Supraclavicular approach for outlet decompression. thoracic. Linda M. Reilly, MD, and Ronald J. Stoney, MD, San Francisco, Calif.
|
|
|
- Suzanna Perkins
- 6 years ago
- Views:
Transcription
1 Supraclavicular approach for outlet decompression thoracic Linda M. Reilly, MD, and Ronald J. Stoney, MD, San Francisco, Calif. Supraclavicular decompression of the thoracic outlet was performed in 40 patients with symptoms arising from brachial plexus compression and irritation. Both osseous and soft tissue structures responsible for this nerve compression were identified and removed without significant neurologic morbidity despite a 25% incidence of secondary operative procedures in this series. The cure or improvement rate matched what we previously reported for combined transaxillary and supraclavicular approach. Further follow-up will auow a determination of the durability of this technique, which, ff acceptable, will justify a confident recommendation for its adoption in patients having thoracic outlet decompression. (J VASC SURG 1988;8: ) Mechanical compression of the brachial plexus within the thoracic outlet is considered the principal cause of neurologic complaints in symptomatic patents. Although there is no consensus regarding a treatment plan, conservative measures are usually initiated, reserving surgical decompression for patients whose treatment fails or whose conditions worsen. Among the varied operative approaches and techniques advocated, _transaxillary resection of the first rib is the most popular. 1 Symptomatic recurrence caused by fibrotic encasement of the plexus trunks and reattachment of the scalene muscle to the first rib bed prompted our use of a combined transaxillary rib resection and supraclavicular radical scalenectomy with improved results? Continued experience has convinced us that the safe exposure of the first rib can be regularly achieved by means of the supraclavicular approach alone. In addition to resection of the first rib, scalenectomy and precise identification and removal of osseous and myofascial abnormalities are simplified with this approach. This article describes our technique and the results achieved in 41 supraclavicular thoracic outlet decompressions in 40 consecutive patients treated at the University of California Medical Center, San Francisco. From the Department of Surgery, University of California, San Francisco. Supported in part by the Pacific Vascular Research Foundation, San Francisco, Calif. Presented at the Second Annual Meeting of the Western Vascular Society, Tucson, Ariz., Jan , Reprint requests: Ronald J. Stoney, MD, Dept. of Surgery, Vascular Surgery, M-488, University of California, San Francisco, 505 Parnassus Ave., San Francisco, CA PATIENTS AND METHODS During the past three years 36 women and four men ranging in age from 18 to 66 years (mean 37 years) had 41 supraclavicular thoracic outlet decompressions to relieve pain and paresthesia mediated through the roots of the brachial plexus. Five additional patients with symptoms arising from compression of the subclavian artery (four patients) or subclavian vein (one patient) also had surgery with an identical supraclavicular approach. However, these patients required either arterial repair or venous decompression and will not be considered in this article. The left upper extremity was the site of neurologic complaint in 22 patients, slightly more than half of the group. In 10 instances, 25%, the procedure was a second operation. The original thoracic outlet decompression that failed was a transaxillary first rib resection in nine patients and a supraclavicular scalenectomy in one patient. A history of cervicothoracic trauma, usually involving a hyperextension force, preceded the onset of symptoms in half of our patients (n = 20). The duration of symptoms ranged from 5 months to 13 years (mean 3 years) before operation. In 30 patients, a supervised conservative treatment program involving analgesics, muscle relaxants, physical therapy, exercise, and occasionally chiropractic, acupuncture, or biofeedback adjuncts had failed to produce sustained improvement. Five patients had no conservative treatment whereas in six others sporadic attempts or undefined nonoperative treatment were noted. Although the pattern of symptoms varied, several consistent features were (1) pain involving the lateral 329
2 330 Reilly and Stoney Journal of VASCULAR SURGERY fa Middle Scaler Nuacle Co~ThoTacic N~Yv~ Fig. 1. Artist's illustration of early stage of right thoracic outlel: decompression. Note the self-retaining retractor. Fat pad is retracted to expose brachial plexus. A~teyior 9calene (cut) ~U l Fig. 3. Illustrated detail of sagittal saw division of neck of first rib. Dong thoracic nerve course parallel and caudad to transected middle scalene is seen. #ll& L 0 ~ ~ I N~.Yv~ t~racl~ Plexu Clgvic: 5uloclav: Arte~'y j~iddl~ Mctscl~ Lo~ T~ NcYv Brachial Clav}cl.C. Fig. 2. Artist's illustration of decompression landmarks, site of retraction of anterior scalene, partial resection of middle scalene muscle and first rib. Transection site (dotted line). Brachial plexus and artery are seen. Medial clavicle and part of subclavian vein are removed for illustrative purposes. R.C.C., Right common carotid artery. neck, shoulder, parascapular region, and upper extrernil~, and (2) paresthesia principally affecting the arm, hand, and fingers. These two principal complaints were brought on or intensified by the use of the ipsilateral arm in extended, elevated, or overhead positions. Ipsilateral headache, facial pain, or both were present in 17 patients (42.5%). Pertinent physical findings were 5ubc]a\ Artery ~b Z ~ Fig. 4. Thoracic outlet decompression shows the relaxed, nonstretched portion of the third division of the brachial plexus nearly contacting the second thoracic rib. Medial clavicle is removed for illustrative purposes. direct tenderness over the brachial plexus, trapezius muscle spasm, and the reproduction or intensification of neurologic symptoms by hyperabduction maneuvers or the elevated arm stress test (EAST). Preoperative evaluation usually included orthopedic and neurologic consultation as well as roent-
3 Volume 8 Number 3 September 1988 Supradavicular decompression of the thoracic outlet 331 genograms of the chest and cervical spine, Nerve conduction studies were used specifically when nerve entrapment at the wrist or elbow was suspected. Myelography, computed tomography, and more recently magnetic resonance imaging have been used to evaluate suspected cervical disk disease. OPERATIVE TECHNIQUE The patient is placed in a semi-fowler position with the head rotated away from the operative side. An incision is made two finger breadths above the davicle, beginning over the clavicular head of the sternocleidomastoid muscle. The incision is carried laterally and posteriorly in a gentle curve for a distance of approximately 10 cm. The platysma is incised and flaps are developed superiorly, to the level of the cricoid cartilage and inferiorly, to the clavicle. The scalene fat pad is mobilized inferiorly, medially, and superiorly and then reflected on a laterally based pedicle (Fig. 1). The clavicular head of the sternocleidomastoid muscle is divided when necessary to gain medial exposure to the lateral edge of the internal jugular vein. The phrenic nerve is mobilized from the adjacent fascia of the anterior scalene muscle and retracted medially. The insertion of the muscle is detached from its tubercle on the first rib. The muscle is elevated to visualize the subclavian artery and the trunks of the brachial plexus. The origins of the anterior scalene muscle are divided from the transverse processes of the upper cervical vertebrae. Any muscle fibers that interdigitate with the middle scalene muscle between the roots of the brachial plexus are now divided and the anterior scalene muscle is then removed. Gentle anterior displacement of the brachial plexus trunks allows their separation from the anterior surface of the middle scalene muscle. The lateral border of the middle scalene muscle is freed and the point of emergence of the long thoracic nerve is identiffed. This point serves to identify the level for middie scalene muscle transection to expose the neck of the first rib (Fig. 2). A sagittal air-drive saw is used to divide the rib posteriorly, while the lower trunk of the plexus is gently displaced anteromedially (Fig. 3). The lateral border of the middle scalene muscle and the first rib are mobilized and the intercostal muscle between the first and second rib as well as the posterior scalene muscle are now divided. Next the trtmks of the plexus are elevated and the medial border of the first rib is freed. The subclavian artery is displaced caudally, which further exposes the course of the first rib. Anomalous myofascial bands Table I. Abnormalities and anomalies No. Scar 13 Osseous anomalies 22 First rib 8 Cervical rib 10 C-7 transverse process 3 Pseudarthrosis 1 Myofascial abnormalities 66 Muscle 44 Fibrous bands 22 that insert on the rib are now identified and resected. Blunt finger dissection inferior to the first rib separates it from the subjacent pleura, which can then be displaced inferiorly. The final dissection of the anterior first rib requires elevation and retraction of the clavicle and the lateral displacement of the trunks of the brachial plexus and subclavian artery. The rib is then divided with a sagittal saw beyond the anterior scalene tubercle (Fig. 3). It is now gently freed of any other attachments and removed from beneath the neurovascular structures. The course of the five roots of the plexus and their fusion into three cords is inspected and any scar tissue or residual muscle fibers are removed by thorough neurolysis. The neurovascular structures lay loosely in the enlarged thoracic outlet (Fig. 4). Should the proximal rib stump impinge on ~the upward course of the first thoracic nerve root, a rongeur is used to resect additional bone from the medial corner of the remnant rib. The mobilized prescalene fat pad is now split into two leaves, which are positioned loosely to surround the trunks of the brachial plexus. This provides a soft fibrous fatty insulating collar to protect the delicate nerve roots. The clavicular head of the sternocleidomastoid muscle and platysma are reapproximated and the skin is closed with a subcuticular suture. If lung inflation shows a plcural defect, a soft catheter is placed through the wound into the pleural cavity before closure. The chest is evacuated by aspiration and the catheter is withdrawn from the closed wound before the bandage is affixed. A portable chest roentgcnograrn in the recovery room will usually show a reexpanded lung or very small apical density or pneumothorax. Any pneumothorax greater than 20% can be evacuated easily with a plastic catheter inserted anteriorly through the third intercostal space. After recovery from anesthesia the patient is allowed unrestricted activity with full range of motion of the major joints of the affected extremity. The patient is usually discharged by the third postoperative day.
4 332 Reilly and Stoney Journal of VASCULAR SURGERY Table II. Thoracic outlet decompressive procedures Scalenectomy Rib resection Neurolysis No. Anterior and middle First rib Brachial plexus 31 ~ Anterior and middle Cervical rib Brachial plexus 6 Anterior and middle First and cervical rib Brachial plexus 2 Anterior Cervical rib Brachial plexus 2 Cervical sympathectomy (one patient). Table III. Follow-up intervals with mtmber of patients at each interval Interval (too) No. < >24 4 OPERATIVE FINDINGS The supraclavicular approach provides unrestricted exposure to the course of the first thoracic rib, the interscalene triangle, and the osseous and musculofascial abnormalities found in this region. Many patients had more than one abnormality noted. The scalene minimus, considered by some authors to be a normal anatomic variant, was noted in 17 patients (42%). Excluding this finding, the mean number of anomalies was 2.5 for the entire group (Table I). These included fibrosis or scarring along the posterior border of the anterior scalene muscle, the anomalous bands overlying the lower roots of the plexus, or a reattachment of the previously divided anterior scalene tendon to the first rib bed after a prior transaxillary rib resection. Osseous abnormalities included a cervical rib in 10 patients, a broad first thoracic rib in eight patients, and an elongated transw:rse process of the seventh cervical vertebra in three patients. Myofascial abnormalities were frequent. Hypertrophy of the anterior scalene muscle (nine patients) was observed in overdeveloped persons who had usually pursued a vigorous muscular development (power-lifting) program. The resected first rib with intact middle scalene muscle insertion provided a specimen to assess the pattern of muscular insertion. A frequent finding was a broad, anteriorly displaced insertion of this muscle that abutted the posterior aspect of the anterior scalene tubercle. The operative procedures required to decompress the thoracic outlet are listed in Table II. As can be seen, the most common procedure used was anterior and subtotal middle scalenectomy and first thoracic rib resection with brachial plexus neurolysis (31 procedures). In 10 procedures, a cervical rib was encountered and resected either alone (eight procedures) or in conjunction with the first thoracic rib (two patients). RESULTS This group of patients were all operated on within the past 30 months. Thirty-eight patients have been personally examined between 1 and 30 months postoperatively (mean 10 months) (Table III). Symptoms were assessed with a scoring system to attempt to objectify the results. The scoring system form is described in Table IV. If all of the preoperative symptoms were consistently relieved, the patients were cured. If greater than 75% of the preoperative symptoms were consistently relieved on follow-up, the patients were classified as markedly improved. Fifty to seventy-five percent preoperative symptomatic relief was considered improved and anything less than that was considered unchanged. Only three patients were believed to be unchanged after operation (8%), 13 patients were cured, 10 patients were markedly improved, and 13 were improved. No patient was worse after this operative approach. Complications. Many patients had some complications of their supraclavicular decompression procedure. Most were minor, involved the wound, and nearly all resolved before hospital discharge. A pneumothorax occurred during 33 of 41 procedures; however, in only half was a chest tube temporarily required as the remainder were evacuated in the operating room. Mild brachial plexus traction palsy was noted in five patients postoperatively. This was transient in all, was substantially improved by discharge, and was completely resolved within 3 months after operation. One patient had a subclavian venous injury repaired and another had a self-limited chylothorax. These patients both had a prior thoracic outlet decompression. One patient had a winged scapula
5 Volume 8 Number 3 September 1988 SupracIavicular decompression of the thoracic outlet 333 Table IV. The supraclavicular thoracic outlet syndrome decompression quantitative symptom assessment form Pain Rest Motion Paresthesia Rest Motion Weakness Reduced motion Headache Neck Shoulder Scapula Thorax Arm Hand Yes No NOTE: One was completed for each patient before operation and at each assessment interval after operation. resulting from a long thoracic nerve injury. Phrenic nerve dysfunction was not specifically evaluated, but in 10% of patients, an elevated ipsilateral hemidiaphragm was noted on postoperative chest x-ray films. Only one patient had persistent mild elevation of the left hemidiaphragm with atypical chest pain and shortness of breath. One patient had minimal ptosis and miosis without the other components of Horner's syndrome. DISCUSSION The factors responsible for brachial plexus compression within the thoracic outlet are multiple. Furthermore, no symptom pattern, physical findings, or electrodiagnostic test can reliably predict the anatomic findings in any individual case. It is obvious from this patient group, that congenital myofibrous and osseous anomalies are frequent and, when combined with acquired structural changes, averaged 2.5 findings per operated patient. Most osseous abnormalities are in the neck itself whereas the muscular anomalies and acquired structural changes are superior to the first rib, involving the scalene triangle and the interroot spaces themselves. None is easily visualized without a thorough anterior scalenectomy 3 and gentle exposure of the roots and trunks of the brachial plexus itself. The transaxillary approach involves a deep narrow exposure and limited visualization of structures cephalad to the superior aspect of the first rib. It cannot reliably and safely permit the precise identification, let alone the resection of, complex anomalies in juxtaposition to the course of the delicate nerve structures themselves. The importance of abnormal and structurally normal-appearing scalene muscle in neurogenic thoracic outlet syndromes has been recognized for half a century. 4's Naffziger and Grant 6 described the scalene anticus syndrome. It was postulated that a chronically contracting, taut anterior scalene muscle elevated the first rib compressing the plexus against the underside of the clavicle. 7 No histopathologic analysis of the anterior scalene muscle in symptomatic patients was obtainable until recently. Machleder et al.s used histochemical studies for fiber typing and quantified hypertrophy and atrophy factors in patients with thoracic outlet neurogenic syndromes and normal patients. They observed scalene hypertrophy of the type 1 fiber system in symptomatic patients with intact anterior scalene muscles. After anterior scalene tenotomy this fiber type atrophied. They con: eluded that these changes substantiated that longterm increased tone in the anterior scalene muscle may explain symptoms in patients without other obvious structural anomalies and symptoms in patients who had stretch injury to the musculature in this region. These observations may further support our view that adequate decompression of the thoracic outlet includes scalene muscle resection. Certainly, the supraclavicular approach 9 affords ideal exposure for this maneuver. Subtotal resection of the middle scalene with the attached first rib is readily accomplished with no significant morbidity. Removal of osseous anomalies when encountered can easily be justified because they are usually precipitating factors for all forms of neurovascular compression in the thoracic outlet. When the varied underlying factors responsible for neurogenic symptoms are considered, any surgical procedure in this region should include a thorough decompression of the plexus. A complete excision of the anterior scalene muscle ensures it will not reattach to the first rib bed with recurrent symptoms. Furthermore, removal of this muscle affords complete exposure of the proximal brachial plexus anteriorly and other soft tissue anomalies. Transection of the middle scalene muscle facilitates exposure of neck of the first rib for precise division and subsequent removal. This results in an
6 334 Reilly and Stoney Journal of VASCULAR SURGERY enlarged space posterior to the brachial plexus and first rib bed. In previous reports, authors usually emphasized the importance of either osseous or soft tissue structures but rarely both. Roos 3 used a combined approach for second operations and in selected patients with middle and upper plexus involvement. Our ]previous report recommended the combined remowd of osseous and soft tissue abnormalities with a combined operative approach? Sanders and Rayner, 9 in describing their supraclavicular approach to scalenectomy and first rib resection reported that in occasional patients, difficult or impossible exposure of the neck of the first rib justified limitation of the operation to scalenectomy alone. If significant symptoms persisted, they proposed later transaxillary resection of the first rib. In our experience, total thoracic outlet decompression including first rib resection by the supraclavicular approach can reliably be achieved. In the eight patients in this study in whom the first rib was not removed, a large cervical rib simulating the course of the first rib was interpreted as the', cause of nerve compression. In such instances, additional removal of the first thoracic rib did not appear justified, but it was technically feasible. Complications in this series are numerous but trivial Pneumothorax is not unexpected after this operation and is easy to treat. The potential for nerve injtu3/in this region is a major risk to a patient having thoracic outlet decompression. Wide exposure, selfretaining retraction, and fiber-optic illumination facilitave the meticulous dissection required. Traction paresis is the cause of most nerve palsies that occur after operations in this region but they resolve quickjty. After resection of the anterior scalene muscle and any osseous or fibrous anomalies, first rib removal without undue traction on the plexus is accompfished because the enlarged area and relaxed strucvares accommodate moderate displacement. The course of the phrenic and long thoracic nerves are reliably constant and can be visualized and retracted to avoid injury. In second operations, the precise identification of delicate nerve trunks and the lymphatic and chylous ducts is difficult when they are enveloped by scar tissue. Nonetheless, these repeat operations can be achieved with only a slightly higher risk of complications. Most are done after failure of transaxillary procedures and the exposure cephalad to the first rib bed is rarely obscured by scar tissue. We deliberately expose and mobilize the roots and trunks of the plexus to conduct a thorough neurolysis in second operations. This assures us that these structures can be protected during the removal of scar tissue and anomalous structures in this vicinity. We have not observed any unusual morbidity associated with careful plexus mobilization and gentle retraction and believe it is safer than the avoidance of the plexus. When adjacent fibrous tissue or soft tissue anomalies are overlooked that are responsible for recurrent or persistent neurogenic symptoms after a prior operation, the interest of the patient is not well served. Furthermore, a substantial scar tissue barrier to brachial plexus decompression awaits the surgeon who may unfortunately be required to perform a later third operation. REFERENCES 1. Roos DB. Experience with first rib resection for thoracic outlet syndrome. Ann Surg 1971;173: Qvaffordt PG, Ehrenfcld WK, Stoney RJ. Supraclavicular radical scalenectomy and transaxillary first rib resection for the thoracic outlet syndrome. Am J Surg 1984;148: Roos DB. The place for scalenectomy and first rib resection in thoracic outlet syndrome. Surgery 1982;92: Adson AW. Surgical treatment for symptoms produced by cervical ribs and the scalenus anticus muscle. Surg Gynccol Obstet 1947;85: Roos DB. Congenital anomalies associated with thoracic outlet syndrome-anatomy, symptoms, diagnosis and treatment. Am Surg 1976;132: Ochsner A, Gage M, DeBakey M. Scalenus anticus (Naffziger) syndrome. Am J Surg 1935;28:669-93, 7. Naffziger HC, Grant WT. Neuritis of the brachial plexus, mechanical in origin: the scalene anticus syndrome. Surg Gynecol Obstet 1938;67: Machleder HI, Moll F, Verity AM. The anterior scalene muscle in thoracic outlet compression syndrome. Arch Surg 1986; I21: Sanders RJ, Kayner S. The supraclavicular approach to scalenectomy and first rib resection: description of techwique. J VASC SURG 1985;2:751-6.
The supraclavicular approach to scalenectomy and first rib resection: Description of technique
 The supraclavicular approach to scalenectomy and first rib resection: Description of technique Richard J. Sanders, M.D., and Susan Raymer, Denver, Colo. Supraclavicular first rib resection has been performed
The supraclavicular approach to scalenectomy and first rib resection: Description of technique Richard J. Sanders, M.D., and Susan Raymer, Denver, Colo. Supraclavicular first rib resection has been performed
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
THORACIC OUTLET SYNDROME: A FREQUENT CAUSE OF NON-DISCOGENIC BRACHIALGIA
 THORACIC OUTLET SYNDROME: A FREQUENT CAUSE OF NON-DISCOGENIC BRACHIALGIA Debora Garozzo Brachial Plexus and Peripheral Nerve Surgery Unit Neurospinal Hospital Dubai, United Arab Emirates THE THORACIC OUTLET
THORACIC OUTLET SYNDROME: A FREQUENT CAUSE OF NON-DISCOGENIC BRACHIALGIA Debora Garozzo Brachial Plexus and Peripheral Nerve Surgery Unit Neurospinal Hospital Dubai, United Arab Emirates THE THORACIC OUTLET
Upper Plexus Thoracic Outlet Syndrome
 Neurol Med Chir (Tokyo) 42, 237 241, 2002 Upper Plexus Thoracic Outlet Syndrome Case Report Takeshi MATSUYAMA, KazuoOKUCHI, andkazuogoda* Department of Emergency and Critical Care Medicine, Nara Medical
Neurol Med Chir (Tokyo) 42, 237 241, 2002 Upper Plexus Thoracic Outlet Syndrome Case Report Takeshi MATSUYAMA, KazuoOKUCHI, andkazuogoda* Department of Emergency and Critical Care Medicine, Nara Medical
Richard Dobrusin DO FACOFP
 Richard Dobrusin DO FACOFP Define Thoracic Outlet Syndrome (TOS) Describe the Mechanisms of Dysfunction List Diagnostic tests for (TOS) Understand (TOS) referral patterns Discuss Treatment Options Definition:
Richard Dobrusin DO FACOFP Define Thoracic Outlet Syndrome (TOS) Describe the Mechanisms of Dysfunction List Diagnostic tests for (TOS) Understand (TOS) referral patterns Discuss Treatment Options Definition:
Thoracic outlet syndrome: first rib resection
 Review rticle Page 1 of 7 Thoracic outlet syndrome: first rib resection ornelis G. Vos 1, Çag das Ünlü 1, Michiel T. Voûte 2, Rob H. W. van de Mortel 3, Jean-Paul P. M. de Vries 3 1 Department of Surgery,
Review rticle Page 1 of 7 Thoracic outlet syndrome: first rib resection ornelis G. Vos 1, Çag das Ünlü 1, Michiel T. Voûte 2, Rob H. W. van de Mortel 3, Jean-Paul P. M. de Vries 3 1 Department of Surgery,
THORACIC OUTLET DECOMPRESSION
 THORACIC OUTLET DECOMPRESSION Thesis Submitted in partial fulfillment of the degree of M.D. in general surgery By Abd El Aty Mohammed Sakr Supervised by Prof. Dr. Amr Ahmed Gad Prof. of vascular surgery
THORACIC OUTLET DECOMPRESSION Thesis Submitted in partial fulfillment of the degree of M.D. in general surgery By Abd El Aty Mohammed Sakr Supervised by Prof. Dr. Amr Ahmed Gad Prof. of vascular surgery
D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y
 Thoracic Outlet (TOS), Winged Scapula, Brachial Plexus Compression 12 D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y 1122 KENILWORTH DRIVE, SUITE 18, TOWSON, MARYLAND
Thoracic Outlet (TOS), Winged Scapula, Brachial Plexus Compression 12 D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y 1122 KENILWORTH DRIVE, SUITE 18, TOWSON, MARYLAND
Compression of neural or vascular structures within the
 Thoracic Outlet Syndrome: Transaxillary Approach Margaret Clarke Tracci, MD, JD Compression of neural or vascular structures within the constrained space of the thoracic outlet may give rise to 3 separate
Thoracic Outlet Syndrome: Transaxillary Approach Margaret Clarke Tracci, MD, JD Compression of neural or vascular structures within the constrained space of the thoracic outlet may give rise to 3 separate
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Most patients with neurologic thoracic outlet syndrome
 ORIGINAL ARTICLES: GENERAL THORACIC Upper Plexus Thoracic Outlet Syndrome: Optimal Therapy Harold C. Urschel, Jr, MD, and Maruf A. Razzuk, MD Division of Thoracic and Cardiovascular Surgery, The University
ORIGINAL ARTICLES: GENERAL THORACIC Upper Plexus Thoracic Outlet Syndrome: Optimal Therapy Harold C. Urschel, Jr, MD, and Maruf A. Razzuk, MD Division of Thoracic and Cardiovascular Surgery, The University
Anatomy and Physiology II. Spine
 Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Tumors of the thoracic apex, even when benign,
 Anterior Cervical Transsternal Approach for Resection of Benign Tumors at the Thoracic Inlet George Ladas, MD, Peter H. Rhys-Evans, FRCS, and Peter Goldstraw, FRCS Department of Thoracic Surgery, Royal
Anterior Cervical Transsternal Approach for Resection of Benign Tumors at the Thoracic Inlet George Ladas, MD, Peter H. Rhys-Evans, FRCS, and Peter Goldstraw, FRCS Department of Thoracic Surgery, Royal
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
The Brachial Plexus and Thoracic Outlet Syndrome
 The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
THORACIC OUTLET SYNDROME (T.O.S.) Prof J van Marle
 THORACIC OUTLET SYNDROME (T.O.S.) Prof J van Marle 1. Definition Clinical syndrome caused by compression of the neurovascular bundle as it passes through the thoracic outlet, a narrow space bordered by
THORACIC OUTLET SYNDROME (T.O.S.) Prof J van Marle 1. Definition Clinical syndrome caused by compression of the neurovascular bundle as it passes through the thoracic outlet, a narrow space bordered by
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Thoracic Outlet Syndrome
 Thoracic Outlet Syndrome Cristina Sola, BSN, RN-BC Nurse Manager Department of Cardiothoracic and Vascular Surgery McGovern Medical School The University of Texas Science Center at Houston Memorial Hermann
Thoracic Outlet Syndrome Cristina Sola, BSN, RN-BC Nurse Manager Department of Cardiothoracic and Vascular Surgery McGovern Medical School The University of Texas Science Center at Houston Memorial Hermann
PLEURAE and PLEURAL RECESSES
 PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
Thyroidectomy. Siu Kwan Ng. Modified Radical Neck Dissection Type II 47
 06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
Resection of malignant tumors invading the thoracic inlet
 Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
EndoBlade Soft Tissue Release System
 Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
University Journal of Medicine and Medical Specialities
 ISSN 2455-2852 2018, Vol. 4(5) Imaging Assessment of Vascular Thoracic Outlet Syndrome BALAJI A AYYAMPERUMAL Department of Radio Diagnosis,MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL Abstract
ISSN 2455-2852 2018, Vol. 4(5) Imaging Assessment of Vascular Thoracic Outlet Syndrome BALAJI A AYYAMPERUMAL Department of Radio Diagnosis,MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL Abstract
Neck-2. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem Solving Torso
 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
thoracic cage inlet and outlet landmarks of the anterior chest wall muscles of the thoracic wall sternum joints ribs intercostal spaces diaphragm
 Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Symptoms and Referred Pain from Myofascial Trigger Points in the Anterior Scalene Muscle or Scalenus Anterior
 Symptoms and Referred Pain from Myofascial Trigger Points in the Anterior Scalene Muscle or Scalenus Anterior picture Symptoms and signs Aching or throbbing in the lateral forearm extending to thumb and
Symptoms and Referred Pain from Myofascial Trigger Points in the Anterior Scalene Muscle or Scalenus Anterior picture Symptoms and signs Aching or throbbing in the lateral forearm extending to thumb and
SOME OBSERVATIONS CONCERNING PAIN IN THE NECK, UPPER CHEST, AND ARMS
 SOME OBSERVATIONS CONCERNING PAIN IN THE NECK, UPPER CHEST, AND ARMS JOHN TUCKER, M.D. Division of Internal Medicine The diagnosis of the specific neurologic lesion that produces pain in the neck and arm
SOME OBSERVATIONS CONCERNING PAIN IN THE NECK, UPPER CHEST, AND ARMS JOHN TUCKER, M.D. Division of Internal Medicine The diagnosis of the specific neurologic lesion that produces pain in the neck and arm
Thoracic Outlet Syndrome
 Thoracic Outlet Syndrome Part 1: The Scalene Triangle TOS: Vascular Symptom Presentation Venous persistent/intermittent edema heaviness and fatigue deep pain in neck/shoulder increased pain at night warm
Thoracic Outlet Syndrome Part 1: The Scalene Triangle TOS: Vascular Symptom Presentation Venous persistent/intermittent edema heaviness and fatigue deep pain in neck/shoulder increased pain at night warm
FUNCTIONAL ANATOMY OF SHOULDER JOINT
 FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
Anatomy notes-thorax.
 Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
T treat empyema, although modern day thoracic
 The Schede and Modern Thoracoplasty Benjamin J. Pomerantz, Joseph C. Cleveland, Jr, and Marvin Pomerantz THORACOPLASTY-GENERAL CONSIDERATIONS horacoplasty evolved as a procedure designed to T treat empyema,
The Schede and Modern Thoracoplasty Benjamin J. Pomerantz, Joseph C. Cleveland, Jr, and Marvin Pomerantz THORACOPLASTY-GENERAL CONSIDERATIONS horacoplasty evolved as a procedure designed to T treat empyema,
THE DESCENDING THORACIC AORTA
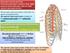 Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
Surgical Anatomy of the Hip. Joseph H. Dimon
 Surgical Anatomy of the Hip Joseph H. Dimon The hip joint is a deep joint surrounded by large and powerful muscles necessary for its proper function. Essential neurovascular structures lie in front and
Surgical Anatomy of the Hip Joseph H. Dimon The hip joint is a deep joint surrounded by large and powerful muscles necessary for its proper function. Essential neurovascular structures lie in front and
Yara saddam & Dana Qatawneh. Razi kittaneh. Maher hadidi
 1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
be very thin and variable. Facial nerve branches that exit the parotid gland are deep to the SMAS.
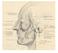 The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
Official Definition. Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist.
 Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
82a Orthopedic Massage! Introduction - Thoracic Outlet"
 82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives
 1 2 Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives List the muscular and ligamentous attachments of the thoracic and lumbar spine Describe how the muscles affect the spine and upper extremity
1 2 Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives List the muscular and ligamentous attachments of the thoracic and lumbar spine Describe how the muscles affect the spine and upper extremity
STERNUM. Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts:
 STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
Cervical Spine: Pearls and Pitfalls
 Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Objective Diagnosis (Ulnar Nerve Conduction Velocity) and Current Therapy of the Thoracic Outlet Syndrome
 Objective Diagnosis (Ulnar Nerve Conduction Velocity) and Current Therapy of the Thoracic Outlet Syndrome Harold C. Urschel, Jr., M.D., Maruf A. Razzuk, M.D., Richard E. Wood, M.D., Manaharlal Parekh,
Objective Diagnosis (Ulnar Nerve Conduction Velocity) and Current Therapy of the Thoracic Outlet Syndrome Harold C. Urschel, Jr., M.D., Maruf A. Razzuk, M.D., Richard E. Wood, M.D., Manaharlal Parekh,
CASE REPORT A LOGICAL APPROACH TO THE THORACIC INLET: THE DARTEVELLE APPROACH REVISITED
 CASE REPORT James I. Cohen, MD, PhD, Section Editor A LOGICAL APPROACH TO THE THORACIC INLET: THE DARTEVELLE APPROACH REVISITED Yadranko Ducic, MD, FRCS(C), 1 Andre Crepeau, MD, FRCS(C), 2 Laura Ducic,
CASE REPORT James I. Cohen, MD, PhD, Section Editor A LOGICAL APPROACH TO THE THORACIC INLET: THE DARTEVELLE APPROACH REVISITED Yadranko Ducic, MD, FRCS(C), 1 Andre Crepeau, MD, FRCS(C), 2 Laura Ducic,
thopaedic Science Diagnosis and treatment of thoracic outlet syndrome* Instructional lecture
 J Orthop Sci (1997) 2:119-127 ~ Journal of thopaedic Science The Japanese Orthopaedic Association Instructional lecture Diagnosis and treatment of thoracic outlet syndrome* MASATAKA ABE, TADASHI SHIMAMURA,
J Orthop Sci (1997) 2:119-127 ~ Journal of thopaedic Science The Japanese Orthopaedic Association Instructional lecture Diagnosis and treatment of thoracic outlet syndrome* MASATAKA ABE, TADASHI SHIMAMURA,
Copyright 2010 Pearson Education, Inc.
 E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
A simple MRI technique for the assessment of thoracic outlet compression syndrome (TOCS)
 A simple MRI technique for the assessment of thoracic outlet compression syndrome (TOCS) Poster No.: C-3128 Congress: ECR 2010 Type: Scientific Exhibit Topic: Vascular Authors: E. Fanou, M. Cowling; Stoke-on-Trent/UK
A simple MRI technique for the assessment of thoracic outlet compression syndrome (TOCS) Poster No.: C-3128 Congress: ECR 2010 Type: Scientific Exhibit Topic: Vascular Authors: E. Fanou, M. Cowling; Stoke-on-Trent/UK
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
The anatomy of the thoracic inlet is an important determinant
 Anterior Approach to Superior Sulcus Tumors Philippe Dartevelle and Steven J. Mentzer The anatomy of the thoracic inlet is an important determinant of the radiographic appearance and clinical syndrome
Anterior Approach to Superior Sulcus Tumors Philippe Dartevelle and Steven J. Mentzer The anatomy of the thoracic inlet is an important determinant of the radiographic appearance and clinical syndrome
Thoracic outlet syndrome (TOS) results from compression
 Safety and Efficacy of the Supraclavicular Approach to Thoracic Outlet Decompression Thomas S. Maxey, MD, T. Brett Reece, MD, Peter I. Ellman, MD, Curtis G. Tribble, MD, Nancy Harthun, MD, Irving L. Kron,
Safety and Efficacy of the Supraclavicular Approach to Thoracic Outlet Decompression Thomas S. Maxey, MD, T. Brett Reece, MD, Peter I. Ellman, MD, Curtis G. Tribble, MD, Nancy Harthun, MD, Irving L. Kron,
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
3 Mohammad Al-Mohtasib Areej Mosleh
 3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
Surgical Anatomy of the Neck. M. J. Jurkiewicz, John Bostwick. Surgical Clinics of North America, Vol 54, No 6, December 1974.
 Surgical Anatomy of the Neck M. J. Jurkiewicz, John Bostwick Surgical Clinics of North America, Vol 54, No 6, December 1974. The radical neck dissection is a safe, effective therapeutic procedure for eradication
Surgical Anatomy of the Neck M. J. Jurkiewicz, John Bostwick Surgical Clinics of North America, Vol 54, No 6, December 1974. The radical neck dissection is a safe, effective therapeutic procedure for eradication
THE MANAGEMENT OF THE SWOLLEN ARM IN CARCINOMA OF THE BREAST
 THE MANAGEMENT OF THE SWOLLEN ARM IN CARCINOMA OF THE BREAST NORMAN TREVES, M.D. The terms "brawny arm" and "lymphedema" have been given to the swollen arm which may complicate the inoperable, recurrent,
THE MANAGEMENT OF THE SWOLLEN ARM IN CARCINOMA OF THE BREAST NORMAN TREVES, M.D. The terms "brawny arm" and "lymphedema" have been given to the swollen arm which may complicate the inoperable, recurrent,
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Karl A. Illig, MD, and Mathew Wooster, MD
 Neurogenic Thoracic Outlet Syndrome Karl A. Illig, MD, and Mathew Wooster, MD Perhaps no condition treated by vascular surgeons has been associated with more confusion, subjectivity, and nihilism than
Neurogenic Thoracic Outlet Syndrome Karl A. Illig, MD, and Mathew Wooster, MD Perhaps no condition treated by vascular surgeons has been associated with more confusion, subjectivity, and nihilism than
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck.
 Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th & 12 th Eds.)
 PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
Infraclavicular brachial plexus blocks have been designed
 The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome)
 A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
Suprascapular Nerve: How to identify when it is a problem and what to do? Speaker Disclosure
 Suprascapular Nerve: How to identify when it is a problem and what to do? Eric C. McCarty, MD Associate Professor Chief of Sports Medicine and Shoulder Surgery University of Colorado School of Medicine
Suprascapular Nerve: How to identify when it is a problem and what to do? Eric C. McCarty, MD Associate Professor Chief of Sports Medicine and Shoulder Surgery University of Colorado School of Medicine
Anatomy of thoracic wall
 Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Pathologic abnormality of the sternoclavicular joint (SCJ)
 Surgical Management of the Infected Sternoclavicular Joint Rubie Sue Jackson, MD, Yvonne M. Carter, MD, and M. Blair Marshall, MD Pathologic abnormality of the sternoclavicular joint (SCJ) is rare. The
Surgical Management of the Infected Sternoclavicular Joint Rubie Sue Jackson, MD, Yvonne M. Carter, MD, and M. Blair Marshall, MD Pathologic abnormality of the sternoclavicular joint (SCJ) is rare. The
Anatomy Lecture #19 AN INTRODUCTION TO THE THORAX April 3, 2012
 Page 1 بسم الله الرحمن الرحيم The Thoracic Wall Firstly, when we talk about thorax, we should begin with the thorax wall which means not only bones that construct the thorax but also the muscles which
Page 1 بسم الله الرحمن الرحيم The Thoracic Wall Firstly, when we talk about thorax, we should begin with the thorax wall which means not only bones that construct the thorax but also the muscles which
Carpal Tunnel Release
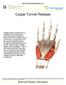 Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
B the mid-l940s, pulmonary resection and thoracoplasty
 - Thoracoplasty in the New Millennium Cleveland W. Lewis, Jr, MD, and Walter G. Wolfe, MD efore the development of antituberculosis drugs in B the mid-l940s, pulmonary resection and thoracoplasty stood
- Thoracoplasty in the New Millennium Cleveland W. Lewis, Jr, MD, and Walter G. Wolfe, MD efore the development of antituberculosis drugs in B the mid-l940s, pulmonary resection and thoracoplasty stood
Modified Radical Mastectomy
 Modified Radical Mastectomy Valerie L. Staradub, MD, and Monica Morrow, MD S urgical management options for breast cancer include modified radical mastectomy (MRM), MRM with immediate reconstruction, and
Modified Radical Mastectomy Valerie L. Staradub, MD, and Monica Morrow, MD S urgical management options for breast cancer include modified radical mastectomy (MRM), MRM with immediate reconstruction, and
SLAP Lesions of the Shoulder
 Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Outcome of Surgical Treatment for Arterial Thoracic Outlet Syndrome
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 09-13 www.iosrjournals.org Outcome of Surgical Treatment for Arterial
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 09-13 www.iosrjournals.org Outcome of Surgical Treatment for Arterial
Centerline Carpal Tunnel Release
 Centerline Endoscopic Carpal Tunnel Release Surgical Technique Centerline Carpal Tunnel Release Centerline Endoscopic Carpal Tunnel Release Surgical Set Up The patient is positioned supine on the operating
Centerline Endoscopic Carpal Tunnel Release Surgical Technique Centerline Carpal Tunnel Release Centerline Endoscopic Carpal Tunnel Release Surgical Set Up The patient is positioned supine on the operating
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Orthopedics - Dr. Ahmad - Lecture 2 - Injuries of the Upper Limb
 The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
Ovid: Oxford Textbook of Endocrinology & Diabetes
 Página 1 de 6 Copyright 2002 Oxford University Press Wass, John A.H., Shalet, Stephen M., Gale, Edwin, Amiel, Stephanie A. Oxford Textbook of Endocrinology & Diabetes, 1st Edition Surgical procedure Part
Página 1 de 6 Copyright 2002 Oxford University Press Wass, John A.H., Shalet, Stephen M., Gale, Edwin, Amiel, Stephanie A. Oxford Textbook of Endocrinology & Diabetes, 1st Edition Surgical procedure Part
Lowe Plastic Surgery (LPS)
 Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
Chapter 3: Thorax. Thorax
 Chapter 3: Thorax Thorax Thoracic Cage I. Thoracic Cage Osteology A. Thoracic Vertebrae Basic structure: vertebral body, pedicles, laminae, spinous processes and transverse processes Natural kyphotic shape,
Chapter 3: Thorax Thorax Thoracic Cage I. Thoracic Cage Osteology A. Thoracic Vertebrae Basic structure: vertebral body, pedicles, laminae, spinous processes and transverse processes Natural kyphotic shape,
Recurrent thoracic outlet syndrome
 Recurrent thoracic outlet syndrome Richard J. Sanders, MD, Craig E. Haug, MD, and William H. Pearce, MD,* Denver, Colo., and Chicago, Ill. Recurrent symptoms develop in 15% to 20% of patients undergoing
Recurrent thoracic outlet syndrome Richard J. Sanders, MD, Craig E. Haug, MD, and William H. Pearce, MD,* Denver, Colo., and Chicago, Ill. Recurrent symptoms develop in 15% to 20% of patients undergoing
Management of Brachial Plexus & Peripheral Nerves Blast Injuries. First Global Conflict Medicine Congress
 Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Day 5 Respiratory & Cardiovascular: Respiratory System
 Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
Anatomy and Physiology II. Review Spine and Neck
 Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
Regional Anaesthesia of the Thoracic Limb
 Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST
 CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
