HOW TO USE THE CLINICAL PATHWAY
|
|
|
- Emil Palmer
- 5 years ago
- Views:
Transcription
1 1. 2. INCLUSION CRITERIA: All Stroke patients over 18 years of age admitted to hospital. HOW TO USE THE CLINICAL PATHWAY This is a proactive tool to avoid delays in treatment and discharge. These are not orders, only a guide to usual order. Place the Clinical Pathway in the nurses clinical area of the chart. All health care professionals should fill in the master signature sheet at the front of the Pathway. Addressograph/sticker each page of the Pathway. 3. MULTIDISCIPLINARY TEAMS: Sign and date appropriate sheet on first contact with patient and each day the patient is seen. 4. HEALTH CARE PROFESSIONALS: Place appropriate symbol in space provided: ie done not done or symbol provided and relevant. Place N/A in any box where the task is not applicable to the patient. Additional tasks due to patient individuality can be added to the pathway in OTHER boxes and/or Progress Notes. NOT ALL TASKS WILL APPLY TO EVERY PATIENT. 5. TRANSFER PATIENTS: If patient is transferred to another hospital in Grey- Bruce or to CCAC, send a copy of the following: m Discharge Criteria - original to stay on patient chart m MAR Sheet - original to stay on patient chart m Anticoagulant Record - original to stay on patient chart m Teaching Checklist - original to stay on patient chart m Caregiver Checklist - original to stay on patient chart Grey Bruce Health Network 1
2 NAME (Please Print) INITIAL SIGNATURE DESIGNATION (RN / RPN/ OTHER) All rights reserved. No part of this document may be reproduced or transmitted, in any form or by any means, without the prior permission of the copyright owner Grey Bruce Health Network 2
3 CLINICAL PATHWAY CHECHLIST EMERGENCY PHASE 0-3 HOURS P = Done O = Not Done N/A = Not Applicable * requires descriptive charting in progress notes INITIAL VITAL SIGNS + O 2 SATS *NOTIFY PHYSICIAN IF SBP > 220 OR DBP > 120 FOR 2 OR MORE READINGS 5-10 MIN APART **Immediate Notification of the Acute Stroke Multidisciplinary Team is recommended on admission** THOSE PATIENTS STAYING LONGER THAN 3 HOURS IN ER WILL HAVE ACUTE PHASE ACTIVATED CONTINUOUS CARDIAC MONITOR / RHYTHM STRIPS INTERPRETTED AND ATTACHED * DOES PATIENT HAVE KNOWLEDGE / DOCUMENTED HISTORY OF HAVING AN IRREGULAR HEART RATE / PREVIOUS? * RELEVENT / EMERGENT COMORBIDITIES DOCUMENTED DATE / TIME ER PHASE DATE / TIME ON TRANSFER ASSESSMENT (OBSERVATIONS/ MEASUREMENTS/ ELIMINATION) TREAT TEMPS >37.5 *NOTIFY PHYSICIAN FOR TEMP > 38.5 CHEST ASSESSMENT: C - Clear *A - Adverse sounds PAIN ASSESSMENT: SCORE 0-10 MONITOR FLUID INTAKE AND OUTPUT: V - Voided C - Catheter I - Incontinent URINE COLOUR: CATHETER TYPE AND SIZE: INITIAL ASSESSMENT NATIONAL INSTITUTES OF HEALTH SCALE (NIHSS) FLOW SHEET, then Q2H x 24 hours (Indicate Score) BLOOD WORK (Specifically CBC, APTT, INR, ELECTROLYTES, CREATININE, GLUCOSE) LABORATORY / DIAGNOSTICS CT SCAN ECG ER ADMISSION SIGNATURE: ER TRANSFER SIGNATURE: Grey Bruce Health Network 3
4 ` GREY BRUCE HEALTH NETWORK EMERGENCY PHASE 0-3 HOURS P = Done O = Not Done N/A = Not Applicable * requires descriptive charting in progress notes DATE / TIME ER PHASE DATE / TIME ON TRANSFER IV SITE ESTABLISHED / INSITU AND SATISFACTORY TREATMENTS/ INTERVENTIONS 2ND IV SITE ESTABLISHED / INSITU AND SATISFACTORY ISCHEMIC NON-THROMBOLYTIC / NON-HEMMORAGIC ONLY: ASA 160 mg MEDICATIONS ISCHEMIC THROMBOLYTIC THERAPY ONLY: ALTEPLASE BEST MEDICATION RECONCILIATION FORM COMPLETED AND SIGNED ACETAMINOPHEN FOR TEMPERATURE > 37.5 NUTRITION MOBILITY/ACTIVITY PSYCHOSOCIAL SUPPORT/ EDUCATION CONSULTS TRANSFER NPO BED REST PATIENT / FAMILY INFORMED OF DIAGNOSIS / REASON FOR ADMISSION ADVANCE DIRECTIVE DISCUSSION ADDRESSED ADDRESS IMMEDIATE CONCERNS CONFIRM ORDER FOR ACUTE MULTIDISCIPLINARY TEAM ENTERED IN CERNER AS: C - Confirmed stroke REPORT CALLED TO RECEIVING UNIT INDICATED TIME: INFECTION CONTROL SCREENING QUESTIONS REVIEWED FOR APPROPRIATE BED PLACEMENT ER ADMISSION SIGNATURE: ER TRANSFER SIGNATURE: Grey Bruce Health Network 4
5 National Institutes of Health Stroke Scale Flow Sheet Category 1a. Level of consciousness (LOC) 1b. LOC, questions (month, age) 1c. LOC, commands (open/close eyes, make fist, release) 2. Best gaze (patient follows examiner's finger) 3. Visual (introduce visual stimulus) 4. Facial palsy (show teeth, raise eyebrowns, squeeze eyes shut) 5a. Motor arm - Left (elevate arm to 90 and score drift/movement) 5b. Motor arm - Right (as above) 6a. Motor leg - Left (elevate leg to 30 and score drift/movement) 6b. Motor leg - Right (as above) 7. Limb ataxia (finger-nose, heel down shin) 8. Sensory (pin prick to face, arm, trunk, and leg - compare side to side) 9. Best language (name item, describe a picture and read sentences) 10. Dysarthria (evaluate speech clarity by patient read or repeat listed words) 11. Extinction and Inattention (use information from prior testing) Date Time Description Score Score Score Score 0 Alert - Alert 1 Drowsy - wakens with stimulation 2 Stuporou - (requires repeated stimuli) 3 Coma 0 Answers both correctly 1 Answers one correctly 2 Answers neither correctly 0 Performs both correctly 1 Performs one correctly 2 Performs neither correctly 0 Normal 1 Partial gaze palsy 2 Forced deviation 0 No visual loss 1 Partial hemianopia 2 Complete hemianopia 3 Bilateral hemianopia 0 Normal 1 Minor asymmetry 2 Partial paralysis (lower face) 3 Complete 0 No drift 1 Drift 2 Some effort against gravity 3 No effort against gravity 4 No movement X Amputation, joint fusion 0 No drift 1 Drift 2 Some effort against gravity 3 No effort against gravity 4 No voluntary movement X Amputation, joint fusion etc 0 Absent 1 Present in one limb 2 Present in two or more limbs X Amputation, joint fusion 0 Normal 1 Partial loss 2 Dense loss 0 No aphasia 1 Mild to moderate aphasia 2 Severe aphasia 3 Mute, global aphasia 0 Normal articulation 1 Mild to moderate slurring 2 Severe (near uninteligible or worse) X Intubated or other physicial barrier 0 No neglect 1 Partial neglect 2 Profound neglect TOTAL SCORE Initials of Examiner For Thrombolytic Strokes: NIHSS - Q2H x 24 hours, then twice per shift x 48 hours, then QSHIFT x 4 days For Non-Thrombolytic Strokes: NIHSS - Q6H x 72 hours or unless change in presentation 5 of 21
6 ACUTE CARE PHASE (Record QSHIFT on Checklist) P = Done O = Not Done N/A = Not Applicable * requires descriptive charting in progress notes DAY 1 DAY 2 DAY 3 PERFORMANCE INDICATORS 1 DYSPHAGIA SCREENING TOOL COMPLETED (Once Q24H) INITIALS: Pass / Fail keep NPO q Met q Not Met q N/A VITAL SIGNS + O 2 SATS: (Thrombolytic increased frequency as ordered) (Non-Thrombolytic - Day 1: Q4H Day 2: QID Day 3: QSHIFT * NOTIFY PHYSICIAN IF SBP > 220 OR DBP > 120 FOR 2 OR MORE READINGS 5-10 MIN APART X 48 HOURS RECORD REGULARITY OF HEART RATE (Note if patient aware of any past anomalies) REG - Regular / IRREG - Irregular TREAT TEMPS >37.5 * NOTIFY PHYSICIAN FOR TEMP > 38.5 CHEST ASSESSMENT Q4H: C - Clear * A - Adverse sounds ASSESSMENT (OBSERVATIONS/ MEASUREMENTS/ ELIMINATION) PAIN ASSESSMENT Q4H: CATHETER REMOVED: * I - Intervention SCORE 0-10 INTAKE AND OUTPUT QSHIFT (Nofity physician for < ml/h) V - Voided C - Catheter I - Incontinent HNV - Has Not Voided URINE COLOUR: BOWEL ROUTINE: C - Continent I - Involuntary O - Ostomy NATIONAL INSTITUTES OF HEALTH SCALE (NIHSS): Q2H x 24 hours, then twice per shift x 48 hours, then QSHIFT x 4 days MODIFIED RANKIN SCALE BRADEN (SKIN) RISK ASSESSMENT COMPLETED ON ADMISSION AND PRN (Indicate Score) (Indicate Score) PATIENT SAFETY CUE CARDS IN PLACE IN ROOM (no straws, acute stroke checklist, fall risk symbol, etc) MORSE FALL RISK ASSESSMENT COMPLETED ON ADMISSION AND PRN (Indicate Score) PATIENT SAFETY CUES * MORSE FALL RISK INTERVENTIONS DOCUMENTED * CONSENT OBTAINED FOR MINIMAL RESTRAINT FOR SAFETY AND REASSESSED Q24H RESTRAINT OBSERVATION Q MIN INITIALS: Grey Bruce Health Network 6
7 ACUTE CARE PHASE (Record Q4H on Checklist) P = Done O = Not Done N/A = Not Applicable * requires descriptive charting in progress notes DAY 1 DAY 2 DAY 3 LABORATORY / DIAGNOSTICS BLOOD WORK AS ORDERED: (Documenting procedure completed) SWABS MRSA & VRE COMPLETED ON ADMISSION THEN Q WEEKLY DIAGNOSTICS: ALTERNATE ROUTES DETERMINED FOR MEDS IF PATIENT NPO MEDICATIONS * ASSESS RISK / NEED FOR DVT PROPHYLAXIS WITH PHYSICIAN (Limited Mobiltiy / type of stroke significant in rationale for ordering) TREATMENTS/ INTERVENTIONS IV AND/OR INTERMITTENT SET OBSERVATION AND SITE CARE Q1H S - Satisfactory C - Changed R - Removed IF NON-AMBULATORY: S - anti-emboli Stockings or C - sequential Compression device DIET TEXTURE AS PER DYSPHAGIA SCREENING TOOL: (Diet order from physician only) NUTRITION F - Feed self A - Assist C - Complete feed (% of diet taken if not NPO) NG FEEDING ESTABLISHED / CLINICAL NUTRITION CONSULT PROTOCOL INITIATED / ENTER FEEDING ORDER SET INITIATED NON-THROMBOLYTIC - ACTIVITY AS TOLERATED THROMBOLYTIC - RESTRICTED AS ORDERED X 24 HOURS HEAD OF BED ELEVATED MINIMUM 30 DEGREES FOR NPO / TUBE FED PATIENTS MOBILITY / ACTIVITY * USE POSITIONING TO MAINTAIN PROPER BODY ALIGNMENT (SEE "TIPS AND TOOLS" BOOK FOR REFERENCE PURPOSES) SPECIAL EQUIPMENT: PERSONAL HYGIENE: C - Complete / Cueing required A - Assist S - Self SLEEP: R - Restless F - Fair W - Well INITIALS: Grey Bruce Health Network 7
8 ACUTE CARE PHASE (Record Q4H on Checklist) P = Done O = Not Done N/A = Not Applicable * requires descriptive charting in progress notes DAY 1 DAY 2 DAY 3 PSYCHOSOCIAL SUPPORT/ EDUCATION DISCHARGE PLANNING * ADDRESS PATIENT AND FAMILY ANXIETY IF APPLICABLE / * ENCOURAGE PATIENT AND FAMILY TO ASK QUESTIONS * BARRIERS TO LEARNING DOCUMENTED (Patient or Family) *SPECIFIC COMMUNICATIN / NEGLECT DEFICITS DOCUMENTED GIVE PATIENT PATHWAY TO PATIENT / FAMILY BEGIN / CONINUE TEACHING CHECKLIST WHEN APPROPRIATE (Patient/family have received "LET'S TALK ABOUT " book) ASSESS DISCHARGE CRITERIA DAILY - Assess readiness for rehabilitation using referral form - Complete Blaylock Discharge Planning Risk Assessment Screen - Fax referral to Community Stroke Team when discharged INITIALS: Progress Notes: Grey Bruce Health Network 8
9 ACUTE CARE PHASE MULTIDISCIPLINARY TEAM P = Individual Disciplines have reviewed and updates recorded accordingly UPDATE PATIENT STATUS IN CERNER AS CONFIRMED OR UNCONFIRMED TO ACTIVATE THE ACUTE MULTIDICIPLINARY TEAM P DATE & TIME SIGNATURE CONSULTS (To be completed by individual discipline and signed with signature) * PHYSIOTHERAPY * OCCUPATIONAL THERAPY * SPEECH/LANGUAGE PATHOLOGIST IF REQUIRED * CLINICAL NUTRITION * PHARMACIST * CCAC / DISCHARGE PLANNING * SOCIAL WORKER * Progress Notes: Grey Bruce Health Network 9
10 MODIFIED RANKIN SCALE q Admission date: q Discharge from Acute Care date: * This is to be completed on all Stroke as baseline (pre-treatment) and discharge from Acute Care* Please indicate who provided the information: q Patient q Family member q Patient s physician q Registered Nurse q Other: Specify GRADE DESCRIPTION QUESTIONS TO CONSIDER FOR GRADING Baseline Discharge q 0 q 0 No symptoms at all. No limitations. q 1 q 1 Does person have difficulty reading or writing, No significant disability speaking, problems with balance/coordination, despite symptoms; able to visual problems, numbness, loss of movement, carry out all usual duties and difficulty swallowing or other symptoms resulting activities. from stroke? q 2 q 2 q 3 q 3 q 4 q 4 q 5 q 5 Slight disability; unable to carry out all previous activities but able to look after own affairs without assistance. Moderate disability; requiring some help, but able to walk without assistance. Moderately severe disability; unable to walk without assistance, and unable to attend to own bodily needs without assistance. Severe disability; bedridden, incontinent, and requiring constant nursing care and attention. Has there been a change in person s ability to work or look after others if these were roles before stroke? Change in person s ability to participate in previous social and leisure activities? Problems with relationships or become isolated? Is assistance essential for preparing a simple meal, doing household chores, looking after money, shopping or traveling locally? Is assistance essential for eating, using the toilet, daily hygiene, or walking? Requires constant care. RN / MD Signature: / Baseline assessment Grey Bruce Health Network Discharge assessment 10
11 CLINICAL PATHWAY Braden Risk Assessment SCORING (Key on Reverse) DATE DATE DATE RISK FACTOR SCORE Sensory Perception: Ability to respond meaningfully to pressure related discomfort Completely Limited Very Limited Slightly Limited No Impairment Moisture: Degree to which skin is exposed to moisture Constantly Moist Often Moist Occasionally Moist Rarely Moist Activity: Degree of Physical Activity Bedfast Chair Fast Walks Occasionally Walks Frequently Mobility: Ability to change and control body position Completely Immobile Very Limited Slightly Limited No Limitations Nutrition: Usual food intake pattern Very Poor Probably Inadequate Adequate Excellent Friction and Sheer Problem Potential Problem No Apparent Problem TOTAL SCORE NURSE S INITIALS Nursing Intervention: Once you have assessed the patient and identified a risk category (high, moderate or low), carry out the following interventions for the patient's risk category. LOW RISK (SCORE > 15) Ongoing assessment for change in status related to any of the six risk areas Document reassessment weekly on Kardex MODERATE RISK (SCORE 13-14) Initiate and document plan of care on Kardex and Unit specific Progress Notes including: -Activity level (i.e. turning, positioning) -Continence management -Monitoring of pressure point areas -Monitor nutritional status -Skin care tools used: prevention mattresses or treatment (i.e. air mattresses), creams, bed hoop, trapeze, dressings -Patient education re: prevention Includes Moderate Risk Intervention plus requested referral to: -Physiotherapy -Occupational Therapy -Dietitian HIGH RISK (SCORE < 12) Grey Bruce Health Network 11
12 Braden Risk Assessment - page 2 RISK FACTOR Sensory Perception Ability to respond meaningfully to pressure related discomfort 1. Completely Limited Unresponsive (does not moan, flinch, or grasp) to painful stimuli, due to diminished level or consciousness or sedation. OR Limited ability to feel pain over most of body surface. 2. Very Limited Responds only to painful stimuli. Cannot communicate discomfort except by moaning or restlessness. OR Has a sensory impairment, which limits the ability to feel pain or discomfort over 1/2 of body. SCORE/DESCRIPTION 3. Slightly Limited Responds to verbal commands but cannot always communicate discomfort or need to be turned. OR Has some sensory Impairment, which limits ability to feel pain or discomfort in 1 or 2 extremities. 4. No Impairment Responds to verbal commands. Has no sensory deficit, which would limit ability to feel or voice pain or discomfort. Moisture Degree to which skin is exposed to moisture Activity Degree of physical activity 1. Constantly Moist Skin is kept moist almost constantly by perspiration, urine, etc. Dampness is detected every time patient is moved or turned. 1. Bedfast Confined to a bed. 2. Often Moist Skin is often, but not always moist. Linen must be changed at least once a shift. 2. Chair Fast Ability to walk severely limited or nonexistent. Cannot bear own weight and/or must be assisted into chair or wheelchair. 3. Occasionally Moist Skin is occasionally moist, requiring an extra linen change approximately once a day. 3. Walks Occasionally Walks occasionally during day, but for very short distances, with or without assistance. Spends majority of each shift in bed or chair. 4. Rarely Moist Skin is usually dry, linen only requires changing at routine intervals. 4. Walks Frequently Walks outside the room at least twice a day and inside room at least once every two hours during waking hours. Mobility Ability to change and control body position Nutrition 1. Completely Immobile Does not make even slight changes in body or extremity position without assistance. 1. Very Poor Never eats a complete meal. Rarely eats more than 1/3 of any food offered. Eats 2 servings or less of protein (meat or dairy products) per day. Takes fluids poorly. Does not take a liquid dietary supplement. OR Is on NPO and/or maintained on clear fluids or IV for more than 5 days. 2. Very Limited Makes occasional slight changes in body or extremity position, but unable to make frequent or significant changes independently. 2. Probably Inadequate Rarely eats a complete meal and generally eats only about 1/2 of any food offered. Protein intake includes only 3 servings of meat or dairy products per day. Occasionally will take a dietary supplement. OR Receives less than optimum amount of liquid diet or tube feeding. 3. Slightly Limited Makes frequent, though slight changes in body or extremity position independently. 3. Adequate 4. Excellent Eats over half of most meals. Eats a total of 4 servings of protein (meat, dairy products) each day. Occasionally, will refuse a meal, but will usually take a supplement if offered. OR Is on a tube feeding or TPN (Total Parenteral Nutrition) regimen, which probably meets most of nutritional needs. 4. No Limitations Makes major and frequent changes in position without assistance. Eats most of every meal. Never refuses a meal. Usually eats a total of 4 or more servings of meat and dairy products. Occasionally eats between meals. Does not require supplementation. Friction and Shear 1. Problem Requires moderate to maximum assistance in moving. Complete lifting without sliding against sheets is impossible. Frequently slides down in bed or chair, requiring frequent repositioning with maximum assistance. Spasticity, contractures or agitation leads to almost constant friction. 2. Potential Problem Moves feebly or requires minimum assistance. During a move, skin probably slides to some extent against sheets, chair, restraints or other devices. Maintains relatively good position in chair or bed most of the time, but occasionally slides down. 3. No Apparent Problem Moves in bed and in chair independently and has sufficient muscle strength to lift up completely during move. Maintains good position in bed or chair at all times Grey Bruce Health Network 12 Review Dec2016
13 TRANSITIONAL PHASE DAY: DAY: DAY: (Record Q4H on Checklist) P = Done O = Not Done N/A = Not Applicable * required descriptive charting in progress notes INITIAL DATE PERFORMANCE INDICATORS 2 3 INTERDISCIPLINARY CONSULTS COMPLETED TRIAGE (TRANSITION PLAN) COMPLETED q Met q Not Met q N/A q Met q Not Met q N/A VITAL SIGNS QSHIFT & PRN INCLUDING 0 2 SATS TREAT TEMPS >37.5 *NOTIFY PHYSICIAN FOR TEMP >38.5 CHEST ASSESSMENT QSHIFT & PRN C - Clear *A - Adverse sounds PAIN ASSESSMENT QID & PRN *N - Needs intervention Score 0-10 ASSESSMENT (OBSERVATIONS/ MEASUREMENTS/ ELIMINATION) SKIN INTEGRITY QSHIFT MONITOR BOWEL AND BLADDER ROUTINE C - Continent *N - Needs intervention I - Incontinent NATIONAL INSTITUTES OF HEALTH SCALE (NIHSS) QSHIFT FOR 4 DAYS REASSESS DYSPHAGIA SCREENING TOOL IF INDICATED P - Pass F - Fail BRADEN (SKIN) RISK ASSESSMENT UPDATED MODIFIED RANKIN SCALE IF PATIENT BEING DISCHARGED FROM ACUTE CARE (Indicate Score) PATIENT SAFETY CUE CARDS IN PLACE IN ROOM (no straws, acute stroke checklist, fall risk symbol) PATIENT SAFETY CUES (UPDATED - PRN) MORSE FALL RISK ASSESSMENT *I - Interventions required *CONSENT OBTAINED FOR MINIMAL RESTRAINT FOR SAFETY AND REASSESSED Q24H RESTRAINT OBSERVATION Q MINUTES LABORATORY / DIAGNOSTICS BLOOD WORK DIAGNOSTICS INITIALS: Grey Bruce Health Network 13
14 TRANSITIONAL PHASE (Record Q4H on Checklist) DAY: DAY: DAY: P = Done O = Not Done N/A = Not Applicable * required descriptive charting in progress notes MEDICATIONS ALL MEDICATIONS AND ROUTES ESTABLISHED REASSESS IV WHEN ORAL INTAKE >1500 ML IN 24 HOURS REMOVE/CHANGE IV SITE Q72H (INCLUDING TUBING) TREATMENTS/ INTERVENTIONS IF NON-ABULATORY BOWEL/BLADDER RETRAINING ONGOING S - anti emboli Stockings or C - sequential Compression device - PLAN DOCUMENTED AND *A - Adjustments made REMIND PHYSICIAN OF REMOVAL OF URINARY CATHETER REMOVAL DATE / TIME: (Recommended after fluid balance established) q DIET TEXTURE AS PER DYSPHAGIA SCREENING TOOL q REGULAR TEXTURE - HEALTHY HEART DIET q SPECIAL DIET: NUTRITION % OF DIET TAKEN IF NOT NPO IF TUBE FEEDING T - Tolerated *A - Adjustments as ordered CONTINUE METHOD OF PATIENT TRANSFER AND DOCUMENT IN PATIENT CARE PLAN (SEE "HEALTHY MOVES" BOOKLET FOR REFERENCE PURPOSES) MOBILITY/ACTIVITY USE POSITIONING TO MAINTAIN PROPER BODY ALIGNMENT (SEE "TIP AND TOOLS" BINDER FOR REFERENCE PURPOSES) DOCUMENT TOLERATED SITTING TIME DAILY REVIEW PATIENT-SPECIFIC RISK FACTORS FOR SECONDARY PREVENTION PSYCHOSOCIAL SUPPORT/ EDUCATION ADDRESS QUESTIONS REGARDING PATIENT PATHWAY AND/OR "LET'S TALK ABOUT " BOOKLET ENGAGE FAMILY IN CAREGIVING (Identify barriers and document for follow-up) ADDRESS ANY QUESTIONS, FEARS AND ANXIETIES THE PATIENT/FAMILY MAY HAVE INITIALS: Grey Bruce Health Network 14
15 TRANSITIONAL PHASE (Record Q4H on Checklist) P = Done O = Not Done N/A = Not Applicable * required descriptive charting in progress notes DAY: DAY: DAY: REHABILITATION CONSULT DISCUSSION INITIATED *BARRIERS TO REHABILITATION READINESS - Plan commenced to optimize readiness / alternate plan DISCHARGE PLANNING UPDATE AND REVIEW PLAN FOR DISCHARGE WITH PATIENT/CAREGIVER CAREGIVER TRAINING/EDUCATION CHECKLIST COMPLETED AND UNDERSTOOD BY CAREGIVER Progress Notes: REFERRAL TO CCAC DISCHARGE PLANNING INITIATED DATE / TIME: ASSESS DISCHARGE CRITERIA DAILY AND NOTIFY COMMUNITY TEAM WHEN PATIENT DISCHARGED INITIALS: Grey Bruce Health Network 15
16 TRANSITIONAL PHASE MULTIDISCIPLINARY TEAM P = Individual Disciplines have reviewed and updates recorded accordingly P DATE & TIME SIGNATURE *PHYSIOTHERAPY CONSULTS (To be completed by individual discipline and signed with signature) *OCCUPATIONAL THERAPY *SPEECH/LANGUAGE PATHOLOGIST IF REQUIRED *CLINICAL NUTRITION *PHARMACIST *CCAC / DISCHARGE PLANNING - assistive device needs identified and arranged - home program developed and discussed *SOCIAL WORKER * Progress Notes: Grey Bruce Health Network 16
17 MAINTENANCE PHASE BEYOND DAY 6 P = Done O = Not Done N/A = Not Applicable "O" requires descriptive charting in progress notes UPDATE THE PATIENT CARE PLAN ACCORDING TO THE FOLLOWING LISTED CRITERIA, THEN DISCONTINUE THE PATHWAY. CHARTING TO BE RESUMED ACCORDING TO UNIT CRITERIA. COMPLETED FOR LONGER TERM PATIENTS CONSIDER OBTAINING ALC ORDERS VITAL SIGNS ACCORDING TO UNIT PROTOCOL CHEST ASSESSMENT Q SHIFT ONLY IF DYSPHAGIC PAIN ASSESSMENT PRN ASSESSMENT (OBSERVATIONS/ MEASUREMENTS/ ELIMINATION) SKIN INTEGRITY Q SHIFT BRADEN RISK ASSESSMENT UPDATED MONITOR BOWEL AND BLADDER ROUTINE MODIFIED RANKIN SCALE IF PATIENT BEING DISCHARGED FROM ACUTE CARE REASSESS DYSPHAGIA SCREENING TOOL IF INDICATED PATIENT SAFETY CUES TREATMENTS/ INTERVENTIONS NUTRITION UPDATE PATIENT SAFETY CUES PRN MRSA AND VRE SWABS Q WEEKLY (Next date to be completed indicated on Care Plan) IF NON-AMBULATORY, ANTI AMBOLI STOCKINGS/SEQUENTIAL COMPRESSION DEVICES q DIET TEXTURE AS PER DYSPHAGIA SCREENING TOOL q REGULAR TEXTURE - HEALTHY HEART DIET q SPECIAL DIET: PUSH ORAL FLUIDS IF NOT NPO DOCUMENTATION FOR TUBE FEEDING AND FEEDING TYPE ACTIVITY AS TOLERATED REVIEWED DAILY MOBILITY/ACTIVITY TRANSFERS INDICATED ON CARE PLAN (SEE "HEALTHY MOVES" BOOKLET FOR REFERENCE PURPOSES) AMBULATION INDICATED ON KARDEX DOCUMENT TOLERATED SITTING TIME DAILY MULTIDICIPLINARY TEAM: RECOMMENDATIONS CLEARLY COMMUNICATED ON CARE PLAN INITIALS: Grey Bruce Health Network 17
18 PSYCHOSOCIAL SUPPORT/ EDUCATION MAINTENANCE PHASE BEYOND DAY 6 P = Done O = Not Done N/A = Not Applicable "O" requires descriptive charting in progress notes TEACHING ON GOING COMPLETED ASSESS DISCHARGE CRITERIA DAILY DISCHARGE PLANNING ONGOING STRATEGY TO OVERCOME BARRIERS TO DISCHARGE IN PLACE UPON PATIENT DISCHARGE, REFER TO PATHWAY DISCHARGE CRITERIA SHEET Progress Notes: INITIALS: Grey Bruce Health Network 18
19 DISCHARGE CRITERIA DATE MET INITIAL 4 DRIVING STATUS REVIEWED q Met q Not Met q N/A PERFORMANCE INDICATORS 5 SECONDARY PREVENTION RISK FACTORS ADDRESSED q Met q Not Met q N/A REFERRAL TO PREVENTION CLINIC COMPLETED ASSESSMENT (OBSERVATIONS/ MEASUREMENTS/ ELIMINATION) LABORATORY / DIAGNOSTICS SPEECH/LANGUAGE AND/OR SWALLOWING FOLLOW UP ARRANGED IF NEEDED SKIN INTEGRITY PLAN REQUISITION FOR OUTPATIENT BLOOD WORK GIVEN DISCHARE MEDICATIONS LIST EXPLAINED TO PATIENT AND FAMILY MEDICATIONS PATIENT / FAMILY INDICATE THEY UNDERSTAND MEDICATIONS PERSCRIPTION GIVEN TREATMENTS/ INTERVENTIONS NUTRITION MOBILITY/ACTIVITY BOWEL AND BLADDER ROUTINE ESTABLISHED NEED FOR COMMUNITY DIETITIAN REFERRAL IDENTIFIED DISCHARGE TRANSPORTATION ARRANGED PATIENT AWARE OF RISK FACTORS AND MANAGEMENT PSYCHOSOCIAL SUPPORT/ EDUCATION PATIENT AND FAMILY AWARE OF MANAGEMENT PLAN PATIENT AND FAMILY HAVE UNDERSTANDING OF EDUCATION CAREGIVER TRAINING/EDUCATION COMPLETED PATIENT AND FAMILY AWARE OF FOLLOW UP APPOINTMENT DISCHARGE PLANNING TRANSFER INFORMATION CHECKLIST COMPLETED CCAC DISCHARGE PLAN COMPLETED - ASSISTIVE DEVICES ARRANGED AND IN HOME FOLLOW UP OUTPATIENT THERAPY AS APPROPRIATE CONSULTS ALL CONSULTS COMPLETED - NOTIFY COMMUNITY TEAM OF DISCHARGE THROUGH REFERRAL Grey Bruce Health Network 19
20 Progress Notes: Grey Bruce Health Network 20
21 TRIAL SEPT 2, 2014 OCT 31, 2014 Affix Patient Label here PLEASE DOCUMENT TO THE HIGHEST LEVEL OF SPECIFICITY Type of Stroke ( check all that apply ) Ischemic / Cerebral Infarction Identify the cause and site i.e. embolism or thrombus and site of arteries (precerebral or cerebral etc.) Hemorrhagic Identify the artery from which bleed originated i.e. middle cerebral, basilar artery, anterior communicating artery etc. Intracerebral Identify the anatomical site of the bleed i.e. hemisphere, subcortical; hemisphere, cortical; brain stem etc. Deficits/Sequelae - related to current admission Hemiplegia Dominant side Non-dominant side Urinary retention Urinary/fecal incontinence Sensory Loss Neglect Speech/language deficits Aphasia/Dysphasia Dysarthria Apraxia Hemianopia None Other Co-morbidities: Diabetes Hypertension Smoking Obesity Dyslipidemia Other Interventions: CT MRI Ventilation Percutaneous endoscopic gastrostomy (PEG) Other Prescription for Antithrombotic medication at discharge Yes No Physician/NP Signature: Date: (Must be signed in order for Health Records to use for coding) 21
Stroke Transfer Checklist
 Stroke Transfer Checklist When preparing to transfer an acute stroke patient to the UF Health Shands Comprehensive Stroke Center, please make every attempt to include the following information: Results
Stroke Transfer Checklist When preparing to transfer an acute stroke patient to the UF Health Shands Comprehensive Stroke Center, please make every attempt to include the following information: Results
NIHSS. Category Scale Definition Date/Time Date/Time Date/Time. Score Initial. Drip & Ship Protocol. Initials: Signature: Initials: Signature:
 NIHSS 1a. Level of Consciousness (Alert, drowsy, etc.) Category Scale Definition Date/Time Date/Time Date/Time 1b. LOC Question (Month, age) 1c. LOC Commands (Open, close eyes, make fist, let go) 2. Best
NIHSS 1a. Level of Consciousness (Alert, drowsy, etc.) Category Scale Definition Date/Time Date/Time Date/Time 1b. LOC Question (Month, age) 1c. LOC Commands (Open, close eyes, make fist, let go) 2. Best
HOW TO USE THE CLINICAL PATHWAY
 ACUTE CORONARY SYNDROMES CLINICAL PATHWAY ACUTE STAGE GREY BRUCE HEALTH SERVICES Lion's Head Markdale Meaford Owen Sound Southampton Tobermory Wiarton PATIENT ID INCLUSION CRITERIA Patients who present
ACUTE CORONARY SYNDROMES CLINICAL PATHWAY ACUTE STAGE GREY BRUCE HEALTH SERVICES Lion's Head Markdale Meaford Owen Sound Southampton Tobermory Wiarton PATIENT ID INCLUSION CRITERIA Patients who present
o Unenhanced Head CT
 Drip & Ship Protocol Acute Stroke Ready Hospital (ASRH) Duluth Area Primary Stroke Center (St. Luke s & St. Mary s Essentia) PATIENT LABEL Patient displays strokelike symptoms EMS/ED CSS > 0 Glucose >
Drip & Ship Protocol Acute Stroke Ready Hospital (ASRH) Duluth Area Primary Stroke Center (St. Luke s & St. Mary s Essentia) PATIENT LABEL Patient displays strokelike symptoms EMS/ED CSS > 0 Glucose >
HOW TO USE THE CLINICAL PATHWAY
 1. 2. 3. 4. INCLUSION CRITERIA Primary admitting diagnosis is Congestive Heart Failure as defined by New York Heart Association. EXCLUSION CRITERIA Patients less than 19 years of age. HOW TO USE THE This
1. 2. 3. 4. INCLUSION CRITERIA Primary admitting diagnosis is Congestive Heart Failure as defined by New York Heart Association. EXCLUSION CRITERIA Patients less than 19 years of age. HOW TO USE THE This
what do the numbers really mean? NIHSS Timothy Hehr, RN MA Stroke Program Outreach Coordinator Allina Health
 what do the numbers really mean? NIHSS Timothy Hehr, RN MA Stroke Program Outreach Coordinator Allina Health NIHSS The National Institutes of Health Stroke Scale (NIHSS) is a tool used to objectively quantify
what do the numbers really mean? NIHSS Timothy Hehr, RN MA Stroke Program Outreach Coordinator Allina Health NIHSS The National Institutes of Health Stroke Scale (NIHSS) is a tool used to objectively quantify
ACCESS CENTER:
 ACCESS CENTER: 1-877-367-8855 Emergency Specialty Services: BRAIN ATTACK Criteria: Stroke symptom onset time less than 6 hours Referring Emergency Department Patient Information Data: Time last known normal:
ACCESS CENTER: 1-877-367-8855 Emergency Specialty Services: BRAIN ATTACK Criteria: Stroke symptom onset time less than 6 hours Referring Emergency Department Patient Information Data: Time last known normal:
HOW TO USE THE CLINICAL PATHWAY
 CONGESTIVE HEART FAILURE CLINICAL PATHWAY ACUTE STAGE GREY BRUCE HEALTH SERVICES Lion's Head Markdale Meaford Owen Sound Southampton Tobermory Wiarton 1. 2. 3. 4. INCLUSION CRITERIA EXCLUSION CRITERIA
CONGESTIVE HEART FAILURE CLINICAL PATHWAY ACUTE STAGE GREY BRUCE HEALTH SERVICES Lion's Head Markdale Meaford Owen Sound Southampton Tobermory Wiarton 1. 2. 3. 4. INCLUSION CRITERIA EXCLUSION CRITERIA
HOW TO USE THE CLINICAL PATHWAY
 CONGESTIVE HEART FAILURE CLINICAL PATHWAY ACUTE STAGE HANOVER AND DISTRICT HOSPITAL 1. 2. 3. 4. INCLUSION CRITERIA Primary admitting diagnosis is Congestive Heart Failure as defined by New York Heart Association.
CONGESTIVE HEART FAILURE CLINICAL PATHWAY ACUTE STAGE HANOVER AND DISTRICT HOSPITAL 1. 2. 3. 4. INCLUSION CRITERIA Primary admitting diagnosis is Congestive Heart Failure as defined by New York Heart Association.
Thrombolysis Assessment
 Thrombolysis Assessment Brief Clinical Summary of symptom onset of arrival of patient of assessment BP GCS BM If BM
Thrombolysis Assessment Brief Clinical Summary of symptom onset of arrival of patient of assessment BP GCS BM If BM
SARASOTA MEMORIAL HOSPITAL. NURSING PROCEDURE NATIONAL INSTITUTE OF HEALTH STROKE SCALE (neu04) Nursing
 SARASOTA MEMORIAL HOSPITAL TITLE: ISSUED FOR: NURSING PROCEDURE NATIONAL INSTITUTE OF HEALTH Nursing DATE: REVIEWED: PAGES: PS1094 7/01 3/18 1 of 5 RESPONSIBILITY: RN, LPN PURPOSE: OBJECTIVE: DEFINITION:
SARASOTA MEMORIAL HOSPITAL TITLE: ISSUED FOR: NURSING PROCEDURE NATIONAL INSTITUTE OF HEALTH Nursing DATE: REVIEWED: PAGES: PS1094 7/01 3/18 1 of 5 RESPONSIBILITY: RN, LPN PURPOSE: OBJECTIVE: DEFINITION:
Alberta Surgical Fractured Hip Care Pathway Version 3: Last Updated February 9, 2018
 Alberta Surgical Fractured Hip Care Pathway Assessment / Pain Mngmt EMS Transport Neurovascular assessment Vital signs Pain assessment Splint only (no traction) Position of comfort Start IV and use appropriate
Alberta Surgical Fractured Hip Care Pathway Assessment / Pain Mngmt EMS Transport Neurovascular assessment Vital signs Pain assessment Splint only (no traction) Position of comfort Start IV and use appropriate
Thrombolysis for acute ischaemic stroke Rapid Assessment Protocol NORTHERN IRELAND Regional Protocol (Version 002 July 08)
 Thrombolysis for acute ischaemic stroke Rapid Assessment Protocol NORTHERN IRELAND Regional Protocol (Version 002 July 08) Patient Details Time of onset? Capillary Blood glucose 2.8-22.2 mmol/l? Blood
Thrombolysis for acute ischaemic stroke Rapid Assessment Protocol NORTHERN IRELAND Regional Protocol (Version 002 July 08) Patient Details Time of onset? Capillary Blood glucose 2.8-22.2 mmol/l? Blood
Acute Stroke with Alteplase Administration Order Set
 Review Due Date: 2017 October PATIENT CARE DERS Weight: Adverse Reactions or Intolerances Drug No Yes (list) Food No Yes (list) _ Latex No Yes Admission Admit to Neurology service: Dr. Critical Care Diagnosis:
Review Due Date: 2017 October PATIENT CARE DERS Weight: Adverse Reactions or Intolerances Drug No Yes (list) Food No Yes (list) _ Latex No Yes Admission Admit to Neurology service: Dr. Critical Care Diagnosis:
Canadian Stroke Best Practices Initial ED Evaluation of Acute Stroke and Transient Ischemic Attack (TIA) Order Set (Order Set 1)
 Canadian Best Practice Recommendations for Stroke Care: All patients presenting to an emergency department with suspected stroke or transient ischemic attack must have an immediate clinical evaluation
Canadian Best Practice Recommendations for Stroke Care: All patients presenting to an emergency department with suspected stroke or transient ischemic attack must have an immediate clinical evaluation
ED Stroke Panel Page 1 of 2
 ED Stroke Panel Page 1 of 2 Reference EMMC *************************Usec: Call Operator to page a Stroke Alert ********************** Laboratory Bedside Glucose Monitoring ONCE Notify provider if glucose
ED Stroke Panel Page 1 of 2 Reference EMMC *************************Usec: Call Operator to page a Stroke Alert ********************** Laboratory Bedside Glucose Monitoring ONCE Notify provider if glucose
Patient Care Orders for CODE STROKE: alteplase Administration order set for Acute Ischemic Stroke less than 4.5 hours
 Allergy Alert: NO YES (Refer to Care-Area Administrative Data Screen in MEDITECH) Orders: The prescriber must check the tick box or complete the blank to activate the order. Any changes to be initialled
Allergy Alert: NO YES (Refer to Care-Area Administrative Data Screen in MEDITECH) Orders: The prescriber must check the tick box or complete the blank to activate the order. Any changes to be initialled
Stroke. Objectives: After you take this class, you will be able to:
 Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
AGWS Stroke Thrombolysis Clinical Profoma
 AGWS Stroke Thrombolysis Clinical Profoma Incorporating Salisbury NHS Foundation Trust guidance Date: On Arrival: Affix patient label here) GCS NIHSS Score: Pulse SaO on Air Give O only if < 95 % on Air
AGWS Stroke Thrombolysis Clinical Profoma Incorporating Salisbury NHS Foundation Trust guidance Date: On Arrival: Affix patient label here) GCS NIHSS Score: Pulse SaO on Air Give O only if < 95 % on Air
Case. Learning objectives. NIHSS values. Presenter Disclosure Information
 1:30 2:30 pm Primary Care of the Stroke Patient SPEAKER Thomas P. Bleck MD, MCCM, FNCS Presenter Disclosure Information The following relationships exist related to this presentation: Thomas P. Bleck,
1:30 2:30 pm Primary Care of the Stroke Patient SPEAKER Thomas P. Bleck MD, MCCM, FNCS Presenter Disclosure Information The following relationships exist related to this presentation: Thomas P. Bleck,
Table 3.1: Canadian Stroke Best Practice Recommendations Screening and Assessment Tools for Acute Stroke Severity
 Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Canadian Stroke Best Practices Table 3.3A Screening and Assessment Tools for Acute Stroke
 Canadian Stroke Best Practices Table 3.3A Screening and s for Acute Stroke Neurological Status/Stroke Severity assess mentation (level of consciousness, orientation and speech) and motor function (face,
Canadian Stroke Best Practices Table 3.3A Screening and s for Acute Stroke Neurological Status/Stroke Severity assess mentation (level of consciousness, orientation and speech) and motor function (face,
Pressure Ulcers ecourse
 Pressure Ulcers ecourse Module 4.1: Prevention of Pressure Ulcers Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Module
Pressure Ulcers ecourse Module 4.1: Prevention of Pressure Ulcers Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Module
Operation Stroke. How to Reduce the Risk of Stroke Complications
 Operation Stroke How to Reduce the Risk of Stroke Complications Objectives Focus on Acute Stroke as an active disease Discuss the most common stroke complications Describe how first 72 hours sets the stage
Operation Stroke How to Reduce the Risk of Stroke Complications Objectives Focus on Acute Stroke as an active disease Discuss the most common stroke complications Describe how first 72 hours sets the stage
Shands at the University of Florida Stroke Program
 Shands at the University of Florida Stroke Program The only Comprehensive Stroke Center in north central Florida as designated by the Florida Agency for Health Care Administration. To transfer a stroke
Shands at the University of Florida Stroke Program The only Comprehensive Stroke Center in north central Florida as designated by the Florida Agency for Health Care Administration. To transfer a stroke
Stroke in the Rural Setting: How You Can Make A Difference. Susie Fisher, RN, BSN Program Manager Providence Stroke Center Portland, OR
 Stroke in the Rural Setting: How You Can Make A Difference. Susie Fisher, RN, BSN Program Manager Providence Stroke Center Portland, OR Outline State Statistics The Oregon Problem Time & Treatments Steps
Stroke in the Rural Setting: How You Can Make A Difference. Susie Fisher, RN, BSN Program Manager Providence Stroke Center Portland, OR Outline State Statistics The Oregon Problem Time & Treatments Steps
ECMO Extracorporeal Membrane Oxygenation
 ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
DATA COLLECTION FORMS PARTICIPATING SITES
 Patient Identification Number: - DATA COLLECTION FORMS PARTICIPATING SITES VISIT 1: BASELINE Inclusion criteria known at time of randomisation Yes No 1. The patient received rt-pa thrombolysis treatment
Patient Identification Number: - DATA COLLECTION FORMS PARTICIPATING SITES VISIT 1: BASELINE Inclusion criteria known at time of randomisation Yes No 1. The patient received rt-pa thrombolysis treatment
Proof 2. CLINICAL PATHWAY PLAN CLINIQUE GENERAL SURGERY CHIRURGIE GÉNÉRAL Enhanced Recovery After Surgery (ERAS) Bowel Surgery /
 CLINICAL PATHWAY PLAN CLINIQUE GENERAL SURGERY CHIRURGIE GÉNÉRAL Enhanced Recovery After Surgery (ERAS) Bowel Surgery / Proof 2 Addressograph/Plaque Cancer Assessment Clinic (CAC) Date: yyaa mm dj Day
CLINICAL PATHWAY PLAN CLINIQUE GENERAL SURGERY CHIRURGIE GÉNÉRAL Enhanced Recovery After Surgery (ERAS) Bowel Surgery / Proof 2 Addressograph/Plaque Cancer Assessment Clinic (CAC) Date: yyaa mm dj Day
Person-centred Nursing Assessment and Plan of Care - Adult Inpatient Care Setting. Check identity PACE. Use addressograph-otherwise write in capitals
 Person-centred Nursing Assessment and Plan of Care - Adult Inpatient Care Setting PACE I would like to be called: First language: Interpreter required: Uses sign language: c British c Irish sign c Makaton
Person-centred Nursing Assessment and Plan of Care - Adult Inpatient Care Setting PACE I would like to be called: First language: Interpreter required: Uses sign language: c British c Irish sign c Makaton
Page 1 of 7. Intraparenchymal hemorrhage or subarachnoid hemorrhage. Consult neurosurgery
 Management of Acute Ischemic Stroke in Adult Patients INITIAL ASSESSMENT Look for signs and symptoms of stroke (see Appendix A) STAT finger stick glucose STAT 12-lead EKG Inform radiology that patient
Management of Acute Ischemic Stroke in Adult Patients INITIAL ASSESSMENT Look for signs and symptoms of stroke (see Appendix A) STAT finger stick glucose STAT 12-lead EKG Inform radiology that patient
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Information about Feeding Tubes
 Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
DIXIE REGIONAL ACUTE REHABILITATION UNIT TEAM CONFERENCE and INDIVIDUALIZED OVERALL PLAN OF CARE SUMMARY
 DIXIE REGIONAL ACUTE REHABILITATION UNIT TEAM CONFERENCE and INDIVIDUALIZED OVERALL PLAN OF CARE SUMMARY Conference Date: Rehab Admitting Diagnosis: Comorbid Conditions: Current Medical Prognosis: New
DIXIE REGIONAL ACUTE REHABILITATION UNIT TEAM CONFERENCE and INDIVIDUALIZED OVERALL PLAN OF CARE SUMMARY Conference Date: Rehab Admitting Diagnosis: Comorbid Conditions: Current Medical Prognosis: New
Suspected spinal cord compression form
 Suspected spinal cord compression form Enter this form into the notes at the appropriate date in the Progress / Evaluation sheets. Please copy this form to Lisa Lewis, Medical PA (ext 4551), for audit
Suspected spinal cord compression form Enter this form into the notes at the appropriate date in the Progress / Evaluation sheets. Please copy this form to Lisa Lewis, Medical PA (ext 4551), for audit
TENNESSEE STROKE REGISTRY QUARTERLY REPORT
 TENNESSEE STROKE REGISTRY QUARTERLY REPORT Volume 1, Issue 3 September 2018 This report is published quarterly using data from the Tennessee Stroke Registry. Inside this report Data on diagnosis, gender
TENNESSEE STROKE REGISTRY QUARTERLY REPORT Volume 1, Issue 3 September 2018 This report is published quarterly using data from the Tennessee Stroke Registry. Inside this report Data on diagnosis, gender
Functional Activity and Mobility
 Functional Activity and Mobility Documentation for Hospitalized Adult The Johns Hopkins University and The Johns Hopkins Health System Corporation Goals for Documentation of Activity and Mobility To develop
Functional Activity and Mobility Documentation for Hospitalized Adult The Johns Hopkins University and The Johns Hopkins Health System Corporation Goals for Documentation of Activity and Mobility To develop
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Esophagectomy Surgery
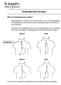 Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Patient Sticky Label. A Resource Guide for Stroke Survivors and their Caregivers
 A Resource Guide for Stroke Survivors and their Caregivers Patient Sticky Label An initiative of the Stroke Services Improvement (SSI) team in collaboration with all public hospitals in Singapore. Learning
A Resource Guide for Stroke Survivors and their Caregivers Patient Sticky Label An initiative of the Stroke Services Improvement (SSI) team in collaboration with all public hospitals in Singapore. Learning
Slide 1. Slide 2 Disclosure. Slide 3 Objectives. Functional Mobility and Activities of Daily Living: Assessing and Treating Patients in Rehabilitation
 Slide 1 Functional Mobility and Activities of Daily Living: Assessing and Treating Patients in Rehabilitation Terry Carolan, MSPT, NCS Slide 2 Disclosure Terry Carolan has no industry disclosures to make
Slide 1 Functional Mobility and Activities of Daily Living: Assessing and Treating Patients in Rehabilitation Terry Carolan, MSPT, NCS Slide 2 Disclosure Terry Carolan has no industry disclosures to make
How to prevent pressure ulcers
 How to prevent pressure ulcers Information for patients Find out more at 01522 511566 StBarnabasHospice.co.uk @StBarnabasLinc StBarnabasLinc Prevention is better than cure You have been given this information
How to prevent pressure ulcers Information for patients Find out more at 01522 511566 StBarnabasHospice.co.uk @StBarnabasLinc StBarnabasLinc Prevention is better than cure You have been given this information
Palliative Performance Scale (PPS)
 Palliative Performance Scale (PPS) Description The Palliative Performance Scale is a reliable and valid tool used for assessing a patient s functional status. PPS was developed by Victoria Hospice Society,
Palliative Performance Scale (PPS) Description The Palliative Performance Scale is a reliable and valid tool used for assessing a patient s functional status. PPS was developed by Victoria Hospice Society,
Please FAX completed form to : Admission request: Immediate ADMISSION REFERRAL TO HOSPICE RENFREW
 Please FAX completed form to : 613-432-3618 Admission request: Immediate ADMISSION REFERRAL TO HOSPICE RENFREW Future Pain and symptom management Referral Principles -Completion of this referral is a request
Please FAX completed form to : 613-432-3618 Admission request: Immediate ADMISSION REFERRAL TO HOSPICE RENFREW Future Pain and symptom management Referral Principles -Completion of this referral is a request
V2.1 Cluster 2 Acute Care to Rehab & Complex Continuing Care (CCC) Referral
 Referral Destination Referral to Rehab: (Please check one) HTSD / Regular stream LTLD/slowstream Either (Receiving facility to determine) Referral to Complex Continuing Care (CCC) (For LTLD / slowstream
Referral Destination Referral to Rehab: (Please check one) HTSD / Regular stream LTLD/slowstream Either (Receiving facility to determine) Referral to Complex Continuing Care (CCC) (For LTLD / slowstream
STROKE INTRODUCTION OBJECTIVES. When the student has finished this module, he/she will be able to:
 STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. There are two types of stroke, but both types of stroke cause the same type of
STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. There are two types of stroke, but both types of stroke cause the same type of
Stroke: clinical presentations, symptoms and signs
 Stroke: clinical presentations, symptoms and signs Professor Peter Sandercock University of Edinburgh EAN teaching course Burkina Faso 8 th November 2017 Clinical diagnosis is important to Ensure stroke
Stroke: clinical presentations, symptoms and signs Professor Peter Sandercock University of Edinburgh EAN teaching course Burkina Faso 8 th November 2017 Clinical diagnosis is important to Ensure stroke
Pediatric Intensive Care Unit (PICU) Pediatric Diabetic Ketoacidosis (DKA) Admission Order Set
 Discontinue all previous orders Weight: kg DKA admit order set is for initial management Ongoing management required based on frequent reassessment of TFI, fluid balance and lab results. Admit to PICU
Discontinue all previous orders Weight: kg DKA admit order set is for initial management Ongoing management required based on frequent reassessment of TFI, fluid balance and lab results. Admit to PICU
Rehab to Home. Stroke Recovery EDUCATION BOOKLET FOR: Care & Safety Tips. Frequently Asked Questions. Working Toward Independence. Adaptive Equipment
 Stroke Recovery Rehab to Home Care & Safety Tips Frequently Asked Questions Working Toward Independence Adaptive Equipment Summary of Progress Different Types of Therapy Personal Goals EDUCATION BOOKLET
Stroke Recovery Rehab to Home Care & Safety Tips Frequently Asked Questions Working Toward Independence Adaptive Equipment Summary of Progress Different Types of Therapy Personal Goals EDUCATION BOOKLET
PATIENT S NOTES History and Physical Brain Attack Stroke
 UNIVERSITY HOSPITALS OF CLEVELAND PATIENT S NOTES History and Physical Brain Attack Stroke 040527.01 page 1 of 8 Name Hospital # Date Sex Age Dr. Service Division Rm No Date and Time: Current inpatient
UNIVERSITY HOSPITALS OF CLEVELAND PATIENT S NOTES History and Physical Brain Attack Stroke 040527.01 page 1 of 8 Name Hospital # Date Sex Age Dr. Service Division Rm No Date and Time: Current inpatient
ABNORMAL STROKE EXAM FINDINGS:
 Stroke Assessment Scenario Case Information PATIENT INFORMATION: 68-year-old male patient complaining of left sided weakness and an unsteady gait. Reported last normal time 3 minutes prior to EMS arrival
Stroke Assessment Scenario Case Information PATIENT INFORMATION: 68-year-old male patient complaining of left sided weakness and an unsteady gait. Reported last normal time 3 minutes prior to EMS arrival
Sample. Fractured Hip Post-Operative Orders. Legend < Mandatory fields o Optional fields. Height Allergies: List or o Up to date in electronic system
 Legend Mandatory fields o Optional fields Height Allergies: List or o Up to date in electronic system cm Weight Diagnosis kg Date (yyyy-mon-dd) Time (hh:mm) Anticipated Date Of Discharge (ADOD) o Greater
Legend Mandatory fields o Optional fields Height Allergies: List or o Up to date in electronic system cm Weight Diagnosis kg Date (yyyy-mon-dd) Time (hh:mm) Anticipated Date Of Discharge (ADOD) o Greater
Primary Stroke Center Acute Stroke Transfer Guidelines When to Consider a Transfer:
 When to Consider a Transfer: Hemorrhagic Stroke Large volume intracerebral hematoma greater than 5cm on CT Concern for expanding hematoma Rapidly declining mental status, especially requiring intubation
When to Consider a Transfer: Hemorrhagic Stroke Large volume intracerebral hematoma greater than 5cm on CT Concern for expanding hematoma Rapidly declining mental status, especially requiring intubation
LSU Health Sciences Center
 LSU Health Sciences Center Speech-Language-Hearing Clinic, Department of Communication Disorders, School of Allied Health Professions, 1900 Gravier Street, 9 th Floor, New Orleans, La 70112 Date: Identification
LSU Health Sciences Center Speech-Language-Hearing Clinic, Department of Communication Disorders, School of Allied Health Professions, 1900 Gravier Street, 9 th Floor, New Orleans, La 70112 Date: Identification
Diagnosis: Allergies with reaction type:
 Patient Name: Diagnosis: Allergies with reaction type: ICU Stroke-Ischemic S/P tpa Version 2 5/29/14 This order set is designed to be used with an admission set or for a patient already admitted Nursing
Patient Name: Diagnosis: Allergies with reaction type: ICU Stroke-Ischemic S/P tpa Version 2 5/29/14 This order set is designed to be used with an admission set or for a patient already admitted Nursing
Stroke: The First Critical Hour. Alina Candal, RN, PCC, MICN Kevin Andruss, MD, FACEP
 Stroke: The First Critical Hour Alina Candal, RN, PCC, MICN Kevin Andruss, MD, FACEP Disclosures We have no actual or potential conflicts of interest in relation to this presentation. Objectives Discuss
Stroke: The First Critical Hour Alina Candal, RN, PCC, MICN Kevin Andruss, MD, FACEP Disclosures We have no actual or potential conflicts of interest in relation to this presentation. Objectives Discuss
The in-hospital management of COPD-exacerbation includes three core processes:
 Appendix 1A. Process flow for in-hospital management of COPDexacerbation The in-hospital management of COPD-exacerbation includes three core processes: 1. Diagnostic assessment 2. Pharmacological management
Appendix 1A. Process flow for in-hospital management of COPDexacerbation The in-hospital management of COPD-exacerbation includes three core processes: 1. Diagnostic assessment 2. Pharmacological management
TABLE OF CONTENTS. MODULE 1: Pathophysiology of Stroke, Neuroanatomy, and Stroke Syndromes. MODULE 2: Acute Stroke Management
 TABLE OF CONTENTS Orientation Pre-Test (ONLINE ONLY) i. Acknowledgements ii. Acute Stroke Unit Orientation Introduction iii. Nursing/Interprofessional (Self Evaluation Tool) MODULE 1: Pathophysiology of
TABLE OF CONTENTS Orientation Pre-Test (ONLINE ONLY) i. Acknowledgements ii. Acute Stroke Unit Orientation Introduction iii. Nursing/Interprofessional (Self Evaluation Tool) MODULE 1: Pathophysiology of
HNHB LHIN COMPLEX CARE INPATIENT ADMISSION APPLICATION
 Complex Care is a specialized, time-limited program providing patients with complex medical conditions who require a hospital stay with ongoing onsite assessment and active care by an interprofessional
Complex Care is a specialized, time-limited program providing patients with complex medical conditions who require a hospital stay with ongoing onsite assessment and active care by an interprofessional
Code Stroke in real life. Disclosures. Parkland Memorial Hospital. I have no disclosures. Has 1 million patient visits annually. Level 1 Trauma Center
 Code Stroke in real life Alejandro Magadán, M.D. University of Texas Southwestern Medical Center Medical Director for Stroke Parkland Memorial Hospital Disclosures I have no disclosures Parkland Memorial
Code Stroke in real life Alejandro Magadán, M.D. University of Texas Southwestern Medical Center Medical Director for Stroke Parkland Memorial Hospital Disclosures I have no disclosures Parkland Memorial
MAJOR TRAUMA REHABILITATION PRESCRIPTION
 MAJOR TRAUMA REHABILITATION PRESCRIPTION Core Information Date Commenced: Time Commenced: Commenced By: GP: Date of Injury: Insert label or: Surname: First Name: MTC: Current Location: Date of Birth: Key
MAJOR TRAUMA REHABILITATION PRESCRIPTION Core Information Date Commenced: Time Commenced: Commenced By: GP: Date of Injury: Insert label or: Surname: First Name: MTC: Current Location: Date of Birth: Key
Test your Knowledge: Recognizing Delirium
 The Ottawa Hospital Name: Unit: Profession: RN RPN PT OT SW Other Note: Each question has only one correct answer. 1. If a patient is identified as being at high risk for developing delirium, his/her mental
The Ottawa Hospital Name: Unit: Profession: RN RPN PT OT SW Other Note: Each question has only one correct answer. 1. If a patient is identified as being at high risk for developing delirium, his/her mental
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Canadian Best Practice Recommendations for Stroke Care. (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management
 Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Apply Label. Page 1 of 7 VALLEY REGIONAL HOSPITAL - KARDEX. Patient Profile: Pt Name: Date Adm to Med/Surg Unit: Physician: Covering/alternate:
 VALLEY REGIONAL HOSPITAL - KARDEX Patient Profile: Pt Name: Date Adm to Med/Surg Unit: Physician: Covering/alternate: Diagnosis Apply Label ALLERGIES: Order entry Y N Admission Ht: Wt: Order entry Y N
VALLEY REGIONAL HOSPITAL - KARDEX Patient Profile: Pt Name: Date Adm to Med/Surg Unit: Physician: Covering/alternate: Diagnosis Apply Label ALLERGIES: Order entry Y N Admission Ht: Wt: Order entry Y N
Nursing Management Plan Small or large bowel
 Nursing Management Plan Small or large bowel Highlight the procedure/s and add other details: Open / Laparoscopic Assisted Hemicolectomy / Right / Left / Extended Sigmoid Colectomy / Transverse Colectomy
Nursing Management Plan Small or large bowel Highlight the procedure/s and add other details: Open / Laparoscopic Assisted Hemicolectomy / Right / Left / Extended Sigmoid Colectomy / Transverse Colectomy
ND STROKE Coordinators Case Studies. STEMI and Stroke Conference, Fargo, ND, August 5, 2014
 ND STROKE Coordinators Case Studies STEMI and Stroke Conference, Fargo, ND, August 5, 2014 STROKE Coordinator Case Study Essentia Health, Fargo Essentia Health Stroke Alert Process Within 24 hours of Last
ND STROKE Coordinators Case Studies STEMI and Stroke Conference, Fargo, ND, August 5, 2014 STROKE Coordinator Case Study Essentia Health, Fargo Essentia Health Stroke Alert Process Within 24 hours of Last
TABLE OF CONTENTS. Page TAB 1. Overview of Resident Assessment Process 6. RAP REVIEW or Working the RAP Steps 10
 TABLE OF CONTENTS Page TAB 1 Overview of Resident Assessment Process 6 RAP REVIEW or Working the RAP Steps 10 Working the RAPS & Documentation Systems 2 TAB 2 RAP Key 31 RAP Training Guidelines and care
TABLE OF CONTENTS Page TAB 1 Overview of Resident Assessment Process 6 RAP REVIEW or Working the RAP Steps 10 Working the RAPS & Documentation Systems 2 TAB 2 RAP Key 31 RAP Training Guidelines and care
(Page 1 of 5) Diagnosis: Procedure: Right Total Knee Replacement Unicompartmental Knee Left Total Hip Revision Total Shoulder
 (Page 1 of 5) Allergies/Sensitivities/Reactions: Height: Inches cm Weight: Kg Pounds = Automatic = Physician s option, Check off to Order Diagnosis: Procedure: Right Total Knee Replacement Unicompartmental
(Page 1 of 5) Allergies/Sensitivities/Reactions: Height: Inches cm Weight: Kg Pounds = Automatic = Physician s option, Check off to Order Diagnosis: Procedure: Right Total Knee Replacement Unicompartmental
NORTHWICK PARK DEPENDENCY SCORE
 NORTHWICK PARK DEPENDENCY SCORE PATIENT DETAILS: Surname:... Forename(s):... Hosp No:... Sex: Male/Female Date of birth:... Diagnosis:... NHS No:. OCCASION: Admission / Fortnightly review /Discharge Date
NORTHWICK PARK DEPENDENCY SCORE PATIENT DETAILS: Surname:... Forename(s):... Hosp No:... Sex: Male/Female Date of birth:... Diagnosis:... NHS No:. OCCASION: Admission / Fortnightly review /Discharge Date
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
nicheprogram.org 16th Annual NICHE Conference Forging New Paths and Partnerships 1
 Improving Patient Outcomes in Geriatric Post-Operative Orthopedic Patients: Translating Research into Practice Tripping into The CAM Presented by: Diana LaBumbard, RN, MSN, ACNP/GNP-BC, CWOCN Denise Williams,
Improving Patient Outcomes in Geriatric Post-Operative Orthopedic Patients: Translating Research into Practice Tripping into The CAM Presented by: Diana LaBumbard, RN, MSN, ACNP/GNP-BC, CWOCN Denise Williams,
Your Care in the Hospital
 ilearning about your health Stroke (Brain Attack) Your Care in the Hospital www.cpmc.org/learning Your Care in the Hospital What is a Stroke (Brain Attack)? A stroke (brain attack) happens when a blood
ilearning about your health Stroke (Brain Attack) Your Care in the Hospital www.cpmc.org/learning Your Care in the Hospital What is a Stroke (Brain Attack)? A stroke (brain attack) happens when a blood
GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE
 2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
Course Handouts & Post Test
 STROKE/COMA: DISEASE TRAJECTORY AND HOSPICE ELIGIBILITY Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Hospice Education Network Course Handouts & Post Test To download presentation
STROKE/COMA: DISEASE TRAJECTORY AND HOSPICE ELIGIBILITY Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Hospice Education Network Course Handouts & Post Test To download presentation
STROKE POSITIONING, TRANSFERRING & SHOULDER MANAGEMENT IN ACUTE AND REHAB
 STROKE POSITIONING, TRANSFERRING & SHOULDER MANAGEMENT IN ACUTE AND REHAB PRESENTED BY: Francine Carrier-Stevens, PT. Natasha Uens, PT. Chelsea Foster, RN. OVERVIEW Objectives Factors affecting mobility
STROKE POSITIONING, TRANSFERRING & SHOULDER MANAGEMENT IN ACUTE AND REHAB PRESENTED BY: Francine Carrier-Stevens, PT. Natasha Uens, PT. Chelsea Foster, RN. OVERVIEW Objectives Factors affecting mobility
NUTRITION CARE ALERTS
 APPENDIX 10 A NUTRITION CARE ALERTS and for Caregivers in Nursing Facilities or at Home Proper nutrition care is vital to the health and well-being of nursing facility residents and seniors living in their
APPENDIX 10 A NUTRITION CARE ALERTS and for Caregivers in Nursing Facilities or at Home Proper nutrition care is vital to the health and well-being of nursing facility residents and seniors living in their
Standards of excellence
 The Accreditation Canada Stroke Distinction program was launched in March 2010 to offer a rigorous and highly specialized process above and beyond the requirements of Qmentum. The comprehensive Stroke
The Accreditation Canada Stroke Distinction program was launched in March 2010 to offer a rigorous and highly specialized process above and beyond the requirements of Qmentum. The comprehensive Stroke
ALL orders are active unless: 1. Order is manually lined through to inactivate 2. Orders with check boxes ( ) are unchecked DRUG AND TREATMENT ORDERS
 DRUG AND TREATMENT Available at: BMC-B BMC-D BMC-N BMC-S Vital Signs Vital Signs Q4H (DEF)* Q2H Q1H Vital Signs Orthostatic Activity Activity Bedrest, for 12 hours then Up ad lib (DEF)* Bedrest, for 24
DRUG AND TREATMENT Available at: BMC-B BMC-D BMC-N BMC-S Vital Signs Vital Signs Q4H (DEF)* Q2H Q1H Vital Signs Orthostatic Activity Activity Bedrest, for 12 hours then Up ad lib (DEF)* Bedrest, for 24
Admit date (YYYY/MM/DD): Cardiologist On-Call: Diagnosis: Lab Tests. CBC, Electrolytes, Urea, Creatinine, Glucose, INR, PTT, Urinalysis
 of nurse 1. Admit under ward Attending Physician: Dr. Admit date (YYYY/MM/DD): Cardiologist On-Call: Diagnosis: Lab Tests 2. On admission (if not already performed in Emergency Department or in Coronary
of nurse 1. Admit under ward Attending Physician: Dr. Admit date (YYYY/MM/DD): Cardiologist On-Call: Diagnosis: Lab Tests 2. On admission (if not already performed in Emergency Department or in Coronary
Urinary dysfunction assessment tool (community)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Primary Stroke Center Quality & Performance Measures
 Primary Stroke Center Quality & Performance Measures This section of the manual contains information related to the quality performance of Primary Stroke Centers. Brain Attack Coalition Definitions Recognition
Primary Stroke Center Quality & Performance Measures This section of the manual contains information related to the quality performance of Primary Stroke Centers. Brain Attack Coalition Definitions Recognition
The road to recovery. The support available to help you with your recovery after stroke
 The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Need to talk? Call our confidential Stroke Helpline on 0303 3033
The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Need to talk? Call our confidential Stroke Helpline on 0303 3033
Objectives. Stroke Facts 2/27/2015. EMS in Stroke Care: A Critical Partnership
 EMS in Stroke Care: A Critical Partnership Spokane County EMS Objectives Identify the types and time limitations for acute ischemic stroke treatment options Identify the importance of early identification
EMS in Stroke Care: A Critical Partnership Spokane County EMS Objectives Identify the types and time limitations for acute ischemic stroke treatment options Identify the importance of early identification
Heart of England Foundation Trust ACUTE STROKE PATHWAY EMERGENCY DEPARTMENT ATTACHMENTS
 STROKE Name: PID: DOB: Consultant: Heart of England Foundation Trust ACUTE STROKE PATHWAY EMERGENCY DEPARTMENT ATTACHMENTS November 2010 TIME IS BRAIN SUSPECTED STROKE Onset Within 6 Hours? (FAST TEST
STROKE Name: PID: DOB: Consultant: Heart of England Foundation Trust ACUTE STROKE PATHWAY EMERGENCY DEPARTMENT ATTACHMENTS November 2010 TIME IS BRAIN SUSPECTED STROKE Onset Within 6 Hours? (FAST TEST
Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF)
 Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF) About your condition The pressure from your bulging disc(s) might be causing your pain, numbness or weakness.
Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF) About your condition The pressure from your bulging disc(s) might be causing your pain, numbness or weakness.
Venous Thromboembolism National Hospital Inpatient Quality Measures
 Venous Thromboembolism National Hospital Inpatient Quality Measures Presentation Overview Review venous thromboembolism as a new mandatory measure set Outline measures with exclusions and documentation
Venous Thromboembolism National Hospital Inpatient Quality Measures Presentation Overview Review venous thromboembolism as a new mandatory measure set Outline measures with exclusions and documentation
DRUG ALLERGIES WT: KG
 DRUG AND TREATMENT Available at: BMC-B BMC-D BMC-N BMC-S Vital Signs Vital Signs Q4H (DEF)* Q2H Q1H Vital Signs Orthostatic Activity Activity Bedrest, for 12 hours then Up ad lib (DEF)* Bedrest, for 24
DRUG AND TREATMENT Available at: BMC-B BMC-D BMC-N BMC-S Vital Signs Vital Signs Q4H (DEF)* Q2H Q1H Vital Signs Orthostatic Activity Activity Bedrest, for 12 hours then Up ad lib (DEF)* Bedrest, for 24
In order to receive the maximum benefit from your rehabilitation program, it is important to understand and comply with the following guidelines:
 Arrival Policy 900 2 nd Ave., Madison, MN 56256 In order to receive the maximum benefit from your rehabilitation program, it is important to understand and comply with the following guidelines: Attend
Arrival Policy 900 2 nd Ave., Madison, MN 56256 In order to receive the maximum benefit from your rehabilitation program, it is important to understand and comply with the following guidelines: Attend
Appendix 3: Specialist Rehabilitation Prescription Proforma (example).
 Appendix 3: Specialist Rehabilitation Prescription Proforma (example). For patients with complex rehabilitation needs requiring Specialist (Level 1 or 2) Rehab services. The specialist rehabilitation Prescription
Appendix 3: Specialist Rehabilitation Prescription Proforma (example). For patients with complex rehabilitation needs requiring Specialist (Level 1 or 2) Rehab services. The specialist rehabilitation Prescription
Understanding late stage dementia Understanding dementia
 Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
PATIENT CARE MANUAL POLICY
 PATIENT CARE MANUAL POLICY NUMBER #VII-F-20 PAGE 1 OF 2 APPROVED BY: CATEGORY: Senior Vice President, Medicine and Chief of Staff; Vice President and Senior Operating Officer, Covenant Health, Rural Health
PATIENT CARE MANUAL POLICY NUMBER #VII-F-20 PAGE 1 OF 2 APPROVED BY: CATEGORY: Senior Vice President, Medicine and Chief of Staff; Vice President and Senior Operating Officer, Covenant Health, Rural Health
URN: Family name: Given name(s): Address: Initial Signature Print Name Role
 Do Not Write in this binding margin v5.00-02/2012 Mat. No.: 10206019 SW030b The State of Queensland (Queensland Health) 2012 Contact CIM@health.qld.gov.au ÌSW030bIÎ Facility: s Never Replace Clinical Judgement
Do Not Write in this binding margin v5.00-02/2012 Mat. No.: 10206019 SW030b The State of Queensland (Queensland Health) 2012 Contact CIM@health.qld.gov.au ÌSW030bIÎ Facility: s Never Replace Clinical Judgement
The Language of Stroke
 The Language of Stroke Examination / Imaging / Diagnosis / Treatment Dr Suzanne Busch A lot of letters! CBF CVA ICH CVD CBV DWI US MRI/MRA CAA CTA CTP ICA MCA SAH WMD TIA MCA Agnosia A lot of big words!
The Language of Stroke Examination / Imaging / Diagnosis / Treatment Dr Suzanne Busch A lot of letters! CBF CVA ICH CVD CBV DWI US MRI/MRA CAA CTA CTP ICA MCA SAH WMD TIA MCA Agnosia A lot of big words!
Department of Physical Medicine and Rehabilitation
 For enquiries and appointments, please contact us at: 物理醫學及復康科部 Department of Physical Medicine and Rehabilitation Department of Physical Medicine and Rehabilitation 5/F, Li Shu Pui Block, Hong Kong Sanatorium
For enquiries and appointments, please contact us at: 物理醫學及復康科部 Department of Physical Medicine and Rehabilitation Department of Physical Medicine and Rehabilitation 5/F, Li Shu Pui Block, Hong Kong Sanatorium
Section K Swallowing/ Nutritional Status
 Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
IDPH EMS Region Five. Stroke Education
 IDPH EMS Region Five Stroke Education Time is Brain!!!!! Time is Brain!!!! Stroke refers to any spontaneous damage to the brain caused by an abnormality of the blood supply by means of a clot or bleed.
IDPH EMS Region Five Stroke Education Time is Brain!!!!! Time is Brain!!!! Stroke refers to any spontaneous damage to the brain caused by an abnormality of the blood supply by means of a clot or bleed.
VENOUS THROMBOEMBOLISM (VTE) PREVENTION MEDICAL PROVIDER EDUCATION JUNE 2017
 VENOUS THROMBOEMBOLISM (VTE) PREVENTION MEDICAL PROVIDER EDUCATION JUNE 2017 VTE IS THE 2 ND MOST COMMON HOSPITAL ACQUIRED CONDITION RISK FACTORS DECREASED ACTIVITY = VTE RISK (NURSES MEASURE WITH BRADEN
VENOUS THROMBOEMBOLISM (VTE) PREVENTION MEDICAL PROVIDER EDUCATION JUNE 2017 VTE IS THE 2 ND MOST COMMON HOSPITAL ACQUIRED CONDITION RISK FACTORS DECREASED ACTIVITY = VTE RISK (NURSES MEASURE WITH BRADEN
TIA AND STROKE. Topics/Order of the day 1. Topics/Order of the day 2 01/08/2012
 Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
About Your Ventricular Assist Device (VAD) Surgery
 About Your Ventricular Assist Device (VAD) Surgery Why do I need surgery for a Heart Pump or Ventricular Assist Device (VAD)? VAD s may help you live longer. These electric powered heart pumps are put
About Your Ventricular Assist Device (VAD) Surgery Why do I need surgery for a Heart Pump or Ventricular Assist Device (VAD)? VAD s may help you live longer. These electric powered heart pumps are put
