Acute proximal hamstring rupture
|
|
|
- Roy Allison
- 5 years ago
- Views:
Transcription
1 Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery June 2007 Acute proximal hamstring rupture Steven B. Cohen Thomas Jefferson University, James Bradley University of Pittsburgh Let us know how access to this document benefits you Follow this and additional works at: Part of the Orthopedics Commons Recommended Citation Cohen, Steven B. and Bradley, James, "Acute proximal hamstring rupture" (2007). Department of Orthopaedic Surgery Faculty Papers. Paper This Article is brought to you for free and open access by the Jefferson Digital Commons. The Jefferson Digital Commons is a service of Thomas Jefferson University's Center for Teaching and Learning (CTL). The Commons is a showcase for Jefferson books and journals, peer-reviewed scholarly publications, unique historical collections from the University archives, and teaching tools. The Jefferson Digital Commons allows researchers and interested readers anywhere in the world to learn about and keep up to date with Jefferson scholarship. This article has been accepted for inclusion in Department of Orthopaedic Surgery Faculty Papers by an authorized administrator of the Jefferson Digital Commons. For more information, please contact: JeffersonDigitalCommons@jefferson.edu.
2 Acute Proximal Hamstring Ruptures: Review of Literature, and Treatment Options Steven Cohen, MD 1 and James Bradley, MD 2 1 Dr. Cohen is Director, Sports Medicine Research, and Assistant Professor, Department of Orthopaedic Surgery, Rothman Institute Orthopaedics, Thomas Jefferson University Medical School, Philadelphia, PA. 2 Dr. Bradley is Clinical Associate Professor, University of Pittsburgh Medical Center, Pittsburgh, PA. Reprint requests: Dr. Cohen Rothman Institute Orthopaedics 925 Chestnut Street Philadelphia, PA This is the authors final version prior to publication in the Journal of the American Academy of Orthopaedic Surgeons, Vol 15, No 6, June 2007, The published version is available at Copyright 2007 the American Academy of Orthopaedic Surgeons, all rights reserved.
3 Abstract The diagnosis and surgical treatment of proximal hamstring ruptures is becoming more common as this injury is more recognized. Nonoperative treatment of complete ruptures has led to complications such as weakness and sciatic nerve neuralgia. As a result, surgical treatment has been advocated to repair the complete rupture of the hamstring tendons from the ischial tuberosity. Surgical repair involves a transverse incision in the gluteal crease, protection of the sciatic nerve, mobilization of the ruptured tendons, and repair to the ischial tuberosity with the use of suture anchors. There have been few reports in the literature and most series have had a relatively small amount of patients. Surgical repair results in a rate of return to function and sports of 58-85%, near normal strength, and decreased pain. Introduction As athletes of all levels have become bigger, stronger, and faster, tendon, musculotendinous junction, and muscle injuries appear to be happening with increasing frequency. Acute hamstring strains are one of the more common injuries occurring in athletes.[1] Strains are most commonly the result of an eccentric muscle contraction and most frequently occur at the musculotendinous junction. In general, mild to moderate strains respond well to conservative treatments such as rest, ice, modalities, nonsteroidal anti-inflammatory drugs (NSAIDs), gentle stretching, therapeutic exercise, and gradual return to athletic activity. Mechanism of Injury Proximal hamstring rupture from the ischial tuberosity although infrequently, occurs acutely both in well-trained athletes, and middle-aged patients, who sustain
4 sudden hip flexion / knee extension causing hamstring contraction. This injury is rather dramatic with patients describing the sensation of being shot in the posterior thigh with subsequent difficulty ambulating. Presentation The gait pattern is one of a stiff legged gait as a result of avoidance of hip and knee flexion. Patients typically present with posterior thigh pain distal to the ischial tuberosity (at the location of the tendon retraction) and significant ecchymosis as a result of the hematoma from the tendon rupture. They will also complain of difficulty sitting secondary to pain at the avulsion site. Examination Physical examination is often difficult to determine the exact nature of the injury due to the deep location of the hamstring muscle group. A common finding is a latent large area of ecchymosis in the posterior middle and distal thigh (approximately 1 week following injury). Tenderness is usually present over the injury however palpation of a defect may or may not be easily established. It is important to test the peroneal branch of the sciatic nerve function because if there is an injury to this branch, this will cause weakness of the short head of the biceps femoris and may slow potential postoperative rehabilitation. Specifically, if there has been a neuropractic injury to the nerve, this may present as a foot drop or more subtly an eversion weakness of the ankle. Radiographs X-rays may show a bony avulsion from the ischial tubersosity if present, but are commonly negative. Magnetic resonance imaging (MRI) is crucial in determining the amount of soft tissue injury, more specifically; complete versus partial rupture, number of
5 tendons ruptured, and amount of retraction (Figure 1). Digital radiographs, in particular MRI, allow extremely accurate measurement of the amount retraction after tendon rupture. The digital imaging we have used is Stentor, Philips Medical System (Brisbane, CA) and is accurate to the accuracy of the DICOM tag parameters for pixel spacing. The isite PACS application automatically adjusts to physical data points, so there is no inaccuracy on interpolated data. Treatment Algorithm The algorithm we generally follow is; a single tendon avulsion is treated nonoperatively despite retraction up to 1 2 cm. In our experience athletes are able to return to high level sports (professional football) approximately 6 weeks after injury. The ruptured single tendon scars to the intact tendons and allows return to full strength. An acute three tendon (semitendinosus, semimembranosus, and long head of biceps femoris) tear typically has a significant amount of retraction of up to 5 cm or more. This is treated with surgical repair. A more difficult decision is how to treat a two of the three tendon rupture. Even though MRI findings may show avulsion of 2 tendons, the third tendon may have a significant injury associated with the musculotendinous junction (MTJ) and may be attenuated. We recommend repair in younger (< 50 years) more active individuals especially those still participating in athletics with retraction of the ruptured tendons of 2 cm or more. There are no specific guidelines in the literature on the amount of retraction that should be treated surgically. Retraction of 2 cm or greater has been a cut off for surgical treatment in our experience. When retraction of the 2 tendons reaches 2 cm this has been indicative of an injury to the third attached tendon usually at the MTJ or
6 muscle belly in our patients that may not be apparent on MRI. Failure to address this surgically may result in residual pain, weakness, and hamstring dysfunction. Overview The frequency of these injuries appears to be increasing both clinically and by report in the literature, as more middle-aged patients remain more active and the recognition and potential for treatment has become better established. Proper treatment includes a thorough evaluation and discussion with the patient regarding treatment options. Many of the series reported in the literature of proximal hamstring repair contain few patients, with the largest series of acute repairs consisting of 7 patients [2]. Additionally, the technique for surgical repair has not been well established. Review of Literature There have been few reports in the literature on the surgical treatment of proximal hamstring injuries. The small numbers of published studies contain both acute and chronic tears and include a relatively small number of patients.[2-7] The findings in these studies are summarized in table 1. Klingele and Sallay reported on the primary surgical repair of complete proximal hamstring ruptures in 11 patients [2]. The average age of the patients was 41.5 years and the mechanism of injury varied. MRI was used to confirm complete injuries in all patients. Surgery was recommended for acute complete rupture in active patients with functional disability, and in chronic cases with pain caused by sciatic nerve compression and inability to return to vigorous activity. Chakravarthy et al reported on the surgical treatment in 4 cases of complete proximal hamstring tendon ruptures in water skiers and bull riders [3]. Two of the three
7 patients initially treated conservatively suffered from sciatic neuralgia, and all 4 patients had significant knee flexion weakness and thigh pain. Cross et al reported on the surgical repair of chronic complete rupture in nine adult patients.[4] They felt that the acute diagnosis of complete ruptures was difficult due to the minimal clinical awareness. Hamstring strength and endurance were an average of 60% and 57% respectively at an average of 48 months although only 7 of the nine patients were available for testing. Brucker and Imhoff described the functional assessment (by performing Cybex dynamometer isokinetic testing measuring maximum hamstring and quadriceps torque and peak torque ratio of hamstring to quadriceps at a velocity of 60 degrees per second) after repair of acute and chronic hamstring repairs in 8 patients.[5] MRI was used to confirm the diagnosis in all cases. Return to sports activities was allowed after 6-8 months. At 20 months follow-up, 50% complained of incisional pain and discomfort with one patient requiring an additional surgery after pullout of a metal suture anchor. Sallay et al described the results of 12 patients with water skiing-related hamstring injuries with an average time from injury to initial evaluation of 5.6 months (range: 6 weeks to 18 years).[6] The mechanism was commonly an eccentric contraction while attempting to get up from the submerged position in novice skiers and injury from a fall in expert skiers. Initial treatment was non-operative and half of the patients had MRI or CT scans to assess the injury. Five MRI and one CT scan were used to evaluate the exact site and extent of the hamstring tear. Five patients ultimately required delayed surgical repair due to persistent functional limitations. This study confirmed the functional deficit associated with complete proximal hamstring tears.
8 Orava and Kujala treated 8 patients with surgical repair who had complete rupture (all 3 tendons) of the hamstrings from the ischial tuberosity.[7] The mean age of their patients was 40 years and the injury was the result of a sudden forceful flexion of the hip when the knee was extended, and occurred during athletics. In 7 of the 8 cases ultrasound was used to confirm complete tendon rupture. The results with regard to function and strength were improved in the 5 patients who underwent repair less than 2 months following the injury compared to the 3 chronic repairs. Acute repair allows easier re-approximation of the tendon to its insertion on the ischial tuberosity. In addition, the authors recommend nonoperative treatment for isolated biceps femoris ruptures as little functional disability results from this injury. Consequently, they recommended prompt surgery to accomplish a primary repair of the tendons to its origin. In summary, complete rupture of the proximal hamstrings is an uncommon injury that if not treated acutely leads to weakness, pain, and potential for sciatic neuralgia, which is similar to hamstring syndrome as described below. Reports in the literature have small series of patients evaluated retrospectively with a variety of surgical techniques and timing to surgery. The consensus in the literature however is an improved result is obtained with earlier treatment of complete proximal hamstring ruptures. Nonoperative Treatment Nonoperative is recommended in the case of single tendon rupture regardless of retraction amount and multiple tendon tear with minimal retraction (< 2 cm). Treatment consists of rest, ice, modalities, NSAIDs, gentle stretching, therapeutic exercise, and gradual return to athletic activity, over approximately 4 to 6 weeks.
9 Nonoperative treatment of significant proximal hamstring ruptures (two or more tendons) may result in knee flexion and mild hip extension weakness, sitting difficulty, deformity, and the potential development of symptoms similar to hamstring syndrome as the tendons scar down to the sciatic nerve. Hamstring syndrome as described by Puranen and Orava consists of local posterior buttock pain and discomfort over the ischial tubersosity [8]. In most cases the pain begins without specific trauma and characteristically is painful during sitting. In addition, the pain may worsen with stretching and during exercise (sprinting, hurdling, or kicking). In some cases of persistent hamstring syndrome, surgical release and sciatic nerve decompression are necessary to relieve the symptoms, which was successful in 52 of 59 patients (88%) in their series [8]. Acute repair allows easier mobilization of the tendons (usually a single tendon wad comprising all three tendons) and repair to the ischial tuberosity. Chronic rupture repair yields less consistent results with the potential issue of scarring to the sciatic nerve possibly requiring concomitant dissection of the nerve from the avulsed tendons followed by sciatic neurolysis. Surgical Treatment / Technique The patient is placed in the prone position and a transverse incision is made in the gluteal crease directly inferior to the ischial tuberosity. We prefer a transverse incision in the gluteal crease for its cosmesis and accessibility to the avulsed tendons, as opposed to a longitudinal incision. If necessary, the transverse incision may be extended to provide greater access for retrieval of any retracted tendons. The incision is taken down to the gluteal fascia taking care to avoid the posterior femoral cutaneous nerve. A transverse
10 incision is made in the gluteal fascia. The gluteus maximus muscle is elevated and retracted superiorly. This allows exposure to the hamstring fascia. A longitudinal incision is made in the hamstring fascia. Typically an additional layer of scar lies over the ruptured coalescence of the hamstring tendons, and it will appear that tendons are not ruptured, but this layer must be incised to locate the tendons. After this layer is entered, this exposes the large amount of hematoma, which is present from the tendon rupture. The sciatic nerve can be palpated and protected by lateral retraction of the group of tendons. After the tendons are identified, the scar on the ends of the tendon is removed and the tendon edges are abraded to normal tendon (Figure 2). It is crucial to remove the scar but not perform excessive removal, which can leave the tendon length shortened. The tendons are mobilized and tagged with a heavy suture. Next, the ischial tuberosity is identified and the lateral aspect is cleared off with a periosteal elevator. It is important to reattach the tendons to their anatomic origin, which is on the lateral aspect of the tuberosity. The anatomical origin of the semimembranosus is the most lateral and the semitendinosus and long head of the biceps femoris are medial to the origin of the semimembranosus arising from a common aponeurosis [8] (Figure 3). The tubersosity is denuded to provide for bony healing using curettes. The tendons are repaired to bone with the use of suture anchors. We prefer the bioabsorbable anchors with abrasion resistant suture due to the strength of the suture and lower knot profile. The anchors are placed in the configuration of an X using a total of five anchors (Figure 4). The sutures are passed through the tendons using horizontal mattress sutures from inferior to superior and tied down from superior to inferior with the knee flexed 30 degrees. We have not had success using Bunnell, modified Kessler, or modified Mason-Allen stitches
11 because those stitches tend to bunch up the tendon at the bony interface on the ishcial tuberosity. The fascia is closed and the wound is closed in layers. The affected leg is then placed in a custom fitted hip orthosis, which restricts hip flexion from 15 to 30 degrees (figure 5). Limiting hip motion limits the stress at the re-attachment site. The patient then ambulates on crutches toe-touch weight bearing. Postoperative rehabilitation: The rehabilitation protocol described below was used for each of the patients in our series. This allowed for consistency regardless of findings at surgery or tension of the repair. The first phase of rehabilitation consists of toe-touch weight bearing for days with advancement to 25% weight bearing for the next three weeks. This allowed slight hip and knee flexion, taking care to prevent any stress on the tendon repair. Passive range of motion (PROM) of the knee and hip is begun at week 2 and gentle active ROM is initiated by week 4. The brace is discontinued by week 6. The second phase starts with full weight bearing at week 5 and normal gait training. PROM and AROM are progressed as well as aqua therapy. Isotonic exercises are begun within a limited range of motion avoiding the terminal ranges of motion. Core pelvic strength training and closed chain exercises are also initiated. At 8 weeks after surgery, isotonic strength training is progressed and dynamic training is advanced. An isometric strength evaluation at 60 degrees of knee flexion is performed at 10 weeks. The final phase of rehabilitation consists of the initiation of dry land jogging after 10 weeks. A full isokinetic evaluation is performed at 60 degrees, 120 degrees, and 180 degrees/second and compared to the nonoperative side. This provides objective evidence of strength deficits for patients and therapists, and allows specific milestones for return to
12 sport. Sports specific activities are continued and return to sporting activity is allowed when isokinetic testing is 80% of the unaffected side, similar to return for patients after ACL reconstruction [9]. This typically occurs between 6 and 9 months. The results of our current series of acute hamstring repairs include 7 patients with 8 hamstring repairs (one bilateral) with an average patient age of 42.7 years (range: 24-58). All injuries occurred via an eccentric contraction of the hamstrings. Subjective complaints consisted of pain, weakness, and difficulty sitting. All repairs were performed with the surgical technique described above at an average of 5.7 days after injury. All patients underwent preoperative MRI. The average time to return to function / athletics was 8.5 months including one patients return to professional football. Five patients who underwent Cybex testing revealed greater than 80% strength compared to the uninjured side at an average of 5.8 months. All patients were satisfied with the procedure at latest follow-up of greater than 6 months and 6 of 7 returned to preoperative sport or activity level. Conclusions Hamstring strains are common injuries, however complete proximal hamstring ruptures occur with less frequency. There must be awareness for this injury as well as a thorough physical examination supplemented by the use of MRI to avoid missing the diagnosis. Acute surgical treatment of proximal hamstring avulsions allows anatomic repair and lessons symptoms similar to hamstring syndrome while allowing the majority of patients functional return to activities including high-level athletics.
13 References 1. Clanton TO, Coupe KJ. Hamstring strains in athletes: Diagnosis and treatment. JAAOS 1998;6: Klingele KE, Sallay PI. Surgical repair of complete proximal hamstring tendon rupture. Am J Sports Med 2002;30: Chakravarthy J, Ramisetty N, Pimpalnerkar A, Mohtadi N. Surgical repair of complete proximal hamstring ruptures in water skiers and bull riders: A report of four cases and review of the literature. Br J Sports Med 2005;39: Cross MJ, Vendersluis R, Wood D, Banff M. Surgical repair of chronic complete hamstring tendon ruptures in the adult patient. Am J Sports Med 1998;26: Brucker PU, Imhoff AB. Functional assessment after acute and chronic complete ruptures of the proximal hamstring tendons. Knee Surg Sports Traumatol Arthrosc 2005;13: Sallay PI, Friedman RI, Coogan PG, Garrett WE. Hamstring muscle injuries among water skiers. Functional outcome and prevention. Am J Sports Med 1996;24: Orava S, Kujala UM. Rupture of the ischial origin of the hamstring muscles. Am J Sports Med 1995;23: Puranen J, Orava S. Hamstring syndrome: A new diagnosis of gluteal sciatic pain. Am J Sports Med 1988;16: Shelbourne KD, Nitz P. Accelerated rehabilitation after anterior cruciate ligament reconstruction. Am J Sports Med 1990;18:
14 Figures Figure 1: MRI example of an acute complete proximal hamstring rupture from the ischial tubersosity. A) Coronal T2 weighted image B) Axial T2 weighted image A.
15 B.
16 Figure 2: Appearance of the proximal hamstring tendons with retraction after rupture from the insertion on the lateral aspect of the ischial tuberosity.
17 Figure 3: Anatomy of the hamstring muscles and their origin on the ischial tuberosity.
18 Figure 4: Depiction of the proximal hamstring repair on the ischial tuberosity with the use of 5 suture anchors in the X configuration.
19 Figure 5: Post-operative brace worn following proximal hamstring repair.
20 Table 1: Summary of studies on proximal hamstring repair Study # of Patients Method of Repair Klingele & 11 (7 acute) Longitudinal Sallay incision with 2-3 anchors Chakravarthy et al 4 (1 acute) Longitudinal incision with metal anchors or primary repair Cross et al 9 (0 acute) Longitudinal incision with and without anchors Brucker & Imhoff 8 (6 acute) Repair with average of 3.5 anchors Sallay et al 12 (0 acute) Not specified (5 of 12 required late surgical repair) Orava & Kujala 8 (5 acute) Primary repair to bone through drill holes with / without augmentation Follow-Up Outcome 34 months 91% satisfaction 73% pain free or mild pain with activity 43% moderate limitations 85% return of strength with Cybex testing 12 months 75% returned to sport all regained strength and near normal motion all sciatic nerve symptoms resolved 48 months Hamstring strength 60% at follow-up 20 months 75% returned to sport, 10% deficit on isokinetic muscle testing 7.45 years (range: 6 mo 18 years) 58% returned to sports (all partial tears) 42% unable to return to sports at same level (all complete tears) 5.7 years 62% good outcome
Dominic Carreira M.D. Matt Kruchten, B.S. Fort Lauderdale, FL
 Dominic Carreira M.D. Matt Kruchten, B.S Fort Lauderdale, FL Disclosures ConMed Linvatec: Consulting and Education Zimmer Biomet Consulting and Education Royalties for Product Development The hamstring
Dominic Carreira M.D. Matt Kruchten, B.S Fort Lauderdale, FL Disclosures ConMed Linvatec: Consulting and Education Zimmer Biomet Consulting and Education Royalties for Product Development The hamstring
Functional results and outcomes after repair of proximal hamstring avulsions.
 Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 9-1-2012 Functional results and outcomes after repair of proximal hamstring avulsions. Steven B Cohen Rothman Institute,
Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 9-1-2012 Functional results and outcomes after repair of proximal hamstring avulsions. Steven B Cohen Rothman Institute,
Surgical repair of complete proximal hamstring tendon ruptures in water- skiers. and bull riders: A report of four cases and review of the literature.
 Surgical repair of complete proximal hamstring tendon ruptures in water- skiers and bull riders: A report of four cases and review of the literature. Key Words Proximal hamstring ruptures Surgical repair
Surgical repair of complete proximal hamstring tendon ruptures in water- skiers and bull riders: A report of four cases and review of the literature. Key Words Proximal hamstring ruptures Surgical repair
John J Christoforetti, MD Pittsburgh, Pennsylvania
 ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Proximal Hamstring Rupture: Physical Therapy Protocol
 Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Niv Marom, MD Department of Orthopaedic surgery Meir medical center
 Niv Marom, MD Department of Orthopaedic surgery Meir medical center Tendons basic science. Tendon avulsion injuries general concepts. Specific tendon avulsion injuries: Distal Biceps. Proximal Hamstrings.
Niv Marom, MD Department of Orthopaedic surgery Meir medical center Tendons basic science. Tendon avulsion injuries general concepts. Specific tendon avulsion injuries: Distal Biceps. Proximal Hamstrings.
Endoscopic Hamstring Repair and Ischial Bursectomy. Carlos A. Guanche, MD Southern California Orthopedic Institute
 Endoscopic Hamstring Repair and Ischial Bursectomy Carlos A. Guanche, MD Southern California Orthopedic Institute cguanche@scoi.com 1 Endoscopic Hamstring Repair and Ischial Bursectomy INTRODUCTION Hamstring
Endoscopic Hamstring Repair and Ischial Bursectomy Carlos A. Guanche, MD Southern California Orthopedic Institute cguanche@scoi.com 1 Endoscopic Hamstring Repair and Ischial Bursectomy INTRODUCTION Hamstring
Alejandro Verdugo m.d.
 Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Clinical Study A Novel Technique for Proximal Hamstring Tendon Repair: High Reoperation Rate in a Series of 56 Patients
 Advances in Orthopedic Surgery, Article ID 891875, 6 pages http://dx.doi.org/10.1155/2014/891875 Clinical Study A Novel Technique for Proximal Hamstring Tendon Repair: High Reoperation Rate in a Series
Advances in Orthopedic Surgery, Article ID 891875, 6 pages http://dx.doi.org/10.1155/2014/891875 Clinical Study A Novel Technique for Proximal Hamstring Tendon Repair: High Reoperation Rate in a Series
Proximal Hamstring Tendon Repair
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Proximal Hamstring Tendon Repair The hamstrings are a group
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Proximal Hamstring Tendon Repair The hamstrings are a group
Hamstring Injury: When to Consider Surgical Treatment
 Hamstring Injury: When to Consider Surgical Treatment Prof. dr. Gino Kerkhoffs Orthopaedic Surgery www.acesamsterdam.nl Gino Kerkhoffs Hans Tol Guus Reurink Mario Maas Pau Golanó Rolf Peters Maarten Moen
Hamstring Injury: When to Consider Surgical Treatment Prof. dr. Gino Kerkhoffs Orthopaedic Surgery www.acesamsterdam.nl Gino Kerkhoffs Hans Tol Guus Reurink Mario Maas Pau Golanó Rolf Peters Maarten Moen
Operative management of partial-thickness tears of the proximal hamstring muscles in athletes.
 Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 6-1-2013 Operative management of partial-thickness tears of the proximal hamstring muscles in athletes. Karl F
Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 6-1-2013 Operative management of partial-thickness tears of the proximal hamstring muscles in athletes. Karl F
Hamstring Injuries and Avulsions. Charles A. Bush-Joseph, MD Rush University Medical Center Team Physician, Chicago White Sox Chicago, IL
 Hamstring Injuries and Avulsions Charles A. Bush-Joseph, MD Rush University Medical Center Team Physician, Chicago White Sox Chicago, IL Disclosures No personal disclosures on this topic Institutional
Hamstring Injuries and Avulsions Charles A. Bush-Joseph, MD Rush University Medical Center Team Physician, Chicago White Sox Chicago, IL Disclosures No personal disclosures on this topic Institutional
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Rehabilitation Guidelines Following Proximal Hamstring Primary Repair
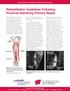 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Proximal Hamstring Primary Repair The hamstring muscle group consists of three muscles: the biceps femoris, semitendinosus and semimembranosus.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Proximal Hamstring Primary Repair The hamstring muscle group consists of three muscles: the biceps femoris, semitendinosus and semimembranosus.
HIP CASESTUDY 3. Body Chart-Initial Hypothesis: Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1
 Body Chart-Initial Hypothesis: HIP CASESTUDY 3 Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT OCS FAAOMPT Hamstring Strain HS Tendinopathy Lumbar Radiculopathy Lumbar
Body Chart-Initial Hypothesis: HIP CASESTUDY 3 Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT OCS FAAOMPT Hamstring Strain HS Tendinopathy Lumbar Radiculopathy Lumbar
With the advent and further refinement of hip arthroscopy
 Endoscopic Proximal Hamstring Repair and Ischial Bursectomy Brian D. Dierckman, M.D., and Carlos A. Guanche, M.D. Abstract: With the significant increase in use of the arthroscope around the hip have come
Endoscopic Proximal Hamstring Repair and Ischial Bursectomy Brian D. Dierckman, M.D., and Carlos A. Guanche, M.D. Abstract: With the significant increase in use of the arthroscope around the hip have come
Sciatic Nerve Injury After Proximal Hamstring Avulsion and Repair
 Sciatic Nerve Injury After Proximal Hamstring Avulsion and Repair Thomas J. Wilson,* MD, Robert J. Spinner, MD, Rohith Mohan, BA, Christopher M. Gibbs, BS, and Aaron J. Krych, MD Investigation performed
Sciatic Nerve Injury After Proximal Hamstring Avulsion and Repair Thomas J. Wilson,* MD, Robert J. Spinner, MD, Rohith Mohan, BA, Christopher M. Gibbs, BS, and Aaron J. Krych, MD Investigation performed
The hamstrings are amongst the most frequently injured
 Bulletin of the NYU Hospital for Joint Diseases 2012;70(1):41-8 41 Hamstring Injuries Christopher R. Ropiak, M.D., and Joseph A. Bosco, M.D. Abstract Hamstring injuries are a frequent injury in athletes.
Bulletin of the NYU Hospital for Joint Diseases 2012;70(1):41-8 41 Hamstring Injuries Christopher R. Ropiak, M.D., and Joseph A. Bosco, M.D. Abstract Hamstring injuries are a frequent injury in athletes.
Achilles Tendon Rupture
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
Posterior compartment of the thigh. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Posterior compartment of the thigh Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Posterior compartment of the thigh 1-Muscles: Biceps femoris Semitendinosus Semimembranosus Adductor magnus
Posterior compartment of the thigh Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Posterior compartment of the thigh 1-Muscles: Biceps femoris Semitendinosus Semimembranosus Adductor magnus
Meniscus Repair Rehabilitation Protocol
 Brian E. Camilleri, DO 2610 Enterprise Dr Anderson, IN 46013 Phone: (765) 683-4400 Fax: (765) 642-7903 www.ciocenter.com Meniscus Repair Rehabilitation Protocol The intent of this protocol is to provide
Brian E. Camilleri, DO 2610 Enterprise Dr Anderson, IN 46013 Phone: (765) 683-4400 Fax: (765) 642-7903 www.ciocenter.com Meniscus Repair Rehabilitation Protocol The intent of this protocol is to provide
A Patient s Guide to Biceps Tendon Tears at the Elbow
 A Patient s Guide to Biceps Tendon Tears at the Elbow Introduction The muscles which flex the elbow are the bicep complex. Like all musculoskeletal units, the end connection is a tendon composed of strong,
A Patient s Guide to Biceps Tendon Tears at the Elbow Introduction The muscles which flex the elbow are the bicep complex. Like all musculoskeletal units, the end connection is a tendon composed of strong,
Prevention and Treatment of Injuries. The Femur. Quadriceps 12/11/2017
 Prevention and Treatment of Injuries The Thigh, Hip, Groin, and Pelvis Oak Ridge High School Conroe, Texas The Femur Is the longest and the second strongest bone in the body and is designed to permit maximum
Prevention and Treatment of Injuries The Thigh, Hip, Groin, and Pelvis Oak Ridge High School Conroe, Texas The Femur Is the longest and the second strongest bone in the body and is designed to permit maximum
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
Hamstring Strain. 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) Website: philip-bayliss.com.
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Hamstring Strain The hamstring muscles are very susceptible to tears, strains and other common sporting
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Hamstring Strain The hamstring muscles are very susceptible to tears, strains and other common sporting
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
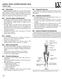 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
ACL Reconstruction Protocol (Allograft)
 ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
A Patient s Guide to Collateral Ligament Injuries
 A Patient s Guide to Collateral Ligament Injuries 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this booklet is
A Patient s Guide to Collateral Ligament Injuries 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this booklet is
TREATMENT GUIDELINES FOR GRADE 3 PCL TEAR
 GENERAL CONSIDERATIONS Posterior cruciate ligament (PCL) injuries occur less frequently than anterior cruciate ligament (ACL) injuries, but are much more common than previously thought. The PCL is usually
GENERAL CONSIDERATIONS Posterior cruciate ligament (PCL) injuries occur less frequently than anterior cruciate ligament (ACL) injuries, but are much more common than previously thought. The PCL is usually
Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair
 Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Prevention and Treatment of Injuries. Anatomy. Anatomy. Tibia: the second longest bone in the body
 Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
l. Initiate early proprioceptive activity and progress by means of distraction techniques: i. eyes open to eyes closed ii. stable to unstable m.
 Meniscus Repair 1. Defined a. Sutures or bioabsorbable fixation devices (arrows, darts, screws, etc.) bring together and fixate the edges of a tear in the meniscus in order to maintain the shock absorption
Meniscus Repair 1. Defined a. Sutures or bioabsorbable fixation devices (arrows, darts, screws, etc.) bring together and fixate the edges of a tear in the meniscus in order to maintain the shock absorption
3/21/2011 PCL INJURY WITH OPERATIVE TREATMENT A CASE STUDY PCL PCL MECHANISM OF INJURY PCL PREVALENCE
 PCL PCL INJURY WITH OPERATIVE TREATMENT A CASE STUDY K. Anderson, S. Hjortedal, Y. Jingi, E. Sutcliffe & S. Witschen Washington State University Origin Posterior aspect of tibia Insertion Medial femoral
PCL PCL INJURY WITH OPERATIVE TREATMENT A CASE STUDY K. Anderson, S. Hjortedal, Y. Jingi, E. Sutcliffe & S. Witschen Washington State University Origin Posterior aspect of tibia Insertion Medial femoral
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Advanced Imaging of Hamstring Injuries in Athletes and Active Patients
 Advanced Imaging of Hamstring Injuries in Athletes and Active Patients Mayo Clinic Sports Symposium 2016 Mark S. Collins MD Musculoskeletal Division Department of Radiology Mayo Clinic Rochester, MN Hamstring
Advanced Imaging of Hamstring Injuries in Athletes and Active Patients Mayo Clinic Sports Symposium 2016 Mark S. Collins MD Musculoskeletal Division Department of Radiology Mayo Clinic Rochester, MN Hamstring
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 Pectoralis Major Tendon Repair The pectoralis major is a thick, fan-shaped
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 Pectoralis Major Tendon Repair The pectoralis major is a thick, fan-shaped
Accelerated Rehabilitation Following ACL-PTG Reconstruction with Medial Collateral Ligament Repair
 Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of
Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
What is an ACL Tear?...2. Treatment Options...3. Surgical Techniques...4. Preoperative Care...5. Preoperative Requirements...6
 Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Toe walking gives rise to parental concern. Therefore, toe-walkers are often referred at the 3 years of age.
 IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
Patella Tendon Repair
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Biceps Tendon Tear at the Elbow
 DISEASES & CONDITIONS Biceps Tendon Tear at the Elbow The biceps muscle is located in the front of your upper arm. It is attached to the bones of the shoulder and elbow by tendons strong cords of fibrous
DISEASES & CONDITIONS Biceps Tendon Tear at the Elbow The biceps muscle is located in the front of your upper arm. It is attached to the bones of the shoulder and elbow by tendons strong cords of fibrous
MR Imaging of the Distribution and Location of Acute Hamstring Injuries in Athletes
 Downloaded from www.ajronline.org by 46.3.197.176 on 2/4/18 from IP address 46.3.197.176. Copyright ARRS. For personal use only; all rights reserved Arthur A. De Smet 1 Thomas M. Best 2 Received May 3,
Downloaded from www.ajronline.org by 46.3.197.176 on 2/4/18 from IP address 46.3.197.176. Copyright ARRS. For personal use only; all rights reserved Arthur A. De Smet 1 Thomas M. Best 2 Received May 3,
Patellar Tendon Repair Rehabilitation Guideline
 Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
OMICS - 3rd Int. Conference & 2
 KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
Knee Injuries. PSK 4U Mr. S. Kelly North Grenville DHS. Medial Collateral Ligament Sprain
 Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Apophysis. Apophyseal Avulsion. Apophyseal avulsion injuries 3/2/2017
 Apophysis 0 Differentiate from Epiphysis: The end of long bones which undergo endochondral ossification to produce longitudinal growth of the bones. i.e. growth plates 0 Apophysis refers to any eminence,
Apophysis 0 Differentiate from Epiphysis: The end of long bones which undergo endochondral ossification to produce longitudinal growth of the bones. i.e. growth plates 0 Apophysis refers to any eminence,
Lower Limb. Hamstring Strains. Risk Factors. Dr. Peter Friis 27/04/15. 16% missed games AFL 6-15% injury in rugby 30% recurrent
 Lower Limb Dr. Peter Friis MB BS FACSP Sports Physician Hamstring Strains 16% missed games AFL 6-15% injury in rugby 30% recurrent Risk Factors Modifiable Warm up Fatigue Strength Flexibility L/Spine Pelvic
Lower Limb Dr. Peter Friis MB BS FACSP Sports Physician Hamstring Strains 16% missed games AFL 6-15% injury in rugby 30% recurrent Risk Factors Modifiable Warm up Fatigue Strength Flexibility L/Spine Pelvic
Biceps Femoris Muscle in Dogs Diana Powell 11/25/2016
 Biceps Femoris Muscle in Dogs Diana Powell 11/25/2016 The Biceps Femoris is the largest muscle in the muscle group that makes up the hamstring. The Biceps Femoris is covered only by fascia and skin and
Biceps Femoris Muscle in Dogs Diana Powell 11/25/2016 The Biceps Femoris is the largest muscle in the muscle group that makes up the hamstring. The Biceps Femoris is covered only by fascia and skin and
Muscle Testing of Knee Extensors. Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department
 Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
MCL Injuries: When and How to Repair Scott D. Mair, MD
 MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
Understanding Your ACL Injury
 Scott Bissell, MD Connecticut Orthopedic Associates www.ctorthoassociates.com Understanding Your ACL Injury The ACL (Anterior Cruciate Ligament) is a commonly injured ligament in the knee. Please see the
Scott Bissell, MD Connecticut Orthopedic Associates www.ctorthoassociates.com Understanding Your ACL Injury The ACL (Anterior Cruciate Ligament) is a commonly injured ligament in the knee. Please see the
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Jumper s Knee in Children and Adolescents
 A Patient s Guide to Jumper s Knee in Children and Adolescents 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Jumper s Knee in Children and Adolescents 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
ACL Rehabilitation and Return To Play
 ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
Rehabilitation and Return to Play Following Achilles Tendon Repair
 Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Lateral knee injuries
 Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
SOFT TISSUE KNEE INJURIES
 SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Sprained Ankle An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ankle sprains are common injuries that occur among people of all ages. They
Sprained Ankle An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ankle sprains are common injuries that occur among people of all ages. They
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Accelerated Rehabilitation Following ACL Allograft Reconstruction
 Page 1 of 7 Accelerated Rehabilitation Following ACL Allograft Reconstruction PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension)
Page 1 of 7 Accelerated Rehabilitation Following ACL Allograft Reconstruction PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension)
Sports Medicine 15. Unit I: Anatomy. The knee, Thigh, Hip and Groin. Part 4 Anatomies of the Lower Limbs
 Sports Medicine 15 Unit I: Anatomy Part 4 Anatomies of the Lower Limbs The knee, Thigh, Hip and Groin Anatomy of the lower limbs In Part 3 of this section we focused upon 11 of the 12 extrinsic muscles
Sports Medicine 15 Unit I: Anatomy Part 4 Anatomies of the Lower Limbs The knee, Thigh, Hip and Groin Anatomy of the lower limbs In Part 3 of this section we focused upon 11 of the 12 extrinsic muscles
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement. Normalize gait pattern with brace (if indicated) and crutches
 General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
Accelerated Rehabilitation Following ACL-PTG Reconstruction
 Accelerated Rehabilitation Following ACL-PTG Reconstruction I. Phase I Preoperative Phase Goals: Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore
Accelerated Rehabilitation Following ACL-PTG Reconstruction I. Phase I Preoperative Phase Goals: Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore
Rehabilitation of an ACL injury in a 29 year old male with closed kinetic chain exercises: A case study
 Abstract Objective: This paper will examine a rehabilitation program for a healthy 29 year old male who sustained an incomplete tear of the left ACL. Results: Following a 9 week treatment plan focusing
Abstract Objective: This paper will examine a rehabilitation program for a healthy 29 year old male who sustained an incomplete tear of the left ACL. Results: Following a 9 week treatment plan focusing
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL. WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches.
 REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION
 REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION I. IMMEDIATE POST OPERATIVE PHASE POD 1 POD 2 to 3 Brace: EZ Wrap brace locked at zero degrees extension or Protonics Rehab System (PRS) as directed by physician
REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION I. IMMEDIATE POST OPERATIVE PHASE POD 1 POD 2 to 3 Brace: EZ Wrap brace locked at zero degrees extension or Protonics Rehab System (PRS) as directed by physician
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 3/2017
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 3/2017
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015
 PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Anterior Cruciate Ligament (ACL) Injuries
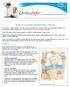 Anterior Cruciate Ligament (ACL) Injuries This article is also available in Spanish: Lesiones del ligamento cruzado anterior (topic.cfm?topic=a00697) and Portuguese: Lesões do ligamento cruzado anterior
Anterior Cruciate Ligament (ACL) Injuries This article is also available in Spanish: Lesiones del ligamento cruzado anterior (topic.cfm?topic=a00697) and Portuguese: Lesões do ligamento cruzado anterior
A Patient s Guide to Posterior Cruciate Ligament Injuries
 A Patient s Guide to Posterior Cruciate Ligament Injuries 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Posterior Cruciate Ligament Injuries 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
Achilles Tendon Repair and Rehabilitation
 1 Achilles Tendon Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The poorest blood supply to the Achilles tendon is in the central part of the tendon approximately
1 Achilles Tendon Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The poorest blood supply to the Achilles tendon is in the central part of the tendon approximately
Mohammad Ashraf. Abdulrahman Al-Hanbali. Ahmad Salman. 1 P a g e
 - 7 Mohammad Ashraf Abdulrahman Al-Hanbali Ahmad Salman 1 P a g e Structures under the cover of Gluteus Maximus: 1-Bones: Ileum, Femur (Head, greater trochanter and gluteal tuberosity), Ischium (ischial
- 7 Mohammad Ashraf Abdulrahman Al-Hanbali Ahmad Salman 1 P a g e Structures under the cover of Gluteus Maximus: 1-Bones: Ileum, Femur (Head, greater trochanter and gluteal tuberosity), Ischium (ischial
Human anatomy reference:
 Human anatomy reference: Weak Glut Activation Weak gluteal activation comes from poor biomechanics, poor awareness when training or prolonged exposure in deactivated positions such as sitting. Weak Glut
Human anatomy reference: Weak Glut Activation Weak gluteal activation comes from poor biomechanics, poor awareness when training or prolonged exposure in deactivated positions such as sitting. Weak Glut
Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Athletic Preparation ACL Reconstruction - Accelerated Rehabilitation. Autologous Bone-Tendon-Bone, Patella Tendon Graft
 Orthopaedic Sports Specialists, P.C. Michael E. Joyce, M.D. 84 Glastonbury Blvd., Suite 101, Glastonbury, Connecticut 06033 Voice: 860-652-8883, Fax: 860-652-8887 Athletic Preparation ACL Reconstruction
Orthopaedic Sports Specialists, P.C. Michael E. Joyce, M.D. 84 Glastonbury Blvd., Suite 101, Glastonbury, Connecticut 06033 Voice: 860-652-8883, Fax: 860-652-8887 Athletic Preparation ACL Reconstruction
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
Knee Movement Coordination Deficits. ICD-9-CM: Sprain of cruciate ligament of knee
 1 Knee Movement Coordination Deficits Anterior Cruciate Ligament ACL Tear ICD-9-CM: 844.2 Sprain of cruciate ligament of knee ACL Insufficiency ICD-9-CM: 717.83 Old disruption of anterior cruciate ligament
1 Knee Movement Coordination Deficits Anterior Cruciate Ligament ACL Tear ICD-9-CM: 844.2 Sprain of cruciate ligament of knee ACL Insufficiency ICD-9-CM: 717.83 Old disruption of anterior cruciate ligament
Index. G Gluteal exercises,
 A Achilles tendon, 66, 74 ACL. See Anterior cruciate ligament (ACL) ACL Quality of Life (ACL-QOL) questionnaire, 83 Active assistive range of motion (AAROM), 122, 129 Active range of motion (AROM), 48,
A Achilles tendon, 66, 74 ACL. See Anterior cruciate ligament (ACL) ACL Quality of Life (ACL-QOL) questionnaire, 83 Active assistive range of motion (AAROM), 122, 129 Active range of motion (AROM), 48,
Rehabilitation Following Acute ACL, PCL, LCL, PL & Lateral Hamstring Repair
 Page 1 of 7 Rehabilitation Following Acute ACL, PCL, LCL, PL & Lateral Hamstring Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of motion (gradual knee
Page 1 of 7 Rehabilitation Following Acute ACL, PCL, LCL, PL & Lateral Hamstring Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of motion (gradual knee
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon
 Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Bone-Patellar tendon-bone Autograft ACL Recon. Date of Surgery: Patient Name:
 Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact)
 STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
Review relevant anatomy of the foot and ankle. Learn the approach to examining the foot and ankle
 Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
