Lower Leg Flaps Comparison Between Free Versus Local Flaps
|
|
|
- Ashley Watson
- 5 years ago
- Views:
Transcription
1 ISPUB.COM The Internet Journal of Plastic Surgery Volume 3 Number 2 Lower Leg Flaps Comparison Between Free Versus Local Flaps A Bhatti, A Adeshola, T Ismael, N Harris Citation A Bhatti, A Adeshola, T Ismael, N Harris. Lower Leg Flaps Comparison Between Free Versus Local Flaps. The Internet Journal of Plastic Surgery Volume 3 Number 2. Abstract Background: In lower leg defects with bone, hardware, or articular joint exposure, a free tissue transfer is often the only valuable option. However, in well-selected clinical cases, local flaps are still indicated because they provide an alternative for the more demanding and risky microsurgical procedure. Methods: Twenty-six muscle flaps (performed in 26 patients) were reviewed retrospectively and compared with a series of 24 free flaps (23 patients) for lower leg reconstruction of almost similar indications. All patients with defects less than 25 cm2, peripheral vascular disease, deep defects, and osteomyelitis were excluded in order to obtain the same surgical indications.also excluded were cases which needed split skin graft. Results: The overall surgical results were comparable, but more medical complications, a longer operative time, and a longer hospital stay were seen in the free muscle group. Conclusions: Free flap coverage is not mandatory to cover bone in the lower leg. The non-free flap can provide a good alternative for free flap coverage. This flap seems to have fewer medical complications, requires a shorter operative time and hospital stay, and can provide better aesthetic results than a free muscle flap depending upon selection of cases. Presented at the Sir Peter Feyer Memorial meeting of surgery, in Galway, Ireland, Sep1 to Sep 2, 2006, INTRODUCTION Whenever bone, osteo-synthesis material, or tendons are exposed in the lower leg, the reconstructive procedure will be a challenge for the reconstructive surgeon. Because of the lack of available local soft tissue, the middle and distal thirds of the lower leg are the most problematic areas. Free flaps are the first choice procedure to manage softtissue defect of the lower limb for many authors, but loco-regional flaps are an alternative since they were described in the 1980s. We analyzed the changes in our practice as it has become prevalent. Microsurgical tissue transfers were predominant in the 1980s and decreased in the 1990s, whereas the local flap had an opposite evolution. In our experience, local flaps are related to a non significant lower rate of complication (18%) than free flaps (27%). Moreover, complications of local and regional flaps are less severe. Our practice has changed to make local flaps as our first choice to cover soft-tissue defects of the lower limb. However, we still use free flaps as a first choice for wide or composite defects, when local flaps are not feasible. Still management of soft-tissue defects of the lower limb remains difficult and the distal third of the leg is considered the most difficult area to reconstruct. 1 of 8
2 The tibia is in a subcutaneous position and therefore often exposed in case of leg injury. Moreover, the lack of both local skin laxity and muscular tissue in this area make the reconstruction difficult. Muscle flap coverage remains the first choice for many surgeons because of the high vascularity and the high tolerance and resistance to infection of these flaps. 3, 4, 5, 6, 7 However, fascial and fasciocutaneous flaps have regained popularity as excellent alternatives for coverage of lower leg defects. 3, 8, 9 the recently described medial adipose-fascial flap 10, 11, 12, 13 has several advantages: it spares all the major vessels of the lower limb and there are multiple harvesting possibilities. Increasingly surgeons are experimenting options of different local flaps like peroneus brevis muscle flap, reverse soleus flap, flexor digitorum longus flapsetc.many studies are also being done to find out the anatomical relationships of vessels feeding different local flaps. There have been many wounds when the options of the local flap would also arise alongside free flap and the surgeons have to make a decision what is the best for the patient at that time?.our study aimed to find out similar indications of the lower leg reconstruction and compare results of free flap versus local flap. We compared our series of non-free flaps with a series of free muscular flaps that had almost similar clinical circumstances and causative factors. In this way, we could compare the clinical results of lower leg defects covered with a highly vascularized, local flap and a free muscular flap. PATIENTS AND METHODS The study was carried out in retrospective manner in which consecutive patients with lower leg defect having coverage by flaps operated by different surgeons in between January 2000 and January 2005 were included.all the patients needing only skin grafts were excluded as well where the options of the local flap was not feasible because of damage to perforators due to severe trauma,fractures or extensive retraction of the vessels due to chronicity of the wound. Also excluded few cases where the application of the external fixator or internal rods makes the option of the local flap very risky. In this way, we obtained two homogeneous groups for which only the surgeon's preference determined the use of a local or free flap. Patients' medical records were reviewed retrospectively to determine the cause and localization of the defect, size of the defect,the tissue that had to be covered, and the type of flap (free or local flap) that had been used. All patients with defects less than 25 cm2, peripheral vascular disease, deep bony defects, and osteomyelitis were excluded in order to obtain the same surgical indications. In both groups, the following features were studied: (1) surgical complications, such as partial or complete flap necrosis, local wound problems, and donor-site problems; (2) medical complications; (3) duration of hospital stay; and (4) final aesthetic outcome. All flaps were harvested using the standard techniques described in literature (Heymans et al). 13 Before incision, if indicated the pedicle and perforating vessels of the local flaps are mapped by Doppler study. Whenever the flap based on the saphenous artery has to be harvested, an incision is made from the medial condyle to the anterior tibial crest and the skin is elevated superficially. The base of the flap should be as large as 5 cm at the level of the medial side of the knee. The fatty tissue is incised anteriorly along the tibial border, distally, and posteriorly until the deep fascia is encountered. Dissection is continued in a plane under the deep fascia, starting distally. If the decision is made to harvest a flap based on the posterior tibial perforators, then the incision is made 1 cm medial to the tibial crest. The dissection is continued subcutaneously along the entire medial side of the lower leg, followed by incision of the deep fascia along the tibial crest. During this dissection, the intermuscular septa are divided, but the perforators, representing the pivot point, are preserved. Depending on the selected perforator (pivot point), the flap will be supplied in an antegrade way (based on a proximal perforator) or in a retrograde way (based on a distal perforator). The adiposofascial flap is covered during the same operative procedure with a thin split-thickness skin graft, and a suction drain is placed at the donor site for 3 days. 2 of 8
3 Similarly the gastrocnemius and soleus muscle were planned by planning the vertical midline incision on the calf and while saving the sural nerve in the line of dissection,the muscle flap were harvested base on the sural arteries. Free flaps used for lower leg reconstruction in this series included lattismus dorsi,rectus abdominus, gracilis, radial forearm and anterolateral free flap. The free flap was harvested according to the standard defined techniques in the literature. Comparisons between groups used the chi-square test and statistical significance was set at the level of RESULTS Out of the total of 26 patients having undergone local flaps 17 were male and nine female ranging in age from 15 to 75 years (mean age, 50 years) Table 1. The mean follow-up time was 6 months (range, 4 to 10 months). Indications for flap coverage were open fracture (n =24), exposure of osteosynthesis material (n = 12), osteotendinous exposure (n = 8), soft-tissue necrosis (n = 6), with bone exposure (Table 2). The size of the wounds, their distribution over the distal leg and distribution of the different surgical procedures according to the size of the defect are shown in tables 3 & 4. Figure 1 six were women, ranging in age from 26 to 72 years (mean age, 47 years). The mean follow-up time was 6 months (range, 4 to 8 months). The distribution of the hospital stay and operative time is compared in tables 5 & 6 respectively. It can be seen the use of newly described flaps like medial adiposofascial flap,sural artery based flap and saphenous flap etc. Surgical results are presented in Table 7. There were two complete flap losses in the free groups and 2 partial flap necrosis each in local and free flap group. In one of the medial adipose-fascial flap series, the flap was lost in the early postoperative period because of venous congestion related to inadequate tunneling of the flap. In the free flap series, venous congestion was the cause of flap loss and even reexploration could not save the flap. One of the free flap failed needed reexploration and cover by another free flap,anterolateral thigh in one case and gracilis muscle free flap in other cases in both the cases the failed flaps were latisimusdorsi flap. The overall graft take was 95 percent in the muscular flaps both in the local and free flap harvest. There were three flaps complicated with bleeding with two hematoma had to be evacuated in the free flap group. Medical complications occurred in both series, although their incidence seemed to be slightly higher in the free flap group (18 percent): there were two cases with DVT, one acute myocardial ischemia, and one sepsis, compared with one local flap necrosis in the local flap group. (Table 7). Out of the total of 24 patients who had free flaps where eighteen patients were men and 3 of 8
4 Figure 2 DISCUSSION Trauma is the most common aetiology in this young and active population. This probably explains the location of the wounds at the lower third of the leg and the rate of bone exposure (43%) which is more likely to occur in this area. The surface of the wounds to cover (mean size: 50 cm2) was equivalent through the years and this factor could not represent a bias for the selection of the procedure. Regarding the procedure used, 35% of the cases were treated with either a skin graft or dressing for secondary healing as a single procedure. As a confirmation of the lack of laxity in this area, local flaps were used in only 7.1% of the cases. The remaining cases required the mobilisation of a local or free flap to achieve the reconstruction. Among the local flaps, the fasciocutanous flap, the bipedicled flap and the distally based muscular soleus flap and gastrocnemius flap were the most commonly used. Among the free flaps, preference was given to the latissimus dorsi myocutaneous flap, thus confirming its facility and reliability. Many factors have always influenced the indications for a procedure (technical skills, wound size and localization as well as the exposed tissues), but the choice has changed with time. Free flaps were the first option from the 1980s to the early 1990s. At this time, the development of many local flaps made them predominant for the last decade. Moreover, the definition of complication differs from one study to another, since vascular thrombosis is not always considered as a complication, 12, 13 and skin grafting of the donor site is considered as such. 21 Nevertheless, the complication rate for free flaps ranges from 10% 11,13 to 38% 10 and from 21% 2, 13, 20 to 46% 22 for local flaps. In our experience, local flaps are related to a lower rate of complication (18%) than free flaps (27%). Moreover, complications of local and regional flaps are less severe. With time our practice has changed to make local flaps our first choice to cover soft tissue defects of the lower limb, because these flaps are less demanding, easier to use and related to less severe and less numerous complications. Should this procedure fail, it does not preclude the use of a free flap as a secondary procedure which remains a rare instance. However, we still use free flaps as a first choice for wide or composite defects. Throughout the literature, numerous studies confirm the advantage of immediate soft tissue coverage of exposed bone. 4, 5, 13, 14, 15 The goal of this study, performed on two homogeneous patient populations, was to answer two questions that remain controversial in the literature. First, is there still place for local flaps in coverage of lower leg defects? Second, the exposed bone covered with local flap have better outcome than free flap or not? Although free flaps have become the first choice for reconstructive procedures in the lower leg since the popularization of microsurgery, local flaps can still be indicated in selected cases. 3, 16 Proper patient and flap selection is key for these conditions. In our study, we excluded all patients with defects larger than100 cm2, 4 of 8
5 peripheral vascular disease, deep defects, and osteomyelitis, because in our department these clinical presentations remain indications for free flap surgery. The use of local muscle flaps, such as the gastrocnemius and the soleus, has proven to be valuable in the management of soft tissue defects over the tibia. 1, 16 However, because of local contusion of the soft tissues after trauma, local muscle flaps are not always perfectly healthy and will not have the trophic qualities of a free flap. Moreover, there will be local devascularization subsequent to the removal of the flap, and the tissue defect will often be covered with the least vascularized distal part of the muscle flap. Local fascial and fasciocutaneous flaps can provide an excellent alternative, 3, 8, 9 but they have limited reach and can be unreliable, especially if the area around the wound has been traumatized or is chronically scarred. Moreover, they often leave ugly donor-site scars because of the need for skin grafting. 2, 9, 17 Among these fasciocutaneous flaps, the distally based sural flap has some exceptional features. Although first described by Masquelet et al. 18 as a "neuroskin" island flap; it can be harvested without sacrificing the sural nerve end, thereby reducing the donor site. It has the largest arc of rotation among flaps that have been described for the lower leg, and it can be elevated in cases of peripheral vascular disease or damage to major vessels caused by trauma, as long as the peroneal artery is preserved. 19 The sural flap is harvested most of the time as a fasciocutaneous flap, leaving an ugly donor-site scar, 20 but it can be harvested as a pure fascial flap, thereby reducing donor-site morbidity. The recently described medial adipose-fascial flap 10, 11, 12, 13 is another exceptional local flap with several advantages. As in the distally based sural flap, no major vessel has to be sacrificed, the flap is reliable even in traumatized areas, and no skin is harvested (although it is possible), leaving minimal donor-site scarring. However, the medial adiposefascial flap has some additional advantages to the sural flap: it can easily be harvested with the patient in the supine position; because of its dual vascularization, 13 the flap can be tailored for proximal and distal defects; and wellvascularized tissue can be harvested to cover a defect of up to 40 cm2, without noticeable venous congestion. In the literature, it has been well documented that after vigorous débridement of lower leg defects, coverage is needed with well-vascularized tissue, preferably muscle. 2, 21, 22 Indeed, since the works of Mathes and coworkers initiated the concept of bone coverage by muscle flaps in the 1980s, 6, 7 a dogma persists on using muscle flaps as coverage whenever bone is exposed. It is a common misconception that muscle provides better vascularity and greater tolerance to infection than adipofascial or fasciocutaneous flaps. Muscle flaps are not the solution for "curing" established infection. Recent clinical work also confirms that nonmuscular tissue can be successfully transferred to cover bone defects after aggressive débridement, which remains the key factor. 23, 24, 25, 26 Moreover, muscle harvesting can induce a certain morbidity of the donor site and may induce some aesthetic disadvantages on the recipient site. Nowadays, successful flap transfer rates approach 98.8 percent in literature, 27 and harvesting of the free flap provides a bulky flap with donor-site morbidity, 28 comparable to local muscle/fascial flap harvesting. In our series, the microsurgical procedure prolonged the operative time. A longer hospital stay was noticed in the free flap group, which increased perioperative costs. 2, 29 we documented a higher medical complication rate after the free flap surgery (45.8% percent than in the local fascial group (11.5%), but we believe this study is too small to determine the reasons for the increased morbidity. Although operation was significantly longer in the free flap group, it has not generally been implicated in increasing the morbidity rate, 30, unless the surgical time exceeds 10 hours, which never occurred in this series. It might be that the longer hospital stay, implying prolonged stress, exposure to the hospital environment, and diminished physical activity, plays an important role in the increased morbidity rate. However, this was not the goal of this study and more extensive work on larger series regarding this subject should be performed. CONCLUSIONS In selected cases of bone, hardware, or articular exposure without obvious osteomyelitis, the final functional outcome after free or fascial coverage is identical. Although free flap surgery has become a versatile procedure, it remains a more demanding and risky procedure than local flap surgery. Moreover, the local fascial flap of the leg can provide a better alternative for free flap coverage with fewer medical complications, a shorter operative time and hospital stay, and better aesthetic results. References 1. Ebraheim, N. A., Madsen, T., and Humphreys, B. The tibialis anterior used as a local muscle flap over the tibia after soft tissue loss. J. Trauma 55: 959, 5 of 8
6 Attinger, C. E., Ducic, I., Cooper, P., and Zelen, C. M. The role of intrinsic muscle flaps of the foot for bone coverage in foot and ankle defects in diabetic and nondiabetic patients. Plast. Reconstr. Surg. 110: 1047, Hallock, G. G. Utility of both muscle and fascia flaps in severe lower extremity trauma. J. Trauma 48: 913, Byrd, H. S., Spicer, T. E., and Cierny, G., III. Management of open tibial fractures. Plast. Reconstr. Surg. 76: 719, Small, J. O., and Mollan, R. A. B. Management of the soft tissues in open tibial fractures. Br. J. Plast. Surg. 45: 571, Chang, N., and Mathes, S. J. Comparison of the effect of bacterial inoculation in musculocutaneous and random-pattern flaps. Plast. Reconstr. Surg. 70: 1, Gosain, A., Chang, N., Mathes, S., Hunt, T. K., and Vasconez, L. A study of the relationship between blood flow and bacterial inoculation in musculocutaneous and fasciocutaneous flaps. Plast. Reconstr. Surg. 86: 1152, Hollier, L., Sharma, S., Babigumira, E., and Klebuc, M. Versatility of the sural fasciocutaneous flap in the coverage of lower extremity wounds. Plast. Reconstr. Surg. 110: 1673, Touam, C., Rostoucher, P., Bhatia, A., and Oberlin, C. Comparative study of two series of distally based fasciocutaneous flaps for coverage of the lower one-fourth of the leg, the ankle and the foot. Plast. Reconstr. Surg. 107: 383, Lin, S. D., Lai, C. S., Chiu, Y. T., Lin, T. M., and Chou, C. K. Adiposofascial flap of the lower leg based on the saphenous artery. Br. J. Plast. Surg. 49: 390, Lin, S. D., Lai, C. S., Tsai, C. C., Chou, C. K., and Tsai, C. W. Clinical application of the distally based medial adiposofascial flap for soft tissue defects on the lower half of the leg. J. Trauma 38: 623, Cavadas, P. C. Reversed saphenous neurocutaneous island flap: Clinical experience and evolution to the posterior tibial perforatorsaphenous subcutaneous flap. Plast. Reconstr. Surg. 111: 837, Heymans, O., Verhelle, N., and Peters, S. The medial adiposofascial flap of the leg: Anatomical basis and clinical applications. Plast. Reconstr. Surg. 115: 793, Yaremchuck, M. J., Brumback, R. J., Manson, P. N., Burgess, A. R., Poka, A., and Weiland, A. J. Acute and definitive management of traumatic osteocutaneous defect of the lower extremity. Plast. Reconstr. Surg. 80: 1, Tropet, Y., Garbuio, P., Obert, L., and Ridoux, P. E. Emergency management of type IIIB open tibial fractures. Br. J. Plast. Surg. 52: 462, Beck, J. B., Stile, F., and Lineaweaver, W. Reconsidering the soleus muscle flap for coverage of wounds of the distal third of the leg. Ann. Plast. Surg. 50: 631, Attinger, C. Soft tissue coverage for lower extremity trauma. Orthop. Clin. North Am. 26: 295, Masquelet, A. C., Romana, M. C., and Wolf, G. Skin island flaps supplied by the vascular axis of sensitive superficial nerves: Anatomical study and clinical experience in the leg. Plast. Reconstr. Surg. 89: 1115, Seng-Feng, J., Ching-Hua, H., Yur-Ren, K., Tsan-Shiun, L., and Fu-Chan, W. Distally based sural island flap. Plast. Reconstr. Surg. 111: 840, Rajacic, N., Gang, K., Krishnan, J., and Kojic, S. Lower leg reconstruction using distally based saphenous island flap. Eur. J. Plast. Surg. 24: 7, Steed, D. L., Donohoe, D., Webster, M. W., and Lindsley, L. Effect of extensive débridement and treatment on the healing of diabetic foot ulcers. J. Am. Coll. Surg. 183: 61, Cheng, H. H., Rong, G. W., Yin, T. C., Wang, H. Y., and Jiao, Y. C. Coverage of wounds in the distal lower leg by advancement of an enlarged medial gastrocnemius skin flap. Plast. Reconstr. Surg. 73: 671, Arnold, P. G., Yugueros, P., and Hanssen, A. D. Muscle flaps in osteomyelitis of the lower extremity: A 20-year account. Plast. Reconstr. Surg. 104: 107, Musharafieh, R., Atiyeh, B., Macari, G., and Haider, R. Radial forearm fasciocutaneous free tissue transfer in ankle and foot reconstruction: Review of 17 cases. J. Reconstr. Microsurg. 17: 147, Blume, P. A., Paragas, L. K., Sumpio, B. E., and Attinger, C. E. Single-stage surgical treatment of noninfected diabetic foot ulcers. Plast. Reconstr. Surg. 109: 601, Weinzweig, N., and Davies, B. W. Foot and ankle reconstruction using the radial forearm flap: A review of 25 cases. Plast. Reconstr. Surg. 102: 1999, Khouri, R. K., Cooley, B. C., Kunselman, A. R., et al. A prospective study of microvascular free flap surgery and outcome. Plast. Reconstr. Surg. 102: 711, Giordano, P. A., Abbes, M., and Pequignot, J. P. Gracilis blood supply: Anatomical and clinical re-evaluation. Br. J. Plast. Surg. 43: 266, Heckler, F. R. Gracilis myocutaneous and muscle flaps. Clin. Plast. Surg. 7: 27, of 8
7 29. Yousif, N. J., Matloub, H. S., Kolashalam, R., Grunert, B. K., and Sanger, J. R. The transverse gracilis musculocutaneous flap. Ann. Plast. Surg. 29: 482, Heinz, T. R., Cowper, P. A., and Levin, L. S. Microsurgery costs and outcome. Plast. Reconstr. Surg. 14: 89, of 8
8 Author Information Asif Zubair Bhatti, MD,FRCS,FCPS Department of Plastic and Reconstructive Surgery, Derriford Hospital Adeniran Adeshola, FRCS(GLASG) Department of Plastic and Reconstructive Surgery, Derriford Hospital Thamer Ismael, FRCS Department of Plastic and Reconstructive Surgery, Derriford Hospital Nathan Harris Department of Plastic and Reconstructive Surgery, Derriford Hospital 8 of 8
ABSTRACT. Key words: Flaps, Adipofascial, Lower limb reconstruction. Khaldoun J. Haddadin, MD*, Samer Y. Haddad, MD. Introduction.
 DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
ORIGINAL ARTICLE DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS
 DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
17 FibulA FlAP Tor Chiu fibula flap 153
 17 Fibula Flap Tor Chiu Fibula Flap 153 Fibula Flap FLAP TERRITORY This flap includes a segment of the fibular bone with or without the overlying skin island on the peroneal/ lateral aspect of the calf.
17 Fibula Flap Tor Chiu Fibula Flap 153 Fibula Flap FLAP TERRITORY This flap includes a segment of the fibular bone with or without the overlying skin island on the peroneal/ lateral aspect of the calf.
Planning and outcome of soft tissue defects of the foot
 206; 2(4): 47-423 ISSN: 2395-958 IJOS 206; 2(4): 47-423 206 IJOS www.orthopaper.com Received: -08-206 Accepted: 2-09-206 Dr. Shuaib Ahmed Dr. Latheesh Leo Hand and Microvascular Surgery, Department of
206; 2(4): 47-423 ISSN: 2395-958 IJOS 206; 2(4): 47-423 206 IJOS www.orthopaper.com Received: -08-206 Accepted: 2-09-206 Dr. Shuaib Ahmed Dr. Latheesh Leo Hand and Microvascular Surgery, Department of
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function
 Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications
 Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Role Of Reverse Sural Artery Flap In Ankle, Foot And Leg Defects
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. VIII (May. 2016), PP 64-68 www.iosrjournals.org Role Of Reverse Sural Artery Flap In
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. VIII (May. 2016), PP 64-68 www.iosrjournals.org Role Of Reverse Sural Artery Flap In
Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients
 JFS (P) Kuldeep Singh et al ORIGINL RTICLE 10.5005/jp-journals-10040-1083 Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients 1 Kuldeep Singh, 2 Zile
JFS (P) Kuldeep Singh et al ORIGINL RTICLE 10.5005/jp-journals-10040-1083 Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients 1 Kuldeep Singh, 2 Zile
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints
 Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
Lower extremity trauma, with open highenergy RECONSTRUCTIVE
 RECONSTRUCTIVE Lower Extremity Trauma: Trends in the Management of Soft-Tissue Reconstruction of Open Tibia-Fibula Fractures Brian M. Parrett, M.D. Evan Matros, M.D. Julian J. Pribaz, M.D. Dennis P. Orgill,
RECONSTRUCTIVE Lower Extremity Trauma: Trends in the Management of Soft-Tissue Reconstruction of Open Tibia-Fibula Fractures Brian M. Parrett, M.D. Evan Matros, M.D. Julian J. Pribaz, M.D. Dennis P. Orgill,
Compartment Syndrome
 Compartment Syndrome Chapter 34 Compartment Syndrome Introduction Compartment syndrome may occur with an injury to any fascial compartment. The fascial defect caused by the injury may not be adequate to
Compartment Syndrome Chapter 34 Compartment Syndrome Introduction Compartment syndrome may occur with an injury to any fascial compartment. The fascial defect caused by the injury may not be adequate to
Versatility of the sural fasciocutaneous flap in coverage defects of the lower limb
 Injury, Int. J. Care Injured (2007) 38, 824 831 www.elsevier.com/locate/injury Versatility of the sural fasciocutaneous flap in coverage defects of the lower limb Antonio Ríos-Luna a,b, *, Manuel Villanueva-Martínez
Injury, Int. J. Care Injured (2007) 38, 824 831 www.elsevier.com/locate/injury Versatility of the sural fasciocutaneous flap in coverage defects of the lower limb Antonio Ríos-Luna a,b, *, Manuel Villanueva-Martínez
TRANSTIBIAL AMPUTATION General Principles & Update on Surgical Techniques
 TRANSTIBIAL AMPUTATION General Principles & Update on Surgical Techniques Douglas G. Smith, MD Harborview Medical Center and University of Washington - Emeritus Prosthetic Research Study Amputee Coalition
TRANSTIBIAL AMPUTATION General Principles & Update on Surgical Techniques Douglas G. Smith, MD Harborview Medical Center and University of Washington - Emeritus Prosthetic Research Study Amputee Coalition
Increased SuccessRate in Delayed Reverse Sural Artery Flap
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 9 Ver. IV (Sep. 2017), PP 24-28 www.iosrjournals.org Increased SuccessRate in Delayed Reverse
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 9 Ver. IV (Sep. 2017), PP 24-28 www.iosrjournals.org Increased SuccessRate in Delayed Reverse
BOAST 4 Algorithm. 6th September 2013
 BOAST 4 Algorithm 6th September 2013 Background The British Orthopaedic Association and the British Association of Plastic, Reconstructive and Aesthetic Surgeons reviewed their 1997 guidance and published
BOAST 4 Algorithm 6th September 2013 Background The British Orthopaedic Association and the British Association of Plastic, Reconstructive and Aesthetic Surgeons reviewed their 1997 guidance and published
The distally-based island ulnar artery perforator flap for wrist defects
 Free full text on www.ijps.org Original Article The distally-based island ulnar artery perforator flap for wrist defects Durga Karki, A. K. Singh Post Graduate Department of Plastic and Reconstructive
Free full text on www.ijps.org Original Article The distally-based island ulnar artery perforator flap for wrist defects Durga Karki, A. K. Singh Post Graduate Department of Plastic and Reconstructive
Malignant soft tissue tumor, wide excision, and sural flap
 CASE REPORT Magetsari et al. 1 PEER REVIEWED OPEN ACCESS Malignant soft tissue tumor, wide excision, and sural flap Rahadyan Magetsari, Yudha Mathan Sakti, Arie Nugroho ABSTRACT Introduction: Soft tissue
CASE REPORT Magetsari et al. 1 PEER REVIEWED OPEN ACCESS Malignant soft tissue tumor, wide excision, and sural flap Rahadyan Magetsari, Yudha Mathan Sakti, Arie Nugroho ABSTRACT Introduction: Soft tissue
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
Lower Extremity Reconstruction
 1 Chapter 21 Overview: Lower Extremity Reconstruction Louis Carter This subject is also partially covered in the chapters Flaps for Wound Coverage and Perforator Flaps. This chapter will deal with reconstruction
1 Chapter 21 Overview: Lower Extremity Reconstruction Louis Carter This subject is also partially covered in the chapters Flaps for Wound Coverage and Perforator Flaps. This chapter will deal with reconstruction
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Outcome of Islanded Gastrocnemius Musculocutaneous Flap in Orthopaedic Practice
 doi: http://dx.doi.org/10.5704/moj.1903.004 Outcome of Islanded Gastrocnemius Musculocutaneous Flap in Orthopaedic Practice Yusof MN, MMed Ortho, Ahmad-Alwi AA*, MSurg (Plastic) Department of Orthopaedics,
doi: http://dx.doi.org/10.5704/moj.1903.004 Outcome of Islanded Gastrocnemius Musculocutaneous Flap in Orthopaedic Practice Yusof MN, MMed Ortho, Ahmad-Alwi AA*, MSurg (Plastic) Department of Orthopaedics,
Closure of Chronic Heel Ulcer by Simple V-Y Flap
 Egypt, J. Plast. Reconstr. Surg., Vol. 40, No. 1, January: 97-101, 2016 Closure of Chronic Heel Ulcer by Simple V-Y lap ESA TAAN,.D.; AYAN ARHAT,.D.; OUSTAA EKY,.D. and AHOUD NASI,.D. The Department of
Egypt, J. Plast. Reconstr. Surg., Vol. 40, No. 1, January: 97-101, 2016 Closure of Chronic Heel Ulcer by Simple V-Y lap ESA TAAN,.D.; AYAN ARHAT,.D.; OUSTAA EKY,.D. and AHOUD NASI,.D. The Department of
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion
 CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
The Lower Limb VI: The Leg. Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa
 The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
The gastrocnemius with soleus bi-muscle flap
 The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
Pedicled medial sural perforator flap for the reconstruction of knee defects
 International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Pedicled medial sural perforator flap for the reconstruction of knee defects I-Han Chiang 1, Chia-Chun Wu 2, Shyi-Gen Chen 1 & Chih-Hsin Wang
International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Pedicled medial sural perforator flap for the reconstruction of knee defects I-Han Chiang 1, Chia-Chun Wu 2, Shyi-Gen Chen 1 & Chih-Hsin Wang
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction
 Original Article Plastic and Aesthetic Research Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction Pradeoth Mukundan
Original Article Plastic and Aesthetic Research Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction Pradeoth Mukundan
Thomas Zgonis a, *, Douglas T. Cromack b, Thomas S. Roukis c, Joann Orphanos d, Vasilios D. Polyzois e CASE REPORT. Introduction.
 Injury Extra (2007) 38, 187 192 www.elsevier.com/locate/inext CASE REPORT Severe degloving injury of the sole and heel treated by a reverse flow sural artery neurofasciocutaneous flap and a modified off-loading
Injury Extra (2007) 38, 187 192 www.elsevier.com/locate/inext CASE REPORT Severe degloving injury of the sole and heel treated by a reverse flow sural artery neurofasciocutaneous flap and a modified off-loading
Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects
 Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects Osman Akdag, MD, a Mehtap Karamese, MD, a Muhammed NebilSelimoglu, MD, a Ahmet Akatekin, MD, a Malik Abacı,
Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects Osman Akdag, MD, a Mehtap Karamese, MD, a Muhammed NebilSelimoglu, MD, a Ahmet Akatekin, MD, a Malik Abacı,
Coverage of exposed hardware after lower leg fractures with free flaps or pedicled flaps
 European Review for Medical and Pharmacological Sciences 2015; 19: 4715-4721 Coverage of exposed hardware after lower leg fractures with free flaps or pedicled flaps N. FALLICO, F. SOMMA, E. CIGNA, L.A.
European Review for Medical and Pharmacological Sciences 2015; 19: 4715-4721 Coverage of exposed hardware after lower leg fractures with free flaps or pedicled flaps N. FALLICO, F. SOMMA, E. CIGNA, L.A.
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 6 Number 1 Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem S Tripathy,
ISPUB.COM The Internet Journal of Plastic Surgery Volume 6 Number 1 Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem S Tripathy,
Leg. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Anatomy MCQs Week 13
 Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
Contents of the Posterior Fascial Compartment of the Thigh
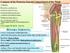 Contents of the Posterior Fascial Compartment of the Thigh 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t
Contents of the Posterior Fascial Compartment of the Thigh 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t
Distal Femoral Resection
 Distal Femoral Resection Annie Arteau, Bruno Fuchs Introduction This text is a general description of a distal femoral resection. Focus is on anatomical structures and muscle resection. Each femoral resection
Distal Femoral Resection Annie Arteau, Bruno Fuchs Introduction This text is a general description of a distal femoral resection. Focus is on anatomical structures and muscle resection. Each femoral resection
Knee Disarticulation Amputation
 Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
The free thoracodorsal artery perforator flap in head and neck reconstruction
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
موسى صالح عبد الرحمن الحنبلي أحمد سلمان
 8 موسى صالح عبد الرحمن الحنبلي أحمد سلمان 1 P a g e Today we will talk about a new region, which is the leg. And as always, we will start with studying the sensory innervation of the leg. What is the importance
8 موسى صالح عبد الرحمن الحنبلي أحمد سلمان 1 P a g e Today we will talk about a new region, which is the leg. And as always, we will start with studying the sensory innervation of the leg. What is the importance
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Wound Coverage Techniques for the Injured Extremity
 Wound Coverage Techniques for the Injured Extremity Gil Ortega, MD, MPH Sonoran Orthopaedic Trauma Surgeons Site Director, Phoenix Orthopaedic Residency Program Scottsdale Healthcare Trauma Center Scottsdale,
Wound Coverage Techniques for the Injured Extremity Gil Ortega, MD, MPH Sonoran Orthopaedic Trauma Surgeons Site Director, Phoenix Orthopaedic Residency Program Scottsdale Healthcare Trauma Center Scottsdale,
S-shaped reverse sural flap for reconstruction of tissue defect on heel
 Burns & Trauma, June 2013, Vol 1, Issue 1 Case Report S-shaped reverse sural flap for reconstruction of tissue defect on heel Hamid Reza Fathi, Mehdi Fathi, Mihan J. Javid 1 Departments of Plastic and
Burns & Trauma, June 2013, Vol 1, Issue 1 Case Report S-shaped reverse sural flap for reconstruction of tissue defect on heel Hamid Reza Fathi, Mehdi Fathi, Mihan J. Javid 1 Departments of Plastic and
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
The Transtibial Amputation
 The Transtibial Amputation Site of Previous Surgeries: Amputation indication: four unsuccessful previous surgeries. Patient experiences chronic pain and disfunction along with a limited range of motion.
The Transtibial Amputation Site of Previous Surgeries: Amputation indication: four unsuccessful previous surgeries. Patient experiences chronic pain and disfunction along with a limited range of motion.
~, /' ~::'~ EXTENSOR HALLUCIS LONGUS. Leg-anterolateral :.:~ / ~\,
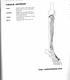 TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION. Adequate speech and swallowing are dependent
 ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
Transtibial Amputation with Extended Flap and Bone Bridging
 Transtibial Amputation with Extended Flap and Bone Bridging Pre-Op Plan: Amputation indication: four years status post a crush injury to his left foot. Patient experiences chronic pain and dysfunction
Transtibial Amputation with Extended Flap and Bone Bridging Pre-Op Plan: Amputation indication: four years status post a crush injury to his left foot. Patient experiences chronic pain and dysfunction
Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle
 Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
1-Muscles: 2-Blood supply: Branches of the profunda femoris artery. 3-Nerve supply: Sciatic nerve
 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t r i n g p a r t o r i s c h i a l p a r t ) 2-Blood supply:
1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t r i n g p a r t o r i s c h i a l p a r t ) 2-Blood supply:
Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps
 e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
Medial elbow reconstruction with perforator based medial arm propeller flap
 Case Report Hand Microsurg 2018;7:58-62 doi:10.5455/handmicrosurg.250701 Medial elbow reconstruction with perforator based medial arm propeller flap Asim Uslu 1, Abdullah Surucu 1, Mehmet Ali Korkmaz 1,
Case Report Hand Microsurg 2018;7:58-62 doi:10.5455/handmicrosurg.250701 Medial elbow reconstruction with perforator based medial arm propeller flap Asim Uslu 1, Abdullah Surucu 1, Mehmet Ali Korkmaz 1,
Distally Based Fasciocutaneous Flaps In the Management of Soft Tissue War Injuries of the Lower Half of the Leg
 THE Distally IRAQI Based POSTEGRADUTE Fasciocutaneous Flaps MEDICAL JOURNAL Tariq Abdul Qadir, etal. Distally Based Fasciocutaneous Flaps In the Management of Soft Tissue War Injuries of the Lower Half
THE Distally IRAQI Based POSTEGRADUTE Fasciocutaneous Flaps MEDICAL JOURNAL Tariq Abdul Qadir, etal. Distally Based Fasciocutaneous Flaps In the Management of Soft Tissue War Injuries of the Lower Half
Perforator flaps for reconstruction of lower limb defects
 International Surgery Journal Yasir M et al. Int Surg J. 2016 Nov;3(4):2109-2114 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163583
International Surgery Journal Yasir M et al. Int Surg J. 2016 Nov;3(4):2109-2114 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163583
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
A systematic approach to the failed plastic surgical reconstruction of the diabetic foot
 æiefs PROCEEDINGS A systematic approach to the failed plastic surgical reconstruction of the diabetic foot Ioannis I. Ignatiadis, MD, PhD 1 *, Vassiliki A. Tsiampa, MD 2 and Apostolos E. Papalois, PhD
æiefs PROCEEDINGS A systematic approach to the failed plastic surgical reconstruction of the diabetic foot Ioannis I. Ignatiadis, MD, PhD 1 *, Vassiliki A. Tsiampa, MD 2 and Apostolos E. Papalois, PhD
FUNCTION-SPARING TIBIALIS ANTERIOR PIVOTED MUSCLE FLAP FOR RECONSTRUCTION OF POST-BURN AND POST-TRAUMATIC MIDDLE-THIRD LEG DEFECTS WITH EXPOSED TIBIA
 FUNCTION-SPARING TIBIALIS ANTERIOR PIVOTED MUSCLE FLAP FOR RECONSTRUCTION OF POST-BURN AND POST-TRAUMATIC MIDDLE-THIRD LEG DEFECTS WITH EXPOSED TIBIA Megahed M.A.* Plastic, Reconstructive and Burn Unit,
FUNCTION-SPARING TIBIALIS ANTERIOR PIVOTED MUSCLE FLAP FOR RECONSTRUCTION OF POST-BURN AND POST-TRAUMATIC MIDDLE-THIRD LEG DEFECTS WITH EXPOSED TIBIA Megahed M.A.* Plastic, Reconstructive and Burn Unit,
Superficial lateral sural artery free flap for intraoral reconstruction: Anatomic study and clinical implications
 ORIGINAL ARTICLE Superficial lateral sural artery free flap for intraoral reconstruction: Anatomic study and clinical implications Klaus-Dietrich Wolff, MD, DDS, PhD, 1 Florian Bauer, MD, DDS, 1 Sebastian
ORIGINAL ARTICLE Superficial lateral sural artery free flap for intraoral reconstruction: Anatomic study and clinical implications Klaus-Dietrich Wolff, MD, DDS, PhD, 1 Florian Bauer, MD, DDS, 1 Sebastian
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
The lumbar artery perforator based island flap: anatomical study and case reports
 British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery
 Original Article Page 1 of 8 Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery Yuanbo Liu, Mengqing Zang, Shan Zhu, Bo Chen, Shanshan Li, Bingjian
Original Article Page 1 of 8 Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery Yuanbo Liu, Mengqing Zang, Shan Zhu, Bo Chen, Shanshan Li, Bingjian
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Original Article Fasciocutaneous flaps in reconstruction of lower extremity: our experience
 Kathmandu University Medical Journal (2004) Vol. 2, No. 4, Issue 8, 344-348 Original Article Fasciocutaneous flaps in reconstruction of lower extremity: our experience Chittoria R 1 Mishra SM 2 1 Assoc.
Kathmandu University Medical Journal (2004) Vol. 2, No. 4, Issue 8, 344-348 Original Article Fasciocutaneous flaps in reconstruction of lower extremity: our experience Chittoria R 1 Mishra SM 2 1 Assoc.
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
Original Article Fasciocutaneous sural nerve flap for lower extremity reconstruction: include or exclude the sural nerve?
 Int J Clin Exp Med 2016;9(11):22289-22295 www.ijcem.com /ISSN:1940-5901/IJCEM0022111 Original Article Fasciocutaneous sural nerve flap for lower extremity reconstruction: include or exclude the sural nerve?
Int J Clin Exp Med 2016;9(11):22289-22295 www.ijcem.com /ISSN:1940-5901/IJCEM0022111 Original Article Fasciocutaneous sural nerve flap for lower extremity reconstruction: include or exclude the sural nerve?
Flaps vs Grafts. Ronen Avram, MD MSc FRCSC
 Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Microvascular reconstruction of traumatic defects requires
 The Journal of TRAUMA Injury, Infection, and Critical Care The Utility of the Anterolateral Thigh Donor Site in Reconstructing the United States Trauma Patient Eduardo D. Rodriguez, DDS, MD, Gedge D. Rosson,
The Journal of TRAUMA Injury, Infection, and Critical Care The Utility of the Anterolateral Thigh Donor Site in Reconstructing the United States Trauma Patient Eduardo D. Rodriguez, DDS, MD, Gedge D. Rosson,
Lower Limb Nerves. Clinical Anatomy
 Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System.
 Case Report Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System. Reconstruction of a Maxillary Oncologic Defect
Case Report Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System. Reconstruction of a Maxillary Oncologic Defect
The Leg. Prof. Oluwadiya KS
 The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
Femoral Artery. Its entrance to the thigh Position Midway between ASIS and pubic symphysis
 Lower Limb Vessels Lecture Objectives Describe the major arteries of the lower limb. Describe the deep and superficial veins of the lower limb. Describe the topographical relationships of the arteries
Lower Limb Vessels Lecture Objectives Describe the major arteries of the lower limb. Describe the deep and superficial veins of the lower limb. Describe the topographical relationships of the arteries
The Boomerang Flap in Managing Injuries of the Dorsum of the Distal Phalanx
 The Boomerang Flap in Managing Injuries of the Dorsum of the Distal Phalanx Shao-Liang Chen, M.D., Trong-Duo Chou, M.D., Shyi-Gen Chen, M.D., Tian-Yeu Cheng, M.D., Tim-Mo Chen, M.D., and Hsian-Jenn Wang,
The Boomerang Flap in Managing Injuries of the Dorsum of the Distal Phalanx Shao-Liang Chen, M.D., Trong-Duo Chou, M.D., Shyi-Gen Chen, M.D., Tian-Yeu Cheng, M.D., Tim-Mo Chen, M.D., and Hsian-Jenn Wang,
Management of a large post-traumatic skin and bone defect using an Ilizarov frame
 Acta Orthop. Belg., 2006, 72, 214-218 TECHNICAL NOTE Management of a large post-traumatic skin and bone defect using an Ilizarov frame Pieter D HOOGHE, Koen DEFOORT, Johan LAMMENS, Jos STUYCK From the
Acta Orthop. Belg., 2006, 72, 214-218 TECHNICAL NOTE Management of a large post-traumatic skin and bone defect using an Ilizarov frame Pieter D HOOGHE, Koen DEFOORT, Johan LAMMENS, Jos STUYCK From the
Amputations. Chapter 23
 Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Kuwabara, Kaoru; Nonaka, Takashi; H. Citation Journal of Clinical Urology, 7(5),
 NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
DISSECTION SCHEDULE. Session I - Hip (Front) & Thigh (Superficial)
 DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
Clinical teaching/experi ence. Lectures/semina rs/conferences Self-directed. learning. Clinical teaching/experi ence
 Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Soft Tissue Reconstruction of the Foot Using the Distally Based Island Pedicle Flap after Resection of Malignant Melanoma
 Original Article Clinics in Orthopedic Surgery 2010;2:244-249 doi:10.4055/cios.2010.2.4.244 Soft Tissue Reconstruction of the Foot Using the Distally Based Island Pedicle Flap after Resection of Malignant
Original Article Clinics in Orthopedic Surgery 2010;2:244-249 doi:10.4055/cios.2010.2.4.244 Soft Tissue Reconstruction of the Foot Using the Distally Based Island Pedicle Flap after Resection of Malignant
Surgical Anatomy of the Medial Sural Artery Perforator Flap
 555 Surgical Anatomy of the Medial Sural Artery Perforator Flap Man-Zhi Wong, M.B.B.S., M.R.C.S., M.Med. 1 Chin-Ho Wong, M.B.B.S., M.R.C.S., M.Med., F.A.M.S. 2 Bien-Keem Tan, M.B.B.S., F.R.C.S., F.A.M.S.
555 Surgical Anatomy of the Medial Sural Artery Perforator Flap Man-Zhi Wong, M.B.B.S., M.R.C.S., M.Med. 1 Chin-Ho Wong, M.B.B.S., M.R.C.S., M.Med., F.A.M.S. 2 Bien-Keem Tan, M.B.B.S., F.R.C.S., F.A.M.S.
EndoBlade Soft Tissue Release System
 Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Which of the following is characteristic of the inflammatory phase of wound healing?
 This open book exam is being provided to you as a study aid and as an outline to guide your reading. It will not be collected or graded. You are encouraged to discuss the questions below with the intern
This open book exam is being provided to you as a study aid and as an outline to guide your reading. It will not be collected or graded. You are encouraged to discuss the questions below with the intern
TRANSPOSITIONAL ADIPOFASCIAL FLAPS FOR COMPLICATED ACUTE FINGER INJURIES
 K.B. Poon, S.H. Chien, G.T. Lin, et al TRANSPSITINAL ADIPFASCIAL FLAPS FR CMPLICATED ACUTE FINGER INJURIES Kein Boon Poon, Song-Hsiung Chien, 1 Gau-Tyan Lin, 1 and Yin-Chih Fu 1 Department of rthopaedic
K.B. Poon, S.H. Chien, G.T. Lin, et al TRANSPSITINAL ADIPFASCIAL FLAPS FR CMPLICATED ACUTE FINGER INJURIES Kein Boon Poon, Song-Hsiung Chien, 1 Gau-Tyan Lin, 1 and Yin-Chih Fu 1 Department of rthopaedic
Jonathan A. Dunne, MBChB, MRCS, a Daniel J. Wilks, MBChB, MRCS, b and Jeremy M. Rawlins, MBChB, MPhil, FRCS (Plast) c INTRODUCTION
 CASE REPORT A Previously Discounted Flap Now Reconsidered: MatriDerm and Split-Thickness Skin Grafting for Tendon Cover Following Dorsalis Pedis Fasciocutaneous Flap in Lower Limb Trauma Jonathan A. Dunne,
CASE REPORT A Previously Discounted Flap Now Reconsidered: MatriDerm and Split-Thickness Skin Grafting for Tendon Cover Following Dorsalis Pedis Fasciocutaneous Flap in Lower Limb Trauma Jonathan A. Dunne,
Disclosures. The Expanding Role of Microvascular Reconstruction. Overview. Things they are a Changing. Surgical Advisory Board, Genentech Corp
 Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Which treatment? How I do a Maquet Osteotomy? Maquet: Maquet: Biomechanics. Maquet: /21/10. Philippe Landreau, MD
 Which treatment? How I do a Maquet Osteotomy? Philippe Landreau, MD Paris, France And if the patient is young?! Anterior displacement of the tibial tuberosity design to reduce the joint reactive force
Which treatment? How I do a Maquet Osteotomy? Philippe Landreau, MD Paris, France And if the patient is young?! Anterior displacement of the tibial tuberosity design to reduce the joint reactive force
Anterior and Medial compartments of the thigh. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Anterior and Medial compartments of the thigh Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Terms Related to Movements Movement Flexion Extension Abduction Adduction Medial (internal)
Anterior and Medial compartments of the thigh Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Terms Related to Movements Movement Flexion Extension Abduction Adduction Medial (internal)
Initial management of war wounds with fractures
 Initial management of war wounds with fractures Presented by Paul Ley ICRC orthopedic surgeon Beirut, Lebanon May 12, 2017 BONE FRACTURES CANNOT BE CONSIDERED AS AN ISOLATED LESION SURROUNDING SOFT TISSUES
Initial management of war wounds with fractures Presented by Paul Ley ICRC orthopedic surgeon Beirut, Lebanon May 12, 2017 BONE FRACTURES CANNOT BE CONSIDERED AS AN ISOLATED LESION SURROUNDING SOFT TISSUES
Reintroducing the latissimus-rib free flap as a long bone substitute in the reconstruction of lower extremity injuries
 Case report Medical Journal of the Islamic Republic of Iran.Vol. 22, No. 2, August 2008. pp.104-110 Reintroducing the latissimus-rib free flap as a long bone substitute in the reconstruction of lower extremity
Case report Medical Journal of the Islamic Republic of Iran.Vol. 22, No. 2, August 2008. pp.104-110 Reintroducing the latissimus-rib free flap as a long bone substitute in the reconstruction of lower extremity
A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity
 Original Article Page 1 of 7 A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity Limin Qing, Panfeng Wu, Zhouzheng Bing, Fang Yu,
Original Article Page 1 of 7 A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity Limin Qing, Panfeng Wu, Zhouzheng Bing, Fang Yu,
Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve
 Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve 2. Gluteus Maximus O: ilium I: femur Action: abduct the thigh Nerve:
Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve 2. Gluteus Maximus O: ilium I: femur Action: abduct the thigh Nerve:
