Surgical treatments of patellar instability have been
|
|
|
- Dorcas Maxwell
- 6 years ago
- Views:
Transcription
1 Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin Lind, M.D., Ph.D. Purpose: We present clinical results in a case series of 44 patients with medial patellofemoral ligament (MPFL) reconstruction with 12 to 32 months follow-up. Methods: Reconstruction was performed via gracilis tendon autograft looped through 2 transverse 4.5-mm drill holes in the patella and fixed at the natural MPFL insertion site on the medial femoral condyle with an interference screw. At follow-up, Kujala scores, Knee Injury and Osteoarthritis Outcome Scores, objective knee function, complications, and reoperations were assessed. Results: Only 1 patella redislocation was observed. Subluxation occurred in 3 patients, whereas 4 patients had chronic pain at follow-up, all of whom had cartilage injury at surgery. The Kujala knee function score improved overall from 46 points (range, 12 to 67 points) to 84 points (range, 62 to 100 points) at follow-up. Conclusions: MPFL reconstruction with double transverse patella drill holes and a gracilis tendon graft provides good postoperative patellar stability. Postoperative pain seems to be related to the degree of patellofemoral injury found at surgery. Level of Evidence: Level IV, therapeutic case series. Key Words: Medial patellofemoral ligament Patellar instability Ligament reconstruction. From the Division of Sportstrauma, Orthopaedic Department, Århus University Hospital, Århus, Denmark. The authors report no conflict of interest. Address correspondence and reprints requests to Martin Lind, M.D., Ph.D., Hvedevangen 9, 8200 Åarhus N, Denmark. martinlind@dadlnet.dk 2008 by the Arthroscopy Association of North America /08/ $34.00/0 doi: /j.arthro Surgical treatments of patellar instability have been numerous and the clinical results variable. 1,2 Recently, reconstruction of the medial patellofemoral ligament (MPFL) has been advocated as a surgical treatment for chronic patellar instability. Among the medial ligamentous retinacular structures (superficial medial patellar retinaculum, MPFL, and medial patellotibial and patellomeniscal ligaments), the MPFL is the primary medial restraining structure against lateralization of the patella and contributes up to 80% of the medial restraining forces to the patella. 3,4 Biomechanical studies have found that the limited ability of the MPFL to elongate results in total rupture of the ligament in cases of full patellar dislocation. 5 In addition, the healing capacity of the MPFL is often insufficient, which leads to increased medial laxity of the patellar retinacular structures. 6,7 The aim of the MPFL reconstruction is to restore the medial tether of the patella. Numerous different techniques for MPFL reconstruction have been described. All techniques aim to supply tendon tissue from the medial aspect of the patella to the insertion site of the natural MPFL at the adductor tubercle of the medial femoral condyle to reconstruct the ligament. The described tendon sources are numerous: semitendinosus, gracilis, partial quadriceps, partial patella tendon, partial semimembranosus, vastus medialis retinaculum, and allografts or artificial tendons The fixation of grafts is ensured by different techniques, such as patellar drill holes, sutures, suture anchors, and interference screws or staples at the femoral condyle. In general, the clinical results of MPFL reconstruction were successful in the previously mentioned studies. The procedure leads to good patellar stability, with rates of redislocation of only 0% to 10% (Table 1). We describe the clinical results of a prospective 82 Arthroscopy: The Journal of Arthroscopic and Related Surgery, Vol 24, No 1 (January), 2008: pp 82-87
2 MEDIAL PATELLOFEMORAL LIGAMENT RECONSTRUCTION 83 TABLE 1. Study Details and Results From Clinical Follow-up Studies of MPFL Reconstruction With Kujala Score Used as Clinical End-point Study Graft N Follow-up Redislocation Kujala Score Deie et al. 17 (2005) Semitendinosus transfer 39 5 yr 0% 92 Schöttle et al. 13 (2005) Semitendinosus autograft 15 4 yr 1/15 87 Steiner et al. 16 (2006) Adductor tendon autograft yr 0% 90 Drez et al. 12 (2001) Various grafts mo 1/19 88 case series of 44 patients treated with MPFL reconstruction for chronic patellar instability via a surgical technique with gracilis tendon autograft fixed in patellar drill holes with an interference screw in the femoral condyle. The rationale for the transpatellar drill hole technique is to obtain an optimal graft fixation in the patella. We hypothesize that results are comparable to previously published data in studies with MPFL reconstruction. Patients METHODS This study included 44 patients who were consecutively operated on. Patients underwent surgery from May 2003 to December Mean follow-up was 22 months (range, 12 to 32 months), and 45% of the patients had 2 years of follow-up or more. The patients median age was 22 years (range, 12 to 47 years). There were 15 male and 29 female patients. All patients had chronic patellar instability with a minimum of 2 total patellar dislocations. The median period of preoperative patellar instability was 7 years (range, 1 to 20 years). Eighteen patients had 1 previous patellar procedure, and eight had 2 previous procedures. These procedures were medial tibial tuberosity transfers, medial plication, lateral release, and MPFL reinsertion. Evaluation All patients with a minimum 1-year follow-up were seen for follow-up again in the fall of The median follow-up was 22 months, with a range from 12 to 36 months. Patients were evaluated by preoperative and follow-up Kujala scores. At follow-up, a subjective Knee Injury and Osteoarthritis Outcome Score (KOOS) profile was obtained. Clinical data included incidence of recurrent subluxation or dislocation. Any complications and reoperations were registered. The following objective measures were recorded at follow-up: pain along MPFL reconstruction, abnormal patellar movement, lateral patellar apprehension, range of motion, and muscle status. Persistent chronic pain was defined as a pain score of 0 or 3 in the pain subscale of the Kujala score. Surgical Technique The gracilis tendon is harvested through a 2- to 3-cm incision over the pes anserinus. The anserinus bursa is opened, and the gracilis tendon is exposed and released with a tendon stripper. The gracilis tendon was used to minimize the effect on hamstring function and to have a tendon that could easily pass through the patellar drill holes. The tendon is fitted with No. 0 FiberWire nonabsorbable suture baseball stitches (Arthrex, Naples, FL) in each end. Then 2 incisions are made transversely on the medial and lateral aspects of the patella at the proximal one-third line. A small 1-cm incision on the lateral side and a 4- to 5-cm incision on the medial side are made from the medial patellar edge to the medial femoral epicondyle. Two transverse 4.5-mm drill holes are made through the patella over initially placed guidewires. The holes are placed in the proximal two thirds of the patella, 10 to 15 mm apart (Fig 1). Care is taken not to violate the chondral surface or the anterior cortex. Then the adductor tubercle is exposed and identified at the medial femoral condyle. The natural MPFL insertion point is just distal to the tubercle. A K-wire is inserted at that point, and an isometry test is performed with looped No. 0 Vicryl sutures (Ethicon, Somerville, NJ) from the K-wire through the 2 patellar holes to test isometry through the motion arc. Excessive tension at flexion should be avoided and can be resolved by a slightly more distal placement of the condyle K-wire. When proper K-wire placement is achieved, a 7-mm drill hole is made at the femoral condyle. The gracilis tendon is then passed through the patellar holes in a looped fashion (Fig 1). On the medial side, the free ends off the tendon are passed under the fascia to the femoral drill hole. The proximal tendon is
3 84 S. E. CHRISTIANSEN ET AL. medial tibial tuberosity transfer in our study. Radiographically, we used a sulcus angle greater than 160 as a sign of Dejour type B or C. In addition, pathologic Q-angles of more than 15 for male patients and more than 20 for female patients indicated tuberosity transfer. Q-angle was assessed with the lateral patellar edge aligned with the lateral femoral condyle. Tibial tuberosity transfer was always performed before MPFL reconstruction so as to obtain correct MPFL tensioning after the transfer of the tuberosity. Rehabilitation A DonJoy brace (DJO, Vista, CA) with 0 to 90 of motion was used for the first 2 weeks, with full weight-bearing on a straight knee. From 2 to 6 weeks, no brace was used, with an allowed range of motion of 0 to 90 and free weight-bearing during standing and walking. After 6 weeks, free activity was allowed. Controlled sports activities after 3 months and contact sports after 6 months were allowed. RESULTS FIGURE 1. Surgical technique of MPFL reconstruction. MPFL reconstruction is performed with the gracilis tendon looped through two 4.5-mm patellar drill holes, passed under the fascia, and fixed in a 7-mm drill hole in the medial femoral condyle with an absorbable interference screw. passed through the vastus medialis aponeurosis midway toward the medial epicondyles to ensure optimized vastus medialis oblique muscle action. Both tendon ends are tightened into the femoral drill hole via a Beath pin pullout technique. The tension of the reconstruction is tested through the arc of motion, and the tendons are fixed in the femoral condyle with a bioresorbable interference screw. The tendons are tensioned at 45 of flexion so that the patella still can be lateralized manually 10 mm. It is important not to overconstrain the reconstruction, thereby creating chondral overload in flexion. We supported the MPFL procedure with a medial tibial tuberosity transfer in patients who had significant trochlear dysplasia. A completely flattened trochlea (Dejour type B) or an absent or severely dysplastic medial femoral condyle (Dejour type C) indicated a Subjective patient assessment revealed that 80% of patients (35/44) felt that their knee function had improved in terms of activities of daily living and 37 of 44 patients indicated that their ability to perform recreational sports activities had improved. Of the patients, 64% (28/44) were completely pain-free when performing activities of daily living and 59% (26/44) were pain-free when performing sport activities. Four patients had persistent chronic pain. All of these patients had cartilage injury with an International Cartilage Repair Society grade of 3 or 4 to the patella or trochlea. In the 40 patients without chronic pain, similar severe cartilage injuries were found in only 20% (8/40). The Kujala knee function score improved overall from 46 points (range, 12 to 67 points) to 84 points (range, 62 to 100 points) at follow-up (Table 2). The mean Tegner activity score at follow-up was 4 (range, 1 to 9). Eight patients were performing competitive sports at follow-up. One patient had a redislocation 6 months postoperatively. This patient was further treated with a brace and was not interested in additional surgical treatment. Three patients had had a sensation of subluxation. Twelve patients had a tibial tuberosity transfer performed according to the criteria mentioned in the Methods section. All had trochlear dysplasia as the indication for the osteotomy, and furthermore, 3 of the patients had an excessive Q-angle. The Kujala and Tegner scores in
4 MEDIAL PATELLOFEMORAL LIGAMENT RECONSTRUCTION 85 TABLE 2. these patients were similar to those in patients without this additional procedure but with a tendency to lower scores in the patients with the combined procedure (Table 2). Objective Patient Assessment Palpable pain was found at the medial patellar edge in 43% of the patients (19/44) and at the medial femoral condyle in 50% (22/44). A positive apprehension sign with patellar lateralization was found in 41% of patients (18/44). Four patients had a loss of flexion of greater than 10, with the greatest flexion loss being 25. Complications Results of KOOS, Kujala, and Tegner Activity Scores Overall (N 44) MPFL Reconstruction (n 32) MPFL Reconstruction and Tibial Tuberosity Transfer (n 12) KOOS, mean (SD) Symptoms 73 (15) 75 (13) 66 (21) Pain 90 (9) 91 (8) 87 (13) Activities of daily living 84 (12) 85 (11) 78 (16) Sports and recreation 80 (10) 81 (9) 78 (13) Quality of life 80 (10) 81 (9) 78 (13) Kujala score [median (range)] 84 (62-100) 88 (68-100) 83 (62-100) Tegner activity score [median (range)] 4 (0-9) 4 (1-8) 4 (0-9) NOTE. The KOOS score contains 5 subscores ranging from 0 to 100, with 100 being the best score. The subscores are symptoms, pain, activities of daily living, sports and recreation, and quality of life. The Kujala score ranges from 0 to 100, with 100 being the best score. The Tegner activity score ranges from 0 to 10, with 10 being the best score. There were 5 reoperations. In 1 patient the knee was forced into maximal flexion while he was under general anesthesia because his flexion ability was less than 90. Three patients had the medial femoral condyle interference screw removed between 6 and 12 months postoperatively because of screw protrusion or pain at the screw position at the medial femoral condyle. A severe complication was seen in 1 patient with a transverse patellar fracture 6 weeks postoperatively. The fracture was caused by a surgical failure: 1 of the transverse drill holes had violated the anterior patellar cortex. The fracture occurred when the patient rose from a chair without support. DISCUSSION The optimal surgical treatment for chronic patellar instability is controversial. Numerous techniques have been used with varying success. Proximal realignment procedures, which cover medial capsule plication and lateral capsule release, have been investigated in a few studies. Scuderi et al. 21 reported a low redislocation rate of 3% with isolated proximal realignment. A similar finding was reported by Aglietti et al. 22 and Zeichen et al. 23 Medial transfer of the tibial tuberosity, called distal realignment, has been used in isolation, with unsatisfactory results in approximately 20% to 25% of patients. 24,25 However, in a study by Shelbourne et al., 26 a redislocation rate of 0% was found in 34 patients with patellar instability but 25% had persistent symptomatic instability. A combination of all 3 of the previously mentioned procedures, called the Roux procedure, has resulted in better redislocation rates of 5% to 10% This study, which contained a large patient group with MPFL reconstruction, had a low redislocation rate of 2%. This is consistent with other MPFL reconstruction studies that report no redislocation or a very low incidence of redislocation after the procedure. 8,9,11-14,16-20 Our follow-up Kujala score of 84 points is slightly lower than that in other studies using this score, ranging from 87 to 92 points (Table 1). One study had poorer outcomes in patients with cartilage damage at the time of surgery. 8 We found a similar tendency, with 100% of patients with persistent chronic pain having grade 3 or 4 chondral lesions, whereas major chondral lesions were found in only 20% of the patients without persistent pain. The usage of additional procedures combined with MPFL reconstruction is controversial. We used medial tibial tuberosity transfer in patients who had pathologic Q-angles of more than 15 for male patients and more than 20 for female patients. Also, significant trochlear dysplasia with a completely flattened trochlea (Dejour type B) or an absent or severely dysplastic medial femoral condyle (Dejour type C) also indicated a medial tibial tuberosity transfer in our study. The dysplasia was thought to lead to excessive load on the MPFL reconstruction, and tibial tuberosity transfer would, in theory, reduce the load to the reconstruction. One study, however, did not find poorer results in patients with dysplasia when performing
5 86 S. E. CHRISTIANSEN ET AL. isolated MPFL reconstruction. This could indicate that the additional procedure might be unnecessary. 16 In the study by Schöttle et al., 13 a tibial tuberosity transfer was performed when the distance between the center of the trochlear sulcus and tibial tuberosity was greater than 15 mm. However, so far, no studies have indicated any need for additional procedures combined with MPFL reconstruction in cases of increased Q-angles or dysplasia. Positive apprehension and pain with palpation were seen in 50% of the patients. The change in anatomy at the medial aspect of the patella as a result of the reconstruction, as well as the fact that several patients had undergone previous surgeries, is considered to be the reason for these findings. We had 2 types of complications that resulted in reoperations. A major complication was a patellar fracture in an obese patient, resulting from a surgical error where a drill hole affected the anterior patella cortex. A concern with our technique is the risk of patellar fracture as a result of cortical weakening after creation of drill holes. Therefore our technique requires careful placement of the drill holes in the patella. A patellar fracture was described in another study in which patella drill holes were used for graft fixation. 9 In that study a drill canal diameter in the patella of 7 mm was used and violation of the anterior cortex was thought to be the cause of the patellar fracture. In our study 3 of 44 patients needed screw removal because of local inflammation. In a study by Steiner et al., 16 10% of patients needed screw removal because of a prominent or painful screw. Screw placement at the medial femoral condyles is susceptible to development of inflammation probably as a result of the extensive mobility of the soft tissues during knee motion or accumulation of small fragments of the biocomposite screw under the fascia during screw resorption. This study is limited by investigating the short-term clinical results after MPFL reconstruction. The mean follow-up was 22 months, but 45% of the patients had more than 2 years follow-up. However, at the time of the mean follow-up, patients typically have returned to the highest level of activity possible and remaining surgical morbidity does not improve significantly more over time. In addition, our material is a prospective patient series including all operated patients at our clinic. This results in a heterogeneous group with respect to the degree of patellofemoral dysplasia and previous surgeries. However, this heterogeneity gives an indication of clinical results with MPFL reconstruction in the typical chronic patellar instability patient population. CONCLUSIONS Early results with MPFL reconstruction with gracilis tendon in patellar drill holes show a low redislocation rate of 2% and medial hardware problems in approximately 7% of patients. The procedure is not able to eliminate apprehension and pain at the medial aspect of the patella. More persistent postoperative pain with activity is a problem that is related to patellofemoral chondral lesions. REFERENCES 1. Davis DK, Fithian DC. Techniques of medial retinacular repair and reconstruction. Clin Orthop Relat Res 2002: Hughston JC. Subluxation of the patella. J Bone Joint Surg Am 1968;50: Hautamaa PV, Fithian DC, Kaufman KR, Daniel DM, Pohlmeyer AM. Medial soft tissue restraints in lateral patellar instability and repair. Clin Orthop Relat Res 1998: Desio SM, Burks RT, Bachus KN. Soft tissue restraints to lateral patellar translation in the human knee. Am J Sports Med 1998;26: Mountney J, Senavongse W, Amis AA, Thomas NP. Tensile strength of the medial patellofemoral ligament before and after repair or reconstruction. J Bone Joint Surg Br 2005;87: Sallay PI, Poggi J, Speer KP, Garrett WE. Acute dislocation of the patella. A correlative pathoanatomic study. Am J Sports Med 1996;24: Nomura E. Classification of lesions of the medial patellofemoral ligament in patellar dislocation. Int Orthop 1999;23: Ellera Gomes JL. Medial patellofemoral ligament reconstruction for recurrent dislocation of the patella: A preliminary report. Arthroscopy 1992;8: Ellera Gomes JL, Stigler Marczyk LR, Cesar de Cesar P, Jungblut CF. Medial patellofemoral ligament reconstruction with semitendinosus autograft for chronic patellar instability: A follow-up study. Arthroscopy 2004;20: Fernandez E, Sala D, Castejon M. Reconstruction of the medial patellofemoral ligament for patellar instability using a semitendinosus autograft. Acta Orthop Belg 2005;71: Muneta T, Sekiya I, Tsuchiya M, Shinomiya K. A technique for reconstruction of the medial patellofemoral ligament. Clin Orthop Relat Res 1999: Drez D Jr, Edwards TB, Williams CS. Results of medial patellofemoral ligament reconstruction in the treatment of patellar dislocation. Arthroscopy 2001;17: Schöttle PB, Fucentese SF, Romero J. Clinical and radiological outcome of medial patellofemoral ligament reconstruction with a semitendinosus autograft for patella instability. Knee Surg Sports Traumatol Arthrosc 2005;13: Steensen RN, Dopirak RM, Maurus PB. Minimally invasive crescentic imbrication of the medial patellofemoral ligament for chronic patellar subluxation. Arthroscopy 2005;21: Camanho GL, Bitar AC, Hernandez AJ, Olivi R. Medial patellofemoral ligament reconstruction: A novel technique using the patellar ligament. Arthroscopy 2007;23:108.e1-108.e4. Available online at Steiner TM, Torga-Spak R, Teitge RA. Medial patellofemoral
6 MEDIAL PATELLOFEMORAL LIGAMENT RECONSTRUCTION 87 ligament reconstruction in patients with lateral patellar instability and trochlear dysplasia. Am J Sports Med 2006;34: Deie M, Ochi M, Sumen Y, Adachi N, Kobayashi K, Yasumoto M. A long-term follow-up study after medial patellofemoral ligament reconstruction using the transferred semitendinosus tendon for patellar dislocation. Knee Surg Sports Traumatol Arthrosc 2005;13: Nomura E, Horiuchi Y, Kihara M. A mid-term follow-up of medial patellofemoral ligament reconstruction using an artificial ligament for recurrent patellar dislocation. Knee 2000;7: Nomura E, Inoue M. Surgical technique and rationale for medial patellofemoral ligament reconstruction for recurrent patellar dislocation. Arthroscopy 2003;19:E47. Available online at Cossey AJ, Paterson R. A new technique for reconstructing the medial patellofemoral ligament. Knee 2005;12: Scuderi G, Cuomo F, Scott WN. Lateral release and proximal realignment for patellar subluxation and dislocation. A long-term follow-up. J Bone Joint Surg Am 1988;70: Aglietti P, Buzzi R, De Biase P, Giron F. Surgical treatment of recurrent dislocation of the patella. Clin Orthop Relat Res 1994: Zeichen J, Lobenhoffer P, Gerich T, Tscherne H, Bosch U. Medium-term results of the operative treatment of recurrent patellar dislocation by Insall proximal realignment. Knee Surg Sports Traumatol Arthrosc 1999;7: Brown DE, Alexander AH, Lichtman DM. The Elmslie-Trillat procedure: Evaluation in patellar dislocation and subluxation. Am J Sports Med 1984;12: Conti C, Berruto M, Bianchi M. The Elmslie-Trillat procedure for recurrent subluxation of the patella. One to five year follow-up. Ital J Orthop Traumatol 1992;18: Shelbourne KD, Porter DA, Rozzi W. Use of a modified Elmslie-Trillat procedure to improve abnormal patellar congruence angle. Am J Sports Med 1994;22: Peterson L, Karlsson J, Brittberg M. Patellar instability with recurrent dislocation due to patellofemoral dysplasia. Results after surgical treatment. Bull Hosp Jt Dis Orthop Inst 1988; 48: Myers P, Williams A, Dodds R, Bulow J. The three-in-one proximal and distal soft tissue patellar realignment procedure. Results, and its place in the management of patellofemoral instability. Am J Sports Med 1999;27: Cox JS. Evaluation of the Roux-Elmslie-Trillat procedure for knee extensor realignment. Am J Sports Med 1982;10:
Reconstruction of the medial patellofemoral ligament for treatment of patellar instability
 354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
Anatomical Medial Patellofemoral Ligament Reconstruction in Management of Cases of Patellar Instability
 Med. J. Cairo Univ., Vol. 84, No. 2, September: 145-151, 2016 www.medicaljournalofcairouniversity.net Anatomical Medial Patellofemoral Ligament Reconstruction in Management of Cases of Patellar Instability
Med. J. Cairo Univ., Vol. 84, No. 2, September: 145-151, 2016 www.medicaljournalofcairouniversity.net Anatomical Medial Patellofemoral Ligament Reconstruction in Management of Cases of Patellar Instability
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis Autograft without Bone Tunnel
 Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Jia Li 1, Yongqian Li 1, Jingchao Wei 2, Jianzhao Wang 1, Shijun Gao 1 and Yong Shen 1*
 Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Abstract. Introduction. Michele Vasso 1 Katia Corona 2 Giuseppe Toro 1 Marco Rossini 1 Alfredo Schiavone Panni 1
 256 Technical Note THIEME Anatomic Double-Bundle Medial Patellofemoral Ligament Reconstruction with Autologous Semitendinosus: Aperture Fixation Both at the Femur and the Patella Michele Vasso 1 Katia
256 Technical Note THIEME Anatomic Double-Bundle Medial Patellofemoral Ligament Reconstruction with Autologous Semitendinosus: Aperture Fixation Both at the Femur and the Patella Michele Vasso 1 Katia
ORIGINAL STUDY INTRODUCTION
 Acta Orthop. Belg., 2006, 72, 65-71 ORIGINAL STUDY Clinical results of isolated reconstruction of the medial patellofemoral ligament for recurrent dislocation and subluxation of the patella Yoshinori MIKASHIMA,
Acta Orthop. Belg., 2006, 72, 65-71 ORIGINAL STUDY Clinical results of isolated reconstruction of the medial patellofemoral ligament for recurrent dislocation and subluxation of the patella Yoshinori MIKASHIMA,
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction
 In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
Medial Patellofemoral Ligament Reconstruction
 53 Medial Patellofemoral Ligament Reconstruction Hany Elrashidy, Joseph Carney, Najeeb Khan, and Donald C. Fithian CHAPTER DEFINITION Stability of the patellofemoral joint (PFJ) is multifactorial as it
53 Medial Patellofemoral Ligament Reconstruction Hany Elrashidy, Joseph Carney, Najeeb Khan, and Donald C. Fithian CHAPTER DEFINITION Stability of the patellofemoral joint (PFJ) is multifactorial as it
Medial patellofemoral ligament reconstruction using dual patella docking technique
 2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
A Systematic Review Of Complications And Failures Associated With Medial Patellofemoral Ligament Reconstruction For Recurrent Patellar Dislocation
 Archived version from NCDOCKS Institutional Repository http://libres.uncg.edu/ir/asu/ A Systematic Review Of Complications And Failures Associated With Medial Patellofemoral Ligament Reconstruction For
Archived version from NCDOCKS Institutional Repository http://libres.uncg.edu/ir/asu/ A Systematic Review Of Complications And Failures Associated With Medial Patellofemoral Ligament Reconstruction For
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability
 Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
Isolated reconstruction of the medial patellofemoral ligament with autologous quadriceps tendon
 J Orthopaed Traumatol (2016) 17:155 162 DOI 10.1007/s10195-015-0375-6 ORIGINAL ARTICLE Isolated reconstruction of the medial patellofemoral ligament with autologous quadriceps tendon Giovanni Vavalle 1,2
J Orthopaed Traumatol (2016) 17:155 162 DOI 10.1007/s10195-015-0375-6 ORIGINAL ARTICLE Isolated reconstruction of the medial patellofemoral ligament with autologous quadriceps tendon Giovanni Vavalle 1,2
The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions T Smith, S Donell Citation T Smith, S Donell. The Rehabilitation
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions T Smith, S Donell Citation T Smith, S Donell. The Rehabilitation
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
MPFL reconstruction with autologous gracilis tendon using the two bone tunnel technique
 *smith&nephew Knee Technique Guide MPFL reconstruction with autologous gracilis tendon using the two bone tunnel technique Prof. Elvire Servien, MD, PhD Prof. Philippe Neyret, MD Knee Hip Shoulder Extremities
*smith&nephew Knee Technique Guide MPFL reconstruction with autologous gracilis tendon using the two bone tunnel technique Prof. Elvire Servien, MD, PhD Prof. Philippe Neyret, MD Knee Hip Shoulder Extremities
Functional outcome following modified Elmslie Trillat procedure
 The Knee 13 (2006) 464 468 www.elsevier.com/locate/knee Functional outcome following modified Elmslie Trillat procedure D. Karataglis, M.A. Green, D.J.A. Learmonth Royal Orthopaedic Hospital, Bristol Road
The Knee 13 (2006) 464 468 www.elsevier.com/locate/knee Functional outcome following modified Elmslie Trillat procedure D. Karataglis, M.A. Green, D.J.A. Learmonth Royal Orthopaedic Hospital, Bristol Road
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Original Article A biomechanical study of different techniques in medial patellofemoral ligament reconstruction
 Int J Clin Exp Med 2016;9(8):15235-15242 www.ijcem.com /ISSN:1940-5901/IJCEM0023348 Original Article A biomechanical study of different techniques in medial patellofemoral ligament reconstruction Junhang
Int J Clin Exp Med 2016;9(8):15235-15242 www.ijcem.com /ISSN:1940-5901/IJCEM0023348 Original Article A biomechanical study of different techniques in medial patellofemoral ligament reconstruction Junhang
Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
 Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Short-/Intermediate-Term Outcomes after Medial Patellofemoral Ligament Reconstruction in the Treatment of Chronic Lateral Patellofemoral Instability
 The Physician and Sportsmedicine ISSN: 0091-3847 (Print) 2326-3660 (Online) Journal homepage: http://www.tandfonline.com/loi/ipsm20 Short-/Intermediate-Term Outcomes after Medial Patellofemoral Ligament
The Physician and Sportsmedicine ISSN: 0091-3847 (Print) 2326-3660 (Online) Journal homepage: http://www.tandfonline.com/loi/ipsm20 Short-/Intermediate-Term Outcomes after Medial Patellofemoral Ligament
Surgical treatment of patellar instability can be
 Medial Patellofemoral Ligament Reconstruction Using a Modified Reverse-Loop Technique Nels E. Sampatacos, M.D., and Mark H. Getelman, M.D. Abstract: Medial patellofemoral ligament reconstruction is a commonly
Medial Patellofemoral Ligament Reconstruction Using a Modified Reverse-Loop Technique Nels E. Sampatacos, M.D., and Mark H. Getelman, M.D. Abstract: Medial patellofemoral ligament reconstruction is a commonly
International Journal of Orthopaedics Sciences 2017; 3(3): Dr. Anas M and Dr. Ansari N. DOI:
 2017; 3(3): 588-592 ISSN: 2395-1958 IJOS 2017; 3(3): 588-592 2017 IJOS www.orthopaper.com Received: 23-05-2017 Accepted: 24-06-2017 Dr. Anas M MS(Orthopaedics) Senior Resident Department of Dr. Ansari
2017; 3(3): 588-592 ISSN: 2395-1958 IJOS 2017; 3(3): 588-592 2017 IJOS www.orthopaper.com Received: 23-05-2017 Accepted: 24-06-2017 Dr. Anas M MS(Orthopaedics) Senior Resident Department of Dr. Ansari
PROSPECTIVE AND COMPAR TMENT (MEDIAL PETELLOFEMOR
 ORIGINAL ARTICLE PROSPECTIVE AND COMPAR ARATIVE STUDY BETWEEN CONSERVATIVE AND SURGICAL TREATMENT TMENT (MEDIAL PETELLOFEMOR OFEMORAL LIGAMENT REPAIR) IN PATELL TELLAR ACUTE DISLOCA OCATIONS GILBERTO LUIS
ORIGINAL ARTICLE PROSPECTIVE AND COMPAR ARATIVE STUDY BETWEEN CONSERVATIVE AND SURGICAL TREATMENT TMENT (MEDIAL PETELLOFEMOR OFEMORAL LIGAMENT REPAIR) IN PATELL TELLAR ACUTE DISLOCA OCATIONS GILBERTO LUIS
Jacques Menetrey, MD, PD. Uniklinik Balgrist. Unité d Orthopédie et Traumatologie du Sport (UOTS)
 Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
DISCLOSURES. Overview 09/24/2015. Patellofemoral Instability and Treatment Options. I do not have anything to disclose
 Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Acute patellar dislocation in adults
 CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery. Restore patella stability.
 Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Extensor Mechanism Rupture
 Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. MPFL RECONSTRUCTION
 ! SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. LATERAL PATELLOFEMORAL INSTABILITY AND THE MEDIAL PATELLOFEMORAL COMPLEX Lateral patellofemoral instability is characterized
! SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. LATERAL PATELLOFEMORAL INSTABILITY AND THE MEDIAL PATELLOFEMORAL COMPLEX Lateral patellofemoral instability is characterized
All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes
 All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes William Godfrey, BS Aaron Gebrelul, BA; John Xerogeanes, MD; Ajay
All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes William Godfrey, BS Aaron Gebrelul, BA; John Xerogeanes, MD; Ajay
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
The American Journal of Sports Medicine
 The American Journal of Sports Medicine http://ajs.sagepub.com/ Femoral Avulsion of the Medial Patellofemoral Ligament After Primary Traumatic Patellar Dislocation Predicts Subsequent Instability in Men
The American Journal of Sports Medicine http://ajs.sagepub.com/ Femoral Avulsion of the Medial Patellofemoral Ligament After Primary Traumatic Patellar Dislocation Predicts Subsequent Instability in Men
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
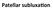 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
8/9/2017. Case Based: Beyond Medial Patellofemoral Ligament. Editorial Board AJSM Social Media. Consultant. Not talking about PF pain/chondrosis Rehab
 Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
The Three-In-One Proximal and Distal Soft Tissue Patellar Realignment Procedure
 0363-5465/99/2727-0575$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 27, No. 5 1999 American Orthopaedic Society for Sports Medicine The Three-In-One Proximal and Distal Soft Tissue Patellar Realignment
0363-5465/99/2727-0575$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 27, No. 5 1999 American Orthopaedic Society for Sports Medicine The Three-In-One Proximal and Distal Soft Tissue Patellar Realignment
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Medial patellofemoral ligament reconstruction
 KNEE Medial patellofemoral ligament reconstruction A PROSPECTIVE OUTCOME ASSESSMENT OF A LARGE SINGLE CENTRE SERIES N. R. Howells, A. J. Barnett, N. Ahearn, A. Ansari, J. D. Eldridge From Bristol Royal
KNEE Medial patellofemoral ligament reconstruction A PROSPECTIVE OUTCOME ASSESSMENT OF A LARGE SINGLE CENTRE SERIES N. R. Howells, A. J. Barnett, N. Ahearn, A. Ansari, J. D. Eldridge From Bristol Royal
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents
 Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Hong-De Wang, Jiang-Tao Dong and Shi-Jun Gao *
 Wang et al. Journal of Orthopaedic Surgery and Research (2016) 11:138 DOI 10.1186/s13018-016-0473-z TECHNICAL NOTE Open Access Medial patellofemoral ligament reconstruction using a bone groove and a suture
Wang et al. Journal of Orthopaedic Surgery and Research (2016) 11:138 DOI 10.1186/s13018-016-0473-z TECHNICAL NOTE Open Access Medial patellofemoral ligament reconstruction using a bone groove and a suture
Retinacular tear knee
 P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
Patellofemoral instability is a common cause of knee
 280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-93 Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common
280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-93 Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia
 Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Introduction. Helmut Wegmann 1 Christoph Würnschimmel 2 Tanja Kraus 2 Georg Singer 1 Robert Eberl 1 Holger Till 1 Matthias Sperl 2
 DOI 10.1007/s00167-017-4425-x KNEE Medial patellofemoral ligament (MPFL) reconstruction in combination with a modified grammont technique leads to favorable mid-term results in adolescents with recurrent
DOI 10.1007/s00167-017-4425-x KNEE Medial patellofemoral ligament (MPFL) reconstruction in combination with a modified grammont technique leads to favorable mid-term results in adolescents with recurrent
Figure 3 Figure 4 Figure 5
 Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
ARTICLE IN PRESS. Technical Note
 Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
Minimally invasive medial patellofemoral ligament reconstruction for patellar instability using an artificial ligament: A two year follow-up
 The University of Notre Dame Australia ResearchOnline@ND Medical Papers and Journal Articles School of Medicine 2016 Minimally invasive medial patellofemoral ligament reconstruction for patellar instability
The University of Notre Dame Australia ResearchOnline@ND Medical Papers and Journal Articles School of Medicine 2016 Minimally invasive medial patellofemoral ligament reconstruction for patellar instability
Patellar Instability With and Without Trochlear Dysplasia: New Arthroscopic Medial Soft Tissue Plication With Pullout Technique
 Patellar Instability With and Without Trochlear Dysplasia: New Arthroscopic Medial Soft Tissue Plication With Pullout Technique Jin Hwan Ahn, MD, PhD; Jun Hee Kang, MD; Niraj Sharad Kasat, MD; Jae Gyoon
Patellar Instability With and Without Trochlear Dysplasia: New Arthroscopic Medial Soft Tissue Plication With Pullout Technique Jin Hwan Ahn, MD, PhD; Jun Hee Kang, MD; Niraj Sharad Kasat, MD; Jae Gyoon
CHRONIC PATELLOFEMORAL INSTABILITY
 INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation
INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation
The role of Tibial Tubercle Osteotomies in 2017
 ISAKOS ICL #7: How to Strategically Manage Complex Patellar Instability The role of Tibial Tubercle Osteotomies in 2017 Elizabeth A. Arendt, MD Department of Orthopaedic Surgery, University of Minnesota,
ISAKOS ICL #7: How to Strategically Manage Complex Patellar Instability The role of Tibial Tubercle Osteotomies in 2017 Elizabeth A. Arendt, MD Department of Orthopaedic Surgery, University of Minnesota,
Medial Patellofemoral Ligament Reconstruction
 Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
The Operative Management of Patella Malalignment
 The Open Orthopaedics Journal, 2012, 6, (Suppl 2: M11) 327-339 327 The Operative Management of Patella Malalignment Alexios Dimitrios Iliadis *,1, Parag Kumar Jaiswal 1, Wasim Khan 2 and David Johnstone
The Open Orthopaedics Journal, 2012, 6, (Suppl 2: M11) 327-339 327 The Operative Management of Patella Malalignment Alexios Dimitrios Iliadis *,1, Parag Kumar Jaiswal 1, Wasim Khan 2 and David Johnstone
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Anatomy and Sports Injuries of the Knee
 Anatomy and Sports Injuries of the Knee I. Anatomy II. Assessment III. Treatment IV. Case Study V. Dissection Anatomy Not a hinge joint 6 degrees of freedom Flexion/Extension Rotation Translation Anatomy
Anatomy and Sports Injuries of the Knee I. Anatomy II. Assessment III. Treatment IV. Case Study V. Dissection Anatomy Not a hinge joint 6 degrees of freedom Flexion/Extension Rotation Translation Anatomy
ACL Reconstruction Cross-Pin Technique
 ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
Valgus instability as a cause for recurrent lateral patellar dislocation : A new mechanism for patellofemoral instability?
 Acta Orthop. Belg., 2013, 79, 495-501 ASPECT OF CURRENT MANAGEMENT Valgus instability as a cause for recurrent lateral patellar dislocation : A new mechanism for patellofemoral instability? Kristof Hermans,
Acta Orthop. Belg., 2013, 79, 495-501 ASPECT OF CURRENT MANAGEMENT Valgus instability as a cause for recurrent lateral patellar dislocation : A new mechanism for patellofemoral instability? Kristof Hermans,
Human ACL reconstruction
 Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Iliotibial Band Tension Reduces Patellar Lateral Stability
 Iliotibial Band Tension Reduces Patellar Lateral Stability Azhar M. Merican, 1,2 Farhad Iranpour, 2 Andrew A. Amis 2,3 1 Department of Orthopaedic Surgery, University Malaya Medical Centre, 50603 Kuala
Iliotibial Band Tension Reduces Patellar Lateral Stability Azhar M. Merican, 1,2 Farhad Iranpour, 2 Andrew A. Amis 2,3 1 Department of Orthopaedic Surgery, University Malaya Medical Centre, 50603 Kuala
Medial Patellofemoral Ligament Reconstruction: A Longitudinal Study Comparison of 2 Techniques with 2 and 5-Years Follow-Up
 Send Orders for Reprints to reprints@benthamscience.ae 198 The Open Orthopaedics Journal, 2015, 9, 198-203 Open Access Medial Patellofemoral Ligament Reconstruction: A Longitudinal Study Comparison of
Send Orders for Reprints to reprints@benthamscience.ae 198 The Open Orthopaedics Journal, 2015, 9, 198-203 Open Access Medial Patellofemoral Ligament Reconstruction: A Longitudinal Study Comparison of
MCL Injuries: When and How to Repair Scott D. Mair, MD
 MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Cronicon ORTHOPAEDICS
 Cronicon OPEN ACCESS ORTHOPAEDICS Research Article Evaluation of Arthroscopic posterior Cruciate ligament reconstruction by using Quadrable hamstring tendon autograft and endobutton fixation: minimal 2
Cronicon OPEN ACCESS ORTHOPAEDICS Research Article Evaluation of Arthroscopic posterior Cruciate ligament reconstruction by using Quadrable hamstring tendon autograft and endobutton fixation: minimal 2
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Jae-Ang Sim 1, Jin-Kyu Lim 2 and Byung Hoon Lee 2*
 Sim et al. BMC Musculoskeletal Disorders (2018) 19:346 https://doi.org/10.1186/s12891-018-2261-x TECHNICAL ADVANCE Open Access Anatomic double-bundle medial patellofemoral ligament reconstruction with
Sim et al. BMC Musculoskeletal Disorders (2018) 19:346 https://doi.org/10.1186/s12891-018-2261-x TECHNICAL ADVANCE Open Access Anatomic double-bundle medial patellofemoral ligament reconstruction with
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Graft choice for anterior cruciate ligament (ACL)
 Technical Note Arthroscopic Anterior Cruciate Ligament Reconstruction Using Quadriceps Tendon Autograft and Bioabsorbable Cross-Pin Fixation Emmanuel Antonogiannakis, M.D., Christos K. Yiannakopoulos,
Technical Note Arthroscopic Anterior Cruciate Ligament Reconstruction Using Quadriceps Tendon Autograft and Bioabsorbable Cross-Pin Fixation Emmanuel Antonogiannakis, M.D., Christos K. Yiannakopoulos,
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
Patellar Instability. Michael J. Alaia, M.D., Randy M. Cohn, M.D., and Eric J. Strauss, M.D. Anatomy and Biomechanics
 6 Bulletin of the Hospital for Joint Diseases 2014;72(1):6-17 Patellar Instability Michael J. Alaia, M.D., Randy M. Cohn, M.D., and Eric J. Strauss, M.D. Abstract Patellar instability is a complex pathoanatomical
6 Bulletin of the Hospital for Joint Diseases 2014;72(1):6-17 Patellar Instability Michael J. Alaia, M.D., Randy M. Cohn, M.D., and Eric J. Strauss, M.D. Abstract Patellar instability is a complex pathoanatomical
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Patellar instability
 Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
ACL Rehabilitation and Return To Play
 ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
MPFL positioning on the femoral side
 MPFL positioning on the femoral side Stephen et al AJSM 2012 Prof Dr med Jacques Menetrey, MD, PhD Dr med Philippe Tscholl, MD Centre de médecine de l appareil moteur et du sport - HUG Swiss Olympic medical
MPFL positioning on the femoral side Stephen et al AJSM 2012 Prof Dr med Jacques Menetrey, MD, PhD Dr med Philippe Tscholl, MD Centre de médecine de l appareil moteur et du sport - HUG Swiss Olympic medical
Shape and size of the medial patellofemoral ligament for the best surgical reconstruction: a human cadaveric study
 Shape and size of the medial patellofemoral ligament for the best surgical reconstruction: a human cadaveric study G. Placella, M. M. Tei, E. Sebastiani, G. Criscenti, A. Speziali, C. Mazzola, A. Georgoulis
Shape and size of the medial patellofemoral ligament for the best surgical reconstruction: a human cadaveric study G. Placella, M. M. Tei, E. Sebastiani, G. Criscenti, A. Speziali, C. Mazzola, A. Georgoulis
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Aperture fixation instead of transverse tunnels at the patella for medial patellofemoral ligament reconstruction
 Knee Surg Sports Traumatol Arthrosc (2012) 20:322 326 DOI 10.1007/s00167-011-1582-1 KNEE Aperture fixation instead of transverse tunnels at the patella for medial patellofemoral ligament reconstruction
Knee Surg Sports Traumatol Arthrosc (2012) 20:322 326 DOI 10.1007/s00167-011-1582-1 KNEE Aperture fixation instead of transverse tunnels at the patella for medial patellofemoral ligament reconstruction
The medial side of the knee has been relatively overlooked
 REVIEW ARTICLE Medial and Posteromedial Instability of the Knee: Evaluation, Treatment, and Results James P. Stannard, MD Abstract: Medial-sided knee ligament injuries are complex and require a thorough
REVIEW ARTICLE Medial and Posteromedial Instability of the Knee: Evaluation, Treatment, and Results James P. Stannard, MD Abstract: Medial-sided knee ligament injuries are complex and require a thorough
Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft
 384 Clinicale Evaluation Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft Swaroop Patel, Resident, Vijendra D. Chauhan, Professor, Anil Juyal, Professor, Rajesh
384 Clinicale Evaluation Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft Swaroop Patel, Resident, Vijendra D. Chauhan, Professor, Anil Juyal, Professor, Rajesh
OMICS - 3rd Int. Conference & 2
 KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
The Role of Medial Patellofemoral Ligament Repair and Imbrication
 A Review Paper The Role of Medial Patellofemoral Ligament Repair and Imbrication Kyle R. Duchman, MD, and Matthew J. Bollier, MD Abstract Repair, reefing, and advancement of the medial patellofemoral ligament
A Review Paper The Role of Medial Patellofemoral Ligament Repair and Imbrication Kyle R. Duchman, MD, and Matthew J. Bollier, MD Abstract Repair, reefing, and advancement of the medial patellofemoral ligament
Bone patellar tendon bone autograft versus LARS artificial ligament for anterior cruciate ligament reconstruction
 Eur J Orthop Surg Traumatol (2013) 23:819 823 DOI 10.1007/s00590-012-1073-1 ORIGINAL ARTICLE Bone patellar tendon bone autograft versus LARS artificial ligament for anterior cruciate ligament reconstruction
Eur J Orthop Surg Traumatol (2013) 23:819 823 DOI 10.1007/s00590-012-1073-1 ORIGINAL ARTICLE Bone patellar tendon bone autograft versus LARS artificial ligament for anterior cruciate ligament reconstruction
K n e e b r a f o r l a t e p a t e l l a r r e t i n a c u
 K n e e b r a f o r l a t e p a t e l l a r r e t i n a c u 20-11-2012 Retinaculum Knee Catherine Blake. Loading. Anatomy Of The Patellar Tendon. Arthroscopic Lateral Release and Medial Imbrication. What
K n e e b r a f o r l a t e p a t e l l a r r e t i n a c u 20-11-2012 Retinaculum Knee Catherine Blake. Loading. Anatomy Of The Patellar Tendon. Arthroscopic Lateral Release and Medial Imbrication. What
AJO. Medial patellar subluxation (MPS) is a disabling condition. Medial Patellar Subluxation: Diagnosis and Treatment.
 A Review Paper Medial Patellar Subluxation: Diagnosis and Treatment Michael G. Saper, DO, and David A. Shneider, MD system with separate distinct anatomical structures. The lateral Abstract retinaculum
A Review Paper Medial Patellar Subluxation: Diagnosis and Treatment Michael G. Saper, DO, and David A. Shneider, MD system with separate distinct anatomical structures. The lateral Abstract retinaculum
World Medical & Health Games
 Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
BioRCI Screw System. Surgical Technique for Hamstring and Patellar Tendon Grafts
 BioRCI Screw System Surgical Technique for Hamstring and Patellar Tendon Grafts Surgical Technique for Hamstring and Patellar Tendon Grafts Using the BioRCI Screw System The Smith & Nephew BioRCI cruciate
BioRCI Screw System Surgical Technique for Hamstring and Patellar Tendon Grafts Surgical Technique for Hamstring and Patellar Tendon Grafts Using the BioRCI Screw System The Smith & Nephew BioRCI cruciate
Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella Treated with a Different Method in Each Knee
 Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Medial Patellofemoral Ligament Reconstruction SURGICAL TECHNIQUE
 SURGICAL TECHNIQUE Contributing Surgeons R. Justin Mistovich, MD Assistant Professor Pediatric Orthopaedic Surgery Case Western Reserve University School of Medicine Cleveland, OH USA Nirav Pandya, MD
SURGICAL TECHNIQUE Contributing Surgeons R. Justin Mistovich, MD Assistant Professor Pediatric Orthopaedic Surgery Case Western Reserve University School of Medicine Cleveland, OH USA Nirav Pandya, MD
