Greater Trochanteric Pain Syndrome
|
|
|
- Warren Horn
- 6 years ago
- Views:
Transcription
1 ORIGINAL RESEARCH Greater Trochanteric Pain Syndrome Percutaneous Tendon Fenestration Versus Platelet-Rich Plasma Injection for Treatment of Gluteal Tendinosis Jon A. Jacobson, MD, Corrie M. Yablon, MD, P. Troy Henning, DO, Irene S. Kazmers, MD, Andrew Urquhart, MD, Brian Hallstrom, MD, Asheesh Bedi, MD, Aishwarya Parameswaran, MS Supported by the American Institute of Ultrasound in Medicine Endowment for Education and Research Received November 20, 2015, from the Departments of Radiology (J.A.J., C.M.Y.), Physical Medicine and Rehabilitation (P.T.H.), and Orthopedic Surgery (A.U., B.H., A.B.), and Michigan Institute for Clinical and Health Research (A.P.), University of Michigan, Ann Arbor, Michigan USA; and Northern Michigan Rheumatology, Petoskey, Michigan USA (I.S.K.). Revision requested December 8, Revised manuscript accepted for publication February 6, This study was funded by a seed grant from the American Institute of Ultrasound in Medicine Endowment for Education and Research and by the National Center for Advanced Translational Sciences of the National Institutes of Health under award UL1TR000433, with research equipment provided by Harvest Terumo. Address correspondence to Jon A. Jacobson, MD, Department of Radiology, University of Michigan, 1500 E Medical Center Dr, TC2910L, Ann Arbor, MI USA. jjacobsn@umich.edu Abbreviations PRP, platelet-rich plasma doi: /ultra Objectives The purpose of this study was to compare ultrasound-guided percutaneous tendon fenestration to platelet-rich plasma (PRP) injection for treatment of greater trochanteric pain syndrome. Methods After Institutional Review Board approval was obtained, patients with symptoms of greater trochanteric pain syndrome and ultrasound findings of gluteal tendinosis or a partial tear (<50% depth) were blinded and treated with ultrasound-guided fenestration or autologous PRP injection of the abnormal tendon. Pain scores were recorded at baseline, week 1, and week 2 after treatment. Retrospective clinic record review assessed patient symptoms. Results The study group consisted of 30 patients (24 female), of whom 50% were treated with fenestration and 50% were treated with PRP. The gluteus medius was treated in 73% and 67% in the fenestration and PRP groups, respectively. Tendinosis was present in all patients. In the fenestration group, mean pain scores were 32.4 at baseline, 16.8 at time point 1, and 15.2 at time point 2. In the PRP group, mean pain scores were 31.4 at baseline, 25.5 at time point 1, and 19.4 at time point 2. Retrospective follow-up showed significant pain score improvement from baseline to time points 1 and 2 (P <.0001) but no difference between treatment groups (P =.1623). There was 71% and 79% improvement at 92 days (mean) in the fenestration and PRP groups, respectively, with no significant difference between the treatments (P >.99). Conclusions Our study shows that both ultrasound-guided tendon fenestration and PRP injection are effective for treatment of gluteal tendinosis, showing symptom improvement in both treatment groups. Key Words fenestration; gluteal; musculoskeletal ultrasound; platelet-rich plasma; tendinosis; tenotomy; trochanter Greater trochanteric pain syndrome is a common condition that most commonly affects middle-aged and elderly women and potentially younger active male and female individuals. 1 Symptoms include pain referable to the lateral hip as well as point tenderness that often interferes with activity and sleeping. 2,3 Contrary to prior misconceptions that symptoms were due to underlying bursitis, it has been shown that the underlying etiology for greater trochanteric pain syndrome is most commonly tendinosis or a tendon tear of the gluteus medius, gluteus minimus, or both at the greater trochanter and that tendon inflammation (or tendinitis) is not a major feature. 4 7 In addition, adjacent bursal distention is uncommon, and the bursa is neither inflamed nor a cause of patient symptoms in most situations. 7,8 Treatment of greater trochanteric 2016 by the American Institute of Ultrasound in Medicine J Ultrasound Med 2016; 35:
2 pain syndrome should therefore be directed to treatment of the underlying tendon condition. Ultrasound-guided percutaneous needle fenestration (or tenotomy) has been used to effectively treat underlying tendinosis and tendon tears, including tendons about the hip and pelvis The rationale behind tendon fenestration is that a chronic degenerative tendon process is converted to an acute process, and inherent growth factors are introduced with bleeding, thereby promoting tendon healing. 10 Similarly, autologous platelet-rich plasma (PRP), often combined with tendon fenestration, has been used throughout the body to treat tendinosis and tendon tears, as injection into a tendon promotes healing via the introduction of growth factors concentrated in and released from platelets. 14 Although studies have shown patient improvement with PRP treatment, the true effectiveness of this treatment compared to other treatments remains uncertain Although percutaneous ultrasound-guided tendon fenestration has been shown to be effective about the hip and pelvis, there are no data describing the use of PRP for treatment of gluteal tendons, and there is no study comparing the effectiveness of each treatment for gluteal tendinopathy. 9 The purpose of this blinded prospective clinical trial was to compare ultrasound-guided tendon fenestration and PRP for treatment of gluteus tendinosis or partial-thickness tears in greater trochanteric pain syndrome. Materials and Methods Institutional Review Board approval was obtained before initiation of this study. Patients were recruited from referring physicians of various departments, including internal medicine, family medicine, rheumatology, sports medicine, physical medicine and rehabilitation, and orthopedic surgery. If a patient had signs and symptoms consistent with the clinical diagnosis of greater trochanteric pain syndrome, which included pain referable to the greater trochanter, and had failed conservative management, including physical therapy and nonsteroidal anti-inflammatory drugs, the patient would be considered for the clinical trial. If the patient was interested in enrolling, the patient would then be referred for an ultrasound examination to evaluate for a gluteal tendon abnormality and to exclude other types of hip disorders as part of patient care. Ultrasound examinations of the hip were performed by 1 of 10 fellowship-trained musculoskeletal radiologists with musculoskeletal ultrasound experience using commercially available ultrasound equipment (iu22 and EPIQ; Philips Healthcare, Bothell, WA; and LOGIQ 9 and E9; GE Healthcare, Milwaukee, WI) and transducers (linear and curvilinear transducers with variable frequencies ranging from 5 to 15 MHz). The hip ultrasound protocol included imaging the gluteus minimus and medius tendons in short and long axes, as well as imaging the greater trochanteric area for the presence of bursal distention. Tendinosis was characterized as abnormal hypoecho - genicity of the tendon with possible enlargement. A tendon tear was characterized as an anechoic tendon defect. In contrast to a partial-thickness tear, a full-thickness tear shows an anechoic defect extending to both tendon surfaces with possible tendon retraction. The principal investigator reviewed the sonograms of the potential participant. Initial inclusion criteria included the presence of tendinosis or a partial-thickness tendon tear (<50% depth) of the gluteus minimus or gluteus medius tendon. If inclusion criteria were met, the primary investigator then contacted the potential participant via phone to explain the study and to assess for exclusion criteria, which included age younger than 18 years, pregnancy, risk of bleeding due to anticoagulant medication, presence of malignancy, and steroid injection less than 3 months before enrollment. Patients were then informed to discontinue aspirin and other nonsteroidal anti-inflammatory drugs for 2 weeks before the procedure. At the time of the procedure, the patient signed the Institutional Review Board approved research consent form. The patient was informed of the procedure risks (bleeding, infection, tendon rupture, allergy to medication, and pain), and the procedure consent form was also signed by the patient and primary investigator. An ultrasound examination of the affected hip was performed to document the presence of gluteus minimus or medius tendinosis or a partial-thickness tear (<50% depth), and the skin was marked at the planned puncture site. If both tendons were abnormal, the most sonographically abnormal tendon that was also symptomatic with transducer pressure was chosen for treatment. The patient also answered a series of questions with regard to hip symptoms (Table 1). Patients were placed into either the tendon fenestration or PRP treatment arm based on the previous patient s treatment so that fenestration and PRP treatments would alternate between each subsequent patient. If there was an error in the PRP process (inadequate venous blood draw or failed PRP preparation), then that patient would be converted to the fenestration treatment arm. Patients were blinded with respect to their treatment arm. In each patient, venous blood was drawn from one of the antecubital veins at the elbow. If the patient was in the tendon fenestration arm, 10 ml of venous blood was 2414 J Ultrasound Med 2016; 35:
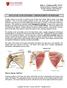
3 drawn and discretely discarded, although the centrifuge lid was opened and closed regardless. If in the PRP treatment arm, 60 ml of blood was drawn into a syringe with the anticoagulant citrate dextrose, placed into a centrifuge (Harvest Technologies, Lakewood, CO), and centrifuged at up to 2650 rpm for approximately 14 minutes. This PRP preparation kit is commercially available and is reported to produce a leukocyte-rich sample (primarily mononuclear) Table 1. Patient-Reported Outcomes Outcome Score Level of pain 0 (no pain) to 10 (pain as bad as could imagine) Pain interfering with 0 (does not interfere) to 10 general activity (completely interferes) Pain interfering with walking 0 (does not interfere) to 10 (completely interferes) Pain interfering with 0 (does not interfere) to 10 climbing stairs (completely interferes) Pain interfering with sleeping 0 (does not interfere) to 10 (completely interferes) with a platelet concentration 4 to 6 times that in whole blood. A successful PRP preparation resulted in approximately 10 ml of PRP. If the PRP sample was less than 7 ml, the sample was discretely discarded, and the patient was switched to the tendon fenestration arm. For the ultrasound-guided percutaneous procedure, the transducer (linear or curvilinear, >7 MHz) was positioned either long or short axis to the involved gluteal tendon. With a sterile technique, a transducer cover, and sterile drapes, a 20-gauge, 3.5-in spinal needle with trocar was inserted in plane with the ultrasound transducer and sound beam. Less than 1 ml of local anesthetic (1% lidocaine) was initially injected with a 25-gauge needle at the skin surface. Subsequently, less than 1 ml of lidocaine was then injected over the surface of the tendon via the 20-gauge spinal needle. In the tendon fenestration arm, the 20- gauge needle with trocar removed was passed approximately 20 to 30 times at various angles through the abnormal tendon until the abnormal area was covered and the tendon softened (Figure 1). In the PRP treatment arm, the needle was inserted into the deepest aspect of the ten- Figure 1. Images from a 55-year-old man with gluteus minimus tendinosis treated with fenestration. A and B, Sonograms short axis (A) and long axis (B) to the gluteus minimus showing a hypoechoic and thickened gluteus minimus tendon (arrows). Note the apex of the greater trochanter (asterisk) separating the anterior facet (AF) and lateral facet (LF) seen short axis to the femur in A, gluteus medius (Gmed), and iliotibial tract (ITB). C, Sonogram long axis to the gluteus minimus showing a 20-gauge spinal needle (arrowheads) with the distal tip in the area of tendinosis (arrow). Right side of A is anterior, and right side of B and C is distal. J Ultrasound Med 2016; 35:
4 don abnormality, and the PRP was injected as the needle was withdrawn through the abnormal tendon segment (Figures 2 and 3). This process was repeated until the entire abnormal tendon segment was treated. In contrast to the tendon fenestration arm, the number of times the needle was passed through the tendon was minimized and estimated as less than 10. During the procedure, the patient was instructed to look away from the procedure area to remain blinded to the treatment arm. After the procedure, the patient was instructed to avoid nonsteroidal anti-inflammatory drugs for 2 weeks. For the first week, the patient was also instructed to avoid strenuous activity with regard to the hip. Activity was gradually increased during the second week as tolerated. Patients were contacted via phone or by the primary investigator at weeks 1 and 2 to assess hip symptoms by asking the same series of questions that was completed before the procedure (Table 1). The patient was instructed to follow-up with the referring clinician to reassess the hip between 4 and 6 weeks. Patients were subsequently e- mailed, and clinical records were reviewed by the primary investigator to determine whether patient symptoms referable to the greater trochanter were improved, similar, or worse compared to before the procedure beyond the initial 2-week data collection. Baseline patient demographics and summated pain scores were compared between the treatment groups (fenestration versus PRP) to determine whether any significant difference existed, using the Fisher exact test for categorical variables and an independent-group t test for continuous variables. Summated patient pain scores were analyzed by repeated-measures 1-way analysis of variance over time adjusted for the treatment group. A paired comparison of different time points was performed by post hoc Tukey correction for multiple comparisons. In addition, the percentages of patients who showed improvement over time based on retrospective clinical chart review were compared between the treatment arms for any significant difference by the Fisher exact test. P <.05 was considered statistically significant. Results Of the 30 patients, 50% were treated with tendon fenestration (Figure 1), and 50% were treated with PRP (Figures 2 and 3). The mean patient age was 57 years (range, 24 to 81 years), with no significant age difference between the treatment groups (Table 2). The patients consisted of 6 men and 24 women, with no significant difference between the treatment groups. The left side was affected in 12 patients Figure 2. Images from a 69-year-old woman with gluteus medius tendinosis treated with PRP injection. A and B, Sonograms short axis (A) and long axis (B) to the gluteus medius showing a hypoechoic and thickened gluteus medius tendon (arrows) at the attachment on the lateral facet (LF) and superoposterior facet (SPF) of the greater trochanter. Note the apex of the greater trochanter (asterisk) separating the anterior facet (AF) and lateral facet seen short axis to the femur in A, gluteus minimus (Gmin), and iliotibial tract (ITB). C, Sonogram long axis to the gluteus medius showing a 20-gauge spinal needle (arrowheads) with the distal tip in the area of tendinosis (arrow). Right side of A is anterior, and right side of B and C is distal J Ultrasound Med 2016; 35:
5 and the right side in 18, with no significant difference between the treatment groups. The gluteus medius was treated in 73% and 67% in the fenestration and PRP groups, respectively, with no significant difference between the treatment groups, with the gluteus minimus treated in the remaining patients. Tendinosis was present in all patients, with no patients having a tendon tear. In no patient was a distended bursa identified in the region of the greater trochanter, and similarly, in no cases were tendon calcifications seen at the ultrasound examination. Two patients initially assigned to the PRP group were moved to the fenestration group because of an error in the PRP preparation process. There were no immediate complications after the procedures. Regarding follow-up intervals after tendon procedures, the mean time from the procedure to symptom assessment at time point 1 in the fenestration group was 7.9 (range, 7 to 13) days, and in the PRP group, it was 8.0 (range, 7 to 10) days, with no significant difference between the groups (P =.8996). At time point 2, the mean time from the procedure to symptom assessment in the fenestration group was 17.6 (range, 14 to 23) days, and in the PRP group, it was 15.3 (range, 14 to 20) days, which was significantly different between the groups (P =.0425). Retrospective clinical follow-up was available in 93% (14 of 15) and 93% (14 of 15) of the fenestration and PRP treatment groups, respectively, with mean intervals of 128 (SD, 141.1; range, 15 to 555) and 55.7 (SD, 27.7; range, 21 to 108) days from baseline, respectively (mean for both groups combined was 92 days), with no significant difference between the treatment groups (P =.0815). When comparing the pain scores between the treatment groups at each time point, at baseline the mean pain score in the fenestration group was 32.4 (SD, 10.2; range, 8 to 49), and in the PRP group, it was 31.4 (SD, 7.3; range, 11 to 41). At time point 1, the mean pain score after fenestration was 16.8 (SD, 11.46; range, 0 to 34), which was lower than the PRP group pain score of 25.5 (SD, 8.77; range, 9 to 40.5). At time point 2, the mean pain score after fenestration was 15.2 (SD, 10.8; range, 0 to 34), and after PRP treatment, it was 19.4 (SD, 10.26; range, 4 to 42). Regarding changes in summated pain scores in each treatment group from baseline, at time point 1, 93% of patients (13 of 14) after fenestration showed improvement (mean improvement, 15; range, 46 to 4), compared with 79% (11 of 14) after PRP treatment (mean improvement, 5.6; range, 21 to 15). At time point 2 compared to baseline, 93% of patients (14 of 15) after fenestration showed improvement (mean improvement, 17; range, 46 to 0), compared with 80% (12 of 15) after PRP treatment (mean improvement, 12; range, 28 to 5). Analysis of summated pain scores showed that overall, there was a significant time effect on the summated pain score (Table 3). The type of treatment had no significant effect on the summated pain score. Pair-wise comparison showed a significant change in summated pain scores between baseline and time point 1, as well as baseline and time point 2. There was no significant change in summated pain scores between time points 1 and 2. At final retrospective clinical follow-up, 71% (10 of 14) of fenestration patients and 79% (11 of 14) of PRP patients showed improvement, with no significant difference between the groups (P >.99). Figure 3. Images from a 61-year-old woman with gluteus medius tendinosis treated with PRP injection. A, Sonogram long axis to the gluteus medius showing hypoechoic tendinosis (arrows) of the gluteus medius tendon predominantly at the attachment on the superoposterior facet (SPF) with less involvement at the lateral facet (LF) and the greater trochanter. B, Sonogram long axis to the gluteus medius showing a 20-gauge spinal needle (arrowheads) with the distal tip in the area of tendinosis (arrow). Right side of images is distal. J Ultrasound Med 2016; 35:
6 Discussion Symptoms from greater trochanteric pain syndrome can be quite substantial and markedly decrease quality of life. The underlying conditions producing such symptoms in most cases are tendinosis and tears of the gluteal tendons at the greater trochanter. 5 7 An effective percutaneous treatment directed at these conditions would therefore be important. Our study has shown that both ultrasoundguided tendon fenestration and PRP injection are effective for treatment of greater trochanteric pain syndrome secondary to tendinosis, with improvement in pain scores from baseline to weeks 1 and 2 and 71% and 79% improvement at 92 days (mean) in the fenestration and PRP groups, respectively, with no significant difference between the treatments. The greater trochanter of the proximal femur serves as the insertion of gluteus minimus and medius tendons. The footprints or bony insertions of the gluteus minimus Table 2. Patient Demographics Characteristic Fenestration PRP P n Age, y.1611 Mean SD Minimum Maximum Side, n (%).2635 Left 8 (53.33) 4 (26.67) Right 7 (46.67) 11 (73.33) Sex, n (%).1686 Female 10 (66.67) 14 (93.33) Male 5 (33.33) 1 (6.67) Tendon, n (%) >.99 Gluteus minimus 4 (26.67) 5 (33.33) Gluteus medius 11 (73.33) 10 (66.67) Table 3. Repeated Measures of Analysis of Pain Score Total Over Time Adjusted for Treatment Type Mean Pain Parameter Score Estimate (SE) P a Visit <.0001 Treatment (1.91) vs (1.91) Pair-wise comparison for visits Time point 1 vs baseline (n = 28) (1.87) vs (1.82) <.0001 Time point 2 vs baseline (n = 30) (1.82) vs (1.82) <.0001 Time point 2 vs 1 (n = 28) (1.82) vs (1.87).0569 a One-way repeated measures analysis of variance for outcome of total pain score over time adjusted for treatment with post hoc Tukey correction to adjust for multiple comparisons. and medius tendons on the greater trochanter are geographically related to the facets of the greater trochanter, where the gluteus minimus tendon inserts onto the anterior facet, and the gluteus medius inserts onto the lateral and superoposterior facets. 18 The gluteus maximus passes superficial to the posterior facet to insert onto the linea aspera of the proximal femur and iliotibial band. Respective bursae are located deep to each gluteal muscle and tendons. Greater trochanteric pain syndrome most commonly involves middle-aged and elderly women. Pain is characteristically referred to the lateral hip over the greater trochanter with point tenderness. Symptoms are exacerbated by walking; pain interfering with sleeping often occurs when patients lie on the lateral affected hip. 2 The underlying condition in the setting of greater trochanteric pain syndrome in most cases has been shown to be tendinosis or a tendon tear of the gluteus medius and, less commonly, the gluteus minimus tendon, with an absence of acute inflammation. 4 6 Bursitis is not a common cause of symptoms. In patients with greater trochanteric pain syndrome, only 20% will have a distended trochanteric bursa on ultrasound imaging. 7 In addition, it has been shown that a distended bursa in this setting is typically not inflamed. 8 The distended bursa is not believed to be the primary cause of symptoms but may be simply a finding associated with the underlying gluteal tendon abnormality. Treatment for trochanteric pain syndrome should therefore be directed to treatment of the underlying tendon disorder. A historic treatment for greater trochanteric pain syndrome has been percutaneous corticosteroid injection, largely because of the misconception that inflammation was present. The use of corticosteroids in this setting is counterintuitive, as true tendinitis is not present, and true bursitis is uncommon. When corticosteroids are injected superficial to tendinosis, pain levels have been shown to improve, with one study reporting that 72% of patients were improved 1 month after injection. 1 However, the pain relief is typically short lived, and there is a risk of tendon rupture if corticosteroids are injected into a tendon. 10 Percutaneous tendon fenestration (also called dry needling or tenotomy) has been used to directly treat tendinosis and partial-thickness tendon tears. 1 The theory behind this treatment is that a chronic degenerative process is converted to an acute process. Bleeding introduces growth factors to induce inflammation and promote healing. The use of ultrasound guidance is important for accurately directing the tendon treatment to the abnormal area. Although studies have shown patient improvement after ultrasound-guided tendon fenestration, there are only limited studies evaluating fenestration of gluteal tendons, and 2418 J Ultrasound Med 2016; 35:
7 there are no studies comparing gluteal tendon fenestration to other tendon treatments such as PRP injection. 9 13,19 21 Although a comprehensive review of PRP treatment is beyond the scope of this discussion and has previously been described in the literature, PRP involves centrifuging autologous venous blood to separate the platelet-rich layer, which can then be injected into an abnormal tendon to promote healing. 14,22,23 Similar to tendon fenestration but in a higher concentration, growth factors are released from α granules in platelets to promote tendon healing. When PRP is injected, the tendon is typically fenestrated as well, and the use of ultrasound guidance ensures accurate localization of the tendon abnormality and targeted injection. There are intrinsic variations in PRP preparations with regard to platelet count and whether PRP preparations are leukocyte rich or leukocyte poor depending on which preparation kit is used. Nonetheless, studies have shown that patients improve after PRP tendon injection. However, most metaanalyses are inconclusive with regard to the effectiveness of PRP compared to other percutaneous tendon treatments, such as fenestration. 15,16 The results of our study show that both ultrasoundguided percutaneous tendon fenestration and PRP injection are effective for treatment of gluteus medius and minimus tendinosis. In 2-week follow-up of patients, improvement in pain scores was seen in 93% (14 of 15) in the fenestration group and 80% (12 of 15) in the PRP group. The lower improvement rate in the PRP group at this time may be explained by the inflammation induced by the PRP injection, which in this study was leukocyte rich; however, there was a significant improvement in summated pain scores between baseline and time points 1 and 2 but no significant difference in pain scores between the treatment types. Subsequent retrospective assessment of symptoms at 92 days after the procedures showed improvement in 71% and 79% of patients in the fenestration and PRP groups, respectively, with no significant difference between the treatments. This finding was also consistent with PRP results from the literature at different tendon injection sites, where symptom improvement continues over time. These results show that the symptom improvement is present early after treatment and is sustained over time. With regard to the PRP procedure, in this study, the tendon fenestration component was intentionally minimized compared to the dedicated tendon fenestration treatment group. In clinical practice, tendon fenestration is commonly performed either before or during the autologous PRP injection. It is not known whether increasing the fenestration component of the procedure would have any effect on patient symptom outcomes after PRP treatment. There were a number of study limitations that need to be addressed. First, long-term symptom improvement was limited by retrospective assessment, with a somewhat short interval and a wide range of follow-up durations. The sample size was limited because of budgetary constraints, and it remains possible that the effect size was not large enough to detect a difference between the treatment groups. Nonetheless, the results do show symptom improvement in the short term and months after treatment. The limited retrospective follow-up could be interpreted as a potential positive outcome if asymptomatic patients did not seek further treatment for their greater trochanter symptoms. Another limitation was that the PRP samples were not individually assessed for platelet count; however, the PRP preparation kit used is commercially available and is reported to concentrate platelets to 4 to 6 times that in whole blood. An additional limitation was that all patients had tendinosis, so it is unclear whether patients with tendon tears would respond in a different manner. One last limitation was that patient care after treatment was not controlled, which may affect longer-term clinical outcomes. Future prospective studies to include more long-term and objective clinical assessment are required. In conclusion, this single-blinded prospective study shows that both ultrasound-guided tendon fenestration and PRP injection are effective for treatment of greater trochanteric pain syndrome, showing improvement in pain scores at 1 and 2 weeks, with no significant difference between the treatments. Improvement was also seen at 92 days (mean) in 71% and 79% of the fenestration and PRP groups, respectively. Future randomized controlled trials are needed to determine more long-term clinical outcomes. References 1. Labrosse JM, Cardinal E, Leduc BE, et al. Effectiveness of ultrasoundguided corticosteroid injection for the treatment of gluteus medius tendinopathy. AJR Am J Roentgenol 2010; 194: Mallow M, Nazarian LN. Greater trochanteric pain syndrome diagnosis and treatment. Phys Med Rehabil Clin N Am 2014; 25: Blankenbaker DG, Ullrick SR, Davis KW, De Smet AA, Haaland B, Fine JP. Correlation of MRI findings with clinical findings of trochanteric pain syndrome. Skeletal Radiol 2008; 37: Fearon AM, Scarvell JM, Cook JL, Smith PN. Does ultrasound correlate with surgical or histologic findings in greater trochanteric pain syndrome? A pilot study. Clin Orthop Relat Res 2010; 468: Connell DA, Bass C, Sykes CA, Young D, Edwards E. Sonographic evaluation of gluteus medius and minimus tendinopathy. Eur Radiol 2003; 13: J Ultrasound Med 2016; 35:
8 6. Kingzett-Taylor A, Tirman PF, Feller J, et al. Tendinosis and tears of gluteus medius and minimus muscles as a cause of hip pain: MR imaging findings. AJR Am J Roentgenol 1999; 173: Long SS, Surrey DE, Nazarian LN. Sonography of greater trochanteric pain syndrome and the rarity of primary bursitis. AJR Am J Roentgenol 2013; 201: Silva F, Adams T, Feinstein J, Arroyo RA. Trochanteric bursitis: refuting the myth of inflammation. J Clin Rheumatol 2008; 14: Jacobson JA, Rubin J, Yablon CM, Kim SM, Kalume-Brigido M, Parameswaran A. Ultrasound-guided fenestration of tendons about the hip and pelvis: clinical outcomes. J Ultrasound Med 2015; 34: Chiavaras MM, Jacobson JA. Ultrasound-guided tendon fenestration. Semin Musculoskelet Radiol 2013; 17: Kanaan Y, Jacobson JA, Jamadar D, Housner J, Caoili EM. Sonographically guided patellar tendon fenestration: prognostic value of preprocedure sonographic findings. J Ultrasound Med 2013; 32: McShane JM, Nazarian LN, Harwood MI. Sonographically guided percutaneous needle tenotomy for treatment of common extensor tendinosis in the elbow. J Ultrasound Med 2006; 25: McShane JM, Shah VN, Nazarian LN. Sonographically guided percutaneous needle tenotomy for treatment of common extensor tendinosis in the elbow: is a corticosteroid necessary? J Ultrasound Med 2008; 27: Lee KS, Wilson JJ, Rabago DP, Baer GS, Jacobson JA, Borrero CG. Musculoskeletal applications of platelet-rich plasma: fad or future? AJR Am J Roentgenol 2011; 196: Sheth U, Simunovic N, Klein G, et al. Efficacy of autologous platelet-rich plasma use for orthopaedic indications: a meta-analysis. J Bone Joint Surg Am 2012; 94: Willits K, Kaniki N, Bryant D. The use of platelet-rich plasma in orthopedic injuries. Sports Med Arthrosc 2013; 21: Mautner K, Colberg RE, Malanga G, et al. Outcomes after ultrasoundguided platelet-rich plasma injections for chronic tendinopathy: a multicenter, retrospective review. PM R 2013; 5: Pfirrmann CW, Chung CB, Theumann NH, Trudell DJ, Resnick D. Greater trochanter of the hip: attachment of the abductor mechanism and a complex of three bursae MR imaging and MR bursography in cadavers and MR imaging in asymptomatic volunteers. Radiology 2001; 221: Housner JA, Jacobson JA, Misko R. Sonographically guided percutaneous needle tenotomy for the treatment of chronic tendinosis. J Ultrasound Med 2009; 28: Housner JA, Jacobson JA, Morag Y, Pujalte GG, Northway RM, Boon TA. Should ultrasound-guided needle fenestration be considered as a treatment option for recalcitrant patellar tendinopathy? A retrospective study of 47 cases. Clin J Sport Med 2010; 20: Testa V, Capasso G, Benazzo F, Maffulli N. Management of Achilles tendinopathy by ultrasound-guided percutaneous tenotomy. Med Sci Sports Exerc 2002; 34: Foster TE, Puskas BL, Mandelbaum BR, Gerhardt MB, Rodeo SA. Platelet-rich plasma: from basic science to clinical applications. Am J Sports Med 2009; 37: Hall MP, Band PA, Meislin RJ, Jazrawi LM, Cardone DA. Platelet-rich plasma: current concepts and application in sports medicine. J Am Acad Orthop Surg 2009; 17: J Ultrasound Med 2016; 35:
Greater Trochanter: Anatomy and Pathology
 Greater Trochanter: Anatomy and Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties:
Greater Trochanter: Anatomy and Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties:
Tendon Fenestration. Disclosures. Outline: questions. Introduction: Peritendon Steroid Injections. Jon A. Jacobson, MD. Patellar Tendon: tendinosis
 Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
Ultrasound of the Hip: Anatomy, Pathology, and Procedures
 Ultrasound of the Hip: Anatomy, Pathology, and Procedures Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Outline Hip Joint Native hip
Ultrasound of the Hip: Anatomy, Pathology, and Procedures Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Outline Hip Joint Native hip
Ultrasound-Guided Tendon Fenestration
 85 Mary M. Chiavaras, MD, PhD 1 Jon A. Jacobson, MD 2 1 Department of Radiology, McMaster University, Hamilton General Hospital, Hamilton, Ontario, Canada 2 Department of Radiology, University of Michigan,
85 Mary M. Chiavaras, MD, PhD 1 Jon A. Jacobson, MD 2 1 Department of Radiology, McMaster University, Hamilton General Hospital, Hamilton, Ontario, Canada 2 Department of Radiology, University of Michigan,
Greater Trochanteric Pain Syndrome
 43 Andrea S. Klauser, MD 1 Carlo Martinoli, MD 2 Alberto Tagliafico, MD 3 Rosa Bellmann-Weiler, MD 4 Gudrun M. Feuchtner, MD, PhD 1 Marius Wick, MD 1 Werner R. Jaschke, MD, PhD 1 1 Department of Diagnostic
43 Andrea S. Klauser, MD 1 Carlo Martinoli, MD 2 Alberto Tagliafico, MD 3 Rosa Bellmann-Weiler, MD 4 Gudrun M. Feuchtner, MD, PhD 1 Marius Wick, MD 1 Werner R. Jaschke, MD, PhD 1 1 Department of Diagnostic
Common Applications for Sonography and Guided Intervention: Shoulder
 Common Applications for Sonography and Guided Intervention: Shoulder Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant:
Common Applications for Sonography and Guided Intervention: Shoulder Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant:
Sonographically Guided Percutaneous Needle Tenotomy for the Treatment of Chronic Tendinosis
 Article Sonographically Guided Percutaneous Needle Tenotomy for the Treatment of Chronic Tendinosis Jeffrey A. Housner, MD, Jon A. Jacobson, MD, Roberta Misko, PT, PA-C Objective. Initial reports have
Article Sonographically Guided Percutaneous Needle Tenotomy for the Treatment of Chronic Tendinosis Jeffrey A. Housner, MD, Jon A. Jacobson, MD, Roberta Misko, PT, PA-C Objective. Initial reports have
Snapping Hip and Impingement
 Snapping Hip and Impingement Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board: GE,
Snapping Hip and Impingement Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board: GE,
Ultrasound-Guided Calcific Tendinitis Lavage: Application, Technique, and Outcome
 Ultrasound-Guided Calcific Tendinitis Lavage: Application, Technique, and Outcome Andrew Schapiro MD, Humberto Rosas MD, Kenneth Lee MD University of Wisconsin Hospital and Clinics aschapiro@uwhealth.org
Ultrasound-Guided Calcific Tendinitis Lavage: Application, Technique, and Outcome Andrew Schapiro MD, Humberto Rosas MD, Kenneth Lee MD University of Wisconsin Hospital and Clinics aschapiro@uwhealth.org
Greater Trochanteric Pain Syndrome (GTPS): Assessment & Management
 Greater Trochanteric Pain Syndrome (GTPS): Assessment & Management Rachael Mary McMillan Physiotherapist, Alphington Sports Medicine Clinic & FFA Australian Women s National Football Teams PhD Candidate
Greater Trochanteric Pain Syndrome (GTPS): Assessment & Management Rachael Mary McMillan Physiotherapist, Alphington Sports Medicine Clinic & FFA Australian Women s National Football Teams PhD Candidate
Pure bone marrow aspirate injection for chronic greater trochanteric pain syndrome: a case report
 Case Report For reprint orders, please contact: reprints@futuremedicine.com Pure bone marrow aspirate injection for chronic greater trochanteric pain syndrome: a case report Rachel G Henderson*,1,2 & Ricardo
Case Report For reprint orders, please contact: reprints@futuremedicine.com Pure bone marrow aspirate injection for chronic greater trochanteric pain syndrome: a case report Rachel G Henderson*,1,2 & Ricardo
Effectiveness of Ultrasound-Guided Corticosteroid Injection for the Treatment of Gluteus Medius Tendinopathy
 Musculoskeletal Imaging Original Research Labrosse et al. Ultrasound-Guided Corticosteroid Injection for Tendinopathy Musculoskeletal Imaging Original Research Julie M. Labrosse 1 Étienne Cardinal 1 Bernard
Musculoskeletal Imaging Original Research Labrosse et al. Ultrasound-Guided Corticosteroid Injection for Tendinopathy Musculoskeletal Imaging Original Research Julie M. Labrosse 1 Étienne Cardinal 1 Bernard
COMPARATIVE EFFECTIVENESS OF ULTRASOUND GUIDED INTRATENDINOUS PROLOTHERAPY INJECTION WITH CONVENTIONAL TREATMENT TO TREAT
 SCIENTIFIC ARTICLE COMPARATIVE EFFECTIVENESS OF ULTRASOUND GUIDED INTRATENDINOUS PROLOTHERAPY INJECTION WITH CONVENTIONAL TREATMENT TO TREAT FOCAL SUPRASPINATUS TENDINOSIS : RANDOMISED CONTROL STUDY 1,2
SCIENTIFIC ARTICLE COMPARATIVE EFFECTIVENESS OF ULTRASOUND GUIDED INTRATENDINOUS PROLOTHERAPY INJECTION WITH CONVENTIONAL TREATMENT TO TREAT FOCAL SUPRASPINATUS TENDINOSIS : RANDOMISED CONTROL STUDY 1,2
Rotator Cuff and Biceps Pathology
 Rotator Cuff and Biceps Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board:
Rotator Cuff and Biceps Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board:
tissue, Interventional non-vascular /ecr2014/C-1241
 Effectiveness of Ultrasound-guided Platelet Rich Plasma (PRP) injections after needle tenotomy in the treatment of chronic tendinopathies : A prospective study. Poster No.: C-1241 Congress: ECR 2014 Type:
Effectiveness of Ultrasound-guided Platelet Rich Plasma (PRP) injections after needle tenotomy in the treatment of chronic tendinopathies : A prospective study. Poster No.: C-1241 Congress: ECR 2014 Type:
Sonographic evaluation of gluteus medius and minimus tendinopathy
 Eur Radiol (2003) 13:1339 1347 DOI 10.1007/s00330-002-1740-4 MUSCULOSKELETAL David A. Connell Cheryl Bass Christopher J. Sykes David Young Elton Edwards Sonographic evaluation of gluteus medius and minimus
Eur Radiol (2003) 13:1339 1347 DOI 10.1007/s00330-002-1740-4 MUSCULOSKELETAL David A. Connell Cheryl Bass Christopher J. Sykes David Young Elton Edwards Sonographic evaluation of gluteus medius and minimus
A Patient s Guide to Trochanteric Bursitis of the Hip
 A Patient s Guide to Trochanteric Bursitis of the Hip Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
A Patient s Guide to Trochanteric Bursitis of the Hip Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation
 Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Ultrasound of the Knee
 Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
DISCLOSURE. The contributing authors have no financial relationships to disclose.
 DISCLOSURE The contributing authors have no financial relationships to disclose. INTRODUCTION Greater trochanteric pain syndrome (GTPS); formerly trochanteric bursitis Common condition, wide differential
DISCLOSURE The contributing authors have no financial relationships to disclose. INTRODUCTION Greater trochanteric pain syndrome (GTPS); formerly trochanteric bursitis Common condition, wide differential
Lateral Elbow Pathology
 Lateral Elbow Pathology Jon A. Jacobson, M.D. Professor of adiology Director, Division of Musculoskeletal adiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board: GE, Philips
Lateral Elbow Pathology Jon A. Jacobson, M.D. Professor of adiology Director, Division of Musculoskeletal adiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board: GE, Philips
Distal Pectoralis Major Tears
 ORIGINAL RESEARCH Distal Pectoralis Major Tears Sonographic Characterization and Potential Diagnostic Pitfalls Sun Joo Lee, MD, Jon A. Jacobson, MD, Sung-Moon Kim, MD, David Fessell, MD, Yebin Jiang, MD,
ORIGINAL RESEARCH Distal Pectoralis Major Tears Sonographic Characterization and Potential Diagnostic Pitfalls Sun Joo Lee, MD, Jon A. Jacobson, MD, Sung-Moon Kim, MD, David Fessell, MD, Yebin Jiang, MD,
Platelet Rich Plasma (PRP) injections. by Dr George Pitsis
 Platelet Rich Plasma (PRP) injections by Dr George Pitsis Platelet Rich Plasma (PRP) injections have in the more recent years attracted significant attention as a clinical tools to assist with treatment
Platelet Rich Plasma (PRP) injections by Dr George Pitsis Platelet Rich Plasma (PRP) injections have in the more recent years attracted significant attention as a clinical tools to assist with treatment
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation. Disclosures. Outline. Joint Effusion. Suprapatellar recess
 Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
High Hamstring Tendinopathy: MRI and Ultrasound Imaging and Therapeutic Efficacy of Percutaneous Corticosteroid Injection
 Musculoskeletal Imaging Clinical Perspective Zissen et al. Imaging of High Hamstring Tendinopathy Musculoskeletal Imaging Clinical Perspective Maurice H. Zissen 1 Grant Wallace 1 Kathryn J. Stevens 1 Michael
Musculoskeletal Imaging Clinical Perspective Zissen et al. Imaging of High Hamstring Tendinopathy Musculoskeletal Imaging Clinical Perspective Maurice H. Zissen 1 Grant Wallace 1 Kathryn J. Stevens 1 Michael
Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions
 APPENDIX G Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions The purpose of this document is to provide information for physiotherapists of common medical and surgical interventions
APPENDIX G Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions The purpose of this document is to provide information for physiotherapists of common medical and surgical interventions
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A ACJ. See Acromioclavicular joint (ACJ) Acromioclavicular joint (ACJ) procedures of, 557 559 Ankle and foot procedures of, 649 671 (See also
Note: Page numbers of article titles are in boldface type. A ACJ. See Acromioclavicular joint (ACJ) Acromioclavicular joint (ACJ) procedures of, 557 559 Ankle and foot procedures of, 649 671 (See also
Tears in the gluteus medius and minimus tendons
 Endoscopic Repair of Full-Thickness Gluteus Medius Tears Benjamin G. Domb, M.D., and Dominic S. Carreira, M.D. Abstract: Tears in the gluteus medius and minimus tendons recently have emerged as an important
Endoscopic Repair of Full-Thickness Gluteus Medius Tears Benjamin G. Domb, M.D., and Dominic S. Carreira, M.D. Abstract: Tears in the gluteus medius and minimus tendons recently have emerged as an important
Technical Note. Arthroscopic Anatomy and Surgical Techniques for Peritrochanteric Space Disorders in the Hip
 Technical Note Arthroscopic Anatomy and Surgical Techniques for Peritrochanteric Space Disorders in the Hip James E. Voos, M.D., Jonas R. Rudzki, M.D., Michael K. Shindle, M.D., Hal Martin, D.O., and Bryan
Technical Note Arthroscopic Anatomy and Surgical Techniques for Peritrochanteric Space Disorders in the Hip James E. Voos, M.D., Jonas R. Rudzki, M.D., Michael K. Shindle, M.D., Hal Martin, D.O., and Bryan
The Role of Sonography in Differentiating Full Versus Partial Distal Biceps Tendon Tears: Correlation With Surgical Findings
 Musculoskeletal Imaging Original Research Da Gama Lobo et al. Sonography in Biceps Tendon Tears Musculoskeletal Imaging Original Research Lucas Da Gama Lobo 1,2 David P. Fessell 1 Bruce S. Miller 1,3 Aine
Musculoskeletal Imaging Original Research Da Gama Lobo et al. Sonography in Biceps Tendon Tears Musculoskeletal Imaging Original Research Lucas Da Gama Lobo 1,2 David P. Fessell 1 Bruce S. Miller 1,3 Aine
Sonographic Findings of Pectoralis Major Tears With Surgical, Clinical, and Magnetic Resonance Imaging Correlation in 6 Patients
 Article Sonographic Findings of Pectoralis Major Tears With Surgical, Clinical, and Magnetic Resonance Imaging Correlation in 6 Patients Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS,
Article Sonographic Findings of Pectoralis Major Tears With Surgical, Clinical, and Magnetic Resonance Imaging Correlation in 6 Patients Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS,
KAPA 2017 Musculoskeletal Aspiration and Injection Workshop. W. Scott Black, MD Physician Assistant Studies Program University of Kentucky
 KAPA 2017 Musculoskeletal Aspiration and Injection Workshop W. Scott Black, MD Physician Assistant Studies Program University of Kentucky Aspiration Relatively quick and inexpensive Can be performed in
KAPA 2017 Musculoskeletal Aspiration and Injection Workshop W. Scott Black, MD Physician Assistant Studies Program University of Kentucky Aspiration Relatively quick and inexpensive Can be performed in
Ultrasound Evaluation of Masses
 Ultrasound Evaluation of Masses Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Panel: GE,
Ultrasound Evaluation of Masses Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Panel: GE,
Original Report. Sonography of Ankle Tendon Impingement with Surgical Correlation
 Downloaded from www.ajronline.org by 162.158.89.91 on 08/23/18 from IP address 162.158.89.91. Copyright RRS. For personal use only; all rights reserved Monisha Shetty 1 David P. Fessell 1 John E. Femino
Downloaded from www.ajronline.org by 162.158.89.91 on 08/23/18 from IP address 162.158.89.91. Copyright RRS. For personal use only; all rights reserved Monisha Shetty 1 David P. Fessell 1 John E. Femino
Subacromial Bursa Injection
 Subacromial Bursa Injection 5 cc syringe, 21 gauge 1.5 inch needle 1% lidocaine - 4cc 40mg triamcinolone - 1 cc of 40mg/ml identify site-seat the patient with weight of arm hanging down, palpate the lateral
Subacromial Bursa Injection 5 cc syringe, 21 gauge 1.5 inch needle 1% lidocaine - 4cc 40mg triamcinolone - 1 cc of 40mg/ml identify site-seat the patient with weight of arm hanging down, palpate the lateral
Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology?
 Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology? Poster No.: C-1603 Congress: ECR 2013 Type: Scientific Exhibit
Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology? Poster No.: C-1603 Congress: ECR 2013 Type: Scientific Exhibit
A Patient s Guide to Trochanteric Bursitis of the Hip. William T. Grant, MD
 A Patient s Guide to Trochanteric Bursitis of the Hip Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C
A Patient s Guide to Trochanteric Bursitis of the Hip Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C
9/18/18. Welcome- MSK Ultrasound Workshop. Introduction to Musculoskeletal Ultrasound. Acknowledgement of Country. The Workshop.
 Acknowledgement of Country Welcome- MSK Ultrasound Workshop I would like to acknowledge that this meeting is being held on the traditional lands of the Wurundjeri and Boonwurrung people and pay my respect
Acknowledgement of Country Welcome- MSK Ultrasound Workshop I would like to acknowledge that this meeting is being held on the traditional lands of the Wurundjeri and Boonwurrung people and pay my respect
Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain. Plamen Todorov
 Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain Plamen Todorov INTRODUCTION Soft tissue rheumatism: nonsystemic, focal pathological syndromes involving the periarticular structures.
Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain Plamen Todorov INTRODUCTION Soft tissue rheumatism: nonsystemic, focal pathological syndromes involving the periarticular structures.
The evaluation and management of patients with
 Greater Trochanteric Hip Pain 1.5 ANCC Contact Hours Diane M. Kimpel Chadwick C. Garner Kevin M. Magone Jedediah H. May Matthew W. Lawless In the patient with lateral hip pain, there is a broad differential
Greater Trochanteric Hip Pain 1.5 ANCC Contact Hours Diane M. Kimpel Chadwick C. Garner Kevin M. Magone Jedediah H. May Matthew W. Lawless In the patient with lateral hip pain, there is a broad differential
Technical application and the level of discomfort associated with an intramuscular
 Original article (short communication) Technical application and the level of discomfort associated with an intramuscular electromyographic investigation into gluteus minimus and gluteus medius. Adam I.
Original article (short communication) Technical application and the level of discomfort associated with an intramuscular electromyographic investigation into gluteus minimus and gluteus medius. Adam I.
Poster No.: P-0101 Congress: ESSR Scientific Exhibit. Authors:
 Calcific shoulder tendinitis: outcomes after percutaneous treatment with Ultrasonography-guided needle aspiration of calcific deposits and bursal injection with steroids and local anaesthetics. Award:
Calcific shoulder tendinitis: outcomes after percutaneous treatment with Ultrasonography-guided needle aspiration of calcific deposits and bursal injection with steroids and local anaesthetics. Award:
US guided Injection in SASD bursitis ( 쉬운가? 어려운가?)
 US guided Injection in SASD bursitis ( 쉬운가? 어려운가?) Jaeki Ahn, M.D. Department of Rehabilitation Medicine, Sanggye Paik Hospital, Inje University 대한신경근골격초음파학회춘계학술대회 2012. 4.14 Contents Cases Bursa? Impingement
US guided Injection in SASD bursitis ( 쉬운가? 어려운가?) Jaeki Ahn, M.D. Department of Rehabilitation Medicine, Sanggye Paik Hospital, Inje University 대한신경근골격초음파학회춘계학술대회 2012. 4.14 Contents Cases Bursa? Impingement
Tendinopathy from Overuse: Overview and a New(er) Treatment Option
 Tendinopathy from Overuse: Overview and a New(er) Treatment Option Robert Flannery MD Assistant Professor, Division of Sports Medicine Department of Orthopedic Surgery, Case Western Reserve University
Tendinopathy from Overuse: Overview and a New(er) Treatment Option Robert Flannery MD Assistant Professor, Division of Sports Medicine Department of Orthopedic Surgery, Case Western Reserve University
Musculoskeletal Sonography of the Tendon
 SOUND JUDGMENT SERIES Musculoskeletal Sonography of the Tendon Kenneth S. Lee, MD Invited paper The Sound Judgment Series consists of invited articles highlighting the clinical value of using ultrasound
SOUND JUDGMENT SERIES Musculoskeletal Sonography of the Tendon Kenneth S. Lee, MD Invited paper The Sound Judgment Series consists of invited articles highlighting the clinical value of using ultrasound
JMSCR Volume 03 Issue 01 Page January 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Management of Chronic Plantar Fasciitis using Hyperosmolar Dextrose Injection Authors Ansarul Haq Lone 1, Omar Khursheed 2, Shakir Rashid
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Management of Chronic Plantar Fasciitis using Hyperosmolar Dextrose Injection Authors Ansarul Haq Lone 1, Omar Khursheed 2, Shakir Rashid
Gluteus Medius Tears After Hip Arthroplasty. John Urse, DO, FAOAO Jason Spangler, DO Dzi-Viet Nguyen, DO Grandview Medical Center Dayton, OH
 Gluteus Medius Tears After Hip Arthroplasty John Urse, DO, FAOAO Jason Spangler, DO Dzi-Viet Nguyen, DO Grandview Medical Center Dayton, OH Disclosures AANA (Arthroscopy Association of North America) Lodging
Gluteus Medius Tears After Hip Arthroplasty John Urse, DO, FAOAO Jason Spangler, DO Dzi-Viet Nguyen, DO Grandview Medical Center Dayton, OH Disclosures AANA (Arthroscopy Association of North America) Lodging
Latest technology in the treatment of chronic recalcitrant tendinopathy
 Latest technology in the treatment of chronic recalcitrant tendinopathy Dr K Arjun Rao Consultant Sport & Exercise Medicine Physician FACSEP FFSEM(UK) Specialist Sportscare W.A. WA Institute of Sport School
Latest technology in the treatment of chronic recalcitrant tendinopathy Dr K Arjun Rao Consultant Sport & Exercise Medicine Physician FACSEP FFSEM(UK) Specialist Sportscare W.A. WA Institute of Sport School
Achilles Tendinopathy: Medical and Surgical Interventions
 APPENDIX D Achilles Tendinopathy: Medical and Surgical Interventions The purpose of this document is to summarize common medical and surgical interventions which may be considered for the management of
APPENDIX D Achilles Tendinopathy: Medical and Surgical Interventions The purpose of this document is to summarize common medical and surgical interventions which may be considered for the management of
MRI Diagnosis of Tears of the Hip Abductor Tendons (Gluteus Medius and Gluteus Minimus)
 Oliver Cvitanic 1 Gregory Henzie 1 Nicholas Skezas 2 Jack Lyons 2 Jon Minter 3 Received October 2, 2002; accepted after revision July 10, 2003. 1 Southwest Oklahoma MRI, 13301 N Meridian Ave., Ste. 600A,
Oliver Cvitanic 1 Gregory Henzie 1 Nicholas Skezas 2 Jack Lyons 2 Jon Minter 3 Received October 2, 2002; accepted after revision July 10, 2003. 1 Southwest Oklahoma MRI, 13301 N Meridian Ave., Ste. 600A,
A Patient s Guide to Arthroscopy of the Hip
 A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
Ultrasound Guided Injections
 Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
Ultrasound of the Shoulder
 Ultrasound of the Shoulder Patrick Battaglia, DC, DACBR Logan University, Department of Radiology Outline Review ultrasound appearance of NMSK tissues Present indications for ultrasound of the shoulder.
Ultrasound of the Shoulder Patrick Battaglia, DC, DACBR Logan University, Department of Radiology Outline Review ultrasound appearance of NMSK tissues Present indications for ultrasound of the shoulder.
Platelet Rich Plasma (PRP) Dania Segreti, SPT Vanguard In-service - July 31, 2013
 Platelet Rich Plasma (PRP) Dania Segreti, SPT Vanguard In-service - July 31, 2013 What is PRP? In medicine since 1970s First uses in bone healing began in late 1990s Gained popularity for tissue healing
Platelet Rich Plasma (PRP) Dania Segreti, SPT Vanguard In-service - July 31, 2013 What is PRP? In medicine since 1970s First uses in bone healing began in late 1990s Gained popularity for tissue healing
Incidental Benign Musculoskeletal Findings on PET-CT: an Educational Pictorial Review
 Incidental Benign Musculoskeletal Findings on PET-CT: an Educational Pictorial Review Poster No.: P-0008 Congress: ESSR 2014 Type: Educational Poster Authors: F. Moloney, J. Ryan, M. Twomey, S. McSweeney;
Incidental Benign Musculoskeletal Findings on PET-CT: an Educational Pictorial Review Poster No.: P-0008 Congress: ESSR 2014 Type: Educational Poster Authors: F. Moloney, J. Ryan, M. Twomey, S. McSweeney;
Original Report. Sonography of Tears of the Distal Biceps Tendon. Theodore T. Miller 1,2 Ronald S. Adler 3
 Theodore T. Miller 1,2 Ronald S. dler 3 Received October 15, 1999; accepted after revision March 21, 2000. Presented at the annual meeting of the merican Roentgen Ray Society, Washington, DC, May 2000.
Theodore T. Miller 1,2 Ronald S. dler 3 Received October 15, 1999; accepted after revision March 21, 2000. Presented at the annual meeting of the merican Roentgen Ray Society, Washington, DC, May 2000.
Clinical Features That Predict the Need for Operative Intervention in Gluteus Medius Tears
 Clinical Features That Predict the Need for Operative Intervention in Gluteus Medius Tears Sivashankar Chandrasekaran,* MBBS, FRACS, S. Pavan Vemula,* MA, Chengcheng Gui,* BSE, Carlos Suarez-Ahedo,* MD,
Clinical Features That Predict the Need for Operative Intervention in Gluteus Medius Tears Sivashankar Chandrasekaran,* MBBS, FRACS, S. Pavan Vemula,* MA, Chengcheng Gui,* BSE, Carlos Suarez-Ahedo,* MD,
Pseudoaneurysm of the Breast During Vacuum-Assisted Removal
 Case Report Pseudoaneurysm of the Breast During Vacuum-Assisted Removal Yu-Mee Sohn, MD, Min Jung Kim, MD, Eun-Kyung Kim, MD, Sang Hoon Chung, MD, Jin Young Kwak, MD, Hee Jung Moon, MD, Soo Jin Kim, MD
Case Report Pseudoaneurysm of the Breast During Vacuum-Assisted Removal Yu-Mee Sohn, MD, Min Jung Kim, MD, Eun-Kyung Kim, MD, Sang Hoon Chung, MD, Jin Young Kwak, MD, Hee Jung Moon, MD, Soo Jin Kim, MD
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging
 Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Fluoroscopically Guided Peritendinous Corticosteroid Injection for Proximal Hamstring Tendinopathy
 Fluoroscopically Guided Peritendinous Corticosteroid Injection for Proximal Hamstring Tendinopathy A Retrospective Review Luke T. Nicholson,* MD, Steven DiSegna,* MD, Joel S. Newman,* MD, and Suzanne L.
Fluoroscopically Guided Peritendinous Corticosteroid Injection for Proximal Hamstring Tendinopathy A Retrospective Review Luke T. Nicholson,* MD, Steven DiSegna,* MD, Joel S. Newman,* MD, and Suzanne L.
Dr Hamish Osborne. Sport & Exercise Medicine Physician Dunedin
 Dr Hamish Osborne Sport & Exercise Medicine Physician Dunedin New Approaches to Handling Tendinopathies By Hamish Osborne Definition Tendinopathy Absence of tightly packed collagen bundles Large amount
Dr Hamish Osborne Sport & Exercise Medicine Physician Dunedin New Approaches to Handling Tendinopathies By Hamish Osborne Definition Tendinopathy Absence of tightly packed collagen bundles Large amount
What Internists Need To Know About Common Orthopedic Problems: Focus on Tendinopathy
 What Internists Need To Know About Common Orthopedic Problems: Focus on Tendinopathy Rebecca Dutton, MD ACP Annual Meeting, November 2, 2018 Disclosures I have no relevant financial or non-financial relationships
What Internists Need To Know About Common Orthopedic Problems: Focus on Tendinopathy Rebecca Dutton, MD ACP Annual Meeting, November 2, 2018 Disclosures I have no relevant financial or non-financial relationships
John J Christoforetti, MD Pittsburgh, Pennsylvania
 ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
PLATELET- RICH PLASMA (PRP) INJECTIONS
 PLATELET- RICH PLASMA (PRP) INJECTIONS Platelet-rich plasma (PRP) injections have become an extremely popular treatment option for patients with chronic tendon injuries. Although PRP injections have received
PLATELET- RICH PLASMA (PRP) INJECTIONS Platelet-rich plasma (PRP) injections have become an extremely popular treatment option for patients with chronic tendon injuries. Although PRP injections have received
The Essentials Tissue Characterization and Knobology
 The Essentials Tissue Characterization and Knobology Randy E. Moore, DC, RDMS RMSK No relevant financial relationships Ultrasound The New Standard of Care Musculoskeletal sonography has become the standard
The Essentials Tissue Characterization and Knobology Randy E. Moore, DC, RDMS RMSK No relevant financial relationships Ultrasound The New Standard of Care Musculoskeletal sonography has become the standard
Alex Garcia, MD Affinity Orthopedics and Sports Medicine
 Alex Garcia, MD Affinity Orthopedics and Sports Medicine Intact Tendon Reactive Inflammatory Tendinopathy Degenerative Chronic Tendinopathy INSULT Neurovascular Mediation Reparative Process? Healed 3
Alex Garcia, MD Affinity Orthopedics and Sports Medicine Intact Tendon Reactive Inflammatory Tendinopathy Degenerative Chronic Tendinopathy INSULT Neurovascular Mediation Reparative Process? Healed 3
Ultrasound-Guided Biceps Peritendinous Injections in the Absence of a Distended Tendon Sheath
 TECHNICAL INNOVATION Ultrasound-Guided Biceps Peritendinous Injections in the Absence of a Distended Tendon Sheath A Novel Rotator Interval Approach Taylor J. Stone, MD, Ronald S. Adler, MD, PhD This retrospective
TECHNICAL INNOVATION Ultrasound-Guided Biceps Peritendinous Injections in the Absence of a Distended Tendon Sheath A Novel Rotator Interval Approach Taylor J. Stone, MD, Ronald S. Adler, MD, PhD This retrospective
Fellowship Program. Musculoskeletal ultrasound and interventions under fluoroscopic guidance
 Fellowship Program Musculoskeletal ultrasound and interventions under fluoroscopic guidance The Montreal University Physical medicine and rehabilitation program offers a 1 year fellowship program. Type
Fellowship Program Musculoskeletal ultrasound and interventions under fluoroscopic guidance The Montreal University Physical medicine and rehabilitation program offers a 1 year fellowship program. Type
Sonography of Intramuscular Myxomas
 Article Sonography of Intramuscular Myxomas The Bright Rim and Bright Cap Signs Gandikota Girish, MBBS, FRCS, FRCR, David A. Jamadar, MBBS, FRCS, FRCR, David Landry, MD, Karen Finlay, MD, Jon A. Jacobson,
Article Sonography of Intramuscular Myxomas The Bright Rim and Bright Cap Signs Gandikota Girish, MBBS, FRCS, FRCR, David A. Jamadar, MBBS, FRCS, FRCR, David Landry, MD, Karen Finlay, MD, Jon A. Jacobson,
Cotswold Diagnostic Clinic Specialist Local Consultant Radiology Reporting Service with Sports Clinic
 Cotswold Diagnostic Clinic Specialist Local Consultant Radiology Reporting Service with Sports Clinic Diagnosis & Treatment of Orthopaedic, Spinal, Rheumatological & Sports conditions Ultrasound Guided
Cotswold Diagnostic Clinic Specialist Local Consultant Radiology Reporting Service with Sports Clinic Diagnosis & Treatment of Orthopaedic, Spinal, Rheumatological & Sports conditions Ultrasound Guided
A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Compliments of: The Central Orthopedic Group
 A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Problems The Central Orthopedic Group 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com
A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Problems The Central Orthopedic Group 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com
Shockwave Therapies for Musculoskeletal Problems Useful Literature
 Shockwave Therapies for Musculoskeletal Problems Useful Literature I have some 1600 references related to shockwave therapy. Those listed below are the main musculoskeletal related papers from 2005-07
Shockwave Therapies for Musculoskeletal Problems Useful Literature I have some 1600 references related to shockwave therapy. Those listed below are the main musculoskeletal related papers from 2005-07
Disclosure. Pre-Procedural Considerations. Transducer Selection. Sterile Procedure. Sterile Procedure. Ultrasound Guided Foot and Ankle Injections
 Ultrasound Guided Foot and Ankle Injections Disclosure No relevant financial relationships exist Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012
Ultrasound Guided Foot and Ankle Injections Disclosure No relevant financial relationships exist Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012
STUDY OF PLATELET RICH PLASMA INJECTIONS IN PATIENTS OF TENDINOPATHY IN SOUTH GUJARAT POPULATION
 ORIGINAL ARTICLE STUDY OF PLATELET RICH PLASMA INJECTIONS IN PATIENTS OF TENDINOPATHY IN SOUTH GUJARAT POPULATION Manish Patel 1, Chintan Sheth 2, Jignesh Patel 1, PrabhavTijoriwala 1 Author s Affiliations:
ORIGINAL ARTICLE STUDY OF PLATELET RICH PLASMA INJECTIONS IN PATIENTS OF TENDINOPATHY IN SOUTH GUJARAT POPULATION Manish Patel 1, Chintan Sheth 2, Jignesh Patel 1, PrabhavTijoriwala 1 Author s Affiliations:
Utility of Ultrasound for Imaging Osteophytes in Patients with Insertional Achilles Tendinopathy
 Digital Commons @ George Fox University Faculty Publications - School of Physical Therapy School of Physical Therapy 2-2015 Utility of Ultrasound for Imaging Osteophytes in Patients with Insertional Achilles
Digital Commons @ George Fox University Faculty Publications - School of Physical Therapy School of Physical Therapy 2-2015 Utility of Ultrasound for Imaging Osteophytes in Patients with Insertional Achilles
Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic 2012 MFMER slide MFMER slide-3
 Ultrasound Foot and Ankle Pathology Disclosures None relevant Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012 MFMER slide-2 Foot and Ankle Fundamentals
Ultrasound Foot and Ankle Pathology Disclosures None relevant Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012 MFMER slide-2 Foot and Ankle Fundamentals
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
A Patient s Guide to Arthroscopy of the Hip
 A Patient s Guide to Arthroscopy of the Hip 6767 Lake Woodlands Drive, Suite F, The Woodlands, TX 77382 20639 Kuykendahl Road, Suite 200, Spring, TX 77379 The Woodlands & Spring, TX. DISCLAIMER: The information
A Patient s Guide to Arthroscopy of the Hip 6767 Lake Woodlands Drive, Suite F, The Woodlands, TX 77382 20639 Kuykendahl Road, Suite 200, Spring, TX 77379 The Woodlands & Spring, TX. DISCLAIMER: The information
Ultrasound Guided Therapeutic Injections in the Treatment of Shoulder Pain: A Multimedia Review
 Ultrasound Guided Therapeutic Injections in the Treatment of Shoulder Pain: A Multimedia Review Poster No.: P-0127 Congress: ESSR 2015 Type: Educational Poster Authors: A. Karsandas, J. Tuckett, R. Sinha,
Ultrasound Guided Therapeutic Injections in the Treatment of Shoulder Pain: A Multimedia Review Poster No.: P-0127 Congress: ESSR 2015 Type: Educational Poster Authors: A. Karsandas, J. Tuckett, R. Sinha,
Anatomy Your shoulder is made up of three bones: your upper arm bone (humerus), your shoulder blade (scapula), and your collarbone (clavicle).
 Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
3/20/2017. Disclosures. Ultrasound Fundamentals. Ultrasound Fundamentals. Bone Anatomy. Tissue Characteristics
 Disclosures Images of ultrasound equipment in this presentation are not an endorsement Fundamentals of Musculoskeletal Ultrasound Physics and Knobology Shane A. Shapiro, M.D. Assistant Professor Orthopedic
Disclosures Images of ultrasound equipment in this presentation are not an endorsement Fundamentals of Musculoskeletal Ultrasound Physics and Knobology Shane A. Shapiro, M.D. Assistant Professor Orthopedic
Trochanteric Bursitis After Total Hip Arthroplasty
 The Journal of Arthroplasty Vol. 25 No. 2 2010 Trochanteric Bursitis After Total Hip Arthroplasty Incidence and Evaluation of Response to Treatment Kevin W. Farmer, MD, Lynne C. Jones, PhD, Kirstyn E.
The Journal of Arthroplasty Vol. 25 No. 2 2010 Trochanteric Bursitis After Total Hip Arthroplasty Incidence and Evaluation of Response to Treatment Kevin W. Farmer, MD, Lynne C. Jones, PhD, Kirstyn E.
ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW
 PRACTICAL ADVICE ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW Written by Akira M. Murakami, USA Ultrasound is a powerful modality for guiding the intra-articular injection of both therapeutic medication
PRACTICAL ADVICE ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW Written by Akira M. Murakami, USA Ultrasound is a powerful modality for guiding the intra-articular injection of both therapeutic medication
MUSCULAR DAMAGE AFTER THA: TRANSGLUTEAL VS ANTERIOR APPROACH
 MUSCULAR DAMAGE AFTER THA: TRANSGLUTEAL VS ANTERIOR APPROACH Fabian Kalberer Department of Orthopedics, Balgrist University of Zurich www.balgrist.ch CHANGING PATIENT S EXPECTATIONS RESIDUAL WEAKNESS,
MUSCULAR DAMAGE AFTER THA: TRANSGLUTEAL VS ANTERIOR APPROACH Fabian Kalberer Department of Orthopedics, Balgrist University of Zurich www.balgrist.ch CHANGING PATIENT S EXPECTATIONS RESIDUAL WEAKNESS,
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME
 ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Problems
 A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with
A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with
Achilles Tendon Anatomy. Achilles Tendon Anatomy. Acute Achilles Rupture. Acute Achilles Rupture 8/19/14. Primary plantarflexor
 Disclosure Conditions of the Achilles Tendon Brian Clowers, M.D. I have no financial relationships that would influence the content of this presentation Oklahoma Sports and Orthopedic Institute September
Disclosure Conditions of the Achilles Tendon Brian Clowers, M.D. I have no financial relationships that would influence the content of this presentation Oklahoma Sports and Orthopedic Institute September
Hospital NEO,Turku, Finland
 Hamstring syndrome from fibrous band to tendinosis Sakari Orava, Janne Sarimo, Lasse Lempainen, Jyrki Heinänen Hospital NEO,Turku, Finland 1 Hamstring muscles- ANATOMY over two big joints pelvic stabilizers
Hamstring syndrome from fibrous band to tendinosis Sakari Orava, Janne Sarimo, Lasse Lempainen, Jyrki Heinänen Hospital NEO,Turku, Finland 1 Hamstring muscles- ANATOMY over two big joints pelvic stabilizers
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
31yo M with chronic basilar thumb and wrist pain that started after cross-country bicycle ride 5 yrs ago.
 31yo M with chronic basilar thumb and wrist pain that started after cross-country bicycle ride 5 yrs ago. EPL EPB APL Full-thickness tear involving the dorsal deltoid ligament of the first carpometacarpal
31yo M with chronic basilar thumb and wrist pain that started after cross-country bicycle ride 5 yrs ago. EPL EPB APL Full-thickness tear involving the dorsal deltoid ligament of the first carpometacarpal
Lateral epicondylitis, or ``tennis elbow,'' is
 Comparison of Sonography and MRI for Diagnosing Epicondylitis Theodore T. Miller, MD, 1,2 Micheal A. Shapiro, MD, 1,2 Elizabeth Schultz, MD, 1,2 Paul E. Kalish, MD 3 1 Department of Radiology, North Shore
Comparison of Sonography and MRI for Diagnosing Epicondylitis Theodore T. Miller, MD, 1,2 Micheal A. Shapiro, MD, 1,2 Elizabeth Schultz, MD, 1,2 Paul E. Kalish, MD 3 1 Department of Radiology, North Shore
Sonographically Guided Intratendinous Injection of Hyperosmolar Dextrose to Treat Chronic Tendinosis of the Achilles Tendon: A Pilot Study
 Sonographically Guided Achilles Tendon Injection for Tendinosis Musculoskeletal Imaging Original Research Sonographically Guided Intratendinous Injection of Hyperosmolar Dextrose to Treat Chronic Tendinosis
Sonographically Guided Achilles Tendon Injection for Tendinosis Musculoskeletal Imaging Original Research Sonographically Guided Intratendinous Injection of Hyperosmolar Dextrose to Treat Chronic Tendinosis
Clinical diagnosis of hip dysfunction
 Clinical diagnosis of hip dysfunction Trish Wisbey-Roth Specialist Sport Physiotherapist (FACP), Olympic Physio, Masters of Sport Physiotherapy ( AIS/UC) Active Rehabilitation Consultant. Case Study: Jane,
Clinical diagnosis of hip dysfunction Trish Wisbey-Roth Specialist Sport Physiotherapist (FACP), Olympic Physio, Masters of Sport Physiotherapy ( AIS/UC) Active Rehabilitation Consultant. Case Study: Jane,
Class Outline: Posterior Anatomy
 Class Outline: Posterior Anatomy 5 minutes Breath of Arrival and Attendance 5 minutes Howdy Partner 35 minutes Posterior Anatomy using Power Point Presentation 5 minutes Overview of skeletal segments 5
Class Outline: Posterior Anatomy 5 minutes Breath of Arrival and Attendance 5 minutes Howdy Partner 35 minutes Posterior Anatomy using Power Point Presentation 5 minutes Overview of skeletal segments 5
Sonographic Examination of Lateral Epicondylitis
 David Connell 1 Frank Burke Peter Coombes Stephen McNealy Donna Freeman David Pryde Greg Hoy Received July 11, 2000; accepted after revision September 18, 2000. 1 All authors: Department of Radiology,
David Connell 1 Frank Burke Peter Coombes Stephen McNealy Donna Freeman David Pryde Greg Hoy Received July 11, 2000; accepted after revision September 18, 2000. 1 All authors: Department of Radiology,
MRI of Quadratus Femoris Muscle Tear: Another Cause of Hip Pain
 MRI of Quadratus Femoris Muscle Tear Musculoskeletal Imaging Clinical Observations Seth D. O Brien 1 Liem T. Bui-Mansfield 1,2,3 O Brien SD, Bui-Mansfield LT Keywords: hip pain, MRI, muscle tear, quadratus
MRI of Quadratus Femoris Muscle Tear Musculoskeletal Imaging Clinical Observations Seth D. O Brien 1 Liem T. Bui-Mansfield 1,2,3 O Brien SD, Bui-Mansfield LT Keywords: hip pain, MRI, muscle tear, quadratus
The psoas minor is medial to the psoas major. The iliacus is a fan-shaped muscle that when contracted helps bring the swinging leg forward in walking
 1 p.177 2 3 The psoas minor is medial to the psoas major. The iliacus is a fan-shaped muscle that when contracted helps bring the swinging leg forward in walking and running. The iliopsoas and adductor
1 p.177 2 3 The psoas minor is medial to the psoas major. The iliacus is a fan-shaped muscle that when contracted helps bring the swinging leg forward in walking and running. The iliopsoas and adductor
Gluteal region DR. GITANJALI KHORWAL
 Gluteal region DR. GITANJALI KHORWAL Gluteal region The transitional area between the trunk and the lower extremity. The gluteal region includes the rounded, posterior buttocks and the laterally placed
Gluteal region DR. GITANJALI KHORWAL Gluteal region The transitional area between the trunk and the lower extremity. The gluteal region includes the rounded, posterior buttocks and the laterally placed
Ricardo E. Colberg, MD, RMSK. PM&R Sports Medicine Physician Andrews Sports Medicine and Orthopedic Center American Sports Medicine Institute
 Ricardo E. Colberg, MD, RMSK PM&R Sports Medicine Physician Andrews Sports Medicine and Orthopedic Center American Sports Medicine Institute Pathophysiology of chronic orthopedic injuries Definition of
Ricardo E. Colberg, MD, RMSK PM&R Sports Medicine Physician Andrews Sports Medicine and Orthopedic Center American Sports Medicine Institute Pathophysiology of chronic orthopedic injuries Definition of
MRI of the Hip. Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
 MRI of the Hip Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Take Home Points Joint effusion: does not collect dependently Imaging
MRI of the Hip Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Take Home Points Joint effusion: does not collect dependently Imaging
