Anchorage. Foot & Ankle. Plating System. Operative Technique
|
|
|
- James Rich
- 5 years ago
- Views:
Transcription
1 Foot & Ankle Anchorage Plating System Operative Technique Foot & Ankle Anchorage Plate System MTP Plates Lapidus Plates Lisfranc Plates Basal Osteotomy Plates Utility Plates Anchorage Cross Plate System MTP Cross Plates Lapidus Cross Plates
2 Acknowledgments Stryker acknowledges the following surgeon for his support in the development of this technique guide: Keith L. Wapner, M.D. This publication sets forth detailed recommended procedures for using Stryker Osteosynthesis devices and instruments. It offers guidance that you should heed, but, as with any such technical guide, each surgeon must consider the particular needs of each patient and make appropriate adjustments when and as required. A workshop training is recommended prior to first surgery. All non-sterile devices must be cleaned and sterilized before use. Follow the appropriate instructions for use (IFU). Multicomponent instruments must be disassembled for cleaning. Please refer to the corresponding assembly / disassembly instructions. See package insert for a complete list of potential adverse effects, contraindications, warnings and precautions. The surgeon must discuss all relevant risks, including the finite lifetime of the device, with the patient, when necessary. Warning: Fixation Screws: Stryker Trauma and Extremities bone screws are not approved or intended for screw attachment or fixation to the posterior elements (pedicles) of the cervical, thoracic or lumbar spine. 2
3 Contents Page 1 Indications, Precautions & Contraindications 4 2 Overview Compression Ramp Technology Operative Technique 9 MTP Plate 9 Lapidus Plate 14 Lisfranc Plate 17 Osteotomy Basal Plate 20 4 Anchorage Cross Plate System Cross Joint Compression Instrumentation Operative Technique 26 Lapidus Cross Plate 26 MTP Cross Plate 28 3
4 Indications, Precautions & Contraindications Indications The Anchorage Bone Plate Systems are indicated for stabilization and fixation of fresh fractures, revision procedures, joint fusion, and reconstruction of small bones of the hand, feet, wrist and ankles, finger and toes. The system may be used in both adults and pediatric patients. Contraindications The following contraindications may be of a relative or absolute nature and must be taken into account by the attending surgeons: Acute or chronic infections, local or systemic. Surgical procedures other than those mentioned in the Indications section. Do not use on patients allergic to the components of the product (Please see Instructions for Use) or having known allergies. The combination of this implant with implants of another origin is contraindicated. Precautions Stryker Osteosynthesis systems have not been evaluated for safety and compatibility in MR environment and have not been tested for heating or migration in the MR environment, unless specified otherwise in the product labeling or respective operative technique. Detailed information is included in the instructions for use being attached to every implant. See package insert for warnings, precautions, adverse effects and other essential product information. 4
5 Overview Implants The is comprised of precontoured locking plates. Examples of Applications: 1st Metatarsal Phalangeal Joint Arthrodesis, with or without interpositional bone graft Proximal Osteotomy of Metatarsals 1 5 Lapidus Fusion Lisfranc Fusion Features Plate Thickness: 1.0 to 1.5mm (plate specific) Threaded holes accept either 3.0mm or 3.5mm locking or nonlocking screws. Nonlocking screws can be angulated 15 o from center Plates, screws and instruments color coded for ease of identification Plate and Screw Material: TiAl6V ELI Compression There are two plate specific options for compression: Cross Plate (CP) Design Compression Ramp Technology Anchorage CP MTP CP Plate Anchorage System MTP Plates Lisfranc Plates Lapidus CP Plates Lapidus Plates Basal Osteotomy Plates 3mm Locking Screws 3.5mm Utility Plates Nonlocking Screws 3.5mm Note: All threaded holes can accommodate either locking or nonlocking screws (3.0mm and 3.5mm diameter). The compression ramp only accepts 3.0mm nonlocking screws. All screws feature Torx heads +/-15 +/-15 Applying excessive torque during screw insertion is not recommended, and may result in damage to the screw head. In particular for nonlocking screws it is recommended to tighten the screw head until contact with the plate, then release from tightening. 5
6 Overview Instrumentation One set of ancillaries and screws for all plating systems. Instruments are color coded for ease of identification 1. K-Wires/tubes 2. Plate Benders 3. Nonlocking Drill Guide 4. Compression ramp Drill Guide 5. Drill bits 6. Driver tips 7. Depth Gauge 8. Locking Drill Guide 9. Forceps 10. Screwdriver handle 11. Cup / Cone Reamers 12. Ruler 13. Plate Trays 14. Screw Trays 15. Cross Plate (CP) Instrumentation Drill Guide bush MTP CP Drill Guide bush Lapidus CP Drill Guide bush for K-Wire CP Polyaxial drill guide bush CP CP Reamer Templates CP Lapidus & MTP Drill Guides 1. Drill Guide for Nonlocking 3.0mm Screws (XVIMQ002020) 1 2. Drill Guide for Nonlocking 3.5mm Screws (XVIMQ002025) 2 3. Drill Guide for 3.0mm Locking Screws (XVIMQ XPR002001) 4. Drill Guide for 3.5mm Locking Screws (XVIMQ XPR002001) Compression Ramp Drill Guide (XVIMQ XVIMQ003020) 6. Lapidus CP Drill Guide (XVIMQ XVIMQ003020) 5 7. MTP CP Drill Guide (XVIMQ XVIMQ003020) 8. Polyaxial CP Drill Guide (XVIMQ XVIMQ003020) K-Wire CP Drill Guide (XVIMQ XPR002001) 9 6
7 Overview Kirschner Wire Standard temporary K-Wires 1.2mm x 70mm (AGK ) and Olive K-Wires* 1.2mm x 65mm (XBR001002) are available to stabilize the Anchorage Plates and Anchorage CP Plates over the joints. *Optional Instrumentation. Screwdriver Assembly Pull the handle collar of the Screwdriver Handle and insert the Driver tips T8 AO quick coupling (XTV008001). The flat surface of the Driver tips needs to align with arrow on the screwdriver handle as pictured. Plate Benders The Anchorage plates are anatomically contoured. In some cases the Plate Benders (XCA001001) may be required. When utilizing the plate benders, the following guidelines should be adhered to: Do not apply on CP Plates Ensure the threaded holes of the plate are not disrupted during bending technique It is not recommended to bend at the plate extremities Plates should only be bent in one direction Do not re-bend plates Verify the angle Two optional plate bender leverage points 7
8 Anchorage Compression Ramp Technology The Compression Ramp provides mechanical compression between two corresponding bone segments. The Compression Ramp Drill Guide (XVIMQ XVIMQ003021) has 2 configurations; Load [compressed] and Neutral [non-compressed]. These are defined by the arrows laser etched in the top of the Drill Channel Head and the Handle Align the Channel Head and Handle arrows to correctly prepare the Drill Channel for either the Load [compressed] or Neutral [non-compressed] configuration Drill through Channel Head using a 2.0mm Drill Bit for a 3.0mm nonlocking screw Measure for appropriate screw length using Gauge and insert nonlocking screw Compression Ramp in Neutral configuration The Compression Ramp generates mechanical compression as the nonlocking screw head is tightened into the elongated screw hole with a graduated depth. As the screw is tightened, the screw head slides down the ramp, sitting deeper into wider portion of the screw hole, mechanically drawing the two bone segments together. 1.5mm of compression can be achieved using the Compression Ramp. The Compression Ramp only accommodates a 3.0mm nonlocking screw. Compression Ramp in Load configuration 1.5mm compression 8
9 MTP Arthrodesis Operative Technique The Anchorage MTP Fusion Plates are available in 3 different shapes, with one specific plate allowing revision surgeries (PLP1046X). MTP Plate Profile: 1.3mm Incision/Exposure A dorsal longitudinal incision is commonly used for MTP joint exposure. A medial approach may also be considered according to surgeon experience and patient indication. The incision is deepened and the EHL tendon retracted laterally. The joint capsule is released medial to the EHB tendon and retractors are placed to expose the base of the proximal phalanx and metatarsal head. An exostosectomy can be performed if necessary. A simulation of correction (metatarsus varus and pronation) is performed. Metatarsal Preparation The amount of bone resection depends upon the desired length of the 1st metatarsal. Note: Some revision cases will not require extensive resection. Option 1: Flat cuts technique Perform a dorsal approach to expose the metatarsal head and the base of the proximal phalanx. Remove the articular surface of metatarsal head perpendicularly to the shaft. Hold the phalanx in position (15 o Valgus; o Dorsiflexion). Make a parallel cut on proximal phalanx and proceed to the Medial Eminence Removal. Place a guidewire into the middle of the base of the proximal Phalanx and drive it out distal medial. Reduce the joint and then drive the pin back in a retrograde fashion into the metatarsal shaft for provisional fixation. 9
10 MTP Arthrodesis Operative Technique Option 2: Cup and Cone Technique Displace the phalanx plantarly or laterally, according to the approach chosen to expose the metatarsal head. Using a powered drill, place a 1.6mm x 100mm K-Wire (AGK16100) proximally through the center of the metatarsal head and into the diaphysis. The largest diameter concave reamer (22mm) (XFR004122) is inserted over the K-Wire. Reaming is performed until bleeding subchondral bone becomes visible on the joint surface. To ensure proper sizing, begin by using the largest size concave reamer, and then downsizing to match the diameter of the metatarsal head. Note: Check the progress of the reamer frequently to prevent excessive shortening of the metatarsal. Take note of the last reamer size used. Once metatarsal reaming is complete, the K-Wire can be used to elevate the metatarsal head to enable the removal of bone on the plantar aspect. Phalangeal Preparation The proximal phalanx is plantarflexed using a curved McGlamry or Hohmann Retractor. A 1.6mm x 100mm K-Wire is inserted into the center of the articular cartilage and directed through the diaphysis. Care should be taken not to penetrate the interphalangeal joint. Reaming is initiated using the smallest size convex reamer (14mm) (XFR004214) inserted over the K-Wire. Progressively increase the diameter of reamer used until the proximal phalanx is prepared with the same diameter utilized to prepare the metatarsal. If the metatarsal reaming stopped at 18mm, the last and largest reamer used on the phalanx will be 18mm. Note: The metatarsal head should be protected when reaming the proximal phalanx. 10
11 MTP Arthrodesis Operative Technique Stabilization/Plantar Compressive Screw Insertion The cup and cone shaped surfaces can be aligned in the desired position. Rotate the surfaces and set the dorsiflexion and valgus angles. Proper positioning can be evaluated by placing a support against the plantar surface of the foot. Once the desired position has been achieved, drive a K-Wire 1.6mm x 150mm (AGK16150) from the mid portion of the base of the proximal phalanx distally out the medial side. Then reduce the joint and drive it back in a retrograde fashion into the metatarsal for provisional fixation. According to surgeon preference, a cannulated or solid screw can then be inserted across the plantar aspect of the MTP joint. Plate Selection With the joint now stationary, the plate should be placed over the joint and evaluated. This evaluation should determine the degree of bend (if any) desired. Plate Benders (XCA001001) can be used to bend the plate if necessary. The plate should then be positioned over the joint and held in place with K-Wires 1.2mm x 70mm (AGK ) (see blue arrow). Note: Plates should only be bent in one direction. Never re-bend plates. 11
12 MTP Arthrodesis Operative Technique Distal Screw Insertion Perform drilling through locking or nonlocking drill guides according to the screw diameter to be utilized. Distal holes can accommodate either locking or nonlocking screws in 3.0mm (blue) or 3.5mm (yellow) diameter. Screws should be placed from medial to lateral. A 2.0mm Drill Bit (XFO082001) (for 3.0mm screws) or 2.5mm Drill Bit (XFO082501) (for 3.5mm screws) can be used in conjunction with the appropriate drill guide to prepare the hole for screw insertion. Insert screw after determining screw length with the Gauge (XJA002004). Note: A nonlocking screw can be inserted prior to introduction of locking screws to flush the plate to the bone surface
13 MTP Arthrodesis Operative Technique Compression Ramp Following distal screw insertion, the Compression Ramp (XVIMQ XVIMQ003021) can be used if compression is desired. Remove the K-Wire before compressing the joint. Refer to page 8 for Compression Ramp Technique. Ramp 1.5mm compression Proximal Screws Insertion Perform drilling through locking or nonlocking drill guides according to the screw diameter to be utilized. Proximal threaded holes can accommodate either locking or nonlocking screws in 3.0mm (blue) or 3.5mm (yellow) diameter. A 2.0mm Drill Bit (XFO082001) (for 3.0mm screws) or 2.5mm Drill Bit (XFO082501) (for 3.5mm screws) can be used in conjunction with the appropriate drill guide to prepare the hole for screw insertion. Insert screw after determining screw length with the Gauge (XJA002004). 13
14 The Anchorage Lapidus Plates are available in Left and Right sides, with 3 step references (0mm, 1mm and 2mm). The 1mm and 2mm step options are appropriate when step-off is observed during first metatarsal alignment. Lapidus Plate Profile: 1.5mm Incision and Joint Preparation An incision is made over the dorsal medial aspect of the 1st MTC joint. Dissection is carried down through the subcutaneous tissues with care to identify and protect the Anterior Tibial Tendon as it passes along the medial side of the medial cuneiform to insert on the plantar base of the first metatarsal. A dorsal capsulotomy is performed and the joint surfaces are debrided back to bleeding bone. After the joint preparation, reduce the fragments and temporarily fix using K-Wires 1.6mm x 150mm (AGK16150). 14
15 Lapidus Arthrodesis Operative Technique Plate Selection Choose the appropriate plate among the three step options according to the first metatarsal translation. Position the plate over the joint and stabilize with temporary K-Wire 1.6mm x 150mm (AGK16150). The plate should be positioned flush against the metatarsal and cuneiform surfaces. If necessary use the plate benders (XCA001001) to adjust the plate shape to the patient anatomy. Note: A temporary K-Wire 1.2mm x 70mm (AGK ) to anchor the plate to the metatarsal should be positioned distally within the slotted hole to accommodate the use of the compression ramp. Proximal Screw Insertion Perform drilling through locking or nonlocking drill guides according to the screw diameter preferred. All proximal holes can accommodate either locking or nonlocking screws in 3.0mm (blue) or 3.5mm (yellow) diameter. A 2.0mm Drill Bit (XFO082001) (for 3.0 screws) or 2.5mm Drill (XFO082501) Bit (for 3.5mm screws) can be used in conjunction with the appropriate drill guide to prepare the hole for screw insertion. Insert screw after determining screw length with the Gauge (XJA002004). Note: A nonlocking screw can be inserted prior to introduction of locking screws to flush the plate to the bone surface. 15
16 Lapidus Arthrodesis Operative Technique Compression Ramp Following proximal screw insertion, the Compression Ramp (XVIMQ XVIMQ003021) can be used if compression is desired. Remove the K-Wires prior to tightening down the screw in the Compression Ramp. Refer to page 8 for Compression Ramp Technique. Distal Screw Insertion A 2.0mm Drill Bit (XFO082001) (for 3.0 screws) or 2.5mm Drill Bit (XFO082501) (for 3.5mm screws) can be used in conjunction with the appropriate drill guide to prepare the hole for screw insertion. Insert screw after determining screw length with the Gauge. Note: A nonlocking screw can be inserted prior to introduction of locking screws to flush the plate to the bone surface. To stabilize the fusion construct, use a nonlocking drill guide and position an additional nonlocking screw (3.0mm) from the plantar aspect of the first metatarsal into medial cuneiform. 16
17 The Anchorage Lisfranc Plate is available in Small, Medium and Large size to accommodate patient anatomies. Lisfranc Plate Profile: 1.5mm Threaded Holes for Locking or NonLocking screws 2 Pin Fixation Holes 3 Compression Ramp Incision After the appropriate incision and joint preparation, reduce the fragments and temporarily fix using K-Wires 1.6mm x 150mm (AGK16150). Plate Positioning Position the plate and stabilize with temporary K-Wires 1.2mm x 70mm (AGK ) through small holes. Plate Benders (XCA001001) can be used to bend the plate if necessary. Note: Additional temporary fixation in distal holes is recommended to mitigate risk of plate sliding. Plates should only be bent in one direction. Never re-bend plates. 17
18 Lisfranc Arthrodesis Operative Technique Proximal Screw Insertion Perform drilling through locking and nonlocking drill guides according to the screw diameter preferred. All proximal holes can accommodate both locking and nonlocking screws in 3.0mm (blue) or 3.5mm (yellow) diameter. Two nonlocking screws can be inserted to flush the plate to the bone surface. A 2.0mm Drill Bit (XFO082001) (for 3.0mm screws) or 2.5mm Drill Bit (XFO082501) (for 3.5mm screws) can be used in conjunction with the appropriate drill guide to prepare the hole for screw insertion. Insert screw after determining screw length with the Gauge. 18
19 Compression Ramp Following proximal screw insertion, the Compression Ramps can be used if compression is desired. Refer to page 8 for Compression Ramp Technique. Distal Screw Insertion Remove the temporary crossing K-Wires. A 2.0mm Drill Bit (XFO082001) (for 3.0mm screws) or 2.5mm Drill Bit (XFO082501) (for 3.5mm screws) can be used in conjunction with the appropriate drill guide to prepare the hole for screw insertion. Insert screw after determining screw length with the Gauge (XJA002004). Note: A nonlocking screw can be inserted prior to introduction of locking screws to flush the plate to the bone surface. Surgical closure should be performed in a normal fashion. 19
20 Basal Osteotomy Operative Technique The Anchorage Basal Osteotomy Plates are available in 4 wedges options (0mm, 3mm, 4mm, 5mm) to ensure appropriate osteotomy correction. Basal Osteotomy Plate Profile: 1.0mm 0 3mm 4mm 5mm 20
21 Basal Osteotomy Operative Technique The most suitable angle of correction is identified on a preoperative X-Ray. Approach According to surgeon preference, one or two dorsal medial incisions are performed from the tarsometatarsal joint to the metatarsophalangeal joint taking care to retract all surrounding soft tissues. Identify the location of the first metatarsal cuneiform joint directly or via fluoroscopy. A K-Wire should be used to indicate the reference point of the osteotomy via fluoroscopy. Osteotomy The osteotomy line is made in a medial to lateral direction, perpendicular to the metatarsal axis and approximately 10 15mm distally to the TMT joint with care not to penetrate the lateral cortex. An osteotome can be utilized to open the osteotomy until the appropriate correction is reached. Care should be taken to preserve the lateral cortex. 21
22 Basal Osteotomy Operative Technique Plate Fixation After plate identification, insert the wedge medially into the osteotomy and secure the plate with temporary K-Wires 1.2mm x 70mm (AGK ). Plate Fixation Perform drilling through locking or nonlocking drill guides according to the screw option desired. All proximal and distal holes can accommodate both locking and nonlocking screws in 3.0mm (blue) or 3.5 mm (yellow) diameter. A 2.0mm Drill Bit (XFO082001) (for 3.0mm screws) or 2.5mm Drill Bit (XFO082501) (for 3.5mm screws) can be used in conjunction with the appropriate drill guide to prepare the hole for screw insertion. Insert screw after determining screw length with the Gauge. Note: A nonlocking screw can be inserted prior to introduction of locking screws to flush the plate to the bone surface. The Gauge (XJA002004) should be utilized to determine appropriate length screw to insert into the screw hole. Following measurement, the appropriate screw can be inserted. 22
23 Basal Osteotomy Operative Technique Locking or nonlocking screws can be inserted into the remaining holes following the same procedure for inserting proximal screws. 23
24 Anchorage Cross Plate System Mechanically Generated, Cross Joint Compression The Anchorage Cross Plate (CP) System uses an inset diagonal, crossjoint screw to develop mechanical compression across the fusion site. This approach minimizes the need for separate, independent stabilization and is designed to create compression. All Anchorage CP Plates include: Oblique screw design which offers an immediate stable construct Low profile design Cannulated instrumentation which helps promote surgical efficiency The CP plate concept was designed to allow maximum transmission of compression force across the joint, with out the risk of the head of the screw fracturing the cortex and thus loosing stability. By creating a recess for the counterbore in the plate it allows positioning of a compression screw through the plate. By first fixing the plate to the bone the force of compression is borne by the plate and screw as the compression screw is set. This allows maximum compression to be placed through the screw without risk of cortical fracture. This combination affords the compression of lag screw fixation combined with the stability of plate fixation. The Cross Joint Counterbore accomodates only nonlocking Screws (3 or 3.5 mm). Anchorage CP System Plates feature built-in, cross joint fixation with compression to simplify the surgical procedure and minimize the need for a separate, independent transverse screw. 24
25 Anchorage Cross Plate System Instrumentation The CP Instrumentation is designed for utilization with the Counterbore oblique holes of the CP plates. Distal and proximal screw insertion are performed with standard Anchorage instrumentation. Do not use the Plate Bender (XCA001001) with the Cross Plate System. Anchorage CP Lapidus Plate The Lapidus CP Plate is accompanied by a matching Location Template (XFA008701) that attaches to the CP 1.2mm K-Wire Guide (XVIMQ001012). The Lapidus Counterbore Drill Guide (XVIMQ004025) is asymmetric with a cylindrical, convex surface that corresponds to the matching concave surface of the Lapidus Plate. Lapidus CP Template with K-Wire Guide Anchorage CP MTP Plate The MTP Plate is also accompanied by a matching a Location Template (XFA008711) that attaches to the K-Wire Drill Guide (XVIMQ001012). The MTP Counterbore Drill Guide (XVIMQ005025) is cylindrical, with a flat edge that corresponds to the matching indentation on the MTP Plate. Lapidus CP Counterbore Drill Guide MTP CP Template with K-Wire Guide MTP CP Counterbore Drill Guide 25
26 Anchorage Cross Plate System Lapidus Arthrodesis Operative Technique CP Preparation Incision and temporary reduction can be achieved using standard procedure (refer to page 14). Once temporarily fixed, the 1.2mm K-Wire (AGK ) is inserted into the 1.2mm K-Wire guide and is attached to the Lapidus CP Template (XFA008701). The 1.2mm K-Wire guide (XVIMQ001012) can be attached to the white Drill Guide Handle or independently used as a joystick to position the template over the joint. The template should be positioned with the raised wedge (a) directly over the joint line. Once position is verified, a 1.2mm K-Wire is advanced through the drill guide and into the metatarsal. The template and drill guide are removed leaving the 1.2mm K-Wire. The CP Reamer (XFR006100) is advanced over the K-Wire to the appropriate depth limit (b). The reamer should not penetrate below the cortex of the bone. Once CP reaming is complete, the guide pin is removed and the CP plate is positioned and held in place with temporary fixation (AGK ). Raised wedge (a) Appropriate depth limit (b) Distal Screw Insertion A 2.0mm Drill Bit (XFO082001) (for 3.0 screws) or 2.5mm Drill Bit (XFO082501) (for 3.5mm screws) can be used in conjunction with the appropriate drill guide to prepare the hole for screw insertion. Insert distal screws after determining screw length with the Gauge (XJA002004). Note: A nonlocking screw can be inserted prior to introduction of locking screws to flush the plate to the bone surface. All threaded holes accommodate either locking or nonlocking screws (3.0mm and 3.5mm). Only nonlocking screws can be used in the Counterbore. 26
27 Anchorage Cross Plate System Lapidus Arthrodesis Operative Technique CP Preparation Continued The CP Lapidus Drill Guide (XVIMQ004025) is positioned over the cross joint hole. Note: The Lapidus CP Drill Guide should be positioned with laser markings on flat surface facing outward from the plate. Depending on the plate positioning (dorsal or medial), the bone quality and the patient anatomy, drilling can be performed across one of the two drill guide holes. Use a 2.0mm Drill Bit (XFO082001) to accommodate a 3.0mm screw or a 2.5mm Drill Bit (XFO082501) to accomodate a 3.5mm screw. Remove Lapidus CP Drill Guide. Medial Positioning Dorsal Positioning Cross Joint Screw Use Gauge (XJA002004) to measure appropriate length screw for insertion. Once measured, all temporary fixation is removed and the appropriate nonlocking screw is placed through the CP hole. As screw seats in the Counterbore of the plate, additional tightening develops compression across the joint with lag effect. Proximal Screw Insertion Insert remaining proximal screws and position under fluoroscopy. 27
28 Anchorage Cross Plate System MTP Arthrodesis Operative Technique Preparation The first MTP joint is prepared using flat cuts technique or the provided cup and cone reamers (XFR0042XX & XFR0041XX) within the Anchorage instrument set (Refer to page 10 for MTP exposure). Once prepared, the cup and cone surfaces can be aligned into desired position and temporarily stabilized using a guide wire. CP Plate Positioning The MTP CP Template is oriented either R or L. The CP 1.2mm K-Wire guide (XVIMQ001012) is screwed into the template and is positioned over the MTP joint. Proper position has been achieved when the raised wedge (a) on the MTP CP Template is directly over the joint line. A 1.2mm K-Wire (AGK ) is inserted through the K-Wire guide. Once the K-Wire is positioned, the drill guide and template are removed. The CP reamer (XFR006100) is advanced over the K-Wire until the appropriate depth limit is achieved (b). The reamer should not penetrate below the cortex of the bone. The plate is positioned and temporarily fixated 1.2mm x 70mm (AGK ). Once fixated, the proximal holes are drilled and filled with appropriate drill bit and screw. Note: All holes accommodate both locking and nonlocking screws [3.0mm and 3.5mm] with the exception of the cross joint Counterbore which utilizes only nonlocking screws. Raised wedge (a) Appropriate depth limit (b) 28
29 Anchorage Cross Plate System MTP Arthrodesis Operative Technique Cross Joint Screw After proximal fixation is achieved, the CP MTP Drill Guide (XVIMQ005025) is positioned in the Counterbore. A 2.0mm Drill Bit(XFO082001) (for 3.0mm screw) or 2.5mm Drill Bit (XFO082501) (for 3.5mm screw) is used to drill to the plantar cortex of the proximal phalanx. Use the Gauge (XJA002004) to measure the appropriate length nonlocking screw to be inserted. Once appropriate length screw is measured, all temporary fixation is removed and the appropriate nonlocking screw is placed through the CP hole. Alternatively, use the Polyaxial Cross Plate Drilling Bush (XVIMQ001045) when an alternate angle for the screw is desired. Repeat above steps. As screw seats in plate, additional tightening develops compression across the joint with lag effect. Distal Screw Insertion Once compressed, the remaining distal screws can be inserted and verified with X-Ray. Note: To avoid any risk of conflict with the cross joint screw, maximum a 12mm screw is recommended. 29
30 Notes 30
31 Notes 31
32 Manufactured by: Stryker Trauma AG Bohnackerweg Selzach Switzerland This document is intended solely for the use of healthcare professionals. A surgeon must always rely on his or her own professional clinical judgment when deciding whether to use a particular product when treating a particular patient. Stryker does not dispense medical advice and recommends that surgeons be trained in the use of any particular product before using it in surgery. The information presented is intended to demonstrate a Stryker Orthopaedics product. A surgeon must always refer to the package insert, product label and/or instructions for use, including the instructions for Cleaning and Sterilization (if applicable), before using any Stryker product. Products may not be available in all markets because product availability is subject to the regulatory and/or medical practices in individual markets. Please contact your Stryker representative if you have questions about the availability of Stryker products in your area. Stryker Corporation or its divisions or other corporate affiliated entities own, use or have applied for the following trademarks or service marks: Anchorage, Stryker. All other trademarks are trademarks of their respective owners or holders. Distributed by: Howmedica Osteonics Corp. 325 Corporate Dr Mahwah NJ The products listed above are CE marked Rev 2 AN-ST-1 Copyright 2013 Stryker 32
Foot & Ankle. EasyClip. Osteosynthesis Compression Staples. Foot & Ankle
 Foot & Ankle EasyClip Osteosynthesis Compression Staples Foot & Ankle Operative Technique EasyClip Osteosynthesis Compression Staples 2 This publication sets forth detailed recommended procedures for using
Foot & Ankle EasyClip Osteosynthesis Compression Staples Foot & Ankle Operative Technique EasyClip Osteosynthesis Compression Staples 2 This publication sets forth detailed recommended procedures for using
Foot & Ankle. Smart Toe II. Intramedullary Implant. Operative Technique. Foot & Ankle
 Foot & Ankle Smart Toe II Intramedullary Implant Operative Technique Foot & Ankle Smart Toe This publication sets forth detailed recommended procedures for using Stryker Osteosynthesis devices and instruments.
Foot & Ankle Smart Toe II Intramedullary Implant Operative Technique Foot & Ankle Smart Toe This publication sets forth detailed recommended procedures for using Stryker Osteosynthesis devices and instruments.
DYNAMIC, TRANSVERSE COMPRESSION. Low Profile, Anatomic Design, Type II Anodized. Mechanical Compression Designed to Stimulate the Fusion Process
 CoLink_XP_ST_080218.pdf 1 8/2/18 8:36 AM SURGICAL TECHNIQUE CoLink XP Plates DYNAMIC, TRANSVERSE COMPRESSION C M Y CM MY CY CMY K MTP Std. Plate MTP Revision Plate Lapidus Standard +1mm and +2mm Y Plate
CoLink_XP_ST_080218.pdf 1 8/2/18 8:36 AM SURGICAL TECHNIQUE CoLink XP Plates DYNAMIC, TRANSVERSE COMPRESSION C M Y CM MY CY CMY K MTP Std. Plate MTP Revision Plate Lapidus Standard +1mm and +2mm Y Plate
4Fusion. Shape Memory Implant. Operative Technique
 4Fusion Shape Memory Implant Operative Technique 4Fusion This publication sets forth detailed recommended procedures for using Stryker devices and instruments. It offers guidance that you should heed,
4Fusion Shape Memory Implant Operative Technique 4Fusion This publication sets forth detailed recommended procedures for using Stryker devices and instruments. It offers guidance that you should heed,
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Asnis. Micro Cannulated screw system. Xpress operative technique
 Asnis Micro Cannulated screw system Xpress operative technique Asnis Micro Cannulated screw system Table of contents Indications, precautions & contraindications 3 Operative technique 4 This publication
Asnis Micro Cannulated screw system Xpress operative technique Asnis Micro Cannulated screw system Table of contents Indications, precautions & contraindications 3 Operative technique 4 This publication
EasyStep. Operative technique
 Operative technique EasyStep - Step staple This publication sets forth detailed recommended procedures for using Stryker Osteosynthesis devices and instruments. It offers guidance that you should heed,
Operative technique EasyStep - Step staple This publication sets forth detailed recommended procedures for using Stryker Osteosynthesis devices and instruments. It offers guidance that you should heed,
The Flower Medial Column Fusion Plate
 The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Forefoot/Midfoot Plating System. Surgical Technique
 Forefoot/Midfoot Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Forefoot/Midfoot Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Forefoot/Midfoot Plating System
 Surgical Technique Forefoot/Midfoot Plating System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Surgical Technique Forefoot/Midfoot Plating System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Flower Opening Wedge Plate
 Flower Opening Wedge Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION T-PLATE, OBLIQUE
Flower Opening Wedge Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION T-PLATE, OBLIQUE
DARCO. Bow 2 Plate SURGIC AL TECHNIQUE
 DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
DARCO. LPS Plate SURGICAL TECHNIQUE
 DARCO LPS Plate SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 5 5 6 7 9 Appendix 10 10 11 Design Rationale Preoperative Planning Surgical Technique Surgical Approach Joint Preparation Surgical
DARCO LPS Plate SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 5 5 6 7 9 Appendix 10 10 11 Design Rationale Preoperative Planning Surgical Technique Surgical Approach Joint Preparation Surgical
CANNULINK. Intraossous Fixation System SURGICAL TECHNIQUE
 CANNULINK Intraossous Fixation System SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction The CANNULINK Advantage Indications for Use Preoperative Planning Chapter 2 5 Surgical Technique CANNULINK Standard
CANNULINK Intraossous Fixation System SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction The CANNULINK Advantage Indications for Use Preoperative Planning Chapter 2 5 Surgical Technique CANNULINK Standard
AxSOS. Locking Plate System. Operative Technique. Small Fragment Basic Fragment
 AxSOS Locking Plate System Operative Technique Small Fragment Basic Fragment Stryker Plating Contents Page 1. Introduction 4 2. Features & Benefits 5 4 and 5 Compression Plates 5 Reconstruction and 1/3
AxSOS Locking Plate System Operative Technique Small Fragment Basic Fragment Stryker Plating Contents Page 1. Introduction 4 2. Features & Benefits 5 4 and 5 Compression Plates 5 Reconstruction and 1/3
Correction System. Surgical Technique
 Nextra Hammertoe Correction System Surgical Technique Maximized Bone Purchase* Stable and Secure Phalanx Optimized Screw Design Adjustable Bone-to-Bone Apposition Progressive Ratchet Tightening Mechanism
Nextra Hammertoe Correction System Surgical Technique Maximized Bone Purchase* Stable and Secure Phalanx Optimized Screw Design Adjustable Bone-to-Bone Apposition Progressive Ratchet Tightening Mechanism
Locking Forefoot/Midfoot Plating System
 Locking Forefoot/Midfoot Plating System Locking Forefoot/Midfoot Plating System Acumed is an industry leader in innovative solutions for extremities and trauma. We are dedicated to pioneering solutions
Locking Forefoot/Midfoot Plating System Locking Forefoot/Midfoot Plating System Acumed is an industry leader in innovative solutions for extremities and trauma. We are dedicated to pioneering solutions
Integra. ADVANSYS Plating System SURGICAL TECHNIQUE
 Integra ADVANSYS Plating System SURGICAL TECHNIQUE Table of Contents Dorsal Lisfranc Plate Indications...2 Contraindications...2 Description...2 Surgical Technique...3 Surgical Site Preparation...3 Step
Integra ADVANSYS Plating System SURGICAL TECHNIQUE Table of Contents Dorsal Lisfranc Plate Indications...2 Contraindications...2 Description...2 Surgical Technique...3 Surgical Site Preparation...3 Step
Surgical Technique. Anterolateral and Medial Distal Tibia Locking Plates
 Surgical Technique Anterolateral and Medial Distal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System Anterolateral and Medial Distal Tibia Locking Plates Surgical Technique Contents Product
Surgical Technique Anterolateral and Medial Distal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System Anterolateral and Medial Distal Tibia Locking Plates Surgical Technique Contents Product
Surgical Technique Guide
 Guide CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Align Anterior Ankle Fusion Plate is intended to facilitate arthrodesis of the
Guide CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Align Anterior Ankle Fusion Plate is intended to facilitate arthrodesis of the
Foot Reconstruction System SURGICAL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System SURGICAL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: Robert B. Anderson, MD OrthoCarolina Charlotte,
ORTHOLOC 3Di Foot Reconstruction System SURGICAL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: Robert B. Anderson, MD OrthoCarolina Charlotte,
VariAx Compression Plating System. Operative technique
 VariAx Compression Plating System Operative technique VariAx Compression Plating System Operative technique VariAx Compression Plating System Contents 1. Introduction... 3 2. Indications, MR safety information
VariAx Compression Plating System Operative technique VariAx Compression Plating System Operative technique VariAx Compression Plating System Contents 1. Introduction... 3 2. Indications, MR safety information
Correction System. Surgical Technique
 Nextra Hammertoe Correction System Surgical Technique Maximized Bone Purchase* Stable and Secure Phalanx Optimized Screw Design Adjustable Bone-to-Bone Apposition Progressive Ratchet Tightening Mechanism
Nextra Hammertoe Correction System Surgical Technique Maximized Bone Purchase* Stable and Secure Phalanx Optimized Screw Design Adjustable Bone-to-Bone Apposition Progressive Ratchet Tightening Mechanism
ORTHOLOC 3Di. Foot Reconstruction System SURGIC AL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
Axi+LineTM Proximal Bunion CorrectionSystem. Surgical Technique
 Axi+LineTM Proximal Bunion CorrectionSystem Surgical Technique A i Line Proximal Bunion Correction System TM Desired angle correction is built into the plate, providing a self-reducing, 5-hole construct
Axi+LineTM Proximal Bunion CorrectionSystem Surgical Technique A i Line Proximal Bunion Correction System TM Desired angle correction is built into the plate, providing a self-reducing, 5-hole construct
Technique Guide. 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia Plates
Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia Plates
PEDUS-L. Locking Plantar Lapidus Plate
 PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot.
 Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Surgical Technique. Proximal Humerus Locking Plate
 Surgical Technique Proximal Humerus Locking Plate PERI-LOC Upper Extremity Locked Plating System 3.5mm & 4.5mm Proximal Humerus Locking PlatesCatalog Infor Table of Contents Introduction.........................................................2
Surgical Technique Proximal Humerus Locking Plate PERI-LOC Upper Extremity Locked Plating System 3.5mm & 4.5mm Proximal Humerus Locking PlatesCatalog Infor Table of Contents Introduction.........................................................2
MICA. Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE
 MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
Technique Guide. 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System.
 Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal
Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal
SMV Scientific Bone Plate and Screw System Surgical Technique
 SMV Scientific Bone Plate and Screw System Surgical Technique Description: The SMV Scientific Bone Plate and Screw System consists of non-locking plates and bone screw fasteners in a variety of lengths,
SMV Scientific Bone Plate and Screw System Surgical Technique Description: The SMV Scientific Bone Plate and Screw System consists of non-locking plates and bone screw fasteners in a variety of lengths,
NeoFit. Metatarsophal angeal Arthrodesis Pl ate
 NeoFit Metatarsophal angeal Arthrodesis Pl ate 2 NEOFIT - TABLE OF CONTENTS PRODUCT DESCRIPTION 3 INDICATIONS 6 Download «PRINT» version (white background) SURGICAL TECHNIQUE 7 1 - Incision 8 2 - Preparation
NeoFit Metatarsophal angeal Arthrodesis Pl ate 2 NEOFIT - TABLE OF CONTENTS PRODUCT DESCRIPTION 3 INDICATIONS 6 Download «PRINT» version (white background) SURGICAL TECHNIQUE 7 1 - Incision 8 2 - Preparation
Surgical Technique. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Surgical Technique. Clavicle Locking Plate
 Surgical Technique Clavicle Locking Plate PERI-LOC Locked Plating System Clavicle Locking Plate Surgical Technique Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient Positioning...4
Surgical Technique Clavicle Locking Plate PERI-LOC Locked Plating System Clavicle Locking Plate Surgical Technique Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient Positioning...4
Flower Medium Headless & Cannulated Screws
 Flower Medium Headless & Cannulated Screws PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Flower Medium Headless & Cannulated Screws PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
AxSOS Locking Plate System
 AxSOS Locking Plate System Operative Technique Small Fragment Basic Fragment 1 2 Contents Page 1. Introduction 4 2. Features & Benefits 5 4 and 5mm Compression Plates 5 Reconstruction and 1/3 Tubular Locking
AxSOS Locking Plate System Operative Technique Small Fragment Basic Fragment 1 2 Contents Page 1. Introduction 4 2. Features & Benefits 5 4 and 5mm Compression Plates 5 Reconstruction and 1/3 Tubular Locking
Contents. Chapter 1 4 Chapter Chapter Chapter Chapter 5 15
 Contents Chapter 1 4 Chapter 2 5 5 Chapter 3 6 6 7 Chapter 4 8 8 8 8 9 10 10 11 12 13 14 14 Chapter 5 15 Introduction Intended Use Indications Device Description Implant Options and Sizing Instrumentation
Contents Chapter 1 4 Chapter 2 5 5 Chapter 3 6 6 7 Chapter 4 8 8 8 8 9 10 10 11 12 13 14 14 Chapter 5 15 Introduction Intended Use Indications Device Description Implant Options and Sizing Instrumentation
CableFIX Xpress Carpometacarpal Fixation System. Operative technique
 CableFIX Xpress Carpometacarpal Fixation System Operative technique CableFIX Xpress Carpometacarpal Fixation System CableFIX Xpress Carpometacarpal Fixation System Contents 1. Indications and contraindications...
CableFIX Xpress Carpometacarpal Fixation System Operative technique CableFIX Xpress Carpometacarpal Fixation System CableFIX Xpress Carpometacarpal Fixation System Contents 1. Indications and contraindications...
Surgical Technique Carpal Fusion
 Carpal Fusion Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Extremity Medical Lag Screw and X-Post System
Carpal Fusion Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Extremity Medical Lag Screw and X-Post System
InCoreTM Lapidus System
 InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
Instrument and Implant for wrist fracture
 Instrument and Implant for wrist fracture Jansri Janpanya Product specialist The Bangkok Unitrade Co,.ltd. Objectives Type of LCP for distal radius Fx. The new LCP design for distal radius Fx. Have knowledge
Instrument and Implant for wrist fracture Jansri Janpanya Product specialist The Bangkok Unitrade Co,.ltd. Objectives Type of LCP for distal radius Fx. The new LCP design for distal radius Fx. Have knowledge
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System.
 LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Distal Radius Plate Instrument and Implant Set. Discontinued December 2017 DSUS/TRM/0916/1063(1)
 Distal Radius Plate Instrument and Implant Set Surgical Technique Discontinued December 2017 DSUS/TRM/0916/1063(1) The Distal Radius Plates Indications For fixation of fractures and osteotomies, including
Distal Radius Plate Instrument and Implant Set Surgical Technique Discontinued December 2017 DSUS/TRM/0916/1063(1) The Distal Radius Plates Indications For fixation of fractures and osteotomies, including
Surgical Technique 4.5/8.5MM BEAMING SYSTEM. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The 4.5/8.5 screw system is intended for fixation arthrodesis of
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The 4.5/8.5 screw system is intended for fixation arthrodesis of
CHARLOTTE Lisfranc. Recontruction System SURGICAL TECHNIQUE
 CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
Surgical Technique. CONQUEST FN Femoral Neck Fracture System
 Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer
 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Surgical Technique. Olecranon Locking Plate
 Surgical Technique Olecranon Locking Plate PERI-LOC Locked Plating System Olecranon Locking Plate Surgical Techniquealog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Surgical Technique Olecranon Locking Plate PERI-LOC Locked Plating System Olecranon Locking Plate Surgical Techniquealog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
SURGICAL TECHNIQUE GUIDE: LAPIDUS ARTHRODESIS USING THE PHANTOM INTRAMEDULLARY NAIL INTRAMEDULLARY NAIL
 LAPIDUS ARTHRODESIS USING THE PHANTOM INTRAMEDULLARY NAIL INTRAMEDULLARY NAIL LAPIDUS ARTHRODESIS USING THE PHANTOM INTRAMEDULLARY NAIL Acknowledgment: Paragon 28 would like to thank James T. Clancy, DPM
LAPIDUS ARTHRODESIS USING THE PHANTOM INTRAMEDULLARY NAIL INTRAMEDULLARY NAIL LAPIDUS ARTHRODESIS USING THE PHANTOM INTRAMEDULLARY NAIL Acknowledgment: Paragon 28 would like to thank James T. Clancy, DPM
Surgical Technique International Version. Clavicle Locking Plate
 Surgical Technique International Version Clavicle Locking Plate PERI-LOC Upper Extremity Locked Plating System Clavicle Surgical Techniquefor Table of Contents Introduction........................................................2
Surgical Technique International Version Clavicle Locking Plate PERI-LOC Upper Extremity Locked Plating System Clavicle Surgical Techniquefor Table of Contents Introduction........................................................2
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique
 PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
Astrid Modular Forefoot System. Surgical Technique
 Astrid Modular Forefoot System Surgical Technique Table of Contents Astrid a System for Surgery of the Forefoot... Scarf Osteotomies...6 Stabilization by Means of Two Parallel Double-Threaded Screws Introduced
Astrid Modular Forefoot System Surgical Technique Table of Contents Astrid a System for Surgery of the Forefoot... Scarf Osteotomies...6 Stabilization by Means of Two Parallel Double-Threaded Screws Introduced
Correction System. Surgical Technique
 Re+Line Bunion Correction System Surgical Technique Bunion Correction System Easy insertion and medial placement accuracy using Landmark Guide technology 1 mm compression slot and fixed tines to encourage
Re+Line Bunion Correction System Surgical Technique Bunion Correction System Easy insertion and medial placement accuracy using Landmark Guide technology 1 mm compression slot and fixed tines to encourage
Distal Ulnar Locking Plate
 INDEX Indications Patient Position Surgical Technique - Step 1 Approach - Step 2 Plate Contouring - Step 3 Fracture Reduction - Step 4 Distal Plate Fixation - Step 5 Confirm Proper Reconstruction - Step
INDEX Indications Patient Position Surgical Technique - Step 1 Approach - Step 2 Plate Contouring - Step 3 Fracture Reduction - Step 4 Distal Plate Fixation - Step 5 Confirm Proper Reconstruction - Step
Hallux Valgus Deformity OPERATIVE TECHNIQUE
 Hallux Valgus Deformity OPERATIVE TECHNIQUE Table of Contents 1 ORDERING INFORMATION 3 OPERATIVE TECHNIQUE 9 INDICATIONS FOR USE The surgical technique shown is for illustrative purposes only. The technique(s)
Hallux Valgus Deformity OPERATIVE TECHNIQUE Table of Contents 1 ORDERING INFORMATION 3 OPERATIVE TECHNIQUE 9 INDICATIONS FOR USE The surgical technique shown is for illustrative purposes only. The technique(s)
MPJ Implant System. Patents Pending Worldwide
 MPJ Implant System Patents Pending Worldwide OVERVIEW ACTIVE STABILIZATION The DynaFORCE Active Stabilization System is the first to offer a hybrid implant system designed to address the most common rearfoot,
MPJ Implant System Patents Pending Worldwide OVERVIEW ACTIVE STABILIZATION The DynaFORCE Active Stabilization System is the first to offer a hybrid implant system designed to address the most common rearfoot,
Technique Guide. 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology.
 Technique Guide 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4 mm Variable Angle LCP
Technique Guide 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4 mm Variable Angle LCP
3. PATIENT POSITIONING & FRACTURE REDUCTION 3 8. DISTAL GUIDED LOCKING FOR PROXIMAL NAIL PROXIMAL LOCKING FOR LONG NAIL 13
 Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL NAIL INSERTION 6-7 7. PROXIMAL LOCKING
Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL NAIL INSERTION 6-7 7. PROXIMAL LOCKING
Surgical Technique. 3.5mm and 4.5mm Lateral Proximal Tibia Locking Plates
 Surgical Technique 3.5mm and 4.5mm Lateral Proximal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System 3.5mm and 4.5mm Lateral Proximal Tibia Locking Plate Surgical Technique Contents Product
Surgical Technique 3.5mm and 4.5mm Lateral Proximal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System 3.5mm and 4.5mm Lateral Proximal Tibia Locking Plate Surgical Technique Contents Product
LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures.
 LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures. Surgical Technique This publication is not intended for distribution in the
LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures. Surgical Technique This publication is not intended for distribution in the
VariAx 2 Plating Solutions
 VariAx 2 Plating Solutions Operative technique VariAx 2 Foot Stryker Foot Plating System VariAx 2 Plating Solutions Table of contents Indications, precaution, and contraindications VariAx 2 Foot - tray
VariAx 2 Plating Solutions Operative technique VariAx 2 Foot Stryker Foot Plating System VariAx 2 Plating Solutions Table of contents Indications, precaution, and contraindications VariAx 2 Foot - tray
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
Silicone PIP, MCP & MCP-X (PreFlex)
 Silicone PIP, MCP & MCP-X (PreFlex) Finger Joint Arthroplasty Operative Technique Silicone PIP Silicone MCP Silicone PreFlex (MCP-X) Stryker Disclaimer This publication sets forth detailed recommended
Silicone PIP, MCP & MCP-X (PreFlex) Finger Joint Arthroplasty Operative Technique Silicone PIP Silicone MCP Silicone PreFlex (MCP-X) Stryker Disclaimer This publication sets forth detailed recommended
Technique Guide. VA-Locking Intercarpal Fusion System. Variable angle locking technology for mediocarpal partial arthrodesis.
 Technique Guide VA-Locking Intercarpal Fusion System. Variable angle locking technology for mediocarpal partial arthrodesis. Table of Contents Introduction VA-Locking Intercarpal Fusion System 2 Indications
Technique Guide VA-Locking Intercarpal Fusion System. Variable angle locking technology for mediocarpal partial arthrodesis. Table of Contents Introduction VA-Locking Intercarpal Fusion System 2 Indications
Technique Guide. 3.5 mm LCP Olecranon Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Olecranon Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Olecranon Plates 2 AO Principles 3 Indications 3 Clinical
Technique Guide 3.5 mm LCP Olecranon Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Olecranon Plates 2 AO Principles 3 Indications 3 Clinical
LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system.
 LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Integra. surgical technique. Advansys Midfoot Plating System. eng. D.L.P. Dorsal Lisfranc Plate. M.L.P. Medial Lisfranc Plate
 eng Integra Advansys Midfoot Plating System surgical technique D.L.P. Dorsal Lisfranc Plate M.L.P. Medial Lisfranc Plate Table of Contents Advansys Medial Lisfranc Plate (DLP)... 4 Indications... 4 Contraindications...
eng Integra Advansys Midfoot Plating System surgical technique D.L.P. Dorsal Lisfranc Plate M.L.P. Medial Lisfranc Plate Table of Contents Advansys Medial Lisfranc Plate (DLP)... 4 Indications... 4 Contraindications...
OBSOLETED. LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Surgical Technique LCP Small Fragment System This publication
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Surgical Technique LCP Small Fragment System This publication
Bunion Correction System
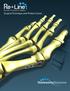 Bunion Correction System Easy insertion and medial placement accuracy using Landmark Guide technology Maximized and repeatable uniform compression across osteotomy site Stable Fixation of the Metatarsal
Bunion Correction System Easy insertion and medial placement accuracy using Landmark Guide technology Maximized and repeatable uniform compression across osteotomy site Stable Fixation of the Metatarsal
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LoCKING FOREFOOT/ MIDFOOT PLATES
 LoCKING FOREFOOT/ MIDFOOT PLATES LoCKING FOREFOOT/ MIDFOOT PLATES Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our
LoCKING FOREFOOT/ MIDFOOT PLATES LoCKING FOREFOOT/ MIDFOOT PLATES Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our
ORTHOLOC 3Di. Foot Reconstruction System Midfoot Fusion Plate SURGICAL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System Midfoot Fusion Plate SURGICAL TECHNIQUE ORTHOLOC Foot Reconstruction System Midfoot Fusion Plate SURGICAL TECHNIQUE Surgeon Design Team The ORTHOLOC 3Di Foot Reconstruction
ORTHOLOC 3Di Foot Reconstruction System Midfoot Fusion Plate SURGICAL TECHNIQUE ORTHOLOC Foot Reconstruction System Midfoot Fusion Plate SURGICAL TECHNIQUE Surgeon Design Team The ORTHOLOC 3Di Foot Reconstruction
Surgical Technique. Forearm Fracture Solutions
 Surgical Technique Forearm Fracture Solutions Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve
Surgical Technique Forearm Fracture Solutions Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve
UltOS Foot Plating System
 UltOS Foot Plating System One System. Multiple Options. Design Rationale & Surgical Technique ORS5539_Ultos_A4.indd 1 12/10/2015 11:59 UltOS Foot Plating System Design Rationale Plate and Screws Low Profile
UltOS Foot Plating System One System. Multiple Options. Design Rationale & Surgical Technique ORS5539_Ultos_A4.indd 1 12/10/2015 11:59 UltOS Foot Plating System Design Rationale Plate and Screws Low Profile
Olecranon Locking Plate II
 INDEX Indications Patient Position Fracture Reduction and Fixation Surgical Technique Step 1 Surgical Approach Step 2 Implantation Step 3 Proximal Locking Screw Insertion Step 4 Distal Screw Insertion
INDEX Indications Patient Position Fracture Reduction and Fixation Surgical Technique Step 1 Surgical Approach Step 2 Implantation Step 3 Proximal Locking Screw Insertion Step 4 Distal Screw Insertion
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
MetaFix Ludloff Plate
 Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM
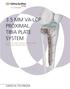 3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM Part of the DePuy Synthes Variable Angle Periarticular Plating System SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION 3.5 mm VA-LCP Proximal Tibial Plate 2 AO
3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM Part of the DePuy Synthes Variable Angle Periarticular Plating System SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION 3.5 mm VA-LCP Proximal Tibial Plate 2 AO
The Flower Forefoot PROCEDURE GUIDE.
 The Flower Forefoot PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION T-PLATE, OBLIQUE MTP
The Flower Forefoot PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION T-PLATE, OBLIQUE MTP
System. Humeral Nail. Surgical Technique
 System Humeral Nail Surgical Technique Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL
System Humeral Nail Surgical Technique Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL
Locking Ankle Plating System. Surgical Technique
 Locking Ankle Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Locking Ankle Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Surgical Technique. Calcaneal Locking Plate
 Surgical Technique Calcaneal Locking Plate PERI-LOC Locked Plating System Calcaneal Locking Plate Surgical TechniqueCatalog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Surgical Technique Calcaneal Locking Plate PERI-LOC Locked Plating System Calcaneal Locking Plate Surgical TechniqueCatalog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Correction System. Surgical Technique
 Re+Line Bunion Correction System Surgical Technique Bunion Correction System Easy insertion and medial placement accuracy using Landmark Guide technology Greater and repeatable uniform compression across
Re+Line Bunion Correction System Surgical Technique Bunion Correction System Easy insertion and medial placement accuracy using Landmark Guide technology Greater and repeatable uniform compression across
LCP Distal Tibia Plate
 Surgical Technique LCP Locking Compression Plate Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF Table of contents Indications 3 Implants/Instruments 5 Surgical
Surgical Technique LCP Locking Compression Plate Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF Table of contents Indications 3 Implants/Instruments 5 Surgical
Femur. Monoaxial Locking Plate System. Operative Technique. Distal Lateral Femur Universal Holes Targeting Instrumentation.
 Femur AxSOS 3 Titanium Monoaxial Locking Plate System Femur Fractures Operative Technique Distal Lateral Femur Universal Holes Targeting Instrumentation This publication sets forth detailed recommended
Femur AxSOS 3 Titanium Monoaxial Locking Plate System Femur Fractures Operative Technique Distal Lateral Femur Universal Holes Targeting Instrumentation This publication sets forth detailed recommended
Integra. DigiFuse Cannulated Intramedullary Fusion System SURGICAL TECHNIQUE
 Integra DigiFuse Cannulated Intramedullary Fusion System SURGICAL TECHNIQUE Table of Contents Design Rationale... 2 System Features... 2 Indications... 2 Contraindications... 2 Surgical Technique...3 Step
Integra DigiFuse Cannulated Intramedullary Fusion System SURGICAL TECHNIQUE Table of Contents Design Rationale... 2 System Features... 2 Indications... 2 Contraindications... 2 Surgical Technique...3 Step
Technique Guide. 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system.
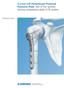 Technique Guide 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Proximal Humerus Plate 2 AO Principles
Technique Guide 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Proximal Humerus Plate 2 AO Principles
2.4 mm Variable Angle LCP Intercarpal Fusion System. Variable angle locking technology for mediocarpal partial arthrodesis.
 2.4 mm Variable Angle LCP Intercarpal Fusion System. Variable angle locking technology for mediocarpal partial arthrodesis. Technique Guide Instruments and implants approved by the AO Foundation Table
2.4 mm Variable Angle LCP Intercarpal Fusion System. Variable angle locking technology for mediocarpal partial arthrodesis. Technique Guide Instruments and implants approved by the AO Foundation Table
SALVATION 3Di. Plating System SURGICAL TECHNIQUE
 SALVATION 3Di Plating System SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Intended use 5 Indications 5 Contraindications Chapter 3 6 Device Description Chapter 4 7 Preoperative Planning
SALVATION 3Di Plating System SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Intended use 5 Indications 5 Contraindications Chapter 3 6 Device Description Chapter 4 7 Preoperative Planning
3.5 mm LCP Extra-articular Distal Humerus Plate
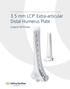 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Extra-articular Distal Humerus Plate Surgical Technique Table of Contents Introduction 3.5 mm LCP Extra-articular Distal Humerus
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Extra-articular Distal Humerus Plate Surgical Technique Table of Contents Introduction 3.5 mm LCP Extra-articular Distal Humerus
TIBIAXYS ANKLE FUSION
 TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
Surgical Technique. Distal Humerus Locking Plate
 Surgical Technique Distal Humerus Locking Plate PERI-LOC Locked Plating System Distal Humerus Locking Plate Surgical Technique Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Surgical Technique Distal Humerus Locking Plate PERI-LOC Locked Plating System Distal Humerus Locking Plate Surgical Technique Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments
 Part of the 3.5 mm LCP 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments Surgical Technique TABLE OF CONTENTS INTRODUCTION 3.5 mm LCP Low Bend Medial Distal Tibia Plate 2 Aiming Instruments
Part of the 3.5 mm LCP 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments Surgical Technique TABLE OF CONTENTS INTRODUCTION 3.5 mm LCP Low Bend Medial Distal Tibia Plate 2 Aiming Instruments
Low Bend Distal Tibia Plates
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Low Bend Medial Distal Tibia Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Low Bend Medial Distal Tibia Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia
Technique Guide. 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot.
 Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
WINSTA-C. Clavicle Plating System
 Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
Surgical Technique. Lower Extremity Plates and Straight Plates
 Surgical Technique Lower Extremity Plates and Straight Plates 2 Table of contents Overview...4 Indications... 4 Contraindications... 4 Screw Options... 5 Straight Plate Options... 6 Proximal Tibia Plate
Surgical Technique Lower Extremity Plates and Straight Plates 2 Table of contents Overview...4 Indications... 4 Contraindications... 4 Screw Options... 5 Straight Plate Options... 6 Proximal Tibia Plate
