Investigation performed at the Department of Orthopaedic Surgery, University of Minnesota, Minneapolis, Minnesota
|
|
|
- Christal Owens
- 5 years ago
- Views:
Transcription
1 514 COPYRIGHT 2006 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Treatment of Primarily Ligamentous Lisfranc Joint Injuries: Primary Arthrodesis Compared with Open Reduction and Internal Fixation A PROSPECTIVE, RANDOMIZED STUDY BY THUAN V. LY, MD, AND J. CHRIS COETZEE, MD, FRCSC Investigation performed at the Department of Orthopaedic Surgery, University of Minnesota, Minneapolis, Minnesota Background: Open reduction and internal fixation is currently the accepted treatment for displaced Lisfranc joint injuries. However, even with anatomic reduction and stable internal fixation, treatment of these injuries does not have uniformly excellent outcomes. The objective of this study was to compare primary arthrodesis with open reduction and internal fixation for the treatment of primarily ligamentous Lisfranc joint injuries. Methods: Forty-one patients with an isolated acute or subacute primarily ligamentous Lisfranc joint injury were enrolled in a prospective, randomized clinical trial comparing primary arthrodesis with traditional open reduction and internal fixation. The patients were followed for an average of 42.5 months. Evaluation was performed with clinical examination, radiography, the American Orthopaedic Foot and Ankle Society (AOFAS) Midfoot Scale, a visual analog pain scale, and a clinical questionnaire. Results: Twenty patients were treated with open reduction and screw fixation, and twenty-one patients were treated with primary arthrodesis of the medial two or three rays. Anatomic initial reduction was obtained in eighteen of the twenty patients in the open-reduction group and twenty of the twenty-one in the arthrodesis group. At two years postoperatively, the mean AOFAS Midfoot score was 68.6 points in the open-reduction group and 88 points in the arthrodesis group (p < 0.005). Five patients in the open-reduction group had persistent pain with the development of deformity or osteoarthrosis, and they were eventually treated with arthrodesis. The patients who had been treated with a primary arthrodesis estimated that their postoperative level of activities was 92% of their preinjury level, whereas the open-reduction group estimated that their postoperative level was only 65% of their preoperative level (p < 0.005). Conclusions: A primary stable arthrodesis of the medial two or three rays appears to have a better short and mediumterm outcome than open reduction and internal fixation of ligamentous Lisfranc joint injuries. Level of Evidence: Therapeutic Level I. See Instructions to Authors for a complete description of levels of evidence. A commentary is available with the electronic versions of this article, on our web site ( and on our quarterly CD-ROM (call our subscription department, at , to order the CD-ROM). Lisfranc joint injuries (tarsometatarsal dislocations or fracture-dislocations) are uncommon, and they are frequently missed or misdiagnosed 1-4. However, even with accurate diagnosis and early treatment, these injuries can result in chronic disability 5. Over the past several decades, Lisfranc complex injuries have been treated with closed reduction and immobilization, closed reduction and percutaneous pinning 3,6-9, or open reduction and percutaneous pinning or screw fixation It has become evident that an anatomic reduction is critical for optimal outcomes and that this is best achieved with open reduction 7, However, the method of treatment is still controversial. Currently, the recommended and accepted treatment of Lisfranc complex injuries is open reduction and internal fixation 10-13, but, despite appropriate initial treatment, painful osteoarthrosis still develops in some patients 3,8, necessitating conversion to an arthrodesis of the
2 515 tarsometatarsal joints to achieve pain relief. According to the current literature, primary arthrodesis is not recommended for Lisfranc complex injuries 9,11. Instead, arthrodesis has been reserved as a salvage procedure after failed open reduction and internal fixation, for a delayed or missed diagnosis, and for severely comminuted intra-articular fractures of the tarsometatarsal joints 7,11, Kuo et al. 12 suggested that there is a subgroup of patients with a purely ligamentous Lisfranc injury who may be better treated with primary fusion. More recently, Mulier et al. 10 compared the results of primary arthrodesis with those of open reduction and internal fixation for severe Lisfranc injuries in a retrospective, surgeonrandomized study. They advocated open reduction and internal fixation or partial arthrodesis for severe Lisfranc injuries, believing that primary complete arthrodesis should be reserved as a salvage procedure. The purpose of the present prospective study was to test the hypothesis that treatment of high-energy ligamentous Lisfranc injuries with primary open reduction and internal fixation would have the same or better functional short and medium-term outcomes as treatment with a primary partial arthrodesis. Materials and Methods e performed a prospective study comparing two groups W of patients with a Lisfranc joint injury. The study design was to include all injuries that were seen up to one month after the accident, although all forty-one patients had the surgery within three weeks from the date of injury and most had it within the first week. The Lisfranc joint injury had to be primarily ligamentous, with no major fractures present (Fig. 1-A). Lisfranc joint injuries with a fleck sign (an avulsion fracture of the Lisfranc ligament) were considered to be primarily ligamentous and were included in the study. Exclusion criteria were a comminuted intra-articular fracture at the base of the first or second metatarsal; any other substantial foot, ankle, or leg injury; a previous attempt at surgical management of the same injury; insulin-dependent diabetes mellitus; ipsilateral ankle fusion; peripheral vascular disease; peripheral neuropathy; and rheumatoid arthritis. Between March 1998 and January 2002, forty-one patients who met the inclusion criteria were enrolled in the study; this was a consecutive series as no patient refused to participate in the study. The study was approved by our institutional review board (IRB-0212M37742), and informed consent was obtained from the patients. All patients had been followed for at least two years. A power analysis done before the study showed that we needed thirty-eight patients to demonstrate a significant difference between the two groups with regard to the American Orthopaedic Foot and Ankle Society (AOFAS) Midfoot Scale scores. This number represented a power of 0.8. Patients were randomized with use of an odd-or-even process, based on the order of presentation, to the arthrodesis group or the open-reduction group as they presented with the Lisfranc joint injury. For example, the first patient was assigned to the arthrodesis group, and the next patient was automatically assigned to the open-reduction group. There was no variation from this protocol at any time during the study. Patients in the arthrodesis group were treated with primary arthrodesis of the medial two or three rays, depending on the instability pattern. If the radiographs and computed tomography scan showed an instability pattern that involved the first and second metatarsal-cuneiform joints but no instability of the third, only the medial two rays were fused. However, if the third metatarsal-cuneiform joint was displaced, it was reduced and fused as well. Three patients also had instability between the medial and middle cuneiforms, and that joint was included in the fusion. The first metatarsal-cuneiform joint was fused in all but one patient, in whom only the second and third metatarsal-cuneiform joints were fused. If the radiographs and computed tomography scan showed a subluxation or dislocation of the lateral two rays, they were assessed under fluoroscopy after treatment of the medial rays. If they appeared to be well reduced and stable, no treatment was provided. If there was still a malreduction or if they were unstable with manipulation, the fourth and fifth rays were reduced and were stabilized with temporary Kirschner-wire fixation, but they were not fused. The Kirschner wires were removed at six weeks. Autogenous bone graft or allograft was not utilized in the primary arthrodesis group. Patients in the open-reduction group were treated in the conventional way with formal open reduction and internal fixation, which was done with screw fixation of the medial two or three rays. The indications for Kirschner-wire fixation of the lateral two rays were exactly the same as those in the arthrodesis group. The lateral two rays were not fused in any of the forty-one patients. Standard 3.5 or 4.0-mm cortical screws were utilized depending on the patient s size. Postoperative follow-up was performed at two weeks, six weeks, three months, and six months, and then annually. We evaluated the outcomes with clinical examination, radiography, a visual analog pain scale (of 0 to 10), the AOFAS Midfoot Scale 18, and a clinical questionnaire. Alignment was assessed on weight-bearing anteroposterior, lateral, and oblique radiographs, which were made at each follow-up visit except for the one at two weeks. Alignment was assessed on the basis of whether the medial border of the second metatarsal lined up with the medial border of the middle cuneiform on the anteroposterior radiograph, whether the medial border of the fourth metatarsal lined up with the medial border of the cuboid on the oblique radiograph, and whether there was any dorsal displacement of the metatarsals relative to the tarsal bones on the lateral radiograph. The clinical questionnaire included questions regarding patient satisfaction (dissatisfied, somewhat dissatisfied, neutral, somewhat satisfied, or very satisfied) with the treatment and questions regarding their return to their previous level of physical or sports activities. In addition, the patients were asked to estimate their level of activities as a percentage of the level before the injury. Finally, the patients were asked to rate the pain on a visual analog pain scale that ranged from 0 (no pain) to 10 (severe pain).
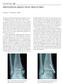
3 516 Arthrodesis Group There were twenty-one patients, fourteen men and seven women, in the arthrodesis group. Ten patients were injured in a motor-vehicle, snowmobile, or dirt-bike accident. Seven patients fell from a height of >4 ft (>1.2 m). Two patients fell off a horse while the foot was stuck in the stirrup, and two patients stepped into a deep hole. The average age at the time of injury was thirty-two years (range, nineteen to forty-two years), and the average duration of follow-up was 43.4 months (range, twenty-five to sixty months). Surgical Technique Open Reduction and Internal Fixation Two dorsal longitudinal incisions one between the first and second metatarsals and the second centered between the fourth and fifth metatarsals were made. Open reduction and screw fixation of the first, second, and third metatarsal-cuneiform joints was performed (Fig. 1-B). Then, if necessary, Kirschner wires were placed in each of the lateral two rays, but the rays were not fused. Seven patients in the open-reduction group required Kirschner-wire fixation of the lateral rays. The Kirschner wires were removed between six and eight weeks postoperatively. The screws were not routinely removed unless they caused symptoms, and they were never removed before three months. Fig. 1-A Anteroposterior radiograph of a primarily ligamentous Lisfranc joint injury, showing the instability pattern of the tarsometatarsal joints. Open-Reduction Group There were twenty patients, thirteen men and seven women, in the open-reduction group. Twelve patients were injured in a motor-vehicle, snowmobile, or all-terrain-vehicle accident. Five patients fell from a height of >4 ft (>1.2 m). One patient was playing basketball when another player fell on his foot. Another patient was injured in a pile-up in an ice hockey game, and one patient stepped into a 2-ft (0.6-m) deep hole in the ground. The average age at the time of injury in this group was 32.4 years (range, nineteen to fifty-two years), and the average duration of follow-up was forty-two months (range, twenty-five to sixty months). Fig. 1-B Intraoperative view of the open reduction and screw fixation of the Lisfranc joints.
4 517 Fig. 1-C The screws were removed at seven months. These radiographs, made at eighteen months, show degenerative changes of the first and second tarsometatarsal joints. Arthrodesis Standard incisions were made as described for the open-reduction group. Open reduction was performed, cartilage and fibrous tissue were resected, and the joints were decorticated. Reduction and screw fixation was then performed. If the third metatarsal-cuneiform joint was seen to be displaced on the computed tomography scan or was clearly unstable on direct examination, it was fused in the same fashion. The rationale for treatment of the lateral two rays was exactly the same as the rationale in the open-reduction group. Nine patients in the arthrodesis group underwent temporary Kirschner-wire fixation of the lateral two rays. Postoperative Management Postoperatively, all patients wore a short leg splint for two weeks followed by a short leg cast for four to six weeks, and all remained non-weight-bearing during this time. The patients then slowly advanced to full weight-bearing over the next four weeks while wearing a prefabricated fracture boot. Physical therapy was started at svix to ten weeks and included gait-training, swelling control, and range-of-motion exercises. Over-the-counter or custom-made orthotics were prescribed on an as-needed basis, depending on residual symptoms. Statistical Analysis GraphPad InStat software (GraphPad Software, San Diego, California) was used to perform the statistical analysis for the study. The Mann-Whitney test was used to derive an unpaired two-tailed p value. A p value of <0.05 indicated significance. Results Open-Reduction Group Complications and Additional Surgery f the twenty patients in the open-reduction group, six- underwent secondary surgery to remove prominent Oteen or painful hardware. The screws were removed at an average of 6.75 months (range, three to sixteen months). Follow-up radiographs showed evidence of loss of correction, increasing deformity, and degenerative joint disease in fifteen patients (Fig. 1-C). Five of these patients required conversion to tarsometatarsal arthrodesis at an average of thirty-five months (range, fourteen to sixty months) after the injury. Two more patients were scheduled for conversion to an arthrodesis at the time of manuscript preparation. Functional Questionnaire We present the functional results that were determined at the most recent follow-up evaluation. The results for the patients
5 518 TABLE I Patient Satisfaction at the Time of the Last Follow-up No. of Patients Open Reduction Arthrodesis and Internal Fixation Very satisfied 16 8 Somewhat satisfied 5 3 Neutral 3 Dissatisfied 6 who underwent a secondary fusion were determined at the last follow-up visit prior to the fusion. Eight patients reported that they were very satisfied with the result, three were somewhat satisfied, three were neutral, and six were dissatisfied (Table I). Five of the six patients who were dissatisfied with the outcome went on to have a tarsometatarsal fusion. All five later reported that they were very satisfied with the result at the time of the last follow-up. Six of the twenty patients reported that they were able to return to their preinjury level of physical or sports activities, and fourteen stated that they were not able to do so. On the average, the patients estimated their return to physical or sports activity, as a percentage of the preinjury level, to be 44% at the sixmonth postoperative visit, 61% at the one-year visit, and 65% at the two-year visit (Table II). Arthrodesis Group The arthrodesis group as a whole did very well. Anatomic reduction was obtained in twenty of the twenty-one patients. The average time to fusion was 10.6 weeks. Nineteen patients had an uncomplicated fusion, one needed treatment with a bone stimulator, and one required bone-grafting and revision fusion. Twelve patients had three rays fused, and nine had two rays fused; there was no difference in outcome between these two subgroups. Complications and Additional Surgery Of the twenty-one patients in the arthrodesis group, four (19%) required a second surgical procedure, primarily for removal of painful hardware. The screws were removed at an average of 6.5 months (range, five to ten months). One patient had a delayed union at seventeen weeks; a bone stimulator was used, and a solid fusion was achieved over the next eight weeks. One patient with a nonunion at twenty weeks underwent a revision arthrodesis with bone graft from the calcaneus. The fusion healed uneventfully at eight weeks after the revision surgery. Another patient had a posttraumatic intrinsic compartment syndrome that resulted in clawtoes. This patient underwent percutaneous flexor tendon release of the lesser toes and was pleased with the result. Functional Questionnaire Sixteen patients reported that they were very satisfied with the result, and five were somewhat satisfied (Table I). Fifteen patients reported that thvey were able to return to their previous level of physical or sports activities, and six stated that they were unable to do so. The patients estimation of their return to physical and sports activity, as a percentage of the preinjury level, averaged 62% at six months postoperatively, 86% at one year, and 92% at two years (Table II). AOFAS Midfoot Scores and Visual Analog Pain Scores At the time of the two-year follow-up, the AOFAS score averaged 88.0 points (range, 63 to 100 points) in the arthrodesis group and 68.6 points (range, 16 to 100 points) in the openreduction group (p = 0.005). At the time of final follow-up (at an average of forty-two months in the open-reduction group and forty-three months in the arthrodesis group), the AOFAS Midfoot score averaged 57.1 points (range, 16 to 100 points) in the open-reduction group (including the five patients who had undergone conversion to a tarsometatarsal arthrodesis) and 86.9 points (range, 63 to 100 points) in the arthrodesis group (p < ). When the five patients in the open-reduction group who had had a conversion to midfoot arthrodesis were excluded, the average final AOFAS Midfoot score for the remaining fifteen patients was 65.2 points (range, 27 to 100 points), and the arthrodesis group still had a better average score than the open-reduction group (p < ). As stated, five of the patients who were originally treated with open reduction and internal fixation had a conversion to a fusion. Three of the four who had the arthrodesis more than two years before our review were available for evaluation. Their mean AOFAS score at two years was 79.0 points, which was better than the mean for the open-reduction group but lower than that for the primary arthrodesis group. These four patients mean estimate of their functional ability after the fusion was 80% of their preinjury level. The number of patients in this subgroup is too small for us to draw any conclusions, but the findings show a trend toward improvement after secondary fusion but results that are not as good as those following a primary fusion. At the time of final follow-up, the average score on the visual analog pain scale was 4.1 points in the open-reduction group and 1.2 points in the arthrodesis group (p = ). Discussion reating intra-articular fractures and dislocations poses T unique challenges. It is important to look at every joint s TABLE II Patient s Estimation of Level of Functional Participation Compared with Preinjury Status Percentage of Preinjury Level 6 Mo 12 Mo 24 Mo* Arthrodesis Open reduction and internal fixation *The difference between the treatment groups was significant (p < 0.005).
6 519 function specifically when deciding which treatment options are realistic. For example, a fusion of the knee is very seldom used, even as a salvage procedure, for the treatment of a distal femoral fracture. In contrast, feet with a Lisfranc joint fracture are often salvaged with a fusion, without a devastating effect on function. However, we are not aware of any prospective studies in the literature focusing on the issue of primary fusion or comparing fusion with open reduction and internal fixation for Lisfranc joint injuries, although it is evident from the literature that the results of open reduction 7,11-13 are better than those of closed reduction and that screw fixation is better than percutaneous pinning 3,6,7,9-13, at least for the medial three rays. Recently, most authors have recommended open reduction and internal fixation instead of primary arthrodesis for Lisfranc joint injuries However, because persistent pain and posttraumatic degenerative changes occur despite anatomic reduction 3,8, we speculated that there may be a subset of Lisfranc injuries that are better treated with primary arthrodesis of the involved tarsometatarsal joints. Kuo et al. 12 pointed out that purely ligamentous Lisfranc injuries do not always heal following open reduction and internal fixation and that there was a tendency for this type of injury to result in osteoarthrosis (a finding in six of their fifteen patients). In our study, fifteen of the twenty patients in the openreduction group lost correction and had at least some deformity and degenerative arthritic changes, which ranged from a minor loss of correction to substantial collapse and degenerative changes. Five of our patients had persistent pain and underwent a salvage arthrodesis, and two more patients were awaiting an arthrodesis at the time of writing. The mean AOFAS Midfoot score in our open-reduction group (57.1 points) was lower than the mean score for the patients in the study by Kuo et al. (78.8 points). However, our arthrodesis group had a better outcome, with a mean AOFAS Midfoot score of 86.9 points. This information suggests that patients with a primarily ligamentous Lisfranc injury should be treated with primary arthrodesis. Sixteen of the twenty patients in our open-reduction group had removal of hardware, and we believe that that was a confounding factor for the poor results seen in that group. However, we also believe that the injury itself, being primarily ligamentous, plays a major part in the healing and outcome of these injuries. A review of the radiographs made prior to hardware removal indicated that some early degenerative changes and collapse of the midfoot had developed in the majority of patients. Radiographs made at a later follow-up visit showed that most of the patients went on to have progressive degenerative changes after the screws were removed. We postulate that, because these injuries were primarily ligamentous, healing of the ligaments and capsules provided insufficient strength to maintain the initial reduction. This is evidenced by the fact that, despite initial anatomic reduction in eighteen of the twenty patients, some loss of correction, further collapse, and degenerative changes of the Lisfranc joint developed after screw removal in fifteen patients. Recent studies 10,14,16 have compared complete and partial arthrodeses for the treatment of Lisfranc joint injuries, and we found one study comparing open reduction and internal fixation with primary arthrodesis. In that surgeon-randomized study of twenty-eight patients, which had some similarities to our study, Mulier et al. 10 compared open reduction and internal fixation (sixteen patients) with complete arthrodesis (six patients) and partial arthrodesis (six patients). They concluded that a complete fusion (of all five tarsometatarsal joints) yields poor results and that open reduction and internal fixation provides a better functional outcome. We agree with that conclusion. Mulier et al. reported that, at the time of final follow-up (at thirty months), 94% of their open-reduction group already had radiographic signs of degenerative changes of the tarsometatarsal joints. At that juncture, the open-reduction group had the same functional score as the group treated with partial fusion, but it can be assumed that the score in the open-reduction group would decrease with time because of the high rate of identified degenerative changes. The authors of two previous studies recommended that only the medial two or three rays be fused. We concur with Komenda et al. 14 and Sangeorzan et al. 16 that it is beneficial for a patient to have motion in the lateral two rays and that it is not necessary to perform a complete fusion to obtain optimum results. Komenda et al. reported the results of arthrodeses that were performed to treat intractable pain at a mean of thirty-five months after traumatic tarsometatarsal joint injury. The mean AOFAS Midfoot score was 78 points at a mean of fifty months postoperatively. In our study, the mean AOFAS Midfoot score in the arthrodesis group was 86.9 points at a mean of 43.4 months postoperatively. This finding suggests that performing immediate primary fusion helps patients to avoid several years of persistent pain and disability. Our study had several limitations. First, the allocation of treatment with an open-randomization, odd-or-even format could have introduced selection bias. Using a random-numbers table or computerized randomization would have been a better way to allocate our patients. Second, the attending surgeon performed the follow-up clinical examination and gathered the questionnaires, which raises a concern about bias. However, the patients were given the questionnaires when they arrived at the clinic and had completed them on their own by the time that they were seen in the clinic. The attending surgeon just gathered the forms and made sure that they were entered into the database. Third, we did not obtain information or determine the outcomes for the patients with Lisfranc joint injuries who were not included in the study because they met our exclusion criteria. Outcome information on the patients with osseous involvement would have provided a group with which to compare our patients, who had the less common, ligamentous Lisfranc injuries. Fourth, hardware removal could have contributed to the poor results that were seen in the openreduction group. In summary, because of the poor healing potential of the ligament-osseous interface and the trend toward a higher rate of correction loss, increasing deformity, and degenerative arthritic changes, we believe that primarily ligamentous injuries are a subset of Lisfranc joint injuries that are not as ame-
7 520 nable to internal fixation. We believe that stable arthrodesis is a better primary treatment for these injuries, with superior short and medium-term outcomes than those following open reduction and internal fixation. Thuan V. Ly, MD J. Chris Coetzee, MD, FRCSC Department of Orthopaedic Surgery, University of Minnesota, 2450 Riverside Avenue, R200, Minneapolis, MN address for J.C. Coetzee: coetz001@umn.edu The authors did not receive grants or outside funding in support of their research for or preparation of this manuscript. They did not receive payments or other benefits or a commitment or agreement to provide such benefits from a commercial entity. No commercial entity paid or directed, or agreed to pay or direct, any benefits to any research fund, foundation, educational institution, or other charitable or nonprofit organization with which the authors are affiliated or associated. doi: /jbjs.e References 1. Teng AL, Pinzur MS, Lomasney L, Mahoney L, Havey R. Functional outcome following anatomic restoration of tarsal-metatarsal fracture dislocation. Foot Ankle Int. 2002;23: Myerson M. The diagnosis and treatment of injuries to the Lisfranc joint complex. Orthop Clin North Am. 1989;20: Granberry W, Lipscomb PR. Dislocation of the tarsometatarsal joints. Surg Gynecol Obstet. 1962;114: Chiodo CP, Myerson MS. Developments and advances in the diagnosis and treatment of injuries to the tarsometatarsal joint. Orthop Clin North Am. 2001;32: Buzzard BM, Briggs PJ. Surgical management of acute tarsometatarsal fracture dislocation in the adult. Clin Orthop Relat Res. 1998;353: Myerson MS, Fisher RT, Burgess AR, Kenzora JE. Fracture dislocation of the tarsometatarsal joints: end results correlated with pathology and treatment. Foot Ankle. 1986;6: Trevino SG, Kodros S. Controversies in tarsometatarsal injuries. Orthop Clin North Am. 1995;26: Hardcastle PH, Reschauer R, Kutscha-Lissberg E, Schoffmann W. Injuries to the tarsometatarsal joint. J Bone Joint Surg Br. 1982;64: Lenczner EM, Waddell JP, Graham JD. Tarsal-metatarsal (Lisfranc) dislocation. J Trauma. 1974;14: Mulier T, Reynders P, Dereymaeker G, Broos P. Severe Lisfrancs injuries: primary arthrodesis or ORIF? Foot Ankle Int. 2002;23: Arntz CT, Veith RG, Hansen ST Jr. Fractures and fracture-dislocations of the tarsometatarsal joint. J Bone Joint Surg Am. 1988;70: Kuo RS, Tejwani NC, Digiovanni CW, Holt SK, Benirschke SK, Hansen ST Jr, Sangeorzan BJ. Outcome after open reduction and internal fixation of Lisfranc joint injuries. J Bone Joint Surg Am. 2000;82: Arntz CT, Hansen ST Jr. Dislocation and fracture dislocations of the tarsometatarsal joints. Orthop Clin North Am. 1987;18: Komenda GA, Myerson MS, Biddinger KR. Results of arthrodesis of the tarsometatarsal joints after traumatic injury. J Bone Joint Surg Am. 1996;78: Mann RA, Prieskorn D, Sobel M. Mid-tarsal and tarsometatarsal arthrodesis for primary degenerative osteoarthrosis or osteoarthrosis after trauma. J Bone Joint Surg Am. 1996;78: Sangeorzan BJ, Veith RG, Hansen ST Jr. Salvage of Lisfranc s tarsometatarsal joint by arthrodesis. Foot Ankle. 1990;10: Treadwell JR, Kahn MD. Lisfranc arthrodesis for chronic pain: a cannulated screw technique. J Foot Ankle Surg. 1998;37: Kitaoka HB, Alexander IJ, Adelaar RS, Nunley JA, Myerson MS, Sanders M. Clinical rating systems for the ankle-hindfoot, midfoot, hallux and lesser toes. Foot Ankle Int. 1994;15:
8
Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment
 Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment S Y Loh, FRCS (Orth)*, J L Soon, MBBS**, W J Verhoeven, FRCS*** *Department of Orthopedic Surgery, Alexandra Hospital,
Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment S Y Loh, FRCS (Orth)*, J L Soon, MBBS**, W J Verhoeven, FRCS*** *Department of Orthopedic Surgery, Alexandra Hospital,
Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E.
 Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E. Easley, MD Duke University Medical Center Durham, NC Disclosures Predictors
Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E. Easley, MD Duke University Medical Center Durham, NC Disclosures Predictors
Lisfranc injuries. Mikko Kirjavainen, MD, PhD. Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland
 Lisfranc injuries Mikko Kirjavainen, MD, PhD Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland Lisfranc injuries are midfoot fracture dislocations. The
Lisfranc injuries Mikko Kirjavainen, MD, PhD Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland Lisfranc injuries are midfoot fracture dislocations. The
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium
 MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations
 Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations Anish R. Kadakia, Mark S. Myerson, and Milap Patel Contents Mechanism of Injury... 2 Radiographic Evaluation... 3 Classification...
Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations Anish R. Kadakia, Mark S. Myerson, and Milap Patel Contents Mechanism of Injury... 2 Radiographic Evaluation... 3 Classification...
Outcome After Open Reduction and Internal Fixation of Lisfranc Joint Injuries *
 Outcome After Open Reduction and Internal Fixation of Lisfranc Joint Injuries * BY R. S. KUO, M.B.B.S., F.R.A.C.S., N. C. TEJWANI, M.D., C. W. DIGIOVANNI, M.D., S. K. HOLT, M.S.P.H.#, S. K. BENIRSCHKE,
Outcome After Open Reduction and Internal Fixation of Lisfranc Joint Injuries * BY R. S. KUO, M.B.B.S., F.R.A.C.S., N. C. TEJWANI, M.D., C. W. DIGIOVANNI, M.D., S. K. HOLT, M.S.P.H.#, S. K. BENIRSCHKE,
Hany El-Rashidy and Anand Vora
 Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY
 60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
Complications of missed or untreated Lisfranc injuries
 Foot Ankle Clin N Am 8 (2003) 61 71 Complications of missed or untreated Lisfranc injuries Terry Philbin, DO a,b, *, Gary Rosenberg, MD c, James J. Sferra, MD d a Orthopedic Foot and Ankle, 6200 Cleveland
Foot Ankle Clin N Am 8 (2003) 61 71 Complications of missed or untreated Lisfranc injuries Terry Philbin, DO a,b, *, Gary Rosenberg, MD c, James J. Sferra, MD d a Orthopedic Foot and Ankle, 6200 Cleveland
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion
 Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion W I L L I A M P. H U N T I N G T O N, M. D. W. H O D G E S D A V I S, M. D. R O B E R T B. A N D E R S O N,
Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion W I L L I A M P. H U N T I N G T O N, M. D. W. H O D G E S D A V I S, M. D. R O B E R T B. A N D E R S O N,
Midfoot arthritis, a specific complaint in adults,
 A Review Paper Midfoot Arthritis Siraj A. Sayeed, MD, Fazel A. Khan, MD, Norman S. Turner III, MD, and Harold B. Kitaoka, MD Abstract Foot and ankle complaints are commonly encountered in orthopedic practice.
A Review Paper Midfoot Arthritis Siraj A. Sayeed, MD, Fazel A. Khan, MD, Norman S. Turner III, MD, and Harold B. Kitaoka, MD Abstract Foot and ankle complaints are commonly encountered in orthopedic practice.
Annual Surgical Conference LisFranc Fractures. Zeeshan S. Husain, DPM, FACFAS, FASPS. Great Lakes Foot and Ankle Institute September 21, 2018
 Annual Surgical Conference 2018 LisFranc Fractures Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Jacques LisFranc 1790 1847 History LisFranc
Annual Surgical Conference 2018 LisFranc Fractures Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Jacques LisFranc 1790 1847 History LisFranc
Foot Injuries. Dr R B Kalia
 Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Complexities surrounding Lisfranc injuries
 Complexities surrounding Lisfranc injuries Lisfranc injuries are commonly associated with sporting injuries and are easily diagnosed with severe midfoot pain, swelling, deformity and inability to bear
Complexities surrounding Lisfranc injuries Lisfranc injuries are commonly associated with sporting injuries and are easily diagnosed with severe midfoot pain, swelling, deformity and inability to bear
Investigation performed at the Department of Orthopaedic and Trauma Surgery, Glasgow Royal Infirmary, Glasgow, United Kingdom
 748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
Clinical Outcomes and Development of Symptomatic Osteoarthritis Two to Twenty- Four Years After Surgery for Tarsometatarsal Joint Complex Injuries
 Clinical Outcomes and Development of Symptomatic Osteoarthritis Two to Twenty- Four Years After Surgery for Tarsometatarsal Joint Complex Injuries Victor Dubois-Ferrière, MD, 1 Anne Lübbeke, MD, MSc, 1
Clinical Outcomes and Development of Symptomatic Osteoarthritis Two to Twenty- Four Years After Surgery for Tarsometatarsal Joint Complex Injuries Victor Dubois-Ferrière, MD, 1 Anne Lübbeke, MD, MSc, 1
Lisfranc fracture-dislocations. Disclosures. It s just a foot
 Lisfranc fracture-dislocations Gregory J. Della Rocca, MD, PhD, FACS Associate Professor Co-director, Orthopaedic Trauma Service University of Missouri Disclosures Consultant: Synthes, Bioventus Stock
Lisfranc fracture-dislocations Gregory J. Della Rocca, MD, PhD, FACS Associate Professor Co-director, Orthopaedic Trauma Service University of Missouri Disclosures Consultant: Synthes, Bioventus Stock
Midfoot - Reduction & Fixation - ORIF - screw fixation - AO Surgery Reference. ORIF - screw fixation
 Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture
 CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
Primary open reduction and fixation compared with delayed corrective arthrodesis in the treatment of tarsometatarsal (Lisfranc) fracture dislocation
 Primary open reduction and fixation compared with delayed corrective arthrodesis in the treatment of tarsometatarsal (Lisfranc) fracture dislocation S. Rammelt, W. Schneiders, H. Schikore, M. Holch, J.
Primary open reduction and fixation compared with delayed corrective arthrodesis in the treatment of tarsometatarsal (Lisfranc) fracture dislocation S. Rammelt, W. Schneiders, H. Schikore, M. Holch, J.
Temporary bridge plating of the medial column in Chopart and Lisfranc injuries
 Temporary bridge plating of the medial column in Chopart and Lisfranc injuries by Alaa Mansour DPM 1*, Lawrence Fallat DPM, FACFAS 2 The Foot and Ankle Online Journal 10 (1): 5 Severe traumatic injuries
Temporary bridge plating of the medial column in Chopart and Lisfranc injuries by Alaa Mansour DPM 1*, Lawrence Fallat DPM, FACFAS 2 The Foot and Ankle Online Journal 10 (1): 5 Severe traumatic injuries
One Month Old Neglected Lisfrancs Fracture Dislocation Treated with Wagner's External Fixator and Percutaneous Screw Fixation : A Case Report
 Case Report Journal of Orthopaedic Case Reports 2014 April-June;4(2): Page 42-46 One Month Old Neglected Lisfrancs Fracture Dislocation Treated with Wagner's External Fixator and Percutaneous Screw Fixation
Case Report Journal of Orthopaedic Case Reports 2014 April-June;4(2): Page 42-46 One Month Old Neglected Lisfrancs Fracture Dislocation Treated with Wagner's External Fixator and Percutaneous Screw Fixation
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury
 Section Editor: Steven F. Harwin, MD Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury Richard E. Stern, MD; Mathieu ssal, MD bstract: Following a Lisfranc joint
Section Editor: Steven F. Harwin, MD Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury Richard E. Stern, MD; Mathieu ssal, MD bstract: Following a Lisfranc joint
LISFRANC FRACTURE-DISLOCATION
 LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
Technique Guide. 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot.
 Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
The influence of approach and implant on reduction accuracy and stability in Lisfranc
 The influence of approach and implant on reduction accuracy and stability in Lisfranc fracture-dislocation at the tarsometatarsal joint T. Schepers MD PhD, P.P. Oprel MD, E.M.M. Van Lieshout PhD Erasmus
The influence of approach and implant on reduction accuracy and stability in Lisfranc fracture-dislocation at the tarsometatarsal joint T. Schepers MD PhD, P.P. Oprel MD, E.M.M. Van Lieshout PhD Erasmus
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Lisfranc and Midfoot Fracture
 Lisfranc and Midfoot Fracture AO Advanced Principles of Fracture Management Middelfart, 11.-14. april 2016 Overlæge Marianne Vestergaard Lind Traumesektionen Ortopædkirurgisk Klinik Rigshospitalet What
Lisfranc and Midfoot Fracture AO Advanced Principles of Fracture Management Middelfart, 11.-14. april 2016 Overlæge Marianne Vestergaard Lind Traumesektionen Ortopædkirurgisk Klinik Rigshospitalet What
Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
 Injury Extra (2008) 39, 291 295 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/inext CASE REPORT Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
Injury Extra (2008) 39, 291 295 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/inext CASE REPORT Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement
 016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
EVALUATION OF THE SURGICAL TREATMENT OF LISFRANC JOINT FRACTURE-DISLOCATION
 Original Article EVALUATION OF THE SURGICAL TREATMENT OF LISFRANC JOINT FRACTURE-DISLOCATION Cléber de Jesus Pereira 1, Eduardo Gomes Espinosa 2, Ivan Miranda 3, Marcelo Bueno Pereira 4, Roberto Sérgio
Original Article EVALUATION OF THE SURGICAL TREATMENT OF LISFRANC JOINT FRACTURE-DISLOCATION Cléber de Jesus Pereira 1, Eduardo Gomes Espinosa 2, Ivan Miranda 3, Marcelo Bueno Pereira 4, Roberto Sérgio
Index. Note: Page numbers of article titles are in boldface type. Hand Clin 21 (2005)
 Hand Clin 21 (2005) 501 505 Index Note: Page numbers of article titles are in boldface type. A Antibiotics, following distal radius fracture treatment, 295, 296 Arthritis, following malunion of distal
Hand Clin 21 (2005) 501 505 Index Note: Page numbers of article titles are in boldface type. A Antibiotics, following distal radius fracture treatment, 295, 296 Arthritis, following malunion of distal
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
American Family Physician
 Page 1 of 12 American Family Physician Return to Previous Page Jul 1, 1998 Table of Contents Lisfranc Injury of the Foot: A Commonly Missed Diagnosis KEVIN E. BURROUGHS, M.D, Moses Cone Family Practice
Page 1 of 12 American Family Physician Return to Previous Page Jul 1, 1998 Table of Contents Lisfranc Injury of the Foot: A Commonly Missed Diagnosis KEVIN E. BURROUGHS, M.D, Moses Cone Family Practice
Matthew Beuchel MD 2 C. Luke Rust MD 3 Jessica Hooper MD 3
 A Prospective, Randomized,Controlled Trial Comparing Early- Weightbearing vs. Non-Weightbearing Following Modified Lapidus Arthrodesis Intermediate Results - Donald R. Bohay, MD, FACS Professor, Michigan
A Prospective, Randomized,Controlled Trial Comparing Early- Weightbearing vs. Non-Weightbearing Following Modified Lapidus Arthrodesis Intermediate Results - Donald R. Bohay, MD, FACS Professor, Michigan
Midfoot Arthritis - Midfoot Fusion / Arthrodesis Surgery
 PATIENT INFORMATION Midfoot Arthritis - Midfoot Fusion / Arthrodesis Surgery The Midfoot The midfoot refers to the bones and joints that make up the arch and connect the forefoot to the hindfoot. Metatarsals
PATIENT INFORMATION Midfoot Arthritis - Midfoot Fusion / Arthrodesis Surgery The Midfoot The midfoot refers to the bones and joints that make up the arch and connect the forefoot to the hindfoot. Metatarsals
6.5 mm midfoot fusion bolt
 6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Section 3: Foot Subluxations and Dislocations
 Section 3: Foot Subluxations and Dislocations Case Study F: Lisfranc s Midfoot Dislocation Clinical History: J.K. a 28 year old female presents complaining of a painful right foot. She sustained an acute
Section 3: Foot Subluxations and Dislocations Case Study F: Lisfranc s Midfoot Dislocation Clinical History: J.K. a 28 year old female presents complaining of a painful right foot. She sustained an acute
CHARLOTTE Lisfranc. Recontruction System SURGICAL TECHNIQUE
 CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
SYMPOSIUM: CURRENT ISSUES IN ORTHOPAEDIC TRAUMA: TRIBUTE TO CLIFFORD H. TUREN
 Clin Orthop Relat Res (2016) 474:1445 1452 DOI 10.1007/s11999-015-4366-y Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: CURRENT ISSUES
Clin Orthop Relat Res (2016) 474:1445 1452 DOI 10.1007/s11999-015-4366-y Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: CURRENT ISSUES
Staged Treatment of High Energy Midfoot Fracture Dislocations
 552077FAIXXX10.1177/1071100714552077Foot & Ankle InternationalKadow et al research-article2014 Article Staged Treatment of High Energy Midfoot Fracture Dislocations Foot & Ankle International 2014, Vol.
552077FAIXXX10.1177/1071100714552077Foot & Ankle InternationalKadow et al research-article2014 Article Staged Treatment of High Energy Midfoot Fracture Dislocations Foot & Ankle International 2014, Vol.
MULTIPLE APPLICATIONS OF THE MINIRAIL
 C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
Treatment of calcaneal fractures: the available evidence
 J Orthopaed Traumatol (2007) 8:36 41 DOI 10.1007/s10195-007-0160-2 EVIDENCE-BASED MEDICINE SECTION R. Bondì R. Padua L. Bondì A. Battaglia E. Romanini A. Campi Treatment of calcaneal fractures: the available
J Orthopaed Traumatol (2007) 8:36 41 DOI 10.1007/s10195-007-0160-2 EVIDENCE-BASED MEDICINE SECTION R. Bondì R. Padua L. Bondì A. Battaglia E. Romanini A. Campi Treatment of calcaneal fractures: the available
Open Reduction and Internal Fixation to Repair a Lisfranc Injury: A Case Report
 Case Report imedpub Journals http://www.imedpub.com 2015 Abstract Open Reduction and Internal Fixation to Repair a Lisfranc Injury: A Case Report Background: Lisfranc complex consists of bony and ligamentous
Case Report imedpub Journals http://www.imedpub.com 2015 Abstract Open Reduction and Internal Fixation to Repair a Lisfranc Injury: A Case Report Background: Lisfranc complex consists of bony and ligamentous
Arthritis of the Foot and Ankle
 Arthritis of the Foot and Ankle Arthritis is inflammation of one or more of your joints. It can cause pain and stiffness in any joint in the body, and is common in the small joints of the foot and ankle.
Arthritis of the Foot and Ankle Arthritis is inflammation of one or more of your joints. It can cause pain and stiffness in any joint in the body, and is common in the small joints of the foot and ankle.
Fractures of the Calcaneus
 Fractures of the Calcaneus Anthony T. Sorkin, M.D. Rockford Orthopedic Trauma Service Rajeev Garapati, MD Illinois Bone and Joint Institute Assistant Clinical Professor University of Illinois at Chicago
Fractures of the Calcaneus Anthony T. Sorkin, M.D. Rockford Orthopedic Trauma Service Rajeev Garapati, MD Illinois Bone and Joint Institute Assistant Clinical Professor University of Illinois at Chicago
19 Arthrodesis of the First Metatarsocuneiform Joint
 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
Epidemiology, Treatment and Outcome of 169 Lisfranc Fracture/Dislocations
 Epidemiology, Treatment and Outcome of 169 Lisfranc Fracture/Dislocations Layseca A, Bastías G, Zagal P, Reyes N, Delgado M, Gutierrez R, Verschae G. Foot and Ankle Unit Hospital del Trabajador Santiago,
Epidemiology, Treatment and Outcome of 169 Lisfranc Fracture/Dislocations Layseca A, Bastías G, Zagal P, Reyes N, Delgado M, Gutierrez R, Verschae G. Foot and Ankle Unit Hospital del Trabajador Santiago,
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation
 Journal of Sport Rehabilitation, 1993, 2, 281-286 O 1993 Human Kinetics Publishers, Inc. A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation Keith M. Gorse, Graham Johnstone, and Jennifer
Journal of Sport Rehabilitation, 1993, 2, 281-286 O 1993 Human Kinetics Publishers, Inc. A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation Keith M. Gorse, Graham Johnstone, and Jennifer
Retrospective Study of Surgical Outcomes for Combined Ankle and Subtalar Joint Arthrodesis, Cavovarus Deformity Correction and Ankle Fractures
 FOOT/ ANKLE RETROSPECTIVE STUDYIC S Retrospective Study of Surgical Outcomes for Combined Ankle and Subtalar Joint Arthrodesis, Cavovarus Deformity Correction and Ankle Fractures Adult & Pediatric Deformity
FOOT/ ANKLE RETROSPECTIVE STUDYIC S Retrospective Study of Surgical Outcomes for Combined Ankle and Subtalar Joint Arthrodesis, Cavovarus Deformity Correction and Ankle Fractures Adult & Pediatric Deformity
ROTATIONAL PILON FRACTURES
 CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Injuries to the Lisfranc Joint and its Significance for the Patient
 Cronicon OPEN ACCESS EC ORTHOPAEDICS Case Report Injuries to the Lisfranc Joint and its Significance for the Patient Ekkehard Pietsch* Orthopaedic and General Surgeon, The-Expert-Witness.de, Hamburg, Germany
Cronicon OPEN ACCESS EC ORTHOPAEDICS Case Report Injuries to the Lisfranc Joint and its Significance for the Patient Ekkehard Pietsch* Orthopaedic and General Surgeon, The-Expert-Witness.de, Hamburg, Germany
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation *
 Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Lisfranc Fracture-Dislocation/ Arthrodesis
 Lisfranc Fracture-Dislocation/ Arthrodesis 16 Lawrence A. Di Domenico and Frank A. Luckino Introduction L.A. Di Domenico (*) Ankle and Foot Care Centers, Youngstown, OH, USA Kent State University, College
Lisfranc Fracture-Dislocation/ Arthrodesis 16 Lawrence A. Di Domenico and Frank A. Luckino Introduction L.A. Di Domenico (*) Ankle and Foot Care Centers, Youngstown, OH, USA Kent State University, College
Diabetics. Referred for management of complex pilon fracture? 5/10/2017. Pilon Fractures: Exfix as definitive treatment (DM?)
 Pilon Fractures: Exfix as definitive treatment (DM?) Nirmal C Tejwani, MD Professor, NYU Langone Orthopedics Chief of Trauma, Bellevue Hospital, New York, NY 29 th Annual Orthopaedic Trauma Meeting May
Pilon Fractures: Exfix as definitive treatment (DM?) Nirmal C Tejwani, MD Professor, NYU Langone Orthopedics Chief of Trauma, Bellevue Hospital, New York, NY 29 th Annual Orthopaedic Trauma Meeting May
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation
 Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation By Leonhard E. Ramseier, MD, Joseph A. Janicki, MD, Shannon Weir, BSc, and Unni G. Narayanan, MBBS, MSc, FRCSC Investigation performed
Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation By Leonhard E. Ramseier, MD, Joseph A. Janicki, MD, Shannon Weir, BSc, and Unni G. Narayanan, MBBS, MSc, FRCSC Investigation performed
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
Tarsometatarsal (Lisfranc) Joint Dislocation
 CHAPTER 106 Tarsometatarsal (Lisfranc) Joint Dislocation Lawrence A. DiDomenico Dawn Y. Stein Fracture dislocations of the tarsal metatarsal (Lisfranc injuries) can be subtle and may be missed in both
CHAPTER 106 Tarsometatarsal (Lisfranc) Joint Dislocation Lawrence A. DiDomenico Dawn Y. Stein Fracture dislocations of the tarsal metatarsal (Lisfranc injuries) can be subtle and may be missed in both
Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini
 Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Treatment of malunited fractures of the ankle
 Treatment of malunited fractures of the ankle A LONG-TERM FOLLOW-UP OF RECONSTRUCTIVE SURGERY I. I. Reidsma, P. A. Nolte, R. K. Marti, E. L. F. B. Raaymakers From Academic Medical Center, Amsterdam, Netherlands
Treatment of malunited fractures of the ankle A LONG-TERM FOLLOW-UP OF RECONSTRUCTIVE SURGERY I. I. Reidsma, P. A. Nolte, R. K. Marti, E. L. F. B. Raaymakers From Academic Medical Center, Amsterdam, Netherlands
Lesser metatarsal cuneiform joint fusion for the treatment of midfoot osteoarthritis. Information for patients Department of Podiatric Surgery
 Lesser metatarsal cuneiform joint fusion for the treatment of midfoot osteoarthritis Information for patients Department of Podiatric Surgery What is midfoot osteoarthritis? Midfoot arthritis is 'wear
Lesser metatarsal cuneiform joint fusion for the treatment of midfoot osteoarthritis Information for patients Department of Podiatric Surgery What is midfoot osteoarthritis? Midfoot arthritis is 'wear
pedcat Clinical Case Studies
 pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Fracture and Dislocation of the Carpus ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
AOFAS 2012 ANNUAL SUMMER MEETING. Subtalar Distraction Two Bone-Block Arthrodesis for Calcaneal Malunion
 AOFAS 2012 ANNUAL SUMMER MEETING Subtalar Distraction Two Bone-Block Arthrodesis for Calcaneal Malunion My disclosure is in the Final AOFAS Program Book. I have no potential conflicts with this presentation.
AOFAS 2012 ANNUAL SUMMER MEETING Subtalar Distraction Two Bone-Block Arthrodesis for Calcaneal Malunion My disclosure is in the Final AOFAS Program Book. I have no potential conflicts with this presentation.
Case Report Lateral Subtalar Dislocation with Tarsometatarsal Dislocation: A Case Report of a Rare Injury
 Hindawi Case Reports in Orthopedics Volume 2017, Article ID 8090721, 6 pages https://doi.org/10.1155/2017/8090721 Case Report Lateral Subtalar Dislocation with Tarsometatarsal Dislocation: A Case Report
Hindawi Case Reports in Orthopedics Volume 2017, Article ID 8090721, 6 pages https://doi.org/10.1155/2017/8090721 Case Report Lateral Subtalar Dislocation with Tarsometatarsal Dislocation: A Case Report
Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture Dislocation of the Elbow in an Adult
 Hindawi Case Reports in Orthopedics Volume 2018, Article ID 5401634, 6 pages https://doi.org/10.1155/2018/5401634 Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture
Hindawi Case Reports in Orthopedics Volume 2018, Article ID 5401634, 6 pages https://doi.org/10.1155/2018/5401634 Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
The Latest Breakthrough in TTC Fusion Technology
 The Latest Breakthrough in TTC Fusion Technology Treatment of Hindfoot Non-Union with DynaNail TTC Fusion System A CASE REPORT Dr. L. Daniel Latt, MD, PhD Background The DynaNail TTC Fusion System is intended
The Latest Breakthrough in TTC Fusion Technology Treatment of Hindfoot Non-Union with DynaNail TTC Fusion System A CASE REPORT Dr. L. Daniel Latt, MD, PhD Background The DynaNail TTC Fusion System is intended
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Ankle Arthritis and Ankle Replacement
 Ankle Arthritis and Ankle Replacement Ryan DeBlis, MD Disclosures I have no disclosures. 1 Diagnosis Ankle arthritis Majority (70%) of patients are post-traumatic (ie, after ankle fracture) Primary arthritis
Ankle Arthritis and Ankle Replacement Ryan DeBlis, MD Disclosures I have no disclosures. 1 Diagnosis Ankle arthritis Majority (70%) of patients are post-traumatic (ie, after ankle fracture) Primary arthritis
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
PRONATION-ABDUCTION FRACTURES
 C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT
 C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Conservative Management of Calcaneal Fractures. A Retrospective Review of Treatment Outcome
 Conservative Management of Calcaneal Fractures. A Retrospective Review of Treatment Outcome HY Wong, MD, AS Vivek*, FRCS (Edin), BC Se To, FRCS (Edin) Department of Orthopaedics and Traumatology, Hospital
Conservative Management of Calcaneal Fractures. A Retrospective Review of Treatment Outcome HY Wong, MD, AS Vivek*, FRCS (Edin), BC Se To, FRCS (Edin) Department of Orthopaedics and Traumatology, Hospital
Injuries of the Foot and Ankle. Introduction. Introduction 10/2/2009. Bryan Lapinski, MD
 Injuries of the Foot and Ankle Bryan Lapinski, MD Introduction The average person takes 1 million steps per year Approximately 30 bones in the foot and ankle are subjected to forces of 3 7 times body weight
Injuries of the Foot and Ankle Bryan Lapinski, MD Introduction The average person takes 1 million steps per year Approximately 30 bones in the foot and ankle are subjected to forces of 3 7 times body weight
The Ludloff Osteotomy
 Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Peggers Super Summaries: Foot Injuries
 Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Lisfranc injuries: Patient- and physician-based functional outcomes
 International Orthopaedics (SICOT) (2003) 27:98 102 DOI 10.1007/s00264-002-0415-8 ORIGINAL ARTICLE P.A. O Connor S. Yeap J. Noël G. Khayyat J.G. Kennedy S. Arivindan A.J. McGuinness Lisfranc injuries:
International Orthopaedics (SICOT) (2003) 27:98 102 DOI 10.1007/s00264-002-0415-8 ORIGINAL ARTICLE P.A. O Connor S. Yeap J. Noël G. Khayyat J.G. Kennedy S. Arivindan A.J. McGuinness Lisfranc injuries:
A Prospective Study on Fractured Tarsal Navicular Bone in a Tertiary Care Teaching Hospital
 Original article: A Prospective Study on Fractured Tarsal Navicular Bone in a Tertiary Care Teaching Hospital Mohammad Azmoddin 1, Surender Rao Yadagiri 2 1Associate Professor, Department of Orthopaedics,
Original article: A Prospective Study on Fractured Tarsal Navicular Bone in a Tertiary Care Teaching Hospital Mohammad Azmoddin 1, Surender Rao Yadagiri 2 1Associate Professor, Department of Orthopaedics,
University of Groningen. Fracture of the distal radius Oskam, Jacob
 University of Groningen Fracture of the distal radius Oskam, Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Fracture of the distal radius Oskam, Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Fracture and Dislocation of Metacarpal Bones, Metacarpophalangeal Joints, Phalanges, and Interphalangeal Joints ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
Double calcaneal osteotomy for severe adolescent flexible flatfoot reconstruction
 Xu et al. Journal of Orthopaedic Surgery and Research (2017) 12:153 DOI 10.1186/s13018-017-0655-3 RESEARCH ARTICLE Open Access Double calcaneal osteotomy for severe adolescent flexible flatfoot reconstruction
Xu et al. Journal of Orthopaedic Surgery and Research (2017) 12:153 DOI 10.1186/s13018-017-0655-3 RESEARCH ARTICLE Open Access Double calcaneal osteotomy for severe adolescent flexible flatfoot reconstruction
Investigation performed at Orthopaedic Hospital Gersthof, Vienna, Austria
 1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Case Report A Case Report of Isolated Cuboid Nutcracker Fracture
 Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
Financial Disclosure. Turf Toe
 Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Tibial plateau fractures: four years review at B&B Hospital
 Kathmandu University Medical Journal (2004) Vol. 2, No. 4, Issue 8, 315-323 Original Article Tibial plateau fractures: four years review at B&B Hospital Shrestha BK 1, Bijukachhe B 2, Rajbhandary T 2,
Kathmandu University Medical Journal (2004) Vol. 2, No. 4, Issue 8, 315-323 Original Article Tibial plateau fractures: four years review at B&B Hospital Shrestha BK 1, Bijukachhe B 2, Rajbhandary T 2,
Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI Procedure. Subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
Radiographic Evaluation of Calcaneal Fractures. Kali Luker, PGY-1
 Radiographic Evaluation of Calcaneal Fractures Kali Luker, PGY-1 Anatomy Extraarticular Fractures Involve body, anterior process or tuberosity Treated with immobilization and NWB x 6 wks UNLESS Displaced
Radiographic Evaluation of Calcaneal Fractures Kali Luker, PGY-1 Anatomy Extraarticular Fractures Involve body, anterior process or tuberosity Treated with immobilization and NWB x 6 wks UNLESS Displaced
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant
 Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
