6/18/2015. Disclosure. Objectives. Star Ratings. Understand the current climate of healthcare reform
|
|
|
- Solomon Butler
- 5 years ago
- Views:
Transcription
1 Star Ratings John A. Galdo, Pharm.D., BCPS, CGP (Jake) Assistant Professor of Pharmacy Practice Community Practice Residency Director Disclosure I do not have (nor does any immediate family member have) actual or potential conflict of interest, within the last twelve months, a vested interest in or affiliation with any corporate organization offering financial support or grant monies for this continuing education activity, or any affiliation with an organization whose philosophy could potentially bias my presentation. I sit on workgroups for PQA and am a PQA Ambassador Objectives Understand the current climate of healthcare reform Describe the principles of quality metrics for healthcare Apply quality measures to geriatric patients Empower technicians to work at the top of their licensure 1
2 Active Learning In 2011, how much did the US spend on healthcare? 1. $500 billion 2. $1,000 billion 3. $1,500 billion 4. >$2,000 billion Public Health GDP $12.96 Trillion Reached $2.7 Trillion in 2011 For healthcare $8,680 per person $1.2 Trillion is Government $848.9 Billion due to hospital costs $320 Billion on medications Expected $4.78 Trillion (2021) Accessed online 10 September Top Therapeutic Classes by U.S. Spending. IMS data updated February 23, Available from Line%20Market%20Data%20&%20Trends/2011%20Topline%20Market%20Data/Top_Therapy_Classes_by_Sales.pdf Accessed online 9 March Healthcare in the US is Broken Medications do not work in patients that do not take them. C. Everett Koop, M.D., Former U.S. Surgeon General Primary non-adherence in post-mi ~24% 34% discontinue at least 1 medication 12% discontinue all medications Industry average adherence ranges from 40 to 80% Ho P, Bryson C, Rumsfield J. Medication Adherence Its Importance in Cardiovascular Outcomes. Circulation. 2009; 119: Forissier, T., Firlik, K. Estimated Annual Pharmaceutical Revenue Loss Due To Medication Non-Adherence, CAPGEMINI CONSULTING
3 Quality in the Health- System Hospital Quality Alliance (HQA) Joint Commission on Accreditation of Healthcare Organizations aka Joint Commission Centers for Medicare and Medicaid Services (CMS) American Hospital Association And others Established in 2001 Performance data sent to CMS Voluntary Friedberg MW, Landon B. Measuring quality in hospitals in the United States: Core process measures. In: Basow DS, ed. UpToDate. Waltham, MA: UpToDate. Accessed March 25 th, Medicare Modernization Act of 2003 Receipt of hospital s full Medicare payment contingent upon reporting the initial 10-measures to CMS Still voluntary Initial starter set of measures reflected three health conditions Acute Myocardial Infarction Heart Failure Pneumonia Friedberg MW, Landon B. Measuring quality in hospitals in the United States: Core process measures. In: Basow DS, ed. UpToDate. Waltham, MA: UpToDate. Accessed March 25 th,
4 Why the fuss? Quality of care delivered by the US healthcare system is suboptimal Principle of quality improvement is that what is not measured cannot be improved Ergo, performance measurement and reporting is vital Documentation is nothing without engagement to understand and improve Friedberg MW, Landon B. Measuring quality in hospitals in the United States: Core process measures. In: Basow DS, ed. UpToDate. Waltham, MA: UpToDate. Accessed March 25 th, Measures of Quality of Healthcare Structure Characteristics of individual healthcare providers, organizations, or facilities Possession of electronic medical record, percentage of board certified Healthcare Processes Delivery of specific clinical services Percentage of patients status post MI who receive a beta blocker Outcomes Ultimate goal of healthcare Affected by healthcare, but also influenced by patient factors 30-day mortality rate Friedberg MW, Landon B. Measuring quality in hospitals in the United States: Core process measures. In: Basow DS, ed. UpToDate. Waltham, MA: UpToDate. Accessed March 25 th, Donabedian A. Evaluating the quality of medical care. Milbank Q 1966; 44:166. Current Health-System Measures Acute myocardial infarction 8 Measures statin at discharge Heart Failure 3 measures ACE or ARB Pneumonia 1 measure Surgical Care 10 measures Emergency department 7 measures Preventive Care 2 measures Children s asthma care 3 measures Stroke Care 8 measures Blood clot prevention and treatment 6 measures Pregnancy and delivery care 1 measure Outpatient imaging efficiency 6 measures Friedberg MW, Landon B. Measuring quality in hospitals in the United States: Core process measures. In: Basow DS, ed. UpToDate. Waltham, MA: UpToDate. Accessed March 25 th, Updated March
5 COMMUNITY BASED QUALITY MEASURES History of PQA PQA was established in 2006 as a public-private partnership with CMS Consensus-based, non-profit alliance with >110 member organizations Work to improve the quality of medication management and use across healthcare settings PQA s measures being used not just in star ratings Nau D. Medicare Star Ratings for Pharmacy Quality Alliance Quality Forum Lecture Series. Webinar aired live October 31, Pharmacy Quality Alliance The Mission: To improve the quality of medication management and use across healthcare settings with the goal of improving patients health through a collaborative process to develop and implement performance measures and recognize examples of exceptional pharmacy quality Accessed March 25th,
6 PQA Measures Proportion of Days Covered (PDC) 18 years or older, threshold of 80 percent Reported for the following medication classes Beta-blocker Renin Angiotensin System Antagonist Calcium Channel Blocker Statin Biguanide Sulfonylurea Thiazolidinedione Dipeptidyl Peptidase-IV Inhibitor Anti-retroviral* *Threshold must be 90% Accessed March 25, 2014 PQA Measures, II Antipsychotic Use in Children Under 5 Years Old Percentage of children Adherence to Non-Warfarin Oral Anticoagulants Still PDC Diabetes Medication Dosing Percentage of patient dispensed a dose higher than the daily recommendation Accessed March 25, 2014 PQA Measures, III Diabetes: Appropriate Treatment of Hypertension Percentage of patients receiving medication for diabetes and hypertension that are receiving an angiotensin converting enzyme inhibitor (ACEI) and angiotensin II receptor blocker (ARB) Medication Therapy for Persons with Asthma Percentage of patients with asthma dispensed more than 3 canisters of shortacting beta2 agonist over a 90-day period and no controller therapy Accessed March 25,
7 PQA Measures, IV Use of High-Risk Medications (HRM) in the Elderly Percentage of patients 65 years of age or older and received two or more prescription fills for a HRM Drug-Drug Interactions Percentage of patients who received a prescription for a target medication during measurement period and dispensed a concurrent prescription for a precipitant medication Accessed March 25, 2014 PQA Measures, V Cholesterol Management in Coronary Artery Disease Percentage that received at least one prescription for HMG-CoA reductase inhibitor Completion Rate for Comprehensive Medication Review (CMR) Percentage that met eligibility criteria for medication therapy management and received a CMR Antipsychotic Use in Persons with Dementia Patients with dementia Accessed March 25, 2014 Where are the Measures Used? Medicare Part D Plan Ratings Star measures: medication adherence & safety Display measures: safety, adherence and MTM Accreditation programs URAC & CPPA National Business Coalition on Health (NBCH) evalue8 (health plan evaluation) P4P Programs Integrated Healthcare Association of California Inland Empire Health Plan PQA Patient Advisory Panel Introduction 7
8 THE PROVERBIAL STAR RATING Ratings are Everywhere! Quality over Quantity 8
9 What is a star rating? Quality measure of the pharmacy benefits manager (PBM) Rate One to Five stars It s a point system Rating is NOT dependent on PQA measure only 5 of the 14 are PQA/Pharmacy related Accessed March 25th, 2014 Sogol E, Galdo JA. Quality Ratings Impact Community Pharmacy: The CMS STAR Ratings. GPhA Journal. January Measure Name Weighting Category Weight Call Center Foreign Language Interpreter and TTY/TDD Available 2015 Star Rating Customer Service 1.5 Appeals Auto-Forward Customer Service 1.5 Appeals Upheld Customer Service 1.5 Complaints about the Drug Plan Member Complaints, Improvement 1.5 Members Choosing to Leave the Plan Member Complaints, Improvement 1.5 Drug Plan Quality Improvement Member Complaints, Improvement 5 Rating of Drug Plan Member Experience with Plan 1.5 Getting Needed Prescription Drugs Member Experience with Plan 1.5 MPF Price Accuracy Patient Safety and Drug Pricing 1 High Risk Medication Patient Safety and Drug Pricing 3 Diabetes Treatment Patient Safety and Drug Pricing 3 Medication Adherence for Oral Diabetes Patient Safety and Drug Pricing 3 Medication Adherence for Hypertension Patient Safety and Drug Pricing 3 Medication Adherence for Cholesterol Patient Safety and Drug Pricing 3 Accessed March 25th, Coverage/PrescriptionDrugCovGenIn/Downloads/2015_Star_Ratings_U er-call-slides_v2014_08_04.pdf. Accessed April 14, 2015 Pharmacy Specific Measures Measure Name High Risk Medication 3 Diabetes Treatment 3 Medication Adherence for Oral Diabetes Medication Adherence for Hypertension Medication Adherence for Cholesterol Weight 14 (was 18) total measures with different weighting 5 Claims Based measures = Pharmacy Account for over 50% of the total rating Accessed March 25th, 2014 Sogol E, Galdo JA. Quality Ratings Impact Community Pharmacy: The CMS STAR Ratings. GPhA Journal. January
10 Impact of Increased Medication Utilization The Congressional Budget Office estimates that a 1% increase in the number of prescriptions filled by beneficiaries would cause Medicare s spending on medical services to drop 0.2%. If a patient takes their medication as Increase certain pieces of the pie (e.g., drug utilization) and you ultimately decrease the bigger pieces and total spend If a patient takes their medication as prescribed, they don t end up in the hospital! Congressional Budget Office. Report Offsetting Effects of Prescription Drug Use on Medicare s Spending for Medical Services. November 29, Quality Bonus Payment Distribution Adapted from PQA Ambassador Progra THE MEASURES IN COMMUNITY PRACTICE 10
11 High Risk Medications Description Percentage of patients 65 years of age and older who received two or more prescriptions fills for a high-risk medication during the measurement period Definition Measurement Period Period of time over which the prescription medication fill pattern is assessed High-Risk Medication Select prescription drugs recommended to avoid in persons 65 years and older per the American Geriatric Society Beers Criteria Murphy E, Newsome R, Galdo JA. High Risk Medications in the Elderly: A Star M America s Pharmacist. May Accessed March 25, 2014 The Case of GG GG is an 85-year old Hispanic male, who resides at home with his family. The patient s son helps maintain GG s medications, and he is prescribed the following medications: Lisinopril 20mg po qday Metoprolol succinate 100 mg po qday Digoxin 250 mcg po qday Furosemide 20 mg po qday prn based on weight gain of 3-pounds in a day or 5-pounds over two days Zolpidem 10 mg po qhs for sleep Indomethacin 25 mg po TID for pain Atorvastatin 40 mg po qday Spironolactone 50 mg po qday Tiotroprium 18 mcg inhaled qday Diphenhydramine 25 mg po TID prn itching (OTC) Multivitamin po qday What are GG s Medical Conditions? Lisinopril; Metoprolol succinate; Digoxin; Furosemide; Zolpidem; Indomethacin; Atorvastatin; Spironolactone; Tiotroprium; Diphenhydramine; Multivitamin 11
12 What are GG s Medical Conditions? Lisinopril; Metoprolol succinate; Digoxin; Furosemide; Zolpidem; Indomethacin; Atorvastatin; Spironolactone; Tiotroprium; Diphenhydramine; Multivitamin Hypertension, Heart Failure, Chronic Obstructive Pulmonary Disease, Insomnia, Chronic Pain, Vitamin Deficiency, and potentially status-post Non-ST Elevated Acute Coronary Syndrome Star Rating Issues? Digoxin Reason: The maximum dose for digoxin is 125 mcg for geriatric patients Recommendation: Decrease digoxin to 125 mcg, monitor levels to 0.5 to 0.8 ng/ml per the DIG trial Zolpidem Reason: All non-benzodiazepine hypnotics are not recommended Recommendation: Non-pharmacological sleep hygiene Indomethacin Reason: Non-COX-selective NSAIDs should be avoided Recommendation: Acetaminophen, another NSAIDs would not be recommended as the patient is status-post NSTEACS and has a diagnosis of heart failure Diphenhydramine Reason: This is not a star rating red flag as the medication is OTC, however geriatric patients should not be on first-generation antihistamines due to the anticholinergic effects. Diabetes Treatment Description Patients who have received a medication for diabetes as well as any drug that could be used for the treatment of hypertension Definition Medication: Proxy for diagnosis of diabetes and hypertension Percentage of these diabetes-hypertension patients who receive an ACEI or ARB Accessed March 25th, 2014 Sogol E, Galdo JA. Quality Ratings Impact Community Pharmacy: The CMS STAR Ratings. GPhA Journal. January
13 Adherence Description Proportion of Days Covered is the PQArecommended metric for estimation of medication adherence for patients using chronic medications Definition Statins Renin angiotensin system antagonists Four classes of oral diabetes Biguanide Sulfonylurea Thiazolidinedione DPP-IV inhibitor Incretin mimetic Meglitinides Accessed March 25th, 2014 Sogol E, Galdo JA. Quality Ratings Impact Community Pharmacy: The CMS STAR Ratings. GPhA Journal. January What is Adherence? Proportion of Days Covered (PDC) (Gold Standard) Denominator = number of days between the first fill of the medication during the measurement period and the end of the measurement period Numerator = number of days covered by the prescription fills during the denominator period Overlapping days covered assumes that previous supply exhausted Medication Possession Ratio (MPR) Summation of the days supply of medication refills across an interval Numerator and denominator calculated in differing ways Time interval as the time between the first fill and last fill of a medication = Overestimate Adapted from PQA Ambassador Program Goals Change <74% >74% >79% >82% 2014 Diabetes PDC -- Five! 13
14 Goals Change <74% >74% >79% >82% 2015 Diabetes PDC >85% -- Five! Goals Change <74% >74% >79% >82% 2014 Diabetes PDC 77% PDC in 2014 is three stars -- Five! Goals Change <74% >74% >79% >82% 2015 Diabetes PDC >85% 77% PDC in 2015 is TWO stars -- Five! 14
15 Caveat: No primary literature exists to support these methods EMPOWERMENT OF THE PHARMACIST EQuIPP Electronic Quality Improvement Platform for Plans & Pharmacies Developed by Pharmacy Quality Solutions (PQS) and CECity Owned by PQA Accessed March 25th, 2015 Sogol E, Galdo JA. Quality Ratings Impact Community Pharmacy: The CMS STAR Ratings. GPhA Journal. January Newsome R, Murphy E, Galdo JA. The ABCs of Quality. GPhA Journal. February Performance Measures Accessed March 25th, 2015 Sogol E, Galdo JA. Quality Ratings Impact Community Pharmacy: The CMS STAR Ratings. GPhA Journal. January Newsome R, Murphy E, Galdo JA. The ABCs of Quality. GPhA Journal. February
16 Patient Outlier App available in Sept 2014 Adapted from PQA Ambassador Progra You Can Make a Difference Most Medicare Part D plans could move from 3 stars to 4 stars on each PDC measure if every pharmacy in its network helped just one more RASA patient, one more diabetes patient, and one more statin patient become highly adherent. David Nau, PhD, RPh, CPHQ, FAPhA President, Pharmacy Quality Solutions, Inc. Nau D. Medicare Star Ratings for Pharmacy Quality Alliance Quality Forum Lecture Series. Webinar aired live October 31, Star Rating of the PBM CMS PQA Community Pharmacy? PQS EQuIPP 16
17 What Pharmacies can do to Improve Results on Quality Measures! Adherence Programs Medication Synchronization Patient Intervention Packaging Behavioral Interviewing Pill Reminder Tools Medication Therapy Management Safety Alerts Targeting of Patients and Providers Adapted from PQA Ambassador Progra Empowerment of the Technician Adherence Programs Medication Synchronization Patient Intervention Packaging Behavioral Interviewing Pill Reminder Tools Medication Therapy Management Safety Alerts Targeting of Patients and Providers Half Full or Empty?? Better Patient Care, Increased Volume, Higher ROI, High Performance Networks, Alternative Revenue Sources Competition, Licking and Where Sticking, will Network you Exclusions be? 17
18 Department of Health and Human Services: Beyond 2015 Incentives to motivate higher-value care 85% of all Medicare fee-for-service payments tied to quality or value by 2016, and 90% by 2018 Increasing tying payment to value through alternative payment models 30% by 2016 and 50% by 2018 Alternative payment models include accountable care organizations and bundled-payment arrangements Changing the model of care delivered Health information technology reforms, eg transparency Leverage ACA established Patient-Centered Outcomes Research Institute (PCORI) to generate and disseminate data Burwell, S. Setting Value-Based Payment Goals HHS Efforts to Improve U.S. Health Care. N Engl J Med 372:10. March 2, April 6, 2015 METHODOLOGICAL CHANGES FOR CALENDAR YEAR 2016 Proposed Changes Eliminate Pre-determined Thresholds CMS found sponsors have more significant levels on improvement AKA must improve x percent is now gone New Measures MTM CMR Rate Assigned weight of 1, and continue to only be 1 LTC beneficiaries are included in the denominator Hospice at any time during the plan year are excluded 18
19 Proposed Changes, II Changes to measures Adherence and Diabetes Treatment Excluding ESRD patients Diabetes: Treatment of Hypertension PQA no longer endorses CMS will retire this measure in the CY2016 Medication Adherence Use actual death date as disenrollment New Measure! Opioids Measure 1 (Opioid High Dosage): The proportion (XX out of 1,000) of individuals without cancer receiving a daily dosage of opioids greater than 120mg morphine equivalent dose (MED) for 90 consecutive days or longer. Measure 2 (Multiple Prescribers and Multiple Pharmacies): The proportion (XX out of 1,000) of individuals without cancer receiving prescriptions for opioids from four (4) or more prescribers AND four (4) or more pharmacies. Measure 3 (Multi-Provider, High Dosage): The proportion (XX out of 1,000) of individuals without cancer receiving prescriptions for opioids greater than 120mg morphine equivalent dose (MED) for 90 consecutive days or longer, AND who received opioid prescriptions from four (4) or more prescribers AND four (4) or more pharmacies. PQA. Use of Opioids from Multiple Providers or at High Dosage in Persons Without Cancer. May Forecasting 2017 and Beyond Updates to the High Risk Medications Statin Therapy in a patient with diabetes Medication Synchronization Program acceptance and participation: Eligible patients who participate. Patient contact rate: % patients participating who were contacted with appointment call Med Sync Completeness: % patients enrolled with all chronic meds included in their sync Med Sync Continuation: % enrolled with chronic meds synced and still in sync after 6 months 19
20 Stakeholder Advisory Panel SAP A Hospital Admission for ADR Anticoagulants Adherence to Immunosuppressants SAP B MTM Patient Satisfaction Transition of Care in LTC Primary Medication Non-Adherence SAP C Hospital Utilization related to ADEs Concomitant Use of Opioids, Benzodiazepines, and Muscle Relaxants Gap in Therapy Glaucoma SAP D MTM: Specific Drug Problem Resolution Hepatitis C - Outcomes Future of Measures for Pharmacy Pharmacists are capable of impacting quality metrics and improving patient outcomes! Each pharmacy is being evaluated on how their patients are performing on quality measures. Health plans are utilizing preferred networks to get high quality results from their patients (often at a lower costs). Different philosophies from health plans and PBMs pertaining to performance on metrics: Pay-for-Performance (P4P)-additional payments or overall payments based on Star Measure Performance Sticks & Carrots -exclusion from network Adapted from PQA Ambassador Progra Take Home Points There is a two year lag on claims data to the CMS star ratings Perform now, stay in business in the future Pharmacies can account for 50% of a PBMs quality rating (aka, star rating ) Non-dispensing services, like medication synchronization, are the future of community pharmacy 20
21 Star Ratings John A. Galdo, Pharm.D., BCPS, CGP (Jake) Assistant Professor of Pharmacy Practice Community Practice Residency Director 21
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis.
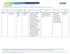 Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DESCRIPTION NUMERATOR DENOMINATOR DM2012-12 Portion of Days Covered
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DESCRIPTION NUMERATOR DENOMINATOR DM2012-12 Portion of Days Covered
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis.
 COMMUNITY PHARMACY V1.1 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. # NAME DESCRIPTION NUMERATOR DENOMINATOR
COMMUNITY PHARMACY V1.1 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. # NAME DESCRIPTION NUMERATOR DENOMINATOR
Medicare Star Ratings and the Shift to Quality- Based Payment Models. David Nau, RPh, PhD, FAPhA PQS President
 Medicare Star Ratings and the Shift to Quality- Based Payment Models David Nau, RPh, PhD, FAPhA PQS President The shift to Value-Driven Healthcare The U.S. health care system is rapidly moving to value-based
Medicare Star Ratings and the Shift to Quality- Based Payment Models David Nau, RPh, PhD, FAPhA PQS President The shift to Value-Driven Healthcare The U.S. health care system is rapidly moving to value-based
Pharmacy Benefit Management
 Benefit Management Measures At A Glance Updated: 10/8/2015 Page 1 of 7 Benefit Management Mandatory Measures (6) Note: Mandatory measures are those measures that are a requirement of accreditation and
Benefit Management Measures At A Glance Updated: 10/8/2015 Page 1 of 7 Benefit Management Mandatory Measures (6) Note: Mandatory measures are those measures that are a requirement of accreditation and
Disease Management. Measures At A Glance
 s At A Glance Updated: 11/2/2017 Page 1 of 7 Cross Cutting Mandatory s (4) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual
s At A Glance Updated: 11/2/2017 Page 1 of 7 Cross Cutting Mandatory s (4) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual
MEASURE STEWARD Pharmacy Quality Alliance (PQA) D ATA SOURCE Enrollment; U R A C DOMAIN Engagement & Experience of Care
 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DM2012-12 DTM2015-01 Portion of Days Covered (PDC) Adherence
MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DM2012-12 DTM2015-01 Portion of Days Covered (PDC) Adherence
Mail Service Pharmacy
 Mail Service s At A Glance Disclaimer: reserves the right to update its measures and measure sets to maintain measure relevancy and to remedy any unintended consequences that may arise during implementation.
Mail Service s At A Glance Disclaimer: reserves the right to update its measures and measure sets to maintain measure relevancy and to remedy any unintended consequences that may arise during implementation.
Drug Therapy Management
 Measures At A Glance Updated: 11/01/2018 2018 Page 1 of 9 Mandatory Measures (10) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to on an annual
Measures At A Glance Updated: 11/01/2018 2018 Page 1 of 9 Mandatory Measures (10) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to on an annual
PATIENT-IMPACT SCORECARD
 UNDERSTANDING THE GSC PATIENT-IMPACT SCORECARD What is the GSC Patient-Impact Scorecard? The GSC Patient-Impact Scorecard shows pharmacy performance scores for GSC patients during the period indicated.
UNDERSTANDING THE GSC PATIENT-IMPACT SCORECARD What is the GSC Patient-Impact Scorecard? The GSC Patient-Impact Scorecard shows pharmacy performance scores for GSC patients during the period indicated.
9/25/15. Pharmacy Quality Measures: Financial Support. Learning Objectives. Speaker Disclosure. Access to Preferred Networks and Clinical Performance
 Pharmacy Quality Measures: Action Steps for Improvement Financial Support Financial support was provided for this activity through an unrestricted grant from Health Mart Systems, Inc. Christine Jacobson
Pharmacy Quality Measures: Action Steps for Improvement Financial Support Financial support was provided for this activity through an unrestricted grant from Health Mart Systems, Inc. Christine Jacobson
2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT
 2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT December 2017 Table of Contents Executive Summary... 1 Pharmacy Benefit Management Organization Characteristics...
2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT December 2017 Table of Contents Executive Summary... 1 Pharmacy Benefit Management Organization Characteristics...
Capital Health Plan CMS Star Ratings Strategies for Improvement
 Capital Health Plan CMS Star Ratings Strategies for Improvement ESTRELLITA REDMON, MD, MBA MEDICAL DIRECTOR The Ultimate Goal Outline Current 5 Star Plans CHP History Importance of Ratings Part C and Part
Capital Health Plan CMS Star Ratings Strategies for Improvement ESTRELLITA REDMON, MD, MBA MEDICAL DIRECTOR The Ultimate Goal Outline Current 5 Star Plans CHP History Importance of Ratings Part C and Part
Disease Management. Measures At A Glance
 s At A Glance Updated: 11/01/2018 URAC 2018 Page 1 of 7 Cross-Cutting Mandatory s (3) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on
s At A Glance Updated: 11/01/2018 URAC 2018 Page 1 of 7 Cross-Cutting Mandatory s (3) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on
116th Annual Convention
 116th Annual Convention Date: Tuesday, October 21, 2014 Time: 8:30 am 10:00 am Location: Austin Convention Center, Room 17AB, Level 4 Title: Activity Type: Speaker: Medicare Part D Star Ratings What They
116th Annual Convention Date: Tuesday, October 21, 2014 Time: 8:30 am 10:00 am Location: Austin Convention Center, Room 17AB, Level 4 Title: Activity Type: Speaker: Medicare Part D Star Ratings What They
USING MTM TO IMPROVE STAR RATINGS : CASE STUDIES
 USING MTM TO IMPROVE STAR RATINGS : CASE STUDIES Sept 13, 2015 Amanda Applegate, PharmD, BCACP Disclosures Nothing to disclose Learning Objectives Describe how MTM can improve star ratings Discuss strategies
USING MTM TO IMPROVE STAR RATINGS : CASE STUDIES Sept 13, 2015 Amanda Applegate, PharmD, BCACP Disclosures Nothing to disclose Learning Objectives Describe how MTM can improve star ratings Discuss strategies
PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter
 Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star
 Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star HEALTH ALLIANCE PLAN Presented by Vanita K. Pindolia, Pharm.D. VP, Ambulatory Clinical Pharmacy Programs_PCM Medicare 5-Star Rating
Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star HEALTH ALLIANCE PLAN Presented by Vanita K. Pindolia, Pharm.D. VP, Ambulatory Clinical Pharmacy Programs_PCM Medicare 5-Star Rating
Condition/Procedure Measure Compliance Criteria Reference Attribution Method
 Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
STARS SYSTEM 5 CATEGORIES
 TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
Quality Metrics & Immunizations
 Optimizing Patients' Health by Improving the Quality of Medication Use Quality Metrics & Immunizations Hannah Fish, PharmD, CPHQ Discussion Objectives 1. Describe the types and distribution of quality
Optimizing Patients' Health by Improving the Quality of Medication Use Quality Metrics & Immunizations Hannah Fish, PharmD, CPHQ Discussion Objectives 1. Describe the types and distribution of quality
Tools for Targeting High Risk Patients in Your Practice. Statement of Disclosure
 Tools for Targeting High Risk Patients in Your Practice Joseph Vande Griend, PharmD, BCPS, CGP Assistant Professor, University of Colorado Departments of Clinical Pharmacy and Family Medicine Skaggs School
Tools for Targeting High Risk Patients in Your Practice Joseph Vande Griend, PharmD, BCPS, CGP Assistant Professor, University of Colorado Departments of Clinical Pharmacy and Family Medicine Skaggs School
Telligen Quality Innovation Network Quality Improvement Organization
 Telligen Quality Innovation Network Quality Improvement Organization PQA Patient Safety Measures for Inappropriate Prescription Opioid Use August 29, 2017 Optimizing Patients' Health by Improving the Quality
Telligen Quality Innovation Network Quality Improvement Organization PQA Patient Safety Measures for Inappropriate Prescription Opioid Use August 29, 2017 Optimizing Patients' Health by Improving the Quality
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare
 Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Assistant Clinical
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Assistant Clinical
Patient-Centered Measurement: Innovation Challenge Series
 Patient-Centered Measurement: Innovation Challenge Series Learning Collaborative 2018 Webinar Thursday, March 1, 2018 1 Hala Durrah, MTA Patient Family Engagement Consultant, Speaker & Advocate 3 2017-18
Patient-Centered Measurement: Innovation Challenge Series Learning Collaborative 2018 Webinar Thursday, March 1, 2018 1 Hala Durrah, MTA Patient Family Engagement Consultant, Speaker & Advocate 3 2017-18
3/17/2017. Innovative Opportunities for Pharmacists in the Evolving World of Healthcare. Elderly represent about of our emergency medical services:
 Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Addolorata
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Addolorata
Rethink. Adherence. David D. Pope, PharmD, CDE Editor-in-Chief, CreativePharmacist.com Brands
 Rethink. Adherence. David D. Pope, PharmD, CDE Editor-in-Chief, CreativePharmacist.com Brands Objectives Identify patient barriers to medication adherence. Describe the clinical and economic impact of
Rethink. Adherence. David D. Pope, PharmD, CDE Editor-in-Chief, CreativePharmacist.com Brands Objectives Identify patient barriers to medication adherence. Describe the clinical and economic impact of
Legislative & Regulatory Update Brad Young, RxPlus Government Affairs
 Legislative & Regulatory Update 2018 Brad Young, RxPlus Government Affairs Disclosures Brad Young reports no actual or potential conflicts of interest associated with this presentation. 2 Learning Objectives
Legislative & Regulatory Update 2018 Brad Young, RxPlus Government Affairs Disclosures Brad Young reports no actual or potential conflicts of interest associated with this presentation. 2 Learning Objectives
The Pharmacy Quality Alliance Optimizing Health by Advancing the Quality of Medication Use
 Optimizing Health by Improving the Quality of Medication Use Adult Immunization Measure Development Update The Optimizing Health by Advancing the Quality of Medication Use Lisa Hines, PharmD Senior Director,
Optimizing Health by Improving the Quality of Medication Use Adult Immunization Measure Development Update The Optimizing Health by Advancing the Quality of Medication Use Lisa Hines, PharmD Senior Director,
HEADED FOR HEDIS AND REACHING FOR THE STARS: THE PHARMACIST S ROLE IN POPULATION HEALTH MANAGEMENT
 HEADED FOR HEDIS AND REACHING FOR THE STARS: THE PHARMACIST S ROLE IN POPULATION HEALTH MANAGEMENT Desola Davis, PharmD, BCPS, BCACP Dalia Zall, PharmD 1 Copyright 2017 Kaiser Foundation Health Plan, Inc.
HEADED FOR HEDIS AND REACHING FOR THE STARS: THE PHARMACIST S ROLE IN POPULATION HEALTH MANAGEMENT Desola Davis, PharmD, BCPS, BCACP Dalia Zall, PharmD 1 Copyright 2017 Kaiser Foundation Health Plan, Inc.
Alabama Medicaid Pharmacy Override
 Alabama Medicaid Pharmacy Override Therapeutic Duplication, Early Refill, Maximum Unit, Prescription Limit Switchover, Dispense as Written, Accumulation Edit, Maintenance Supply Opt Out, and Maximum Cost
Alabama Medicaid Pharmacy Override Therapeutic Duplication, Early Refill, Maximum Unit, Prescription Limit Switchover, Dispense as Written, Accumulation Edit, Maintenance Supply Opt Out, and Maximum Cost
Drug Utilization Review & Cost Reduction Strategies. Esther Liu, PharmD, MSIA, CGP Clinical Pharmacist Outcome Resources
 Drug Utilization Review & Cost Reduction Strategies Esther Liu, PharmD, MSIA, CGP Clinical Pharmacist Outcome Resources Goals and Objectives Define Drug Utilization Reviews Interpret various performance
Drug Utilization Review & Cost Reduction Strategies Esther Liu, PharmD, MSIA, CGP Clinical Pharmacist Outcome Resources Goals and Objectives Define Drug Utilization Reviews Interpret various performance
PQA Measure Development Update: June 2017
 PQA Measure Development Update: June 2017 The Measure Development Teams and Task Forces have been meeting monthly via webinar, and the Stakeholder Advisory Panels had their first meetings in March. Additionally,
PQA Measure Development Update: June 2017 The Measure Development Teams and Task Forces have been meeting monthly via webinar, and the Stakeholder Advisory Panels had their first meetings in March. Additionally,
Disclosure. Learning Objectives 6/4/2014. Medication Adherence: Challenges and Opportunities
 Medication Adherence: Challenges and Opportunities Jessica W. Skelley, Pharm D., BCACP Assistant Professor of Pharmacy Practice McWhorter School of Pharmacy, Samford University jmwhalen@samford.edu Disclosure
Medication Adherence: Challenges and Opportunities Jessica W. Skelley, Pharm D., BCACP Assistant Professor of Pharmacy Practice McWhorter School of Pharmacy, Samford University jmwhalen@samford.edu Disclosure
Pharmacy Technician Course
 Pharmacy Technician Course VERSION HISTORY SECTION 1: History and Scope of the Pharmacy Technician Scope of the Pharmacy Technician Section 1 Quiz Check Your Knowledge Section 1 Quiz Answers SECTION 2:
Pharmacy Technician Course VERSION HISTORY SECTION 1: History and Scope of the Pharmacy Technician Scope of the Pharmacy Technician Section 1 Quiz Check Your Knowledge Section 1 Quiz Answers SECTION 2:
From Channeling to GRACE: Approaching Reduction in Readmissions and Adverse Drug Events
 From Channeling to GRACE: Approaching Reduction in Readmissions and Adverse Drug Events Michael Wasserman, MD, CMD Executive Director, Care Continuum Health Services Advisory Group September 15, 2016 Quality
From Channeling to GRACE: Approaching Reduction in Readmissions and Adverse Drug Events Michael Wasserman, MD, CMD Executive Director, Care Continuum Health Services Advisory Group September 15, 2016 Quality
Medication Adherence
 Medication Adherence 1-30-15 Presented by: Alexander Luong, Pharm.D. Candidate 2015 University of the Pacific Preceptor: Dr. Craig Stern Pharm.D., MBA President Pro Pharma Pharmaceutical Consultants, Inc
Medication Adherence 1-30-15 Presented by: Alexander Luong, Pharm.D. Candidate 2015 University of the Pacific Preceptor: Dr. Craig Stern Pharm.D., MBA President Pro Pharma Pharmaceutical Consultants, Inc
PHARMACY QUALITY MEASURES: Improving Performance Playbook
 PHARMACY QUALITY MEASURES: Improving Performance Playbook Table of Contents How to Use This Resource 4 Why Performance Measures Matter to Your Pharmacy 5 The Medicare Star Ratings System 5 For More Information
PHARMACY QUALITY MEASURES: Improving Performance Playbook Table of Contents How to Use This Resource 4 Why Performance Measures Matter to Your Pharmacy 5 The Medicare Star Ratings System 5 For More Information
Understanding Your Patient Care Opportunity Report (PCOR)
 Understanding Your Patient Care Opportunity Report (PCOR) Use your January/February 208 PCOR to help improve performance on Medicare Part D Clinical Star Ratings measures. Your January/February 208 Patient
Understanding Your Patient Care Opportunity Report (PCOR) Use your January/February 208 PCOR to help improve performance on Medicare Part D Clinical Star Ratings measures. Your January/February 208 Patient
HEART FAILURE QUALITY IMPROVEMENT. American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement
 HEART FAILURE QUALITY IMPROVEMENT American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement 1 DISCLOSURES NONE 2 3 WHY IS THIS IMPORTANT? WHY? Heart Failure Currently, an
HEART FAILURE QUALITY IMPROVEMENT American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement 1 DISCLOSURES NONE 2 3 WHY IS THIS IMPORTANT? WHY? Heart Failure Currently, an
2018 MIPS Reporting Family Medicine
 2018 MIPS Reporting Family Medicine Quality Reporting Requirements: Report on 6 quality measures or a specialty measure set Include at least ONE outcome or high-priority measure Report on patients of All-Payers
2018 MIPS Reporting Family Medicine Quality Reporting Requirements: Report on 6 quality measures or a specialty measure set Include at least ONE outcome or high-priority measure Report on patients of All-Payers
16 th Annual IHA Stakeholders Meeting Session 2C
 16 th Annual IHA Stakeholders Meeting Session 2C September 19, 2017 Hilton Los Angeles Airport Thank you to our Content Partner: Medication Adherence AppleCare Pharmacy Programs Confidential and proprietary.
16 th Annual IHA Stakeholders Meeting Session 2C September 19, 2017 Hilton Los Angeles Airport Thank you to our Content Partner: Medication Adherence AppleCare Pharmacy Programs Confidential and proprietary.
How Independent Pharmacies Can Use Medicare Star Ratings to Improve Their Businesses
 How Independent Pharmacies Can Use Medicare Star Ratings to Improve Their Businesses We are in a new, changing healthcare environment that is affecting every stakeholder in the market hospitals, doctors,
How Independent Pharmacies Can Use Medicare Star Ratings to Improve Their Businesses We are in a new, changing healthcare environment that is affecting every stakeholder in the market hospitals, doctors,
Amy Larrick Chavez-Valdez, Director, Medicare Drug Benefit and C & D Data Group
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, Maryland 21244-1850 CENTER FOR MEDICARE TO: FROM: SUBJECT: All Part D Sponsors Amy Larrick
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, Maryland 21244-1850 CENTER FOR MEDICARE TO: FROM: SUBJECT: All Part D Sponsors Amy Larrick
2012 Chronic Respiratory. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2012 Chronic Respiratory Program Evaluation Our mission is to improve the health and quality of life of our members 2012 Chronic Respiratory Program Evaluation Program Title: Chronic Respiratory Program
2012 Chronic Respiratory Program Evaluation Our mission is to improve the health and quality of life of our members 2012 Chronic Respiratory Program Evaluation Program Title: Chronic Respiratory Program
Pharmacy Partnership to Improve Patient Outcomes
 Pharmacy Partnership to Improve Patient Outcomes Minnesota Rural Health Conference Session 2B Ryan M. Harden, MD MS Kendra Metz, Pharm D Sarah Nelson, MD June 25, 2018 Involved Partners Involved Partners
Pharmacy Partnership to Improve Patient Outcomes Minnesota Rural Health Conference Session 2B Ryan M. Harden, MD MS Kendra Metz, Pharm D Sarah Nelson, MD June 25, 2018 Involved Partners Involved Partners
Bob Davis, PharmD, FAPhA Professor and Chair, KPIC South Carolina Primary Health Care Association September 19, 2015
 Bob Davis, PharmD, FAPhA Professor and Chair, KPIC davisb@kennedycenter.sc.edu South Carolina Primary Health Care Association September 19, 2015 Myrtle Beach, SC Kennedy Pharmacy Innovation Center Foundation
Bob Davis, PharmD, FAPhA Professor and Chair, KPIC davisb@kennedycenter.sc.edu South Carolina Primary Health Care Association September 19, 2015 Myrtle Beach, SC Kennedy Pharmacy Innovation Center Foundation
Opioid Safety: Prescribing Guidelines, Quality Measures and Care Coordination Best-Practices
 Opioid Safety: Prescribing Guidelines, Quality Measures and Care Coordination Best-Practices August 25, 2017 Presented by Michael Crooks, PharmD. Medication Safety and Care Coordination Task Lead 8/28/2017
Opioid Safety: Prescribing Guidelines, Quality Measures and Care Coordination Best-Practices August 25, 2017 Presented by Michael Crooks, PharmD. Medication Safety and Care Coordination Task Lead 8/28/2017
September 22, National Association of Attorneys General 1850 M Street, NW, 12 th Floor Washington, DC Prescription Opioid Epidemic
 National Association of Attorneys General 1850 M Street, NW, 12 th Floor Washington, DC 20036 RE: Prescription Opioid Epidemic On behalf of America s Health Insurance Plans (AHIP), thank you for your leadership
National Association of Attorneys General 1850 M Street, NW, 12 th Floor Washington, DC 20036 RE: Prescription Opioid Epidemic On behalf of America s Health Insurance Plans (AHIP), thank you for your leadership
Statement Of. The National Association of Chain Drug Stores. For. U.S. Senate Committee on Finance. Hearing on:
 Statement Of The National Association of Chain Drug Stores For U.S. Senate Committee on Finance Hearing on: 10:00 a.m. National Association of Chain Drug Stores (NACDS) 1776 Wilson Blvd., Suite 200 Arlington,
Statement Of The National Association of Chain Drug Stores For U.S. Senate Committee on Finance Hearing on: 10:00 a.m. National Association of Chain Drug Stores (NACDS) 1776 Wilson Blvd., Suite 200 Arlington,
Reduction of High Risk Medications Using A Quality Initiative Perspective
 Reduction of High Risk Medications Using A Quality Initiative Perspective Richard Mueller PharmD, MBA, MS, Director of Pharmacy Dianne Hempel BSN, RN Quality Improvement Coordinator Objectives Learn what
Reduction of High Risk Medications Using A Quality Initiative Perspective Richard Mueller PharmD, MBA, MS, Director of Pharmacy Dianne Hempel BSN, RN Quality Improvement Coordinator Objectives Learn what
Submitted to the House Energy and Commerce Committee. Federal Efforts to Combat the Opioid Crisis
 STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
The University of Mississippi School of Pharmacy
 LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights
 Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights Align. Measure. Perform. (AMP) Programs Launched in 2003, VBP4P is a statewide performance improvement program and one of
Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights Align. Measure. Perform. (AMP) Programs Launched in 2003, VBP4P is a statewide performance improvement program and one of
Thank you for your continued engagement and member support of the Pharmacy Quality Alliance.
 Optimizing Health by Advancing the Quality of Medication Use November 14, 2017 FROM: Jacqueline Green, Chief Operating Officer, Pharmacy Quality Alliance SUBJECT: PQA Headlines & Highlights as we head
Optimizing Health by Advancing the Quality of Medication Use November 14, 2017 FROM: Jacqueline Green, Chief Operating Officer, Pharmacy Quality Alliance SUBJECT: PQA Headlines & Highlights as we head
Cardiology Pharmacist. Melanie Madorsky, PharmD, BCPS TSHP Annual Meeting April 7, 2018
 Cardiology Pharmacist Melanie Madorsky, PharmD, BCPS TSHP Annual Meeting April 7, 2018 Melanie.Madorsky@memorialhermann.org Objectives Explain the daily responsibilities of the Cardiology Pharmacist Identify
Cardiology Pharmacist Melanie Madorsky, PharmD, BCPS TSHP Annual Meeting April 7, 2018 Melanie.Madorsky@memorialhermann.org Objectives Explain the daily responsibilities of the Cardiology Pharmacist Identify
QIOs: Partners for Quality Improvement Under the Medicare Drug Benefit
 QIOs: Partners for Quality Improvement Under the Medicare Drug Benefit Presentation to The 2 nd Annual National Medicare Prescription Drug Congress David Schulke Executive Vice President The American Health
QIOs: Partners for Quality Improvement Under the Medicare Drug Benefit Presentation to The 2 nd Annual National Medicare Prescription Drug Congress David Schulke Executive Vice President The American Health
Achieving Quality and Value in Chronic Care Management
 The Burden of Chronic Disease One of the greatest burdens on the US healthcare system is the rapidly growing rate of chronic disease. These statistics illustrate the scope of the problem: Nearly half of
The Burden of Chronic Disease One of the greatest burdens on the US healthcare system is the rapidly growing rate of chronic disease. These statistics illustrate the scope of the problem: Nearly half of
Measuring and Improving Quality in Accountable Care Organizations
 Measuring and Improving Quality in Accountable Care Organizations Joachim Roski, PhD MPH Fellow, Economic Studies Managing Director, High Value Healthcare Initiative Overview ACOs and health care reform
Measuring and Improving Quality in Accountable Care Organizations Joachim Roski, PhD MPH Fellow, Economic Studies Managing Director, High Value Healthcare Initiative Overview ACOs and health care reform
Panel Discussion: Orals Adherence & Challenges Friday, April 28 th, 2017
 Panel Discussion: Orals Adherence & Challenges Friday, April 28 th, 2017 1 2017 Community Oncology Alliance Panel Discussion: Orals Adherence & Challenges Ray Bailey, RPh, Director of Pharmacy Florida
Panel Discussion: Orals Adherence & Challenges Friday, April 28 th, 2017 1 2017 Community Oncology Alliance Panel Discussion: Orals Adherence & Challenges Ray Bailey, RPh, Director of Pharmacy Florida
PCMH 2018 Enrollment and Update August 25, 2017
 PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
January 16, Dear Administrator Verma:
 Ms. Seema Verma Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services Attention: CMMI New Direction P.O. Box 8011 Baltimore, MD 21244-1850 Re: (CMS-4182-P) Medicare
Ms. Seema Verma Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services Attention: CMMI New Direction P.O. Box 8011 Baltimore, MD 21244-1850 Re: (CMS-4182-P) Medicare
Provider Perspective of Quality Measurement
 Provider Perspective of Quality Measurement The American Medical Group Association supports its members in enhancing population health and care for patients through integrated systems of care Improve
Provider Perspective of Quality Measurement The American Medical Group Association supports its members in enhancing population health and care for patients through integrated systems of care Improve
Deconstructing Polypharmacy. Alan B. Douglass, M.D. Director
 Deconstructing Polypharmacy Alan B. Douglass, M.D. Director Recognize this patient? Mrs. Brown- 82 years young Active Medical Problems Hypertension Hyperlipidemia Type 2 Diabetes Peripheral edema Osteoarthritis
Deconstructing Polypharmacy Alan B. Douglass, M.D. Director Recognize this patient? Mrs. Brown- 82 years young Active Medical Problems Hypertension Hyperlipidemia Type 2 Diabetes Peripheral edema Osteoarthritis
Value Based Pay for Performance Results & Highlights Measurement Year September 2017
 Value Based Pay for Performance Results & Highlights Measurement Year 2016 September 2017 IHA s Value Based Pay for Performance (VBP4P) ~200 Medical Groups & IPAs 9 Health Plans Common Measurement Public
Value Based Pay for Performance Results & Highlights Measurement Year 2016 September 2017 IHA s Value Based Pay for Performance (VBP4P) ~200 Medical Groups & IPAs 9 Health Plans Common Measurement Public
COMMON DRUG RELATED PROBLEMS SEEN IN PACE AND MECHANISMS TO MITIGATE RISK
 COMMON DRUG RELATED PROBLEMS SEEN IN PACE AND MECHANISMS TO MITIGATE RISK Robert L Alesiani, PharmD, CGP Chief Pharmacotherapy Officer CareKinesis, Inc. (a Tabula Rasa Healthcare Company) 2 3 4 5 Pharmacogenomics
COMMON DRUG RELATED PROBLEMS SEEN IN PACE AND MECHANISMS TO MITIGATE RISK Robert L Alesiani, PharmD, CGP Chief Pharmacotherapy Officer CareKinesis, Inc. (a Tabula Rasa Healthcare Company) 2 3 4 5 Pharmacogenomics
This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings.
 2019 HEDIS AT-A-GLANCE GUIDE STAR MEASURES This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. At WellCare, we value everything
2019 HEDIS AT-A-GLANCE GUIDE STAR MEASURES This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. At WellCare, we value everything
Star Measures At-A-Glance Guide
 Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At Easy Choice, we
Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At Easy Choice, we
Member-centered cancer care In Georgia
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Member-centered cancer care In Georgia Ira Klein, MD, MBA, FACP GASCO Annual Meeting September 5, 2015 > One
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Member-centered cancer care In Georgia Ira Klein, MD, MBA, FACP GASCO Annual Meeting September 5, 2015 > One
Modernized Reference Drug Program
 Modernized Reference Drug Program Monitoring Report For the period ending May 31, 2017 Issued: November 2017 Published by: Pharmaceutical Services Division and Health Sector Information, Analysis and Reporting
Modernized Reference Drug Program Monitoring Report For the period ending May 31, 2017 Issued: November 2017 Published by: Pharmaceutical Services Division and Health Sector Information, Analysis and Reporting
HEALTHCARE REFORM. September 2012
 HEALTHCARE REFORM Accountable Care Organizations: ACOs 101 September 2012 The enclosed slides are intended to provide you with a general overview of accountable care organizations (ACOs), created within
HEALTHCARE REFORM Accountable Care Organizations: ACOs 101 September 2012 The enclosed slides are intended to provide you with a general overview of accountable care organizations (ACOs), created within
Star Measures At-A-Glance Guide
 Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At WellCare, we value
Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At WellCare, we value
Your Partnership in Health Report: Chronic Conditions ABC Company and Kaiser Permanente
 Your Partnership in Health Report: s ABC Company and Kaiser Permanente Measurement Period: JUL-01-2012 through JUN-30-2013 Report Date: DEC-31-2013 Commercial All Members Partnership in Health (PIH) reports:
Your Partnership in Health Report: s ABC Company and Kaiser Permanente Measurement Period: JUL-01-2012 through JUN-30-2013 Report Date: DEC-31-2013 Commercial All Members Partnership in Health (PIH) reports:
Across The Chasm: The Transition From Volume To Value
 Across The Chasm: The Transition From Volume To Value Joseph Bisordi, MD, Executive Vice President & CMO Ochsner Health System Our Mission is to Serve, Heal, Lead, Educate, and Innovate $1.6 Revenue ($B)
Across The Chasm: The Transition From Volume To Value Joseph Bisordi, MD, Executive Vice President & CMO Ochsner Health System Our Mission is to Serve, Heal, Lead, Educate, and Innovate $1.6 Revenue ($B)
ADVANCED PRACTICE PROVIDER ROUNDS:
 ADVANCED PRACTICE PROVIDER ROUNDS: UTILIZING CMS CHRONIC CARE MANAGEMENT FOR DIFFICULT CASES APARNA GUPTA, MSN, MBA, RN Senior CRNP, Benedum Geriatric Center, UPMC Chair, UPMC APP Preceptor Academy Director,
ADVANCED PRACTICE PROVIDER ROUNDS: UTILIZING CMS CHRONIC CARE MANAGEMENT FOR DIFFICULT CASES APARNA GUPTA, MSN, MBA, RN Senior CRNP, Benedum Geriatric Center, UPMC Chair, UPMC APP Preceptor Academy Director,
Improving Quality of Care for Medicare Patients: Accountable Care Organizations
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
QUALITY IMPROVEMENT Section 9
 Quality Improvement Program The Plan s Quality Improvement Program serves to improve the health of its members through emphasis on health maintenance, education, diagnostic testing and treatment. The Quality
Quality Improvement Program The Plan s Quality Improvement Program serves to improve the health of its members through emphasis on health maintenance, education, diagnostic testing and treatment. The Quality
Deprescribing Unnecessary Medications: A Four-Part Process
 Deprescribing Unnecessary Medications: A Four-Part Process Scott Endsley, MD Fam Pract Manag. 2018;25(3):28-32. Abstract and Introduction Introduction www.medscape.com Ms. Horatio is a 76-year-old patient
Deprescribing Unnecessary Medications: A Four-Part Process Scott Endsley, MD Fam Pract Manag. 2018;25(3):28-32. Abstract and Introduction Introduction www.medscape.com Ms. Horatio is a 76-year-old patient
Proposed Changes to Existing Measure for HEDIS : Use of Opioids at High Dosage (UOD)
 Proposed Changes to Existing Measure for HEDIS 1 2020: Use of Opioids at High Dosage (UOD) NCQA seeks comments on proposed revisions to the Use of Opioids at High Dosage HEDIS measure. The current measure
Proposed Changes to Existing Measure for HEDIS 1 2020: Use of Opioids at High Dosage (UOD) NCQA seeks comments on proposed revisions to the Use of Opioids at High Dosage HEDIS measure. The current measure
New Measure Recommended for Endorsement by PQA
 New Measure Recommended for Endorsement by PQA Measure: Statin Use in Persons with Diabetes Description: The percentage of patients ages 40 75 years who were dispensed a medication for diabetes that receive
New Measure Recommended for Endorsement by PQA Measure: Statin Use in Persons with Diabetes Description: The percentage of patients ages 40 75 years who were dispensed a medication for diabetes that receive
Atrius Health Pioneer ACO: Structure, Activities and Results
 Atrius Health Pioneer ACO: Structure, Activities and Results Emily Brower Executive Director Accountable Care Programs Emily_Brower@AtriusHealth.org March 2014 1 Atrius Health. 2 Atrius Health Structure
Atrius Health Pioneer ACO: Structure, Activities and Results Emily Brower Executive Director Accountable Care Programs Emily_Brower@AtriusHealth.org March 2014 1 Atrius Health. 2 Atrius Health Structure
The Pharmacy Quality Alliance Optimizing Health by Advancing the Quality of Medication Use
 Optimizing Health by Improving the Quality of Medication Use The Optimizing Health by Advancing the Quality of Medication Use Who is the? Mission Statement Optimizing health by advancing the quality of
Optimizing Health by Improving the Quality of Medication Use The Optimizing Health by Advancing the Quality of Medication Use Who is the? Mission Statement Optimizing health by advancing the quality of
Provider STAR Ratings Quick Reference Guide 2016 Dates of Service. Updated January 20, 2016
 Provider STAR Ratings Quick Reference Guide 2016 Dates of Service Updated January 20, 2016 Adult BMI (Body Mass Index) Assessment (ABA) EXCLUSIONS: Members who have a diagnosis of pregnancy during the
Provider STAR Ratings Quick Reference Guide 2016 Dates of Service Updated January 20, 2016 Adult BMI (Body Mass Index) Assessment (ABA) EXCLUSIONS: Members who have a diagnosis of pregnancy during the
ENSURING EXCELLENCE IN PRESCRIBING FOR OLDER ADULTS
 ENSURING EXCELLENCE IN PRESCRIBING FOR OLDER ADULTS Philip J. Schneider, MS, FASHP The University of Arizona College of Pharmacy Learning Objectives: Describe the medication-use system and all interdependent
ENSURING EXCELLENCE IN PRESCRIBING FOR OLDER ADULTS Philip J. Schneider, MS, FASHP The University of Arizona College of Pharmacy Learning Objectives: Describe the medication-use system and all interdependent
Blue Shield Participation
 9 th Annual Right Care Initiative Summit Blue Shield Participation Scott Flinn, MD Regional Medical Director Blue Shield of California 1 Care Worthy of our Family and Friends 2 Bottom Line Up Front Blue
9 th Annual Right Care Initiative Summit Blue Shield Participation Scott Flinn, MD Regional Medical Director Blue Shield of California 1 Care Worthy of our Family and Friends 2 Bottom Line Up Front Blue
Affordability AMGA - MIPS Webinar
 Affordability AMGA - MIPS Webinar Beth Averbeck, MD Senior Medical Director Primary Care, HealthPartners Consumer-governed, non-profit HealthPartners Medical Group Primary Care: 500,000 patients 29 locations
Affordability AMGA - MIPS Webinar Beth Averbeck, MD Senior Medical Director Primary Care, HealthPartners Consumer-governed, non-profit HealthPartners Medical Group Primary Care: 500,000 patients 29 locations
Meds and Falls: Keep in Step with your Meds
 Meds and Falls: Keep in Step with your Meds Donna Bartlett PharmD, CGP, RPh Associate Professor-Pharmacy Practice MCPHS University Clinical Pharmacist-MCPHS University- Pharmacy Outreach Program donna.bartlett@mcphs.edu
Meds and Falls: Keep in Step with your Meds Donna Bartlett PharmD, CGP, RPh Associate Professor-Pharmacy Practice MCPHS University Clinical Pharmacist-MCPHS University- Pharmacy Outreach Program donna.bartlett@mcphs.edu
HEDIS/CAHPS 101 August 13, 2012 Minnesota Measurement and Reporting Workgroup
 HEDIS/CAHPS 101 Minnesota Measurement and Reporting Workgroup MNsure s Accessibility & Equal Opportunity (AEO) office can provide this information in accessible formats for individuals with disabilities.
HEDIS/CAHPS 101 Minnesota Measurement and Reporting Workgroup MNsure s Accessibility & Equal Opportunity (AEO) office can provide this information in accessible formats for individuals with disabilities.
ProviderNews FEBRUARY
 ProviderNews FEBRUARY 2017 Reminder: decimal billing required on time-based therapy codes for BadgerCare Plus members In accordance with Forward Health guidelines, Security Health Plan requires decimal
ProviderNews FEBRUARY 2017 Reminder: decimal billing required on time-based therapy codes for BadgerCare Plus members In accordance with Forward Health guidelines, Security Health Plan requires decimal
DUPLICATION DISTRIBUTION PROHIBBITED AND. Utilizing Economic and Clinical Outcomes to Eliminate Health Disparities and Improve Health Equity
 General Session IV Utilizing Economic and Clinical Outcomes to Eliminate Health Disparities and Improve Health Equity Accreditation UAN 0024-0000-12-012-L04-P Participation in this activity earns 2.0 contact
General Session IV Utilizing Economic and Clinical Outcomes to Eliminate Health Disparities and Improve Health Equity Accreditation UAN 0024-0000-12-012-L04-P Participation in this activity earns 2.0 contact
Statement Of. The National Association of Chain Drug Stores. For. U.S. House of Representatives Committee on the Budget.
 Statement Of The National Association of Chain Drug Stores For U.S. House of Representatives Committee on the Budget Hearing on: 2:00 p.m. 210 Cannon House Office Building National Association of Chain
Statement Of The National Association of Chain Drug Stores For U.S. House of Representatives Committee on the Budget Hearing on: 2:00 p.m. 210 Cannon House Office Building National Association of Chain
Hypertension Update 2014:
 GSHTP Webinar Hypertension Update 2014: The Kaiser Permanente Northern California Experience Presented by: Marc Jaffe, MD Associate Clinical Professor of Medicine, UCSF Kaiser Permanente Northern California
GSHTP Webinar Hypertension Update 2014: The Kaiser Permanente Northern California Experience Presented by: Marc Jaffe, MD Associate Clinical Professor of Medicine, UCSF Kaiser Permanente Northern California
Medicare Part D Prescription Opioid Policies for 2019 Information for Pharmacists
 CENTERS FOR MEDICARE & MEDICAID SERVICES Medicare Part D Prescription Opioid Policies for 2019 Information for Pharmacists Background Opioid medications are effective at treating certain types of pain,
CENTERS FOR MEDICARE & MEDICAID SERVICES Medicare Part D Prescription Opioid Policies for 2019 Information for Pharmacists Background Opioid medications are effective at treating certain types of pain,
Payers continue to search for effective ways to control
 At a Glance Practical Implications p 218 Author Information p 221 Full text and PDF www.ajpblive.com Value-Based Benefit Design and Healthcare Utilization in Asthma, Hypertension, and Diabetes Benefit
At a Glance Practical Implications p 218 Author Information p 221 Full text and PDF www.ajpblive.com Value-Based Benefit Design and Healthcare Utilization in Asthma, Hypertension, and Diabetes Benefit
Long-Term Care Updates
 Long-Term Care Updates August 2015 By Darren Hein, PharmD Hypertension is a clinical condition in which the force of blood pushing on the arteries is higher than normal. This increases the risk for heart
Long-Term Care Updates August 2015 By Darren Hein, PharmD Hypertension is a clinical condition in which the force of blood pushing on the arteries is higher than normal. This increases the risk for heart
Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015
 Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015 Amerivantage is an HMO plan with a contract with the New Mexico Medicare program.
Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015 Amerivantage is an HMO plan with a contract with the New Mexico Medicare program.
Idaho DUR Board Meeting Minutes
 Idaho DUR Board Meeting Minutes Date: January 21, 2016 Time: 9am-1:30pm Location: Idaho Medicaid, 3232 Elder Street, Boise, Idaho, Conference Room D-West Moderator: Mark Turner, M.D. Committee Members
Idaho DUR Board Meeting Minutes Date: January 21, 2016 Time: 9am-1:30pm Location: Idaho Medicaid, 3232 Elder Street, Boise, Idaho, Conference Room D-West Moderator: Mark Turner, M.D. Committee Members
What s at the Heart of the Matter?
 What s at the Heart of the Matter? Inpatient Pharmacy Services for Heart Failure Patients Jason Williamson, PharmD, BCPS Clinical Pharmacy Manager, PGY1 Pharmacy Residency Director Genesys Regional Medical
What s at the Heart of the Matter? Inpatient Pharmacy Services for Heart Failure Patients Jason Williamson, PharmD, BCPS Clinical Pharmacy Manager, PGY1 Pharmacy Residency Director Genesys Regional Medical
Performance Measurement: HEDIS, STARS and More. Margaret E. O Kane NCQA President CAPG Educational Series October 27, 2016
 Performance Measurement: HEDIS, STARS and More Margaret E. O Kane NCQA President CAPG Educational Series October 27, 2016 Defining Quality & Performance Trends The Triple Aim and National Priorities Partnership
Performance Measurement: HEDIS, STARS and More Margaret E. O Kane NCQA President CAPG Educational Series October 27, 2016 Defining Quality & Performance Trends The Triple Aim and National Priorities Partnership
Improving Medication Adherence through Collaboration between Colleges of Pharmacy and Community Pharmacies
 Improving Medication Adherence through Collaboration between Colleges of Pharmacy and Community Pharmacies Megan Willson, PharmD, BCPS; Catrina Schwartz, PharmD, BS; Jennifer Robinson, PharmD Spokane,
Improving Medication Adherence through Collaboration between Colleges of Pharmacy and Community Pharmacies Megan Willson, PharmD, BCPS; Catrina Schwartz, PharmD, BS; Jennifer Robinson, PharmD Spokane,
Issues for Part D Compliance
 HCCA- MEDICARE PRESCRIPTION DRUG PART D COMPLIANCE CONFERENCE Issues for Part D Compliance Craig Miner, RPh, JD Division of Drug Plan Policy Babette S. Edgar, Pharm.D., MBA Division of Finance and Operations
HCCA- MEDICARE PRESCRIPTION DRUG PART D COMPLIANCE CONFERENCE Issues for Part D Compliance Craig Miner, RPh, JD Division of Drug Plan Policy Babette S. Edgar, Pharm.D., MBA Division of Finance and Operations
