CNA Training Advisor
|
|
|
- Christopher O’Brien’
- 6 years ago
- Views:
Transcription
1 CNA Training Advisor Volume 12 Issue No. 8 AUGUST 2014 Contractures are joint deformities that can be triggered by even temporary immobility. They can severely limit or prevent a sufferer s range of motion (ROM) and require intensive treatment programs; however, residents often remain silent about the pain they cause. This makes a proactive approach to identification and treatment critical. Splinting is one strategy used for preventing and relieving the symptoms of contractures, as well as to help residents recover joint mobility. Stringent splint care, which includes applying, cleaning, and fitting devices properly, is crucial for ensuring the effectiveness of the treatment. As CNAs, you play an essential role in caring for patients with contractures and other joint mobility problems. You can help identify early signs of contractures an important task due to their quick onset and lengthy course of treatment. You are also instrumental in alleviating residents discomfort and facilitating their recovery process through splint maintenance. This issue of CNA Training Advisor will focus on the prevention and treatment of contractures and will specifically address the use of splinting best practices to promote joint mobility. Have a good day of training, and stay tuned for next month s issue of CNA Training Advisor about Autism. Tips for Contracture Prevention Physical movement and activity is a resident s first line of defense against contractures. For those who may be at risk at your facility, give the following restorative care strategies a try: Help residents assume a position of function, which is the body s normal anatomic posture. Use pillows, splints, footboards, or other supportive devices if necessary. Ensure residents exercise joints several times a day. This is much more beneficial than exercising them once a day for an extended period of time. For example, encourage residents to perform five ROM exercises two or three times a day rather than 15 repetitions in one sitting. Quiz answer key 1. b 2. d 3. c 4. b 5. b 6. a 7. a 8. b 9. b 10. d Program Prep Program time Approximately 30 minutes Learning objectives Participants in this activity will be able to: Understand the implications of contractures for long-term care residents and facilities Identify signs of joint mobility problems in residents, particularly the significance of limited ranges of motion (ROM) Appropriate specific strategies for splint care Preparation Review the material on pp. 2 4 Duplicate the CNA Professor insert for participants Gather equipment for participants (e.g., an attendance sheet, pencils, etc.) Method 1. Place a copy of CNA Professor and a pencil at each participant s seat 2. Conduct the questionnaire as a pretest or, if participants reading skills are limited, as an oral posttest 3. Present the program material 4. Review the questionnaire 5. Discuss the answers SEE ALSO hcpro.com/long-term-care
2 CNA Training Advisor August 2014 This document contains privileged, copyrighted information. If you have not purchased it or are not otherwise entitled to it by agreement with HCPro, any use, disclosure, forwarding, copying, or other communication of the contents is prohibited without permission. EDITORIAL ADVISORY BOARD Product Manager Adrienne Trivers Associate Editor Delaney Rebernik STAY CONNECTED Interact with us and the rest of the HCPro community at HCPro.com Become a fan at facebook.com/hcproinc Follow us at twitter.com/hcpro_inc us at customerservice@hcpro.com Questions? Comments? Ideas? Contact Editor Delaney Rebernik at drebernik@ hcpro.com or , Ext Don t miss your next issue If it s been more than six months since you purchased or renewed your subscription to CNA Training Advisor, be sure to check your envelope for your renewal notice or call customer service at Renew your subscription early to lock in the current price. Relocating? Taking a new job? If you re relocating or taking a new job and would like to continue receiving CNA Training Advisor, you are eligible for a free trial subscription. Contact customer serv ice with your moving information at At the time of your call, please share with us the name of your replacement. CNA Training Advisor (ISSN: [print]; [online]) is published monthly by HCPro, a division of BLR, 75 Sylvan Street, Suite A-101, Danvers, MA Subscription rate: $159/year; back issues are available at $15 each. Copyright 2014 HCPro, a division of BLR. All rights reserved. Printed in the USA. Except where specifically encouraged, no part of this publication may be reproduced, in any form or by any means, without prior written consent of HCPro, a division or BLR, or the Copyright Clearance Center at Please notify us immediately if you have received an unauthorized copy. For editorial comments or questions, call or fax For renewal or subscription information, call customer service at , fax , or customerservice@hcpro. com. Visit our website at Occasionally, we make our subscriber list available to selected companies/vendors. If you do not wish to be included on this mailing list, please write to the marketing department at the address above. Opinions expressed are not necessarily those of CTA. Mention of products and serv ices does not constitute en dorse ment. Advice given is general, and readers should consult professional counsel for specific legal, ethical, or clinical questions. Contractures Joint movement is similar to the hinge on a door. Regularly moving the door keeps it working properly, so the door opens and closes easily. When the door isn t moved regularly, the hinge may rust from lack of use, making the door harder to open and close. Similarly, the structures in and around the joints stretch, flex, and move all day long, keeping them functional. If the joint is not moved, it shrinks, becomes stiff, and loses the ability to stretch and move. This causes changes in the fluids that lubricate the inside of the joint. Movement squeezes and pushes the fluids around, lubricating the joint. When a joint stops moving, so does the fluid. Now both the outside and inside of the joint are immobile. Contractures are joint deformities caused by immobility. Each muscle has an opponent muscle that works in the opposite direction. If a muscle or group of muscles is not moved or body alignment is not maintained, the stronger muscles take over. The muscles used for flexion are much stronger than those used for extension. A contracture causes the muscle fibers to pull inward (flexion) and tighten because the resident cannot move them regularly. Connective tissue shortens intersecting points, limiting range of motion (ROM). Joint mobility assessment To know if nursing care is effective, we must know the resident s baseline function. Assessing joint ROM is important. The restorative nurse or therapist will measure the residents ROM on admission and quarterly after that. Some facilities use forms with pictures that show degrees of joint mobility so screeners can compare the resident s joint mobility with that in the picture. If the angle of mobility is abnormal, the resident will be referred to therapy for follow-up joint measurement with an instrument called a goniometer and possible intervention. The importance of early identification When muscles are weak, contractures place them in a position of mechanical disadvantage. Weakness and muscle wasting from lack of use is called atrophy. Residents who have contractures always have a high risk for developing more contractures. Those with paralysis, spasticity, and diseases of the nervous system are also at risk. Research has shown that nursing home residents are eight times more likely to develop contractures than people living in the general community. Contractures can begin to form in as little as four days of immobility. After 10 days, they become significant. After 14 days, they are severe 2 HCPRO.COM 2014 HCPro, a division of BLR. For permission to reproduce part or all of this newsletter for external distribution or use in educational packets, contact the Copyright Clearance Center at copyright.com or
3 August 2014 CNA Training Advisor and deformities are evident. For each day after day four, it will take 10 or more days of therapy to restore the joint to a functional state, but normal ROM may never return. When you do the math, 14 days of contracture will take at least 100 days of treatment for recovery. As you can see, even early contractures need months or years of care. If contractures are identified before the joint is completely immobile, they can usually be reversed. A resident with non-fixed contractures has some ROM in the joint. If a fixed contracture is present, the resident has no movement. Contractures also occlude the capillaries in the joint. The relationship between contractures and pressure ulcers may be as high as 60%. Prevention and treatment Keeping residents active and moving is the best way to prevent contractures. Exercising a joint several times each day is much better than exercising it once for a long time. If a resident is at risk, use restorative care to prevent contractures. This involves putting the resident in a position of function (i.e., the normal anatomic position of the body) as this is how the body works best. Inability to assume a position of function is a red flag that suggests a contracture or nerve, muscle, or tendon injury. Pillows, props, splints, footboards, and supportive devices may also be used to maintain good body alignment. Foot drop, which causes the joint to move away from the body (in extension), is an example of a contracture that can be helped by such devices. In this case, the foot drops until the toes point forward. The feet become fixed in a painful position called plantar flexion, and the contracture will continue to worsen if the joint is not supported. The resident cannot stand, walk, wear shoes, or place the heels flat on the floor. Footboards and other supports are essential for preventing plantar flexion. To help alleviate the symptoms of foot drop, some CNAs make a toe pleat at the foot when making the bed. The toe pleat prevents the linen from pulling the feet downward, which is much more comfortable for the resident and provides extra space for his or her feet. To make a toe pleat, stand at the foot of the bed, and pull the top sheet straight up at the bottom of the mattress, where the feet go. Fanfold the top sheet about 2 4 inches, forming a pleat to make room for the feet. To treat existing contractures, such as foot drop, you will work closely with the therapist and restorative nurse. Contractures resulting from immobility respond best to slow, gentle stretching and massage. If this is necessary, a therapist will supervise care and make recommendations for the restorative program. Contractures caused by trauma or surgery form scar tissue containing thick collagen fibers, but there are no collagen fibers in immobility contractures. Because of this, treatment differs. Contractures with collagen fibers can be surgically released. Splinting A splint is a type of orthotic device that supports or corrects musculoskeletal deformities or abnormalities. Splinting can be a beneficial way to prevent and treat contractures, as well as to alleviate other joint problems. The physical or occupational therapist will order or make a splint to treat the condition and will be highly involved if splinting is ordered. The physician will decide at which times the splint is to be worn. Splints are used to: Improve alignment Prevent skin breakdown Prevent deformities and contractures of the joints Protect the joints during activities Promote healing Support and stabilize joints Position joints in good alignment during rest Relieve muscle strain around weak joints Relieve pain Maintain and improve mobility and ROM Increase ability to use arms and legs functionally Before applying the splint: Monitor for swelling, bruising, and skin irritation Be sure the skin is clean and dry 2014 HCPro, a division of BLR. For permission to reproduce part or all of this newsletter for external distribution or use in educational packets, contact the Copyright Clearance Center at copyright.com or HCPRO.COM 3
4 CNA Training Advisor August 2014 Perform ROM exercises to decrease tone Clean the splint, if needed To clean the splint: Wash with soap and lukewarm water, scrubbing with a small brush, if needed Rub alcohol on the inside to reduce odor Press Velcro straps together during washing Hand wash the Velcro straps and stockinette with lukewarm, soapy water Let it air dry Avoid heat sources such as direct sunlight or a heater Splints are custom-fit. Never interchange splints between residents. A splint that fits correctly: Should look like it is molded to fit the joint Does not dig into or rub against the skin Will keep the joint in good alignment Will be snug, but not tight Will allow you to fit one to two fingers between the splint liner and the skin, and between the strap and the skin Is fastened correctly To care for and monitor assistive devices: Be sure you understand how to apply and care for the device and that you are permitted to apply it. Follow instructions for use of the device. Apply the device according to the resident s plan of care. Keep the device and the skin under the device clean and dry. Keep nails short and clean. If you are not permitted to provide nail care or if the resident is a diabetic, consult the nurse. Check the device for rough edges, cracks, or tears. Pad the device to protect the skin or notify the restorative nurse if the device needs modification or repair. Check the device for breakage, loose or missing parts, deterioration, and wear and tear. If you identify a problem, check with the restorative nurse before proceeding. Pad and protect bony prominences. Inspect the skin for red and open areas before applying the device. If present, notify the nurse. Support the extremity when applying and removing the device. Avoid unnecessary pulling, twisting, or rubbing. Report signs of skin irritation, such as redness, pain, abrasions, or breakdown. Monitor the area for signs of impaired circulation, such as numbness, tingling, cyanosis, color or temperature changes, or edema. Inform the nurse promptly if noted. Check the skin after the device is removed. Notify the nurse if the resident complains of pain or you observe signs of pressure, red or open areas, blisters, edema, cyanosis, irritation, temperature changes, or other problems in the area of the splint. Static splints A static splint is used to stabilize a joint to prevent motion. There are no movable parts. The splint supports and immobilizes the joint during healing and maintains it in a position of function. A static splint also helps relieve pain and prevent and correct deformities and contractures. It prevents weak or injured muscles from being overstretched. A static splint is used on a shortterm basis and only when a dynamic splint would not produce a better outcome. Long-term use will result in joint immobility. Dynamic splints A dynamic splint is the splint of choice when trying to gain joint motion. This splint moves with the resident. A spring or elastic band creates tension, causing the joint to move in the desired direction. The therapist will reposition the splint gradually to get a greater degree of stretch. The wear schedule is ordered by the physician or therapist. Editor s note: This issue of CNA Training Advisor was adapted from The Long-Term Care Nursing Assistant s Guide to Advanced Restorative Skills, written by Barbara Acello, MS, RN. 4 HCPRO.COM 2014 HCPro, a division of BLR. For permission to reproduce part or all of this newsletter for external distribution or use in educational packets, contact the Copyright Clearance Center at copyright.com or
5 AUGUST 2014 Volume 12 Issue No. 8 CNA Professor QUIZ Mark the correct response. Name: 1. When contractures occur, what happens? a. Muscle fibers of the stronger opponent muscle extend outward and loosen b. Muscle fibers of the stronger opponent muscle pull inward and tighten c. The weaker opponent muscle takes over d. The opponent muscle groups work together 2. Why is regular assessment and monitoring of a resident s joint mobility important? a. It allows long-term care providers to track the effectiveness of nursing care and treatment b. If residents angles of joint mobility are abnormal, they will need to be referred to therapy for further tests and possible intervention c. The conditions of residents joints may change rapidly, so consistent monitoring can help providers spot early signs of contractures and quickly intervene d. All of the above 3. Which of the following conditions does NOT put a resident at greater risk for contractures? a. Preexisting contractures b. Paralysis c. Diseases of the glandular system d. Diseases of the nervous system 4. How quickly can contractures form if a resident is immobile? a. In 2 days b. In 4 days c. In 10 days d. In 14 days 5. Exercising a joint several times each day is less effective than exercising it once a day for a longer period of time. a. True b. False Date: 6. Why does treatment differ between contractures resulting from immobility and those caused by trauma or surgery? a. There are no collagen fibers in immobility contractures b. There are no collagen fibers in contractures from surgery or trauma c. Unlike contractures caused by trauma or surgery, those resulting from immobility don t respond well to gentle stretching and massage d. None of the above 7. Which of the following are splints NOT used for? a. Restraining residents b. Preventing skin breakdown c. Maintaining and improving mobility and range of motion d. Increasing ability to use arms and legs functionally 8. Which of the following is a step in the splint cleaning process? a. Washing the device with soap and cold water b. Rubbing alcohol on the inside of the device to reduce odor c. Ensuring Velcro straps are separated while washing d. Placing the device in direct sunlight to dry 9. Interchanging a splint between residents is acceptable as long as you clean the device thoroughly beforehand and the residents are similar in size. a. True b. False 10. What are static splints used for? a. Enabling joint motion b. Stretching weak or injured muscles c. Long-term joint support d. Stabilizing a joint to prevent motion A supplement to CNA Training Advisor
CNA Training Advisor
 CNA Training Advisor Volume 11 Issue No. 8 August 2013 Vaccinations are an important part of being healthy, and they become even more important as we grow older. With age, the body s defenses against disease
CNA Training Advisor Volume 11 Issue No. 8 August 2013 Vaccinations are an important part of being healthy, and they become even more important as we grow older. With age, the body s defenses against disease
CNA Training Advisor
 CNA Training Advisor Volume 12 Issue No. 1 January 2014 Pain management Pain affects many nursing home residents. It often results from injury or sensory stimulation. A variety of factors affect recognition,
CNA Training Advisor Volume 12 Issue No. 1 January 2014 Pain management Pain affects many nursing home residents. It often results from injury or sensory stimulation. A variety of factors affect recognition,
CNA Training Advisor
 CNA Training Advisor Volume 12 Issue No. 2 February 2014 Bowel and bladder management Although the likelihood of incontinence the loss of bladder or bowel control increases as an individual gets older,
CNA Training Advisor Volume 12 Issue No. 2 February 2014 Bowel and bladder management Although the likelihood of incontinence the loss of bladder or bowel control increases as an individual gets older,
CNA Training Advisor
 CNA Training Advisor Volume 14 Issue No. 11 NOVEMBER 2016 Excessive, unrealistic worry about everyday tasks or events, or specific to certain objects or rituals, may indicate an anxiety disorder. Anxiety
CNA Training Advisor Volume 14 Issue No. 11 NOVEMBER 2016 Excessive, unrealistic worry about everyday tasks or events, or specific to certain objects or rituals, may indicate an anxiety disorder. Anxiety
Range of motion and positioning
 Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
ANKLE SPRAINS. Explanation. Causes. Symptoms
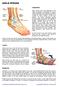 ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
CAST CARE. Helping Broken Bones Heal
 CAST CARE Helping Broken Bones Heal When You Need a Cast Are you injured and in need of a cast? Don t worry, you ll get through it. Wearing a cast will help your injured body part heal. Healing takes time,
CAST CARE Helping Broken Bones Heal When You Need a Cast Are you injured and in need of a cast? Don t worry, you ll get through it. Wearing a cast will help your injured body part heal. Healing takes time,
pull your toes and foot toward your head, you will feel this tissue tighten. WHAT CAUSES PLANTAR
 PLANTAR FASCIITIS AOSSM SPORTS TIPS WHAT IS PLANTAR FASCIITIS? Plantar fasciitis is pain felt at the bottom of the heel. It is usually felt on the first step out of bed in the morning or when walking again
PLANTAR FASCIITIS AOSSM SPORTS TIPS WHAT IS PLANTAR FASCIITIS? Plantar fasciitis is pain felt at the bottom of the heel. It is usually felt on the first step out of bed in the morning or when walking again
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
Lesson Sixteen Flexibility and Muscular Strength
 Lesson Sixteen Flexibility and Muscular Strength Objectives After participating in this lesson students will: Be familiar with why we stretch. Develop a stretching routine to do as a pre-activity before
Lesson Sixteen Flexibility and Muscular Strength Objectives After participating in this lesson students will: Be familiar with why we stretch. Develop a stretching routine to do as a pre-activity before
CUBITAL TUNNEL SYNDROME
 WHAT IS CUBITAL TUNNEL SYNDROME? SYMPTOMS Cubital tunnel syndrome is the second most commonly occurring nerve compression in the upper body It is caused by compression of the ulnar nerve at the elbow The
WHAT IS CUBITAL TUNNEL SYNDROME? SYMPTOMS Cubital tunnel syndrome is the second most commonly occurring nerve compression in the upper body It is caused by compression of the ulnar nerve at the elbow The
Patient and Family Education. SupER Splint. Why does my baby need a splint? What is a SupER splint and how does it work?
 Patient and Family Education SupER Splint Shoulder External Rotation and Forearm Supination Wrap Why does my baby need a splint? Your baby has been diagnosed with brachial plexus palsy. This causes your
Patient and Family Education SupER Splint Shoulder External Rotation and Forearm Supination Wrap Why does my baby need a splint? Your baby has been diagnosed with brachial plexus palsy. This causes your
ANTERIOR ANKLE IMPINGEMENT
 ANTERIOR ANKLE IMPINGEMENT Description Possible Complications Pinching of bone or soft tissue, including scar tissue, at the Frequent recurrence of symptoms, resulting in chronically front of the ankle
ANTERIOR ANKLE IMPINGEMENT Description Possible Complications Pinching of bone or soft tissue, including scar tissue, at the Frequent recurrence of symptoms, resulting in chronically front of the ankle
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Back Safety Healthcare #09-066
 Back Safety Healthcare Version #09-066 I. Introduction A. Scope of training This training program applies to healthcare employees whose job requires them to lift patients or other heavy objects. Lifting
Back Safety Healthcare Version #09-066 I. Introduction A. Scope of training This training program applies to healthcare employees whose job requires them to lift patients or other heavy objects. Lifting
Chapter 23. Assisting With Exercise and Activity
 Chapter 23 Assisting With Exercise and Activity Exercise and Activity Illness, surgery, injury, pain, and aging can limit activity. Inactivity, whether mild or severe: Affects every body system Affects
Chapter 23 Assisting With Exercise and Activity Exercise and Activity Illness, surgery, injury, pain, and aging can limit activity. Inactivity, whether mild or severe: Affects every body system Affects
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
Back Protection. Training Guide
 Back Protection Training Guide Use a Back Support Belt to Prevent Back Injuries Because of the incidious progression of back problems, it is always difficult to determine how a back problem began. If you
Back Protection Training Guide Use a Back Support Belt to Prevent Back Injuries Because of the incidious progression of back problems, it is always difficult to determine how a back problem began. If you
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
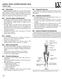 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
General Cast and Splint Care
 General Cast and Splint Care Casts and splints provide limb support after a fracture or surgery. They may also be used to stretch the muscles in a limb. The cast or splint keeps the arm or leg in the proper
General Cast and Splint Care Casts and splints provide limb support after a fracture or surgery. They may also be used to stretch the muscles in a limb. The cast or splint keeps the arm or leg in the proper
PATELLAR DISLOCATION AND SUBLUXATION
 PATELLAR DISLOCATION AND SUBLUXATION Description For jumping (basketball, volleyball) or contact sports, Patellar dislocation and subluxation are injuries to the protect the patella with supportive devices,
PATELLAR DISLOCATION AND SUBLUXATION Description For jumping (basketball, volleyball) or contact sports, Patellar dislocation and subluxation are injuries to the protect the patella with supportive devices,
Sky Ridge Medical Center, Aspen Building Ridgegate Pkwy., Suite 309 Lone Tree, Colorado Office: Fax:
 ANKLE SPRAIN What is the ATFL? The ankle joint is made up of the tibia, fibula (bones in the lower leg) and the talus (bone below the tibia and fibula). Ligaments in the ankle connect bone to bone and
ANKLE SPRAIN What is the ATFL? The ankle joint is made up of the tibia, fibula (bones in the lower leg) and the talus (bone below the tibia and fibula). Ligaments in the ankle connect bone to bone and
Range of motion and positioning
 Range of motion and positioning Teaching guide To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may give each learner
Range of motion and positioning Teaching guide To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may give each learner
ACHILLES TENDON RUPTURE
 ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
Community Caregivers. Effects of Immobility, Transfers and Positioning Test
 Community Caregivers Effects of Immobility, Transfers and Positioning Test Name: Date: For each question, choose the best response or responses. 1. The key effect of immobility is: a. Increased incontinence
Community Caregivers Effects of Immobility, Transfers and Positioning Test Name: Date: For each question, choose the best response or responses. 1. The key effect of immobility is: a. Increased incontinence
CNA Training Advisor. Complementary Therapies and Alternative Medicine. Program Prep
 CNA Training Advisor Volume 25 Issue No. 2 Program Prep Program time Approximately 30 minutes Learning objectives Participants in this activity will be able to: Explain the difference between complementary
CNA Training Advisor Volume 25 Issue No. 2 Program Prep Program time Approximately 30 minutes Learning objectives Participants in this activity will be able to: Explain the difference between complementary
Instructions for Ilizarov and Taylor Spatial Frame Foot Drop Splints and Shoes
 Instructions for Ilizarov and Taylor Spatial Frame Foot Drop Splints and Shoes Irving Building Occupational Therapy, Rehabilitation Services 0161 206 519 G1809190W. Design Services, Salford Royal NHS Foundation
Instructions for Ilizarov and Taylor Spatial Frame Foot Drop Splints and Shoes Irving Building Occupational Therapy, Rehabilitation Services 0161 206 519 G1809190W. Design Services, Salford Royal NHS Foundation
May 2014 Knife-free Relief for Knee Arthritis More than a million surgeries are
 Knife-free Relief for Knee Arthritis More than a million surgeries are performed every year to help people suffering from arthritis of the knee. While such surgery is sometimes the best option, two studies
Knife-free Relief for Knee Arthritis More than a million surgeries are performed every year to help people suffering from arthritis of the knee. While such surgery is sometimes the best option, two studies
Everything. You Should Know. About Your Ankles
 Everything You Should Know About Your Ankles How Your Ankle Works The ankle joint is a hinge type joint that participates in movement and is involved in lower limb stability. There are 2 types of motions
Everything You Should Know About Your Ankles How Your Ankle Works The ankle joint is a hinge type joint that participates in movement and is involved in lower limb stability. There are 2 types of motions
Plantar Fasciitis and Heel Pain
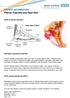 PATIENT INFORMATION Plantar Fasciitis and Heel Pain What is plantar fasciitis? Heel pain and plantar fasciitis Plantar fasciitis causes pain under your heel. It usually goes in time. Treatment may speed
PATIENT INFORMATION Plantar Fasciitis and Heel Pain What is plantar fasciitis? Heel pain and plantar fasciitis Plantar fasciitis causes pain under your heel. It usually goes in time. Treatment may speed
It is also important to make note of your function, as this may be your first indication of improvement.
 Back Pain 1 Management of Back Pain The resolution of pain involves gradually increasing the number of repetitions or resistance of the exercises performed. However, it is important to stay within a range
Back Pain 1 Management of Back Pain The resolution of pain involves gradually increasing the number of repetitions or resistance of the exercises performed. However, it is important to stay within a range
Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life
 Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life. powered by WELLSTAR 360 Session 6: Overview Be Active It s Your Choice! This session focuses on how to become more physically
Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life. powered by WELLSTAR 360 Session 6: Overview Be Active It s Your Choice! This session focuses on how to become more physically
ANKLE SPRAIN, ACUTE. Description
 Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
Osteoporosis Exercise:
 Osteoporosis Exercise: Balance, Posture and Functional Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction You can help improve and maintain your balance, posture
Osteoporosis Exercise: Balance, Posture and Functional Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction You can help improve and maintain your balance, posture
Information for Families. Serial Casting
 Information for Families Serial Casting Serial Casting Casting is a treatment used to provide a sustained stretch to tight muscles. Serial casting is when a series of casts are placed on the limb over
Information for Families Serial Casting Serial Casting Casting is a treatment used to provide a sustained stretch to tight muscles. Serial casting is when a series of casts are placed on the limb over
White Sands Guide for a Healthy Back
 White Sands Guide for a Healthy Back 7157 Curtiss Ave. Sarasota, FL 34231 Phone: (941) 924-9525 www.aquaticsphysicaltherapy.com Home of the Spinal Solutions Program 1 What Causes Back Pain? Since the lower
White Sands Guide for a Healthy Back 7157 Curtiss Ave. Sarasota, FL 34231 Phone: (941) 924-9525 www.aquaticsphysicaltherapy.com Home of the Spinal Solutions Program 1 What Causes Back Pain? Since the lower
This advice and exercises have been selected to help you manage the symptoms of your arthritis
 This advice and exercises have been selected to help you manage the symptoms of your arthritis 1. GENERAL ADVICE Movement is good for your arthritic knee it helps to keep the tissue healthy, increases
This advice and exercises have been selected to help you manage the symptoms of your arthritis 1. GENERAL ADVICE Movement is good for your arthritic knee it helps to keep the tissue healthy, increases
Infosheet. Exercises for myeloma patients. Exercise safety tips
 Infosheet Exercises for myeloma patients As a rough guide, you should aim to do some of the exercises suggested below every few days, (approximately three times a week). They can be done on the same day
Infosheet Exercises for myeloma patients As a rough guide, you should aim to do some of the exercises suggested below every few days, (approximately three times a week). They can be done on the same day
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
Exercises After Breast Surgery
 PATIENT & CAREGIVER EDUCATION Exercises After Breast Surgery This information describes how to do arm and shoulder exercises, a breathing exercise, and scar massage after your breast surgery. Starting
PATIENT & CAREGIVER EDUCATION Exercises After Breast Surgery This information describes how to do arm and shoulder exercises, a breathing exercise, and scar massage after your breast surgery. Starting
EXTENSION KNEE FITTING INSTRUCTIONS. INITIAL SETUP: SET DRIVE ARMS IN CORRECT EXTENSION Drive Arm HOLE SETTINGS (see additional information on page 4)
 KNEE FITTING INSTRUCTIONS It is best to apply the JAS Knee device sitting at the very edge of a seat. Once the device is applied choose any comfortable position (lying or sitting) to carry out your 30-minute
KNEE FITTING INSTRUCTIONS It is best to apply the JAS Knee device sitting at the very edge of a seat. Once the device is applied choose any comfortable position (lying or sitting) to carry out your 30-minute
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
BODY MECHANICS CMHA-CEI
 BODY MECHANICS CMHA-CEI Basics about backs Facts about Back Disorders Maintaining a Healthy Back Common activities Lifting Techniques Stretching Techniques Topics Your back Spine & Vertebrae Discs Nerves
BODY MECHANICS CMHA-CEI Basics about backs Facts about Back Disorders Maintaining a Healthy Back Common activities Lifting Techniques Stretching Techniques Topics Your back Spine & Vertebrae Discs Nerves
Advice and exercises for managing knee and hip osteoarthritis October 2018 V1.2 April 2018 April 2021
 Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Caring For Your Lateral Ankle Middlebury College
 Caring For Your Lateral Ankle Sprain @ Middlebury College ** severe sprains or medial (inner side of ankle) sprains may require a different program Anatomy, Pathology, and Classification of Ankle Sprains
Caring For Your Lateral Ankle Sprain @ Middlebury College ** severe sprains or medial (inner side of ankle) sprains may require a different program Anatomy, Pathology, and Classification of Ankle Sprains
DIABETES AND FOOTCARE
 DIABETES AND FOOTCARE Self-Care and Treatment for Healthy Feet Don t Take Your Feet for Granted Every day, you depend on your feet to keep you moving. But when you have diabetes, your feet need special
DIABETES AND FOOTCARE Self-Care and Treatment for Healthy Feet Don t Take Your Feet for Granted Every day, you depend on your feet to keep you moving. But when you have diabetes, your feet need special
ILIOTIBIAL BAND SYNDROME
 Dr. S. Matthew Hollenbeck, MD Kansas Orthopaedic Center, PA 7550 West Village Circle, Wichita, KS 67205 2450 N Woodlawn, Wichita, KS 67220 Phone: (316) 838-2020 Fax: (316) 838-7574 Description ILIOTIBIAL
Dr. S. Matthew Hollenbeck, MD Kansas Orthopaedic Center, PA 7550 West Village Circle, Wichita, KS 67205 2450 N Woodlawn, Wichita, KS 67220 Phone: (316) 838-2020 Fax: (316) 838-7574 Description ILIOTIBIAL
Commonwealth Health Corporation NEXT
 Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
POSTERIOR TIBIAL TENDON RUPTURE
 POSTERIOR TIBIAL TENDON RUPTURE Description Expected Outcome Posterior tibial tendon rupture is a complete tear of the posterior tibial tendon. This structure is the tendon attachment of leg muscles (posterior
POSTERIOR TIBIAL TENDON RUPTURE Description Expected Outcome Posterior tibial tendon rupture is a complete tear of the posterior tibial tendon. This structure is the tendon attachment of leg muscles (posterior
CARING FOR THE CLIENT ON COMPLETE BEDREST
 CARING FOR THE CLIENT ON COMPLETE BEDREST INTRODUCTION The human body is designed to move. And just as the human body thrives on movement, it suffers when for one reason or another there is enforced immobility.
CARING FOR THE CLIENT ON COMPLETE BEDREST INTRODUCTION The human body is designed to move. And just as the human body thrives on movement, it suffers when for one reason or another there is enforced immobility.
Vancouver. CoastalHealth. Promoting wellness. Ensuring care. Mary Pack Arthritis Program Occupational Therapy
 Vancouver CoastalHealth Promoting wellness. Ensuring care. Mary Pack Arthritis Program Occupational Therapy O.T. IVA-9 01 12005 PATIENT EDUCATION: JOINT PROTECTION AND ENERGY CONSERVATION The goals of
Vancouver CoastalHealth Promoting wellness. Ensuring care. Mary Pack Arthritis Program Occupational Therapy O.T. IVA-9 01 12005 PATIENT EDUCATION: JOINT PROTECTION AND ENERGY CONSERVATION The goals of
Guide to Knee Surgery
 Guide to Knee Surgery Jeffrey B. Witty, M.D. North Oaks Orthopaedic Specialty Center Hammond, LA 70403 Day phone: (985) 230 2663 After hours number: (985) 345-2700 Fax: (985) 230 2665 Website: drjeffreywitty.com
Guide to Knee Surgery Jeffrey B. Witty, M.D. North Oaks Orthopaedic Specialty Center Hammond, LA 70403 Day phone: (985) 230 2663 After hours number: (985) 345-2700 Fax: (985) 230 2665 Website: drjeffreywitty.com
LOW BACK PAIN. what you can do
 LOW BACK PAIN what you can do Back pain Nearly 80 percent of adults will experience back pain at some point in their life. The good news is that back pain will normally go away within four to six weeks
LOW BACK PAIN what you can do Back pain Nearly 80 percent of adults will experience back pain at some point in their life. The good news is that back pain will normally go away within four to six weeks
ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An IPRS Guide to provide you with exercises and advice to ease your condition
 Contents What causes an A/C joint sprain?..................................3 What treatment can I receive?.....................................4 YOUR GUIDE TO ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An
Contents What causes an A/C joint sprain?..................................3 What treatment can I receive?.....................................4 YOUR GUIDE TO ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An
Dr. Abigail R. Hamilton, MD
 ACHILLES TENDINITIS Dr. Abigail R. Hamilton, MD ANATOMY The Achilles tendon is a strong tendon that connects the calf muscles to the heel. When the calf muscles contract, they pull on the Achilles tendon
ACHILLES TENDINITIS Dr. Abigail R. Hamilton, MD ANATOMY The Achilles tendon is a strong tendon that connects the calf muscles to the heel. When the calf muscles contract, they pull on the Achilles tendon
Urgent care. Ankle sprain advice
 Ankle sprain advice What is an ankle sprain? An ankle sprain is an injury to the ligaments of the ankle joint. These are elastic-band-like structures which hold the bones of the ankle joint together and
Ankle sprain advice What is an ankle sprain? An ankle sprain is an injury to the ligaments of the ankle joint. These are elastic-band-like structures which hold the bones of the ankle joint together and
Chapter 9: Exercise Instructions
 RESOURCES RESEARCHERS / MEDICAL HOW TO HELP SPONSORS GEHRIG CONNECTION MEDIA TELETHON MDA.ORG search our site Go MDA/ALS Newsmagazine Current Issue Home> Publications >Everyday Life With ALS: A Practical
RESOURCES RESEARCHERS / MEDICAL HOW TO HELP SPONSORS GEHRIG CONNECTION MEDIA TELETHON MDA.ORG search our site Go MDA/ALS Newsmagazine Current Issue Home> Publications >Everyday Life With ALS: A Practical
Why is positioning important after a stroke?
 POSITIONING Information for Patients and Families Authors*: Erica Kader; Nicol Korner-Bitensky, PhD OT; Elissa Sitcoff, BA BSc; Leila Goulamhoussen, BSc OT; Rabiaa Laroui, BSc OT; Sheila Liu, BSc OT; Anita
POSITIONING Information for Patients and Families Authors*: Erica Kader; Nicol Korner-Bitensky, PhD OT; Elissa Sitcoff, BA BSc; Leila Goulamhoussen, BSc OT; Rabiaa Laroui, BSc OT; Sheila Liu, BSc OT; Anita
Correcting Joint Contractures
 559 Correcting Joint Contractures CHAPTER 59 In this chapter we discuss different aids used for gradually straightening limbs that have joint contractures. Information on contractures, their causes and
559 Correcting Joint Contractures CHAPTER 59 In this chapter we discuss different aids used for gradually straightening limbs that have joint contractures. Information on contractures, their causes and
Bunions. A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus.
 Bunions A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus. Bunions develop slowly. Pressure on the big toe joint
Bunions A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus. Bunions develop slowly. Pressure on the big toe joint
Dr. Michael Gambacorta Myrtle Beach Spine Center
 10 Exercises for Plantar Fasciitis Dr. Michael Gambacorta Myrtle Beach Spine Center 843-236-9090 10 Exercises for Plantar Fasciitis Plantar Fasciitis is the most common form of foot and heel pain due to
10 Exercises for Plantar Fasciitis Dr. Michael Gambacorta Myrtle Beach Spine Center 843-236-9090 10 Exercises for Plantar Fasciitis Plantar Fasciitis is the most common form of foot and heel pain due to
How do you do exercises for patellar tracking disorder?
 To print: Use your web browser's print feature. Close this window after printing. Patellar Tracking Disorder: Exercises Table of Contents Patellar Tracking Disorder: Exercises Patellar Tracking Disorder:
To print: Use your web browser's print feature. Close this window after printing. Patellar Tracking Disorder: Exercises Table of Contents Patellar Tracking Disorder: Exercises Patellar Tracking Disorder:
Plantar fasciitis occurs when the strong band of tissue that supports the arch of your foot becomes irritated and inflamed.
 Plantar Fasciitis and Bone Spurs Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition every year.
Plantar Fasciitis and Bone Spurs Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition every year.
People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy.
 Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Sleep disorders. Program Prep. Tips and tools for CNA training. About your CNA training advisor. Questionnaire answer key.
 June 2009 Vol. 7, No. 6 Sleep disorders As we age, our sleep patterns change. They often become fragmented and leave older individuals vulnerable to cognitive impairment and an increased risk of falls.
June 2009 Vol. 7, No. 6 Sleep disorders As we age, our sleep patterns change. They often become fragmented and leave older individuals vulnerable to cognitive impairment and an increased risk of falls.
Stretch Beyond Your Expectations.
 CLINICIAN INSTRUCTIONS Dynasplint Toe Metatarsophalangeal Extension System Type III Corporate Headquarters: 800.638.6771 toll-free 800.380.3784 fax Canada: 800.668.9139 toll-free 905.851.3494 fax Europe:
CLINICIAN INSTRUCTIONS Dynasplint Toe Metatarsophalangeal Extension System Type III Corporate Headquarters: 800.638.6771 toll-free 800.380.3784 fax Canada: 800.668.9139 toll-free 905.851.3494 fax Europe:
Make sure you have properly fitting running shoes and break these in gradually. Never wear new running shoes for a race or a long run.
 Common Running Injuries We are delighted that you have decided to run in the next Bath Half Marathon and very much hope that you have good running shoes, undertake a regular training programme and don
Common Running Injuries We are delighted that you have decided to run in the next Bath Half Marathon and very much hope that you have good running shoes, undertake a regular training programme and don
Excision of Morton s Neuroma
 Excision of Morton s Neuroma Day Surgery Unit Patient information leaflet This leaflet outlines the risks, general advice and information about foot surgery called an excision of a Morton s Neuroma. If
Excision of Morton s Neuroma Day Surgery Unit Patient information leaflet This leaflet outlines the risks, general advice and information about foot surgery called an excision of a Morton s Neuroma. If
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
The A-Stretch penis enlargement and male enhancement exercise benefits: erect penis length flaccid penis length
 The A-Stretch The A-Stretch exercise pushes the penis up, while pulling it forward. This penis enlargement exercise mainly stretches the upper part of the shaft. It is the opposite exercise of the V-Stretch.
The A-Stretch The A-Stretch exercise pushes the penis up, while pulling it forward. This penis enlargement exercise mainly stretches the upper part of the shaft. It is the opposite exercise of the V-Stretch.
Source: Exercise in Arthritis
 Exercise in Arthritis Regular exercise boosts fitness and helps reverse joint stiffness with RA. Decrease Pain, Increase Energy Exercise more to decrease pain and feel more energetic? Hardly seems possible
Exercise in Arthritis Regular exercise boosts fitness and helps reverse joint stiffness with RA. Decrease Pain, Increase Energy Exercise more to decrease pain and feel more energetic? Hardly seems possible
Ankle Sprain - treatment and exercises. Ankle Sprain. A sprain is a twisting injury to the ankle.
 Ankle Sprain A sprain is a twisting injury to the ankle. Most (80%) are caused by rolling the foot inward. This stretches or tears the ligaments that hold the ankle and foot bones together and can lead
Ankle Sprain A sprain is a twisting injury to the ankle. Most (80%) are caused by rolling the foot inward. This stretches or tears the ligaments that hold the ankle and foot bones together and can lead
POST OPERATIVE ROTATOR CUFF REPAIR PROTOCOL. Home Program
 MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to your surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to your surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
Contents The Ankle Joint What is a sprained ankle? What treatment can I receive? Exercises Introduction Please take note of the following
 Contents The Ankle Joint................................ 3 What is a sprained ankle?.................... 4 MUSCULOSKELETAL YOUR GUIDE TO ANKLE SPRAINS An IPRS Guide to provide you with exercises and advice
Contents The Ankle Joint................................ 3 What is a sprained ankle?.................... 4 MUSCULOSKELETAL YOUR GUIDE TO ANKLE SPRAINS An IPRS Guide to provide you with exercises and advice
GENERAL EXERCISES SHOULDER BMW MANUFACTURING CO. PZ-AM-G-US I July 2017
 GENERAL EXERCISES SHOULDER BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to
GENERAL EXERCISES SHOULDER BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to
DEEP TISSUE FOAM ROLLER MASSAGE GUIDE
 Recover, Recharge, & Renew your body and mind with RE by Empower. Soothe everyday aches & pains; reduce tension & stress; and improve your overall health. DEEP TISSUE FOAM ROLLER MASSAGE GUIDE Three phases
Recover, Recharge, & Renew your body and mind with RE by Empower. Soothe everyday aches & pains; reduce tension & stress; and improve your overall health. DEEP TISSUE FOAM ROLLER MASSAGE GUIDE Three phases
Essential intervention No.1 Health education and self-care KEY OBJECTIVES
 Essential intervention No.1 Health education and self-care Health education bridges the gap between health information and behaviour. The person affected by BU must have the knowledge, skills, resources,
Essential intervention No.1 Health education and self-care Health education bridges the gap between health information and behaviour. The person affected by BU must have the knowledge, skills, resources,
YOUR FREE COMPREHENSIVE GUIDE TO HELP RELIEVE LOWER BACK PAIN NATURALLY
 YOUR FREE COMPREHENSIVE GUIDE TO HELP RELIEVE LOWER BACK PAIN NATURALLY By: helpwithsciatica HTTPS://HELPWITHSCIATICA.COM Table of contents 1 Introduction 2 Exercise: Extensions 3 Exercise: Curl-Ups 4
YOUR FREE COMPREHENSIVE GUIDE TO HELP RELIEVE LOWER BACK PAIN NATURALLY By: helpwithsciatica HTTPS://HELPWITHSCIATICA.COM Table of contents 1 Introduction 2 Exercise: Extensions 3 Exercise: Curl-Ups 4
Below Knee Amputation: Post-op Information
 Below Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Below Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Exercises Following Foot/Toe Injury
 2012 Exercises Following Foot/Toe Injury Exercises following Foot/Toe Injury Foot/Toe Exercises Patient Information You are now allowed to move your foot/toe. You may feel discomfort when doing exercise
2012 Exercises Following Foot/Toe Injury Exercises following Foot/Toe Injury Foot/Toe Exercises Patient Information You are now allowed to move your foot/toe. You may feel discomfort when doing exercise
What Are Bursitis and Tendinitis?
 Shoulder Tendinitis, Bursitis, and Impingement Syndrome What Are Bursitis and Tendinitis? Two types of tendinitis can affect the shoulder. Biceps tendinitis causes pain in the front or side of the shoulder.
Shoulder Tendinitis, Bursitis, and Impingement Syndrome What Are Bursitis and Tendinitis? Two types of tendinitis can affect the shoulder. Biceps tendinitis causes pain in the front or side of the shoulder.
WHAT IS PLANTAR FASCIITIS?
 WHAT IS PLANTAR FASCIITIS? If you're finding when you climb out of bed each morning that your first couple steps cause your foot and heel to hurt, this might be a sign of plantar fasciitis. A common condition
WHAT IS PLANTAR FASCIITIS? If you're finding when you climb out of bed each morning that your first couple steps cause your foot and heel to hurt, this might be a sign of plantar fasciitis. A common condition
ROTATOR CUFF (R/C) LESIONS. Contents What is the Rotator Cuff?...3
 Contents What is the Rotator Cuff?.........................................3 What causes an Rotator Cuff lesion?................................4 YOUR GUIDE TO ROTATOR CUFF (R/C) What treatment can I receive?.....................................5
Contents What is the Rotator Cuff?.........................................3 What causes an Rotator Cuff lesion?................................4 YOUR GUIDE TO ROTATOR CUFF (R/C) What treatment can I receive?.....................................5
Routine For: OT - General Guidelines/Energy Conservation (Caregiver)
 GENERAL GUIDELINES - 9 Tips for Exercise: Body Mechanics for Helper - To protect back, stay as upright as possible and keep head in line with trunk. - Always position yourself as close as possible to the
GENERAL GUIDELINES - 9 Tips for Exercise: Body Mechanics for Helper - To protect back, stay as upright as possible and keep head in line with trunk. - Always position yourself as close as possible to the
Stretching - At the Workstation Why is stretching important?
 Stretching - At the Workstation Why is stretching important? No matter how well a workstation is designed, problems may arise if attention is not paid to the way the work is done. Working at a computer
Stretching - At the Workstation Why is stretching important? No matter how well a workstation is designed, problems may arise if attention is not paid to the way the work is done. Working at a computer
Physiotherapy Services. Physiotherapy Guide. Hip Replacement
 Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
 www.fitnessfirst-usa.com Chest Fly Shoulders, elbows and wrists aligned in same plane with elbows at 90 degrees Feet should be staggered, and body leaning slightly forward for leverage Step far enough
www.fitnessfirst-usa.com Chest Fly Shoulders, elbows and wrists aligned in same plane with elbows at 90 degrees Feet should be staggered, and body leaning slightly forward for leverage Step far enough
Knee Pain Solutions. Assess Your Pain. Make a Plan. Take Action
 Knee Pain Solutions Assess Your Pain Make a Plan Take Action By Jared Evans Certified Strength and Conditioning Specialist Giammalva Fitness Director There are many different causes of knee pain and understanding
Knee Pain Solutions Assess Your Pain Make a Plan Take Action By Jared Evans Certified Strength and Conditioning Specialist Giammalva Fitness Director There are many different causes of knee pain and understanding
BIG TOE FUSION. Patient Information
 Patient Information BIG TOE FUSION This may have been caused by an old injury, previous surgery or a long-standing bunion deformity. Pain at the joint can start to affect your daily activities and even
Patient Information BIG TOE FUSION This may have been caused by an old injury, previous surgery or a long-standing bunion deformity. Pain at the joint can start to affect your daily activities and even
A patient s guide to. Inferior Heel Pain
 A patient s guide to Inferior Heel Pain The Foot & Ankle Unit at the Royal National Orthopaedic Hospital is made up of a multi-disciplinary team. The team consists of four specialist orthopaedic foot and
A patient s guide to Inferior Heel Pain The Foot & Ankle Unit at the Royal National Orthopaedic Hospital is made up of a multi-disciplinary team. The team consists of four specialist orthopaedic foot and
Diabetes - Foot Care
 Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Essential intervention No. 3 Oedema control KEY OBJECTIVES. Danger
 Essential intervention No. 3 Oedema control KEY OBJECTIVES To know what causes oedema. To know which kind of oedema needs to be referred for emergency surgery and why. To know the effects of oedema on
Essential intervention No. 3 Oedema control KEY OBJECTIVES To know what causes oedema. To know which kind of oedema needs to be referred for emergency surgery and why. To know the effects of oedema on
Above Knee Amputation: Post-op Information
 Above Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Above Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron
 Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron Orthopaedic Department Patient information leaflet This patient information booklet is designed to provide you with information
Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron Orthopaedic Department Patient information leaflet This patient information booklet is designed to provide you with information
Ankle Syndesmosis Injuries
 A Patient s Guide to Ankle Syndesmosis Injuries 1436 Exchange Street Middlebury, VT 05753 Phone: 802-388-3194 Fax: 802-388-4881 cvo@champlainvalleyortho.com DISCLAIMER: The information in this booklet
A Patient s Guide to Ankle Syndesmosis Injuries 1436 Exchange Street Middlebury, VT 05753 Phone: 802-388-3194 Fax: 802-388-4881 cvo@champlainvalleyortho.com DISCLAIMER: The information in this booklet
A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) William T. Grant, MD
 A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh,
A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh,
Cheilectomy. Your guide to a successful outcome following surgery. Orthopaedic Department. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Cheilectomy Your guide to a successful outcome following surgery Orthopaedic Department What is Cheilectomy? This is surgery
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Cheilectomy Your guide to a successful outcome following surgery Orthopaedic Department What is Cheilectomy? This is surgery
