L. J. PROBYN, 1 J. S. WUNDER, 1,2 R. S. BELL, 1,2 A. M. GRIFFIN 1 & A. M. DAVIS 1,3. Sarcoma (1998) 2, 163± 170 O RIGINAL ARTIC LE
|
|
|
- Leonard Byrd
- 6 years ago
- Views:
Transcription
1 Sarcoma (1998) 2, 163± 170 O RIGINAL ARTIC LE A com parison of outcom e of osteoarticular allograft reconstruction and shoulder arthrodesis following resection of prim ary tum ours of the proxim al humerus L. J. PROBYN, 1 J. S. WUNDER, 1,2 R. S. BELL, 1,2 A. M. GRIFFIN 1 & A. M. DAVIS 1,3 1 University M usculoskeletal Oncology Unit, M ount Sinai Hospital & 2 Department of Surgery, University of Toronto & 3 Departments of Physical Therapy and Surgery and Graduate Departments of Rehabilitation Science and Public Health Science, University of Toronto, Toronto, Canada A bstract Purpose. The purpose of this study was to compare the oncologic, reconstructive and functional outcomes of patients who underwent osteoarticular allograft reconstruction with those who underwent arthrodesis for a primary malignant bone tumour of the proximal humerus. Patients. Eleven patients were treated with osteoarticular allograft reconstruction of the proximal humerus. Five of these reconstructions failed, necessitating revision to a secondary arthrodesis. Five patients underwent arthrodesis as a primary reconstruction, for a total of ten patients in the arthrodesis group. M ethods. End points included local and systemic disease recurrence, complications and functional outcome (measured using the 1987 and 1993 Musculoskeletal Tumour Society Rating Scales (MSTS) and the Toronto Extremity Salvage Score (TESS)). Results. One patient died of systemic disease 2 years post-operatively and one patient had an axillary node recurrence resected 10 months post-operatively and remains free of disease 53 months later. The other 14 patients were alive with no evidence of disease at the time of the last follow-up. Complications after the osteochondral allografts (n 5 11) included two infections, four fractures and three subluxations in eight patients. Six of these patients required removal of the allograft; one had a repeat osteochondral allograft and ve were converted to an arthrodesis. Complications after arthrodesis in the ten patients ( ve primary and ve secondary arthrodeses) included two non-unions, one infection and one fracture in three patients. Patients who underwent shoulder arthrodesis scored better in all outcome measures and this was statistically signi cant in the MSTS 1993 (p , Mann± Whitney U Test). D iscussion. In this study, there was a trend towards improved function following arthrodesis compared to osteochondral allograft reconstruction following proximal humerus bone tumour resection. K ey words: sarcoma, proximal humerus, reconstruction, outcom e, function. Introduction Reconstruction of the shoulder following resection of a primary tumour of the proximal humerus is a challenging clinical problem, particularly since the resection may result in de cits of the deltoid, rotator cuff, joint capsule, glenoid and scapula. The reconstructive options following proximal humerus tumour resection include: preservation of a mobile glenohumeral joint using a prosthesis, osteoarticular allograft or an allograft± prosthesis composite; arthrodesis using an allograft or bular transplant; or, a ail joint (Tikhoff± Linberg procedure). 1± 4 W hen suf cient deltoid, rotator cuff and joint capsule can be preserved to power the glenohumeral joint, our group has undertaken reconstruction with osteoarticular allograft. When insuf cient soft tissues remain, we have utilized an allograft arthrodesis. W hen resection of the proximal humerus, glenoid and scapula leaves insuf cient bone stock to permit shoulder fusion, the Tikhoff± Linberg procedure is undertaken to avoid forequarter am putation whenever possible. 5,6 The perceived advantage of an osteoarticular allograft reconstruction compared to shoulder fusion is based on the potential for improved function due to a mobile glenohumeral joint. However, there is often considerable mobility imparted to the upper extremity by the scapulothoracic joint follow ing arthrodesis. There is no inform ation in the literature comparing the results of a mobile shoulder versus Correspondence to: A. M. Davis, Suite 476, Mount Sinai Hospital, 600 University Avenue, Toronto, Canada M5G 1X5. Tel: 1 1 (416) ; Fax: 1 1 (416) ; davis@mshri.on.ca X/98/030163± 08 $9.00 Ó 1998 Carfax Publishing Ltd
2 164 L. J. Probyn et al. arthrodesis reconstruction following proximal humerus tumour resection. The purpose of this study was to compare the oncologic, reconstructive and functional outcomes of patients who underwent osteoarticular allograft reconstruction with those who underwent arthrodesis for a prim ary bone tumour of the proximal humerus. M ethods Patients were eligible for this study if they had resection of a primary bone tumour of the proximal humerus and reconstruction with an osteoarticular allograft or shoulder arthrodesis. All patients had a minimum of two years follow-up from their index surgery. Between 1986 and 1995, eleven patients were identi ed who underwent osteoarticular allograft reconstruction of the proximal humerus. During the sam e period, ten patients underwent shoulder arthrodesis. Five of these ten were initially treated with an osteoarticular allograft that subsequently failed. These ve patients underwent arthrodesis as a secondary procedure. All patients underwent clinical, radiographical (computerized tomography in the initial years and then both computerized tomography and magnetic resonance imaging in the latter years), and pathological staging prior to surgery. All resections were classi ed according to the system of the M usculoskeletal Tumour Society. 7 If the abductor mechanism (deltoid and rotator cuff) was intact following tumour resection, the case was denoted with an A, or a B if the abductor mechanism was disrupted. All of the osteoarticular allografts were classi ed as S345A. At least a portion of the deltoid was disrupted in all of these cases but the rotator cuff remained intact. All of the primary arthrodeses (that is, arthrodeses done immediately following tumour resection, rather than to salvage a failed osteochondral allograft reconstruction) were classi ed as S345B and had resection of their rotator cuff and joint capsule as well as the deltoid. be preserved. The patients undergoing Tikhoff± Linberg procedures were not included in this study. Osteoarticular allograft An osteoarticular allograft of appropriate size (size match performed using standardized radiographs) was chosen from the bone bank prior to surgery. All allografts were harvested and stored according to the standards of the American Association of Tissue Bank 8 and all grafts were treated with 2.5 megarads of radiation following harvest. Osteoarticular allografts were thawed in the operating room and cut to t the humeral defect. Prior to xing the allograft to host humerus, a rotator cuff repair was performed Reconstructive procedures Tumour resection was performed following accepted oncologic principles aim ing for negative operative margins. The status of the abductor mechanism was the most important factor in selecting the reconstruction method. 4 An osteoarticular allograft was performed if the rotator cuff and capsule (and rarely the deltoid) were intact, and an arthrodesis was performed if the rotator cuff, capsule and/or glenoid surface were resected (Figs 1 and 2). If there was involvement of the scapula including the glenoid with or without the proximal humerus, a Tikhoff± Linberg procedure was performed providing the neurovascular structures could Fig. 1. Anteroposterior plain radiograph of a 35-year-old man 4.5 years post-osteochondral allograft of the shoulder for a grade 2 chondrosarcoma.
3 Proxim al humeral osteoarticular allografts versus arthrodeses 165 Fig. 2. Plain radiograph 2 years following allograft arthrodesis for a grade 1 chondrosarcoma in a 19-year-old woman. between the host and the allograft tendons using non-absorbable sutures. A stable repair of the rotator cuff was achieved in all cases. Fixation of the allograft to host humerus was then perform ed using a dynam ic compression plating technique. Autograft from the iliac crest was placed around the osteotomy site in eight of the eleven cases. The insertions of the latissimus dorsi and pectoralis major muscles were repaired to the corresponding areas on the allograft if possible. The biceps, brachialis and triceps were advanced for soft tissue coverage of the allograft. Arthrodesis Eight of the eleven arthrodeses performed in ten patients were achieved using allograft. The allograft was prepared by osteotomizing the articular surface so that the remaining humeral head was congruent with the glenoid and acromion at thirty degrees exion, thirty degrees of abduction and thirty degrees of internal rotation. 9,10 Soft tissues and cartilage were cleaned from the under-surface of the acromion. A very long (18± 26 hole) 4.5 mm broad plate was contoured to lie along the spine of the scapula, over the acromion and down along the allograft onto the patient s remaining distal humerus. Interfragmentary compression screws were used following provisional stabilization with K-w ires and passed through the plate and allograft, obtaining purchase into the glenoid and neck of scapula. Further interfragmentary screws were then passed through the acromion into the graft to achieve rm contact with the superior portion of the allograft humeral head. A dynamic compression plating technique was then used to stabilize the distal osteotomy between the allograft and the host humerus. Neutralization of the reconstruction was accomplished by insertion of screws through the plate into the allograft and the scapular spine. Iliac crest bone graft was packed around the proximal and distal osteotomies. Three arthrodeses were performed using a vascularized bular graft instead of an allograft as each of these had developed an infection; two following an osteoarticular allograft (Fig. 3) and one following an allograft arthrodesis. The infections were treated in a two-stage process with removal of the allograft and replacement with a cement spacer until the infection cleared and then subsequent arthrodesis with the vascularized bular graft. A broad plate was contoured along the spine of the scapula to the distal humerus. A microvascular bula was harvested and a hole was ream ed in the glenoid where the bular graft was slotted into place. The distal humerus was also reamed and the bula was inserted about 2± 3 cm into the humerus. The bula was held in place proximally by a single screw through the bula into the glenoid. The plate was secured to the bula with screws. The microvascular repair was then performed with an end-to-side repair between the brachial artery and vein and the peroneal artery and vein. Iliac crest bone graft was applied at both anastom osis sites. A latissimus dorsi muscle ap was required in ve of the eleven arthrodesis reconstructions to provide complete soft tissue coverage over the graft site. All patients in the osteoarticular and arthrodesis groups received peri-operative antibiotics and were immobilized in a Velpeau sling for 6 weeks. The osteoarticular allograft patients were started on physiotherapy at 6 weeks post-surgery with shoulder shrugs and active-assisted forward exion exercises. Their rehabilitation program s were progressed as tolerated and according to radiographic evidence of healing. The arthrodesis patients were started on range of motion (ROM ) exercises of the scapulothoracic joint when there was radiographic evidence of healing of the glenoid osteotomy. All patients were
4 166 L. J. Probyn et al. to function (activities of daily living, ADLs, leisure activities, work, and pain levels. Results Oncologic results Fig. 3. Plain radiograph of a vascularized bular graft arthrodesis 3 years after surgery to revise an infected osteoarticular allograft. started on early gentle ROM exercises of the elbow, wrist and hand. Demographic, oncological outcome, treatment complication and functional data at most recent follow-up were collected for all patients. Function was recorded using the M usculoskeletal Tumour Society Rating Scale, 1987 version (MSTS, 1987), 11 the M usculoskeletal Tumour Society Rating Scale, 1993 version (MSTS, 1993), 12 and the Toronto Extremity Salvage Score (TESS). 13 The functional data of the six patients, who had an osteoarticular allograft (without revision to an arthrodesis), were compared to the 10 patients who had an arthrodesis using non-param etric statistics. The ve patients who had a primary osteoarticular allograft and went on to a secondary arthrodesis were interviewed and asked speci c questions comparing the two different types of surgery with respect There were seven males and four females who underwent an osteochondral allograft, and their average age at surgery was 34 years (range, 10± 78 years). Seven of the patients had osteosarcoma (two IB parosteal and ve IIB central osteosarcomas) and four of the patients had chondrosarcoma (all IIB lesions). 14 Three males and seven females underwent an arthrodesis ( ve of the ten after failed osteoarticular allograft reconstruction). The average age at surgery was 22 years (range, 12± 35 years). Of the ve patients undergoing prim ary arthrodesis immediately after tumour removal, three had a IIB osteosarcoma, one a IB malignant giant cell tumour and one a IB chondrosarcoma. Table 1 summarizes the results. The average length of bone resection was similar for the osteoarticular allograft and arthrodesis groups, 15.2 cm (range, 7.3± 25 cm) and 17.3 cm (range, 7.5± 25 cm) respectively. Adjuvant treatment varied depending on the grade and stage of the tumour. For the osteochondral allografts, six of eleven patients received chemotherapy. For the primary arthrodesis group, three of ve patients received chemotherapy. None of the patients in the study was treated with radiotherapy. Nine of the patients undergoing osteoarticular allografts had negative margins and two patients had positive microscopic margins. Four of the ve patients undergoing prim ary arthrodesis had negative margins and one patient had positive microscopic margins. At the time of the last follow-up, all of the patients who had an osteochondral allograft were alive with no evidence of disease. One patient with osteosarcoma treated with an osteoarticular allograft (negative margin surgery at initial operation) developed a high axillary nodal recurrence ten months after initial resection. Fifty-three months after wide resection of this nodal recurrence, the patient remains disease-free. One osteosarcoma patient treated by arthrodesis developed lung and pelvic metastases eight months post-operatively and died of disease at two years. This patient had positive resection margins at the time of surgery but did not develop a local recurrence. The other patients reconstructed by arthrodesis were alive with no evidence of disease. Reconstructive results Of the eleven patients who had an osteoarticular allograft, ve patients required revision, all to a glenohumeral arthrodesis. Two of these patients sustained late infections (greater than six months
5 Proxim al humeral osteoarticular allografts versus arthrodeses 167 Fig. 4. Plain radiograph showing an atraumatic fracture of an osteoarticular allograft 6 years post-operatively. post-surgery) and underwent staged salvage procedures with removal of the osteochondral graft, implantation of an antibiotic cement spacer and subsequent reconstruction using a vascularized bula. Two patients with painful subluxation of the shoulder and one patient with an osteoarticular allograft fracture were also revised to an allograft arthrodesis. The length of time between the osteochondral allograft and the arthrodesis varied from 12 to 81 months (average 48.6 months). Of the remaining six patients with osteochondral allografts, one patient developed an inferior dislocation of the allograft four months post-operatively. This was stable and the patient did not want further treatment despite limited glenohumeral motion. One patient sustained a fracture of the allograft after a fall and required replacement of the graft while two patients developed a fracture of the allograft without trauma. In one of these two patients, atraumatic fracture resulted in formation of callus around the allograft fracture site with eventual stabilization of the fracture, while the second patient is presently aw aiting revision. Two patients have not had speci c complications although one of these patients has moderate to severe shoulder pain but does not wish to undergo further surgery. Of the ve patients who had a primary arthrodesis, four patients have had no complications. One patient had a fracture of the allograft and developed chronic infection which was treated with a cement spacer and eventual microvascular bular graft arthrodesis. Of the ve patients who had a secondary arthrodesis, three patients have had no complications. Two patients sustained non-unions which healed after repeat bone grafting. Functional data were availab le for all but one patient with an osteoarticular allograft who did not return for follow-up assessm ent. M ean follow-up time was 45.6 months (range, 24± 81 months) for the osteochondral allografts and 48.6 months (range, 24± 132 months) for the arthrodesis patients. Patients with a shoulder arthrodesis scored better in all outcome measures. The mean scores for osteochondral allografts and arthrodeses, respectively, for the M STS 1987 was 19.3 (range, 7± 27) and 21.1 (range, 17± 25), for the M STS 1993 was 50 (range, 36± 70) and 68.2 (range, 53± 80) and for the TESS score was 74 (range, 39± 95) and 78.5 (range, 42± 98). This difference was statistically signi cant only in the MSTS 1993 (p , M ann± Whitney U) favouring improved function in the arthrodesis group. The active range of motion achieved by the two groups was especially striking. For all but one patient who experienced chronic, debilitating pain from an unstable osteoarticular reconstruction and continued to experience som e pain following conversion to an arthrodesis, patients with an arthrodesis had better active forward exion (range 45± 85) than any patient with an osteoarticular allograft (range 30± 70). This was re ected in the M STS 1987 range of motion ratings in which no patient with an osteoarticular allograft received more than one of ve points whereas eight of the ten patients in the arthrodesis group ( ve prim ary and ve secondary arthrodeses) received three of ve points for range of motion. The subjective description of the comparison of the osteochondral allograft versus the arthrodesis from the ve patients undergoing both surgeries seemed to support the trend favouring arthrodesis (see Table 2). Increased stability was noted after the fusion. The pain was also reported as the sam e or better after arthrodesis. D iscussion It has been well documented that limb-salvage surgery for tumours of the shoulder is an alternative to amputation. 4 Careful performance of the biopsy, the use of neoadjuvant chemotherapy when indicated and proper attention to complete surgical resection of the tumour are essential in permitting limb salvage without comprom ising tumour control. Successful local resection, avoiding am putation while controlling sarcoma, is demonstrated by the
6 168 L. J. Probyn et al. Table 1. Sample characteristics and outcom es Osteochondral Arthrodesis allograft* n 5 primary n 11 n 5 secondary Age (years) mean 33.6, sd 21.5 mean 22.4, sd 8.5 Gender Male 7 3 Female 4 7 Pathology Osteosarcoma 7 7 Chondrosarcoma 4 2 Giant cell tumour 0 1 Adjuvant Rx None 5 6 Pre-op chemo 1 0 Post-op chemo 3 0 Pre & Post-op chemo 2 4 Margins Negative 9 9 Positive 2 1 Bone resection (cm) mean 15.2, sd 4.5 mean 17.3, sd 5.1 Complications Non-union 0 2 Infection 2 1 Fracture 4 1 Subluxation/instability 3 0 Functional outcome MSTS 1987 mean 19.3, sd 6.1 mean 21.1, sd 2.4 MSTS 1993 mean 50.0,sd 9.8 mean 68.2, sd 7.7 TESS mean 74.0, sd 23.5 mean 78.5, sd 19.2 Follow-up mean 45.6,sd 20.6 mean 48.6, sd 39.0 *Five patients with osteoarticular allografts were complications. converted to arthodesis due to fact that there was only one nodal recurrence and one system ic relapse in the patients in this study. H owever, the choice of the best limb-reconstruction method for tumours of the proximal humerus is a dif cult clinical decision. In this study, patients were selected for osteoarticular allograft reconstruction when suf cient abductor musculotendinous tissue remained to provide a stable soft tissue repair to the rotator cuff and tendon of the allograft. Fusion was undertaken when the osteoarticular allograft failed due to infection, instability or fracture, or if the glenoid bone stock or soft tissues after resection were insuf cient to reconstruct a stable, mobile shoulder. In both of these types of reconstructions, complications were frequent and serious. In the osteoarticular group, ve have been revised to an arthrodesis: two for infection, two for instability and one for fracture. In the remaining six patients, three further fractures were documented (one requiring allograft replacement and one for which revision surgery is still pending), one patient dislocated the shoulder and one patient has chronic pain of moderate intensity. In comparison, three of the ten arthrodeses were complicated by non-union requiring repeat bone grafting (n 5 2) and fracture/infection requiring a staged microvascular bula arthrodesis. The rates and types of complications experienced by both the osteoarticular allograft and arthrodesis patients in this study are similar to those reported by other authors. Gebhardt et al. 2 reported four complications in three of seven patients undergoing shoulder arthrodesis. These included a wound slough, median nerve palsy and two patients with prominent hardware. Layton et al. 15 reported on nine patients treated by shoulder arthrodesis. Two patients died of metastases prior to healing of the arthrodesis and there were complications consisting of infection and fracture in four of the remaining seven patients. 15 Gebhardt et al. 3 also reported on twenty patients who underwent osteoarticular allograft of the proximal humerus. In this group, one had a non-union, four fractured and three became infected. 3 O Connor et al. 4 reported osseous union in all eight patients treated with osteoarticular allograft, but four of these patients suffered collapse and fracture of the subchondral region of the allograft. A further patient suffered a fracture and required revision to a second osteoarticular allograft. In the same study, ten patients treated by arthrodesis developed one infection and two stress fractures. 4 In the present study, the arthrodesis patients tended to have higher scores on all functional measures although only the M STS 1993 demonstrated a
7 Proximal humeral osteoarticular allografts versus arthrodeses 169 Table 2. Summary of responses by subjects undergoing shoulder fusion following complications for osteochrondral allograft Case 1. When you were the 2. Are there any 3. Aside from any 4. If you had 5. Why? most functional after activities that you were complications the option of either the able to do after one of (fracture, having only osteochrondral the surgeries but not the subluxation, one of the two allograft or the fusion, other (not including any infection), how did sugeries after which surgery restrictions that the the level of pain again, which would you say that doctor gave you)? compare after each of would you your function was the surgeries? choose? better (with respect to ADLs, leisure activities, work)? 1 fusion, because of increased ROM able to golf, swim, waterski after fusion the same up until the fusion because it is more (70% compared to 45% of not working, looking after 1 1/2 year complications stable, and I am able to shoulder exion) old child do more activities 2 fusion, because my arm feels more can do all the same things (read, walk), much better after the fusion, had fusion because my arm is like my own (more stable) and not doesn t do any sports (never has) severe pain after the allograft more stable, and feels an extra appendage, although I have works at desk job, uses arm rest for (even before she had the problems more like my own about the same movement arm with subluxation) 3 osteochondral allograft, because I was able to eat better after the about the same (hard to allograftð if it was in because the had better movement osteochondral allograft, because of remember) right arm (dominant movement was better better movement, I could bring my arm) hand to my mouth better (although my movement is improving, and fusionð in the left arm because it still I am getting better at it) (which he had) functions O.K. other activities about the same (now plays hockey (non-contact), races cars, rides bike, has own business in lawn care) 4 difficult to tell because of all the the same(slight increased ROM after minimal pain after both surgeries fusion because the slight complications with the allograft the allograft) although ROM the same increased ROM didn t fracture and infection), but it in forward flexion (80%) after both outweigh the was about the same after both, complications, but if I although my arm feels as though didn t have those, then it is improving. likely the allograft 5 function is about the same although the same worse after osteochondral fusion because the pain is the circulation to the arm seems to allograft, even before the better be better after the fusion complications happened
8 170 L. J. Probyn et al. statistically signi cant difference between the two clinical groups. The M STS 1987 and the TESS showed only a trend toward improved function in the arthrodesis group. The lack of statistical signi cance in these two functional measures must be considered in view of the sm all numbers of patients in each treatment group as well as the differences in the measures. The M STS 1987 looks at items that are likely to have low scores in both groups (i.e. range of motion, strength, deform ity). Four of the six items of the M STS 1993 are more likely to vary am ongst the two groups. These are pain, function, emotional acceptance and lifting ability, which were generally higher in the arthrodesis patients than the osteochondral allograft patients. There was less of a difference in hand positioning and dexterity. W ith regards to the TESS scores, most of the patients in both groups were clustered around the mid to high range. This means that all of the patients were able to do basic activities of daily living (eating, bathing, grooming) but experienced dif culty perform ing high-level activities such as sports, work, endurance and leisure activities. M ost of these patients also classi ed themselves as `somewhat disabled. Although the number of patients in the study was relatively small and ve of the patients were in both groups, there is a trend towards improved function after an arthrodesis compared to an osteochondral allograft. Subjective comparison also favoured the arthrodesis. These results are sim ilar to those of O Connor in which patients treated with primary arthrodesis had higher M STS 1993 scores than those reconstructed with osteoarticular allografts. 4 The arthrodesis provides a stable shoulder girdle with motion of the scapulothoracic joint to position the arm in space. 2 Subjective responses from patients in this study indicated a feeling of increased stability and decreased pain after an arthrodesis compared to an osteochondral allograft. These qualitative responses were obtained from patients who had undergone both procedures due to complications from an osteoarticular allograft and were based on patients remembering their `best function after their osteoarticular allograft. These results must be interpreted cautiously and in recognition of all the biases imposed in the method. It is recognized that this study did not include patients with a prosthesis or allograft± prosthesis composite as these reconstructive techniques have not been utilized around the shoulder by our group. Recent work by O Connor et al. 4, however, suggests that the complications and function in patients reconstructed with a prosthesis or allograft± prosthesis composite provides inferior results when compared to an osteochondral allograft or arthrodesis. In conclusion, complications seemed to be more apparent in patients undergoing osteoarticular allograft. Patients treated with shoulder arthrodesis tended to have better functional scores. References 1 Frassica FJ, Sim FH, Chao EY. Primary malignant bone tumours of the shoulder girdle: Surgical technique of resection and reconstruction. Am Surg 1987; 53(5); 264± 9. 2 Gebhardt MC, McGuire MH, Mankin HJ. Resection and allograft arthrodesis for malignant bone tumours of the extremity. In: Enneking WF, ed. Limb salvage in musculoskeletal oncology. New York: Churchill Livingston, 1987; 567± Gebhardt MC, Roth YF, and Mankin HJ. Osteoarticular allografts for reconstruction in the proximal part of the humerus after excision of a musculoskeletal tumour. J Bone Joint Surg [Am] 1990; 72-A; 334± O Connor MI, Sim FH, Chao EYS. Limb salvage for neoplasms of the shoulder girdle. J Bone Joint Surg [Am] 1996; 78-A; 1872± Malawer MM, Sugarbaker PH, Lampert M, et al. The Tikhoff± Linberg procedure: report of ten patients and presentation of a modi ed technique for tumours of the proximal humerus. Surgery 1985; 97(5); 518± Malawer MM. Tumours of the shoulder girdle. Technique of resection and description of a surgical classi cation. Clin Orthop 1991; 22(1); 7± Enneking WF, Dunham W, Gebhardt M, Malawer M, Pritchard D. A system for the classi cation of skeletal resections. Chir Og M ov 1990; 75(Suppl. 1); 217± Friedlaender GE, Mankin HJ, Sell KW. Osteochondral allografts. Biology, banking and clinical applications. Boston: Little Brown and Company, Hawkins RJ, Neer CS. A functional analysis of shoulder fusions. Clin Orthop 1987; 223; 65± Richards RR, Sherman RM, Hudson AR, Waddell JP. Shoulder arthrodesis using a pelvic-reconstruction plate. A report of eleven cases. J Bone Joint Surg [Am] 1988; 70-A; 416± Enneking WF. Modi cation of the system for functional evaluation in the surgical management of musculoskeletal tumours. In: Enneking WF ed. Limb salvage in musculoskeletal oncology. New York: Churchill Livingston, 1987; 626± Enneking WF, Dunham W, Gebhardt MC, et al. A system for the functional evaluation of reconstructive procedures after surgical treatment of tumours of the musculoskeletal system. Clin Orthop 1993; 286; 24± Davis AM, Wright JG, Williams JE, et al. Development of a measure of physical function for patients with bone and soft tissue sarcoma. Quality of Life Research 1996; 5; 508± Enneking WF, Spanier SS, Goodman MA. A system for the surgical staging of musculoskeletal sarcoma. Clin Orthop 1980; 153; 106± Layton T, Scarborough M, Vander Griend, RA. Allograft arthrodesis of the shoulder following resection of the proximal humerus. Contem porary Orthopaedics 1994; 29(6); 421± 26.
9 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Growth in the lower lim b following chem otherapy for a malignant prim ary bone tumour: a straight-line graph
 Sarcoma (1997) 1, 75± 77 O RIGINAL ARTIC LE Growth in the lower lim b following chem otherapy for a malignant prim ary bone tumour: a straight-line graph PAUL COOL, M ARK D AVIES, ROB J. GRIM ER, SIM ON
Sarcoma (1997) 1, 75± 77 O RIGINAL ARTIC LE Growth in the lower lim b following chem otherapy for a malignant prim ary bone tumour: a straight-line graph PAUL COOL, M ARK D AVIES, ROB J. GRIM ER, SIM ON
Functional outcom e in sarcom as treated with lim b-salvage surgery or am putation
 1357-714 X/98/040019± 05 Ó 1998 Carfax Publishing Ltd Sarcoma (1998) 2, 19± 23 O RIGINAL ARTIC LE Functional outcom e in sarcom as treated with lim b-salvage surgery or am putation RIKKE JO HAN SEN, OLE
1357-714 X/98/040019± 05 Ó 1998 Carfax Publishing Ltd Sarcoma (1998) 2, 19± 23 O RIGINAL ARTIC LE Functional outcom e in sarcom as treated with lim b-salvage surgery or am putation RIKKE JO HAN SEN, OLE
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
BONE TRANSPLANTATION IN LIMB SAVING SURGERIES: THE PHILIPPINE EXPERIENCE
 BONE TRANSPLANTATION IN LIMB SAVING SURGERIES: THE PHILIPPINE EXPERIENCE EDWARD HM WANG, MD UP-Musculoskeletal Tumor Unit and Tissue & Bone Bank Dept. of Orthopedics University of the Philippines-Philippine
BONE TRANSPLANTATION IN LIMB SAVING SURGERIES: THE PHILIPPINE EXPERIENCE EDWARD HM WANG, MD UP-Musculoskeletal Tumor Unit and Tissue & Bone Bank Dept. of Orthopedics University of the Philippines-Philippine
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
Objectives. Limb salvage surgery. Age distribution bone cancer. Age distribution soft tissue sarcomas
 LifeSource October, 2011 Disclosure Information Putting humpty dumpty back together again is easier with tissue allografts! Limb Salvage Surgery for Bone Tumors Edward Cheng, MD October 6, 2011 Disclosure
LifeSource October, 2011 Disclosure Information Putting humpty dumpty back together again is easier with tissue allografts! Limb Salvage Surgery for Bone Tumors Edward Cheng, MD October 6, 2011 Disclosure
Recurrent Shoulder Dislocation.
 Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Utilitarian Shoulder Approach for Malignant. tumor resection.
 Utilitarian Shoulder Approach for Malignant Tumor Resection James C. Wittig, MD* Jacob Bickels, MDt Felasfa Wodajo, MDT Kristen L. Kellar-Graney, BS$ Isaac Meller, MDt Martin M. Malawer, MDT Malignant
Utilitarian Shoulder Approach for Malignant Tumor Resection James C. Wittig, MD* Jacob Bickels, MDt Felasfa Wodajo, MDT Kristen L. Kellar-Graney, BS$ Isaac Meller, MDt Martin M. Malawer, MDT Malignant
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES. Clavicle fractures Proximal head of humerus fractures
 REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Shoulder Labral Tear and Shoulder Dislocation
 Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Anterior Stabilization of the Shoulder: Latarjet Protocol Dr. Abigail R. Hamilton, M.D. Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation.
Anterior Stabilization of the Shoulder: Latarjet Protocol Dr. Abigail R. Hamilton, M.D. Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation.
The Shoulder Complex. Anatomy. Articulations 12/11/2017. Oak Ridge High School Conroe, Texas. Clavicle Collar Bone Scapula Shoulder Blade Humerus
 The Shoulder Complex Oak Ridge High School Conroe, Texas Anatomy Clavicle Collar Bone Scapula Shoulder Blade Humerus Articulations Sternoclavicular SC joint. Sternum and Clavicle. Acromioclavicular AC
The Shoulder Complex Oak Ridge High School Conroe, Texas Anatomy Clavicle Collar Bone Scapula Shoulder Blade Humerus Articulations Sternoclavicular SC joint. Sternum and Clavicle. Acromioclavicular AC
Orthopedics - Dr. Ahmad - Lecture 2 - Injuries of the Upper Limb
 The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
Synthetic Mesh Improves Shoulder Function After Intraarticular Resection and Prosthetic Replacement of Proximal Humerus
 Clin Orthop Relat Res (2015) 473:1464 1471 DOI 10.1007/s11999-015-4139-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Synthetic
Clin Orthop Relat Res (2015) 473:1464 1471 DOI 10.1007/s11999-015-4139-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Synthetic
Shoulder Joint Examination. Shoulder Joint Examination. Inspection. Inspection Palpation Movement. Look Feel Move
 Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing Tumor Resections
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 426, pp. 97 102 2004 Lippincott Williams & Wilkins Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 426, pp. 97 102 2004 Lippincott Williams & Wilkins Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing
Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft
 900 Original Article Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft Ayman Abdelaziz Bassiony, 1 MD Abstract Introduction: Giant
900 Original Article Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft Ayman Abdelaziz Bassiony, 1 MD Abstract Introduction: Giant
 Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Case Report Arthroscopic Bony Bankart Repair Using Double-Threaded Headless Screw: A Case Report
 Case Reports in Orthopedics Volume 2012, Article ID 789418, 4 pages doi:10.1155/2012/789418 Case Report Arthroscopic Bony Bankart Repair Using Double-Threaded Headless Screw: A Case Report Takeshi Kokubu,
Case Reports in Orthopedics Volume 2012, Article ID 789418, 4 pages doi:10.1155/2012/789418 Case Report Arthroscopic Bony Bankart Repair Using Double-Threaded Headless Screw: A Case Report Takeshi Kokubu,
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX Tel#
 Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
 www.fisiokinesiterapia.biz Shoulder Problems Fractures Instability Impingement Miscellaneous Anatomy Bones Joints / Ligaments Muscles Neurovascular Anatomy Anatomy Supraspinatus Anterior Posterior Anatomy
www.fisiokinesiterapia.biz Shoulder Problems Fractures Instability Impingement Miscellaneous Anatomy Bones Joints / Ligaments Muscles Neurovascular Anatomy Anatomy Supraspinatus Anterior Posterior Anatomy
Trapezius transfer in brachial plexus palsy
 Upper limb Trapezius transfer in brachial plexus palsy CORRELATION OF THE OUTCOME WITH MUSCLE POWER AND OPERATIVE TECHNIQUE O. Rühmann, S. Schmolke, M. Bohnsack, J. Carls, C. J. Wirth From Hannover Medical
Upper limb Trapezius transfer in brachial plexus palsy CORRELATION OF THE OUTCOME WITH MUSCLE POWER AND OPERATIVE TECHNIQUE O. Rühmann, S. Schmolke, M. Bohnsack, J. Carls, C. J. Wirth From Hannover Medical
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Fractures of the shoulder girdle, elbow and fractures of the humerus. H. Sithebe 2012
 Fractures of the shoulder girdle, elbow and fractures of the humerus H. Sithebe 2012 Fractures of the Clavicle (mid-shaft). Fractures of the clavicle Fractures of the clavicle Treatment- conservative.
Fractures of the shoulder girdle, elbow and fractures of the humerus H. Sithebe 2012 Fractures of the Clavicle (mid-shaft). Fractures of the clavicle Fractures of the clavicle Treatment- conservative.
(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
Massive Rotator Cuff Tears. Rafael M. Williams, MD
 Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Reverse Total Shoulder Replacement
 Reverse Total Shoulder Replacement Reverse Total Shoulder Replacement is a surgery performed to improve shoulder function and decrease pain. This procedure is performed on patients who have suffered massive
Reverse Total Shoulder Replacement Reverse Total Shoulder Replacement is a surgery performed to improve shoulder function and decrease pain. This procedure is performed on patients who have suffered massive
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Extended Long-Term (5 Years) Outcomes of Triangle Tilt Surgery in Obstetric Brachial Plexus Injury
 Send Orders of Reprints at reprints@benthamscience.net 94 The Open Orthopaedics Journal, 2013, 7, 94-98 Open Access Extended Long-Term (5 Years) Outcomes of Triangle Tilt Surgery in Obstetric Brachial
Send Orders of Reprints at reprints@benthamscience.net 94 The Open Orthopaedics Journal, 2013, 7, 94-98 Open Access Extended Long-Term (5 Years) Outcomes of Triangle Tilt Surgery in Obstetric Brachial
Christopher K. Jones, MD Colorado Springs Orthopaedic Group
 Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
FUNCTIONAL ANATOMY OF SHOULDER JOINT
 FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
OBJECTIVES. Therapists Management of Shoulder Instability SHOULDER STABILITY SHOULDER STABILITY WHAT IS SHOULDER INSTABILITY? SHOULDER INSTABILITY
 Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Case Report Acute Posterior Shoulder Dislocation with Reverse Hill-Sachs Lesion of the Epiphyseal Humeral Head
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 851051, 4 pages doi:10.5402/2011/851051 Case Report Acute Posterior Shoulder Dislocation with Reverse Hill-Sachs Lesion of
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 851051, 4 pages doi:10.5402/2011/851051 Case Report Acute Posterior Shoulder Dislocation with Reverse Hill-Sachs Lesion of
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
Shoulder Biomechanics
 Shoulder Biomechanics Lecture originally developed by Bryan Morrison, Ph.D. candidate Arizona State University Fall 2000 1 Outline Anatomy Biomechanics Problems 2 Shoulder Complex Greatest Greatest Predisposition
Shoulder Biomechanics Lecture originally developed by Bryan Morrison, Ph.D. candidate Arizona State University Fall 2000 1 Outline Anatomy Biomechanics Problems 2 Shoulder Complex Greatest Greatest Predisposition
Clinical Study Distal Femur Allograft Prosthetic Composite Reconstruction for Short Proximal Femur Segments following Tumor Resection
 Advances in Orthopedics Volume 2013, Article ID 397456, 5 pages http://dx.doi.org/10.1155/2013/397456 Clinical Study Distal Femur Allograft Prosthetic Composite Reconstruction for Short Proximal Femur
Advances in Orthopedics Volume 2013, Article ID 397456, 5 pages http://dx.doi.org/10.1155/2013/397456 Clinical Study Distal Femur Allograft Prosthetic Composite Reconstruction for Short Proximal Femur
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
Research Article A Novel Surgical Approach to Lipomatous Tumours of the Deltoid Region
 Sarcoma Volume 2010, Article ID 495834, 4 pages doi:10.1155/2010/495834 Research Article A Novel Surgical Approach to Lipomatous Tumours of the Deltoid Region Emad Al Absi, Tamanna Karim, Nigel Colterjohn,
Sarcoma Volume 2010, Article ID 495834, 4 pages doi:10.1155/2010/495834 Research Article A Novel Surgical Approach to Lipomatous Tumours of the Deltoid Region Emad Al Absi, Tamanna Karim, Nigel Colterjohn,
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Patient Presentation. Prevalence of Rotator Cu Tears. By Derek S. Shia, M.D.
 Rotator Cu Tears By Derek S. Shia, M.D. Rotator cu tears are one of the most common orthopedic problems and e ect more than 17 million persons annually in the United States. The rotator cu is an essential
Rotator Cu Tears By Derek S. Shia, M.D. Rotator cu tears are one of the most common orthopedic problems and e ect more than 17 million persons annually in the United States. The rotator cu is an essential
Acute Management of Shoulder Dislocation. Mr. Paul Halliwell Royal Surrey County Hospital, Guildford.
 Acute Management of Shoulder Dislocation Mr. Paul Halliwell Royal Surrey County Hospital, Guildford. Acute: Injury to rehab. Management: Hx, O/E, x-ray, Rx Shoulder: Glenohumeral Dislocation: Complete
Acute Management of Shoulder Dislocation Mr. Paul Halliwell Royal Surrey County Hospital, Guildford. Acute: Injury to rehab. Management: Hx, O/E, x-ray, Rx Shoulder: Glenohumeral Dislocation: Complete
Chondrosarcoma with a late local relapse
 Chondrosarcoma with a late local relapse J. Shinoda, T. Ozaki, T. Oka, T. Kunisada, H. Inoue Department of Orthopaedic Surgery, Okayama University Medical School, Okayama, 700-8558, Japan Correspondence:
Chondrosarcoma with a late local relapse J. Shinoda, T. Ozaki, T. Oka, T. Kunisada, H. Inoue Department of Orthopaedic Surgery, Okayama University Medical School, Okayama, 700-8558, Japan Correspondence:
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty
 Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
Total Shoulder Arthroplasty
 1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol:
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Longitudinal growth following treatm ent for osteosarcom a
 1357-714 X/98/020115± 05 Ó 1998 Carfax Publishing Ltd Sarcoma (1998) 2, 115± 119 O RIGINAL ARTIC LE Longitudinal growth following treatm ent for osteosarcom a W. PAUL COOL, ROBERT J. GRIM ER, SIMON R.
1357-714 X/98/020115± 05 Ó 1998 Carfax Publishing Ltd Sarcoma (1998) 2, 115± 119 O RIGINAL ARTIC LE Longitudinal growth following treatm ent for osteosarcom a W. PAUL COOL, ROBERT J. GRIM ER, SIMON R.
Excision arthroplasty following shoulder replacement
 Acta Orthop. Belg., 2011, 77, 448-452 ASPECT OF CURRENT MANAGEMENT Excision arthroplasty following shoulder replacement Charalambos P. CHARALAMBOUS, Shivappa SAIDAPUR, Farhan ALVI, John HAINES, Ian TRAIL
Acta Orthop. Belg., 2011, 77, 448-452 ASPECT OF CURRENT MANAGEMENT Excision arthroplasty following shoulder replacement Charalambos P. CHARALAMBOUS, Shivappa SAIDAPUR, Farhan ALVI, John HAINES, Ian TRAIL
JMSCR Vol 06 Issue 12 Page December 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.140 A Case Report of Recurrent
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.140 A Case Report of Recurrent
Shoulder Impingement Rehabilitation Recommendations
 Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
Laura M. Fayad, MD. Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University
 Society of Pediatric Radiology, May 2013 Laura M. Fayad, MD Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University Describes surgical techniques that resect and reconstruct
Society of Pediatric Radiology, May 2013 Laura M. Fayad, MD Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University Describes surgical techniques that resect and reconstruct
SHOULDER JOINT ANATOMY AND KINESIOLOGY
 SHOULDER JOINT ANATOMY AND KINESIOLOGY SHOULDER JOINT ANATOMY AND KINESIOLOGY The shoulder joint, also called the glenohumeral joint, consists of the scapula and humerus. The motions of the shoulder joint
SHOULDER JOINT ANATOMY AND KINESIOLOGY SHOULDER JOINT ANATOMY AND KINESIOLOGY The shoulder joint, also called the glenohumeral joint, consists of the scapula and humerus. The motions of the shoulder joint
Returning the Shoulder Back to Optimal Function. Scapula. Clavicle. Humerus. Bones of the Shoulder (Osteology) Joints of the Shoulder (Arthrology)
 Returning the Shoulder Back to Optimal Function Sternum Clavicle Ribs Scapula Humerus Bones of the Shoulder (Osteology) By Rick Kaselj Clavicle Scapula Medial Left Anterior Clavicle Inferior View 20 degree
Returning the Shoulder Back to Optimal Function Sternum Clavicle Ribs Scapula Humerus Bones of the Shoulder (Osteology) By Rick Kaselj Clavicle Scapula Medial Left Anterior Clavicle Inferior View 20 degree
I have no relevant disclosures pertaining to this talk.
 Bryan Houseman, D.O., ATC Orthopaedic Trauma and Fracture Surgeon New Hampshire Orthopaedic Center September 10, 2016 I have no relevant disclosures pertaining to this talk. From Rockwood & Green, 8 th
Bryan Houseman, D.O., ATC Orthopaedic Trauma and Fracture Surgeon New Hampshire Orthopaedic Center September 10, 2016 I have no relevant disclosures pertaining to this talk. From Rockwood & Green, 8 th
SHOULDER ARTHROPLASTY (TOTAL, HEMI, REVERSE)/ARTHRODESIS
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Joint G*H. Joint S*C. Joint A*C. Labrum. Humerus. Sternum. Scapula. Clavicle. Thorax. Articulation. Scapulo- Thoracic
 A*C Joint Scapulo- Thoracic Articulation Thorax Sternum Clavicle Scapula Humerus S*C Joint G*H Joint Labrum AC Ligaments SC Ligaments SC JOINT AC Coracoacromial GH GH Ligament Complex Coracoclavicular
A*C Joint Scapulo- Thoracic Articulation Thorax Sternum Clavicle Scapula Humerus S*C Joint G*H Joint Labrum AC Ligaments SC Ligaments SC JOINT AC Coracoacromial GH GH Ligament Complex Coracoclavicular
Result of extracorporeal irradiation and re-implantation for malignant bone tumors: A review of 30 patients
 bs_bs_banner Asia-Pacific Journal of Clinical Oncology 2012 doi: 10.1111/ajco.12036 ORIGINAL ARTICLE Result of extracorporeal irradiation and re-implantation for malignant bone tumors: A review of 30 patients
bs_bs_banner Asia-Pacific Journal of Clinical Oncology 2012 doi: 10.1111/ajco.12036 ORIGINAL ARTICLE Result of extracorporeal irradiation and re-implantation for malignant bone tumors: A review of 30 patients
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Clinical Study Primary Malignant Tumours of Bone Following Previous Malignancy
 Sarcoma Volume 2008, Article ID 418697, 4 pages doi:10.1155/2008/418697 Clinical Study Primary Malignant Tumours of Bone Following Previous Malignancy J. T. Patton, S. M. M. Sommerville, and R. J. Grimer
Sarcoma Volume 2008, Article ID 418697, 4 pages doi:10.1155/2008/418697 Clinical Study Primary Malignant Tumours of Bone Following Previous Malignancy J. T. Patton, S. M. M. Sommerville, and R. J. Grimer
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Surgical. Technique. AEQUALIS Spherical Base Glenoid. Shoulder Prosthesis.
 Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Why are these shoulder replacements called a reverse prosthesis?
 PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Latissimus Dorsi Transfer
 Latissimus Dorsi Transfer 1. Defined a. Transfer of the latissimus dorsi from it insertion anteriorly on the proximal humeral shaft to a superior and posterior insertion on the humeral head in the subacromial
Latissimus Dorsi Transfer 1. Defined a. Transfer of the latissimus dorsi from it insertion anteriorly on the proximal humeral shaft to a superior and posterior insertion on the humeral head in the subacromial
Patient ID. Case Conference. Physical Examination. Image examination. Treatment 2011/6/16
 Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
Les séquelles traumatiques. Ph. Valenti, J. Kany, D. Katz
 Indications et Techniques Les séquelles traumatiques Ph. Valenti, J. Kany, D. Katz Paris Shoulder Unit Clinique Bizet (Paris, France) Disclosures Arthroplasty Consultant : FH orthopaedics receive royalties
Indications et Techniques Les séquelles traumatiques Ph. Valenti, J. Kany, D. Katz Paris Shoulder Unit Clinique Bizet (Paris, France) Disclosures Arthroplasty Consultant : FH orthopaedics receive royalties
The Upper Limb II. Anatomy RHS 241 Lecture 11 Dr. Einas Al-Eisa
 The Upper Limb II Anatomy RHS 241 Lecture 11 Dr. Einas Al-Eisa Sternoclavicular joint Double joint.? Each side separated by intercalating articular disc Grasp the mid-portion of your clavicle on one side
The Upper Limb II Anatomy RHS 241 Lecture 11 Dr. Einas Al-Eisa Sternoclavicular joint Double joint.? Each side separated by intercalating articular disc Grasp the mid-portion of your clavicle on one side
The Shoulder. Anatomy and Injuries PSK 4U Unit 3, Day 4
 The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
WHAT YOU IS BACK WITHIN ARM S REACH
 YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
Biomechanical concepts of total shoulder replacement. «Shoulder Course» Day 1. Richard W. Nyffeler Orthopädie Sonnenhof Bern. 11. Sept.
 Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
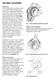 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture Dislocation of the Elbow in an Adult
 Hindawi Case Reports in Orthopedics Volume 2018, Article ID 5401634, 6 pages https://doi.org/10.1155/2018/5401634 Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture
Hindawi Case Reports in Orthopedics Volume 2018, Article ID 5401634, 6 pages https://doi.org/10.1155/2018/5401634 Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture
UPPER EXTREMITY INJURIES. Recognizing common injuries to the upper extremity
 UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
Clinical Study The Use of Massive Endoprostheses for the Treatment of Bone Metastases
 Hindawi Publishing Corporation Sarcoma Volume 2007, Article ID 62151, 5 pages doi:10.1155/2007/62151 Clinical Study The Use of Massive Endoprostheses for the Treatment of Bone Metastases D. H. Park, P.
Hindawi Publishing Corporation Sarcoma Volume 2007, Article ID 62151, 5 pages doi:10.1155/2007/62151 Clinical Study The Use of Massive Endoprostheses for the Treatment of Bone Metastases D. H. Park, P.
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries The Latarjet Procedure (coracoid transfer) Shoulder Stabilisation Surgery Ms. Ruth Delaney Consultant Orthopaedic Surgeon
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries The Latarjet Procedure (coracoid transfer) Shoulder Stabilisation Surgery Ms. Ruth Delaney Consultant Orthopaedic Surgeon
What s New in the Treatment of Proximal Humerus Fractures?
 NHMI Winter Meeting Stowe, VT January 2015 What s New in the Treatment of Proximal Humerus Fractures? John Bell, M.D., M.S. Associate Professor Shoulder and Elbow Surgery Dartmouth-Hitchcock Medical Center
NHMI Winter Meeting Stowe, VT January 2015 What s New in the Treatment of Proximal Humerus Fractures? John Bell, M.D., M.S. Associate Professor Shoulder and Elbow Surgery Dartmouth-Hitchcock Medical Center
Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft
 Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
Postoperative Treatment For Pectoralis Major Repair-- Dr. Trueblood
 Postoperative Treatment For Pectoralis Major Repair-- Dr. Trueblood Indications: Full thickness avulsion injuries of the pectoralis usually result from eccentric extension and external rotation of the
Postoperative Treatment For Pectoralis Major Repair-- Dr. Trueblood Indications: Full thickness avulsion injuries of the pectoralis usually result from eccentric extension and external rotation of the
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Rehab Protocol Dr. Payne
 Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of
 Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck.
 Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
Progression to the next phase based on clinical criteria and time frames as appropriate
 Indications Reverse total shoulder replacement is indicated for use in grossly rotator cuff deficient joints with severe arthropathy, or for use when a previous joint replacement has failed with a grossly
Indications Reverse total shoulder replacement is indicated for use in grossly rotator cuff deficient joints with severe arthropathy, or for use when a previous joint replacement has failed with a grossly
Methods Used for Reconstruction in Aggressive Bone Tumours: An Early Experience
 ORIGINAL ARTICLE Methods Used for Reconstruction in Aggressive Bone Tumours: An Early Experience K L Pan, FRCS*, S STing, FRCS**, A W K Mohamad, MS (Orth)*, W GLee, FRCS**, C C Wong, FRCS**, A H Rasit,
ORIGINAL ARTICLE Methods Used for Reconstruction in Aggressive Bone Tumours: An Early Experience K L Pan, FRCS*, S STing, FRCS**, A W K Mohamad, MS (Orth)*, W GLee, FRCS**, C C Wong, FRCS**, A H Rasit,
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT
 SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
Title Protocol for the Management of Shoulder Injuries in MIUs and WICs
 Document Control Title in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate, Logistics and Resilience Department Emergency Department Version Date Issued Status
Document Control Title in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate, Logistics and Resilience Department Emergency Department Version Date Issued Status
Hemiplegic Shoulder Power Point for staff education sessions
 Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
