The medial side of the knee has been relatively overlooked
|
|
|
- Mariah Young
- 5 years ago
- Views:
Transcription
1 REVIEW ARTICLE Medial and Posteromedial Instability of the Knee: Evaluation, Treatment, and Results James P. Stannard, MD Abstract: Medial-sided knee ligament injuries are complex and require a thorough understanding of the anatomy and the scope of injury to successfully treat. Patients with isolated medical collateral ligament (MCL) tears can normally be treated with bracing followed by physical therapy with outstanding results. Patients with isolated Grade III injuries to the MCL are controversial. A reason for the disparity in results reported may be due to the fact that many (if not most) Grade III MCL tears have associated injuries to the anterior cruciate ligament and/or posteromedial corner injury. Patients with combination injuries should be treated surgically with repair or reconstruction in most cases. Either allograft or autograft reconstructions of both the MCL and posteromedial corner can be successful. Successful elimination of anteromedial rotary instability is the key to successfully treating posteromedial corner injuries. Key Words: medial collateral ligament, posteromedial corner injury, multi-ligament knee injury, autograft reconstruction, allograft reconstruction, anteromedial rotary instability (Sports Med Arthrosc Rev 2010;18: ) The medial side of the knee has been relatively overlooked compared with the central pivot and the lateral side. It has also been the source of a moderate amount of controversy regarding the appropriate treatment of medial instability. It is critical to distinguish between a pure medial injury in the form of a torn medial collateral ligament (MCL) and a posteromedial corner (PMC) injury that also has a rotatory component to the instability. It is also crucial to determine if the patient has an isolated injury to the MCL or whether the medial ligament injury is a component of a multi-ligament knee injury (MLKI). The MCL is the most commonly injured ligament in the knee, and has the greatest healing potential of any ligament in the knee. 1 It is the primary medial stabilizer against valgus stress, and along with the PMC provides resistance to external rotation forces applied to the lower leg. 2 A thorough understanding of a medial knee injury requires a clear understanding of the anatomy. ANATOMY There are 2 major systems that have been proposed for describing the anatomy of the medial side of the knee. Warren and coauthors described the anatomy using a From the Department of Orthopaedic Surgery, University of Missouri School of Medicine, One Hospital Drive, Columbia, MO. Reprints: James P. Stannard, MD, Department of Orthopaedic Surgery, University of Missouri School of Medicine, One Hospital Drive, 213 McHaney; DC053.00, Columbia, MO ( stannardj@health.missouri.edu). Copyright r 2010 by Lippincott Williams & Wilkins 3-layer system. 2 An alternative scheme evaluates the structures of the PMC by dividing the medial side into thirds: anterior; middle; and posterior. 3,4 Both systems have advantages and should be understood, but the system of Robinson et al 4 that divides the medial side into thirds is more clinically relevant. The anterior third of the knee consists of capsular ligaments covered by the extensor retinaculum of the quadriceps. 3 It is by far the least important third of the medial part of the knee. The middle third has a layer of fascia, the superficial MCL and the deep MCL. 4 The posterior third has the structures that make up the PMC. This includes a layer of fascia, the posterior oblique ligament (POL), the oblique popliteal ligament, the semimembranous attachments, and the posteromedial meniscus. 3 6 The middle third has a more prominent role of stability against valgus stress, whereas the posterior third has a greater role in resisting anteromedial rotary instability (AMRI). The layered approach describing the anatomy of the medial side of the knee originated with Warren et al 2 and has been presented by many others. 3,4,7 Layer I is composed of the crural fascia, which blends with the tendons of the pes anserinus and tibial periosteum distally. It covers the Sartorius and Quadriceps muscles proximally. Layer II includes the superficial MCL; the medial patellofemoral ligament; and the ligaments of the PMC (merges with layer III at this point). Layer III consists of the capsule of the knee joint, the deep MCL, and the ligaments of the PMC. The conjoined tissues of layers II and III form the PMC. Figure 1 is an axial drawing demonstrating the layered concept of anatomy around the knee. The PMC has been referred to by Muller as the semimembranosus corner of the knee. 3 It plays a role in dynamic stabilization and reinforces the PMC. The semimembranosus has 5 expansions or insertions. They are: (1) the anterior arm, which passes anteriorly beneath the MCL and inserts onto the tibia; (2) the direct arm, which inserts onto the posteromedial tibia; (3) an oblique popliteal ligament arm; (4) a capsular arm with an expansion to the POL; and (5) an inferior arm with a popliteus aponeurosis expansion. 3 The major insertions onto the tibia are important for knee stability and must be replicated to achieve optimal reconstruction results. Selective sectioning cadaveric studies have helped elucidate the role of various structures on the PMC. The posteromedial capsule and POL help control valgus, internal rotation, and posterior drawer in extension. The superficial MCL resisted valgus stress at all angles of flexion and was the dominant structure from 30 to 90 degrees of flexion. It also resists internal rotation in flexion. The deep MCL controlled tibial anterior drawer of the flexed and externally rotated knee and was also a secondary restraint to valgus stress. 8 Cadaveric studies have also demonstrated Sports Med Arthrosc Rev Volume 18, Number 4, December
2 Stannard Sports Med Arthrosc Rev Volume 18, Number 4, December 2010 that the POL and posteromedial capsule have a significant role in the prevention of additional posterior translation in a posterior cruciate ligament (PCL)-deficient knee. 6 This role makes a functional PMC particularly important in the MLKI patient who is undergoing PCL reconstruction. An unstable PMC will place high stress on the reconstructed PCL, increasing the risk of failure. EVALUATION Physical Examination The history of the injury and a good examination of the medial side of the knee remain the most valuable diagnostic tools when evaluating patients with medial knee injuries. Most low-grade sprains occur as noncontact injuries, whereas complete MCL disruptions often result from a direct blow to the lateral leg. These pure valgus forces result in an isolated MCL injury. 1 The addition of external rotation forces to the tibia expands the zone of injury to include the PMC and/or the anterior cruciate ligament. 9 The likelihood of injury to multiple structures within the knee rises with high energy injuries such as involvement in a motor vehicle collision. The index of suspicion for an MLKI or PMC tear should be high in patients involved in high energy injuries. A thorough physical examination of the knee involves careful assessment of the skin for degree of soft tissue injury, palpation of the anatomic structures, assessment of knee motion, and tests for joint stability. 3 There are several important principles that must be followed to obtain a good physical examination of the medial side of an injured knee. First, the patient must be relaxed as muscle spasm and guarding may yield an inaccurate examination. Second, the contralateral limb should be used for side-to-side comparisons. Third, a thorough examination must be conducted looking for associated pathology. 1 It is very important to document the neurologic and vascular status of the limb. This last point becomes even more important in patients who have sustained high energy injuries. Initially, the examiner must establish that the neurologic and vascular examinations of the extremity are normal. This is critical if the patient has an MLKI, as two-thirds of the knee dislocation patients present with the knee reduced. 10 If there is any abnormality in the vascular examination, a vascular consultation and additional diagnostic studies should be performed immediately. 11 After this, a careful examination of the knee for point tenderness can provide important information regarding the precise location of the injury. Hughston et al found that point tenderness enabled them to localize the site of the injury in 78% of cases. 12 Valgus stress testing with the knee in full extension and 30 degrees of flexion is the most important test of the stability of the medial side of the knee. To perform the test, the patient should be supine and the examiner should grasp the foot while applying a valgus stress to the knee (Fig. 2). This maneuver with the knee in 30 degrees of flexion helps isolate the medial side of the knee. It is important to try to differentiate between an isolated MCL injury and an AMRI pattern that includes the PMC. The difference is an isolated valgus laxity compared with valgus laxity coupled with anterior rotatory subluxation of the medial tibial plateau on the medial femoral condyle. The difference is easier to appreciate when the examination is performed while holding the limb by the foot rather than the distal portion FIGURE 1. An axial drawing of the anatomy of the knee. Reprinted with permission from Thieme Medical Publishers Inc, of the leg. 3,13 The difference between the 2, however, cannot always be determined on the valgus stress examination. Instability in full extension implies that there is a tear of the MCL as well as in 1 or both of the cruciate ligaments. 1 Sims and Jacobson documented that anterior cruciate ligament tears occurred in 78% of Grade III ACL tears. 13 Perhaps the most useful test to differentiate between an isolated MCL injury and a PMC injury is the anterior drawer test performed with the foot in external rotation. 1,3,13,14 The examiner should evaluate for anterior subluxation of the medial tibial plateau from under the medial femoral condyle while the foot is internally rotated 10 to 15 degrees. The presence of anterior subluxation of the medial tibial plateau from under the femoral condyle is diagnostic of a PMC injury. It is very important to evaluate your patient for AMRI and to document the results. Sims and Jacobson found that 99% of their patients with a medial-sided injury that required surgical treatment had AMRI and a POL injury. 13 FIGURE 2. Valgus stress testing of a patient with a posteromedial corner injury. Note the examiner is holding the patient s foot with his hand, allowing a better appreciation of any rotatory instability r 2010 Lippincott Williams & Wilkins
3 Sports Med Arthrosc Rev Volume 18, Number 4, December 2010 Medial and Posteromedial Instability of the Knee FIGURE 3. Algorithm for treatment of patients with medial instability of the knee. FIGURE 4. Patient positioned supine with the knee in a figure 4 position for reconstruction of the posteromedial corner. Imaging Studies All patients should have plain radiographs taken in orthogonal planes to evaluate for fractures, avulsions, or a dislocation. Stress radiographs are occasionally helpful, particularly in pediatric patients to help distinguish between physeal and ligament injuries. Magnetic resonance imaging is the imaging study of choice to evaluate the MCL and the PMC. A cadaveric study demonstrated that T1-weighted fat-saturated sequences acquired after injection of intraarticular contrast demonstrated the best visualization of the POL and posteromedial capsule. However, most surgeons do not obtain magnetic resonance imaging scans with contrast. Noncontrast T1 coronal images showed the course of the MCL and segmental visualization of the oblique course of the POL, but poor visualization of the semimembranosus attachments. Axial images provide visualization of the MCL, POL, and the semimembranosus attachments, 15 and are the images that are most helpful to evaluate the PMC. It is important to realize that magnetic resonance images obtained in general practice may not have the resolution to routinely elucidate the full extent of the injury to the posteromedial structures. Physical examination remains the cornerstone of diagnosis of these injuries. r 2010 Lippincott Williams & Wilkins 265
4 Stannard Sports Med Arthrosc Rev Volume 18, Number 4, December 2010 FIGURE 5. Fluoroscopic technique for finding the isometric point on the medial side of the knee. A line is drawn from the anterior aspect of the posterior femoral cortex to Blumensaat line. Reprinted with permission from Thieme Medical Publishers Inc, TREATMENT Nonoperative Of the 4 major ligaments in the knee, the MCL, as a result of its anatomic and biologic properties, has the greatest capacity for healing. 16 Because of these properties, nonoperative treatment is recommended for most of the Grade I and II isolated tears of the MCL. Treatment in a hinged knee brace for 3 to 6 weeks with rehabilitation yields good results in most cases. 1,3 However, the treatment of isolated Grade III injuries is more controversial. Initially, many authors recommended surgical treatment of isolated Grade III MCL tears. 1,3 More recently, several authors have reported good results with nonoperative management of isolated MCL tears. 17,18 Kannus published a study with 9-year follow-up of patients with MCL tears. He noted that patients with Grade I and II injuries did well, but patients with Grade III injuries did not have good results. This study was not limited to athletes. Patients experienced multiple reinjuries to their knee, 22% had to change occupations because of their knee, and 63% had to decrease their level of physical activity as a result of their knee injury. The mean Lysholm score in patients with long-term follow-up of Grade III injuries was only 66. He noted that many of his Grade III patients had either ACL instability or AMRI. His conclusion was that nonoperative treatment was ideal for Grade I and II MCL tears, but that it was not an appropriate choice for patients with Grade III tears. 19 Combined ACL/MCL tears represent a completely different injury than isolated tears, and their treatment is quite controversial. Some authors advocate nonoperative treatment of the MCL initially with combination ACL/ MCL tears. 1,3,20 After brace treatment of the MCL, the ACL is reconstructed if medial stability has been restored. If the patient remains unstable medially, then both the ACL FIGURE 6. Drawing of the autograft technique of posteromedial corner reconstruction. Reprinted with permission from Thieme Medical Publishers Inc, and MCL are reconstructed. Biomechanical studies indicate that the 2 ligaments share responsibilities to an extent. The ACL is the primary restraint to anterior translation, and acts as a secondary restraint to valgus stress. On the other hand, the MCL is the primary restraint to valgus stress at 30 degrees, whereas the POL, the posteromedial capsule, and the posterior horn of the medial meniscus all act as secondary restraints to anterior instability. 21 Whether the MCL is treated operatively or nonoperatively, it is important that medial stability is restored for optimal function of the knee. There is a current trend toward nonoperative care of the MCL initially, but medial stability must be restored to achieve good results. 19 When MCL tears are combined with other ligament injuries or with injuries to the structures of the PMC, surgical treatment is necessary. Failure to achieve PMC stability will lead to failure of the MCL repair or reconstruction in many cases. The same is true for patients with a torn PCL and posterior instability. My algorithm for treatment of patients with medial instability is depicted in Figure 3. Operative Many techniques have been proposed for repair or reconstruction of the MCL and/or PMC. 1,3,14,22 If repair is r 2010 Lippincott Williams & Wilkins
5 Sports Med Arthrosc Rev Volume 18, Number 4, December 2010 Medial and Posteromedial Instability of the Knee undertaken, it is very important to understand the anatomy of the medial side of the knee and to repair all structures that are torn. The PMC was torn in 99% (92/93) of operatively treated medial knee ligament injuries in the experience of Sims and Jacobson. 13 Failure to address PMC injuries or anterior instability leads to poor outcomes in most patients. 19 Kim et al 22 have published a technique that provides a concomitant reconstruction of both PMC and MCL using semitendinosus autograft. They reported excellent results in 24 knees with minimum 2 years of follow-up using stress radiographs and the Lysholm knee score. Stannard 23 reported on the results of repair versus reconstruction of the PMC in patients who had sustained a knee dislocation. He noted significantly better results in patients treated with a reconstruction (4% failure) when compared with patients treated with a repair (20% failure). On the basis of these results, I recommend reconstruction of the MCL/PMC in patients who have sustained a knee dislocation and have medial instability. Surgical Technique: Autograft Reconstruction My preferred autograft reconstruction is based on the technique reported by Kim et al. 22 The patient is placed supine, the hip is externally rotated, and the knee flexed for the majority of the operation. This figure four position allows easy access to the posteromedial part of the knee (Fig. 4). The posteromedial border of the tibia is palpated, and a straight incision is made from the level of the insertion of the pes anserinus tendons to the medial femoral condyle. A fluoroscope is then brought into the surgical field and a good lateral view of the knee and distal femur is obtained. The isometric point is determined by the intersection of a line drawn down the anterior aspect of the posterior femoral cortex and Blumensaat line (Fig. 5). A 3.2-mm drill is placed at the isometric point and the drill is directed approximately 30 degrees proximally and 30 degrees anteriorly to avoid interference with tunnels for ACL, PCL, and posterolateral corner reconstructions in patients with multi-ligament knee injuries. A bicortical 4.5- mm screw and an 18-mm spiked ligament washer are placed at this isometric point and inserted approximately threequarters of the way in. Decortication of the femur is performed for a radius of approximately 6 mm under the washer as described by Kim. 22 The end of the semitendinosus graft is prepared using whip stitching with a strong permanent suture. The graft is then passed around the screw and washer, under the direct head of the semimembranosus tendon, and then back to the intact insertion of the semitendinosus on the tibia. The graft is then tensioned with the knee in approximately 40 degrees of flexion and a slight varus stress. The 4.5-mm screw and washer are then tightened down to the femoral condyle and the graft is sutured back to the insertion of the semitendinosus using a strong permanent suture (Fig. 6). The stability of the PMC is then assessed. If it is not as tight as desired, it can be further tightened by suturing the distal 2 arms of this triangular construct together in a V Y fashion. My results with this technique in knee dislocation patients with a minimum 2-year follow-up were excellent with only a 3.7% failure rate (1/27). Surgical Technique: Allograft Reconstruction Patient positioning and surgical approach are identical to the autograft technique described above. The isometric point is identified using the fluoroscopic technique described above, and a guide pin for a biotenodesis screw (Arthrex Inc, Naples, FL) is drilled into the femoral condyle. A socket is drilled to a depth of 20 mm. Allograft choices are either 1 large tibialis anterior tendon split in half or 2 semitendinosus tendons. The 2 grafts are affixed to the femur using the biotenodesis screw with 1 end emerging in line with the superficial MCL and the other in line with the POL. The 2 grafts are then routed exactly as described in the autograft technique. A 3.2-mm drill bit is used to drill a bicortical screw at the point of insertion of the conjoined tendon of semitendinosus and gracilis. A 4.5-mm screw with a ligament washer is placed into the drill hole and inserted three-quarters of the way into the bone. The knee is then flexed approximately 40 degrees and a slight varus stress is applied. The 2 grafts are passed around the screw in opposite directions and tensioned, and the 4.5-mm screw and washer are tightened securely to the tibia. Results with this technique have also been outstanding, with only a 4.8% failure rate (1/21) in knee dislocation patients with a minimum 2-year follow-up. CONCLUSIONS Medial-sided knee ligament injuries are complex and require a thorough understanding of the anatomy and the scope of injury to successfully treat. Patients with Grade I or II isolated MCL tears can normally be treated with bracing followed by physical therapy with outstanding results. Patients with isolated Grade III injuries to the MCL are controversial. A major reason for the disparity in results reported may be due to the fact that many (if not most) Grade III MCL tears have associated injuries to the ACL and/or PMC. Patients with combination injuries should be treated surgically with repair or reconstruction in most cases. In my practice, I have had very good results with either allograft or autograft reconstructions of both the MCL and PMC. Successful elimination of AMRI is the key to successfully treating PMC injuries. REFERENCES 1. Fanelli GC, Harris JD. Surgical treatment of acute medial collateral ligament and posteromedial corner injuries of the knee. Sports Med Arthrosc Rev. 2006;14: Warren LF, Marshall JL, Girgis FG. The prime static stabilizer of the medial side of the knee. J Bone Joint Surg. 1974;56: Jacobson KE, Chi FS. Evaluation and treatment of medial collateral ligament and medial-sided injuries of the knee. Sports Med Arthrosc Rev. 2006;14: Robinson JR, Sanchez-Ballester J, Bull AM, et al. The posteromedial corner revisited. An anatomical description of the passive restraining structures of the medial aspect of the human knee. J Bone Joint Surg Br. 2004;86: LaPrade RF, Engebresten AH, Ly TV, et al. The anatomy of the medial part of the knee. J Bone Joint Surg Am. 2007;89: Petersen W, Loerch S, Schanz S, et al. The role of the posterior oblique ligament in controlling posterior tibial translation in the posterior cruciate ligament-deficient knee. Am J Sports Med. 2008;36: Epub January 8, Wymenga AB, Kats JJ, Kooloos J, et al. Surgical anatomy of the medial collateral ligament and the posteromedial capsule of the knee. Knee Surg Sports Traumatol Arthrosc. 2006;14: Epub October 26, Robinson JR, Bull AM, Thomas RR, et al. The role of the medial collateral ligament and posteromedial capsule in controlling knee r 2010 Lippincott Williams & Wilkins 267
6 Stannard Sports Med Arthrosc Rev Volume 18, Number 4, December 2010 laxity. Am J Sports Med. 2006;34: Epub June 30, Shapiro MS, Markolf KL, Finerman GA, et al. The effect of section of the medial collateral ligament on force generated in the anterior cruciate ligament. J Bone Joint Surg Am. 1991; 73: Twaddle BC, Bidwell TA, Chapman JR. Knee dislocations: where are the lesions? A prospective evaluation of surgical findings in 63 cases. J Orthop Trauma. 2003;17: Stannard JP, Shiels TM, Lopez-Ben RR, et al. Vascular injuries in knee dislocation following blunt trauma: evaluating the role of physical examination to determining the need for arteriography. J Bone Joint Surg Am. 2004;86-A: Hughston JC, Andrews JR, Cross MJ, et al. Classification of knee ligament instabilities. Part I. The medial compartment and cruciate ligaments. J Bone Joint Surg Am. 1976;58: Sims WF, Jacobson KE. The posteromedial corner of the knee: medial-sided injury patterns revisited. Am J Sports Med. 2004; 32: Benjamin Jackson J III, Ferguson CM, Martin DF. Surgical treatment of chronic posteromedial instability using capsular procedures. Sports Med Arthrosc. 2006;14: Loredo R, Hodler J, Pedowitz R, et al. Posteromedial corner of the knee: MR imaging with gross anatomic correlation. Skeletal Radiol. 1999;28: Woo SL, Inoue M, McGurk-Burleson E, et al. Treatment of the medial collateral ligament injury. II: structure and function of canine knees in response to differing treatment regimens. Am J Sports Med. 1987;15: Hasting DE. The non-operative management of collateral ligament injuries of the knee joint. Clin Orthop Relat Res. 1980;147: Indelicato PA. Non-operative treatment of complete tears of the medial collateral ligament of the knee. J Bone Joint Surg Am. 1983;65: Kannus P. Long-term results of conservatively treated medial collateral ligament injuries of the knee joint. Clin Orthop Relat Res. 1988;226: Halinen J, Lindahl J, Hirvensalo E, et al. Operative and nonoperative treatments of medial collateral ligament rupture with early anterior cruciate ligament reconstruction: a prospective randomized study. Am J Sports Med. 2006;34: Epub February 1, Fischer RA, Arms SW, Johnson RJ, et al. The functional relationship of the posterior oblique ligament to the medial collateral ligament of the human knee. Am J Sports Med. 1985; 13: Kim SJ, Lee DH, Kim TE, et al. Concomitant reconstruction of the medial collateral and posterior oblique ligaments for medial instability of the knee. J Bone Joint Surg Br. 2008; 90: Stannard JP. Posteromedial Corner Injury in Knee Dislocations. Podium Presentation, American Orthopaedic Society for Sports Medicine. 35th Annual Meeting, Keystone, CO, July r 2010 Lippincott Williams & Wilkins
Financial Disclosure. Medial Collateral Ligament
 Matthew Murray, M.D. UTHSCSA Sports Medicine Financial Disclosure Dr. Matthew Murray has no relevant financial relationships with commercial interests to disclose. Medial Collateral Ligament Most commonly
Matthew Murray, M.D. UTHSCSA Sports Medicine Financial Disclosure Dr. Matthew Murray has no relevant financial relationships with commercial interests to disclose. Medial Collateral Ligament Most commonly
MCL Injuries: When and How to Repair Scott D. Mair, MD
 MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
SLARD Symposium: MCL s Injuries
 SLARD Symposium: MCL s Injuries ISAKOS 11 th Biennial Congress Tue June 6 th 2017 13:30 14:15 Shanghai, China Gustavo A. Rincón, MD Chairman Department Orthopedic Surgery Hospital de San José Bogotá -
SLARD Symposium: MCL s Injuries ISAKOS 11 th Biennial Congress Tue June 6 th 2017 13:30 14:15 Shanghai, China Gustavo A. Rincón, MD Chairman Department Orthopedic Surgery Hospital de San José Bogotá -
POSTEROLATERAL CORNER RECONSTRUCTION WHEN AND HOW?
 OTHER KNEE SURGERIES POSTEROLATERAL CORNER RECONSTRUCTION WHEN AND HOW? Written by Jacques Ménétrey, Eric Dromzée and Philippe M. Tscholl, Switzerland Injury of the posterolateral corner (PLC) is relatively
OTHER KNEE SURGERIES POSTEROLATERAL CORNER RECONSTRUCTION WHEN AND HOW? Written by Jacques Ménétrey, Eric Dromzée and Philippe M. Tscholl, Switzerland Injury of the posterolateral corner (PLC) is relatively
Knee Injury Assessment
 Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
Knee Injuries. PSK 4U Mr. S. Kelly North Grenville DHS. Medial Collateral Ligament Sprain
 Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Medial collateral ligament (MCL) injury, is one
 )3( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY EDITORIAL Medial Collateral Ligament Injury; A New Classification Based on MRI and Clinical Findings. A Guide for Patient Selection and Early
)3( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY EDITORIAL Medial Collateral Ligament Injury; A New Classification Based on MRI and Clinical Findings. A Guide for Patient Selection and Early
Ligamentous and Meniscal Injuries: Diagnosis and Management
 Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Knee ligament injuries account for a large percentage of. Evaluation and Treatment of Chronic Medial Collateral Ligament Injuries of the Knee
 REVIEW ARTICLE Evaluation and Treatment of Chronic Medial Collateral Frederick M. Azar, MD Abstract: Injuries to the medial collateral ligament (MCL) can occur as isolated injuries or in conjunction with
REVIEW ARTICLE Evaluation and Treatment of Chronic Medial Collateral Frederick M. Azar, MD Abstract: Injuries to the medial collateral ligament (MCL) can occur as isolated injuries or in conjunction with
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
What s your diagnosis?
 Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Disclosures. Outline. The Posterior Cruciate Ligament 5/3/2016
 The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
Anterior Cruciate Ligament Surgery
 Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES
 HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES Written by Philippe Landreau, Qatar The treatment of anterior cruciate ligament injuries remains challenging in young athletic populations. A residual
HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES Written by Philippe Landreau, Qatar The treatment of anterior cruciate ligament injuries remains challenging in young athletic populations. A residual
Differential Diagnosis
 Case 31yo M who sustained an injury to L knee while playing Basketball approximately 2 weeks ago. He describes pivoting and hyperextending his knee, which swelled over the next few days. He now presents
Case 31yo M who sustained an injury to L knee while playing Basketball approximately 2 weeks ago. He describes pivoting and hyperextending his knee, which swelled over the next few days. He now presents
Prevention and Treatment of Injuries. Anatomy. Anatomy. Chapter 20 The Knee Westfield High School Houston, Texas
 Prevention and Treatment of Injuries Chapter 20 The Knee Westfield High School Houston, Texas Anatomy MCL, Medial Collateral Ligament LCL, Lateral Collateral Ligament PCL, Posterior Cruciate Ligament ACL,
Prevention and Treatment of Injuries Chapter 20 The Knee Westfield High School Houston, Texas Anatomy MCL, Medial Collateral Ligament LCL, Lateral Collateral Ligament PCL, Posterior Cruciate Ligament ACL,
Posterolateral Corner Injuries of the Knee: Pearls and Pitfalls
 Posterolateral Corner Injuries of the Knee: Pearls and Pitfalls Robert A. Arciero,MD,Col,ret Professor, Orthopaedics University of Connecticut Incidence of PLC Injuries with ACL Tears Fanelli, 1995 12%
Posterolateral Corner Injuries of the Knee: Pearls and Pitfalls Robert A. Arciero,MD,Col,ret Professor, Orthopaedics University of Connecticut Incidence of PLC Injuries with ACL Tears Fanelli, 1995 12%
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Management of Knee Dislocations
 Management of Knee Dislocations Thomas J. Gill, MD Chief, Sports Medicine Service Massachusetts General Hospital Associate Professor of Orthopedic Surgery Harvard Medical School Complex Challenging Multi-Ligament
Management of Knee Dislocations Thomas J. Gill, MD Chief, Sports Medicine Service Massachusetts General Hospital Associate Professor of Orthopedic Surgery Harvard Medical School Complex Challenging Multi-Ligament
Please differentiate an internal derangement from an external knee injury.
 Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Anatomy and Sports Injuries of the Knee
 Anatomy and Sports Injuries of the Knee I. Anatomy II. Assessment III. Treatment IV. Case Study V. Dissection Anatomy Not a hinge joint 6 degrees of freedom Flexion/Extension Rotation Translation Anatomy
Anatomy and Sports Injuries of the Knee I. Anatomy II. Assessment III. Treatment IV. Case Study V. Dissection Anatomy Not a hinge joint 6 degrees of freedom Flexion/Extension Rotation Translation Anatomy
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
A biomechanical analysis of triangular medial knee reconstruction
 Wang et al. BMC Musculoskeletal Disorders (2018) 19:125 https://doi.org/10.1186/s12891-018-2039-1 RESEARCH ARTICLE Open Access A biomechanical analysis of triangular medial knee reconstruction Xiaomeng
Wang et al. BMC Musculoskeletal Disorders (2018) 19:125 https://doi.org/10.1186/s12891-018-2039-1 RESEARCH ARTICLE Open Access A biomechanical analysis of triangular medial knee reconstruction Xiaomeng
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
ARTICLE IN PRESS. Technical Note
 Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
MCL Tears: They all heal..or Do They? ERIK D. PETERSON, MD ORTHOPEDIC SPORTS MEDICINE SURGEON CORE ORTHOPEDICS
 MCL Tears: They all heal..or Do They? ERIK D. PETERSON, MD ORTHOPEDIC SPORTS MEDICINE SURGEON CORE ORTHOPEDICS Incidence Most Commonly Injured Ligament in the knee Mechanism Valgus applied stress to fixed/planted
MCL Tears: They all heal..or Do They? ERIK D. PETERSON, MD ORTHOPEDIC SPORTS MEDICINE SURGEON CORE ORTHOPEDICS Incidence Most Commonly Injured Ligament in the knee Mechanism Valgus applied stress to fixed/planted
Figure 3 Figure 4 Figure 5
 Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes
 Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Joints of the Lower Limb II
 Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management
 SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact)
 STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
The Knee. Prof. Oluwadiya Kehinde
 The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System
 Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Posterior cruciate ligament (PCL) reconstructions
 All-Inside Posterior Cruciate Ligament Reconstruction With a GraftLink Gerard G. Adler, M.D. Abstract: Posterior cruciate ligament (PCL) reconstructions are challenging surgeries. Recent advances have
All-Inside Posterior Cruciate Ligament Reconstruction With a GraftLink Gerard G. Adler, M.D. Abstract: Posterior cruciate ligament (PCL) reconstructions are challenging surgeries. Recent advances have
In the name of god. Knee. By: Tofigh Bahraminia Graduate Student of the Pathology Sports and corrective actions. Heat: Dr. Babakhani. Nov.
 In the name of god Knee By: Tofigh Bahraminia Graduate Student of the Pathology Sports and corrective actions Heat: Dr. Babakhani Nov. 2014 1 Anatomy-Bones Bones Femur Medial/lateral femoral condyles articulate
In the name of god Knee By: Tofigh Bahraminia Graduate Student of the Pathology Sports and corrective actions Heat: Dr. Babakhani Nov. 2014 1 Anatomy-Bones Bones Femur Medial/lateral femoral condyles articulate
Avulsion fracture of femoral attachment of posterior cruciate ligament: a case report and literature review
 Case Report Page 1 of 5 Avulsion fracture of femoral attachment of posterior cruciate ligament: a case report and literature review Yongwei Zhou, Qining Yang, Yang Cao Department of Orthopedics, Jinhua
Case Report Page 1 of 5 Avulsion fracture of femoral attachment of posterior cruciate ligament: a case report and literature review Yongwei Zhou, Qining Yang, Yang Cao Department of Orthopedics, Jinhua
Anterolateral Ligament. Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine
 Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Lateral ligament injuries of the knee
 Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Fibular collateral ligament reconstruction of knee using titanium button: a new fixation technique and an outcome of 35 cases
 International Journal of Research in Orthopaedics Rai SK et al. Int J Res Orthop. 2017 May;3(3):573-577 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20171904
International Journal of Research in Orthopaedics Rai SK et al. Int J Res Orthop. 2017 May;3(3):573-577 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20171904
Medical Diagnosis for Michael s Knee
 Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
On Field Assessment and Management of Acute Knee Injuries: A Physiotherapist s Perspective
 On Field Assessment and Management of Acute Knee Injuries: A Physiotherapist s Perspective Jessica Condliffe Physiotherapist / Clinic Manager TBI Health Wellington Presentation Outline Knee anatomy review
On Field Assessment and Management of Acute Knee Injuries: A Physiotherapist s Perspective Jessica Condliffe Physiotherapist / Clinic Manager TBI Health Wellington Presentation Outline Knee anatomy review
A Patient s Guide to Collateral Ligament Injuries
 A Patient s Guide to Collateral Ligament Injuries 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this booklet is
A Patient s Guide to Collateral Ligament Injuries 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this booklet is
Imaging the Athlete s Knee. Peter Lowry, MD Musculoskeletal Radiology University of Colorado
 Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Knee Joint Assessment and General View
 Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Hua Feng, Guan-yang Song, Jie-wei Shen, Hui Zhang & Man-yi Wang
 The lateral gutter drive-through sign revisited: a cadaveric study exploring its real mechanism based on the individual posterolateral structure of knee joints Hua Feng, Guan-yang Song, Jie-wei Shen, Hui
The lateral gutter drive-through sign revisited: a cadaveric study exploring its real mechanism based on the individual posterolateral structure of knee joints Hua Feng, Guan-yang Song, Jie-wei Shen, Hui
Grant H Garcia, MD Sports and Shoulder Surgeon
 What to Expect from your Anterior Cruciate Ligament Reconstruction Surgery A Guide for Patients Grant H Garcia, MD Sports and Shoulder Surgeon Important Contact Information Grant Garcia, MD Wallingford:
What to Expect from your Anterior Cruciate Ligament Reconstruction Surgery A Guide for Patients Grant H Garcia, MD Sports and Shoulder Surgeon Important Contact Information Grant Garcia, MD Wallingford:
Injury to the proximal deep medial collateral ligament
 Injury to the proximal deep medial collateral ligament A PROBLEMATICAL SUBGROUP OF INJURIES A. Narvani, T. Mahmud, J. Lavelle, A. Williams From the Chelsea and Westminster Hospital, London, England Most
Injury to the proximal deep medial collateral ligament A PROBLEMATICAL SUBGROUP OF INJURIES A. Narvani, T. Mahmud, J. Lavelle, A. Williams From the Chelsea and Westminster Hospital, London, England Most
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
ACL RECONSTRUCTION HAMSTRING METHOD. Presents ACL RECONSTRUCTION HAMSTRING METHOD. Multimedia Health Education
 HAMSTRING METHOD Presents HAMSTRING METHOD Multimedia Health Education Disclaimer Stephen J. Incavo MD This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate
HAMSTRING METHOD Presents HAMSTRING METHOD Multimedia Health Education Disclaimer Stephen J. Incavo MD This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate
and K n e e J o i n t Is the most complicated joint in the body!!!!
 K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
Management of Multi-ligament Knee Sports Injuries
 Management of Multi-ligament Knee Sports Injuries Aimee S. Klapach, MD Sports and Orthopaedic Specialists Allina Health Sports Medicine Conference June 15, 2018 Objectives Background On field assessment
Management of Multi-ligament Knee Sports Injuries Aimee S. Klapach, MD Sports and Orthopaedic Specialists Allina Health Sports Medicine Conference June 15, 2018 Objectives Background On field assessment
MRI of ligaments. Ligament biomechanics Spine Shoulder Elbow Hand/wrist Pelvis/hip Knee Foot/ankle
 MRI of ligaments Chang Ho Kang M.D. Korea University Anam Hospital Spine Shoulder Elbow Hand/wrist Pelvis/hip Knee Foot/ankle Introduction Ligament Fibrous connective tissue Attaches bone to bone Holds
MRI of ligaments Chang Ho Kang M.D. Korea University Anam Hospital Spine Shoulder Elbow Hand/wrist Pelvis/hip Knee Foot/ankle Introduction Ligament Fibrous connective tissue Attaches bone to bone Holds
Knee Surgical Technique
 Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
Lateral knee injuries
 Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
to the setting in which the patient is evaluated. Athletes are more likely. to sustain "isolated" PCL injuries as a result of a hyperflexion
 - -- MATTHEW D. PEPE, MD a Thomas Jefferson University, Philadelphia CHRISTOPHER D. HARNER, MD University of Pittsburgh Medical Center out by Key Wo The true incidence of posterior cruciate ligament (PCL)
- -- MATTHEW D. PEPE, MD a Thomas Jefferson University, Philadelphia CHRISTOPHER D. HARNER, MD University of Pittsburgh Medical Center out by Key Wo The true incidence of posterior cruciate ligament (PCL)
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
Case Report Reverse Segond Fracture Associated with Anteromedial Tibial Rim and Tibial Attachment of Anterior Cruciate Ligament Avulsion Fractures
 Hindawi Case Reports in Orthopedics Volume 2017, Article ID 9637153, 4 pages https://doi.org/10.1155/2017/9637153 Case Report Reverse Segond Fracture Associated with Anteromedial Tibial Rim and Tibial
Hindawi Case Reports in Orthopedics Volume 2017, Article ID 9637153, 4 pages https://doi.org/10.1155/2017/9637153 Case Report Reverse Segond Fracture Associated with Anteromedial Tibial Rim and Tibial
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
The Knee. Two Joints: Tibiofemoral. Patellofemoral
 Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Part 2, Load Sharing Between the Posterior Oblique Ligament and Superficial Medial Collateral Ligament
 Medial Knee Injury Part 2, Load Sharing Between the Posterior Oblique Ligament and Superficial Medial Collateral Ligament Coen A. Wijdicks,* MSc, Chad J. Griffith,* MD, Robert F. LaPrade,* MD, PhD, Stanislav
Medial Knee Injury Part 2, Load Sharing Between the Posterior Oblique Ligament and Superficial Medial Collateral Ligament Coen A. Wijdicks,* MSc, Chad J. Griffith,* MD, Robert F. LaPrade,* MD, PhD, Stanislav
ACL Injury: Does It Require Surgery?-OrthoInfo - AAOS
 ACL Injury: Does It Require Surgery?-OrthoInfo - AAOS ACL Injury: Does It Require Surgery? The following article provides in-depth information about treatment for anterior cruciate ligament injuries. The
ACL Injury: Does It Require Surgery?-OrthoInfo - AAOS ACL Injury: Does It Require Surgery? The following article provides in-depth information about treatment for anterior cruciate ligament injuries. The
How to avoid tunnel convergence in a multiligament injured knee
 Review Article Page 1 of 7 How to avoid tunnel convergence in a multiligament injured knee Gilbert Moatshe 1,2, Robert F. LaPrade 3, Lars Engebretsen 1,2 1 Orthopaedic Clinic, Oslo University Hospital
Review Article Page 1 of 7 How to avoid tunnel convergence in a multiligament injured knee Gilbert Moatshe 1,2, Robert F. LaPrade 3, Lars Engebretsen 1,2 1 Orthopaedic Clinic, Oslo University Hospital
FUNCTIONAL ANATOMY: Knee and Leg
 ACSM Team Physician Course San Antonio Feb 2015 FUNCTIONAL ANATOMY: Knee and Leg Marlene DeMaio, MD Professor, Orthopaedic Surgery Marshall University VAMC Huntington, WV Mary Lloyd Ireland, MD Professor
ACSM Team Physician Course San Antonio Feb 2015 FUNCTIONAL ANATOMY: Knee and Leg Marlene DeMaio, MD Professor, Orthopaedic Surgery Marshall University VAMC Huntington, WV Mary Lloyd Ireland, MD Professor
Direct Measurement of Graft Tension in Anatomic Versus Non-anatomic ACL Reconstructions during a Dynamic Pivoting Maneuver
 Direct Measurement of Graft Tension in Anatomic Versus Non-anatomic ACL Reconstructions during a Dynamic Pivoting Maneuver Scott A. Buhler 1, Newton Chan 2, Rikin Patel 2, Sabir K. Ismaily 2, Brian Vial
Direct Measurement of Graft Tension in Anatomic Versus Non-anatomic ACL Reconstructions during a Dynamic Pivoting Maneuver Scott A. Buhler 1, Newton Chan 2, Rikin Patel 2, Sabir K. Ismaily 2, Brian Vial
Rehabilitation of an ACL injury in a 29 year old male with closed kinetic chain exercises: A case study
 Abstract Objective: This paper will examine a rehabilitation program for a healthy 29 year old male who sustained an incomplete tear of the left ACL. Results: Following a 9 week treatment plan focusing
Abstract Objective: This paper will examine a rehabilitation program for a healthy 29 year old male who sustained an incomplete tear of the left ACL. Results: Following a 9 week treatment plan focusing
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Abstract. Introduction. Michele Vasso 1 Katia Corona 2 Giuseppe Toro 1 Marco Rossini 1 Alfredo Schiavone Panni 1
 256 Technical Note THIEME Anatomic Double-Bundle Medial Patellofemoral Ligament Reconstruction with Autologous Semitendinosus: Aperture Fixation Both at the Femur and the Patella Michele Vasso 1 Katia
256 Technical Note THIEME Anatomic Double-Bundle Medial Patellofemoral Ligament Reconstruction with Autologous Semitendinosus: Aperture Fixation Both at the Femur and the Patella Michele Vasso 1 Katia
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 43 rd Annual Symposium on Sports Medicine UT Health Science Center San Antonio School of Medicine January 22-23, 2016 Intra-articular / Extra-synovial 38 mm length / 13 mm width Fan-shaped structure narrowest-midportion
43 rd Annual Symposium on Sports Medicine UT Health Science Center San Antonio School of Medicine January 22-23, 2016 Intra-articular / Extra-synovial 38 mm length / 13 mm width Fan-shaped structure narrowest-midportion
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Sports Medicine 15. Unit I: Anatomy. The knee, Thigh, Hip and Groin. Part 4 Anatomies of the Lower Limbs
 Sports Medicine 15 Unit I: Anatomy Part 4 Anatomies of the Lower Limbs The knee, Thigh, Hip and Groin Anatomy of the lower limbs In Part 3 of this section we focused upon 11 of the 12 extrinsic muscles
Sports Medicine 15 Unit I: Anatomy Part 4 Anatomies of the Lower Limbs The knee, Thigh, Hip and Groin Anatomy of the lower limbs In Part 3 of this section we focused upon 11 of the 12 extrinsic muscles
Knee Movement Coordination Deficits. ICD-9-CM: Sprain of cruciate ligament of knee
 1 Knee Movement Coordination Deficits Anterior Cruciate Ligament ACL Tear ICD-9-CM: 844.2 Sprain of cruciate ligament of knee ACL Insufficiency ICD-9-CM: 717.83 Old disruption of anterior cruciate ligament
1 Knee Movement Coordination Deficits Anterior Cruciate Ligament ACL Tear ICD-9-CM: 844.2 Sprain of cruciate ligament of knee ACL Insufficiency ICD-9-CM: 717.83 Old disruption of anterior cruciate ligament
AFX. Femoral Implant. System. The AperFix. AM Portal Surgical Technique Guide. with the. The AperFix System with the AFX Femoral Implant
 The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
Knee: Cruciate Ligaments
 72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
Why anteromedial portal is the best
 Controversies in ACL Reconstruction Why anteromedial portal is the best Robert A. Gallo, MD Associate Professor Nothing to disclose Case presentation 20-year-old Division III track athlete sustained ACL
Controversies in ACL Reconstruction Why anteromedial portal is the best Robert A. Gallo, MD Associate Professor Nothing to disclose Case presentation 20-year-old Division III track athlete sustained ACL
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
Human ACL reconstruction
 Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Double Bundle PCL Reconstruction. Surgical Technique
 Double Bundle PCL Reconstruction Surgical Technique Double Bundle PCL Reconstruction With recent interest in double tunnel endoscopic PCL reconstruction, Arthrex has created a series of Femoral PCL Drill
Double Bundle PCL Reconstruction Surgical Technique Double Bundle PCL Reconstruction With recent interest in double tunnel endoscopic PCL reconstruction, Arthrex has created a series of Femoral PCL Drill
Learning IRM. The Knee: lateral ligaments and anatomical quadrants.
 Learning IRM. The Knee: lateral ligaments and anatomical quadrants. Poster No.: C-1733 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Amador Gil, M. D. C. Jurado Gómez, V. de Lara Bendahan ;
Learning IRM. The Knee: lateral ligaments and anatomical quadrants. Poster No.: C-1733 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Amador Gil, M. D. C. Jurado Gómez, V. de Lara Bendahan ;
KNEE EXAMINATION. Tips & Tricks from an Emergency Physician Perspective. EM Physicians Less Exposed to MSK Medicine
 KNEE EXAMINATION Tips & Tricks from an Emergency Physician Perspective Dr P O CONNOR Emergency Medicine Physician EUSEM 10/09/2018 EM Physicians Less Exposed to MSK Medicine Musculoskeletal Medicine becoming
KNEE EXAMINATION Tips & Tricks from an Emergency Physician Perspective Dr P O CONNOR Emergency Medicine Physician EUSEM 10/09/2018 EM Physicians Less Exposed to MSK Medicine Musculoskeletal Medicine becoming
Reconstruction of the Ligaments of the Knee
 Reconstruction of the Ligaments of the Knee Contents ACL reconstruction Evaluation Selection Evolution Graft issues Notchplasty Tunnel issues MCL PCL Posterolateral ligament complex Combined injuries Evaluation
Reconstruction of the Ligaments of the Knee Contents ACL reconstruction Evaluation Selection Evolution Graft issues Notchplasty Tunnel issues MCL PCL Posterolateral ligament complex Combined injuries Evaluation
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player
 UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
Physical Examination of the Knee
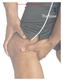
 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
Biomechanical Analysis of Internal Bracing for Treatment of Medial Knee Injuries
 Biomechanical Analysis of Internal Bracing for Treatment of Medial Knee Injuries Brian B. Gilmer, MD; Timothy Crall, MD; Jeffrey DeLong, BS; Takanori Kubo, MD; Gordon Mackay, MD; Sunil S. Jani, MD, MS
Biomechanical Analysis of Internal Bracing for Treatment of Medial Knee Injuries Brian B. Gilmer, MD; Timothy Crall, MD; Jeffrey DeLong, BS; Takanori Kubo, MD; Gordon Mackay, MD; Sunil S. Jani, MD, MS
Physical Examination and Imaging of the Lateral Collateral Ligament and Posterolateral Corner of the Knee
 REVIEW ARTICLE Physical Examination and Imaging of the Lateral Collateral Ligament and Posterolateral Corner of the Knee Michael S. Bahk, MD and Andrew J. Cosgarea, MD Abstract: Diagnosis of posterolateral
REVIEW ARTICLE Physical Examination and Imaging of the Lateral Collateral Ligament and Posterolateral Corner of the Knee Michael S. Bahk, MD and Andrew J. Cosgarea, MD Abstract: Diagnosis of posterolateral
Extensor Mechanism Rupture
 Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
An In Vitro Analysis of an Anatomical Medial Knee Reconstruction
 Winner of the 2009 Excellence in Research Award An In Vitro Analysis of an Anatomical Medial Knee Reconstruction Benjamin R. Coobs, * MD, Coen A. Wijdicks, * MSc, Bryan M. Armitage, * MD, MSc, Stanislav
Winner of the 2009 Excellence in Research Award An In Vitro Analysis of an Anatomical Medial Knee Reconstruction Benjamin R. Coobs, * MD, Coen A. Wijdicks, * MSc, Bryan M. Armitage, * MD, MSc, Stanislav
CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY
 CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY _ 1. The hip joint is the articulation between the and the. A. femur, acetabulum B. femur, spine C. femur, tibia _ 2. Which of the following is
CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY _ 1. The hip joint is the articulation between the and the. A. femur, acetabulum B. femur, spine C. femur, tibia _ 2. Which of the following is
Your Practice Online
 Your Practice Online Disclaimer P R E S E N T S - PATELLAR TENDON This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate Ligament (ACL) Reconstruction.
Your Practice Online Disclaimer P R E S E N T S - PATELLAR TENDON This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate Ligament (ACL) Reconstruction.
Retinacular tear knee
 P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
SAMPLE ONLY. NOT FOR DISTRIBUTION. The Knee
 SAMPLE ONLY. NOT FOR DISTRIBUTION. 1 The Knee 2 CHAPTER 1 SAMPLE ONLY. NOT FOR DISTRIBUTION. THEY ARE NOT CUSHIONS! I can t tell you how many times I ve heard it said that the meniscus cartilages are the
SAMPLE ONLY. NOT FOR DISTRIBUTION. 1 The Knee 2 CHAPTER 1 SAMPLE ONLY. NOT FOR DISTRIBUTION. THEY ARE NOT CUSHIONS! I can t tell you how many times I ve heard it said that the meniscus cartilages are the
Treatment of Acute Traumatic Knee Dislocations
 Treatment of Acute Traumatic Knee Dislocations Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
Treatment of Acute Traumatic Knee Dislocations Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
