Serum Inorganic Phosphorus
|
|
|
- Bertha Nichols
- 6 years ago
- Views:
Transcription
1 198 Serum Inorganic Phosphorus VINOD K. BANSAL Definition Phosphorus is an abundant element that is widespread in its distribution. It is a major intracellular anion in mammals. Total body phosphorus in a 70-kg man is about 700 to 800 mg, 85% of which is in the skeleton in hydroxyapatite phase ; the remaining 15% is in soft tissues. Almost all of the phosphorus found in the extracellular fluid space is in the form of inorganic phosphate. Serum inorganic phosphate reflects only a very minor percentage of total body phosphorus ; however, it is easily measurable and gives a clue to the status of body phosphorus stores. The majority of the phosphate in the body is in the organic form as a complex with carbohydrates, lipids, and proteins. Phosphorus is an essential element in the cellular structure, cytoplasm, and mitochondrium. It is necessary for several enzymatic processes in glycolysis, ammoniagenesis as well as in oxidative phosphorylation, resulting in energy from the formation of adenosine triphosphate from adenosine diphosphate. In addition, it influences oxygen-carrying capacity of hemoglobin by its role in the regulation of 2, 3-diphosphoglycerate (2,3-DPG) synthesis. The normal serum phosphorus concentration is 3.4 to 4.5 mg/dl (1.12 to 1.45 mmol/l). This fluctuates with age (it is higher in children than adults), dietary intake, and acid-base status. There is a diurnal variation, which reaches its nadir between 8 and 11 A.M. The concentration of serum phosphate is generally expressed in milligrams per deciliter because concentration in millimoles can vary with acid-base status. In serum, phosphate exists in two forms, dihydrogen phosphate (H 2PO4 and its salt, mono-hydrogen phosphate (HPO,). The relationship between these two can be determined by the Henderson-Hasselbalch equation. At the physiologic ph of 7.40, the pk of H2PO4 is 6.8 and the ratio of HPO, to H2PO4 is 4 : 1. The valence of phosphorus at a ph of 7.40 is l.8. Serum levels expressed in milligrams can be converted to millimoles per liter by multiplying by To convert to milliequivalents, multiply the concentration in millimoles by the valence (1.8 at ph of 7.40). About 85 to 90% of serum phosphate is free and is ultrafiltrable ; 10 to 15% is bound with protein. Technique Serum inorganic phosphate is measured either colorimetrically or isotopically (32P) ; the latter is not in routine use. The usual colorimetric technique is that of Fiske and Subbarow, or its modification. The principle behind the colorimetric method is the formation of phosphomolybdic acid, which is then reduced to molybdenum blue by an agent such as stannous chloride. Molybdenum blue absorbs at 660 nm. The automated method is generally offered as a part of a package with several other chemistries. In occasional cases, the determination may be interfered with by proteins, bilirubin, or organic phosphates, but these conditions are rare. Serum phosphate should ideally be determined in the fasting state. A recent meal, high glucose ingestion, insulin release or administration, muscular activity, and hyperventilation can all lower serum phosphate by causing a shift from the plasma into the cells. Basic Science Phosphorus is present in ample amounts in many foods (e..g., red meat, dairy products, legumes). An average diet contains about 1.0 to 1.5 g a day. The gastrointestinal (GI) tract absorbs 75 to 80% of the ingested phosphate, and the rest is excreted in the feces. Higher phosphate intakes lead to high absorption, but the percentage of GI absorption is about the same. Low phosphate intake results in more complete absorption. Phosphate absorption is most likely via passive diffusion between cells through paracellular pathways. There is also an active transport that may be carrier mediated. At physiologic ph, phosphate uptake by luminal cells may be dependent on intraluminal sodium. Phosphate is absorbed throughout the entire intestine, but the major site is the jejunum, followed by the duodenum and ileum. Jejunal absorption is vitamin D dependent. The major route of excretion is by the kidneys. About 80% of the plasma protein is ultrafiltrable. Under usual conditions, about 85 to 90% of filtered phosphorus is reabsorbed. The reabsorption of phosphate is passive, occurring primarily in the proximal tubules. The reabsorption of phosphate by proximal tubules is not homogeneous. A large component of filtered phosphate is reabsorbed in the early portions of the tubules, and the rest by the remaining part of the proximal tubule. Beyond the proximal tubule, the mode and sites of phosphate reabsorption are controversial, but it appears that phosphate transport probably occurs in the pars recta as well as the early and late distal tubules. Micropuncture studies virtually exclude the loop of Henle as a site of transport. Phosphate reabsorption in the proximal tubule appears to be closely linked to sodium transport, but is independent of sodium in response to glucose load and insulin administration. Several factors modify the reabsorption of phosphate and can be classified as hormonal and nonhormonal (Table 198.1). Tubular reabsorption of phosphate has a maximum, the Tm, which will be altered by many of the factors described in Table 198.l. The tubular reabsorption of phosphorus has been used as a clinical test for parathyroid activity. Disorders of serum phosphorus may occur from three possible mechanisms : dietary intake, GI disorders, and renal handling. Phosphorus is abundant in the diet ; therefore, dietary deficiency of phosphate is unlikely, although it can occur in prolonged starvation or with certain GI disorders 895
2 896 XIV. THE GENITOURINARY SYSTEM Table Factors Affecting the Tubular Reabsorption of Phosphate Increased reabsorption Hormonal Insulin Growth hormone Vitamin D or its metabolite (acute administration) Nonhormonal Hypercalcemia Hypermagnesemia Dietary restriction of phosphate intake Decreased reabsorption Hormonal Parathyroid hormone Calcitonin Glucocorticoids Thyroid Nonhormonal Extracellular volume expansion Diuretics Alcohol ingestion High dietary intake Urinary alkalinization such as intractable vomiting, malabsorptive states, and acute diarrheas. The kidney remains the most significant organ regulating phosphate homeostasis, and most of the clinical perturbations seen are caused by renal phosphate wasting. Phosphorus forms cell membranes and participates in the activity of mitochondria, DNA, RNA, and various nucleotides. It regulates oxygen-carrying capacity by its role in regulating the level of 2,3-DPG, and takes part in enzymatic reactions involving glycolysis, ammoniagenesis, and 1,25-hydroxyvitamin D s hydroxylase. Deficiency of phosphate therefore has far-ranging effects and affects virtually every part of the body. The consequences of phosphate deficiency are summarized in Table Most of the adverse effects occur only with marked phosphate depletion. Mild to moderate phosphate deficiency is generally well tolerated (serum phosphorus levels between I and 3.5 mg/ dl), but phosphorus is an integral part of the cell's energy production and any phosphate deficiency can affect vital cellular functions. The symptoms of phosphate deficiency generally occur with serum phosphate levels below 1 mg/ dl. In general, patients become anorectic, weak, and may complain of bone pain. Abnormalities of red blood cells include a decrease in 2,3-DPG and adenosine triphosphate, resulting in depression of P50 values with a decreased release of oxygen to peripheral tissue. Hemolytic anemia may also develop in severe deficiency states. Leukocyte functions such as chemotaxis and phagocytosis may also be impaired. Severe phosphate deficiency might also produce severe reversible cardiomyopathy. In the presence of phosphate deficiency, an impairment of bone mineralization leads to widening of the osteoid seam. Mental confusion is a recognized complication of severe phosphate depletion and may result from a decrease in 2,3-DPG, interfering with oxygen release. A characteristic of severe hypophosphatemia is skeletal muscle damage with an elevation of the serum creatine phosphokinase and aldolase levels, and in some cases rhabdomyolysis. Pulmonary muscle weakness may result from hypophosphatemia and, in some cases, may impede weaning from a ventilator. Hypophosphatemia causes decreased absorption of calcium in the renal tubules, leading to hypercalciuria. In addition, hypophosphatemia alters renal acid-base status by four possible mechanisms : depressed proximal tubular reabsorption of bicarbonate, leading to bicarbonate wasting ; impaired distal tubular acidification ; decreased buffer excretion due to low phosphate excretion ; and diminished renal ammoniagenesis. Table Clinical and Biochemical Manifestations of Marked Hypophosphatemia Hematologic alterations Red blood cells Decreased ATP Decreased 2,3-DPG Decreased P50 Increased oxygen affinity Decreased lifespan Hemolysis Spherocytosis Leukocytes Decreased phagocytosis Decreased chemotaxis Decreased bactericidal activity Platelets Impaired clot retraction Thrombocytopenia Decreased ATP Megakaryocytosis Decreased lifespan Skeletal abnormalities Bone pain Radiolucent areas (x-ray) Pseudofractures Rickets or osteomalacia Central nervous system Anorexia Irritability Confusion Paresthesias Dysarthria Coma Cardiovascular Decreased cardiac output Increased left ventricular end-diastolic pressure Muscular Muscle weakness Rhabdomyolysis Decreased transmembrane resting potential Biochemical Low PTH levels Increased 1,25-(OH) 2Ds Hypercalcemia Hypomagnesemia Hypermagnesuria Hypophosphaturia Decreased GFR Decreased Tm for bicarbonate Decreased renal gluconeogenesis Decreased titrable acid excretion Increased creatine phosphokinase Increased aldolase Source: Reproduced with permission from Slatopolsky E. Pathophysiology of calcium, magnesium, and phosphate metabolism. In : Klahr S, ed. The kidney and body fluids in health and disease. New York: Plenum, Clinical Significance Disorders of phosphate homeostasis occur in a wide range of clinical conditions. Both hyper- and hypophosphatemia can be caused by cellular shifts of phosphate. The three primary conditions that lead to phosphate dysfunction are dietary intake, GI, and renal status. Since serum inorganic phosphate is only a minute portion of body phosphate, al-
3 198. SERUM INORGANIC PHOSPHORUS 897 terations in the serum level can occur when the body phosphate is low, normal, or high. Hyperphosphatemia The common causes of hyperphosphatemia are summarized in Table Apart from cellular shifts, most hyperphosphatemia occurs in the presence of renal insufficiency with a decrease in phosphate excretion. In chronic renal failure, significant hyperphosphatemia is not seen until the GFR has fallen below 25 ml/min, although early phosphate retention causes a decrease in ionized calcium, leading to increased parathyroid hormone and initiation of a whole cascade of events that ultimately produce renal osteodystrophy. Hyperphosphatemia occurs in several endocrine conditions associated with increased tubular reabsorption of phosphate. In pseudohypoparathyroidism, there is failure of parathyroid hormone to act on renal tubules, resulting in a high Tm which is responsible for the high serum phosphate in the presence of an abnormal circulating parathyroid hormone. In acromegaly, excess growth hormone leads to increased tubular reabsorption of phosphate. In other clinical situations with a high serum phosphate, there is increased tubular reabsorption of phosphate. Thus, in magnesium deficiency there is decreased release of parathyroid hormone, producing a picture similar to hypoparathyroidism. In tumoral calcinosis, a condition seen more frequently in blacks, there appears to be primary increased tubular reabsorption of phosphate with normal GI absorption of calcium. With the administration of vitamin D or its analogs, there is increased absorption of calcium and phosphate from the gastrointestinal tract ; if there is some degree of renal insufficiency, hyperphosphatemia may result. Table Causes of Hyperphosphatemia Cellular shift (from cells to ECV) Neoplastic : leukemias, lymphomas Increased catabolism, e.g., rhabdomyolysis Respiratory acidosis, diabetic ketoacidosis, tissue ischemia Decreased renal excretion Renal failure, acute and chronic Hypoparathyroidism Pseudohypoparathyroidism, Type I and II Abnormal circulating parathyroid hormone Other endocrine disorders, hyperthyroidism, acromegaly, juvenile hypogonadism Increased phosphate load Oral loads : vitamin D intoxication, phosphate-containing laxatives, high dietary phosphate (in presence of decreased GFR) Parenteral : intravenous phosphorus, transfusion of old blood (hemolysis) Miscellaneous Cortical hyperosteosis Volume contraction Familial intermittent hyperphosphatemia Magnesium deficiency (impaired PTH secretion) Tumoral calcinosis Source: Adapted with permission from Slatopolsky E. Pathology of calcium, magnesium, and phosphate metabolism. In : Klahr S, ed. The kidney and body fluids in health and disease. New York : Plenum, The symptomatology of hyperphosphatemia is related to the conditions producing it. The most common risk is ectopic or metastatic calcification, which may occur if the product of the serum calcium and phosphorus exceeds 70. The calcification may occur in any organ, although it is seen most commonly in the cornea, conjunctiva, lungs, and skin. The calcification is facilitated by alkalosis. Vascular calcification can produce gangrene as well as deposits in the cardiac conducting system. Therapy consists of identifying the underlying cause and correcting it. In renal insufficiency, therapy consists of controlling dietary intake of phosphates and use of phosphate binders. Initiation of dialysis helps in controlling serum phosphate levels, but in itself is rarely effective. Hypophosphatemia Hypophosphatemia usually implies a serum concentration of less than 2.5 mg/dl. However, phosphate levels below 1 mg/dl are commonly symptomatic, and such levels are often labeled as severe hypophosphatemia. Phosphorus depletion is characterized by reduction in total body phosphorus stores. However, hypophosphatemia (mild, moderate, or severe) can occur without phosphate depletion. The common causes of hypophosphatemia are listed in Table Hypophosphatemia is seen most frequently in hospitalized patients. The three primary mechanisms leading to hypophosphatemia are : (1) transcellular shift of phosphorus (from extracellular volume to either soft tissues or bones) ; (2) poor dietary intake, especially when associated with impaired GI absorption or diarrhea ; and (3) increased phosphate excretion resulting from renal and nonrenal causes. The nonrenal loss occurs through the gut, primarily malabsorptive states or diarrheal conditions. A simple deficiency of vitamin D will lead to rickets in childhood and osteomalacia in adults, along with poor phosphate absorption. Phosphate binders, such as nonabsorbable antacids containing aluminum, bind phosphorus in the gut and block the absorption of both ingested and secreted phosphate. Major losses of phosphorus can occur through the kidneys. The usual cause of renal phosphate wasting is excess parathyroid hormone, which reduces the maximum renal tubular reabsorption of phosphorus. These defects may be congenital or acquired. Among the congenital defects, the best known is Fanconi's syndrome-a proximal tubular disorder producing phosphaturia, glycosuria, aminoaciduria, uricosuria, and bicarbonaturia. A similar picture may also be seen in cystinosis, Wilson's disease, hereditary fructose intolerance, and glycogen storage disease. Acquired defects include multiple myeloma, amyloidosis, and heavy metal intoxication. In postrenal transplantation, a state of secondary hyperparathyroidism may exist, with high circulating parathyroid hormone resulting in phosphate wasting by normal renal tubules. Such a state may persist for several months. Vitamin D-resistant rickets is believed to be caused by a phosphate leak from renal tubules along with defective intestinal absorption of phosphate. Renal tubular wasting can also occur during extracellular volume expansion with saline or bicarbonate. Such a picture can be seen during the diuretic phase of acute tubular necrosis or with the use of diuretic agents. In several clinical settings, hypophosphatemia may be the result of a combination of factors. In diabetic ketoaci-
4 898 XIV. THE GENITOURINARY SYSTEM Table Causes of Hypophosphatemia Cellular shift (from ECV to soft tissues and bone) Glucose ingestion or IV infusion High carbohydrate diet Fructose or glycerol administration Insulin administration Total parenteral nutrition (hyperalimentation) Gram-negative bacteremia secondary to hyperventilation Salicylate poisoning secondary to hyperventilation Respiratory alkalosis GI Poor dietary intake Starvation and malnutrition Malabsorption D deficiency Phosphate binders Renal loss Primary hyperparathyroidism Secondary hyperparathyroidism with normal renal function ECV expansion Sodium bicarbonate infusion Diuretic therapy Renal tubular defects (acquired and congenital) Post renal transplantation (persistant secondary hyperparathyroidism) Hypokalemia Hypomagnesemia Abnormalities in vitamin D metabolism Vitamin D-deficient rickets Vitamin D-resistant rickets Vitamin D-dependent rickets Miscellaneous Alcoholism Alcohol withdrawal Pharmacologic phosphate binders Severe burns Nutritional recovery syndromes Severe respiratory alkalosis Source : Adapted with permission from Slatopolsky E, Pathology of calcium, magnesium, and phosphate metabolism. In : Klahr S, ed., The kidney and body fluids in health and disease. New York : Plenum, dosis, initially there is a higher serum phosphate due to the acidosis. With treatment, there is increased urinary excretion along with translocation of phosphate into cells during the administration of insulin and glucose. Hypophosphatemia may be seen in 50% of patients hospitalized with chronic alcoholism. Mechanisms include poor dietary intake, vomiting, diarrhea as well as magnesium deficiency, ketoacidosis, and an effect of ethanol per se. Alcoholic ke- toacidosis probably produces decomposition of intracellular organic phosphate with the release of phosphate, leading to phosphaturia. In severe burns, hypophosphatemia is usually seen from the second to the fifth day after the injury and may persist up to ten days. The mechanism for hypophosphatemia is not known, but may include respiratory alkalosis resulting from gram-negative sepsis, renal phosphate wasting secondary to volume expansion, and in- Figure Clinical approach to hypophosphatemia. (Reproduced with permission from Berkelhammer CA, Bear RA. A clinical approach to common electrolyte problems : 3. Hypophosphatemia. Can Med Assoc J 1984 ; 130 :17-23.)
5 198. SERUM INORGANIC PHOSPHORUS 899 creased calcitonin and catecholamine levels. Similarly, in patients recovering from starvation (nutritional recovery) or maintained on intravenous nutrition, especially if without phosphates, anabolism leads to cellular uptake of phosphate. At times, there may be marked symptomatic hypophosphatemia. Urinary phosphate determination can be a valuable guide in the diagnosis of hypophosphatemia. Kidneys avidly conserve phosphate when hypophosphatemia is present and may produce virtually a phosphate-free urine. Thus, when the serum level of phosphate is very low (1.5 mg/dl or 0.48 mmol/l), increased urinary phosphorus excretion (higher than 3.2 mmol/dl or fractional excretion of 20%) is inappropriate and clearly indicates renal wasting. In contrast, if urinary phosphate is low in the setting of low serum phosphate (i.e., if the urinary phosphate excretion is less than 3.2 mmol/day or the fractional excretion is less than 10%) then nonrenal causes should be investigated. The approach is summarized in Figure The therapy of hypophosphatemia involves recognizing the cause and correcting the underlying condition. Phosphate supplementation is not required for mild to moderate asymptomatic hypophosphatemia. But severe hypophosphatemia (less than l.0 mg/dl) or symptomatic hypophosphatemia requires prompt correction. Phosphate can be replaced by either oral or parenteral administration. Like potassium, phosphate replacement therapy is empiric because total body phosphorus is not determined easily. Periodic checking of the serum phosphate is required during replacement therapy. References Berkelhammer C, Bear RA. A clinical approach to common electrolyte problems : 3. hypophosphatemia. Can Med Assoc J 1984; 130 : Betro MG, Pain RW. Hypophosphatemia and hyperphosphatemia in a hospital population. Br Med J 1972 ;1 : Brautbar N, Kleeman CR. Hypophosphatemia and hyperphosphatemia : clinical and pathophysiologic aspects. In : Maxwell MH, Kleeman CR, Narins RG, eds. Clinical disorders of fluid and electrolyte metabolism. New York: McGraw-Hill, 1987 ; Conner CS. Hypophosphatemia. Drug Intell Clin Pharm 1984 ; 18 : Fitzgerald F. Clinical hypophosphatemia. Annu Rev Med 1978 ; 29 : Knochel JP. The pathophysiology and clinical characteristics of severe hypophosphatemia. Arch Intern Med 1977 ;137 : Narins RG, Jones ER, Stom MC, et al. Diagnostic strategies in disorders of fluid, electrolyte and acid-base homeostasis. Am J Med 1982 ;72 : Slatopolsky E. Pathophysiology of calcium, magnesium, and phosphorus metabolism. In : Klahr S, ed. The kidney and body fluids in health and disease. New York : Plenum Press, 1983 ; Stoff JS. Phosphate homeostasis and hypophosphatemia. Am J Med 1982 ;72 : Vannatta JB, Whang R, Papper S. Efficacy of intravenous phosphorous therapy in severely hypophosphatemic patients. Arch Intern Med 1981 ;141 :
6
CALCIUM BALANCE. James T. McCarthy & Rajiv Kumar
 CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
WATER, SODIUM AND POTASSIUM
 WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
Major intra and extracellular ions Lec: 1
 Major intra and extracellular ions Lec: 1 The body fluids are solutions of inorganic and organic solutes. The concentration balance of the various components is maintained in order for the cell and tissue
Major intra and extracellular ions Lec: 1 The body fluids are solutions of inorganic and organic solutes. The concentration balance of the various components is maintained in order for the cell and tissue
5/18/2017. Specific Electrolytes. Sodium. Sodium. Sodium. Sodium. Sodium
 Specific Electrolytes Hyponatremia Hypervolemic Replacing water (not electrolytes) after perspiration Freshwater near-drowning Syndrome of Inappropriate ADH Secretion (SIADH) Hypovolemic GI disease (decreased
Specific Electrolytes Hyponatremia Hypervolemic Replacing water (not electrolytes) after perspiration Freshwater near-drowning Syndrome of Inappropriate ADH Secretion (SIADH) Hypovolemic GI disease (decreased
SERUM PHOSPHORUS TESTING
 MEDICAL POLICY For use with the UnitedHealthcare Laboratory Benefit Management Program, administered by BeaconLBS SERUM PHOSPHORUS TESTING Policy Number: CMP - 035 Effective Date: January 21, 2017 Table
MEDICAL POLICY For use with the UnitedHealthcare Laboratory Benefit Management Program, administered by BeaconLBS SERUM PHOSPHORUS TESTING Policy Number: CMP - 035 Effective Date: January 21, 2017 Table
BUFFERING OF HYDROGEN LOAD
 BUFFERING OF HYDROGEN LOAD 1. Extracellular space minutes 2. Intracellular space minutes to hours 3. Respiratory compensation 6 to 12 hours 4. Renal compensation hours, up to 2-3 days RENAL HYDROGEN SECRETION
BUFFERING OF HYDROGEN LOAD 1. Extracellular space minutes 2. Intracellular space minutes to hours 3. Respiratory compensation 6 to 12 hours 4. Renal compensation hours, up to 2-3 days RENAL HYDROGEN SECRETION
Instrumental determination of electrolytes in urine. Amal Alamri
 Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Acid-Base Balance 11/18/2011. Regulation of Potassium Balance. Regulation of Potassium Balance. Regulatory Site: Cortical Collecting Ducts.
 Influence of Other Hormones on Sodium Balance Acid-Base Balance Estrogens: Enhance NaCl reabsorption by renal tubules May cause water retention during menstrual cycles Are responsible for edema during
Influence of Other Hormones on Sodium Balance Acid-Base Balance Estrogens: Enhance NaCl reabsorption by renal tubules May cause water retention during menstrual cycles Are responsible for edema during
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance
 Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 20 8/23/2016. Fluids and Electrolytes. Fluid (Water) Fluid (Water) (Cont.) Functions
 Chapter 20 Fluids and Electrolytes All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Fluid (Water) Functions Provides an extracellular transportation
Chapter 20 Fluids and Electrolytes All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Fluid (Water) Functions Provides an extracellular transportation
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 7 Caring for Clients with Altered Fluid, Electrolyte, or Acid-Base Balance Water Primary component of
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 7 Caring for Clients with Altered Fluid, Electrolyte, or Acid-Base Balance Water Primary component of
H 2 O, Electrolytes and Acid-Base Balance
 H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
CHAPTER 27 LECTURE OUTLINE
 CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
Acid Base Balance. Professor Dr. Raid M. H. Al-Salih. Clinical Chemistry Professor Dr. Raid M. H. Al-Salih
 Acid Base Balance 1 HYDROGEN ION CONCENTRATION and CONCEPT OF ph Blood hydrogen ion concentration (abbreviated [H + ]) is maintained within tight limits in health, with the normal concentration being between
Acid Base Balance 1 HYDROGEN ION CONCENTRATION and CONCEPT OF ph Blood hydrogen ion concentration (abbreviated [H + ]) is maintained within tight limits in health, with the normal concentration being between
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE
 Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
David Bruyette, DVM, DACVIM
 VCAwestlaspecialty.com David Bruyette, DVM, DACVIM Disorders of calcium metabolism are common endocrine disorders in both dogs and cats. In this article we present a logical diagnostic approach to patients
VCAwestlaspecialty.com David Bruyette, DVM, DACVIM Disorders of calcium metabolism are common endocrine disorders in both dogs and cats. In this article we present a logical diagnostic approach to patients
Potassium regulation. -Kidney is a major regulator for potassium Homeostasis.
 Potassium regulation. -Kidney is a major regulator for potassium Homeostasis. Normal potassium intake, distribution, and output from the body. Effects of severe hyperkalemia Partial depolarization of cell
Potassium regulation. -Kidney is a major regulator for potassium Homeostasis. Normal potassium intake, distribution, and output from the body. Effects of severe hyperkalemia Partial depolarization of cell
Renal Tubular Acidosis
 1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
Case 4 Generalised bone pain
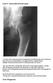 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Prevention of Electrolyte Disorders Refeeding Syndrome พญ.น นทพร เต มพรเล ศ
 Prevention of Electrolyte Disorders Refeeding Syndrome พญ.น นทพร เต มพรเล ศ Outline Refeeding Syndrome What is refeeding syndrome? What Electrolytes and minerals are involved? Who is at risk? How to manage
Prevention of Electrolyte Disorders Refeeding Syndrome พญ.น นทพร เต มพรเล ศ Outline Refeeding Syndrome What is refeeding syndrome? What Electrolytes and minerals are involved? Who is at risk? How to manage
CCRN Review - Renal. CCRN Review - Renal 10/16/2014. CCRN Review Renal. Sodium Critical Value < 120 meq/l > 160 meq/l
 CCRN Review Renal Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Sodium 136-145 Critical Value < 120 meq/l > 160 meq/l Sodium Etiology
CCRN Review Renal Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Sodium 136-145 Critical Value < 120 meq/l > 160 meq/l Sodium Etiology
Acid-base balance is one of the most important of the body s homeostatic mechanisms Acid-base balance refers to regulation of hydrogen ion (H + )
 Acid-base balance is one of the most important of the body s homeostatic mechanisms Acid-base balance refers to regulation of hydrogen ion (H + ) concentration in body fluids Precise regulation of ph at
Acid-base balance is one of the most important of the body s homeostatic mechanisms Acid-base balance refers to regulation of hydrogen ion (H + ) concentration in body fluids Precise regulation of ph at
Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis
 Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis Tutorial for Specialist Portfolio Biomedical Scientists 03/02/2014 Dr Petros Kampanis Clinical Scientist 1. Calcium Most abundant
Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis Tutorial for Specialist Portfolio Biomedical Scientists 03/02/2014 Dr Petros Kampanis Clinical Scientist 1. Calcium Most abundant
RENAL TUBULAR ACIDOSIS An Overview
 RENAL TUBULAR ACIDOSIS An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY CLINICAL BIOCHEMISTRY PBL MBBS IV VJ. Temple 1 What is Renal Tubular
RENAL TUBULAR ACIDOSIS An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY CLINICAL BIOCHEMISTRY PBL MBBS IV VJ. Temple 1 What is Renal Tubular
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
CASE 27. What is the response of the kidney to metabolic acidosis? What is the response of the kidney to a respiratory alkalosis?
 CASE 27 A 21-year-old man with insulin-dependent diabetes presents to the emergency center with mental status changes, nausea, vomiting, abdominal pain, and rapid respirations. On examination, the patient
CASE 27 A 21-year-old man with insulin-dependent diabetes presents to the emergency center with mental status changes, nausea, vomiting, abdominal pain, and rapid respirations. On examination, the patient
BIO132 Chapter 27 Fluid, Electrolyte and Acid Base Balance Lecture Outline
 BIO132 Chapter 27 Fluid, Electrolyte and Acid Base Balance Lecture Outline Fluid divisions 1. Extracellular fluid (ECF) 2. Intracellular fluid (ICF) Stabilization 1. Fluid balance 2. Electrolyte balance
BIO132 Chapter 27 Fluid, Electrolyte and Acid Base Balance Lecture Outline Fluid divisions 1. Extracellular fluid (ECF) 2. Intracellular fluid (ICF) Stabilization 1. Fluid balance 2. Electrolyte balance
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Acid-Base Balance Dr. Gary Mumaugh
 Acid-Base Balance Dr. Gary Mumaugh Introduction Acid-base balance is one of the most important of the body s homeostatic mechanisms Acid-base balance refers to regulation of hydrogen ion (H + ) concentration
Acid-Base Balance Dr. Gary Mumaugh Introduction Acid-base balance is one of the most important of the body s homeostatic mechanisms Acid-base balance refers to regulation of hydrogen ion (H + ) concentration
Chapter 24 Water, Electrolyte and Acid-Base Balance
 Chapter 24 Water, Electrolyte and Acid-Base Balance Total body water for 150 lb. male = 40L 65% ICF 35% ECF 25% tissue fluid 8% blood plasma, lymph 2% transcellular fluid (CSF, synovial fluid) Water Movement
Chapter 24 Water, Electrolyte and Acid-Base Balance Total body water for 150 lb. male = 40L 65% ICF 35% ECF 25% tissue fluid 8% blood plasma, lymph 2% transcellular fluid (CSF, synovial fluid) Water Movement
Body water content. Fluid compartments. Regulation of water output. Water balance and ECF osmolallty. Regulation of water intake
 Body water content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; females 50% This difference reflects
Body water content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; females 50% This difference reflects
Answers and Explanations
 Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
Salicylate (Aspirin) Ingestion California Poison Control Background 1. The prevalence of aspirin-containing analgesic products makes
 Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Hypophosphatemia is an uncommon condition
 HYPOPHOSPHATEMIA AND REFEEDING SYNDROME Nathan Lippo, DVM Resident, Emergency and Critical Care Medicine Christopher G. Byers, DVM, DACVECC Director, Intensive Care Internal Medicine Critical Care Department
HYPOPHOSPHATEMIA AND REFEEDING SYNDROME Nathan Lippo, DVM Resident, Emergency and Critical Care Medicine Christopher G. Byers, DVM, DACVECC Director, Intensive Care Internal Medicine Critical Care Department
Calcium (Ca 2+ ) mg/dl
 Quick Guide to Laboratory Values Use this handy cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal values may vary according to techniques used
Quick Guide to Laboratory Values Use this handy cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal values may vary according to techniques used
Water, Electrolytes, and Acid-Base Balance
 Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Chapter 15 Fluid and Acid-Base Balance
 Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 16 Nutrition, Fluids and Electrolytes, and Acid-Base Balance Nutrition Nutrients Water o Functions Promotes metabolic processes Transporter
 Chapter 16 Nutrition, Fluids and Electrolytes, and Acid-Base Balance Nutrition Nutrients Water o Functions Promotes metabolic processes Transporter for nutrients and wastes Lubricant Insulator and shock
Chapter 16 Nutrition, Fluids and Electrolytes, and Acid-Base Balance Nutrition Nutrients Water o Functions Promotes metabolic processes Transporter for nutrients and wastes Lubricant Insulator and shock
UNIT VI: ACID BASE IMBALANCE
 UNIT VI: ACID BASE IMBALANCE 1 Objectives: Review the physiological mechanism responsible to regulate acid base balance in the body i.e.: Buffers (phosphate, hemoglobin, carbonate) Renal mechanism Respiratory
UNIT VI: ACID BASE IMBALANCE 1 Objectives: Review the physiological mechanism responsible to regulate acid base balance in the body i.e.: Buffers (phosphate, hemoglobin, carbonate) Renal mechanism Respiratory
3/19/2009. The task of the kidney in acid-base balance Excretion of the daily acid load. Buffering of an acid load. A o B - + H + B - A o +OH - C +
 The task of the kidney in acid-base balance Excretion of the daily acid load Buffering of an acid load Oxidation of amino acids, fats and carbohydrates often lead to acid production. On an average American
The task of the kidney in acid-base balance Excretion of the daily acid load Buffering of an acid load Oxidation of amino acids, fats and carbohydrates often lead to acid production. On an average American
D fini n tion: p = = -log [H+] ph=7 me m an s 10-7 Mol M H+ + (100 nmol m /l); ) p ; H=8 me m an s 10-8 Mol M H+ + (10 (10 n nmol m /l) Nor
![D fini n tion: p = = -log [H+] ph=7 me m an s 10-7 Mol M H+ + (100 nmol m /l); ) p ; H=8 me m an s 10-8 Mol M H+ + (10 (10 n nmol m /l) Nor D fini n tion: p = = -log [H+] ph=7 me m an s 10-7 Mol M H+ + (100 nmol m /l); ) p ; H=8 me m an s 10-8 Mol M H+ + (10 (10 n nmol m /l) Nor](/thumbs/75/72756397.jpg) Definition: ph regulation ph = -log [H + ] ph=7 means 10-7 Mol H + (100 nmol/l); ph=8 means 10 Normal plasma value: 7.35-7.45; 7.45; (H Acidosis: ph7.45 Intracellular ph = 7.1-7.3
Definition: ph regulation ph = -log [H + ] ph=7 means 10-7 Mol H + (100 nmol/l); ph=8 means 10 Normal plasma value: 7.35-7.45; 7.45; (H Acidosis: ph7.45 Intracellular ph = 7.1-7.3
Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES
 Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES Body Water Content Water Balance: Normal 2500 2000 1500 1000 500 Metab Food Fluids Stool Breath Sweat Urine
Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES Body Water Content Water Balance: Normal 2500 2000 1500 1000 500 Metab Food Fluids Stool Breath Sweat Urine
Chapter 2. Fluid, Electrolyte, and Acid-Base Imbalances
 Chapter 2 Fluid, Electrolyte, and Acid-Base Imbalances Review of Concepts and Processes The major component of the body is water. Water is located in these compartments: Intracellular fluid (ICF) compartment
Chapter 2 Fluid, Electrolyte, and Acid-Base Imbalances Review of Concepts and Processes The major component of the body is water. Water is located in these compartments: Intracellular fluid (ICF) compartment
Amani Alghamdi. Slide 1
 Minerals in the body Amani Alghamdi Slide 1 The Minerals Small, naturally occurring, inorganic, chemical elements Serve as structural components Minerals classification The minerals present in the body
Minerals in the body Amani Alghamdi Slide 1 The Minerals Small, naturally occurring, inorganic, chemical elements Serve as structural components Minerals classification The minerals present in the body
Acid and Base Balance
 Acid and Base Balance 1 2 The Body and ph Homeostasis of ph is tightly controlled Extracellular fluid = 7.4 Blood = 7.35 7.45 < 7.35: Acidosis (acidemia) > 7.45: Alkalosis (alkalemia) < 6.8 or > 8.0: death
Acid and Base Balance 1 2 The Body and ph Homeostasis of ph is tightly controlled Extracellular fluid = 7.4 Blood = 7.35 7.45 < 7.35: Acidosis (acidemia) > 7.45: Alkalosis (alkalemia) < 6.8 or > 8.0: death
Part 1 The Cell and the Cellular Environment
 1 Chapter 3 Anatomy and Physiology Part 1 The Cell and the Cellular Environment 2 The Human Cell The is the fundamental unit of the human body. Cells contain all the necessary for life functions. 3 Cell
1 Chapter 3 Anatomy and Physiology Part 1 The Cell and the Cellular Environment 2 The Human Cell The is the fundamental unit of the human body. Cells contain all the necessary for life functions. 3 Cell
Fluid and Electrolytes P A R T 4
 Fluid and Electrolytes P A R T 4 Mechanisms that control acid-base homeostasis Acids and bases continually enter and leave body Hydrogen ions also result from metabolic activity Acids Hydrogen ion donors
Fluid and Electrolytes P A R T 4 Mechanisms that control acid-base homeostasis Acids and bases continually enter and leave body Hydrogen ions also result from metabolic activity Acids Hydrogen ion donors
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS
 Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Acid - base equilibrium
 Acid base equilibrium ph concept ph = log [H + ] ph [H+] 1 100 mmol/l D = 90 mmol/l 2 10 mmol/l D = 9 mmol/l 3 1 mmol/l 2 ph = log [H + ] 3 ph ph = log [H + ] ph of capillary blood norm: 7,35 7,45 Sorensen
Acid base equilibrium ph concept ph = log [H + ] ph [H+] 1 100 mmol/l D = 90 mmol/l 2 10 mmol/l D = 9 mmol/l 3 1 mmol/l 2 ph = log [H + ] 3 ph ph = log [H + ] ph of capillary blood norm: 7,35 7,45 Sorensen
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are
 Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION
 DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
ELECTROLYTES RENAL SHO TEACHING
 ELECTROLYTES RENAL SHO TEACHING Metabolic Alkalosis 2 factors are responsible for generation and maintenance of metabolic alkalosis this includes a process that raises serum bicarbonate and a process that
ELECTROLYTES RENAL SHO TEACHING Metabolic Alkalosis 2 factors are responsible for generation and maintenance of metabolic alkalosis this includes a process that raises serum bicarbonate and a process that
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Acid Base Balance. Chapter 26 Balance. ph Imbalances. Acid Base Balance. CO 2 and ph. Carbonic Acid. Part 2. Acid/Base Balance
 Acid Base Balance Chapter 26 Balance Part 2. Acid/Base Balance Precisely balances production and loss of hydrogen ions (ph) The body generates acids during normal metabolism, tends to reduce ph Kidneys:
Acid Base Balance Chapter 26 Balance Part 2. Acid/Base Balance Precisely balances production and loss of hydrogen ions (ph) The body generates acids during normal metabolism, tends to reduce ph Kidneys:
Draft Labeling Package Insert Not Actual Size. BRAINTREE LABORATORIES, INC. PhosLo Capsules (Calcium Acetate)
 Draft Labeling Package Insert Not Actual Size BRAINTREE LABORATORIES, INC. PhosLo Capsules (Calcium Acetate) DESCRIPTION: Full Size: Each opaque capsule with a white cap and white body is spin printed
Draft Labeling Package Insert Not Actual Size BRAINTREE LABORATORIES, INC. PhosLo Capsules (Calcium Acetate) DESCRIPTION: Full Size: Each opaque capsule with a white cap and white body is spin printed
Biochemistry of acid-base disorders. Alice Skoumalová
 Biochemistry of acid-base disorders Alice Skoumalová Main topics of the lecture: Measurement of acid-base dysbalance Classification of the acid-base disorders 4 basic acid-base disorders and their compensaiton
Biochemistry of acid-base disorders Alice Skoumalová Main topics of the lecture: Measurement of acid-base dysbalance Classification of the acid-base disorders 4 basic acid-base disorders and their compensaiton
Nutritional Demands of Disease and Trauma
 al Demands of Disease and Trauma Lecture 89 Medical School al Requirements Based on needs to support optimal physiological function Are changed by disease or injury metabolism is altered to prevent further
al Demands of Disease and Trauma Lecture 89 Medical School al Requirements Based on needs to support optimal physiological function Are changed by disease or injury metabolism is altered to prevent further
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
HIHIM 409 7/26/2009. Kidney and Nephron. Fermamdo Vega, M.D. 1
 Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Non-Protein Nitrogenous Compounds. Non-Protein Nitrogenous Compounds. NPN s. Urea (BUN) Creatinine NH 3. University of Cincinnati MLS Program 1
 Non-Protein Nitrogenous Compounds NPN s Urea (BUN) Creatinine NH 3 Uric Acid Ammonia University of Cincinnati MLS Program 1 Urea Metabolic product derived from catabolism of proteins Proteolysis of proteins
Non-Protein Nitrogenous Compounds NPN s Urea (BUN) Creatinine NH 3 Uric Acid Ammonia University of Cincinnati MLS Program 1 Urea Metabolic product derived from catabolism of proteins Proteolysis of proteins
RENAL FUNCTION An Overview
 RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
PRINCIPLES OF DIURETIC ACTIONS:
 DIURETIC: A drug that increases excretion of solutes Increased urine volume is secondary All clinically useful diuretics act by blocking Na + reabsorption Has the highest EC to IC ratio = always more sodium
DIURETIC: A drug that increases excretion of solutes Increased urine volume is secondary All clinically useful diuretics act by blocking Na + reabsorption Has the highest EC to IC ratio = always more sodium
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Fluid, Electrolyte, and Acid Base Balance
 25 Fluid, Electrolyte, and Acid Base Balance Lecture Presentation by Lori Garrett Note to the Instructor: For the third edition of Visual Anatomy & Physiology, we have updated our PowerPoints to fully
25 Fluid, Electrolyte, and Acid Base Balance Lecture Presentation by Lori Garrett Note to the Instructor: For the third edition of Visual Anatomy & Physiology, we have updated our PowerPoints to fully
NHS Grampian Staff Guideline For The Management Of Acute Hypophosphataemia In Adults
 NHS Grampian Staff Guideline For The Management Of Acute Hypophosphataemia In Adults Co-ordinators: Medicine Information Pharmacist Consultation Group: See Page 5 Approver: Medicine Guidelines and Policies
NHS Grampian Staff Guideline For The Management Of Acute Hypophosphataemia In Adults Co-ordinators: Medicine Information Pharmacist Consultation Group: See Page 5 Approver: Medicine Guidelines and Policies
Acids and Bases their definitions and meanings
 Acids and Bases their definitions and meanings Molecules containing hydrogen atoms that can release hydrogen ions in solutions are referred to as acids. (HCl H + Cl ) (H 2 CO 3 H + HCO 3 ) A base is an
Acids and Bases their definitions and meanings Molecules containing hydrogen atoms that can release hydrogen ions in solutions are referred to as acids. (HCl H + Cl ) (H 2 CO 3 H + HCO 3 ) A base is an
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology
 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Urinary Calculus Disease. Urinary Stones: Simplified Metabolic Evaluation. Urinary Calculus Disease. Urinary Calculus Disease 2/8/2008
 Urinary Stones: Simplified Metabolic Evaluation Marshall L. Stoller, M.D. Professor and Vice Chairman Department of Urology University of California San Francisco Incidence: 7-21/10,000 3 men: 1 woman
Urinary Stones: Simplified Metabolic Evaluation Marshall L. Stoller, M.D. Professor and Vice Chairman Department of Urology University of California San Francisco Incidence: 7-21/10,000 3 men: 1 woman
Acid/Base Balance. the concentrations of these two ions affect the acidity or alkalinity of body fluids
 Acid/Base Balance some of most critical ions in body fluids are H + (hydrogen) and OH - (hydroxyl) ions the concentrations of these two ions affect the acidity or alkalinity of body fluids acidity/alkalinity
Acid/Base Balance some of most critical ions in body fluids are H + (hydrogen) and OH - (hydroxyl) ions the concentrations of these two ions affect the acidity or alkalinity of body fluids acidity/alkalinity
12/7/10. Excretory System. The basic function of the excretory system is to regulate the volume and composition of body fluids by:
 Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Diuretic Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Water in the Body. Page Water = ~50 to 70% of body weight, depending on body fat % (higher body fat=lower water content)
 Water in the Body Page 373-375 Water = ~50 to 70% of body weight, depending on body fat % (higher body fat=lower water content) Major fluid compartments: Intracellular fluid: cytoplasm of cells is an aqueous
Water in the Body Page 373-375 Water = ~50 to 70% of body weight, depending on body fat % (higher body fat=lower water content) Major fluid compartments: Intracellular fluid: cytoplasm of cells is an aqueous
Renal Control of Calcium, Phosphate, and Magnesium Homeostasis
 Renal Physiology Renal Control of Calcium, Phosphate, and Magnesium Homeostasis Judith Blaine, Michel Chonchol, and Moshe Levi Abstract Calcium, phosphate, and magnesium are multivalent cations that are
Renal Physiology Renal Control of Calcium, Phosphate, and Magnesium Homeostasis Judith Blaine, Michel Chonchol, and Moshe Levi Abstract Calcium, phosphate, and magnesium are multivalent cations that are
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University
 RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Na concentration in the extracellular compartment is 140
 هللامسب Na regulation: Na concentration in the extracellular compartment is 140 meq\l. Na is important because: -It determines the volume of extracellular fluid : the more Na intake will expand extracellular
هللامسب Na regulation: Na concentration in the extracellular compartment is 140 meq\l. Na is important because: -It determines the volume of extracellular fluid : the more Na intake will expand extracellular
Introduction. Acids, Bases and ph; a review
 0 P a g e Introduction In this sheet, we discuss acidbase balance in our body and the role of kidneys in its establishment. Arrangement of topics is different from that of the lecture, to assure consistency
0 P a g e Introduction In this sheet, we discuss acidbase balance in our body and the role of kidneys in its establishment. Arrangement of topics is different from that of the lecture, to assure consistency
ACID-BASE BALANCE URINE BLOOD AIR
 ACIDBASE BALANCE URINE BLOOD AIR H 2 PO 4 NH 4 HCO 3 KIDNEY H H HCO 3 CELLS Hb H LUNG H 2 CO 3 HHb CO 2 H 2 O ph = 7.4 [HCO 3 ] = 24 meq/l PCO 2 = 40 mm Hg CO 2 PRIMARY RENAL MECHANISMS INVOLVED IN ACIDBASE
ACIDBASE BALANCE URINE BLOOD AIR H 2 PO 4 NH 4 HCO 3 KIDNEY H H HCO 3 CELLS Hb H LUNG H 2 CO 3 HHb CO 2 H 2 O ph = 7.4 [HCO 3 ] = 24 meq/l PCO 2 = 40 mm Hg CO 2 PRIMARY RENAL MECHANISMS INVOLVED IN ACIDBASE
Renal Physiology. April, J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine.
 Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
11/05/1431. Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate
 Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Adaptation and re-feeding Hypokalemia Bone complications
 Adaptation and re-feeding Hypokalemia Bone complications René Klinkby Støving Odense University Hospital Denmark 10% 20% 30% 40% BMI 18.5 BMI 16.5 BMI 14.5 BMI 12.5 Willmore DW, The Metabolic Management
Adaptation and re-feeding Hypokalemia Bone complications René Klinkby Støving Odense University Hospital Denmark 10% 20% 30% 40% BMI 18.5 BMI 16.5 BMI 14.5 BMI 12.5 Willmore DW, The Metabolic Management
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
1. 09/07/16 Ch 1: Intro to Human A & P 1
 Table of Contents # Date Title Page # 1. 09/07/16 Ch 1: Intro to Human A & P 1 2. 09/19/16 Ch 18: Water, Electrolyte, and Acid-Base Balance 5 i 1 09/19/16 Chapter 18: Water, Electrolyte, and Acid-Base
Table of Contents # Date Title Page # 1. 09/07/16 Ch 1: Intro to Human A & P 1 2. 09/19/16 Ch 18: Water, Electrolyte, and Acid-Base Balance 5 i 1 09/19/16 Chapter 18: Water, Electrolyte, and Acid-Base
BIOL 2402 Renal Function
 BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
What location in the gastrointestinal (GI) tract has tight, or impermeable, junctions between the epithelial cells?
 CASE 32 A 17-year-old boy presents to his primary care physician with complaints of diarrhea for the last 2 days. The patient states that he just returned to the United States after visiting relatives
CASE 32 A 17-year-old boy presents to his primary care physician with complaints of diarrhea for the last 2 days. The patient states that he just returned to the United States after visiting relatives
POTASSIUM DIHYDROGEN PHOSPHATE 13.6% CONCENTRATED INJECTION
 POTASSIUM DIHYDROGEN PHOSPHATE 13.6% CONCENTRATED INJECTION NAME OF THE MEDICINE Potassium Dihydrogen Phosphate Synonyms: potassium biphosphate, potassium acid phosphate, monopotassium phosphate, or monoibasic
POTASSIUM DIHYDROGEN PHOSPHATE 13.6% CONCENTRATED INJECTION NAME OF THE MEDICINE Potassium Dihydrogen Phosphate Synonyms: potassium biphosphate, potassium acid phosphate, monopotassium phosphate, or monoibasic
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Hypoglycemia, Electrolyte disturbances and acid-base imbalances
 Hypoglycemia, Electrolyte disturbances and acid-base imbalances Pediatric emergency PICU division Pediatric department Medical faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Hypoglycemia
Hypoglycemia, Electrolyte disturbances and acid-base imbalances Pediatric emergency PICU division Pediatric department Medical faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Hypoglycemia
REGULATION OF CALCIUM AND PHOSPHATE HOMEOSTASIS
 REGULATION OF CALCIUM AND PHOSPHATE HOMEOSTASIS Linda S. Costanzo Virginia Commonwealth University, Medical College of Virginia, Richmond, Virginia 23298 Teaching Ca 2 and phosphate homeostasis in a physiology
REGULATION OF CALCIUM AND PHOSPHATE HOMEOSTASIS Linda S. Costanzo Virginia Commonwealth University, Medical College of Virginia, Richmond, Virginia 23298 Teaching Ca 2 and phosphate homeostasis in a physiology
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Acid-Base Tutorial 2/10/2014. Overview. Physiology (2) Physiology (1)
 Overview Acid-Base Tutorial Nicola Barlow Physiology Buffering systems Control mechanisms Laboratory assessment of acid-base Disorders of H + ion homeostasis Respiratory acidosis Metabolic acidosis Respiratory
Overview Acid-Base Tutorial Nicola Barlow Physiology Buffering systems Control mechanisms Laboratory assessment of acid-base Disorders of H + ion homeostasis Respiratory acidosis Metabolic acidosis Respiratory
Electrolyte Imbalance and Resuscitation. Dr. Mehmet Okumuş Sütçü Imam University Faculty of Medicine Department of Emergency Medicine
 Electrolyte Imbalance and Resuscitation Dr. Mehmet Okumuş Sütçü Imam University Faculty of Medicine Department of Emergency Medicine Presentation plan Definition of the electrolyte disturbances Conditions
Electrolyte Imbalance and Resuscitation Dr. Mehmet Okumuş Sütçü Imam University Faculty of Medicine Department of Emergency Medicine Presentation plan Definition of the electrolyte disturbances Conditions
Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD
 Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD Reprinted with permission from: E-Medicine: Instant Access to the Minds of Medicine http://www.emedicine.com/emerg/topic276.htm
Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD Reprinted with permission from: E-Medicine: Instant Access to the Minds of Medicine http://www.emedicine.com/emerg/topic276.htm
