FLK /08. Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom. Tel Fax:
|
|
|
- Christian Simon
- 6 years ago
- Views:
Transcription
1 FLK /08 Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel Fax:
2 Premier Instrumentation CR or PS Surgical Technique
3 Introduction The AGC Knee System offers the flexibility to change from a cruciate retaining to a posterior stabilised knee within a single system. The transition between constraint level can be made with ease, allowing the physician to evaluate soft tissue and bone deficiencies intraoperatively without making a preoperative commitment to the level of constraint. Biomet does not practice medicine and does not recommend this or any other surgical technique for use on a specific patient. The surgeon who performs any implant procedure is responsible for determining and using the appropriate techniques for implanting the prosthesis in each individual patient. Biomet is not responsible for selection of the appropriate products and or surgical technique(s) to be used on any individual patient. For product information, including indications, contraindications, warnings, precautions and potential adverse effects, see the package insert herein and Biomet s website. This material is intended for the sole use and benefit of the Biomet sales force and physicians. It is not to be redistributed, duplicated or disclosed without the express written consent of Biomet.
4 AGC Total Knee System Premier Instrumentation CR or PS Surgical Technique Contents Preface Product description Pre-operative assessment... 4 Surgical approach Principles of ligamentous balancing The correction of varus deformity The correction of valgus deformity... 6 Posterior cruciate release... 7 Surgical technique AGC V2 Cruciate Retaining & AGC V2 Posterior Stabilised (Cam & Groove) Femoral Intramedullary Technique... 8 Intermedullary Femoral Distal Resection Guide... 8 Distal Femoral Resection Femoral Component Sizing Femoral Contour Resection Extramedullary Tibial Resection Intramedullary Tibial Resection Balancing the Flexion/Extension Gaps Trial Reduction Tibial Sizing Tibial Alignment Stem Preparation Patella Preparation Cementing Components Post Operative Care Ordering Information
5 Preface The AGC Knee System is indicated for use in total knee arthroplasty. THIS DOCUMENT IS INTENDED AS A GUIDE ONLY FOR THOSE ORTHOPAEDIC SURGEONS PROFICIENT IN THE PROCEDURES FOR PRIMARY TOTAL KNEE ARTHROPLASTY. the guide does not take account of the individuality of patients and the surgeon performing the procedure is responsible for deciding upon and implementing the appropriate technique or implanting the prosthesis in each patient. Product Description Introduced in 1983, the AGC (Anatomically Graduated Components) Total Knee is a proven clinical success unsurpassed by any other knee system available today. Ritter et al (1) reported a 97.8% tibiofemoral survival rate for the AGC Knee at 20 years. Independent data from the Swedish Knee Study reported a cumulative survival rate of 96% at 10 years for 14,307 AGC total knee arthroplasties (2). Results from the Finnish Arthroplasty Study further supports these excellent results (3). AGC Posterior Cruciate Retaining Femoral Component with ArCom polyethylene Patella. AGC Posterior Cruciate Substituting (Cam & Groove) Femoral Component with moulded Tibia. 2
6 The AGC Knee offers the following features: AGC Posterior Cruciate Substituting (High Post) Femoral & Tibial Components. ArCom compression moulded polyethylene provides a highly consolidated bearing material with an increased resistance to wear (4)(5). Full interchangeability of femoral, tibial and patellar components allows independent sizing, meeting the specific anatomical demands of the individual patient (6). Cruciate-retaining and cruciate substituting implant options enable the surgeon to select intraoperatively the most appropriate AGC component for the patient (7). Cobalt chromium femoral articular surface for maximum durability of the tibiofemoral and patellofemoral articulation, reduces the potential for wear and loosening of the implant. Titanium alloy plasma sprayed porous coating for cementless fixation, or Interlok finish for cemented use, offer proven clinical biocompatibility (8), and have been in use with the AGC system since A deep, wide trochlear groove articulates with the dome shaped patellar component, creating a congruent and forgiving patellofemoral joint. Wide femoral condyles provide line contact with the articulating surfaces, reducing the contact stresses. (Please refer to page 27 for complete product and instrument catalogue numbers). References 1. Ritter M. et al. 20 year Follow-Up of the AGC Total Kntee June JBJS Supplement Knutson K. ; Lewold S. ; Robertsson O. ; Lidgren L. The Swedish Knee Arthroplasty Register. A nation-wide study of 30,003 knees Acta Orthop Scand. 1994;65 (4): Paavolainen P. ; Slätis F. ; Hämäläinen M. ; Visuri T ; Pulkkinen P. Long Term Results of Total Joint Arthroplasty. Results of a 15-year follow-up on a nationwide registration programme in Finland with 67,714 TJA Data on File. Biomet Inc. Warsaw Bankston A. B. Keating E. M. Ranawat C. Comparison of polyethylene wear in machined versus molded polyethylene. Clin. Ortho. & Rel. Res No. 317: Incavo S. J. et al. Tibial Plateau Coverage in Total Knee Arthroplasty. Clinical Orthopaedics and Related Research Number 299, pp Greenwald A.S; Stability Characteristic Comparison of the AGC and AGC Posterior Stabilized Total Knee Systems., Mt. Sinai Medical Centre, Cleveland, Ohio, U.S.A Hoffman A.A. Response of Human Cancellous Bone to Identically Structured Commercially Pure Titanium and Cobalt-Chromium Alloy Porous Coated Cylinders, Clinical Materials, Vol.14, p ,
7 Pre-operative Assessment In Total Knee Arthroplasty (T.K.A.) it is most important to ensure both correct leg alignment and soft tissue tension. While the instrumentation will help considerably with the problems associated with alignment and bone cuts, care needs to be taken by the surgeon to attain correct tension of the soft tissues. Long-leg standing radiographs are recommended to determine both the mechanical and anatomical axis. The mechanical axis passes from the centre of the femoral head to the centre of the ankle passing slightly medial to the centre of the knee. The tibiofemoral (valgus) angle can be measured and is usually found to be between 5º and 10º. This angle represents the final transverse cut of the distal femur and restores the mechanical axis of the limb. Failure to achieve normal limb alignment is one of the common errors in T.K.A. and may lead to premature failure of the implant. It may also be helpful to use x-ray templates to get an indication of the probable size of the prosthesis required, and to determine whether additional support in the form of bone graft or augmentation blocks/wedges will be necessary. A lateral template overlaid on an M/L radiograph of the distal femur gives an indication of the correct size which will avoiding notching the femur. Using the A/P view template an indication is gained of the size required to provide adequate coverage of both medial and lateral femoral condyles, and the probable size and thickness of the tibial component. 4
8 Surgical Approach A thigh tourniquet is recommended but is not mandatory. Prepare and drape the limb so as to allow the centre of the ankle and the hip to be palpated during the course of the operation. This will be necessary when using extra-medullary instrumentation and also to check the limb alignment. Fig 1 Skin marks provide a useful guide to aid closure - cross hatching over a mid-line longitudinal incision for a standard approach as shown [Figure 1]. Position the leg in 90º of flexion with the aid of a sandbag placed under the foot. A standard medial parapatellar approach can be made in the majority of cases, although a lateral approach may be indicated in the severe valgus knee. A mid-line longitudinal, or slightly medial, skin incision is conventional. The existence of previous transverse scars e.g. prior upper tibial osteotomy, are not a cause for concern, but care should be taken if there are longitudinal scars. Use the most lateral of the pre-existing scars to minimise the risk of post-operative wound edge necrosis (the lateral wound edge is the most sensitive to hypoxia). Fig 2 The incision is either longitudinal or slightly curved beginning approximately 5cm proximal to the patella, and extending to approximately 4cm below the tibial tubercle. Dissect the soft tissues until the quadriceps tendon and patella tendon are clearly exposed. Identify the interval between the rectus femoris and vastus medialis and incise the extensor mechanism on the medial aspect to leave a cuff of soft tissue around the patella for subsequent repair [Figure 2]. Evert the patella to complete the exposure of the joint. If difficulty is encountered in undertaking this step, the lateral patellofemoral ligaments should be divided first. Occasionally it may be necessary to perform a lateral release. Principles of Ligamentous Balancing The importance of soft tissue balancing in T.K.A. cannot be over stressed. Failure to achieve correct soft tissue balancing may result in premature wear of the implant and early failure. Ligamentous balancing is generally carried out in three phases: 1. A preliminary soft tissue release is performed at the beginning of surgery and is, essentially, part of the surgical exposure. This should be combined with excision of any peripheral osteophytes. 2. Ligamentous balancing is achieved by correction of soft tissue contractures and not by modification of the bone cuts. 3. Fine tuning the soft tissue balancing is achieved at trial reduction and may include further soft tissue releases, especially lateral retinacular release to correct the patellar tracking. 5
9 The Correction of Varus Deformity The medial tissues are generally released to some extent during the course of the surgical approach. This routinely involves resection of osteophytes, the meniscus, the capsule and the release of deep collateral ligament. Following resection of the anterior cruciate it is possible to completely expose the proximal tibia by gently elevating the capsular-ligamentous complex as far as the semi-membranosus bursa in the postero-medial corner and then externally rotating the tibia to deliver the tibial plateau into the wound. In the majority of varus knees this is usually sufficient as there is no real tightening of the medial structures. However, when there is true fixed varus, care must be taken to perform a more extensive release without jeopardising future stability. The following principles of the correction are essentially to elevate an intact periosteal sleeve from the medial tibia: 1. Excision of medial osteophytes and medial meniscal remnants. 2. Complete capsular release from the periphery of the tibial plateau. 3. Release of the posterior portion of the deep medial collateral ligament. 4. Release of the superficial collateral ligament. 5. Release of the pes anserinus. The Correction of Valgus Deformity For the severe valgus knee a lateral approach should be considered. A lateral retinacular release and recession of the posterior cruciate ligament are almost inevitable. The sequence of correction of a valgus deformity are as follows: 1. Standard medial releases to include the dissection of the anterior half of the deep medial collateral ligament, leaving the superficial and the pes anserinus group intact. 2. Complete exposure of the lateral aspect of the tibial plateau taking care to excise all peripheral osteophytes and meniscal remnants. 3. Transverse division of the tensor fascia lata some 10-12cm proximal to its insertion. This is best accomplished from its deep surface. 4. Resection of the popliteus tendon. 5. Release or recession of the posterior cruciate ligament. 6. Release of the lateral head of the gastrocnemius from the posterior aspect of the femur. 7. Occasionally it may be necessary to release the lateral collateral ligament from the femoral condyle. This must be undertaken very carefully to allow the attachment to slide distally as a periosteal flap. 8. As a last resort the biceps tendon may be step lengthened, but this is a hazardous procedure and is often associated with a post-operative foot drop as a result of damage and stretching of the lateral popliteal nerve. Correct Mechanical Axis Varus Deformity Axis Correct Mechanical Axis Valgus Deformity Axis Varus Deformity Valgus Deformity 6
10 Posterior Cruciate Release The understanding of posterior cruciate balancing is fundamental to achieving a tripod balance. There are arguments for and against retention of the posterior cruciate, but these of course relate to the choice of prosthesis and its ability to substitute posterior cruciate function. In the absence of the anterior cruciate there is no true four-bar linkage and roll back is altered. Nevertheless, a retained posterior cruciate will provide some A/P stability and preserve proprioception. If the posterior cruciate is retained, it is of great importance that there is no residual tightness. This can be identified by either limited flexion, with excessive femoral roll back, anterior lift of the tibial tray in flexion and a palpable ligamentous tension in flexion. The likely causes of residual tightness of the posterior cruciate includes residual posterior osteophytes and incomplete resection of the menisci, or pre-operative fixed flexion deformity, especially in rheumatoid disease. The cruciate can be lengthened by recession from the tibial attachment using cutting diathermy or a knife. In addition, further space can be gained by cutting the tibial plateau with a posterior slope. This may lead to division of the posterior cruciate by division of the tibial attachment. Further release can be gained by a posterior capsular release, stripping the posterior capsule off the femoral condyle using a curved-on-flat osteotome. Care must be taken to protect the popliteal vessels in these circumstances. 7
11 Step 1 Premier Technique for AGC Knee Figure 1 Initial I/M Drill Penetration Intermedullary Femoral Distal Resection Guide The.375" I/M drill is utilized to penetrate the cortex and dense cancellous bone to a depth of approximately one and one-half to two inches (3.5 to 5cm). The canal entry location is placed 1cm above the insertion of the posterior cruciate ligament and slightly medial in the intercondylar notch (Figure 1). Set the adjustable distal femoral resection guide to the desired valgus angle by pressing and turning the most distal knob. A valgus angle setting of zero to nine degrees is available. Select the depth of distal resection by turning the most proximal dial. The distal resection depth can range from a simple 1mm clean-up cut for revision scenarios up to 11mm (Figure 2). Note: The standard distal resection is 9mm matching the distal thickness of the implant. Insert the I/M rod through the central hole in the adjustable guide. Insert the T-handle I/M rod into the prepared I/M canal hole. Slowly advance and rotate the I/M rod until the canal contents are aspirated. Slide the adjustable distal resection guide until it rests flush with the distal femur. Attach the femoral distal cut block to the distal resection guide adapter by sliding the magnetized distal resection block into the adjustable distal guide adapter. Attach the adjustable distal guide adapter and the femoral distal cut block to the adjustable femoral resection guide by sliding the two legs on the distal resection guide adapter through the anterior holes of the adjustable guide block until the resection cut block contacts the anterior cortex of the femur. Pin the resection block into place using 1/8" quick release drill bits in the most proximal holes (Figure 3). Figure 2 Adjustable Distal Femoral Resection Guide Figure 3 Placement of Cut Head and Adjustable Resection Guide To confirm the valgus angle, the alignment tower handle can be inserted into the distal resection block and a ¼" alignment rod can be inserted and extended to the femoral head. 8
12 Step 1 (continued) Premier Technique for AGC Knee The adjustable block can now be removed by disengaging the I/M rod and pulling the guide block and bracket distally away from the distal resection block, leaving the distal resection block in place. Two resection slots of 0mm or +3mm are available for the distal resection. The 0mm slot will resect the depth level that was determined by setting the most proximal adjustable dial. If additional distal resection is required, the +3mm slot will resect 3mm more than the distal thickness of the femoral component. If additional distal resection is required beyond the additional 3mm slot, shift the resection block proximal by utilizing the +2mm or +4mm 1/8" pin holes (Figure 4). Figure 4 Anterior View of Distal Femoral Cut Guide Figure 5 Distal Femoral Cut Complete the distal resection through the selected slot using a.054" saw blade (Figure 5). Check the resected distal femur using a flat instrument. Recut or file as necessary to ensure a proper resection. 9
13 Step 2 Premier Technique for AGC Knee Figure 1 A/P Sizer with Standard Feet Distal Femoral Sizing The A/P sizer is placed flat against the resected distal surface with the feet in contact with the posterior condyles of the femur. Three options are available for the external rotation feet: 3 degrees (left and right) external rotation and neutral (Figure 1). Place the sizer flush on the resected distal femur. (Figure 2) Figure 2 A/P Sizer with Standard Feet Note: An alignment handle can be attached to the front of the A/P sizer for added insertion ease. (Figure 3) Place the stylus slightly lateral to the midline on the anterior cortex. The femoral component size can now be read from the central scale. If the size indicated is in-between standard sizing then a choice of up sizing or down sizing the femoral component can be made. Increase the Femoral component size This will avoid the risk of notching but because the anterior cortex of the implant has been moved anteriorly there is potential of over stuffing the patella/femoral tracking of the joint. Figure 3 Placement of A/P Sizer Example: If the guide measures between 65 and 70. Drill the standard holes and use a 70 contour block and femoral impant. Decrease the size of the femoral component and move its position anteriorly. Example: If the guide measures between 65 and 70. Drill the +2 holes and use a 65 contour block and femoral implant. Figure 4 A/P Sizer with +2 Holes Note: The final medial/lateral position of the component is not determined during this step, but is addressed later in the technique. 10
14 Step 3 Premier Technique for AGC Knee Figure 1 Placement of Contour Block with Handles Femoral Contour Resection Choose the slotted femoral contour guide which matches the selected size on the adjustable A/P sizing instrument, and place it into the 1/8" holes drilled into the distal femur. Attach the handles into the sides of the contour block and make sure the contour guide is sitting flush against the flat area of the distal femur (Figure 1). If additional stability is required, pins can be placed in the side holes provided (Figure 2). A.054" feeler blade can be used to determine the amount of anterior bone resection (Figure 3). Figure 2 Premier TM Contour Block with Pin Fixation Once the block position is satisfactory, resect the anterior and posterior bone, and the anterior and posterior chamfers with a.054" saw blade (Figure 4). Note: When posterior referencing, the same amount of posterior condyle will be removed each time regardless of size. Figure 3 Premier Contour Block with Feeler Blade Figure 4 Premier TM Contour Block 11
15 Step 4 Premier Technique for AGC Knee Figure 1 Placement of Ankle Clamp Extramedullary Tibial Resection With the knee flexed, place the spring loaded arms of the ankle clamp around the distal tibia just above the malleoli. The red bolt on the body of the tibial resector is loosened to change the height of the resection guide (Figure 1). The tibial resection block is then placed against the proximal tibia (Figure 2). Adjust the resection guide until the tubular body is parallel (for 0 degree posterior slope) with the shaft of the tibia (Figure 3), by adjusting the ankle clamp locking mechanism. Adjust the varus/valgus slope of the cutting head by adjusting the M/L position of the resector ankle clamp assembly (the average anatomy offset equals 5mm medial) (Figure 4). Figure 2 Setting of E/M Tibial Resection Guide Figure 3 Placement of Tibial Cut Block Figure 4 Placement of EM Tibial Resection Guide 12
16 Step 4 (continued) Premier Technique for AGC Knee Figure 5 Tibial Stylus Attached to Resection Block Once adjustment of the resector axis is correct in the M/L view, rotate the resector until the shaft of the resector is just medial to the tibial tubercle. Push the gold button located on the top of the stylus to release the stylus locking mechanism and snap the stylus into the top of the cutting block (Figure 5). Set the stylus to read 8-10 mm and then use the angled end of the stylus to reference the deepest portion of the unaffected tibial condyle (Figure 6). (In contrast approximately 2 4 mm should be resected if referencing the most affected tibial condyle.) The resector head is locked into place by tightening the resector head assembly. Starting with the most lateral hole, pin the resector head with 1/8" headless pins in the most distal holes (Figure 7). Note: If a larger tibial resection is required, the tibial cutting block contains 2 sets of holes that allow for a +2mm or +4mm resection. Leaving the pins in place, remove the cutting block by sliding it off the pins and repositioning it at the desired +2 or +4 holes (Figure 8). Figure 6 EM Tibial Resection Guide with Alignment Handle Figure 7 Resection Guide with Pins in Distal Position Figure 8 Tibial Resection Guide 13
17 Step 4 (continued) Premier Technique for AGC Knee Figure 9 Proximal Tibial Resection Remove the stylus from the resector and resect the tibial plateau through the slot in the head with a.054" saw blade (Figure 9). The resector assembly may be removed or kept attached to the head, taking care not to cut the posterior cruciate ligament inadvertently. 14
18 Step 5 Premier Technique for AGC Knee Figure 1 Initial Tibial I/M Drill Penetration Intramedullary Tibial Resection The knee is fully flexed and the center of the tibial plateau is identified. A.375" I/M drill is then utilized to enter the medullary canal. The point of entry is just posterior to the anterior cruciate ligament attachment (Figure 1). Upon removal of the drill, slide the T-Handle fluted rod through the body of the tibial resection guide with the tibial resection block in place and insert it into the canal. The fluted rod allows for the release of marrow. To properly position the resection head, a silver button is located on the left side of the body of the guide. Press the button and slide the resection guide forward until the tibial cutting block becomes flush to the anterior cortex of the tibia (Figure 2). Figure 2 Placement of I/M Tibial Resection Guide The posterior slope of the resection is controlled by using a cutting head with the desired slope. The tibial depth gauge is placed along the side of the resection guide on the side of the least affected condyle (usually the lateral). The tibial depth gauge reflects the total amount of bone to be resected. The amount of bone resected varies depending on the anterior dial setting. The resection level can be changed by pressing the dial and rotating it to the appropriate resection level. The dial will snap into place at each 1mm increment (Figure 3). Figure 3 Dial for Setting Resection Level 15
19 Step 5 (continued) Premier Technique for AGC Knee Slide the cutting head adaptor against the proximal tibia by pressing the silver button on the resector body and sliding the block toward the tibia. To confirm alignment, an alignment tower/handle can be placed on the cutting block and a 1 4" alignment rod can be inserted into medial hole of the guide (Figure 4). Once the correct position is established, 1/8" drill bits are used to secure the cutting block to the tibia through the most distal holes. Note: If a larger tibial resection is required, the tibial cut head contains 2 sets of holes that allow for a +2mm or +4mm resection. Leaving the pins in place, remove the cut by sliding it off the pins and repositioning it at the desired +2 or +4 holes. (Figure 5). Figure 4 I/M Tibial Resection Guide with Alignment Handle Figure 5 Tibial Resection Guide The tibial resection guide, alignment tower and rod are then removed, leaving the resection block in place. The plateau is resected using a.054" saw blade. 16
20 Step 6 Premier Technique for AGC Knee Figure 1 Flexion/ Extension Guage in Extension Balancing the Flexion and Extension Gaps In balancing the flexion and extension gaps the following principles are fundamental: 1. The amount of distal femoral bone resected affects the soft tissue tension in extension. 2. The amount of posterior femoral condylar bone resected affects the soft tissue tension in flexion. 3. The amount of tibial bone resected effects the soft tissue tension in both extension and flexion. Figure 2 Flexion/ Extension Guage in Flexion Correct leg alignment may have been achieved simply by the bone resections. However, it still may be necessary to further fine tune leg alignment by either a medial or lateral collateral ligament release, this should be performed carefully and the flexion/extension gaps checked again [Figures 1 & 2]. 17
21 Step 6 (Continued) Premier Technique for AGC Knee The following procedures may be necessary in some exceptional cases: 1. Residual Flexion Contracture. A residual flexion contracture in full extension implies that the extension gap is tighter than the flexion gap. The extension gap should be cut to match the flexion gap by resecting more distal femur, consequently placing the femoral component more proximal. This may however be at the expense of elevation of the joint line and subsequent patellar baja. In case of fixed flexion deformity there are essentially two procedures which may be used to remove additional bone: (i) With the distal femoral resector in its existing position, i.e. nailed at its original fixation points on the anterior surface, an additional 3mm of bone may be resected by placing the blade through the slot 3 on the resector [Figure 3]. Note: Resection of the chamfer cuts will also be necessary. OR (ii) If the distal cut has already been made the Tibial Resection Guide assembly can be used to remove additional bone. Turn the proximal dial and reset to the desired resection, e.g. the dial is normally set to 9 but moving this to 3 will effectively take an extra 3mm of bone off the distal cut and a total of 12mm of bone is therefore removed (9mm already having been resected at the initial distal resection) [Figure 4]. 2. Residual Tightness in Flexion and Extension. This would imply either inadequate soft tissue releases or, more commonly inadequate bone cuts. Increase in the flexion and extension gaps can be achieved by resecting more proximal tibia. It is often helpful to leave the tibial resection guide in situ whilst attempting the trial reduction. This facilitates further resection of the proximal tibia if required. 3. Residual Tightness in Flexion i.e. flexion gap less than extension gap. It is advisable in the first instance to check for posterior osteophytes which may be restricting flexion. Recession of the PCL may also allow greater flexion. The flexion gap can be increased by cutting the tibia with a posterior slope (no more than 7º). Figure 3 Tibial Resection Guide Figure 4 Tibial Resection Guide 18
22 Step 7 Premier Technique for AGC Knee Figure 1 Initial Placement of CR Femoral Trial Trial Reduction Once bony surfaces have been prepared, a trial reduction may be completed. The trial femoral component is placed on the distal femur with the femoral inserter and initially impacted. Fully seat the femoral trial with the final femoral impactor (Figure 1). Trial bearing inserts are sequentially selected to determine the appropriate thickness of tibial component. Select the appropriate trial patellar component and place onto the patella (If used). With the trial components in place, check the range of motion and stability of the knee (Figure 2). If tightness is found medial/laterally, in flexion, or in extension, appropriate soft tissue releases may be performed. With correct soft tissue tension the knee can be put through a range of motion several times and the trial tibial bearing will self align. Using electrocautery mark the anterior cortex of the tibia directly under the reference lines on the trial, these can be used to determine the position of the definitive implant. Identification of the final position can be determined alternatively using an alignment rod (Step 8). Placement of the Femoral Component Figure 2 Complete CR Trial in Place Figure 3 Final Medial/ Lateral Femoral Preparation with 1/4" Drill Bit With the trial femoral and tibial components in place, determine the final M/L placement of the femoral component. Place the patella back into its normal anatomic position (with the trial patella button if used). Manipulate the knee through a normal range-of-motion, observing and noting the tracking and tension of the patellofemoral joint. If necessary, evert the patella and move the femoral component either laterally or medially to improve patella tracking. Replace the patella and repeat the range-of-motion exercise. Repeat as necessary until the patella tracks satisfactorily. Evert the patella and drill 1 4" diameter holes through the holes in the distal condyles of the femoral trial (Figure 3). 19
23 Step 8 Premier Technique for AGC Knee Figure 1 Tibial Template with fixation pins Tibial Plateau Sizing and Alignment The knee is placed in maximum flexion and the tibia is subluxed anteriorly. The tibial tray that provides the greatest amount of coverage both in the M/L and A/P planes is selected (Figure 1). Tibial Alignment using the Extramedullary rod. Rotation should be based upon position relative to the tibial tubercle as well as the malleolar axis. An extramedullary alignment check is made by placing the external alignment rod through the hole in the handle (Figure 2). Slight external rotation is preferred to optimize patellofemoral tracking. An initial trial reduction can be performed to confirm proper rotation. When correct rotation has been determined, the tibial tray can be stabilized using short fixation pins. Figure 2 Tibial Template and alignment handle Figure 3 Tibial Alignment using Trial Reduction With the femoral trial in place (figure 3) it is possible to determine the correct orientation and thickness of the tibial component using the tibial trial. 20
24 Step 9 Premier Technique for AGC Knee Figure 1 Tibial Punch Guide Tibial Stem-Punch Guide The stems of the tibial components are of different lengths according to the size of the component. To prepare the resected tibia for accepting the stem the following procedure is followed. 1. Locate the tibial tower guide onto the tibial plateau template handle assembly and attach it with the captured thumb screw, located anteriorly (Figure 1). 2. Insert the punch correctly oriented into the tower (Figure 2) and drive it down until the mark on the punch corresponds to the size of the tibia chosen as indicated on the tower guide (Figure 3). 3. For cementless procedures use the Cementless I-Beam Tibial Chisel in the same manner as described for the punch (Figure 2). This provides a tapered I-Beam profile channel, fitting the stem exactly. For dense bone when cementing it may be useful to first use the cementless I-Beam tibial Chisel prior to using the solid tibial punch. Figure 2 With Tibial Punch Guide Figure 3 Tibial Punch Guide 21
25 Step 10 Premier Technique for AGC Knee Figure 1 Patellar Caliper Measurement Patella Resection Surface Clamp The patella is everted and the osteophytes and peripatellar tissues are removed down to the level of the tendinous insertions of the quadriceps and patellar tendons. The level of the cut is determined through caliper measurement of the total patellar thickness (Figure 1). The initial patellar resection is performed utilizing the patella clamp surface cut guide. The guide is clamped to perform a flat cut across the patella. A magnetic depth stylus may be utilized to determine the appropriate resection level (Figure 2). Care should be taken to restore original patella height to prevent overstuffing of the patellofemoral joint. If a single peg patellar component is utilized, the single peg patellar drill guide is used to locate the placement of the central peg. The central hole is drilled using the patellar peg drill. A trial patellar component is selected to optimize coverage without increasing patellar thickness beyond pre-resection height. If a 3-peg patellar component is to be implanted, the 3-peg drill guide is placed onto the resected patella and the drill bit is used to make the holes for the pegs (Figure 3). Figure 2 Patellar Clamp with Magnetic Depth Stylus Figure 3 3-Peg Patellar Drill Guide AGC Patellas Diameter peg Std Thin peg Std Thin The 23mm Single-Peg Patella Components should be used only with an inset mill surgical technique. 22
26 Step 11 Premier Technique for AGC Knee Figure 1 Final Tibial Component Implant Femoral and Tibial Implant Insertion Cementing the Tibia 1. Use a small piece of resected bone to plug the femoral intramedullary canal to post-operative blood loss. 2. All resected surfaces must be thoroughly cleaned, preferably with pressurised lavage and dried. It is advisable to use suction to remove the debris and liquid trapped in the cavities of the trabecular bone 3. Ideally cement is applied to all the internal surfaces of the femoral component and to all of the resected femoral bone surfaces. Similary, cement is applied to the underside of the tibial stem hole. The components can be implanted simutaneously or sequentially. 4. After impacting the implants, care should be taken to remove all extruded surplus cement,especially from the posterior condyles of the femoral component. The cement can be pressurised whilst setting by extending the leg to 0 or slight hyperextension. 23
27 Step 13 Premier Technique for AGC Knee Figure 1 Final Patella Component Implant Patella Component Cement is applied to one or both surfaces of the resected patella and patella button. The patella component is placed onto the appropriate patellar component is placed into the patella and pushed into position with finger pressure so the peg engages the prepared hole(s). Extruded cement is removed with a curette. The patellar clamp is positioned onto the component and the cap screwed down until it contacts the component. The ratchet handle is then tightened to compress the implant (Figure 1). As the clamp is tightened, extruded cement is removed with a curette. The clamp should be left in position until the cement cures. 24
28 Ordering information - AGC Implants Femoral Components Universal V2 Porous Femoral Components mm mm mm mm mm mm Universal V2 Interlok Femoral Components mm mm mm mm mm mm Anatomic Porous Femoral Components Right Left mm mm mm mm mm mm mm mm mm mm mm mm Anatomic Interlok Femoral Components Right Left mm mm mm mm mm mm mm mm mm mm mm mm PCL Substituting - Cam & Groove Universal V2 PS Porous Femoral Components mm mm mm mm mm mm Universal V2 PS Interlok Femoral Components mm mm mm mm mm mm Anatomic PS Porous Femoral Components Right Left mm mm mm mm mm mm mm mm mm mm mm mm Anatomic PS Interlok Femoral Components Right Left mm mm mm mm mm mm mm mm mm mm mm mm PCL Substituting - High Post Posterior Stabilised (HPPS) Universal Interlok Femoral Components mm mm mm mm mm Porous coated components are designed for press fit application. Interlok components are designed for cemented application. 25
29 Tibial Components PCL Retaining and Substituting - (Cam & Groove) V2 Porous Moulded Tibial Components (ArCom ) x 63mm x 79mm x 63mm x 63mm x 63mm x 63mm x 63mm x 79mm x 79mm x 79mm x 79mm x 79mm V2 Interlok Moulded Tibial Components (ArCom ) x 63mm x 79mm x 63mm x 79mm x 63mm x 79mm x 63mm x 79mm x 63mm x 79mm x 63mm x 79mm x 67mm x 83mm x 67mm x 83mm x 67mm x 83mm x 67mm x 83mm x 67mm x 83mm x 67mm x 83mm x 67mm x 83mm x 67mm x 83mm x 67mm x 83mm x 67mm x 83mm x 67mm x 83mm x 67mm x 83mm x 71mm x 87mm x 71mm x 87mm x 71mm x 87mm x 71mm x 87mm x 71mm x 87mm x 71mm x 87mm x 71mm x 87mm x 71mm x 87mm x 71mm x 87mm x 71mm x 87mm x 71mm x 87mm x 71mm x 87mm x 75mm x 91mm x 75mm x 91mm x 75mm x 91mm x 75mm x 91mm x 75mm x 91mm x 75mm x 91mm x 75mm x 91mm x 75mm x 91mm x 75mm x 91mm x 75mm x 91mm x 75mm x 91mm x 75mm x 91mm 26
30 Tibial Components (continued) PCL Substituting - High Post (HPPS) x10mm x12mm x14mm x16mm x18mm x22mm x10mm x12mm x14mm x16mm x18mm x22mm x10mm x12mm x14mm x16mm x18mm x22mm x10mm x12mm x14mm x16mm x18mm x22mm x10mm x12mm x14mm x16mm x18mm x22mm x10mm x12mm x14mm x16mm x18mm x22mm x10mm x12mm x14mm x16mm x18mm x22mm Patella Components ArCom Patella Components ArCom Poly Patella Button 31mm ArCom Poly Patella Button 34mm ArCom Poly Patella Button 37mm 27
31 28 Notes
32 Notes 29
33 30
34 31
FLK167 02/08. Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom. Tel Fax:
 FLK167 02/08 Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel. 01656 655221 Fax: 01656 645454 Premier Instrumentation CR or PS Surgical Technique Vanguard Premier
FLK167 02/08 Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel. 01656 655221 Fax: 01656 645454 Premier Instrumentation CR or PS Surgical Technique Vanguard Premier
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
AGC Total Knee System. Concise Surgical Technique Featuring EquiFlex Instrumentation
 AGC Total Knee System Concise Surgical Technique Featuring EquiFlex Instrumentation AGC TOTAL KNEE SYSTEM Concise Surgical Technique Instrumentation Disclaimer This brochure provides a description of the
AGC Total Knee System Concise Surgical Technique Featuring EquiFlex Instrumentation AGC TOTAL KNEE SYSTEM Concise Surgical Technique Instrumentation Disclaimer This brochure provides a description of the
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Premier Total Knee Instrumentation
 Premier Total Knee Instrumentation Vanguard Complete Knee System Surgical Technique Table of Contents Indications and Contraindications... 3 Introduction... 4 Patient Selection Preoperative Planning Approaches...
Premier Total Knee Instrumentation Vanguard Complete Knee System Surgical Technique Table of Contents Indications and Contraindications... 3 Introduction... 4 Patient Selection Preoperative Planning Approaches...
Surgical Technique with Millennium Instrumentation
 Surgical Technique with Millennium Instrumentation Surgical Technique with Millennium Instrumentation 1 This document includes the operative techniques for AGC primary knees including AGC posterior cruciate
Surgical Technique with Millennium Instrumentation Surgical Technique with Millennium Instrumentation 1 This document includes the operative techniques for AGC primary knees including AGC posterior cruciate
Triathlon Knee System
 Triathlon Knee System Express Instruments Surgical Protocol Posterior Stabilized & Cruciate Retaining TriathlonKneeSystem Express Instruments Surgical Protocol Acknowledgments..........................................................2
Triathlon Knee System Express Instruments Surgical Protocol Posterior Stabilized & Cruciate Retaining TriathlonKneeSystem Express Instruments Surgical Protocol Acknowledgments..........................................................2
TOTAL KNEE ARTHROPLASTY SYSTEM
 SURGICAL TECHNIQUE TOTAL KNEE ARTHROPLASTY SYSTEM 90-SRK-700000 B.0 0 Contents 1. Implant Sizing 2. Surgical Technique a. Incision and Exposure b. Distal Femoral Resection c. Tibial Resection d. Femoral
SURGICAL TECHNIQUE TOTAL KNEE ARTHROPLASTY SYSTEM 90-SRK-700000 B.0 0 Contents 1. Implant Sizing 2. Surgical Technique a. Incision and Exposure b. Distal Femoral Resection c. Tibial Resection d. Femoral
TRK REVISION KNEE Surgical Technique
 1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
Microplasty Elite Total Knee Instrumentation
 Microplasty Elite Total Knee Instrumentation Vanguard Complete Knee System Surgical Technique Table of Contents Indications and Contraindications... 3 Introduction... 4 Patient Selection Preoperative
Microplasty Elite Total Knee Instrumentation Vanguard Complete Knee System Surgical Technique Table of Contents Indications and Contraindications... 3 Introduction... 4 Patient Selection Preoperative
ANATOMIC SURGICAL TECHNIQUE. 5 in 1. Conventional instrumentation 07/11/2013
 ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
Extramedullary Tibial Preparation
 Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Zimmer FuZion Instruments. Surgical Technique (Beta Version)
 Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION. Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique
 POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees
POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION. Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique
 ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
OPERATIVE TECHNIQUE SKS Total Knee Replacement
 OPERATIVE TECHNIQUE SKS Total Knee Replacement Femoral preparation A40577 1 2 5 1: Alignment rod A30049 + A30124 2: Centromedullary rod A40224 4: T-handle A40232 6: Femoral measuring device A40411 + A40414
OPERATIVE TECHNIQUE SKS Total Knee Replacement Femoral preparation A40577 1 2 5 1: Alignment rod A30049 + A30124 2: Centromedullary rod A40224 4: T-handle A40232 6: Femoral measuring device A40411 + A40414
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
Knee. Surgical Protocol
 U2 TM PS CR Knee Surgical Protocol Table of Contents Pre-Operative Planning... Surgical Incision... 1 2 A. Femoral Preparation A.1. Pilot Hole... A.2. Femoral Valgus Angle Confirmation... A.3. Distal
U2 TM PS CR Knee Surgical Protocol Table of Contents Pre-Operative Planning... Surgical Incision... 1 2 A. Femoral Preparation A.1. Pilot Hole... A.2. Femoral Valgus Angle Confirmation... A.3. Distal
Vanguard ID Total Knee. Surgical Technique
 Vanguard ID Total Knee Surgical Technique Table of Contents Overview... 2 Preoperative Planning... 4 Incision... 4 Patella Preparation... 5 Patella Resection Femoral Preparation... 8 Distal Femoral Resection
Vanguard ID Total Knee Surgical Technique Table of Contents Overview... 2 Preoperative Planning... 4 Incision... 4 Patella Preparation... 5 Patella Resection Femoral Preparation... 8 Distal Femoral Resection
Surgical Technique. VISIONAIRE Disposable Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
NexGen Cruciate Retaining (CR) and Revision Instrumentation. Surgical Technique
 NexGen Cruciate Retaining (CR) and Revision Instrumentation Surgical Technique Table of Contents Introduction... 4 Revision Arthroplasty... 4 Multi-Reference 4-in-1 Instrumentation System MICRO-MILL Instrumentation
NexGen Cruciate Retaining (CR) and Revision Instrumentation Surgical Technique Table of Contents Introduction... 4 Revision Arthroplasty... 4 Multi-Reference 4-in-1 Instrumentation System MICRO-MILL Instrumentation
NATURAL MOTION TECHNOLOGY SURGICAL TECHNIQUE. EMPOWR 3D Knee. EMPOWR PS Knee
 NATURAL MOTION TECHNOLOGY EMPOWR 3D Knee EMPOWR PS Knee SURGICAL TECHNIQUE Contents System Features.... 3 Indications and Contraindications.... 4 Surgical Snap Shot.... Preoperative Planning.... Surgical
NATURAL MOTION TECHNOLOGY EMPOWR 3D Knee EMPOWR PS Knee SURGICAL TECHNIQUE Contents System Features.... 3 Indications and Contraindications.... 4 Surgical Snap Shot.... Preoperative Planning.... Surgical
Surgical Technique. VISIONAIRE FastPak Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
Knee. Surgical Protocol
 U2 TM PS CR Knee Surgical Protocol Table of Contents Pre-Operative Planning... Surgical Incision... 1 2 A. Femoral Preparation A.1. Pilot Hole... A.2. Femoral Valgus Angle Confirmation... A.3. Distal
U2 TM PS CR Knee Surgical Protocol Table of Contents Pre-Operative Planning... Surgical Incision... 1 2 A. Femoral Preparation A.1. Pilot Hole... A.2. Femoral Valgus Angle Confirmation... A.3. Distal
ClassiQ. Scorpio. Anterior Referencing Surgical Protocol. Anterior Referencing. For use with Scorpio ClassiQ Instrument System
 Scorpio ClassiQ Anterior Referencing Surgical Protocol For use with Scorpio ClassiQ Instrument System For use with Scorpio ClassiQ Single Radius Total Knee System AR Anterior Referencing This document
Scorpio ClassiQ Anterior Referencing Surgical Protocol For use with Scorpio ClassiQ Instrument System For use with Scorpio ClassiQ Single Radius Total Knee System AR Anterior Referencing This document
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Triathlon Knee System Posterior Stabilized & Cruciate Retaining Table of Contents Acknowledgments.......................................................1
The information contained in this document is intended for healthcare professionals only. Triathlon Knee System Posterior Stabilized & Cruciate Retaining Table of Contents Acknowledgments.......................................................1
Persona. The Personalized Knee. Trabecular Metal Tibia. Surgical Technique
 Persona The Personalized Knee Trabecular Metal Tibia Surgical Technique Table of Contents Resect the Tibia... 4 Size and Finish the Tibia... 4 Trial Fit... 6 Component Implantation... 7 Inserter/Implant
Persona The Personalized Knee Trabecular Metal Tibia Surgical Technique Table of Contents Resect the Tibia... 4 Size and Finish the Tibia... 4 Trial Fit... 6 Component Implantation... 7 Inserter/Implant
Profix. Total Knee System. As described by
 Profix Total Knee System P R I M A R Y P R O C E D U R E As described by Leo A. Whiteside, M.D. Associate Research Professor Washington University School of Medicine Director, Biomechanical Research Laboratory
Profix Total Knee System P R I M A R Y P R O C E D U R E As described by Leo A. Whiteside, M.D. Associate Research Professor Washington University School of Medicine Director, Biomechanical Research Laboratory
Dual Articular.
 Dual Articular 2000 www.biomet.co.uk D e s i g n R a t i o n a l e The Dual Articular Knee has been in use since 1991 and offers a flexible reconstructive solution for total knee surgery; for both revision
Dual Articular 2000 www.biomet.co.uk D e s i g n R a t i o n a l e The Dual Articular Knee has been in use since 1991 and offers a flexible reconstructive solution for total knee surgery; for both revision
U2 KNEE SYSTEM. High Flexion Engineered
 U2 KNEE SYSTEM High Flexion Engineered TABLE OF CONTENTS Pre-Operative Planning...1 Surgical Incision...2 A. Femoral Preparation A.1. Pilot Hole...3 A.2. Femoral Valgus Angle Confirmation...4 A.3. Distal
U2 KNEE SYSTEM High Flexion Engineered TABLE OF CONTENTS Pre-Operative Planning...1 Surgical Incision...2 A. Femoral Preparation A.1. Pilot Hole...3 A.2. Femoral Valgus Angle Confirmation...4 A.3. Distal
Zimmer NexGen Trabecular Metal Tibial Tray
 Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Triathlon Knee System. Universal Baseplate Surgical Protocol
 Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments..........................................................2 Introduction...............................................................2
Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments..........................................................2 Introduction...............................................................2
Aesculap Orthopaedics Columbus MIOS
 Aesculap Orthopaedics Columbus MIOS Minimally Invasive Orthopaedic Solutions Manual TKA Surgical Technique MIOS 4-in-1 Cutting Block MIOS Distal Femoral Cutting Block MIOS Tibial Left and Right Cutting
Aesculap Orthopaedics Columbus MIOS Minimally Invasive Orthopaedic Solutions Manual TKA Surgical Technique MIOS 4-in-1 Cutting Block MIOS Distal Femoral Cutting Block MIOS Tibial Left and Right Cutting
unicompartmental knee SURGICAL TECHNIQUE limacorporate.com
 unicompartmental knee SURGICAL TECHNIQUE limacorporate.com Index INTRAMEDULLARY (IM) SURGICAL PROCEDURE Introduction Page >> 04 Rationale Page >> 05 Preoperative Planning Page >> 07 Patient Preparation
unicompartmental knee SURGICAL TECHNIQUE limacorporate.com Index INTRAMEDULLARY (IM) SURGICAL PROCEDURE Introduction Page >> 04 Rationale Page >> 05 Preoperative Planning Page >> 07 Patient Preparation
1. Pre-Operative Planning Skin Incision and Arthrotomy
 Stage of Operation 1. Pre-Operative Planning --------------------------1 2. Skin Incision and Arthrotomy ------------------1 3. Femoral valgus angle confirmation ------------2 4. Distal Femur Cutting -----------------------------3
Stage of Operation 1. Pre-Operative Planning --------------------------1 2. Skin Incision and Arthrotomy ------------------1 3. Femoral valgus angle confirmation ------------2 4. Distal Femur Cutting -----------------------------3
Anterior Cut First Surgical Technique
 Anterior Cut First Surgical Technique GENESIS II Anterior Cut First Surgical Technique Table of Contents Introduction....................................... 2 Preop Planning....................................
Anterior Cut First Surgical Technique GENESIS II Anterior Cut First Surgical Technique Table of Contents Introduction....................................... 2 Preop Planning....................................
Triathlon Knee System Universal Baseplate Surgical Protocol
 Triathlon Knee System Universal Baseplate Surgical Protocol Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments... 2 Introduction... 2 Assembly Instructions...
Triathlon Knee System Universal Baseplate Surgical Protocol Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments... 2 Introduction... 2 Assembly Instructions...
Uniglide. Unicompartmental Knee Replacement Mk III surgical technique
 Uniglide Unicompartmental Knee Replacement Mk III surgical technique Uniglide Contents Operative summary 4 Pre-operative assessment 6 Preparation 7 Incision 7 Approach 7 Medial procedure 8 Tibial preparation
Uniglide Unicompartmental Knee Replacement Mk III surgical technique Uniglide Contents Operative summary 4 Pre-operative assessment 6 Preparation 7 Incision 7 Approach 7 Medial procedure 8 Tibial preparation
Zimmer Unicompartmental High Flex Knee. Intramedullary, Spacer Block Option and Extramedullary Minimally Invasive Surgical Techniques
 Zimmer Unicompartmental High Flex Knee Intramedullary, Spacer Block Option and Extramedullary Minimally Invasive Surgical Techniques ZIMMER UNICOMPARTMENTAL HIGH FLEX KNEE INTRAMEDULLARY, SPACER BLOCK
Zimmer Unicompartmental High Flex Knee Intramedullary, Spacer Block Option and Extramedullary Minimally Invasive Surgical Techniques ZIMMER UNICOMPARTMENTAL HIGH FLEX KNEE INTRAMEDULLARY, SPACER BLOCK
Zimmer Unicompartmental High Flex Knee. Spacer Block Surgical Technique
 Zimmer Unicompartmental High Flex Knee Spacer Block Surgical Technique INTRO Zimmer Unicompartmental High Flex Knee Spacer Block Surgical Technique Introduction Unicompartmental knee arthroplasty (UKA)
Zimmer Unicompartmental High Flex Knee Spacer Block Surgical Technique INTRO Zimmer Unicompartmental High Flex Knee Spacer Block Surgical Technique Introduction Unicompartmental knee arthroplasty (UKA)
Resurfacing Distal Femur. Orthopaedic Salvage System
 Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
PIN GUIDE SYSTEM SURGICAL TECHNIQUE. with the SIGMA High Performance Instruments System. This publication is not intended for distribution in the USA.
 PIN GUIDE SYSTEM with the SIGMA High Performance Instruments System This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Pin Guide Surgical Technique The following steps are
PIN GUIDE SYSTEM with the SIGMA High Performance Instruments System This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Pin Guide Surgical Technique The following steps are
NexGen Complete Knee Solution. Cruciate Retaining (CR) and Revision Instrumentation Surgical Technique for Cruciate Retaining Augmentable (CRA) Knees
 NexGen Complete Knee Solution Cruciate Retaining (CR) and Revision Instrumentation Surgical Technique for Cruciate Retaining Augmentable (CRA) Knees INTRODUCTION This surgical technique document combines
NexGen Complete Knee Solution Cruciate Retaining (CR) and Revision Instrumentation Surgical Technique for Cruciate Retaining Augmentable (CRA) Knees INTRODUCTION This surgical technique document combines
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
S U R G I C A L T E C H N I Q U E David A. McQueen, MD Return to Menu
 S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
Zimmer NexGen Tibial Stem Extension & Augmentation. Surgical Technique IMAGE TO COME. Stem Extensions and Augments
 Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique IMAGE TO COME Stem Extensions and Augments Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique 1 Zimmer NexGen Tibial
Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique IMAGE TO COME Stem Extensions and Augments Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique 1 Zimmer NexGen Tibial
Unicondylar Surgical Technique
 Unicondylar Surgical Technique Contents Indications, Contra-indications and X-ray Templating 2 Approach and Exposure 3 Proximal Tibial Resection 4 Tibial Jig Alignment 6 Tibial Sizing 9 Balancing 10 Distal
Unicondylar Surgical Technique Contents Indications, Contra-indications and X-ray Templating 2 Approach and Exposure 3 Proximal Tibial Resection 4 Tibial Jig Alignment 6 Tibial Sizing 9 Balancing 10 Distal
Triathlon TS Knee System. Surgical Protocol
 Triathlon TS Knee System Surgical Protocol Triathlon TS Knee System Surgical Protocol Table of Contents Acknowledgments..........................................................2 Exposure...................................................................4
Triathlon TS Knee System Surgical Protocol Triathlon TS Knee System Surgical Protocol Table of Contents Acknowledgments..........................................................2 Exposure...................................................................4
BIOTECH FUTURE KNEE Minimal Invasive (and classic) Surgical Technique
 BIOTECH FUTURE KNEE Minimal Invasive (and classic) Surgical Technique Page No. Product description 2. Pre-operational planning 3. 1st step Femoral resection 4. P/S Femoral component 7. 2nd step Proximal
BIOTECH FUTURE KNEE Minimal Invasive (and classic) Surgical Technique Page No. Product description 2. Pre-operational planning 3. 1st step Femoral resection 4. P/S Femoral component 7. 2nd step Proximal
Zimmer NexGen MIS Tibial Component. Cemented Surgical Technique IMAGE TO COME
 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Persona The Personalized Knee. Surgical Technique
 Persona The Personalized Knee Surgical Technique Table of Contents Introduction... 2 Constraint Options Preoperative Planning Surgical Approach Patient Preparation Magnet Usage Symbols Screw/Pin Information
Persona The Personalized Knee Surgical Technique Table of Contents Introduction... 2 Constraint Options Preoperative Planning Surgical Approach Patient Preparation Magnet Usage Symbols Screw/Pin Information
MRH Knee System Modular Peg Baseplate Surgical Protocol
 MRH Knee System Modular Peg Baseplate Surgical Protocol Using Monogram IM Revision Instruments 4 N 4 N Modular Rotating Hinge Knee System Using Monogram IM Revision Instruments Mr C R Howie FRCS Consultant
MRH Knee System Modular Peg Baseplate Surgical Protocol Using Monogram IM Revision Instruments 4 N 4 N Modular Rotating Hinge Knee System Using Monogram IM Revision Instruments Mr C R Howie FRCS Consultant
MIS Cemented Tibial Component
 MIS Cemented Tibial Component NexGen Complete Knee Solution Surgical Technique Table of Contents Surgical Exposure... 2 Finish the Tibia... 2 Position Based on Anatomic Landmarks... 3 Lateral Posterior
MIS Cemented Tibial Component NexGen Complete Knee Solution Surgical Technique Table of Contents Surgical Exposure... 2 Finish the Tibia... 2 Position Based on Anatomic Landmarks... 3 Lateral Posterior
NEXGEN COMPLETE KNEE SOLUTION S A. Tibial Stem Extension & Augmentation Surgical. ATechnique
 NEXGEN COMPLETE KNEE SOLUTION ATechnique Tibial Stem Extension & Augmentation Surgical INTRODUCTION The NexGen Complete Knee Solution Intramedullary Tibial Instruments have been designed to provide an
NEXGEN COMPLETE KNEE SOLUTION ATechnique Tibial Stem Extension & Augmentation Surgical INTRODUCTION The NexGen Complete Knee Solution Intramedullary Tibial Instruments have been designed to provide an
Triathlon with Single-Use Instrumentation Optimize Your TKA Experience. Posterior Referencing Surgical Protocol
 Triathlon with Single-Use Instrumentation Optimize Your TKA Experience Posterior Referencing Surgical Protocol Introduction............................................................2 Assembly Instructions...................................................6
Triathlon with Single-Use Instrumentation Optimize Your TKA Experience Posterior Referencing Surgical Protocol Introduction............................................................2 Assembly Instructions...................................................6
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer
 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Minimally Invasive Surgical Techniques for the Medial Compartment. Intramedullary, Spacer Block and Extramedullary techniques
 Minimally Invasive Surgical Techniques for the Medial Compartment Intramedullary, Spacer Block and Extramedullary techniques Unicompartmental High Flex Knee Intramedullary, Spacer Block and Extramedullary
Minimally Invasive Surgical Techniques for the Medial Compartment Intramedullary, Spacer Block and Extramedullary techniques Unicompartmental High Flex Knee Intramedullary, Spacer Block and Extramedullary
FOREWORD PRESERVATION UNICOMPARTMENTAL KNEE SYSTEM
 Surgical Technique FOREWORD PRESERVATION UNICOMPARTMENTAL KNEE SYSTEM Our surgeon design team first implanted the Preservation Unicompartmental Knee System in 2001. The system was developed with over
Surgical Technique FOREWORD PRESERVATION UNICOMPARTMENTAL KNEE SYSTEM Our surgeon design team first implanted the Preservation Unicompartmental Knee System in 2001. The system was developed with over
NexGen Intramedullary Instrumentation. Surgical Technique
 NexGen Intramedullary Instrumentation Surgical Technique Table of Contents Introduction... 2 Preoperative Planning... 2 Surgical Technique... 3 Step One: Size the Femur/Establish External Rotation...
NexGen Intramedullary Instrumentation Surgical Technique Table of Contents Introduction... 2 Preoperative Planning... 2 Surgical Technique... 3 Step One: Size the Femur/Establish External Rotation...
Contact your Zimmer representative or visit us at
 Please refer to the package inserts for complete product information, including contraindications, warnings, precautions, and adverse effects. Contact your Zimmer representative or visit us at www.zimmer.com
Please refer to the package inserts for complete product information, including contraindications, warnings, precautions, and adverse effects. Contact your Zimmer representative or visit us at www.zimmer.com
Constrained Posterior Stabilized (CPS)
 Constrained Posterior Stabilized (CPS) Persona The Personalized Knee Surgical Technique Table of Contents Introduction... 2 Constraint Options Initial Knee Assessment... 3 Femoral Box Cut CPS Tibial Bearing
Constrained Posterior Stabilized (CPS) Persona The Personalized Knee Surgical Technique Table of Contents Introduction... 2 Constraint Options Initial Knee Assessment... 3 Femoral Box Cut CPS Tibial Bearing
INSTRUMENTS. Measured Resection Classic Surgical Technique
 INSTRUMENTS Measured Resection Classic Surgical Technique RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to knee arthroplasty that places equal importance on recovery, function and survivorship.
INSTRUMENTS Measured Resection Classic Surgical Technique RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to knee arthroplasty that places equal importance on recovery, function and survivorship.
Constrained Posterior Stabilized (CPS) Surgical Technique
 Constrained Posterior Stabilized (CPS) Surgical Technique Constrained Posterior Stabilized (CPS) Surgical Technique INTRO Introduction The Constrained Posterior Stabilized (CPS) articular surfaces can
Constrained Posterior Stabilized (CPS) Surgical Technique Constrained Posterior Stabilized (CPS) Surgical Technique INTRO Introduction The Constrained Posterior Stabilized (CPS) articular surfaces can
Total Knee Replacement
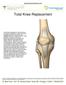 Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
The ACL-PCL Substituting Knee. BioFoam Tibial Bases. Surgical Technique For Cementless Tibial Fixation
 The CL-PCL Substituting Knee BioFoam Surgical Technique For Cementless Tibial Fixation Surgical techniques and instrument recommendations were provided by: Michael nderson, MD Milwaukee, WI G. Lynn Rasmussen,
The CL-PCL Substituting Knee BioFoam Surgical Technique For Cementless Tibial Fixation Surgical techniques and instrument recommendations were provided by: Michael nderson, MD Milwaukee, WI G. Lynn Rasmussen,
NexGen Trabecular Metal Tibial Tray. Surgical Technique
 NexGen Trabecular Metal Tibial Tray Surgical Technique Table of Contents Surgical Technique...2 Resect the Tibia...2 Finish the Tibia...2 Position Based Anatomic Landmarks...3 Position Based on Trial
NexGen Trabecular Metal Tibial Tray Surgical Technique Table of Contents Surgical Technique...2 Resect the Tibia...2 Finish the Tibia...2 Position Based Anatomic Landmarks...3 Position Based on Trial
Table of Contents. Step One: Locate Medullary Canal 4 Step Two: Prepare Femur 4. Step Three: Size Femur 5. Step Four: Prepare Tibia 5
 Zimmer Natural-Knee Unicompartmental MIS Intramedullary Surgical Technique Zimmer MIS Surgical Technique for Unicompartmental Knee Arthroplasty Developed in conjunction with Aaron A. Hofmann, MD Professor
Zimmer Natural-Knee Unicompartmental MIS Intramedullary Surgical Technique Zimmer MIS Surgical Technique for Unicompartmental Knee Arthroplasty Developed in conjunction with Aaron A. Hofmann, MD Professor
Zimmer MIS Intramedullary Instrumentation
 Zimmer MIS Intramedullary Instrumentation Surgical Technique For NexGen Cruciate Retaining & NexGen Legacy Posterior Stabilized Knees Zimmer MIS Intramedullary Instrumentation Surgical Technique Surgical
Zimmer MIS Intramedullary Instrumentation Surgical Technique For NexGen Cruciate Retaining & NexGen Legacy Posterior Stabilized Knees Zimmer MIS Intramedullary Instrumentation Surgical Technique Surgical
Wichita Fusion Nail Surgical Technique. David A. McQueen, MD
 Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
SIGMA High Performance Partial Knee. Unicondylar. Surgical Technique
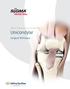 SIGMA High Performance Partial Knee Unicondylar Surgical Technique Table of Contents Surgical Technique X-ray Templating 3 Approach and Exposure 4 Proximal Tibial Resection 5 Tibial Jig Alignment 7 Tibial
SIGMA High Performance Partial Knee Unicondylar Surgical Technique Table of Contents Surgical Technique X-ray Templating 3 Approach and Exposure 4 Proximal Tibial Resection 5 Tibial Jig Alignment 7 Tibial
RESECTION GUIDE SYSTEM. TRUMATCH Personalized Solutions Surgical Technique with ATTUNE Knee INTUITION Instruments
 RESECTION GUIDE SYSTEM TRUMATCH Personalized Solutions Surgical Technique with ATTUNE Knee INTUITION Instruments RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the ATTUNE Knee
RESECTION GUIDE SYSTEM TRUMATCH Personalized Solutions Surgical Technique with ATTUNE Knee INTUITION Instruments RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the ATTUNE Knee
Single Axis Revision Knee System
 Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical Protocol Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical
Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical Protocol Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical
Triathlon Tritanium. Surgical Protocol. with Triathlon Cementless Beaded PA Femoral Component
 Triathlon Tritanium Surgical Protocol with Triathlon Cementless Beaded PA Femoral Component Triathlon Tritanium Surgical Protocol with Triathlon Cementless Beaded PA Femoral Component Description...............................
Triathlon Tritanium Surgical Protocol with Triathlon Cementless Beaded PA Femoral Component Triathlon Tritanium Surgical Protocol with Triathlon Cementless Beaded PA Femoral Component Description...............................
Trabecular Metal Primary Patella
 Trabecular Metal Primary Patella NexGen Complete Knee Solution Surgical Technique Table of Contents Introduction... 2 Prepare the Patella... 2 Patella Reamer Technique... 3 Insetting Technique... 5 Universal
Trabecular Metal Primary Patella NexGen Complete Knee Solution Surgical Technique Table of Contents Introduction... 2 Prepare the Patella... 2 Patella Reamer Technique... 3 Insetting Technique... 5 Universal
INTUITION INSTRUMENTS SURGICAL TECHNIQUE
 INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System Family of Knee Implants with the INTUITION Instrumentation.
INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System Family of Knee Implants with the INTUITION Instrumentation.
FLH /11
 FLH 225 04/11 This publication has been issued by: European Central Marketing Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel: +44 (0)1656 655221 Fax: +44 (0)1656 645454 www.biomet.com
FLH 225 04/11 This publication has been issued by: European Central Marketing Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel: +44 (0)1656 655221 Fax: +44 (0)1656 645454 www.biomet.com
Surgical Technique. Hinge Disassembly and Rebuild Technique
 Surgical Technique Hinge Disassembly and Rebuild Technique Revision Knee Arthroplasty Surgical Technique LEGION HK Hinge Knee System Introduction The LEGION HK Hinge Knee System has been designed as an
Surgical Technique Hinge Disassembly and Rebuild Technique Revision Knee Arthroplasty Surgical Technique LEGION HK Hinge Knee System Introduction The LEGION HK Hinge Knee System has been designed as an
SCORE Revision. Revision Total Knee Arthroplasty Cemented. Surgical Technique With Conventional Instrumentation Primary cases
 SCORE Revision Revision Total Knee Arthroplasty Cemented Surgical Technique With Conventional Instrumentation Primary cases SCORE REVISION FOR PRIMARY CASES The SCORE Revision is a revision total knee
SCORE Revision Revision Total Knee Arthroplasty Cemented Surgical Technique With Conventional Instrumentation Primary cases SCORE REVISION FOR PRIMARY CASES The SCORE Revision is a revision total knee
Signature Personalized Patient Care*
 Signature Personalized Patient Care* Surgical Technique Addendum Vanguard Complete Knee System One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care
Signature Personalized Patient Care* Surgical Technique Addendum Vanguard Complete Knee System One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care
Zenith. Total Ankle Replacement Surgical technique
 Total Ankle Replacement Surgical technique Contents Operative summary 4 Pre-operative planning and templating 6 Patient positioning 6 Exposure 6 Saw blades 7 Joint line definition 7 Tibial alignment jig
Total Ankle Replacement Surgical technique Contents Operative summary 4 Pre-operative planning and templating 6 Patient positioning 6 Exposure 6 Saw blades 7 Joint line definition 7 Tibial alignment jig
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Pin Guide System SURGICAL TECHNIQUE PIN GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA High Performance
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Pin Guide System SURGICAL TECHNIQUE PIN GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA High Performance
INTUITION INSTRUMENTS SURGICAL TECHNIQUE
 INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System Family of Knee Implants with the INTUITION Instrumentation.
INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System Family of Knee Implants with the INTUITION Instrumentation.
A novel cementless option. Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
 A novel cementless option Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique Zimmer Trabecular Metal Primary Patella 1 Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
A novel cementless option Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique Zimmer Trabecular Metal Primary Patella 1 Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Zimmer NexGen LPS-Flex Mobile and LPS-Mobile Bearing Knees. Surgical Technique United States Version IMAGE TO COME
 Zimmer NexGen LPS-Flex Mobile and LPS-Mobile Bearing Knees Surgical Technique United States Version IMAGE TO COME Zimmer NexGen LPS-Flex Mobile and LPS-Mobile Bearing Knees Surgical Technique 1 Zimmer
Zimmer NexGen LPS-Flex Mobile and LPS-Mobile Bearing Knees Surgical Technique United States Version IMAGE TO COME Zimmer NexGen LPS-Flex Mobile and LPS-Mobile Bearing Knees Surgical Technique 1 Zimmer
Patella Planing System
 REFERENCE GUIDE AND SURGICAL TECHNIQUE Patella Planing System SPECIALIST INSTRUMENTS AN ONLAY PATELLA PREPARATION SYSTEM TECHNIQUE FOR PRIMARY PATELLAR RESURFACING The Specialist 2 Patellar Planer System
REFERENCE GUIDE AND SURGICAL TECHNIQUE Patella Planing System SPECIALIST INSTRUMENTS AN ONLAY PATELLA PREPARATION SYSTEM TECHNIQUE FOR PRIMARY PATELLAR RESURFACING The Specialist 2 Patellar Planer System
ZIMMER NEXGEN CRUCIATE RETAINING (CR) AND LEGACY KNEE POSTERIOR STABILIZED (LPS) TRABECULAR METAL MONOBLOCK TIBIAS. Surgical Technique Addendum
 ZIMMER NEXGEN CRUCIATE RETAINING (CR) AND LEGACY KNEE POSTERIOR STABILIZED (LPS) TRABECULAR METAL MONOBLOCK TIBIAS Surgical Technique Addendum SURGICAL TECHNIQUE FOR NEXGEN CRUCIATE RETAINING (CR) AND
ZIMMER NEXGEN CRUCIATE RETAINING (CR) AND LEGACY KNEE POSTERIOR STABILIZED (LPS) TRABECULAR METAL MONOBLOCK TIBIAS Surgical Technique Addendum SURGICAL TECHNIQUE FOR NEXGEN CRUCIATE RETAINING (CR) AND
Triathlon Knee System. Anterior Referencing Surgical Protocol
 Triathlon Knee System Anterior Referencing Surgical Protocol Triathlon Knee System Anterior Referencing Surgical Protocol Table of Contents Acknowledgments..........................................................2
Triathlon Knee System Anterior Referencing Surgical Protocol Triathlon Knee System Anterior Referencing Surgical Protocol Table of Contents Acknowledgments..........................................................2
Proven Gen-Flex Revision Knee System. Surgical Protocol
 Proven Gen-Flex Revision Knee System Surgical Protocol Proven Gen-Flex Revision Knee System Surgeon Design Team The Proven Gen-Flex Revision Knee System Instrumentation and Surgical Protocol were developed
Proven Gen-Flex Revision Knee System Surgical Protocol Proven Gen-Flex Revision Knee System Surgeon Design Team The Proven Gen-Flex Revision Knee System Instrumentation and Surgical Protocol were developed
Inspiring people, Enriching lives
 TM Inspiring people, Enriching lives Encore Medical, L.P. 9800 Metric Blvd. Austin, Texas 78758 512-832-9500 www.encoremed.com Encore Medical, L.P. Cat. # 0152-017 2.5k/rev. A Encore and Foundation are
TM Inspiring people, Enriching lives Encore Medical, L.P. 9800 Metric Blvd. Austin, Texas 78758 512-832-9500 www.encoremed.com Encore Medical, L.P. Cat. # 0152-017 2.5k/rev. A Encore and Foundation are
NexGen LPS Fixed Bearing Knee. Surgical Technique
 NexGen LPS Fixed Bearing Knee Surgical Technique Table of Contents Introduction...2 Preoperative Planning...2 Surgical Technique...3 Step One: Align the Tibia...3 MICRO-MILL Hand Piece Assembly and Usage
NexGen LPS Fixed Bearing Knee Surgical Technique Table of Contents Introduction...2 Preoperative Planning...2 Surgical Technique...3 Step One: Align the Tibia...3 MICRO-MILL Hand Piece Assembly and Usage
Surgical Technique Final Trial Reduction and Component Implantation of
 Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Mobile Bearing TC-PLUS PRIMARY Mobile Bearing Final Trial Reduction and Component Implantation of
Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Mobile Bearing TC-PLUS PRIMARY Mobile Bearing Final Trial Reduction and Component Implantation of
Trabecular Metal Femoral Component. Surgical Technique
 Trabecular Metal Femoral Component Surgical Technique INTRO Trabecular Metal Femoral Component Surgical Technique Introduction The Persona Trabecular Metal Femoral Component is designed to unite stable
Trabecular Metal Femoral Component Surgical Technique INTRO Trabecular Metal Femoral Component Surgical Technique Introduction The Persona Trabecular Metal Femoral Component is designed to unite stable
LCS COMPLETE SURGICAL TECHNIQUE. MILESTONE Instruments with MBT Tray Preparation
 LCS COMPLETE MILESTONE Instruments with MBT Tray Preparation SURGICAL TECHNIQUE CONTENTS Preface 2 Surgical Concepts 3 Instruments 4 Surgical Technique Summary 6 Surgical Technique 8 Preparation 8 Incision
LCS COMPLETE MILESTONE Instruments with MBT Tray Preparation SURGICAL TECHNIQUE CONTENTS Preface 2 Surgical Concepts 3 Instruments 4 Surgical Technique Summary 6 Surgical Technique 8 Preparation 8 Incision
Surgical Technique Final Trial Reduction and Component Implantation of
 Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Fixed Bearing TC-PLUS PRIMARY Fixed Bearing Final Trial Reduction and Component Implantation of
Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Fixed Bearing TC-PLUS PRIMARY Fixed Bearing Final Trial Reduction and Component Implantation of
