Association Between Patient Factors and Outcome of Synthetic Cartilage Implant. Hemiarthroplasty versus First Metatarsophalangeal Joint Arthrodesis
|
|
|
- Gladys Gallagher
- 5 years ago
- Views:
Transcription
1 Association Between Patient Factors and Outcome of Synthetic Cartilage Implant Hemiarthroplasty versus First Metatarsophalangeal Joint Arthrodesis in Advanced Hallux Rigidus Andy Goldberg, MBBS MD, FRCS (Tr&Orth), 1,2 Dishan Singh, FRCS, 1 Mark Glazebrook, MSc, MD, PhD, FRCSC, 3 Chris M. Blundell, MBChB, FRCS, 4 Gwyneth De Vries, MSc, MD, FRCSC, 5 Ian L. D. Le, MD, FRCSC, 6 Dominic Nielsen, FRCS, 7 M. Elizabeth Pedersen, MD, FRCSC, 8 Anthony Sakellariou, MBBS, FRCS, 9 Matthew Solan, FRCS, 10 Alastair S. E. Younger, MBChB, MSc, ChM, FRCSC, 11 Timothy R. Daniels, MD, FRCSC, 12 and Judith F. Baumhauer, MD, MPH, 13 on behalf of the Cartiva MOTION Study Group Author affiliations: 1 Stanmore Royal National Orthopaedic Hospital, Stanmore, Middlesex, United Kingdom 2 Division of Surgery & Interventional Science, UCL, London, United Kingdom 3 Dalhousie University and Queen Elizabeth II Health Sciences Center, Halifax, Nova Scotia, Canada 4 Northern General Hospital, Sheffield, United Kingdom 5 Dalhousie University and Memorial University of Newfoundland, Fredericton, New Brunswick, Canada 6 University of Calgary, Calgary, Alberta, Canada 7 St. George s Hospital, London, United Kingdom 8 University of Alberta, Edmonton, Alberta, Canada 9 Frimley Park Hospital, Frimley, Camberley, Surrey, United Kingdom 10 Royal Surrey County Hospital, Guildford, Surrey, United Kingdom FAI R Jun5 1
2 11 Department of Orthopaedics, University of British Columbia, Vancouver, British Columbia, Canada 12 Division of Orthopaedic Surgery, St. Michael s Hospital, Toronto, Ontario, Canada 13 Department of Orthopaedics, University of Rochester School of Medicine and Dentistry, Rochester, New York, USA Address for correspondence: Mr. Andy Goldberg OBE, Consultant Orthopaedic Surgeon, Stanmore Royal National Orthopaedic Hospital NHS Trust, Brockley Hill, Stanmore, Middlesex, UK, HA7 4LP. Phone: +44 (208) ; andy.goldberg@rnoh.nhs.uk Conflict of interest statement: One or more of the authors has received or will receive benefits for personal or professional use from a commercial party related directly or indirectly to the subject of this article. Funding: The authors disclosed receipt of research and institutional support, consulting fees and support for travel expenses from Cartiva Inc. for the research, authorship, and/or publication of this article. Word length: 3,473 words Number of Tables: 2 Number of Figures: 2 FAI R Jun5 2
3 ACKNOWLEDGEMENTS Special recognition goes to Nick Cullen, MBBS, FRCS; Mark Davies, BM, FRCS; Howard Davies, MBChB, MSc, FRCS; James Davis, MBBS, FRCS; Anna Fox, MBChB, MSc, FRCS; Gordon Goplen, MD, FRCSC; Murray Penner, MD, FRCSC; and all the MOTION study coordinators from the United Kingdom and Canada. The authors thank Dagmar Gross for assistance with preparation of this manuscript. FAI R Jun5 3
4 Association Between Patient Factors and Outcome of Synthetic Cartilage Implant Hemiarthroplasty versus First Metatarsophalangeal Joint Arthrodesis in Advanced Hallux Rigidus ABSTRACT (max 250 words) Background: We evaluated data from a clinical trial of first metatarsophalangeal joint (MTPJ1) implant hemiarthroplasty and arthrodesis to determine the association between patient factors and clinical outcomes. Methods: Patients 18 years with hallux rigidus grade 2, 3, or 4 were treated with synthetic cartilage implant MTPJ1 hemiarthroplasty or arthrodesis. Pain VAS, Foot and Ankle Ability Measure (FAAM) Sports and ADL scores, and SF-36 PF subscore were obtained preoperatively, and at 2, 6, 12, 24, 52 and 104 weeks postoperatively. Final outcome data, great toe active dorsiflexion motion, secondary procedures, radiographs and safety parameters were evaluated for 129 implant hemiarthroplasties and 47 arthrodeses. The composite primary endpoint criteria for clinical success included VAS pain reduction 30%, maintenance/improvement in function, no radiographic complications, and no secondary surgical intervention at 24 months. Predictor variables included: hallux rigidus grade; gender; age; BMI; symptom duration; prior MTPJ1 surgery; preoperative hallux valgus angle, ROM, and pain. Two-sided Fisher s Exact test was used (p<0.05). Results: Patient demographics and baseline outcome measures were similar. Success rates between implant MTPJ1 hemiarthroplasty and arthrodesis were similar (p>0.05) when stratified by hallux rigidus grade, gender, age, BMI, symptom duration, prior MTPJ1 surgery status, and preoperative VAS pain, hallux valgus and ROM. FAI R Jun5 4
5 Conclusion: Synthetic cartilage implant hemiarthroplasty is appropriate for patients with grade 2, 3 or 4 hallux rigidus. Its results in those with associated mild hallux valgus ( 20 ) or substantial preoperative stiffness are equivalent to MTPJ1 fusion, irrespective of gender, age, BMI, hallux rigidus grade, preoperative pain or symptom duration. Level of Evidence: II, randomized clinical trial Keywords: First metatarsophalangeal joint; Hallux rigidus; Hemiarthroplasty; Synthetic cartilage implant. INTRODUCTION Arthritis of the first metatarsophalangeal joint (MTPJ), or hallux rigidus, is a common problem affecting one in 40 people over 50 years of age 11 and 45% of people aged 75 to 79 years 21. Moderate to severe hallux rigidus is often treated with arthrodesis, historically considered the most reliable option. 16 However, the loss of motion through the MTPJ following arthrodesis can interfere with activities that require great toe motion, such as jumping and running, or the wearing of high heels, and can lead to transfer metatarsalgia or adjacent joint arthritis. A desire to preserve motion at the first MTPJ has prompted the development of several great toe implants, many of which demonstrated high rates of failure due to loosening, malalignment, dislocation, subsidence, implant fragmentation and bone loss. 23,24 A polyvinyl alcohol (PVA) hydrogel implant has been developed for use in first MTPJ hemiarthroplasty. The PVA hydrogel has a cartilage-like viscoelasticity, 18 a tensile strength of 17 MPa comparable to that of human articular cartilage, 18 and biomechanical properties (i.e., compression-compressive modulus, shear-shear FAI R Jun5 5
6 modulus, compressive creep-creep and creep recovery, and kinetic friction) very similar to cartilage. 2 Its high biocompatibility with cartilage, bone, synovium and muscle, 18 combined with its compressibility, low friction, and durable bearing surface make it a suitable synthetic cartilage implant. 2,3 Since the implant has similar osmotic, physical and frictional properties to cartilage, replacement of the opposing articular surface is not required, permitting a hemiarthroplasty that maintains articulation through the joint. In a recent prospective, randomized, multicenter, clinical trial of 202 patients with moderate to severe hallux rigidus, hemiarthroplasty of the first MTPJ with a synthetic cartilage implant demonstrated equivalent pain relief, functional outcomes and safety to first MTPJ arthrodesis at two years follow-up, with no cases of implant fragmentation, wear or bone loss. 4 First MTPJ active dorsiflexion motion improved by a mean of 6.2 (27.3%) in 152 synthetic cartilage implant hemiarthroplasty patients and was maintained at 24 months. In a subset of 27 implant hemiarthroplasty patients who reached five years follow-up, functional outcomes improved significantly and pain was reduced significantly compared to preoperative measures, and only one implant was removed and converted to fusion at two years postoperative, because of persistent pain. 7 There is a paucity of data regarding the association between patient factors and clinical outcomes following hallux rigidus surgery. Several studies have directly compared the short- to mid-term outcomes (i.e., 2 to 4 years) of first MTPJ hemiarthroplasty with various implants to MTPJ arthrodesis. 9,10,13,17,19,20,22 However, these studies either did not evaluate the association between patient factors and outcomes, 10,20,22 or the sample sizes were too small to permit such analyses. 9,17,19 FAI R Jun5 6
7 The purpose of this study was to evaluate the longitudinal data from the aforementioned randomized, clinical trial comparing synthetic cartilage implant first MTPJ hemiarthroplasty with arthrodesis, 4 to determine the association between numerous patient factors and the success or failure of these procedures. Success rates were also compared between treatment groups within each category of the patient factors. PATIENTS AND METHODS Patients 18 years of age and older who had been diagnosed with Coughlin hallux rigidus grade 2, 3, or 4 based on combined radiological and clinical observations 5 including moderate to severe pain, and who were considered surgical candidates for arthrodesis, were treated with either hemiarthroplasty of the first MTPJ using a synthetic polyvinyl alcohol hydrogel implant (Cartiva Synthetic Cartilage Implant, Cartiva, Inc., Alpharetta, GA, USA) or first MTPJ arthrodesis in a multicenter, noninferiority clinical trial, as previously reported. 4 Patients were randomized 72 hours or less prior to surgery, in a 2:1 allotment of implant hemiarthroplasty to arthrodesis. The randomized clinical trial was approved by each site s institutional review board, and all patients provided informed consent. The efficacy and safety data for the clinical trial have been previously reported. 4 For the current study, patient demographic data and preoperative data collected prospectively for the original trial were assessed for the Safety population, comprising 152 hemiarthroplasties and 50 arthodeses (Figure 1). Osseous union was determined by independent radiographic review of foot radiographs, which were taken preoperatively and at 2, 6, 12, 24, 52 and 104 weeks postoperatively. A patient s outcome was deemed successful if composite primary endpoint criteria for FAI R Jun5 7
8 clinical success were met at 24 months, namely: 1) VAS pain reduction 30%; 2) maintenance or improvement in function; 3) freedom from radiographic complications; and 4) no secondary surgical intervention. Final outcome data were assessed in the modified Intent to Treat (mitt) population (Figure 1). The standardized operative technique used for the synthetic cartilage implant and postoperative protocol has been published previously. 4,24 Briefly, the first MTPJ was accessed via a straight dorsal incision, or a standard mid-medial approach. The neurovascular structures and tendons were protected as appropriate and a capsular incision made to expose the first metatarsal (MT) head (Figure 2a). The articular cartilage wear was examined, and the medial, lateral and dorsal osteophytes were carefully removed from the metatarsal head; in some cases, the osteophyte on the dorsal side of the proximal phalanx was also removed (Figure 2b). A central guide wire was placed in the MT head and extended into the shaft, and the MT head was drilled (Figures 2c, 2d). An appropriately sized 8 or 10 mm implant was seated in the MT head to allow approximately mm of the implant to extend beyond the adjacent native cartilage (Figures 2e, 2f). With the implant at the correct depth, range of motion was checked against the implant, ensuring there was no restriction or limitation of the joint movement. Layered closure of the capsule and skin was performed. A soft dressing was applied, and postoperative shoes were used. Patients could bear weight immediately as tolerated. At 2 weeks, skin sutures were removed, range of motion (ROM) exercises were begun, and patients resumed wearing regular shoes, as tolerated. First MTPJ arthrodesis was performed using standard techniques, as described in the literature. 6 For this study, the first MTPJ was exposed as per the synthetic cartilage implant technique. The base of the proximal phalanx and the first MT head were aligned FAI R Jun5 8
9 and positioned in slight dorsiflexion and valgus with neutral rotation and held with K- wires. A simulated weight bearing test was used to confirm grip of the big toe when plantigrade and sufficient lift off to enable comfortable walking. The construct was then stabilized with crossed screws or plate and screws. Layered closure of the capsule and skin were performed. The foot was placed in a sterile dressing and immobilized in a heel wedge shoe or boot for six to ten weeks, or until osseous union occurred, at which time weight bearing was begun at the discretion of the surgeon. Data Collection Outcome measures included a pain visual analogue scale (VAS), the Foot and Ankle Ability Measure (FAAM) Sports and Activities of Daily Living (ADL) subscales, and Short Form-36 Physical Functioning (SF-36 PF) subscore, which were prospectively recorded for all study patients preoperatively and at 2 (pain VAS and FAAM only), 6, 12, 24, 52 and 104 weeks postoperatively. The Initiative on Methods, Measurement, and Pain Assessment in Clinical Trials (IMMPACT) consensus group defined a decrease in pain of 30% to be a clinically meaningful improvement for patients and recommended this value be reported in clinical trials. 8 The FAAM has been validated in subjects with a leg, foot, or ankle musculoskeletal disorder; 15 the minimal clinically important difference (MCID) is 9 points for the FAAM Sports score and 8 points for the FAAM ADL score. 4 The SF-36 is a generic measure of general health status and has been validated in the endstage ankle arthritis population; 14 the MCID for the SF-36 PF subscore is 3.3 points. 1 Great toe active dorsiflexion motion, secondary procedures, radiographs and safety parameters were also evaluated. Patient demographic and preoperative data assessed as predictor FAI R Jun5 9
10 variables included hallux rigidus grade, 5 hallux valgus angle, preoperative ROM, gender, age, body mass index (BMI), preoperative symptom duration, preoperative pain level, and prior first MTPJ surgery (e.g. joint debridement or cheilectomy), all of which were captured prospectively at baseline. Statistical Analysis Categorical data are presented as numbers and percentages. Continuous data are presented as means and standard deviations with ranges. Two-sided Fisher s Exact test was used to assess the association between patient demographic and preoperative variables and clinical success, within each treatment group. In secondary analyses, success rates were compared between groups within each level of the patient demographic and preoperative variables. A p-value <0.05 was considered statistically significant. RESULTS The original randomized clinical trial reported equivalent pain relief and functional outcomes in the synthetic implant first MTPJ hemiarthroplasty group and the first MTPJ arthrodesis group. 4 Complete data at 24 months follow-up (mitt Completers; Figure 1) included 129 patients with synthetic cartilage implant hemiarthroplasty and 47 patients who underwent an arthrodesis. Patient demographics and baseline outcome measures were similar for both groups (Table 1). There were no significant differences in success rates for either first MTPJ synthetic cartilage implant hemiarthroplasty or arthrodesis when stratified by hallux rigidus grade, degree of preoperative hallux valgus, extent of preoperative ROM, gender, age, BMI, duration of symptoms, prior MTPJ1 surgery status (including joint FAI R Jun5 10
11 debridement and/or cheilectomy), and preoperative VAS pain score (all p>0.05; Table 2). There were also no significant differences between treatment groups within any level of the patient or preoperative factors evaluated (Table 2). Males tended to have greater clinical success with implant hemiarthroplasty versus arthrodesis, but this difference was not statistically significant. Patients with less preoperative motion had marginally higher success rates with hemiarthroplasty versus fusion, but these differences were not statistically significant. DISCUSSION In a large, randomized, clinical trial, synthetic cartilage implant hemiarthroplasty of the first MTPJ demonstrated equivalent success rates compared to first MTPJ arthrodesis, regardless of hallux rigidus grade, gender, age, BMI, degree of preoperative hallux valgus, extent of preoperative ROM, preoperative duration of symptoms, prior first MTPJ surgery, and preoperative VAS pain score. Notably, patients with larger BMI, patients with minimal ROM (i.e., stiff joints), and patients with mild hallux valgus had equivalent success rates for both procedures, indicating that synthetic implant first MTPJ hemiarthroplasty could be considered as a reasonable operative option for moderate to severe hallux rigidus. Only one other study has compared the short-term outcomes (i.e., 2 to 3 years) of metatarsal head-resurfacing hemiarthroplasty to those of MTPJ arthrodesis. Erdil et al 9 retrospectively reviewed patients with advanced hallux rigidus who underwent resurfacing hemiarthroplasty with the HemiCAP (n=14) or arthrodesis with 2 cannulated compression screws (n=12). They also had a third cohort of patients who underwent total joint arthroplasty with the ToeFit-Plus (n=12), They reported similar functional FAI R Jun5 11
12 outcomes following arthroplasty and hemiarthroplasty, and less function due to less range of motion in arthrodesis patients, who also had less pain, at 28 to 35 months follow-up. However, they did not evaluate the association between patient factors and clinical outcomes; there is a notable lack of such data available in the literature. To be included in the original clinical trial, patients had to be diagnosed with Coughlin grade 2, 3, or 4 hallux rigidus, which is based on a combination of radiological and clinical observations, 5 and all patients had to be considered surgical candidates for arthrodesis. It is important to point out that Coughlin grade 2 includes moderate to severe pain and stiffness, which may be constant. 5 The literature generally holds that joint-sparing procedures should be reserved for mild to moderate osteoarthritis, and that fusion should be used in late-stage moderate to severe osteoarthritis. 5,12,23 Our findings do not support this proposition, as we found no significant difference in outcome between the groups, irrespective of the hallux rigidus grade, preoperative presence of a stiff toe, a high BMI, or the presence of mild hallux valgus ( 20 ). Synthetic implant first MTPJ hemiarthroplasty can be used to successfully treat patients with mild hallux valgus; however, patients with >20 hallux valgus were excluded from the clinical trial, and concomitant valgus correction procedures were also not permissible. Hence, we are unable to comment on the outcome of synthetic cartilage implant first MTPJ replacement in cases with >20 hallux valgus. We acknowledge the limitations of this study. The original clinical trial was powered for non-inferiority to demonstrate equivalence of the two procedures, whereas the current study retrospectively analyzed success rates for variations in patient factors within each treatment group and may not have been sufficiently FAI R Jun5 12
13 powered for some patient factors, thus a type II error cannot be excluded in the subgroup analysis. Some patient factors that may be associated with clinical outcomes may not have been recorded in the original trial. Exclusion criteria for the original trial also excluded some patient factors that would have been of interest to evaluate within the current study, such as the presence of hallux valgus >20 or an associated deformity correction. Another limitation is the loss of 15 patients who initially consented to randomization and treatment and subsequently withdrew from the original trial following randomization to arthrodesis; statistical analyses were therefore performed on the modified intent to treat population, so as to address the potential bias in favor of the implant. The current study did not assess surgeon factors such as type of approach, type of fixation used, or position of construct in the arthrodesis group, which could be confounding variables, and we intend to assess these in a subsequent study. Finally, this study evaluated association of patient factors based on two-year outcomes. As data for five years and longer follow-up become available, it is possible there may be some failures, which could potentially modify some of the associations observed here. Strengths of this study include the rigorous quality of the longitudinal data obtained as part of a large, multicenter, well controlled, randomized clinical trial, the large sample sizes (hemiarthroplasty n=129; arthrodesis n=47) and the low rate of patients lost to follow-up (2%). Most previous comparative studies of operative treatment for hallux rigidus have small numbers in each treatment arm. 9,10,16,17,19,22 The data from this study are broadly generalizable, as they represent patients enrolled by 49 surgeons from 12 centers across two countries. This study provides the first thorough evidence of the association between patient factors and clinical outcomes following hallux rigidus surgery. FAI R Jun5 13
14 In conclusion, based on our short-term data of two-year follow-up, synthetic cartilage implant hemiarthroplasty is an appropriate treatment for patients with hallux rigidus of Coughlin grade 2, 3 or 4. Our results demonstrate that it is a reasonable choice in hallux rigidus associated with mild hallux valgus ( 20 ), and in patients with a high degree of preoperative stiffness, irrespective of gender, age, BMI, hallux rigidus grade, preoperative pain, or duration of symptoms, in contrast to what might have been expected. REFERENCES 1. Angst F, Aeschlimann A, Stucki G. Smallest detectable and minimal clinically important differences of rehabilitation intervention with their implications for required sample sizes using WOMAC and SF-36 quality of life measurement instruments in patients with osteoarthritis of the lower extremities. Arthritis Rheum. 2001;45(4): doi: / (200108)45:4<384::aidart352>3.0.co; Baker MI, Walsh SP, Schwartz Z, Boyan BD. A review of polyvinyl alchohol and its uses in cartilage and orthopedic applications. J Biomed Mater Res B Appl Biomater. 2012;100(5): doi: /jbm.b Baumhauer JF, Marcolongo M. The science behind wear testing for great toe implants for hallux rigidus. Foot Ankle Clin. 2016;21(4): doi: /j.fcl Baumhauer JF, Singh D, Glazebrook M, et al. Prospective, randomized, multicentered clinical trial assessing safety and efficacy of a synthetic cartilage FAI R Jun5 14
15 implant versus first metatarsophalangeal arthrodesis in advanced hallux rigidus. Foot Ankle Int. 2016;37(5): doi: / Coughlin MJ, Shurnas PS. Hallux rigidus. Grading and long-term results of operative treatment. J Bone Joint Surg Am. 2003;85-A(11): Coughlin MJ, Shurnas PS. Hallux rigidus. J Bone Joint Surg Am. 2004;86-A Suppl 1(Pt 2): doi:86/suppl_2/119 [pii]. 7. Daniels TR, Younger AS, Penner MJ, et al. Midterm outcomes of polyvinyl alcohol hydrogel hemiarthroplasty of the first metatarsophalangeal joint in advanced hallux rigidus. Foot Ankle Int. 2017;38(3): doi: / Dworkin RH, Turk DC, Wyrwich KW, et al. Interpreting the clinical importance of treatment outcomes in chronic pain clinical trials: IMMPACT recommendations. J Pain. 2008;9(2): doi: /j.jpain Erdil M, Elmadag NM, Polat G, et al. Comparison of arthrodesis, resurfacing hemiarthroplasty, and total joint replacement in the treatment of advanced hallux rigidus. J Foot Ankle Surg. 2013;52(5): doi: /j.jfas Gibson JN, Thomson CE. Arthrodesis or total replacement arthroplasty for hallux rigidus: a randomized controlled trial. Foot Ankle Int. 2005;26(9): doi: [pii]. 11. Gould N, Schneider W, Ashikaga T. Epidemiological survey of foot problems in the continental United States: Foot Ankle. 1980;1(1): Ho B, Baumhauer J. Hallux rigidus. EFORT Open Rev. 2017;2: doi: / FAI R Jun5 15
16 13. Kim PJ, Hatch D, Didomenico LA, et al. A multicenter retrospective review of outcomes for arthrodesis, hemi-metallic joint implant, and resectional arthroplasty in the surgical treatment of end-stage hallux rigidus. J Foot Ankle Surg. 2012;51(1): doi: /j.jfas Madeley NJ, Wing KJ, Topliss C, et al. Responsiveness and validity of the SF-36, Ankle Osteoarthritis Scale, AOFAS Ankle Hindfoot Score, and Foot Function Index in end stage ankle arthritis. Foot Ankle Int. 2012;33(1): doi: /fai Martin RL, Irrgang JJ, Burdett RG, Conti SF, Van Swearingen JM. Evidence of validity for the Foot and Ankle Ability Measure (FAAM). Foot Ankle Int. 2005;26(11): McNeil DS, Baumhauer JF, Glazebrook MA. Evidence-based analysis of the efficacy for operative treatment of hallux rigidus. Foot Ankle Int. 2013;34(1): doi: / Mermerkaya MU, Adli H. A comparison between metatarsal head-resurfacing hemiarthroplasty and total metatarsophalangeal joint arthroplasty as surgical treatments for hallux rigidus: a retrospective study with short- to midterm follow-up. Clin Interv Aging. 2016;11: doi: /cia.s Noguchi T, Yamamuro T, Oka M, et al. Poly(vinyl alcohol) hydrogel as an artificial articular cartilage: evaluation of biocompatibility. J Appl Biomater. 1991;2(2): doi: /jab Raikin SM, Ahmad J, Pour AE, Abidi N. Comparison of arthrodesis and metallic hemiarthroplasty of the hallux metatarsophalangeal joint. J Bone Joint Surg Am. 2007;89(9): doi:89/9/1979 [pii]. FAI R Jun5 16
17 /JBJS.F Simons KH, van der Woude P, Faber FW, van Kampen PM, Thomassen BJ. Shortterm clinical outcome of hemiarthroplasty versus arthrodesis for end-stage hallux rigidus. J Foot Ankle Surg. 2015;54(5): doi: /j.jfas van Saase JL, van Romunde LK, Cats A, Vandenbroucke JP, Valkenburg HA. Epidemiology of osteoarthritis: Zoetermeer survey. Comparison of radiological osteoarthritis in a Dutch population with that in 10 other populations. Ann Rheum Dis. 1989;48(4): Voskuijl T, Onstenk R. Operative treatment for osteoarthritis of the first metatarsophalangeal joint: Arthrodesis versus hemiarthroplasty. J Foot Ankle Surg. 2015;54(6): doi: /j.jfas Yee G, Lau J. Current concepts review: hallux rigidus. Foot Ankle Int. 2008;29(6): doi: /fai Younger ASE, Baumhauer JF. Polyvinyl alcohol hydrogel hemiarthroplasty of the great toe: Technique and indications. Techniques in Foot and Ankle Surgery. 2013;12(3): FAI R Jun5 17
18 Figure 1: Pivotal Trial Study Enrollment Subject accountability tree. The Safety Population consisted of 152 patients (22 roll-in and 130 randomized) treated with synthetic cartilage implant hemiarthroplasty and 50 control patients treated with arthrodesis. The modified Intent to Treat (mitt) Population included 130 patients randomized and treated with synthetic cartilage implant hemiarthroplasty and 50 patients randomized and treated with arthrodesis, of whom 129 hemiarthroplasty and 47 arthrodesis patients had complete data available at 24 months follow-up (mitt Completers) FAI R Jun5 18
19 Figure 2: Overview of operative technique for synthetic cartilage implant first metatarsophalangeal joint hemiarthroplasty: (a) Straight dorsal or medial incision and exposure of the entire joint to gain access to the first metatarsal head; (b) Resection of osteophytes from the metatarsal head; (c) Guide wire placement and advancement of the cannulated drill bit; (d) Drilling of metatarsal head to produce cavity for the implant; (e) Implant compressed within the introducer tube and positioned for insertion into the metatarsal head cavity; (f) Implant seated into metatarsal head with expected 1.5 to 2.0 mm implant prominence. FAI R Jun5 19
20 Figure 2 FAI R Jun5 20
21 Table 1: Baseline demographics and outcome measure scores of implant hemiarthroplasty and arthrodesis modified Intent to Treat (mitt) cohorts, shown as mean ± standard deviation, with the range in brackets Factor Implant Hemiarthroplasty Arthrodesis (n=50) t-test p-value a Wilcoxon p-value b (n=130) Age at surgery (years) 57.4 ± ± ( ) ( ) Gender, n (%) Male 26 (20%) 12 (24%) Female 104 (80%) 38 (76%) BMI (kg/m 2 ) 27.2 ± ± ( ) ( ) Outcome Measures VAS Pain 68.0 ± ± ( ) ( ) FAAM Sports 36.9 ± 20.9 d 35.6 ± ( ) ( ) FAAM ADL 59.4 ± 16.9 c 56.0 ± ( ) ( ) SF-36 PF 52.4 ± 22.8 ( ) 49.8 ± 23.6 ( ) Abbreviations: BMI, body mass index; FAAM, Foot and Ankle Ability Measure; ADL, Activities of Daily Living; SF-36 PF, Short Form-36 Physical Function subscore a Two-sample pooled t-test p-value (chi-square test for gender). b Two-sample Wilcoxon rank-sum test p-value (Fisher s exact test for gender). c n=129 for this score only. d n=127 for this score only FAI R Jun5 21
22 Table 2: Success rates of synthetic cartilage implant hemiarthroplasty of the first metatarsophalangeal joint (n=129) and first metatarsophalangeal joint arthrodesis (n=47), stratified by patient factors. Patient Variable Stratification Synthetic Implant Hemiarthroplasty Arthrodesis p-valueǂ N^ n~ % Success p-value* N^ n~ % p-value* Success Coughlin 5 Hallux % % Rigidus Grade % % % % Preoperative Hallux Valgus Angle Preoperative Active Peak Dorsiflexion 0 to < % % to % % to % % to < % % >10 to < % % % % Gender Female % % Male % % Age 65 years % % <65 years % % Body Mass Index (BMI) Duration of Symptoms Prior to Surgery <30 kg/m % % kg/m % % <24 months % % months % % Prior MTPJ1 Surgery Prior surgery % % FAI R Jun5 22
23 Status No prior surgery % % Preoperative Pain Mild (0 to < VAS Score mm) % % Moderate ( 40 to % % mm) Severe (>58 to % % mm) * p-values were determined using Fisher's Exact test, within group. ǂ p-values were determined using Fisher s Exact test, between groups within strata. ^ N = total number of patients in the treatment cohort with that variable. ~ n = total number of patients in the treatment cohort with that variable who met the composite primary endpoint criteria for clinical success (i.e., VAS pain reduction 30%, maintenance or improvement in function, freedom from radiographic complications, and no secondary surgical intervention). 1 Prior surgery other than arthroplasty or arthrodesis, for example, joint debridement or cheilectomy. 2 VAS pain <40 mm was an exclusion criterion for the study; these patients were protocol violations. 3 Coughlin MJ, Shurnas PS. Hallux rigidus. Grading and long-term results of operative treatment. J Bone Joint Surg Am. 2003;85-A(11): FAI R Jun5 23
Introduction. Article
 723334FAIXXX10.1177/1071100717723334Foot & Ankle InternationalGoldberg et al research-article2017 Article Association Between Patient Factors and Outcome of Synthetic Cartilage Implant Hemiarthroplasty
723334FAIXXX10.1177/1071100717723334Foot & Ankle InternationalGoldberg et al research-article2017 Article Association Between Patient Factors and Outcome of Synthetic Cartilage Implant Hemiarthroplasty
Synthetic Cartilage Implants for Joint Pain
 Synthetic Cartilage Implants for Joint Pain Policy Number: 7.01.160 Last Review: 3/2018 Origination: 2/2018 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Synthetic Cartilage Implants for Joint Pain Policy Number: 7.01.160 Last Review: 3/2018 Origination: 2/2018 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Synthetic Cartilage Implants for Joint Pain
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Synthetic Cartilage Implant for 1st MTP Osteoarthritis: The Difference is DATA
 Synthetic Cartilage Implant for 1st MTP Osteoarthritis: The Difference is DATA This educational activity is supported by an educational grant from Cartiva, Inc. Faculty Peter A. Blume, DPM, FACFAS Attending
Synthetic Cartilage Implant for 1st MTP Osteoarthritis: The Difference is DATA This educational activity is supported by an educational grant from Cartiva, Inc. Faculty Peter A. Blume, DPM, FACFAS Attending
A perspective on MPJ implant arthroplasty.
 A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
Disclosures. 55 year old Male 2/23/2018. Recurrent Hallux Rigidus: Options Other than Arthrodesis
 Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
Great Toe Joint Replacement Patient Guide
 Great Toe Joint Replacement Patient Guide The BioPro First MPJ Hemi Implant The proven long-term joint fusion alternative. Long-term use Clinically proven High implant survivorship Long-term implant survivorship
Great Toe Joint Replacement Patient Guide The BioPro First MPJ Hemi Implant The proven long-term joint fusion alternative. Long-term use Clinically proven High implant survivorship Long-term implant survivorship
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint
 Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus. Anand Vora, MD
 Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis
 SPECIAL FOCUS Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis Alastair S.E. Younger a, Judith F. Baumhauer b and Mark Glazebrook c ABSTRACT End stage arthritis
SPECIAL FOCUS Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis Alastair S.E. Younger a, Judith F. Baumhauer b and Mark Glazebrook c ABSTRACT End stage arthritis
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
-97% +176% 93% SUBSTANTIAL FUNCTIONAL IMPROVEMENT
 LOWER EXTREMITIES CARTIVA Synthetic Cartilage Implant The First and Only PMA Approved Product for the Treatment of First MTP Joint Osteoarthritis FOOT First MTP Joint THE DIFFERENCE IS MOVING. CARTIVA
LOWER EXTREMITIES CARTIVA Synthetic Cartilage Implant The First and Only PMA Approved Product for the Treatment of First MTP Joint Osteoarthritis FOOT First MTP Joint THE DIFFERENCE IS MOVING. CARTIVA
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
PATIENT INFORMATION THE DIFFERENCE IS MOVING.
 PATIENT INFORMATION THE DIFFERENCE IS MOVING. THIS BROCHURE IS WRITTEN TO HELP YOU MAKE AN INFORMED DECISION ABOUT YOUR SURGERY. Please read this entire brochure carefully. Keep this brochure. You may
PATIENT INFORMATION THE DIFFERENCE IS MOVING. THIS BROCHURE IS WRITTEN TO HELP YOU MAKE AN INFORMED DECISION ABOUT YOUR SURGERY. Please read this entire brochure carefully. Keep this brochure. You may
NORTHERN OHIO FOUNDATION
 NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS
 arthrosurface.com PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS A NATIONWIDE SURGEON SURVEY ON OVER 2,000 HEMICAP TOE PROCEDURES INCLUDES: Patient Function and Activity Milestones Patient Rehabilitation
arthrosurface.com PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS A NATIONWIDE SURGEON SURVEY ON OVER 2,000 HEMICAP TOE PROCEDURES INCLUDES: Patient Function and Activity Milestones Patient Rehabilitation
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Merete BLP. Surgical Technique. - Bunion Locking Plate - Low Profile Locking Bone Plate System
 Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Mid-Term Results of Triple Osteotomy in Hallux Valgus with Highly Increased Distal Metatarsal Articular Angle
 AOFAS Annual Meeting 2012 The Korean Foot & Ankle Society Mid-Term Results of Triple Osteotomy in Hallux Valgus with Highly Increased Distal Metatarsal Articular Angle Kyung Tai Lee, M.D., Ki Won Young,
AOFAS Annual Meeting 2012 The Korean Foot & Ankle Society Mid-Term Results of Triple Osteotomy in Hallux Valgus with Highly Increased Distal Metatarsal Articular Angle Kyung Tai Lee, M.D., Ki Won Young,
SURGICAL TECHNIQUE CHI. Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY
 CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
Are you living with toe pain?
 Are you living with toe pain? Unlike a toe fusion, the Arthrosurface Joint Restoration Systems can allow you to resume full activity and preserves the natural anatomy of your joint. Find out if the Arthrosurface
Are you living with toe pain? Unlike a toe fusion, the Arthrosurface Joint Restoration Systems can allow you to resume full activity and preserves the natural anatomy of your joint. Find out if the Arthrosurface
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
First MPJ Hemi Implant
 First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
The impact of ankle arthritis treatment on quality adjusted life years
 The impact of ankle arthritis treatment on quality adjusted life years Hynes, K., Wing, K., Penner, M., A, Veljkovic, Younger, A., Sutherland, J. The University of British Columbia, St. Paul s Hospital,
The impact of ankle arthritis treatment on quality adjusted life years Hynes, K., Wing, K., Penner, M., A, Veljkovic, Younger, A., Sutherland, J. The University of British Columbia, St. Paul s Hospital,
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Finite Element Analysis (FEA) of Swanson Flexible Hinge Toe Implant
 Finite Element Analysis (FEA) of Swanson Flexible Hinge Toe Implant Xiao (Cathy) Zhou (1), Agustín Vidal Lesso (2) 1 Candidate for Bachelors of Science in Mechanical Engineering, Massachusetts Institute
Finite Element Analysis (FEA) of Swanson Flexible Hinge Toe Implant Xiao (Cathy) Zhou (1), Agustín Vidal Lesso (2) 1 Candidate for Bachelors of Science in Mechanical Engineering, Massachusetts Institute
WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
Disclosures. The authors disclosures are in the Final AOFAS Mobile App. The authors may have a potential conflict with this presentation due to:
 COFAS Multicenter Study Comparing Ankle Replacement and Ankle Fusion: The effect of Ipsilateral peri-articular deformity and arthritis on Mid-term outcome Murray J. Penner, MD, FRCSC Kevin J. Wing, MD,
COFAS Multicenter Study Comparing Ankle Replacement and Ankle Fusion: The effect of Ipsilateral peri-articular deformity and arthritis on Mid-term outcome Murray J. Penner, MD, FRCSC Kevin J. Wing, MD,
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation
 First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation Bryan Van Dyke, DO Gregory C. Berlet, MD Justin L. Daigre, MD Christopher F. Hyer, DPM,
First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation Bryan Van Dyke, DO Gregory C. Berlet, MD Justin L. Daigre, MD Christopher F. Hyer, DPM,
1 st MP Arthrodesis. - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA
 1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations
 ORIGINAL ARTICLES Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations A Retrospective Review Marc D. Jones, DPM* Kerry J. Sweet, DPM Background:
ORIGINAL ARTICLES Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations A Retrospective Review Marc D. Jones, DPM* Kerry J. Sweet, DPM Background:
RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS
 RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS RACHEL ALBRIGHT DPM, MOIZ HASSAN MS, ROBERT O KEEFE DPM, ERIN E. KLEIN DPM, MS, LOWELL WEIL JR. DPM, MBA, LOWELL WEIL SR. DPM,
RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS RACHEL ALBRIGHT DPM, MOIZ HASSAN MS, ROBERT O KEEFE DPM, ERIN E. KLEIN DPM, MS, LOWELL WEIL JR. DPM, MBA, LOWELL WEIL SR. DPM,
SURGICAL APPROACHES TO FIRST RAY ELIZABETH BASS DAUGHTRY, DPM, FACFAS AAWP TREASURER INSTRIDE PIEDMONT FOOT & ANKLE CLINIC DUNN, NC
 SURGICAL APPROACHES TO FIRST RAY ELIZABETH BASS DAUGHTRY, DPM, FACFAS AAWP TREASURER INSTRIDE PIEDMONT FOOT & ANKLE CLINIC DUNN, NC HALLUX ABDUCTOVALGUS DEFORMITY Bunion Categories PASA Deformity only
SURGICAL APPROACHES TO FIRST RAY ELIZABETH BASS DAUGHTRY, DPM, FACFAS AAWP TREASURER INSTRIDE PIEDMONT FOOT & ANKLE CLINIC DUNN, NC HALLUX ABDUCTOVALGUS DEFORMITY Bunion Categories PASA Deformity only
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
ORTHOLOC 3Di. Foot Reconstruction System SURGIC AL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
CARTIVA. Synthetic Cartilage Implant PRODUCT MONOGRAPH. The Only PMA Approved Product for the Treatment of 1st MTP Osteoarthritis
 Synthetic Cartilage Implant The Only PMA Approved Product for the Treatment of 1st MTP Osteoarthritis PRODUCT MONOGRAPH TABLE OF CONTENTS I. INTRODUCTION...1 II. OVERVIEW OF OSTEOARTHRITIS...2 A. Epidemiology
Synthetic Cartilage Implant The Only PMA Approved Product for the Treatment of 1st MTP Osteoarthritis PRODUCT MONOGRAPH TABLE OF CONTENTS I. INTRODUCTION...1 II. OVERVIEW OF OSTEOARTHRITIS...2 A. Epidemiology
QUICK REFERENCE GUIDE. MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING
 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
ABSTRACT. Key Words: Hallux Rigidus, toe, arthrodesis, fusion, arthroplasty, MTP, HemiCAP resurfacing. Level of Evidence: Review
 RESURFACING OF THE FIRST METATARSAL HEAD FOR THE TREATMENT OF HALLUX RIGIDUS: EVOLUTION OF IMPLANT DESIGN, REVIEW OF CLINICAL EXPERIENCE AND PRELIMINARY 5 YEAR RESULTS OF METATARSAL HEAD RESURFACING MTP
RESURFACING OF THE FIRST METATARSAL HEAD FOR THE TREATMENT OF HALLUX RIGIDUS: EVOLUTION OF IMPLANT DESIGN, REVIEW OF CLINICAL EXPERIENCE AND PRELIMINARY 5 YEAR RESULTS OF METATARSAL HEAD RESURFACING MTP
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
DARCO. Bow 2 Plate SURGIC AL TECHNIQUE
 DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
PEDUS-L. Locking Plantar Lapidus Plate
 PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
Gender Differences in End-Stage Ankle Arthritis
 Gender Differences in End-Stage Ankle Arthritis Andrew Dodd MD, FRCSC Ellie Pinsker BA&Sc, PhD Cand. Elizabeth Jose Ryan Khan BA Mark Glazebrook MSc, PhD, MD, FRCSC Kevin Wing MD, FRCSC Murray Penner MD,
Gender Differences in End-Stage Ankle Arthritis Andrew Dodd MD, FRCSC Ellie Pinsker BA&Sc, PhD Cand. Elizabeth Jose Ryan Khan BA Mark Glazebrook MSc, PhD, MD, FRCSC Kevin Wing MD, FRCSC Murray Penner MD,
Technique Guide. 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot.
 Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Health-Related Quality of Life and Functional Outcomes in Ankle Arthritis Patients Based on Treating with and without Total Ankle Replacement Surgery
 Health-Related Quality of Life and Functional Outcomes in Ankle Arthritis Patients Based on Treating with and without Total Ankle Replacement Surgery Chayanin Angthong MD* * Division of Foot and Ankle
Health-Related Quality of Life and Functional Outcomes in Ankle Arthritis Patients Based on Treating with and without Total Ankle Replacement Surgery Chayanin Angthong MD* * Division of Foot and Ankle
Axi+LineTM Proximal Bunion CorrectionSystem. Surgical Technique
 Axi+LineTM Proximal Bunion CorrectionSystem Surgical Technique A i Line Proximal Bunion Correction System TM Desired angle correction is built into the plate, providing a self-reducing, 5-hole construct
Axi+LineTM Proximal Bunion CorrectionSystem Surgical Technique A i Line Proximal Bunion Correction System TM Desired angle correction is built into the plate, providing a self-reducing, 5-hole construct
Introduction Basics MIS Screw 2 System Characteristics 2 Indication 2
 Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Metatarsophalangeal joint replacement for hallux rigidus: a developing field
 OPN issue 168 Metatarsophalangeal joint replacement for hallux rigidus: a developing field Maire-Clare Killen, Liam McEntee, Mohan Emmanuel, Prasad Karpe and Rajiv Limaye describe the use of arthroplasty
OPN issue 168 Metatarsophalangeal joint replacement for hallux rigidus: a developing field Maire-Clare Killen, Liam McEntee, Mohan Emmanuel, Prasad Karpe and Rajiv Limaye describe the use of arthroplasty
INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement
 016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
Technique Guide Toe Hemiarthroplasty
 Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Technique Guide Toe Hemiarthroplasty
 Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
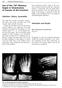 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy
 Surgical Technique Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa Iowa
Surgical Technique Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa Iowa
Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy
 Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES
 PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities
 Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
DYNAMIC, TRANSVERSE COMPRESSION. Low Profile, Anatomic Design, Type II Anodized. Mechanical Compression Designed to Stimulate the Fusion Process
 CoLink_XP_ST_080218.pdf 1 8/2/18 8:36 AM SURGICAL TECHNIQUE CoLink XP Plates DYNAMIC, TRANSVERSE COMPRESSION C M Y CM MY CY CMY K MTP Std. Plate MTP Revision Plate Lapidus Standard +1mm and +2mm Y Plate
CoLink_XP_ST_080218.pdf 1 8/2/18 8:36 AM SURGICAL TECHNIQUE CoLink XP Plates DYNAMIC, TRANSVERSE COMPRESSION C M Y CM MY CY CMY K MTP Std. Plate MTP Revision Plate Lapidus Standard +1mm and +2mm Y Plate
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT. Miss Sue Kendall PhD FRCS (Orth&Trauma)
 THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito
 Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Shoulder Joint Replacement
 Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Foot & Ankle. EasyClip. Osteosynthesis Compression Staples. Foot & Ankle
 Foot & Ankle EasyClip Osteosynthesis Compression Staples Foot & Ankle Operative Technique EasyClip Osteosynthesis Compression Staples 2 This publication sets forth detailed recommended procedures for using
Foot & Ankle EasyClip Osteosynthesis Compression Staples Foot & Ankle Operative Technique EasyClip Osteosynthesis Compression Staples 2 This publication sets forth detailed recommended procedures for using
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
ToeMobile. Surgical Technique. Great Toe Endoprosthesis
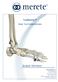 Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
Patients Expectations of Foot and Ankle Surgery: Variations by Diagnosis
 Patients Expectations of Foot and Ankle Surgery: Variations by Diagnosis Elizabeth A Cody, MD; Jayme C. B. Koltsov, PhD; Anca Marinescu; Carol A. Mancuso, MD; Scott J Ellis, MD; HSS Orthopaedic Foot and
Patients Expectations of Foot and Ankle Surgery: Variations by Diagnosis Elizabeth A Cody, MD; Jayme C. B. Koltsov, PhD; Anca Marinescu; Carol A. Mancuso, MD; Scott J Ellis, MD; HSS Orthopaedic Foot and
Utility of Ultrasound for Imaging Osteophytes in Patients with Insertional Achilles Tendinopathy
 Digital Commons @ George Fox University Faculty Publications - School of Physical Therapy School of Physical Therapy 2-2015 Utility of Ultrasound for Imaging Osteophytes in Patients with Insertional Achilles
Digital Commons @ George Fox University Faculty Publications - School of Physical Therapy School of Physical Therapy 2-2015 Utility of Ultrasound for Imaging Osteophytes in Patients with Insertional Achilles
PATIENT INFORMATION Cartiva implant surgery
 PATIENT INFORMATION Cartiva implant surgery Introduction This leaflet will explain what will happen when you come to the hospital for an operation to have a Cartiva implant inserted into your toe joint.
PATIENT INFORMATION Cartiva implant surgery Introduction This leaflet will explain what will happen when you come to the hospital for an operation to have a Cartiva implant inserted into your toe joint.
The Stanmore Orthopaedic Series
 RNOH EDUCATION The Stanmore Orthopaedic Series 20 th Stanmore Foot & Ankle Course 17 th - 19 th May 2016 The Course Aimed at Consultant Orthopaedic Surgeons, Higher Surgical Trainees & Orthopaedic Career
RNOH EDUCATION The Stanmore Orthopaedic Series 20 th Stanmore Foot & Ankle Course 17 th - 19 th May 2016 The Course Aimed at Consultant Orthopaedic Surgeons, Higher Surgical Trainees & Orthopaedic Career
Flower Medium Headless & Cannulated Screws
 Flower Medium Headless & Cannulated Screws PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Flower Medium Headless & Cannulated Screws PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot.
 Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
5 COMMON CONDITIONS IN THE FOOT & ANKLE
 5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
6.5 mm midfoot fusion bolt
 6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD
 Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E.
 Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E. Easley, MD Duke University Medical Center Durham, NC Disclosures Predictors
Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E. Easley, MD Duke University Medical Center Durham, NC Disclosures Predictors
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System.
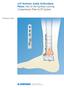 LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
innovative and comprehensive product line Metatarsophalangeal Joint Lower Hallux Limitus Hallux Rigidus Extremity
 Surgical Solutions innovative and comprehensive product line Metatarsophalangeal Joint Hallux Limitus Hallux Rigidus Lower Extremity Solutions Hallux Limitus and Hallux Rigidus Hallux limitus is a progressive
Surgical Solutions innovative and comprehensive product line Metatarsophalangeal Joint Hallux Limitus Hallux Rigidus Lower Extremity Solutions Hallux Limitus and Hallux Rigidus Hallux limitus is a progressive
Intramedullary fibular fixation in the operative management of fractures of the distal tibia and fibula
 Royal Liverpool & Broadgreen University Hospitals NHS Foundation Trust Intramedullary fibular fixation in the operative management of fractures of the distal tibia and fibula Michael Smith MBChB, Zuned
Royal Liverpool & Broadgreen University Hospitals NHS Foundation Trust Intramedullary fibular fixation in the operative management of fractures of the distal tibia and fibula Michael Smith MBChB, Zuned
Lapidus procedure and Akin osteotomy
 Lapidus procedure and Akin osteotomy Bunion surgery Information for patients Department of Podiatric Surgery What is a bunion? A bunion is a bony deformity of the joint at the base of the big toe (hallux).
Lapidus procedure and Akin osteotomy Bunion surgery Information for patients Department of Podiatric Surgery What is a bunion? A bunion is a bony deformity of the joint at the base of the big toe (hallux).
Investigation performed at the Department of Orthopaedic and Trauma Surgery, Glasgow Royal Infirmary, Glasgow, United Kingdom
 748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Lesser metatarsal cuneiform joint fusion for the treatment of midfoot osteoarthritis. Information for patients Department of Podiatric Surgery
 Lesser metatarsal cuneiform joint fusion for the treatment of midfoot osteoarthritis Information for patients Department of Podiatric Surgery What is midfoot osteoarthritis? Midfoot arthritis is 'wear
Lesser metatarsal cuneiform joint fusion for the treatment of midfoot osteoarthritis Information for patients Department of Podiatric Surgery What is midfoot osteoarthritis? Midfoot arthritis is 'wear
Comparing Fixation Used for Calcaneal Displacement Osteotomies: A look at removal rates and cost
 Comparing Fixation Used for Calcaneal Displacement Osteotomies: A look at removal rates and cost Douglas E. Lucas, DO 1 G. Alex Simpson, DO 1 Terrence M. Philbin, DO 2 Advanced Orthopedic Foot & Ankle
Comparing Fixation Used for Calcaneal Displacement Osteotomies: A look at removal rates and cost Douglas E. Lucas, DO 1 G. Alex Simpson, DO 1 Terrence M. Philbin, DO 2 Advanced Orthopedic Foot & Ankle
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant
 Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Does the SF-36 Mental Health Composite Score Predict Functional Outcome after Surgery in Patients with End Stage Ankle Arthritis?
 Does the SF-36 Mental Health Composite Score Predict Functional Outcome after Surgery in Patients with End Stage Ankle Arthritis? Kennedy SA, Barske H, Penner M, Daniels T, Glazebrook M, Wing K, Dryden
Does the SF-36 Mental Health Composite Score Predict Functional Outcome after Surgery in Patients with End Stage Ankle Arthritis? Kennedy SA, Barske H, Penner M, Daniels T, Glazebrook M, Wing K, Dryden
Transmetatarsal amputation in an at-risk diabetic population: a retrospective study
 The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
MetaFix Ludloff Plate
 Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
Metallic hemiarthroplasty for the treatment of end-stage hallux rigidus
 FOOT AND ANKLE Metallic hemiarthroplasty for the treatment of end-stage hallux rigidus MID-TERM IMPLANT SURVIVAL, FUNCTIONAL OUTCOME AND COST ANALYSIS N. D. Clement, D. MacDonald, G. F. Dall, I. Ahmed,
FOOT AND ANKLE Metallic hemiarthroplasty for the treatment of end-stage hallux rigidus MID-TERM IMPLANT SURVIVAL, FUNCTIONAL OUTCOME AND COST ANALYSIS N. D. Clement, D. MacDonald, G. F. Dall, I. Ahmed,
)221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE
 )221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE First Metatarsophalangeal Joint Arthrodesis: A Retrospective Comparison of Crossed-screws, Locking and Non-Locking Plate
)221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE First Metatarsophalangeal Joint Arthrodesis: A Retrospective Comparison of Crossed-screws, Locking and Non-Locking Plate
How to avoid complications of distraction osteogenesis for first brachymetatarsia
 220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
