Comparison of anterolateral and posterior approaches in the management of thoracolumbar burst fractures
|
|
|
- Kerrie Susan Hopkins
- 5 years ago
- Views:
Transcription
1 J Neurosurg Spine 5: , 2006 Comparison of anterolateral and posterior approaches in the management of thoracolumbar burst fractures PATRICK W. HITCHON, M.D., JAMES TORNER, PH.D., KURT M. EICHHOLZ, M.D., AND STEPHANIE N. BEELER, B.A. Departments of Neurosurgery and Preventative Medicine and Environmental Health, University of Iowa Carver College of Medicine, Iowa City, Iowa Object. The authors undertook a retrospective cohort study of patients with T11 L2 thoracolumbar burst fractures who underwent decompression and the placement of instrumentation via the anterolateral or posterior approach. Methods. There were 63 thoracolumbar burst fractures in 45 male and 18 female patients. The instrumentation was placed posteriorly in 25 patients and anterolaterally in 38. The mean follow-up duration after discharge from the hospital was 1.8 years (range 6 months 8 years). The mean preoperative Frankel scores in the anterolateral and posterior groups were and , respectively (p = ). Preoperative angular deformity in the anterolateral and posterior groups measured and , respectively (p = ). Postoperatively, angular deformity had been corrected to and in both groups, respectively (p = 0.565). The follow-up Frankel scores had improved to and (p = 0.461). At the latest follow-up examination, angular deformity had progressed to in the anterolateral group and to in the posterior group (p = 0.024). Although surgeons fees were significantly (p = ) higher for patients who underwent anterolateral procedures ($27, ) than for those who underwent posterior surgery ($18, ), there was no intergroup difference in total cost of hospitalization. Conclusions. Rigid guidelines for the selection of anterior or posterior approaches are lacking. Evaluation of the authors results and those of others shows that angular deformity is more successfully corrected and maintained when the anterior approach is used. KEY WORDS thoracolumbar burst fracture anterior approach posterior approach corpectomy spinal instrumentation S URGICAL intervention is indicated in the treatment of burst fractures involving the anterior and posterior halves of the VB when the individual presents with associated deficit, pain, or spinal instability. 8 The goal of surgical intervention is decompression of the neural elements, restoration of VB height, correction of angular deformity, and stabilization. Such decompression and stabilization can be performed anterolaterally through the retroperitoneal flank approach 20,25 or posteriorly with decompression through laminectomy or the transpedicular transfacetal route. 7,21,36 The anterolateral retroperitoneal flank approach allows the surgeon to perform corpectomy and fusion, reconstructing the anterior and middle columns of the spine. Bone fragments can be removed from the canal under direct vision. Following corpectomy, the vertebral column is reconstructed by inserting a graft or Abbreviations used in this paper: AP = anteroposterior; CFC = carbon fiber cage; CT = computed tomography; MR = magnetic resonance; PS = pedicle screw; SF-36 = 36-Item Short Form Health Survey; VB = vertebral body. prosthesis, correcting angulation and loss in VB height. When placing anterior instrumentation for immobilization and fusion, the hardware generally incorporates one VB rostral and one caudal to the fracture. When the posterior route is used, access to the canal is gained by laminectomy or the removal of the facet joints and pedicle, generally on one side, and decompression is achieved by disimpaction. Posterior stabilization generally requires that the instrumentation be placed two levels above and below the site of injury. Both anterolateral and posterior approaches have been associated with favorable results, 7,12,15,27 as well as complications. 24,26 This study is a retrospective cohort investigation of cases in which T11 L2 burst fractures were treated with anterior instrumentation and corpectomy performed via the retroperitoneal flank approach or the midline posterior approach. Until 1998, most burst fractures were treated via the posterior approach. Thereafter, they were treated preferentially via the anterolateral approach. Outcomes in angulation, neurological status, patient-rated satisfaction, and cost analysis were examined and compared. 117
2 P. W. Hitchon, et al. Clinical Material and Methods Data obtained in 63 patients with T11 L2 burst fractures treated between July 1992 and April 2005 were reviewed. There were 45 males, and 18 females, and their levels of involvement are shown in Fig. 1. Neurological status was assessed using the Frankel motor score system. 14 For ease of statistical analysis, the Frankel grade was converted into a numerical score in which A is equal to 1 (complete motor and sensory paralysis below the lesion), B is 2 (complete motor paralysis but some residual sensory perception), C is 3 (residual motor function but not of practical usefulness to the patient), D is 4 (useful but subnormal motor function below the lesion), and E is 5 (normal motor and sensory function). Results are expressed as the means the standard deviations. On admission all patients underwent plain (AP and lateral) supine radiographs in CT and MR imaging. Spinal angulation was determined by evaluating lateral radiographs on which we measured the angle of intersection of the adjacent intact endplates rostral and caudal to the fracture. The AP canal diameter at the fracture site was measured on CT scans and it was expressed as a percentage of the average normal canal above and below the fracture site. Surgery was performed when the patient s condition (related to other injuries) was deemed stable, and when there was neurological dysfunction or persistent pain associated with retropulsion of bone into the canal. Regardless of which approach was used, the intent of surgery was to decompress the canal, correct the kyphosis, and stabilize the spine. Posterior Approach Until 1998, the posterior route was the predominant approach; thereafter this approach was performed in only four of 25 patients. This approach was undertaken in 19 men and six women whose mean age was years (range years) (Fig. 2). The period between admission and surgery was 4 3 days (range 0 14 days). Pedicle screws were used in 18 patients, both PSs and hooks in six, and hooks alone in one. Decompression was achieved through a laminectomy and disimpaction in 10 patients, a transpedicular or transfacet approach in eight, and ligamentotaxis in seven. For fusion, bone harvested from the decompression site or iliac crest autograft augmented with demineralized bone matrix was used. Anterolateral Approach From 1998 onward, the anterolateral flank approach was favored; in only five of 38 patients had this approach been used prior to To avoid injury to the vena cava, the anterolateral approach was performed on the patient s left side and with the patient in the decubitus position. 17,24 Of the 38 patients in this group, 26 were men and 12 were woman whose mean age was years (range years) (Fig. 3). The mean period between admission and surgery was 6 12 days (range 0 20 days in all, but one patient in whom surgery was performed 73 days after admission because multiple injuries prevented earlier surgery). Stackable CFCs (DePuy Spine, Raynham, MA) were placed in 17 patients, allograft in 15, iliac crest autograft in four, and a telescoping titanium cylinder (Vertispan; Medtronic Sofamor-Danek, Memphis, TN) in two. Femoral allografts and synthetic anterior strut grafts were packed with autograft from the corpectomy site and augmented with autogenous rib. Grafts were impacted under distraction and held in place under compression. Lateral instrumentation involved the implantation of dual rods and screws in 31 patients (Antares [Medtronic Sofamor- FIG. 1. Bar graph showing the distribution of thoracolumbar burst fractures by level in both anterior and posterior surgical groups. 118
3 Approaches to thoracolumbar burst fractures FIG. 2. The posterior approach. Studies obtained in a 47-year-old man who fell off a grain truck and sustained an L-1 burst fracture. He was neurologically intact but complained of back and hip pain. A: Plain lateral radiograph revealing significant VB height loss and canal compromise. B: Axial CT scan showing canal narrowing, retropulsion of bone, and increase in interpedicular distance. C: Sagittal T 2 -weighted MR image demonstrating cauda equina compression. Three days following his injury, the patient underwent placement of posterior instrumentation comprising PSs, hooks, and an iliac crest graft. D and E: Five-year follow-up plain AP (D) and lateral (E) radiographs showing a solid fusion at T-12, L-1, and L-2. The rostral hooks are dislodged but stable. The patient remains neurologically intact but is disabled from pain. Danek, Memphis, TN]; or Kaneda [Depuy Spine]), and plates and screws in seven (Profile [DePuy Spine]; anterior thoracolumbar locking plate system [ATLP; Synthes Spine, Paoli, PA]; or Z-plate [Medtronic Sofamor-Danek]). One patient with a T-12 burst fracture, T11 12 dislocation, and paraplegia required contemporaneous anterior posterior instrumentation. Follow-Up Data Patients were mobilized gradually after surgery while wearing lumbar orthoses. A portable lateral radiographic system was used to obtain x-ray films, first at 45 angles and then upright or standing at 90. Braces were generally worn for 3 months postoperatively. Follow-up examinations, including standing or upright AP and lateral radiography, were scheduled at 1.5, 3, 6, and 12 months and annually thereafter. The mean clinical follow-up period after discharge was 1.8 years (range years). All patients were sent the Rand SF-36 questionnaire. The completed forms were received from 1.5 to 12 years (mean
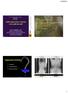
4 P. W. Hitchon, et al. FIG. 3. The anterolateral approach. Studies obtained in a 47-year-old man who fell off a horse and sustained an L-2 burst fracture. A: Plain lateral radiograph showing loss in VB height and retropulsion of bone into the canal. B: Axial CT scan obtained through the fracture showing the compromised canal with a 40% residual AP dimension. C: Sagittal T 2 -weighted MR image demonstrating retropulsion of bone and the compromised canal. D and E: To decompress the canal, a left-sided flank approach was selected for an L-2 corpectomy, anterior CFCs containing autologous strut graft, and lateral dual rod screw fixation, as seen in the AP (D) and lateral (E) projections. Angulation was corrected from 0 on admission to months after surgery. years) after surgery. The responses were grouped into eight categories: physical functioning (the mean of Questions 3 12), limitations due to physical health (the mean of Questions 13 16), limitations due to emotional health (the mean of Questions 17 19), energy/fatigue (the mean of Questions 23 31), emotional well-being (the mean of Questions 24 30), social functioning (the mean of Questions 20 and 32), pain (the mean of Questions 21 and 22), and general health (the mean of Questions 1 and 33 36). Statistical Analysis Data were analyzed using analysis of variance, the Wilcoxon test, and the Fisher exact test. Significance was accepted at a probability value of less than or equal to Results Clinical and Radiographic Parameters Preoperative and postoperative neurological status, represented by Frankel scores, is summarized in Table 1. The mean preoperative Frankel scores in the anterior and posterior groups were and , respectively (p = ). Preoperative angular deformity in the anterior and posterior groups measured and , re- 120
5 Approaches to thoracolumbar burst fractures TABLE 1 Summary of pre- and postoperative neurological changes in patients who underwent either anterior or posterior surgery Preop Postop Frankel Grade (score) Frankel No. of Grade (score) Patients A (1) B (2) C (3) D (4) E (5) anterior op A (1) B (2) C (3) D (4) E (5) 9 9 total 38 posterior op A (1) B (2) C (3) D (4) E (5) 8 8 total 25 spectively (p = ) (Fig. 4). Preoperative CT scanning demonstrated that the residual canal at the fracture site averaged % in the anterior group and % in the posterior group (p = 0.708), whereas postoperatively angular deformity had been corrected to and in the anterior and posterior groups, respectively (p = 0.565). Patients in the anterior group underwent follow-up examination for a mean of years, whereas those in the posterior group underwent follow up for a mean of years. This disparity reflects the fact that most anterior approaches have been undertaken since 1998, whereas most posterior approaches were performed prior to The follow-up Frankel scores for both groups are presented in Table 1. There was a trend for improvement in each treatment group, with the mean Frankel scores improving to (mean change 0.5) and (mean change 0.5) in the anterior (p = 0.461) and posterior (p = 0.676) groups, respectively (Fig. 5). The improvement of the Frankel scores, however, was significant in each group anterolateral (p = ) and posterior (p = 0.004). In only one case was there a worsening of neurological status reflected by a decrease in Frankel score from 2 to 1 in a 2-day period prior to surgery, necessitating urgent surgery. Otherwise all patients underwent surgery as soon as was feasible and as soon as medical stabilization had been achieved. There was no case of surgery-induced clinical deterioration. At the latest follow-up examination, angular deformity had progressed to in the anterolateral group and to in the posterior group (p = 0.024) (Fig. 4). Compared with the extent of angulation on admission, it had decreased by in the anterolateral group and had increased by in the posterior group (p ). The postadmission changes in angulation were significant in both groups anterolateral (p 0.001) and posterior (p = ). Although angulation progressed regardless of the approach taken, at the latest follow up there was no indication that a solid fusion was absent. Fusion was confirmed by the presence of bridging bone across the fracture on plain radiographs or the absence of motion on lateral flexion extension standing radiographs when fusion status was uncertain. Eighteen patients in the posterior group and 22 in the anterior responded to the SF-36 questionnaire, for a response rate of 72 and 58%, respectively. Two patients in the anterior group and one in the posterior group are now deceased. Three patients in the anterior group refused to answer the questionnaire. Two patients in the posterior group provided incomplete returns and their responses were discounted. Except for health and emotional limitations, responses appeared slightly higher in the anterolateral group compared with the posterior in the remaining categories (Fig. 6). The differences between the two groups did not achieve significance in any category. Summary of Complications There were two patients in the anterior group in whom the construct failed and necessitated repeated surgery; thus, the failure rate was 5%. In a 37-year-old man with paraparesis and a plate-treated L-1 fracture, the femoral allograft migrated into the canal after the patient was mobilized. This was attributed to a three-column injury that had gone unnoticed. Eight days later, he underwent the placement of posterior PS instrumentation and adjustment of his strut graft. The second complication occurred in a 49-year-old man with an L-2 fracture who had undergone anterior surgery involving the placement of a strut graft (femoral allograft) and dual rod screw instrumentation. Postoperatively, angulation increased due to the small size of the graft and its posterior location. Revision surgery was undertaken 11 days later and the femoral allograft was replaced with a large, stackable CFC and reinforced with posterior PSs. FIG. 4. Bar graph showing deformity angles at admission, discharge, and latest follow up in the anterior (black bars) and posterior (white bars) instrumentation groups. Values on the y axis reflect degrees. The asterisks denote statistical significance (p 0.05). 121
6 P. W. Hitchon, et al. group that ultimately required removal of the hardware 6 months postoperatively after failure to eradicate the persistent Staphylococcus aureus infection. FIG. 5. Bar graph showing preoperative and follow-up Frankel scores (y axis). At follow up, improvement in Frankel scores is noted irrespective of the approach (p 0.05). The difference in Frankel scores between the two groups is not significant on admission or at follow up; however, the improvement in the Frankel score was significant within each group anterolateral (p = ; black bars) and posterior (p = 0.004; white bars). There were five patients in the posterior group in whom we noted postoperative complications for a complication rate of 20%. Four patients required revision, and in one patient an infection necessitated the removal of the hardware. The difference in complication rates between the anterior and posterior groups, however, was not significant (p = 0.097, Fisher exact test). A 27-year-old woman with an L-1 fracture and a Frankel score of 4, was treated with posterior decompression, and the implantation of L2 3 PSs and a T-11 claw-hook construct. Postoperatively, the rostral hooks became disengaged and caused progressive angulation. Three months later we undertook revision surgery that involved the replacement of the hooks with screws; angulation improved thereafter. A second patient (a 52-year-old man with an L-1 burst fracture) was treated with posterior decompression and PS fixation at T-11, T-12, L-2, and L-3. Two days later revision was undertaken to replace screws whose trajectories had traversed the disc spaces. A third patient (a 36-year-old man with an L-1 burst fracture and paraplegia) underwent initial surgery in which PSs were placed at L-1 and L-2 and claw hooks were inserted across T-10 and T-11. This construct failed and required revision at an outside institution 6 weeks later, when L1 3 screws were placed, and claw hooks were implanted across the T3 4, T6 7, and T9 10 segments. Because this procedure was a revision surgery, we would have implanted a longer-length construct than the original extending at least four levels rostrally, but not necessarily to the T3 4 level. The fourth complication occurred in 64-year-old man with paraparesis and an L-1 burst fracture who had undergone T12 L2 PS fixation. During the following year, progressive angulation and pain developed after the T-12 screws fractured bilaterally. The patient has undergone conservative treatment thus far. There was one case of wound infection in the posterior Economic Impact The duration of hospitalization from admission to discharge in the anterior group was days and that in the posterior group was days (p = 0.444). This difference is less a reflection of the technique than of the efficiency in recent years of transferring patients to rehabilitation. To compare costs, the expenses incurred by the last 10 patients who underwent posterior surgery between May 1997 and May 2002 were compared with those incurred by nine patients who underwent anterior surgery between January 1998 and January The mean operating times between entering and exiting the operating room were and minutes for posterior and anterior groups, respectively (p = 0.823). Operating room expenses for supplies and expendables were $ and $ for the posterior and anterior groups, respectively (p = 0.53). The implant cost averaged $ for posterior instrumentation and $ for anterior instrumentation (p = 0.269). The mean total of the surgeon s fees was $18, for posterior surgery, whereas it was $27, for anterior surgery (p = ). Total hospital charges collected were $80,040 32,535 for posterior surgery and $89,090 27,340 for anterior surgery (p = 0.523) (Fig. 7). Discussion In the posterior group, angulation decreased only 0.7 between admission and discharge, whereas it progressed to at the final follow-up examination (Fig. 4). In the anterior group, however, angulation was corrected by 9.9 between admission and discharge, and the correction persisted at at follow up. At the follow-up evaluation, the angulation in the posterior group was significantly greater than that in the anterior group (p = 0.024). The anterior approach allows removal of retropulsed bone from the canal under direct vision as well as reconstruction of the anterior column with a strut graft. This approach protects the integrity of the posterior column and is associated with a sustained correction of angular deformity. 12,20,24 Anterior graft materials have included autografts, 6,28 allografts, 4,13,22,29 titanium mesh cages, 10,11 and stackable CFCs. 3,24 We favor CFCs because they can be easily stacked to span the corpectomy defect and, with appropriate instruments and fluoroscopic guidance, can be impacted easily into place. These cages are available in different sizes, allowing adaptation to the adjacent endplates. The largest endplate is selected to reduce the incidence of subsidence and telescoping of the graft within the VBs adjacent to the fracture. Complications necessitating repeated operation occurred in five patients (20%) in the posterior group. Two of these five complications involved hooks. Posterior approaches in cases of burst fractures may entail laminotomy or laminectomy, as well as sacrifice of the facet joint on at least one side, if disimpaction of the canal is to be undertaken. This complication rate associated with poste- 122
7 Approaches to thoracolumbar burst fractures FIG. 6. Bar graph illustrating the distribution of mean SF-36 scores obtained in 22 patients who underwent anterolateral surgery (black bars) and 18 patients who underwent posterior surgery (white bars). No significant intergroup difference in scores is noted. rior instrumentation has been underscored by other published data. In one series of 70 patients with thoracic and lumbar fractures, 25% of the screws adjacent to the fracture bent or broke, and in four patients hardware was removed for pain or when it became prominent -that is, when it could be felt through the skin. 26 Alvine and colleagues 1 also used PS fixation in the treatment of 41 thoracolumbar fractures from T-11 to L-5. In their study, implant breakage occurred in 16 (39%) of the 41 fractures. In seven cases the implant breakages necessitated repeated surgery. In the retrospective review of thoracolumbar fractures conducted by Danisa and associates, 7 however, posterior instrumentation was shown to be safe, simple, and cost effective in 27 patients compared with anterior surgery in 16 patients. Two (5%) of our 38 patients treated with the anterolateral approach required repeated surgery that involved posterior instrumentation-augmented fusion. The rates of repeated operation in the anterolateral and posterior groups were not significantly different (p = 0.097). In the 150 cases reported by Kaneda, et al., 20 there were 10 cases (7%) of pseudarthrosis necessitating posterior instrumentation and fusion. McAfee 24 reported on complications associated with the anterior approach when used in patients with thoracolumbar fractures undergoing decompression and stabilization with various implants. The failure rate was only 6% (two of 35 implants) in cases in which the Kaneda dual rod screw construct was used. The anterior approach in patients with VB fractures requires fixation of only one level rostral and caudal to the fractured VB, whereas in the posterior approach instrumentation may span five or more levels where the anterior column has been disrupted with secondary deformity. To optimize fusion, bone grafts are better maintained under compression, and this is achieved more effectively by using an anterior approach and the insertion of dual rods and bicortical screws. 20,24,25 The authors of in vitro biomechanical tests in cadaveric spines have shown that the stiffness of the construct (that is, that afforded by the spine and the implant combined) was attributable to many factors, including the constraint of the screws to the plate or rods, the bicortical engagement of the screws, and the ability of these devices to compress the graft between the vertebral endplates. 17 Furthermore, although surgeons fees for the anterior approach were nearly $10,000 higher, our cost analysis showed no significant difference between the two approaches in the duration of the procedure, cost of the implant, or overall hospital charges. Analysis of our results and those of others demonstrates that several parameters need to be examined prior to the selection of treatment options. Rather than being random, this selection should be based on clinical and radiological criteria including neurological deficit, pain, deformity angulation, residual canal diameter, and VB height. 2,19,31 In flexion compression fractures in which the anterior column alone is affected by loss of height but not canal compromise, 8,16 surgery is generally not needed. For patients with burst fractures who are neurologically intact, in whom angular deformity is less than 20, and in whom the residual spinal canal is greater than 50% of normal, nonoperative treatment is sufficient. 5,9,18,19,30,32 35 Surgery is undertaken when neurological deficits either complete or incomplete and persistent pain are present. If the fractured VB is sufficiently preserved to provide some load sharing, then posterior instrumentation may be sufficient. 31 When significant fragmentation of the VB exists and there is poor apposition of the fragments and loss in height, 31 anterior grafts and instrumentation are necessary. Neurological improvement was documented in our patients regardless of which approach was used (Tables 1 and 2; Fig. 5); the same was shown in the Scoliosis Research Society Multicenter Spine Fracture Study. 15 In the latter, functional recovery at 2 years in patients in whom either an anterior and posterior approach was used was shown to be comparable when using the Frankel or motor score grading system. When using the Manabe 123
8 guidelines for the treatment of these fractures were absent and suggested that, for a better comparison of surgical techniques, randomized controlled trials were necessary. We agree with their conclusions but recognize, as others do, the advantages of the anterior approach. 1 Conclusions P. W. Hitchon, et al. Our results and those of others demonstrate that angular deformity is more successfully corrected and maintained, and fewer spinal segments are immobilized, when using the anterior approach. In cases of burst fractures in which neurological deficit and angular deformity are present, the anterior approach with anterior-column reconstruction appears to be advantageous. 12,15 The supplementation of an anterior construct with posterior instrumentation is generally unnecessary, but it may be indicated in unique cases in which there are two adjacent VB fractures or three-column injuries. FIG. 7. Bar graph showing operating room charges, surgeon s fee, implant cost, and total hospital charges. Asterisk indicates statistically significant difference. Black bars = anterior surgery; white bars = posterior surgery. Scale, which incorporates neurological function and pain, 23 however, significantly greater improvement was documented in 183 patients in whom the anterior approach was used (p , chi-square test) than in the 163 individuals in whom the posterior route was used. Additionally, unsatisfactory results at 1 year appeared more prevalent in patients treated with a posterior approach. In our study, Rand SF-36 scores in the anterior group were slightly higher than those in the posterior group, but statistical significance in any category was not achieved. Higher scores in the anterior group were in part a reflection of the shorter-length instrumentation, lower rate of repeated operation, and sustained deformity correction. Currently, guidelines based on randomized trials for the treatment of thoracolumbar burst fractures are unavailable. 37 Verlaan, et al., 37 conducted a literature review of 132 papers, involving 5748 patients with thoracic and lumbar fractures treated with posterior, anterior, or combined approaches. They concluded that evidence-based Acknowledgments We thank Marge Rogers, R.N., Melanie Frees, B.S.N., Hayan Dayoub, M.D., and Arnold Entame, M.D., for their help in data collection and in the preparation of this manuscript. References 1. Alvine GF, Swain JM, Asher MA, Burton DC: Treatment of thoracolumbar burst fractures with variable screw placement or Isola instrumentation and arthrodesis: case series and literature review. J Spinal Disord Tech 17: , Bohlman HH: Treatment of fractures and dislocations of the thoracic and lumbar spine. J Bone Joint Surg Am 67: , Boriani S, Biagini R, Bandiera S, Gasbarrini A, De Lure F: Reconstruction of the anterior column of the thoracic and lumbar spine with a carbon fiber stackable cage system. Orthopedics 25:37 42, Bridwell KH, Lenke LG, McEnery KW, Baldus C, Blanke K: Anterior fresh frozen structural allografts in the thoracic and lumbar spine. Do they work if combined with posterior fusion and instrumentation in adult patients with kyphosis or anterior column defects? Spine 20: , Cantor JB, Lebwohl NH, Garvey T, Eismont FJ: Nonoperative management of stable thoracolumbar burst fractures with early ambulation and bracing. Spine 18: , Cotler HB, Cotler JM, Stoloff A, Cohn HE, Jerrell BE, Martinez L, et al: The use of autografts for vertebral body replacement of the thoracic and lumbar spine. Spine 10: , 1985 TABLE 2 Summary of SF-36 scores obtained in patients undergoing anterior and posterior surgery for thoracolumbar burst fractures No. of Physical Health Emotional Energy/ Emotional Social General Group Cases Function Limitations Limitations Fatigue Well-Being Function Pain Health anterior* posterior* p value * Values are presented as the means standard deviations. 124
9 Approaches to thoracolumbar burst fractures 7. Danisa OA, Shaffrey CI, Jane JA, Whitehill R, Wang GW, Szabo TA, et al: Surgical approaches for the correction of unstable thoracolumbar burst fractures: a retrospective analysis of treatment outcomes. J Neurosurg 83: , Denis F: The three column spine and its significance in the classification of acute thoracolumbar spinal injuries. Spine 8: , Domenicucci M, Preite R, Ramieri A, Ciapetta P, Delfini R, Romanini L: Thoracolumbar fractures without neurosurgical involvement: surgical or conservative treatment. J Neurosurg Sci 40:1 10, Dvorak MF, Kwon BK, Fisher CG, Eiserloh HL III, Boyd M, Wing PC: Effectiveness of titanium mesh cylindrical cages in anterior column reconstruction after thoracic and lumbar vertebral body resection. Spine 28: , Eck KR, Bridwell KH, Ungacta FF, Lapp MA, Lenke LG, Riew KD: Analysis of titanium mesh cages in adults with minimum two-year follow-up. Spine 25: , Esses SI, Botsford DJ, Kostuik JP: Evaluation of surgical treatment for burst fractures. Spine 15: , Finkelstein JA, Chapman JR, Mirza S: Anterior cortical allograft in thoracolumbar fractures. J Spinal Disord 12: , Frankel HL, Hancock DO, Hyslop G, Melzack J, Michaelis LS, Ungar GH, et al: The value of postural reduction in the initial management of closed injuries of the spine with paraplegia and tetraplegia. I. Paraplegia 7: , Gertzbein SD: Scoliosis Research Society: multicenter spine fracture study. Spine 17: , Gertzbein SD: Spine update. Classification of thoracic and lumbar fractures. Spine 19: , Hitchon PW, Goel VK, Rogge TN, Torner JC, Dooris AP, Drake JS, et al: In vitro biomechanical analysis of three anterior thoracolumbar implants. J Neurosurg 93 (2 Suppl): , Hitchon PW, Torner JC: Recumbency in thoracolumbar fractures. Neurosurg Clin N Am 8: , Hitchon PW, Torner JC, Haddad SF, Follett KA: Management options in thoracolumbar burst fractures. Surg Neurol 49: , Kaneda K, Taneichi H, Abumi K, Hashimoto T, Satoh S, Fujiya M: Anterior decompression and stabilization with the Kaneda device for thoracolumbar burst fractures associated with neurological deficits. J Bone Joint Surg Am 79:69 83, Lemons VR, Wagner FC, Montesano PX: Management of thoracolumbar fractures with accompanying neurological injury. Neurosurgery 30: , Lewandrowski K, Hecht AC, DeLaney TF, Chapman PA, Hornicek FJ, Pedlow FX: Anterior spinal arthrodesis with structural cortical allografts and instrumentation for spine tumor surgery. Spine 29: , Manabe S, Tateishi A, Abe M, Ohno T: Surgical treatment of metastatic tumors of the spine. Spine 14:41 47, McAfee PC: Complications of anterior approaches to the thoracolumbar spine. Emphasis on Kaneda instrumentation. Clin Orthop Relat Res 306: , McAfee PC, Bohlman HH, Yuan HA: Anterior decompression of traumatic thoracolumbar fractures with incomplete neurological deficit using a retroperitoneal approach. J Bone Joint Surg Am 67:89 104, McLain RF: Functional outcomes after surgery for spinal fractures: return to work and activity. Spine 29: , McLain RF, Burkus JK, Benson DR: Segmental instrumentation for thoracic and thoracolumbar fractures: prospective analysis of construct survival and 5 year follow-up. Spine J 1: , Meding JB, Stambough JL: Critical analysis of strut grafts in anterior spinal fusions. J Spinal Disord 6: , Molinari RW, Bridwell KH, Klepps SJ, Baldus C: Minimum 5- year follow-up of anterior column structural allografts in the thoracic and lumbar spine. Spine 23: , Mumford J, Weinstein JN, Spratt KF, Goel VK: Thoracolumbar burst fractures. The clinical efficacy and outcome of nonoperative management. Spine 18: , Parker JW, Lane JR, Karaikovic EE, Gaines RW: Successful short-segment instrumentation and fusion for thoracolumbar spine fractures: a consecutive 4 1 / 2 year series. Spine 25: , Rechtine GR II, Cahill D, Chrin AM: Treatment of thoracolumbar trauma: comparison of complications of operative versus nonoperative treatment. J Spinal Disord 12: , Reid DC, Hu R, Davis LA, Saboe LA: The nonoperative treatment of burst fractures of the thoracolumbar junction. J Trauma 28: , Seybold EA, Sweeney CA, Fredrickson BE, Warhold LG, Bernini PM: Functional outcome of low lumbar burst fractures. A multicenter review of operative and nonoperative treatment of L3-l5. Spine 24: , Shen WJ, Liu TJ, Shen YS: Nonoperative treatment versus posterior fixation for thoracolumbar junction burst fractures without neurologic deficits. Spine 26: , Stephens GC, Devito DP, McNamara MJ: Segmental fixation of lumbar burst fractures with Cotrel-Dubousset instrumentation. J Spinal Disord 5: , Verlaan JJ, Diekerhof CH, Buskens E, van der Tweel I, Verbout AJ, Dhert WJ, et al: Surgical treatment of traumatic fractures of the thoracic and lumbar spine: a systematic review of the literature on techniques, complications, and outcome. Spine 29: , 2004 Manuscript received December 9, Accepted in final form May 8, Address reprint requests to: Patrick W. Hitchon, M.D., Department of Neurosurgery, University of Iowa Hospitals and Clinics, 200 Hawkins Drive, Iowa City, Iowa patrick-hitchon@uiowa.edu. 125
Although unstable thoracolumbar injuries are a common
 ORIGINAL ARTICLE Anterior-Only Stabilization of Three-Column Thoracolumbar Injuries Rick C. Sasso, MD, Natalie M. Best, BS, Thomas M. Reilly, MD, and Robert A. McGuire, Jr., MD Objective: The optimal treatment
ORIGINAL ARTICLE Anterior-Only Stabilization of Three-Column Thoracolumbar Injuries Rick C. Sasso, MD, Natalie M. Best, BS, Thomas M. Reilly, MD, and Robert A. McGuire, Jr., MD Objective: The optimal treatment
Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life
 Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Short segment pedicle screw fixation for unstable T11-L2 fractures : with or without fusion? A three-year follow-up study
 Acta Orthop. Belg., 2009, 75, 822-827 ORIGINAL STUDY Short segment pedicle screw fixation for unstable T11-L2 fractures : with or without fusion? A three-year follow-up study Jin-Ho HWANG, Hitesh N. MODI,
Acta Orthop. Belg., 2009, 75, 822-827 ORIGINAL STUDY Short segment pedicle screw fixation for unstable T11-L2 fractures : with or without fusion? A three-year follow-up study Jin-Ho HWANG, Hitesh N. MODI,
Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia: A Case Series
 C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture: Severe Canal Compromise but Neurologically Intact Cases
 CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Treatment of thoracolumbar burst fractures by vertebral shortening
 Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Original Article Clinics in Orthopedic Surgery 2016;8:
 Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Advantages of MISS. Disclosures. Thoracolumbar Trauma: Minimally Invasive Techniques. Minimal Invasive Spine Surgery 11/8/2013.
 3 rd Annual UCSF Techniques in Complex Spine Surgery Program Thoracolumbar Trauma: Minimally Invasive Techniques Research Support: Stryker Disclosures Murat Pekmezci, MD Assistant Clinical Professor UCSF/SFGH
3 rd Annual UCSF Techniques in Complex Spine Surgery Program Thoracolumbar Trauma: Minimally Invasive Techniques Research Support: Stryker Disclosures Murat Pekmezci, MD Assistant Clinical Professor UCSF/SFGH
CLINICAL ARTICLE. Page 68 / SA ORTHOPAEDIC JOURNAL Winter 2009
 Page 68 / SA ORTHOPAEDIC JOURNAL Winter 2009 C L I N I C A L A RT I C L E Short-segment posterior instrumentation of thoracolumbar fractures as standalone treatment J Davis, Registrar, Department of Orthopaedics,
Page 68 / SA ORTHOPAEDIC JOURNAL Winter 2009 C L I N I C A L A RT I C L E Short-segment posterior instrumentation of thoracolumbar fractures as standalone treatment J Davis, Registrar, Department of Orthopaedics,
The Neurologic Outcome Of Posterior Fixation Of Thoraco- Lumbar Spine Fractures In A Rural Tertiary Care Centre Without Help Of Image Intensifier
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 4, Issue 6 (Jan.- Feb. 2013), PP 36-40 The Neurologic Outcome Of Posterior Fixation Of Thoraco- Lumbar
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 4, Issue 6 (Jan.- Feb. 2013), PP 36-40 The Neurologic Outcome Of Posterior Fixation Of Thoraco- Lumbar
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Classification? Classification system should be: Comprehensive Usable Accurate Predictable Able to guide intervention
 Moderator: Dr. P.S. Chandra Dr. Dr Deepak Gupta Classification? Classification system should be: Comprehensive Usable Accurate Predictable Able to guide intervention A precise, comprehensive, ideal
Moderator: Dr. P.S. Chandra Dr. Dr Deepak Gupta Classification? Classification system should be: Comprehensive Usable Accurate Predictable Able to guide intervention A precise, comprehensive, ideal
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
SHORT SEGMENT FIXATION THORACOLUMBAR UNSTABLE BURST FRACTURES USING DC PLATES & PEDICLE SCREWS
 STUDY SHORT SEGMENT FIXATION THORACOLUMBAR UNSTABLE BURST FRACTURES USING DC PLATES & PEDICLE SCREWS *Hashem, N.; **A Subai, N. *Faculty of Medicine, Ains Shams University, Egypt ^Department of Orthopedics,
STUDY SHORT SEGMENT FIXATION THORACOLUMBAR UNSTABLE BURST FRACTURES USING DC PLATES & PEDICLE SCREWS *Hashem, N.; **A Subai, N. *Faculty of Medicine, Ains Shams University, Egypt ^Department of Orthopedics,
INTRODUCTION.
 www.jkns.or.kr http://dx.doi.org/1.334/jkns.212.51.4.23 J Korean Neurosurg Soc 51 : 23-27, 212 Print ISSN 25-3711 On-line ISSN 1598-7876 Copyright 212 The Korean Neurosurgical Society Clinical Article
www.jkns.or.kr http://dx.doi.org/1.334/jkns.212.51.4.23 J Korean Neurosurg Soc 51 : 23-27, 212 Print ISSN 25-3711 On-line ISSN 1598-7876 Copyright 212 The Korean Neurosurgical Society Clinical Article
Postero-lateral approach with open view vertebroplasty - eggshell technique
 Romanian Neurosurgery (2013) XX 4: 357-368 357 Postero-lateral approach with open view vertebroplasty - eggshell technique E.Fl. Exergian 1, I.Fl. Luca-Husti 2, D. Şerban 1 1 Spine Surgery Department,
Romanian Neurosurgery (2013) XX 4: 357-368 357 Postero-lateral approach with open view vertebroplasty - eggshell technique E.Fl. Exergian 1, I.Fl. Luca-Husti 2, D. Şerban 1 1 Spine Surgery Department,
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Spinal Cord (2011) 49, & 2011 International Spinal Cord Society All rights reserved /11 $
 (2011) 49, 573 579 & 2011 International Society All rights reserved 1362-4393/11 $32.00 www.nature.com/sc ORIGINAL ARTICLE Posterior/anterior combined surgery for thoracolumbar burst fracturesfposterior
(2011) 49, 573 579 & 2011 International Society All rights reserved 1362-4393/11 $32.00 www.nature.com/sc ORIGINAL ARTICLE Posterior/anterior combined surgery for thoracolumbar burst fracturesfposterior
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
ASJ. Study of Vertebral Body Replacement with Reconstruction Spinal Cages in Dorsolumbar Traumatic and Koch s Spine. Asian Spine Journal.
 Asian Spine Journal 786 Rohit Anilbhai Clinical Thaker Studyet al. http://dx.doi.org/10.4184/asj.2014.8.6.786 Study of Vertebral Body Replacement with Reconstruction Spinal Cages in Dorsolumbar Traumatic
Asian Spine Journal 786 Rohit Anilbhai Clinical Thaker Studyet al. http://dx.doi.org/10.4184/asj.2014.8.6.786 Study of Vertebral Body Replacement with Reconstruction Spinal Cages in Dorsolumbar Traumatic
Posterior Instrumentation of Thoracolumbar Fracture
 Posterior Instrumentation of Thoracolumbar Fracture Jin-Young Lee, MD, and Gab-Lae Kim, MD Department of Orthopedic Surgery, Hallym University College of Medicine, Seoul, Korea Abstract The thoracolumbar
Posterior Instrumentation of Thoracolumbar Fracture Jin-Young Lee, MD, and Gab-Lae Kim, MD Department of Orthopedic Surgery, Hallym University College of Medicine, Seoul, Korea Abstract The thoracolumbar
Anterior Corpectomy with Expandable Titanium Cages for Thoraco Lumbar Fractures Audrey Paulzak, MD Pat O'Brien, BS W. George Rusyniak, MD Anthony
 Anterior Corpectomy with Expandable Titanium Cages for Thoraco Lumbar Fractures Audrey Paulzak, MD Pat O'Brien, BS W. George Rusyniak, MD Anthony Martino, MD University of South Alabama, Department of
Anterior Corpectomy with Expandable Titanium Cages for Thoraco Lumbar Fractures Audrey Paulzak, MD Pat O'Brien, BS W. George Rusyniak, MD Anthony Martino, MD University of South Alabama, Department of
Comparison of clinical, radiological and functional outcome of short segment V/S long segment posterior fixation of tuberculosis of spine
 2018; 2(4): 104-108 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(4): 104-108 Received: 20-08-2018 Accepted: 21-09-2018 Dr. Mitul Mistry Assistant Professor,
2018; 2(4): 104-108 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(4): 104-108 Received: 20-08-2018 Accepted: 21-09-2018 Dr. Mitul Mistry Assistant Professor,
Synex System TECHNIQUE GUIDE. An expandable vertebral body replacement device
 Synex System TECHNIQUE GUIDE An expandable vertebral body replacement device Original Instruments and Implants of the Association for the Study of Internal Fixation AO ASIF Synex System Overview The Synex
Synex System TECHNIQUE GUIDE An expandable vertebral body replacement device Original Instruments and Implants of the Association for the Study of Internal Fixation AO ASIF Synex System Overview The Synex
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
FUNCTIONAL OUTCOMES OF TRAUMATIC PARAPLEGIA PATIENTS: DOES SURGERY IMPROVE THE QUALITY OF LIFE?
 FUNCTIONAL OUTCOMES OF TRAUMATIC PARAPLEGIA PATIENTS: DOES SURGERY IMPROVE THE QUALITY OF LIFE? Original Article Orthopaedics R S Bajoria 1, Mahendra Panwar 2, Anand Rao 3, Sameer Gupta 4 1 - Associate
FUNCTIONAL OUTCOMES OF TRAUMATIC PARAPLEGIA PATIENTS: DOES SURGERY IMPROVE THE QUALITY OF LIFE? Original Article Orthopaedics R S Bajoria 1, Mahendra Panwar 2, Anand Rao 3, Sameer Gupta 4 1 - Associate
Dynamic anterior cervical plating for multi-level spondylosis: Does it help?
 Original research Dynamic anterior cervical plating for multi-level spondylosis: Does it help? 41 41 46 Dynamic anterior cervical plating for multi-level spondylosis: Does it help? Authors Ashraf A Ragab,
Original research Dynamic anterior cervical plating for multi-level spondylosis: Does it help? 41 41 46 Dynamic anterior cervical plating for multi-level spondylosis: Does it help? Authors Ashraf A Ragab,
Results of Two Above- One Below Approach with Intermediate Screws at the Fracture Site in the Surgical Treatment of Thoracolumbar Burst Fractures
 Kobe J. Med. Sci., Vol. 56 No2, pp. E67-E78 2010 Results of Two Above- One Below Approach with Intermediate Screws at the Fracture Site in the Surgical Treatment of Thoracolumbar Burst Fractures ONAT UZUMCUGIL
Kobe J. Med. Sci., Vol. 56 No2, pp. E67-E78 2010 Results of Two Above- One Below Approach with Intermediate Screws at the Fracture Site in the Surgical Treatment of Thoracolumbar Burst Fractures ONAT UZUMCUGIL
Thoracolumbar fractures. Treatment options. A long trip.
 Thoracolumbar fractures. Treatment options. A long trip. MIS SURGERY. WHY NOT? Murcia. October 5, 2012. Dr. Pedro Cortés García. Spinal Unit. Orthopaedic department. Canary Islands University Hospital
Thoracolumbar fractures. Treatment options. A long trip. MIS SURGERY. WHY NOT? Murcia. October 5, 2012. Dr. Pedro Cortés García. Spinal Unit. Orthopaedic department. Canary Islands University Hospital
Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
 Journal of Spinal Disorders & Techniques Vol. 16, No. 3, pp. 229 235 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
Journal of Spinal Disorders & Techniques Vol. 16, No. 3, pp. 229 235 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients
 Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Traumatic thoracic spinal fracture dislocation with minimal or no cord injury
 J Neurosurg (Spine 3) 96:333 337, 2002 Traumatic thoracic spinal fracture dislocation with minimal or no cord injury Report of four cases and review of the literature SCOTT SHAPIRO M.D., TODD ABEL, M.D.,
J Neurosurg (Spine 3) 96:333 337, 2002 Traumatic thoracic spinal fracture dislocation with minimal or no cord injury Report of four cases and review of the literature SCOTT SHAPIRO M.D., TODD ABEL, M.D.,
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Int J Clin Exp Med 2016;9(9): /ISSN: /IJCEM
 Int J Clin Exp Med 2016;9(9):17435-17441 www.ijcem.com /ISSN:1940-5901/IJCEM0028090 Original Article Comparison of posterior vertebral column resection and anterior corpectomy and instrumentation for correcting
Int J Clin Exp Med 2016;9(9):17435-17441 www.ijcem.com /ISSN:1940-5901/IJCEM0028090 Original Article Comparison of posterior vertebral column resection and anterior corpectomy and instrumentation for correcting
 www.chirurgieorthopedique.com www.chirurgieorthopedique.com www.chirurgieorthopedique.com Vertebral body cage use in thoracolumbar fractures: Outcomes in a prospective series of 23 cases at 2 years follow-up
www.chirurgieorthopedique.com www.chirurgieorthopedique.com www.chirurgieorthopedique.com Vertebral body cage use in thoracolumbar fractures: Outcomes in a prospective series of 23 cases at 2 years follow-up
Treatment Options for Thoracolumbar Spine Fractures
 & Treatment Options for Thoracolumbar Spine Fractures Eldin E. Karaiković¹*, Hector O. Pacheco² 1. Assistant Professor, Northwestern University, and Director of the Spine Center and Lead Physician, Orthopaedic
& Treatment Options for Thoracolumbar Spine Fractures Eldin E. Karaiković¹*, Hector O. Pacheco² 1. Assistant Professor, Northwestern University, and Director of the Spine Center and Lead Physician, Orthopaedic
Distraction injury to thoracic spine treated with thoracoscopic dual-rod fixation
 The Spine Journal 6 (2006) 330 334 Distraction injury to thoracic spine treated with thoracoscopic dual-rod fixation Gregory P. Lekovic, MD, PhD, JD, Eric M. Horn, MD, PhD, Curtis A. Dickman, MD* Division
The Spine Journal 6 (2006) 330 334 Distraction injury to thoracic spine treated with thoracoscopic dual-rod fixation Gregory P. Lekovic, MD, PhD, JD, Eric M. Horn, MD, PhD, Curtis A. Dickman, MD* Division
Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion and Posterior Instrumentation
 Original Paper Med Princ Pract 2003;12:92 96 DOI: 10.1159/000069113 Received: April 21, 2002 Revised: August 3, 2002 Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion
Original Paper Med Princ Pract 2003;12:92 96 DOI: 10.1159/000069113 Received: April 21, 2002 Revised: August 3, 2002 Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
of thoracolumbar burst fractures
 Clin Orthop Relat Res (2016) 474:619 624 / DOI 10.1007/s11999-015-4305-y Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons Published online: 23 April
Clin Orthop Relat Res (2016) 474:619 624 / DOI 10.1007/s11999-015-4305-y Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons Published online: 23 April
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit
 Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis
 J Child Orthop (2012) 6:137 143 DOI 10.1007/s11832-012-0400-8 ORIGINAL CLINICAL ARTICLE Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis Bradley P. Jaquith
J Child Orthop (2012) 6:137 143 DOI 10.1007/s11832-012-0400-8 ORIGINAL CLINICAL ARTICLE Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis Bradley P. Jaquith
Classification of Thoracolumbar Spine Injuries
 Classification of Thoracolumbar Spine Injuries Guillem Saló Bru 1 IMAS. Hospitals del Mar i de l Esperança. ICATME. Institut Universitari Dexeus USP. UNIVERSITAT AUTÒNOMA DE BARCELONA Objectives of classification
Classification of Thoracolumbar Spine Injuries Guillem Saló Bru 1 IMAS. Hospitals del Mar i de l Esperança. ICATME. Institut Universitari Dexeus USP. UNIVERSITAT AUTÒNOMA DE BARCELONA Objectives of classification
Dorsal Cervical Surgeries and Techniques
 Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Subaxial Cervical Spine Trauma Dr Hesarikia BUMS
 Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Combined Anterior-Posterior Surgery Versus Posterior Surgery for Thoracolumbar Burst Fractures: A Systematic Review of the Literature
 The Open Orthopaedics Journal, 2010, 4, 93-100 93 Open Access Combined Anterior-Posterior Surgery Versus Posterior Surgery for Thoracolumbar Burst Fractures: A Systematic Review of the Literature Pim P.
The Open Orthopaedics Journal, 2010, 4, 93-100 93 Open Access Combined Anterior-Posterior Surgery Versus Posterior Surgery for Thoracolumbar Burst Fractures: A Systematic Review of the Literature Pim P.
Thoracolumbar Spine Trauma: II. Principles of Management
 Thoracolumbar Spine Trauma: II. Principles of Management Jeffrey M. Spivak, MD, Alexander R. Vaccaro, MD, and Jerome M. Cotler, MD Abstract The care of patients with thoracolumbar spine trauma with or
Thoracolumbar Spine Trauma: II. Principles of Management Jeffrey M. Spivak, MD, Alexander R. Vaccaro, MD, and Jerome M. Cotler, MD Abstract The care of patients with thoracolumbar spine trauma with or
PARAPLEGIA. B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture.
 16 PARAPLEGIA A B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture. a grotesque deformity of the spine and trunk with
16 PARAPLEGIA A B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture. a grotesque deformity of the spine and trunk with
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D.
 J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
R A (2005)
 4, 2005 2, 3 1 J Sp inal Surg, February 2005, Vol 3, No 1,,,,,, 1999 3 2004 568 45, 23,14 61,36. 7 : T 11 1 T 12 20 L 1 33 L 2 12, L 1, 2 1L 2, 3 1 : 10, 58 : Z2PLATE43, PROF ILE19, ALPS6 : 45 23 Frankel
4, 2005 2, 3 1 J Sp inal Surg, February 2005, Vol 3, No 1,,,,,, 1999 3 2004 568 45, 23,14 61,36. 7 : T 11 1 T 12 20 L 1 33 L 2 12, L 1, 2 1L 2, 3 1 : 10, 58 : Z2PLATE43, PROF ILE19, ALPS6 : 45 23 Frankel
VLIFT System Overview. Vertebral Body Replacement System
 VLIFT System Overview Vertebral Body Replacement System VLIFT System System Description The VLIFT Vertebral Body Replacement System consists of a Distractible In Situ (DIS) implant, which enables the surgeon
VLIFT System Overview Vertebral Body Replacement System VLIFT System System Description The VLIFT Vertebral Body Replacement System consists of a Distractible In Situ (DIS) implant, which enables the surgeon
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Bone Cement-Augmented Short Segment Fixation with Percutaneous Screws for Thoracolumbar Burst Fractures Accompanied by Severe Osteoporosis
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2012.52.4.353 J Korean Neurosurg Soc 52 : 353-358, 2012 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2012 The Korean Neurosurgical Society Clinical
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2012.52.4.353 J Korean Neurosurg Soc 52 : 353-358, 2012 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2012 The Korean Neurosurgical Society Clinical
Fixation of Thoracolumbar Fractures by Fixator Internae
 Proceeding S.Z.P.G.M.I. Vol: 26(1): pp. 41-46, 2012. Fixation of Thoracolumbar Fractures by Fixator Internae Shafique Ahmed Shafaq, Abbas Bajwa and Zaigham Ali Department of Orthopaedics, Shaikh Zayed
Proceeding S.Z.P.G.M.I. Vol: 26(1): pp. 41-46, 2012. Fixation of Thoracolumbar Fractures by Fixator Internae Shafique Ahmed Shafaq, Abbas Bajwa and Zaigham Ali Department of Orthopaedics, Shaikh Zayed
Subaxial Cervical Spine Trauma. Introduction. Anatomic Considerations 7/23/2018
 Subaxial Cervical Spine Trauma Sheyan J. Armaghani, MD Florida Orthopedic Institute Assistant Professor USF Dept of Orthopedics Introduction Trauma to the cervical spine accounts for 5 of all spine injuries
Subaxial Cervical Spine Trauma Sheyan J. Armaghani, MD Florida Orthopedic Institute Assistant Professor USF Dept of Orthopedics Introduction Trauma to the cervical spine accounts for 5 of all spine injuries
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine.
 Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine. Technique Guide Instruments and implants approved by the AO Foundation
Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine. Technique Guide Instruments and implants approved by the AO Foundation
Adolescent Idiopathic Scoliosis
 Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Definitive single-stage posterior surgical correction of complete traumatic spondyloptosis at the thoracolumbar junction
 spine case report J Neurosurg Spine 22:653 657, 2015 Definitive single-stage posterior surgical correction of complete traumatic spondyloptosis at the thoracolumbar junction Lee Sandquist, DO, lexander
spine case report J Neurosurg Spine 22:653 657, 2015 Definitive single-stage posterior surgical correction of complete traumatic spondyloptosis at the thoracolumbar junction Lee Sandquist, DO, lexander
Successful Short-Segment Instrumentation and Fusion for Thoracolumbar Spine Fractures
 Successful Short-Segment Instrumentation and Fusion for Thoracolumbar Spine Fractures A Consecutive 4 1 2-Year Series Jeffrey W. Parker, MD, Joel R. Lane, MD, Eldin E. Karaikovic, MD, PhD, and Robert W.
Successful Short-Segment Instrumentation and Fusion for Thoracolumbar Spine Fractures A Consecutive 4 1 2-Year Series Jeffrey W. Parker, MD, Joel R. Lane, MD, Eldin E. Karaikovic, MD, PhD, and Robert W.
Asymmetric T5 Pedicle Subtraction Osteotomy (PSO) for complex posttraumatic deformity
 Eur Spine J (2013) 22:2130 2135 DOI 10.1007/s00586-013-2942-y OPEN OPERATING THEATRE (OOT) Asymmetric T5 Pedicle Subtraction Osteotomy (PSO) for complex posttraumatic deformity Ibrahim Obeid Fethi Laouissat
Eur Spine J (2013) 22:2130 2135 DOI 10.1007/s00586-013-2942-y OPEN OPERATING THEATRE (OOT) Asymmetric T5 Pedicle Subtraction Osteotomy (PSO) for complex posttraumatic deformity Ibrahim Obeid Fethi Laouissat
Efficiency of Ligamentotaxis Using PLL for Thoracic and Lumbar Burst Fractures in the Load-sharing Classification
 Efficiency of Ligamentotaxis Using PLL for Thoracic and Lumbar Burst Fractures in the Load-sharing Classification Won-Ju Jeong, MD; Joon-Woo Kim, MD; Dong-Kyo Seo, MD; Hyun-Joo Lee, MD; Jun-Young Kim,
Efficiency of Ligamentotaxis Using PLL for Thoracic and Lumbar Burst Fractures in the Load-sharing Classification Won-Ju Jeong, MD; Joon-Woo Kim, MD; Dong-Kyo Seo, MD; Hyun-Joo Lee, MD; Jun-Young Kim,
Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse of a Lumbar Spine Vertebral Body
 Case Reports in Orthopedics Volume 2013, Article ID 682075, 5 pages http://dx.doi.org/10.1155/2013/682075 Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse
Case Reports in Orthopedics Volume 2013, Article ID 682075, 5 pages http://dx.doi.org/10.1155/2013/682075 Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse
Hemivertebra Resection Combined With Wedge Osteotomy for the Treatment of Severe Rigid Congenital Kyphoscoliosis in Adolescence
 Hemivertebra Resection Combined With Wedge Osteotomy for the Treatment of Severe Rigid Congenital Kyphoscoliosis in Adolescence Comparison of Clinical, Radiographic, and Health-Related Quality of Life
Hemivertebra Resection Combined With Wedge Osteotomy for the Treatment of Severe Rigid Congenital Kyphoscoliosis in Adolescence Comparison of Clinical, Radiographic, and Health-Related Quality of Life
Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion
 Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity: Technical Note Involving 13 Cases
 Technical Note Clinics in Orthopedic Surgery 2013;5:225-229 http://dx.doi.org/10.4055/cios.2013.5.3.225 Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity:
Technical Note Clinics in Orthopedic Surgery 2013;5:225-229 http://dx.doi.org/10.4055/cios.2013.5.3.225 Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity:
GIZA Surgical Technique
 GIZA Surgical Technique Vertebral Body Replacement System Manufactured by Titanium alloy material provides mechanical integrity during insertion and distraction, x-ray visibility, and biocompatibility*
GIZA Surgical Technique Vertebral Body Replacement System Manufactured by Titanium alloy material provides mechanical integrity during insertion and distraction, x-ray visibility, and biocompatibility*
Pedicle Subtraction Osteotomy. Case JB. Antonio Castellvi 5/19/2017
 Pedicle Subtraction Osteotomy John M. Small MD Florida Orthopedic Institute University South Florida Department Orthopedic Surgery Castellvi Spine May 11, 2017 Case JB 66 y/o male 74 235 lbs Retired police
Pedicle Subtraction Osteotomy John M. Small MD Florida Orthopedic Institute University South Florida Department Orthopedic Surgery Castellvi Spine May 11, 2017 Case JB 66 y/o male 74 235 lbs Retired police
The Fusion of. Strength, Design. Performance. and
 The Fusion of Strength, Design and Performance Interbody Fusion Platform Interbody Fusion Platform The DePuy Spine Interbody Fusion platform is designed to provide an open architecture implant in a load-sharing
The Fusion of Strength, Design and Performance Interbody Fusion Platform Interbody Fusion Platform The DePuy Spine Interbody Fusion platform is designed to provide an open architecture implant in a load-sharing
Simultaneous anterior vertebral column resection-distraction and posterior rod contouring for restoration of sagittal balance: report of a technique
 Case Report Simultaneous anterior vertebral column resection-distraction and posterior rod contouring for restoration of sagittal balance: report of a technique Shaishav Bhagat 1, Alexander Z. E. Durst
Case Report Simultaneous anterior vertebral column resection-distraction and posterior rod contouring for restoration of sagittal balance: report of a technique Shaishav Bhagat 1, Alexander Z. E. Durst
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
Anterior Decompression and Stabilization with the Kaneda Device for Thoracolumbar Burst Fractures Associated with Neurological Deficits* 1
 Copyright 1997 by The Journal of Bone and Joint Surgery, Incorporated Anterior Decompression and Stabilization with the Kaneda Device for Thoracolumbar Burst Fractures Associated with Neurological Deficits*
Copyright 1997 by The Journal of Bone and Joint Surgery, Incorporated Anterior Decompression and Stabilization with the Kaneda Device for Thoracolumbar Burst Fractures Associated with Neurological Deficits*
Functional Outcome of Transpedicular Screw Fixation in patients with unstable Thoracolumbar Spine Injury
 ORIGINAL ARTICLE Functional Outcome of Transpedicular Screw Fixation in patients with unstable Thoracolumbar Spine Injury MIRZA SAMAR AHMAD, IJAZ AHMAD, AIQ UZ ZAMAN, RIZWAN AKRAM, AMER AZIZ ABSTRACT Background:
ORIGINAL ARTICLE Functional Outcome of Transpedicular Screw Fixation in patients with unstable Thoracolumbar Spine Injury MIRZA SAMAR AHMAD, IJAZ AHMAD, AIQ UZ ZAMAN, RIZWAN AKRAM, AMER AZIZ ABSTRACT Background:
Adult degenerative scoliosis: Is it worth the risk?
 3 rd Annual UCSF Techniques in Complex Spine Surgery Las Vegas, NV Nov 8-9 th 2013 Adult degenerative scoliosis: Is it worth the risk? Jens R. Chapman, M.D. HansJörg Wyss Professor and Chair Department
3 rd Annual UCSF Techniques in Complex Spine Surgery Las Vegas, NV Nov 8-9 th 2013 Adult degenerative scoliosis: Is it worth the risk? Jens R. Chapman, M.D. HansJörg Wyss Professor and Chair Department
Results of surgical treatment for kyphotic deformity of the spine secondary to trauma or Scheuermann s disease
 Acta Orthop. Belg., 2004, 70, 344-348 Results of surgical treatment for kyphotic deformity of the spine secondary to trauma or Scheuermann s disease Teoman ATICI, Ufuk AYDINLI, Burak AKESEN, Rasim ŠERIFOĞLU
Acta Orthop. Belg., 2004, 70, 344-348 Results of surgical treatment for kyphotic deformity of the spine secondary to trauma or Scheuermann s disease Teoman ATICI, Ufuk AYDINLI, Burak AKESEN, Rasim ŠERIFOĞLU
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Radiographic Outcome and Complications after Single-level Lumbar Extended Pedicle Subtraction Osteotomy for Fixed Sagittal Malalignment:
 Radiographic Outcome and Complications after Single-level Lumbar Extended Pedicle Subtraction Osteotomy for Fixed Sagittal Malalignment: Traditional A PSO Retrospective Analysis of 55 Adult Spinal Deformity
Radiographic Outcome and Complications after Single-level Lumbar Extended Pedicle Subtraction Osteotomy for Fixed Sagittal Malalignment: Traditional A PSO Retrospective Analysis of 55 Adult Spinal Deformity
Codes for Back and Spinal Procedures
 20930 Allograft for spine surgery only; morselized 20931 Allograft for spine surgery only; structural 20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process,
20930 Allograft for spine surgery only; morselized 20931 Allograft for spine surgery only; structural 20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process,
Spinal deformities, such as increased thoracic
 An Original Study Clinical and Radiographic Evaluation of Sagittal Imbalance: A New Radiographic Assessment Hossein Elgafy, MD, MCh, FRCS Ed, FRCSC, Rick Bransford, MD, Hassan Semaan, MD, and Theodore
An Original Study Clinical and Radiographic Evaluation of Sagittal Imbalance: A New Radiographic Assessment Hossein Elgafy, MD, MCh, FRCS Ed, FRCSC, Rick Bransford, MD, Hassan Semaan, MD, and Theodore
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
CLINICAL SCIENCE. Yueju Liu, I,II,# Guangbin Li, III,# Tianhua Dong, I,II Yingze Zhang, I,II Heng Li I,II * & INTRODUCTION
 CLINICAL SCIENCE One-stage partial vertebrectomy, titanium mesh implantation and pedicle screw fixation in the treatment of thoracolumbar burst fractures through a posterior approach Yueju Liu, I,II,#
CLINICAL SCIENCE One-stage partial vertebrectomy, titanium mesh implantation and pedicle screw fixation in the treatment of thoracolumbar burst fractures through a posterior approach Yueju Liu, I,II,#
Spine and Fusion. Adjacent Segment Disease. 36Ihsan SOLAROGLU M.D., M. Ozerk OKUTAN M.D., Gurdal NUSRAN M.D.
 Lumbar Posterior Hybrid Dynamic Stabilisation and Fusion Systems 36Ihsan SOLAROGLU M.D., M. Ozerk OKUTAN M.D., Gurdal NUSRAN M.D. Spine and Fusion It has been more than a century since 1911 when Albee
Lumbar Posterior Hybrid Dynamic Stabilisation and Fusion Systems 36Ihsan SOLAROGLU M.D., M. Ozerk OKUTAN M.D., Gurdal NUSRAN M.D. Spine and Fusion It has been more than a century since 1911 when Albee
ASJ. A Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia. Asian Spine Journal. Introduction
 sian Spine Journal 126 Dong-Eun Case Shin Report et al. http://dx.doi.org/10.4184/asj.2013.7.2.126 Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia Dong-Eun Shin, Ki-Sik
sian Spine Journal 126 Dong-Eun Case Shin Report et al. http://dx.doi.org/10.4184/asj.2013.7.2.126 Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia Dong-Eun Shin, Ki-Sik
Department of Orthopedic Surgery, Akita Kumiai General Hospital, Akita, Japan 2
 Asian Spine Journal Vol. 6, No. 2, pp 123~130, 2012 Surgery for lumbar burst fracture / 123 http://dx.doi.org/10.4184/asj.2012.6.2.123 Anterior Decompression and Shortening Reconstruction with a Titanium
Asian Spine Journal Vol. 6, No. 2, pp 123~130, 2012 Surgery for lumbar burst fracture / 123 http://dx.doi.org/10.4184/asj.2012.6.2.123 Anterior Decompression and Shortening Reconstruction with a Titanium
Prevention of PJF: Surgical Strategies to Reduce PJF. Robert Hart, MD Professor OHSU Orthopaedics Portland OR. Conflicts
 Prevention of PJF: Surgical Strategies to Reduce PJF Robert Hart, MD Professor OHSU Orthopaedics Portland OR Conflicts Consultant Depuy Spine, Medtronic Royalties Seaspine, Depuy Research/Fellowship Support
Prevention of PJF: Surgical Strategies to Reduce PJF Robert Hart, MD Professor OHSU Orthopaedics Portland OR Conflicts Consultant Depuy Spine, Medtronic Royalties Seaspine, Depuy Research/Fellowship Support
Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF)
 Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF) Calusa Ambulatory Spine Conference 2016 Jason Inzana, PhD 1 ; Anup Gandhi,
Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF) Calusa Ambulatory Spine Conference 2016 Jason Inzana, PhD 1 ; Anup Gandhi,
Procedure Coding Made Simple Five principles will help you capture appropriate charges for spine surgeries.
 Coding/Billing By Kim Pollock, MS, RN, MBA, CPC Procedure Coding Made Simple Five principles will help you capture appropriate charges for spine surgeries. It seems like coding spine cases is as complicated
Coding/Billing By Kim Pollock, MS, RN, MBA, CPC Procedure Coding Made Simple Five principles will help you capture appropriate charges for spine surgeries. It seems like coding spine cases is as complicated
Pelvic Fixation. Disclosures 5/19/2017. Rationale for Lumbo-pelvic Fixation
 Pelvic Fixation Joseph M Zavatsky, MD Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - DePuy Synthes Spine, Zimmer Biomet, Amendia, Stryker Stock - Innovative Surgical Solutions, Vivex
Pelvic Fixation Joseph M Zavatsky, MD Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - DePuy Synthes Spine, Zimmer Biomet, Amendia, Stryker Stock - Innovative Surgical Solutions, Vivex
