical Assistant Professor of Dermatology Tufts University,
A RARE CASE OF VERRUCOUS CARCINOMA IN MIDDLE AGED MALE
 A RARE CASE OF VERRUCOUS CARCINOMA IN MIDDLE AGED MALE *Alagar Samy R. and Elankumar S. ESIC Medical College and Hospital, Coimbatore, Tamilnadu, India *Author for Correspondence ABSTRACT Penile verrucous
A RARE CASE OF VERRUCOUS CARCINOMA IN MIDDLE AGED MALE *Alagar Samy R. and Elankumar S. ESIC Medical College and Hospital, Coimbatore, Tamilnadu, India *Author for Correspondence ABSTRACT Penile verrucous
Frequently Asked Questions
 Ida Orengo, M.D. Mohsin Mir, M.D. Department of Dermatology 1977 Butler Boulevard, Suite E6.200 Houston, TX 77030 (713) 798-6925 / (713) 798-6624 telephone (713) 798-5535 fax Frequently Asked Questions
Ida Orengo, M.D. Mohsin Mir, M.D. Department of Dermatology 1977 Butler Boulevard, Suite E6.200 Houston, TX 77030 (713) 798-6925 / (713) 798-6624 telephone (713) 798-5535 fax Frequently Asked Questions
Squamous carcinoma of the penis: a case report
 Squamous carcinoma of the penis: a case report De Fiores A., Diosi D., Bella G., De Marco V. Introdution Penile cancer is a relatively rare neoplasm in the developed world and 95% of the cases histologically
Squamous carcinoma of the penis: a case report De Fiores A., Diosi D., Bella G., De Marco V. Introdution Penile cancer is a relatively rare neoplasm in the developed world and 95% of the cases histologically
Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012
 Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012 Case Presentation 57 yo man with 3 month hx of a nonhealing < 1 cm right
Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012 Case Presentation 57 yo man with 3 month hx of a nonhealing < 1 cm right
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Rebecca Vogel, PGY-4 March 5, 2012
 Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
THE USE OF DEEPITHELIALIZATION
 THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
Disclosures. SLNB for Melanoma 25/02/2014 SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION
 8 th Canadian Melanoma Conference February 22, 2014 Rimrock Resort Hotel, Banff, Alberta SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION Christopher Bichakjian,
8 th Canadian Melanoma Conference February 22, 2014 Rimrock Resort Hotel, Banff, Alberta SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION Christopher Bichakjian,
Mohs surgery for the nail unit
 Mohs surgery for the nail unit olivier.cogrel@chu-bordeaux.fr Dermatologic surgery, Mohs surgery and lasers unit CHU Bordeaux, France Squamous cell carcinoma +++ Acral lentiginous melanoma Lichte et al.
Mohs surgery for the nail unit olivier.cogrel@chu-bordeaux.fr Dermatologic surgery, Mohs surgery and lasers unit CHU Bordeaux, France Squamous cell carcinoma +++ Acral lentiginous melanoma Lichte et al.
Cancer of the Oral Cavity
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
Mohs. Micrographic Surgery. For Treating Skin Cancer
 Mohs Micrographic Surgery For Treating Skin Cancer Skin Cancer Basics Skin cancer is common. Over the past three decades, more people have had skin cancer than all other cancers combined. Each year in
Mohs Micrographic Surgery For Treating Skin Cancer Skin Cancer Basics Skin cancer is common. Over the past three decades, more people have had skin cancer than all other cancers combined. Each year in
Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer
 Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
BLADDER CANCER: PATIENT INFORMATION
 BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
Da Costa was the first to coin the term. Marjolin s Ulcer: A Case Report and Literature Review. Case Report. Introduction
 E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
University of Kentucky. Markey Cancer Center
 University of Kentucky Markey Cancer Center Invasive Cancer of the Vagina and Urethra Fred Ueland, MD No matter what you accomplish in your life, the size of your funeral will still be determined by the
University of Kentucky Markey Cancer Center Invasive Cancer of the Vagina and Urethra Fred Ueland, MD No matter what you accomplish in your life, the size of your funeral will still be determined by the
Radical Surgical Treatment For Marjolin Ulcer Occurring After Chronic Osteomyelitis.(Letters To The Editor): An Article From: Southern Medical
 Radical Surgical Treatment For Marjolin Ulcer Occurring After Chronic Osteomyelitis.(Letters To The Editor): An Article From: Southern Medical Journal [HTML] [Digital] By Livia S. Smidt;Luis Felipe S.
Radical Surgical Treatment For Marjolin Ulcer Occurring After Chronic Osteomyelitis.(Letters To The Editor): An Article From: Southern Medical Journal [HTML] [Digital] By Livia S. Smidt;Luis Felipe S.
Original article. Key words: brachytherapy, inguinal metastases, penile carcinoma, prognostic factors, squamous cell, survival.
 Annals of Oncology 8: 089-098, 997. O 997 Kluwer Academic Publishers. Printed in the Netherlands. Original article Squamous cell carcinoma of the penis: Multivariate analysis of prognostic factors and
Annals of Oncology 8: 089-098, 997. O 997 Kluwer Academic Publishers. Printed in the Netherlands. Original article Squamous cell carcinoma of the penis: Multivariate analysis of prognostic factors and
Using the Mohs Technique for Thin Melanomas
 Dermatology Associates Mohs Micrographic Surgery 2300 W Stone Drive Kingsport TN 37660 Telephone 423-246-4961 1-800-445-7274 (VA Toll Free) Fax 423-245-1200 Using the Mohs Technique for Thin Melanomas
Dermatology Associates Mohs Micrographic Surgery 2300 W Stone Drive Kingsport TN 37660 Telephone 423-246-4961 1-800-445-7274 (VA Toll Free) Fax 423-245-1200 Using the Mohs Technique for Thin Melanomas
MALE GENITAL SURGICAL PROCEDURES
 Male Genital Surgical ProceduresDecember 22, 2015 (effective March 1, 201) PENIS Slit of prepuce (complete care) S5 - newborn... 14.35 S58 - infant... 21.50 S59 - adult or child... 30.25 EXCISION Circumcision
Male Genital Surgical ProceduresDecember 22, 2015 (effective March 1, 201) PENIS Slit of prepuce (complete care) S5 - newborn... 14.35 S58 - infant... 21.50 S59 - adult or child... 30.25 EXCISION Circumcision
Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision
 Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision Christopher J. Miller, MD Director of Penn Dermatology Oncology Center Associate
Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision Christopher J. Miller, MD Director of Penn Dermatology Oncology Center Associate
Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy
 American Academy of Dermatology 2018 Annual Meeting San Diego, CA, February 17, 2018 Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy Christopher Bichakjian,
American Academy of Dermatology 2018 Annual Meeting San Diego, CA, February 17, 2018 Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy Christopher Bichakjian,
Clinical characteristics
 Skin Cancer Fernando Vega, MD Seattle Healing Arts Clinical characteristics Precancerous lesions Common skin cancers ACTINIC KERATOSIS Precancerous skin lesions Actinic keratoses Dysplastic melanocytic
Skin Cancer Fernando Vega, MD Seattle Healing Arts Clinical characteristics Precancerous lesions Common skin cancers ACTINIC KERATOSIS Precancerous skin lesions Actinic keratoses Dysplastic melanocytic
Topics for Discussion. Malignant Melanoma. Surgical Treatment. Current Treatment of Cutaneous Melanoma 5/17/2013. Lymph Regional nodes:
 Topics for Discussion What is a sentinel lymph node (SLN)? Utility of sentinel lymph biopsies: therapeutic or staging? Current Treatment of Cutaneous Melanoma Carlos Corvera, M.D. Associate Professor of
Topics for Discussion What is a sentinel lymph node (SLN)? Utility of sentinel lymph biopsies: therapeutic or staging? Current Treatment of Cutaneous Melanoma Carlos Corvera, M.D. Associate Professor of
MEDitorial March Bladder Cancer
 MEDitorial March 2010 Bladder Cancer Last month, my article addressed the issue of blood in the urine ( hematuria ). A concerning cause of hematuria is bladder cancer, a variably malignant tumor starting
MEDitorial March 2010 Bladder Cancer Last month, my article addressed the issue of blood in the urine ( hematuria ). A concerning cause of hematuria is bladder cancer, a variably malignant tumor starting
URETHRAL CANCER EPIDEMIOLOGY - 1
 URETHRAL CANCER Diagnosis & Management Case Conferences Jennie Mickelson Grand Rounds November 15, 2006 EPIDEMIOLOGY - 1 RARE 2200 reported cases F:M - 4:1 1 FEMALE URETHRAL CA any age but >60 most common
URETHRAL CANCER Diagnosis & Management Case Conferences Jennie Mickelson Grand Rounds November 15, 2006 EPIDEMIOLOGY - 1 RARE 2200 reported cases F:M - 4:1 1 FEMALE URETHRAL CA any age but >60 most common
Melanoma Surgery Update James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division
 Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
- Questions concerning your upcoming surgery can be addressed by our Mohs Support Specialist:
 Dermatology Associates Mohs Micrographic Surgery 2300 W Stone Drive Kingsport TN 37660 Telephone 423-246-4961 1-800-445-7274 (VA Toll Free) Fax 423-245-1200 In preparation for your upcoming appointment
Dermatology Associates Mohs Micrographic Surgery 2300 W Stone Drive Kingsport TN 37660 Telephone 423-246-4961 1-800-445-7274 (VA Toll Free) Fax 423-245-1200 In preparation for your upcoming appointment
Kentaro Tanaka, 1 Hiroki Mori, 1 Mutsumi Okazaki, 1 Aya Nishizawa, 2 and Hiroo Yokozeki Introduction. 2. Case Presentation
 Case Reports in Oncological Medicine Volume 2013, Article ID 259326, 4 pages http://dx.doi.org/10.1155/2013/259326 Case Report Long-Term Treatment Outcome after Only Popliteal Lymph Node Dissection for
Case Reports in Oncological Medicine Volume 2013, Article ID 259326, 4 pages http://dx.doi.org/10.1155/2013/259326 Case Report Long-Term Treatment Outcome after Only Popliteal Lymph Node Dissection for
Policy #: 127 Latest Review Date: June 2011
 Name of Policy: Mohs Micrographic Surgery Policy #: 127 Latest Review Date: June 2011 Category: Surgery Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates. Background/Definitions:
Name of Policy: Mohs Micrographic Surgery Policy #: 127 Latest Review Date: June 2011 Category: Surgery Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates. Background/Definitions:
Melanoma Quality Reporting
 Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Diseases of the vulva
 Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Commissioning Policy Individual Funding Request
 Commissioning Policy Individual Funding Request Penile Conditions - Surgical Opinion and Treatment Policy including Circumcision in all male patients over the age of 18 years Prior Approval Policy Date
Commissioning Policy Individual Funding Request Penile Conditions - Surgical Opinion and Treatment Policy including Circumcision in all male patients over the age of 18 years Prior Approval Policy Date
UWMC Roosevelt Clinic Rotation Goals 2011 Procedural Dermatology Fellowship Program 1
 Procedural Dermatology Fellowship Objectives University of Washington Medical Center-Roosevelt Rotation The primary goal of the University of Washington rotation of the Procedural Dermatology fellowship
Procedural Dermatology Fellowship Objectives University of Washington Medical Center-Roosevelt Rotation The primary goal of the University of Washington rotation of the Procedural Dermatology fellowship
Knowledge-Powered Medicine
 mohs surgery A patient guide to specialized treatment for skin cancer Knowledge-Powered Medicine upgdocs.org/dermatology upgdocs.org/dermatology A patient guide Preparing for Mohs Surgery > What is Mohs
mohs surgery A patient guide to specialized treatment for skin cancer Knowledge-Powered Medicine upgdocs.org/dermatology upgdocs.org/dermatology A patient guide Preparing for Mohs Surgery > What is Mohs
ACGME Clinical Fellowship Program: Micrographic Surgery and Dermatologic Oncology Fellowship. Program Demographics
 ACGME Clinical Fellowship Program: Micrographic Surgery and Dermatologic Oncology Fellowship Program Demographics 1. Name of Host Institution: University of California San Francisco 2. Program: Dermatology
ACGME Clinical Fellowship Program: Micrographic Surgery and Dermatologic Oncology Fellowship Program Demographics 1. Name of Host Institution: University of California San Francisco 2. Program: Dermatology
Proposed All Wales Vulval Cancer Guidelines. Dr Amanda Tristram
 Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
Carcinoma of the Lung
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
Complications of Circumcision in Male Children: Report of Sixty-one Cases
 Bahrain Medical Bulletin, Vol. 32, No. 3, September 2010 Complications of Circumcision in Male Children: Report of Sixty-one Cases Mahmood Abbas, CABS, EBPS* Hussain Mohamed, MD, MRCSI** Nader Rabea, MBBS,
Bahrain Medical Bulletin, Vol. 32, No. 3, September 2010 Complications of Circumcision in Male Children: Report of Sixty-one Cases Mahmood Abbas, CABS, EBPS* Hussain Mohamed, MD, MRCSI** Nader Rabea, MBBS,
BREAST CANCER SURGERY. Dr. John H. Donohue
 Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER
 GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER (Limited text update December 21) M. Babjuk, W. Oosterlinck, R. Sylvester, E. Kaasinen, A. Böhle, J. Palou, M. Rouprêt Eur Urol 211 Apr;59(4):584-94 Introduction
GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER (Limited text update December 21) M. Babjuk, W. Oosterlinck, R. Sylvester, E. Kaasinen, A. Böhle, J. Palou, M. Rouprêt Eur Urol 211 Apr;59(4):584-94 Introduction
Guidelines for Management of Penile Cancer
 Guidelines for Management of Penile Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Sections 3, 5, 6 and 16 updated. Page 1 of 10 1. Scope
Guidelines for Management of Penile Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Sections 3, 5, 6 and 16 updated. Page 1 of 10 1. Scope
Dermatology Associates Mohs Micrographic Surgery
 Dermatology Associates Johnson City 2885 Boones Creek Road 423-928-9014 Kingsport 2300 W Stone Drive 423-246-4961 1-800-445-7274 Bristol 3183 W State Street 423-764-7131 In preparation for your upcoming
Dermatology Associates Johnson City 2885 Boones Creek Road 423-928-9014 Kingsport 2300 W Stone Drive 423-246-4961 1-800-445-7274 Bristol 3183 W State Street 423-764-7131 In preparation for your upcoming
UICC TNM 8 th Edition Errata
 UICC TNM 8 th Edition Errata ions are in italics Page 28 Oropharynx p16 positive Pathological Stage II,T2 N2 M0 T3 N0,N1 M0 Stage II,T2 N2 M0 T3,T4 N0,N1 M0 Page 61 Oesophagus Adenocarcinoma Pathological
UICC TNM 8 th Edition Errata ions are in italics Page 28 Oropharynx p16 positive Pathological Stage II,T2 N2 M0 T3 N0,N1 M0 Stage II,T2 N2 M0 T3,T4 N0,N1 M0 Page 61 Oesophagus Adenocarcinoma Pathological
Head & Neck Squamous Carcinoma: Artifacts, Challenges, and Controversies. Agenda
 Head & Neck Squamous Carcinoma: Artifacts, Challenges, and Controversies Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University
Head & Neck Squamous Carcinoma: Artifacts, Challenges, and Controversies Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University
Guideline for the Management of Vulval Cancer
 Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
MOHS MICROGRAPHIC SURGERY
 MOHS MICROGRAPHIC SKIN CANCER Skin cancer is by far the most common malignant tumor in humans. The most common types of skin cancer are basal cell carcinoma, squamous cell carcinoma, and melanoma. Both
MOHS MICROGRAPHIC SKIN CANCER Skin cancer is by far the most common malignant tumor in humans. The most common types of skin cancer are basal cell carcinoma, squamous cell carcinoma, and melanoma. Both
6 UROLOGICAL CANCERS. 6.1 Key Points
 6 UROLOGICAL CANCERS 6.1 Key Points Prostate Cancer Commonest cancer in males in Scotland Approximately 99% of cases occur in men aged > 50 years About 40% of cases present in men aged < 70 years when
6 UROLOGICAL CANCERS 6.1 Key Points Prostate Cancer Commonest cancer in males in Scotland Approximately 99% of cases occur in men aged > 50 years About 40% of cases present in men aged < 70 years when
ORIGINAL ARTICLE. Clinical Node-Negative Thick Melanoma
 ORIGINAL ARTICLE Clinical Node-Negative Thick Melanoma George I. Salti, MD; Ashwin Kansagra, MD; Michael A. Warso, MD; Salve G. Ronan, MD ; Tapas K. Das Gupta, MD, PhD, DSc Background: Patients with T4
ORIGINAL ARTICLE Clinical Node-Negative Thick Melanoma George I. Salti, MD; Ashwin Kansagra, MD; Michael A. Warso, MD; Salve G. Ronan, MD ; Tapas K. Das Gupta, MD, PhD, DSc Background: Patients with T4
Squamous cell carcinoma of the nail bed: Three case reports
 Journal of Orthopaedic Surgery 2004:12(2):248 252 Squamous cell carcinoma of the nail bed: Three case reports TC Wong, FK Ip, WC Wu Department of Orthopaedics and Traumatology, Pamela Youde Nethersole
Journal of Orthopaedic Surgery 2004:12(2):248 252 Squamous cell carcinoma of the nail bed: Three case reports TC Wong, FK Ip, WC Wu Department of Orthopaedics and Traumatology, Pamela Youde Nethersole
Case Report Pannus Is the New Prepuce? Penile Cancer in a Buried Phallus
 Case Reports in Urology Volume 2015, Article ID 403545, 4 pages http://dx.doi.org/10.1155/2015/403545 Case Report Pannus Is the New Prepuce? Penile Cancer in a Buried Phallus Jared Manwaring, 1 Srinivas
Case Reports in Urology Volume 2015, Article ID 403545, 4 pages http://dx.doi.org/10.1155/2015/403545 Case Report Pannus Is the New Prepuce? Penile Cancer in a Buried Phallus Jared Manwaring, 1 Srinivas
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Malignant melanoma: assessment and management of malignant melanoma 1.1 Short title Malignant Melanoma 2 The remit The Department
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Malignant melanoma: assessment and management of malignant melanoma 1.1 Short title Malignant Melanoma 2 The remit The Department
EAU Guidelines on Penile Cancer
 EAU Guidelines on Penile Cancer O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson European Association of Urology 2017 TABLE OF CONTENTS
EAU Guidelines on Penile Cancer O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson European Association of Urology 2017 TABLE OF CONTENTS
Staging and Grading Last Updated Friday, 14 November 2008
 Staging and Grading Last Updated Friday, 14 November 2008 There is a staging graph below Blood in the urine is the most common indication that something is wrong. Often one will experience pain or difficulty
Staging and Grading Last Updated Friday, 14 November 2008 There is a staging graph below Blood in the urine is the most common indication that something is wrong. Often one will experience pain or difficulty
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type)
 Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
Lecture name: Urethra and peniile diseases. By Dr.Salam almosawi (F.I.B.M.S)
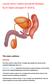 Lecture name: Urethra and peniile diseases. By Dr.Salam almosawi (F.I.B.M.S) The male urethera: Anatomy: The male urethra is about 20 cm. in length and classify into 2 parts by the urogenital diaphragm
Lecture name: Urethra and peniile diseases. By Dr.Salam almosawi (F.I.B.M.S) The male urethera: Anatomy: The male urethra is about 20 cm. in length and classify into 2 parts by the urogenital diaphragm
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Information for Patients. Primary urethral cancer. English
 Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
Surgical Management of Squamous Cell Carcinoma of the Penis
 Articles TheScientificWorldJOURNAL (2004) 4 (S1), 179 191 ISSN 1537-744X; DOI 10.1100/tsw.2004.66 Surgical Management of Squamous Cell Carcinoma of the Penis Donald F. Lynch, M.D. and Paul F. Schellhammer,
Articles TheScientificWorldJOURNAL (2004) 4 (S1), 179 191 ISSN 1537-744X; DOI 10.1100/tsw.2004.66 Surgical Management of Squamous Cell Carcinoma of the Penis Donald F. Lynch, M.D. and Paul F. Schellhammer,
Poor Outcomes in Head and Neck Non-Melanoma Cutaneous Carcinomas
 10 The Open Otorhinolaryngology Journal, 2011, 5, 10-14 Open Access Poor Outcomes in Head and Neck Non-Melanoma Cutaneous Carcinomas Kevin C. Huoh and Steven J. Wang * Head and Neck Surgery and Oncology,
10 The Open Otorhinolaryngology Journal, 2011, 5, 10-14 Open Access Poor Outcomes in Head and Neck Non-Melanoma Cutaneous Carcinomas Kevin C. Huoh and Steven J. Wang * Head and Neck Surgery and Oncology,
Cervical Cancer 3/25/2019. Abnormal vaginal bleeding
 Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
Melanoma. Kaushik Mukherjee MD A. Scott Pearson MD
 Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Moh's Surgery Information Packet
 Moh's Surgery Information Packet BE SURE TO BRING THE FOLLOWING TO YOUR APPOINTMENT Insurance card Insurance referral (if required by your insurance) Name and address of your primary care provider as well
Moh's Surgery Information Packet BE SURE TO BRING THE FOLLOWING TO YOUR APPOINTMENT Insurance card Insurance referral (if required by your insurance) Name and address of your primary care provider as well
Decision making in surgical oncology- when to cut big, when to cut small
 Decision making in surgical oncology- when to cut big, when to cut small Simon T. Kudnig, BVSc, MVS, MS, FANZCVSc, Dipl. ACVS ACVS Founding Fellow in Surgical Oncology Animal Referral Hospital, Melbourne,
Decision making in surgical oncology- when to cut big, when to cut small Simon T. Kudnig, BVSc, MVS, MS, FANZCVSc, Dipl. ACVS ACVS Founding Fellow in Surgical Oncology Animal Referral Hospital, Melbourne,
Alcohol should be avoided for 3 days prior to surgery and 2 days after the procedure.
 Mohs Surgery Information Packet Be sure to bring the following to your appointment: Insurance Card Insurance Referral ( If required by your insurance) Name and address of your primary care provider as
Mohs Surgery Information Packet Be sure to bring the following to your appointment: Insurance Card Insurance Referral ( If required by your insurance) Name and address of your primary care provider as
Management of Neck Metastasis from Unknown Primary
 Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
Technicians & Nurses Program
 ASCRS ASOA Symposium & Congress Technicians & Nurses Program May 6-10, 2016 New Orleans Evaluation and Treatment of Eyelid Malignancies Richard C. Allen MD PhD FACS Professor Section of Ophthalmology Dept.
ASCRS ASOA Symposium & Congress Technicians & Nurses Program May 6-10, 2016 New Orleans Evaluation and Treatment of Eyelid Malignancies Richard C. Allen MD PhD FACS Professor Section of Ophthalmology Dept.
Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva Malignant melanoma sho
 Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
UICC TNM 8 th Edition Errata
 UICC TNM 8 th Edition Errata ions are in italics Head and Neck Tumours Pages 20, p27, p34, p38, p41, and p49 ly pn2a Metastasis in a single ipsilateral lymph node, less than 3cm in greatest dimension with
UICC TNM 8 th Edition Errata ions are in italics Head and Neck Tumours Pages 20, p27, p34, p38, p41, and p49 ly pn2a Metastasis in a single ipsilateral lymph node, less than 3cm in greatest dimension with
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches
 Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
Merkel Cell Carcinoma Case # 2
 DISCHARGE SUMMARY Admitted: 10/11/2010 Discharged: 10/13/2010 Merkel Cell Carcinoma Case # 2 Chief Compliant: A 79 year old lady status post tumor on the scalp excision and left neck likely dissection
DISCHARGE SUMMARY Admitted: 10/11/2010 Discharged: 10/13/2010 Merkel Cell Carcinoma Case # 2 Chief Compliant: A 79 year old lady status post tumor on the scalp excision and left neck likely dissection
When to Integrate Surgery for Metatstatic Urothelial Cancers
 When to Integrate Surgery for Metatstatic Urothelial Cancers Wade J. Sexton, M.D. Senior Member and Professor Department of Genitourinary Oncology Moffitt Cancer Center Case Presentation #1 67 yo male
When to Integrate Surgery for Metatstatic Urothelial Cancers Wade J. Sexton, M.D. Senior Member and Professor Department of Genitourinary Oncology Moffitt Cancer Center Case Presentation #1 67 yo male
Radionuclide detection of sentinel lymph node
 Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Update on SLN and Melanoma: DECOG and MSLT-II. Gordon H. Hafner, MD, FACS
 Update on SLN and Melanoma: DECOG and MSLT-II Gordon H. Hafner, MD, FACS No disclosures The surgery of malignant disease is not the surgery of organs, it is of the lymphatic system. Lord Moynihan Lymph
Update on SLN and Melanoma: DECOG and MSLT-II Gordon H. Hafner, MD, FACS No disclosures The surgery of malignant disease is not the surgery of organs, it is of the lymphatic system. Lord Moynihan Lymph
A REPORT OF TWO CASES OF SQUAMOUS CELL CARCINOMA OF THE HAND IN PATIENTS WITH EPIDERMOLYSIS BULLOSA DYSTROPHICA
 Basrah Journal Case Report Of Surgery A REPORT OF TWO CASES OF SQUAMOUS CELL CARCINOMA OF THE HAND IN PATIENTS WITH EPIDERMOLYSIS BULLOSA DYSTROPHICA MB,ChB, Assist. Prof., FICMS, Consultant Orthopaedic
Basrah Journal Case Report Of Surgery A REPORT OF TWO CASES OF SQUAMOUS CELL CARCINOMA OF THE HAND IN PATIENTS WITH EPIDERMOLYSIS BULLOSA DYSTROPHICA MB,ChB, Assist. Prof., FICMS, Consultant Orthopaedic
Soft Tissue Sarcoma. Presley Regional Trauma Center Department of Surgery University of Tennessee Health Science Center Memphis, Tennessee
 Soft Tissue Sarcoma Presley Regional Trauma Center Department of Surgery University of Tennessee Health Science Center Memphis, Tennessee Soft Tissue Sarcoma Collective term for an unusual and diverse
Soft Tissue Sarcoma Presley Regional Trauma Center Department of Surgery University of Tennessee Health Science Center Memphis, Tennessee Soft Tissue Sarcoma Collective term for an unusual and diverse
Modalities of Radiation
 Modalities of Radiation Superficial radiotherapy Orthovoltage Megavoltage Photons Electrons Brachytherapy Interstitial Moulds When to refer? The vast majority of skin cancers will be managed without any
Modalities of Radiation Superficial radiotherapy Orthovoltage Megavoltage Photons Electrons Brachytherapy Interstitial Moulds When to refer? The vast majority of skin cancers will be managed without any
Title: Male Circumcision Policy
 Item 16.120cii The Clinical Commissioning Groups for Great Yarmouth and Waveney, North Norfolk, Norwich, South Norfolk and West Norfolk, supported by North East London Commissioning Support Unit Policy
Item 16.120cii The Clinical Commissioning Groups for Great Yarmouth and Waveney, North Norfolk, Norwich, South Norfolk and West Norfolk, supported by North East London Commissioning Support Unit Policy
