Slide 1. Slide 2 OBJECTIVES. Slide 3. Lymphedema & Chronic Edema: Management Strategies for Nursing to Promote Wound Healing.
|
|
|
- August McKinney
- 6 years ago
- Views:
Transcription
1 Slide 1 Lymphedema & Chronic Edema: Management Strategies for Nursing to Promote Wound Healing Nancy Fellows, PT, CLT-LANA nancy.fellows@unitypoint.org John Stoddard Cancer Center Slide 2 OBJECTIVES Understand basic anatomy and physiology of the lymphatic system. Understand basic pathophysiology relating to common swelling pathologies: Differentiate lymphedema from other edema related conditions. Identify treatment precautions/contraindications based on medical diagnosis for edema management. Identify common edema management strategies and limitations. Identify goals for wound healing by applying lymphedema compression principles. Identify the differences and applications for use of long and short stretch compression bandages. Understand factors that influence optimal compression management selection. Slide 3 Relevance The #1 cause of lymphedema world wide is due to chronic venous insufficiency (CVI) resulting in an estimated incidence of 300 million. Chronic wounds >3 million/year in US Any condition/treatment that disrupts or destroys lymph node and lymph channel drainage and function can predispose the occurrence of lymphedema.
2 Slide 4 Definitions - Swelling Edema Observable fluid accumulation Generalized or localized Pitting or Non-pitting Increased interstitial fluid outside the cells & blood vessels Lymphatics always involved Symptom of a disease process Lymphedema Protein rich fluid in tissues Insufficiency or damage to lymphatic system or chronic overload-lymphedema dependency A clinical diagnosis Slide 5. Slide 6 Lymphatic System Veins Lymphatic capillaries Lymph Vessels Interstitial Tissue Lymph nodes & organs Arteries Heart Venous angle Lymphatic Trunks/ducts
3 Slide 7 Microcirculation Normal circulation at the capillary level is a balance of fluids transported by the arterioles & reabsorbed by the venules & initial lymphatics. Slide 8 Microcirculation The lymphatic system functions as a one-way transport system of lymph fluid from the interstitial tissue back to the venous blood circulation where it originated. Slide 9 Lymph Capillary and Blood Capillary Loop. 1. Arterial side of blood capillary 2. Venous side of blood capillary 3. Lymph capillary 4. Open junction swinging flap 5. Fibrocyte 6. Anchoring filaments 7. Interstitial space
4 Slide 10 Lymphatic Fluid Protein Molecules Water Cellular Components WBCs, CA cells, bacterial/viral cells and debris from proteolysis/phagocytosis Fatty Acids Slide 11 Reabsorption 90% by the venule 10% by the lymphatic vessels Transport of the lymphatic load depends on tissue pressure, blood capillary pressure and colloid osmotic pressure. Slide 12 LYMPHATIC ULTRAFILTRATION AND REABSORPTION
5 Slide 13 Interstitial Fluid Balance between hydrostatic and oncotic pressures in blood capillaries and interstitial space. Lymphatic system protein and fluid exchange Diffusion- passive from high to low concentrations Transport Capacity Slide 14 Transport Capacity The lymphatic system can transport 10 times its normal daily load L per day This allows the body a safety reserve Slide 15 Drainage Possibilities of Lymph Territories (A) 1. Lymphatic skin area 2. Pre-collector 3. Subcutaneous Collector (B) 3. Subcutaneous collector 4. Lymphatic skin zone
6 Slide 16 Lymphatic Transport Superficial: - passive - initial lymphatics - pre-collectors Dermal: - collectors - valves Subfascial: - valves - active transport - lymph angion Slide 17 Lymphatic Network Slide 18 Lymph Angion Stimulation Pressure of interstitial fluid Pulsation of arteries Skeletal muscle contraction Deep breathing
7 Slide 19 Lymph Angion Slide 20 Interstitial Fluid Volume Increases if : Decreased venous uptake No increased lymphatic uptake Results in accumulation of plasma proteins triggering chronic inflammation and fibrosis - edema. Slide 21 Venous Return Muscle Pump Healthy venous system-sufficient valves Abdominal breathing Suction effect of heart in diastole Pulsation of adjacent arteries Tissue pressure
8 Slide 22 PATHOPHYSIOLOGY VENOUS AND LYMPHATIC FAILURE SWELLING Slide 23 Mechanisms of Swelling Edema vs Lymphedema Edema intact lymphatic system Lymphedema damaged, insufficient, overloaded lymphatic system Inflammation - burn, bite Trauma fractures Infections/Cellulitis/Wounds Slide 24 Mechanisms Post Operative Acute injuries sprain, strain Neurological paralysis Venous DVT, CVI Medical/Systemic heart, lungs, liver, kidneys CHF, CRF, medications Lifestyle obesity, dependent position, sedentary
9 Slide 25 Risk Factors Lymph vessel destruction secondary to surgical technique Obesity Insufficient muscle contraction Infection or problems with healing Trauma Prolonged dependency of extremity Fibrosis/scarring within the lymph vessel Recurrent infections Hypertension Slide 26 High Volume Edema Dynamic insufficiency occurs when lymphatic load exceeds the Transport Capacity of the anatomically and functionally intact lymphatic system. Edema is temporary and will gradually improve over time (6-12 weeks). Lymph system is Normal. Symptom of a medical condition. Quick onset. Responds to diuretics. Local or general. Slide 27 Chronic Venous Insufficiency Valvular failure of veins causing regurgitation Recanalization/collaterals: proximal blood flow will go through collaterals unsuccessful recanalization; distal blood tries to flow through blocked area causing constant reflux and increased blood pressure resulting in passive hyperemia blood volume, lymph load, fatigue, resorption time, edema
10 Slide 28 Leaky Veins Slide 29 Chronic Venous Insufficiency Damage to dermal and subcutaneous lymphatic network Inflammation with lipodermatosclerosis Increased lymph filtration which overloads an impaired transport system Increased risk of infection and cellulitis Contributes to wound exudate May produce fibrosis, hyperkeratosis, and papillomas of subcutaneous tissue Slide 30 Chronic Venous Insufficiency
11 Slide 31 Stages of CVI Stage Current Suprafascial Pathophysiology Symptoms Water Protein Lymphatics Sufficiency/Insufficiency 0 Asymptomatic high normal normal Suff./safety factor Varicosities, heavy, LTV tired legs I Mild (swelling) high normal normal Phlebo lympho - Stemmer Dynamic insufficiency II Moderate high high Partly Phlebo lympho Hyperpigmentation altered Static insufficiency + Stemmer, Valve/mural Safety valve insuff. lymphangiitis III Severe Ulcerative high Very Partly Extreme phlebo lympho changes; diffusion, high severly static insufficiency O2, tissue death, altered necrosis, ulceration Slide 32 Lipodermatosclerosis Slide 33 Chronic Inflammation Delays wound healing Persistent tissue edema Damaged or blocked lymph vessels Decreased ability to control content and volume of interstitial fluid Impaired macromolecule transport of large proteins, cellular by-products, foreign materials, immune cell, T-lymphocytes, macrophages
12 Slide 34 Chronic Edema Increased tissue pressure Increased diffusion distance Lack of Oxygen Impeded transport Delayed healing, stress on wound edge Impeded supply of basic substances for tissue neoformation Irritation of nociceptors Scar disturbances -keloids, hypertrophy Slide 35 Tissue Changes Due to Protein Accumulation Increased swelling hydrophilic Proteins denature chronic inflammation Connective tissue cells proliferate Collagen fibers are produced Fibrotic changes, sclerosis, induration Fatty tissue increases Slide 36 Impaired Wound Healing Delays due to upset homeostasis Increased volume of interstitial fluid Increased congestion Decreased Oxygen and nutrient diffusion Increased diffusion distance for connective tissue repair Interrupted blood supply Mechanical stress Increased infection risk
13 Slide 37 Signs and Symptoms Increase in Limb size Puffiness Heaviness Fullness/Tightness Bursting sensation Aching/Fatigue Stiffness Hardness Weeping or Leaking Slide 38 Lymphedema Lymphedema occurs if the lymphatic load exceeds the maximum transport capacity resulting in an abnormal accumulation of protein rich fluid. The lymphatic system is not able to maintain the tissue homeostasis. Slide 39 Lymphedema Classification Congenital - at birth Primary Precox - teen years Tarda > 35 years
14 Slide 40 Lymphedema Classification Secondary Acquired lymphedema as a result of a disease process or tissue insult. CVI (#1 world wide), Surgery (#1 - US), radiation therapy (#2 - US), trauma, infection, malignancy, silica dust, filariasis (#2 - world), iatrogenic or self-induced. Slide 41 Lymphedema Classification Secondary - Oncology Surgery damages and removes lymphatic structures and tissue, stimulates increased arterial blood flow Radiation scarring and fibrosis of lymph structures and tissue Infection scarring and fibrosis of lymph vessels, immune system compromise Slide 42 LYMPHEDEMA Mechanical insufficiency : Lymphatic mechanism is impaired/damaged Transport capacity of the lymph system drops below the lymphatic load Lymphatic system is not able to pick up the lymph load Protein accumulation (low volume edema) Compare to Dynamic Insufficiency
15 Slide 43 Stages of Lymphedema Stage 0 Latent / Subclinical primarily oncology patients at risk Stage I - Reversible Lymphedema accumulation of protein-rich edema fluid Stage II - Spontaneously Irreversible Lymphedema protein-rich edema fluid connective & scar tissue Slide 44 Stage II Slide 45 Stage III - Lymphostatic Elephantiasis protein-rich edema fluid connective & scar tissue hardening of dermal tissues papillomas of the skin
16 Slide 46 Stage III Elephantiasis Slide 47 Slide 48
17 Slide 49 PREVENTION Extremity care is essential & the best method for prevention & management. Leg swelling guidelines. Monitoring sign, symptoms, and tissue quality Lymphedema education and prevention. Slide 50 Monitoring Measurements Clothing Fit Mobility Body Awareness Skin and Tissue Quality Early detection Lifetime Slide 51 ASSESSMENT Patient History PMH / Co-morbidities Surgical / XRT Injury / Trauma Infections /Wounds Mobility / Function Lymphedema Onset Treatment Regimens - prior therapies, compliance
18 Slide 52 ASSESSMENT Skin Condition Degree / Location of Swelling Texture / Turgor Temperature / Color Wounds Stemmer s Sign Lymphedema Complications Sensation / Pain Slide 53 Stemmer s Sign Slide 54
19 Slide 55 Slide 56 Slide 57
20 Slide 58 Slide 59 Treatment CDT Slide 60 Complete Decongestive Therapy Skin and wound care Manual lymphatic drainage Compression bandaging Compression Garment/Device Exercises Education in prevention and self care techniques
21 Slide 61 Goals Reduction of swelling to restore function & cosmetic appearance Increase lymph flow from extremity or trunk utilizing remaining vessels & other lymphatic pathways Prevent Re-accumulation of lymph fluid Minimize formation of new lymph fluid Eliminate fibrotic tissue Prevent & eliminate infections Slide 62 Goals - continued Can reduce lymphedema volume by 68% Excellent repair/good skin coverage Promotes softening of tissues, decreasing pitting and induration Decrease edema, redness, pain Decrease limb circumference Decrease wound size Slide 63 PRECAUTIONS Active untreated cancer Dependent on goals of oncology tx Acute inflammation/infection HOLD treatment until pt on ATB >72 and showing signs of improvement Thrombosis (blood clots) HOLD compression x 2 weeks once therapeutically anticoagulated HOLD MLD x 6 wks
22 Slide 64 PRECAUTIONS PAD May need a vascular consult Hypercoagulable risk May need a vascular consult Systemic conditions heart, lungs, liver, kidneys Are they compensated? Medically stable? Precautions need to be addressed prior to referral or treatment. Slide 65 Increased Tissue Pressure Compression bandages Compression garments Manual Lymphatic Drainage (MLD) Underwater Slide 66 Skin & Nail Care Goals Prevent accumulation of bacteria Minimize risk of secondary infection Provide superficial moisturization to dry skin Improves suppleness of skin Barrier to infection
23 Slide 67 Meticulous Skin & Nail Care Hygiene soap and water, gentle exfoliation, tissue movement Moisturization balanced low ph, skin contours/protection, friction (Curel, Eucerin, Nivea, Attractain, 24 hour Sween, Olivamine,) Wound dressings no tape on skin Nail care Proper foot protection/covering Slide 68 Manual Lymph Drainage (MLD) Manual therapy technique Subcutaneous tissue is gently stretched to effect lymph vessels Begins proximally to decrease resistance to fluid movement Minimize formation of new lymph fluid Eliminate fibrotic tissue Prevent & eliminate infections Slide 69 Manual Lymphatic Drainage Goals Stimulates lymphokinetic activity Maximizes drainage, open collaterals Clears lymphostasis Promotes wound healing Decreases volume tension on wound periphery which hinders closing Improves local tissue environment increasing oxygen and nutrients Decreases volume and protein composition of edema Breaks down hard, fibrotic areas
24 Slide 70 Thoracic Duct Slide 71 Lower Extremity Pathways Slide 72 MLD: Wound Healing Indications Compression ineffective reducing edema Extensive fibrosis Tissue injury Traumatic edema Surgery CVI Post-infectious episode Chronic wounds
25 Slide 73 MLD Goals for Wound Healing Improve lymphatic vessel activity Decreased swelling of traumatized area Analgesic effect via - gate control - suppresses sympathetic activity - increased drainage of pain triggering hormones Improve vascular inflow (oxygen, nutrients) and outflow (debris, metabolic waste) Improved speed and quality of tissue repair Sufficient lymphatic flow Slide 74 Treatment Sequence Wound cleansing and debridement Manual lymphatic drainage Wound dressing Compression bandaging Exercises Slide 75 COMPRESSION GUIDELINES Complete testing prior to compression - rule out DVT, infection, mass - vascular consult Medically stabilize patient Results before lymphedema consult DVT wait 2 weeks after therapeutic anticoagulation Cellulitis/infection wait 72 hours if stable and improving on effective ATB
26 Slide 76 Covering v Constriction v Compression v Containment Covering - Comperm/Tubigrip no gradient, unfinished, rolls - Wear-Ease- no gradient, unfinished, rolls Constriction - Ace Wraps long stretch; high resting pressure, low working pressure; uneven pressure; use only on healthy, normal systems Slide 77 Covering v Constriction v Compression v Containment Constriction - TED HOSE - NOT for swelling; NOT appropriate medical compression socks during the day. Primary use for circulation such as post-op, bedridden or prolong immobilization, anti-embolic or general prevention. TEDS are for beds Slide 78 Therapeutic Compression Compression Bandages gradient compression - short stretch; low resting pressure, high working pressure; restores pressure gradient Compression Garments elastic containment - Success equals proper selection - Proper donning/doffing - Compliance Velcro Compression Devices inelastic containment - Consider if donning issues, safety, wounds, caregiver, fragile skin, sensitivity, tolerance
27 Slide 79 Lymphedema Compression Bandage Supplies Slide 80 Compression Bandaging Use of short-stretch multilayered (NOT ACE) bandages Short stretch bandages: Low resting pressure - better tolerance High working pressure less yield Compensates for elastic insufficiency of connective tissue Increases tissue pressure to assist evacuation of fluid Slide 81 Short Stretch Bandage Advantages Figure I Resting pressure Pressure provided by applied bandages (while resting or sleeping) Figure II Working Pressure Pressure exerted by the contraction of muscles within bandaged limb (while walking or exercising)
28 Slide 82 Compressive Bandaging (Cont.) Provides resistance to prevent re-accumulation of lymph fluid reduced filtration, increased reabsorption Break up deposits of accumulated scar or hardened tissue Restores compression gradient of limb Enhanced lymphatic drainage over high stretch Less yielding nature during activity With exercise, it provides a counterforce by creating a muscle pump Slide 83 Thigh High Compression Bandage Slide 84 Modified Compression Bandage Surepress or Rosidal with padding - Leg hygiene and wound care - Liner - Padding - Compression bandage: even, gradient pressure distal to proximal multiple layers proper bandage width
29 Slide 85 Modified Compression Bandage - overlap layers - cover foot and and entire limb segment - use fresh washed bandages - change frequently, minimize slippage/bunching Monitor skin for any irritation/pressure areas Neurocirculation checks-sensation, pain, color, T Assess effectiveness for : slippage/bunching tension tolerance pressure points Slide 86 Law of LaPlace Slide 87 Compression Gradient Bandage pressure is greatest in the distal areas of the extremity and least in the proximal areas.
30 Slide 88 Compression Bandage Guidelines and Precautions Bandages will feel secure and snug. Leg movement maybe somewhat limited. Continue to participate in regular daily activities as tolerated as long as the bandages are not causing any irritation of slippage Wear bandages day and night until ready to progress to the next stage of therapy (i.e. compression garment or device.) Elevate legs when sitting or lying down. Perform exercises ankle pumps,walking If itching occurs, pat the bandages or place a dry cold pack on the outer bandage. Do NOT stick anything down the bandages as this may tear the skin. Slide 89 Slide 90 Nursing Considerations Short stretch gradient compression bandage Padding Elevation Exercise activate ms pump Positioning With sustained short stretch compression the basic wound dressing becomes a dynamic wound dressing. Short stretch does the work.
31 Slide 91 Exercise/Activity in Compression Increase in lymph flow & a dilation of lymph vessels Improves lymph circulation & lymph vessel activity Causes a suction effect, negative pressure gradient, and muscle pump Slide 92 Muscle Pump Muscle activity decompresses both the venous & lymphatic system. Figure II shows contracted muscles, figure III shows relaxed muscle. Slide 93 Compression Garment Goals Provide long term preservation of reduced limb circumferences Prevent re-accumulation of lymph fluid in the interstitium by controlling hydrostatic pressure Provides support for tissues that have lost their elasticity Provide extracellular tissue pressures to facilitate lymph fluid uptake and continued softening of fibrotic tissues
32 Slide 94 Compression Garments Fit after limb volume reduction Garments are the container Garment worn during the day, possibly at night Nighttime management to be determined by tissue response and therapist assessment. Assess for effectiveness Donn/Doff with adaptive equipment Replacement schedule every 4-6 months Slide 95 Compression Garment Success Must be the correct: Time Fit / measurements / size Compression level Fabric Features Application Wearing schedules Other options: compression Velcro devices Slide 96 Compression garments SELECTION CRITERIA Correct Size: Leg circumference (ankle and calf) and leg length, size verified with a measuring chart. May need to consider custom. Correct Style: Knee high/thigh high/panty hose, Open/Closed toe, Silicone band, Off-the-shelf/Custom Correct Fabric: Sheer/Transparent, Thick/Heavy, Circular knit, Flat knit. Bridging and garment fatigue. Don t base selection on cosmesis or cost. Correct Timing: Compression stockings are used to maintain not reduce swelling. Compression bandages required to reduce leg swelling before wearing compression garments.
33 Slide 97 Compression garments Correct Compression Level : < mmhg Heavy, tight, aching legs mmhg Mild swelling mmhg Moderate swelling mmhg Difficult to control swelling Correct Wearing Schedule: Wear compression every day, lifetime. Apply first thing in the morning before legs swell Slide 98 Garment Donning/Doffing Aids Slippee/footies Donning Gloves Donning Frames Gripper Pads Don-n-Doffer Easy Slide, Magnide, Juzo Gator, etc Long handled shoe horns Reacher Silicone Fitting Lotions Consider ease of use, durability, mobility, cost Slide 99 Proper Fit of Garments Do not gather or pull on bands massage fabric Use rubber gloves and donning tools Wear on clean skin Clean garment every day Heel position Toe and knee band Fabric distribution No wrinkles or rolling Adjust fit throughout the day
34 Slide 100 Garment Care Wash daily to regain elasticity. Hand wash, air dry (some exceptions will allow machine wash/dry using permanent press cycle). Do NOT use bleach, fabric softener, dish soap, or Woolite. Lotion will break down the elastic fibers, thus the pressure will be not adequate to control swelling. Skin prep: Cutimed, Compression Assist Lotion Replace compression garments every 4-6 months. Slide 101 Garment Gradient Slide 102 Velcro Compression Devices Limited ability to donn/doff compression garment Safety unreliable use or care of garment Wounds Fragile Skin Hypersensitive skin Compression tolerance Limp shape garment unable to bridge over tissue crevice between folds Prolonged wearing Limited caregiver resources
35 Slide 103 Long Term Effectiveness Ambulatory vs Non Ambulatory Skin integrity / Wounds Tolerance for compression Compliance Ease of use, donn/doff Pt goals Co-morbidities Night time compression needs Cost Slide 104 Long Term Effectiveness Compression garment failure, not appropriate Chronic wound dressings Mobility Function Need for 24 hr compression Vasopneumatic compression device - preservation Sustainability Slide 105 Long Term Effects of CDP 300 Maintained Patients 9 (Initial) Months Limb Reduction UE 59.1% 86% compliant maintained 90%* Limb Reduction LE 67.7% Decreased Infections 1.1 per pt/yr 0.65 per pt/yer *Non-compliant patients lost 33% of initial reduction Reduction sustained over the next 36 months
36 Slide 106 Complementary Strategies Positioning / Elevation Exercise Nutrition Weight Loss Diuretics Vasopneumatic Pumps Slide 107 Pneumatic Compression Pumps Target venous water based fluid not lymph Immobile May cause genital swelling Does not facilitate protein uptake May traumatize functioning lymphatics Settings may be inaccurate avoid high pressures Still need to stimulate proximal lymph system Still requires continuous compression after use Use to sustain/preserve outcomes of other modalities and to continued use of compression garment/device. Slide 108 Leg Swelling Guidelines Elevation - at least 6, legs straight, trunk reclined Position - change hourly; avoid prolonged sit/stand Exercise ankle pumps, walking Healty Body Weight well balanced diet, glasses water, avoid salt and caffeine Don t smoke No constrictive clothing Avoid heat Avoid trauma Monitor legs for infection Podiatry if indicated Daily skin care Wear recommended compression as prescribed
37 Slide 109 Limitations of Common Interventions Interventions Why they don t work Diuretics leave the protein behind - which are hydrophilic anti embolism socks for post op or bed rest patients; only TED hose 8-15mmHg - not enough for swelling management long stretch, high resting pressures, low working pressure, Ace Wraps uncomfortable, constrict, reduce circulation, extensible, no resistance to muscle contraction not functional, sometimes co morbidities do not allow, lymph Elevation fluid is thick and doesn't respond as well to elevation need to follow up with compression, not all pumps are the same, be aware of co morbidities, passive/immobile, may Compression Pumps cause genital swelling, no protein uptake, may traumatize functioning lymphatics, settings may be inaccurate Weight Loss can't diet it off, it's not fat; helpful for long term management often over compressive; need follow up lymphedema UNNA Boots treatment once tissue integrity is improved Skin sensitivity/irritation, intact skin only, follow up with KT Tape compression Slide 110 Provider Credentials Usually PT or OT Certified Lymphedema Therapist, LANA preferred (CLT-LANA) CDT Treatment Protocol Dedicated provider / facility Insurance Coverage / Resources Slide 111 Referral Process JSCC Lymphedema Clinic UnityPoint Des Moines Iowa Methodist 1200 Pleasant St, Suite 450 Des Moines, Iowa P: F: Once pt is therapeutically ready: Phone / FAX Send Demographics Send H&P and last office visit notes
38 HYGIENE Wash leg thoroughly with an antibacterial soap then dry well. Apply lotion to intact skin. Lotions low in ph are recommended, e.g. Curel, Eucerin, and Nivea. Complete wound care (If needed) The bandage and padding should cover the foot and lower leg. STOCKINET Apply clean stockinet over the leg. When making a new piece of stockinet, cut it twice the length of the leg from the toes to knee. PRESSURE GRADIENT Be sure to apply more layers of Surepress bandage at the foot to create a pressure gradient. By providing higher pressure (more layers) at the foot and less pressure (layers) at the calf you will help push the fluid upward and out of the leg. WHITE FOAM Start at the end of the foot near the toes. Make a circular turn around the foot then proceed around the ankle and spiral up the calf. Use mild tension when applying the foam. The heel is left uncovered. Do NOT apply tape directly on white foam May use white fluff for added padding to foot/ankle or to even out tissue shape, pressure areas OPTION #2 ROSIDAL 1. 8 cm to foot and ankle as above 2-3 layers at ball of foot 1-2 layers at arch Proceed to ankle then up leg 2. Begin at ankle and then proceed up leg, overlapping 50% with gentle tugs on the sides. Finish just below the knee. Tape down. SURE PRESS BANDAGE Begin the bandage at the foot. Make 1-3 circles around the foot near the toes, then 1-2 circles around the mid foot (arch). Use even firm tension, smoothing bandage at each turn. Proceed to the ankle (heel will be open) and then up the calf with the remaining bandage using firm tension with gentle tugs on the sides. Be sure to overlap each layer by about 1/2 as you spiral up the calf. End the bandage just below knee crease and tape in place. Paper tape is recommended. OTHER SWELLING REDUCTION STRATEGIES Elevate legs Perform ankle pumps Slide 112 OBJECTIVES - LAB Demonstrate proper application of modified edema compression bandage. Identify precautions for compression application and guidelines for transition to successful home management Demonstrate adaptive techniques and devices used to assist with application of compression garments. Demonstrate ability to compare and contrast complementary edema management strategies. Slide 113 Lab Let s practice Surepress/Short Stretch Edema compression Toes, padding, bandage Compression Garments Features Compression Garment Donning/Doffing Velcro Compression Devices Accessing Suppliers/Vendors Slide 114 EDEMA BANDAGING FOR THE LOWER EXTREMITY
39 Slide 115 WEARING SCHEDULE WASHING INSTRUCTIONS REPLACEMENT SUPPLIES Wear bandages Hand wash in warm soapy during the day. water and rinse well. Squeeze 1. TG Stockinet: (not wring) bandage/stockinet Size: Wear bandages to remove excess moisture during the night. then air dry. Keep bandages away from direct heat sources 2. White Foam Change the when drying. Rosidol Soft: bandages every Size: days. Sure press and short stretch compression 3. Sure Press Bandage *** If slippage or bandagse: needs to be OR Short Stretch discomfort occurs, change washed at least every 4 8cm and 10 cm the bandages more days, more frequent if frequently. soiled or stretched out 4. Optional: White fluff 10 cm (Artiflex / Stockinet: Apply a clean Cellona) stockinet each day. Hand wash and reuse the stockinet. White Foam/Fluff This product does not need to be washed routinely. It can be washed if soiling occurs. See instructions above. Slide 116 Bandaging Tolerance Bandages should not increase any baseline symptoms. Monitor for any new or increasing symptoms: Pins and Needles abnormal sensation of the toes Numbness and Tingling abnormal sensation of the toes Pain in leg or foot Discoloration of the toes toes bluish or pale color Temperature toes cool Interventions if problems develop with bandages: Elevation Elevate legs on pillows Exercise Perform ankle pumps, walk Remove the bandages Modify padding or layers with next bandage Slide 117 Compression Garment Success Must be the correct: Time Fit / measurements / size Compression level Fabric Features Application Wearing schedules Other options: compression Velcro devices
40 Slide 118 Compression garments SELECTION CRITERIA Correct Size: Leg circumference (ankle and calf) and leg length, size verified with a measuring chart. May need to consider custom. Correct Style: Knee high/thigh high/panty hose, Open/Closed toe, Silicone band, Off-the-shelf/Custom Correct Fabric: Sheer/Transparent, Thick/Heavy, Circular knit, Flat knit. Bridging and garment fatigue. Don t base selection on cosmesis or cost. Correct Timing: Compression stockings are used to maintain not reduce swelling. Compression bandages required to reduce leg swelling before wearing compression garments. Slide 119 Compression garments Correct Compression Level : < mmhg Heavy, tight, aching legs mmhg Mild swelling mmhg Moderate swelling mmhg Difficult to control swelling Correct Wearing Schedule: Wear compression every day, lifetime. Apply first thing in the morning before legs swell Slide 120 Garment Donning/Doffing Aids Slippee/footies Donning Gloves Donning Frames Gripper Pads Don-n-Doffer Easy Slide, Magnide, Juzo Gator, etc Long handled shoe horns Reacher Silicone Fitting Lotions Consider ease of use, durability, mobility, cost
41 Slide 121 Velcro Compression Devices Limited ability to donn/doff compression garment Safety unreliable use or care of garment Wounds Fragile Skin Hypersensitive skin Compression tolerance Limp shape garment unable to bridge over tissue crevice between folds Prolonged wearing Limited caregiver resources Slide 122 Compression Garments/Devices Local Providers CHLADEK ORTHOTIC & PROSTHETIC, INC. FITTINGS UNLIMITED, INC. HANGER CLINIC: PROSTHETICS & ORTHOTICS NUCARA UNITY POINT HOME STORE Slide 123 Lymphedema Compression Product Resources Academy of Lymphatic Studies Bandages Plus, Inc Prism Medical Products * SunMed Medical Solutions * Lohman & Rauscher/Solaris BSN Medical/Farrow North America Rehabilitation BrightLife Direct, Inc. Academy of Lymphatic Studies All provide bandages, garments and devices. * will verify insurance benefits
LYMPHEDEMA GOALS FOR TODAY WELL-INTENTIONED, BUT. the more you know TEDS. Diuretics. Prescribe compression garments without first reducing edema
 LYMPHEDEMA the more you know GOALS FOR TODAY WELL-INTENTIONED, BUT TEDS Recognize full Continuum of Lymphedema stages Identify Range of Lymphedema Diagnoses Differentiate Effective Treatment Options from
LYMPHEDEMA the more you know GOALS FOR TODAY WELL-INTENTIONED, BUT TEDS Recognize full Continuum of Lymphedema stages Identify Range of Lymphedema Diagnoses Differentiate Effective Treatment Options from
Catherine Holley, RN Operating Room Nurse Massachusetts General Hospital
 Operating Room Nurse Massachusetts General Hospital March 13, 2019 What is Lymphedema? Swelling (edema) that occurs due to injury or impairment of the lymphatic system Causes: Anything that disrupts the
Operating Room Nurse Massachusetts General Hospital March 13, 2019 What is Lymphedema? Swelling (edema) that occurs due to injury or impairment of the lymphatic system Causes: Anything that disrupts the
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
SOLARIS. Exo. Off-the-Shelf Gradient Compression Garments
 SOLARIS F R E E D O M T O L I V E Exo B Y S O L A R I S Off-the-Shelf Gradient Compression Garments Table of Contents 3 4 6 8 4 6 3 Contact Information Why Choose Exo Exo Quick Reference Chart Upper Extremity
SOLARIS F R E E D O M T O L I V E Exo B Y S O L A R I S Off-the-Shelf Gradient Compression Garments Table of Contents 3 4 6 8 4 6 3 Contact Information Why Choose Exo Exo Quick Reference Chart Upper Extremity
Velcro Compression Devices
 Velcro Compression Devices Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University of Chicago
Velcro Compression Devices Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University of Chicago
What is Lymphedema? Primary lymphedema: a person is born with the condition where the lymphatic vessels are not formed completely or malformed
 Lymphedema What is Lymphedema? Lymphedema is a chronic health condition which causes localized swelling. There are 2 types: Primary lymphedema: a person is born with the condition where the lymphatic vessels
Lymphedema What is Lymphedema? Lymphedema is a chronic health condition which causes localized swelling. There are 2 types: Primary lymphedema: a person is born with the condition where the lymphatic vessels
Self Management with Compression
 Self Management with Compression Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University
Self Management with Compression Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University
9 Day Certified Lymphedema & Wound Therapist (62.5 CE hrs On-line + 9 Days Live Training (8am 8pm *daily times vary; 153 CE hrs Total!
 1 9 Day Certified Lymphedema & Wound Therapist (62.5 CE hrs On-line + 9 Days Live Training (8am 8pm *daily times vary; 153 CE hrs Total!) On-Line COURSE OUTLINE/Overview of Topics (62.5hrs): Lymphatics
1 9 Day Certified Lymphedema & Wound Therapist (62.5 CE hrs On-line + 9 Days Live Training (8am 8pm *daily times vary; 153 CE hrs Total!) On-Line COURSE OUTLINE/Overview of Topics (62.5hrs): Lymphatics
Juxta CURES Compression Ulcer Recovery System
 medi UK Ltd. Plough Lane Hereford HR4 OEL United Kingdom T 01432 37 35 00 F 01432 37 35 10 enquiries@mediuk.co.uk www.mediuk.co.uk 97C28/01.2013 Juxta CURES Compression Ulcer Recovery System Patient Information
medi UK Ltd. Plough Lane Hereford HR4 OEL United Kingdom T 01432 37 35 00 F 01432 37 35 10 enquiries@mediuk.co.uk www.mediuk.co.uk 97C28/01.2013 Juxta CURES Compression Ulcer Recovery System Patient Information
Cancer Support V.I. Presents
 Cancer Support V.I. Presents Overview & Discussion of Manual Lymph Drainage/Complete Decongestive Therapy (MLD/CDT) Presented by: Christopher A. Borgesen, MS,OTR September 3 rd, 2008 Christopher A. Borgesen,
Cancer Support V.I. Presents Overview & Discussion of Manual Lymph Drainage/Complete Decongestive Therapy (MLD/CDT) Presented by: Christopher A. Borgesen, MS,OTR September 3 rd, 2008 Christopher A. Borgesen,
Lymphatic Facilitation for Athletic Injuries. Director of Instruction Discoverypoint School of Massage Seattle WA
 Lymphatic Facilitation for Athletic Injuries Pat Archer ATC, LMP Director of Instruction Discoverypoint School of Massage Seattle WA Lymphatic Facilitation A specific lymphatic technique proven as an easy
Lymphatic Facilitation for Athletic Injuries Pat Archer ATC, LMP Director of Instruction Discoverypoint School of Massage Seattle WA Lymphatic Facilitation A specific lymphatic technique proven as an easy
4-layer compression bandaging system (includes microbe binding wound contact layer) Latex-free, 4-layer compression bandaging system
 JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
Catherine Holley, RN Operating Room Nurse Massachusetts General Hospital
 Operating Room Nurse Massachusetts General Hospital March 15, 2017 Background Nurse 34 years Operating room RN at Massachusetts General Hospital 1979 surgery to remove varicose veins right leg Strong family
Operating Room Nurse Massachusetts General Hospital March 15, 2017 Background Nurse 34 years Operating room RN at Massachusetts General Hospital 1979 surgery to remove varicose veins right leg Strong family
Course Objectives. Circulatory system. Understand the basic design of the lymphatic system
 Lymphedema: What Every Healthcare Practitioner Needs to Know Debbie Chasse DPT, WCS, CLT-LANA www.functionabilitypt.com Understand the basic design of the lymphatic system Course Objectives Circulatory
Lymphedema: What Every Healthcare Practitioner Needs to Know Debbie Chasse DPT, WCS, CLT-LANA www.functionabilitypt.com Understand the basic design of the lymphatic system Course Objectives Circulatory
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
JOINT JACKETS. Play Hard, Heal Fast.
 JOINT JACKETS M A N U F A C T U R E D B Y S O L A R I S Play Hard, Heal Fast www.solarismed.com Resolves Inflammation. Joint Jackets use a unique foam chip technology which: Provides a micro-massage to
JOINT JACKETS M A N U F A C T U R E D B Y S O L A R I S Play Hard, Heal Fast www.solarismed.com Resolves Inflammation. Joint Jackets use a unique foam chip technology which: Provides a micro-massage to
Medical Policy Original Effective Date: 01/23/2019
 Page 1 of 12 Disclaimer Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans or the plan may have broader or more limited benefits
Page 1 of 12 Disclaimer Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans or the plan may have broader or more limited benefits
Supporting Information Leaflet (11): Managing Oedema and Circulatory Problems in Neuromuscular Disorders
 Supporting Information Leaflet (11): Managing Oedema and Circulatory Problems in Neuromuscular Disorders Oedema, sometimes known as Lymphoedema or fluid retention is the build up of fluid and other elements
Supporting Information Leaflet (11): Managing Oedema and Circulatory Problems in Neuromuscular Disorders Oedema, sometimes known as Lymphoedema or fluid retention is the build up of fluid and other elements
Chapter 28. Wound Care. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 28 Wound Care Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 28.1 Define the key terms and key abbreviations in this chapter. Describe skin tears, circulatory ulcers, and diabetic
Chapter 28 Wound Care Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 28.1 Define the key terms and key abbreviations in this chapter. Describe skin tears, circulatory ulcers, and diabetic
UNDERSTANDING VEIN PROBLEMS
 UNDERSTANDING VEIN PROBLEMS Varicose Veins, Chronic Venous Insufficiency, and DVT Do You Have a Vein Problem? Have you noticed pain or swelling in your legs? Do your symptoms worsen when you re sitting
UNDERSTANDING VEIN PROBLEMS Varicose Veins, Chronic Venous Insufficiency, and DVT Do You Have a Vein Problem? Have you noticed pain or swelling in your legs? Do your symptoms worsen when you re sitting
CaresiaTM. Off-the-Shelf Bandage Liners
 CaresiaTM M A N U F A C T U R E D B Y S O L A R I S Off-the-Shelf Bandage Liners Table of Contents 2 3 4 6 8 10 11 Contact Information About Caresia Upper Extremity Garments Lower Extremity Garments Donning
CaresiaTM M A N U F A C T U R E D B Y S O L A R I S Off-the-Shelf Bandage Liners Table of Contents 2 3 4 6 8 10 11 Contact Information About Caresia Upper Extremity Garments Lower Extremity Garments Donning
When is it lymphedema, when is it not lymphedema? UNDERSTANDING EDEMA. John Mulligan, RMT/CLT-LANA
 When is it lymphedema, when is it not lymphedema? UNDERSTANDING EDEMA John Mulligan, RMT/CLT-LANA Learning Objectives How to identify stages of lymphedema The Gold Standard of Treatment for Lymphedema
When is it lymphedema, when is it not lymphedema? UNDERSTANDING EDEMA John Mulligan, RMT/CLT-LANA Learning Objectives How to identify stages of lymphedema The Gold Standard of Treatment for Lymphedema
Dear Medical Professional,
 www.solarismed.com Dear Medical Professional, My co-workers and I would like to take this opportunity to thank you for partnering with us in providing a comprehensive lymphedema management program for
www.solarismed.com Dear Medical Professional, My co-workers and I would like to take this opportunity to thank you for partnering with us in providing a comprehensive lymphedema management program for
Chronic Venous Insufficiency Compression and Beyond
 Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Treating your leg ulcer
 Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device
 VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
Training Outline. History of medi. Circulation in the body. Medical Conditions. Athletic Conditions. Compression in Sports. Compression for recovery
 Compression 101 1 Training Outline History of medi Circulation in the body Medical Conditions Athletic Conditions Compression in Sports Compression for recovery Tips 2 History of medi medi began in the
Compression 101 1 Training Outline History of medi Circulation in the body Medical Conditions Athletic Conditions Compression in Sports Compression for recovery Tips 2 History of medi medi began in the
Sores That Will Not Heal
 Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Patient Information. Venous Insufficiency and Varicose Veins
 Patient Information Venous Insufficiency and Varicose Veins What is a Varicose Vein? Gitter Vein Institute-revised 3/8/2016 2 Frequently Asked Questions What is the difference between varicose and spider
Patient Information Venous Insufficiency and Varicose Veins What is a Varicose Vein? Gitter Vein Institute-revised 3/8/2016 2 Frequently Asked Questions What is the difference between varicose and spider
CASE STUDY. Potential conflict of interest:
 CASE STUDY presented by MICHEL EID, Lymphedema therapist Vodder School Teacher Physio Extra 2014 1 Potential conflict of interest: Invited speaker for: Physio Extra Jobst Medi Valco 1 What is lymphedema?
CASE STUDY presented by MICHEL EID, Lymphedema therapist Vodder School Teacher Physio Extra 2014 1 Potential conflict of interest: Invited speaker for: Physio Extra Jobst Medi Valco 1 What is lymphedema?
Alberta Health. Alberta Aids to Daily Living Compression Stockings and Lymphedema Sleeves Ready Made Benefits Policy & Procedures Manual
 Alberta Health Alberta Aids to Daily Living Compression Stockings and Lymphedema Sleeves Ready Made Benefits Policy & Procedures Manual March 7, 2016 Revision History Description Date N-03, N 05 and N-07:
Alberta Health Alberta Aids to Daily Living Compression Stockings and Lymphedema Sleeves Ready Made Benefits Policy & Procedures Manual March 7, 2016 Revision History Description Date N-03, N 05 and N-07:
PRACTICAL TIPS FOR LOOKING AFTER YOUR SKIN
 Being an active partner in your care www.veteransmates.net.au PRACTICAL TIPS FOR LOOKING AFTER YOUR SKIN As we get older, our skin becomes more delicate and dry, and skin tears are common. However, the
Being an active partner in your care www.veteransmates.net.au PRACTICAL TIPS FOR LOOKING AFTER YOUR SKIN As we get older, our skin becomes more delicate and dry, and skin tears are common. However, the
Use of a velcro wrap system in the management of lower limb lymphoedema/chronic oedema. Sue Lawrance
 Use of a velcro wrap system in the management of lower limb lymphoedema/chronic oedema Sue Lawrance Abstract Lymphoedema and chronic lower limb oedema are conventionally treated with multi-layer bandaging,
Use of a velcro wrap system in the management of lower limb lymphoedema/chronic oedema Sue Lawrance Abstract Lymphoedema and chronic lower limb oedema are conventionally treated with multi-layer bandaging,
How varicose veins occur
 Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Treatment of lymphoedema surgical and conservative approaches
 Treatment of lymphoedema surgical and conservative approaches Nina Linnitt RN Clinical Manager medi UK Current Chair British Lymphology Society (BLS) What is lymphoedema? International Societie de Lymphologue
Treatment of lymphoedema surgical and conservative approaches Nina Linnitt RN Clinical Manager medi UK Current Chair British Lymphology Society (BLS) What is lymphoedema? International Societie de Lymphologue
ANKLE SPRAINS. Explanation. Causes. Symptoms
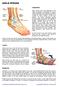 ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
Rosidal TCS Trust our strength
 Rosidal TCS Trust our strength effective, comfortable, safe compression www.lohmann-rauscher.us Rosidal TCS provides effective compression The two components of Rosidal TCS work together to deliver effective
Rosidal TCS Trust our strength effective, comfortable, safe compression www.lohmann-rauscher.us Rosidal TCS provides effective compression The two components of Rosidal TCS work together to deliver effective
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 6 Roller Bandages. LESSON ASSIGNMENT Paragraphs 6-1 through 6-10. LESSON OBJECTIVES After completing this lesson, you should be able to: 6-1. Identify the functions of roller bandages.
LESSON ASSIGNMENT LESSON 6 Roller Bandages. LESSON ASSIGNMENT Paragraphs 6-1 through 6-10. LESSON OBJECTIVES After completing this lesson, you should be able to: 6-1. Identify the functions of roller bandages.
Improving customer care in compression hosiery
 Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
{loadposition nhschoices} {loadposition relatedart} Condition Legs - tired, aching, heavy. Class Circulatory system. Description
 - Condition - Class - Description - Causes - Symptoms - Treatment - When to see your pharmacist - When to see your doctor - Living with tired, aching legs - Useful Tips {loadposition nhschoices} {loadposition
- Condition - Class - Description - Causes - Symptoms - Treatment - When to see your pharmacist - When to see your doctor - Living with tired, aching legs - Useful Tips {loadposition nhschoices} {loadposition
Lymphedema Myths Realities - Hope
 Lymphedema Myths Realities - Hope Texas Health Presbyterian Hospital of Dallas Lymphedema Therapy Department 214-345-7680 Lymphatic System Divided into sections - watersheds Lymph nodes act as filtration
Lymphedema Myths Realities - Hope Texas Health Presbyterian Hospital of Dallas Lymphedema Therapy Department 214-345-7680 Lymphatic System Divided into sections - watersheds Lymph nodes act as filtration
JOBST FARROWWRAP LYMPHOEDEMA MANAGEMENT MADE SIMPLE THROUGH ADJUSTABLE SHORT-STRETCH WRAP SOLUTIONS THERAPIES. HAND IN HAND.
 JOBST FARROWWRAP LYMPHOEDEMA MANAGEMENT MADE SIMPLE THROUGH ADJUSTABLE SHORT-STRETCH WRAP SOLUTIONS THERAPIES. HAND IN HAND. HOW DO YOU STRIKE THE RIGHT BALANCE BETWEEN BOTH YOUR PATIENT S MEDICAL NEEDS
JOBST FARROWWRAP LYMPHOEDEMA MANAGEMENT MADE SIMPLE THROUGH ADJUSTABLE SHORT-STRETCH WRAP SOLUTIONS THERAPIES. HAND IN HAND. HOW DO YOU STRIKE THE RIGHT BALANCE BETWEEN BOTH YOUR PATIENT S MEDICAL NEEDS
Welcome to Allied Health Telehealth
 Welcome to Allied Health Telehealth Paediatric lymphoedema A challenge for clinicians and families To receive an attendance certificate please complete your online evaluation at: https://www.surveymonkey.com/s/paedlymphoedema
Welcome to Allied Health Telehealth Paediatric lymphoedema A challenge for clinicians and families To receive an attendance certificate please complete your online evaluation at: https://www.surveymonkey.com/s/paedlymphoedema
Patient Self-Bandaging Leg and Individual Toe Application Guide
 3M Coban 2 for Lymphoedema Compression System Patient Self-Bandaging Leg and Individual Toe Application Guide Disclaimer: This guide is to be used under supervision by your healthcare practitioner following
3M Coban 2 for Lymphoedema Compression System Patient Self-Bandaging Leg and Individual Toe Application Guide Disclaimer: This guide is to be used under supervision by your healthcare practitioner following
Knee Replacement Recovery Guide
 Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
CARESIA QUICK REFERENCE GUIDE. Standard size bandage liners that simplify your therapy.
 CARESIA QUICK REFERENCE GUIDE M A N U F A C T U R E D B Y S O L A R I S Standard size bandage liners that simplify your therapy. Caresia Quick Reference Guide Solaris Quick Reference Guides are your helpful
CARESIA QUICK REFERENCE GUIDE M A N U F A C T U R E D B Y S O L A R I S Standard size bandage liners that simplify your therapy. Caresia Quick Reference Guide Solaris Quick Reference Guides are your helpful
How is 1st MTP joint fusion carried out? Patient Information: Big Toe Fusion Metatarsophalangeal (MTP)
 Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
CARING FOR THE CLIENT ON COMPLETE BEDREST
 CARING FOR THE CLIENT ON COMPLETE BEDREST INTRODUCTION The human body is designed to move. And just as the human body thrives on movement, it suffers when for one reason or another there is enforced immobility.
CARING FOR THE CLIENT ON COMPLETE BEDREST INTRODUCTION The human body is designed to move. And just as the human body thrives on movement, it suffers when for one reason or another there is enforced immobility.
KINESIOLOGY TAPING GUIDE
 KINESIOLOGY TAPING GUIDE What is Kinesiology tape and how does Kinesiology tape work? How to apply Kinesiology tape Examples of application of UP Kinesiology tape for common injuries and conditions Introduction
KINESIOLOGY TAPING GUIDE What is Kinesiology tape and how does Kinesiology tape work? How to apply Kinesiology tape Examples of application of UP Kinesiology tape for common injuries and conditions Introduction
Prosthetic Rehab Plan
 Prosthetic Rehab Plan First 4 6 weeks after surgery Until sutures are removed, follow the instructions below: Gently wash your limb daily with anti-bacterial soap and water Wear the brown stump shrinker
Prosthetic Rehab Plan First 4 6 weeks after surgery Until sutures are removed, follow the instructions below: Gently wash your limb daily with anti-bacterial soap and water Wear the brown stump shrinker
JOBST FarrowWrap LYMPHEDEMA MANAGEMENT MADE SIMPLE WITH FARROWWRAP ELASTIC SHORT-STRETCH. THERAPIES. HAND IN HAND.
 JOBST FarrowWrap LYMPHEDEMA MANAGEMENT MADE SIMPLE WITH FARROWWRAP ELASTIC SHORT-STRETCH THERAPIES. HAND IN HAND. www.bsnmedical.com HOW DO YOU STRIKE A BALANCE BETWEEN YOUR PATIENT S MEDICAL NEEDS AND
JOBST FarrowWrap LYMPHEDEMA MANAGEMENT MADE SIMPLE WITH FARROWWRAP ELASTIC SHORT-STRETCH THERAPIES. HAND IN HAND. www.bsnmedical.com HOW DO YOU STRIKE A BALANCE BETWEEN YOUR PATIENT S MEDICAL NEEDS AND
Compression Garment Guide
 Compression Garment Guide BOOK AN APPOINTMENT Please be aware that for all Sigvaris Medical compression garments Surgical House staff require the garment wearer to attend a fitting appointment to ascertain
Compression Garment Guide BOOK AN APPOINTMENT Please be aware that for all Sigvaris Medical compression garments Surgical House staff require the garment wearer to attend a fitting appointment to ascertain
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL Policy Number: MP.015.MH Last Review Date: 11/08/2018 Effective Date: 02/01/2019
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL This policy applies to the following lines of business: MedStar Employee (Select) MedStar CareFirst PPO MedStar Health considers Compression Garments and
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL This policy applies to the following lines of business: MedStar Employee (Select) MedStar CareFirst PPO MedStar Health considers Compression Garments and
Lymphoedema Network Northern Ireland. Advice for patients at risk of developing lymphoedema
 Lymphoedema Network Northern Ireland Advice for patients at risk of developing lymphoedema Conditions related to increased risk of developing lymphoedema: High risk referral criteria Do you have any of
Lymphoedema Network Northern Ireland Advice for patients at risk of developing lymphoedema Conditions related to increased risk of developing lymphoedema: High risk referral criteria Do you have any of
CaresiaTM. user guide
 CaresiaTM M A N U F A C T U R E D B Y S O L A R I S user guide Your Caresia Bandage Liner Thank you for purchasing your Caresia! Your Caresia is a standard sized, foam particle liner, designed by professionals,
CaresiaTM M A N U F A C T U R E D B Y S O L A R I S user guide Your Caresia Bandage Liner Thank you for purchasing your Caresia! Your Caresia is a standard sized, foam particle liner, designed by professionals,
TREATING LOWER LIMB LYMPHOEDEMA WITH COMPRESSION BANDAGING
 TREATING LOWER LIMB LYMPHOEDEMA WITH COMPRESSION BANDAGING Debra Doherty is Senior Lecturer, Centre for Research and implementation of Clinical Practice, Thames Valley University Multilayer continues to
TREATING LOWER LIMB LYMPHOEDEMA WITH COMPRESSION BANDAGING Debra Doherty is Senior Lecturer, Centre for Research and implementation of Clinical Practice, Thames Valley University Multilayer continues to
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
CAST CARE. Helping Broken Bones Heal
 CAST CARE Helping Broken Bones Heal When You Need a Cast Are you injured and in need of a cast? Don t worry, you ll get through it. Wearing a cast will help your injured body part heal. Healing takes time,
CAST CARE Helping Broken Bones Heal When You Need a Cast Are you injured and in need of a cast? Don t worry, you ll get through it. Wearing a cast will help your injured body part heal. Healing takes time,
This article is intended as a
 Compression Hosiery and Multilayer Wraps: Proper Prescription and Usage The effect of this therapy on venous ulcers is impressive. By Steven Kravitz, DPM 123 This article is intended as a reference for
Compression Hosiery and Multilayer Wraps: Proper Prescription and Usage The effect of this therapy on venous ulcers is impressive. By Steven Kravitz, DPM 123 This article is intended as a reference for
Rehabilitation After Patellar Tendon Debridement Surgery
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Ligation with Stripping
 Ligation with Stripping Understanding Problem Leg Veins Do your legs feel tired and achy at the end of the day? Have you stopped wearing shorts because you don t like the way your legs look? Vein problems
Ligation with Stripping Understanding Problem Leg Veins Do your legs feel tired and achy at the end of the day? Have you stopped wearing shorts because you don t like the way your legs look? Vein problems
Your Caresia Bandage Liner
 user guide Your Caresia Bandage Liner Thank you for purchasing your Caresia! Your Caresia is a standard sized, foam particle liner, designed by professionals, to help simplify your multilayered bandaging
user guide Your Caresia Bandage Liner Thank you for purchasing your Caresia! Your Caresia is a standard sized, foam particle liner, designed by professionals, to help simplify your multilayered bandaging
WOUND CARE. By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare
 WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
Latmedical, LLC is the exclusive Caribbean distributor
 No-Varix Graduated Compression Hosiery is manufactured by TEXPON S.A., the only Latin- American company certified with the norm ISO 9001:00 with scope of manufacture of graduate compression hosiery for
No-Varix Graduated Compression Hosiery is manufactured by TEXPON S.A., the only Latin- American company certified with the norm ISO 9001:00 with scope of manufacture of graduate compression hosiery for
Our Vision NADA BoD Strategic Planning Session -
 Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
DIABETES AND FOOTCARE
 DIABETES AND FOOTCARE Self-Care and Treatment for Healthy Feet Don t Take Your Feet for Granted Every day, you depend on your feet to keep you moving. But when you have diabetes, your feet need special
DIABETES AND FOOTCARE Self-Care and Treatment for Healthy Feet Don t Take Your Feet for Granted Every day, you depend on your feet to keep you moving. But when you have diabetes, your feet need special
The Standard of Care for Lymphedema: Current Concepts and Physiological Considerations
 The Standard of Care for Lymphedema: Current Concepts and Physiological Considerations Harvey N. Mayrovitz PhD Professor of Physiology College of Medical Sciences Nova Southeastern University mayrovit@nova.edu
The Standard of Care for Lymphedema: Current Concepts and Physiological Considerations Harvey N. Mayrovitz PhD Professor of Physiology College of Medical Sciences Nova Southeastern University mayrovit@nova.edu
OV United Soccer Club
 Preventing disease transmission Place an effective barrier between you and the victim s blood when you give first aid. Examples of such barriers are: the victim s hand, a piece of plastic, clean folded
Preventing disease transmission Place an effective barrier between you and the victim s blood when you give first aid. Examples of such barriers are: the victim s hand, a piece of plastic, clean folded
This booklet has been developed to help guide you through your post-operative rehabilitation.
 Patient Information Physiotherapy following Breast Surgery Physiotherapy Directorate Keep this booklet as a reminder with your exercises long term. If you start to develop stiffness, pain, weakness, or
Patient Information Physiotherapy following Breast Surgery Physiotherapy Directorate Keep this booklet as a reminder with your exercises long term. If you start to develop stiffness, pain, weakness, or
Exercises After Breast Surgery
 PATIENT & CAREGIVER EDUCATION Exercises After Breast Surgery This information describes how to do arm and shoulder exercises, a breathing exercise, and scar massage after your breast surgery. Starting
PATIENT & CAREGIVER EDUCATION Exercises After Breast Surgery This information describes how to do arm and shoulder exercises, a breathing exercise, and scar massage after your breast surgery. Starting
Total Hip Replacement: Your Guide to Preparation and Recovery
 Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Beyond the Basics ImprovingYour Wound Care Knowledge. Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN
 Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
HOW TO USE NOW ROLLER MASSAGER & LACROSSE BALL - EXERCISES AND TIPS -
 HOW TO USE ROLLER MASSAGER & LACROSSE BALL - EXERCISES AND TIPS - BOOST YOUR RECOVERY NOW Thank you! Hi, it s Jeff again, Co-Founder of Maogani. Our team would like to thank you for giving us the opportunity
HOW TO USE ROLLER MASSAGER & LACROSSE BALL - EXERCISES AND TIPS - BOOST YOUR RECOVERY NOW Thank you! Hi, it s Jeff again, Co-Founder of Maogani. Our team would like to thank you for giving us the opportunity
Advice and exercises for managing knee and hip osteoarthritis October 2018 V1.2 April 2018 April 2021
 Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Lymphedema 101. Andréa Leiserowitz, DPT, CLT. Oncology Physical Therapy;
 Lymphedema 101 Andréa Leiserowitz, DPT, CLT Oncology Physical Therapy; oncologypt@gmail.com Note: this information is the property of Dr. Leiserowitz and should not be copied, distributed, or otherwise
Lymphedema 101 Andréa Leiserowitz, DPT, CLT Oncology Physical Therapy; oncologypt@gmail.com Note: this information is the property of Dr. Leiserowitz and should not be copied, distributed, or otherwise
Dawn Heal RN, MLD/CDT MLD Therapist/Lymphoedema Nurse Specialist The Hampshire Lymphoedema Clinic
 Dawn Heal RN, MLD/CDT MLD Therapist/Lymphoedema Nurse Specialist The Hampshire Lymphoedema Clinic Aims Anatomy & Physiology Signs & Symptoms Preventative Measures Maintenance What is lymphoedema? Lymphoedema
Dawn Heal RN, MLD/CDT MLD Therapist/Lymphoedema Nurse Specialist The Hampshire Lymphoedema Clinic Aims Anatomy & Physiology Signs & Symptoms Preventative Measures Maintenance What is lymphoedema? Lymphoedema
A Patient Guide to Understanding and Managing Chronic Swelling
 A Patient Guide to Understanding and Managing Chronic Swelling WHAT IS CHRONIC SWELLING? As a normal part of your blood circulation, your vascular system leaks fluid into the surrounding tissues. Your
A Patient Guide to Understanding and Managing Chronic Swelling WHAT IS CHRONIC SWELLING? As a normal part of your blood circulation, your vascular system leaks fluid into the surrounding tissues. Your
Fracture Surgery. Post-Operative Care. And. Rehabilitation Protocol
 PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
What is Lymphoedema? Incidence and Prevalence
 What is Lymphoedema? Incidence and Prevalence North of England Cancer Network Lymphoedema Conference - A problem shared 8 March 2013 Dr Andrew Hughes Consultant in Palliative Medicine Outline 1) What is
What is Lymphoedema? Incidence and Prevalence North of England Cancer Network Lymphoedema Conference - A problem shared 8 March 2013 Dr Andrew Hughes Consultant in Palliative Medicine Outline 1) What is
EDUCATION. Peripheral Artery Disease
 EDUCATION Peripheral Artery Disease Peripheral Artery Disease You may have circulation problems that have to do with your blood vessels. You may feel aches, pains, cramps, numbness or muscle fatigue when
EDUCATION Peripheral Artery Disease Peripheral Artery Disease You may have circulation problems that have to do with your blood vessels. You may feel aches, pains, cramps, numbness or muscle fatigue when
Essential intervention No. 3 Oedema control KEY OBJECTIVES. Danger
 Essential intervention No. 3 Oedema control KEY OBJECTIVES To know what causes oedema. To know which kind of oedema needs to be referred for emergency surgery and why. To know the effects of oedema on
Essential intervention No. 3 Oedema control KEY OBJECTIVES To know what causes oedema. To know which kind of oedema needs to be referred for emergency surgery and why. To know the effects of oedema on
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
Dr Paul Thibault. Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology
 Dr Paul Thibault Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology Prescribing Effective Compression and PTS Dr Paul Thibault Phlebologist, Newcastle,
Dr Paul Thibault Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology Prescribing Effective Compression and PTS Dr Paul Thibault Phlebologist, Newcastle,
A Patient Guide to Understanding and Managing Chronic Swelling
 A Patient Guide to Understanding and Managing Chronic Swelling WHAT IS LYMPHEDEMA? Most of us know the circulatory system pumps blood from the heart to the rest of the body. But many people are not aware
A Patient Guide to Understanding and Managing Chronic Swelling WHAT IS LYMPHEDEMA? Most of us know the circulatory system pumps blood from the heart to the rest of the body. But many people are not aware
Curi-Med. Compression bandages. Compression treatments. Product description. Application techniques
 Curi-Med Compression bandages Compression treatments. Product description. Application techniques 2 When the vein system is not working The vein muscle pump helps the blood back to the heart. If the vein
Curi-Med Compression bandages Compression treatments. Product description. Application techniques 2 When the vein system is not working The vein muscle pump helps the blood back to the heart. If the vein
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre.
 Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Diabetes is a serious disease that can develop from lack of insulin production in the body or due to
 Page 1 The Diabetic Foot Definition Diabetes is a serious disease that can develop from lack of insulin production in the body or due to the inability of the body's insulin to perform its normal everyday
Page 1 The Diabetic Foot Definition Diabetes is a serious disease that can develop from lack of insulin production in the body or due to the inability of the body's insulin to perform its normal everyday
Table of Contents. Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings
 Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Solving the Compliance Riddle with Compression Garments Jeffrey D. Lehrman, DPM, FASPS, MAPWCA, CPC
 Solving the Compliance Riddle with Compression Garments Jeffrey D. Lehrman, DPM, FASPS, MAPWCA, CPC Advisor, APMA Coding Committee Advisor, APMA MACRA Task Force Expert Panelist, Codingline Fellow, American
Solving the Compliance Riddle with Compression Garments Jeffrey D. Lehrman, DPM, FASPS, MAPWCA, CPC Advisor, APMA Coding Committee Advisor, APMA MACRA Task Force Expert Panelist, Codingline Fellow, American
Autosana. Compression bandages for phlebology, lymphology and orthopaedic use
 Autosana Compression bandages for phlebology, lymphology and orthopaedic use Autosana Foam, long-stretch compression bandage VERSATILE HIGH NUMBER OF OPEN PORES KIND TO THE SKIN Overview Composition High-grade,
Autosana Compression bandages for phlebology, lymphology and orthopaedic use Autosana Foam, long-stretch compression bandage VERSATILE HIGH NUMBER OF OPEN PORES KIND TO THE SKIN Overview Composition High-grade,
Make sure you have properly fitting running shoes and break these in gradually. Never wear new running shoes for a race or a long run.
 Common Running Injuries We are delighted that you have decided to run in the next Bath Half Marathon and very much hope that you have good running shoes, undertake a regular training programme and don
Common Running Injuries We are delighted that you have decided to run in the next Bath Half Marathon and very much hope that you have good running shoes, undertake a regular training programme and don
Traumatic Instability Understanding your shoulder injury and its repair
 Patient Education Traumatic Instability Understanding your shoulder injury and its repair Your upper arm bone popped out of the socket of your shoulder blade. When this happened, it tore your ligaments
Patient Education Traumatic Instability Understanding your shoulder injury and its repair Your upper arm bone popped out of the socket of your shoulder blade. When this happened, it tore your ligaments
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Below Knee Amputation: Post-op Information
 Below Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Below Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
2015 Product Catalog
 Serving the industry since 1937. Elastic Bandages Lymphedema Care Wound Care Products Compression Braces 2015 Product Catalog 866.203.4760 www.ambraleroy.com Supreme The latex-free Supreme is the ideal
Serving the industry since 1937. Elastic Bandages Lymphedema Care Wound Care Products Compression Braces 2015 Product Catalog 866.203.4760 www.ambraleroy.com Supreme The latex-free Supreme is the ideal
MICROFRACTURE & PASTE GRAFT
 MICROFRACTURE & PASTE GRAFT Overview This is a protocol that provides you with general information and guidelines for the initial stage and progression of rehabilitation according to the listed timeframes.
MICROFRACTURE & PASTE GRAFT Overview This is a protocol that provides you with general information and guidelines for the initial stage and progression of rehabilitation according to the listed timeframes.
