SILVER CROSS EMS SEPTEMBER 2014 EMD CE
|
|
|
- Marshall Rich
- 5 years ago
- Views:
Transcription
1 SILVER CROSS EMS SEPTEMBER 2014 EMD CE
2 Sudden illness and medical emergencies are common in children and infants. Anatomical differences exist between adults and children. Respiratory care for children is extremely important.
3 Managing a pediatric emergency can be one of the most stressful situations you face as an EMD. You must remain calm and professional. Unless you are prepared, your anxiety and fear may interfere with your ability to deliver proper instructions. Caller may be at a higher state of anxiety. Ask simple questions about the emergency. Ask to speak to someone else if caller is hysterical and unable to focus on interrogation process.
4 REVIEW OF A, B, C S AND BLS FOR INFANTS AND CHILDREN
5 Differences between children and adults A child s airway is smaller in relation to the rest of the body compared to an adult s airway. A child s tongue is relatively larger than an adult s.
6 A child s upper airway is more flexible than that of an adult. The airway is narrow and more easily obstructed. For at least the first 6 months of their lives, infants can breathe only through their noses. When the demands on a child s respiratory system change, the child is able to quickly compensate by increasing breathing efforts. The child can only compensate for so long before they tire and quickly decompensate.
7 Used with permission of the American Academy of Pediatrics, Pediatric Education for Prehospital Professionals, American Academy of Pediatrics, Gathering information from the caller about the child s, level of consciousness, respiratory effort and skin will quickly give you a general impression of the emergency.
8 Indicator of how well the heart, lungs, and central nervous system are working Compare the child s appearance with what you would expect from a healthy child. Assess eye contact, muscle tone, and skin color. Red Flags: Limp, glassy stare, not interacting with environment or caregivers, high pitched cry or inconsolable.
9 Ask about child s level of distress: Labored breathing with signs of muscles retractions Abnormal sounds like wheezing or gurgling Positioning: tripod sitting up and leaning forward Nasal flaring or grunting
10 Red Flags: Pallor - pale skin or mucous membranes. Mottling blotching skin discoloration that is caused by too much or too little blood flow to skin. Cyanosis bluish tint to skin and mucous membranes from a lack of oxygen.
11 High temperatures are accompanied by: Flushed, red skin Sweating Restlessness Heart rate increases Fevers accompanied with rashes are concerning and could be a sign of a serious illness
12 Causes of cardiopulmonary arrest in children Choking Infections of the airway such as croup and epiglottitis Sudden infant death syndrome (SIDS) Accidental poisonings Injuries around the head and neck ANY RESPIRATORY EMERGENCY CAN LEAD TO CARDIAC ARREST IN PEDIATRIC PATIENTS IF NOT CORRECTED IN A TIMELY MANNER!
13 Opening the airway Use the head tilt chin lift maneuver on children to open the airway. Do not hyperextend the child s neck when you tilt the head back. Because of anatomical differences their airway should be in a more neutral or sniffing position. If no breathing or only gasping, begin CPR.
14 Basic life support for ages 1 and over Use the heel of one hand or two hands to perform chest compressions. Compress the sternum one half to one third the depth of the chest depending on the size of the child. Give breaths, making sure chest is rising. Compression to breath ratio is 30:2.
15 Basic life support for children under 1 year CPR for infants is different from adult CPR. Check for responsiveness by tapping the infant s foot or gently shaking the shoulder. Use your middle and ring fingers to compress the sternum just below the nipple line. Compress the sternum one half to one third the depth of the chest. Give gentle rescue breaths. Compression to Breath ratio is 30:2
16 Severe airway obstruction is a serious emergency. Signs and symptoms Poor air exchange Increased breathing difficulty Silent cough Inability to speak No movement
17 Use Abdominal Thrusts to expel object. Wrap arms around the patient s midsection (above belly button but below ribs) Provide quick inward and upward thrusts
18 If the child becomes unconscious, begin the steps of CPR. Remember to check the mouth for object after the compressions and before giving breaths.
19 An infant is very fragile. If you suspect an airway obstruction, assess the infant to determine whether any air exchange is occurring. If the infant is crying, the airway is not completely obstructed. If no air is moving in or out of the infant s mouth and nose, suspect an obstructed airway. The infant will start to change colors very quickly.
20 Use a combination of back slaps and the chest-thrust maneuver. Assess the infant s airway and breathing. Place the infant in a face-down position over your one arm and deliver five back slaps between the shoulder blades.
21 Use a combination of back slaps and the chest-thrust maneuver. Turn the infant face-up. Deliver five chest thrusts in the middle of the sternum with your two fingers. Repeat these steps until the object is expelled or until the infant becomes unresponsive.
22 If the infant becomes unresponsive, continue with the following steps: Begin CPR, remembering to check the airway for the object prior to giving breaths. Once the airway is clear, assess for breathing. If breathing is present, roll infant into their side and monitor until help arrives. If infant is not breathing, continue the steps of CPR giving 30 compressions and 2 breaths, alternating, until help arrives.
23 If small, round objects do not become airway obstructions, they usually pass uneventfully through the child. Sharp or straight objects are dangerous if swallowed. Arrange for prompt transport.
24
25 Causes of altered mental status in children Low blood glucose level Poisoning Post-seizure state Infection Head trauma Decreased oxygen levels
26 Because infants breathe primarily through their noses, even a minor cold can cause breathing difficulties. Asthma Caused by a spasm or constriction and inflammation of smaller airways in the lungs Usually produces a wheezing sound Advise caller to get child into a position of comfort and follow their doctor s order for medication Arrange for prompt transport
27 Croup Infection of the upper airway that occurs mainly in children between 6 months and 6 years of age Results in a hoarse, whooping noise during inhalation and a seal-like, barking cough Often occurs in colder climate A lack of fright and the willingness to lie down are important signs that distinguish croup from epiglottitis. Moist, warm air helps to relax the vocal cords.
28 Epiglottitis Severe inflammation of the epiglottis The flap is so inflamed and swollen that air movement into the trachea is completely blocked. Usually occurs in children between ages 3 and 6 years The child is usually sitting upright, with chin thrust forward cannot swallow or cough. is drooling. is anxious and frightened. Make the child comfortable with as little handling as possible. Keep everyone calm.
29 Signs of respiratory distress A breathing rate of more than 60 breaths/min in infants A breathing rate of more than 30 to 40 breaths/min in children Nasal flaring on each breath Retraction of the skin between the ribs and around the neck muscles Stridor a high pitched crowing, upper airway sound, indicating swelling or a partial obstruction Cyanosis of the skin Altered mental status Combativeness or restlessness
30 Treatment of respiratory distress Try to determine the cause. Support the child s respirations by placing the child in a comfortable position, usually sitting. Keep the child as calm as possible by letting a parent hold the child if practical. Arrange for prompt transport.
31 Often results as respiratory distress proceeds Signs and symptoms A breathing rate of fewer than 20 breaths/min in an infant A breathing rate of fewer than 10 breaths/min in a child Limp muscle tone Unresponsiveness Decreased or absent heart rate A child in respiratory failure is on the verge of experiencing respiratory and cardiac arrest.
32 Circulatory failure The most common cause of circulatory failure in children is respiratory failure. Can lead to cardiac arrest Indicated by an increased heart rate, pale or bluish skin, and changes in mental status
33 Fevers are common in children. Because the temperature-regulating mechanism in young children has not fully developed, a very high temperature can occur quickly. Most children can tolerate temperatures as high as 104 F (40 C). Treatment Uncover the child so that body heat can escape. Protect the child during any seizure, and make certain that normal breathing resumes after each seizure.
34 Can result from a high fever or from disorders such as epilepsy. Seizures are relatively common in children who have sustained a serious head injury. During a seizure: The child loses consciousness. The eyes roll back. The teeth become clenched. The body shakes with jerking movements. The child s skin becomes pale or turns blue. Sometimes the child loses bladder and bowel control.
35 Treatment Move objects away to prevent injury. Maintain an adequate airway after the seizure ends. Arrange for prompt transport. Monitor and support the ABCs. After the seizure is over, cool the patient if he or she has a high fever.
36 Usually caused by gastrointestinal infections May produce severe dehydration The dehydrated child is lethargic and has very dry skin. Can lead to shock. Hospitalization may be required to replace fluids. If you suspect dehydration, arrange for transport.
37 One of the most serious causes of abdominal pain in children is appendicitis. More commonly seen in people between 10 and 25 years Usually the child is nauseated, has no appetite, and occasionally will vomit. Treat every child with a sore or tender abdomen as an emergency. Arrange for prompt transport.
38 Also called crib death Sudden and unexpected death of an apparently healthy infant Usually occurs in infants between the ages of 3 weeks and 7 months No adequate scientific explanation exists for SIDS. Be compassionate with the parents.
39 Trauma is the number one killer of children. Treat an injured child as you would treat an injured adult, but remember these differences: A child cannot communicate symptoms as well as an adult. You may need to adapt materials and equipment to the child s size. A child does not show signs of shock as early as an adult but can progress into severe shock quickly.
40 The patterns of injury sustained by children will be related to three factors: Type of trauma they experience Type of activity causing the injury Child s anatomy Motor vehicle crashes Unrestrained patients have more head and neck injuries. Restrained patients often suffer head, spinal, and abdominal injuries. Bicycle accidents Children often suffer head, spinal, abdominal, and extremity injuries. The use of bicycle helmets can greatly reduce the number and severity of head injuries.
41 Children hit by cars often sustain chest, abdominal, thigh, and extremity injuries. Falls from a height or diving accidents cause head, spinal, and extremity injuries. Burns are a major cause of injuries to children.
42 Treatment regardless of the cause of injury Do not move patient, unless in immediate danger. Check the patient s ABCs. Stop severe bleeding. Treat the patient for shock. Children show shock symptoms much more slowly than adults do, but they progress through the stages of shock quickly. Stabilize all injuries you find.
43 A child s injuries could be a result of abuse. If you suspect abuse, ensure the child s safety. Signs and symptoms Multiple fractures Bruises in various stages of healing Human bites Burns Reports of bizarre accidents Signs and symptoms of neglect Lack of adult supervision Malnourished-appearing child Unsafe living environment Untreated chronic illness In addition to experiencing abuse the child could be a victim of sexual assault.
44 Calls involving children tend to produce strong emotional reactions. You may need to talk about feelings of anger or frustration with a counselor. By attending debriefing sessions, you can: Express your feelings Learn some coping strategies Maintain a healthy approach to future calls CISD, WCSP SOCIAL WORKER , JPD SOCIAL WORKER
45 Emergency Medical Responder, 5 th edition Will County EMDPRS, June 2012 American Heart Association, 2010 guidelines American Academy of Pediatrics PEPP, 2000 Google Images
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway management. Dr. Dóra Ujvárosy Medical Unversity of Debrecen Emergency Department
 Airway management Dr. Dóra Ujvárosy Medical Unversity of Debrecen Emergency Department Airway management Airway management is the medical process of ensuring there is an open pathway between a patient
Airway management Dr. Dóra Ujvárosy Medical Unversity of Debrecen Emergency Department Airway management Airway management is the medical process of ensuring there is an open pathway between a patient
Airway and Breathing
 Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
BASIC LIFE SUPPORT (BLS)
 ADULT Suspected Foreign Body Airway Obstruction (FBAO) 1 If conscious, ask, "Are you choking?" 2 If patient is unable to speak and/or shakes head yes, give abdominal thrusts, (chest thrusts if pregnant
ADULT Suspected Foreign Body Airway Obstruction (FBAO) 1 If conscious, ask, "Are you choking?" 2 If patient is unable to speak and/or shakes head yes, give abdominal thrusts, (chest thrusts if pregnant
PEDIATRIC EMERGENCIES Sandra Horning, MD Sacred Heart Medical Center Emergency Department
 PEDIATRIC EMERGENCIES Sandra Horning, MD Sacred Heart Medical Center Emergency Department Overview Roles of the EMS in Pediatric Care Growth and Development Assessment Airway Adjuncts and Intravenous Access
PEDIATRIC EMERGENCIES Sandra Horning, MD Sacred Heart Medical Center Emergency Department Overview Roles of the EMS in Pediatric Care Growth and Development Assessment Airway Adjuncts and Intravenous Access
Bayfield-Ashland Counties EMS Council Pediatric Protocol PP-001 PREHOSPITAL CARE GUIDELINE
 INTRODUCTION: Pediatric emergencies may present a daunting challenge to prehospital care providers for a variety of reasons including: 1. The historical scarceness of primary training materials about the
INTRODUCTION: Pediatric emergencies may present a daunting challenge to prehospital care providers for a variety of reasons including: 1. The historical scarceness of primary training materials about the
Pediatric Patients. BCFPD Paramedic Education Program. EMS Education Paramedic Level
 Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Review. 1. How does a child s anatomy differ from an adult s anatomy?
 Chapter 32 Review Review 1. How does a child s anatomy differ from an adult s anatomy? A. The child s trachea is more rigid B. The tongue is proportionately smaller C. The epiglottis is less floppy in
Chapter 32 Review Review 1. How does a child s anatomy differ from an adult s anatomy? A. The child s trachea is more rigid B. The tongue is proportionately smaller C. The epiglottis is less floppy in
Topics. Seattle/King County EMT-B Class. Pediatric Emergencies: Chapter 31. Pediatric Assessment: Chapter Pediatric SICK/NOT SICK
 Seattle/King County EMT-B Class Topics Pediatric Emergencies: Chapter 3 Pediatric Assessment: Chapter 3 3 Pediatric SICK/NOT SICK Pediatric Emergencies Airway Differences Larger tongue relative to the
Seattle/King County EMT-B Class Topics Pediatric Emergencies: Chapter 3 Pediatric Assessment: Chapter 3 3 Pediatric SICK/NOT SICK Pediatric Emergencies Airway Differences Larger tongue relative to the
BLS Guideline 1 AIRWAY MANAGEMENT
 Australian Resuscitation Advisory Network BLS Guideline 1 AIRWAY MANAGEMENT Scope Who does this guideline apply to? This guideline applies to all persons who need airway management. Airway management is
Australian Resuscitation Advisory Network BLS Guideline 1 AIRWAY MANAGEMENT Scope Who does this guideline apply to? This guideline applies to all persons who need airway management. Airway management is
Pediatric Emergencies. Lesson Goal. Lesson Objectives 9/10/2012
 Pediatric Emergencies Lesson Goal Explain special characteristics of infants and children to become both comfortable & efficient in treating pediatric emergencies Lesson Objectives Identify physical &
Pediatric Emergencies Lesson Goal Explain special characteristics of infants and children to become both comfortable & efficient in treating pediatric emergencies Lesson Objectives Identify physical &
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006 SUBJECT: MANAGEMENT OF FOREIGN-BODY AIRWAY OBSTRUCTION (CHOKING VICTIM)
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 701 Effective Date: August 31, 2006 SUBJECT: MANAGEMENT OF FOREIGN-BODY AIRWAY OBSTRUCTION (CHOKING
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 701 Effective Date: August 31, 2006 SUBJECT: MANAGEMENT OF FOREIGN-BODY AIRWAY OBSTRUCTION (CHOKING
Homework Assignment Complete and Place in Binder
 Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Cardio Pulmonary Resuscitation
 Cardio Pulmonary Resuscitation The following lesson in Cardiopulmonary Resuscitation is intended solely as a review. We urge, encourage and require all foster families to take a formal class that meets
Cardio Pulmonary Resuscitation The following lesson in Cardiopulmonary Resuscitation is intended solely as a review. We urge, encourage and require all foster families to take a formal class that meets
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
Shelley Westwood, RN, BSN
 Shelley Westwood, RN, BSN The body requires a constant supply of oxygen for survival. AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross
Shelley Westwood, RN, BSN The body requires a constant supply of oxygen for survival. AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross
Acting in an emergency. Dr. Samer Sara
 Acting in an emergency Dr. Samer Sara 1 Acting in an emergency basic steps to follow: 1. Recognize the emergency. 2. Check the scene. 3. Call 110. 4. Check the victim. 5. Give first aid. 2 Dr. Samer Sara
Acting in an emergency Dr. Samer Sara 1 Acting in an emergency basic steps to follow: 1. Recognize the emergency. 2. Check the scene. 3. Call 110. 4. Check the victim. 5. Give first aid. 2 Dr. Samer Sara
Firefighter Pre-Hospital Care Program Recruit Presentation. Respiratory Emergencies
 Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Managing Illness 8/9/2010 1
 Managing Illness 1 Fainting Caused by a temporary drop in blood pressure thus causing a reduction in oxygen to the brain. Insufficient oxygen causes casualty to black out and fall. Consciousness normally
Managing Illness 1 Fainting Caused by a temporary drop in blood pressure thus causing a reduction in oxygen to the brain. Insufficient oxygen causes casualty to black out and fall. Consciousness normally
BLS Guideline 1 AIRWAY MANAGEMENT
 Australian Resuscitation Advisory Network BLS Guideline 1 AIRWAY MANAGEMENT Scope Who does this guideline apply to? This guideline applies to all persons who need airway management. Airway management is
Australian Resuscitation Advisory Network BLS Guideline 1 AIRWAY MANAGEMENT Scope Who does this guideline apply to? This guideline applies to all persons who need airway management. Airway management is
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Pediatric Patient Overview
 Emergency Medical Services Seattle/King County Public Health 401 5th Avenue, Suite 1200 Seattle, WA 98104 206.296.4863 Last Updated December 14, 2015 Pediatric Patient Overview Contents PEDIATRIC BASICS...
Emergency Medical Services Seattle/King County Public Health 401 5th Avenue, Suite 1200 Seattle, WA 98104 206.296.4863 Last Updated December 14, 2015 Pediatric Patient Overview Contents PEDIATRIC BASICS...
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Airway Management From Brady s First Responder (8th Edition) 82 Questions
 Airway Management From Brady s First Responder (8th Edition) 82 Questions 1. What color will cyanotic skin be? p. 119 *A.) Blue B.) Red C.) Yellow D.) Green 2. Which is the primary path for air to enter
Airway Management From Brady s First Responder (8th Edition) 82 Questions 1. What color will cyanotic skin be? p. 119 *A.) Blue B.) Red C.) Yellow D.) Green 2. Which is the primary path for air to enter
McHenry Western Lake County EMS System Optional CE for Paramedics, EMT-B and PHRN s Croup vs. Epiglottitis. Optional #2 2017
 McHenry Western Lake County EMS System Optional CE for Paramedics, EMT-B and PHRN s Croup vs. Epiglottitis Optional #2 2017 The tones go out at 3 am for a child with difficulty breathing. As it is a kid
McHenry Western Lake County EMS System Optional CE for Paramedics, EMT-B and PHRN s Croup vs. Epiglottitis Optional #2 2017 The tones go out at 3 am for a child with difficulty breathing. As it is a kid
VAO BASIC SUPPORT CLINICAL APPROACH TO THE PATIENT HANDOUT
 CLINICAL APPROACH TO THE PATIENT HANDOUT 1 I am the most important part of patient care. How can you expect to treat a patient appropriately if you don t follow through on basic primary care? Remember:
CLINICAL APPROACH TO THE PATIENT HANDOUT 1 I am the most important part of patient care. How can you expect to treat a patient appropriately if you don t follow through on basic primary care? Remember:
CRITERIA BASED DISPATCH (CBD)
 CRITERIA BASED DISPATCH (CBD) Key Concepts of CBD Critical/Non-Critical Criteria Based Dispatch (also referred to as CBD) is centered on two dimensions that characterize all pre-hospital emergency response.
CRITERIA BASED DISPATCH (CBD) Key Concepts of CBD Critical/Non-Critical Criteria Based Dispatch (also referred to as CBD) is centered on two dimensions that characterize all pre-hospital emergency response.
CPR & First Aid Resources
 CPR & First Aid Resources A resource guide to assist the Trainer in locating CPR/FA classes in Clare, Isabella, Mecosta, Osceola, Gladwin, and Midland Counties. This guide also contains: CPR Chart, Heart
CPR & First Aid Resources A resource guide to assist the Trainer in locating CPR/FA classes in Clare, Isabella, Mecosta, Osceola, Gladwin, and Midland Counties. This guide also contains: CPR Chart, Heart
QI. Read the following questions and choose the most correct answer (20 Marks):
 Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions
 Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Pediatric Advanced Life Support
 Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Principles of First Aid and Medical Emergencies
 Rationale Principles of First Aid and Medical Emergencies Many emergency situations involve medical episodes instead of injury situations. Healthcare workers must prepare themselves to respond to all types
Rationale Principles of First Aid and Medical Emergencies Many emergency situations involve medical episodes instead of injury situations. Healthcare workers must prepare themselves to respond to all types
Module Summaries: The emergency plan is a crucial part of the total sports program.
 Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Pediatric Emergencies. September, 2018
 Pediatric Emergencies September, 2018 Introduction Children s bodies respond to significant injury and shock differently than adults. These differences may be subtle and difficult to recognize EMS providers
Pediatric Emergencies September, 2018 Introduction Children s bodies respond to significant injury and shock differently than adults. These differences may be subtle and difficult to recognize EMS providers
Asthma. If an Ambulance is required - call immediately - do not delay. H & A Training PL RTO No:90871
 Asthma is a reversible breathing problem caused from sudden or progressive narrowing and spasming of the smaller airways and includes mucus production, which interferes with oxygen exchange. People who
Asthma is a reversible breathing problem caused from sudden or progressive narrowing and spasming of the smaller airways and includes mucus production, which interferes with oxygen exchange. People who
Topic: Baseline Vitals and Sample History Company Drill
 Baseline Vitals and Sample History Company Drill Instructor Guide Session Reference: 1 Topic: Baseline Vitals and Sample History Company Drill Level of Instruction: 2 Time Required: Three Hours Materials
Baseline Vitals and Sample History Company Drill Instructor Guide Session Reference: 1 Topic: Baseline Vitals and Sample History Company Drill Level of Instruction: 2 Time Required: Three Hours Materials
CETEP PRE-TEST For questions 1 through 3, consider the following scenario:
 CETEP PRE-TEST For questions 1 through 3, consider the following scenario: A two and half month infant comes to the health centre looking very lethargic. Her mother reports that the infant has felt very
CETEP PRE-TEST For questions 1 through 3, consider the following scenario: A two and half month infant comes to the health centre looking very lethargic. Her mother reports that the infant has felt very
Pediatric Assessment Triangle
 Pediatric Assessment Triangle Katherine Remick, MD, FAAP Associate Medical Director Austin Travis County EMS Pediatric Emergency Medicine Dell Children s Medical Center Objectives 1. Discuss why the Pediatric
Pediatric Assessment Triangle Katherine Remick, MD, FAAP Associate Medical Director Austin Travis County EMS Pediatric Emergency Medicine Dell Children s Medical Center Objectives 1. Discuss why the Pediatric
Infants and Children From Bradys Emergency Care 10 th Edition. 2. Why should moist dressings be used sparingly in a pediatric burn patient?
 Infants and Children From Bradys Emergency Care 10 th Edition 1. Which is the most frequent sign of head injury in a child? A.) Nausea B.) Vomiting C.) Altered mental status D.) Shock 2. Why should moist
Infants and Children From Bradys Emergency Care 10 th Edition 1. Which is the most frequent sign of head injury in a child? A.) Nausea B.) Vomiting C.) Altered mental status D.) Shock 2. Why should moist
FIRST AID WRITTEN EXAM. Team Name: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. a. TRUE b. FALSE
 2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
Module 2: Facilitator instructions for Airway & Breathing Skills Station
 Module 2: Facilitator instructions for Airway & Breathing Skills Station 1. Preparation a. Assemble equipment beforehand. b. Make sure that you have what you need and that it is functioning properly. 2.
Module 2: Facilitator instructions for Airway & Breathing Skills Station 1. Preparation a. Assemble equipment beforehand. b. Make sure that you have what you need and that it is functioning properly. 2.
BEHAVIORAL EMERGENCIES
 LESSON 21 BEHAVIORAL EMERGENCIES 21-1 Behavioral Emergencies Process of giving first aid may be complicated by victim s behavior Many injuries or illnesses can cause altered mental status or emotional
LESSON 21 BEHAVIORAL EMERGENCIES 21-1 Behavioral Emergencies Process of giving first aid may be complicated by victim s behavior Many injuries or illnesses can cause altered mental status or emotional
BLS ROUTINE MEDICAL CARE
 BLS ROUTINE MEDICAL CARE Scene safety # Assure scene safety prior to patient contact C-spine # Perform manual cervical spine stabilization if indicated (Follow the cervical spine protocol.) ABCs # Assess
BLS ROUTINE MEDICAL CARE Scene safety # Assure scene safety prior to patient contact C-spine # Perform manual cervical spine stabilization if indicated (Follow the cervical spine protocol.) ABCs # Assess
Skill Evaluation Sheets
 Skill Evaluation Sheets Skill Drill 2-: How to Remove Gloves Skill Drill 4-: Primary Check: RAP-CAB Skill Drill 4-2: Perform a Secondary Check Skill Drill 5-: Adult CPR Skill Drill 5-2: Child CPR Skill
Skill Evaluation Sheets Skill Drill 2-: How to Remove Gloves Skill Drill 4-: Primary Check: RAP-CAB Skill Drill 4-2: Perform a Secondary Check Skill Drill 5-: Adult CPR Skill Drill 5-2: Child CPR Skill
The Pediatric Patient. Morgen Bernius, MD NCEMS Conference February 24, 2007
 The Pediatric Patient Morgen Bernius, MD NCEMS Conference February 24, 2007 Rule #1: Everyone Loves the Pediatric Patient Pediatrics in EMS Approximately 10% of all EMS treatment is for children younger
The Pediatric Patient Morgen Bernius, MD NCEMS Conference February 24, 2007 Rule #1: Everyone Loves the Pediatric Patient Pediatrics in EMS Approximately 10% of all EMS treatment is for children younger
Cardiac arrest Cardiac arrest (CA) occurs when the heart ceases to produce an effective pulse and circulate blood It includes four conditions:
 Basic Life Support: Cardiopulmonary Resuscitation (CPR). 2017 Lecture prepared by, Amer A. Hasanien RN, CNS, PhD Cardiac arrest Cardiac arrest (CA) occurs when the heart ceases to produce an effective
Basic Life Support: Cardiopulmonary Resuscitation (CPR). 2017 Lecture prepared by, Amer A. Hasanien RN, CNS, PhD Cardiac arrest Cardiac arrest (CA) occurs when the heart ceases to produce an effective
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Emergency Department Triage
 Emergency Department Triage Julia Fuzak, MD, Patrick Mahar, MD The Children s Hosital Denver, CO, USA 1/30/09 Hospital Pediatrico Juan Manuel Marquez Habana, Cuba Objectives What is does triage mean? Why
Emergency Department Triage Julia Fuzak, MD, Patrick Mahar, MD The Children s Hosital Denver, CO, USA 1/30/09 Hospital Pediatrico Juan Manuel Marquez Habana, Cuba Objectives What is does triage mean? Why
Respiratory Management in Pediatrics
 Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Medical & Safety. Stay safe at Kamp Dovetail 2011
 Medical & Safety Stay safe at Kamp Dovetail 2011 Seizures Seizures are very misunderstood and may be caused by many different types of conditions, such as: Insulin shock High fevers Viral infections of
Medical & Safety Stay safe at Kamp Dovetail 2011 Seizures Seizures are very misunderstood and may be caused by many different types of conditions, such as: Insulin shock High fevers Viral infections of
Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1
 Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1 For questions 1 through 3, consider the following scenario: A three year old comes with burns to her face and chest after a kerosene
Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1 For questions 1 through 3, consider the following scenario: A three year old comes with burns to her face and chest after a kerosene
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: Pediatric Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: Pediatric Revised: 11/2013 (10 questions from this outline in the blue section) Emergency Medical
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: Pediatric Revised: 11/2013 (10 questions from this outline in the blue section) Emergency Medical
The assessment helps decide if the patient is an emergency, priority or non-urgent case.
 Emergency Triage Assessment and Treatment The World Health Organisation (WHO) has produced some useful guidelines about how to improve the care of our patients and their survival in hospital. This is a
Emergency Triage Assessment and Treatment The World Health Organisation (WHO) has produced some useful guidelines about how to improve the care of our patients and their survival in hospital. This is a
RIB FRACTURE. Explanation. Causes. Symptoms. Diagnosis
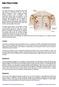 RIB FRACTURE Explanation The heart and lungs are encased by the chest wall, which is composed of the ribs. The ribs must be flexible in order to allow movement during expansion and contraction. This movement
RIB FRACTURE Explanation The heart and lungs are encased by the chest wall, which is composed of the ribs. The ribs must be flexible in order to allow movement during expansion and contraction. This movement
Pediatric Assessment Lesson 3
 1 Pediatric Assessment Lesson 3 2 Pediatric Assessment Initial assessment methods used for adults are modified for children due to developmental and physiological considerations. 3 In this lesson, the
1 Pediatric Assessment Lesson 3 2 Pediatric Assessment Initial assessment methods used for adults are modified for children due to developmental and physiological considerations. 3 In this lesson, the
CENTRAL CARE POLICY SYMPTOMS OF ILLNESS. Policy: Consumers will be observed for symptoms of physical problems, distress, pain, or unusual behaviors.
 Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Overview. The Respiratory System. Chapter 18. Respiratory Emergencies 9/11/2012
 Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
First aid for seizures
 First aid for seizures What is epilepsy? Epilepsy is a tendency to have repeated seizures that begin in the brain. For most people with epilepsy their seizures will be controlled by medication. Around
First aid for seizures What is epilepsy? Epilepsy is a tendency to have repeated seizures that begin in the brain. For most people with epilepsy their seizures will be controlled by medication. Around
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Appendix (i) The ABCDE approach to the sick patient
 Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Signs and Symptoms Of Common Health Concerns
 Signs and Symptoms Of Common Health Concerns New York Statewide School Health Services Center www.schoolhealthservicesny.com Phone: 585.617-2384 Fax: 585.352.9131 The pages in this chart list common symptoms
Signs and Symptoms Of Common Health Concerns New York Statewide School Health Services Center www.schoolhealthservicesny.com Phone: 585.617-2384 Fax: 585.352.9131 The pages in this chart list common symptoms
Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION
 Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION Major Concepts. Proper planning of an emergency response is essential for appropriate first aid management of an injury. Anything that can be done
Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION Major Concepts. Proper planning of an emergency response is essential for appropriate first aid management of an injury. Anything that can be done
CBT/OTEP 537 Pediatric Emergencies
 Seattle-King County EMS Emergency Medical Services Division Public Health - Seattle/King County 999 3 rd Avenue, Suite 700 Seattle, Washington 98104 (206) 296-4863 January 2007 (rev 1/8/2008) CBT/OTEP
Seattle-King County EMS Emergency Medical Services Division Public Health - Seattle/King County 999 3 rd Avenue, Suite 700 Seattle, Washington 98104 (206) 296-4863 January 2007 (rev 1/8/2008) CBT/OTEP
Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2
 Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
WHY IS FIRST AID IMPORTANT?
 Chapter 1 -BACKGROUND INFORMATION WHY IS FIRST AID IMPORTANT? 1. 2. SOME THINGS I SHOULD HAVE IN MY FIRST AID KIT 1. 2. 3. 4. 5. VOCABULARY Place the key points of the first aid term in the box provided
Chapter 1 -BACKGROUND INFORMATION WHY IS FIRST AID IMPORTANT? 1. 2. SOME THINGS I SHOULD HAVE IN MY FIRST AID KIT 1. 2. 3. 4. 5. VOCABULARY Place the key points of the first aid term in the box provided
Emergency Medical Technician Common Course Outline
 Emergency Medical Technician Common Course Outline Course Information Organization South Central College Revision History 2008-2009 Course Number HEMS1200 Department EMS Total Credits 6 Description This
Emergency Medical Technician Common Course Outline Course Information Organization South Central College Revision History 2008-2009 Course Number HEMS1200 Department EMS Total Credits 6 Description This
First Aid Preparedness. Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division
 First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division Epilepsy Basics Seizures are a bit like an electrical brainstorm. The chaos that occurs in the brain during a seizure
First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division Epilepsy Basics Seizures are a bit like an electrical brainstorm. The chaos that occurs in the brain during a seizure
Opiate Overdose Treatment: Naloxone Training Protocol
 OREGON STATE PUBLIC HEALTH DIVISION EMS & Trauma Systems Kate Brown, Governor September 22, 2016 For more information, contact David Lehrfeld, MD, Medical Director, EMS & Trauma Systems: (971) 673-0520
OREGON STATE PUBLIC HEALTH DIVISION EMS & Trauma Systems Kate Brown, Governor September 22, 2016 For more information, contact David Lehrfeld, MD, Medical Director, EMS & Trauma Systems: (971) 673-0520
Quick review of Assessment. Pediatric Medical Assessment Review And Case Studies. Past Medical History. S.A.M.P.L.E. History is a great start.
 EMS Live at Night January 12 th, 2010 Pediatric Medical Assessment Review And Case Studies Brian Rogge RN Northwest Medstar Pediatric/Perinatal Team Quick review of Assessment S.A.M.P.L.E. History is a
EMS Live at Night January 12 th, 2010 Pediatric Medical Assessment Review And Case Studies Brian Rogge RN Northwest Medstar Pediatric/Perinatal Team Quick review of Assessment S.A.M.P.L.E. History is a
CHAPTER 9. Shock National Safety Council
 CHAPTER 9 Shock Shock Dangerous condition: Not enough oxygen-rich blood reaching vital organs, such as brain and heart Caused by anything that significantly reduces blood flow Life-threatening emergency
CHAPTER 9 Shock Shock Dangerous condition: Not enough oxygen-rich blood reaching vital organs, such as brain and heart Caused by anything that significantly reduces blood flow Life-threatening emergency
EMT. Chapter 8 Review
 EMT Chapter 8 Review 1. During the scene size-up, you should routinely determine all of the following, EXCEPT: A. the mechanism of injury or nature of illness. B. the ratio of pediatric patients to adult
EMT Chapter 8 Review 1. During the scene size-up, you should routinely determine all of the following, EXCEPT: A. the mechanism of injury or nature of illness. B. the ratio of pediatric patients to adult
Chapter 11 - The Primary Assessment
 Introduction to Emergency Medical Care 1 OBJECTIVES 11.1 Define key terms introduced in this chapter. Slides 11 12, 14, 19 21, 28 11.2 Explain the purpose of the primary assessment. Slides 11 13 OBJECTIVES
Introduction to Emergency Medical Care 1 OBJECTIVES 11.1 Define key terms introduced in this chapter. Slides 11 12, 14, 19 21, 28 11.2 Explain the purpose of the primary assessment. Slides 11 13 OBJECTIVES
Key Words. clammy closed fracture dislocation fainting ligament open fracture splint sprain strain trauma. Linked Core Abilities
 Lesson 4 Treating for Shock and Immobilizing Fractures Key Words clammy closed fracture dislocation fainting ligament open fracture splint sprain strain trauma What You Will Learn to Do Determine first
Lesson 4 Treating for Shock and Immobilizing Fractures Key Words clammy closed fracture dislocation fainting ligament open fracture splint sprain strain trauma What You Will Learn to Do Determine first
Asthma With a Slight Chance of Anaphylaxis
 Asthma With a Slight Chance of Anaphylaxis An Update for Alberta Oral Health Professionals Sept 25/13 Presented by Val Olson CRE Community Pediatric Asthma Service Air passes through the: Nose or mouth
Asthma With a Slight Chance of Anaphylaxis An Update for Alberta Oral Health Professionals Sept 25/13 Presented by Val Olson CRE Community Pediatric Asthma Service Air passes through the: Nose or mouth
EMT OPTIONAL SKILL. Cell Phones and Pagers. Epinephrine Auto-injector. Course Outline 9/2017
 EMT OPTIONAL SKILL Epinephrine Auto-injector Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and
EMT OPTIONAL SKILL Epinephrine Auto-injector Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and
Restore adequate respiratory and circulatory conditions. Reduce pain
 Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Chapter 11. Learning Objectives. Learning Objectives 9/18/2012. Respiratory Emergencies
 Chapter 11 Respiratory Learning Objectives List structures & functions of the respiratory system State signs/symptoms of patient with breathing difficulty Describe emergency medical care of patient with
Chapter 11 Respiratory Learning Objectives List structures & functions of the respiratory system State signs/symptoms of patient with breathing difficulty Describe emergency medical care of patient with
Chapter 38. Objectives. Objectives 01/09/2013. Pediatrics
 Chapter 38 Pediatrics Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced
Chapter 38 Pediatrics Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced
APPLY FIRST AID ONLINE WORKBOOK
 APPLY FIRST AID ONLINE WORKBOOK STUDENT NAME: ADDRESS: PHONE CONTACT: DATE OF COURSE: Welcome to CYNERGEX GROUP pre-learning package for the APPLY FIRST AID course. This workbook is to be completed in
APPLY FIRST AID ONLINE WORKBOOK STUDENT NAME: ADDRESS: PHONE CONTACT: DATE OF COURSE: Welcome to CYNERGEX GROUP pre-learning package for the APPLY FIRST AID course. This workbook is to be completed in
Medical First Responder Program Protocols
 Medical Scene Safety Protocol Verify Scene Safety with Police or Dispatch UNKWN Scene Safe? Enter Continue to Appropriate Protocol Possible to Make Safe Make Safe Then Continue Exit Area and Stage Outside
Medical Scene Safety Protocol Verify Scene Safety with Police or Dispatch UNKWN Scene Safe? Enter Continue to Appropriate Protocol Possible to Make Safe Make Safe Then Continue Exit Area and Stage Outside
Hockey New South Wales Head Injury Guidelines Effective November
 Hockey New South Wales Effective November 2011 1 Table of Contents Part 1: Guidelines Statement 3 Head Injuries 3 Two Types of Head Injuries 3 Symptoms of Head Injuries 3 Head Injury Notifications 3 Important
Hockey New South Wales Effective November 2011 1 Table of Contents Part 1: Guidelines Statement 3 Head Injuries 3 Two Types of Head Injuries 3 Symptoms of Head Injuries 3 Head Injury Notifications 3 Important
Basic First Aid. Sue Fisher Emergency Management Coordinator CSUF University Police
 Basic First Aid Sue Fisher Emergency Management Coordinator CSUF University Police Information given for this lecture is not meant to replace any official training by the American Red Cross, or any other
Basic First Aid Sue Fisher Emergency Management Coordinator CSUF University Police Information given for this lecture is not meant to replace any official training by the American Red Cross, or any other
Core Subject Part 4. Identify the principles of approaching the sick patient.
 The Role of The Dental Care Professional During a Medical Emergency: General Dental Council Standards and The Management of The Collapsed Patient Using the ABCDE Approach Aims: Core Subject Part 4 To provide
The Role of The Dental Care Professional During a Medical Emergency: General Dental Council Standards and The Management of The Collapsed Patient Using the ABCDE Approach Aims: Core Subject Part 4 To provide
Pediatric Assessment Objectives
 Pediatric Assessment Objectives Distinguish the 3 components of the PAT. Assess pediatric-specific features of initial assessment. Integrate findings to form a general impression. Describe the focused
Pediatric Assessment Objectives Distinguish the 3 components of the PAT. Assess pediatric-specific features of initial assessment. Integrate findings to form a general impression. Describe the focused
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Laryngoscopy Examinations
 Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
How to Perform CPR on a Cardiac Arrest Victim (Adult Victim Only)
 1 How to Perform CPR on a Cardiac Arrest Victim (Adult Victim Only) A cardiac arrest occurs when the heart stops pumping blood throughout the human body, either because it stopped beating or it is beating
1 How to Perform CPR on a Cardiac Arrest Victim (Adult Victim Only) A cardiac arrest occurs when the heart stops pumping blood throughout the human body, either because it stopped beating or it is beating
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
REGION 1 EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic, EMT Intermediate, EMT Paramedic. SMO: Pediatric Assessment Guidelines
 REGION 1 EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic, EMT Intermediate, EMT Paramedic SMO: Pediatric Assessment Guidelines Overview: Pediatric patients account for about 10% or less of
REGION 1 EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic, EMT Intermediate, EMT Paramedic SMO: Pediatric Assessment Guidelines Overview: Pediatric patients account for about 10% or less of
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Abdominal/Back/Groin Pain. Vital Points. Dispatch Criteria. Pre-arrival Instructions
 1M1 Unconscious or not breathing 1M2 Signs of shock (three required): Diaphoresis Pale, clammy skin Nausea 1M3 Vomiting red blood, with three signs of shock 1M4 Black tarry stool with three signs of shock
1M1 Unconscious or not breathing 1M2 Signs of shock (three required): Diaphoresis Pale, clammy skin Nausea 1M3 Vomiting red blood, with three signs of shock 1M4 Black tarry stool with three signs of shock
