Revision Surgical Technique
|
|
|
- Marsha McCormick
- 5 years ago
- Views:
Transcription
1 TOTAL KNEE SYSTEM Revision Surgical Technique
2
3 GENESIS II Revision Surgical Technique TABLE OF CONTENTS Introduction Preop Planning Short Technique Tibial Preparation Femoral Preparation Patellar Preparation Component Implantation Nota Bene: The technique description herein is made available to the healthcare professional to illustrate the authors suggested treatment for the uncomplicated procedure. In the final analysis, the preferred treatment is that which addresses the needs of the patient.
4 INTRODUCTION T he GENESIS II Total Knee System has been designed to offer the orthopaedic surgeon solutions to address intraoperative situations. Implant function is directly related to accurate surgical technique. The GENESIS II instrumentation has been developed to be an easy-to-use system that will assist the surgeon in obtaining accurate and reproducible knee alignment. The use of patent pending locking cams and quick connects will save time and allow the surgeon to easily align cutting blocks and assemble instrumentation. The patented intramedullary reference guide for the femoral cuts makes even the most difficult revision case a little easier. The angled/stepped hemi-wedge guide takes the Ramon B. Gustilo, M.D., P.A. Professor of Orthopaedic Surgery University of Minnesota Director of Orthopaedic Learning Center Hennepin County Medical Center Minneapolis, Minnesota Contributing Clinicians Steven B. Haas, M.D., MPH Assistant Professor of Orthopaedic Surgery Cornell University Medical College Attending Orthopaedic Surgeon The Hospital for Special Surgery New York, New York guesswork out of making wedge cuts with guides for 20 and 30 angled wedges and 10 mm and 15 mm stepped wedges. Trial stems and wedges attach directly to the femoral finishing block to provide the most accurate cuts possible and optimize implant fit. The same stem and wedge trials mate with the corresponding implant trial so that fit can be confirmed prior to cementing. While it has been the designer s objective to develop accurate, easy-to-use instrumentation, each surgeon must evaluate the appropriateness of the following technique based on his or her medical training, experience, and patient evaluation. Mark A. Snyder, M.D. Clinical Instructor University of Cincinnati Orthopaedic Surgeon Christ Hospital Cincinnati, Ohio Richard S. Laskin, M.D. Professor of Clinical Orthopaedic Surgery Cornell University Medical College Attending Orthopaedic Surgeon The Hospital for Special Surgery New York, New York James A. Rand, M.D. Professor of Orthopaedic Surgery Mayo Medical School Consultant in Orthopaedics Mayo Clinic Scottsdale Scottsdale, Arizona Robert B. Bourne, M.D., F.R.C.S.C. Chief of Orthopaedic Surgery University Hospital The University of Western Ontario London, Ontario, Canada Michael Ries, M.D. Clinical Assistant Professor of Orthopaedic Surgery S.U.N.Y. Stony Brook Attending Orthopaedic Surgeon The Mary Imogene Bassett Hospital Cooperstown, New York G. Lynn Rasmussen, M.D. Clinical Instructor Department of Orthopaedics University of Utah Co-Director Total Joint Replacement Orthopaedic Specialty Hospital Salt Lake City, Utah Jan Victor, M.D. Department of Orthopaedics St. Lucas Hospital Brugge, Belgium Todd V. Swanson, M.D. Desert Orthopaedic Center Las Vegas, Nevada John A. L. Hart, M.B.B.S., F.R.A.C.S. Senior Lecturer, Department of Surgery Monash University Senior Orthopaedic Surgeon Alfred Hospital Melbourne, Australia Craig G. Mohler, M.D. Orthopaedic and Fracture Clinic of Eugene Sacred Heart Medical Center Eugene, Oregon William B. Smith, M.D. Assistant Clinical Professor in Orthopaedic Surgery Medical College of Wisconsin Columbia Hospital Milwaukee, Wisconsin Kurt E. Blasser, M.D. Instructor of Orthopaedic Surgery Mayo Medical School Consultant in Orthopaedics Mayo Clinic Jacksonville Jacksonville, Florida J. Patrick Evans, M.D. Clinical Professor of Orthopaedic Surgery University of Oklahoma Chief of Staff Bone & Joint Hospital Oklahoma City, Oklahoma 2
5 PREOP PLANNING D etermine the approximate size of the femoral and tibial components as well as the length and diameter of any long stems to be used. Bone defects can also be templated to determine approximate size needed. This can be accomplished by using long standing A-P and lateral X-rays of both the involved and uninvolved extremities with radiographic markers for magnification. Recommended GENESIS II Sawblade: M Stryker Amsco-Hall New Stryker or a.050 or 1.27 mm Thickness Sawblade 3
6 SHORT TECHNIQUE Note: The insert shown is for illustration purposes only. Actual implants will vary. 1 After making the pilot hole into the tibial canal, ream 2 Attach the long-stem extractor rod to the appropriate the canal until cortical contact is achieved using progressively larger diameter long-stem reamers. tibial trial stem (same diameter as last reamer used) and insert into the tibial intramedullary canal. 5 After assessing the level of resection, resect the proximal 6 After opening the femoral intramedullary canal, ream the tibia. canal until cortical contact is achieved using progressively larger diameter stem reamers. 4 9 Pin the Revision A-P cutting block to the distal femur. 10 Attach the femoral trial stem adapter to the correctly Remove the revision distal femoral cutting block from the revision A-P cutting block and resect the posterior and anterior condyles over the surface of the cutting block. sized housing resection block. Attach the correct trial stem to the adapter. Add any distal or posterior wedges to the housing resection block.
7 SHORT TECHNIQUE 3 Attach the correct left or right tibial cutting block to the 4 Attach the revision tibial stylus to the tibial cutting intramedullary tibial alignment guide and place the I/M alignment guide over the long-stem extractor rod. block. Lower the cutting block until the stylus touches the side of the proximal tibia with the least amount of bone loss. Pin the cutting block to the tibia. 7 Add the revision cutting block stem adapter to the correctly 8 The revision distal femoral cutting block is attached to sized revision A-P cutting block. Attach the correct trial stem to the stem adapter and insert the trial into the intramedullary canal. the revision A-P cutting block. Place the revision A-P cutting block in the correct neutral rotational alignment and pin the revision distal femoral cutting block to the anterior cortex. Now the distal femoral resection is performed. 11 After pinning the housing resection block to the distal 12 Attach the revision housing resection collet to the housing resection block. Attach the housing reamer dome to the femur, remove the trial stem adapter and stem trial from the intramedullary canal. patellar reamer shaft and ream through the appropriate collet. 5
8 SHORT TECHNIQUE 13 Impact the housing box chisel/sizer through the appropriate collet until the stop hits the collet. through the chamfer slots in the housing resection 14 Perform the anterior and posterior chamfer resections block. 17 Properly position the appropriate tibial wedge resection 18 Pin the resection block to the tibia and remove the block against the anterior tibia. modular handle and tibial trial assembly. Resect the proximal tibia to accept the appropriate wedge. 21 Insert cement onto the distal surface of the femur and 22 Using the tibial insertion tool, fully seat the tibial articular onto the posterior aspect of the femoral prosthesis. Insert the insert. femoral implant into position. 6
9 SHORT TECHNIQUE 15 Measure the patellar thickness and determine correct 16 Assemble the appropriate tibial trials and seat this patellar implant. Attach the correct patellar reamer to the assembly onto the proximal tibia. patellar reamer shaft. Ream the patella until an adequate bed is prepared. Be careful not to over ream! 19 After inserting the appropriate femoral, tibial, and patellar trials, gently perform a trial range of motion to ascertain patellar implant onto the prepared surface of the patella. 20 After cementing the tibial baseplate in place, cement the proper joint tension and patellar tracking. 7
10 TIBIAL PREPARATION STEP 1: TIBIAL ALIGNMENT O bjective Align the resection for the tibial baseplate perpendicular to the mechanical axis. The following describes the technique for intramedullary tibial alignment, which is recommended for long-stem surgery. If extramedullary tibial alignment is preferred, the extramedullary tibial alignment technique follows on page 10. Figure 1 OPTION A: INTRAMEDULLARY TIBIAL ALIGNMENT Make a 9.5 mm pilot hole into the tibial canal. This can be made through the tibial drill guide with the IM tibial collet in place to ascertain correct placement (Figure 1). Using progressively larger diameter long-stem reamers, ream the tibial canal until cortical contact is achieved. Longstems are offered in 100, 150, and 200 mm lengths. Each reamer is marked with these different lengths (Figure 2). Attach the long-stem extractor rod to the appropriate tibial trial stem (same diameter as last reamer used) and insert into the tibial intramedullary canal (Figure 3). Figure 2 Figure 3 8
11 TIBIAL PREPARATION Figure The cannulated alignment sleeve of the intramedullary tibial alignment assembly is placed over the long-stem extractor rod. The intramedullary tibial alignment assembly is rotated until the alignment rod is centered over the medial third of the tibial tubercle. Rotational alignment is critical due to the 3 posterior sloped cut. The center of the cutting block will also be the center of the tibial tray and articular surface. The rotational orientation is locked in place by impacting the proximal end of the cannulated alignment sleeve to drive the distal spikes into the proximal tibia (Figure 4). Attach the correct left or right tibial cutting block to the intramedullary tibial alignment guide (Figure 5). Figure 5 9
12 TIBIAL PREPARATION OPTION B: EXTRAMEDULLARY TIBIAL ALIGNMENT Assemble the extramedullary tibial alignment guide and place the guide onto the tibia (Figure 6). Make sure that the correct left or right tibial cutting block is chosen and that the alignment guide is correctly set distally for the left or right leg. Impact the longer spike of the spiked fixation rod into the proximal tibia. Assess rotation of the alignment guide and slope of the cutting plane and impact the second spike to secure the assembly. Rotational alignment is critical due to the 3 posterior sloped cut. The center of the cutting block will also be the center of the tibial tray and articular surface. The goal is to align the extramedullary alignment assembly rotationally so that it aligns over the medial third of the tibial tubercle and over the center of the ankle. The slope can be adjusted according to the patient s anatomy. However, if a long-stem is needed, the extramedullary rod should be parallel to the tibial shaft. Note: 4 of slope is built into the articular insert and 3 of slope is built into the tibial cutting block. Figure 6 10
13 TIBIAL PREPARATION STEP 2: TIBIAL RESECTION O bjective Resect a minimal amount of bone from the proximal tibia while providing a good foundation for implant fixation. Figure Attach the revision tibial stylus to the tibial cutting block. Lower the cutting block until the stylus touches the side of the proximal tibia with the least amount of bone loss (Figure 7). The revision stylus will remove 1 mm from this point. In case of bony defects, it may be necessary to adjust the cutting level proximal to or above the level of maximum bone loss and to subsequently bone graft the defect or use an augmentation wedge. Insert pins through the central holes to secure the tibial cutting block to the tibia (Figure 8). Remove the alignment assembly leaving the tibial cutting block on the anterior tibia (Figure 9). Figure 8 Figure 9 11
14 TIBIAL PREPARATION 4 5 Attach the quick connect handle to the tibial cutting block. Pass the alignment rod through the hole in the handle to check tibial alignment (Figure 10). Resect the proximal tibia with a GENESIS II Sawblade (Figure 11). Note: A modular slot can be added to the nonslotted tibial cutting block or permanently slotted tibial cutting blocks are available. The GENESIS II Sawblades are specifically manufactured to fit these slots so as to provide a more precise resection. Figure 10 Figure 11 12
15 STEP 3: TIBIAL SIZING TIBIAL PREPARATION O bjective Select the appropriate size tibial implant and prepare for long-stem if extramedullary alignment was used. Figure 12 Figure Use the tibial viewing template to determine the tibial implant size that best fits the proximal tibia (Figure 12). Note: If extramedullary tibial alignment has been used, proceed with the following steps. If intramedullary tibial alignment has been used, proceed to Step 4. Select the appropriate tibial drill guide and place it on the proximal tibia. Once the tibial drill guide has been centralized on the proximal tibia, pin the drill guide in place. Ream the tibial intramedullary canal using progressively larger diameter tibial collets and reamers until cortical contact is made. Long-stems are available in 100, 150, and 200 mm lengths. Each reamer is marked with these lengths (Figure 13). Remove the tibial drill guide. Perform a trial seating of the tibial trial with the tibial trial stem attached (same size as last reamer used) to be sure that the implant will seat correctly. 13
16 FEMORAL PREPARATION STEP 1: INTRAMEDULLARY FEMORAL ALIGNMENT O bjective Align the distal femoral resection at the correct valgus angle using the femoral canal as the primary reference If necessary, open the femoral intramedullary canal using the 9.5 mm femoral drill (Figure 14). Using progressively larger diameter stem reamers, ream the femoral intramedullary canal until cortical contact is achieved (Figure 15). Stems are available in 100, 150, and 200 mm lengths. Each reamer is marked with these lengths. Note: Because of the internal dimensions, each size femoral component has a maximum allowable diameter of femoral stem that can be used. The limitations are as follows: Femoral Maximum Component Size Stem Diameter Remove the reamer and note diameter and length. Add the revision cutting block stem adapter to the correctly sized revision A-P cutting block. The revision A-P cutting blocks are the same size M-L as the implants. Make sure that the distal end of the stem adapter points to the correct indication for a left or right knee. Attach the correct trial stem to the stem adapter (Figure 16). Handles may be connected to the revision cutting block, if necessary. Insert the trial stem into the intramedullary canal until the revision A-P cutting block touches the distal femur. Do not affix the cutting block to bone at this time. Figure 14 Figure 15 Figure 16 14
17 FEMORAL PREPARATION STEP 2: DISTAL FEMORAL RESECTION O bjective Resect the distal femur at the correct valgus angle. Figure 17 Figure 18 Figure Attach the revision distal femoral cutting block to the anterior surface of the revision A-P cutting block (Figure 17). Place the revision A-P cutting block in the correct neutral rotational alignment using the cut proximal tibia, the epicondyles, and the patellar groove as references. The revision distal femoral cutting block is pinned to the anterior cortex of the femur locking the rotational alignment of the cutting assembly (Figure 18). The resection check can be used on top of the anterior surface of the revision A-P cutting block to make sure that the anterior cortex will not be notched. Make the distal femoral resection. If the distal slot is used, 1.5 mm of bone will be removed from the distal femur. If a distal femoral wedge is needed to fill a bony defect, two more proximal slots are available for 5 and 10 mm distal femoral wedges (Figure 19). 15
18 FEMORAL PREPARATION STEP 3: ANTERIOR/POSTERIOR FEMORAL FINISHING RESECTIONS O bjective Perform final anterior and posterior resections to prepare the femur for the femoral implant. Figure Before the pins are removed from the revision distal femoral cutting block, pin the revision A-P cutting block to the distal femur. This will ensure that the rotational orientation and level of resection does not change (Figure 20). Remove the revision distal femoral cutting block from the revision A-P cutting block. Resect the posterior condyles over the posterior surface of the revision A-P cutting block. If wedges are needed to fill bony defects, two more posterior slots are available for 5 and 10 mm augmentation wedges (Figure 21). Perform the anterior cut (Figure 22). Figure 21 Figure 22 16
19 FEMORAL PREPARATION STEP 4: FEMORAL HOUSING AND CHAMFER RESECTIONS O bjective Perform the housing and chamfer resections for either the posterior stabilized or constrained femoral implants. Figure 23 Figure 24 Figure If a stem is to be used, attach the femoral trial stem adapter to the correspondingly sized housing resection block. The correct trial stem is connected to the femoral trial stem adapter. Any distal or posterior wedges that have been prepared should also be added to the housing resection block to ensure proper reaming depth for housing. The wedges are magnetized and automatically adhere to the cutting block (Figure 23). Insert the trial stem into the femoral intramedullary canal and impact the housing resection block until it contacts the distal aspect of the femur. The housing resection block can be anchored to the femur with drill bits or bone spikes (Figure 24). Remove the femoral trial stem adapter and trial stem from the housing resection block and the femoral intramedullary canal after the housing resection block is pinned into place. This can be accomplished by loosening the screw attachment of the femoral trial stem adapter and extracting the trial stem from the intramedullary canal with the universal extractor (Figure 25). 17
20 FEMORAL PREPARATION Attach the revision housing resection collet to the housing resection block by sliding the collet into the block from the posterior aspect of the central opening. This collet will prepare for a posterior stabilized with stem or a constrained femoral implant (Figure 26). Note: If a stem will not be needed and a primary posterior stabilized implant will be used, the primary posterior stabilized collet should be used in place of the revision housing collet. Attach the housing reamer dome to the patellar reamer shaft. The reamer dome is both an end-cutting and a side-cutting reamer. Ream through the appropriate collet (Figure 27). Ream until the automatic depth stop contacts the collet. Then move the reamer anterior and posterior until it contacts the automatic stop (Figure 28). Figure 26 Figure 27 Figure 28 18
21 FEMORAL PREPARATION Figure Impact the housing box chisel/sizer through the appropriate collet until the stop hits the collet. Depending upon implant size, this step might be needed twice in order to cover the full A-P dimension of the implant box. This will square off the corners of the housing (Figure 29). Perform the anterior and posterior chamfer resections through the chamfer slots in the housing resection block (Figure 30). Remove the housing resection block from the distal femur. Figure 30 19
22 PATELLAR PREPARATION STEP 1: PATELLAR RESECTION O bjective Prepare the patella for the patellar implant ensuring that the original thickness of the patella is restored Measure patellar thickness with the patellar calipers. Determine the correct design and diameter of patellar implant to be used. A resurfacing, Biconvex, or Revision Biconvex patellar implant may be chosen. The resurfacing patella is 9 mm thick and a sawblade or reamer can be chosen as a means of bony preparation. The Biconvex patella is 13 mm thick and the Revision Biconvex patella is 17 mm thick. A reamer is used to prepare for both Biconvex patellae. Select the correct diameter of patellar reamer collet and slide it into place on the patellar reamer guide. Attach the patellar reamer guide to the patella. Secure the patellar reamer guide on the patella by tightening the set screw (Figure 31). Figure 31 20
23 PATELLAR PREPARATION Figure Attach the correct patellar reamer to the patellar reamer shaft. Lower the assembly through the patellar reamer guide until the reamer dome contacts the patella (Figure 32). Note: The patellar reamer stop can be used to avoid over reaming. Once the patellar reamer is placed against the patella, the depth stop is dropped until it contacts the surface of the patellar reamer guide. The depth stop can then be backed off a couple of millimeters to allow for minimal reaming. Ream the patella until an adequate bed is prepared for the implant. After reaming is complete, remove the reamer guide and place the appropriate trial patellar button in the recess to check position and total thickness. If necessary, use a rongeur to remove any prominent patellar surface. If a resurfacing patellar prosthesis has been used, drill the three fixation holes at this time using the correctly sized resurfacing drill guide and resurfacing drill. Place the patellar trial and measure the thickness of the composite (Figure 33). Figure 33 21
24 COMPONENT IMPLANTATION STEP 1: FEMORAL TRIAL ASSEMBLY AND POSITIONING O bjective Correctly assemble the femoral trial and confirm proper fit on the femur Select the appropriately sized femoral trial. If a longstemmed conversion module is to be used, place it onto the posterior stabilized or cruciate retaining femoral trial at this time. The conversion module trial is held in place with augmentation lugs. These are placed through the distal aspect of the conversion module trial and threaded into the femoral trial. If distal and/or posterior femoral wedge trials are to be used, the trial wedges are magnetized and can be simply placed onto the femoral trial. Lastly, screw the correct trial stem onto the femoral trial. Impact the femoral trial onto the distal femur (Figure 34). Figure 34 22
25 COMPONENT IMPLANTATION STEP 2: TIBIAL TRIAL PLACEMENT AND TIBIAL WEDGE RESECTION O bjective Prepare for any tibial wedge augmentation and ensure proper fit of the tibial trial. Figure Place a towel or lap against the distal aspect of the femoral trial. Using a Hohmann or similar retractor, sublux the tibia anteriorly. Select the appropriate trial tibial base. If a tibial longstem is to be used, screw it onto the tibial trial at this time. Seat this assembly onto the proximal tibia (Figure 35). The tibial trial should be rotationally symmetric with the femoral trial in full extension with the extensor mechanism reduced. Make sure that the rotational marks on the femoral trial and the articular insert trial are aligned. Mark the rotation on the tibia and remove the articular insert trial. Use spikes through the tibial trial into the proximal tibia to lock the rotational orientation of the tibial trial (Figure 36). Figure 36 23
26 COMPONENT IMPLANTATION If tibial wedges will be used, select either the full tibial wedge or the angled/stepped tibial wedge resection block. Position the appropriate tibial wedge resection block and run a modular handle through the most proximal hole of the block and into the anterior portion of the tibial trial. This will properly position the tibial wedge resection block against the anterior tibia (Figure 37). Stabilize the tibial wedge resection block by placing pins through the block and into the tibia. The modular handle and tibial trial assembly are removed. Resect the proximal tibia over the surface of the tibial wedge resection block to prepare the bone for placement of a tibial wedge (Figure 38). Place the appropriate tibial wedge(s) onto the distal aspect of the tibial trial. Again, the trial wedges are magnetized so that they can be simply seated onto the trials. Replace the tibial trial assembly onto the proximal tibia. Replace any pins needed for stability and, using the appropriately sized fin punch, punch for the tibial fins (Figure 39). Figure 37 Figure 38 Figure 39 24
27 COMPONENT IMPLANTATION STEP 3: FINAL TRIAL SEATING/CHECK O bjective Confirm implant fit and function. Figure Place the correct tibial trial articular insert onto the tibial trial. Note: If a constrained prosthesis is to be used, it may be necessary to lock the constrained tibial articular insert trial to the trial baseplate using one of the constrained tibial articular trial screws provided. This will ensure a stable construct when assessing joint stability. Place the correct patellar trial onto the patella. With the trials in place, gently perform a trial range of motion to ascertain proper joint tension and patellar tracking (Figure 40). Note: If the joint is loose in flexion, it may be necessary to use the next larger size of femoral trial, adding posterior augmentation to fill the flexion space. If this is necessary, a narrower diameter stem may be needed to allow proper placement of the femoral trial onto the anterior cortex. If the joint is loose in extension, distal augmentation may be added to the femoral trial to fill the extension space. 25
28 COMPONENT IMPLANTATION 4 5 Add a modular handle onto the anterior surface of the tibial trial. With the knee in full extension, check the mechanical axis of the limb using the long alignment rod (Figure 41). Remove the trials. Note: Hold onto the side of the trials to help prevent the trial wedges from disassembly during removal extraction. Figure 41 STEP 4: IMPLANT ASSEMBLY O bjective Properly assemble all implants so that they will properly fit the bony resections made. 1 Choose the correctly sized femoral component, conversion module, wedges, stem, and patellar implant. Assemble them in the same manner that the trial was assembled. If distal wedges are chosen, use the lug that is packaged sterile along with the implant wedge. It is important to turn the torque wrench until you feel a break when tightening the femoral fixation lugs in place (Figure 42). Figure 42 26
29 COMPONENT IMPLANTATION Figure The femoral stem is attached to the femoral component via a Morse-type taper. If using a slotted stem, make sure that the rotational mark on the stem lines up with the rotational mark on the Morse-taper of the femoral implant. The stem should be impacted at least twice on a stable surface to ensure that the lock has been properly engaged (Figure 43). If posterior wedges are used, these will be cemented to the femoral component. The wedge cement clamp is used to hold the wedges in place until the cement has hardened (Figure 44). Note: All of the posterior femoral wedges, the tibial wedges, and the patellar implant can be cemented simultaneously to avoid wasting time and cement. Select the correctly sized tibial baseplate, tibial wedges, and stem. The tibial stem and wedges are assembled in the same manner as the femoral stem and posterior wedges. Figure 44 27
30 COMPONENT IMPLANTATION STEP 5: IMPLANTATION O bjective Place all implants into position so as to optimize implant function. 1 2 Sublux the tibia anteriorly using a Hohmann or similar retractor. Place cement onto the proximal tibia. Insert the tibial implant onto the proximal tibia and remove any excess cement. Place the correct trial tibial articular insert into the tibial baseplate and hold the limb in full extension until all cement hardens. Place cement onto the distal surface of the femur and onto the posterior aspect of the femoral prosthesis. Insert the femoral implant into position (Figure 45). Remove any excess cement. Note: It is important to remove all excess cement from the housing of the posterior stabilized or constrained implant. Figure 45 28
31 COMPONENT IMPLANTATION Figure 46 Figure If the patellar implant has not yet been cemented, do so at this time. Assemble the patellar cement clamp adapter to the patellar reamer guide. Apply bone cement to the patella. Place the patellar implant onto the prepared surface of the patella. Note: If using a resurfacing patellar implant, it is helpful to identify the three fixation holes drilled prior to positioning the patellar implant. This will help you to identify the correct rotational orientation of the implant. Clamp the patellar implant onto the bone and remove the extruded cement (Figure 46). Slide the tibial articular insert into the tibial baseplate as far posteriorly as possible, engaging the peripheral locking mechanism. Attach the tibial insertion tool to the tibial tray. Rotate the tool superiorly until the anterior lip of the articular insert is fully seated (Figure 47). Note: A mallet should not be used when inserting the polyethylene. A mallet can cause damage to the insert s locking mechanism. CLOSURE Close in the usual manner. 29
32 IMPORTANT MEDICAL INFORMATION Warnings and Precautions Smith & Nephew, Inc. Knee System For Cemented Use Only MATERIALS Femoral components and conversion modules are cobalt chromium alloy (ASTM F 75 and ISO 5832/4). Tibial trays are cobalt chromium alloy (ASTM F 75 and ISO 5832/4) or titanium 6Al-4V alloy (ISO 5832/3). Porous patellar bases are cobalt chromium alloy (ASTM F 75 and ISO 5832/4) or titanium 6Al-4V alloy (ISO 5832/3). Tibial and femoral wedges, tibial and femoral stems, screws, and pegs are titanium 6Al-4V alloy (ISO 5823/3) or stainless steel (ASTM F 745 and ISO 5832/1). Patellar components, all polyethylene tibial components, tibial component articular inserts, and Flex-Lok pegs are ultra-high molecular weight polyethylene (ASTM F 648). Components that are made of only polyethylene include X-ray marking wire made of stainless steel (ASTM F 138 and ISO 5832/1) or cobalt chromium (ASTM F 90). Porous coated cobalt chromium components feature a porous coating of cobalt chromium beads (ASTM F 75 and ISO 5832/4). Porous coated titanium components feature a porous coating of unalloyed titanium beads (ASTM F 67 and ISO 5832/2). The specific component material is listed on the outside carton label. Each total knee system is designed as a system and does not allow the substitution of components from other systems. All implantable devices are for single use. Some of the alloys needed to produce orthopaedic implants contain some metallic components that may be carcinogenic in tissue cultures or intact organisms under very unique circumstances. Questions have been raised in the scientific literature as to whether or not these alloys may be carcinogenic in implant recipients. Studies conducted to evaluate this issue have not identified convincing evidence of such phenomenon, in spite of the millions of implants in use. INDICATIONS, CONTRAINDICATIONS, AND ADVERSE EFFECTS The general principles of good patient selection and sound surgical judgment apply to the total knee procedure. Preoperative planning and meticulous surgical technique are essential to achieve optimum results. Considerations of anatomic loading, soft-tissue condition, and component placement are critical to minimize a variety of postoperative complications. Indications for Total Knee Replacement 1. Rheumatoid arthritis. 2. Post-traumatic arthritis, osteoarthritis, or degenerative arthritis in older patients whose age, weight, and activity level are compatible with an adequate long-term result. 3. Failed osteotomies, unicompartmental replacement, or total knee replacement. 4. Posterior stabilized knee systems and systems with a deep articular surface are designed for use in patients in primary and revision surgery, where the anterior and posterior cruciate ligaments are incompetent and the collateral ligaments remain intact. 5. The Tricon -M and Tricon-P Total Knee System can be implanted with or without cement; the Flex-Lok pegs are driven into cancellous bone to secure the components in place. 6. Constrained knee systems are designed for use in patients in primary and revision surgery, where the posterior cruciate ligament and one or both of the collateral ligaments (i.e. medial collateral and/or lateral collateral ligament) are absent or incompetent. Contraindications for Total Knee Replacement 1. Inadequate bony support or cement support. 2. Previous intra-articular infections. 3. Mental or neurologic conditions that tend to preempt the patient s ability or willingness to restrict activities. 4. Neuropathic (Charcot) joint. 5. Conditions that tend to place increased loads on implants such as age, weight, and activity level, which are incompatible with a satisfactory long-term result. 6. Use of slotted femoral and tibial stems without adequate bony support. 7. Collateral ligament insufficiency (except in cases where a constrained knee system is indicated and used). 8. Cementless application for the Tricon-M and Tricon-P Total Knee System is contraindicated with noncorrectable ligamentous laxity of the affected knee. 9. Skeletally immature patients. Conditions presenting increased risk of failure include: osteoporosis, metabolic disorders which may impair bone formation, and osteomalacia. Indications for Unicompartmental Knee Replacement 1. Post-traumatic arthritis, osteoarthritis, or degenerative arthritis in older patients whose age, weight, and activity level are compatible with an adequate long-term result. 2. Failed osteotomies. Contraindications for Unicompartmental Knee Replacement The contraindications for Unicompartmental Knee Replacement include all of the contraindications listed for Total Knee Replacement and also inflammatory arthritis, such as rheumatoid arthritis, gout, lupus, etc. Possible Adverse Effects 1. Wear of the polyethylene articulating surfaces of knee replacement components has been reported following total knee replacement. Higher rates of wear may be initiated by particles of cement, metal, or other debris which can cause abrasion of the articulating surfaces. Higher rates of wear may shorten the useful life of the prosthesis, and lead to early revision surgery to replace the worn prosthetic components. 2. With all joint replacements, asymptomatic, localized, progressive bone resorption (osteolysis) may occur around the prosthetic components as a consequence of foreign-body reaction to particulate matter. Particulate material is generated by interaction between components, as well as between the components and bone, primarily through wear mechanisms of adhesion, abrasion, and fatigue. Secondarily, particles can also be generated by thirdbody wear. Osteolysis can lead to future complications necessitating the removal and replacement of prosthetic components. See the Important Physician Information section for more information. 3. Loosening, bending, cracking, or fracture of femoral or tibial, or patellar components. 4. Dislocation, subluxation, excessive rotation, flexion contracture, decreased range of motion, lengthening or shortening of the leg, looseness of components, extraneous bone, or ligament laxity. 5. Tibial, femoral, or patellar fractures. 6. Acute post-surgical wound infection, late deep wound sepsis, and/or low-grade synovitis. 7. Neuropathies. 8. Cardiovascular disorders: wound hematoma, thromboembolic diseases including venous thrombosis, pulmonary embolus, or myocardial infarction. 9. Tissue reactions: Lysis, macrophage particles and foreign body reaction. Also myositis ossificans. 10. Skin sloughs or delayed wound healing. 11. Although rare, metal sensitivity reactions in patients following joint replacement have been reported. Implantation of foreign material in tissues can result in histological reactions involving macrophages and fibroblasts. 12. Implants can loosen or migrate due to trauma or loss of fixation. 13. While rare, fatigue fracture of the implant can occur as a result of trauma, strenuous activity, improper alignment, or duration of service. Implants can loosen or migrate due to trauma or loss of fixation. 14. Allergic reactions to the material utilized in the implants, although uncommon, can occur. 15. Damage to blood vessels. 16. Temporary or permanent nerve damage resulting in pain or numbness of the affected limb. 17. Varus-valgus deformity. 18. Delayed wound healing. 19. Periarticular calcification or ossification, with or without impediment to joint mobility. 20. Inadequate range of motion due to improper selection or positioning of components, or by periarticular calcification. 30
33 WARNINGS AND PRECAUTIONS The patient should be warned of surgical risks, and made aware of possible adverse effects. The patient should be warned that the device does not replace normal healthy bone, and that the implant can break or become damaged as a result of strenuous activity or trauma, and has a finite expected service life and may need to be replaced in the future. Preoperative 1. Use care in handling and storing of implant components. Cutting, bending, or scratching the surfaces of components can significantly reduce the strength, fatigue resistance and/or wear characteristics of the implant system. These in turn may induce internal stresses that are not obvious to the eye and may lead to fracture of the component. Do not allow the porous surfaces to come in contact with cloth or other fiber releasing material. 2. Surgical Technique Brochures are available upon request. The surgeon should be familiar with the technique. 3. An adequate inventory of implant sizes should be available at the time of surgery. 4. Intraoperative fracture or breaking of instruments can occur. Instruments which have experienced extensive use or excessive force are susceptible to fracture. Instruments should be examined for wear and damage prior to surgery. Intraoperative 1. The correct selection of the implant is extremely important. The appropriate type and size should be selected for patients with consideration of anatomical and biomechanic fractures such as patient age and activity levels, weight, bone and muscle conditions, and others: generally, the largest cross-section component which will allow adequate bone support to be maintained is preferred. Failure to use the optimum size component may result in loosening, bending, cracking, or fracture of the component and/or bone. 2. Improper selection, placement, positioning, and fixation of the implant components may result in unusual stress concentrations and a subsequent reduction in service life of the prosthetic implant. 3. Do not mix femoral, tibial, and patellar components of different prosthetic systems or from different manufacturers. Modular components must be assembled securely to prevent disassociation. Avoid repeated assembly and disassembly of the modular components which could compromise a critical locking action of the components. Surgical debris must be cleaned from components before assembly. Debris inhibits the proper fit and locking modular components which may lead to early failure of the procedure. 4. Adequate and continuous support of components by cement and bone and proper component size is important. 5. Proper alignment, axially and rotationally, is important. 6. Care is to be taken to assure complete support of all parts of the device embedded in bone cement to prevent stress concentration which may lead to failure of the procedure. During curing of cement, care should be taken to prevent movement of the implant components. 7. Fixation screws, when used, should be fully seated to assure stable fixation, and to avoid interference with the proper seating of components. Use only screws recommended by the manufacturer of the specific prosthesis to avoid improper fit, and to avoid improper mixing of metals. 8. Prior to closure, the surgical site should be thoroughly cleaned of bone chips, extraneous cement, ectopic bone, etc. Foreign particles at the metal and/or plastic interfaces may cause excessive wear and/or friction. 9. Posterior stabilized knee systems, constrained knee systems, and systems with a deep articular surface should not be utilized without significant adjunctive fixation (stems, screws, cement, etc). 10. It is essential that the patient s bone stock be of sufficient quality to support the plastic and metallic fixation pegs in the Tricon- M and Tricon-P Total Knee Systems. 11. An implant should never be reused. While it may appear undamaged, imperfection may exist which could reduce the service life of the implant. 12. Use the Richards Torque Wrench to secure the distal femoral wedges and the conversion modules to the GENESIS femoral component. The femoral lugs should be torqued to 70 in-lbs. Postoperative 1. Postoperative patient care and directions and warnings to patients by physicians are extremely important. Protected weight bearing with external support is recommended for a period of time to allow healing. 2. Use extreme care in patient handling. 3. Postoperative therapy should be structured to prevent excessive loading of the operative knee and to encourage bone healing. 4. Patients should be cautioned to limit their activities as directed by their surgeon. 5. Periodic, long-term follow-up is recommended to monitor the position and state of the prosthetic components, as well as the condition of the adjoining bone. Important Physician Information Bone resorption is a natural consequence of total joint arthroplasty due to changes in bone remodeling patterns. Bone remodeling is mediated by the changes in stress distribution caused by implantation. Extensive resorption around the prosthesis leads to implant loosening and failure. Progressive bone resorption due to reasons other than stress shielding or infection has been termed osteolysis. It is generally agreed that osteolysis is the result of localized foreign-body reaction to particulate debris generated by cement, metal, ultra high molecular weight polyethylene (UHMWPE), and ceramic. Regarding the etiology, it has been hypothesized that particulate debris generated by the components of a prosthesis migrate into the synovial cavity and the boneimplant interface, where they recruit macrophages and stimulate phagocytic action. The degree of recruitment is determined by the size, distribution, and amount of particulate debris (rate of debris generation). The phagocytic action results in the release of cytokines and intercellular mediators (IL-1, 2, PE2) which encourages osteoclastic bone resorption. Clinical and basic research is continuing in order to provide scientific basis for the causes of this phenomenon and potential ways to reduce its occurrence. Osteolysis can be asymptomatic, and, therefore, routine periodic radiographic examination is vital to prevent any serious future complication. Presence of focal lesions which are progressive may necessitate replacement of the prosthetic component(s). Packaging and Labeling Knee implants are sterilized products and should only be accepted if received by the hospital or surgeon with the factory packing and labeling intact. If the sterile barrier has been broken, refer to the Resterilization section below. STERILIZATION All metal components have been sterilized by a minimum of 25 kilograys of gamma irradiation. Plastic components have been sterilized by ethylene oxide gas. All components are supplied in protective trays. Inspect packages for punctures or other damage prior to surgery. RESTERILIZATION Metal Components Metal components may be resterilized, if necessary, by steam autoclaving in appropriate protective wrapping, after removal of all the original packaging and labeling. Protect prosthesis, particularly mating surfaces, from contact with metal or other hard objects. The following process parameters are recommended for these devices: Prevacuum cycle, 4 minutes at 132 to 135 C, followed by 20 minutes of drying time. If porous coated implants are inadvertently contaminated, return the unsoiled prosthesis to Smith & Nephew for resterilization. DO NOT RESTERILIZE porous coated implants. The porous coating requires special cleaning procedures. Plastic Components Plastic components may be resterilized by ethylene oxide gas, using the following procedures: Sterilant Temperature Humidity Maximum Concentration Exposure Pressure Time 88% Freon 130 O C % 21 psia mg/l 105 minutes 12% EtO or 40 60% 100 O C 50% 21 psia 650 mg/l 6 hours Suggested aeration time is 12 hours at 50 C with power aeration. Consult aerator manufacturer for more specific instructions. INFORMATION For further information, please contact Customer Service at Caution: Federal Law (USA) restricts this device to sale by or on the order of a physician /95 31
34 32
35
36 1997 Smith & Nephew, Inc. Patent numbers 4,950,298; 5,047,058; 5,053,037; 5,100,408; 5,282,803; 5,514,140; 5,354,075; 5,417,694, and 5,549,688. Additional patents pending. GENESIS, Flex-Lok and Tricon are registered trademarks of Smith & Nephew, Inc. This system is intended for cemented use only. 4/
Anterior Cut First Surgical Technique
 Anterior Cut First Surgical Technique GENESIS II Anterior Cut First Surgical Technique Table of Contents Introduction....................................... 2 Preop Planning....................................
Anterior Cut First Surgical Technique GENESIS II Anterior Cut First Surgical Technique Table of Contents Introduction....................................... 2 Preop Planning....................................
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Extramedullary Tibial Preparation
 Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique. VISIONAIRE FastPak Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
Surgical Technique. VISIONAIRE Disposable Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Important notice: the device(s) can be prescribed and implanted only by a doctor legally authorized to perform this type of surgery.
 rev.10 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH - EVOLIS/GMK KNEE PROSTHESIS - INSTRUCTIONS FOR USE Important notice: the device(s) can be prescribed
rev.10 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH - EVOLIS/GMK KNEE PROSTHESIS - INSTRUCTIONS FOR USE Important notice: the device(s) can be prescribed
Técnica Quirúrgica. Mejoramos su calidad de vida GENESIS II. Prótesis total de Rodilla
 Técnica Quirúrgica Mejoramos su calidad de vida GENESIS II Prótesis total de Rodilla INTRODUCTION T he GENESIS II Total Knee System has been designed to offer the orthopaedic surgeon solutions to address
Técnica Quirúrgica Mejoramos su calidad de vida GENESIS II Prótesis total de Rodilla INTRODUCTION T he GENESIS II Total Knee System has been designed to offer the orthopaedic surgeon solutions to address
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Description Materials Indications Patient selection factors to be considered include: Contraindications Absolute contraindications include:
 Description The Patello-Femoral Wave Arthroplasty Systems incorporate a distal femoral trochlear surface articular component that mates to a taper post via a taper interlock, and an all-polyethylene patella
Description The Patello-Femoral Wave Arthroplasty Systems incorporate a distal femoral trochlear surface articular component that mates to a taper post via a taper interlock, and an all-polyethylene patella
REPIPHYSIS LIMB SALVAGE SYSTEM
 REPIPHYSIS LIMB SALVAGE SYSTEM 150800-0 For additional information please contact the manufacturer or local distributor. M MicroPort Orthopedics Inc. 5677 Airline Rd Arlington, TN 38002 U.S.A. i Y October
REPIPHYSIS LIMB SALVAGE SYSTEM 150800-0 For additional information please contact the manufacturer or local distributor. M MicroPort Orthopedics Inc. 5677 Airline Rd Arlington, TN 38002 U.S.A. i Y October
Zimmer NexGen MIS Tibial Component. Cemented Surgical Technique IMAGE TO COME
 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
ANATOMIC SURGICAL TECHNIQUE. 5 in 1. Conventional instrumentation 07/11/2013
 ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
Technique Guide Small Bone Fusion System
 Technique Guide Small Bone Fusion System The Pinit Plate Small Bone Fusion System is a super low profile, modular bone plate and screw system designed to stabilize a bunionectomy with a medial to lateral
Technique Guide Small Bone Fusion System The Pinit Plate Small Bone Fusion System is a super low profile, modular bone plate and screw system designed to stabilize a bunionectomy with a medial to lateral
Pinit Plate Small Bone Fusion System Bone Plate & Screw System
 Pinit Plate Small Bone Fusion System Bone Plate & Screw System Description The Pinit Plate Small Bone Fusion System consists of 2-hole bone plates made available in three length options and two thickness
Pinit Plate Small Bone Fusion System Bone Plate & Screw System Description The Pinit Plate Small Bone Fusion System consists of 2-hole bone plates made available in three length options and two thickness
TC-PLUS Primary Knee IMPORTANT MEDICAL INFORMATION SPECIAL NOTE. This Package Insert is for product distributed in the US only.
 TC-PLUS Primary Knee IMPORTANT MEDICAL INFORMATION SPECIAL NOTE This Package Insert is for product distributed in the US only. The component material is provided on the outside carton label. Components
TC-PLUS Primary Knee IMPORTANT MEDICAL INFORMATION SPECIAL NOTE This Package Insert is for product distributed in the US only. The component material is provided on the outside carton label. Components
Lapidus Arthrodesis System Instructions for Use
 Lapidus Arthrodesis System Instructions for Use Description The AlignMATE Lapidus Arthrodesis System consists of bone plates and bone screws (locking, non-locking and interfragmentary), which are intended
Lapidus Arthrodesis System Instructions for Use Description The AlignMATE Lapidus Arthrodesis System consists of bone plates and bone screws (locking, non-locking and interfragmentary), which are intended
Positioning Sleeve Surgical Technique
 Positioning Sleeve Surgical Technique Surgical Technique The Comprehensive Fracture System offers a unique tool to evaluate and re-establish humeral height, which can be critical to restoring proper biomechanics
Positioning Sleeve Surgical Technique Surgical Technique The Comprehensive Fracture System offers a unique tool to evaluate and re-establish humeral height, which can be critical to restoring proper biomechanics
THE P.F.C. SIGMA FEMORAL ADAPTER. Surgical Technique
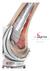 THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
WristMotion Wrist Hemiarthroplasty System Instructions for Use
 WristMotion Wrist Hemiarthroplasty System Instructions for Use Description The Arthrosurface WristMotion Wrist Hemiarthroplasty System consists of a contoured capitate articular implant designed to articulate
WristMotion Wrist Hemiarthroplasty System Instructions for Use Description The Arthrosurface WristMotion Wrist Hemiarthroplasty System consists of a contoured capitate articular implant designed to articulate
MIS Cemented Tibial Component
 MIS Cemented Tibial Component NexGen Complete Knee Solution Surgical Technique Table of Contents Surgical Exposure... 2 Finish the Tibia... 2 Position Based on Anatomic Landmarks... 3 Lateral Posterior
MIS Cemented Tibial Component NexGen Complete Knee Solution Surgical Technique Table of Contents Surgical Exposure... 2 Finish the Tibia... 2 Position Based on Anatomic Landmarks... 3 Lateral Posterior
Document No Rev. B Pg. 1 of 5 Approvals / Date Title: INSTRUCTIONS FOR USE DJO SURGICAL MODULAR REVISION HIP SYSTEM AND ACETABULAR CAGE
 Document No. 0400-0205 Rev. B Pg. 1 of 5 Approvals / Date Title: INSTRUCTIONS FOR USE DJO SURGICAL MODULAR REVISION HIP SYSTEM AND ACETABULAR CAGE Revision ECO Date ECO Summary of Changes Deann Rector
Document No. 0400-0205 Rev. B Pg. 1 of 5 Approvals / Date Title: INSTRUCTIONS FOR USE DJO SURGICAL MODULAR REVISION HIP SYSTEM AND ACETABULAR CAGE Revision ECO Date ECO Summary of Changes Deann Rector
- October 2013 English
 TOTAL HIP JOINT REPLACEMENT FOR CEMENTED APPLICATIONS FOR THE ATTENTION OF THE OPERATING SURGEON Total hip replacement provides the surgeon with a means of restoring mobility and reducing pain with the
TOTAL HIP JOINT REPLACEMENT FOR CEMENTED APPLICATIONS FOR THE ATTENTION OF THE OPERATING SURGEON Total hip replacement provides the surgeon with a means of restoring mobility and reducing pain with the
CAUTION: Ceramic liners are not approved for use in the United States.
 Total Hip Prostheses, Self-Centering Hip Prostheses and Hemi-Hip Prostheses IMPORTANT: This essential product information sheet does not include all of the information necessary for selection and use of
Total Hip Prostheses, Self-Centering Hip Prostheses and Hemi-Hip Prostheses IMPORTANT: This essential product information sheet does not include all of the information necessary for selection and use of
SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS
 SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS INTRODUCTION The Summit Tapered Hip System s comprehensive set of implants and instruments
SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS INTRODUCTION The Summit Tapered Hip System s comprehensive set of implants and instruments
EXACTECH KNEE. Operative Technique ADDENDUM. Metaphyseal Cones. Surgeon focused. Patient driven. TM
 EXACTECH KNEE Operative Technique ADDENDUM Metaphyseal Cones Surgeon focused. Patient driven. TM TABLE OF CONTENTS INTRODUCTION...1 DESCRIPTION...1 DETAILED OPERATIVE TECHNIQUE Initial Preparation and
EXACTECH KNEE Operative Technique ADDENDUM Metaphyseal Cones Surgeon focused. Patient driven. TM TABLE OF CONTENTS INTRODUCTION...1 DESCRIPTION...1 DETAILED OPERATIVE TECHNIQUE Initial Preparation and
Triathlon Knee System. Universal Baseplate Surgical Protocol
 Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments..........................................................2 Introduction...............................................................2
Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments..........................................................2 Introduction...............................................................2
TOTAL KNEE ARTHROPLASTY SYSTEM
 SURGICAL TECHNIQUE TOTAL KNEE ARTHROPLASTY SYSTEM 90-SRK-700000 B.0 0 Contents 1. Implant Sizing 2. Surgical Technique a. Incision and Exposure b. Distal Femoral Resection c. Tibial Resection d. Femoral
SURGICAL TECHNIQUE TOTAL KNEE ARTHROPLASTY SYSTEM 90-SRK-700000 B.0 0 Contents 1. Implant Sizing 2. Surgical Technique a. Incision and Exposure b. Distal Femoral Resection c. Tibial Resection d. Femoral
Triathlon Knee System
 Triathlon Knee System Express Instruments Surgical Protocol Posterior Stabilized & Cruciate Retaining TriathlonKneeSystem Express Instruments Surgical Protocol Acknowledgments..........................................................2
Triathlon Knee System Express Instruments Surgical Protocol Posterior Stabilized & Cruciate Retaining TriathlonKneeSystem Express Instruments Surgical Protocol Acknowledgments..........................................................2
Hip Resurfacing System
 Hip Resurfacing System The Arthrosurface HemiCAP Hip Hemiarthroplasty System restores the articular surface geometry of the femoral head and preserves functional structures using an innovative 3 dimensional
Hip Resurfacing System The Arthrosurface HemiCAP Hip Hemiarthroplasty System restores the articular surface geometry of the femoral head and preserves functional structures using an innovative 3 dimensional
Proven Gen-Flex Revision Knee System. Surgical Protocol
 Proven Gen-Flex Revision Knee System Surgical Protocol Proven Gen-Flex Revision Knee System Surgeon Design Team The Proven Gen-Flex Revision Knee System Instrumentation and Surgical Protocol were developed
Proven Gen-Flex Revision Knee System Surgical Protocol Proven Gen-Flex Revision Knee System Surgeon Design Team The Proven Gen-Flex Revision Knee System Instrumentation and Surgical Protocol were developed
Triathlon Knee System Universal Baseplate Surgical Protocol
 Triathlon Knee System Universal Baseplate Surgical Protocol Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments... 2 Introduction... 2 Assembly Instructions...
Triathlon Knee System Universal Baseplate Surgical Protocol Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments... 2 Introduction... 2 Assembly Instructions...
Surgical Technique. Anterior Cut First Surgical Technique
 Surgical Technique Anterior Cut First Surgical Technique Introduction The GENESIS II Total Knee System has been designed to offer the orthopaedic surgeon solutions to address intraoperative situations.
Surgical Technique Anterior Cut First Surgical Technique Introduction The GENESIS II Total Knee System has been designed to offer the orthopaedic surgeon solutions to address intraoperative situations.
Talar Dome System Surgical Technique
 Talar Dome System Surgical Technique CAP TALAR DOME RESURFACING HEMIARTHROPLASTY IMPLANT Surgical Technique Guide Description The HemiCAP Contoured Articular Prosthetic incorporates an articular resurfacing
Talar Dome System Surgical Technique CAP TALAR DOME RESURFACING HEMIARTHROPLASTY IMPLANT Surgical Technique Guide Description The HemiCAP Contoured Articular Prosthetic incorporates an articular resurfacing
Surgical Technique. Hinge Disassembly and Rebuild Technique
 Surgical Technique Hinge Disassembly and Rebuild Technique Revision Knee Arthroplasty Surgical Technique LEGION HK Hinge Knee System Introduction The LEGION HK Hinge Knee System has been designed as an
Surgical Technique Hinge Disassembly and Rebuild Technique Revision Knee Arthroplasty Surgical Technique LEGION HK Hinge Knee System Introduction The LEGION HK Hinge Knee System has been designed as an
Profix. Total Knee System. As described by
 Profix Total Knee System P R I M A R Y P R O C E D U R E As described by Leo A. Whiteside, M.D. Associate Research Professor Washington University School of Medicine Director, Biomechanical Research Laboratory
Profix Total Knee System P R I M A R Y P R O C E D U R E As described by Leo A. Whiteside, M.D. Associate Research Professor Washington University School of Medicine Director, Biomechanical Research Laboratory
Resurfacing Patellar Preparation
 Surgical Technique Resurfacing Patellar Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Resurfacing Patellar preparation Contents Introduction...2 Instrument assembly...3 Resurfacing
Surgical Technique Resurfacing Patellar Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Resurfacing Patellar preparation Contents Introduction...2 Instrument assembly...3 Resurfacing
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 2 Tibial Preparation... 2.1 Tibial Canal Preparation... 2.2 Proximal Tibial Resection... 2.3 Non Offset Tibial Preparation...
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 2 Tibial Preparation... 2.1 Tibial Canal Preparation... 2.2 Proximal Tibial Resection... 2.3 Non Offset Tibial Preparation...
CONSENSUS ORTHOPEDICS INC. CONSENSUS KNEE SYSTEM
 CONSENSUS ORTHOPEDICS INC. CONSENSUS KNEE SYSTEM IMPORTANT INFORMATION FOR SURGEON: PLEASE READ PRIOR TO IMPLANTING THIS DEVICE IN A CLINICAL SETTING. THE SURGEON SHOULD BE FAMILIAR WITH THE SURGICAL TECHNIQUE.
CONSENSUS ORTHOPEDICS INC. CONSENSUS KNEE SYSTEM IMPORTANT INFORMATION FOR SURGEON: PLEASE READ PRIOR TO IMPLANTING THIS DEVICE IN A CLINICAL SETTING. THE SURGEON SHOULD BE FAMILIAR WITH THE SURGICAL TECHNIQUE.
MRH Knee System Modular Peg Baseplate Surgical Protocol
 MRH Knee System Modular Peg Baseplate Surgical Protocol Using Monogram IM Revision Instruments 4 N 4 N Modular Rotating Hinge Knee System Using Monogram IM Revision Instruments Mr C R Howie FRCS Consultant
MRH Knee System Modular Peg Baseplate Surgical Protocol Using Monogram IM Revision Instruments 4 N 4 N Modular Rotating Hinge Knee System Using Monogram IM Revision Instruments Mr C R Howie FRCS Consultant
Zimmer NexGen Trabecular Metal Tibial Tray
 Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
NEXGEN COMPLETE KNEE SOLUTION S A. Tibial Stem Extension & Augmentation Surgical. ATechnique
 NEXGEN COMPLETE KNEE SOLUTION ATechnique Tibial Stem Extension & Augmentation Surgical INTRODUCTION The NexGen Complete Knee Solution Intramedullary Tibial Instruments have been designed to provide an
NEXGEN COMPLETE KNEE SOLUTION ATechnique Tibial Stem Extension & Augmentation Surgical INTRODUCTION The NexGen Complete Knee Solution Intramedullary Tibial Instruments have been designed to provide an
Encina Taper Stem. Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer
 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Doc. No.: IU/8 for. Rev. No.: 07 ResTOR Prosthesis
 0434 Page 1 of 5 For use by an Accredited Orthopaedic Surgeon only IMPORTANT MEDICAL INFORMATION PURPOSE: The ResTOR system is designed to restore structural skeletal stability and enable functional joint
0434 Page 1 of 5 For use by an Accredited Orthopaedic Surgeon only IMPORTANT MEDICAL INFORMATION PURPOSE: The ResTOR system is designed to restore structural skeletal stability and enable functional joint
ClassiQ. Scorpio. Anterior Referencing Surgical Protocol. Anterior Referencing. For use with Scorpio ClassiQ Instrument System
 Scorpio ClassiQ Anterior Referencing Surgical Protocol For use with Scorpio ClassiQ Instrument System For use with Scorpio ClassiQ Single Radius Total Knee System AR Anterior Referencing This document
Scorpio ClassiQ Anterior Referencing Surgical Protocol For use with Scorpio ClassiQ Instrument System For use with Scorpio ClassiQ Single Radius Total Knee System AR Anterior Referencing This document
CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician.
 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH Mpact 3D Metal Implants and Augments 3D Metal INSTRUCTION FOR USE Important notice: the device(s) can
CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH Mpact 3D Metal Implants and Augments 3D Metal INSTRUCTION FOR USE Important notice: the device(s) can
MICROPORT KNEE SYSTEMS The following languages are included in this packet:
 EN English (en) MICROPORT KNEE SYSTEMS 151251-0 The following languages are included in this packet: For additional languages, visit our website ortho.microport.com Then click on the Prescribing Information
EN English (en) MICROPORT KNEE SYSTEMS 151251-0 The following languages are included in this packet: For additional languages, visit our website ortho.microport.com Then click on the Prescribing Information
Patella Planing System
 REFERENCE GUIDE AND SURGICAL TECHNIQUE Patella Planing System SPECIALIST INSTRUMENTS AN ONLAY PATELLA PREPARATION SYSTEM TECHNIQUE FOR PRIMARY PATELLAR RESURFACING The Specialist 2 Patellar Planer System
REFERENCE GUIDE AND SURGICAL TECHNIQUE Patella Planing System SPECIALIST INSTRUMENTS AN ONLAY PATELLA PREPARATION SYSTEM TECHNIQUE FOR PRIMARY PATELLAR RESURFACING The Specialist 2 Patellar Planer System
ESC. Enhanced Stability Liners. Design Rationale & Surgical Technique
 ESC Enhanced Stability Liners Design Rationale & Surgical Technique Choice Without Compromise DePuy Synthes PINNACLE Hip Solutions are designed with a wide range of acetabular cup options, biological and
ESC Enhanced Stability Liners Design Rationale & Surgical Technique Choice Without Compromise DePuy Synthes PINNACLE Hip Solutions are designed with a wide range of acetabular cup options, biological and
S U R G I C A L T E C H N I Q U E David A. McQueen, MD Return to Menu
 S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
Technique Guide KISSloc Suture System
 Technique Guide KISSloc Suture System The KISSloc Suture System consists of a strong self-cinching suture assembly, a unique load-dispersing Arrow Plate and procedure specific instrumentation. Simple,
Technique Guide KISSloc Suture System The KISSloc Suture System consists of a strong self-cinching suture assembly, a unique load-dispersing Arrow Plate and procedure specific instrumentation. Simple,
Cementless Tapered Femoral Stem Surgical technique
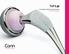 Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Regenerex Primary Tibial Tray
 Cruciate Retaining and Posterior Stabilized Surgical Technique Addendum to the Vanguard Complete Knee System Knees Hips Extremities Cement and Accessories PMI Technology Contents Microplasty Knee Instrumentation
Cruciate Retaining and Posterior Stabilized Surgical Technique Addendum to the Vanguard Complete Knee System Knees Hips Extremities Cement and Accessories PMI Technology Contents Microplasty Knee Instrumentation
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
Knee Surgical Technique
 Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
Technique Guide Wrist Hemiarthroplasty System
 Technique Guide Wrist Hemiarthroplasty System The WristMotion TM Wrist Hemiarthroplasty System restores mobility and maintains native biomechanics using a dual curvature HemiCAPITATE implant that locks
Technique Guide Wrist Hemiarthroplasty System The WristMotion TM Wrist Hemiarthroplasty System restores mobility and maintains native biomechanics using a dual curvature HemiCAPITATE implant that locks
SURGICAL TECHNIQUE GUIDE
 DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
Technique Guide Hip Resurfacing System
 Technique Guide Hip Resurfacing System Approximately 5%-18% of all hip arthroplasties are completed on patients with a primary diagnosis of osteonecrosis. Patients are generally younger adults age 35 years
Technique Guide Hip Resurfacing System Approximately 5%-18% of all hip arthroplasties are completed on patients with a primary diagnosis of osteonecrosis. Patients are generally younger adults age 35 years
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
TRK REVISION KNEE Surgical Technique
 1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
Resurfacing Distal Femur. Orthopaedic Salvage System
 Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
THE NATURAL FIT. Surgical Technique. Hip Knee Spine Navigation
 THE NATURAL FIT Surgical Technique Hip Knee Spine Navigation MiniMAX Surgical Technique Hip Knee Spine Navigation INTRODUCTION The MiniMAX TM is a cementless anatomic stem available in 9 right sizes and
THE NATURAL FIT Surgical Technique Hip Knee Spine Navigation MiniMAX Surgical Technique Hip Knee Spine Navigation INTRODUCTION The MiniMAX TM is a cementless anatomic stem available in 9 right sizes and
Surgical Technique Final Trial Reduction and Component Implantation of
 Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Mobile Bearing TC-PLUS PRIMARY Mobile Bearing Final Trial Reduction and Component Implantation of
Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Mobile Bearing TC-PLUS PRIMARY Mobile Bearing Final Trial Reduction and Component Implantation of
Zimmer NexGen Tibial Stem Extension & Augmentation. Surgical Technique IMAGE TO COME. Stem Extensions and Augments
 Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique IMAGE TO COME Stem Extensions and Augments Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique 1 Zimmer NexGen Tibial
Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique IMAGE TO COME Stem Extensions and Augments Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique 1 Zimmer NexGen Tibial
Wichita Fusion Nail Surgical Technique. David A. McQueen, MD
 Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
INNOVATIONS IN MINIMALLY INVASIVE
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY *smith&nephew Minimally Invasive TKA GENESIS II Distal Cut First Instruments Valgus Alignment Guide 7144-1144 A-P Cutting Block Size 1
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY *smith&nephew Minimally Invasive TKA GENESIS II Distal Cut First Instruments Valgus Alignment Guide 7144-1144 A-P Cutting Block Size 1
The ACL-PCL Substituting Knee. BioFoam Tibial Bases. Surgical Technique For Cementless Tibial Fixation
 The CL-PCL Substituting Knee BioFoam Surgical Technique For Cementless Tibial Fixation Surgical techniques and instrument recommendations were provided by: Michael nderson, MD Milwaukee, WI G. Lynn Rasmussen,
The CL-PCL Substituting Knee BioFoam Surgical Technique For Cementless Tibial Fixation Surgical techniques and instrument recommendations were provided by: Michael nderson, MD Milwaukee, WI G. Lynn Rasmussen,
Cementless Tapered Femoral Stem Surgical technique
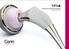 Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION. Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique
 ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
CMA TM Cemented Modular Augmentable. Baseplate. 2 Knee
 CMA TM Cemented Modular Augmentable Baseplate 2 Knee More can be addressed The U2 Cemented Modular Augmentable Baseplate is an optimal solution for tibial bone defect in primary total knee replacement.
CMA TM Cemented Modular Augmentable Baseplate 2 Knee More can be addressed The U2 Cemented Modular Augmentable Baseplate is an optimal solution for tibial bone defect in primary total knee replacement.
Surgical Technique Final Trial Reduction and Component Implantation of
 Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Fixed Bearing TC-PLUS PRIMARY Fixed Bearing Final Trial Reduction and Component Implantation of
Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Fixed Bearing TC-PLUS PRIMARY Fixed Bearing Final Trial Reduction and Component Implantation of
ACETABULAR CUP SURGICAL TECHNIQUE
 ACETABULAR CUP SURGICAL TECHNIQUE ACETABULAR CUP DEVICE INDICATIONS FOR USE The ICONACY I-Hip total hip replacement is indicated for the following conditions: 1. A severely painful and/or disabled hip
ACETABULAR CUP SURGICAL TECHNIQUE ACETABULAR CUP DEVICE INDICATIONS FOR USE The ICONACY I-Hip total hip replacement is indicated for the following conditions: 1. A severely painful and/or disabled hip
A novel cementless option. Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
 A novel cementless option Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique Zimmer Trabecular Metal Primary Patella 1 Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
A novel cementless option Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique Zimmer Trabecular Metal Primary Patella 1 Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
Duraloc CONSTRAINED LINER
 SURGICAL TECHNIQUE Duraloc CONSTRAINED LINER A COMPREHENSIVE ACETABULAR REVISION SYSTEM DURALOC CONSTRAINED LINER Introduction Dislocation is the most common postoperative complication in total hip reconstruction.
SURGICAL TECHNIQUE Duraloc CONSTRAINED LINER A COMPREHENSIVE ACETABULAR REVISION SYSTEM DURALOC CONSTRAINED LINER Introduction Dislocation is the most common postoperative complication in total hip reconstruction.
Progeny Hip Stem. Surgical Protocol and Product Specifications
 Progeny Hip Stem Surgical Protocol and Product Specifications Progeny Hip Stem Introduction With emphasis on maximum stability and ease of use, the StelKast ProgenyTM Hip System provides the surgeon with
Progeny Hip Stem Surgical Protocol and Product Specifications Progeny Hip Stem Introduction With emphasis on maximum stability and ease of use, the StelKast ProgenyTM Hip System provides the surgeon with
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
Clinical Evaluation Surgical Technique
 Clinical Evaluation Surgical Technique Table of Contents EMPERION Specifications 3 EMPERION Surgical Technique 9 EMPERION Catalog 18 Nota Bene: This technique description herein is made available to the
Clinical Evaluation Surgical Technique Table of Contents EMPERION Specifications 3 EMPERION Surgical Technique 9 EMPERION Catalog 18 Nota Bene: This technique description herein is made available to the
28 Surgical Technique
 Surgical Technique 10 12 14 16 18 20 22 24 28 26 Technique described by James L. Guyton, MD Campbell Clinic Memphis, Tennessee James W. Harkess, MD Campbell Clinic Memphis, Tennessee David G. LaVelle,
Surgical Technique 10 12 14 16 18 20 22 24 28 26 Technique described by James L. Guyton, MD Campbell Clinic Memphis, Tennessee James W. Harkess, MD Campbell Clinic Memphis, Tennessee David G. LaVelle,
Minimally Invasive TKA PROFIX Distal Cut First
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive TKA PROFIX Distal Cut First Instruments Femoral Sizing Guide 7151-3311 Femoral Anterior Referencing Stylus 7151-3313
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive TKA PROFIX Distal Cut First Instruments Femoral Sizing Guide 7151-3311 Femoral Anterior Referencing Stylus 7151-3313
Trabecular Metal Primary Patella
 Trabecular Metal Primary Patella NexGen Complete Knee Solution Surgical Technique Table of Contents Introduction... 2 Prepare the Patella... 2 Patella Reamer Technique... 3 Insetting Technique... 5 Universal
Trabecular Metal Primary Patella NexGen Complete Knee Solution Surgical Technique Table of Contents Introduction... 2 Prepare the Patella... 2 Patella Reamer Technique... 3 Insetting Technique... 5 Universal
PRIMARY POROUS PATELLA WITH TRABECULAR METAL. Surgical Technique
 PRIMARY POROUS PATELLA WITH TRABECULAR METAL Surgical Technique 1 SURGICAL TECHNIQUE FOR NEXGEN PRIMARY POROUS PATELLA * WITH TRABECULAR METAL CONTENTS PREPARE THE PATELLA............... 2 Patella Reamer
PRIMARY POROUS PATELLA WITH TRABECULAR METAL Surgical Technique 1 SURGICAL TECHNIQUE FOR NEXGEN PRIMARY POROUS PATELLA * WITH TRABECULAR METAL CONTENTS PREPARE THE PATELLA............... 2 Patella Reamer
REFLECTION Constrained Liner Introduction
 Surgical Technique REFLECTION Constrained Liner Introduction Surgical treatment of recurrent dislocation should be directed toward correction of any mechanical abnormalities. If dislocation is caused
Surgical Technique REFLECTION Constrained Liner Introduction Surgical treatment of recurrent dislocation should be directed toward correction of any mechanical abnormalities. If dislocation is caused
Salto Talaris Total Ankle Prosthesis
 Instructions for Use Salto Talaris Total Ankle Prosthesis Federal (USA) law restricts this device to sale by or on the order of a physician. Important The manufacturer recommends that all personnel responsible
Instructions for Use Salto Talaris Total Ankle Prosthesis Federal (USA) law restricts this device to sale by or on the order of a physician. Important The manufacturer recommends that all personnel responsible
INBONE II. Total Ankle System SURGICAL TECHNIQUE SUPPLEMENT TIBIAL REAMING SPECIFICATION
 INBONE II Total Ankle System SURGICAL TECHNIQUE SUPPLEMENT TIBIAL REAMING SPECIFICATION INBONE II Total Ankle System SURGICAL TECHNIQUE SUPPLEMENT Tibial Reaming Specification Contents Chapter 1 4 Product
INBONE II Total Ankle System SURGICAL TECHNIQUE SUPPLEMENT TIBIAL REAMING SPECIFICATION INBONE II Total Ankle System SURGICAL TECHNIQUE SUPPLEMENT Tibial Reaming Specification Contents Chapter 1 4 Product
Single Axis Revision Knee System
 Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical Protocol Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical
Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical Protocol Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical
NATURAL MOTION TECHNOLOGY SURGICAL TECHNIQUE. EMPOWR 3D Knee. EMPOWR PS Knee
 NATURAL MOTION TECHNOLOGY EMPOWR 3D Knee EMPOWR PS Knee SURGICAL TECHNIQUE Contents System Features.... 3 Indications and Contraindications.... 4 Surgical Snap Shot.... Preoperative Planning.... Surgical
NATURAL MOTION TECHNOLOGY EMPOWR 3D Knee EMPOWR PS Knee SURGICAL TECHNIQUE Contents System Features.... 3 Indications and Contraindications.... 4 Surgical Snap Shot.... Preoperative Planning.... Surgical
ELEOS Limb Salvage System
 ELEOS Limb Salvage System Surgical Technique Total Femoral Replacement The ELEOS Limb Salvage System offers options for patients with significant bone loss due to cancer, trauma, or previous surgical procedures.
ELEOS Limb Salvage System Surgical Technique Total Femoral Replacement The ELEOS Limb Salvage System offers options for patients with significant bone loss due to cancer, trauma, or previous surgical procedures.
Persona. The Personalized Knee. Trabecular Metal Tibia. Surgical Technique
 Persona The Personalized Knee Trabecular Metal Tibia Surgical Technique Table of Contents Resect the Tibia... 4 Size and Finish the Tibia... 4 Trial Fit... 6 Component Implantation... 7 Inserter/Implant
Persona The Personalized Knee Trabecular Metal Tibia Surgical Technique Table of Contents Resect the Tibia... 4 Size and Finish the Tibia... 4 Trial Fit... 6 Component Implantation... 7 Inserter/Implant
POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION. Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique
 POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees
POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Zimmer NexGen Rotating Hinge Knee Primary/ Revision
 Zimmer NexGen Rotating Hinge Knee Primary/ Revision Surgical Technique Designed for use in revision and difficult primary surgeries 1 INTRODUCTION The NexGen Rotating Hinge Knee Components are designed
Zimmer NexGen Rotating Hinge Knee Primary/ Revision Surgical Technique Designed for use in revision and difficult primary surgeries 1 INTRODUCTION The NexGen Rotating Hinge Knee Components are designed
Knee Revision. Portfolio
 Knee Revision Portfolio I use the DePuy Revision Knee System because of its versatility. With this system I can solve nearly any situation I encounter in the OR. Dr. Thomas Fehring, OrthoCarolina Hip and
Knee Revision Portfolio I use the DePuy Revision Knee System because of its versatility. With this system I can solve nearly any situation I encounter in the OR. Dr. Thomas Fehring, OrthoCarolina Hip and
Total Knee Replacement
 Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
REVISION SYSTEM DIFFERENT NEEDS...YOUR GLOBAL SOLUTION. Hip Knee Spine Navigation GLOBAL MEDACTA KNEE
 GLOBAL MEDACTA KNEE REVISION SYSTEM DIFFERENT NEEDS......YOUR GLOBAL SOLUTION Surgical Technique Hip Knee Spine Navigation GMK REVISION SYSTEM Surgical Technique Hip Knee Spine Navigation INTRODUCTION
GLOBAL MEDACTA KNEE REVISION SYSTEM DIFFERENT NEEDS......YOUR GLOBAL SOLUTION Surgical Technique Hip Knee Spine Navigation GMK REVISION SYSTEM Surgical Technique Hip Knee Spine Navigation INTRODUCTION
Tibial & Femoral Opening Wedge Osteotomy System. Surgical Technique
 Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
