Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations
|
|
|
- Ashlyn Robinson
- 5 years ago
- Views:
Transcription
1 Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations Anish R. Kadakia, Mark S. Myerson, and Milap Patel Contents Mechanism of Injury... 2 Radiographic Evaluation... 3 Classification... 4 Treatment... 5 Surgical Technique... 5 Postoperative Rehabilitation... 7 Summary... 8 References... 8 A.R. Kadakia (*) Northwestern University Feinberg School of Medicine, Northwestern Memorial Hospital, Chicago, IL, USA kadak259@gmail.com M.S. Myerson Mercy Medical Center, Baltimore, MD, USA mark4feet@aol.com M. Patel Department of Orthopedic Surgery, Northwestern University Feinberg School of Medicine, Chicago, IL, USA patelm0923@gmail.com Abstract Lisfranc injuries encompass a variety of trauma to the midfoot. These range from lowenergy mechanisms to high-energy crush injuries. No single approach is appropriate for all injury patterns. Current controversy has focused on the decision to fix or fuse the midfoot when treating a Lisfranc injury. This concept is an overly simplistic thought process for such a complex variety of soft tissue and bony injury patterns. Minimally invasive approaches to these injuries decrease the risk of further soft tissue trauma and allow for satisfactory reduction and stabilization in certain low-energy injury patterns. Additionally, patients comorbidities including diabetes, vascular disease, smoking, multitrauma may drive the surgeon to seek less invasive techniques to avoid wound complications while achieving the goals of creating a stable midfoot. The goal of the chapter is to delineate the indications and review the technique of a minimally invasive approach to Lisfranc injuries. Keywords Lisfranc Lisfranc fracture dislocation Lisfranc injury Percutaneous Percutaneous fixation Ligamentous Lisfranc # Springer International Publishing Switzerland 2015 G.R.Scuderi, A.J.Tria (eds.), Minimally Invasive Surgery in Orthopedics, DOI / _75-1 1
2 2 A.R. Kadakia et al. Fig. 1 An AP radiograph of a direct injury mechanism with significant displacement and bony comminution that is not amenable to percutaneous treatment The success of minimally invasive percutaneous reduction and fixation of tarsometatarsal or Lisfranc injuries lies in understanding the appropriate injury pattern for this method of treatment. The eponym Lisfranc dislocation is derived from injuries sustained to cavalry troops in the Napoleonic era. These were associated with significant vascular and soft tissue injury, as they were treated with an amputation through the tarsometatarsal joints by Lisfranc, Napoleon s surgeon. Although the injuries secondary to equestrian activity have declined, the injury pattern is commonly associated with high-energy motor vehicle accidents, falls, and crushing injuries to the foot [1 4]. These mechanisms typically involve significant bony and soft tissue injury that rarely can be managed by closed methods (Fig. 1). Percutaneous fixation is most amenable in those patients with low-energy mechanisms, particularly in the athletic and elderly populations involving primarily a ligamentous injury (Fig. 2). Fig. 2 An AP radiograph of a pure ligamentous injury that is ideally treated by percutaneous methods Mechanism of Injury The indirect mechanism associated with the low-energy injury typically results from an axial longitudinal force with rotation on a plantar flexed foot [5 9]. The plantar flexed position of the foot places the weaker dorsal ligamentous restraints on tension, resulting in their failure allowing further displacement and rupture of the plantar ligamentous restraints or metatarsal base fracture [1, 6, 10]. This type of injury may not produce the obvious clinical picture associated with direct high-energy injuries of severe swelling, deformity, inability to bear weight, and neurovascular compromise [11, 13]. Typical presentation includes swelling throughout the midfoot that improves after 1 week and therefore delayed presentations may not appear to have a significant
3 Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations 3 Fig. 3 (a) Note that the base of the second metatarsal is in continuity with the medial aspect of the middle cuneiform. (b) In a patient with a Lisfranc injury note the lateral injury upon visual examination [5]. Persistent pain and tenderness across the midfoot that is aggravated with stress testing of the tarsometatarsal joints is indicative of this injury pattern [12]. Radiographic Evaluation The radiographic series for a suspected Lisfranc injury should include anteroposterior (AP), lateral, and 30 internal oblique views of both feet. Additionally, external oblique views in both 10 and 20 have demonstrated efficacy in delineating the amount of displacement in the transverse plane [12]. In order to stress the midfoot and demonstrate the injury radiographically, the X-rays should be performed with as much weight bearing as possible. Occasionally, weight bearing is too difficult for the patient, therefore, if the nonweight-bearing X-ray results are normal, repeat weight-bearing views should be performed at days [6]. Stress radiographs can be performed to diagnose the instability; however, they should be performed under anesthesia to prevent a false negative finding. The foot is displacement of the second metatarsal in relation to the medial aspect of the middle cuneiform stressed with pronation combined with abduction to detect subtle diastasis or angulation [5, 6, 13]. Coss et al. [14] have shown in a cadaveric model that disruption of the dorsal and Lisfranc ligamentous restraints resulted in a radiographic instability pattern consistently noted on abduction stress examination, verifying the utility of the clinical examination. The anatomic relationships of the tarsometatarsal joints have consistent radiographic appearances; deviations from these patterns are consistent with injury [15]. The medial border of the second metatarsal is in colinearity with the medial border of the middle cuneiform on the AP radiographic exam along with the first intermetatarsal space and the space between the medial and middle cuneiforms (Fig. 3a, b). The lateral border of the third metatarsal is colinear with the lateral border of the lateral cuneiform on the internal oblique radiograph. In addition, the medial border of the fourth metatarsal is colinear with the medial border of the cuboid. Subtle radiographic findings include minor angulation or displacement of the first metatarsal (Fig. 4). Myerson et al. [3] described the fleck sign, a small avulsion fracture of either the medial cuneiform or the base of the second metatarsal, which is diagnostic
4 4 A.R. Kadakia et al. Fig. 4 An AP radiograph demonstrating lateral translation of the first metatarsal consistent with a Lisfranc injury of a Lisfranc disruption. Careful review of the radiographs should be performed so that Lisfranc variants with intercuneiform instability are not overlooked (Fig. 5). Classification Multiple classification systems exist to describe the injury to this joint complex [2, 3, 16]. The use of the columnar classification developed by Myerson [6, 13, 17] divides the midfoot based on the respective motion segments. The medial column includes the first tarsometatarsal and the medial cuneiform-navicular joints (Fig. 6a). The middle column includes the second and third tarsometatarsal, intercuneiform, and the naviculocuneiform joints (between the middle and lateral cuneiforms) (Fig. 6b). The lateral column includes the articulations between the fourth and fifth metatarsals and the cuboid (Fig. 6c). This system of classification has prognostic implications based Fig. 5 Note that the diastasis exists between the medial and middle cuneiforms, consistent with a Lisfranc injury, despite the normal relationship between the second metatarsal and the middle cuneiform on the motion of the midfoot. The medial and middle columns have minimal motion (3.5 and 0.6 mm, respectively) and do not tolerate incongruity, suffering the highest incidence of posttraumatic arthritis [17, 18]. Nunley and Vertullo have proposed a classification system to define the midfoot sprain typically seen in athletes [19]. Stage 1 is consistent with pain at the Lisfranc joint without any evidence of diastasis on weightbearing radiographs. Stage 2 involved 1 5mmof diastasis between the first and second metatarsal on the AP radiograph, with evidence of lateral arch collapse. Stage 3 is greater than 5 mm of diastasis and loss of midfoot arch height. Patients with stage 1 injuries were successfully treated with a nonoperative treatment protocol that included an initial 6 weeks of a non-weight-bearing fiberglass cast.
5 Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations 5 Fig. 6 The medial (a), middle (b), and lateral columns (c) are depicted Treatment Although recent literature may suggest that primary arthrodesis offers improved scores at a mean of 42.5 months of follow-up in ligamentous injuries over reduction and internal fixation, the longer-term complications of early arthrodesis may diminish these early results [20]. The current lack of a superior operative treatment method is indicative that treatment may consist of internal fixation or primary arthrodesis of Lisfranc injuries and stage 2 and 3 midfoot sprains via either percutaneous or open approaches. Percutaneous approaches are most amenable for patients with a stress only instability pattern, where the alignment of the midfoot is normal in a non-weightbearing position. This finding assures the surgeon that an acceptable alignment will be achieved without direct visualization. In patients with poor soft tissue status, vascular disease, neuropathy, or smoking, the use of a minimally invasive technique allows for stabilization of the midfoot while controlling for the risk of wound dehiscence and infection. In these cases, even in the setting of a frank disruption, near anatomic reduction may be preferred over a wound complication. Nonoperative treatment of these injuries is inappropriate as greater than 2 mm of displacement or 15 of angulation is associated with a poor outcome [3]. Surgical Technique The use of a percutaneous technique requires a thorough understanding of the anatomy of the tarsometatarsal joints and their appearance under fluoroscopy. The undertaking of a percutaneous approach should not be performed unless the surgeon is capable of performing an open reduction, as, on occasion, soft tissue or bony fragment interposition may prevent an anatomic reduction using closed methods. 3.5 mm solid or 4.0 mm cannulated screws are utilized. Initial attention must be performed to obtaining an anatomic reduction prior to any attempts at fixation. Longitudinal traction is required to reduce the tarsometatarsal joints, and utilization of gauze rolls secured around the phalanges is a powerful aid in reduction (Fig. 7). Initial attention is paid to the medial column, which provides a stable post to which the middle column is reduced. The reduction maneuver involves grasping the hallux firmly and placing a medial- or lateraldirected force to the base of the metatarsal to reduce the deformity. Once an anatomic reduction is achieved, provisional fixation is achieved with a guidewire for a cannulated screw (Fig. 8a, b). A screw is placed if appropriate reduction has been achieved. In this case, a fully threaded screw is utilized. A large bone clamp facilitates reduction of the second metatarsal into the mortise (Fig. 9a, b). If persistent diastasis remains despite
6 6 A.R. Kadakia et al. adjustment of the clamp, then conversion to an open reduction should be performed. Typically, this realigns the third and fourth metatarsals into an anatomic position. A fully threaded screw is then placed obliquely from the medial cuneiform to the base of the second metatarsal. In cases where the third TMT requires stabilization, placement of a screw from the proximal lateral third metatarsal into the middle cuneiform is performed. The guidewire should begin midway between the proximal metatarsal and the metatarsal head with regard to the entry position in the skin. The wire should be placed as parallel to the foot as possible to ensure a neutral position. A partially threaded screw of appropriate length is then placed in order to aid in reduction as it can be very difficult to clamp across this joint. Stability of the lateral column is assessed fluoroscopically and, if persistent instability exists, stabilization is performed with either a 1.6-mm K-wire (Fig. 10). If K-wire fixation is utilized for the lateral column, subcutaneous placement is important to prevent infection and premature removal. Fig. 7 Use of the gauze roll to create phalangeal slings to provide longitudinal traction and aid in closed reduction of the deformity Fig. 8 Lisfranc injury with displacement (a) and after closed reduction with provisional fixation of the medial column (b)
7 Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations 7 Fig. 9 Clinical (a) and fluoroscopic (b) depicting of the use of the bone clamp to reduce the base of the second metatarsal into the mortise Postoperative Rehabilitation Fig. 10 Final view of the foot after closed reduction and fixation Initial immobilization is a below knee posterior plaster splint to decrease swelling and enhance wound healing. Early mobilization and range of motion are encouraged and rigid fixation with screws is important to prevent loss of reduction. Removal of the splint at 2 weeks is followed by placement into a removable boot, although nonweight-bearing is continued for 6 weeks. Patients are allowed to begin range of motion and strengthening in a pool at 4 weeks and stationary biking is allowed at 6 weeks. Transition to full weight bearing in a removable boot is allowed at 6 weeks. Full weight bearing is allowed at 12 weeks, with conversion to an athletic shoe with a carbon fiber plate orthotic. Hardware removal is typically performed between 4 and 5 months, after which aggressive rehabilitation is performed under the direction of a therapist. Single plane running is initiated at 20 weeks and cutting sports are allowed at 24 weeks. In cases of poor soft tissue, vascular disease, neuropathy, smoking, or heavy labor, the screws may be left in place to decrease the risk of late diastasis. Although leaving the hardware in place may carry the risk of screw breakage, this risk is balanced by avoiding infection and late diastasis. In a healthy individual, screw removal
8 8 A.R. Kadakia et al. is appropriate to avoid the complications of hardware failure and further articular injury. Summary Disruptions of the tarsometatarsal joints can lead to significant disability if misdiagnosed and undertreated. Detailed review of weight-bearing radiographs of the affected extremity and a thorough understanding of the normal anatomic landmarks will consistently lead the clinician to diagnose of even subtle injuries to the midfoot. Percutaneous treatment of these injuries is a very appropriate option in select patients as it avoids the risk of wound complications and morbidity associated with extensile incisions. However, if any question of malreduction exists, conversion to an open reduction must be performed. References 1. Myerson M. Tarsometatarsal arthrodesis: technique and results of treatment after injury. Foot Ankle Clin. 1996;1: Hardcastle P, Reschauer R, Kutscha-Lissberg E, Schoffmann W. Injuries to the tarsometatarsal joint. Incidence, classification and treatment. J Bone Joint Surg (Br). 1982;64B(3): Myerson M, Fisher R, Burgess A, Kenzora J. Fracture dislocations of the tarsometatarsal joints: end results correlated with pathology and treatment. Foot Ankle. 1986;6(5): Gossens M, De Stoop N. Lisfranc fracture dislocations: etiology, radiology, and results of treatment. A review of 20 cases. Clin Orthop Relat Res. 1983;176: Curtis M, Myerson M, Szura B. Tarsometatarsal joint injuries in the athlete. Am J Sports Med. 1993;21: Chiodo C, Myerson M. Developments and advances in the diagnosis and treatment of injuries to the tarsometatarsal joint. Orthop Clin North Am. 2001;32 (1): Hatem ST, Davis A, Sundaram M. Your diagnosis? Midfoot sprain: Lisfranc ligament disruption. Orthopedics. 2005;28(1):2, Myerson MS, Cerrato RA. Current management of tarsometarsal injuries in the athlete. J Bone Joint Surg Am. 2008;90(11): Coetzee JC. Making sense of Lisfranc injuries. Foot Ankle Clin. 2008;13: Buzzard B, Briggs P. Surgical management of acute tarsometatarsal fracture dislocation in the adult. Clin Orthop Relat Res. 1998;353: Aronow M. Treatment of the missed Lisfranc injury. Foot Ankle Clin North Am. 2006;11: Myerson M. The diagnosis and treatment of injuries to the Lisfranc joint complex. Orthop Clin North Am. 1989;20: Myerson M. The diagnosis and treatment of injury to the tarsometatarsal joint complex. J Bone Joint Surg (Br). 1999;81-B: Coss H, Manos R, Buoncristiani A, Mills W. Abduction stress AP weightbearing radiography of purely ligamentous injury in the tarsometatarsal joint. Foot Ankle Int. 1998;19(8): Stein R. Radiological aspects of the tarsometatarsal joints. Foot Ankle. 1983;3: Quenu E, Kuss G. Etude sur les luxations du metatarse. Reb Chir Paris. 1909;39: Komenda G, Myerson M, Biddinger K. Results of arthrodesis of the tarsometatarsal joints after traumatic injury. J Bone Joint Surg Am. 1996;78: Ouzounian T, Shereff M. In vitro determination of midfoot motion. Foot Ankle. 1989;10: Nunley J, Vertullo C. Classification, investigation, and management of midfoot sprains. Lisfranc injuries in the athlete. Am J Sports Med. 2002;30(6): Ly T, Coetzee J. Treatment of the primarily ligamentous Lisfranc joint injuries: primary arthrodesis compared with open reduction and internal fixation. J Bone Joint Surg Am. 2006;88-A(3):
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium
 MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
Complexities surrounding Lisfranc injuries
 Complexities surrounding Lisfranc injuries Lisfranc injuries are commonly associated with sporting injuries and are easily diagnosed with severe midfoot pain, swelling, deformity and inability to bear
Complexities surrounding Lisfranc injuries Lisfranc injuries are commonly associated with sporting injuries and are easily diagnosed with severe midfoot pain, swelling, deformity and inability to bear
Midfoot - Reduction & Fixation - ORIF - screw fixation - AO Surgery Reference. ORIF - screw fixation
 Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Practical Management of Lisfranc injuries in Athletes
 Practical Management of Lisfranc injuries in Athletes Christian Lattermann, MD * ; Jordan L Goldstein, MD* ; Dane K. Wukich # ; Simon Lee, MD* and Bernard R. Bach Jr., MD 1* *Department of Orthopedic Surgery
Practical Management of Lisfranc injuries in Athletes Christian Lattermann, MD * ; Jordan L Goldstein, MD* ; Dane K. Wukich # ; Simon Lee, MD* and Bernard R. Bach Jr., MD 1* *Department of Orthopedic Surgery
Hany El-Rashidy and Anand Vora
 Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Complications of missed or untreated Lisfranc injuries
 Foot Ankle Clin N Am 8 (2003) 61 71 Complications of missed or untreated Lisfranc injuries Terry Philbin, DO a,b, *, Gary Rosenberg, MD c, James J. Sferra, MD d a Orthopedic Foot and Ankle, 6200 Cleveland
Foot Ankle Clin N Am 8 (2003) 61 71 Complications of missed or untreated Lisfranc injuries Terry Philbin, DO a,b, *, Gary Rosenberg, MD c, James J. Sferra, MD d a Orthopedic Foot and Ankle, 6200 Cleveland
Lisfranc and Midfoot Fracture
 Lisfranc and Midfoot Fracture AO Advanced Principles of Fracture Management Middelfart, 11.-14. april 2016 Overlæge Marianne Vestergaard Lind Traumesektionen Ortopædkirurgisk Klinik Rigshospitalet What
Lisfranc and Midfoot Fracture AO Advanced Principles of Fracture Management Middelfart, 11.-14. april 2016 Overlæge Marianne Vestergaard Lind Traumesektionen Ortopædkirurgisk Klinik Rigshospitalet What
Annual Surgical Conference LisFranc Fractures. Zeeshan S. Husain, DPM, FACFAS, FASPS. Great Lakes Foot and Ankle Institute September 21, 2018
 Annual Surgical Conference 2018 LisFranc Fractures Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Jacques LisFranc 1790 1847 History LisFranc
Annual Surgical Conference 2018 LisFranc Fractures Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Jacques LisFranc 1790 1847 History LisFranc
Outcome After Open Reduction and Internal Fixation of Lisfranc Joint Injuries *
 Outcome After Open Reduction and Internal Fixation of Lisfranc Joint Injuries * BY R. S. KUO, M.B.B.S., F.R.A.C.S., N. C. TEJWANI, M.D., C. W. DIGIOVANNI, M.D., S. K. HOLT, M.S.P.H.#, S. K. BENIRSCHKE,
Outcome After Open Reduction and Internal Fixation of Lisfranc Joint Injuries * BY R. S. KUO, M.B.B.S., F.R.A.C.S., N. C. TEJWANI, M.D., C. W. DIGIOVANNI, M.D., S. K. HOLT, M.S.P.H.#, S. K. BENIRSCHKE,
Open Reduction and Internal Fixation to Repair a Lisfranc Injury: A Case Report
 Case Report imedpub Journals http://www.imedpub.com 2015 Abstract Open Reduction and Internal Fixation to Repair a Lisfranc Injury: A Case Report Background: Lisfranc complex consists of bony and ligamentous
Case Report imedpub Journals http://www.imedpub.com 2015 Abstract Open Reduction and Internal Fixation to Repair a Lisfranc Injury: A Case Report Background: Lisfranc complex consists of bony and ligamentous
American Family Physician
 Page 1 of 12 American Family Physician Return to Previous Page Jul 1, 1998 Table of Contents Lisfranc Injury of the Foot: A Commonly Missed Diagnosis KEVIN E. BURROUGHS, M.D, Moses Cone Family Practice
Page 1 of 12 American Family Physician Return to Previous Page Jul 1, 1998 Table of Contents Lisfranc Injury of the Foot: A Commonly Missed Diagnosis KEVIN E. BURROUGHS, M.D, Moses Cone Family Practice
Investigation performed at the Department of Orthopaedic Surgery, University of Minnesota, Minneapolis, Minnesota
 514 COPYRIGHT 2006 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Treatment of Primarily Ligamentous Lisfranc Joint Injuries: Primary Arthrodesis Compared with Open Reduction and Internal Fixation
514 COPYRIGHT 2006 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Treatment of Primarily Ligamentous Lisfranc Joint Injuries: Primary Arthrodesis Compared with Open Reduction and Internal Fixation
Lisfranc injuries. Mikko Kirjavainen, MD, PhD. Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland
 Lisfranc injuries Mikko Kirjavainen, MD, PhD Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland Lisfranc injuries are midfoot fracture dislocations. The
Lisfranc injuries Mikko Kirjavainen, MD, PhD Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland Lisfranc injuries are midfoot fracture dislocations. The
Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment
 Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment S Y Loh, FRCS (Orth)*, J L Soon, MBBS**, W J Verhoeven, FRCS*** *Department of Orthopedic Surgery, Alexandra Hospital,
Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment S Y Loh, FRCS (Orth)*, J L Soon, MBBS**, W J Verhoeven, FRCS*** *Department of Orthopedic Surgery, Alexandra Hospital,
Foot Injuries. Dr R B Kalia
 Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Section 3: Foot Subluxations and Dislocations
 Section 3: Foot Subluxations and Dislocations Case Study F: Lisfranc s Midfoot Dislocation Clinical History: J.K. a 28 year old female presents complaining of a painful right foot. She sustained an acute
Section 3: Foot Subluxations and Dislocations Case Study F: Lisfranc s Midfoot Dislocation Clinical History: J.K. a 28 year old female presents complaining of a painful right foot. She sustained an acute
No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture
 CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
PRONATION-ABDUCTION FRACTURES
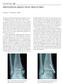 C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
LISFRANC FRACTURE-DISLOCATION
 LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
Lisfranc fracture-dislocations. Disclosures. It s just a foot
 Lisfranc fracture-dislocations Gregory J. Della Rocca, MD, PhD, FACS Associate Professor Co-director, Orthopaedic Trauma Service University of Missouri Disclosures Consultant: Synthes, Bioventus Stock
Lisfranc fracture-dislocations Gregory J. Della Rocca, MD, PhD, FACS Associate Professor Co-director, Orthopaedic Trauma Service University of Missouri Disclosures Consultant: Synthes, Bioventus Stock
Injuries to the Lisfranc Joint and its Significance for the Patient
 Cronicon OPEN ACCESS EC ORTHOPAEDICS Case Report Injuries to the Lisfranc Joint and its Significance for the Patient Ekkehard Pietsch* Orthopaedic and General Surgeon, The-Expert-Witness.de, Hamburg, Germany
Cronicon OPEN ACCESS EC ORTHOPAEDICS Case Report Injuries to the Lisfranc Joint and its Significance for the Patient Ekkehard Pietsch* Orthopaedic and General Surgeon, The-Expert-Witness.de, Hamburg, Germany
Temporary bridge plating of the medial column in Chopart and Lisfranc injuries
 Temporary bridge plating of the medial column in Chopart and Lisfranc injuries by Alaa Mansour DPM 1*, Lawrence Fallat DPM, FACFAS 2 The Foot and Ankle Online Journal 10 (1): 5 Severe traumatic injuries
Temporary bridge plating of the medial column in Chopart and Lisfranc injuries by Alaa Mansour DPM 1*, Lawrence Fallat DPM, FACFAS 2 The Foot and Ankle Online Journal 10 (1): 5 Severe traumatic injuries
Tarsometatarsal (Lisfranc) Joint Dislocation
 CHAPTER 106 Tarsometatarsal (Lisfranc) Joint Dislocation Lawrence A. DiDomenico Dawn Y. Stein Fracture dislocations of the tarsal metatarsal (Lisfranc injuries) can be subtle and may be missed in both
CHAPTER 106 Tarsometatarsal (Lisfranc) Joint Dislocation Lawrence A. DiDomenico Dawn Y. Stein Fracture dislocations of the tarsal metatarsal (Lisfranc injuries) can be subtle and may be missed in both
Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury
 Section Editor: Steven F. Harwin, MD Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury Richard E. Stern, MD; Mathieu ssal, MD bstract: Following a Lisfranc joint
Section Editor: Steven F. Harwin, MD Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury Richard E. Stern, MD; Mathieu ssal, MD bstract: Following a Lisfranc joint
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
radiologymasterclass.co.uk
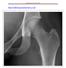 http://radiologymasterclass.co.uk Hip X-ray anatomy - Normal AP (anterior-posterior) Shenton's line is formed by the medial edge of the femoral neck and the inferior edge of the superior pubic ramus Loss
http://radiologymasterclass.co.uk Hip X-ray anatomy - Normal AP (anterior-posterior) Shenton's line is formed by the medial edge of the femoral neck and the inferior edge of the superior pubic ramus Loss
Traumatic Injuries to the Foot and Ankle
 Traumatic Injuries to the Foot and Ankle Dr. Joseph N. Daniel Clinical Associate Professor of Orthopaedic Surgery Foot and Ankle Service, The Rothman Institute Thomas Jefferson University Hospital Philadelphia,
Traumatic Injuries to the Foot and Ankle Dr. Joseph N. Daniel Clinical Associate Professor of Orthopaedic Surgery Foot and Ankle Service, The Rothman Institute Thomas Jefferson University Hospital Philadelphia,
Technique Guide. 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot.
 Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Deltoid and Syndesmosis Ligament Injury of the Ankle Without Fracture
 Deltoid and Syndesmosis Ligament Injury of the Ankle Without Fracture Chris D. Miller, MD, Walter R. Shelton,* MD, Gene R. Barrett, MD, F. H. Savoie, MD, and Andrea D. Dukes, MS From the Mississippi Sports
Deltoid and Syndesmosis Ligament Injury of the Ankle Without Fracture Chris D. Miller, MD, Walter R. Shelton,* MD, Gene R. Barrett, MD, F. H. Savoie, MD, and Andrea D. Dukes, MS From the Mississippi Sports
5 COMMON INJURIES IN THE FOOT & ANKLE
 5 COMMON INJURIES IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA MECHANISM OF INJURY HOW DID IT HAPPEN? HIGH ENERGY VS LOW ENERGY DIRECTION OF FORCES INVOLVED LIVING
5 COMMON INJURIES IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA MECHANISM OF INJURY HOW DID IT HAPPEN? HIGH ENERGY VS LOW ENERGY DIRECTION OF FORCES INVOLVED LIVING
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
ROTATIONAL PILON FRACTURES
 CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
Lisfranc Fracture-Dislocation/ Arthrodesis
 Lisfranc Fracture-Dislocation/ Arthrodesis 16 Lawrence A. Di Domenico and Frank A. Luckino Introduction L.A. Di Domenico (*) Ankle and Foot Care Centers, Youngstown, OH, USA Kent State University, College
Lisfranc Fracture-Dislocation/ Arthrodesis 16 Lawrence A. Di Domenico and Frank A. Luckino Introduction L.A. Di Domenico (*) Ankle and Foot Care Centers, Youngstown, OH, USA Kent State University, College
pedcat Clinical Case Studies
 pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
One Month Old Neglected Lisfrancs Fracture Dislocation Treated with Wagner's External Fixator and Percutaneous Screw Fixation : A Case Report
 Case Report Journal of Orthopaedic Case Reports 2014 April-June;4(2): Page 42-46 One Month Old Neglected Lisfrancs Fracture Dislocation Treated with Wagner's External Fixator and Percutaneous Screw Fixation
Case Report Journal of Orthopaedic Case Reports 2014 April-June;4(2): Page 42-46 One Month Old Neglected Lisfrancs Fracture Dislocation Treated with Wagner's External Fixator and Percutaneous Screw Fixation
Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E.
 Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E. Easley, MD Duke University Medical Center Durham, NC Disclosures Predictors
Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E. Easley, MD Duke University Medical Center Durham, NC Disclosures Predictors
LISFRANC FRACTURE-DISLOCATION IN A FEMALE SOCCER ATHLETE Beth Haddix, DPT 1 Karen Ellis, DPT 2 Estee Saylor-Pavkovich, DPT 3
 IJSPT DIAGNOSTICS CORNER LISFRANC FRACTURE-DISLOCATION IN A FEMALE SOCCER ATHLETE Beth Haddix, DPT 1 Karen Ellis, DPT 2 Estee Saylor-Pavkovich, DPT 3 ABSTRACT Individuals with midfoot injuries may present
IJSPT DIAGNOSTICS CORNER LISFRANC FRACTURE-DISLOCATION IN A FEMALE SOCCER ATHLETE Beth Haddix, DPT 1 Karen Ellis, DPT 2 Estee Saylor-Pavkovich, DPT 3 ABSTRACT Individuals with midfoot injuries may present
Clinical evaluation where no obvious fracture a. Squeeze test
 7:43 am The Syndesmotic Injury: From Subtle to Severe Robert B. Anderson, MD Chief, Foot and Ankle Carolinas Medical Center OrthoCarolina (Charlotte, North Carolina) 7:30-8:25 am Symposium 1: Management
7:43 am The Syndesmotic Injury: From Subtle to Severe Robert B. Anderson, MD Chief, Foot and Ankle Carolinas Medical Center OrthoCarolina (Charlotte, North Carolina) 7:30-8:25 am Symposium 1: Management
CASE ONE CASE ONE. RADIAL HEAD FRACTURE Mason Classification. RADIAL HEAD FRACTURE Mechanism of Injury. RADIAL HEAD FRACTURE Imaging
 CASE ONE An eighteen year old female falls during a basketball game, striking her elbow on the court. She presents to your office that day with a painful, swollen elbow that she is unable to flex or extend
CASE ONE An eighteen year old female falls during a basketball game, striking her elbow on the court. She presents to your office that day with a painful, swollen elbow that she is unable to flex or extend
6.5 mm midfoot fusion bolt
 6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation
 Journal of Sport Rehabilitation, 1993, 2, 281-286 O 1993 Human Kinetics Publishers, Inc. A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation Keith M. Gorse, Graham Johnstone, and Jennifer
Journal of Sport Rehabilitation, 1993, 2, 281-286 O 1993 Human Kinetics Publishers, Inc. A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation Keith M. Gorse, Graham Johnstone, and Jennifer
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/08/2012 Radiology Quiz of the Week # 102 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/08/2012 Radiology Quiz of the Week # 102 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Peggers Super Summaries: Foot Injuries
 Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
Midfoot arthritis, a specific complaint in adults,
 A Review Paper Midfoot Arthritis Siraj A. Sayeed, MD, Fazel A. Khan, MD, Norman S. Turner III, MD, and Harold B. Kitaoka, MD Abstract Foot and ankle complaints are commonly encountered in orthopedic practice.
A Review Paper Midfoot Arthritis Siraj A. Sayeed, MD, Fazel A. Khan, MD, Norman S. Turner III, MD, and Harold B. Kitaoka, MD Abstract Foot and ankle complaints are commonly encountered in orthopedic practice.
Lisfranc Injury Imaging and Surgical Management
 139 Lisfranc Injury Imaging and Surgical Management Eva Llopis, MD 1 Javier Carrascoso, MD 2 Inigo Iriarte, MD 3 Mariano de Prado Serrano, MD 4 Luis Cerezal, MD 5 1 Department of Radiology, Hospital de
139 Lisfranc Injury Imaging and Surgical Management Eva Llopis, MD 1 Javier Carrascoso, MD 2 Inigo Iriarte, MD 3 Mariano de Prado Serrano, MD 4 Luis Cerezal, MD 5 1 Department of Radiology, Hospital de
Case Report A Case Report of Isolated Cuboid Nutcracker Fracture
 Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Locking Forefoot/Midfoot Plating System
 Locking Forefoot/Midfoot Plating System Locking Forefoot/Midfoot Plating System Acumed is an industry leader in innovative solutions for extremities and trauma. We are dedicated to pioneering solutions
Locking Forefoot/Midfoot Plating System Locking Forefoot/Midfoot Plating System Acumed is an industry leader in innovative solutions for extremities and trauma. We are dedicated to pioneering solutions
Surgical Technique. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
Lisfranc Injury: Imaging Findings for this Important but Often-Missed Diagnosis
 Lisfranc Injury: Imaging Findings for this Important but Often-Missed Diagnosis Rajan T. Gupta, MD, a Rakhee P. Wadhwa, MD, b Thomas J. Learch, MD, b and Steven M. Herwick, MD a The Lisfranc injury is
Lisfranc Injury: Imaging Findings for this Important but Often-Missed Diagnosis Rajan T. Gupta, MD, a Rakhee P. Wadhwa, MD, b Thomas J. Learch, MD, b and Steven M. Herwick, MD a The Lisfranc injury is
Fracture and Dislocation of Metacarpal Bones, Metacarpophalangeal Joints, Phalanges, and Interphalangeal Joints ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
CHARLOTTE Lisfranc. Recontruction System SURGICAL TECHNIQUE
 CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
FOOSH It sounded like a fun thing at the time!
 FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
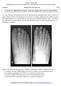 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/29/2012 Radiology Quiz of the Week # 105 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/29/2012 Radiology Quiz of the Week # 105 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Sports Injuries of the Foot and Ankle. Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018
 Sports Injuries of the Foot and Ankle Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018 I. Objectives A. By the end of the lecture attendees will
Sports Injuries of the Foot and Ankle Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018 I. Objectives A. By the end of the lecture attendees will
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation *
 Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Surgical Technique 4.5/8.5MM BEAMING SYSTEM. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The 4.5/8.5 screw system is intended for fixation arthrodesis of
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The 4.5/8.5 screw system is intended for fixation arthrodesis of
Fractures and dislocations around elbow in adult
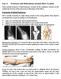 Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Goals. Initial management skeletal trauma. Physical Exam ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT 12/4/2010
 ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
EVALUATION OF THE SURGICAL TREATMENT OF LISFRANC JOINT FRACTURE-DISLOCATION
 Original Article EVALUATION OF THE SURGICAL TREATMENT OF LISFRANC JOINT FRACTURE-DISLOCATION Cléber de Jesus Pereira 1, Eduardo Gomes Espinosa 2, Ivan Miranda 3, Marcelo Bueno Pereira 4, Roberto Sérgio
Original Article EVALUATION OF THE SURGICAL TREATMENT OF LISFRANC JOINT FRACTURE-DISLOCATION Cléber de Jesus Pereira 1, Eduardo Gomes Espinosa 2, Ivan Miranda 3, Marcelo Bueno Pereira 4, Roberto Sérgio
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Hand and wrist emergencies
 Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
CURRENT TREATMENT OPTIONS
 CURRENT TREATMENT OPTIONS Fix single column or both: Always fix both. A study by Svend-Hansen corroborated the poor results associated with isolated medial malleolar fixation in bimalleolar ankle fractures.
CURRENT TREATMENT OPTIONS Fix single column or both: Always fix both. A study by Svend-Hansen corroborated the poor results associated with isolated medial malleolar fixation in bimalleolar ankle fractures.
Open Access Case Report DOI: /cureus.599. Ashok K. Rathod 1, Rakesh P. Dhake 1, Aditya Pawaskar 1
 Open Access Case Report DOI: 10.7759/cureus.599 Minimally Invasive Treatment of a Complex Tibial Plateau Fracture with Diaphyseal Extension in a Patient with Uncontrolled Diabetes Mellitus: A Case Report
Open Access Case Report DOI: 10.7759/cureus.599 Minimally Invasive Treatment of a Complex Tibial Plateau Fracture with Diaphyseal Extension in a Patient with Uncontrolled Diabetes Mellitus: A Case Report
FOOSH It sounded like a fun thing at the time!
 FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Paul Alley MD,DPM,MS,FACS,FAAOS,BFD Eby Orthopaedics,Jasper,Indiana
 Paul Alley MD,DPM,MS,FACS,FAAOS,BFD Eby Orthopaedics,Jasper,Indiana Very common Bone=fractures Description (cracked,broke,busted,or smashed) A=anatomic area of bone eg: head,neck,shaft B=bone involved
Paul Alley MD,DPM,MS,FACS,FAAOS,BFD Eby Orthopaedics,Jasper,Indiana Very common Bone=fractures Description (cracked,broke,busted,or smashed) A=anatomic area of bone eg: head,neck,shaft B=bone involved
«Foot & Ankle Surgery» 04. Sept THE PAINFUL FLATFOOT. Norman Espinosa, MD
 THE PAINFUL FLATFOOT Norman Espinosa, MD Department of Orthopaedics University of Zurich Balgrist Switzerland www.balgrist.ch WHAT TO DO? INTRINSIC > EXTRINSIC ETIOLOGIES Repetitive microtrauma combined
THE PAINFUL FLATFOOT Norman Espinosa, MD Department of Orthopaedics University of Zurich Balgrist Switzerland www.balgrist.ch WHAT TO DO? INTRINSIC > EXTRINSIC ETIOLOGIES Repetitive microtrauma combined
The evaluation and management of acute musculoskeletal
 ONLINE EXCLUSIVE George E. Eldayrie, MD; Kristy Smith, MD; Michael Seth Smith, MD, CAQSM, PharmD Department of Community Health and Family Medicine (Drs. Eldayrie and K. Smith) and Department of Orthopedics
ONLINE EXCLUSIVE George E. Eldayrie, MD; Kristy Smith, MD; Michael Seth Smith, MD, CAQSM, PharmD Department of Community Health and Family Medicine (Drs. Eldayrie and K. Smith) and Department of Orthopedics
Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES
 Updated 2/8/10 Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES INTERPERSONAL AND COMMUNICATION SKILLS Resident will at all times demonstrate behavior that is beyond reproach. Residents must be
Updated 2/8/10 Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES INTERPERSONAL AND COMMUNICATION SKILLS Resident will at all times demonstrate behavior that is beyond reproach. Residents must be
The influence of approach and implant on reduction accuracy and stability in Lisfranc
 The influence of approach and implant on reduction accuracy and stability in Lisfranc fracture-dislocation at the tarsometatarsal joint T. Schepers MD PhD, P.P. Oprel MD, E.M.M. Van Lieshout PhD Erasmus
The influence of approach and implant on reduction accuracy and stability in Lisfranc fracture-dislocation at the tarsometatarsal joint T. Schepers MD PhD, P.P. Oprel MD, E.M.M. Van Lieshout PhD Erasmus
Finger Mobility Deficits Fracture of metacarpal Fracture of phalanx of phalanges
 1 Finger Mobility Deficits ICD-9-CM codes: 715.4 Osteoarthrosis of the hand 815.0 Fracture of metacarpal 816.0 Fracture of phalanx of phalanges ICF codes: Activities and Participation code: d4301 Carrying
1 Finger Mobility Deficits ICD-9-CM codes: 715.4 Osteoarthrosis of the hand 815.0 Fracture of metacarpal 816.0 Fracture of phalanx of phalanges ICF codes: Activities and Participation code: d4301 Carrying
MEDIAL EPICONDYLE FRACTURES
 MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
Treatment of malunited fractures of the ankle
 Treatment of malunited fractures of the ankle A LONG-TERM FOLLOW-UP OF RECONSTRUCTIVE SURGERY I. I. Reidsma, P. A. Nolte, R. K. Marti, E. L. F. B. Raaymakers From Academic Medical Center, Amsterdam, Netherlands
Treatment of malunited fractures of the ankle A LONG-TERM FOLLOW-UP OF RECONSTRUCTIVE SURGERY I. I. Reidsma, P. A. Nolte, R. K. Marti, E. L. F. B. Raaymakers From Academic Medical Center, Amsterdam, Netherlands
Orthopedics in Motion Tristan Hartzell, MD January 27, 2016
 Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Primary open reduction and fixation compared with delayed corrective arthrodesis in the treatment of tarsometatarsal (Lisfranc) fracture dislocation
 Primary open reduction and fixation compared with delayed corrective arthrodesis in the treatment of tarsometatarsal (Lisfranc) fracture dislocation S. Rammelt, W. Schneiders, H. Schikore, M. Holch, J.
Primary open reduction and fixation compared with delayed corrective arthrodesis in the treatment of tarsometatarsal (Lisfranc) fracture dislocation S. Rammelt, W. Schneiders, H. Schikore, M. Holch, J.
Basic Care of Common Fractures Utku Kandemir, MD
 Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Index. Note: Page numbers of article titles are in boldface type. Hand Clin 21 (2005)
 Hand Clin 21 (2005) 501 505 Index Note: Page numbers of article titles are in boldface type. A Antibiotics, following distal radius fracture treatment, 295, 296 Arthritis, following malunion of distal
Hand Clin 21 (2005) 501 505 Index Note: Page numbers of article titles are in boldface type. A Antibiotics, following distal radius fracture treatment, 295, 296 Arthritis, following malunion of distal
Injuries to the lower extremity II Aree Tanavalee MD Associate Professor Department of Orthopaedics Faculty of Medicine Chulalongkorn University
 Injuries to the lower extremity II Aree Tanavalee MD Associate Professor Department of Orthopaedics Faculty of Medicine Chulalongkorn University Topics Fracture of the shaft of the femur Fractures around
Injuries to the lower extremity II Aree Tanavalee MD Associate Professor Department of Orthopaedics Faculty of Medicine Chulalongkorn University Topics Fracture of the shaft of the femur Fractures around
InCoreTM Lapidus System
 InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
The Flower Medial Column Fusion Plate
 The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Journal reading. Introduction. Introduction. Ottawa Ankle Rules. Method
 Journal reading Presenter: PGY 林聖傑 Supervisor: Dr. 林俊龍 102.12.23 The accuracy of ultrasound evaluation in foot and ankle trauma Salih Ekinci, MD American Journal of Emergency Medicine 31 (2013) 1551 1555
Journal reading Presenter: PGY 林聖傑 Supervisor: Dr. 林俊龍 102.12.23 The accuracy of ultrasound evaluation in foot and ankle trauma Salih Ekinci, MD American Journal of Emergency Medicine 31 (2013) 1551 1555
Fractures of the Calcaneus
 Fractures of the Calcaneus Anthony T. Sorkin, M.D. Rockford Orthopedic Trauma Service Rajeev Garapati, MD Illinois Bone and Joint Institute Assistant Clinical Professor University of Illinois at Chicago
Fractures of the Calcaneus Anthony T. Sorkin, M.D. Rockford Orthopedic Trauma Service Rajeev Garapati, MD Illinois Bone and Joint Institute Assistant Clinical Professor University of Illinois at Chicago
DARCO. Bow 2 Plate SURGIC AL TECHNIQUE
 DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
Peritalar Dislocation After Tibio-Talar Arthrodesis: Fact or Fiction?
 AOFAS Annual Meeting, July 17-20th 2013 Hollywood, Florida Peritalar Dislocation After Tibio-Talar Arthrodesis: Fact or Fiction? Fabrice Colin, MD; Lukas Zwicky, MSc; Alexej Barg, MD; Beat Hintermann,
AOFAS Annual Meeting, July 17-20th 2013 Hollywood, Florida Peritalar Dislocation After Tibio-Talar Arthrodesis: Fact or Fiction? Fabrice Colin, MD; Lukas Zwicky, MSc; Alexej Barg, MD; Beat Hintermann,
Evaluation and Treatment of Intra-articular Fractures. Benjamin Maxson, DO Florida Orthopaedic Institute Orthopaedic Trauma Service
 Evaluation and Treatment of Intra-articular Fractures Benjamin Maxson, DO Florida Orthopaedic Institute Orthopaedic Trauma Service Disclosures Nothing to disclose Articular Fractures: Overview Require
Evaluation and Treatment of Intra-articular Fractures Benjamin Maxson, DO Florida Orthopaedic Institute Orthopaedic Trauma Service Disclosures Nothing to disclose Articular Fractures: Overview Require
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Pediatric Fractures. Objectives. Epiphyseal Complex. Anatomy and Physiology. Ligaments. Bony matrix
 1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
Fractures of the Hand in Children Which are simple? And Which have pitfalls??
 Fractures of the Hand in Children Which are simple? And Which have pitfalls?? Kaye E Wilkins DVM, MD Professor of Orthopedics and Pediatrics Departments of Orthopedics and Pediatrics University of Texas
Fractures of the Hand in Children Which are simple? And Which have pitfalls?? Kaye E Wilkins DVM, MD Professor of Orthopedics and Pediatrics Departments of Orthopedics and Pediatrics University of Texas
Staged Treatment of High Energy Midfoot Fracture Dislocations
 552077FAIXXX10.1177/1071100714552077Foot & Ankle InternationalKadow et al research-article2014 Article Staged Treatment of High Energy Midfoot Fracture Dislocations Foot & Ankle International 2014, Vol.
552077FAIXXX10.1177/1071100714552077Foot & Ankle InternationalKadow et al research-article2014 Article Staged Treatment of High Energy Midfoot Fracture Dislocations Foot & Ankle International 2014, Vol.
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot.
 Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report
 CASE REPORT 41 OPEN ACCESS A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report Aysha Rajeev, John Harrison ABSTRACT Introduction: The phalangeal
CASE REPORT 41 OPEN ACCESS A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report Aysha Rajeev, John Harrison ABSTRACT Introduction: The phalangeal
