Indian Journal of Endocrinology & Metabolism
|
|
|
- Rafe Booker
- 6 years ago
- Views:
Transcription
1 Spine 6.5 mm ISSN Vol. 20 Issue 5 September-October 2016 Indian Journal of Endocrinology and Metabolism Indian Journal of Endocrinology & Metabolism Volume 20 Issue 5 September-October 2016 Pages Official Publication of Endocrine Society of India
2 Original Article Clinical and laboratory profile of primary hyperparathyroidism in Kashmir Valley: A single center experience Raiz Ahmad Misgar, Parvez Mohiuddin Dar 1, Shariq Rashid Masoodi, Munir Ahmad 1, Khursheed Alam Wani 1, Arshad Iqbal Wani, Mir Iftikhar Bashir Departments of Endocrinology and 1 General Surgery, Sher i Kashmir Institute of Medical Sciences, Srinagar, Jammu and Kashmir, India ABSTRACT Background: Although primary hyperparathyroidism (PHPT) has become an asymptomatic disease in the West, in India, PHPT is still an uncommonly diagnosed, overtly symptomatic disease with skeletal, muscular, and renal manifestations. Aims: To describe the profile and surgical outcome of 78 consecutive PHPT patients over a period of two decades at a single center. Materials and Methods: All patients who underwent evaluation and surgery for PHPT from January 1996 to December 2015 were included. Evaluation included measurement of serum total calcium, inorganic phosphorus, alkaline phosphatase, intact parathyroid hormone, 25 hydroxy Vitamin D, 24 hour urinary calcium and radiological survey. Ultrasonography neck and technetium 99m sestamibi scan were used for preoperative localization. Results: A total of 78 patients were identified during the two decades of whom 29 patients were studied retrospectively and 49 patients prospectively. Mean age of patients was ± 12.46, and male:female ratio was 1:6. The most common presenting features were nephrolithiasis and/or nephrocalcinosis (64.10%), bone pain (44.1%), abdominal pain (39%), constipation (26%), and myopathy (14.10%). Fractures were present only in 10.25%, and brown tumors in 6.41% patients. The cure rate in our series was 96.15%. The mean parathyroid gland weight was 2.05 ± 3.03 g. None of the 41 patients in whom long term follow up was available, had recurrence of PHPT. Conclusions: The profile of PHPT is changing with older age at presentation, and emergence of renal stone disease and decline in overt skeletal disease as common presentation. The parathyroid weight in our study resembles that reported from developed countries. Key words: Fractures, hypercalcemia, nephrolithiasis, parathyroid adenoma, primary hyperparathyroidism Introduction Primary hyperparathyroidism (PHPT) is a disease characterized by hypercalcemia due to autonomous production of parathyroid hormone (PTH). The classic description of PHPT was given by Albright et al., about Corresponding Author: Dr. Shariq Rashid Masoodi, Department of Endocrinology, Sher i Kashmir Institute of Medical Sciences, Srinagar, Jammu and Kashmir, India. E mail: shariq.masoodi@gmail.com Quick Response Code: Access this article online Website: DOI: / years ago. [1] PHPT is the third most common endocrine disorder in the West after diabetes mellitus and thyroid disorders. [2] Overall, about 1% of the adults have PHPT in the West, and this figure rises to 2% in people older than 55 years. [3] With the advent of multichannel biochemical screening in the 1970s, the incidence of PHPT increased around the world. The clinical profiles of PHPT remarkably differ with regions of the world. In developing countries, such as India, PHPT is still uncommonly diagnosed, overtly symptomatic disease with skeletal, muscular, This is an open access article distributed under the terms of the Creative Commons Attribution NonCommercial ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non commercially, as long as the author is credited and the new creations are licensed under the identical terms. For reprints contact: reprints@medknow.com Cite this article as: Misgar RA, Dar PM, Masoodi SR, Ahmad M, Wani KA, Wani AI, et al. Clinical and laboratory profile of primary hyperparathyroidism in Kashmir Valley: A single-center experience. Indian J Endocr Metab 2016;20: Indian Journal of Endocrinology and Metabolism Published by Wolters Kluwer - Medknow
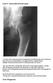
3 and renal manifestations. [4 7] In contrast, PHPT has become an asymptomatic disease in the West with classic manifestations seen only in 2% cases nowadays. [8] In this study, we describe the clinical characteristics, biochemical profile, and outcome of 78 patients with PHPT seen over a period of two decades at a single center from the Kashmir valley. Materials and Methods All patients who underwent evaluation and surgery for PHPT from January 1996 to December 2015 at Sher i Kashmir Institute of Medical Sciences were included in the study. A total of 78 patients were identified during the two decades, of whom 29 patients were studied retrospectively ( ) and remaining 49 patients were studied prospectively ( ). The diagnosis of PHPT was based on the following: (i) persistent elevation of serum calcium above the upper limit of normal range (10.5 mg/ dl); (ii) increased intact PTH (ipth); and (iii) histological evidence (after parathyroid surgery) of parathyroid adenoma or hyperplasia. Evaluation of the patients included the measurement of serum total calcium, inorganic phosphorus, total alkaline phosphatase (ALP), ipth, 25 hydroxy Vitamin D (25 OHD), serum albumin, and 24 hour urinary calcium and creatinine. Serum total calcium, inorganic phosphorus, total ALP, and serum creatinine were measured by automated techniques. The normal laboratory range was mg/dl for total serum calcium, mg/dl for serum phosphorus, and IU/L for serum ALP. Radiological survey of hands, skull, lumbar spine, pelvis, and any other suspected or known site of fracture was performed. Imaging studies for localization of parathyroid adenoma included ultrasonography (USG) neck and technetium 99m ( 99m Tc) sestamibi scan. Serum ipth was measured by chemiluminescent immunometric assay and serum 25 OHD was measured by radioimmunoassay. Vitamin D deficiency was defined as serum 25 OHD level <20 ng/ml. [9] Parathyroid surgery In patients in whom a single parathyroid adenoma was localized on 99m Tc sestamibi scan, unilateral neck exploration was performed with removal of the adenoma. Patients with doubtful lesion or nonlocalized lesions underwent bilateral neck exploration, and all parathyroid glands were examined with the removal of 3½ glands. Statistical analysis Statistical analysis was done on PC Windows using Statistical Package for Social Sciences (SPSS), version , from SPSS Inc.,Chicago IL. The results were expressed as percentage or mean ± standard deviation, as specified. Pearson s Chi square method was used for comparing proportions and percentages, whereas Student s t test was used for comparing continuous variables. ANOVA was used wherever needed. Where the data were not uniformly distributed nonparametric test such as Mann Whitney U test, Kolmogorov Smirnov Z test, or Kruskal Wallis H test was used. A P < 0.05 was taken as statistically significant. Results The clinical characteristics of patients are shown in Table 1. An overwhelming majority (67/78; 85.7%) of the patients were females giving a male: female ratio of 1:6. The mean age of patients was ± with a median of 45 years and a range of years. Nephrolithiasis and/or nephrocalcinosis [Figure 1] was the most common presentation, seen in 50 (64.10%) patients followed by bone pain in 26 (44.1%), abdominal pain in 24 (39%), constipation in 16 (26%), and myopathy in 11 (14.10%). Seven (8.97%) patients manifested psychiatric abnormalities. A parathyroid nodule was Table 1: Clinical characteristics of 78 patients with primary hyperparathyroidism Variable Frequency (%) Age (years), mean (SD) (12.46) Male:female ratio 1:6 Clinical/radiological feature Nephrolithiasis 50 (64.10) Bone pains 26 (44.10) Abdominal pain 24 (39) Constipation 16 (26) Proximal muscle weakness 11 (14.10) Polyuria and polydipsia 9 (11.54) Fractures 8 (10.25) Psychiatric abnormalities 7 (8.97) Graveluria 6 (7.69) Pancreatitis 3 (4.41) Sub periosteal resorption 16 (20.51) Salt pepper skull 15 (19.23) Brown tumors 5 (6.41) SD: Standard deviation a Figure 1: (a) Radiograph of abdomen showing extensive bilateral nephrolithiasis; (b) striking improvement after successful parathyroid surgery b Indian Journal of Endocrinology and Metabolism / Sep-Oct 2016 / Vol 20 Issue 5 697
4 palpable in three patients. Skeletal involvement (osteopenia, sub periosteal resorption, pathological fractures, salt and pepper appearance of skull, brown tumors) was present in 31 (39.74%) patients; 8 (10.25%) had fractures [Figure 2]. About one fourth (19; 24.38%) of our patients had both renal and skeletal manifestations. Out of fifty patients with nephrolithiasis, 15 (30%) had a past history of at least one surgery for renal stones prior to the diagnosis of PHPT, and another four patients had received extracorporeal shock wave lithotripsy at least once prior to diagnosis of PHPT. The biochemical variables of the patients are shown in Table 2. All patients had hypercalcemia. The mean serum calcium level was 12.5 ± 1.7 mg/dl, (median12, range ). The mean serum ipth level was ± pg/ml (median 224.5, range ). Hypophosphatemia (serum inorganic phosphorus < 2.5 mg/dl) was documented in 54 (69.23%) patients. The mean serum inorganic phosphorus level was 2.2 ± 0.6 mg/dl (median 2.2). Hypercalciuria (24 h urinary calcium 4 mg/kg) was present in 41 (52.56%) patients. The serum total ALP was elevated (>140 IU/L) in 40 (51.28%) patients. The mean serum ALP was ± IU/L (median 154). a Figure 2: Radiograph showing advanced bone disease. (a) Fracture of femur; (b) brown tumor of tibia Table 2: Biochemical variables of 78 patients with primary hyperparathyroidism Variable Mean (SD) Median (range) Serum calcium 12.5 (1.7) 12 ( ) Serum phosphate (mg/dl) 2.2 (0.6) 2.2 ( ) Serum ALP (U/L) (336.8) 154 ( ) Serum ipth (pg/ml) (386.1) ( ) Serum 25 OHD (ng/ml) 37.2 (58.1) 22.8 ( ) ALP: Alkaline phosphatase, 25 OHD: 25 hydroxyvitamin D, ipth: Intact parathyroid hormone, SD: Standard deviation b Serum 25 OHD was available for 54 patients. The mean 25 OHD level was 37.2 ± 58.1 ng/ml (median 22.8, range ). Vitamin D deficiency was present in 38% patients. We did not find any correlation between Vitamin D status and biochemical parameters (serum calcium and ipth) or adenoma weight. A few of our patients had rare and unusual features. There was clinical suspicion of multiple endocrine neoplasia 1 (MEN 1) in 3 patients. Two females; aged 25 and 23 years had PHPT and microprolactinoma, whereas a 58 year old female patient had PHPT and acromegaly. Two of our patients had associated adrenal incidentalomas causing sub clinical Cushing s syndrome in one of them. A 27 year old female patient presented in postpartum period with nephrogenic diabetes insipidus as the sole manifestation of PHPT, which settled immediately after parathyroid surgery. All our patients underwent USG neck and Tc 99m sestamibi scan for localization of parathyroid adenoma. In our series, the sensitivity of USG and Tc 99m sestamibi scan for the localization of adenoma was 89.8% and 95.3%, respectively. Operative findings and pathological features At the time of surgery, single adenoma was involved in 69 (88.46%) double adenomas in 6 (8.57%) and more than 2 gland involvement in 3 (4.28%) patients. Among the 69 patients with single adenoma, right inferior gland was involved most often (40; 57.97%), followed by left inferior (22; 31.88%) and right superior (7; 0.14%); none of the patients had involvement of left superior gland. On histopathology, adenoma was found in 75 (94.44%), hyperplasia in 3 (3.79%) patients. There was no case of parathyroid carcinoma. The mean parathyroid gland weight was 2.05 ± 3.03 g (median 1.05; range ). Using Pearson s correlation coefficient, the mean parathyroid gland weight showed a strong correlation with serum calcium and ipth. Postoperative course The mean postoperative serum ipth level was 61.8 ± 43.8 pg/ml (range: ). Postoperative hungry bone syndrome (HBS) was observed in 8 (10.12%) patients. This was managed with oral calcium and calcitriol in five patients, whereas three patients needed parenteral calcium gluconate infusion. Permanent hypoparathyroidism was observed in a single patient, and postoperative pancreatitis was documented in one patient. There was no perioperative mortality. Transient vocal cord paralysis and surgical wound hematoma were observed in one patient each. No patient sustained permanent vocal cord paralysis, wound infection, or sepsis. 698 Indian Journal of Endocrinology and Metabolism / Sep-Oct 2016 / Vol 20 Issue 5
5 The surgical success (cure) for PHPT is defined by the maintenance of eucalcemia at the arbitrarily accepted interval of 6 months after surgery. [10] Based on this definition, the overall cure rate in our series was 96.15% (75 out of our 78 patients achieved cure). Persistent disease was seen in three patients. One of these patients had MEN 1 (PHPT and acromegaly); she underwent the removal of all four parathyroid glands. The second patient was a young male in whom preoperatively left inferior adenoma was localized but had a persistent disease; however, he achieved cure after second surgery. Out of 75 patients who achieved cure, long term follow up (more than one year, range 1 9 years) was available for 41 patients. During this follow up period, none had recurrence of PHPT. Discussion The comparison of our study with other Indian studies is shown in Table 3. The traditional age of presentation of PHPT in India is in the 4 th decade. [4 7,11] In our study, the mean age of presentation was 44 years. Another recent Indian study has reported a mean age of presentation of 48 years. [12] Our results reflect a shift in the presentation of PHPT from fourth to fifth decade in India. However, our patients continue to be much younger than patients from the developed countries. [13,14] One reason for early presentation in Indian patients could be associated Vitamin D deficiency. [4,11] Renal stone disease (50:64.10% patients) was the most common presentation in our series. Other Indian studies have reported 31 70% prevalence of renal stone disease in PHPT. [4 7] A significant (52.56%) proportion of our patients had hypercalciuria. Most of the Indian studies have not reported data on hypercalciuria. One Indian study has reported hypercalciuria in 85% patients. [7] The prevalence of renal stones has fallen from 57% to <5% in the West due to the detection of more and more asymptomatic cases. [15] Thirty percent of our patients with renal stones had a past history of at least one surgery for renal stones and another four patients (8%) had received lithotripsy prior to diagnosis of PHPT. Surprisingly, in none of these patients serum calcium estimation had been advised during previous evaluation. This significant delay in the diagnosis of PHPT reflects the lack of awareness among urologists, nephrologists, and general practitioners regarding PHPT. Skeletal manifestations account for most of the morbidity associated with PHPT. Mishra et al. in 2001 in a study of 29 patients reported osteitis fibrosa cystica in all of them and fractures in 57% of the patients. [4] Four years later, Bhansali et al. in a study of 52 patients reported bone disease in 67% and fractures in 48% patients. [5] A systematic review of PHPT in India has reported fractures in 40% and brown tumors in 42% patients. [16] A recent Indian study reported fractures in 25.8% of PHPT patients and brown tumors in none. [12] In our study, fractures were present only in 10.25% and brown tumors in 6.41% patients. This is the lowest prevalence of fractures in a cohort of PHPT patients from India. Our results reflect a changing trend in the presentation of PHPT in India wherein the overt skeletal disease in the form of fractures and brown tumors is on the decline. The remarkably low prevalence of fractures in our series probably is due to earlier diagnosis of PHPT for last few years (more than half of our subjects were enrolled from 2013 onwards). Another reason may be the improvement in calcium and Vitamin D nutrition. The improvement in Vitamin D nutrition is reflected by the mean serum 25 OHD of 37.2 ng/ml in our patients. The frequency of specific radiological manifestations of PHPT in the United States declined from 23% in the 1960s to a remarkably low 2% in the 1990s. [8,17] The difference in the severity of skeletal disease in PHPT between Western and Eastern populations is determined by calcium and Vitamin D nutrition, but additional factors also play a role. [18,19] PHPT can present as recurrent acute pancreatitis or chronic pancreatitis. [20,21] Previous data from India report that 12 13% patients with PHPT have pancreatitis. [6,7,22] In our series, pancreatitis was present in only 3 (4.41%) patients. The mechanisms of PHPT induced pancreatitis include hypercalcemia induced activation of trypsinogen to trypsin, Table 3: Comparison of present study with other Indian studies Present study (n=78) Harinarayan et al. [11] (n=20) Mishra et al. [4] (n=29) Bhansali et al. [5] (n=52) Gopal et al. [6] (n=79) Priya et al. [7] (n=39) Mithal et al. [12] (n=50) Place Kashmir Delhi Lucknow Chandigarh Mumbai Delhi Delhi Age (years) 44.7 (12.5) 38 (15) (13) 33.5 (8.82) 38.4 (15) 48.3 (15.8) Serum calcium (mg/dl) 12.5 (1.7) 10.9 (0.9) 12.4 (3.1) 12.2 (1.1) (1.77) (1.60) 12.2 (1.9) Serum phosphate (mg/dl) 2.2 (0.6) 3.1 (0.9) 2.2 (0.7) 2.8 (0.6) 1.81 (0.68) 2.58 (0.56) 2.3 (0.7) Serum ALP (U/l) (336.8) 425 (249) (360) (1551) 872 (1401.8) Serum ipth (pg/ml) (386.1) 438 (350) pmol/l 82.7 pmol/l 809 (696) (799) 662 (446) (657.5) Serum 25 OHD (ng/ml) 37.2 (58.1) 8.39 (5.09) NR NR (5.82) 18.2 (15.3) Parathyroid weight (g) 2.05 (3.03) (4.4) (5.87) 4.2 (5.9) Unless otherwise stated, values are mean (SD). ALP: Alkaline phosphatase, NR: Not reported, 25 OHD: 25 hydroxy Vitamin D, ipth: Intact parathyroid hormone, SD: Standard deviation Indian Journal of Endocrinology and Metabolism / Sep-Oct 2016 / Vol 20 Issue 5 699
6 ductal obstruction due to pancreatic calculi, and finally genetic risk factors. All our patients had hypercalcemia and their mean serum calcium level was 12.5 mg/dl, which is remarkably similar to that reported by other Indian studies. [4 7] We documented hypophosphatemia in 69.23% patients, which is in agreement with Western data. [23] A previous Indian study has reported hypophosphatemia in 65% patients with PHPT, but another Indian study has reported a normal mean serum phosphorus in PHPT patients. [5,10] The mean serum ipth level in our patients was pg/ml, which is lower than that reported by previous Indian studies. [4 7] The serum total ALP was elevated in 51.28% patients. Elevated ALP has been consistently reported by other Indian series due to high prevalence of bone disease in PHPT patients. The mean parathyroid weight (2.05 ± 3.03 g) in our study is markedly lower than that reported by other Indian studies [Table 3]. The mean parathyroid weight in our study resembles that reported from developed countries. [15] We found a strong correlation of parathyroid gland weight with serum calcium and ipth, as has been reported previously. [7,24] The mean serum 25 OHD (37.2 ± 58.1 ng/ml) in our study was higher than that reported by previous Indian studies; [3,6,10,11] however, Vitamin D deficiency was present in 38% of our patients. An inverse correlation between serum 25 OHD concentration and parathyroid gland weight has been reported previously. [4,24,25] We did not find any correlation between Vitamin D status and biochemical parameters (serum calcium and ipth) or adenoma weight. These results are consistent with a recent Indian study. [12] The likely reason is the possibility of prior Vitamin D treatment and uncertainty about its timing and amount, which could have confounded the 25 OHD measurements at the time of presentation. In addition, Vitamin D may not be the only significant factor in the development of bone disease in PHPT patients, other factors could be playing a significant role. The preoperative localization of an abnormal parathyroid gland can reduce operative time, postoperative morbidity, and the need for repeat surgery. The imaging methods for localization include high resolution USG, 99m Tc sestamibi scan, computerized tomography, and magnetic resonance imaging. The sensitivity of USG to localize the adenoma has been reported as 65 77%, [5,6] whereas the sensitivity of 99m Tc sestamibi scan has been reported as %. [6,26] In our series, the sensitivity of USG and 99m Tc sestamibi scan for localization of adenoma was 89.8% and 95.3%, respectively. With a sensitivity of 89.8%, we conclude that USG is an effective localization modality as it is inexpensive and is widely available. The overall cure rate for our series was 96.15%. Mishra et al., in a study of 29 patients reported a cure rate of 100%. [4] Another Indian study has reported a cure rate of 96%. [5] Previous Indian studies have reported postoperative HBS in a large proportion of patients from 24% to 82%. [5,6,11,27,28] In our study, postoperative HBS was observed in only 10.12% patients. Our results are in agreement with a recent Indian study in which postoperative HBS was seen in only four patients (8%) out of fifty. [12] Our policy to treat all patients with preoperative serum 25 OHD level <30 ng/ml with Vitamin D is in all probability, responsible for much lower prevalence of postoperative HBS in our series. Consistent with the data about recurrent PHPT on long term follow up revealing recurrence rates of zero to 41.6%, [5,6,27,29,30] none of the 41 patients in our series on whom follow up was available for 1 9 years, had recurrence of PHPT. The strengths of our study include its large size and largely prospective nature with about two thirds (62%) of the subjects evaluated prospectively. Lack of data on bone mineral density and for many patients, on Vitamin D status are the limitations of the study. Conclusion In conclusion, our study reflects a changing trend in the clinical profile of PHPT in India. There is a shift in the age of presentation of PHPT from fourth to fifth decade. Renal stone disease is emerging, the most common presentation, whereas overt skeletal disease in the form of fractures and brown tumors is on the decline. The mean parathyroid weight in our study resembles that reported from the developed countries. Financial support and sponsorship Nil. Conflicts of interest There are no conflicts of interest. References 1. Albright F, Aub JC, Bauer W. Hyperparathyroidism: A common and polymorphic condition as illustrated by seventeen proved cases from one clinic. JAMA 1934;102: Ruda JM, Hollenbeak CS, Stack BC Jr. A systematic review of the diagnosis and treatment of primary hyperparathyroidism from 1995 to Otolaryngol Head Neck Surg 2005;132: AACE/AAES Task Force on Primary Hyperparathyroidism. The American Association of Clinical Endocrinologists and the American Association of Endocrine Surgeons position statement on the diagnosis and management of primary hyperparathyroidism. Endocr Pract 2005;11: Indian Journal of Endocrinology and Metabolism / Sep-Oct 2016 / Vol 20 Issue 5
7 4. Mishra SK, Agarwal G, Kar DK, Gupta SK, Mithal A, Rastad J. Unique clinical characteristics of primary hyperparathyroidism in India. Br J Surg 2001;88: Bhansali A, Masoodi SR, Reddy KS, Behera A, das Radotra B, Mittal BR, et al. Primary hyperparathyroidism in North India: A description of 52 cases. Ann Saudi Med 2005;25: Gopal RA, Acharya SV, Bandgar T, Menon PS, Dalvi AN, Shah NS. Clinical profile of primary hyperparathyroidism from Western India: A single center experience. J Postgrad Med 2010;56: Priya G, Jyotsna VP, Gupta N, Chumber S, Bal CS, Karak AK, et al. Clinical and laboratory profile of primary hyperparathyroidism in India. Postgrad Med J 2008;84: Silverberg SJ, Shane E, Jacobs TP, Siris E, Bilezikian JP. The natural history of treated and untreated asymptomatic primary hyperparathyroidism: A ten year prospective study. N Engl J Med 1999;341: Holick MF, Binkley NC, Bischoff Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. Evaluation, treatment, and prevention of Vitamin D deficiency: An Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 2011;96: Udelsman R. Six hundred fifty six consecutive explorations for primary hyperparathyroidism. Ann Surg 2002;235: Harinarayan CV, Gupta N, Kochupillai N. Vitamin D status in primary hyperparathyroidism in India. Clin Endocrinol (Oxf) 1995;43: Mithal A, Kaur P, Singh VP, Sarin D, Rao DS. Asymptomatic primary hyperparathyroidism exists in North India: Retrospective data from 2 tertiary care centers. Endocr Pract 2015;21: Rao DS, Wilson RJ, Kleerekoper M, Parfitt AM. Lack of biochemical progression or continuation of accelerated bone loss in mild asymptomatic primary hyperparathyroidism: Evidence for biphasic disease course. J Clin Endocrinol Metab 1988;67: Parfitt AM, Rao DS, Kleerekoper M. Asymptomatic primary hyperparathyroidism discovered by multichannel biochemical screening: Clinical course and considerations bearing on the need for surgical intervention. J Bone Miner Res 1991;6 Suppl 2:S Heath H 3 rd. Clinical spectrum of primary hyperparathyroidism: Evolution with changes in medical practice and technology. J Bone Miner Res 1991;6 Suppl 2:S Pradeep PV, Jayashree B, Mishra A, Mishra SK. Systematic review of primary hyperparathyroidism in India: The past, present, and the future trends. Int J Endocrinol 2011;2011: Cope O. The study of hyperparathyroidism at the Massachusetts General Hospital. N Engl J Med 1966;274: Mithal A, Agarwal G, Singh AK, Mishra SK, Rao DS. Severe bone disease in primary hyperparathyroidism in Indians: A reflection of calcium and Vitamin D nutritional status? J Bone Miner Res 1997;12 Suppl 1:S Carling T, Rastad J, Akerström G, Westin G. Vitamin D receptor (VDR) and parathyroid hormone messenger ribonucleic acid levels correspond to polymorphic VDR alleles in human parathyroid tumors. J Clin Endocrinol Metab 1998;83: Prinz RA, Aranha GV. The association of primary hyperparathyroidism and pancreatitis. Am Surg 1985;51: Misgar RA, Mathew V, Pandit K, Chowdhury S. Primary hyperparathyroidism presenting as recurrent acute pancreatitis: A case report and review of literature. Indian J Endocrinol Metab 2011;15: Jacob JJ, John M, Thomas N, Chacko A, Cherian R, Selvan B, et al. Does hyperparathyroidism cause pancreatitis? A South Indian experience and a review of published work. ANZ J Surg 2006;76: Bilezikian JP, Silverberg SJ, Shane E, Parisien M, Dempster DW. Characterization and evaluation of asymptomatic primary hyperparathyroidism. J Bone Miner Res 1991;6 Suppl 2:S Rao DS, Honasoge M, Divine GW, Phillips ER, Lee MW, Ansari MR, et al. Effect of Vitamin D nutrition on parathyroid adenoma weight: Pathogenetic and clinical implications. J Clin Endocrinol Metab 2000;85: Silverberg SJ, Shane E, Dempster DW, Bilezikian JP. The effects of Vitamin D insufficiency in patients with primary hyperparathyroidism. Am J Med 1999;107: Bhansali A, Masoodi SR, Bhadada S, Mittal BR, Behra A, Singh P. Ultrasonography in detection of single and multiple abnormal parathyroid glands in primary hyperparathyroidism: Comparison with radionuclide scintigraphy and surgery. Clin Endocrinol (Oxf) 2006;65: Pradeep PV, Mishra A, Agarwal G, Agarwal A, Verma AK, Mishra SK. Long term outcome after parathyroidectomy in patients with advanced primary hyperparathyroidism and associated Vitamin D deficiency. World J Surg 2008;32: Soin AS, Gupta S, Kochupillai N, Sharma LK. Primary hyperparathyroidism An Indian study. Indian J Cancer 1994;31: Shrikande SS, Talvalkar GV. Parathyroid tumors: A study of 10 cases. Indian J Cancer 1980;17: Kapur MM, Agarwal MS, Gupta A, Misra MC, Ahuja MM. Clinical & biochemical features of primary hyperparathyroidism. Indian J Med Res 1985;81: Indian Journal of Endocrinology and Metabolism / Sep-Oct 2016 / Vol 20 Issue 5 701
The disease spectrum in primary hyperparathyroidism
 Original Article Symptomatic Primary Hyperparathyroidism : A Retrospective Analysis of Fifty One Cases from a Single Centre J Muthukrishnan*, Sangeeta Jha*, KD Modi*, R Jha**, J Kumar**, A Verma*, KVS
Original Article Symptomatic Primary Hyperparathyroidism : A Retrospective Analysis of Fifty One Cases from a Single Centre J Muthukrishnan*, Sangeeta Jha*, KD Modi*, R Jha**, J Kumar**, A Verma*, KVS
Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand
 International Endocrinology Volume 2012, Article ID 952426, 4 pages doi:10.1155/2012/952426 Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand Poramaporn
International Endocrinology Volume 2012, Article ID 952426, 4 pages doi:10.1155/2012/952426 Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand Poramaporn
Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma
 ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 2 Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma P George, N Philip, B Pawar Citation P George,
ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 2 Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma P George, N Philip, B Pawar Citation P George,
4/20/2015. The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy. Learning Objectives
 The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning
The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Primary Hyperparathyroidism: A Tale of Two Cities Revisited New York and Shanghai
 ORIGINAL ARTICLE Bone Research (2013) 2: 162-169. www.boneresearch.org Primary Hyperparathyroidism: A Tale of Two Cities Revisited New York and Shanghai Jian-min Liu 1, Natalie E. Cusano 2, Barbara C.
ORIGINAL ARTICLE Bone Research (2013) 2: 162-169. www.boneresearch.org Primary Hyperparathyroidism: A Tale of Two Cities Revisited New York and Shanghai Jian-min Liu 1, Natalie E. Cusano 2, Barbara C.
Effect of open minimally invasive parathyroidectomy in the management of primary hyperparathyroidism
 International Surgery Journal Kumar SR et al. Int Surg J. 2017 Nov;4(11):3660-3664 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174881
International Surgery Journal Kumar SR et al. Int Surg J. 2017 Nov;4(11):3660-3664 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174881
JMSCR Vol 05 Issue 02 Page February 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i2.134 Original Article Unique Clinical Characteristics
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i2.134 Original Article Unique Clinical Characteristics
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE
 HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
ORIGINAL ARTICLE. Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism
 Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism Elizabeth A. Mittendorf, MD; Christopher R. McHenry, MD ORIGINAL ARTICLE Background: Persistent
Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism Elizabeth A. Mittendorf, MD; Christopher R. McHenry, MD ORIGINAL ARTICLE Background: Persistent
Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from the West?
 ecommons@aku Section of Urology Department of Surgery August 1999 Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from
ecommons@aku Section of Urology Department of Surgery August 1999 Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones
 Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) 30 yr-old woman with 7 yr history
Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) 30 yr-old woman with 7 yr history
PRIMARY HYPERPARATHYROIDISM PRIMARY HYPERPARATHYROIDISM. Hyperparathyroidism Etiology. Common Complex Insidious Chronic Global Only cure is surgery
 ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Southern Derbyshire Shared Care Pathology Guidelines. Primary Hyperparathyroidism
 Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor
 Case Reports in Medicine Volume 2012, Article ID 432676, 4 pages doi:10.1155/2012/432676 Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor F. Mantar, 1 S. Gunduz,
Case Reports in Medicine Volume 2012, Article ID 432676, 4 pages doi:10.1155/2012/432676 Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor F. Mantar, 1 S. Gunduz,
Primary Hyperparathyroidism
 Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Cases in Endocrinology
 Bones, Moans and Groans Diagnosing and Treating Primary Hyperparathyroidism By M. Usman Chaudhry, MD Table 1 Laboratory parameters Her bone density had osteopenic T-Scores of -2.3 at lumbar spine, and
Bones, Moans and Groans Diagnosing and Treating Primary Hyperparathyroidism By M. Usman Chaudhry, MD Table 1 Laboratory parameters Her bone density had osteopenic T-Scores of -2.3 at lumbar spine, and
The parathyroid glands participate in the regulation
 41 HERNAN I. VARGAS STANLEY R. KLEIN The parathyroid glands participate in the regulation of calcium metabolism. Disorders of the parathyroid gland are most commonly a result of hyperfunction and rarely
41 HERNAN I. VARGAS STANLEY R. KLEIN The parathyroid glands participate in the regulation of calcium metabolism. Disorders of the parathyroid gland are most commonly a result of hyperfunction and rarely
Parathyroid Imaging. A Guide to Parathyroid Surgery
 Parathyroid Imaging A Guide to Parathyroid Surgery Primary Hyperparathyroidism (PHPT) 3 rd most common endocrine disorder after diabetes and hyperthyroidism Prevalence in women 2% Often discovered in asymptomatic
Parathyroid Imaging A Guide to Parathyroid Surgery Primary Hyperparathyroidism (PHPT) 3 rd most common endocrine disorder after diabetes and hyperthyroidism Prevalence in women 2% Often discovered in asymptomatic
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy
 "Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
Case Report Rare Skeletal Complications in the Setting of Primary Hyperparathyroidism
 Case Reports in Endocrinology Volume 2015, Article ID 139751, 4 pages http://dx.doi.org/10.1155/2015/139751 Case Report Rare Skeletal Complications in the Setting of Primary Hyperparathyroidism Nikos Sabanis,
Case Reports in Endocrinology Volume 2015, Article ID 139751, 4 pages http://dx.doi.org/10.1155/2015/139751 Case Report Rare Skeletal Complications in the Setting of Primary Hyperparathyroidism Nikos Sabanis,
PRIMARY HYPERPARATHYROIDISM
 PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM WITH RICKETS. KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College
 PRIMARY HYPERPARATHYROIDISM WITH RICKETS KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College Presenting Complaints v 17 year old developmentally normal adolescent boy, first of a twin pregnancy,
PRIMARY HYPERPARATHYROIDISM WITH RICKETS KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College Presenting Complaints v 17 year old developmentally normal adolescent boy, first of a twin pregnancy,
Marcin Barczynski, 1 Aleksander Konturek, 2 Alicja Hubalewska-Dydejczyk, 2. Filip Gołkowski, 1 Stanislaw Cichon, 1 Piotr Richter, 1 Wojciech Nowak
 3 rd Chair and Department of General Surgery 1 and Chair and Department of Endocrinology 2 Jagiellonian University, Medical College Head: Prof. Wojciech Nowak, MD, PhD INTRAOPERATIVE BILATERAL INTERNAL
3 rd Chair and Department of General Surgery 1 and Chair and Department of Endocrinology 2 Jagiellonian University, Medical College Head: Prof. Wojciech Nowak, MD, PhD INTRAOPERATIVE BILATERAL INTERNAL
Normal PTH Levels in Primary Hyperparathyroidism: Still the Same Disease?
 Ann Surg Oncol (2011) 18:3437 3442 DOI 10.1245/s10434-011-1744-x ORIGINAL ARTICLE ENDOCRINE TUMORS Normal PTH Levels in Primary Hyperparathyroidism: Still the Same Disease? Amanda L. Amin, MD, Tracy S.
Ann Surg Oncol (2011) 18:3437 3442 DOI 10.1245/s10434-011-1744-x ORIGINAL ARTICLE ENDOCRINE TUMORS Normal PTH Levels in Primary Hyperparathyroidism: Still the Same Disease? Amanda L. Amin, MD, Tracy S.
JOURNAL OF INTERNATIONAL ACADEMIC RESEARCH FOR MULTIDISCIPLINARY Impact Factor 1.393, ISSN: , Volume 2, Issue 7, August 2014
 HYPOVITAMINOSIS D IN INDIAN FEMALES WITH POSTMENOPAUSAL OSTEOPOROSIS DR. SHAH WALIULLAH 1 DR. VINEET SHARMA 2 DR. R N SRIVASTAVA 3 DR. YASHODHARA PRADEEP 4 DR. A A MAHDI 5 DR. SANTOSH KUMAR 6 1 Research
HYPOVITAMINOSIS D IN INDIAN FEMALES WITH POSTMENOPAUSAL OSTEOPOROSIS DR. SHAH WALIULLAH 1 DR. VINEET SHARMA 2 DR. R N SRIVASTAVA 3 DR. YASHODHARA PRADEEP 4 DR. A A MAHDI 5 DR. SANTOSH KUMAR 6 1 Research
Parathyroid Disease Scenarios for the Practicing Clinician. Vijaya Chockalingam MD Faculty Endocrinologist Banner University Medical Center- Phoenix
 Parathyroid Disease Scenarios for the Practicing Clinician Vijaya Chockalingam MD Faculty Endocrinologist Banner University Medical Center- Phoenix Clinical Scenario-1 73 year man (BK) with hypercalcemia
Parathyroid Disease Scenarios for the Practicing Clinician Vijaya Chockalingam MD Faculty Endocrinologist Banner University Medical Center- Phoenix Clinical Scenario-1 73 year man (BK) with hypercalcemia
Role of Imaging in the Localization of Parathyroid Adenoma
 Role of Imaging in the Localization of Parathyroid Adenoma Authors S A Kabir 1, Z Khanzada 2, S I Akhtar 3, S I Kabir 4, N Wariach 1, 1. Department of Surgery, Lincoln County Hospital, Lincoln LN2 5QY,
Role of Imaging in the Localization of Parathyroid Adenoma Authors S A Kabir 1, Z Khanzada 2, S I Akhtar 3, S I Kabir 4, N Wariach 1, 1. Department of Surgery, Lincoln County Hospital, Lincoln LN2 5QY,
Coexistence of parathyroid adenoma and papillary thyroid carcinoma. Yong Sang Lee, Kee-Hyun Nam, Woong Youn Chung, Hang-Seok Chang, Cheong Soo Park
 J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
Antithyroid drugs in Graves disease: Are we stretching it too far?
 Original Article Antithyroid drugs in Graves disease: Are we stretching it too far? Muthukrishnan Jayaraman, Anil Kumar Pawah, C. S. Narayanan 1 Department of Internal Medicine, Armed Forces Medical College,
Original Article Antithyroid drugs in Graves disease: Are we stretching it too far? Muthukrishnan Jayaraman, Anil Kumar Pawah, C. S. Narayanan 1 Department of Internal Medicine, Armed Forces Medical College,
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Pituitary, Parathyroid Pheochromocytomas & Paragangliomas: The 4 Ps of NETs
 Pituitary, Parathyroid Pheochromocytomas & Paragangliomas: The 4 Ps of NETs Shereen Ezzat, MD, FRCP(C), FACP Professor Of Medicine & Oncology Head, Endocrine Oncology Princess Margaret Hospital/University
Pituitary, Parathyroid Pheochromocytomas & Paragangliomas: The 4 Ps of NETs Shereen Ezzat, MD, FRCP(C), FACP Professor Of Medicine & Oncology Head, Endocrine Oncology Princess Margaret Hospital/University
Vitamin D Therapy in Patients with Primary Hyperparathyroidism and Hypovitaminosis D
 Page 1 of 17 Accepted Preprint first posted on 21 April 2009 as Manuscript EJE-08-0901 Vitamin D Therapy in Patients with Primary Hyperparathyroidism and Hypovitaminosis D JR Tucci, MD, FACP, FACE, Director,
Page 1 of 17 Accepted Preprint first posted on 21 April 2009 as Manuscript EJE-08-0901 Vitamin D Therapy in Patients with Primary Hyperparathyroidism and Hypovitaminosis D JR Tucci, MD, FACP, FACE, Director,
Hyperparathyroidism. When to Suspect, How to Diagnose, When and How to Intervene. Johanna A. Pallotta, MD, FACP, FACE
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
RADIOGUIDED PARATHYROIDECTOMY IS SUCCESSFUL IN 98.7% OF SELECTED PATIENTS
 Original Article RADIOGUIDED PARATHYROIDECTOMY IS SUCCESSFUL IN 98.7% OF SELECTED PATIENTS Charles D. Livingston, MD, FACS ABSTRACT Objective: To examine an individualized approach to patients with primary
Original Article RADIOGUIDED PARATHYROIDECTOMY IS SUCCESSFUL IN 98.7% OF SELECTED PATIENTS Charles D. Livingston, MD, FACS ABSTRACT Objective: To examine an individualized approach to patients with primary
Adenoma weight and biochemical parameters in primary hyperparathyroidism
 Original Research Medical Journal of Islamic Republic of Iran, Vol. 25, No. 3, Nov. 2011, pp. 136-141 Adenoma weight and biochemical parameters in primary hyperparathyroidism Downloaded from mjiri.iums.ac.ir
Original Research Medical Journal of Islamic Republic of Iran, Vol. 25, No. 3, Nov. 2011, pp. 136-141 Adenoma weight and biochemical parameters in primary hyperparathyroidism Downloaded from mjiri.iums.ac.ir
The Impact of Vitamin D Status on Preoperative Ultrasound Findings and Parathyroidectomy Outcomes in Patients With Primary Hyperparathyroidism
 Original Article J Endocrinol Metab. 2017;7(6):172-177 The Impact of Vitamin D Status on Preoperative Ultrasound Findings and Parathyroidectomy Outcomes in Patients With Primary Hyperparathyroidism Ashutosh
Original Article J Endocrinol Metab. 2017;7(6):172-177 The Impact of Vitamin D Status on Preoperative Ultrasound Findings and Parathyroidectomy Outcomes in Patients With Primary Hyperparathyroidism Ashutosh
Primary hyperparathyroidism in Hong Kong: an analysis of 44 cases
 Primary hyperparathyroidism in Hong Kong: an analysis of 44 cases FKW Chan, SC Tiu, KL Choi, TK Au Yong, LF Tang Primary hyperthyroidism in Hong Kong Primary hyperparathyroidism is increasingly being diagnosed
Primary hyperparathyroidism in Hong Kong: an analysis of 44 cases FKW Chan, SC Tiu, KL Choi, TK Au Yong, LF Tang Primary hyperthyroidism in Hong Kong Primary hyperparathyroidism is increasingly being diagnosed
Elena Castellano, Roberto Attanasio, Laura Gianotti, Flora Cesario, Francesco Tassone, and Giorgio Borretta
 ORIGINAL ARTICLE Forearm DXA Increases the Rate of Patients With Asymptomatic Primary Hyperparathyroidism Meeting Surgical Criteria Elena Castellano, Roberto Attanasio, Laura Gianotti, Flora Cesario, Francesco
ORIGINAL ARTICLE Forearm DXA Increases the Rate of Patients With Asymptomatic Primary Hyperparathyroidism Meeting Surgical Criteria Elena Castellano, Roberto Attanasio, Laura Gianotti, Flora Cesario, Francesco
Case Report: Chronic Unclassified Polyarthritis: A Rare Presentation of
 Med. J. Cairo Univ., Vol. 84, No. 2, June: 265-269, 2016 www.medicaljournalofcairouniversity.net Case Report: Chronic Unclassified Polyarthritis: A Rare Presentation of Primary Hyperparathyroidism ABDULRAHMAN
Med. J. Cairo Univ., Vol. 84, No. 2, June: 265-269, 2016 www.medicaljournalofcairouniversity.net Case Report: Chronic Unclassified Polyarthritis: A Rare Presentation of Primary Hyperparathyroidism ABDULRAHMAN
Complementary sestamibi scintigraphy and ultrasound for primary hyperparathyroidism
 Nuclear Medicine and Biomedical Imaging Research Article Complementary sestamibi scintigraphy and ultrasound for primary hyperparathyroidism Yang Z 1,3 *, Li AY 2, Alexander G 3 and Chadha M 3 1 Department
Nuclear Medicine and Biomedical Imaging Research Article Complementary sestamibi scintigraphy and ultrasound for primary hyperparathyroidism Yang Z 1,3 *, Li AY 2, Alexander G 3 and Chadha M 3 1 Department
Vitamin D therapy in patients with primary hyperparathyroidism and hypovitaminosis D
 European Journal of Endocrinology (2009) 161 189 193 ISSN 0804-4643 CLINICAL STUDY Vitamin D therapy in patients with primary hyperparathyroidism and hypovitaminosis D J R Tucci 1,2,3 1 Division of Endocrinology,
European Journal of Endocrinology (2009) 161 189 193 ISSN 0804-4643 CLINICAL STUDY Vitamin D therapy in patients with primary hyperparathyroidism and hypovitaminosis D J R Tucci 1,2,3 1 Division of Endocrinology,
Case study Group 2 presentation
 Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
UPDATES ON PRIMARY HYPERPARATHYROIDISM. Natalie E. Cusano, MD, MS Director, Bone Metabolism Program Lenox Hill Hospital New York, NY
 UPDATES ON PRIMARY HYPERPARATHYROIDISM Natalie E. Cusano, MD, MS Director, Bone Metabolism Program Lenox Hill Hospital New York, NY Disclosures Speaker (Honorarium): Shire Off-label use of estrogen, raloxifene
UPDATES ON PRIMARY HYPERPARATHYROIDISM Natalie E. Cusano, MD, MS Director, Bone Metabolism Program Lenox Hill Hospital New York, NY Disclosures Speaker (Honorarium): Shire Off-label use of estrogen, raloxifene
Decrease in the Prevalence of Pancreatitis Associated with Primary Hyperparathyroidism: Experience at a Tertiary Referral Center
 REVISTA DE INVESTIGACIÓN CLÍNICA Contents available at PubMed www.clinicalandtranslationalinvestigation.com PERMANYER Rev Inves Clin. 2015;67:177-81 ORIGINAL ARTICLE Decrease in the Prevalence of Pancreatitis
REVISTA DE INVESTIGACIÓN CLÍNICA Contents available at PubMed www.clinicalandtranslationalinvestigation.com PERMANYER Rev Inves Clin. 2015;67:177-81 ORIGINAL ARTICLE Decrease in the Prevalence of Pancreatitis
Potential conflicts of interest: None
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene November 6, 2013 Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene November 6, 2013 Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline
Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid Carcinoma: A Case Report
 CASE REPORT Hip Pelvis 28(3): 173-177, 2016 http://dx.doi.org/10.5371/hp.2016.28.3.173 Print ISSN 2287-3260 Online ISSN 2287-3279 Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid
CASE REPORT Hip Pelvis 28(3): 173-177, 2016 http://dx.doi.org/10.5371/hp.2016.28.3.173 Print ISSN 2287-3260 Online ISSN 2287-3279 Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS. BY: Shifaa Qa qa
 NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
Hypercalcemia. Hypercalcemia: When to Worry, When to Treat! Mineral Metabolism : A Short Course
 Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
OSTEITIS FIBROSA CYSTICA IN A YOUNG MALE
 OSTEITIS FIBROSA CYSTICA IN A YOUNG MALE Sankaran Sriram, Post Graduate [1] Rajeswari Sankaralingam Director, Professor and Head of the Department [2] Institute of Rheumatology, Madras Medical College
OSTEITIS FIBROSA CYSTICA IN A YOUNG MALE Sankaran Sriram, Post Graduate [1] Rajeswari Sankaralingam Director, Professor and Head of the Department [2] Institute of Rheumatology, Madras Medical College
When the level of calcium in the blood falls too low, the parathyroid glands secrete just enough PTH to restore the blood calcium level.
 Hyperparathyroidism Primary hyperparathyroidism is a disorder of the parathyroid glands, also called parathyroids. Primary means this disorder originates in the parathyroids: One or more enlarged, overactive
Hyperparathyroidism Primary hyperparathyroidism is a disorder of the parathyroid glands, also called parathyroids. Primary means this disorder originates in the parathyroids: One or more enlarged, overactive
Six hundred fifty-six consecutive explorations for primary hyperparathyroidism Udelsman R
 Six hundred fifty-six consecutive explorations for primary hyperparathyroidism Udelsman R Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS
Six hundred fifty-six consecutive explorations for primary hyperparathyroidism Udelsman R Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS
Original Article. Introduction ABSTRACT
 Original Article Usefulness of pre and post operative calcium and Vitamin D supplementation in prevention of hypocalcemia after total thyroidectomy: A randomized controlled trial Sumiya Jaan, Ashish Sehgal
Original Article Usefulness of pre and post operative calcium and Vitamin D supplementation in prevention of hypocalcemia after total thyroidectomy: A randomized controlled trial Sumiya Jaan, Ashish Sehgal
Clinical Approach to Hypercalcemia For the Primary Care Provider
 Clinical Approach to Hypercalcemia For the Primary Care Provider Christina Maser, MD FACS UCSF Fresno Department of Surgery, Endocrine Surgery 2/2/19 Objectives Recognition of pitfalls of diagnosis of
Clinical Approach to Hypercalcemia For the Primary Care Provider Christina Maser, MD FACS UCSF Fresno Department of Surgery, Endocrine Surgery 2/2/19 Objectives Recognition of pitfalls of diagnosis of
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
ISSN East Cent. Afr. J. s
 56 The Surgical Management of Primary Hyperparathyroidism: The Experience in Tikur Anbessa Specialized Tertiary Referral and Teaching Hospital, Addis Ababa, Ethiopia Sahilu Wondimu 1, Berhanu Nega 2 1
56 The Surgical Management of Primary Hyperparathyroidism: The Experience in Tikur Anbessa Specialized Tertiary Referral and Teaching Hospital, Addis Ababa, Ethiopia Sahilu Wondimu 1, Berhanu Nega 2 1
A large parathyroid adenoma presenting with pathological fractures in a young male
 International Journal of Otorhinolaryngology and Head and Neck Surgery http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Case Report DOI: http://dx.doi.org/10.18203/issn.2454-5929.ijohns20150907 A large
International Journal of Otorhinolaryngology and Head and Neck Surgery http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Case Report DOI: http://dx.doi.org/10.18203/issn.2454-5929.ijohns20150907 A large
THE ASSOCIATION OF PRIMARY HYPERPARATHYROIDISM WITH DISORDERS OF THE THYROID GLAND AND CARPENTRY OUR EXPERIENCE
 24 MEDICINSKI GLASNIK / str. 24-30 Snežana Marinković, Nenad Laketić 1 THE ASSOCIATION OF PRIMARY HYPERPARATHYROIDISM WITH DISORDERS OF THE THYROID GLAND AND CARPENTRY OUR EXPERIENCE Introduction Primary
24 MEDICINSKI GLASNIK / str. 24-30 Snežana Marinković, Nenad Laketić 1 THE ASSOCIATION OF PRIMARY HYPERPARATHYROIDISM WITH DISORDERS OF THE THYROID GLAND AND CARPENTRY OUR EXPERIENCE Introduction Primary
Primary hyperparathyroidism A clinical study
 Med. J. Malaysia Vol. 43 No. 3 September 1988 Primary hyperparathyroidism A clinical study K. L. Goh, MBBS(Mal), MRCP(UK) Lecturer in Medicine F. Wang, MBBS(Sing), FRCP(Edin), FRACP, FACP Professor ofmedicine
Med. J. Malaysia Vol. 43 No. 3 September 1988 Primary hyperparathyroidism A clinical study K. L. Goh, MBBS(Mal), MRCP(UK) Lecturer in Medicine F. Wang, MBBS(Sing), FRCP(Edin), FRACP, FACP Professor ofmedicine
HPI joint pain/arthritis serum calcium 11.5 PTH 147pg/ml
 HPI 45 yo female Increased calcium level during evaluation for joint pain/arthritis W/U showed serum calcium 11.5 and PTH 147pg/ml (Normal 11-67pg/ml) Otherwise asymptomatic PMH/PSH Arthritis Tonsillectomy
HPI 45 yo female Increased calcium level during evaluation for joint pain/arthritis W/U showed serum calcium 11.5 and PTH 147pg/ml (Normal 11-67pg/ml) Otherwise asymptomatic PMH/PSH Arthritis Tonsillectomy
Magnesium Homeostasis
 ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
INDEX. Note: Page numbers of issue and article titles are in boldface type. cell carcinoma. ENDOCRINE SURGERY
 ENDOCRINE SURGERY INDEX Note: Page numbers of issue and article titles are in boldface type. Adenylate cyclase, in signal transduction 425-426 Adrenal incidentalomas, 499-509 imaging of, 502-504 in patients
ENDOCRINE SURGERY INDEX Note: Page numbers of issue and article titles are in boldface type. Adenylate cyclase, in signal transduction 425-426 Adrenal incidentalomas, 499-509 imaging of, 502-504 in patients
Since the advent of multichannel serum chemistry
 ONLINE EXCLUSIVE Padmaja Sanapureddy, MD; Vishnu Vardhan Garla, MD; Mallikarjuna Reddy Pabbidi, DVM, PhD Department of Primary Care and Medicine, G.V. (Sonny) Montgomery VA Medical Center, Jackson, Miss
ONLINE EXCLUSIVE Padmaja Sanapureddy, MD; Vishnu Vardhan Garla, MD; Mallikarjuna Reddy Pabbidi, DVM, PhD Department of Primary Care and Medicine, G.V. (Sonny) Montgomery VA Medical Center, Jackson, Miss
Case Report Persistent Primary Hyperparathyroidism, Severe Vitamin D Deficiency, and Multiple Pathological Fractures
 Case Reports in Endocrinology Volume 2016, Article ID 3016201, 4 pages http://dx.doi.org/10.1155/2016/3016201 Case Report Persistent Primary Hyperparathyroidism, Severe Vitamin D Deficiency, and Multiple
Case Reports in Endocrinology Volume 2016, Article ID 3016201, 4 pages http://dx.doi.org/10.1155/2016/3016201 Case Report Persistent Primary Hyperparathyroidism, Severe Vitamin D Deficiency, and Multiple
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 341 O CTOBER 21, 1999 NUMBER 17 A 10-YEAR PROSPECTIVE STUDY OF PRIMARY HYPERPARATHYROIDISM WITH OR WITHOUT
The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 341 O CTOBER 21, 1999 NUMBER 17 A 10-YEAR PROSPECTIVE STUDY OF PRIMARY HYPERPARATHYROIDISM WITH OR WITHOUT
DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS
 DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS XLH IS CHARACTERIZED BY CHRONIC HYPOPHOSPHATEMIA XLH is a hereditary, progressive, lifelong disorder. In children and adults,
DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS XLH IS CHARACTERIZED BY CHRONIC HYPOPHOSPHATEMIA XLH is a hereditary, progressive, lifelong disorder. In children and adults,
Outline. Parathyroid Localization Studies. Mira Milas MD, FACS Associate Professor of Surgery Director, The Thyroid Center
 Parathyroid Localization Studies Mira Milas MD, FACS Associate Professor of Surgery Director, The Thyroid Center Outline Clinical Context of Primary Hyperparathyroidism Ultrasound, Sestamibi, and Other
Parathyroid Localization Studies Mira Milas MD, FACS Associate Professor of Surgery Director, The Thyroid Center Outline Clinical Context of Primary Hyperparathyroidism Ultrasound, Sestamibi, and Other
Yueming Sun Æ Huihua Cai Æ Jianfeng Bai Æ Hanlin Zhao Æ Yi Miao
 World J Surg (2009) 33:1674 1679 DOI 10.1007/s00268-009-0086-3 Endoscopic Total Parathyroidectomy and Partial Parathyroid Tissue Autotransplantation for Patients with Secondary Hyperparathyroidism: A New
World J Surg (2009) 33:1674 1679 DOI 10.1007/s00268-009-0086-3 Endoscopic Total Parathyroidectomy and Partial Parathyroid Tissue Autotransplantation for Patients with Secondary Hyperparathyroidism: A New
Case 4 Generalised bone pain
 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Surgical treatment of primary hyperparathyroidism due to parathyroid tumor: A 15-year experience
 ONCOLOGY LETTERS 12: 1989-1993, 2016 Surgical treatment of primary hyperparathyroidism due to parathyroid tumor: A 15-year experience LU FENG, XU ZHANG and SHAN TING LIU Department of Head and Neck Surgery,
ONCOLOGY LETTERS 12: 1989-1993, 2016 Surgical treatment of primary hyperparathyroidism due to parathyroid tumor: A 15-year experience LU FENG, XU ZHANG and SHAN TING LIU Department of Head and Neck Surgery,
JMSCR Vol 06 Issue 12 Page December 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.157 A comparative study of two
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.157 A comparative study of two
Vitamin D receptor gene polymorphism and serum levels of Fetuin-A, Vitamin D and ipth in the hemodialysis patients
 In The Name of GOD Vitamin D receptor gene polymorphism and serum levels of Fetuin-A, Vitamin D and ipth in the hemodialysis patients Authors & Affiliations: 1-jamal hallajzadeh; Maraghe University of
In The Name of GOD Vitamin D receptor gene polymorphism and serum levels of Fetuin-A, Vitamin D and ipth in the hemodialysis patients Authors & Affiliations: 1-jamal hallajzadeh; Maraghe University of
2016 Arizona AACE Meeting: Updated Guidelines for the Management of Primary Hyperparathyroidism (PHPT)
 2016 Arizona AACE Meeting: Updated Guidelines for the Management of Primary Hyperparathyroidism (PHPT) Scott M. Wilhelm, MD, FACS Associate Professor and Section Head Endocrine Surgery University Hospitals-Cleveland
2016 Arizona AACE Meeting: Updated Guidelines for the Management of Primary Hyperparathyroidism (PHPT) Scott M. Wilhelm, MD, FACS Associate Professor and Section Head Endocrine Surgery University Hospitals-Cleveland
THE 20TH CENTURY witnessed major advances in several
 JOURNAL OF BONE AND MINERAL RESEARCH Volume 22, Supplement 2, 2007 doi: 10.1359/JBMR.07S202 2007 American Society for Bone and Mineral Research Vitamin D Deficiency and Primary Hyperparathyroidism Shonni
JOURNAL OF BONE AND MINERAL RESEARCH Volume 22, Supplement 2, 2007 doi: 10.1359/JBMR.07S202 2007 American Society for Bone and Mineral Research Vitamin D Deficiency and Primary Hyperparathyroidism Shonni
Original Research Article
 Medrech ISSN No. 2394-3971 Original Research Article TYPE 2 DIABETES WITH RECURRENT OSTEOPOROTIC FRACTURES, OR CUSHING S SYNDROME? Blertina Dyrmishi¹*; Taulant Olldashi²; Prof Asc Thanas Fureraj 3 ; Prof
Medrech ISSN No. 2394-3971 Original Research Article TYPE 2 DIABETES WITH RECURRENT OSTEOPOROTIC FRACTURES, OR CUSHING S SYNDROME? Blertina Dyrmishi¹*; Taulant Olldashi²; Prof Asc Thanas Fureraj 3 ; Prof
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Minimally invasive parathyroidectomy
 Minimally invasive parathyroidectomy Jessica E. Gosnell MD Assistant Professor of Surgery March 22, 2011 1 Minimally invasive parathyroidectomy 1. What? 2. When? 3. How? 4. Convert? 5. What adjuncts? Primary
Minimally invasive parathyroidectomy Jessica E. Gosnell MD Assistant Professor of Surgery March 22, 2011 1 Minimally invasive parathyroidectomy 1. What? 2. When? 3. How? 4. Convert? 5. What adjuncts? Primary
Primary Hyperparathyroidism
 November 2002 Primary Hyperparathyroidism Lori Coburn, Harvard Medical School Year III Hyperparathyroidism An increase in parathyroid hormone (PTH) production Divided into Primary, Secondary and Tertiary
November 2002 Primary Hyperparathyroidism Lori Coburn, Harvard Medical School Year III Hyperparathyroidism An increase in parathyroid hormone (PTH) production Divided into Primary, Secondary and Tertiary
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Peroperative PTH testing:
 07. hoofdstuk 07 23-07-2001 09:52 Pagina 69 Peroperative PTH testing: confirmation of successful surgical treatment of primary hyperparathyroidism 7 Smit PC, Thijssen JHH, Borel Rinkes IHM, van Vroonhoven
07. hoofdstuk 07 23-07-2001 09:52 Pagina 69 Peroperative PTH testing: confirmation of successful surgical treatment of primary hyperparathyroidism 7 Smit PC, Thijssen JHH, Borel Rinkes IHM, van Vroonhoven
Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Medical Expert
 Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Introduction Medical Expert This is a three month PGY 1-5 rotation in which residents gain exposure in the care and management of patients
Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Introduction Medical Expert This is a three month PGY 1-5 rotation in which residents gain exposure in the care and management of patients
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
Comparison Of Sestamibi Scintigraphy And Ultrasonography In Preoperative Localization Of Primary Hyperparathyroidism
 ISPUB.COM The Internet Journal of Surgery Volume 16 Number 1 Comparison Of Sestamibi Scintigraphy And Ultrasonography In Preoperative Localization Of Primary S Nasiri, A Sorush, A Hashemi, F Mehrkhani,
ISPUB.COM The Internet Journal of Surgery Volume 16 Number 1 Comparison Of Sestamibi Scintigraphy And Ultrasonography In Preoperative Localization Of Primary S Nasiri, A Sorush, A Hashemi, F Mehrkhani,
MEDIASTINAL PARATHYROID ADENOMA MIMICKING CANCER METASTATIC TO BONE
 Case Report MEDIASTINAL PARATHYROID ADENOMA MIMICKING CANCER METASTATIC TO BONE Ping Yu Xiong, MD 1 ; Joshua Lakoff, MD, FRCPC 2 ; Robyn L. Houlden, MD, FRCPC 2 ABSTRACT Objective: Mediastinal parathyroid
Case Report MEDIASTINAL PARATHYROID ADENOMA MIMICKING CANCER METASTATIC TO BONE Ping Yu Xiong, MD 1 ; Joshua Lakoff, MD, FRCPC 2 ; Robyn L. Houlden, MD, FRCPC 2 ABSTRACT Objective: Mediastinal parathyroid
Current Concepts in the Evaluation and Management of Abnormal Parathyroid Hormone (PTH) Levels Shireen Fatemi, M.D. April, 2012.
 Current Concepts in the Evaluation and Management of Abnormal Parathyroid Hormone (PTH) Levels Shireen Fatemi, M.D. April, 2012 Disclosures I have no financial relationships with commercial interests,
Current Concepts in the Evaluation and Management of Abnormal Parathyroid Hormone (PTH) Levels Shireen Fatemi, M.D. April, 2012 Disclosures I have no financial relationships with commercial interests,
Postresection Parathyroid Hormone and Parathyroid Hormone Decline Accurately Predict Hypocalcemia After Thyroidectomy
 Clinical Chemistry / PTH PREDICTS HYPOCALCEMIA AFTER THYROIDECTOMY Postresection Parathyroid Hormone and Parathyroid Hormone Decline Accurately Predict Hypocalcemia After Thyroidectomy Pedro Alía, PhD,
Clinical Chemistry / PTH PREDICTS HYPOCALCEMIA AFTER THYROIDECTOMY Postresection Parathyroid Hormone and Parathyroid Hormone Decline Accurately Predict Hypocalcemia After Thyroidectomy Pedro Alía, PhD,
Asymptomatic Primary Hyperparathyroidism
 The new england journal of medicine clinical practice Asymptomatic Primary Hyperparathyroidism John P. Bilezikian, M.D., and Shonni J. Silverberg, M.D. This Journal feature begins with a case vignette
The new england journal of medicine clinical practice Asymptomatic Primary Hyperparathyroidism John P. Bilezikian, M.D., and Shonni J. Silverberg, M.D. This Journal feature begins with a case vignette
Head and Neck Endocrine Surgery
 Objectives Endocrine Physiology Risk factors for hypocalcemia Management strategies Passive vs. active Treatment of hypocalcemia Department of Head and Neck Management of Calcium in Thyroid and Parathyroid
Objectives Endocrine Physiology Risk factors for hypocalcemia Management strategies Passive vs. active Treatment of hypocalcemia Department of Head and Neck Management of Calcium in Thyroid and Parathyroid
Effects of surgery on outcome of primary hyperparathyroidism
 1 Effects of surgery on outcome of primary hyperparathyroidism Peter Vestergaard Leif Mosekilde Peer Christiansen Introduction Primary hyperparathyroidism is a disease with effects on many organ systems
1 Effects of surgery on outcome of primary hyperparathyroidism Peter Vestergaard Leif Mosekilde Peer Christiansen Introduction Primary hyperparathyroidism is a disease with effects on many organ systems
The CaPTHUS Scoring Model revisited: Applicability from. with Primary Hyperparathyroidism
 wjoes The CaPTHUS Scoring Model revisited: Applicability from a UK Cohort 10.5005/jp-journals-10002-1199 with Primary Hyperparathyroidism Original Article The CaPTHUS Scoring Model revisited: Applicability
wjoes The CaPTHUS Scoring Model revisited: Applicability from a UK Cohort 10.5005/jp-journals-10002-1199 with Primary Hyperparathyroidism Original Article The CaPTHUS Scoring Model revisited: Applicability
Challenges in the Management of Primary HPTH. Zaher Ajam, MD Ghada El-Hajj Fuleihan, MD, MPH
 Challenges in the Management of Primary HPTH Zaher Ajam, MD Ghada El-Hajj Fuleihan, MD, MPH Case Presentation 1 This a case of a 41-year-old gentleman who is referred to Endocrinology clinic for low BMD,
Challenges in the Management of Primary HPTH Zaher Ajam, MD Ghada El-Hajj Fuleihan, MD, MPH Case Presentation 1 This a case of a 41-year-old gentleman who is referred to Endocrinology clinic for low BMD,
Effect of oral versus intramuscular Vitamin D replacement in apparently healthy adults with Vitamin D deficiency
 Original Article Effect of oral versus intramuscular Vitamin D replacement in apparently healthy adults with Vitamin D deficiency Nitin Gupta, Khalid J. Farooqui 1, Chandar M. Batra 2, Raman K. Marwaha
Original Article Effect of oral versus intramuscular Vitamin D replacement in apparently healthy adults with Vitamin D deficiency Nitin Gupta, Khalid J. Farooqui 1, Chandar M. Batra 2, Raman K. Marwaha
Post-operative Transient Hypoparathyroidism: Incidence and Risk Factors
 ORIGINAL ARTICLE Post-operative Transient Hypoparathyroidism: Incidence and Risk Factors sensitivity (2)(3), which can cause significant morbidity for patients if it goes unrecognized (4). Symptomatic
ORIGINAL ARTICLE Post-operative Transient Hypoparathyroidism: Incidence and Risk Factors sensitivity (2)(3), which can cause significant morbidity for patients if it goes unrecognized (4). Symptomatic
Women s Health in General Practice Symposium 2015 Thyroid & Parathyroid Cases
 Women s Health in General Practice Symposium 2015 Thyroid & Parathyroid Cases Bill Fleming Epworth Freemasons Hospital 1 Common Endocrine Presentations anatomical problems thyroid nodule / goitre embryological
Women s Health in General Practice Symposium 2015 Thyroid & Parathyroid Cases Bill Fleming Epworth Freemasons Hospital 1 Common Endocrine Presentations anatomical problems thyroid nodule / goitre embryological
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Severe Hypocalcemia Complicated by Postsurgical Hypoparathyroidism and Hungry Bone Syndrome in a Patient with Primary Hyperparathyroidism, Graves Disease, and Acromegaly Seigo Tachibana 1,ShinyaSato
CASE REPORT Severe Hypocalcemia Complicated by Postsurgical Hypoparathyroidism and Hungry Bone Syndrome in a Patient with Primary Hyperparathyroidism, Graves Disease, and Acromegaly Seigo Tachibana 1,ShinyaSato
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
