Ultrasound Evaluation of Morton Neuroma Before and After Laser Therapy
|
|
|
- Rosanna Kennedy
- 6 years ago
- Views:
Transcription
1 Musculoskeletal Imaging Original Research Gimber et al. Ultrasound of Morton Neuroma Musculoskeletal Imaging Original Research Lana H. Gimber 1 David M. Melville 1 Darin A. Bocian 2 Elizabeth A. Krupinski 3 Matthew P. Del Guidice 1 Mihra S. Taljanovic 1 Gimber LH, Melville DM, Bocian D, Krupinski EA, Del Guidice MP, Taljanovic MS Keywords: laser therapy, metatarsalgia, Morton neuroma, ultrasound DOI: /AJR Received March 1, 2016; accepted after revision August 9, Based on a presentation at the Radiological Society of North America 2015 annual meeting, Chicago, IL, and on a presentation at the Society of Skeletal Radiology 2016 annual meeting, New Orleans, LA. 1 Department of Medical Imaging, University of Arizona Health Sciences Center, 1501 N Campbell Ave, Tucson, AZ Address correspondence to M. S. Taljanovic (mihrat@radiology.arizona.edu) 2 Department of Surgery, University of Arizona Health Sciences Center, Tucon, AZ. 3 Department of Radiology and Imaging Sciences, Emory University, Atlanta, GA. AJR 2017; 208: X/17/ American Roentgen Ray Society Ultrasound Evaluation of Morton Neuroma Before and After Laser Therapy OBJECTIVE. The objective of our study was to retrospectively assess for differences in imaging appearances of Morton neuromas before and after laser therapy using diagnostic ultrasound (US). MATERIALS AND METHODS. A retrospective review was performed to identify patients who underwent US imaging to evaluate for Morton neuroma during the study period (June 1, 2013 July 1, 2014); of the 42 patients identified, 21 underwent US evaluations before and after laser therapy. US reports and images were reviewed and correlated with clinical history. The final study group consisted of 21 patients who had a total of 31 Morton neuromas evaluated using US after treatment. A retrospective review was then performed to characterize the appearances of these lesions before and after therapy followed by an analysis of variables. RESULTS. Retrospective US review of 31 pretreatment Morton neuromas showed fusiform, heterogeneously hypoechoic masses with well-defined borders in most cases and that pain was reported when transducer pressure was applied in 97% (30/31) of cases. After treatment, lesions showed ill-defined borders (23/31), and pain with application of transducer pressure was either significantly decreased or absent (29/31); these findings were concordant with the clinical findings. Both of these characteristics were statistically significant (p < ). In addition, more Morton neuromas occurred in the second intermetatarsal space than in the third intermetatarsal space (p < ). CONCLUSION. US may be used to identify posttreatment changes after laser therapy of Morton neuromas. Posttreatment changes include ill-defined borders and less pain or the absence of pain with the application of transducer pressure. These criteria may be applied in future clinical studies evaluating the efficacy of laser therapy for Morton neuroma. M orton neuroma results from the nonneoplastic fusiform enlargement of the plantar digital nerve and is not a true neuroma; rather, Morton neuroma consists of edema, perineural fibrosis, axonal degeneration, and local vascular proliferation at the level of the metatarsal heads just plantar to the intermetatarsal ligament [1, 2]. This lesion is a common cause of forefoot pain, which manifests as metatarsalgia. Pain radiates from the midfoot to the toes and may be associated with the Tinel sign (i.e., light percussion over the nerve elicits a sensation of tingling or pins and needles in the distribution of the nerve) and the Mulder sign (a palpable click elicited by squeezing the metatarsal heads together with one hand while concomitantly putting pressure on the interdigital space with the other hand) [3]. Morton neuromas may be multiple and bilateral and, according to the literature, occur most commonly at the third intermetatarsal space [4]. Although clinical examination remains the diagnostic reference standard for Morton neuroma [5], evaluations with ultrasound (US) and MRI have been shown to be useful for the diagnosis and preoperative localization of Morton neuroma, particularly when lesions are multiple or the presentation is atypical [2, 6]. Previous studies have found that large Morton neuromas (> 5 mm) are more likely to be symptomatic and are more commonly treated surgically than small Morton neuromas [7]. A variety of therapeutic approaches are available for the treatment of symptomatic Morton neuromas beginning with conservative measures, such as footwear modification and steroid injections, followed by more invasive methods, including ultrasound-guided cryoneurolysis, radiofrequency or alcohol ablation with progression to digital neurecto- 380 AJR:208, February 2017
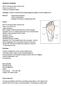
2 Ultrasound of Morton Neuroma my, percutaneous osteotomy, and intermetatarsal ligament release for refractory lesions [5, 8 11]. We have seen increasing US referrals for pretreatment diagnosis and posttreatment follow-up of Morton neuromas before and after high-intensity laser therapy (HILT). HILT has not been previously reported, to our knowledge, as a treatment method for Morton neuroma in the English-language literature. Currently, HILT has been approved by the U.S. Food and Drug Administration for the treatment of various skin lesions, hair removal, tattoo removal, and onychomycosis but not for the treatment of Morton neuroma. The purpose of our study was to retrospectively determine the differences in US appearances of Morton neuromas before and after HILT. Materials and Methods Institutional review board approval was obtained, and informed consent was waived. Musculoskeletal US case logs from June 1, 2013, through July 1, 2014, were searched to identify patients who underwent US for evaluation of Morton neuroma. Medical records, including other correlative imaging findings and clinical history, were reviewed. The initial review of musculoskeletal US case logs identified 42 patients who underwent forefoot US for suspected Morton neuroma and 21 patients who underwent US evaluations before and after HILT. The inclusion criteria for the HILT procedure were the presence of symptomatic Morton neuroma that had been confirmed with a baseline diagnostic US examination. Conservative treatment of Morton neuroma in these patients had failed. The exclusion criteria were prior surgery for Morton neuroma or A C the presence of peripheral or diabetic neuropathy. A follow-up diagnostic US examination was performed to evaluate for imaging changes seen after laser treatment. The decision to use HILT to treat symptomatic Morton neuromas in our patients was based on the safety, effectiveness, and clinical applications of a neodymium:yttrium-aluminumgarnet (Nd:YAG) laser (GenesisPlus, Cutera). In our patients, the HILT treatment of Morton neuroma was performed as a series of 10 treatments once a week in an office setting after informed consent was obtained. The procedures were performed in a designated laser treatment room. Protective glasses were worn by the treating physician. The lesions were localized under US guidance. The procedures were performed without anesthesia. A topical compounded medication containing verapamil 15%, pentoxifylline Fig year-old man with metatarsalgia at second interspace who underwent high-intensity laser therapy (HILT) for treatment of Morton neuroma. A and B, Gray-scale short-axis (transverse) (A) and long-axis (B) ultrasound (US) images obtained before HILT show round hypoechoic lesion between second (MT 2) and third (MT 3) metatarsal heads with well-defined borders (arrows). In real-time ultrasound examination, lesion was seen in continuity with digital plantar nerve. C and D, Gray-scale transverse (C) and long-axis (D) US images obtained after HILT show round hypoechoic lesion in similar position with ill-defined borders (arrows) relative to adjacent soft tissues. In D, cursors and 1 indicate calipers for measurement of lesion. MT 2 = second metatarsal head, MT 3 = third metatarsal head. B D AJR:208, February
3 Gimber et al. 3%, and tranilast 1% was applied directly to the area demarcated at the location of the neuroma at the plantar aspect of the foot. HILT was performed using a Nd:YAG laser with the following parameters: fluence, 15 J/cm 2 ; pulse width, 0.3 ms; and repetition rate, 7 Hz. Laser energy (total = 1000 pulses) was directed at the lesion site. The laser treatment was briefly interrupted to allow gentle massage of the area and was then immediately resumed until a total of 1000 pulses had been delivered to the site. During the HILT treatment, all patients experienced little to no discomfort throughout the entire procedure. The patients were allowed to return to normal shoe gear and to resume normal activities as tolerable. Tight shoes (high heels) are not allowed during the course of the 10-week treatment. US examinations were performed as part of routine clinical practice at our institution on a US machine with a high-resolution 8-18 MHz multifrequency linear hockey stick transducer (Logiq E9, GE Healthcare) by a musculoskeletal US technologist. US examinations performed after HILT were performed by a fellowship-trained musculoskeletal radiologist. US examinations were performed with the patient supine, and evaluations of all intermetatarsal spaces were performed using a plantar approach as described by Quinn and collaborators [2]. We also examined the adjacent plantar plates and flexor tendons to exclude other abnormalities that could cause pain in the same region. Equal pressure was applied on the dorsal aspect of the imaged intermetatarsal head space from the sonographer s nonimaging finger to assist in visualization by splaying the metatarsals. Imaging from the dorsal aspect of the intermetatarsal head spaces was not performed. Liberal sonographic transmission gel was used in place of a standoff pad. Dynamic US imaging was performed to assess for the Mulder sign and to evaluate for reproducible pain during application of transducer pressure. Gray-scale images were acquired in the transverse (short axis) and longitudinal (long axis) planes relative to the metatarsal shafts, perpendicular to and in the plane of the plantar digital nerve, respectively, with routine use of color and power Doppler imaging. Static images and cine clips were stored on the department s PACS. A retrospective consensus review of the US images of the final study group was then performed by two fellowship-trained musculoskeletal radiologists (3 and 20 years of experience). Static and cine images were reviewed, and each pretreatment Morton neuroma was evaluated for size, location, echogenicity, echotexture, overall shape (round or fusiform), borders (well defined or ill defined), hyperemia, presence of bursa, presence of pain with transducer pressure, and presence of Mulder sign. Each posttreatment Morton neuroma was also reviewed with attention to these same parameters. These data were then evaluated to determine whether any of the US variables permitted differentiation of pretreatment Morton neuroma from posttreatment Morton neuroma. Chi-square tests were used for all categoric variables. Results The final study group of 21 subjects consisted of 81% women (17/21) and 19% men (4/21) with an average age of 62.5 years (range, years). The right foot was involved in 38% (8/21), the left foot in 48% (10/21), and both feet in 14% (3/21). A total of 31 Morton neuromas were treated, including 12 left foot lesions and 19 right foot lesions. Of the treated lesions, 77% (24/31) were located in the second intermetatarsal space and the remaining 23% (7/31) were located in the third intermetatarsal space, which was a statistically significant difference (p < ). Retrospective review of the initial US studies of Morton neuromas (Table 1) showed the average lesion size before treatment was 4.1 mm (range, mm). All lesions were heterogeneously hypoechoic with fusiform shape in 97% (30/31) (Figs. 1 and 2). There was associated pain with transducer pressure in 97% of lesions (30/31). The lesion borders were well defined in 87% of cases and ill defined in the remaining 13%. There was TABLE 1: Ultrasound Characteristics of Morton Neuromas Before and After High-Intensity Laser Therapy (HILT) Ultrasound Characteristics Before HILT After HILT Lesion size (mm) Average Range Lesion size after HILT a Stable 48 (14/29) Decreased 59 (17/29) Pain Moderate to severe 97 (30/31) 6 (2/31) Mild 0 (0/31) 13 (4/31) Absent 3 (1/31) 81 (25/31) Echogenicity Hypoechoic 100 (31/31) 100 (29/29) Echotexture Heterogeneous 100 (31/31) 100 (29/29) Shape Round 3 (1/31) 14 (4/29) Fusiform 97 (30/31) 86 (25/29) Borders Well defined 87 (27/31) 28 (8/29) Ill defined 13 (4/31) 72 (21/29) Hyperemia Absent 0 (0/31) 0 (0/31) Mulder sign Present 3 (1/31) 0 (0/29) Absent 97 (30/31) 100 (29/29) Associated bursa Present 10 (3/31) 0 (0/31) Absent 90 (28/31) 100 (31/31) Note All results except size data are presented as % (no. of cases / total no. of cases). a Two lesions were not seen on ultrasound after HILT. 382 AJR:208, February 2017
4 Ultrasound of Morton Neuroma no evidence of lesion hyperemia on color or power Doppler imaging. A positive Mulder sign was present in only 3% (1/31) with an associated intermetatarsal bursa in 10% (3/31) (Figs. 2A and 2B). The average time from initial US to treatment completion was 103 days (range, days). The average time from treatment to follow-up US was 51 days (range, days). Review of posttreatment images revealed persistently visible lesions in 94% (29/31) and nonvisualization in 6% (2/31). Lesion size decreased in 59% (17/29) and remained stable in 48% (14/29). All visualized posttreatment lesions remained heterogeneously hypoechoic; 86% of posttreatment lesions were fusiform and 14% were round. In addition, 72% of lesions had ill-defined borders TABLE 2: Analysis of Ultrasound (US) Findings Before and After High-Intensity Laser Therapy of Morton Neuroma US Findings A C Statistical Results Change in lesion size 1.03 Pain with transducer pressure < a Echogenicity 0 Echotexture 0 Shape 4.30 < 0.05 a Borders < a Hyperemia 0 Mulder sign 1.03 Associated bursa 5.16 < 0.05 a a Statistically significant. Fig year-old woman with right foot metatarsalgia at second interspace who underwent high-intensity laser therapy (HILT) for treatment of Morton neuroma. A and B, Gray-scale short-axis (transverse) (A) and long-axis (B) ultrasound (US) images obtained before HILT during positive Mulder test show hypoechoic lesion (arrows) arising between second (MT 2) and third (MT 3) metatarsal heads surrounded by hypoechoic bursal fluid (arrowheads, A); these findings are consistent with Morton neuroma and associated bursitis. In real-time US examination, lesion was seen in continuity with digital plantar nerve. C and D, Gray-scale short-axis transverse (C) and long-axis (D) US images obtained after HILT show smaller hypoechoic lesion in same location (arrows) without surrounding bursal fluid; these findings are consistent with posttreatment changes. On follow-up study, Mulder test was negative. In C, MT 2 indicates second metatarsal head; MT 3, third metatarsal head; cursors and I and 2 indicate calipers for measurement of lesion. In D, cursors and 1 indicate calipers for measurement of lesion. χ 2 p B D AJR:208, February
5 Gimber et al. (21/29) (Figs. 1C and 1D), whereas 28% remained well defined (8/29). There was no bursa, Mulder sign, or Doppler signal associated with any of the treated lesions. Pain with transducer pressure resolved in 81% (25/31) of lesions and decreased to mild in 13% (4/31); moderate to severe pain persisted in only 6% (2/31) of lesions. Additionally, all patients who did not have pain with transducer pressure on follow-up US studies reported complete resolution of pain including with weight-bearing and ambulation. Likewise, patients who had decreased or persistent pain with transducer pressure on posttreatment follow-up US studies reported pain with weight-bearing and ambulation. When comparing the US findings of preand post-hilt lesions (Table 2), there were significant differences (p < 0.05) with regard to the presence of pain and bursa and to lesion borders and shape (Fig. 1). In general, posttreatment lesions were associated with decreased pain and showed ill-defined lesion borders; some posttreatment lesions transitioned from fusiform to round shape, and associated bursa, when present, resolved in some cases (Figs. 2C and 2D). Aside from mild osteoarthritis at the adjacent metatarsophalangeal joints, no additional findings, including plantar plate injuries or tendon abnormalities, were noted to suggest an alternative cause of metatarsalgia in our patients. Discussion US has been identified as the most cost-effective and accurate imaging method for diagnosing Morton neuroma [6, 12]. The results of our retrospective study showed that decreased pain with transducer pressure and ill-defined margins were characteristic US features of most Morton neuromas after HILT. The diagnosis of metatarsalgia due to Morton neuroma requires the exclusion of alternate diagnoses and accurate localization of the symptomatic plantar digital nerves, which can be confounded by lesion multiplicity and small size. Although a transverse diameter of 5 mm has been established to identify Morton neuromas that are likely symptomatic, Bencardino et al. [13] discovered a significant overlap in the sizes of symptomatic and asymptomatic Morton neuromas on MRI and recommended careful clinical correlation. Mahadevan et al. [14] found no correlation between the size of Morton neuroma on US and positive clinical examination findings except the Mulder sign. US permits dynamic assessment of the lesion and allows investigation of the pain source, including evaluation for Mulder signal and correlation for pain with applied transducer pressure [12]. Pain with transducer pressure was present in all but one of the lesions identified before treatment; however, the average size of the treated lesions was 4.1 mm, and only one lesion measuring 12.0 mm showed the Mulder sign. Real-time US examination allows the effective identification of smaller symptomatic Morton neuromas that may benefit from treatment. Real-time US examination may be particularly useful in identifying symptomatic lesions that are too small to necessitate aggressive operative intervention but that may benefit from a less invasive treatment such as HILT. In all treated lesions, no alternative cause of metatarsalgia was identified on US, including tendon abnormalities and plantar plate tears. Although it has been theorized that a thicker third intermetatarsal nerve formed by the medial and lateral plantar nerves leads to more frequent entrapment and purportedly results in most neuromas occurring in the third intermetatarsal space, other studies have found that other intermetatarsal spaces may be involved, including the second intermetatarsal space [13, 15, 16], which was the most common site in our study. After diagnosis and conservative measures, many Morton neuromas are treated by excision of the plantar digital nerve, often through a dorsal approach; however, up to 20 30% of these patients experience recurrent symptoms [17, 18]. Surgical failures have been attributed to recurrent neuroma formation, symptomatic stump neuroma, scar tissue, or inadequate resection [10]. Postsurgical MRI for recurrent metatarsalgia can reveal neuromalike fibrosis and an increased prevalence of intermetatarsal bursitis in symptomatic patients [19]. In a study of 58 consecutive patients undergoing MRI after neuroma resection, prospectively diagnosed recurrent neuromas in seven patients were found to be fibrotic scar without nerve tissue [20]. To date, no studies have detailed the postsurgical US findings after plantar digital nerve excision. After surgical excision, pain may also persist because of referred symptoms secondary to additional neuromas in adjacent intermetatarsal spaces because most surgeons attempt to avoid excising neuromas in adjacent webspaces [11]. Less invasive methods such as HILT and radiofrequency ablation can be used pre- or postoperatively to address small adjacent neuromas identified on US, thus reducing the risk for recurrent symptoms. Less invasive nonsurgical approaches attempt to reduce the risk of painful scar formation by minimizing impact on adjacent soft tissues; however, all less invasive treatment methods, including ethanol ablation, radiofrequency ablation, cryoablation, and steroid injection, are believed to alter the relationship of the digital plantar nerve with the surrounding soft tissues. Chuter et al. [11] addressed concerns about perilesion scar formation after radiofrequency ablation impacting future surgical intervention by sharing the surgical observation that posttreatment lesions were firm, scarred, or adherent but remained identifiable without apparent effect on operating time or outcome. After HILT was performed to treat Morton neuroma in our patients, all but two Morton neuromas remained identifiable on US and showed similar echogenicity and echotexture; however, most lesions developed ill-defined borders with the adjacent soft tissues, which is suggestive of scar forming around the treated lesion. There was no evidence of masslike scar surrounding the treated lesions, which could predispose to recurrent impingement or entrapment. Because none of the lesions in our study progressed to excision, the presence of scar tissue around the treated lesion could not be confirmed. Overall, there was no significant interval change in size between the pre- and post-hilt lesions. This finding differs from a report of US findings after ethanol ablation of Morton neuromas that showed a 30% decrease in the size of the neuromas [9]. Although US has also been used to guide cryoneurolysis with a reported 75% positive response rate, no studies have been performed to date to assess the posttreatment US appearance. The characteristic US appearance of Morton neuroma is a well-defined hypoechoic intermetatarsal mass in continuity with the digital plantar nerve that may be associated with an adjacent intermetatarsal bursa [2]. In our study, a bursa was associated with only three lesions before treatment, and the presence of a bursa may reflect a relationship between the size of the neuroma and the presence of bursal fluid; however, a prior study by Zanetti et al. [21] found no statistically significant correlation between fluid in the intermetatarsal bursa and Morton neuroma in the first and second intermetatarsal spaces on MRI. In our study, all intermetatarsal bursae resolved after treatment, and no lesions showed interval development of bursal fluid. These US findings are similar to previously reported MRI find- 384 AJR:208, February 2017
6 Ultrasound of Morton Neuroma ings after Morton neuroma resection in which bursitis was seen in only 9% of asymptomatic patients as opposed to 27% of patients with recurrent symptoms [20]. Dynamic US examination can reveal the presence of the Mulder sign, and the US transducer may be used to elicit pain at the site of the abnormality. Pain was absent or had lessened after HILT in all lesions except two; these findings emphasize the importance of both the posttreatment clinical examination and real-time assessment for pain during US. There are several limitations to this study. This study was retrospective and included fewer than 50 patients undergoing US evaluation. The retrospective review of the US images was limited to what was initially imaged prospectively and is subject to inter- and intraobserver variability. A selection bias existed because all patients were referred for evaluation of suspected Morton neuroma, and all patients with symptomatic Morton neuromas underwent treatment with HILT. No additional alternative treatment methods were imaged after intervention, and no pathologic correlation was available. In addition, the pre- and post-hilt clinical pain assessments were not standardized. The patients were imaged in a short-term follow-up interval after HILT, and no long-term follow-up imaging was performed. Additionally, there was no control group in our study. In conclusion, US can be used to identify posttreatment changes after HILT for Morton neuroma. These changes consist of illdefined lesion borders, a transition in lesion shape from round to fusiform, the resolution of bursa, and resolution or decrease in pain with transducer pressure. The resolved or decreased pain with transducer pressure emphasizes the importance of physical examination findings over imaging features for posttreatment follow-up. Additional prospective studies with long-term imaging follow-up after HILT would be helpful to determine whether the ill-defined lesion borders are a transient treatment effect and to assess whether symptomatic improvement persists. References 1. Shereff MJ, Grande DA. Electron microscopic analysis of the interdigital neuroma. Clin Orthop Relat Res 1991; 271: Quinn TJ, Jacobson JA, Craig JG, van Holsbeeck MT. Sonography of Morton s neuromas. AJR 2000; 174: Pastides P, El-Sallakh S, Charalambides C. Morton s neuroma: a clinical versus radiological diagnosis. Foot Ankle Surg 2012; 18: Shapiro PP, Shapiro SL. Sonographic evaluation of interdigital neuromas. Foot Ankle Int 1995; 16: Kasparek M, Schneider W. Surgical treatment of Morton s neuroma: clinical results after open excision. Int Orthop 2013; 37: Bignotti B, Signori A, Sormani MP, Molfetta L, Martinoli C, Tagliafico A. Ultrasound versus magnetic resonance imaging for Morton neuroma: systematic review and meta-analysis. Eur Radiol 2015; 25: Zanetti M, Strehle JK, Kundert HP, Zollinger H, Hodler J. Morton neuroma: effect of MR imaging findings on diagnostic thinking and therapeutic decisions. Radiology 1999; 213: Friedman T, Richman D, Adler R. Sonographically guided cryoneurolysis: preliminary experience and clinical outcomes. J Ultrasound Med 2012; 31: Hughes RJ, Ali K, Jones H, Kendall S, Connell DA. Treatment of Morton s neuroma with alcohol injection under sonographic guidance: follow-up of 101 cases. AJR 2007; 188: Bauer T, Gaumetou E, Klouche S, Hardy P, Maffulli N. Metatarsalgia and Morton s disease: comparison of outcomes between open procedure and neurectomy versus percutaneous metatarsal osteotomies and ligament release with a minimum of 2 years of follow-up. J Foot Ankle Surg 2015; 54: Chuter GS, Chua YP, Connell DA, Blackney MC. Ultrasound-guided radiofrequency ablation in the management of interdigital (Morton s) neuroma. Skeletal Radiol 2013; 42: Xu Z, Duan X, Yu X, Wang H, Dong X, Xiang Z. The accuracy of ultrasonography and magnetic resonance imaging for the diagnosis of Morton s neuroma: a systematic review. Clin Radiol 2015; 70: Bencardino J, Rosenberg ZS, Beltran J, Liu X, Marty-Delfaut E. Morton s neuroma: is it always symptomatic? AJR 2000; 175: Mahadevan D, Venkatesan M, Bhatt R, Bhatia M. Diagnostic accuracy of clinical tests for Morton s neuroma compared with ultrasonography. J Foot Ankle Surg 2015; 54: Mendicino SS, Rockett MS. Morton s neuroma: update on diagnosis and imaging. Clin Podiatr Med Surg 1997; 14: Terk MR, Kwong PK, Suthar M, Horvath BC, Colletti PM. Morton neuroma: evaluation with MR imaging performed with contrast enhancement and fat suppression. Radiology 1993; 189: Bradley N, Miller WA, Evans JP. Plantar neuroma: analysis of results following surgical excision in 145 patients. South Med J 1976; 69: Ruuskanen MM, Niinimäki T, Jalovaara P. Results of the surgical treatment of Morton s neuralgia in 58 operated intermetatarsal spaces followed over 6 (2 12) years. Arch Orthop Trauma Surg 1994; 113: Zanetti M, Saupe N, Espinosa N. Postoperative MR imaging of the foot and ankle: tendon repair, ligament repair, and Morton s neuroma resection. Semin Musculoskelet Radiol 2010; 14: Espinosa N, Schmitt JW, Saupe N, et al. Morton neuroma: MR imaging after resection postoperative MR and histologic findings in asymptomatic and symptomatic intermetatarsal spaces. Radiology 2010; 255: Zanetti M, Strehle JK, Zollinger H, Hodler J. Morton neuroma and fluid in the intermetatarsal bursae on MR images of 70 asymptomatic volunteers. Radiology 1997; 203: AJR:208, February
Morton s Neuroma: Is It Always Symptomatic?
 Jenny Bencardino 1 Zehava S. Rosenberg 2 Javier Beltran 3 Xiang Liu 4 Emmanuelle Marty-Delfaut 2 Received August 5, 1999; accepted after revision February 16, 2000. 1 Department of Radiology, Massachusetts
Jenny Bencardino 1 Zehava S. Rosenberg 2 Javier Beltran 3 Xiang Liu 4 Emmanuelle Marty-Delfaut 2 Received August 5, 1999; accepted after revision February 16, 2000. 1 Department of Radiology, Massachusetts
Treatment of Morton s Neuroma with Alcohol Injection Under Sonographic Guidance: Follow-Up of 101 Cases
 Alcohol Injection to Treat Morton s Neuroma Musculoskeletal Imaging Original Research Richard J. Hughes 1 Kaline Ali 1 Hugh Jones 2 Sue Kendall 3 David A. Connell 1 Hughes RJ, Ali K, Jones H, Kendall S,
Alcohol Injection to Treat Morton s Neuroma Musculoskeletal Imaging Original Research Richard J. Hughes 1 Kaline Ali 1 Hugh Jones 2 Sue Kendall 3 David A. Connell 1 Hughes RJ, Ali K, Jones H, Kendall S,
Ultrasound-guided Treatment of Morton's Syndrome: comparison among three different injection techniques
 Ultrasound-guided Treatment of Morton's Syndrome: comparison among three different injection techniques Poster No.: C-1701 Congress: ECR 2015 Type: Scientific Exhibit Authors: D. Orlandi, C. Messina, A.
Ultrasound-guided Treatment of Morton's Syndrome: comparison among three different injection techniques Poster No.: C-1701 Congress: ECR 2015 Type: Scientific Exhibit Authors: D. Orlandi, C. Messina, A.
Ultrasound-guided Radiofrequency Ablation of Morton's Neuroma
 Ultrasound-guided Radiofrequency Ablation of Morton's Neuroma Poster No.: P-0044 Congress: ESSR 2016 Type: Authors: Keywords: DOI: Scientific Poster R. Mazzetti, A. Cosentino, F. Gobbi, D. Righi, G. Gandini;
Ultrasound-guided Radiofrequency Ablation of Morton's Neuroma Poster No.: P-0044 Congress: ESSR 2016 Type: Authors: Keywords: DOI: Scientific Poster R. Mazzetti, A. Cosentino, F. Gobbi, D. Righi, G. Gandini;
Why? Ultrasound of the Foot. Ultrasound of the Foot. General Rules. Plantar Fascia. Plantar Fasciitis 18/09/2018
 Ultrasound of the Foot Why? Ultrasound of the Foot Plantar fasciitis Plantar fascia fibromatosis Morton s neuroma Intermetatarsal bursitis Adventitial bursitis Plantar plate tears MTP joint synovitis Ganglia
Ultrasound of the Foot Why? Ultrasound of the Foot Plantar fasciitis Plantar fascia fibromatosis Morton s neuroma Intermetatarsal bursitis Adventitial bursitis Plantar plate tears MTP joint synovitis Ganglia
Corporate Medical Policy
 Corporate Medical Policy Ablation Procedures for Peripheral Neuromas and Peripheral Nerves File Name: Origination: Last CAP Review: Next CAP Review: Last Review: ablation_procedures_for_peripheral_neuromas_and_peripheral_nerves
Corporate Medical Policy Ablation Procedures for Peripheral Neuromas and Peripheral Nerves File Name: Origination: Last CAP Review: Next CAP Review: Last Review: ablation_procedures_for_peripheral_neuromas_and_peripheral_nerves
Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve. Lumbar radiculopathy Instability MTPJ joint or inflammatory MPJ
 MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma)
 A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma) The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of two specialist
A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma) The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of two specialist
Commonly Missed Foot and Ankle Conditions. David Miller, DPM AMG Podiatry
 Commonly Missed Foot and Ankle Conditions David Miller, DPM AMG Podiatry Lisfranc Injuries Wide spectrum of injuries High energy Subtle subluxation which could be easily missed injuries Men are 2-4x s
Commonly Missed Foot and Ankle Conditions David Miller, DPM AMG Podiatry Lisfranc Injuries Wide spectrum of injuries High energy Subtle subluxation which could be easily missed injuries Men are 2-4x s
Anatomy 1% 29% 64% 6%
 Mortons Neuroma Perineural fibrosis of the plantar digital nerve Females 8-10 3 rd plantar webspace most commonly effected Burning pain Sensory changes 3&4 digits / interdigital space Etiology Excessive
Mortons Neuroma Perineural fibrosis of the plantar digital nerve Females 8-10 3 rd plantar webspace most commonly effected Burning pain Sensory changes 3&4 digits / interdigital space Etiology Excessive
fitting shoes, or repetitive stress. It also frequently arises from unknown causes.
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Morton's Neuroma Morton's Neuroma, also sometimes referred to as plantar Neuroma or intermetatarsal Neuroma,
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Morton's Neuroma Morton's Neuroma, also sometimes referred to as plantar Neuroma or intermetatarsal Neuroma,
MRI and ultrasonography in Morton s neuroma: Diagnostic accuracy and correlation
 Original Article MRI and ultrasonography in Morton s neuroma: Diagnostic accuracy and correlation Torres-Claramunt R, Ginés A, Pidemunt G, Puig Ll, de Zabala S Abstract Background: The diagnosis of Morton
Original Article MRI and ultrasonography in Morton s neuroma: Diagnostic accuracy and correlation Torres-Claramunt R, Ginés A, Pidemunt G, Puig Ll, de Zabala S Abstract Background: The diagnosis of Morton
RECURRENT INTERMETATARSAL NEUROMA
 4 th Foot & Ankle Symposium RECURRENT INTERMETATARSAL NEUROMA Martin Berli, MD Department of Prosthetics and Orthotics Uniklinik Balgrist, Zurich martin.berli@balgrist.ch Recurrence: General Topics Pain
4 th Foot & Ankle Symposium RECURRENT INTERMETATARSAL NEUROMA Martin Berli, MD Department of Prosthetics and Orthotics Uniklinik Balgrist, Zurich martin.berli@balgrist.ch Recurrence: General Topics Pain
Peripheral Nerve Ultrasound
 Peripheral Nerve Ultrasound Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Normal Peripheral Nerve Ultrasound appearance: Hypoechoic
Peripheral Nerve Ultrasound Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Normal Peripheral Nerve Ultrasound appearance: Hypoechoic
Ultrasound-guided radiofrequency ablation in the management of interdigital (Morton s) neuroma
 Skeletal Radiol (2013) 42:107 111 DOI 10.1007/s00256-012-1527-x SCIENTIFIC ARTICLE Ultrasound-guided radiofrequency ablation in the management of interdigital (Morton s) neuroma Graham S. J. Chuter & Yeok
Skeletal Radiol (2013) 42:107 111 DOI 10.1007/s00256-012-1527-x SCIENTIFIC ARTICLE Ultrasound-guided radiofrequency ablation in the management of interdigital (Morton s) neuroma Graham S. J. Chuter & Yeok
Common Foot and Ankle Pathology DOTS 17th April Nick Savva Orthopaedic Foot and Ankle Surgeon. Monday, 29 April 13
 Common Foot and Ankle Pathology DOTS 17th April 2013 Nick Savva Orthopaedic Foot and Ankle Surgeon Monday, 29 April 13 Topics Forefoot pain Hindfoot/Ankle pain Hallux rigidus Bunions Toe deformity Mortons
Common Foot and Ankle Pathology DOTS 17th April 2013 Nick Savva Orthopaedic Foot and Ankle Surgeon Monday, 29 April 13 Topics Forefoot pain Hindfoot/Ankle pain Hallux rigidus Bunions Toe deformity Mortons
Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic 2012 MFMER slide MFMER slide-3
 Ultrasound Foot and Ankle Pathology Disclosures None relevant Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012 MFMER slide-2 Foot and Ankle Fundamentals
Ultrasound Foot and Ankle Pathology Disclosures None relevant Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012 MFMER slide-2 Foot and Ankle Fundamentals
Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation
 Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Painful forefoot: A practical approach based on MRI findings
 Painful forefoot: A practical approach based on MRI findings Poster No.: C-2434 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal - Miscellaneous Authors: E. E. Martin, F. Delgado, J.
Painful forefoot: A practical approach based on MRI findings Poster No.: C-2434 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal - Miscellaneous Authors: E. E. Martin, F. Delgado, J.
Disclosure. Pre-Procedural Considerations. Transducer Selection. Sterile Procedure. Sterile Procedure. Ultrasound Guided Foot and Ankle Injections
 Ultrasound Guided Foot and Ankle Injections Disclosure No relevant financial relationships exist Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012
Ultrasound Guided Foot and Ankle Injections Disclosure No relevant financial relationships exist Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012
Imaging of Ankle and Foot pain
 Imaging of Ankle and Foot pain Pramot Tanutit, M.D. Department of Radiology Faculty of Medicine, Prince of Songkla University 1 Outlines Plain film: anatomy Common causes of ankle and foot pain Exclude:
Imaging of Ankle and Foot pain Pramot Tanutit, M.D. Department of Radiology Faculty of Medicine, Prince of Songkla University 1 Outlines Plain film: anatomy Common causes of ankle and foot pain Exclude:
Treatment of intermetatarsal Morton s neuroma with alcohol injection under US guide: 10-month follow-up
 Eur Radiol (2004) 14:514 518 DOI 10.1007/s00330-003-2057-7 MUSCULOSKELETAL Ezio Fanucci Salvatore Masala Sebastiano Fabiano Dario Perugia Ettore Squillaci Viviana Varrucciu Giovanni Simonetti Treatment
Eur Radiol (2004) 14:514 518 DOI 10.1007/s00330-003-2057-7 MUSCULOSKELETAL Ezio Fanucci Salvatore Masala Sebastiano Fabiano Dario Perugia Ettore Squillaci Viviana Varrucciu Giovanni Simonetti Treatment
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
Common Applications for Sonography and Guided Intervention: Shoulder
 Common Applications for Sonography and Guided Intervention: Shoulder Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant:
Common Applications for Sonography and Guided Intervention: Shoulder Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant:
Morton's Neurectomy Outcomes: Comparison of Plantar versus Dorsal Approaches
 Morton's Neurectomy Outcomes: Comparison of Plantar versus Dorsal Approaches Alexander Habashy, 1 MD, Gonzalo Sumarriva, 2 MBBS Robert Treu@ng, 1 MD March 18-19, 2016 1 Department of Orthopedics, Ochsner
Morton's Neurectomy Outcomes: Comparison of Plantar versus Dorsal Approaches Alexander Habashy, 1 MD, Gonzalo Sumarriva, 2 MBBS Robert Treu@ng, 1 MD March 18-19, 2016 1 Department of Orthopedics, Ochsner
MRI in Patients with Forefoot Pain Involving the Metatarsal Region
 MRI in Patients with Forefoot Pain Involving the Metatarsal Region Poster No.: C-0151 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit R. Vukojevi#, M. Mustapic, D. Marjan; Zagreb/HR
MRI in Patients with Forefoot Pain Involving the Metatarsal Region Poster No.: C-0151 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit R. Vukojevi#, M. Mustapic, D. Marjan; Zagreb/HR
Dynamic high resolution sonography (d-hrus) of the foot: a detailed didactic approach.
 Dynamic high resolution sonography (d-hrus) of the foot: a detailed didactic approach. Poster No.: C-1871 Congress: ECR 2013 Type: Educational Exhibit Authors: S. Perugin Bernardi, A. Arcidiacono, A. Corazza,
Dynamic high resolution sonography (d-hrus) of the foot: a detailed didactic approach. Poster No.: C-1871 Congress: ECR 2013 Type: Educational Exhibit Authors: S. Perugin Bernardi, A. Arcidiacono, A. Corazza,
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Diagnostic benefits of ultrasound-guided. CNB) versus mammograph-guided biopsy for suspicious microcalcifications. without definite breast mass
 Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Early Experience with Morton s Neuroma
 Med. J. Cairo Univ., Vol. 80, No. 2, December: 197-201, 2012 www.medicaljournalofcairouniversity.com Early Experience with Morton s Neuroma SAMEH BADRAN, M.D.; TAMER M. EWADI, M.D. and AMR ABDALKADER,
Med. J. Cairo Univ., Vol. 80, No. 2, December: 197-201, 2012 www.medicaljournalofcairouniversity.com Early Experience with Morton s Neuroma SAMEH BADRAN, M.D.; TAMER M. EWADI, M.D. and AMR ABDALKADER,
Ultrasound Evaluation of Masses
 Ultrasound Evaluation of Masses Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Panel: GE,
Ultrasound Evaluation of Masses Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Panel: GE,
MRI IN NONOSSEOUS ABNORMALITIES OF THE FOREFOOT: A PICTORIAL REVIEW
 MRI IN NONOSSEOUS ABNORMALITIES OF THE FOREFOOT: A PICTORIAL REVIEW I Delgado, P Melloni, M Veintemillas, R Valls, M Vilagran, A Valera UDIAT. Sabadell (Barcelona). Spain. PURPOSE To catalog the wide spectrum
MRI IN NONOSSEOUS ABNORMALITIES OF THE FOREFOOT: A PICTORIAL REVIEW I Delgado, P Melloni, M Veintemillas, R Valls, M Vilagran, A Valera UDIAT. Sabadell (Barcelona). Spain. PURPOSE To catalog the wide spectrum
Sonography of Intramuscular Myxomas
 Article Sonography of Intramuscular Myxomas The Bright Rim and Bright Cap Signs Gandikota Girish, MBBS, FRCS, FRCR, David A. Jamadar, MBBS, FRCS, FRCR, David Landry, MD, Karen Finlay, MD, Jon A. Jacobson,
Article Sonography of Intramuscular Myxomas The Bright Rim and Bright Cap Signs Gandikota Girish, MBBS, FRCS, FRCR, David A. Jamadar, MBBS, FRCS, FRCR, David Landry, MD, Karen Finlay, MD, Jon A. Jacobson,
Imhoff, A. und Zollinger, H.: (Hrsg.): Fusschirurgie Thieme, Stuttgart (2004)
 Bücher: Imhoff, A. und Zollinger, H.: (Hrsg.): Fusschirurgie Thieme, Stuttgart (2004) Zollinger, H. (Hrsg.): Sehnenschädigungen am Rückfuss H. Huber, Bern, Stuttgart, Toronto (l993) Zollinger, H.: Osteonekrosen
Bücher: Imhoff, A. und Zollinger, H.: (Hrsg.): Fusschirurgie Thieme, Stuttgart (2004) Zollinger, H. (Hrsg.): Sehnenschädigungen am Rückfuss H. Huber, Bern, Stuttgart, Toronto (l993) Zollinger, H.: Osteonekrosen
3/20/2017. Disclosures. Ultrasound Fundamentals. Ultrasound Fundamentals. Bone Anatomy. Tissue Characteristics
 Disclosures Images of ultrasound equipment in this presentation are not an endorsement Fundamentals of Musculoskeletal Ultrasound Physics and Knobology Shane A. Shapiro, M.D. Assistant Professor Orthopedic
Disclosures Images of ultrasound equipment in this presentation are not an endorsement Fundamentals of Musculoskeletal Ultrasound Physics and Knobology Shane A. Shapiro, M.D. Assistant Professor Orthopedic
HIGH FREQUENCY ULTRASOUND EVALUATION OF PERIPHERAL NERVES ULTRAEMG
 HIGH FREQUENCY ULTRASOUND EVALUATION OF PERIPHERAL NERVES ULTRAEMG 5-11-17 Jeffrey A. Strakowski, MD Clinical Associate Professor, Dept of PM&R The Ohio State University Associate Director of Medical Education,
HIGH FREQUENCY ULTRASOUND EVALUATION OF PERIPHERAL NERVES ULTRAEMG 5-11-17 Jeffrey A. Strakowski, MD Clinical Associate Professor, Dept of PM&R The Ohio State University Associate Director of Medical Education,
Ablation Procedures for Peripheral Neuromas. Summary
 Subject: Ablation Procedures for Peripheral Neuromas Page: 1 of 9 Last Review Status/Date: March 2015 Ablation Procedures for Peripheral Neuromas Summary Morton s neuroma is a common and painful compression
Subject: Ablation Procedures for Peripheral Neuromas Page: 1 of 9 Last Review Status/Date: March 2015 Ablation Procedures for Peripheral Neuromas Summary Morton s neuroma is a common and painful compression
Original Report. Sonography of Ankle Tendon Impingement with Surgical Correlation
 Downloaded from www.ajronline.org by 162.158.89.91 on 08/23/18 from IP address 162.158.89.91. Copyright RRS. For personal use only; all rights reserved Monisha Shetty 1 David P. Fessell 1 John E. Femino
Downloaded from www.ajronline.org by 162.158.89.91 on 08/23/18 from IP address 162.158.89.91. Copyright RRS. For personal use only; all rights reserved Monisha Shetty 1 David P. Fessell 1 John E. Femino
Longitudinal Split of the Peroneus Longus and Peroneus Brevis Tendons with Disruption of the Superior Peroneal Retinaculum
 Longitudinal Split of the Peroneus Longus and Peroneus Brevis Tendons with Disruption of the Superior Peroneal Retinaculum Gregory C. Diaz, MD, Marnix van Holsbeeck, MD, Jon A. Jacobson, MD Longitudinal
Longitudinal Split of the Peroneus Longus and Peroneus Brevis Tendons with Disruption of the Superior Peroneal Retinaculum Gregory C. Diaz, MD, Marnix van Holsbeeck, MD, Jon A. Jacobson, MD Longitudinal
ELENI ANDIPA General Hospital of Athens G. Gennimatas
 ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
Ultrasound of the Knee
 Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Ultrasound (US) of the posterior interosseous nerve (PIN) around the distal edge of the supinator tunnel.
 Ultrasound (US) of the posterior interosseous nerve (PIN) around the distal edge of the supinator tunnel. Poster No.: C-0024 Congress: ECR 2013 Type: Scientific Exhibit Authors: C. Rolla Bigliani 1, G.
Ultrasound (US) of the posterior interosseous nerve (PIN) around the distal edge of the supinator tunnel. Poster No.: C-0024 Congress: ECR 2013 Type: Scientific Exhibit Authors: C. Rolla Bigliani 1, G.
Alcoholization under sonographic guidance in Morton's neuroma: follow up in 250 cases
 Alcoholization under sonographic guidance in Morton's neuroma: follow up in 250 cases Poster No.: C-0572 Congress: ECR 2014 Type: Scientific Exhibit Authors: L. Perini, C. Perini, M. Tagliapietra, S. Puggina,
Alcoholization under sonographic guidance in Morton's neuroma: follow up in 250 cases Poster No.: C-0572 Congress: ECR 2014 Type: Scientific Exhibit Authors: L. Perini, C. Perini, M. Tagliapietra, S. Puggina,
The Role of Sonography in Differentiating Full Versus Partial Distal Biceps Tendon Tears: Correlation With Surgical Findings
 Musculoskeletal Imaging Original Research Da Gama Lobo et al. Sonography in Biceps Tendon Tears Musculoskeletal Imaging Original Research Lucas Da Gama Lobo 1,2 David P. Fessell 1 Bruce S. Miller 1,3 Aine
Musculoskeletal Imaging Original Research Da Gama Lobo et al. Sonography in Biceps Tendon Tears Musculoskeletal Imaging Original Research Lucas Da Gama Lobo 1,2 David P. Fessell 1 Bruce S. Miller 1,3 Aine
The Pitfalls of Radiological Ordering and Documentation- Can you Pass an Audit? David J. Freedman, DPM, FASPS Laura J. Pickard, DPM October 26, 2017
 The Pitfalls of Radiological Ordering and Documentation- Can you Pass an Audit? David J. Freedman, DPM, FASPS Laura J. Pickard, DPM October 26, 2017 1 Surgical Coding Webinar Series Register for these
The Pitfalls of Radiological Ordering and Documentation- Can you Pass an Audit? David J. Freedman, DPM, FASPS Laura J. Pickard, DPM October 26, 2017 1 Surgical Coding Webinar Series Register for these
Podiatry Ultrasound Report Templates
 Podiatry Ultrasound Report Templates 1 st Edition Compiled exclusively for the clients of Fisher Biomedical Inc. Podiatric Ultrasound Report Templates Welcome to our first edition of sample podiatric ultrasound
Podiatry Ultrasound Report Templates 1 st Edition Compiled exclusively for the clients of Fisher Biomedical Inc. Podiatric Ultrasound Report Templates Welcome to our first edition of sample podiatric ultrasound
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Alcohol Injection Therapy for Morton's Neuroma Page 1 of 11 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Alcohol Injection Therapy for Morton's Neuroma Professional
Alcohol Injection Therapy for Morton's Neuroma Page 1 of 11 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Alcohol Injection Therapy for Morton's Neuroma Professional
Dynamic high-resolution ultrasound (DHRUS) and MRI of plantar plate: role in diagnostic iter
 Dynamic high-resolution ultrasound (DHRUS) and MRI of plantar plate: role in diagnostic iter Poster No.: C-1003 Congress: ECR 2012 Type: Scientific Exhibit Authors: R. Saporiti, S. Migone, V. Prono, R.
Dynamic high-resolution ultrasound (DHRUS) and MRI of plantar plate: role in diagnostic iter Poster No.: C-1003 Congress: ECR 2012 Type: Scientific Exhibit Authors: R. Saporiti, S. Migone, V. Prono, R.
Message of the Month for GPs June 2013
 Message of the Month for GPs June 2013 Dr Winn : Consultant Musculoskeletal Radiologist, Manchester Royal Infirmary Imaging of the musculoskeletal system Musculoskeletal pain is a common problem in the
Message of the Month for GPs June 2013 Dr Winn : Consultant Musculoskeletal Radiologist, Manchester Royal Infirmary Imaging of the musculoskeletal system Musculoskeletal pain is a common problem in the
ORIGINAL PAPERS. Long-Term Results of Neurectomy Through a Dorsal Approach in the Treatment of Morton s Neuroma
 ORIGINAL PAPERS Adv Clin Exp Med 2016, 25, 2, 295 302 DOI: 10.17219/acem/60249 Copyright by Wroclaw Medical University ISSN 1899 5276 Paweł Reichert A F, Krzysztof Zimmer A, D F, Jarosław Witkowski A D,
ORIGINAL PAPERS Adv Clin Exp Med 2016, 25, 2, 295 302 DOI: 10.17219/acem/60249 Copyright by Wroclaw Medical University ISSN 1899 5276 Paweł Reichert A F, Krzysztof Zimmer A, D F, Jarosław Witkowski A D,
Sonographic Differences in the Appearance of Acute and Chronic Full-Thickness Rotator Cuff Tears
 Sonographic Differences in the Appearance of Acute and Chronic Full-Thickness Rotator Cuff Tears Sharlene A. Teefey, MD, William D. Middleton, MD, Gregory S. Bauer, MD, Charles F. Hildebolt, DDS, PhD,
Sonographic Differences in the Appearance of Acute and Chronic Full-Thickness Rotator Cuff Tears Sharlene A. Teefey, MD, William D. Middleton, MD, Gregory S. Bauer, MD, Charles F. Hildebolt, DDS, PhD,
BUCKS MSK: FOOT AND ANKLE PATHWAY GP MANAGEMENT. Hallux Valgus. Assessment: Early Management. (must be attempted prior to any referral to imsk):
 Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Surgical Off-loading. Reiber et al Goals of Diabetic Foot Surgery 4/28/2012. The most common causal pathway to a diabetic foot ulceration
 Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Musculoskeletal Ultrasound Fundamentals
 Fundamentals Benjamin D. Levine, M.D. Associate Professor of Radiology Musculoskeletal Imaging Dept. of Radiological Sciences UCLA Health System I. Image Optimization II. Image Interpretation Artifacts
Fundamentals Benjamin D. Levine, M.D. Associate Professor of Radiology Musculoskeletal Imaging Dept. of Radiological Sciences UCLA Health System I. Image Optimization II. Image Interpretation Artifacts
Principles of Ultrasound. Cara C. Prideaux, M.D. University of Utah PM&R Sports Medicine Fellow March 14, 2012
 Principles of Ultrasound Cara C. Prideaux, M.D. University of Utah PM&R Sports Medicine Fellow March 14, 2012 None Disclosures Outline Introduction Benefits and Limitations of US Ultrasound (US) Physics
Principles of Ultrasound Cara C. Prideaux, M.D. University of Utah PM&R Sports Medicine Fellow March 14, 2012 None Disclosures Outline Introduction Benefits and Limitations of US Ultrasound (US) Physics
Ultrasound assessment of most frequent shoulder disorders
 Ultrasound assessment of most frequent shoulder disorders Poster No.: C-2026 Congress: ECR 2014 Type: Educational Exhibit Authors: S. P. Ivanoski; Ohrid/MK Keywords: Trauma, Athletic injuries, Arthritides,
Ultrasound assessment of most frequent shoulder disorders Poster No.: C-2026 Congress: ECR 2014 Type: Educational Exhibit Authors: S. P. Ivanoski; Ohrid/MK Keywords: Trauma, Athletic injuries, Arthritides,
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities
 Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
WHAT CAN ULTRASOUND SEE IN THE CARPAL TUNNEL REGION?
 WHAT CAN ULTRASOUND SEE IN THE CARPAL TUNNEL REGION? Jay Smith, M.D. CMO, Sonex Health LLC June 2017 Modern day ultrasound (US) machines provide a powerful combination of submillimeter resolution and dynamic
WHAT CAN ULTRASOUND SEE IN THE CARPAL TUNNEL REGION? Jay Smith, M.D. CMO, Sonex Health LLC June 2017 Modern day ultrasound (US) machines provide a powerful combination of submillimeter resolution and dynamic
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/22/2012 Radiology Quiz of the Week # 104 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/22/2012 Radiology Quiz of the Week # 104 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Achilles tendinopathy: new insights in cause of pain, diagnosis and management van Sterkenburg, M.N.
 UvA-DARE (Digital Academic Repository) Achilles tendinopathy: new insights in cause of pain, diagnosis and management van Sterkenburg, M.N. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Achilles tendinopathy: new insights in cause of pain, diagnosis and management van Sterkenburg, M.N. Link to publication Citation for published version (APA): van
Original Report. Sonography of Ankle Ganglia with Pathologic Correlation in 10 Pediatric and Adult Patients
 Downloaded from www.ajronline.org by 148.251.232.83 on 04/11/18 from IP address 148.251.232.83. Copyright RRS. For personal use only; all rights reserved Robert Ortega 1 David P. Fessell 1 Jon. Jacobson
Downloaded from www.ajronline.org by 148.251.232.83 on 04/11/18 from IP address 148.251.232.83. Copyright RRS. For personal use only; all rights reserved Robert Ortega 1 David P. Fessell 1 Jon. Jacobson
Extraarticular Lateral Ankle Impingement
 Extraarticular Lateral Ankle Impingement Poster No.: C-1282 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Cevikol; Keywords: Trauma, Diagnostic procedure, MR, CT, Musculoskeletal system, Musculoskeletal
Extraarticular Lateral Ankle Impingement Poster No.: C-1282 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Cevikol; Keywords: Trauma, Diagnostic procedure, MR, CT, Musculoskeletal system, Musculoskeletal
Digital Surgery Complications
 Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. PODIATRY CLINICAL GUIDELINES TABLE OF CONTENTS. Diabetes Mellitus and Podiatric Care 2
 NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. PODIATRY 2012-2013 CLINICAL GUIDELINES TABLE OF CONTENTS CONDITION PAGE(S) Diabetes Mellitus and Podiatric Care 2 Fractures 3-4 Heel Pain (Posterior) Retrocalcaneal
NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. PODIATRY 2012-2013 CLINICAL GUIDELINES TABLE OF CONTENTS CONDITION PAGE(S) Diabetes Mellitus and Podiatric Care 2 Fractures 3-4 Heel Pain (Posterior) Retrocalcaneal
High-resolution ultrasound of the sural nerve
 High-resolution ultrasound of the sural nerve Poster No.: C-2084 Congress: ECR 2012 Type: Educational Exhibit Authors: D. Belsack, T. Jager, M. De Maeseneer, K. Vanderdood, S. 1 5 1 2 3 2 3 4 4 Marcelis
High-resolution ultrasound of the sural nerve Poster No.: C-2084 Congress: ECR 2012 Type: Educational Exhibit Authors: D. Belsack, T. Jager, M. De Maeseneer, K. Vanderdood, S. 1 5 1 2 3 2 3 4 4 Marcelis
High-resolution ultrasound of the sural nerve
 High-resolution ultrasound of the sural nerve Poster No.: C-2084 Congress: ECR 2012 Type: Educational Exhibit Authors: D. Belsack, T. Jager, M. De Maeseneer, K. Vanderdood, S. 1 5 1 2 3 2 3 4 4 Marcelis
High-resolution ultrasound of the sural nerve Poster No.: C-2084 Congress: ECR 2012 Type: Educational Exhibit Authors: D. Belsack, T. Jager, M. De Maeseneer, K. Vanderdood, S. 1 5 1 2 3 2 3 4 4 Marcelis
Ankle and Foot Orthopaedic Tests Orthopedics and Neurology DX 612
 Ankle and Foot Orthopaedic Tests Orthopedics and Neurology DX 612 James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Ankle & Foot Anatomy Stability of the ankle is dependent
Ankle and Foot Orthopaedic Tests Orthopedics and Neurology DX 612 James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Ankle & Foot Anatomy Stability of the ankle is dependent
ORTHOTIC ARCH SUPPORTS
 ORTHOTIC ARCH SUPPORTS COMMON FOOT PROBLEMS & ORTHOTIC THERAPY The foot and ankle are the foundation for the overall posture of the skeletal body. Many problems with the feet, legs, knees, hips and lower
ORTHOTIC ARCH SUPPORTS COMMON FOOT PROBLEMS & ORTHOTIC THERAPY The foot and ankle are the foundation for the overall posture of the skeletal body. Many problems with the feet, legs, knees, hips and lower
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging
 Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Ultrasonographic Evaluation of Cervical Lymphadenopathy with Cytological Correlation
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/74 Ultrasonographic Evaluation of Cervical Lymphadenopathy with Cytological Correlation Suresh Kumar 1, Sonjjay Pande
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/74 Ultrasonographic Evaluation of Cervical Lymphadenopathy with Cytological Correlation Suresh Kumar 1, Sonjjay Pande
Urgent Cases and Foreign Bodies
 Urgent Cases and Foreign Bodies Catherine J. Brandon, MD, MS University of Michigan Ann Arbor, MI, USA Introduction: Patients added on to the schedule from the emergency department or as urgent add-on
Urgent Cases and Foreign Bodies Catherine J. Brandon, MD, MS University of Michigan Ann Arbor, MI, USA Introduction: Patients added on to the schedule from the emergency department or as urgent add-on
Injuries to the Foot. NOCROP Sports Medicine and Therapy
 Injuries to the Foot Arches of the Foot Plantar Fascia - a flat band of connective tissue that connects your heel bone to your toes. It supports the arch of your foot. Muscle of the Foot and Lower Leg
Injuries to the Foot Arches of the Foot Plantar Fascia - a flat band of connective tissue that connects your heel bone to your toes. It supports the arch of your foot. Muscle of the Foot and Lower Leg
Conditions Information on common problems we treat.
 Conditions Information on common problems we treat. Perthpodiatricsurgery.com 9383 3851 Perth Podiatric Surgery 01 Problems affecting the big toe 01 Bunions Bunions are a common foot problem which affect
Conditions Information on common problems we treat. Perthpodiatricsurgery.com 9383 3851 Perth Podiatric Surgery 01 Problems affecting the big toe 01 Bunions Bunions are a common foot problem which affect
Contribution of ultrasound in the assessment of patients with suspect idiopathic pudendal nerve disease
 Contribution of ultrasound in the assessment of patients with suspect idiopathic pudendal nerve disease Poster No.: C-1555 Congress: ECR 2014 Type: Scientific Exhibit Authors: B. Bignotti 1, A. Tagliafico
Contribution of ultrasound in the assessment of patients with suspect idiopathic pudendal nerve disease Poster No.: C-1555 Congress: ECR 2014 Type: Scientific Exhibit Authors: B. Bignotti 1, A. Tagliafico
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
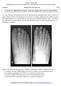 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/29/2012 Radiology Quiz of the Week # 105 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/29/2012 Radiology Quiz of the Week # 105 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Index. Clin Sports Med 23 (2004) Note: Page numbers of article titles are in boldface type.
 Clin Sports Med 23 (2004) 169 173 Index Note: Page numbers of article titles are in boldface type. A Achilles enthesopathy, calcaneal spur with, 133 clinical presentation of, 135 136 definition of, 131
Clin Sports Med 23 (2004) 169 173 Index Note: Page numbers of article titles are in boldface type. A Achilles enthesopathy, calcaneal spur with, 133 clinical presentation of, 135 136 definition of, 131
THYROID NODULES: THE ROLE OF ULTRASOUND
 THYROID NODULES: THE ROLE OF ULTRASOUND NOVEMBER 2017 DR. DEAN DURANT DEFINITION Thyroid nodule: Focal area within the thyroid gland with echogenicity different from surrounding parenchyma. THYROID NODULES
THYROID NODULES: THE ROLE OF ULTRASOUND NOVEMBER 2017 DR. DEAN DURANT DEFINITION Thyroid nodule: Focal area within the thyroid gland with echogenicity different from surrounding parenchyma. THYROID NODULES
Osteotomy vs No Osteotomy Second Ray
 Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
Post-catheterization pseudoaneurysms treatment with ultrasound-guided thrombin injection
 Post-catheterization pseudoaneurysms treatment with ultrasound-guided thrombin injection Poster No.: C-2107 Congress: ECR 2010 Type: Topic: Scientific Exhibit Interventional Radiology Authors: A. Ladas,
Post-catheterization pseudoaneurysms treatment with ultrasound-guided thrombin injection Poster No.: C-2107 Congress: ECR 2010 Type: Topic: Scientific Exhibit Interventional Radiology Authors: A. Ladas,
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatry. Procedure List. As Of. 01 April Government of Alberta
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Sonographic Target Sign in Neurofibromas
 Sonographic Target Sign in Neurofibromas John Lin, MD, Jon A. Jacobson, MD, Curtis W. Hayes, MD Neurofibromas are the most common tumors of the peripheral nerves. They may be solitary lesions, multiple
Sonographic Target Sign in Neurofibromas John Lin, MD, Jon A. Jacobson, MD, Curtis W. Hayes, MD Neurofibromas are the most common tumors of the peripheral nerves. They may be solitary lesions, multiple
Original Report. Sonography of Tears of the Distal Biceps Tendon. Theodore T. Miller 1,2 Ronald S. Adler 3
 Theodore T. Miller 1,2 Ronald S. dler 3 Received October 15, 1999; accepted after revision March 21, 2000. Presented at the annual meeting of the merican Roentgen Ray Society, Washington, DC, May 2000.
Theodore T. Miller 1,2 Ronald S. dler 3 Received October 15, 1999; accepted after revision March 21, 2000. Presented at the annual meeting of the merican Roentgen Ray Society, Washington, DC, May 2000.
Ablation Procedures for Peripheral Neuromas
 Ablation Procedures for Peripheral Neuromas Policy Number: 7.01.147 Last Review: 08/2018 Origination: 08/2015 Next Review: 08/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Ablation Procedures for Peripheral Neuromas Policy Number: 7.01.147 Last Review: 08/2018 Origination: 08/2015 Next Review: 08/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
Rotator Cuff and Biceps Pathology
 Rotator Cuff and Biceps Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board:
Rotator Cuff and Biceps Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board:
Proceedings of the 56th Annual Convention of the American Association of Equine Practitioners - AAEP -
 http://www.ivis.org Proceedings of the 56th Annual Convention of the American Association of Equine Practitioners - AAEP - December 4-8, 2010 Baltimore, Maryland, USA Next Meeting : Nov. 18-22, 2011 -
http://www.ivis.org Proceedings of the 56th Annual Convention of the American Association of Equine Practitioners - AAEP - December 4-8, 2010 Baltimore, Maryland, USA Next Meeting : Nov. 18-22, 2011 -
Detection and Measurement of Rotator Cuff Tears with Sonography: Analysis of Diagnostic Errors
 Musculoskeletal Imaging Teefey et al. Detection of Rotator Cuff Tears with Sonography Sharlene A. Teefey 1 William D. Middleton 1 William T. Payne 2 Ken Yamaguchi 3 Teefey SA, Middleton WD, Payne WT, Yamaguchi
Musculoskeletal Imaging Teefey et al. Detection of Rotator Cuff Tears with Sonography Sharlene A. Teefey 1 William D. Middleton 1 William T. Payne 2 Ken Yamaguchi 3 Teefey SA, Middleton WD, Payne WT, Yamaguchi
2015 ARDMS Musculoskeletal Sonographer Job Task Analysis Summary Report
 P a g e 1 2015 ARDMS Musculoskeletal Sonographer Job Task Analysis Summary Report American Registry for Diagnostic Medical Sonography (ARDMS) P a g e 2 Table of Contents ABOUT THE REPORT... 3 METHODOLOGY...
P a g e 1 2015 ARDMS Musculoskeletal Sonographer Job Task Analysis Summary Report American Registry for Diagnostic Medical Sonography (ARDMS) P a g e 2 Table of Contents ABOUT THE REPORT... 3 METHODOLOGY...
Greater Trochanter: Anatomy and Pathology
 Greater Trochanter: Anatomy and Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties:
Greater Trochanter: Anatomy and Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties:
Sonography of Plantar Fibromatosis
 James F. Griffith 1 Tammy Y. Y. Wong 1 Shiu Man Wong 2 Margaret Wan Nar Wong 3 Constantine Metreweli 1 Received October 22, 2001; accepted after revision April 24, 2002. 1 Department of Diagnostic Radiology
James F. Griffith 1 Tammy Y. Y. Wong 1 Shiu Man Wong 2 Margaret Wan Nar Wong 3 Constantine Metreweli 1 Received October 22, 2001; accepted after revision April 24, 2002. 1 Department of Diagnostic Radiology
A Patient s Guide to Posterior Tibial Tendon Problems
 A Patient s Guide to Posterior Tibial Tendon Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
A Patient s Guide to Posterior Tibial Tendon Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Imaging of the Elbow. Marco Zanetti Radiology Balgrist University Hospital Zurich
 Imaging of the Elbow Marco Zanetti Radiology Balgrist University Hospital Zurich Elbow Case 1 Case 8 Case 2 Case 9 Case 3 Case 10 Case 4 Case 11 Case 5 Case 12 Case 6 Case 13 Case 7 Case 14 Elbow Imaging
Imaging of the Elbow Marco Zanetti Radiology Balgrist University Hospital Zurich Elbow Case 1 Case 8 Case 2 Case 9 Case 3 Case 10 Case 4 Case 11 Case 5 Case 12 Case 6 Case 13 Case 7 Case 14 Elbow Imaging
Musculoskeletal Ultrasound: Basics, Utility, and Clinical Applications
 Musculoskeletal Ultrasound: Basics, Utility, and Clinical Applications Andrew Lavigne, MD, FRCPC Physical Medicine and Rehabilitation CSCN Diplomat (EMG) Dip Sport Medicine Eugene Maida, MD, PGY-4 Resident
Musculoskeletal Ultrasound: Basics, Utility, and Clinical Applications Andrew Lavigne, MD, FRCPC Physical Medicine and Rehabilitation CSCN Diplomat (EMG) Dip Sport Medicine Eugene Maida, MD, PGY-4 Resident
THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery
 C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
 Case Reports in Radiology Volume 2016, Article ID 8739362, 4 pages http://dx.doi.org/10.1155/2016/8739362 Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
Case Reports in Radiology Volume 2016, Article ID 8739362, 4 pages http://dx.doi.org/10.1155/2016/8739362 Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
Hindfoot Alignment Measurements: Rotation-Stability of Measurement Techniques on Hindfoot Alignment View and Long Axial View Radiographs
 Musculoskeletal Imaging Original Research Buck et al. Measurements Musculoskeletal Imaging Original Research FOCUS ON: Florian M. Buck 1 Adrienne Hoffmann 1 Nadja Mamisch-Saupe 1 Norman Espinosa 2 Donald
Musculoskeletal Imaging Original Research Buck et al. Measurements Musculoskeletal Imaging Original Research FOCUS ON: Florian M. Buck 1 Adrienne Hoffmann 1 Nadja Mamisch-Saupe 1 Norman Espinosa 2 Donald
