SURGICAL TECHNIQUE FRACTURE - SUBTALAR ARTHRODESIS
|
|
|
- Felicity Jordan
- 6 years ago
- Views:
Transcription
1 SURGICAL TECHNIQUE FRACTURE - SUBTALAR ARTHRODESIS Mario GOLDZAK *, Thomas MITTLMEIER** and Patrick SIMON *** * Clinique de l Union Saint Jean - France ** Chirurgischen Klinik und Policlinik der Universität Rostock - D Rostock - Germany *** Centre hospitalier Saint Joseph Saint Luc - 20 quai Claude Bernard Lyon - France
2 2 - FRACTURE - CALCAnail technique: - Minimally invasive percutaneous approach at the posterior calcaneal tuberosity avoids complications associated with standard lateral ORIF approach - Locking nail holds posterior facet articular surface in the proper position after intrafocal reduction - Option to convert easily from internal fixation procedure to subtalar fusion SURGICAL - FOR FRACTURES - Anatomopathology of posterior facet fractures of the calcaneus Calcaneal fractures can be easily understood and analysed on the preoperative CT-scan once the position of the Palmer s fundamental fracture line has been located. When the shear line is medial, a large lateral articular fragment will tilt and pivot, pushing into the calcaneal body behind the angle of Gissane or «crucial angle», just behind the sinus tarsi. This is a vertical fracture (Fig.1a). When the shear line is lateral, there is a large medial fragment that may or may not push down: most often the posterior calcaneal tuberosity and the rest of the calcaneus are moved up and displaced in a varus, flexed position. This is a horizontal fracture (Fig.1b). When the shear line is located in the middle of the dorsal side of the talar articular surface, the lateral fragment tilts and the medial fragment pushes down to create a double contour. This is a mixed fracture (Fig.1c). The posterior ending of the fracture line must also be analyzed: if the retrothalmic line is located on the upper cortex of the fractured calcaneum, it is a tongue-type fracture (Fig.1d); if the line goes toward the posterior facet of the posterior calcaneal tuberosity, it is a joint depression-type fracture (Fig.1e). Fig.1a vertical fracture Fig.1d Tongue-Type fracture Fig.1b horizontal fracture Fig.1c mixed fracture Fig.1e Depression-Type fracture Surgical technique
3 3 Preoperative planning Preoperative CT scans for articular fractures of the calcaneus have become routine. A minimum of 250 thin, contiguous slices of the calcaneus must be made in order to obtain volume rendering reconstructions. Simple sagittal and horizontal reconstructions are not, in fact, sufficient for a quality analysis. Radiology station software or the software Osirix for Mac make it possible to create the reconstructions on one s own. The bones surrounding the calcaneus must be removed step-by-step by rotating the calcaneus on its axis. This may take 5 to 15 minutes depending on practice. At the end of the procedure, the superior, lateral, medial, and anterior views will make it possible to closely analyse the type of fracture, the exact position of the separation line, and the size of the depressed fragment(s). Surgical indications Vertical and mixed fractures are incongruent, so surgical indications are logical. Fractures with a horizontal depression should be operated if the loss of height assessed with the Böhler angle is significant, or roughly <10. Horizontal and vertical fractures, which affect the whole joint unit, are easy to reduce. Whether the line is medial (vertical fractures) or lateral (horizontal fractures), a large, intact articular fragment only needs to be repositioned under the talus. Mixed fractures are more difficult to treat. First the medial fragment must be reduced to correct the overlap on the medial cortex which is very visible on the CT scan, then the lateral fragment is reduced without a step between these two fragments. Patient positioning Two positions are possible: The patient is usually placed on his/her side with the flexed limb resting on a pad and the foot off the table. Lateral and retrotibial fluoroscopy views are taken by externally rotating the foot and tipping the C-arm along the table axis. Alternatively, the patient can be placed prone with the knee flexed so the leg is placed at 45 relative to the table, particularly if it is a bilateral fracture.
4 4 Step 1: Placement of K-wire in posterior tuberosity Fig.2a Lateral view At the junction between the posterior and plantar aspect of the heel, use a scalpel to perform a posterior incision down to the bone. The incision starts from the lowest part of the posterior calcaneal tuberosity and goes up in a posterior direction for 20 mm. The Φ10 mm K-wire with stopper (Ref ) is inserted under power; it must be placed in the correct position as this determines the orientation of the work chamber and later on, the nail position. On the lateral view, the K-wire must be aligned with the posterior calcaneal bone trabeculae, about 45 top to bottom and back to front. Its proximal end must be placed under the displaced talar fragments and above the angle of Gissane (Fig.2a). On the retrotibial view, the K-wire is typically aligned with the middle of the calcaneal tuberosity axis; this roughly corresponds to the axis of the 4th interdigital space. Depending on the location of the primary fracture line the K-wire should be placed into the larger fragment (eg. Sanders II-B fracture). At this point, the varus displacement of the posterior tuberosity can be ignored as it will be automatically corrected when the distractor is positioned in place (Fig.2b). Fig.3a Fig.2b Retrotibial view Step 2: Placement of subtalar distractor Fig.3b The second surgical step consists of placing a Caspar-type subtalar distractor on two K-wires, one in the talus and one in the posterior calcaneal tuberosity. This distractor (Ref ) is used to correct the varus deformity of the posterior tuberosity and to distract the subtalar joint so the depressed articular surface can be reduced. Two Φ3.2 mm K-wires (Ref ) will be placed across the foot axis. They cross the talus and the calcaneum, must be palpable under the medial aspect of the foot, and must not breach the skin. For a depression fracture, place the calcaneal K-wire in the posterosuperior part of the posterior tuberosity at least 10 mm above the future tunneling point in the tuberosity ( denotes the position). For a tongue-type fracture place the K-wire in the inferior part of the poste rior tuberosity 10 mm below the future tunnel ( denotes the position). A positioning square is available (Ref ) to position this K-wire perpendicular to the previously positioned K-wire with stopper (Fig. 3a). Place the talar K-wire perpendicular to the lateral aspect of the talus, in the lateral tubercle at the center of the talar dome, making sure not to injure the lateral peroneal tendons (Fig. 3b). Position the Caspar distractor onto the K-wires in a non-distracted position and tighten the thumb screws to the K-wires (Fig. 4). Surgical technique
5 5 Fig.4 Step 3: Preparation of work chamber The third step consists of introducing the Φ10 mm hollow reamer (Ref ) over the K-wire with stopper (Fig. 5). Make sure the K-wire does not poke out of the reamer windows. Aim the hollow reamer below the depressed articular fragments, without making them more fragile, and above the critical angle (Angle of Gissane). Under fluoroscopy ensure the hollow reamer does not deviate from the axis of the K-wire. If deviation occurs, withdraw the hollow reamer and reinsert ensuring axial alignment with the K-wire is maintained. Remove the hollow reamer and the K-wire with stopper; a 2-3 cm bone plug can then be removed and may be used at the end of the procedure to fill the hollow nail and/or graft the subtalar joint in an arthrodesis. (Fig. 6). Fig.5 Fig.6 SURGICAL TIPS AND TRICKS To remove the bone plug, grip it with a Kelly or Kocher clamp and slowly remove the K-wire with stopper using a motor drive.
6 6 Step 4: Fracture reduction To correct the posterior tuberosity varus and loss of calcaneal height, turn the large thumbscrew on the distractor several turns to gradually distract the subtalar joint.. The distractor can be used with some force, even if it causes minor damage to the skin, near the K-wires, which can be sutured when the incision is closed (Fig. 6a). Use the curved tamp (Ref ), straight tamp (Ref ), spatula (Ref ), and light mallet taps to free up the fragments and push them towards the talus into the empty space created by the distractor. Begin by pushing the medial fragment to correct the overlap of the medial cortex (Fig. 6b and 6c), then reduce the lateral fragment by changing the orientation of the curved tamp (Fig. 6d and 6e). Use lateral fluoroscopy views to track the reduction until the subtalar joint line is congruent and the critical angle of Gissane and Bohler s angle are restored (Fig. 7). At the end of the procedure, verify the reduction on the retrotibial view. Fig.6a Fig.6b Fig.7 Fig.6c Fig.6d Fig.6e Surgical technique
7 7 Step 5: Nail introduction The length of nail required is determined using the nail guide (Ref ) and nail length gauge (Ref ). The nail length gauge must be inserted until the tip is against the cortex of the posterior facet (Fig. 8a). The nail is available in three lengths: 45, 50 and 55 mm (see reference table 1 ). Place the selected nail onto the nail holder with the ball end of the T-handle on the same side as the D-shaped holes on the medial side of the nail. Use the handlenail connector screw (Φ10 mm) to secure the nail holder to the nail. Handle-nail connector screw Ø10 mm: Ref Nail holder Ø10 mm: Ref Fig. 8a If desired, insert the harvested cancellous bone plug into the nail and position it to cover the nail windows (Fig. 8b). Alternatively, all or part of the bone plug can be used to graft the underside of the articular surface before the nail is introduced. Introduce the nail into the work chamber using small rotating motions, and then bring it up to the underside of the previously raised articular fragments (Fig. 8c). Make sure the teeth on the nail make contact with the cancellous bone in the articular fragments to support them. The nail holder is positioned so that the ball end of the T-handle is on the medial side. To ensure the proximal end of the nail is fully engaged in the bone, loosen the handle nail connector (Ref ) one full turn and pull back on the T-handle to create separation with the nail. Now the proximal end of the nail is visible under fluoroscopy. Fig. 8b Once the nail is in place, put the Φ10 mm fracture nail alignment frame (Ref ) onto the lateral arm of the nail holder and secure in place using the nail holder connecting screw (Ref ) (Fig. 9a). After placement of the drill guide for K-wires (Ref ), through the holes of the nail alignment frame corresponding to the nail length selected, under power the K-wires for cannulated screws Φ1.6 x 200 mm (Ref ) are introduced until bicortical (Fig. 9b and 9c). Fig.8c SURGICAL TIPS AND TRICKS: POSITIONING THE K-WIRES FOR SCREWS Take care, the K-wires can accidentally go through the skin and cause the measuring to be wrong. Fig.9a Fig.9b Fig.9c
8 8 Remove the drill guide and use the cannulated screw length gauge (Ref ) to measure the required screw length. Typically, 30 mm to 32 mm screws are used (see reference table 2). The K-wires can be further inserted to puncture through the medial skin so they can be retained with hemostats. Use the Φ 3.7 mm cannulated drill bit (Ref ) over the Φ1.6 mm K-wires (Fig.10a). The screws are placed using a cannulated screwdriver (Ref ) and tightened enough to compress the fragments and transversely reduce the calcaneus (Fig. 10b and 10c). On the axial view, check that the screws are well inserted, and not too long. Furthermore, if the interfragmentary gap needs to be reduced at the separation line, the screw can be tightened until the screw head makes contact with the lateral wall of the nail, which will provide excellent interfragmentary compression. Fig.10a Once the locking step is completed, the distractor can be withdrawn. SURGICAL TIPS AND TRICKS: JOINT DEPRESSION-TYPE FRACTURES Tongue-type fractures or depression fractures are sometimes difficult to reduce. It may be helpful to insert a Steinmann pin in the fragment and reduce the displacement using a levering motion as one would for closed lifting-nailing. It may also be useful to open up access to the fragment at the Angle of Gissane using a sinus tarsi incision. Lastly, it is possible to perfect the closure of the posterior facet by introducing an oblique screw through the fibers of the Achilles tendon and putting it though the slots of the nail and the plantar cortex. Fig.10c Fig.10b Depending on the distance between the end of the nail and posterior tuberosity cortex, a cap can be placed on the nail to make it easier to remove later on. The cap is positioned with the cannulated screwdriver. Engagement can be facilitated by insertion of a Φ1.6 mm K-wire into the nail (Fig. 10d). Fig.10d Surgical technique
9 9 >>>>> Final appearance 1 1 Reference Fracture Nail Φ10 mm CALCAnail Nail Φ10 L 45 + Cap CALCAnail Nail Φ10 L 50 + Cap CALCAnail Nail Φ10 L 55 + Cap 2 Reference Screw Cannulated screw Φ5 L 24 mm Cannulated screw Φ5 L 26 mm Cannulated screw Φ5 L 28 mm Cannulated screw Φ5 L 30 mm Cannulated screw Φ5 L 32 mm Cannulated screw Φ5 L 34 mm Cannulated screw Φ5 L 36 mm Cannulated screw Φ5 L 38 mm Cannulated screw Φ5 L 40 mm Post-operative care The patient may begin ambulating immediately following surgery using crutches and non-weight bearing. A pain relieving foot brace is recommended and good wound healing must be observed. Treatment continues for the first 15 days. Afterwards, the patient may then begin walking using two crutches and a heel rest for the following three weeks. After the fifth week, the patient can walk in normal shoes and subtalar physical therapy is started.
10 10 - SUBTALAR ARTHRODESIS - The arthrodesis version of the CALCAnail is used in the following scenarios: - Recent comminuted fractures where internal fixation is impossible or destined to fail because of the seriousness of the cartilage injuries (mixed fractures with 2 or more fracture lines; comminuted fractures) - Calcaneal fracture sequelae in cases with post-traumatic osteoarthritis and/or poor functional results - Degeneration of the posterior subtalar joint or valgus flatfoot deformities. SURGICAL TECHNIQUE - FOR SUBTALAR ARTHRODESIS - Patient positioning Two positions are possible: lateral and prone. The patient is usually placed on his/her side with the flexed limb resting on a pad and the foot off the table. Lateral and retrotibial fluoroscopy views are taken by externally rotating the foot and tipping the C-arm along the table axis. Alternatively, the patient can be placed prone with the knee flexed so the leg is placed at 45 relative to the table, particularly if it is a bilateral fracture. Surgical technique
11 11 Step 1: Placement of K-wire in posterior tuberosity At the junction between the posterior and plantar aspect of the heel, use a scalpel to perform a posterior incision down to the bone. The incision starts from the lowest part of the posterior calcaneal tuberosity and goes up in a posterior direction for 20 mm. The Φ12 K-wire with stopper (Ref ) must be placed in the correct position as this determines the orientation of the work chamber and later on, the nail position (Fig. 1a, 1b and 1c). On the lateral view, the K-wire should be positioned in the direction of the talar dome and above the angle of Gissane. The K-wire should not be too vertical and should pass through the sinus tarsi to avoid future conflict between the fibula and CALCAnail talar screw. On the retrotibial view, K-wire placement must take into account the subtalar angle; this roughly corresponds to the axis of the first interdigital space. Depending on the location of the primary fracture line the K-wire may be positioned more Fig.2 Fig.1a Fig.1b Fig.1c Step 2: Placement of subtalar distractor The second surgical step consists of placing a Caspar-type subtalar distractor (Ref ) onto two K-wires, one in the talus and one in the posterior calcaneal tuberosity. If needed, these Φ3.2 mm K-wires (Ref ) are used with the distractor to correct the varus deformity of the posterior tuberosity and distract the subtalar joint so the depressed articular surface can be reduced. Conversely, they can be used with the compressor (Ref ) to remove the joint space and bring the freshened talar and calcaneal articular surfaces together. Two Φ3.2 mm K-wires (Ref ) will be placed across the foot axis. Place the calcaneal K-wire in the posterosuperior part of the posterior tuberosity at least 10 mm above for a depression fracture or below for a tongue fracture of the future tunneling point in the tuberosity. A positioning square is available (Ref ) to position this wire perpendicular to the previously positioned K-wire with stopper. Place the talar K-wire perpendicular to the lateral aspect of the talus, in the lateral tubercle at the center of the talar dome, making sure not to injure the lateral peroneal tendons. Palpate the medial aspect of the foot to locate the K-wires crossing the talus and calcaneus and make sure they do not perforate the skin. Position the distractor or compressor onto the K-wires and tighten the thumb screws (Fig. 2).
12 12 Step 3: Preparation of work chamber If a varus deformity is to be corrected then first insert the Φ12 mm K-wire with stopper so that it is only engaged in the calcaneous. To accomplish this either select the short Φ12 mm K-wire with stopper or if not available only insert the K-wire such that it does not cross the subtalar joint. This may leave the stopper short of being in contact with the calcaneal tuberosity. If there is no varus deformity to be corrected then select the length of Φ12 mm K-wire with stopper so that the talus is also engaged. The third step consists of introducing the Φ12 mm hollow reamer (Ref ) over the first K-wire with stopper. Make sure the K-wire does not poke out of the reamer windows. Ream until the articular surface of the calcaneus is crossed; remove the reamer and bone plug. If necessary activate the distractor so that a varus deformity can be corrected and/or an intrafocal reduction completed. Reintroduce the Φ12 mm K-wire with stopper (Ref ) into the created calcaneal tunnel and into the talus. Reintroduce the Φ12 mm hollow reamer (Ref ) into the calcaneal tunnel and ream until 10 mm below the anterior talar cortex. It is not necessary to retrieve the talar bone plug if it is not retained within the hollow reamer as it will fit into the hollow nail. Fig.3 This reaming must be performed in two steps, as too much heat would be created if it was performed in a single step (Fig. 3). Step 4: Freshening of articular surfaces Fig.4 This surgical step is best performed under distraction and is very important as it will determine the success of the fusion. Depending on the patient s case and surgical indication, articular debridement can be performed either through the tunnel or more commonly and more easily, by a small sinus tarsi incision on the lateral aspect of the calcaneus below the tip of the lateral malleolus. Reflect the lateral peroneal tendons, and then under power use a burr and/or the Φ10 mm hollow reamer (Ref ) with K-wire (Ref ) to carefully remove the subtalar joint cartilage (Fig. 4). Step 5: Bone graft Depending on the surgical indication, a bone graft may be necessary. It isn t always necessary for comminuted fractures. The bone plug removed at the beginning of the surgery may be sufficient. Care must be taken to insert the nail before the distractor is released. The distractor should always be released before inserting the screws. For secondary arthrodesis after malunion or an orthopaedic indication, bone grafts are common practice. Compression may be useful after placing the bone graft. The distractor must be withdrawn and the compressor (Ref ) assembled on to the same talar and tuberosity K-wires (Fig. 5). Fig.5 Surgical technique
13 13 Step 6: Nail placement The length of nail required is determined after placing the nail guide (Ref ) and the nail length gauge (Ref ). The nail length gauge must be pushed in until it is against the cortex (Fig. 6a). The nail is available in three lengths: 65, 75, and 85 mm (see reference table 3 ). Place the selected nail on to the nail holder with the ball end of the T-handle on the same side as the D-shaped holes on the medial side of the nail. Use the handle-nail connector screw Φ12 mm to secure the nail holder to the nail. Handle-nail connector screw Φ12 mm: Ref Nail holder Φ12 mm Ref At this stage, it is important to slide the spongy bone plug(s) that was/were removed with the hollow reamer inside the nail and to position it/them against the nail slots. This will help the arthrodesis to fuse together. The nail is then introduced into the work chamber with small rotating motions, then pushed up until it reaches the talar body. Its proximal tip must be at least 10 mm from the anterior cortex of the talus. To ensure the proximal end of the nail is fully engaged in the bone, loosen the handle nail connector (Ref ) one full turn and pull back on the T-handle to create separation with the nail. Now the proximal end of the nail is visible on fluoroscopy. Fig.6a Fig.6b Once the nail is in place, put the Φ12 arthrodesis nail alignment frame (Ref ) onto the lateral arm of the nail holder (Ref ), and secure the assembly using the alignment frame-nail holder connecting screw (Ref ). If the talar screw conflicts with fibula, then rotate the nail so that the screw holes are oblique in lateral view and the trajectory of the screw is a bit anterior to posterior. After placement of the drill guide for K-wires (Ref ) in the holes of the nail alignment frame corresponding to the nail length selected, K-wires Φ1.6 X 200 mm (Ref ) are introduced under power until the bicortical. Remove the drill guide and use the cannulated screw length gauge (Ref ) to measure the required screw length. Typically, 30 mm or 32 mm screws are used (see reference table 4 ) The K-wires can be further inserted to puncture through the medial skin so they can be retained with hemostats. Use the Φ3.7 mm cannulated drill bit (Ref ) over the Φ1.6 mm K-wires. A screw is placed in the talar body and one or two screws in the calcaneus using the cannulated screwdriver (Ref ) (Fig. 6b and 6c). Fig.6c Depending on the distance between the end of the nail and posterior tuberosity cortex, a cap can be placed on the nail to make it easier to remove later on. For secondary fusion indications (malunion with posterior tuberosity varus), a corticocancellous bone graft can be used. Once the graft is positioned between the talus and calcaneus (Fig. 7), the nail can be placed through the graft (Fig. 7). Fig.7
14 14 >>>>> Final appearance 3 Reference Arthrodesis Nail Φ12 mm CALCAnail Nail Φ12 x 65 mm + Cap CALCAnail Nail Φ12 x 75 mm + Cap CALCAnail Nail Φ12 x 85 mm + Cap Post-operative care The patient may begin ambulating immediately following surgery using crutches and non-weight bearing. A pain relieving brace is recommended and good wound healing must be observed. Treatment continues for the first 15 days. Afterwards and after verifying that the wound is healing, a new cast is applied for one month. Physical therapy is usually not needed. After the sixth week, depending on the indication of the surgery, walking with progressive weight bearing using crutches may resume; a walking cast may also be used for added support. Physical therapy is usually not needed. Implant Removal Removal of the implant after a calcaneal fracture or subtalar arthrodesis is rarely indicated. If it proves to be necessary, removal of the screws can be done easily by locating the screw heads on the lateral side of the calcaneus and reinserting the Φ1.6 mm K-wires. The screwdriver guided by the K-wires will enable the screws to be extracted without difficulty. After making an incision over the posterior calcaneal tuberosity, the cap can be removed (if one was placed). The nail holder is repositioned after first cleaning the female screw threads. If the rotating motions of the nail holder are ineffective as a result of bone regrowth around the nail the larger-sized hollow reamer should be used round the nail: the Φ12 mm hollow reamer for the Φ10 mm fracture nail and the Φ14 mm hollow reamer for the Φ12 mm arthrodesis nail. 4 Reference Screw Cannulated screw Φ5 x 24 mm Cannulated screw Φ5 x 26 mm Cannulated screw Φ5 x 28 mm Cannulated screw Φ5 x 30 mm Cannulated screw Φ5 x 32 mm Cannulated screw Φ5 x 34 mm Cannulated screw Φ5 x 36 mm Cannulated screw Φ5 x 38 mm Cannulated screw Φ5 x 40 mm Removal will then be straight forward after reassembling the nail holder. Surgical technique
15 INSTRUMENTATION SET Compressor... Ref Distractor... Ref CALCAnail Positioning square... Ref Hollow reamer Φ14 mm for arthrodesis nail removal... Ref CALCAnail Hollow reamer Φ12 mm... Ref CALCAnail Hollow reamer Φ10 mm... Ref CALCAnail K-wire with stopper Φ12 mm (x2)... Ref CALCAnail K-wire with stopper Φ10 mm (x2)... Ref K-wire for cannulated screws Φ1.6 x 200 mm (x4)... Ref Drill bit Φ3.7 for cannulated screws... Ref K-wire for distractor Φ3.2 x 150 mm (x4)... Ref Nail length gauge... Ref Cannulated screw length gauge... Ref CALCAnail Nail guide... Ref Spatula... Ref Cannulated Φ3.5 mm hex screwdriver... Ref Straight tamp... Ref Curved tamp... Ref Alignment frame-nail holder connecting screw (x2)... Ref Bone tunnel plug Φ12 mm... Ref Bone tunnel plug Φ10 mm... Ref Drill guide for K-wire Φ1.6 x 200 mm (x2)... Ref Alignment frame for Fracture nail Φ10 mm... Ref CALCAnail Handle-nail connector Φ10 mm... Ref Alignment frame for Arthrodesis nail Φ12 mm... Ref CALCAnail Handle-nail connector Φ12 mm... Ref CALCAnail Nail holder Φ10 mm... Ref CALCAnail Nail holder Φ12 mm... Ref
16 FHO com - Illustrations Marc Donon - to_calcanail_us_1.2 Surgical technique FHINC
The Vilex FUZETM. Dual Thread Screw & Intramedullary Nail in One Implant. The Ultimate TTC Arthrodesis Internal Fixator
 The Vilex FUZETM Dual Thread Screw & Intramedullary Nail in One Implant The Ultimate TTC Arthrodesis Internal Fixator Introduction The Vilex FUZE TM TTC Arthrodesis Compression Nail combines the attributes
The Vilex FUZETM Dual Thread Screw & Intramedullary Nail in One Implant The Ultimate TTC Arthrodesis Internal Fixator Introduction The Vilex FUZE TM TTC Arthrodesis Compression Nail combines the attributes
wave Calcaneal Fracture Plate
 wave Calcaneal Fracture Plate s u r g i c a l t e c h n i q u e Tornier WAVE Calcaneal fracture plate system surgical procedure Indications for Use: The Tornier Calcaneal Fracture Plate System is indicated
wave Calcaneal Fracture Plate s u r g i c a l t e c h n i q u e Tornier WAVE Calcaneal fracture plate system surgical procedure Indications for Use: The Tornier Calcaneal Fracture Plate System is indicated
Arthrodesis of the Ankle
 TM Arthrodesis of the Ankle Plantar View of the Foot 1. Make a lateral incision to expose the tibia-talus joint and the talo-calcaneal joint. Prepare the arthrodesis sites surgically with a rasp or an
TM Arthrodesis of the Ankle Plantar View of the Foot 1. Make a lateral incision to expose the tibia-talus joint and the talo-calcaneal joint. Prepare the arthrodesis sites surgically with a rasp or an
3. PATIENT POSITIONING & FRACTURE REDUCTION 3 8. DISTAL GUIDED LOCKING FOR PROXIMAL NAIL PROXIMAL LOCKING FOR LONG NAIL 13
 Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL NAIL INSERTION 6-7 7. PROXIMAL LOCKING
Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL NAIL INSERTION 6-7 7. PROXIMAL LOCKING
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
System. Humeral Nail. Surgical Technique
 System Humeral Nail Surgical Technique Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL
System Humeral Nail Surgical Technique Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL
Radiographic Evaluation of Calcaneal Fractures. Kali Luker, PGY-1
 Radiographic Evaluation of Calcaneal Fractures Kali Luker, PGY-1 Anatomy Extraarticular Fractures Involve body, anterior process or tuberosity Treated with immobilization and NWB x 6 wks UNLESS Displaced
Radiographic Evaluation of Calcaneal Fractures Kali Luker, PGY-1 Anatomy Extraarticular Fractures Involve body, anterior process or tuberosity Treated with immobilization and NWB x 6 wks UNLESS Displaced
NeoGen Tibia Nail System
 NeoGen Tibia Nail System LESS IS MORE TE-2070-03 Surgical Technique BLE OF CONTENT Preface Surgical Technique Appendix Products Information Patient Preparation Entry Portal Fracture Reduction Canal Preparation
NeoGen Tibia Nail System LESS IS MORE TE-2070-03 Surgical Technique BLE OF CONTENT Preface Surgical Technique Appendix Products Information Patient Preparation Entry Portal Fracture Reduction Canal Preparation
Surgical Technique. Calcaneal Locking Plate
 Surgical Technique Calcaneal Locking Plate PERI-LOC Locked Plating System Calcaneal Locking Plate Surgical TechniqueCatalog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Surgical Technique Calcaneal Locking Plate PERI-LOC Locked Plating System Calcaneal Locking Plate Surgical TechniqueCatalog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
TRIGEN Hindfoot Fusion Nail Surgical Technique
 Surgical Technique TRIGEN Hindfoot Fusion Nail Surgical Technique As described by: Thomas A. Russell, MD Roy W. Sanders, MD John S. Early, MD Contents Design Rationale...3 Indications...3 Design Features...4
Surgical Technique TRIGEN Hindfoot Fusion Nail Surgical Technique As described by: Thomas A. Russell, MD Roy W. Sanders, MD John S. Early, MD Contents Design Rationale...3 Indications...3 Design Features...4
Open reduction; plate fixation 1 Principles
 Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Lateral TTC Plate SURGICAL TECHNIQUE
 MAXLOCK EXTREME Lateral TTC Plate SURGICAL TECHNIQUE Contents Overview 2 Exposure 3 Surgical Technique 4 Implants and Instruments 10 11 Proper surgical procedures and techniques are the responsibility
MAXLOCK EXTREME Lateral TTC Plate SURGICAL TECHNIQUE Contents Overview 2 Exposure 3 Surgical Technique 4 Implants and Instruments 10 11 Proper surgical procedures and techniques are the responsibility
TRK REVISION KNEE Surgical Technique
 1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]
![FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test] FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]](/thumbs/83/88335212.jpg) FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
Surgical Technique. Targeter Systems Overview
 Surgical Technique Targeter Systems Overview PERI-LOC Locked Plating System Targeter Systems Overview Table of contents Product overview... 2 Introduction... 2 Indications... 2 Design features and benefits...
Surgical Technique Targeter Systems Overview PERI-LOC Locked Plating System Targeter Systems Overview Table of contents Product overview... 2 Introduction... 2 Indications... 2 Design features and benefits...
S U R G I C A L T E C H N I Q U E David A. McQueen, MD Return to Menu
 S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Surgical Technique Guide
 Guide CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Align Anterior Ankle Fusion Plate is intended to facilitate arthrodesis of the
Guide CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Align Anterior Ankle Fusion Plate is intended to facilitate arthrodesis of the
3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM
 3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM Part of the DePuy Synthes Variable Angle Periarticular Plating System SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION 3.5 mm VA-LCP Proximal Tibial Plate 2 AO
3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM Part of the DePuy Synthes Variable Angle Periarticular Plating System SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION 3.5 mm VA-LCP Proximal Tibial Plate 2 AO
Supplemental Use Guide Standard Triple Arthrodesis
 Acutrak 2 Headless Compression Screw System 4.7 mm and 7.5 mm Screws Supplemental Use Guide Standard Triple Arthrodesis Acumed is a global leader of innovative orthopaedic and medical solutions. We are
Acutrak 2 Headless Compression Screw System 4.7 mm and 7.5 mm Screws Supplemental Use Guide Standard Triple Arthrodesis Acumed is a global leader of innovative orthopaedic and medical solutions. We are
CHARLOTTE. 7.0 Multi-Use Compression Screw System SURGICAL TECHNIQUE
 CHARLOTTE 7.0 Multi-Use Compression Screw System SURGICAL TECHNIQUE Contents Chapter 1 1 Chapter 2 2 Chapter 3 3-9 Chapter 4 10-12 Appendix A 13-14 Design Rationale Screw Behavior Surgical Technique Procedure
CHARLOTTE 7.0 Multi-Use Compression Screw System SURGICAL TECHNIQUE Contents Chapter 1 1 Chapter 2 2 Chapter 3 3-9 Chapter 4 10-12 Appendix A 13-14 Design Rationale Screw Behavior Surgical Technique Procedure
NeoGen Femoral Nail System
 NeoGen Femoral Nail System LESS IS MORE TE-2070-04 Surgical Technique BLE OF CONTENT Preface Standard Femoral Mode Recon Mode Post-Operative Management Appendix Products Information Indication Patient
NeoGen Femoral Nail System LESS IS MORE TE-2070-04 Surgical Technique BLE OF CONTENT Preface Standard Femoral Mode Recon Mode Post-Operative Management Appendix Products Information Indication Patient
Introduction Basics MIS Screw 2 System Characteristics 2 Indication 2
 Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Wichita Fusion Nail Surgical Technique. David A. McQueen, MD
 Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
Technique Guide. 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System.
 Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal
Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal
ORTHOLOC Calcaneal Fracture System SURGICAL TECHNIQUE
 ORTHOLOC Calcaneal Fracture System SURGICAL TECHNIQUE ORTHOLOC Calcaneal Fracture System SURGICAL TECHNIQUE Contents Chapter 1 4 Chapter 2 5 Chapter 3 6 7 8 9 Appendix 1 10-12 ORTHOLOC Calcaneal Fracture
ORTHOLOC Calcaneal Fracture System SURGICAL TECHNIQUE ORTHOLOC Calcaneal Fracture System SURGICAL TECHNIQUE Contents Chapter 1 4 Chapter 2 5 Chapter 3 6 7 8 9 Appendix 1 10-12 ORTHOLOC Calcaneal Fracture
Zimmer MIS Periarticular Distal Femoral Locking Plate
 For Clinical Evaluations Zimmer MIS Periarticular Distal Femoral Locking Plate Surgical Technique The Science of the Landscape Zimmer MIS Periarticular Distal Femoral Locking Plate Surgical Technique
For Clinical Evaluations Zimmer MIS Periarticular Distal Femoral Locking Plate Surgical Technique The Science of the Landscape Zimmer MIS Periarticular Distal Femoral Locking Plate Surgical Technique
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate
 Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique 1 Zimmer MIS
Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique 1 Zimmer MIS
M.I.S. MAKE IT SMART IN ONE SYSTEM. Surgical Technique. Hip Knee Spine Navigation
 M.I.S. MAKE IT SMART IN ONE SYSTEM Surgical Technique Hip Knee Spine Navigation M.U.S.T. Mini Open Surgical Technique Hip Knee Spine Navigation 2 C O N T E N T S 1 INTRODUCTION 4 2 SURGICAL TECHNIQUE 5
M.I.S. MAKE IT SMART IN ONE SYSTEM Surgical Technique Hip Knee Spine Navigation M.U.S.T. Mini Open Surgical Technique Hip Knee Spine Navigation 2 C O N T E N T S 1 INTRODUCTION 4 2 SURGICAL TECHNIQUE 5
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer
 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
EVOS MINI with IM Nailing
 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
The NBX Non-Bridging External Fixator A Non-Bridging External Fixator/Locking Plate capturing a series of.062mm K-wires and 3mm half-pins that are
 The NBX Non-Bridging External Fixator A Non-Bridging External Fixator/Locking Plate capturing a series of.062mm K-wires and 3mm half-pins that are inserted in a multiplanar and multi-directional fashion
The NBX Non-Bridging External Fixator A Non-Bridging External Fixator/Locking Plate capturing a series of.062mm K-wires and 3mm half-pins that are inserted in a multiplanar and multi-directional fashion
Aesculap Targon TX. Intramedullary Nail for Tibial Fractures...going to X-tremes. Aesculap Orthopaedics
 Aesculap Targon TX Intramedullary Nail for Tibial Fractures...going to X-tremes Aesculap Orthopaedics Surgical Technique Preoperative Planning KH483 X-ray template Targon TX (KH483200 : 375 mm-420 mm KH48320
Aesculap Targon TX Intramedullary Nail for Tibial Fractures...going to X-tremes Aesculap Orthopaedics Surgical Technique Preoperative Planning KH483 X-ray template Targon TX (KH483200 : 375 mm-420 mm KH48320
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
CHARLOTTE. 7.0 Multi-Use Compression Screw System SURGICAL TECHNIQUE
 CHARLOTTE 7.0 Multi-Use Compression Screw System SURGICAL TECHNIQUE Contents Chapter 1 1 Chapter 2 2 2 3 4 Appendix A 5 6 Appendix B 7 8 Preoperative Planning Surgical Technique Subtalar Arthrodesis Guide
CHARLOTTE 7.0 Multi-Use Compression Screw System SURGICAL TECHNIQUE Contents Chapter 1 1 Chapter 2 2 2 3 4 Appendix A 5 6 Appendix B 7 8 Preoperative Planning Surgical Technique Subtalar Arthrodesis Guide
PROXIMAL TIBIAL PLATE
 SURGICAL NÁSTROJE TECHNIQUE PRO ARTROSKOPII PROXIMAL INSTRUMENTS TIBIAL FOR PLATE ARTHROSCOPY Proximal Tibial Plate Description of medical device The Proximal Tibial Plate is used in epyphyseal and metaphyseal
SURGICAL NÁSTROJE TECHNIQUE PRO ARTROSKOPII PROXIMAL INSTRUMENTS TIBIAL FOR PLATE ARTHROSCOPY Proximal Tibial Plate Description of medical device The Proximal Tibial Plate is used in epyphyseal and metaphyseal
Foot Injuries. Dr R B Kalia
 Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
TIBIAXYS ANKLE FUSION
 TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
Zimmer NexGen MIS Tibial Component. Cemented Surgical Technique IMAGE TO COME
 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
PediNail Pediatric Femoral Nail
 PediNail Pediatric Femoral Nail Surgical Technique Table of Contents Indications...3 Patient Positioning...3 Approach...4 Reaming...5 Nail Placement...6 Proximal Interlocking...7 Distal Interlocking...8
PediNail Pediatric Femoral Nail Surgical Technique Table of Contents Indications...3 Patient Positioning...3 Approach...4 Reaming...5 Nail Placement...6 Proximal Interlocking...7 Distal Interlocking...8
Foot & Ankle T2. Ankle Arthrodesis Nail. Foot & Ankle
 Foot & Ankle T2 Ankle Arthrodesis Nail Operative Technique Foot & Ankle 1 Ankle Arthrodesis Nailing System This publication sets forth detailed recommended procedures for using Stryker devices and instruments.
Foot & Ankle T2 Ankle Arthrodesis Nail Operative Technique Foot & Ankle 1 Ankle Arthrodesis Nailing System This publication sets forth detailed recommended procedures for using Stryker devices and instruments.
Midfoot - Reduction & Fixation - ORIF - screw fixation - AO Surgery Reference. ORIF - screw fixation
 Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Periarticular Aiming Arm Instruments for LCP Proximal Tibial Plate 4.5/5.0. Part of the LCP Periarticular Aiming Arm Instrument System (large).
 Technique Guide Periarticular Aiming Arm Instruments for LCP Proximal Tibial Plate 4.5/5.0. Part of the LCP Periarticular Aiming Arm Instrument System (large). Image intensifier control Warning This description
Technique Guide Periarticular Aiming Arm Instruments for LCP Proximal Tibial Plate 4.5/5.0. Part of the LCP Periarticular Aiming Arm Instrument System (large). Image intensifier control Warning This description
VA LOCKING CALCANEAL PLATES 2.7
 VA LOCKING CALCANEAL PLATES 2.7 Instruments and Implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control Warning
VA LOCKING CALCANEAL PLATES 2.7 Instruments and Implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control Warning
GREENS SURGICALS. Redefining Excellence INSTRUMENT SYSTEM PREPARED BY: DR. VINAY KUMAR
 GREENS SURGICALS Redefining Excellence TIBIA AND FEMUR INSTRUMENT SYSTEM PREPARED BY: DR. VINAY KUMAR OPERATIVE TECHNIQUES INDEX SR.NO CONTENTS 1 LIST OF INSTRUMENT FOR TIBIA AND FEMUR. 2 RADIO GRAPH OF
GREENS SURGICALS Redefining Excellence TIBIA AND FEMUR INSTRUMENT SYSTEM PREPARED BY: DR. VINAY KUMAR OPERATIVE TECHNIQUES INDEX SR.NO CONTENTS 1 LIST OF INSTRUMENT FOR TIBIA AND FEMUR. 2 RADIO GRAPH OF
STS. Subtalar Spacer System SURGICAL TECHNIQUE
 STS Subtalar Spacer System SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction 4 Device Description Chapter 2 5 Intended Use 5 Indications Chapter 3 6 Surgical Technique 9 Postoperative Protocol 9 Explant
STS Subtalar Spacer System SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction 4 Device Description Chapter 2 5 Intended Use 5 Indications Chapter 3 6 Surgical Technique 9 Postoperative Protocol 9 Explant
Calcaneal Fractures: Lateral Extensile Incision
 Calcaneal Fractures: Lateral Extensile Incision AS Flemister JR, MD University of Rochester Disclosures I have no financial disclosures 1/27/2016 2 Mechanism Axial Loading Fall From Height MVA BAD SOFT
Calcaneal Fractures: Lateral Extensile Incision AS Flemister JR, MD University of Rochester Disclosures I have no financial disclosures 1/27/2016 2 Mechanism Axial Loading Fall From Height MVA BAD SOFT
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System.
 LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
Humerus Block. Discontinued December 2016 DSEM/TRM/0115/0296(1) Surgical Technique. This publication is not intended for distribution in the USA.
 Humerus Block Surgical Technique Discontinued December 2016 DSEM/TRM/0115/0296(1) This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Contents
Humerus Block Surgical Technique Discontinued December 2016 DSEM/TRM/0115/0296(1) This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Contents
Surgical Technique Carpal Fusion
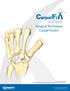 Carpal Fusion Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Extremity Medical Lag Screw and X-Post System
Carpal Fusion Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Extremity Medical Lag Screw and X-Post System
Surgical Technique. Intramedullary locked Nailing With Screws for Humerus Fractures Solid/Cannulated. Humeral Interlocking Nail.
 Screws for Humerus Fractures Surgical Technique Humeral Interlocking Nail Approved by Humerus Nail Kit Code 08050001 Contents Introduction Implant design Indications Pre-operative planning Patient positioning
Screws for Humerus Fractures Surgical Technique Humeral Interlocking Nail Approved by Humerus Nail Kit Code 08050001 Contents Introduction Implant design Indications Pre-operative planning Patient positioning
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Talus Fractures: When and Why on Screws and Plates
 Talus Fractures: When and Why on Screws and Plates Frank A. Liporace, MD Associate Professor Director of Orthopaedic Research New York University / Hospital for Joint Diseases, NY, NY Director Orthopaedic
Talus Fractures: When and Why on Screws and Plates Frank A. Liporace, MD Associate Professor Director of Orthopaedic Research New York University / Hospital for Joint Diseases, NY, NY Director Orthopaedic
ORTHOLOC Calcaneal Fracture System SURGIC AL TECHNIQUE
 ORTHOLOC Calcaneal Fracture System SURGIC AL TECHNIQUE Contents Chapter 1 4 Chapter 2 5 Chapter 3 6 7 8 9 Appendix 1 10-12 ORTHOLOC Calcaneal Fracture System - Introduction - ORTHOLOC Polyaxial Locking
ORTHOLOC Calcaneal Fracture System SURGIC AL TECHNIQUE Contents Chapter 1 4 Chapter 2 5 Chapter 3 6 7 8 9 Appendix 1 10-12 ORTHOLOC Calcaneal Fracture System - Introduction - ORTHOLOC Polyaxial Locking
LUMBAR POSTERIOR MINIMALLY INVASIVE SYSTEM. Surgical Technique
 LUMBAR POSTERIOR MINIMALLY INVASIVE SYSTEM Surgical Technique Joint Spine Sports Med M.U.S.T. Mini Open Surgical Technique Joint Spine Sports Med CAUTION Federal law (USA) restricts this device to sale
LUMBAR POSTERIOR MINIMALLY INVASIVE SYSTEM Surgical Technique Joint Spine Sports Med M.U.S.T. Mini Open Surgical Technique Joint Spine Sports Med CAUTION Federal law (USA) restricts this device to sale
Extramedullary Tibial Preparation
 Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique. CONQUEST FN Femoral Neck Fracture System
 Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique 4.5/8.5MM BEAMING SYSTEM. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The 4.5/8.5 screw system is intended for fixation arthrodesis of
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The 4.5/8.5 screw system is intended for fixation arthrodesis of
L8 Spine System SURGICAL TECHNIQUE. Add: No.1-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China
 Add: No.-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China 23022 Tel: 0086 59 8595556 Fax: 0086 59 859555 Http://www.kanghui.com Add: F25, Shanghai International Pharmaceutical Trad & Exhibition
Add: No.-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China 23022 Tel: 0086 59 8595556 Fax: 0086 59 859555 Http://www.kanghui.com Add: F25, Shanghai International Pharmaceutical Trad & Exhibition
POLYAXIAL SPINE SYSTEM D E G E N E R A T I V E
 S U R G I C A L T E C H N I Q U E En POLYAXIAL SPINE SYSTEM D E G E N E R A T I V E LOW PROFILE POLYAXIAL SPINE SYSTEM A01110050 Straight spatula A01110060 Curved spatula A01110070 Bone probe A01114500
S U R G I C A L T E C H N I Q U E En POLYAXIAL SPINE SYSTEM D E G E N E R A T I V E LOW PROFILE POLYAXIAL SPINE SYSTEM A01110050 Straight spatula A01110060 Curved spatula A01110070 Bone probe A01114500
The Locking Calcaneal Plate Instrument and Implant Sets
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System The Locking Calcaneal Plate Instrument and Implant Sets Surgical Technique Table of Contents Introduction Locking Calcaneal Plate 2 AO
Part of the DePuy Synthes Locking Compression Plate (LCP ) System The Locking Calcaneal Plate Instrument and Implant Sets Surgical Technique Table of Contents Introduction Locking Calcaneal Plate 2 AO
GLENOID SURGICAL TECHNIQUE
 UP. EXTREMITY Dual-Platform Shoulder Prosthesis GLENOID SURGICAL TECHNIQUE ANATOMICAL REVERSE SURGICAL TECHNIQUE REFERENCE NUMBERS HUMERAL STEM REFERENCE DIAMETER HEIGHT 267 360 Ø 06 100 265 102 Ø 08 120
UP. EXTREMITY Dual-Platform Shoulder Prosthesis GLENOID SURGICAL TECHNIQUE ANATOMICAL REVERSE SURGICAL TECHNIQUE REFERENCE NUMBERS HUMERAL STEM REFERENCE DIAMETER HEIGHT 267 360 Ø 06 100 265 102 Ø 08 120
Locking Ankle Plating System. Surgical Technique
 Locking Ankle Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Locking Ankle Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Workshop Outline. Pre-operative planning
 Workshop Objective To build and apply the True/Lok TM circular external fixator frame for correction of the Charcot forefoot deformity (Lisfranc fracture dislocation) Workshop Outline Pre-operative planning
Workshop Objective To build and apply the True/Lok TM circular external fixator frame for correction of the Charcot forefoot deformity (Lisfranc fracture dislocation) Workshop Outline Pre-operative planning
Zenith. Total Ankle Replacement Surgical technique
 Total Ankle Replacement Surgical technique Contents Operative summary 4 Pre-operative planning and templating 6 Patient positioning 6 Exposure 6 Saw blades 7 Joint line definition 7 Tibial alignment jig
Total Ankle Replacement Surgical technique Contents Operative summary 4 Pre-operative planning and templating 6 Patient positioning 6 Exposure 6 Saw blades 7 Joint line definition 7 Tibial alignment jig
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Fractures of the Calcaneus
 Fractures of the Calcaneus Anthony T. Sorkin, M.D. Rockford Orthopedic Trauma Service Rajeev Garapati, MD Illinois Bone and Joint Institute Assistant Clinical Professor University of Illinois at Chicago
Fractures of the Calcaneus Anthony T. Sorkin, M.D. Rockford Orthopedic Trauma Service Rajeev Garapati, MD Illinois Bone and Joint Institute Assistant Clinical Professor University of Illinois at Chicago
FlexitSystem EFFICIENT MOBILITY. High Tibial Opening Wedge Osteotomy (HTO)
 FlexitSystem EFFICIENT MOBILITY HTO OPENING Surgical Technique FlexitSystem High Tibial Opening Wedge Osteotomy (HTO) FlexitSystem SURGICAL TECHNIQUE NEW ANATOMIC DESIGN LOW PROFILE 2.8 mm RESISTANT AND
FlexitSystem EFFICIENT MOBILITY HTO OPENING Surgical Technique FlexitSystem High Tibial Opening Wedge Osteotomy (HTO) FlexitSystem SURGICAL TECHNIQUE NEW ANATOMIC DESIGN LOW PROFILE 2.8 mm RESISTANT AND
Technique Guide. 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm LCP Distal Fibula Plates 2 AO Principles
Technique Guide 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm LCP Distal Fibula Plates 2 AO Principles
3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments
 Part of the 3.5 mm LCP 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments Surgical Technique TABLE OF CONTENTS INTRODUCTION 3.5 mm LCP Low Bend Medial Distal Tibia Plate 2 Aiming Instruments
Part of the 3.5 mm LCP 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments Surgical Technique TABLE OF CONTENTS INTRODUCTION 3.5 mm LCP Low Bend Medial Distal Tibia Plate 2 Aiming Instruments
Surgical Technique.
 Surgical Technique www.biomet.co.uk INTRODUCTION design principals Recent advances in imaging technology have enabled orthopaedic surgeons to extend closed treatment of femoral fractures to include more
Surgical Technique www.biomet.co.uk INTRODUCTION design principals Recent advances in imaging technology have enabled orthopaedic surgeons to extend closed treatment of femoral fractures to include more
The Flower Medial Column Fusion Plate
 The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Surgical Technique International Version
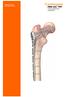 Surgical Technique International Version PERI-LOC PFP 4.5mm Proximal Femur Locking Plate Surgical Technique Table of contents Product overview...2 Introduction...2 Indications...3 Case examples...4 Design
Surgical Technique International Version PERI-LOC PFP 4.5mm Proximal Femur Locking Plate Surgical Technique Table of contents Product overview...2 Introduction...2 Indications...3 Case examples...4 Design
Zimmer Natural Nail System
 Zimmer Natural Nail System Antegrade Femoral Nail Surgical Technique (Piriformis Fossa & Greater Trochanteric Approaches) Zimmer Natural Nail System Antegrade Femoral Surgical Technique 1 Zimmer Natural
Zimmer Natural Nail System Antegrade Femoral Nail Surgical Technique (Piriformis Fossa & Greater Trochanteric Approaches) Zimmer Natural Nail System Antegrade Femoral Surgical Technique 1 Zimmer Natural
STRENGTH FROM WITHIN. Surgical Technique for Representatives
 STRENGTH FROM WITHIN Surgical Technique for Representatives Table of Contents PREOPERATIVE TEMPLATING... p.3 OUTRIGGER DRILL GUIDE OVERVIEW... p.4 PATIENT POSITIONING...p.5 STEP 1: REDUCE THE FRACTURE...p.5-6
STRENGTH FROM WITHIN Surgical Technique for Representatives Table of Contents PREOPERATIVE TEMPLATING... p.3 OUTRIGGER DRILL GUIDE OVERVIEW... p.4 PATIENT POSITIONING...p.5 STEP 1: REDUCE THE FRACTURE...p.5-6
Conventus CAGE PH Surgical Techniques
 Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Femur. Monoaxial Locking Plate System. Operative Technique. Distal Lateral Femur Universal Holes Targeting Instrumentation.
 Femur AxSOS 3 Titanium Monoaxial Locking Plate System Femur Fractures Operative Technique Distal Lateral Femur Universal Holes Targeting Instrumentation This publication sets forth detailed recommended
Femur AxSOS 3 Titanium Monoaxial Locking Plate System Femur Fractures Operative Technique Distal Lateral Femur Universal Holes Targeting Instrumentation This publication sets forth detailed recommended
Surgical Technique. Olecranon Locking Plate
 Surgical Technique Olecranon Locking Plate PERI-LOC Locked Plating System Olecranon Locking Plate Surgical Techniquealog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Surgical Technique Olecranon Locking Plate PERI-LOC Locked Plating System Olecranon Locking Plate Surgical Techniquealog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Surgical Technique Guide
 Surgical Technique Guide Minimally Invasive, Intramedullary Device For Distal Radius Fragility Fractures The Sonoma WRx Wrist Fracture Repair Device is flexible, inserting easily through a small incision
Surgical Technique Guide Minimally Invasive, Intramedullary Device For Distal Radius Fragility Fractures The Sonoma WRx Wrist Fracture Repair Device is flexible, inserting easily through a small incision
Pre-Operative Planning. Positioning of the Patient
 Surgical Technique Pre-Operative Planning Decide upon the size and angle of the barrel plate to be used from measuring the x-rays. To maximise the sliding action when using shorter lag screws, the Short
Surgical Technique Pre-Operative Planning Decide upon the size and angle of the barrel plate to be used from measuring the x-rays. To maximise the sliding action when using shorter lag screws, the Short
WINSTA-C. Clavicle Plating System
 Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
The Titanium Tibial Nail System
 The Titanium Tibial Nail System Solid Tibial Nails (UTN) and Cannulated Tibial Nails (CTN) Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
The Titanium Tibial Nail System Solid Tibial Nails (UTN) and Cannulated Tibial Nails (CTN) Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
Double Engine Orthopedic Bone Nail System Universal Humeral Nail
 Double Engine Orthopedic Bone Nail System ----------- Universal Humeral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic
Double Engine Orthopedic Bone Nail System ----------- Universal Humeral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic
DARCO. CPS Plate SURGICAL TECHNIQUE
 DARCO CPS Plate SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 5 Chapter 3 6 Appendix 9 Introduction - CPS Features Preoperative Planning Surgical Technique - Surgical Approach and Retraction
DARCO CPS Plate SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 5 Chapter 3 6 Appendix 9 Introduction - CPS Features Preoperative Planning Surgical Technique - Surgical Approach and Retraction
MetaFix Ludloff Plate
 Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
TIBIAL NAILING SYSTEM OPTIONS MADE EASY
 S U R G I C A L T E C H N I Q U E TIBIAL NAILING SYSTEM OPTIONS MADE EASY TABLE OF CONTENTS DESIGN SUMMARY INSTRUMENT OVERVIEW AND JIG OPTIONS 1 2 ENTRY AND CANAL PREP NAIL INSERTION LOCKING NAIL REMOVAL
S U R G I C A L T E C H N I Q U E TIBIAL NAILING SYSTEM OPTIONS MADE EASY TABLE OF CONTENTS DESIGN SUMMARY INSTRUMENT OVERVIEW AND JIG OPTIONS 1 2 ENTRY AND CANAL PREP NAIL INSERTION LOCKING NAIL REMOVAL
Zimmer Periarticular Proximal Humeral Locking Plate
 Zimmer Periarticular Proximal Humeral Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Humeral Locking Plate 1 Surgical Technique Table of Contents Introduction
Zimmer Periarticular Proximal Humeral Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Humeral Locking Plate 1 Surgical Technique Table of Contents Introduction
QUICK REFERENCE GUIDE. Arthrodiatasis. Articulated Joint Distraction
 4 Arthrodiatasis Articulated Joint Distraction ARTHRODIATASIS OF THE HIP To prepare the assembly, remove the female component and replace it with the ProCallus articulated body for the hip. Remove cam
4 Arthrodiatasis Articulated Joint Distraction ARTHRODIATASIS OF THE HIP To prepare the assembly, remove the female component and replace it with the ProCallus articulated body for the hip. Remove cam
NCB Distal Femur System. Surgical Technique
 NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
Surgical Technique. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Pediatric Tibia Fractures Key Points. Christopher Iobst, MD
 Pediatric Tibia Fractures Key Points Christopher Iobst, MD Goals Bone to heal Return to full weight bearing Acceptable alignment rule of 10s 10 degrees of varus 8 degrees of valgus 12 degrees of procurvatum
Pediatric Tibia Fractures Key Points Christopher Iobst, MD Goals Bone to heal Return to full weight bearing Acceptable alignment rule of 10s 10 degrees of varus 8 degrees of valgus 12 degrees of procurvatum
Olecranon Osteotomy Nail. For simple fractures and osteotomies of the olecranon.
 Olecranon Osteotomy Nail. For simple fractures and osteotomies of the olecranon. Technique Guide Discontinued June 2016; AVAILABLE FOR IMPLANT REMOVAL PURPOSES ONLY DSEM/TRM/0517/0843 Table of Contents
Olecranon Osteotomy Nail. For simple fractures and osteotomies of the olecranon. Technique Guide Discontinued June 2016; AVAILABLE FOR IMPLANT REMOVAL PURPOSES ONLY DSEM/TRM/0517/0843 Table of Contents
SURGICAL TECHNIQUE ROI-T TM TLIF INTERSOMATIC IMPLANT TRANS-FORAMINAL APPROACH
 TLIF INTERSOMATIC IMPLANT TRANS-FORAMINAL APPROACH Table of Contents page Step 1 - Articular resection.................................................................................. 3 Step 2 - Pedicle
TLIF INTERSOMATIC IMPLANT TRANS-FORAMINAL APPROACH Table of Contents page Step 1 - Articular resection.................................................................................. 3 Step 2 - Pedicle
operative technique Universal Application
 operative technique Universal Application Introduction Introduction Building upon the design rationale of the Xia Spinal System, the new Xia Spinal System represents the latest advancement in spinal implant
operative technique Universal Application Introduction Introduction Building upon the design rationale of the Xia Spinal System, the new Xia Spinal System represents the latest advancement in spinal implant
