Does Open Reduction of the Developmental Dislocated Hip Increase the Risk of Osteonecrosis?
|
|
|
- Agatha Ramsey
- 5 years ago
- Views:
Transcription
1 Clin Orthop Relat Res (2012) 470: DOI /s CLINICAL RESEARCH Does Open Reduction of the Developmental Dislocated Hip Increase the Risk of Osteonecrosis? Renata Pospischill MD, Julia Weninger MD, Rudolf Ganger MD, PhD, Johannes Altenhuber MD, Franz Grill MD Received: 3 November 2010 / Accepted: 18 May 2011 / Published online: 4 June 2011 Ó The Association of Bone and Joint Surgeons Abstract Background Osteonecrosis (ON) of the femoral head is one of the main complications associated with treatment of developmental dysplasia of the hips (DDH). The reported rates of ON vary widely between 6% and 48%, suggesting varying factors in these studies influence the rate. Several studies suggest open reduction combined with femoral shortening provides protection against ON. However, it is unclear whether confounders such as failed Pavlik harness treatment, preliminary traction, closed versus open reduction, and redislocation influence the rate of ON. Questions/purpose We therefore asked whether open reduction with concomitant osteotomies without femoral shortening, redislocation, and secondary surgical procedures for residual acetabular dysplasia influenced the rate of ON. Methods We retrospectively reviewed 64 children (78 hips) hospitalized with developmental dislocation of the hip between January 1998 and February Patients younger than 12 months were treated with closed or open reduction. Open reduction combined with concomitant pelvic and femoral osteotomies was performed in patients Each author certifies that he or she has no commercial associations (eg, consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article. Each author certifies that his or her institution approved the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research, and that informed consent for participation in the study was obtained. R. Pospischill (&), J. Weninger, R. Ganger, J. Altenhuber, F. Grill Pediatric Orthopaedic Department, Orthopaedic Hospital Vienna-Speising, Speisinger Strasse 109, 1130 Vienna, Austria renata.pospischill@oss.at past walking age. ON was diagnosed from radiographs obtained at last followup. We used logistic regression analysis to identify predictors for the development of ON. The minimum followup was 3.2 years (mean, 6.8 years; range, years). Results The overall rate of ON was 40%. Patients who underwent open reduction combined with concomitant osteotomies, experienced redislocation, or required secondary reconstructive procedures after initial reduction were at higher risk for having ON develop. Conclusions We advocate early reduction of the dislocated hip in the first year of life to avoid the need for concomitant osteotomies combined with open reduction. Level of Evidence Level III, therapeutic study. See Guidelines for Authors for a complete description of levels of evidence. Introduction ON of the proximal femoral epiphysis is one of the main complications associated with the treatment of developmental dislocated hips. The overall rates of ON reported in studies have been inconsistent, ranging from 6% to 48% after treatment of the dislocated hip [1, 6, 7, 20, 29, 30]. The complication can lead to acetabular dysplasia and joint incongruity, resulting in early osteoarthritis [4, 5, 8 10, 16, 21]. However, it is widely accepted that early reduction of the developmental dislocated hip and maintained concentric reduction can lead to a satisfactory long-term outcome [17, 20, 23]. The widely varying rates reported in the literature suggest differences in diagnostic criteria, patient demographics, or treatments in the studies influence the rates. For example, the use of extreme positions of immobilization with the hips in
2 Volume 470, Number 1, January 2012 Risk Factors of Osteonecrosis abduction (frog-leg position) is reportedly a major risk factor for having ON develop [10, 15, 28, 34]. Preliminary traction and femoral shortening facilitate reduction and decrease the incidence of ON [3, 6, 18, 20, 29, 30]. One study suggested the appearance of the ossific nucleus of the femoral head provided protection against ON after reduction [30]. Other reports have documented conflicting data on the importance of the ossific nucleus [20, 25]. A delay in reduction decreases the possibility of spontaneous resolution of dysplastic features because maximal osseous remodeling of the hip occurs during the first year of life [14]. In older children, a pelvic or femoral osteotomy may be necessary in addition to open reduction to address the problem of acetabular dysplasia. Debate continues regarding whether concomitant osteotomies should be performed in children after walking age [19, 26, 27]. Some authors believe pelvic osteotomy may be unnecessary in children who are 5 years or younger [19]. Although Lindstrom et al. [19] suggested there was considerable potential for acetabular remodeling up to age 8, Salter [26, 27] believed the potential for acetabular remodeling rapidly declines after age 18 months and therefore recommended a pelvic osteotomy at the time of open reduction to directly correct residual dysplasia. Owing to the controversies in risk factors. we therefore asked whether (1) open reduction without preliminary traction or femoral shortening performed in children after walking age, (2) redislocation requiring subsequent open reduction, and (3) numerous other factors (gender, Pavlik harness treatment, age at reduction, appearance of the ossific nucleus at the time of reduction, hip position in the spica cast after reduction, type of reduction [closed, open, or open with concomitant osteotomies], and secondary reconstructive procedures), predicted ON after adjusting for potential confounders. Patients and Methods We retrospectively reviewed 233 pediatric patients with 290 abnormal hips who had been treated at our institution between January 1998 and February 2007 with closed or open reduction for developmental dislocation of the hip. We excluded 149 patients with 188 abnormal hips who had teratologic hip dislocation resulting from associated syndromes or other musculoskeletal abnormalities, those who had concomitant neuromuscular diseases, and those who had undergone previous operative reduction at another medical institution. Seventeen patients (21 hips) with less than 3 years of followup and one patient (one hip) who had septic arthritis develop after the reduction were excluded. Eight patients were lost to followup because of emigration of their families, but because six already had shown signs of ON, we included these six in the analysis and excluded the other two. After these exclusions, 64 children (78 hips) remained (Fig. 1). The minimum followup was 3.2 years (mean, 6.8 years, range, years). Patients were recalled specifically for this study, and all data were obtained from clinical examinations, medical records, and radiographs. Prior institutional review board approval was obtained. We identified three groups based on patient age and treatment: Group A consisted of patients who underwent closed reduction and were treated before 12 months of age; Group B consisted of patients who underwent open reduction and were treated before 12 months of age; Group C consisted of patients older than 12 months at the time of reduction who previously had not been treated. Patients in Groups A and B had all been treated previously with a Pavlik harness. All except two children in Group B had been hospitalized for preliminary traction before undergoing reduction. The severity of dislocation, as noted on the sonograms, was graded according to the Graf classification [12]. Arthrography of the dislocated hip was performed after traction in both groups with the patients under general anesthesia. In Group A patients, closed reduction was performed if the femoral head was well covered by the labrum, as shown on the arthrogram, and felt stable in the primary acetabulum (Fig. 2). If the hip was unstable after initial closed reduction, or if obstructions to reduction such as an infolded labrum or a constricted capsule were visible on the arthrogram (Fig. 3), open reduction using an anterolateral approach was performed during the same session. These patients were assigned to Group B. Patients in Group C all underwent open reduction through an anterolateral approach performed simultaneously with either a Pemberton [24] (Fig. 4) or varus derotation osteotomy of the proximal part of the femur (Fig. 5). The femoral osteotomies were performed either alone or with a combined procedure. At presentation, the severity of the dislocation was graded on radiographs according to the classification presented by Tönnis [32]. At the time of open reduction, pelvic osteotomy was performed to directly correct residual dysplasia in two scenarios. The first was if the acetabular index was greater than 2 standard deviations from the normal mean (greater than 30 ) in children 2 years and older. The second was if the center-edge angle of Wiberg was 2 standard deviations or more greater than normal (less than 20 ) in children older than 5 years [31, 32]. Thirty-six patients (46 hips) in Group A and 13 patients (15 hips) in Group B were available for statistical analysis (Table 1). The mean patient age at the time of closed reduction was 4 months (range, months), and was 3.6 months (range, months) at the time of open reduction. Adductor tenotomies were not routinely
3 252 Pospischill et al. Clinical Orthopaedics and Related Research 1 Fig. 1 The flowchart shows the sample selection of patients with developmental dislocated hips. Fig. 2 An arthrogram of the left hip of a 3-month-old patient shows the hip in a flexion-abduction position. The reduction was maintained. The labrum lies flat over the femoral head and has a sharp border. Fig. 3 An arthrogram is shown of the right hip of a 4-month-old patient before open reduction of a developmental dislocated hip. When the head was docked, the labrum was interposed between the femoral head and the acetabular wall. Because of capsular constriction of the iliopsoas, stable reduction was not possible.
4 Volume 470, Number 1, January 2012 Risk Factors of Osteonecrosis 253 Fig. 4A B AP view radiographs of the pelvis of a 3-year-old patient show developmental dislocation of the right hip. The radiographs were obtained (A) at the time of presentation and (B) 6 months after open reduction with capsulorrhaphy and Pemberton osteotomy. Successful reduction is shown. Fig. 5A B Preoperative and postoperative AP view radiographs of a patient managed with open reduction, capsulorrhaphy, and femoral varus derotation osteotomy for the treatment of a dislocated right hip are shown. (A) This radiograph was obtained at first presentation when the patient was 17 months old. (B) Six months after surgery, the radiograph shows successful reduction. performed before reduction. Group C consisted of 15 patients (17 hips) (Table 1). The mean patient age at the time of reduction was 3.8 years (range, years). Three hips (18%) were treated by open reduction and Pemberton osteotomy and one hip (6%) by open reduction and varus derotation osteotomy only. Twelve hips (71%) were managed with open reduction, Pemberton osteotomy, and concomitant varus derotation osteotomy. Femoral shortening was performed in only one case (6%). In two hips (12%), an additional adductor tenotomy was performed before open reduction. Patients in Groups A and B were compared regarding age at the time of reduction, gender, Pavlik harness treatment, duration of preliminary traction, severity of dislocation, appearance of the ossific nucleus at the time of reduction, spica cast immobilization after reduction, and duration of followup (Table 2). At baseline, Groups A and B were similar. Except for gender ratio, demographic findings differed between patients of Group C treated past walking age and patients of Groups A and B. Reductions of dislocated hips were performed at the earliest possible time after patients first presented at our
5 254 Pospischill et al. Clinical Orthopaedics and Related Research 1 Table 1. Baseline characteristics Variable Group A (46 hips) Group B (15 hips) Group C (17 hips) Type of reduction Closed Open* Open + PO + VDO Age at reduction 4.0 months 3.6 months 45.5 months (3.8 years) Gender ratio (female:male) 30:6 10:3 12:3 Pavlik harness treatment Yes: 28 (61%) Yes: 6 (40%) Yes: 0 Preceding reduction No: 18 (39%) No: 9 (60%) No: 17 (100%) Duration of preliminary traction 3.7 weeks 3.6 weeks No Preceding reduction Preoperative severity of dislocation Graf III 6 (13%) 1 (7%) Graf IV 40 (87%) 14 (93%) Tönnis Grade I 0 Tönnis Grade II 1 (6%) Tönnis Grade III 13 (76%) Tönnis Grade IV 3 (18%) Ossific nucleus at time of reduction Present 14 (30%) 8 (53%) 17 (100%) Absent 32 (70%) 7 (47%) 0 Spica cast immobilization after reduction Human position 21 (46%) 10 (67%) Modified human position 25 (54%) 5 (33%) One and one-half spica cast 17 (100%) Osteonecrosis grade I 4 (9%) 2 (13%) 4 (24%) II 7 (15%) 0 4 (24%) III 1 (2%) 0 6 (35%) IV 1 (2%) 1 (7%) 1 (6%) Total 13 (28%) 3 (20%) 15 (88%) Osteonecrosis Grades II to IV 9 (20%) 1 (7%) 11 (65%) Redislocation 8 (17%) 0 1 (6%) Secondary reconstructive procedures 7 (15%) 2 (13%) 5 (29%) Postoperative complications Skin excoriation requiring cast changes (12%) Superficial wound infections (12%) Septic arthritis Followup 6.3 years 7.4 years 6.7 years PO = Pemberton osteotomy; VDO = varus derotation osteotomy; * open reduction through an anterolateral approach; open reduction through an anterolateal approach with concomitant Pemberton and/or varus derotation osteotomies. outpatient clinic. All reductions were performed by two experienced pediatric orthopaedic surgeons (JA, FG) with similar treatment algorithms and techniques. After the primary reduction, redislocations were treated by open reduction. Secondary reconstructive procedures for residual acetabular dysplasia were performed if, in the judgment of the surgeon, the hips showed signs of subluxation or deficient progressive acetabular development. Pelvic osteotomy in patients younger than 4 years was performed only if the persisting dysplasia was deteriorating, as revealed by serial followup radiographs [19]. The indication for varus derotation osteotomy was failure of concentric reduction after open reduction and pelvic osteotomy. The derotation ranged from 25 (14 hips) to 50 (one hip) and the varus from 10 to 30. After closed or open reduction, a spica cast was applied in the human position as described by Salter et al. [28] (100 to 110 flexion, 40 to 60 abduction, and no rotation) or in a modified human position with the hips in 100 to 110 flexion and greater than 60 abduction for the patients in Groups A and B. Casts were retained for 12 weeks. After removal of the spica cast, a full-time
6 Volume 470, Number 1, January 2012 Risk Factors of Osteonecrosis 255 Table 2. Comparison of demographic factors between Groups A and B Variable Group A Group B p Value Mean age at reduction (months) 4.0 ± 2.3 ( ) 3.6 ± 2.0 ( ) Gender (female:male) 30:6 10: Side (unilateral:bilateral) 26:10 11: Pavlik harness treatment preceding reduction (yes: no) 28:18 6: Mean duration of preliminary traction preceding reduction (weeks) 3.7 ± 1.0 ( ) 3.6 ± 1.6 ( ) Preoperative severity of dislocation (number of hips - Graf III: Graf IV) 6:40 1: Ossific nucleus at time of reduction (present:absent) 14:32 8: Spica cast immobilization after reduction 21:25 10: (human position:modified human position) Mean followup (years) 6.3 ± 2.5 ( ) 7.4 ± 2.3 ( ) Differences between proportions of gender, side, Pavlik harness treatment, severity of dislocation, presence of the ossific nucleus, and spica cast immobilization tested with Fisher s exact test; values of continuous variables are reported as mean ± standard deviation with the 95% confidence interval in the parenthesis abduction orthosis maintained the hip at 60 total abduction until acetabular development was normalized, as revealed by radiographs, or until the children started to crawl or sit. For Group C patients, a one and one-half hip spica cast was applied postoperatively for 6 weeks with the hip in 20 flexion, 30 abduction, and 10 internal rotation. During that time, weightbearing was not permitted. The same radiographic protocol was used for all patients. The radiographs were reviewed independently by two observers (RP and JW). The severity of dislocation as shown on radiographs was classified according to Tönnis [32] and as shown on ultrasound images, according to Graf [12]. Presence of nucleus was determined preoperatively on radiographs and on sonograms of patients younger than 12 months at the time of reduction. The development of ON of the femoral head after reduction, as observed on the final followup radiograph, was classified according to the method presented by Bucholz and Odgen [5]. All grades of ON (Grades I through IV) were considered in the analysis. The intraobserver and interobserver intraclass correlation coefficients were 0.87 (95% confidence interval, ) and 0.80 (95% confidence interval, ), respectively. Normally distributed data are presented as means with 95% confidence intervals. The differences between the groups regarding gender, Pavlik harness treatment, preoperative severity of dislocation, appearance of the ossific nucleus at the time of reduction, spica cast immobilization, incidences of ON, rates of redislocation, and secondary reconstructive procedures resulting from residual acetabular dysplasia were tested with Fisher s exact test for nonparametric data. Continuous numeric variables in the two groups were compared with two-sided unpaired Student s t-test. Treatment effect of redislocation was reported as the relative risk. Multivariate logistic regression was used to develop models predicting ON. Gender, Pavlik harness treatment, age at reduction, appearance of the ossific nucleus at the time of reduction, hip position in the spica cast after reduction, type of reduction (closed, open, or open with concomitant osteotomies), and secondary reconstructive procedures were entered as risk factors. Post hoc analyses for all outcomes were conducted. Statistical analysis was conducted with the use of the SPSS software (Version 17.0; SPSS Inc, Chicago, IL, USA). Results Open reduction without preliminary traction or femoral shortening performed in children after walking age was associated with a greater (p \ 0.001) incidence of ON of the femoral head compared with patients with early reductions (Groups A and B) (Table 3). The overall rate of ON for the cohort (all patients with developmental dislocation of the hips treated between 1998 and 2007) was 40%. Compared with patients for whom the initial reduction was maintained, the patients with redislocation had a 67% increased probability of having ON develop (relative risk, 0.33; 95% confidence interval, ). All hips for which initial reduction failed were treated with an open procedure and subsequent maintenance of reduction. The overall redislocation rate for our series was 12% (nine hips). We found no difference in the rate of redislocation among the groups (Table 3). We observed no association between ON and gender (p = 0.69), failed Pavlik harness treatment before reduction (p = 0.08), or the presence of the ossific nucleus at reduction (p = 0.14) (Table 4). When controlling for age, preliminary traction, hip position in the spica cast after reduction, type of reduction, and secondary reconstructive procedures, only type of reduction (odds ratio, 11.04; 95% confidence interval, ; p = 0.003) and secondary
7 256 Pospischill et al. Clinical Orthopaedics and Related Research 1 Table 3. Comparison of outcome measures among the study groups Outcome variable* Group A Group B Group C Total p Value Osteonecrosis Grades I to IV 13 (28%) 3 (20%) 15 (88%) 31 (40%) \ à \ Osteonecrosis Grades II to IV 9 (20%) 1 (7%) 11 (65%) 21 (27%) Redislocation 8 (17%) 0 1 (6%) 9 (12%) Secondary reconstructive procedure required to treat residual acetabular dysplasia à à (15%) 2 (13%) 5 (29%) 14 (18%) * Differences tested with Fisher s exact test; difference between Group A and Group B; à difference between Group A and Group C; difference between Group B and Group C à Table 4. Univariate logistic regression for predictors of osteonecrosis Independent variable Odds ratio p Value 95% Confidence interval Age at reduction \ Age younger than 12 months versus age older than 12 months Previous Pavlik harness treatment Preliminary traction \ Spica cast immobilization Human position versus modified human position Type of reduction \ Closed versus open versus open with concomitant osteotomies Secondary procedures* Presence of the ossific nucleus Gender Female versus male * Secondary procedures required to treat residual acetabular dysplasia without signs of osteonecrosis at time of surgery. reconstructive procedures (odds ratio, 13.97; 95% confidence interval, ; p = 0.004) were associated with increased rates of ON (Table 5). Compared with open reduction with concomitant osteotomies, closed reduction reduced the possibility of ON developing by 99% (odds ratio, 0.01; 95% confidence interval, ). Open reduction alone led to a decrease of 89% (odds ratio, 0.12; 95% confidence interval, ). Patients with persisting residual acetabular dysplasia after initial reduction who were treated with pelvic or femoral osteotomies were 14 times more likely to have ON develop than were patients without reconstructive interventions. Discussion One of the main complications associated with treatment of developmental dislocated hips is the development of ON of the femoral head [4, 5, 8 10, 16, 21]. Although children undergoing open reduction may have greater risk of ON [1, 6, 7, 20, 30], the importance of the various risk factors is unclear. We therefore asked whether open reduction without femoral shortening performed in children after walking age was associated with a greater incidence of ON of the femoral head, whether redislocation requiring subsequent open reduction increased the risk of ON, and
8 Volume 470, Number 1, January 2012 Risk Factors of Osteonecrosis 257 Table 5. Multivariate logistic regression for adjusted predictors of osteonecrosis Model Overall success rate for predicted occurrences (cutoff = 0.3) (%) Constant only 40 Model including all covariates 86 Sensitivity 94 Specificity 79 False-positive rate 26 False-negative rate 5 Independent variable Odds ratio p Value 95% Confidence interval Age at reduction Age younger than 12 months versus age older than 12 months Preliminary traction Spica cast immobilization Human position versus modified human position Type of reduction Closed versus open versus open with concomitant osteotomies Secondary procedures* * Secondary procedures required to treat residual acetabular dysplasia without signs of osteonecrosis at time of surgery. whether any of a number of factors predicted ON after adjusting for potential confounders. Our study has several limitations. First, as with all retrospective studies, there was a risk of selection bias. However, we included all patients hospitalized at our institution for developmental dislocation of the hip and all were documented in our surgery records program and could be identified for a designated time. Second, we had a relatively small number of patients in the various groups. Post hoc power analysis determined that our sample size was sufficient to achieve a power of 88% to enable detection of a difference of 30% in the incidence of ON. Third, the three groups were heterogeneous regarding the variables previous treatment and type of reduction; the ages of the patients at reduction differed. We addressed this with logistic regression analysis for key variables, although we did not include all potential confounding variables. Fourth, we had a small number of redislocated hips, such that redislocation could not be included as a factor in the logistic regression analysis. Fifth, assessing ON in patients treated after walking age is problematic: 35% (six hips) in Group C had a smaller ossific nucleus on the dislocated hip compared with the unaffected side before reduction. Nearly half the affected hips had an ossific nucleus continuing to grow but remaining dysplastic. It therefore is reasonable to assume that clinically asymptomatic and active patients with mild radiographic changes should not be considered to have ON. However, future studies to follow the children to skeletal maturity and to determine the clinical relevance and whether such changes should be defined as ON are important. The overall rate of Grade I ON or worse was 40% in our study compared with reported incidences of 6% to 48% in some studies [1, 6, 7, 20, 30] (Table 6). The use of various classification systems to diagnose or grade ON could have contributed to the variation in the incidences among the studies. Our rates of ON are similar to those in several studies in which a cohort design was used [1, 7]. Segal et al. [30] conducted a case-control study and reported a similar rate of 32%. In the current study, the incidence of ON in patients treated after walking age was 88%. Several authors evaluated results comparable to our findings, with an increase in the rate of ON in dislocated hips treated with open reduction and combined pelvic osteotomy [22, 33]. Carney et al. [6] found an incidence of 48% in older children treated after walking. They concluded that adductor tenotomy reduced the rate of ON. Gulman et al. [13] reported a rate of Grades II through IV ON of 35% in 52 hips after anterior open reduction combined with innominate osteotomy. Most of the patients in the current study who were diagnosed after walking age were treated with open reduction and concomitant osteotomies without femoral shortening. The high rate of ON in this age group may indicate that open reduction combined with pelvic osteotomy should not be performed simultaneously without femoral shortening, as was previously reported [3, 11, 18, 29].
9 258 Pospischill et al. Clinical Orthopaedics and Related Research 1 Table 6. Series with incidences of osteonecrosis as reported in the literature Study Number of hips Treatment FS performed (%) Adductor tenotomy (%) Mean age at reduction (years) Duration of followup (years) Rate of ON (%) Redislocation (%) Secondary reconstructive procedures (%) Klisic and Jankovic [18] 1976 Mardam-Bey and MacEwen [22] OR + osteotomies (grades not reproducible) CR (Grades I IV) 4 66 OR 46 (Grades I IV) 8 OR + osteotomies 14 (Grades I IV) 6 Schoenecker 39 OR + osteotomies (Grades NR) 31 NR and Strecker [29] 1984 OR + osteotomies 100 NR (Grades NR) 8 NR Barrett et al. [2] OR + Salter 0 NR (Grades NR) 7 NR Galpin et al. [11] OR + Salter 100 NR (only Grade IV) 12 NR Brougham et al. [4] CR [ 2 47 (Grades I IV) NR 13 Tönnis [33] OR 0 NR NR NR 8 (Grades NR) NR NR OR 100 NR NR NR 6 (Grades NR) OR + Salter 0 NR NR NR 10 (Grades NR) OR + FO 0 NR NR NR 22 (Grades NR) Gulman et al. [13] OR + Salter 0 NR Mean, NR; (Grades II IV) 71 NR Range, Luhmann et al. [20] CR [ 3 4 (Grades I IV) OR 12 (Grades I IV) 12 Segal et al. [30] CR (Grades I IV) NR NR OR 0.5 Clarke et al. [7] CR [ 1 [ 3 18 (Grades I IV) NR 57 OR [ 1 [ 3 50 (Grades I IV) NR 41 Current study 78 CR (Grades I IV) OR (Grades I IV) 0 13 OR + osteotomies (Grades I IV) 6 29 OR = open reduction; CR = closed reduction; FO = femoral osteotomy; FS = femoral shortening; NR = not reported; ON = osteonecrosis.
10 Volume 470, Number 1, January 2012 Risk Factors of Osteonecrosis 259 Nine patients (12%) required secondary reduction, which was performed by an open procedure in each case. All except one hip initially had been reduced closed. In each case, the individual surgery report suggested forced reduction considering that obstacles to successful closed reduction, such as the presence of a constricted capsule, were described. All of the hips showed signs of ON at latest followup. Thus, in retrospect, immediate open reduction would have been the appropriate choice. It remains unclear whether this finding is related mostly to the second reduction, which was an open procedure, or to the primary suboptimal closed reduction. Nevertheless, redislocation has been reported with different incidences but with comparable rates of 0% to 20% for the anterior approach [17, 20, 23]. Our observations suggest open reduction with concomitant osteotomies without femoral shortening and secondary reconstructive procedures for acetabular dysplasia predict the development of ON. Patient age at the time of reduction, preliminary traction, history of failed Pavlik harness treatment, and hip immobilization after reduction do not seem to influence the incidence of ON. The need for open reduction with concomitant osteotomies increased the risk of ON by a factor of 11, and patients who underwent secondary reconstructive procedures were 14 times more likely to have ON develop than were patients who did not undergo additional surgery. Although increasing age at reduction was not a risk factor for ON in the final model, it is acknowledged that older patients are more likely to require open reduction with concomitant osteotomies. It seems that early diagnosis with immediate adequate treatment, and thus a greater chance of achieving closed reduction, influences outcome regarding ON. Our observations suggest shortening of the femur when performing open reduction with concomitant pelvic and/or femoral osteotomies in children after walking age might have reduced the rate of ON. Our results also confirm redislocation resulting from a suboptimal initial primary procedure and the need to consider secondary reconstructive procedures for residual acetabular dysplasia when assessing ON risk. To minimize the risk of the development of ON, we advocate early reduction of the dislocated hip during the first year of life to avoid the need for concomitant osteotomies. Acknowledgment We thank Dori Kelly MA, for English language editing of the manuscript. References 1. Aguş H, Omeroğlu H, Uçar H, Biçimoglu A, Türmer Y. Evaluation of the risk factors of avascular necrosis of the femoral head in developmental dysplasia of the hip in infants younger than 18 months of age. J Pediatr Orthop B. 2002;11: Barrett WP, Staheli LT, Chew DE. The effectiveness of the Salter innominate osteotomy in the treatment of congenital dislocation of the hip. J Bone Joint Surg Am. 1986;68: Berkeley ME, Dickson JH, Cain TE, Donovan MM. Surgical therapy for congenital dislocation of the hip in patients who are twelve to thirty-six months old. J Bone Joint Surg Am. 1984;66: Brougham DI, Broughton NS, Cole WG, Menelaus MB. Avascular necrosis following closed reduction of congenital dislocation of the hip: review of influencing factors and long-term follow-up. J Bone Joint Surg Br. 1990;72: Bucholz RW, Ogden J. Patterns of ischemic necrosis of the proximal femur in nonoperatively treated congenital hip disease. The Hip. Proceedings of the Sixth Open Scientific Meeting of the Hip Society. St Louis, MO: CV Mosby; 1978:20 6. Carney BT, Clark D, Minter CL. Is the absence of the ossific nucleus prognostic for avascular necrosis after closed reduction of developmental dysplasia of the hip? J Surg Orthop Adv. 2004;13: Clarke NM, Jowett AJ, Parker L. The surgical treatment of established congenital dislocation of the hip: results of surgery after planned delayed intervention following the appearance of the capital femoral ossific nucleus. J Pediatr Orthop. 2005;25: Cooperman DR, Wallensten R, Stulberg SD. Post-reduction avascular necrosis in congenital dislocation of the hip. J Bone Joint Surg Am. 1980;62: Cooperman DR, Wallensten R, Stulberg SD. Acetabular dysplasia in the adult. Clin Orthop Relat Res. 1983;175: Gage JR, Winter RB. Avascular necrosis of the capital femoral epiphysis as a complication of closed reduction of congenital dislocation of the hip: a critical review of twenty years experience at Gillette Children s Hospital. J Bone Joint Surg Am. 1972;54: Galpin RD, Roach JW, Wenger DR, Herring JA, Birch JG. Onestage treatment of congenital dislocation of the hip in older children, including femoral shortening. J Bone Joint Surg Am. 1989;71: Graf R. Fundamentals of sonographic diagnosis of infant hip dysplasia. J Pediatr Orthop. 1984;4: Gulman B, Tuncay IC, Dabak N, Karaismailoglu N. Salter s innominate osteotomy in the treatment of congenital hip dislocation: a long-term review. J Pediatr Orthop. 1994;14: Harris NH, Lloyd-Roberts GC, Gallien R. Acetabular development in congenital dislocation of the hip: with special reference to the indications for acetabuloplasty and pelvic or femoral realignment osteotomy. J Bone Joint Surg Br. 1975;57: Kahle WK, Anderson MB, Alpert J, Stevens PM, Coleman SS. The value of preliminary traction in the treatment of congenital dislocation of the hip. J Bone Joint Surg Am. 1990;72: Keret D, MacEwen GD. Growth disturbance of the proximal part of the femur after treatment for congenital dislocation of the hip. J Bone Joint Surg Am. 1991;73: Kershaw CJ, Ware HE, Pattinson R, Fixsen JA. Revision of failed open reduction of congenital dislocation of the hip. J Bone Joint Surg Br. 1993;75: Klisic P, Jankovic L. Combined procedure of open reduction and shortening of the femur in treatment of congenital dislocation of the hips in older children. Clin Orthop Relat Res. 1976;119: Lindstrom JR, Ponseti IV, Wenger DR. Acetabular development after reduction in congenital dislocation of the hip. J Bone Joint Surg Am. 1979;61: Luhmann SJ, Schoenecker PL, Anderson AM, Bassett GS. The prognostic importance of the ossific nucleus in the treatment of congenital dysplasia of the hip. J Bone Joint Surg Am. 1998;80:
11 260 Pospischill et al. Clinical Orthopaedics and Related Research Malvitz TA, Weinstein SL. Closed reduction for congenital dysplasia of the hip: functional and radiographic results after an average of thirty years. J Bone Joint Surg Am. 1994;76: Mardam-Bey TH, MacEwen GD. Congenital hip dislocation after walking age. J Pediatr Orthop. 1982;2: McCluskey WP, Bassett GS, Mora-Garcia G, MacEwen GD. Treatment of failed open reduction for congenital dislocation of the hip. J Pediatr Orthop. 1989;9: Pemberton PA. Pericapsular osteotomy of the ilium for treatment of congenital subluxation and dislocation of the hip. J Bone Joint Surg Am. 1965;47: Roposch A, Stöhr KK, Dobson M. The effect of the femoral head ossific nucleus in the treatment of developmental dysplasia of the hip: a meta-analysis. J Bone Joint Surg Am. 2009;91: Salter RB. Role of innominate osteotomy in the treatment of congenital dislocation and subluxation of the hip in the older child. J Bone Joint Surg Am. 1966;48: Salter RB. The classic: innominate osteotomy in the treatment of congenital dislocation and subluxation of the hip by Robert B. Salter, J Bone Joint Surg (Brit) 43B:3:518, Clin Orthop Relat Res. 1978;137: Salter RB, Kostuik J, Dallas S. Avascular necrosis of the femoral head as a complication of treatment for congenital dislocation of the hip in young children: a clinical and experimental investigation. Can J Surg. 1969;12: Schoenecker PL, Strecker WB. Congenital dislocation of the hip in children: comparison of the effects of femoral shortening and of skeletal traction in treatment. J Bone Joint Surg Am. 1984;66: Segal LS, Boal DK, Borthwick L, Clark MW, Localio AR, Schwentker EP. Avascular necrosis after treatment of DDH: the protective influence of the ossific nucleus. J Pediatr Orthop. 1999;19: Tönnis D. Normal values of the hip joint for the evaluation of X-rays in children and adults. Clin Orthop Relat Res. 1976;119: Tönnis D. Congenital Dysplasia and Dislocation of the Hip in Children and Adults. Berlin, Germany: Springer-Verlag; Tönnis D. Surgical treatment of congenital dislocation of the hip. Clin Orthop Relat Res. 1990;258: Weiner DS, Hoyt WA Jr, O Dell HW. Congenital dislocation of the hip: the relationship of premanipulation traction and age to avascular necrosis of the femoral head. J Bone Joint Surg Am. 1977;59:
Reduction of a dislocation of the hip due to developmental dysplasia: Implications for the need for future surgery
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2-1-2003 Reduction of a dislocation of the hip due to developmental dysplasia: Implications for the need for future
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2-1-2003 Reduction of a dislocation of the hip due to developmental dysplasia: Implications for the need for future
The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH)
 The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH) Perajit Eamsobhana MD*, Kamwong Saisamorn MD*, Tanatip Sisuchinthara MS* Thunchanok Jittivilai PN*, Kamolporn Keawpornsawan
The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH) Perajit Eamsobhana MD*, Kamwong Saisamorn MD*, Tanatip Sisuchinthara MS* Thunchanok Jittivilai PN*, Kamolporn Keawpornsawan
Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study
 Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
Original Article Results of simultaneous open reduction and Salter innominate osteotomy for developmental dysplasia of the hip
 Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 6-10 Original Article Results of simultaneous open reduction and Salter innominate osteotomy for developmental dysplasia of the hip Banskota
Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 6-10 Original Article Results of simultaneous open reduction and Salter innominate osteotomy for developmental dysplasia of the hip Banskota
Abstract. Introduction
 Outcome of Triple Procedure in Older Children with Developmental Dysplasia of Hip (DDH) Masood Umer, Haq Nawaz 2, Pashtoon Murtaza Kasi 2, Mahmood Ahmed 3, Syed Sohail Ali 2 Department of Surgery, Medical
Outcome of Triple Procedure in Older Children with Developmental Dysplasia of Hip (DDH) Masood Umer, Haq Nawaz 2, Pashtoon Murtaza Kasi 2, Mahmood Ahmed 3, Syed Sohail Ali 2 Department of Surgery, Medical
Subluxation of the hip presenting for the first time
 The treatment of subluxation of the hip in children over the age of four years John A. Fixsen, Patrick L. S. Li From the Hospitals for Sick Children, Great Ormond Street, London, England Subluxation of
The treatment of subluxation of the hip in children over the age of four years John A. Fixsen, Patrick L. S. Li From the Hospitals for Sick Children, Great Ormond Street, London, England Subluxation of
Risk factors for avascular necrosis after closed reduction for developmental dysplasia of the hip
 J Child Orthop (2016) 10:185 192 DOI 10.1007/s11832-016-0743-7 ORIGINAL CLINICAL ARTICLE Risk factors for avascular necrosis after closed reduction for developmental dysplasia of the hip Mathew D. Schur
J Child Orthop (2016) 10:185 192 DOI 10.1007/s11832-016-0743-7 ORIGINAL CLINICAL ARTICLE Risk factors for avascular necrosis after closed reduction for developmental dysplasia of the hip Mathew D. Schur
A One Stage Open Reduction With Salter's Innominate Osteotomy And Corrective Femoral Osteotomy For The Treatment Of Congenital Dysplasia Of The Hip
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 1 Number 2 A One Stage Open Reduction With Salter's Innominate Osteotomy And Corrective Femoral Osteotomy For The Treatment Of Congenital Dysplasia
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 1 Number 2 A One Stage Open Reduction With Salter's Innominate Osteotomy And Corrective Femoral Osteotomy For The Treatment Of Congenital Dysplasia
REDISLOCATION FOLLOWING OPERATIONS TO REDUCE HIP OR TREATING DYSPLASIA IN DEVELOPMENTAL DYSPLASIA OF THE HIP
 Original Article REDISLOCATION FOLLOWING OPERATIONS TO REDUCE HIP OR TREATING DYSPLASIA IN DEVELOPMENTAL DYSPLASIA OF THE HIP Saeid Tabatabaei 1, Ahmad Dashtbozorg 2, Sharareh Shalamzari 3 ABSTRACT Objectives:
Original Article REDISLOCATION FOLLOWING OPERATIONS TO REDUCE HIP OR TREATING DYSPLASIA IN DEVELOPMENTAL DYSPLASIA OF THE HIP Saeid Tabatabaei 1, Ahmad Dashtbozorg 2, Sharareh Shalamzari 3 ABSTRACT Objectives:
After open reduction for developmental dysplasia of
 Test of stability as an aid to decide the need for osteotomy in association with open reduction in developmental dysplasia of the hip A LONG-TERM REVIEW H. G. Zadeh, A. Catterall, A. Hashemi-Nejad, R.
Test of stability as an aid to decide the need for osteotomy in association with open reduction in developmental dysplasia of the hip A LONG-TERM REVIEW H. G. Zadeh, A. Catterall, A. Hashemi-Nejad, R.
Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip
 International Orthopaedics (SICOT) (2012) 36:1661 1668 DOI 10.1007/s00264-012-1587-5 ORIGINAL PAPER Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip Michiel A. J. van de
International Orthopaedics (SICOT) (2012) 36:1661 1668 DOI 10.1007/s00264-012-1587-5 ORIGINAL PAPER Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip Michiel A. J. van de
Outcome of surgical management of late presenting developmental dysplasia of hip with pelvic and femoral osteotomies
 Original Research Article DOI: 10.18231/2395-1362.2018.0012 Outcome of surgical management of late presenting developmental dysplasia of hip with pelvic and femoral osteotomies G. Jagadesh 1, Venugopal
Original Research Article DOI: 10.18231/2395-1362.2018.0012 Outcome of surgical management of late presenting developmental dysplasia of hip with pelvic and femoral osteotomies G. Jagadesh 1, Venugopal
The surgical treatment of developmental dislocation of the hip in older children : A comparative study
 Acta Orthop. Belg., 2005, 71, 678-685 ORIGINAL STUDY The surgical treatment of developmental dislocation of the hip in older children : A comparative study Gunduz TEZEREN, Mehmet TUKENMEZ, Okay BULUT,
Acta Orthop. Belg., 2005, 71, 678-685 ORIGINAL STUDY The surgical treatment of developmental dislocation of the hip in older children : A comparative study Gunduz TEZEREN, Mehmet TUKENMEZ, Okay BULUT,
ONE STAGE COMBINED SURGICAL TREATMENT FOR DEVELOPMENTAL DISLOCATION OF THE HIP IN OLDER CHILDREN INCLUDING FEMORAL SHORTENING
 Basrah Journal Original Article Of Surgery Bas J Surg, March, 17, 2011 ONE STAGE COMBINED SURGICAL TREATMENT FOR DEVELOPMENTAL DISLOCATION OF THE HIP IN OLDER CHILDREN INCLUDING FEMORAL SHORTENING MBChB,
Basrah Journal Original Article Of Surgery Bas J Surg, March, 17, 2011 ONE STAGE COMBINED SURGICAL TREATMENT FOR DEVELOPMENTAL DISLOCATION OF THE HIP IN OLDER CHILDREN INCLUDING FEMORAL SHORTENING MBChB,
Surgical Therapy for Congenital Dislocation of the Hip in Patients Who Are Twelve to Thirty-six Months Old
 Copyright 984 by The Journal of Bone and Joint Surgers. Incorporated Surgical Therapy for Congenital Dislocation of the Hip in Patients Who Are Twelve to Thirty-six Months Old BY MICHAEL E. BERKELEY, M.D.*,
Copyright 984 by The Journal of Bone and Joint Surgers. Incorporated Surgical Therapy for Congenital Dislocation of the Hip in Patients Who Are Twelve to Thirty-six Months Old BY MICHAEL E. BERKELEY, M.D.*,
Downloaded from:
 Niziol, R; Elvey, M; Protopapa, E; Roposch, A (2017) Association between the ossific nucleus and osteonecrosis in treating developmental dysplasia of the Hip: updated meta-analysis. BMC Musculoskelet Disord,
Niziol, R; Elvey, M; Protopapa, E; Roposch, A (2017) Association between the ossific nucleus and osteonecrosis in treating developmental dysplasia of the Hip: updated meta-analysis. BMC Musculoskelet Disord,
TREATMENT OF DEVELOPMENTAL DISLOCATION OF THE HIP IN CHILDREN AFTER WALKING AGE
 TREATMENT OF DEVELOPMENTAL DISLOCATION OF THE HIP IN CHILDREN AFTER WALKING AGE INDICATIONS FROM TWO-DIRECTIONAL ARTHROGRAPHY SHIGERU MITANI, YOICHI NAKATSUKA, HIROFUMI AKAZAWA, KIYOSHI AOKI, HAJIME INOUE
TREATMENT OF DEVELOPMENTAL DISLOCATION OF THE HIP IN CHILDREN AFTER WALKING AGE INDICATIONS FROM TWO-DIRECTIONAL ARTHROGRAPHY SHIGERU MITANI, YOICHI NAKATSUKA, HIROFUMI AKAZAWA, KIYOSHI AOKI, HAJIME INOUE
Evaluation of the results of operative treatment of hip dysplasia in children after the walking age
 Alexandria Journal of Medicine (2012) 48, 115 122 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Evaluation of the results of operative
Alexandria Journal of Medicine (2012) 48, 115 122 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Evaluation of the results of operative
Evaluation of the Results of Operative Treatment of Hip Dysplasia in Children after the walking age
 ORIGINAL ARTICLE Evaluation of the Results of Operative Treatment of Hip Dysplasia in Children after the walking age MUHAMMAD KAMRAN SIDDIQUI, MUHAMMAD KAMRAN SHAFI, BASHIR QAISRANI ABSTRACT Background:
ORIGINAL ARTICLE Evaluation of the Results of Operative Treatment of Hip Dysplasia in Children after the walking age MUHAMMAD KAMRAN SIDDIQUI, MUHAMMAD KAMRAN SHAFI, BASHIR QAISRANI ABSTRACT Background:
Subsartorial Approach in Open Reduction of Developmental Dysplasia of Hip
 Med. J. Cairo Univ., Vol. 84, No. 2, March: 287-291, 2016 www.medicaljournalofcairouniversity.net Subsartorial Approach in Open Reduction of Developmental Dysplasia of Hip MOHAMED M. HEGAZY, M.D.; MOHAMED
Med. J. Cairo Univ., Vol. 84, No. 2, March: 287-291, 2016 www.medicaljournalofcairouniversity.net Subsartorial Approach in Open Reduction of Developmental Dysplasia of Hip MOHAMED M. HEGAZY, M.D.; MOHAMED
The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip
 The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip Firas A. Suleiman, MD*, Fadi Al Rousan, MD*, Ahmad Almarzoq, MD *, Razi Altarawneh, MD*, Hidar Soudi, MD* ABSTRACT
The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip Firas A. Suleiman, MD*, Fadi Al Rousan, MD*, Ahmad Almarzoq, MD *, Razi Altarawneh, MD*, Hidar Soudi, MD* ABSTRACT
EARLY OPEN REDUCFION FOR CONGENITAL DISLOCATION OF THE HIP
 EARLY OPEN REDUCFION FOR CONGENITAL DISLOCATION OF THE HIP SUNIL DHAR, J. F. TAYLOR, W. A. JONES, R. OWEN From Alder Hey Children s Hospital, Liverpool We have reviewed 82 children with congenital dislocation
EARLY OPEN REDUCFION FOR CONGENITAL DISLOCATION OF THE HIP SUNIL DHAR, J. F. TAYLOR, W. A. JONES, R. OWEN From Alder Hey Children s Hospital, Liverpool We have reviewed 82 children with congenital dislocation
Surgical treatment for developmental dysplasia of the hip- a single surgeon series of 47 hips with a 7 year mean follow up
 754 Acta Orthop. Belg., 2016, 82, j. 754-761 mcfarlane, j. h. kuiper, n. kiely ORIGINAL STUDY Surgical treatment for developmental dysplasia of the hip- a single surgeon series of 47 hips with a 7 year
754 Acta Orthop. Belg., 2016, 82, j. 754-761 mcfarlane, j. h. kuiper, n. kiely ORIGINAL STUDY Surgical treatment for developmental dysplasia of the hip- a single surgeon series of 47 hips with a 7 year
Acetabular dysplasia after treatment for developmental dysplasia of the hip
 Children s orthopaedics Acetabular dysplasia after treatment for developmental dysplasia of the hip IMPLICATIONS FOR SECONDARY PROCEDURES J. Albinana, L. A. Dolan, K. F. Spratt, J. Morcuende, M. D. Meyer,
Children s orthopaedics Acetabular dysplasia after treatment for developmental dysplasia of the hip IMPLICATIONS FOR SECONDARY PROCEDURES J. Albinana, L. A. Dolan, K. F. Spratt, J. Morcuende, M. D. Meyer,
Bo Ning, Yi Yuan, Jie Yao, Sichng Zhang and Jun Sun *
 Ning et al. BMC Musculoskeletal Disorders 2014, 15:401 RESEARCH ARTICLE Open Access Analyses of outcomes of one-stage operation for treatment of late-diagnosed developmental dislocation of the hip: 864
Ning et al. BMC Musculoskeletal Disorders 2014, 15:401 RESEARCH ARTICLE Open Access Analyses of outcomes of one-stage operation for treatment of late-diagnosed developmental dislocation of the hip: 864
Avascular necrosis following closed reduction for treatment of developmental dysplasia of the hip: a systematic review
 J Child Orthop (2016) 10:627 632 DOI 10.1007/s11832-016-0776-y ORIGINAL CLINICAL ARTICLE Avascular necrosis following closed reduction for treatment of developmental dysplasia of the hip: a systematic
J Child Orthop (2016) 10:627 632 DOI 10.1007/s11832-016-0776-y ORIGINAL CLINICAL ARTICLE Avascular necrosis following closed reduction for treatment of developmental dysplasia of the hip: a systematic
Childhood hip conditions. Belen Carsi Paediatric Orthopaedic Consultant
 Childhood hip conditions Belen Carsi Paediatric Orthopaedic Consultant Developmental Dysplasia of the Hip Legg-Calve-Perthes disease Slipped Capital femoral epiphysis Limp Arthritis Developmental Dysplasia
Childhood hip conditions Belen Carsi Paediatric Orthopaedic Consultant Developmental Dysplasia of the Hip Legg-Calve-Perthes disease Slipped Capital femoral epiphysis Limp Arthritis Developmental Dysplasia
Surgical Treatment of Developmental Dysplasia of the Hip in Children Three to Five Years of Age
 ISSN: 2572-2964 Volume 2, Issue 1, 8 Pages Research Article Introduction The neglected DDH with adaptive changes in bone and soft tissue is difficult to treat and can lead to permanent disability. [1].
ISSN: 2572-2964 Volume 2, Issue 1, 8 Pages Research Article Introduction The neglected DDH with adaptive changes in bone and soft tissue is difficult to treat and can lead to permanent disability. [1].
Is ultrasound screening for DDH in babies born breech sufficient?
 J Child Orthop (2010) 4:3 8 DOI 10.1007/s11832-009-0217-2 ORIGINAL CLINICAL ARTICLE Is ultrasound screening for DDH in babies born breech sufficient? Meghan Imrie Vanessa Scott Philip Stearns Tracey Bastrom
J Child Orthop (2010) 4:3 8 DOI 10.1007/s11832-009-0217-2 ORIGINAL CLINICAL ARTICLE Is ultrasound screening for DDH in babies born breech sufficient? Meghan Imrie Vanessa Scott Philip Stearns Tracey Bastrom
Treatment of DDH before Walking Age 고려대학안암병원
 Treatment of DDH before Walking Age 이 순혁 고려대학안암병원 Subluxated Hip Always to deg. hip The more, the earlier Even in 2nd Decade Dysplastic Hip Eventually to osteoarthritis but later Etiology of end-stage
Treatment of DDH before Walking Age 이 순혁 고려대학안암병원 Subluxated Hip Always to deg. hip The more, the earlier Even in 2nd Decade Dysplastic Hip Eventually to osteoarthritis but later Etiology of end-stage
Mohamed El-Sayed Tarek Ahmed Sameh Fathy Hosam Zyton. Introduction
 J Child Orthop (2012) 6:471 477 DOI 10.1007/s11832-012-0451-x ORIGINAL CLINICAL ARTICLE The effect of Dega acetabuloplasty and Salter innominate on acetabular remodeling monitored by the acetabular index
J Child Orthop (2012) 6:471 477 DOI 10.1007/s11832-012-0451-x ORIGINAL CLINICAL ARTICLE The effect of Dega acetabuloplasty and Salter innominate on acetabular remodeling monitored by the acetabular index
Popliteal angle as an indicator for successful closed reduction of developmental dysplasia of the hip.
 Popliteal angle as an indicator for successful closed reduction of developmental dysplasia of the hip. Item Type Article Authors Molony, Diarmuid C;Harty, James A;Burke, Thomas E;D'Souza, Lester G Citation
Popliteal angle as an indicator for successful closed reduction of developmental dysplasia of the hip. Item Type Article Authors Molony, Diarmuid C;Harty, James A;Burke, Thomas E;D'Souza, Lester G Citation
Ultrasound-guided gradual reduction using flexion and abduction continuous traction for developmental dysplasia of the hip
 K. Fukiage, T. Futami, Y. Ogi, Y. Harada, F. Shimozono, N. Kashiwagi, T. Takase, S. Suzuki From Shiga Medical Center for Children, Japan K. Fukiage, MD, PhD, Paediatric Orthopaedic Surgeon T. Futami, MD,
K. Fukiage, T. Futami, Y. Ogi, Y. Harada, F. Shimozono, N. Kashiwagi, T. Takase, S. Suzuki From Shiga Medical Center for Children, Japan K. Fukiage, MD, PhD, Paediatric Orthopaedic Surgeon T. Futami, MD,
DDH: Pathology Diagnosis, and Treatment before Walking Age
 DDH: Pathology Diagnosis, and Treatment before Walking Age 영남의대 김세동 Ⅰ. Terminology of hip dysplasia a. Congenital dysplasia or dislocation of the hip(cdh): Hippocrates Congenital -Existing at Birth but
DDH: Pathology Diagnosis, and Treatment before Walking Age 영남의대 김세동 Ⅰ. Terminology of hip dysplasia a. Congenital dysplasia or dislocation of the hip(cdh): Hippocrates Congenital -Existing at Birth but
Developmental Dislocation of the Hip Successfully Treated by Preoperative Traction and Medial Open Reduction: A 22-year Mean Followup
 Clin Orthop Relat Res (2015) 473:2658 2669 DOI 10.1007/s11999-015-4264-3 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Developmental
Clin Orthop Relat Res (2015) 473:2658 2669 DOI 10.1007/s11999-015-4264-3 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Developmental
EVALUATION OF MEDIAL APPROACH (LUDLLOF) FOR OPEN REDUCTION OF DEVELOPMENTAL DYSPLASIA OF THE HIP IN CHILDREN
 Basrah Journal Original Article Of Surgery EVALUATION OF MEDIAL APPROACH (LUDLLOF) FOR OPEN REDUCTION OF DEVELOPMENTAL DYSPLASIA OF THE HIP IN CHILDREN Haider R Majeed *, Ali A Ahmed Al-Iedan @ & Haider
Basrah Journal Original Article Of Surgery EVALUATION OF MEDIAL APPROACH (LUDLLOF) FOR OPEN REDUCTION OF DEVELOPMENTAL DYSPLASIA OF THE HIP IN CHILDREN Haider R Majeed *, Ali A Ahmed Al-Iedan @ & Haider
Long-term outcome following medial open reduction in developmental dysplasia of the hip: a retrospective cohort study
 J Child Orthop (2016) 10:179 184 DOI 10.1007/s11832-016-0729-5 ORIGINAL CLINICAL ARTICLE Long-term outcome following medial open reduction in developmental dysplasia of the hip: a retrospective cohort
J Child Orthop (2016) 10:179 184 DOI 10.1007/s11832-016-0729-5 ORIGINAL CLINICAL ARTICLE Long-term outcome following medial open reduction in developmental dysplasia of the hip: a retrospective cohort
DDH New Developments and Timeless Classics. DDH Define Treatment Group. (by age) DDH Imaging Choice in 6wk old Infant?
 The 59 th Annual Edward T. Smith Orthopaedic Lectureship Emerging Concepts in the Surgical Management of the Hip: Deformity, Impingement and Fracture DDH New Developments and Timeless Classics Perry L.
The 59 th Annual Edward T. Smith Orthopaedic Lectureship Emerging Concepts in the Surgical Management of the Hip: Deformity, Impingement and Fracture DDH New Developments and Timeless Classics Perry L.
Does Salter Innominate Osteotomy Predispose the Patient to Acetabular Retroversion in Adulthood?
 Clin Orthop Relat Res (2015) 473:1755 1762 DOI 10.1007/s11999-014-4053-4 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Does Salter
Clin Orthop Relat Res (2015) 473:1755 1762 DOI 10.1007/s11999-014-4053-4 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Does Salter
ORIGINAL ARTICLE. Anisuddin Bhatti, Jagdesh Kumar, Siraj Ahmed Butt
 1015 ORIGINAL ARTICLE Outcome of one stage combined open reduction, pelvic and derotation femoral osteotomy in congenital dislocated hips of children younger than three years age Anisuddin Bhatti, Jagdesh
1015 ORIGINAL ARTICLE Outcome of one stage combined open reduction, pelvic and derotation femoral osteotomy in congenital dislocated hips of children younger than three years age Anisuddin Bhatti, Jagdesh
OPEN REDUCTION OF HIP DISLOCATION IN PATIENTS WITH ARTHROGRYPOSIS MULTIPLEX CONGENITA - AN ANTEROMEDIAL APPROACH
 ARTIGO ORIGINAL OPEN REDUCTION OF HIP DISLOCATION IN PATIENTS WITH ARTHROGRYPOSIS MULTIPLEX CONGENITA - AN ANTEROMEDIAL APPROACH Luis Eduardo Munhoz da Rocha 2, Fábio Koiti Nishimori 3, Daniel Carvalho
ARTIGO ORIGINAL OPEN REDUCTION OF HIP DISLOCATION IN PATIENTS WITH ARTHROGRYPOSIS MULTIPLEX CONGENITA - AN ANTEROMEDIAL APPROACH Luis Eduardo Munhoz da Rocha 2, Fábio Koiti Nishimori 3, Daniel Carvalho
DEVELOPMENTAL HIP DYSPLASIA PREDICTING OUTCOME AND IMPLICATIONS FOR SECONDARY PROCEDURES. Dr G B Firth
 DEVELOPMENTAL HIP DYSPLASIA PREDICTING OUTCOME AND IMPLICATIONS FOR SECONDARY PROCEDURES Dr G B Firth A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg,
DEVELOPMENTAL HIP DYSPLASIA PREDICTING OUTCOME AND IMPLICATIONS FOR SECONDARY PROCEDURES Dr G B Firth A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg,
SCREENING THE NEWBORN FOR DEVELOPMENTAL DYSPLASIA OF THE HIP: REVIEW
 SCREENING THE NEWBORN FOR DEVELOPMENTAL DYSPLASIA OF THE HIP: REVIEW Dr. Upendra Yadav *1, 3, Dr. Zhu Xiao Fang 3, Dr. Ajit Kumar Yadav 1, 2, Dr. Sudhir Kumar Yadav 4 and Dr. Jeetendra Yadav 4 1 Yangtze
SCREENING THE NEWBORN FOR DEVELOPMENTAL DYSPLASIA OF THE HIP: REVIEW Dr. Upendra Yadav *1, 3, Dr. Zhu Xiao Fang 3, Dr. Ajit Kumar Yadav 1, 2, Dr. Sudhir Kumar Yadav 4 and Dr. Jeetendra Yadav 4 1 Yangtze
One-stage Hip Reconstruction for Developmental Hip Dysplasia in Children over 8 Years of Age
 ORIGINAL ARTICLE http://dx.doi.org/10.5371/hp.2018.30.4.260 Print ISSN 2287-3260 Online ISSN 2287-3279 One-stage Hip Reconstruction for Developmental Hip Dysplasia in Children over 8 Years of Age Irfan
ORIGINAL ARTICLE http://dx.doi.org/10.5371/hp.2018.30.4.260 Print ISSN 2287-3260 Online ISSN 2287-3279 One-stage Hip Reconstruction for Developmental Hip Dysplasia in Children over 8 Years of Age Irfan
DDH. Abnormal hip development Traditionally CDH (congenital dysplasia of the hip) Today DDH(developmental dysplasia of the hip)
 DDH Update on Screening Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics Children s Mercy Kansas
DDH Update on Screening Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics Children s Mercy Kansas
DDH: Pathology, Diagnosis & Treatment before Walking Age 고려대학안암병원
 DDH: Pathology, Diagnosis & Treatment before Walking Age 이 순혁 고려대학안암병원 Developmental Hip Dysplasia (DDH) Klisic 1988 AAOS 1991 Congenital Hip Dislocation Not always congenital or dislocated Causes, Risk
DDH: Pathology, Diagnosis & Treatment before Walking Age 이 순혁 고려대학안암병원 Developmental Hip Dysplasia (DDH) Klisic 1988 AAOS 1991 Congenital Hip Dislocation Not always congenital or dislocated Causes, Risk
Developmental dysplasia of the hip: What has changed in the last 20 years?
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v6.i11.886 World J Orthop 2015 December 18; 6(11): 886-901 ISSN 2218-5836 (online)
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v6.i11.886 World J Orthop 2015 December 18; 6(11): 886-901 ISSN 2218-5836 (online)
Society for Pediatric Radiology 2015 Hands on Session. DDH: Pitfalls and Practical Tips
 Society for Pediatric Radiology 2015 Hands on Session DDH: Pitfalls and Practical Tips Michael A. DiPietro, M.D. John F. Holt Collegiate Professor of Radiology Professor of Pediatrics and Communicable
Society for Pediatric Radiology 2015 Hands on Session DDH: Pitfalls and Practical Tips Michael A. DiPietro, M.D. John F. Holt Collegiate Professor of Radiology Professor of Pediatrics and Communicable
Hip ultrasound for developmental dysplasia: the 50% rule
 Pediatr Radiol (2017) 47:817 821 DOI 10.1007/s00247-017-3802-4 COMMENTARY Hip ultrasound for developmental dysplasia: the 50% rule H. Theodore Harcke 1 & B. Pruszczynski 2 Received: 27 October 2016 /Revised:
Pediatr Radiol (2017) 47:817 821 DOI 10.1007/s00247-017-3802-4 COMMENTARY Hip ultrasound for developmental dysplasia: the 50% rule H. Theodore Harcke 1 & B. Pruszczynski 2 Received: 27 October 2016 /Revised:
Radiological Sequelae of developmental dysplasia of the hip: a Review
 Radiological Sequelae of developmental dysplasia of the hip: a Review Poster No.: P-0037 Congress: ESSR 2012 Type: Scientific Exhibit Authors: S. G. Flanagan, J. Sarkodieh, K. Mcdonald, M. Ramachandran,
Radiological Sequelae of developmental dysplasia of the hip: a Review Poster No.: P-0037 Congress: ESSR 2012 Type: Scientific Exhibit Authors: S. G. Flanagan, J. Sarkodieh, K. Mcdonald, M. Ramachandran,
A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip
 Acta Orthop. Belg., 2013, 79, 524-529 ORIGINAL STUDY A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip Hakan Atalar, Halil Dogruel,
Acta Orthop. Belg., 2013, 79, 524-529 ORIGINAL STUDY A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip Hakan Atalar, Halil Dogruel,
L side 65% Torticollis, Plagiocephaly, Metatarsus varus Flat foot.
 DEVELOPMENTAL DISLOCATION OF THE HIP [DDH] Older terminology was Congenital dislocation of the hip. DDH means developmental dysplasia of the hip. DDH is better than CDH as dislocation is not always congenital.
DEVELOPMENTAL DISLOCATION OF THE HIP [DDH] Older terminology was Congenital dislocation of the hip. DDH means developmental dysplasia of the hip. DDH is better than CDH as dislocation is not always congenital.
Classifications in Brief
 Clin Orthop Relat Res (2013) 471:2068 2072 DOI 10.1007/s11999-013-2992-9 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons IN BRIEF Classifications
Clin Orthop Relat Res (2013) 471:2068 2072 DOI 10.1007/s11999-013-2992-9 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons IN BRIEF Classifications
Hip Biomechanics and Osteotomies
 Hip Biomechanics and Osteotomies Organization Introduction Hip Biomechanics Principles of Osteotomy Femoral Osteotomies Pelvic Osteotomies Summary Inroduction Osteoarthritis is very prevalent Primary OA
Hip Biomechanics and Osteotomies Organization Introduction Hip Biomechanics Principles of Osteotomy Femoral Osteotomies Pelvic Osteotomies Summary Inroduction Osteoarthritis is very prevalent Primary OA
Hip Dysplasia for the Primary Care Physician George Gantsoudes, MD. November 4, 2017
 Hip Dysplasia for the Primary Care Physician George Gantsoudes, MD November 4, 2017 Introduction Developmental Dysplasia of the Hip DDH - preferred term Teratologic hips Subluxation Dislocation-usually
Hip Dysplasia for the Primary Care Physician George Gantsoudes, MD November 4, 2017 Introduction Developmental Dysplasia of the Hip DDH - preferred term Teratologic hips Subluxation Dislocation-usually
Copyright Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited.
 Original article 222 Legg Calvé Perthes disease in patients under 5 years of age does not always result in a good outcome. Personal experience and meta-analysis of the literature Kristof Fabry, Guy Fabry
Original article 222 Legg Calvé Perthes disease in patients under 5 years of age does not always result in a good outcome. Personal experience and meta-analysis of the literature Kristof Fabry, Guy Fabry
The surgical treatment of Perthes disease by
 Lateral shelf acetabuloplasty in Perthes disease A REVIEW AT THE END OF GROWTH K. Daly, C. Bruce, A. Catterall From the Royal National Orthopaedic Hospital, Stanmore, England The surgical treatment of
Lateral shelf acetabuloplasty in Perthes disease A REVIEW AT THE END OF GROWTH K. Daly, C. Bruce, A. Catterall From the Royal National Orthopaedic Hospital, Stanmore, England The surgical treatment of
The Pavlik harness is a positioning device commonly
 RESEARCH PAPERS Ultrasound Evaluation of Hip Position in the Pavlik Harness Leslie E. Grissom, MD*, H. Theodore Harcke, MD*, S. Jay Kumar, MOt, George S. Bassett, MOt, G. Dean MacEwen, MOt Fifty infants
RESEARCH PAPERS Ultrasound Evaluation of Hip Position in the Pavlik Harness Leslie E. Grissom, MD*, H. Theodore Harcke, MD*, S. Jay Kumar, MOt, George S. Bassett, MOt, G. Dean MacEwen, MOt Fifty infants
Hip Dysplasia David S. Feldman, MD
 Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Hip dysplasia
Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Hip dysplasia
Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ
 Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ C Fernández, MD; M Guasp, MD; J Gómez Fernández-Montes,
Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ C Fernández, MD; M Guasp, MD; J Gómez Fernández-Montes,
A novel method for assessing postoperative femoral head reduction in developmental dysplasia of the hip
 J Child Orthop (2014) 8:319 324 DOI 10.1007/s11832-014-0600-5 ORIGINAL CLINICAL ARTICLE A novel method for assessing postoperative femoral head reduction in developmental dysplasia of the hip Anthony Cooper
J Child Orthop (2014) 8:319 324 DOI 10.1007/s11832-014-0600-5 ORIGINAL CLINICAL ARTICLE A novel method for assessing postoperative femoral head reduction in developmental dysplasia of the hip Anthony Cooper
)318( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )318( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Outcome of Salter Innominate Osteotomy for Developmental Hip Dysplasia before and after 3 Years Old Taghi Baghdadi, MD;
)318( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Outcome of Salter Innominate Osteotomy for Developmental Hip Dysplasia before and after 3 Years Old Taghi Baghdadi, MD;
Acta Medica Okayama JUNE 2009
 Acta Medica Okayama Volume 63, Issue 3 29 Article 1 JUNE 29 Radiographic Prediction of the Results of Long-term Treatment with the Pavlik Harness for Developmental Dislocation of the Hip Takao Ohmori Hirosuke
Acta Medica Okayama Volume 63, Issue 3 29 Article 1 JUNE 29 Radiographic Prediction of the Results of Long-term Treatment with the Pavlik Harness for Developmental Dislocation of the Hip Takao Ohmori Hirosuke
Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation
 Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation Chatupon Chotigavanichaya MD*, Duangjai Leeprakobboon MD*, Perajit Eamsobhana MD*, Kamolporn Kaewpornsawan
Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation Chatupon Chotigavanichaya MD*, Duangjai Leeprakobboon MD*, Perajit Eamsobhana MD*, Kamolporn Kaewpornsawan
CLINICAL AND RADIOLOGICAL EVALUATION ON DEVELOPMENTAL HIP DYSPLASIA AFTER SALTER AND OMBRÉDANNE PROCEDURE
 ORIGINAL ARTICLE CLINICAL AND RADIOLOGICAL EVALUATION ON DEVELOPMENTAL HIP DYSPLASIA AFTER SALTER Válney Luiz da Rocha 1, André Luiz Coelho Thomé 2, Daniel Labres da Silva Castro 2, Leandro Zica de Oliveira
ORIGINAL ARTICLE CLINICAL AND RADIOLOGICAL EVALUATION ON DEVELOPMENTAL HIP DYSPLASIA AFTER SALTER Válney Luiz da Rocha 1, André Luiz Coelho Thomé 2, Daniel Labres da Silva Castro 2, Leandro Zica de Oliveira
Surgical treatment of developmental dysplasia of the hip in the periadolescent period
 J Orthop Sci (2005) 10:15 21 DOI 10.1007/s00776-004-0850-z Original article Surgical treatment of developmental dysplasia of the hip in the periadolescent period Vasilios A. Papavasiliou 1 and Athanasios
J Orthop Sci (2005) 10:15 21 DOI 10.1007/s00776-004-0850-z Original article Surgical treatment of developmental dysplasia of the hip in the periadolescent period Vasilios A. Papavasiliou 1 and Athanasios
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (4), Page
 The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (4), Page 64466451 Outcome of delayed surgery in developmental hip dysplasia in a tertiary care setting Mohammad Khabti Alnamshan, Ayman
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (4), Page 64466451 Outcome of delayed surgery in developmental hip dysplasia in a tertiary care setting Mohammad Khabti Alnamshan, Ayman
Developmental dysplasia of the hip
 Developmental dysplasia of the hip Shahryar Noordin, Masood Umer, Kamran Hafeez, Haq Nawaz Section of Orthopedics, Dept. of Surgery, Aga Khan University, Karachi, Pakistan Abstract Developmental dysplasia
Developmental dysplasia of the hip Shahryar Noordin, Masood Umer, Kamran Hafeez, Haq Nawaz Section of Orthopedics, Dept. of Surgery, Aga Khan University, Karachi, Pakistan Abstract Developmental dysplasia
The McHale procedure in the treatment of the painful chronically dislocated hip in adolescents and adults with cerebral palsy
 Acta Orthop. Belg., 2009, 75, 181-188 ORIGINAL STUDY The McHale procedure in the treatment of the painful chronically dislocated hip in adolescents and adults with cerebral palsy Anne VAN RIET, Pierre
Acta Orthop. Belg., 2009, 75, 181-188 ORIGINAL STUDY The McHale procedure in the treatment of the painful chronically dislocated hip in adolescents and adults with cerebral palsy Anne VAN RIET, Pierre
Severin Classification System for Evaluation of the Results of Operative Treatment of Congenital Dislocation of the Hip
 Copyright ] 997 by The Journal of Bone and Joint Surgery, Incorporated Severin Classification System for Evaluation of the Results of Operative Treatment of Congenital Dislocation of the Hip A STUDY OF
Copyright ] 997 by The Journal of Bone and Joint Surgery, Incorporated Severin Classification System for Evaluation of the Results of Operative Treatment of Congenital Dislocation of the Hip A STUDY OF
Surgical release of neurological hip luxation in children H. Klima Ostschweizer Kinderspital St. Gallen Abteilung für Kinderorthopädie
 Surgical release of neurological hip luxation in children H. Klima Ostschweizer Kinderspital St. Gallen Abteilung für Kinderorthopädie Development of hip luxation At birth these hips are normal developed,
Surgical release of neurological hip luxation in children H. Klima Ostschweizer Kinderspital St. Gallen Abteilung für Kinderorthopädie Development of hip luxation At birth these hips are normal developed,
ORDER OF VERBAL EXAMS
 ORDER OF VERBAL EXAMS The students are able to register for the exam on the NEPTUN system. The students pick two titles, from the title list available at the beginning of the Semester. This list can be
ORDER OF VERBAL EXAMS The students are able to register for the exam on the NEPTUN system. The students pick two titles, from the title list available at the beginning of the Semester. This list can be
Original Article Clinics in Orthopedic Surgery 2015;7: Kyung Sup Lim, MD, Jong Sup Shim, MD*
 Original Article Clinics in Orthopedic Surgery 2015;7:497-504 http://dx.doi.org/10.4055/cios.2015.7.4.497 Outcomes of Combined Shelf Acetabuloplasty with Femoral Varus Osteotomy in Severe Legg-Calve-Perthes
Original Article Clinics in Orthopedic Surgery 2015;7:497-504 http://dx.doi.org/10.4055/cios.2015.7.4.497 Outcomes of Combined Shelf Acetabuloplasty with Femoral Varus Osteotomy in Severe Legg-Calve-Perthes
Osteogenesis imperfecta (OI) is a genetically determined
 ORIGINAL ARTICLE Hip Dysplasia in Children With Osteogenesis Imperfecta: Association With Collagen Type I C-Propeptide Mutations Waleed Kishta, MBBCH, PhD, FRCSC,*w Fahad H. Abduljabbar, MBBS, FRCSC,*z
ORIGINAL ARTICLE Hip Dysplasia in Children With Osteogenesis Imperfecta: Association With Collagen Type I C-Propeptide Mutations Waleed Kishta, MBBCH, PhD, FRCSC,*w Fahad H. Abduljabbar, MBBS, FRCSC,*z
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail?
 Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail? Andrew J. Bryan 1, MD K. Poehling-Monaghan 1, MD Rohith Mohan 1, BA Nick R Johnson 1, BS Aaron J. Krych 1, MD Bruce A. Levy
Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail? Andrew J. Bryan 1, MD K. Poehling-Monaghan 1, MD Rohith Mohan 1, BA Nick R Johnson 1, BS Aaron J. Krych 1, MD Bruce A. Levy
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH)
 Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Open reduction for developmental dysplasia of the hip: failures of screening or failures of treatment?
 lower limb doi 10.1308/003588413X13511609957137 Open reduction for developmental dysplasia of the hip: AP Sanghrajka 1, CF Murnaghan 2, A Shekkeris 3, DM Eastwood 4 1 Norfolk and Norwich University Hospitals
lower limb doi 10.1308/003588413X13511609957137 Open reduction for developmental dysplasia of the hip: AP Sanghrajka 1, CF Murnaghan 2, A Shekkeris 3, DM Eastwood 4 1 Norfolk and Norwich University Hospitals
Acta Medica Okayama AUGUST 2009
 Acta Medica Okayama Volume 63, Issue 4 2009 Article 2 AUGUST 2009 Radiological and clinical results of rotational acetabular osteotomy combined with femoral intertrochanteric osteotomy for avascular necrosis
Acta Medica Okayama Volume 63, Issue 4 2009 Article 2 AUGUST 2009 Radiological and clinical results of rotational acetabular osteotomy combined with femoral intertrochanteric osteotomy for avascular necrosis
The Hip Baby?? Baby Hippie??
 In Need of a Title? The Hip Baby?? Baby Hippie?? Review of Developmental Dysplasia of the Hip in the Newborn OCR Symposium 2018 Ryan L. Hartman, MD Specialty: Pediatric and Sports Orthopaedics 23 month
In Need of a Title? The Hip Baby?? Baby Hippie?? Review of Developmental Dysplasia of the Hip in the Newborn OCR Symposium 2018 Ryan L. Hartman, MD Specialty: Pediatric and Sports Orthopaedics 23 month
How Does Bony Surgery Affect Results of Anterior Open Reduction in Walking-age Children With Developmental Hip Dysplasia?
 Clin Orthop Relat Res (2016) 474:1199 1208 DOI 10.1007/s11999-015-4598-x Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: THE HIP FROM CHILDHOOD
Clin Orthop Relat Res (2016) 474:1199 1208 DOI 10.1007/s11999-015-4598-x Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: THE HIP FROM CHILDHOOD
Treatment of congenital subluxation and dislocation of the hip by knee splint harness
 Prosthetics and Orthotics International, 1994,18, 34-39 Treatment of congenital subluxation and dislocation of the hip by knee splint harness M. FUKUSHIMA Fukushima Orthopaedic Clinic, Hiroshima City,
Prosthetics and Orthotics International, 1994,18, 34-39 Treatment of congenital subluxation and dislocation of the hip by knee splint harness M. FUKUSHIMA Fukushima Orthopaedic Clinic, Hiroshima City,
Developmental dysplasia of the hip angle trends after operation in different age groups
 Clinical research Developmental dysplasia of the hip angle trends after operation in different age groups Sonja Milasinovic 1, Radivoj Brdar 2, Ivana Petronic 3, Dejan Nikolic 3, Dragana Cirovic 3 1Institute
Clinical research Developmental dysplasia of the hip angle trends after operation in different age groups Sonja Milasinovic 1, Radivoj Brdar 2, Ivana Petronic 3, Dejan Nikolic 3, Dragana Cirovic 3 1Institute
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH)
 Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS
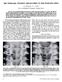 HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS A. B. NEVELOS, p. R. J. BURCH From Leeds/Bradford Orthopaedic Training Schetne Six boys were examined during the second year of life, each with symptoms
HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS A. B. NEVELOS, p. R. J. BURCH From Leeds/Bradford Orthopaedic Training Schetne Six boys were examined during the second year of life, each with symptoms
Early Results of One-Stage Correction for Hip Instability in Cerebral Palsy
 Original Article Clinics in Orthopedic Surgery 2012;4:139-148 http://dx.doi.org/10.4055/cios.2012.4.2.139 Early Results of One-Stage Correction for Hip Instability in Cerebral Palsy Hui Taek Kim, MD, Jae
Original Article Clinics in Orthopedic Surgery 2012;4:139-148 http://dx.doi.org/10.4055/cios.2012.4.2.139 Early Results of One-Stage Correction for Hip Instability in Cerebral Palsy Hui Taek Kim, MD, Jae
Supine and Standing AP Pelvis Radiographs in the Evaluation of Pincer Femoroacetabular Impingement
 Clin Orthop Relat Res (2016) 474:1692 1696 DOI 10.1007/s11999-016-4766-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Supine
Clin Orthop Relat Res (2016) 474:1692 1696 DOI 10.1007/s11999-016-4766-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Supine
A modified surgical approach of the hip in children: is it safe and reliable in patients with developmental hip dysplasia?
 J Child Orthop (2015) 9:199 207 DOI 10.1007/s11832-015-0659-7 ORIGINAL CLINICAL ARTICLE A modified surgical approach of the hip in children: is it safe and reliable in patients with developmental hip dysplasia?
J Child Orthop (2015) 9:199 207 DOI 10.1007/s11832-015-0659-7 ORIGINAL CLINICAL ARTICLE A modified surgical approach of the hip in children: is it safe and reliable in patients with developmental hip dysplasia?
Preoperative Planning for DDH Revision Surgery Tips and Tricks
 Review Article Preoperative Planning for DDH Revision Surgery Tips and Tricks Mousa M. Alhaosawi MD 1, Amir Shahryar Ariamanesh MD 2* 1- King Fahad Hospital, Almadinah Almunawwarah, Saudi Arabia 2- Mashhad
Review Article Preoperative Planning for DDH Revision Surgery Tips and Tricks Mousa M. Alhaosawi MD 1, Amir Shahryar Ariamanesh MD 2* 1- King Fahad Hospital, Almadinah Almunawwarah, Saudi Arabia 2- Mashhad
Delayed fixation of an unstable Slipped capital femoral epiphysis: A case report and review of literature
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Delayed fixation of an unstable Slipped capital femoral epiphysis: A case report and review of literature S Lowndes, A Khanna, D
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Delayed fixation of an unstable Slipped capital femoral epiphysis: A case report and review of literature S Lowndes, A Khanna, D
Hip subluxation and dislocation in cerebral palsy : Outcome of bone surgery in 21 hips
 Acta Orthop. Belg., 2008, 74, 609-614 ORIGINAL STUDY Hip subluxation and dislocation in cerebral palsy : Outcome of bone surgery in 21 hips Pietro PERSIANI, Iakov MOLAYEM, Alessandro CALISTRI, Stefano
Acta Orthop. Belg., 2008, 74, 609-614 ORIGINAL STUDY Hip subluxation and dislocation in cerebral palsy : Outcome of bone surgery in 21 hips Pietro PERSIANI, Iakov MOLAYEM, Alessandro CALISTRI, Stefano
Legg-Calvé-Perthes Disease PART II: PROSPECTIVE MULTICENTER STUDY OF THE EFFECT OF TREATMENT ON OUTCOME
 2121 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Legg-Calvé-Perthes Disease PART II: PROSPECTIVE MULTICENTER STUDY OF THE EFFECT OF TREATMENT ON OUTCOME BY JOHN A. HERRING, MD,
2121 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Legg-Calvé-Perthes Disease PART II: PROSPECTIVE MULTICENTER STUDY OF THE EFFECT OF TREATMENT ON OUTCOME BY JOHN A. HERRING, MD,
Advice for parents about osteotomy of the hip
 Advice for parents about osteotomy of the hip What is an osteotomy and why does my child/young person need this operation? An osteotomy is an operation performed to place and hold the hip in an improved
Advice for parents about osteotomy of the hip What is an osteotomy and why does my child/young person need this operation? An osteotomy is an operation performed to place and hold the hip in an improved
Predictors of femoral shortening for pediatric developmental hip dysplasia surgery: an observational study in 435 patients
 Alassaf Patient Safety in Surgery (2018) 12:29 https://doi.org/10.1186/s13037-018-0176-y RESEARCH Open Access Predictors of femoral shortening for pediatric developmental hip dysplasia surgery: an observational
Alassaf Patient Safety in Surgery (2018) 12:29 https://doi.org/10.1186/s13037-018-0176-y RESEARCH Open Access Predictors of femoral shortening for pediatric developmental hip dysplasia surgery: an observational
What is a Hip Dysplasia?
 What is a Hip Dysplasia? Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia of the hip (CDH)[2] is a congenital or acquired deformation or misalignment of the hip joint.
What is a Hip Dysplasia? Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia of the hip (CDH)[2] is a congenital or acquired deformation or misalignment of the hip joint.
Case Presentations The Child with a Limp
 Case Presentations The Child with a Limp Douglas G. Armstrong, M.D. Professor, PennState Hershey College of Medicine Division Head, Pediatric Orthopaedics Dept. of Orthopaedics and Rehabilitation PennState
Case Presentations The Child with a Limp Douglas G. Armstrong, M.D. Professor, PennState Hershey College of Medicine Division Head, Pediatric Orthopaedics Dept. of Orthopaedics and Rehabilitation PennState
The Proximal Femoral Growth Plate in Perthes Disease
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 458, pp. 150 158 2007 Lippincott Williams & Wilkins The Proximal Femoral Growth Plate in Perthes Disease Marcin E. Domzalski, MD * ; Muharrem Inan, MD
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 458, pp. 150 158 2007 Lippincott Williams & Wilkins The Proximal Femoral Growth Plate in Perthes Disease Marcin E. Domzalski, MD * ; Muharrem Inan, MD
Peggers Super Summaries: Paediatric Hip
 EMBRYOLOGY Development o Mesenchymal stem cells cartilage blood supply bone Dates o 6/40 Limb development o 8-11/40 hip development (acetabulum and hip formed from one bone splitting by apoptosis) o 16/40
EMBRYOLOGY Development o Mesenchymal stem cells cartilage blood supply bone Dates o 6/40 Limb development o 8-11/40 hip development (acetabulum and hip formed from one bone splitting by apoptosis) o 16/40
Radiographic Evaluation Of Dynamic Hip Instability In Lequesne s False Profile View
 Radiographic Evaluation Of Dynamic Hip Instability In Lequesne s False Profile View Ryo Mori 1, Yuji Yasunaga 2, Takuma Yamasaki 1, Michio Hamanishi 1, Takeshi Shoji 1, Sotaro Izumi 1, Susumu Hachisuka
Radiographic Evaluation Of Dynamic Hip Instability In Lequesne s False Profile View Ryo Mori 1, Yuji Yasunaga 2, Takuma Yamasaki 1, Michio Hamanishi 1, Takeshi Shoji 1, Sotaro Izumi 1, Susumu Hachisuka
DEVELOPMENTAL DYSPLASIA OF THE HIP CURRENT TRENDS APLLIED IN ARAD
 DEVELOPMENTAL DYSPLASIA OF THE HIP CURRENT TRENDS APLLIED IN ARAD PAVEL Adrian Ionel 1, BOIA Eugen Sorin 2, 1 PhD, Victor Babes University of Medicine and Pharmacy, Timisoara, Romania 2 Prof., PhD, MD,
DEVELOPMENTAL DYSPLASIA OF THE HIP CURRENT TRENDS APLLIED IN ARAD PAVEL Adrian Ionel 1, BOIA Eugen Sorin 2, 1 PhD, Victor Babes University of Medicine and Pharmacy, Timisoara, Romania 2 Prof., PhD, MD,
