Experts Corner. two conditions, I would perform PPD skin test and chest x-ray/ HRCT. If PPD skin test is
|
|
|
- Kerry Carroll
- 5 years ago
- Views:
Transcription
1 Experts Corner S.P. Garg Uveitis is a common and confusing entity in the practice of ophthalmology. Improper diagnosis or management lead to sight threatening complications. Medications used in treating cases of uveitis may have serious systemic side effects. So it is imperative to properly analyse cases before initiating by Senior Resident Uvea and Vitreo-retina services from R.P. Centre for Ophthalmic Sciences, All India Institute for Medical Sciences, Ansari Nagar, New Delhi. MD, MNAMS, Consultant, Vitreo Retina Service, Vision Eye Center, Siri Fort Road, New Delhi MS, FMRF, FNAMS, FIC Path., FAICO, Director of Uveitis and Ocular Pathology Department, Sankara Nethralaya, 18, College Road, Nungambakkam, Chennai. Additional Professor, Advanced Eye Centre, Post Graduate Institute of Medical Education and Research, Chandigarh Consultant, Uvea Service, L.V. Prasad Eye Institute, Kallam Anji Reddy Campus, Banjara Hills, Hyderabad, Telangana. MS, FRCSEd, FRCOphth, FMRF, Uveitis and Retina Services, Shroff Eye Centre, East of Kailash, New Delhi. does not merit investigation. A case of recurrent / chronic uveitis, or granulomatous uveitis or history/examination suggestive of systemic disease should be investigated. As a routine for most cases we do a chest X-ray and mantoux test. A CT chest and serum ACE levels are done usually in cases of granulomatous uveitis or chronic anterior uveitis. If history is suggestive suggest an associated collagen vascular disease or in children where JRA is suspected. Rare cases of leprosy would require a skin consultation. Syphilis is now seen rarely but if suspected a VDRL and a TPHA test is done. order any investigations as the outcome is usually quite good. However, in cases of recurrent anterior uveitis, based on the morphologic pattern, I order investigations. In non-granulomatous anterior uveitis, I order HLA B27, ESR, and ANA. In granulomatous uveitis, I order Mantoux, QuantiFERON TB gold test, sarcoid work up (serum angiotensin converting enzyme, serum lysozyme assay, serum calcium and inorganic phosphorus), and HRCT chest. If the patient has presented with granulomatous anterior uveitis and his IOP is two conditions, I would perform PPD skin test and chest x-ray/ HRCT. If PPD skin test is Jyotirmay Biswas Vishali Gupta Somasheila Murthy Shishir Narain www. dosonline.org l 15
2 Experts Corner: Uvea positive (induration of 10mm or more after 72 hours) and lymphadenopathy, I would consider TB as diagnosis. On the other hand, if PPD skin test is negative, and chest shows hilar gland enlargement, I would think of sarcoidosis and do ACE levels as well as consult pulmonologist for trans bronchial lung biopsy or bronchoalveloar lavage for proceed with quantiferon TB Gold or PCR to establish the diagnosis of TB. In another situation of a patient presenting with granulomatous anterior uveitis with raised IOP, I would like to rule out viral etiology and would look for features PCR from the aqueous tap. On the other hand, if patient has come with an acute attack of non-granulomatous anterior uveitis, I would like to rule out sacroilitis and HLA-B27 related spondyloarthritides. The simplest test in these patients would be x-ray sacroiliac spine to look for any evidence of sacroilitis. HLA B27 if available adds to the diagnosis but is not must. In a child presenting with chronic anterior uveitis with band shaped keratopathy, I would like to do ANA to rule out juvenile idiopathic arthritis. In other less common diseases like TINU syndrome etc, the investigations shall be customized depending upon the differential diagnosis. I investigate most cases of non-granulomatous uveitis when in young male or female (uniliateral or bilateral), when recurrent and when severe. The investigations I prefer are: HLA B27 in males and RA, ANA and CRP in young female patients. In bilateral granulomatous anterior uveitis, I usually ask for CBC, ESR, X Ray chest, PPD, S. ACE and sometimes VDRL. In case of unilateral anterior uveitis, with elevated IOP, I would consider it as Viral and not investigate. I would also rule out FHC and not investigate in those cases. Approach to Anterior uveitis: Is it painful symptomatic uveitis? HLA B27 related is usually very painful with obvious photophobia. One important aspect is the absence of posterior segment involvement except CME. Will like to know the HLA status, whether negative or positive as it affects systemic screening and dosage of treatment and possibility of ankylosis in early life. Is it painless, asymptomatic uveitis? In a child this is very crucial. If it is a girl child then investigate with ANA and keep JIA in differential diagnosis. If there is mild anterior uveitis, look for intermediate uveitis as it needs more aggressive management in children compared to adults. In adults with unilateral anterior uveitis rule out fuch s uveitis (FHU). If the diagnosis is FHU do not investigate or treat the disease except when more symptomatic. If suspecting CMV anterior uveitis can do AC tap antimicrobial treatment. Aim of FFA in posterior uveitis is to identify any typical pattern of leakage which may suggest / help So where we do suspect VKH, MEWDS, APMPPE we do perform FFA. CME or a secondary choroidal neovascular membrane can now be picked up easily by OCT. So an FFA for these would only be done in case there is some doubt on OCT. I perform an FFA in all cases of posterior uveitis, except in Toxoplasmic retinochoroiditis, where I do not. Quite frequently in patients with posterior uveitis especially in patients with retinal vasculitis to look non-perfusion and any neovascularisation. I would also do it at presentation in entities like VKH, sympathetic picture is diagnostic and helps in making the diagnosis. Less frequently for some of the conditions like cystoid macular edema where I have switched over to OCTs. Also for conditions like Serpiginous choroidits, we Very rare as I mainly see more of anterior FFA is rapidly being substituted by choroidopathy For Diagnosis especially to differentiate CSR and VKH as the treatment are reverse. For Treatment to look for areas of CNP especially prophylactic laser in such situations. As mentioned above we do not do a battery of tests and depending on any systemic history or examination and the ocular examination / chronicity of the disease we and should rather be condemned. HIV / Toxoplasma / Toxocara serology where there is a clinical suspicion. Viral serology for Herpes / CMV again does not give any meaningful results. 16 l DOS Times - Vol. 20, No. 3 September, 2014
3 Uvea I do serum ELISA for Toxoplasmosis in clinically suspected Toxoplasma retinochoroiditis. I value both IgM and IgG titres. Even in undiluted serum, positivity is quite relevant in suspected cases. I also do an ELISA for HIV in suspected viral retinitis, especially CMV retinitis and acute retinal necrosis (ARN). In most of the infectious conditions serological tests are unhelpful and should not be done especially for disease like TB or viral infections. We rely on the serological tests for very few infectious diseases like syphilis and toxoplasmosis. However, analysis of local intraocular antibody production by analyzing paired serum and aqueous samples for presence of antibodies against CMV, toxoplasmosis, HSV and VZV can be useful. Serological tests may be useful in certain autoimmune conditions like Systemic lupus erythematosus, polymyositis/dermatomyositis, connective tissue disease, and polyarteritis nodosa etc. Obvious infective etiologies like toxoplasma to be ruled out. The clinical diagnosis is of paramount importance and the serological tests are performed to support or refute the diagnosis. Please interpret the tests in the light of immune status, present systemic treatment, false negative and positive indices. For example, if the IgG Toxoplasma is negative then the likelihood of the retinal lesion being due to Toxoplasma is unlikely. Vice versa does not necessarily hold true, as it is often a positive test. We do routinely investigate for tuberculosis, sarcoidosis and syphilis. For this we generally do a chest X-ray, Mantoux, serum ACE level and VDRL as baseline. If suspicion is high due to any granulomatous nature of or a child with severe vasculitis a CT chest would also be done. Other tests depend on associated ocular and systemic Yes, I recommend investigations to rule out sarcoidosis, Behçet s disease, collagen vascular diseases, and tuberculosis. Nowadays, I do HRCT chest in all cases of Eales disease. Certainly yes. I personally use the term retinal vasculitis and in my practice all the cases of the underlying aetiology. However we would do only tailored investigations. The investigations would depend characteristics, associated systemic diseases etc. e.g., in a patient with occlusive vasculitis, I would think of TB and Behcets. If the patient has active periphlebitis with areas of capillary non-perfusion, with or without neovascularization or associated choroiditis lesions, I would consider the diagnosis of TB very likely and would investigate him for that. On the other hand, if he has patches of retinitis from the capillaries and also gives history of oral/genital ulcers, I would think about Behcets disease. The further investigation will be tailored towards the shortlisted differential diagnosis. If you mean retinal vascultis, then I would try to investigate to rule out TB/Sarcoid/Syphilis/Lyme s disease if there is such a history or assume a viral etiology and may periphlebitis like Eale s disease, still prefer to do a TB work up. Yes. Retinal phlebitis may have serious consequences if it involves the posterior pole. Rule out Sarcoidosis and TB hypersensitivity status and look for systemic auto-immune vasculitis with screening using ANA titres. We do UBM in cases of chronic hypotony to distinguish between ciliary body atrophy or formation of membranes over the ciliary body. In case of the latter a vitrectomy with removal of membranes may be planned. A few cases of mild recurrent chronic uveitis due to IOL haptic contact with ciliary body have been detected on UBM. Yes. UBM can be done in cases with small pupil, where peripheral retina is not seen to rule out pars planitis, particularly in the presence of vitreous cells or in with hypotony to rule out ciliary body pathology and in caterpillar hair induced uveitis. UBM helps in looking at the pathologies in the ciliary body region that may otherwise be obscured due to the development of synichae or media opacities. It can be used to diagnose granuloma of ciliary body in conditions like TB, a foreign body, haptic of an IOL in sulcus rubbing against the ciliary body, caterpillar hair or a mass in the ciliary body region in case of Masquerade syndromes. In patients with hypotony, UBM helps in diagnosing the cause for hypotony e.g., ciliary body atrophy or presence of a cyclitic membrane over the ciliary body. This would also help us in planning the strategy as in patients with complicated cataract, hypotony and ciliary membrane in a child with JIA, we would prefer pars plana lensectomy and vitrectomy with peeling of the ciliary membrane and silicon oil tamponade if required. We will not consider doing phacoaspiration with IOL implant in such a situation. www. dosonline.org l 17
4 Experts Corner: Uvea Yes, I routinely ask for UBM in cases with cataract and chronic hypotony, in cases of post-cataract surgery uveitis to rule out UGH like syndrome and chronic pars planitis. Helps in assessing response to treatment in cases of VKH also. Yes. In a selected group of patients with persistent hypotony to look for cyclitic membranes and atrophy of ciliary processes. This is crucial in advanced cases where mercenary vitreo-retinal procedures with long term silicone oil tamponade may be considered in desperate situations. We are generally doing a vitreous biopsy where a masquerade syndrome is suspected. Most commonly here we are looking for lymphoma. So a cytology after cytospin is generally ordered. Rarely in some cases we would do a vitreous biopsy for viral markers like HSV, HZV, CMV. Routinely we donot do these tests and would rather treat empirically on basis of clinical presentation. intraocular lymphoma. I also do a vitreous tap in suspected viral retinitis, suspected tubercular uveitis, and endogenous endophthalmitis. I do a smear, culture and PCR for detection of bacteria, especially Mycobacterium, fungus and virus. My indications for the vitreous biopsy are as follows: 1. Suspicion of intraocular malignancy. 2. Atypical presentation of uveitis where other noninvasive investigations are non contributory 3. In certain cases of suspected infectious uveitis, where we would like to collect vitreous sample for treatment. Whenever we plan a vitreous biopsy, handling of the specimen is of utmost importance as otherwise the cells will degenerate by the time the specimen reaches laboratory and no positive information can be obtained. One needs a very expert cytologist who can tell the precise cell morphology as the cells are very few. In addition, we also do molecular diagnostic tests depending upon the suspected pathology and cytokines e.g., IL 6 and IL 10 in cases of suspected primary vitreoretinal lymphomas. Unilateral pan or posterior uveitis with dense lesions suggestive of abscess. Masquerade like lymphoma. Perform microbiology and histopah to rule out fungus, PCR for HSV, CMV, VZV in cases looking like viral retinitis, ARN, and histopath for lymphoma. Usually to rule out intraocular lymphoma best detected with vitreous biopsy. Needs an expert cytologist to settle the diagnostic dilemma. Keep high index of suspicion even in cases with normal MR imaging of brain in some cases. steroid/ intravitreal steroid/ intravitreal Ozurdex Our preferred treatment of intermediate uveitis and many cases of serpigenous choroiditis, idiopathic vasculitis and multifocal choroiditis with panuveitis is posterior subtenon steroid. Most cases do respond well. If properly given, as far posteriorly as possible the incidence of glaucoma is also not very high. We rarely give intravitreal tricort / Ozurdex for uveitis. I give posterior subtenon steroid injection as a as it can cause ptosis and steroid-induced glaucoma, I give it less frequently. I give intravitreal steroid in recalcitrant cystoid macular edema (CME) in intermediate uveitis. If in these cases, the CME is huge, I prefer an intravitreal implant of Ozurdex. Local corticosteroid treatment is the mainstay of therapy in patients with unilateral non-infectious variety of uveitis e.g., pars planitis with cystoid macular edema. I personally prefer intravitreal ozurdex implants in uveitic eyes as it gives a sustained release of drug over a period of time. In other autoimmune conditions associated with systemic manifestations, the patients would need systemic immunosuppressive drugs but adding intravitreal ozurdex implant rather than administering high dose of systemic corticosteroids can manage the local unilateral exacerbations in these eyes. In cases of unilateral intermediate/posterior uveitis where infection has been ruled out, and patients have CME. Or post-op patients after cataract surgery, sometime combine with cataract surgery. Intermediate uveitis with CME in cases who are not steroid responders. Intravitreal ozurdex can also be used for recalcitrant treatment of peri-operative CME. For unilateral CME our preferred treatment is posterior subtenon tricort. Risk of glaucoma is explained to the patient. Even for bilateral cases we would initially start 18 l DOS Times - Vol. 20, No. 3 September, 2014
5 Uvea the patient on oral steroids and give a subtenon tricort in one eye if there are no additional risk factors of glaucoma. can be given in both eyes in case of a relapse. In case risk of glaucoma is perceived to be high or the patient is not willing to take the risk of glaucoma, oral steroids and in recurrent cases steroids with immunosuppressants are used. In case of unilateral CME, I give posterior intravitreal Ozurdex injection. In bilateral CME, I give immunosuppressive agents like Mycophenolate mofetil with low dose oral steroids. I add Nepafenac eyedrops three times daily in both eyes. Firstly I would investigate the patients with would have an underlying disease like TB, syphilis etc. etiology, this becomes pars planitis. The main cause of vision decrease in these patients is cystoid macular edema. element as the presence of vitreomacular traction would be an indication for pars plana vitrectomy. For unilateral edema, I prefer intravitreal ozurdex implant whereas for bilateral condition it can be systemic therapy with corticosteroids/ immmunosppressives with addition of local therapy to the worse eye if needed. The presence of concomitant pathologies like vitritis, choroiditis etc would Uniliateral; generally regional steroids, Ozurdex if affording, bilateral: oral steroids and other immunumodulators. For u/l cases sub-tenon steroids are the preferred choice of treatment. In bilateral IU with b/l CME, I prefer to investigate thoroughly for a systemic cause and prefer systemic oral steroids, and may need a steroid sparing immunosuppressive if the disease requires long term systemic treatment. Our preferred management is with sulfamethoxazole and trimethoprim followed by oral steroids. In cases which relapse frequently, therapy with a combination of Clindamycin and Azithromycin can also be tried. We do not have much experience with Intravitreal Clindamycin. I always give anti-toxoplasma treatment whatever the location of the lesion (ie) posterior pole or periphery. My preferred drug of choice is Clindamycin 300 mg 1 tablet 4 times daily for 6 weeks. I add tablet Prednisolone 1 mg/kg body weight after 48 hours of starting Clindamycin. I combine tablet Azithromycin 250mg 2 tablets stat and 1 tablet daily for 6 weeks. The diagnosis of Toxoplasmosis is based on the typical appearance of focal necrotizing retinitis and I generally do not wait for the serology results or obtain initiating treatment. I use a convenient combination of a dihydrofolate reductase inhibitor and sulfonamide that is trimethoprim/sulfamethoxazole (Bactrim, Septran) in the dose of double strength tablet (Trimethoprim 160mg; sulphamethaxazole 800 mg) per oral twice daily. Another convenient alternative drug is Clindamycin in the dose of 300 mg four times a day. The corticosteroids in the dose of mg per day are started 24 hours after initiating the antibiotic therapy. With regard to duration of therapy, I would continue corticosteroids until lesion borders begin to become more sharply demarcated and distinct that generally occurs by 4 to 6 weeks, at which time I will rapidly taper and discontinue corticosteroids and then stop antimicrobials completely after corticosteroids have been stopped. Antibiotics should not be tapered. Recently we have started treating our patients with local intravitreal injections of clindamycin (1.5 mg/0.1 ml) and dexamethasone (400 microg/0.1 ml) weekly for 4 weeks and are getting very encouraging results. This strategy can be used even in patients where systemic therapy may be contraindicated as in pregnancy or not tolerated. Usually with Bactrim DS or Clindamycin. Any lesion at or threatening the macula needs immediate anti-toxo agent, usually clindamycin and start with oral steroids within hrs after initiating co-trimoxazole and some cases may require prolonged treatment to prevent recurrences. Pyrimethamine along with sulphamethoxazole (Daraprim) can cause decreased platelet count and is now less commonly available at drug counters. Concomitant Folic acid treatment prevents bone marrow suppression. Recent reports show an increasing trend for using intravitreal clindamycin (with dexamethasone), is seen more commonly in recent practice with good results. Average case needs two to three injections per eye to bring about control of Retinochoroiditis. We would give ATT if there is evidence of systemic tuberculosis like a positive chest X-ray / CT chest or proven active extrapulmonary tuberculosis of any other organ. Only on the basis of a positive mantoux or Quantiferon gold test we will not start ATT. www. dosonline.org l 19
6 Experts Corner: Uvea I give ATT in multifocal serpiginoid choroiditis when Mantoux or QuantiFERON TB gold tests are positive and/or HRCT chest shows lesions suggestive of TB. In our clinic, all the patients of Serpiginouslike choroiditis are investigated for TB. The initial tests include Mantoux skin test and x-ray/cect of the chest and if Mantoux shows an induration of more than 10mm after hilar lymph nodes / Ghons focus, the patient receives ATT. In situations where these tests are equivocal, and the clinical indicators point towards the diagnosis of possible tubercular etiology, I would do quantiferon TB gold and if that too is negative, PCR from the vitreous humor for detection of Mycobacterial DNA. It is important to remember that the disease represents hypersentivity reaction to Mycobacterium tuberculosis and would need concomitant systemic steroids in the dose of 1-1.5mg/kg/day till the lesions are healed (4-6 weeks) following which steroids can be tapered and ATT continued. Failure to give systemic steroids may result in continued progression and paradoxical worsening of the lesions. If Mantoux positive, almost always. Generally start with high dose oral steroids (and IVMP if macula is involved). If investigation results suggest TB hypersensitivity add ATT after a week or so). Sometimes there may be a paradoxical reaction, which is largely initiation of ATT. We generally admit the patient and start IV Acylovir for about a week and then switch to oral acyclovir for 6-8 wks. After 48 hours of IV acyclovir oral steroids are also added. Despite aggressive therapy some patient s would develop retinal detachment and would require vitreo-retinal surgery with silicon oil injection. Role of prophylactic laser posterior to areas of necrotic retina to prevent retinal detachment is controversial We donot do prophylactic laser at margins of necrotic retina unless a distinct break is visible. I always give I.V Acyclovir 500 mg every 8th hourly for 7 days, followed by oral Acyclovir 800 mg 5 times daily or Valacyclovir 1 g 3 times daily for 12 weeks. I add tablet Prednisolone 1 mg/kg body weight after 48 hours. Yes, there is a role for prophylactic laser. I do it posterior to the lesion to create a new ora serrata once the lesion has healed completely to prevent retinal detachment, although its role is doubtful. We still treat our patients of ARN in a conservative manner where the patient is hospitalized and receives induction dose of intravenous acyclovis typically in the doses of 10-15mg per kg every 8 hours for one week for three to four months. Recently, we have also started treating some of patients on oral valacyclovir at 2 g TID that can achieve systemic levels similar to intravenous acyclovir but is more expensive than former. In addition, patients with severe disease may receive intravitreal injections of foscarnet (2.4 mg /0.1 ml) or ganciclovir in the dose of 2 mg/0.1 ml per injection given two or three times weekly. Prednisolone in the dose of 1-1.5mg/kg/day is started hours after the initiation of anti-viral therapy and aspirin added to minimize vascular thrombosis. The use of laser photocoagulation in patients with ARN is controversial, and the level of evidence supporting its use is generally weak. Currently, I am not doing any prophylactic laser in these patients. Usually with oral valacyclovir at therapeutic dose for 4 to 6 weeks, at the early breaks. Again the same scenario to other infectious empirical antimicrobial treatment with a strong clinical systemic tests. We start with IV aciclovir 500mg/m2 TDS and add systemic steroids after 24-48hrs later to prevent necrosis of retina. In patients not willing for IV treatment, alernatively Valaciclovir 1000mg tds is a good option. We with clear media, we do barrage laser to ward off the necrotic retina and prevent posterior RD from developing following large breaks, Usually RD occurs typically following acute These require extensive vitreoretinal surgery with long term silicone oil tamponade to prevent recurrence of RD. Primary immunosuppressive therapy is mostly considered in cases of VKH, Sympathetic Ophthalmia, Behcet s disease with panuveitis and necrotising scleritis. Secondary immunotherapy for steroid dependent or frequently relapsing chronic intermediate uveitis and similar steroid dependent or frequently relapsing chronic serpigeneous choroiditis or multifocal choroiditis with panuveitis. I give immunosuppressive therapy for Behçet s disease, sympathetic ophthalmia, Vogt- Koyanagi-Harada disease (once the acute phase is over), 20 l DOS Times - Vol. 20, No. 3 September, 2014
7 Uvea recalcitrant intermediate uveitis and JIA associated uveitis (methotrexate). I give immunosuppressive therapy in steroidresistant non-infectious uveitis like intermediate uveitis (mycophenolate mofetil). Most of my patients with chronic, recurrent noninfectious variety who need a maintaince dose of more than control would need immunosuppressive therapy. in patients with Behcets disease provided his PPD skin test is not positive and patient can afford it. Steroids in most cases of non-infectious bilateral panuveitis, intermediate uveitis, retinal vasculitisetc,and other immunosuppressive agents in most of these cases, which I would start either right away (for example in VKH or in Pars planitis) or after one month. Also prefer some immunosuppressant treatment if VKH or sympathetic ophthalmia is the clinical diagnosis. Another area of primary immunosuppressive agents is ANCA positive necrotizing scleritis. In children JIA associated uveitis requires primary immunosuppressive therapy. Secondary immunosuppressive treatment is used as steroid-sparing low dose maintenance in chronic diseases. We generally use Methotrexate or Azathioprine. I choose the agent according to the disease. I use Cyclosporine in Behçet s disease, mycophenolate mofetil in intermediate uveitis, azathioprine in non-tubercular serpiginous choroiditis, methotrexate in JIA associated uveitis, cyclophosphamide in Wegener s granulomatosis. We prefer oral azathioprine a lot as it seems to work very well in our population and is well tolerated. Also it is easy to monitor during the follow up. If patient is not responding to azathioprine, we do add/switch to methotraete that is also preferred drug in children and can be given by subcutaneous weekly injections. One needs to remember that most of these drugs extinguisher. Also it is important to remember that unlike corticosteroids, immunosuppressive drugs are started in lower dose and then the dose is gradually increased. It is very important to administer these drugs under the supervision of an internist who can monitor the toxic effects of these drugs. Azathioprine, methotrexate, Mycophemolate, cyclosporine and Cyclophosphmide, based on indication and affordability. Any agent which you are most familiar with and take shared responsibility to monitor and manage. Usually antimetabolites either Azathiprin or methotrexate or mycophenolate mofetil are easier to monitor. Cyclophosphamide is helpful in scleritis and needs rheumatology / internist supervision, Likewise Cyclosporin needs blood pressure and creatinine level monitoring and physician assistance. Before initiating immunosuppressive treatment we take an informed consent from every patient requiring these agents. Cases of secondary uveitis like those due to nucleus drop or intravitreal cysticercosis. Cases of intermediate uveitis where too high a dose of steroids and or immunosuppressives are required. Some cases of pars membranes. Cases of hypotony due to cyclitic membrane I advise vitrectomy in uveitis in recalcitrant intermediate uveitis and panuveitis. I would consider therapeutic vitrectomy in patients with suspected endogenous endophthalmitis, primary vitreoretinal lymphomas, vitreomacular traction, vitreous haemorrhage and tractional retinal detachment. Non-responsive dense vitirits as therapy, also where biopsy is needed, in JIA, comnine with PPL. Diagnostic vitrectomy as a procedure for obtaining vitreous specimen in infectious situations or suspected masquerade syndromes. Therapeutic vitrectomy in possible infective pathology including post-operative situations like P Acnes related chronic uveitis also requiring IOL explanation. In severe vitritis, vitrectomy alongside clearing the media also helps in removing the sequestered antigen and sometimes bring about remission in uveitis. In severe hyportony related uveitis vitrectomy with long term silicone oil tamponade is helpful. Most cases of CMV retinitis that we see today are already on HAART therapy. If not they are started on HAART therapy. In all cases intravenous ganciclovir therapy is given for 1 wk as induction therapy followed by oral valgancylovir. Duration of therapy depends on level of immune recovery and the clinical picture. For zone 1 unilateral cases intravitreal ganciclovir twice a week for 2-4 www. dosonline.org l 21
8 Experts Corner: Uvea wks followed by once a week intravitreal injections and simultaneous oral valgancyclovir therapy is given. These patients also can develop retinal detachment due to breaks at the edges of necrotic retina. This would require a vitreoretinal surgery with silicon oil injection. I give I.V Ganciclovir 5 mg/kg body weight every 12th hourly for days. If the patient is unable to afford, I give intravitreal ganciclovir. If the patient can afford, I give tablet valganciclovir 900 mg BD orally. HAART is the most important weapon in treating CMV retinitis. Sustained immune reconstitution (maintaining CD4 cells above 100/ mm³) generally allows discontinuation of anti-cmv treatment that otherwise must immune status, location and severity of the retinitis, concomitant medications and compliance with therapy. Therapy is induced at high doses for two to three weeks or until the retinitis stabilizes. The induction therapy includes intravenous ganciclovir 5mg/kg twice daily for 2 weeks with a maintaince dose of 5mg/kg/day. Alternately, Oral ganciclovir 1gm three times a day can be used for maintaince. Other alternatives include using intravenous foscarnet in the dose of 60mg/kg every night for 14 days with a maintaince dose of 90mg/kg/day. This is combined with local intravitreal injections of ganciclovir 2mg twice weekly for 3 weeks with maintaince of 2mg every week or intravitreal foscarnet 2.4 mg twice weekly for 3 weeks and maintaince of 2.4mg/weekly. Drug resistance may develop in 25-35% of cases and would need detection in case of replapses seen after long term therapy. Intravitreal gancyclovir at repeated intervals (two per week). My retinal colleagues manage. Frank CMV retinitis requires intravitreal ganciclovir injections with good response. If the disease is secondary to systemic immunosuppression (HIV related or drug related) then systemic intravenous ganciclovir and recently available oral val-ganciclovir can be added to the regimen. Peripheral suspected small CMV retinitis patches may be observed and all forms of systemic or periocular steroids avoided. If you want to sell your used Ophthalmic Equipments at Good Price OR If you are Interested to Purchase Second hand Ophthalmic Equipments at Reasonable Prices in Good Condition Please Contact: Manoj Pandey B-503, Plot No. 23, Sector-6, Dwarka, NEW DELHI-75 Ph.: , pandeymanoj67@yahoo.co.in 22 l DOS Times - Vol. 20, No. 3 September, 2014
Management of uveitis
 Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Uveitis. Pt Info Brochure. Q: What is Uvea?
 Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Differential diagnosis of posterior uveitis
 Differential diagnosis of posterior uveitis Diagnostic approach 45-year old male. Floaters and decreased vision since 1 week Fever, lymphadenopathy, myalgias, night sweats, two months ago Oral ulcer sporadically
Differential diagnosis of posterior uveitis Diagnostic approach 45-year old male. Floaters and decreased vision since 1 week Fever, lymphadenopathy, myalgias, night sweats, two months ago Oral ulcer sporadically
Update on management of Anterior Uveitis
 Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
Diagnosis of uveitis, how to proceed?
 EOS meeting Cairo, 2018 Diagnosis of uveitis, how to proceed? Mohamed G.A Saleh Lecturer of Ophthalmology Assiut University Size of the problem 15/100000 in US every year. 10% of blindness Prevalence varies
EOS meeting Cairo, 2018 Diagnosis of uveitis, how to proceed? Mohamed G.A Saleh Lecturer of Ophthalmology Assiut University Size of the problem 15/100000 in US every year. 10% of blindness Prevalence varies
Nausheen Khuddus, MD Melissa Elder, MD, PhD
 Nausheen Khuddus, MD Melissa Elder, MD, PhD Nausheen Khuddus, MD Pediatric Ophthalmologist and Strabismus Specialist Accent Physicians Gainesville, Florida What Is Uveitis? Uveitis is caused by inflammatory
Nausheen Khuddus, MD Melissa Elder, MD, PhD Nausheen Khuddus, MD Pediatric Ophthalmologist and Strabismus Specialist Accent Physicians Gainesville, Florida What Is Uveitis? Uveitis is caused by inflammatory
REFRESHER: ANTERIOR UVEITIS
 REFRESHER: ANTERIOR UVEITIS 2. SAoO Kongress 28.2.2018 Messe Luzern Dr. med. Christian Böni Augenklinik Universitätsspital Zürich Christian Böni Seite 1 Anterior Uveitis: Clinical Issues Diagnostics: yes
REFRESHER: ANTERIOR UVEITIS 2. SAoO Kongress 28.2.2018 Messe Luzern Dr. med. Christian Böni Augenklinik Universitätsspital Zürich Christian Böni Seite 1 Anterior Uveitis: Clinical Issues Diagnostics: yes
Various presentations of herpes simplex retinochoroiditis A case series
 Various presentations of herpes simplex retinochoroidits 47 Various presentations of herpes simplex retinochoroiditis A case series M. T. K. Perera 1, T. S. Keragala 1, M. Gamage 2 The Journal of the College
Various presentations of herpes simplex retinochoroidits 47 Various presentations of herpes simplex retinochoroiditis A case series M. T. K. Perera 1, T. S. Keragala 1, M. Gamage 2 The Journal of the College
Role of high-resolution computerized tomography chest in identifying tubercular etiology in patients diagnosed as Eales disease
 Kharel (Sitaula) et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:4 DOI 10.1186/s12348-016-0120-1 Journal of Ophthalmic Inflammation and Infection ORIGINAL RESEARCH Open Access Role of
Kharel (Sitaula) et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:4 DOI 10.1186/s12348-016-0120-1 Journal of Ophthalmic Inflammation and Infection ORIGINAL RESEARCH Open Access Role of
Ophthalmology. Juliette Stenz, MD
 Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
Bilateral multiple choroidal granulomas and systemic vasculitis as presenting features of tuberculosis in an immunocompetent patient
 Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Approach to Pediatric Uveitis. Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Service
 Approach to Pediatric Uveitis Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Service Epidemiology Uveitis is the 3 rd leading cause of blindness in USA 5-10% of uveitis cases involve children
Approach to Pediatric Uveitis Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Service Epidemiology Uveitis is the 3 rd leading cause of blindness in USA 5-10% of uveitis cases involve children
Regional vs. Systemic Therapy. Corticosteroids. Regional vs. Systemic Therapy for Uveitis. Considerations
 Regional vs. Systemic Therapy for Uveitis Nisha Acharya,, M.D., M.S. Director, Uveitis Service F.I. Proctor Foundation University of California, San Francisco December 4, 2010 No financial disclosures
Regional vs. Systemic Therapy for Uveitis Nisha Acharya,, M.D., M.S. Director, Uveitis Service F.I. Proctor Foundation University of California, San Francisco December 4, 2010 No financial disclosures
Surgery in patients with uveitis. Lyndell Lim and Anthony Hall
 Surgery in patients with uveitis Lyndell Lim and Anthony Hall Disclosures Off label treatments Paid advisory board Bayer Paid research support Allergan (makers of Ozurdex) Paid research support B and L
Surgery in patients with uveitis Lyndell Lim and Anthony Hall Disclosures Off label treatments Paid advisory board Bayer Paid research support Allergan (makers of Ozurdex) Paid research support B and L
Re-emerging infections: Syphilis & Tuberculosis
 Re-emerging infections: Syphilis & Tuberculosis Nicholas Jones Manchester Royal Eye Hospital Syphilis and TB - historical plagues? Syphilis incidence over 40yrs Manchester: Manchester: The Syphilis Capital
Re-emerging infections: Syphilis & Tuberculosis Nicholas Jones Manchester Royal Eye Hospital Syphilis and TB - historical plagues? Syphilis incidence over 40yrs Manchester: Manchester: The Syphilis Capital
UVEITIS. Dr. Yılmaz ÖZYAZGAN
 UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient
 CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between
 In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between the two, we also propose a classification system for
In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between the two, we also propose a classification system for
Uveitis unplugged: systemic therapy
 Uveitis unplugged: systemic therapy Hobart 2017 Peter McCluskey Save Sight Institute Sydney Eye Hospital Sydney Medical School University of Sydney Sydney Australia No financial or proprietary interest
Uveitis unplugged: systemic therapy Hobart 2017 Peter McCluskey Save Sight Institute Sydney Eye Hospital Sydney Medical School University of Sydney Sydney Australia No financial or proprietary interest
Retinal Manifestations of Systemic Disease Part 1
 The Retina and Systemic diseases Retinal Manifestations of Systemic Disease Part 1 Sundeep Dev, MD VRSF Retinal Update 2019 VitreoRetinal Surgery, PA 1 Retinitis/Vasculitis Vitreous cells Serous detachments
The Retina and Systemic diseases Retinal Manifestations of Systemic Disease Part 1 Sundeep Dev, MD VRSF Retinal Update 2019 VitreoRetinal Surgery, PA 1 Retinitis/Vasculitis Vitreous cells Serous detachments
Head prof. MUDr. E. Vlková, CSc.
 MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
Choroidal Neovascularization in Sympathetic Ophthalmia
 Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
3 main underlying causes are:
 Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu
Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu
Uveitis literature 2014: the year in review. Russell N. Van Gelder, MD, PhD Department of Ophthalmology University of Washington Seattle, WA
 Uveitis literature 2014: the year in review Russell N. Van Gelder, MD, PhD Department of Ophthalmology University of Washington Seattle, WA Disclosures RVG serves as Associate Editor of IOVS Editorial
Uveitis literature 2014: the year in review Russell N. Van Gelder, MD, PhD Department of Ophthalmology University of Washington Seattle, WA Disclosures RVG serves as Associate Editor of IOVS Editorial
Approach to Intermediate Uveitis
 Ophthalmic Deliberations Approach to Intermediate Uveitis Kirti Jaisingh, Amit Khosla, Murthy Somasheila, Reema Bansal, Parthopratim Dutta Majumder, Padmamalini Mahendradas Kirti Jaisingh MS, DNB, FICO
Ophthalmic Deliberations Approach to Intermediate Uveitis Kirti Jaisingh, Amit Khosla, Murthy Somasheila, Reema Bansal, Parthopratim Dutta Majumder, Padmamalini Mahendradas Kirti Jaisingh MS, DNB, FICO
Uveitis. What is Uveitis?
 Uveitis What is Uveitis? Uveitis [u-vee-i-tis] is a term for inflammation of the eye. It can occur in one eye or both eyes and affects the layer of the eye called the uvea [u-vee-uh]. It also can be associated
Uveitis What is Uveitis? Uveitis [u-vee-i-tis] is a term for inflammation of the eye. It can occur in one eye or both eyes and affects the layer of the eye called the uvea [u-vee-uh]. It also can be associated
2/16/17. 3 main underlying causes are:
 Definition Etiology Signs/Symptoms Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College
Definition Etiology Signs/Symptoms Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College
Dr Mallika Goyal, MD, DNBE
 Dr Mallika Goyal, MD, DNBE Address Ophthalmology Department International Pavilion Apollo Health City Near Check Post Jubilee Hills, Hyderabad 500 033 Telephone +91-40-23554563 (office) Mobile: +91-9849270994
Dr Mallika Goyal, MD, DNBE Address Ophthalmology Department International Pavilion Apollo Health City Near Check Post Jubilee Hills, Hyderabad 500 033 Telephone +91-40-23554563 (office) Mobile: +91-9849270994
Evolving therapies for posterior uveitis. Infliximab (Remicade) Infliximab: pharmacology. FDA-approved monoclonal antibody therapy Target
 Evolving therapies for posterior uveitis Sam Dahr, M.D. September 17, 2005 Midwest Ophthalmology Conference Infliximab (Remicade) FDA approved for Crohn s disease, rheumatoid arthritis, and psoriatic arthritis
Evolving therapies for posterior uveitis Sam Dahr, M.D. September 17, 2005 Midwest Ophthalmology Conference Infliximab (Remicade) FDA approved for Crohn s disease, rheumatoid arthritis, and psoriatic arthritis
!! Definition. !! Etiology. !! Signs/Symptoms. !! Classification/Diagnosis. !! Systemic Associations. !! Lab Testing. !! Treatment. !!
 Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu!!
Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu!!
Bilateral acute retinal necrosis in a patient with multiple sclerosis on natalizumab
 Bilateral acute retinal necrosis in a patient with multiple sclerosis on natalizumab Arjun B. Sood, Emory University Gokul Kumar, Emory University Joshua Robinson, Emory University Journal Title: Journal
Bilateral acute retinal necrosis in a patient with multiple sclerosis on natalizumab Arjun B. Sood, Emory University Gokul Kumar, Emory University Joshua Robinson, Emory University Journal Title: Journal
Uveitis / Iritis. Introduction. Other formats
 Other formats Introduction Uveitis / Iritis If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or translated
Other formats Introduction Uveitis / Iritis If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or translated
What do you need to know about posterior uveitis
 What do you need to know about posterior uveitis Dr. Anthony Hall MD FRANZCO Director of Ophthalmology Alfred Hospital, Melbourne, Australia Alfred Hospital Disclosures Off label treatments Paid advisory
What do you need to know about posterior uveitis Dr. Anthony Hall MD FRANZCO Director of Ophthalmology Alfred Hospital, Melbourne, Australia Alfred Hospital Disclosures Off label treatments Paid advisory
Cataract Surgery in Patients with Uveitis
 Cataract Surgery in Patients with Uveitis Chris Kalogeropoulos MD, PhD, FEBO Professor of Ophthalmology Faculty of Medicine, University of Ioannina President of Hellenic Society for the Study of Ocular
Cataract Surgery in Patients with Uveitis Chris Kalogeropoulos MD, PhD, FEBO Professor of Ophthalmology Faculty of Medicine, University of Ioannina President of Hellenic Society for the Study of Ocular
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
OCCASIONAL COMMUNICATIONS
 UVEITIS: DIAGNOSIS AND MANAGEMENT T. Akerele and S. Lightman, Department of Clinical Ophthalmology, Institute of Ophthalmology, London and Moorfields Eye Hospital, London Uveitis is a generic term which
UVEITIS: DIAGNOSIS AND MANAGEMENT T. Akerele and S. Lightman, Department of Clinical Ophthalmology, Institute of Ophthalmology, London and Moorfields Eye Hospital, London Uveitis is a generic term which
COVER FOCUS AT A GLANCE. BY LISA J. FAIA, MD, and KIMBERLY A. DRENSER, MD, PhD
 PEDIATRIC UVEITIS: CHALLENGING FOR OPHTHALMOLOGISTS, PATIENTS, AND PARENTS Management of these complicated diseases differs between pediatric and adult patient populations. BY LISA J. FAIA, MD, and KIMBERLY
PEDIATRIC UVEITIS: CHALLENGING FOR OPHTHALMOLOGISTS, PATIENTS, AND PARENTS Management of these complicated diseases differs between pediatric and adult patient populations. BY LISA J. FAIA, MD, and KIMBERLY
Uveitis and treatments; What's new?
 Uveitis and treatments; What's new? M Usman Saeed MBBS, MRCOphth, MRCS, FRCOphth (London),FRCS ( Edinburgh) Consultant Ophthalmologist, Epsom and St Helier NHS Trust Carshalton, London www.londoneyedoctors.co.uk
Uveitis and treatments; What's new? M Usman Saeed MBBS, MRCOphth, MRCS, FRCOphth (London),FRCS ( Edinburgh) Consultant Ophthalmologist, Epsom and St Helier NHS Trust Carshalton, London www.londoneyedoctors.co.uk
Patterns of uveitis in a Philippine eye clinic
 VOL. NO. PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE - MARCH 5 Harvey S. Uy, MD Irene W. Tam, OD Asian Eye Institute Makati, Philippines Patterns of uveitis in a Philippine eye clinic
VOL. NO. PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE - MARCH 5 Harvey S. Uy, MD Irene W. Tam, OD Asian Eye Institute Makati, Philippines Patterns of uveitis in a Philippine eye clinic
Laboratory Testing and Systemic Investigations in Uveitis
 Laboratory Testing and Systemic Investigations in Uveitis Investigating Uveitis A Tailored Approach Nicholas Jones The Royal Eye Hospital Manchester, UK Nicholas Jones Manchester Uveitis Clinic Manchester
Laboratory Testing and Systemic Investigations in Uveitis Investigating Uveitis A Tailored Approach Nicholas Jones The Royal Eye Hospital Manchester, UK Nicholas Jones Manchester Uveitis Clinic Manchester
Cerebral Toxoplasmosis in HIV-Infected Patients. Ahmed Saad,MD,FACP
 Cerebral Toxoplasmosis in HIV-Infected Patients Ahmed Saad,MD,FACP Introduction Toxoplasmosis: Caused by the intracellular protozoan, Toxoplasma gondii. Immunocompetent persons with primary infection
Cerebral Toxoplasmosis in HIV-Infected Patients Ahmed Saad,MD,FACP Introduction Toxoplasmosis: Caused by the intracellular protozoan, Toxoplasma gondii. Immunocompetent persons with primary infection
WAEPS Medical Personnel Conference March 20, Deanne M. Nakamoto, MD Achieve Eye and Laser Specialists Silverdale, WA
 WAEPS Medical Personnel Conference March 20, 2015 Deanne M. Nakamoto, MD Achieve Eye and Laser Specialists Silverdale, WA Up to half of UVEITIS pa/ents have GLAUCOMA. What is uvei/s? Why should we care?
WAEPS Medical Personnel Conference March 20, 2015 Deanne M. Nakamoto, MD Achieve Eye and Laser Specialists Silverdale, WA Up to half of UVEITIS pa/ents have GLAUCOMA. What is uvei/s? Why should we care?
D JO. Bilateral Shallow Anterior Chamber And Transient Myopia As A Presenting Feature Of Vogt Koyanagi Harada Syndrome
 46 Bilateral Shallow Anterior Chamber And Transient Myopia As A Presenting Feature Of Vogt Koyanagi Harada Syndrome Abstract Rahul Kumar Sharma, Abhishek Dagar, Vivek Kumar Vitreo-Retina Department, Venu
46 Bilateral Shallow Anterior Chamber And Transient Myopia As A Presenting Feature Of Vogt Koyanagi Harada Syndrome Abstract Rahul Kumar Sharma, Abhishek Dagar, Vivek Kumar Vitreo-Retina Department, Venu
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Rhegmatogenous retinal detachment in uveitis
 De Hoog et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:22 DOI 10.1186/s12348-017-0140-5 Journal of Ophthalmic Inflammation and Infection ORIGINAL ARTICLE Open Access Rhegmatogenous retinal
De Hoog et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:22 DOI 10.1186/s12348-017-0140-5 Journal of Ophthalmic Inflammation and Infection ORIGINAL ARTICLE Open Access Rhegmatogenous retinal
Mycobacterial Ocular Inflammation. Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah
 Mycobacterial Ocular Inflammation Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah Financial Disclosure I have no financial interests or relationships to disclose. Applied anatomy What
Mycobacterial Ocular Inflammation Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah Financial Disclosure I have no financial interests or relationships to disclose. Applied anatomy What
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Glaucoma & Inflammation. Jorge L. Fernandez Bahamonde, MD.
 Glaucoma & Inflammation. Jorge L. Fernandez Bahamonde, MD. Definition. Inflammatory ocular conditions compromise outflow of aqueous humor. Keratitis Episcleritis. Scleritis. Uveitis Glaucoma & Keratitis.
Glaucoma & Inflammation. Jorge L. Fernandez Bahamonde, MD. Definition. Inflammatory ocular conditions compromise outflow of aqueous humor. Keratitis Episcleritis. Scleritis. Uveitis Glaucoma & Keratitis.
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia
 JKAU: Med. Sci., Vol. 19 No. 3, pp: 73-83 (2012 A.D. / 1433 A.H.) DOI: 10.4197/Med. 19-3.6 Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia Nizamuddin Shaik Hakim Mohammad
JKAU: Med. Sci., Vol. 19 No. 3, pp: 73-83 (2012 A.D. / 1433 A.H.) DOI: 10.4197/Med. 19-3.6 Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia Nizamuddin Shaik Hakim Mohammad
Eye (2013) 27, & 2013 Macmillan Publishers Limited All rights reserved X/13 S Basu, S Nayak, TR Padhi and T Das
 (2013) 27, 657 662 & 2013 Macmillan Publishers Limited All rights reserved 0950-222X/13 www.nature.com/eye Progressive ocular inflammation following antitubercular therapy for presumed ocular tuberculosis
(2013) 27, 657 662 & 2013 Macmillan Publishers Limited All rights reserved 0950-222X/13 www.nature.com/eye Progressive ocular inflammation following antitubercular therapy for presumed ocular tuberculosis
The Wilmer Eye Institute s 34 th Annual Current Concepts in Ophthalmology March 13-17, 2017 Vail Marriott * Vail, Colorado
 The Wilmer Eye Institute s 34 th Annual Current Concepts in Ophthalmology March 13-17, 2017 Vail Marriott * Vail, Colorado Tentative 1/23/17 PROGRAM MONDAY, MARCH 13, 2017 Morning Session 6:00-7:00 Registration
The Wilmer Eye Institute s 34 th Annual Current Concepts in Ophthalmology March 13-17, 2017 Vail Marriott * Vail, Colorado Tentative 1/23/17 PROGRAM MONDAY, MARCH 13, 2017 Morning Session 6:00-7:00 Registration
The uvea and vitreous body
 The uvea and vitreous body Development of the eye Primary vitreous Mesenchymal invasion Secondary vitreous From the retina: tertiary vitreous Mesenchymal cells: uvea, cornea stroma, slera Vascular tunic
The uvea and vitreous body Development of the eye Primary vitreous Mesenchymal invasion Secondary vitreous From the retina: tertiary vitreous Mesenchymal cells: uvea, cornea stroma, slera Vascular tunic
Optical coherence tomography findings in a child with posterior scleritis
 European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D.
 A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D. I. Introduction II. III. IV. A. Why I am giving this talk B. What to take from lecture Diagnosis 1. Better understanding
A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D. I. Introduction II. III. IV. A. Why I am giving this talk B. What to take from lecture Diagnosis 1. Better understanding
Author Manuscript Faculty of Biology and Medicine Publication
 Serveur Académique Lausannois SERVAL serval.unil.ch Author Manuscript Faculty of Biology and Medicine Publication This paper has been peer-reviewed but dos not include the final publisher proof-corrections
Serveur Académique Lausannois SERVAL serval.unil.ch Author Manuscript Faculty of Biology and Medicine Publication This paper has been peer-reviewed but dos not include the final publisher proof-corrections
Recalcitrant Diabetic Macular Oedema: Therapeutic Options
 December 2007 A. Giridhar et al. - Recalcitrant DME 451 CONSULTATION S E C T I O N Recalcitrant Diabetic Macular Oedema: Therapeutic Options Dr. Cyrus M Shroff 1, Dr. N S Muralidhar 2, Dr. R Narayanan
December 2007 A. Giridhar et al. - Recalcitrant DME 451 CONSULTATION S E C T I O N Recalcitrant Diabetic Macular Oedema: Therapeutic Options Dr. Cyrus M Shroff 1, Dr. N S Muralidhar 2, Dr. R Narayanan
UNDERSTAND MORE ABOUT UVEITIS UVEITIS
 UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
PDF of Trial CTRI Website URL -
 Clinical Trial Details (PDF Generation Date :- Sun, 07 Apr 2019 21:50:45 GMT) CTRI Number Last Modified On 11/03/2019 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Clinical Trial Details (PDF Generation Date :- Sun, 07 Apr 2019 21:50:45 GMT) CTRI Number Last Modified On 11/03/2019 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Slide 4. Slide 5. Slide 6
 Slide 1 Slide 4 Demographics El Paso Eye Care Border Healthcare-Based Grand Rounds Derek N. Cunningham, O.D. 80-90% Mexican-Americans Diabetes Hypertension Hyperlipidemia Obesity 70% uninsured High poverty
Slide 1 Slide 4 Demographics El Paso Eye Care Border Healthcare-Based Grand Rounds Derek N. Cunningham, O.D. 80-90% Mexican-Americans Diabetes Hypertension Hyperlipidemia Obesity 70% uninsured High poverty
Retina Grand Rounds. Stephen Huddleston MD Charles Retina Institute University of Tennessee Hamilton Eye Institute
 Retina Grand Rounds Stephen Huddleston MD Charles Retina Institute University of Tennessee Hamilton Eye Institute Fundus Autoflourescence 2013 2016 Plaquenil Toxicity Excellent treatment for a variety
Retina Grand Rounds Stephen Huddleston MD Charles Retina Institute University of Tennessee Hamilton Eye Institute Fundus Autoflourescence 2013 2016 Plaquenil Toxicity Excellent treatment for a variety
Abbreviated Drug Evaluation: Fluocinolone acetonide intravitreal implant (Retisert )
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
PDF of Trial CTRI Website URL -
 Clinical Trial Details (PDF Generation Date :- Sat, 09 Mar 2019 11:07:43 GMT) CTRI Number Last Modified On 08/08/2018 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Clinical Trial Details (PDF Generation Date :- Sat, 09 Mar 2019 11:07:43 GMT) CTRI Number Last Modified On 08/08/2018 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Sudden Vision Loss. Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists
 Sudden Vision Loss Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists My Credentials -Residency in Ophthalmology at the LSU Eye Center in New Orleans, LA -Fellowship
Sudden Vision Loss Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists My Credentials -Residency in Ophthalmology at the LSU Eye Center in New Orleans, LA -Fellowship
UVEITIS IN GENERAL. Information for patients UVEITIS CLINIC WHAT IS UVEITIS? MAIN CATEGORIES OF UVEITIS
 Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
The White Re)na. Joseph Alsberge, MD January 20, 2018
 The White Re)na Joseph Alsberge, MD January 20, 2018 58 y/o man with floaters and pain OD x 2 weeks PMH: oral and genital herpes Va OD 20/50 Anterior OD: KP and 3+ AC cell Posterior: Vitri)s, occlusive
The White Re)na Joseph Alsberge, MD January 20, 2018 58 y/o man with floaters and pain OD x 2 weeks PMH: oral and genital herpes Va OD 20/50 Anterior OD: KP and 3+ AC cell Posterior: Vitri)s, occlusive
10/18/2018. Unraveling Uveitis
 Unraveling Uveitis Trenton Cleghern, OD, FAAO VisionAmerica UAB School of Optometry 11/10/2018 1 Disclosure Statement: Nothing to disclose 2 Objectives Classify uveitis Current and new therapeutic options
Unraveling Uveitis Trenton Cleghern, OD, FAAO VisionAmerica UAB School of Optometry 11/10/2018 1 Disclosure Statement: Nothing to disclose 2 Objectives Classify uveitis Current and new therapeutic options
Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 743-748 Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 743-748 Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
A Clinical Study of Anterior Uveitis in a Rural Hospital
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. III. (Mar. 2014), PP 55-59 A Clinical Study of Anterior Uveitis in a Rural Hospital
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. III. (Mar. 2014), PP 55-59 A Clinical Study of Anterior Uveitis in a Rural Hospital
Anthony DeWilde, O.D Linwood Blvd. Kansas City, MO x
 Anthony DeWilde, O.D. 4801 Linwood Blvd. Kansas City, MO 64128 816-861-4700 x 57411 anthony.dewilde@va.gov Uveitis and Glaucoma: The Seven Reasons Why IOP Can Increase in Uveitis (and What to do About
Anthony DeWilde, O.D. 4801 Linwood Blvd. Kansas City, MO 64128 816-861-4700 x 57411 anthony.dewilde@va.gov Uveitis and Glaucoma: The Seven Reasons Why IOP Can Increase in Uveitis (and What to do About
o White dot syndromes pattern recognition o Activity and damage o Quality of life o Key points o Idiopathic o Sarcoidosis o Multiple sclerosis
 Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Algorithm of Choroiditis
 10.5005/jp-journals-10020-1027 REVIEW ARTICLE Ovi Sofia, Sudharshan Sridharan, Jyotirmay Biswas ABSTRACT Choroiditis may present as focal or multifocal lesions, and could be due to infectious or noninfectious
10.5005/jp-journals-10020-1027 REVIEW ARTICLE Ovi Sofia, Sudharshan Sridharan, Jyotirmay Biswas ABSTRACT Choroiditis may present as focal or multifocal lesions, and could be due to infectious or noninfectious
Opportunistic Infections BHIVA Guidelines
 Opportunistic Infections BHIVA Guidelines Mark Nelson David Dockrell Simon Edwards I have.. 1. Read all of the BHIVA guidelines 12% 2. Read some of the BHIVA guidelines in their entirety 3. Browsed some
Opportunistic Infections BHIVA Guidelines Mark Nelson David Dockrell Simon Edwards I have.. 1. Read all of the BHIVA guidelines 12% 2. Read some of the BHIVA guidelines in their entirety 3. Browsed some
Case Study: Fuzz April 18th
 Case Study: Fuzz April 18th 33 year old Quarter Horse Had been battling corneal ulcer for several weeks before seeing us No foreign debris found Culture and cytology were taken. Started on topical antibiotics,
Case Study: Fuzz April 18th 33 year old Quarter Horse Had been battling corneal ulcer for several weeks before seeing us No foreign debris found Culture and cytology were taken. Started on topical antibiotics,
How and Why Should we Care? Muge R. Kesen, MD Retina Specialty Institute (RSI)
 How and Why Should we Care? Muge R. Kesen, MD Retina Specialty Institute (RSI) Disclosure No financial interest or relationships to disclose. Objectives Overview of different types of uveitis Diagnostic
How and Why Should we Care? Muge R. Kesen, MD Retina Specialty Institute (RSI) Disclosure No financial interest or relationships to disclose. Objectives Overview of different types of uveitis Diagnostic
Fever in Lupus. 21 st April 2014
 Fever in Lupus 21 st April 2014 Fever in lupus Cause of fever N= 487 % SLE fever 206 42 Infection in SLE 265 54.5 Active SLE and infection 8 1.6 Tumor fever 4 0.8 Miscellaneous 4 0.8 Crucial Question Infection
Fever in Lupus 21 st April 2014 Fever in lupus Cause of fever N= 487 % SLE fever 206 42 Infection in SLE 265 54.5 Active SLE and infection 8 1.6 Tumor fever 4 0.8 Miscellaneous 4 0.8 Crucial Question Infection
Uveitis: Classification, Etiologies and Clinical Signs
 E-ISSN 2454-2784 Recent Advances Uveitis: Classification, Etiologies and Clinical Signs Aditya Shreekant Kelkar 1, Ekta Rakesh Arora 1, B.Sowkath 2, Jyotirmay Biswas 3 1 National Institute of Ophthalmology,Pune
E-ISSN 2454-2784 Recent Advances Uveitis: Classification, Etiologies and Clinical Signs Aditya Shreekant Kelkar 1, Ekta Rakesh Arora 1, B.Sowkath 2, Jyotirmay Biswas 3 1 National Institute of Ophthalmology,Pune
Title. CitationJapanese Journal of Ophthalmology, 50(6): Issue Date Doc URL. Rights. Type. File Information
 Title Chronic panuveitis and scleritis in a patient with c Author(s)Saito, Wataru; Saito, Akari; Namba, Kenichi; Kase, S CitationJapanese Journal of Ophthalmology, 50(6): 558-561 Issue Date 2006 Doc URL
Title Chronic panuveitis and scleritis in a patient with c Author(s)Saito, Wataru; Saito, Akari; Namba, Kenichi; Kase, S CitationJapanese Journal of Ophthalmology, 50(6): 558-561 Issue Date 2006 Doc URL
a mimicker of Wegener s Granulomatosis
 a mimicker of Wegener s Granulomatosis Combined Meeting October 2009 a story of 2 ladies Madam JA 56 year-old Madam RH 36 year-old Madam JA 56 year-old Apr 2008 May Jun Jul Aug Sept Oct Nov 2008 Madam
a mimicker of Wegener s Granulomatosis Combined Meeting October 2009 a story of 2 ladies Madam JA 56 year-old Madam RH 36 year-old Madam JA 56 year-old Apr 2008 May Jun Jul Aug Sept Oct Nov 2008 Madam
Intravitreal Corticosteroid Implants
 Intravitreal Corticosteroid Implants Policy Number: 9.03.23 Last Review: 4/2018 Origination: 07/2015 Next Review: 4/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Intravitreal Corticosteroid Implants Policy Number: 9.03.23 Last Review: 4/2018 Origination: 07/2015 Next Review: 4/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Sarcoidosis and Uveitis
 Sarcoidosis and Uveitis Nicholas Jones Royal Eye Hospital Manchester, UK Sarcoidosis a multisystem chronic inflammation causing multifocal non-caseating granulomas BUT Diagnosis often made indirectly (without
Sarcoidosis and Uveitis Nicholas Jones Royal Eye Hospital Manchester, UK Sarcoidosis a multisystem chronic inflammation causing multifocal non-caseating granulomas BUT Diagnosis often made indirectly (without
WHAT IS YOUR DIAGNOSIS? By ADREA R. BENKOFF M.D.
 WHAT IS YOUR DIAGNOSIS? By ADREA R. BENKOFF M.D. Anterior Chamber Inflammation and Iris Depigmentation Noted 25 Years After Cataract Extraction Decreasing Vision Over a 5- Year Period 64 year old white
WHAT IS YOUR DIAGNOSIS? By ADREA R. BENKOFF M.D. Anterior Chamber Inflammation and Iris Depigmentation Noted 25 Years After Cataract Extraction Decreasing Vision Over a 5- Year Period 64 year old white
The Leeds Teaching Hospitals NHS Trust Uveitis in children and young people
 n The Leeds Teaching Hospitals NHS Trust Uveitis in children and young people A guide for young people and parents/carers This leaflet is for parents who have a child with uveitis and for young people
n The Leeds Teaching Hospitals NHS Trust Uveitis in children and young people A guide for young people and parents/carers This leaflet is for parents who have a child with uveitis and for young people
Clinical Course of Uveitis in Children in a Tertiary Ophthalmology Center in Northwest Iran
 http://www.cjmb.org Open Access Original Article Crescent Journal of Medical and Biological Sciences Vol. 4, No. 4, October 2017, 200 204 eissn 2148-9696 Clinical Course of Uveitis in Children in a Tertiary
http://www.cjmb.org Open Access Original Article Crescent Journal of Medical and Biological Sciences Vol. 4, No. 4, October 2017, 200 204 eissn 2148-9696 Clinical Course of Uveitis in Children in a Tertiary
Department of Ophthalmology
 Period : 03/July/17 to 07/September/17 Semester : 7 th Semester Department of Ophthalmology Lecture Lesson Plan Sr 1 03.07.17 Uvea-Anatomy, Uvea-Anatomy, Classification of Uveitis Dr R Paranjpe Classification
Period : 03/July/17 to 07/September/17 Semester : 7 th Semester Department of Ophthalmology Lecture Lesson Plan Sr 1 03.07.17 Uvea-Anatomy, Uvea-Anatomy, Classification of Uveitis Dr R Paranjpe Classification
Intravitreal Corticosteroid Implants. Description
 Subject: Intravitreal Corticosteroid Implants Page: 1 of 20 Last Review Status/Date: June 2015 Intravitreal Corticosteroid Implants Description An intravitreal implant is a drug delivery system, injected
Subject: Intravitreal Corticosteroid Implants Page: 1 of 20 Last Review Status/Date: June 2015 Intravitreal Corticosteroid Implants Description An intravitreal implant is a drug delivery system, injected
Department of Ophthalmology
 Department of Ophthalmology Period : 02/July/18 to 30/August/18 Semester : 7 th Semester Lecture Lesson Plan Sr. Date Topic Lesson plan Name of Faculty No. 1 02.07.18 Lens- Lens-Anatomy, Classification
Department of Ophthalmology Period : 02/July/18 to 30/August/18 Semester : 7 th Semester Lecture Lesson Plan Sr. Date Topic Lesson plan Name of Faculty No. 1 02.07.18 Lens- Lens-Anatomy, Classification
in Uveitis Euretina Hamburg 2013 Nicholas Jones Royal Eye Hospital Manchester, UK
 Cataract Surgery in Uveitis Euretina Hamburg 2013 Nicholas Jones Royal Eye Hospital Manchester, UK Cataract surgery in eyes with uveitis is not routine It requires much more pre-operative planning It may
Cataract Surgery in Uveitis Euretina Hamburg 2013 Nicholas Jones Royal Eye Hospital Manchester, UK Cataract surgery in eyes with uveitis is not routine It requires much more pre-operative planning It may
Ocular Pathology. I. Congenital and/or developmental. A. Trisomy 21. Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea)
 I. Congenital and/or developmental Robbins Pathologic Basis of Disease, 6 th Ed. A. Trisomy 21 Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea) Focal hypoplasia of iris Cataracts frequently
I. Congenital and/or developmental Robbins Pathologic Basis of Disease, 6 th Ed. A. Trisomy 21 Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea) Focal hypoplasia of iris Cataracts frequently
Vanderbilt Eye Institute Clinical Trials
 April, 2010 Vanderbilt Eye Institute Clinical Trials Ophthalmology Actively Recruiting Studies For information on our clinical trials and other studies, please contact: Sandy Owings, COA, CCRP Clinic Director
April, 2010 Vanderbilt Eye Institute Clinical Trials Ophthalmology Actively Recruiting Studies For information on our clinical trials and other studies, please contact: Sandy Owings, COA, CCRP Clinic Director
ISPUB.COM. An Atypical Presentation of Posterior Scleritis. A Ramanathan, A Gaur CASE REPORT
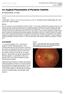 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
Anti VEGF Agents in Retinal Disorders Current Scenario
 Retina Anti VEGF Agents in Retinal Disorders Current Scenario Charu Gupta MS Charu Gupta MS, Cyrus M. Shroff MD Shroff Eye Centre, New Delhi T is a group of proteins involved in the regulation of angiogenesis,
Retina Anti VEGF Agents in Retinal Disorders Current Scenario Charu Gupta MS Charu Gupta MS, Cyrus M. Shroff MD Shroff Eye Centre, New Delhi T is a group of proteins involved in the regulation of angiogenesis,
84 Year Old with Rosacea
 84 Year Old with Rosacea S/p tap and injection of intravitreal vancomycin, ceftazidime, dexamethasone Post-injection day#1 Va HM IOP 14 mmhg Post-injection week#3 BCVA 20/20-3 (plano +0.50 x 180) IOP 23
84 Year Old with Rosacea S/p tap and injection of intravitreal vancomycin, ceftazidime, dexamethasone Post-injection day#1 Va HM IOP 14 mmhg Post-injection week#3 BCVA 20/20-3 (plano +0.50 x 180) IOP 23
Necrotizing retinitis of multifactorial etiology
 Romanian Journal of Ophthalmology, Volume 61, Issue 1, January-March 2017. pp:49-53 CASE REPORT Necrotizing retinitis of multifactorial etiology Pirvulescu Ruxandra Angela* **, Popa Cherecheanu Alina*
Romanian Journal of Ophthalmology, Volume 61, Issue 1, January-March 2017. pp:49-53 CASE REPORT Necrotizing retinitis of multifactorial etiology Pirvulescu Ruxandra Angela* **, Popa Cherecheanu Alina*
Original Effective Date: 12/13/2017. Subject: Intravitreal corticosteroid implants: Retisert (fluocinolone acetonide intravitreal implant)
 Subject: Intravitreal corticosteroid implants: Retisert (fluocinolone acetonide intravitreal implant) Policy Number: MCP-302 Original Effective Date: 12/13/2017 Revision Date(s): Review Date: DISCLAIMER
Subject: Intravitreal corticosteroid implants: Retisert (fluocinolone acetonide intravitreal implant) Policy Number: MCP-302 Original Effective Date: 12/13/2017 Revision Date(s): Review Date: DISCLAIMER
Management of Immune Reconstitution Inflammatory Syndrome (IRIS)
 Management of Immune Reconstitution Inflammatory Syndrome (IRIS) Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the IRIS Guideline
Management of Immune Reconstitution Inflammatory Syndrome (IRIS) Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the IRIS Guideline
DNB Question Paper. December 1
 DNB Question Paper December 1 December,2013 DNB Examination 2013 (December) IMPORTANT INSTRUCTIONS: This question paper consists of 10 questions divided into Part A and Part B, each part containing 5 questions.
DNB Question Paper December 1 December,2013 DNB Examination 2013 (December) IMPORTANT INSTRUCTIONS: This question paper consists of 10 questions divided into Part A and Part B, each part containing 5 questions.
DIAGNOSIS AND MANAGEMENT OF ANTERIOR UVEITIS POA SPRING CONFERENCE BERNARD H. BLAUSTEIN, O.D., F.A.A.O.
 DIAGNOSIS AND MANAGEMENT OF ANTERIOR UVEITIS POA SPRING CONFERENCE - 2009 Classification of Anterior Uveitis BERNARD H. BLAUSTEIN, O.D., F.A.A.O. A. Anatomic location 1. Iritis Cells and flare mostly in
DIAGNOSIS AND MANAGEMENT OF ANTERIOR UVEITIS POA SPRING CONFERENCE - 2009 Classification of Anterior Uveitis BERNARD H. BLAUSTEIN, O.D., F.A.A.O. A. Anatomic location 1. Iritis Cells and flare mostly in
Ganciclovir-resistant CMV retinitis in a patient with wild-type plasma CMV. North Carolina School of Medicine, Chapel Hill, NC
 JCM Accepts, published online ahead of print on 15 February 2012 J. Clin. Microbiol. doi:10.1128/jcm.00029-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 Ganciclovir-resistant
JCM Accepts, published online ahead of print on 15 February 2012 J. Clin. Microbiol. doi:10.1128/jcm.00029-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 Ganciclovir-resistant
