Interlocking Telescopic Rod for Patients with Osteogenesis Imperfecta
|
|
|
- Barnard Benedict Perry
- 5 years ago
- Views:
Transcription
1 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Interlocking Telescopic Rod for Patients with Osteogenesis Imperfecta Tae-Joon Cho, In Ho Choi, Chin Youb Chung, Won Joon Yoo, Ki Seok Lee and Dong Yeon Lee J Bone Joint Surg Am. 2007;89: doi: /jbjs.f This information is current as of September 4, 2009 Supplementary material Reprints and Permissions Publisher Information Commentary and Perspective, data tables, additional images, video clips and/or translated abstracts are available for this article. This information can be accessed at Click here to order reprints or request permission to use material from this article, or locate the article citation on jbjs.org and click on the [Reprints and Permissions] link. The Journal of Bone and Joint Surgery 20 Pickering Street, Needham, MA
2 1028 COPYRIGHT 2007 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Interlocking Telescopic Rod for Patients with Osteogenesis Imperfecta By Tae-Joon Cho, MD, In Ho Choi, MD, Chin Youb Chung, MD, Won Joon Yoo, MD, Ki Seok Lee, MD, and Dong Yeon Lee, MD Investigation performed at the Department of Orthopaedic Surgery, Seoul National University Children s Hospital, Seoul, South Korea Background: Intramedullary fixation with use of a telescopic rod with a T-piece is one of the standard methods for long-bone stabilization in growing children with osteogenesis imperfecta. However, installation and removal of this device can cause substantial damage to the distal joint, which limits its use, especially in the tibia. We devised a modification of the telescopic rod system the interlocking telescopic rod in which the obturator is a simple rod with a hole, instead of a T-piece, at its distal end. Methods: The clinical and radiographic outcomes were evaluated more than two years following treatment of thirtytwo limb segments (twenty-three tibiae and nine femora) with this new rod system in fifteen patients with osteogenesis imperfecta. Results: All rods were inserted without an arthrotomy of the distal joint, and all telescoped successfully. The interlocking pin used in the first five limb segments backed out between five and thirty-three months postoperatively. A revised fixation technique was used in the remaining twenty-seven limb segments, and the interlocking pin had not backed out at an average 3.1 years postoperatively. Proximal migration of the obturator was observed in four tibiae after 2.5 years. The cumulative survival rate of the rod at four years postoperatively was 88.7%. Conclusions: Both insertion and removal of an interlocking telescopic rod are much less invasive than insertion and removal of a conventional telescopic rod with a T-piece anchor. The interlocking pin at the distal epiphysis provides effective anchorage for telescoping. Our interim results showed survival of the device to be comparable with, or better than, that of the conventional telescopic rod. Level of Evidence: Therapeutic Level IV. See Instructions to Authors for a complete description of levels of evidence. The concept of multiple osteotomies and internal fixation with an intramedullary rod for deformity correction and prevention of long-bone fractures in patients with osteogenesis imperfecta was first described by Sofield and Millar in and has been widely accepted. In 1963, Bailey and Dubow 2 introduced an elongating rod system, whereby a hollow sleeve and an internal obturator were engaged and anchored by T-pieces at the proximal and distal epiphyses of the long bones. This design allowed telescoping elongation as the long bone grew at the physes, and effectively decreased the number and frequency of operations required in growing children 3-8. However, its use was technically demanding, and high rates of operative and postoperative complications were reported 6,9-15. The Sheffield telescopic rod was devised to eliminate problems associated with the T-piece 10 but was nevertheless associated with other complications, such as intra-articular, metaphyseal, or extracortical rod migration. Injuries caused by the implantation of elongating rods with a T-piece are substantial but are rarely discussed. Insertion of the distal obturator is more invasive than is insertion of the proximal sleeve in both the femur and the tibia, as it requires an arthrotomy of the distal joint, which may damage the articular cartilage 5,8. Installation of the obturator with a T-piece into the tibia is even more traumatic, requiring com- Disclosure: The authors did not receive any outside funding or grants in support of their research for or preparation of this work. Neither they nor a member of their immediate families received payments or other benefits or a commitment or agreement to provide such benefits from a commercial entity. No commercial entity paid or directed, or agreed to pay or direct, any benefits to any research fund, foundation, division, center, clinical practice, or other charitable or nonprofit organization with which the authors, or a member of their immediate families, are affiliated or associated. J Bone Joint Surg Am. 2007;89: doi: /jbjs.f.00814
3 1029 plete dislocation of the ankle joint or a medial malleolar osteotomy 5,8, possibly damaging the weight-bearing area of the distal tibial articular cartilage. These possible iatrogenic problems along with higher complication rates 13,16 have made use of the telescopic rod in the tibia controversial, and as a result some authors prefer rods that do not elongate 5,8. We developed a new anchorage system to be used in the distal epiphysis to allow telescoping of an elongating rod. This system does not require arthrotomy for insertion of the obturator, and thus damage to ligaments and articular cartilage can be avoided. The system was originally devised for the tibia, but with accumulated experience its use was extended to the femur. The purposes of this study were to introduce this new design and to report the intermediate follow-up results of its use in patients with osteogenesis imperfecta. Materials and Methods Implant Design he interlocking telescopic rod is composed of a hollow T sleeve and an internal obturator. The sleeves are of the same shape and dimension as those used in the telescopic intramedullary rod system (Sheffield Rod; Downs Surgical, Sheffield, England) 10,17. The obturators (Dyna-Locking Telescopic Rod; U&I, Gyeonggi, Korea) have the same diameters as those of the Sheffield rod system. The interlocking telescopic rod does not have a T-piece at the distal end but instead has a small hole that allows the placement of an interlocking pin (a Kirschner wire, with a threaded tip, of 1.4 mm in diameter [for 3, 4, and 5-mm-diameter sleeves] or 1.8 mm in diameter [for 6 and 8-mm-diameter sleeves]) (Fig. 1). The obturators pass all of the way through the corresponding sleeves except for the 3-mm-diameter sleeve, for which the obturator has a widened distal tip to receive a 1.4-mm-diameter interlocking pin. Surgical Technique Preoperative radiographs are thoroughly evaluated to assess the deformity and to estimate the lengths and diameters of the rods to be used. However, for severely angulated limb segments, we determined the rod length intraoperatively, after performing multiple osteotomies. The surgical procedure (Figs. 2-A and 2-B) consists of multilevel osteotomies performed to realign the limb segment along the rod. Percutaneous osteotomies 8 are preferred, but open osteotomies are performed if intramedullary reaming is needed for a narrow or obliterated medullary cavity or resection of a substantial wedge of bone is needed to correct an acute angulation. A Kirschner wire is then inserted through the medullary canal of the osteotomy fragments. The sleeve is cut to an appropriate length and is inserted over the Kirschner wire in an antegrade direction. It is important to ensure that the distal tip of the sleeve points to the center of the distal epiphysis on both anteroposterior and lateral projections of radiographs. The Kirschner wire is then replaced with the obturator, which is advanced antegrade inside the sleeve into the distal epiphysis. The rotational orientation of the hole at its distal end can be controlled and adjusted with use of an obturator-impactor (Fig. 1). With use of a free-hand technique with fluoroscopic imaging, the obturator is then anchored in the distal epiphysis with a Kirschner wire. As the cortex of the Fig. 1 The interlocking telescopic rod system. The hollow sleeve is the same as that used in the Sheffield telescopic rod system (A). The obturator has a hole at its distal tip to receive the interlocking pin (B). The flat proximal end can be fitted and assembled with a rotator-impactor (C).
4 1030 Fig. 2-A Fig. 2-B Schematic drawing of the surgical procedure for insertion of an interlocking telescopic rod in the tibia (Fig. 2-A) and the femur (Fig. 2-B). The obturator is inserted within the sleeve in an antegrade manner and is transfixed at the distal epiphysis.
5 1031 Fig. 3 Anteroposterior and lateral radiographs of the tibia of a five-year-old boy with type-ivb osteogenesis imperfecta. Marked angulation of the tibia (A) was corrected with use of an interlocking telescopic rod (B), which telescoped successfully for three years (C). distal epiphysis is thin in patients with osteogenesis imperfecta, the Kirschner wire can be inserted manually and then advanced by gentle tapping. The wire is cut to an appropriate length and is pushed deep, preferably within the osseous epiphysis. Finally, in the femur, the sleeve position is adjusted so that the T-piece abuts the greater trochanter cartilage within the gluteal muscles. In the tibia, the T-piece of the sleeve is buried within the osseous epiphysis. In this series, it was rotated 90 in ten cases as recommended by Marafioti and Westin 3, but it was placed only subchondrally to facilitate future rod replacement in thirteen cases. In the case of the 3-mm sleeve, through which the obturator cannot pass because of its widened distal tip, the sleeve and obturator are assembled and then inserted as one piece through the osteotomy fragments. When the sleeve reaches its destination, the obturator is further advanced into the distal epiphysis and is transfixed with use of the technique described above. All limbs are immobilized with a long leg splint for four to six weeks postoperatively. Patients and Evaluation This study was approved by our institutional review board, and the patients and/or their parents gave informed consent to participate. The first fifteen consecutive patients (seven girls and eight boys) with osteogenesis imperfecta who had undergone insertion of an interlocking telescopic rod into the femur or tibia and had been followed for more than two years after the index operation were included. Three patients had osteogenesis imperfecta type I according to the classification system of Sillence et al. 18, three had type III, and nine had type IV. Twenty-three tibiae and nine femora underwent surgery. The patient s age at the time of the surgery and the follow-up period were recorded separately for each operatively treated limb segment. The mean age at the time of the surgery was 7.3 years (range, 1.9 to 11.9 years), and the mean duration of follow-up was 3.3 years (range, 2.0 to 6.9 years). Follow-up was considered to be complete when any part of the rod system was removed or when skeletal maturity was reached. All patients received a bisphosphonate, either oral alendronate or cyclic intravenous pamidronate, before and after the index operations. The patients were examined clinically every three to six months, and radiographs were made every six to twelve months. The fracture history and complications were recorded. Survival analysis with the Kaplan-Meier method was performed with use of SPSS for Windows software (version 12.0; SPSS, Chicago, Illinois). In the calculation of surgeryfree survival, any additional surgical intervention such as removal or replacement of the interlocking telescopic rod, advancement of the proximally migrated sleeve, or adjustment of the interlocking pin was defined as the end point. In the calculation of rod survival, the end point was defined as removal or replacement of the rod due to a complication. As long as a rod remained in the operatively treated limb segment, regardless of whether it was elongating, it was considered to have not reached the end point. Results pplication of the intramedullary rod and the interlocking A pin fixation were performed successfully in all limb segments, and telescoping took place uneventfully in all of the segments for at least eighteen months (Figs. 3 and 4). Five operatively treated limb segments sustained a fracture postoperatively: one femur showed a stress fracture, and the other femur and the three tibiae sustained a linear fracture
6 1032 Fig. 4 Anteroposterior radiographs of the femur of a two-year-old girl with type-iii osteogenesis imperfecta. She sustained a femoral shaft fracture (A), which was fixed with an interlocking telescopic rod (B). The rod telescoped successfully for 2.3 years (C). Fig. 5 Anteroposterior radiographs of the tibia of a 4.5-year-old girl with type-iva osteogenesis imperfecta. Repeated tibial shaft fractures were treated with use of an interlocking telescopic rod. Radiographs made at one month (A), 1.5 years (B), two years (C), and three years (D) showed proximal migration of the obturator with the interlocking pin cutting through the physis, although no obvious physeal closure was detected at this site. The interlocking telescopic rod eventually functioned as a non-elongating rod. following minor trauma. All healed uneventfully after a brief period of immobilization with a splint. In one tibia, in which the interlocking pin had been placed eccentrically at the anterior part of the distal epiphysis, the rod cut through the anterior cortex of the distal part of the tibia. Gradual anterior angulation at the distal part of the tibia resulted in the need for a closing anterior wedge osteotomy and insertion of another interlocking telescopic rod four years postoperatively. Proximal migration of the sleeve was observed in two limb segments. One tibial sleeve, which had
7 1033 Fig. 6 Survival curves for the interlocking telescopic rod. The end point of surgery-free survival was any surgical intervention after the installation of the interlocking telescopic rod. The end point of rod survival was removal or replacement of the rod due to any complication. The dotted lines represent the 95% confidence intervals. been implanted subchondrally, migrated proximally into the knee joint. It was repositioned through a small arthrotomy and then remained subcortical for the next two years. One femoral sleeve migrated proximally and was relocated and tied to the proximal part of the femur with a wire. At the time of the latest follow-up, seven patients could walk without limitation, six could walk a short distance without a walking aid but required an aid for long distances, one required a walking aid at all times, and one could stand and walk only during rehabilitation sessions. Backing out of the interlocking pin was observed, at five to thirty-three months postoperatively, in the first four tibiae and the first femur treated in this series. In these five cases, a smooth Kirschner wire had been used as the interlocking pin. In three of the tibiae, the backed-out interlocking pin was removed, allowing the rod to function as a non-elongating rod. One of these patients reached skeletal maturity without the development of any angulation or fracture of the tibia, whereas the other two patients underwent removal of the rod to treat progressive tibial angulation at the tip of the rod or osteomyelitis. In the remaining two cases, the interlocking pin was replaced with a pin with a threaded tip, which was inserted deep into the epiphysis, as soon as backing out was detected. The new pin did not back out in either of the two cases, which were followed for three and four years. None of the twenty-seven limb segments in which a Kirschner wire with a threaded tip had been used initially had backing out at the time of follow-up, at an average of 3.1 years. Proximal migration of the obturator with the interlocking pin cutting through the physis was observed in four tibiae in two patients. Both had Sillence type-iva osteogenesis imperfecta, and they underwent the index operation at the ages of three and 4.5 years. The proximal migration was detected at 2.5 and three years postoperatively, as the rods failed to telescope even though they appeared straight. In one patient, both interlocking pins were repositioned within the distal epiphysis, after which the sleeves started to migrate distally. In the second patient, no additional surgery was done and the intramedullary rods functioned as non-elongating rods (Fig. 5). Twenty-three (72%) of the thirty-two rods telescoped for an average of 2.8 years without any complications. The cumulative surgery-free survival rate of the rods was 90.6% (95% confidence interval, 80.5% to 100.7%) at two years, 71.6% (95% confidence interval, 53.1% to 90.0%) at three years, and 58.7% (95% confidence interval, 36.4% to 81.0%) at four years (Fig. 6). The rod had to be removed or replaced in only three cases. The cumulative survival rate of the rod itself was 88.7% (95% confidence interval, 73.7% to 103.6%) at four years (Fig. 6).
8 1034 Discussion ultiple osteotomies with intramedullary fixation are the M mainstay of treatment of the long bones of growing children with osteogenesis imperfecta. We believe that the use of an elongating rod is beneficial in patients with substantial remaining growth. However, the Bailey-Dubow elongating nail has been associated with a high complication rate, particularly related to the T-piece 6,9-15. The Sheffield telescopic rod system, a modification of the Bailey-Dubow nail, eliminated T-piece-related complications by permanently fixing the T- piece to the sleeve 10,17, but it shares the problems of traumatic insertion and rod migration with its predecessor 19,20. Placement of an obturator with a T-piece at the distal fragment is an invasive procedure, especially in the tibia. It requires almost complete dislocation of the ankle joint with use of either extensive division of the deltoid ligament or medial malleolar osteotomy 7,11,17,19,20. Also, the T-piece has to be inserted through the weight-bearing surface of the distal tibial articular cartilage, which leaves a large scar in a relatively narrow area. Some authors 3,9,20 have reported no functional change of the ankle joint after ankle arthrotomy, but damaged articular cartilage and subsequent fibrocartilaginous healing are highly likely to have a detrimental effect on the ankle joint in the long run, especially in patients who can walk. Therefore, installation of the telescopic rod with a T- piece remains controversial for tibial bones 8. Janus et al. 15 described a modification of the Sheffield rod system for the tibia in which a prebent obturator was anchored at the medial malleolus, eliminating the need for an arthrotomy of the ankle joint. However, ankle valgus deformity due to an inadequately prebent obturator was observed in some cases. With use of the interlocking telescopic rod reported on here, not only can ankle joint arthrotomy and damage to the distal tibial articular cartilage be avoided, but accurate anatomic alignment of the tibia can be restored. Another problem associated with distal tibial fixation is that often the distal tibial epiphysis in patients with osteogenesis imperfecta is hypoplastic compared with the proximal epiphysis. As the distal fixation pin of the interlocking telescopic rod is thinner than the T-piece, the interlocking telescopic rod can be used in younger children. In the current series, the youngest patient treated with a tibial interlocking telescopic rod was 3.2 years old. It is not uncommon for patients with osteogenesis imperfecta to require revision surgery as they age. Sometimes an obturator with a T-piece is impossible to remove without causing serious damage to the joint or surrounding tissue 7. In the interlocking telescopic rod system, the obturator can be converted into a smooth rod simply by removing the interlocking pin. Then the obturator can be easily removed through the diaphyseal medullary cavity or through the articular cartilage with minimal injury. The concept of interlocking the telescopic rod at the distal part of the tibia is not new. Bailey 4 reported a case in which the sleeve was placed distally and then transfixed with use of a cross-wire passed through the epiphysis. However, this configuration failed as the interlocking pin backed out. The smooth interlocking pins that we used initially, in the first four tibiae and the first femur that we treated, backed out, but this problem was overcome by using a Kirschner wire with a threaded tip and inserting it deep into the chondroepiphysis. Failure of telescoping and subsequent intramedullary migration of the rod have been reported in several clinical series 6,7,9-11,13-16,20. A telescopic rod elongates only when the forces generated by proximal and distal fixation points exceed the friction forces between the sleeve and the obturator and between the hardware and the surrounding tissue. However, there appears to be a gray zone since, although the rod appears straight and continues to telescope to some extent, the fixation end of the device may cut through the physis (Fig. 5). Karbowski et al. reported that the tibia has a higher rate of this complication than does the femur and that cutting through by the T-piece occurs more frequently at the distal part of the tibia 16. We believe that the interlocking pin used with the interlocking telescopic rod, if properly implanted, provides stronger anchorage than does a T-piece. However, the obturator migrated proximally along with its interlocking pin in four of our thirty-two cases. If this complication occurs, we recommend no additional surgery; instead, we believe that the implant should be allowed to function as a non-elongating rod. Revision surgery is indicated only if substantial angulation, symptomatic anterior cortical cutting through, or a fracture developed at the tip of the outgrown rod. All patients in the present series received bisphosphonate therapy for varying periods to strengthen the cortical bone and thereby prevent gradual angulation of the diaphysis, which helped to minimize the chance of the telescoping failing. However, the bisphosphonate may not have contributed appreciably to the strength of the distal fixation because additional bone formation on the epiphyseal side is less apparent than on the metaphyseal side 21. It is difficult to compare the survival of the interlocking telescopic rod with that of previously described telescopic rods because all series differ in terms of the definitions of complications or failure, surgical procedures used for insertion, and patient profiles. Marafioti and Westin 3 reported that the three-year rate of survival of the elongating rods in their series was 77%. In our series, all of the rods survived for three years postoperatively, and the four-year survival rate was 89%. In summary, we described a new telescopic intramedullary rod system that does not cause injury to the distal articular cartilage of the long bones and that anchors the obturator to the distal epiphysis. The interlocking telescopic rod also appears to be easier to remove, with less trauma, during revision surgery. Our interim results show survivorship comparable with, or better than, that reported for a telescopic rod with a T-piece. Long-term follow-up until skeletal maturity or longer will be necessary to fully evaluate the benefits and limitations of this system.
9 1035 Tae-Joon Cho, MD In Ho Choi, MD Won Joon Yoo, MD Ki Seok Lee, MD Dong Yeon Lee, MD Department of Orthopaedic Surgery, Seoul National University Hospital, 28 Yeongeon-dong, Jongno-gu, Seoul , South Korea. address for I.H. Choi: Chin Youb Chung, MD Department of Orthopaedic Surgery, Seoul National University Bundang Hospital, 300 Gumi-dong, Bundang-gu, Seongnam-si, Gyeonggi-do, , South Korea References 1. Sofield HA, Millar EA. Fragmentation, realignment, and intramedullary rod fixation of deformities of the long bones in children. A ten-year appraisal. J Bone Joint Surg Am. 1959;41: Bailey RW, Dubow HI. Studies of longitudinal bone growth resulting in an extensible nail. Surg Forum. 1963;14: Marafioti RL, Westin GW. Elongating intramedullary rods in the treatment of osteogenesis imperfecta. J Bone Joint Surg Am. 1977;59: Bailey RW. Further clinical experience with the extensible nail. Clin Orthop Relat Res. 1981;159: Niemann KM. Surgical treatment of the tibia in osteogenesis imperfecta. Clin Orthop Relat Res. 1981;159: Gamble JG, Strudwick WJ, Rinsky LA, Bleck EE. Complications of intramedullary rods in osteogenesis imperfecta: Bailey-Dubow rods versus nonelongating rods. J Pediatr Orthop. 1988;8: Mulpuri K, Joseph B. Intramedullary rodding in osteogenesis imperfecta. J Pediatr Orthop. 2000;20: Zeitlin L, Fassier F, Glorieux FH. Modern approach to children with osteogenesis imperfecta. J Pediatr Orthop B. 2003;12: Lang-Stevenson AI, Sharrard WJ. Intramedullary rodding with Bailey-Dubow extensible rods in osteogenesis imperfecta. An interim report of results and complications. J Bone Joint Surg Br. 1984;66: Stockley I, Bell MJ, Sharrard WJ. The role of expanding intramedullary rods in osteogenesis imperfecta. J Bone Joint Surg Br. 1989;71: Nicholas RW, James P. Telescoping intramedullary stabilization of the lower extremities for severe osteogenesis imperfecta. J Pediatr Orthop. 1990;10: Porat S, Heller E, Seidman DS, Meyer S. Functional results of operation in osteogenesis imperfecta: elongating and nonelongating rods. J Pediatr Orthop. 1991;11: Zionts LE, Ebramzadeh E, Stott NS. Complications in the use of the Bailey- Dubow extensible nail. Clin Orthop Relat Res. 1998;348: Jerosch J, Mazzotti I, Tomasevic M. Complications after treatment of patients with osteogenesis imperfecta with a Bailey-Dubow rod. Arch Orthop Trauma Surg. 1998;117: Janus GJ, Vanpaemel LA, Engelbert RH, Pruijs HE. Complications of the Bailey-Dubow elongating nail in osteogenesis imperfecta: 34 children with 110 nails. J Pediatr Orthop B. 1999;8: Karbowski A, Schwitalle M, Brenner R, Lehmann H, Pontz B, Worsdorfer O. Experience with Bailey-Dubow rodding in children with osteogenesis imperfecta. Eur J Pediatr Surg. 2000;10: Wilkinson JM, Scott BW, Clarke AM, Bell MJ. Surgical stabilisation of the lower limb in osteogenesis imperfecta using the Sheffield Telescopic Intramedullary Rod System. J Bone Joint Surg Br. 1998;80: Sillence DO, Senn A, Danks DM. Genetic heterogeneity in osteogenesis imperfecta. J Med Genet. 1979;16: Finidori G, Rigault P, Padovani JP, Bensahel H. L enclouage centro-médullaire télescopique chez l enfant atteint d ostéogenèse imparfaite. [Expanding intramedullary rods in the treatment of osteogenesis imperfecta (author s transl)]. Rev Chir Orthop Reparatrice Appar Mot. 1979;65: French. 20. Luhmann SJ, Sheridan JJ, Capelli AM, Schoenecker PL. Management of lower-extremity deformities in osteogenesis imperfecta with extensible intramedullary rod technique: a 20-year experience. J Pediatr Orthop. 1998;18: Rauch F, Travers R, Munns C, Glorieux FH. Sclerotic metaphyseal lines in a child treated with pamidronate: histomorphometric analysis. J Bone Miner Res. 2004;19:
Telescoping versus non-telescoping rods in the treatment of osteogenesis imperfecta
 Acta Orthop. Belg., 2009, 75, 200-208 ORIGINAL STUDY Telescoping versus non-telescoping rods in the treatment of osteogenesis imperfecta Gamal EL-ADL, Mohamed A. KHALIL, Ahmed ENAN, Mohamed F. MOSTAFA,
Acta Orthop. Belg., 2009, 75, 200-208 ORIGINAL STUDY Telescoping versus non-telescoping rods in the treatment of osteogenesis imperfecta Gamal EL-ADL, Mohamed A. KHALIL, Ahmed ENAN, Mohamed F. MOSTAFA,
A Locking IM Rod that won't back out. Simple and straight to the point! SURGICAL TECHNIQUE
 A Locking IM Rod that won't back out. Simple and straight to the point! SURGICAL TECHNIQUE The SLIM (Simple Locking IntraMedullary) System is a new generation of pediatric orthopedic nails specifically
A Locking IM Rod that won't back out. Simple and straight to the point! SURGICAL TECHNIQUE The SLIM (Simple Locking IntraMedullary) System is a new generation of pediatric orthopedic nails specifically
The Surgical Management of Rickets & Osteogenesis Imperfecta
 The Surgical Management of Rickets & Osteogenesis Imperfecta Dr Greg Firth Chris Hani Baragwanath Academic Hospital Department of Orthopaedics University of the Witwatersrand Rickets Inadequate mineralization
The Surgical Management of Rickets & Osteogenesis Imperfecta Dr Greg Firth Chris Hani Baragwanath Academic Hospital Department of Orthopaedics University of the Witwatersrand Rickets Inadequate mineralization
Case Report. Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology
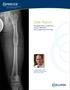 Case Report Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology S. Robert Rozbruch, MD Hospital for Special Surgery New York, NY, USA ABSTRACT This is a case illustrating a 4.5 cm
Case Report Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology S. Robert Rozbruch, MD Hospital for Special Surgery New York, NY, USA ABSTRACT This is a case illustrating a 4.5 cm
Limb lengthening and correction of deformity in the lower limbs of children with osteogenesis imperfecta
 Limb lengthening and correction of deformity in the lower limbs of children with osteogenesis imperfecta K. A. N. Saldanha, M. Saleh, M. J. Bell, J. A. Fernandes From Sheffield Children s Hospital, Sheffield,
Limb lengthening and correction of deformity in the lower limbs of children with osteogenesis imperfecta K. A. N. Saldanha, M. Saleh, M. J. Bell, J. A. Fernandes From Sheffield Children s Hospital, Sheffield,
LOCKING TEP LOCKING TITANIUM ELASTIC PIN INTRAMEDULLARY NAIL
 LOCKING TEP LOCKING TITANIUM ELASTIC PIN INTRAMEDULLARY NAIL ... Index -3 3-8 8 9 9 0 7 Introduction Features Indicatiıons Surgical Technique Femoral Surgical Technique Tibial Surgical Technique Ulna Radius
LOCKING TEP LOCKING TITANIUM ELASTIC PIN INTRAMEDULLARY NAIL ... Index -3 3-8 8 9 9 0 7 Introduction Features Indicatiıons Surgical Technique Femoral Surgical Technique Tibial Surgical Technique Ulna Radius
Change in Effective Leg Length after Angular Deformity Correction by Hemiepiphyseal Stapling
 Original Article Clinics in Orthopedic Surgery 2010;2:85-89 doi:10.4055/cios.2010.2.2.85 Change in Effective Leg Length after Angular Deformity Correction by Hemiepiphyseal Stapling Ho-Joong Jung, MD,
Original Article Clinics in Orthopedic Surgery 2010;2:85-89 doi:10.4055/cios.2010.2.2.85 Change in Effective Leg Length after Angular Deformity Correction by Hemiepiphyseal Stapling Ho-Joong Jung, MD,
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
CASE REPORT. Antegrade tibia lengthening with the PRECICE Limb Lengthening technology
 CASE REPORT Antegrade tibia lengthening with the PRECICE Limb Lengthening technology Austin T. Fragomen, M.D. Hospital for Special Surgery New York, NY 1 1 PR O D U CTS CONDITION Nonunion of an attempted
CASE REPORT Antegrade tibia lengthening with the PRECICE Limb Lengthening technology Austin T. Fragomen, M.D. Hospital for Special Surgery New York, NY 1 1 PR O D U CTS CONDITION Nonunion of an attempted
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
Gentle Guided Growth to Correct Knock Knees and Bowed Legs in Children
 PATIENT INFORMATION Gentle Guided Growth to Correct Knock Knees and Bowed Legs in Children The Guided Growth System eight-plate quad-plate INTRODUCTION Children need gentle guidance and correction in many
PATIENT INFORMATION Gentle Guided Growth to Correct Knock Knees and Bowed Legs in Children The Guided Growth System eight-plate quad-plate INTRODUCTION Children need gentle guidance and correction in many
Study of Ender s Nailing in Paediatric Tibial Shaft Fractures
 Study of Ender s Nailing in Paediatric Tibial Shaft Fractures Dr. Himanshu G. Ladani 1* 1 Ex. Assistant Professor of Orthopaedics, M.P.Shah Medical College, Jamnagar, Gujarat. ABSTRACT Background: Closed
Study of Ender s Nailing in Paediatric Tibial Shaft Fractures Dr. Himanshu G. Ladani 1* 1 Ex. Assistant Professor of Orthopaedics, M.P.Shah Medical College, Jamnagar, Gujarat. ABSTRACT Background: Closed
GREENS SURGICALS. Redefining Excellence INSTRUMENT SYSTEM PREPARED BY: DR. VINAY KUMAR
 GREENS SURGICALS Redefining Excellence TIBIA AND FEMUR INSTRUMENT SYSTEM PREPARED BY: DR. VINAY KUMAR OPERATIVE TECHNIQUES INDEX SR.NO CONTENTS 1 LIST OF INSTRUMENT FOR TIBIA AND FEMUR. 2 RADIO GRAPH OF
GREENS SURGICALS Redefining Excellence TIBIA AND FEMUR INSTRUMENT SYSTEM PREPARED BY: DR. VINAY KUMAR OPERATIVE TECHNIQUES INDEX SR.NO CONTENTS 1 LIST OF INSTRUMENT FOR TIBIA AND FEMUR. 2 RADIO GRAPH OF
Sirus Antegrade Femoral Nail System Surgical Technique
 Sirus Antegrade Femoral Nail System Surgical Technique The Cannulated Titanium Nail with Anatomical Shape and Lateral Entry Point Disclaimer This document is intended exclusively for experts in the field,
Sirus Antegrade Femoral Nail System Surgical Technique The Cannulated Titanium Nail with Anatomical Shape and Lateral Entry Point Disclaimer This document is intended exclusively for experts in the field,
Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation
 Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation By Leonhard E. Ramseier, MD, Joseph A. Janicki, MD, Shannon Weir, BSc, and Unni G. Narayanan, MBBS, MSc, FRCSC Investigation performed
Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation By Leonhard E. Ramseier, MD, Joseph A. Janicki, MD, Shannon Weir, BSc, and Unni G. Narayanan, MBBS, MSc, FRCSC Investigation performed
Isolated congenital anterolateral bowing of the fibula : A case report with 24 years follow-up
 Acta Orthop. Belg., 2009, 75, 842-846 CASE REPORT Isolated congenital anterolateral bowing of the fibula : A case report with 24 years follow-up Karolien LELIEFELD, Hans VAN DER SLUIJS, Ibo VAN DER HAVEN
Acta Orthop. Belg., 2009, 75, 842-846 CASE REPORT Isolated congenital anterolateral bowing of the fibula : A case report with 24 years follow-up Karolien LELIEFELD, Hans VAN DER SLUIJS, Ibo VAN DER HAVEN
Principles of intramedullary nailing. Management for ORP
 Principles of intramedullary nailing Eakachit Sikarinklul,MD Basic Principles of Fracture Management for ORP Bangkok Medical Center Bangkok, 22-24 July 2016 Learning outcomes At the end of this lecture
Principles of intramedullary nailing Eakachit Sikarinklul,MD Basic Principles of Fracture Management for ORP Bangkok Medical Center Bangkok, 22-24 July 2016 Learning outcomes At the end of this lecture
THE RING BUTTERFLY FRAGMENT
 THE RING BUTTERFLY FRAGMENT Pages with reference to book, From 80 To 82 Philip D`Sousa, Masood Umer, Riaz Hussain Lakdawala ( Department of Surgery (Orthopaedics), The Aga Khan University, Karachi. ) In
THE RING BUTTERFLY FRAGMENT Pages with reference to book, From 80 To 82 Philip D`Sousa, Masood Umer, Riaz Hussain Lakdawala ( Department of Surgery (Orthopaedics), The Aga Khan University, Karachi. ) In
CASE REPORT. Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur
 PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
Tibial deformity correction by Ilizarov method
 International Journal of Research in Orthopaedics http://www.ijoro.org Case Report DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180422 Tibial deformity correction by Ilizarov method Robert
International Journal of Research in Orthopaedics http://www.ijoro.org Case Report DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180422 Tibial deformity correction by Ilizarov method Robert
Surgical Technique. Fibula Rod System
 Surgical Technique Fibula Rod System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve patient
Surgical Technique Fibula Rod System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve patient
Technique Guide. TomoFix Osteotomy System. A comprehensive plating system for stable fixation of osteotomies around the knee.
 Technique Guide TomoFix Osteotomy System. A comprehensive plating system for stable fixation of osteotomies around the knee. Table of Contents Introduction TomoFix Osteotomy System 2 AO Principles 4 Indications
Technique Guide TomoFix Osteotomy System. A comprehensive plating system for stable fixation of osteotomies around the knee. Table of Contents Introduction TomoFix Osteotomy System 2 AO Principles 4 Indications
Conventus CAGE PH Surgical Techniques
 Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Intramedullary Rodding and Bisphosphonate Treatment of Polyostotic Fibrous Dysplasia Associated With the. rodding McCune-Albright syndrome.
 Journal of Pediatric Orthopaedics 22:255 260 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Intramedullary Rodding and Bisphosphonate Treatment of Polyostotic Fibrous Dysplasia Associated With
Journal of Pediatric Orthopaedics 22:255 260 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Intramedullary Rodding and Bisphosphonate Treatment of Polyostotic Fibrous Dysplasia Associated With
Lower Extremity Alignment: Genu Varum / Valgum
 Lower Extremity Alignment: Genu Varum / Valgum Arthur B Meyers, MD Nemours Children s Hospital & Health System Associate Professor of Radiology, University of Central Florida Clinical Associate Professor
Lower Extremity Alignment: Genu Varum / Valgum Arthur B Meyers, MD Nemours Children s Hospital & Health System Associate Professor of Radiology, University of Central Florida Clinical Associate Professor
Knee spanning solutions
 Knee spanning solutions System features Indications Intended to be used on adults or pediatric patients as required for fracture fixation (open or closed); post-traumatic joint contracture which has resulted
Knee spanning solutions System features Indications Intended to be used on adults or pediatric patients as required for fracture fixation (open or closed); post-traumatic joint contracture which has resulted
Fibula Rod System. Lateral Malleolus Fracture Indications:
 Fibula Rod System Fibula Rod System Since 1988, Acumed has been designing solutions for the demanding situations facing orthopaedic surgeons, hospitals and their patients. Our strategy has been to know
Fibula Rod System Fibula Rod System Since 1988, Acumed has been designing solutions for the demanding situations facing orthopaedic surgeons, hospitals and their patients. Our strategy has been to know
THE NANCY NAIL. The End Caps ADVANTAGES OF NANCY NAIL
 NANCY NAIL THE NANCY NAIL Nancy nails are manufactured from a specific titanyum alloy with proprietary surface treatment, which provides increased fatigue resistance. Six nail diameters (1.5 mm 2.0 mm
NANCY NAIL THE NANCY NAIL Nancy nails are manufactured from a specific titanyum alloy with proprietary surface treatment, which provides increased fatigue resistance. Six nail diameters (1.5 mm 2.0 mm
Multiapical Deformities p. 97 Osteotomy Concepts and Frontal Plane Realignment p. 99 Angulation Correction Axis (ACA) p. 99 Bisector Lines p.
 Normal Lower Limb Alignment and Joint Orientation p. 1 Mechanical and Anatomic Bone Axes p. 1 Joint Center Points p. 5 Joint Orientation Lines p. 5 Ankle p. 5 Knee p. 5 Hip p. 8 Joint Orientation Angles
Normal Lower Limb Alignment and Joint Orientation p. 1 Mechanical and Anatomic Bone Axes p. 1 Joint Center Points p. 5 Joint Orientation Lines p. 5 Ankle p. 5 Knee p. 5 Hip p. 8 Joint Orientation Angles
EVOS MINI with IM Nailing
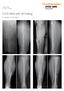 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Techique. Results. Discussion. Materials & Methods. Vol. 2 - Year 1 - December 2005
 to each other. The most distal interlocking hole is 3 mm proximal to distal end of nail, is in anteroposterior direction & proximal distal interlocking hole is in medial to lateral direction i.e. at right
to each other. The most distal interlocking hole is 3 mm proximal to distal end of nail, is in anteroposterior direction & proximal distal interlocking hole is in medial to lateral direction i.e. at right
Lengthening & Deformity correction with. Fixator Assisted Nailing
 Lengthening & Deformity correction with Fixator Assisted Nailing External Fixation Used as *Intra-Op Alignment tool * for lengthening with the main intention of reducing External fixation time! Advantages
Lengthening & Deformity correction with Fixator Assisted Nailing External Fixation Used as *Intra-Op Alignment tool * for lengthening with the main intention of reducing External fixation time! Advantages
LCP Distal Tibia Plate
 Surgical Technique LCP Locking Compression Plate Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF Table of contents Indications 3 Implants/Instruments 5 Surgical
Surgical Technique LCP Locking Compression Plate Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF Table of contents Indications 3 Implants/Instruments 5 Surgical
ROTATIONAL PILON FRACTURES
 CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
Pediatric Tibia Fractures Key Points. Christopher Iobst, MD
 Pediatric Tibia Fractures Key Points Christopher Iobst, MD Goals Bone to heal Return to full weight bearing Acceptable alignment rule of 10s 10 degrees of varus 8 degrees of valgus 12 degrees of procurvatum
Pediatric Tibia Fractures Key Points Christopher Iobst, MD Goals Bone to heal Return to full weight bearing Acceptable alignment rule of 10s 10 degrees of varus 8 degrees of valgus 12 degrees of procurvatum
LCP Metaphyseal Plate for distal medial tibia. Anatomically precontoured metaphyseal plate.
 Indications The LCP Metaphyseal Plate for distal medial tibia is a preshaped plate that allows optimal treatment of juxta-articular fractures of the distal tibia extending into the shaft area. This plate
Indications The LCP Metaphyseal Plate for distal medial tibia is a preshaped plate that allows optimal treatment of juxta-articular fractures of the distal tibia extending into the shaft area. This plate
Patient Guide. Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening
 Patient Guide Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening Introduction You have decided to have a limb lengthening operation. The surgery you have chosen uses a device
Patient Guide Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening Introduction You have decided to have a limb lengthening operation. The surgery you have chosen uses a device
ANATOMIC SURGICAL TECHNIQUE. 5 in 1. Conventional instrumentation 07/11/2013
 ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
S U R G I C A L T E C H N I Q U E David A. McQueen, MD Return to Menu
 S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Lower Extremity Fracture Management. Fractures of the Hip. Lower Extremity Fractures. Vascular Anatomy. Lower Extremity Fractures in Children
 Lower Extremity Fracture Management Brian Brighton, MD, MPH Levine Children s s Hospital Carolinas Medical Center Charlotte, NC Oscar Miller Day October 16, 2009 Lower Extremity Fractures in Children Anatomic
Lower Extremity Fracture Management Brian Brighton, MD, MPH Levine Children s s Hospital Carolinas Medical Center Charlotte, NC Oscar Miller Day October 16, 2009 Lower Extremity Fractures in Children Anatomic
Physeal Fractures and Growth Arrest
 Physeal Fractures and Growth Arrest Raymond W. Liu, M.D. Victor M. Goldberg Master Clinician-Scientist in Orthopaedics Rainbow Babies and Children s Hospital Case Western Reserve University Outline General
Physeal Fractures and Growth Arrest Raymond W. Liu, M.D. Victor M. Goldberg Master Clinician-Scientist in Orthopaedics Rainbow Babies and Children s Hospital Case Western Reserve University Outline General
Large Distractor Femur
 Fracture Reduction and Provisional Stabilization Large Distractor Femur Surgical Technique Table of Contents Introduction Standard Femoral Distraction 2 Large Distractor System 4 Surgical Technique Prepare
Fracture Reduction and Provisional Stabilization Large Distractor Femur Surgical Technique Table of Contents Introduction Standard Femoral Distraction 2 Large Distractor System 4 Surgical Technique Prepare
Wichita Fusion Nail Surgical Technique. David A. McQueen, MD
 Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
Alignment Rod. For intraoperatively confirming correction of the mechanical leg axis.
 Alignment Rod. For intraoperatively confirming correction of the mechanical leg axis. Easy to use Accuracy of surgery Reduces X-ray exposure Table of Contents Introduction Alignment Rod 2 Handling Technique
Alignment Rod. For intraoperatively confirming correction of the mechanical leg axis. Easy to use Accuracy of surgery Reduces X-ray exposure Table of Contents Introduction Alignment Rod 2 Handling Technique
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation *
 Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System.
 LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM
 3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM Part of the DePuy Synthes Variable Angle Periarticular Plating System SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION 3.5 mm VA-LCP Proximal Tibial Plate 2 AO
3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM Part of the DePuy Synthes Variable Angle Periarticular Plating System SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION 3.5 mm VA-LCP Proximal Tibial Plate 2 AO
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
A locking plate system that expands a surgeon s options in trauma surgery. Zimmer NCB Plating System
 A locking plate system that expands a surgeon s options in trauma surgery Zimmer NCB Plating System The Power of Choice The power of having true intraoperative options is at your fingertips. Using standard
A locking plate system that expands a surgeon s options in trauma surgery Zimmer NCB Plating System The Power of Choice The power of having true intraoperative options is at your fingertips. Using standard
NEXGEN COMPLETE KNEE SOLUTION S A. Tibial Stem Extension & Augmentation Surgical. ATechnique
 NEXGEN COMPLETE KNEE SOLUTION ATechnique Tibial Stem Extension & Augmentation Surgical INTRODUCTION The NexGen Complete Knee Solution Intramedullary Tibial Instruments have been designed to provide an
NEXGEN COMPLETE KNEE SOLUTION ATechnique Tibial Stem Extension & Augmentation Surgical INTRODUCTION The NexGen Complete Knee Solution Intramedullary Tibial Instruments have been designed to provide an
Clinical Evaluation Surgical Technique
 Clinical Evaluation Surgical Technique Table of Contents EMPERION Specifications 3 EMPERION Surgical Technique 9 EMPERION Catalog 18 Nota Bene: This technique description herein is made available to the
Clinical Evaluation Surgical Technique Table of Contents EMPERION Specifications 3 EMPERION Surgical Technique 9 EMPERION Catalog 18 Nota Bene: This technique description herein is made available to the
PediNail Pediatric Femoral Nail
 PediNail Pediatric Femoral Nail Surgical Technique Table of Contents Indications...3 Patient Positioning...3 Approach...4 Reaming...5 Nail Placement...6 Proximal Interlocking...7 Distal Interlocking...8
PediNail Pediatric Femoral Nail Surgical Technique Table of Contents Indications...3 Patient Positioning...3 Approach...4 Reaming...5 Nail Placement...6 Proximal Interlocking...7 Distal Interlocking...8
IMPLANT REMOVAL: AN UNSOLVED CHALLENGE TO ORTHOPAEDICIAN Varunjikar M. D 1, S. C. Joshi 2, Bejoy E Jayan 3, A. M. Varunjikar 4, C. R.
 IMPLANT REMOVAL: AN UNSOLVED CHALLENGE TO ORTHOPAEDICIAN Varunjikar M. D 1, S. C. Joshi 2, Bejoy E Jayan 3, A. M. Varunjikar 4, C. R. Joshi 5 HOW TO CITE THIS ARTICLE: Varunjikar M. D, S. C. Joshi, Bejoy
IMPLANT REMOVAL: AN UNSOLVED CHALLENGE TO ORTHOPAEDICIAN Varunjikar M. D 1, S. C. Joshi 2, Bejoy E Jayan 3, A. M. Varunjikar 4, C. R. Joshi 5 HOW TO CITE THIS ARTICLE: Varunjikar M. D, S. C. Joshi, Bejoy
OPERATING MANUAL AND TECHNIQUE GUIDE FOR TITANIUM FEMORAL AND TIBIAL NAILING SYSTEMS
 OPERATING MANUAL AND TECHNIQUE GUIDE FOR TITANIUM FEMORAL AND TIBIAL NAILING SYSTEMS ORTHO-MEDICAL GMBH TITANIUM FEMORAL NAIL OPERATIVE TECHNIQUE Introduction: Why a new type of femoral nail? The latest
OPERATING MANUAL AND TECHNIQUE GUIDE FOR TITANIUM FEMORAL AND TIBIAL NAILING SYSTEMS ORTHO-MEDICAL GMBH TITANIUM FEMORAL NAIL OPERATIVE TECHNIQUE Introduction: Why a new type of femoral nail? The latest
COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION
 C H A P T E R 3 0 COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION Scott R. Roman, DPM INTRODUCTION The most common fixation for proximal interphalangeal fusion
C H A P T E R 3 0 COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION Scott R. Roman, DPM INTRODUCTION The most common fixation for proximal interphalangeal fusion
2017 Resident Advanced Trauma Techniques Course COMPLICATIONS / CHALLENGES MALUNIONS/DEFORMITY
 2017 Resident Advanced Trauma Techniques Course COMPLICATIONS / CHALLENGES MALUNIONS/DEFORMITY What is a Malunion? Definition: a fracture that has healed in a nonanatomic (i.e. deformed) position Must
2017 Resident Advanced Trauma Techniques Course COMPLICATIONS / CHALLENGES MALUNIONS/DEFORMITY What is a Malunion? Definition: a fracture that has healed in a nonanatomic (i.e. deformed) position Must
REVISION KNEE PROSTHESIS ROTARY PIVOT TOTAL KNEE REPLACEMENT. w w w. a s t o n - m e d i c a l. c o m
 OPERATING TECHNIQUE REVISION KNEE PROSTHESIS ROTARY PIVOT TOTAL KNEE REPLACEMENT w w w. a s t o n - m e d i c a l. c o m I N T R O D U C T I O N O D U C T I O N Parameters to be taken into account: - Failure
OPERATING TECHNIQUE REVISION KNEE PROSTHESIS ROTARY PIVOT TOTAL KNEE REPLACEMENT w w w. a s t o n - m e d i c a l. c o m I N T R O D U C T I O N O D U C T I O N Parameters to be taken into account: - Failure
NeoGen Femoral Nail System
 NeoGen Femoral Nail System LESS IS MORE TE-2070-04 Surgical Technique BLE OF CONTENT Preface Standard Femoral Mode Recon Mode Post-Operative Management Appendix Products Information Indication Patient
NeoGen Femoral Nail System LESS IS MORE TE-2070-04 Surgical Technique BLE OF CONTENT Preface Standard Femoral Mode Recon Mode Post-Operative Management Appendix Products Information Indication Patient
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
NCB Distal Femur System. Surgical Technique
 NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation
 Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation Chatupon Chotigavanichaya MD*, Duangjai Leeprakobboon MD*, Perajit Eamsobhana MD*, Kamolporn Kaewpornsawan
Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation Chatupon Chotigavanichaya MD*, Duangjai Leeprakobboon MD*, Perajit Eamsobhana MD*, Kamolporn Kaewpornsawan
UNCORRECTED PROOF. Femoral elastic nailing in the older child: proceed with caution. V.S. Pai a, *, P. David Gwynne-Jones a, Jean Claude Theis b
 Injury Extra (2004) xxx, xxx xxx 1 www.elsevier.com/locate/inext 2 3 Femoral elastic nailing in the older child: proceed with caution 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 V.S. Pai a,
Injury Extra (2004) xxx, xxx xxx 1 www.elsevier.com/locate/inext 2 3 Femoral elastic nailing in the older child: proceed with caution 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 V.S. Pai a,
Femoral elastic nailing in the older child: proceed with caution
 Injury Extra (2005) 36, 185 189 www.elsevier.com/locate/inext Femoral elastic nailing in the older child: proceed with caution V.S. Pai a, *, P. David Gwynne-Jones a, Jean Claude Theis b a Dunedin Hospital,
Injury Extra (2005) 36, 185 189 www.elsevier.com/locate/inext Femoral elastic nailing in the older child: proceed with caution V.S. Pai a, *, P. David Gwynne-Jones a, Jean Claude Theis b a Dunedin Hospital,
TIBIAL NAILING SYSTEM OPTIONS MADE EASY
 S U R G I C A L T E C H N I Q U E TIBIAL NAILING SYSTEM OPTIONS MADE EASY TABLE OF CONTENTS DESIGN SUMMARY INSTRUMENT OVERVIEW AND JIG OPTIONS 1 2 ENTRY AND CANAL PREP NAIL INSERTION LOCKING NAIL REMOVAL
S U R G I C A L T E C H N I Q U E TIBIAL NAILING SYSTEM OPTIONS MADE EASY TABLE OF CONTENTS DESIGN SUMMARY INSTRUMENT OVERVIEW AND JIG OPTIONS 1 2 ENTRY AND CANAL PREP NAIL INSERTION LOCKING NAIL REMOVAL
IMPORTANT MEDICAL INFORMATION Advanced Orthopaedic Solutions INTRAMEDULLARY NAILS Warnings and Precautions (SINGLE USE ONLY)
 IMPORTANT MEDICAL INFORMATION Advanced Orthopaedic Solutions INTRAMEDULLARY NAILS Warnings and Precautions (SINGLE USE ONLY) IMPORTANT NOTE Intramedullary nails provide an alternative to open reduction
IMPORTANT MEDICAL INFORMATION Advanced Orthopaedic Solutions INTRAMEDULLARY NAILS Warnings and Precautions (SINGLE USE ONLY) IMPORTANT NOTE Intramedullary nails provide an alternative to open reduction
Knee Surgical Technique
 Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
PROXIMAL TIBIAL PLATE
 SURGICAL NÁSTROJE TECHNIQUE PRO ARTROSKOPII PROXIMAL INSTRUMENTS TIBIAL FOR PLATE ARTHROSCOPY Proximal Tibial Plate Description of medical device The Proximal Tibial Plate is used in epyphyseal and metaphyseal
SURGICAL NÁSTROJE TECHNIQUE PRO ARTROSKOPII PROXIMAL INSTRUMENTS TIBIAL FOR PLATE ARTHROSCOPY Proximal Tibial Plate Description of medical device The Proximal Tibial Plate is used in epyphyseal and metaphyseal
Treatment Alternatives for Pediatric Femoral Fractures
 Treatment Alternatives for Pediatric Femoral Fractures Gregory A. Schmale, MD Seattle Children's Hospital, USA, gregory.schmale@seattlechildrens.org version 2 I have no conflicts of interest to report
Treatment Alternatives for Pediatric Femoral Fractures Gregory A. Schmale, MD Seattle Children's Hospital, USA, gregory.schmale@seattlechildrens.org version 2 I have no conflicts of interest to report
TRAUMATOLOGY. Trochanter
 TRAUMATOLOGY Trochanter 1 References Prof. Dr. András Sárváry Head of Department Fővárosi Önkormányzat Péterfy Sándor úti Kórház Rendelőintézet és Baleseti Központ Budapest The following surgical description
TRAUMATOLOGY Trochanter 1 References Prof. Dr. András Sárváry Head of Department Fővárosi Önkormányzat Péterfy Sándor úti Kórház Rendelőintézet és Baleseti Központ Budapest The following surgical description
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of The Tibia
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of R Gupta, T Motten, N Kalsotra,
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of R Gupta, T Motten, N Kalsotra,
The Vilex FUZETM. Dual Thread Screw & Intramedullary Nail in One Implant. The Ultimate TTC Arthrodesis Internal Fixator
 The Vilex FUZETM Dual Thread Screw & Intramedullary Nail in One Implant The Ultimate TTC Arthrodesis Internal Fixator Introduction The Vilex FUZE TM TTC Arthrodesis Compression Nail combines the attributes
The Vilex FUZETM Dual Thread Screw & Intramedullary Nail in One Implant The Ultimate TTC Arthrodesis Internal Fixator Introduction The Vilex FUZE TM TTC Arthrodesis Compression Nail combines the attributes
QUICK REFERENCE GUIDE. The PreFix Fixator (92000 Series) ALWAYS INNOVATING
 21 The PreFix Fixator (92000 Series) ALWAYS INNOVATING INTRODUCTION The PreFix fixator is designed to provide temporary external fixation. This may be needed when local facilities or the condition of the
21 The PreFix Fixator (92000 Series) ALWAYS INNOVATING INTRODUCTION The PreFix fixator is designed to provide temporary external fixation. This may be needed when local facilities or the condition of the
QUICK REFERENCE GUIDE. The Orthofix Femoral Nailing System. By Prof. Dr. D. Pennig
 QUICK REFERENCE GUIDE The Orthofix Femoral Nailing System By Prof. Dr. D. Pennig Whenever possible, femoral fractures should be stabilized within the first 24 hours following injury, provided the patient
QUICK REFERENCE GUIDE The Orthofix Femoral Nailing System By Prof. Dr. D. Pennig Whenever possible, femoral fractures should be stabilized within the first 24 hours following injury, provided the patient
Adult Posttraumatic Reconstruction Using a Magnetic Internal Lengthening Nail
 SUPPLEMENT ARTICLE Adult Posttraumatic Reconstruction Using a Magnetic Internal Lengthening Nail S. Robert Rozbruch, MD Summary: A new generation of internal lengthening nail is now available that has
SUPPLEMENT ARTICLE Adult Posttraumatic Reconstruction Using a Magnetic Internal Lengthening Nail S. Robert Rozbruch, MD Summary: A new generation of internal lengthening nail is now available that has
LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia.
 LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia. LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia.
LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia. LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia.
Use of Unlocked Intramedullary Nailing in Winquist Type I and II Femoral Isthmus Fracture
 Use of Unlocked Intramedullary Nailing in Winquist Type I and II Femoral Isthmus Fracture HT Ling, MBBS (UM), WM Ng, MS Ortho (UM), MK Kwan, MS Ortho (UM), LK Fathi Aizuddeen, MBBS (UM), PCM Tay, MBBS
Use of Unlocked Intramedullary Nailing in Winquist Type I and II Femoral Isthmus Fracture HT Ling, MBBS (UM), WM Ng, MS Ortho (UM), MK Kwan, MS Ortho (UM), LK Fathi Aizuddeen, MBBS (UM), PCM Tay, MBBS
A locking plate system that expands a surgeon s options in trauma surgery. Zimmer NCB Plating System
 A locking plate system that expands a surgeon s options in trauma surgery Zimmer NCB Plating System The Power of Choice The power of having true intraoperative options is at your fingertips. Using standard
A locking plate system that expands a surgeon s options in trauma surgery Zimmer NCB Plating System The Power of Choice The power of having true intraoperative options is at your fingertips. Using standard
THE NATURAL FIT. Surgical Technique. Hip Knee Spine Navigation
 THE NATURAL FIT Surgical Technique Hip Knee Spine Navigation MiniMAX Surgical Technique Hip Knee Spine Navigation INTRODUCTION The MiniMAX TM is a cementless anatomic stem available in 9 right sizes and
THE NATURAL FIT Surgical Technique Hip Knee Spine Navigation MiniMAX Surgical Technique Hip Knee Spine Navigation INTRODUCTION The MiniMAX TM is a cementless anatomic stem available in 9 right sizes and
Zimmer MIS Periarticular Distal Femoral Locking Plate
 For Clinical Evaluations Zimmer MIS Periarticular Distal Femoral Locking Plate Surgical Technique The Science of the Landscape Zimmer MIS Periarticular Distal Femoral Locking Plate Surgical Technique
For Clinical Evaluations Zimmer MIS Periarticular Distal Femoral Locking Plate Surgical Technique The Science of the Landscape Zimmer MIS Periarticular Distal Femoral Locking Plate Surgical Technique
Minimally Invasive Plating of Fractures:
 Minimally Invasive Plating of Fractures: Advantages, Techniques and Trade-offs Matthew Garner, MD Created January 2016 OUTLINE Principles of fracture management The importance of vascular supply Equipment
Minimally Invasive Plating of Fractures: Advantages, Techniques and Trade-offs Matthew Garner, MD Created January 2016 OUTLINE Principles of fracture management The importance of vascular supply Equipment
Technique Guide. 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System.
 Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal
Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal
INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement
 016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
Surgical Technique.
 Surgical Technique www.biomet.co.uk INTRODUCTION design principals Recent advances in imaging technology have enabled orthopaedic surgeons to extend closed treatment of femoral fractures to include more
Surgical Technique www.biomet.co.uk INTRODUCTION design principals Recent advances in imaging technology have enabled orthopaedic surgeons to extend closed treatment of femoral fractures to include more
TRK REVISION KNEE Surgical Technique
 1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
Technique Guide. 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Proximal Humerus Plate 2 AO Principles
Technique Guide 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Proximal Humerus Plate 2 AO Principles
Influence of bone morphology and injured ligament of the ankle on ankle stress radiographs
 Influence of bone morphology and injured ligament of the ankle on ankle stress radiographs Gye Wang Lee, MD, Chin Youb Chung, MD, Moon Seok Park, MD Seung Yeol Lee, MD, Myung Ki Chung, MD, Byung Chae Jo,
Influence of bone morphology and injured ligament of the ankle on ankle stress radiographs Gye Wang Lee, MD, Chin Youb Chung, MD, Moon Seok Park, MD Seung Yeol Lee, MD, Myung Ki Chung, MD, Byung Chae Jo,
Fractures of the Ankle Region in the Skeletally Immature Patient. The Salter Classification is Worthless!!
 Fractures of the Ankle Region in the Skeletally Immature Patient. The Salter Classification is Worthless!! Kaye E Wilkins D.V.M,M.D. President's Council/Dielmann Chair in Pediatric Orthopedics Professor
Fractures of the Ankle Region in the Skeletally Immature Patient. The Salter Classification is Worthless!! Kaye E Wilkins D.V.M,M.D. President's Council/Dielmann Chair in Pediatric Orthopedics Professor
Practical Reduction Techniques: Diaphyseal Reduction. Philip Wolinsky University of California at Davis Medical Center
 OTA Specialty Day 2016 Practical Reduction Techniques: Diaphyseal Reduction Philip Wolinsky University of California at Davis Medical Center 8:55 am 9:55 am Tips and Tricks: Practical Reduction Techniques
OTA Specialty Day 2016 Practical Reduction Techniques: Diaphyseal Reduction Philip Wolinsky University of California at Davis Medical Center 8:55 am 9:55 am Tips and Tricks: Practical Reduction Techniques
Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate
 Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique 1 Zimmer MIS
Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique 1 Zimmer MIS
Technique Guide. LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System.
 Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
Introduction to the Taylor Spatial Frame Hardware. Trademark of Smith & Nephew. Certain marks Reg. US Pat. & TM Off.
 Introduction to the Taylor Spatial Frame Hardware Trademark of Smith & Nephew. Certain marks Reg. US Pat. & TM Off. What is the Taylor Spatial Frame? Next generation circular fixator capable of 6 axes
Introduction to the Taylor Spatial Frame Hardware Trademark of Smith & Nephew. Certain marks Reg. US Pat. & TM Off. What is the Taylor Spatial Frame? Next generation circular fixator capable of 6 axes
TIPMED EXTERNAL FIXATION SYSTEMS
 TIPMED EXTERNAL FIXATION SYSTEMS ANATOMICAL LOCATIONS FOR EXTERNAL FIXATION SYSTEMS Humeral Dynamic Axial Fixator Elbow Fixator Pelvic Dynamic Axial Fixator Pennig Wrist Fixator Hand Fixator Finger Fixator
TIPMED EXTERNAL FIXATION SYSTEMS ANATOMICAL LOCATIONS FOR EXTERNAL FIXATION SYSTEMS Humeral Dynamic Axial Fixator Elbow Fixator Pelvic Dynamic Axial Fixator Pennig Wrist Fixator Hand Fixator Finger Fixator
Axial alignment of the lower extremity in Chinese adults. Journal Of Bone And Joint Surgery - Series A, 2000, v. 82 n. 11, p.
 Title Axial alignment of the lower extremity in Chinese adults Author(s) Tang, WM; Zhu, YH; Chiu, KY Citation Journal Of Bone And Joint Surgery - Series A, 2000, v. 82 n. 11, p. 1603-1608 Issued Date 2000
Title Axial alignment of the lower extremity in Chinese adults Author(s) Tang, WM; Zhu, YH; Chiu, KY Citation Journal Of Bone And Joint Surgery - Series A, 2000, v. 82 n. 11, p. 1603-1608 Issued Date 2000
ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS
 Bahrain Medical Bulletin, Volume 17, Number 2, June 1995 Original ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS Saleh W. Al-Harby, FRCS(Glasg)* This is a prospective study of
Bahrain Medical Bulletin, Volume 17, Number 2, June 1995 Original ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS Saleh W. Al-Harby, FRCS(Glasg)* This is a prospective study of
