Abstract. Introduction. Chapter 7. Phase I/II study for treatment of refractory CMV reactivation
|
|
|
- Carmella Kelley
- 5 years ago
- Views:
Transcription
1 Treatment of refractory cytomegalovirus reactivation after allogeneic stem cell transplantation with in vitro generated cytomegalovirus pp65-specific CD8+ T cell lines Pauline Meij, Inge Jedema, Maarten L. Zandvliet, Pim L.J. van der Heiden, H.M. Esther van Egmond, Ellis van Liempt, Conny Hoogstraten, Marian van de Meent, Sabrina Veld, W.A. Erik Marijt, Peter A von dem Borne, Arjan C. Lankester, Constantijn J.M. Halkes J.H. Frederik Falkenburg Submitted
2 Abstract To treat patients with refractory cytomegalovirus (CMV) reactivation after allogeneic stem cell transplantation a phase I/II clinical study on adoptive transfer of in vitro generated donor or patient derived CMV pp65-specific CD8+ T cell lines was performed. Peripheral blood mononuclear cells from CMV seropositive donors or patients were stimulated with HLA-A*0201 and/or HLA-B*002 restricted pp65 peptides (NLV/TPR) and one day after stimulation interferon-gamma (IFNγ) producing cells were enriched using the IFNγ capture assay, and cultured with autologous feeders and low dose IL-2. After 8-14 days of culture quality controls were performed and the CMV-specific T cell lines were administered or cryopreserved. The T cell lines generated contained 1-1x10 6 cells, comprising 54-96% CMV pp65-specific CD8+ T cells, and showed CMV-specific lysis of target cells. To date 14 CMVspecific T cell lines were generated of which were administered to patients with refractory CMV reactivation. After administration no adverse events were observed and CMV load decreased and remained negative. In several patients a direct relation between administration of the T cell line and the in vivo appearance of CMV pp65-specific T cells could be documented. In conclusion, administration of CMV pp65-specific CD8+ T cell lines was found to be feasible and safe, and efficacy of administered CMV pp65-specific CD8+ T cell lines was demonstrated. Introduction Allogeneic stem cell transplantation (allosct) is a potentially curative treatment for a variety of hematological malignancies and inherited hematopoietic disorders. A significant complication of allosct is the development of severe graft versus host disease (GvHD), which can be treated by immune suppression. Depletion of T cells from the stem cell graft can also be performed to prevent the development of severe GvHD after allosct. However, T cell depletion or immune suppression significantly delays immune reconstitution in patients after allosct, which is associated with an increased risk of opportunistic infections including CMV infection [1-3]. Reactivation of CMV can cause serious morbidity and mortality during the prolonged period of immune deficiency following allosct, which is also illustrated by increased CMV-related morbidity in patients receiving a graft from a CMV seronegative donor [4,5]. The availability of antiviral agents like ganciclovir and foscarnet has contributed to a significant reduction of CMV-related morbidity and mortality following allosct. However, if appropriate T cell responses against CMV do not develop after allosct subsequent viral reactivations and refractory disease are commonly observed. Reconstitution of the CMV-specific T cell repertoire directed against immunodominant proteins, like CMV pp65, in the first year after allosct has been demonstrated to confer sustained protection from CMV disease. Furthermore, for the long-term protection against CMV the development of CMV-specific T cell immunity has been found to be essential [6-9]. Therefore, adoptive transfer of donor-derived virus-specific T cells is an attractive strategy for treatment of viral disease in allosct recipients. Clinical studies have demonstrated that the adoptive transfer of donor-derived CMV-specific memory T cells can be a safe and effective treatment for patients with refractory CMV reactivation [10-18]. In most clinical studies CMV-specific CD8+ T cell lines were generated by repetitive stimulation of the T cells in vitro for several weeks to obtain highly pure T cell lines to minimize the risk of the induction of GvHD [10-16]. However, isolation of CMV-specific T cells from peripheral blood also allows the generation of highly specific T cell lines without prolonged culture and repetitive stimulation. Since it has been demonstrated that adoptive transfer of interferon-gamma (IFNγ)-producing memory T cells can provide longlived functional memory T cell reconstitution and that the presence of IFNγ producing CMV-specific T cells is associated with protection from CMV reactivation isolation of CMVspecific memory CD8+ T based on their IFNγ production is an attractive strategy for generating effective CMV-specific CD8+ T cell lines [4,6,,9,15,18,19]. Although clinical studies have shown that adoptive transfer of CMV-specific T cells is safe en effective, in
3 these studies the infusion of CMV specific CD8+ T cells could not always be directly correlated to a clinical effect. In this study, a phase I/II clinical protocol for the adoptive transfer of donor or patient derived CMV pp65-specific CD8+ T cell lines for patients with refractory CMV reactivation after allosct was conducted. CMV-specific T cells were isolated using a IFNγ-based isolation technique and cultured for 1 to 2 weeks. Five patients with CMV reactivation failing antiviral therapy were treated with these CMV pp65-specific CD8+ T cell lines. In all five patients CMV DNA load turned negative and CMV-specific T cells could be detected in the peripheral blood. In two patients a direct relation was shown between the administration of CMV-specific T cells, the appearance of CMV-specific T cells in the peripheral blood and the clearance of CMV reactivation. Materials and Methods Study design Adult and pediatric patients with refractory CMV reactivation after allosct were eligible. Patients were weekly monitored for CMV reactivation after receiving a stem cell transplant. Refractory CMV reactivation was defined as high CMV load for more than two weeks while receiving pharmacotherapy or as early relapse after therapy. Since only peptides binding HLA-A*0201 or HLA-B*002 were available for clinical use and therefore only T cells specific for these epitopes could be isolated, only HLA-A*0201 and/or HLA-B*002 positive patients were eligible. When the donor was CMV seropositive a donor-derived T cell line was generated, when the donor was CMV seronegative a patient-derived T cell line was generated. When the CMV pp65-specific T cell line met the release criteria and CMV load was still positive the T cell line was administered to the patient. The procedure could be repeated two times in case of stable or progressive disease and no severe toxicity. Collection of peripheral blood cells After informed consent at least 2x10 9 peripheral blood mononuclear cells (PBMC) were harvested by leukopheresis from each donor or patient. Red blood cells were lysed using a NH4Cl (8.4 g/l) and KHCO3 (1 g/l) buffer (ph=.4) (Leiden University Medical Center, Department of Clinical Pharmacy, Leiden, The Netherlands). PBMC were directly used or cryopreserved in the vapor phase of liquid nitrogen until further use. Cells were cryopreserved in Iscove's modified Dulbecco's medium (IMDM) (Lonza, Basel, Switzerland) containing 20 g/l human albumin (CeAlb, Sanquin, Amsterdam, The Netherlands) and 10% dimethyl sulphoxide (DMSO) (Leiden University Medical Center, Department of Clinical Pharmacy, Leiden, The Netherlands). Generation and administration of clinical grade CMV-specific CD8+ T cell lines Donor or patient PBMC were resuspended in medium consisting of IMDM supplemented with 3 mmol/l L-glutamine (Lonza) and 100 U/ml penicillin and 100 µg/ml streptomycin (Lonza) plus 10% heat-inactivated pooled prescreened AB serum from healthy blood bank donors. Cells were cultured at a cell concentration of 10x10 6 cells/ml and 1 µg/ml of peptide was added. Peptides used were the HLA-A*0201 binding peptide NLVPMVATV (NLV) and the HLA-B*002 binding peptide TPRVTGGGAM (TPR) both purchased from Bachem (Bubendorf, Switzerland). After overnight stimulation IFNγ secreting cells were isolated using the CliniMACS cytokine capture system (Miltenyi Biotec, Bergisch Gladbach, Germany) according to manufacturer s instructions. After washing the positive fraction was resuspended in culture medium containing 10 IU/ml IL-2 (Proleukin, Novartis Pharma B.V., Arnhem, The Netherlands). Cells were cultured at a 1:10 ratio with irradiated (30 kgy) feeder cells, which were obtained from the negative fraction after isolation. Cultures were refreshed every 3 to 4 days and after 8 to 14 days the T cell lines were analyzed. Cultures were evaluated for the presence of CMV NLV- and/or TPR-specific CD8+ T cells by tetramer staining and quality control was performed. Quality assurance specifications included: (1) no microbiological contamination, (2) confirmation of the origin of the material (donor or patient), (3) the presence of minimally 50% of CMV-specific CD8+ T cells within the CD3+ population, (4) the presence of maximally 10% CD19+ B-cells and (5) functionality in a 51 Cr release assay defined as minimally 20% lysis of positive target cells and maximally 10% lysis of negative target cells. When released for administration, the CMV-specific T cell lines were resuspended in 100 ml NaCl 0.9% (LUMC Pharmacy) supplemented with 2% human albumin (Sanquin) in a 500 ml Cryocyte Freezing Container (Baxter, Deerfield, IL). Phenotypic analysis To determine the composition and phenotype of the starting material, the fractions after isolation and the T cell line, cells were stained using FITC-labeled TCRαβ, CD14, CD4 and HLA-DR (BD Biosciences, San Jose, CA), PE-labeled TCRγδ, CD56, CD25 (BD) and IFNγ (Miltenyi Biotec), PerCP-labeled CD8 and CD3 (BD), APC labeled CD19, CD33 (BD) and CD4 (Beckman Coulter, Fullerton, CA) and PE- or APC-labeled tetramers of the NLVPMVATV bound to HLA-A*0201 or TPRVTGGGAM bound to HLA-B*002, which
4 were prepared as described previously [20]. After labeling cells were analyzed on a FACSCalibur (BD). Cytotoxicity assay To determine the cytotoxicity of the T cell lines standard 51 Chromium ( 51 Cr) release assays were performed as described previously [21]. Target cells (donor and patient phytohemagglutinin (PHA) blasts) were loaded with 100 µci of Na 51 Cr2O4 (Amersham, Roosendaal, The Netherlands) for 1 hour and when necessary 1µM of peptide (NLV or TPR) was also added. Effector/Target (E/T) ratios ranged from 30:1 to 1:1 and after 4 hours of incubation 51 Cr release was determined. days of culture respectively (Figure 1C and 1G), specific proliferation of the NLV-specific CD8+ T cells resulted in the donor-derived T cell line containing 83% NLV-specific CD8+ T cells and the patient-derived T cell line containing 66% NLV-specific CD8+ T cells. Ex vivo identification of CMV-specific CD8+ T cells To identify donor or recipient origin of CMV-specific T cells reconstituting in peripheral blood after infusion of the CMV pp65-specific CD8+ T cell lines, PBMC from the patient were stained using HLA class I tetramers specific for NLV or TPR. Subsequently, the-hla tetramer-positive CD8+ T cells were selected by flow cytometric sorting using a FACSDiva and Cellquest software (BD). The DNA profile of the sorted cells was established by chimerism analysis based on short tandem repeats polymorphism as previously described [22]. Results Generation of clinical grade CMV specific CD8+ T cell lines A total of 11 donor-derived and 3 patient-derived CMV-specific T cell lines specific for the HLA-A*0201 restricted NLV epitope and/or for the HLA-B*002 restricted TPR epitope were generated for patients failing antiviral therapy after allosct. Donor-derived T cell lines were generated when both donor and patient were CMV seropositive, whereas patient derived T cell lines were generated when the donor was CMV seronegative and the patient CMV seropositive. Figure 1 shows the data of a representative donor-derived (1A - 1D) and patient-derived (1E 1H) CMV specific T cell line. The precursor frequencies of the NLVspecific T cells in the PBMC starting material were 0.4% in the donor material (Figure 1A) and 1.45% in the patient material (Figure 1E). After overnight stimulation with the HLA-A*0201 binding NLV peptide, IFNγ producing cells were isolated using the Cytokine Capture System. The positive fraction contained between 20 25% IFNγ positive CD8+ T cells within the T cell fraction (Figure 1B and Figure 1F). Other T cells present in the positive fraction were CD4+ T cells and IFNγ negative CD8+ T cells. After 10 days and Figure 1. Composition and functionality of donor derived (A-D) and patient derived (E-H) CMV-specific T cell lines. (A, E) the percentage of NLV (A) and TPR (E) -specific T cells in the starting material (day 0); (B, F) the percentage of IFNγ positive cells in the positive fraction directly after isolation; (C, G) the percentage of NLV (C) or TPR (G) in the T cell line after culture (day ); (D, H) functionality of the T cell lines in a 51 Cr release assay. Dot plots are shown and events shown are gated on lymfogate and PI-negative gate. Percentage lysis after 4 hours in a 51 Cr release assay at an E:T ratio of 3:1 is depicted
5 Less than 1% of CD19+ B-cells were detected in the T cell lines (data not shown). As is shown in Figure 1D and 1H both T cell lines showed reactivity against NLV- or TPR peptide-loaded target cells and no reactivity against donor or patient cells. Furthermore, both T cell lines also showed recognition of endogenously presented antigen using pp65 transduced EBV-LCL. Table 1 shows the results of all the CMV-specific T cell lines generated. Precursor frequencies of NLV- and/or TPR-specific CD8+ T cells in the donor or patient starting material used for the generation of the T cell lines ranged from % of total PBMC. Cell numbers obtained direct after isolation ranged from 1.0 to 14.4x10 6 cells and contained between 3 to 45 % IFNγ positive CD8+ T cells within the T cell population. Total cell numbers obtained after culture ranged from 1.0 to 1.1x10 6 cells. During culture no increase in total cell numbers was observed, however, enrichment of CMV-specific T cells was observed, since the T cell lines contained between 54-96% of NLV-and/or TPR-specific T cells. Table1. Characteristics of the CMV-specific T cell lines T cell line Specificity Frequency in PBMC # cells (x10 6 ) 2 Phenotype (% positive cells) 2 # cells (x10 6 ) 2 Cytotoxicity 2,3 PHA Donor - peptide + peptide CD4 CD8 CD8+ CD8+ Tet+ Tet+ P1-a TPR P1-b TPR P2-a TPR P3-a TPR P4-a NLV/TPR <0.01 / / P4-b NLV/TPR <0.01 / / P5-a TPR P-a NLV/TPR 0.04 / / P8-a 1 TPR P9-a NLV P9-b NLV P10-a 1 NLV P11-a 1 NLV P12-a NLV patient-derived T cell line; 2 after -14 days culture; 3 percentage lysis after 4 hours in a 51 Cr release assay, E:T ratio of 3:1; 4 measured in a CFSE based cytotoxicity assay [2]; Tet = tetramer; PHA = phytohemagglutinin blast. PHA patient All 14 donor and patient derived CMV specific T cell lines generated met the quality control criteria. No microbiological contamination was detected in any of the T cell lines and chimerism analysis showed the correct origin of the material. As is shown in Table 1 all T cell lines contained more than 50% of NLV- and/or TPR- specific T cells within the CD3+ population and all T cell lines showed recognition of peptide-loaded PHA blasts and no reactivity against donor or patient derived PHA blasts. Administration of CMV-specific CD8+ T cell lines In a phase I/II study the toxicity and the potential antiviral effect of treatment with CMV pp65-specific T cell lines for refractory CMV reactivation following allogeneic SCT was investigated. Five patients with refractory CMV reactivation following allosct received donor derived CMV pp65-specific T cell line(s). Three patients (patient 2, 3 and 4) received one CMV pp65-specific T cell line and two patients (patient 1 and 9) received two CMV pp65-specific T cell lines. The other T cell lines generated were not administrated, since patients were CMV load negative (n=4), had relapsed (n=1) or deceased due to CMV disease (n=2) at the time the production of the CMV pp65-specific T cell line was completed. Despite treatment with antiviral agents all five patients who received a CMV pp65-specific T cell line had positive CMV DNA loads (log 2.5 to log 3.2) at the time of administration of the CMV specific T cell lines. The patients received a total cell dose ranging from 1.0 to.5x10 6 cells, corresponding to 0.6 to 6.1x10 6 NLV- and/or TPR-specific T cells. None of the five patients developed any complications during infusion of the T cell lines and all patients cleared CMV reactivation within weeks after administration of the CMV pp65-specific T cell line. Reconstitution of CMV-specific T cells after administration of the CMV-specific CD8+ T cell lines In all patients CMV-specific NLV- and/or TPR-specific CD8+ T cells could be detected after administration of the T cell lines. To determine the correlation between the infusion of the CMV-specific T cell lines and the appearance of CMV-specific T cells in peripheral blood of the patients, the presence of CMV-specific T cells was analyzed at different time points before and after administration of the T cell lines. Prior to infusion of the CMV-specific T cell lines in 3 of the 5 patients CMV pp65-specific T cells with the same specificity as the T cell line could already be detected in peripheral blood. In two of these patients a rise in CMVspecific T cells in peripheral blood was observed after infusion of the T cell line. In the other patient the numbers of CMV-specific T cells remained stable after infusion, however, in this
6 patient a very high level of CMV-specific T cells was already observed prior to infusion of the T cell line. In 2 of the 5 patients (patient 4 and 9) no CMV-specific T cells were detected prior to infusion of the T cell line, and a direct relation was observed between infusion of the CMV pp65-specific T cell line, the appearance of CMV-pp65 specific T cells in peripheral blood, and the clinical effect. Patient 4 developed CMV reactivation within the first month after allosct which was treated with antiviral drugs (Figure 2). The rise in CMV coincided with a rise in CMV TPRspecific T cells. Four months after allosct the patient received unmanipulated donor lymphocyte infusion (DLI), and six months after allosct the patient developed GvHD for which he was treated. The CMV-specific T cells disappeared, and the patient developed refractory CMV reactivation. A CMV TPR-specific T cell line was administered 8 months after allosct (1x10 5 T cells/kg) and within 2 weeks TPR-specific CD8 + T cells appeared in peripheral blood and the CMV load turned negative and remained negative (follow up >4 years). To asses why no persistence of the TPR-specific T cells from the first peak response was observed and to determine whether the TPR-specific T cells appearing in the second peak response were the same as the T cells in the first peak response, the patient or donor origin of the CMV-specific T cells from both peak responses (day 33 and day 289 after allosct respectively) was determined. The TPR-specific T cells were isolated from both peak responses by FACS sorting and DNA profiling showed that the CMV-specific T cells during the first response (day 33) were patient derived, and that the CMV-specific T cells that appeared after administration of the T cell line (day 289) were completely donor derived, illustrating the correlation between the infusion of the TPR-specific T cell line and the in vivo appearance of the donor derived TPR-specific T cells. Patient 9 developed refractory CMV reactivation post allosct in the absence of CMVspecific T cells (Figure 3). A CMV NLV- specific T cell line was administrated (day 2), but no CMV NLV-specific T cells appeared in peripheral blood and the CMV load remained positive. The quality of this T cell line was very poor due to poor quality of the starting material and this might explain that there was non in vivo persistence of the infused T cells. A second CMV NLV-specific T cell line was generated, from new starting material, that was administered at day 116 after allosct (3.1x10 5 T cells/kg) and after two weeks CMV NLVspecific T cells appeared in peripheral blood, which was coincided with a disappearance of CMV DNA load (follow up >2 years). Figure 2. CMV pp65-specific T cells in peripheral blood from patient 4 in relation to the CMV DNA load in peripheral blood. CMV-specific T cells (CD8+/tetramer+) are expressed as absolute numbers per liter in peripheral blood (left axis)., TPR-specific T cells;, NLV-specific T cells;, RPH-specific T cells. CMV DNA load ( ) is depicted as log CMV DNA load in peripheral blood (right axis).the lower level of detection is log 2.5. Figure 3. CMV pp65 (NLV)-specific T cells in peripheral blood from patient 9 in relation to the CMV DNA load in peripheral blood. CMV-specific T cells (, CD8+/NLV-tetramer+) are expressed as absolute numbers per liter in peripheral blood (left axis) and CMV DNA load ( ) is depicted as log CMV DNA load in peripheral blood (right axis). The lower level of detection is log
7 Discussion In this study, a phase I/II clinical protocol for the adoptive transfer of donor- or patientderived CMV pp65-specific CD8+ T cell lines for patients with refractory CMV reactivation after allosct was conducted. No toxicity was observed after administration of the T cell lines and all patients who received a CMV-specific T cell line cleared CMV reactivation. A direct relation between administration of donor derived CMV pp65-specific T cell lines and clinical effect could be demonstrated. Both donor- and patient-derived CMV pp65-specific CD8+ T cell lines could be reproducible generated, even when precursor frequencies of CMV pp65-specific CD8+ T cells were very low (<0.01%). Directly after isolation the purity of the positive fraction (% CD8+/IFNγ+ T cells) appeared to be low for some isolations, which was also observed in other studies using the IFNγ based isolation method [18,23]. This can be due to nonspecific co-isolation of other cells and may also be due to the fact that the antibody on the microbeads used for isolation and the antibody used for analysis of the population recognize the same epitope. Preferential expansion of the CMV-specific CD8+ T cells during the subsequent culture period led to T cell lines with a high purity of CMV-specific CD8+ T cells, reducing the risk of the induction of GvHD after administration. In the current study five patients with refractory CMV reactivation received one or two donor-derived CMV-specific CD8+ T cell line(s). Administration was safe, no toxicity was observed after infusion, and all patients cleared CMV reactivation after treatment with the CMV-specific CD8+ T cell lines. In three patients, T cells with the same reactivity as the T cell line could already be detected in peripheral blood of the patients prior to administration of the T cell lines. Although it is likely that the infused T cells contributed to the clearance of CMV reactivation in these patients, direct evidence for this can not be provided. However, in two of the five patients a direct correlation between the administration of donor derived CMV pp65-specific T cell lines, the appearance of CMVspecific CD8+ T cells and clearance of CMV reactivation was demonstrated. No CMVspecific T cells were present prior to the administration of the T cell lines, and within two weeks after administration of the T cell line increasing numbers of NLV- or TPR-specific CD8+ T cells could be detected in peripheral blood of the patients, illustrating persistence and in vivo proliferation of the infused T cells. The appearance of the CMV-specific CD8+ T cells co-incided with the clearance of CMV reactivation. Although CMV-specific CD8+ T cells have been detected in peripheral blood after the adoptive transfer of CD8+ T cell lines in previous studies, this study shows a direct correlation between the administration of a CD8+ T cell line and the clinical effect [10-1]. Two patients eligible for the study deceased due to CMV disease. CMV-specific T cell lines could be generated for these patients, however both patients deceased before the T cell line could be administered. Decreasing the time interval between the appearance of the clinical need and administration of the T cell product by direct administration of the isolated CMV pp65-specific T cells may improve the efficacy. Although in vivo proliferation is also likely to be necessary in these patients to allow a clinical effect, it has been shown that direct administration of CMV-specific T cells isolated based on their IFNγ production is effective and does not lead to GvHD induction [18]. In the current protocol T cell lines only could be generated for patients who were HLA-A*0201 and HLA-B*002 positive. To increase the potential clinical use of CMV specific T cells a CMV pp65 whole protein overlapping 15 mer (11 mer overlapping) peptide pool may be used for the generation of CMV pp65-specific T cell lines. It has been shown by us and others that using this peptide pool CMV pp65-specific T cells can be isolated irrespective of HLA restriction of the donor and patient [24-26]. Furthermore, using these peptide pools also CMV-specific CD4+ T cells will be isolated and studies have indicated that adoptively transferred CMV-specific CD4+ T cells may promote development of a CMV-specific CD8+ T cell response in vivo and that adoptively transferred CMV-specific CD8+ T cells show better persistence in the presence of CMV-specific CD4+ T cells [10, 12, 14-16, 26]. In conclusion, we have shown that the clinical grade generation of donor and patient derived CMV pp65-specific CD8+ T cell lines is feasible, and that administration of CMVspecific T cell lines to patients with refractory CMV reactivation after allosct was safe. A direct relation between infusion of CMV specific CD8+ T cells and clinical effect could be demonstrated. References 1. Chakrabarti S, Mackinnon S, Chopra R et al: High incidence of cytomegalovirus infection after nonmyeloablative stem cell transplantation: potential role of Campath-1H in delaying immune reconstitution. Blood 99: , Gandhi MK, Khanna R: Human cytomegalovirus: clinical aspects, immune regulation, and emerging treatments. Lancet Infect Dis 4: 25-38, Schaenman JM, Shashidhar S, Rhee C et al: Early CMV viremia is associated with impaired viral control following nonmyeloablative hematopoietic cell transplantation with a total lymphoid irradiation and antithymocyte globulin preparative regimen. Biol Blood Marrow Transplant, Epub ahead of print. 4. Ganepola S, Gentilini C, Hilbers U et al: Patients at high risk for CMV infection and disease show delayed CD8+ T-cell immune recovery after allogeneic stem cell transplantation. Bone Marrow Transplant 39: , Ljungman P, Brand R, Einsele H et al: Donor CMV serologic status and outcome of CMV-seropositive recipients after unrelated donor stem cell transplantation: an EBMT megafile analysis. Blood 102: ,
8 6. Hebart H, Daginik S, Stevanovic S et al: Sensitive detection of human cytomegalovirus peptide-specific cytotoxic T-lymphocyte responses by interferon-gamma-enzyme-linked immunospot assay and flow cytometry in healthy individuals and in patients after allogeneic stem cell transplantation. Blood 99: , Avetisyan G, Larsson K, Aschan J et al: Impact on the cytomegalovirus (CMV) viral load by CMV-specific T-cell immunity in recipients of allogeneic stem cell transplantation. Bone Marrow Transplant 38: , Gratama JW, Boeckh M, Nakamura R et al: Immune monitoring with itag MHC Tetramers for prediction of recurrent or persistent cytomegalovirus infection or disease in allogeneic hematopoietic stem cell transplant recipients: a prospective multicenter study. Blood 116: , Lilleri D, Fornara C, Chiesa A et al: Human cytomegalovirus-specific CD4+ and CD8+ T-cell reconstitution in adult allogeneic hematopoietic stem cell transplant recipients and immune control of viral infection. Haematologica 93: , Walter EA, Greenberg PD, Gilbert MJ et al: Reconstitution of cellular immunity against cytomegalovirus in recipients of allogeneic bone marrow by transfer of T-cell clones from the donor. N Engl J Med 333: , Einsele H, Roosnek E, Rufer N et al: Infusion of cytomegalovirus (CMV)-specific T cells for the treatment of CMV infection not responding to antiviral chemotherapy. Blood 99: , Peggs KS, Mackinnon S: Augmentation of virus-specific immunity after hematopoietic stem cell transplantation by adoptive T-cell therapy. Hum Immunol 65: , Micklethwaite KP, Clancy L, Sandher U et al: Prophylactic infusion of cytomegalovirus-specific cytotoxic T lymphocytes stimulated with Ad5f35pp65 gene-modified dendritic cells after allogeneic hemopoietic stem cell transplantation. Blood 112: , Peggs KS, Verfuerth S, Pizzey A et al: Adoptive cellular therapy for early cytomegalovirus infection after allogeneic stem-cell transplantation with virus-specific T-cell lines. Lancet 362: , Mackinnon S, Thomson K, Verfuerth S: Adoptive cellular therapy for cytomegalovirus infection following allogeneic stem cell transplantation using virus-specific T cells. Blood Cells Mol Dis 40: 63-6, Peggs KS, Verfuerth S, Pizzey A et al: Cytomegalovirus-specific T cell immunotherapy promotes restoration of durable functional antiviral immunity following allogeneic stem cell transplantation. Clin Infect Dis 49: , Cobbold M, Khan N, Pourgheysari B et al: Adoptive transfer of cytomegalovirus-specific CTL to stem cell transplant patients after selection by HLA-peptide tetramers. J Exp Med 202: , Feuchtinger T, Opherk K, Bethge WA et al: Adoptive transfer of pp-65 specific T-cells for the treatment of chemorefractory cytomegalovirus disease or reactivation after haploidentical and matched unrelated stem cell transplantation. Blood 116: , Lohning M, Hegazy AN, Pinschewer DD et al: Long-lived virus-reactive memory T cells generated from purified cytokine-secreting T helper type 1 and type 2 effectors. J Exp Med 205: 53-61, Altman JD, Moss PA, Goulder PJ et al: Phenotypic analysis of antigen-specific T lymphocytes. Science 24: 94-96, Faber LM, Luxemburg-Heijs SA, Willemze R et al: Generation of leukemia-reactive cytotoxic T lymphocyte clones from the HLA-identical bone marrow donor of a patient with leukemia. J Exp Med 16: , Marijt WA, Heemskerk MH, Kloosterboer FM et al: Hematopoiesis-restricted minor histocompatibility antigens HA-1- or HA-2-specific T cells can induce complete remissions of relapsed leukemia. Proc Natl Acad Sci USA100:242-24, Moosmann A, Bigalke I, Tischer J et al. Effective and long-term control of EBV PTLD after transfer of peptideselected T cells. Blood Kern F, Faulhaber N, Frommel C et al: Analysis of CD8 T cell reactivity to cytomegalovirus using proteinspanning pools of overlapping pentadecapeptides. Eur J Immunol 30: , Zandvliet ML, Liempt EV, Jedema I et al: Coordinated isolation of CD8+ and CD4+ T cells recognizing a broad repertoire of cytomegalovirus pp65 and IE1 epitopes for highly specific adoptive immunotherapy. Cytotherapy 12: , Bollard CM: Isolating cytomegalovirus-specifi c T cells for adoptive transfer: are we there yet? Cytotherapy 12: , Jedema I, van der Werff NM, Barge RM et al: New CFSE-based assay to determine susceptibility to lysis by cytotoxic T cells of leukemic precursor cells within a heterogeneous target cell population. Blood 103: ,
Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2*
 Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2* 1 Department of Laboratory Medicine - Laboratory of Hematology, Radboud University
Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2* 1 Department of Laboratory Medicine - Laboratory of Hematology, Radboud University
T cell manipulation of the graft: Yes
 T cell manipulation of the graft: Yes J.H. Frederik Falkenburg Department of Hematology L M U C Allogeneic Hematopoietic Stem Cell Transplantation (SCT) for non-malignant disorders: no need for anti-tumor
T cell manipulation of the graft: Yes J.H. Frederik Falkenburg Department of Hematology L M U C Allogeneic Hematopoietic Stem Cell Transplantation (SCT) for non-malignant disorders: no need for anti-tumor
Multi-Virus-Specific T cell Therapy for Patients after HSC and CB Transplant
 Multi-Virus-Specific T cell Therapy for Patients after HSC and CB Transplant Hanley PJ, Krance BR, Brenner MK, Leen AM, Rooney CM, Heslop HE, Shpall EJ, Bollard CM Hematopoietic Stem Cell Transplantation
Multi-Virus-Specific T cell Therapy for Patients after HSC and CB Transplant Hanley PJ, Krance BR, Brenner MK, Leen AM, Rooney CM, Heslop HE, Shpall EJ, Bollard CM Hematopoietic Stem Cell Transplantation
The future of HSCT. John Barrett, MD, NHBLI, NIH Bethesda MD
 The future of HSCT John Barrett, MD, NHBLI, NIH Bethesda MD Transplants today Current approaches to improve SCT outcome Optimize stem cell dose and source BMT? PBSCT? Adjusting post transplant I/S to minimize
The future of HSCT John Barrett, MD, NHBLI, NIH Bethesda MD Transplants today Current approaches to improve SCT outcome Optimize stem cell dose and source BMT? PBSCT? Adjusting post transplant I/S to minimize
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Kinetic preservation of dual-specificity of coprogrammed minor histocompatibility antigen-reactive virus-specific T-cells
 Kinetic preservation of dual-specificity of coprogrammed minor histocompatibility antigen-reactive virus-specific T-cells 3 Cancer Res. 2009 Mar 1;69(5):2034-41. Epub 2009 Feb 17. Reprinted with permission.
Kinetic preservation of dual-specificity of coprogrammed minor histocompatibility antigen-reactive virus-specific T-cells 3 Cancer Res. 2009 Mar 1;69(5):2034-41. Epub 2009 Feb 17. Reprinted with permission.
Broad spectrum antiviral T cells for viral complications after hematopoietic stem cell transplantation
 Editorial Page 1 of 5 Broad spectrum antiviral T cells for viral complications after hematopoietic stem cell transplantation Britta Maecker-Kolhoff 1,2, Britta Eiz-Vesper 2,3 1 Department of Pediatric
Editorial Page 1 of 5 Broad spectrum antiviral T cells for viral complications after hematopoietic stem cell transplantation Britta Maecker-Kolhoff 1,2, Britta Eiz-Vesper 2,3 1 Department of Pediatric
Cytotoxicity assays. Rory D. de Vries, PhD 1. Viroscience lab, Erasmus MC, Rotterdam, the Netherlands
 Cytotoxicity assays Rory D. de Vries, PhD 1 1 Viroscience lab, Erasmus MC, Rotterdam, the Netherlands Anti-influenza immunity Humoral / CD4+ / CD8+ / NK? Function of CTL Elimination of virus-infected cells?
Cytotoxicity assays Rory D. de Vries, PhD 1 1 Viroscience lab, Erasmus MC, Rotterdam, the Netherlands Anti-influenza immunity Humoral / CD4+ / CD8+ / NK? Function of CTL Elimination of virus-infected cells?
One Day BMT Course by Thai Society of Hematology. Management of Graft Failure and Relapsed Diseases
 One Day BMT Course by Thai Society of Hematology Management of Graft Failure and Relapsed Diseases Piya Rujkijyanont, MD Division of Hematology-Oncology Department of Pediatrics Phramongkutklao Hospital
One Day BMT Course by Thai Society of Hematology Management of Graft Failure and Relapsed Diseases Piya Rujkijyanont, MD Division of Hematology-Oncology Department of Pediatrics Phramongkutklao Hospital
Minor H Antigen-Specific T Cells -The Black Box of the GVL Effect
 Minor H Antigen-Specific T Cells -The Black Box of the GVL Effect All Allogeneic Stem Cell Transplants Are Blind Doctor Donor Patient Genetic polymorphism gives rise to unique peptides in donor and recipient
Minor H Antigen-Specific T Cells -The Black Box of the GVL Effect All Allogeneic Stem Cell Transplants Are Blind Doctor Donor Patient Genetic polymorphism gives rise to unique peptides in donor and recipient
CONTRACTING ORGANIZATION: Johns Hopkins University School of Medicine Baltimore, MD 21205
 AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
Selective graft-versus-leukemia depends on magnitude and diversity of the alloreactive T cell response
 Selective graft-versus-leukemia depends on magnitude and diversity of the alloreactive T cell response Cornelis A.M. van Bergen,, Marieke Griffioen, J.H. Frederik Falkenburg J Clin Invest. 2017;127(2):517-529.
Selective graft-versus-leukemia depends on magnitude and diversity of the alloreactive T cell response Cornelis A.M. van Bergen,, Marieke Griffioen, J.H. Frederik Falkenburg J Clin Invest. 2017;127(2):517-529.
Detailed step-by-step operating procedures for NK cell and CTL degranulation assays
 Supplemental methods Detailed step-by-step operating procedures for NK cell and CTL degranulation assays Materials PBMC isolated from patients, relatives and healthy donors as control K562 cells (ATCC,
Supplemental methods Detailed step-by-step operating procedures for NK cell and CTL degranulation assays Materials PBMC isolated from patients, relatives and healthy donors as control K562 cells (ATCC,
Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE)
 Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central
Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central
Administration of Tumor-Specific Cytotoxic T Lymphocytes Engineered to Resist TGF-ß to Patients with EBV-Associated Lymphomas
 Administration of Tumor-Specific Cytotoxic T Lymphocytes Engineered to Resist TGF-ß to Patients with EBV-Associated Lymphomas CM. Bollard, G Dotti, S Gottschalk, E Liu, A Sheehan, M Mims, H Liu, AP. Gee,
Administration of Tumor-Specific Cytotoxic T Lymphocytes Engineered to Resist TGF-ß to Patients with EBV-Associated Lymphomas CM. Bollard, G Dotti, S Gottschalk, E Liu, A Sheehan, M Mims, H Liu, AP. Gee,
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
Clinical Policy: Donor Lymphocyte Infusion
 Clinical Policy: Reference Number: PA.CP.MP.101 Effective Date: 01/18 Last Review Date: 11/16 Coding Implications Revision Log This policy describes the medical necessity requirements for a donor lymphocyte
Clinical Policy: Reference Number: PA.CP.MP.101 Effective Date: 01/18 Last Review Date: 11/16 Coding Implications Revision Log This policy describes the medical necessity requirements for a donor lymphocyte
Is in vitro T-cell depletion necessary for Haploidentical TransplantationTitle of Presentation. Disclosure of Interest: Nothing to Disclose
 Rupert Handgretinger Children s University Hospital, Tübingen, Germany Is in vitro T-cell depletion necessary for Haploidentical TransplantationTitle of Presentation Disclosure of Interest: Nothing to
Rupert Handgretinger Children s University Hospital, Tübingen, Germany Is in vitro T-cell depletion necessary for Haploidentical TransplantationTitle of Presentation Disclosure of Interest: Nothing to
Dr. Yi-chi M. Kong August 8, 2001 Benjamini. Ch. 19, Pgs Page 1 of 10 TRANSPLANTATION
 Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20522 holds various files of this Leiden University dissertation. Author: Stevanović, Sanja Title: Exploiting HLA-class II disparity for anti-tumor immunity
Cover Page The handle http://hdl.handle.net/1887/20522 holds various files of this Leiden University dissertation. Author: Stevanović, Sanja Title: Exploiting HLA-class II disparity for anti-tumor immunity
Trends in Hematopoietic Cell Transplantation. AAMAC Patient Education Day Oct 2014
 Trends in Hematopoietic Cell Transplantation AAMAC Patient Education Day Oct 2014 Objectives Review the principles behind allogeneic stem cell transplantation Outline the process of transplant, some of
Trends in Hematopoietic Cell Transplantation AAMAC Patient Education Day Oct 2014 Objectives Review the principles behind allogeneic stem cell transplantation Outline the process of transplant, some of
CHAPTER 3 LABORATORY PROCEDURES
 CHAPTER 3 LABORATORY PROCEDURES CHAPTER 3 LABORATORY PROCEDURES 3.1 HLA TYPING Molecular HLA typing will be performed for all donor cord blood units and patients in the three reference laboratories identified
CHAPTER 3 LABORATORY PROCEDURES CHAPTER 3 LABORATORY PROCEDURES 3.1 HLA TYPING Molecular HLA typing will be performed for all donor cord blood units and patients in the three reference laboratories identified
Cultivated anti-aspergillus T H 1 Cells. Thomas Lehrnbecher Pediatric Hematology and Oncology Frankfurt/Main, Germany
 Cultivated anti-aspergillus T H 1 Cells Thomas Lehrnbecher Pediatric Hematology and Oncology Frankfurt/Main, Germany Invasive fungal infection after allogeneic SCT Incidence of proven invasive fungal infections
Cultivated anti-aspergillus T H 1 Cells Thomas Lehrnbecher Pediatric Hematology and Oncology Frankfurt/Main, Germany Invasive fungal infection after allogeneic SCT Incidence of proven invasive fungal infections
The question is not whether or not to deplete T-cells, but how to deplete which T-cells
 The question is not whether or not to deplete T-cells, but how to deplete which T-cells CD34+ positive selection Negative Depletion of: CD3/CD19 TcRαβ/CD19 T-cell depletion: positive selection versus negative
The question is not whether or not to deplete T-cells, but how to deplete which T-cells CD34+ positive selection Negative Depletion of: CD3/CD19 TcRαβ/CD19 T-cell depletion: positive selection versus negative
Rapid generation of clinical-grade antiviral T cells: selection of suitable T-cell donors and GMP-compliant manufacturing of antiviral T cells
 Tischer et al. Journal of Translational Medicine (2014) 12:336 DOI 10.1186/s12967-014-0336-5 RESEARCH Open Access Rapid generation of clinical-grade antiviral T cells: selection of suitable T-cell donors
Tischer et al. Journal of Translational Medicine (2014) 12:336 DOI 10.1186/s12967-014-0336-5 RESEARCH Open Access Rapid generation of clinical-grade antiviral T cells: selection of suitable T-cell donors
Rapid antigen-specific T cell enrichment (Rapid ARTE)
 Direct ex vivo characterization of human antigen-specific CD154+CD4+ T cell Rapid antigen-specific T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central role
Direct ex vivo characterization of human antigen-specific CD154+CD4+ T cell Rapid antigen-specific T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central role
Generation of CMV-specific T lymphocytes using protein-spanning pools of pp65-derived overlapping pentadecapeptides for adoptive immunotherapy
 IMMUNOBIOLOGY Generation of CMV-specific T lymphocytes using protein-spanning pools of pp65-derived overlapping pentadecapeptides for adoptive immunotherapy Deepa Trivedi, Roxanne Y. Williams, Richard
IMMUNOBIOLOGY Generation of CMV-specific T lymphocytes using protein-spanning pools of pp65-derived overlapping pentadecapeptides for adoptive immunotherapy Deepa Trivedi, Roxanne Y. Williams, Richard
Adoptive Immunotherapy for Posttransplantation Viral Infections
 Biology of Blood and Marrow Transplantation 10:143-155 (2004) 2004 American Society for Blood and Marrow Transplantation 1083-8791/04/1003-0001$30.00/0 doi:10.1016/j.bbmt.2003.09.017 Adoptive Immunotherapy
Biology of Blood and Marrow Transplantation 10:143-155 (2004) 2004 American Society for Blood and Marrow Transplantation 1083-8791/04/1003-0001$30.00/0 doi:10.1016/j.bbmt.2003.09.017 Adoptive Immunotherapy
Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to
 Class II tetramer staining Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to PE were combined with dominant HIV epitopes (DRB1*0101-DRFYKTLRAEQASQEV, DRB1*0301- PEKEVLVWKFDSRLAFHH,
Class II tetramer staining Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to PE were combined with dominant HIV epitopes (DRB1*0101-DRFYKTLRAEQASQEV, DRB1*0301- PEKEVLVWKFDSRLAFHH,
Growth Inhibition of Clonogenic Leukemic Precursor Cells by Minor Histocompatibility Antigen-specific Cytotoxic T Lymphocytes
 Published Online: 1 July, 1991 Supp Info: http://doi.org/1.184/jem.174.1.27 Downloaded from jem.rupress.org on December 22, 18 Growth Inhibition of Clonogenic Leukemic Precursor Cells by Minor Histocompatibility
Published Online: 1 July, 1991 Supp Info: http://doi.org/1.184/jem.174.1.27 Downloaded from jem.rupress.org on December 22, 18 Growth Inhibition of Clonogenic Leukemic Precursor Cells by Minor Histocompatibility
The Role of Conventional Donor Lymphocyte Transfusions. Hans-Jochem Kolb 3rd Med. Dept. Klinikum re der Isar Technische Universitaet Muenchen Germany
 The Role of Conventional Donor Lymphocyte Transfusions Hans-Jochem Kolb 3rd Med. Dept. Klinikum re der Isar Technische Universitaet Muenchen Germany Survival of Patients with Allogeneic SCT for AML CR1:
The Role of Conventional Donor Lymphocyte Transfusions Hans-Jochem Kolb 3rd Med. Dept. Klinikum re der Isar Technische Universitaet Muenchen Germany Survival of Patients with Allogeneic SCT for AML CR1:
Kymriah. Kymriah (tisagenlecleucel) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.101 Subject: Kymriah Page: 1 of 5 Last Review Date: September 20, 2018 Kymriah Description Kymriah
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.101 Subject: Kymriah Page: 1 of 5 Last Review Date: September 20, 2018 Kymriah Description Kymriah
Ferrata Storti Foundation
 Immunotherapy A Good Manufacturing Practice procedure to engineer donor virus-specific T cells into potent anti-leukemic effector cells ARTICLES Marleen M. van Loenen, 1 Renate de Boer, 1 Ellis van Liempt,
Immunotherapy A Good Manufacturing Practice procedure to engineer donor virus-specific T cells into potent anti-leukemic effector cells ARTICLES Marleen M. van Loenen, 1 Renate de Boer, 1 Ellis van Liempt,
Virological Surveillance in Paediatric HSCT Recipients
 Virological Surveillance in Paediatric HSCT Recipients Dr Pamela Lee Clinical Assistant Professor Department of Paediatrics & Adolescent Medicine Queen Mary Hospital LKS Faculty of Medicine, The University
Virological Surveillance in Paediatric HSCT Recipients Dr Pamela Lee Clinical Assistant Professor Department of Paediatrics & Adolescent Medicine Queen Mary Hospital LKS Faculty of Medicine, The University
EBV in HSCT 2015 update of ECIL guidelines
 ECIL-6 EBV in HSCT 2015 update of ECIL guidelines Jan Styczynski (Poland, chair), Walter van der Velden (Netherlands), Christopher Fox (United Kingdom), Dan Engelhard (Israel), Rafael de la Camara (Spain),
ECIL-6 EBV in HSCT 2015 update of ECIL guidelines Jan Styczynski (Poland, chair), Walter van der Velden (Netherlands), Christopher Fox (United Kingdom), Dan Engelhard (Israel), Rafael de la Camara (Spain),
Donor Lymphocyte Infusion for Malignancies Treated with an Allogeneic Hematopoietic Stem-Cell Transplant
 Last Review Status/Date: September 2014 Page: 1 of 8 Malignancies Treated with an Allogeneic Description Donor lymphocyte infusion (DLI), also called donor leukocyte or buffy-coat infusion is a type of
Last Review Status/Date: September 2014 Page: 1 of 8 Malignancies Treated with an Allogeneic Description Donor lymphocyte infusion (DLI), also called donor leukocyte or buffy-coat infusion is a type of
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20898 holds various files of this Leiden University dissertation. Author: Jöris, Monique Maria Title: Challenges in unrelated hematopoietic stem cell transplantation.
Cover Page The handle http://hdl.handle.net/1887/20898 holds various files of this Leiden University dissertation. Author: Jöris, Monique Maria Title: Challenges in unrelated hematopoietic stem cell transplantation.
KEY WORDS: Cytomegalovirus, Bone marrow transplantation, Nonmyeloablative, Immune reconstitution, Antithymocyte globulin
 Early CMV Viremia Is Associated with Impaired Viral Control following Nonmyeloablative Hematopoietic Cell Transplantation with a Total Lymphoid Irradiation and Antithymocyte Globulin Preparative Regimen
Early CMV Viremia Is Associated with Impaired Viral Control following Nonmyeloablative Hematopoietic Cell Transplantation with a Total Lymphoid Irradiation and Antithymocyte Globulin Preparative Regimen
TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer
 AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke,. CONTRACTING ORGANIZATION: Johns Hopkins
AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke,. CONTRACTING ORGANIZATION: Johns Hopkins
Original Articles ABSTRACT
 Original Articles Successful generation of primary virus-specific and anti-tumor T-cell responses from the naïve donor T-cell repertoire is determined by the balance between antigen-specific precursor
Original Articles Successful generation of primary virus-specific and anti-tumor T-cell responses from the naïve donor T-cell repertoire is determined by the balance between antigen-specific precursor
Stem Cell Sources 2/22/13. Cellular Therapy Today and Tomorrow. Cellular Therapy in HCT. Bone Marrow
 2/22/13 Cellular Therapy Today and Tomorrow Robert S. Negrin, MD Division Chief, Stanford Bone and Marrow Transplant Program Professor of Medicine Cellular Therapy in Clinical Medicine Established Hematopoietic
2/22/13 Cellular Therapy Today and Tomorrow Robert S. Negrin, MD Division Chief, Stanford Bone and Marrow Transplant Program Professor of Medicine Cellular Therapy in Clinical Medicine Established Hematopoietic
ASBMT and Marrow Transplantation
 Biol Blood Marrow Transplant 19 (213) 725e734 Cytomegalovirus-Specific Cytotoxic T Lymphocytes Can Be Efficiently Expanded from Granulocyte Colony-Stimulating FactoreMobilized Hemopoietic Progenitor Cell
Biol Blood Marrow Transplant 19 (213) 725e734 Cytomegalovirus-Specific Cytotoxic T Lymphocytes Can Be Efficiently Expanded from Granulocyte Colony-Stimulating FactoreMobilized Hemopoietic Progenitor Cell
staining and flow cytometry
 Detection of influenza virus-specific T cell responses by intracellular by cytokine intracellular staining cytokine staining and flow cytometry Detection of influenza virus-specific T cell responses and
Detection of influenza virus-specific T cell responses by intracellular by cytokine intracellular staining cytokine staining and flow cytometry Detection of influenza virus-specific T cell responses and
CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads (Miltenyi Biotec) for depletion of CD25 +
 Supplements Supplemental Materials and Methods Depletion of CD25 + T-cells from PBMC. Fresh or HD precultured PBMC were stained with the conjugate CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads
Supplements Supplemental Materials and Methods Depletion of CD25 + T-cells from PBMC. Fresh or HD precultured PBMC were stained with the conjugate CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/28890 holds various files of this Leiden University dissertation. Author: Hombrink, Pleun Title: Identification of minor histocompatibility antigens by
Cover Page The handle http://hdl.handle.net/1887/28890 holds various files of this Leiden University dissertation. Author: Hombrink, Pleun Title: Identification of minor histocompatibility antigens by
& 2005 Nature Publishing Group All rights reserved /05 $
 (5) 3, 797 & 5 Nature Publishing Group All rights reserved -339/5 $3. www.nature.com/bmt Post-transplant events Cytomegalovirus (CMV) infections and CMV-specific cellular immune reconstitution following
(5) 3, 797 & 5 Nature Publishing Group All rights reserved -339/5 $3. www.nature.com/bmt Post-transplant events Cytomegalovirus (CMV) infections and CMV-specific cellular immune reconstitution following
Institut für Medizinische Immunologie, Berliner Hochschulmedizin Charite, Charité Campus Mitte, Berlin, Germany
 Flow Cytometric Methods Journal of Biological Regulators and Homeostatic Agents A protocol for combining proliferation, tetramer staining and intracellular cytokine detection for the flow-cytometric analysis
Flow Cytometric Methods Journal of Biological Regulators and Homeostatic Agents A protocol for combining proliferation, tetramer staining and intracellular cytokine detection for the flow-cytometric analysis
TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer
 AD Award Number: W8XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
AD Award Number: W8XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/24366 holds various files of this Leiden University dissertation Author: Buddingh, Emilie Pauline Title: Innate immunity in osteosarcoma Issue Date: 2014-03-05
Cover Page The handle http://hdl.handle.net/1887/24366 holds various files of this Leiden University dissertation Author: Buddingh, Emilie Pauline Title: Innate immunity in osteosarcoma Issue Date: 2014-03-05
Regular Article. Adoptive T-cell therapy with hexon-specific Th1 cells as a treatment of refractory adenovirus infection after HSCT TRANSPLANTATION
 Regular Article From www.bloodjournal.org by guest on January 21, 2019. For personal use only. TRANSPLANTATION Adoptive T-cell therapy with hexon-specific Th1 cells as a treatment of refractory adenovirus
Regular Article From www.bloodjournal.org by guest on January 21, 2019. For personal use only. TRANSPLANTATION Adoptive T-cell therapy with hexon-specific Th1 cells as a treatment of refractory adenovirus
Revista Cubana de Hematología, Inmunología y Hemoterapia. 2017; 36 (Suplemento).
 Depletion of TCR alpha/beta+ T-lymphocytes from grafts for haplo haematopoietic CELL transplantation (HCT) in children Heilmann C, Ifversen M, Haastrup E, Fischer-Nielsen A. Haematopoietic Cell Transplantation
Depletion of TCR alpha/beta+ T-lymphocytes from grafts for haplo haematopoietic CELL transplantation (HCT) in children Heilmann C, Ifversen M, Haastrup E, Fischer-Nielsen A. Haematopoietic Cell Transplantation
Biol Blood Marrow Transplant 19 (2013) 40e48
 Biol Blood Marrow Transplant 19 (2013) 40e48 Clinical Research Patient HLA-DPeSpecific CD4 þ T Cells from HLA-DPB1eMismatched Donor Lymphocyte Infusion Can Induce Graft-versus-Leukemia Reactivity in the
Biol Blood Marrow Transplant 19 (2013) 40e48 Clinical Research Patient HLA-DPeSpecific CD4 þ T Cells from HLA-DPB1eMismatched Donor Lymphocyte Infusion Can Induce Graft-versus-Leukemia Reactivity in the
Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4
 Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4 Ankita Garg, Rodney Trout and Stephen A. Spector,,* Department
Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4 Ankita Garg, Rodney Trout and Stephen A. Spector,,* Department
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_cell_transplantation_for_cll_and_sll 2/2001
Corporate Medical Policy Hematopoietic Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_cell_transplantation_for_cll_and_sll 2/2001
Preventative/Preemptive Adoptive Transfer of Peptide Stimulated CMV/EBV Specific T-cells in Patients After Allogeneic Stem Cell Transplantation
 Find Studies About Studies Submit Studies Resources About Site Preventative/Preemptive Adoptive Transfer of Peptide Stimulated CMV/EBV Specific T-cells in Patients After Allogeneic Stem Cell Transplantation
Find Studies About Studies Submit Studies Resources About Site Preventative/Preemptive Adoptive Transfer of Peptide Stimulated CMV/EBV Specific T-cells in Patients After Allogeneic Stem Cell Transplantation
Original article Failure of pre-emptive treatment of cytomegalovirus infections and antiviral resistance in stem cell transplant recipients
 Antiviral Therapy ; 7: (doi:.8/imp899) Original article Failure of pre-emptive treatment of cytomegalovirus infections and antiviral resistance in stem cell transplant recipients Martha T van der Beek
Antiviral Therapy ; 7: (doi:.8/imp899) Original article Failure of pre-emptive treatment of cytomegalovirus infections and antiviral resistance in stem cell transplant recipients Martha T van der Beek
Determinants of Immunogenicity and Tolerance. Abul K. Abbas, MD Department of Pathology University of California San Francisco
 Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Haploidentical Transplantation Helen Heslop
 Haploidentical Transplantation Helen Heslop Outline Haplodentical transplantation Indications Regimens Outcomes KIR mismatching and NK cells Reconstituting T cell immunity Allodepleted T cells Cytotoxic
Haploidentical Transplantation Helen Heslop Outline Haplodentical transplantation Indications Regimens Outcomes KIR mismatching and NK cells Reconstituting T cell immunity Allodepleted T cells Cytotoxic
Supplementary Figure 1. Enhanced detection of CTLA-4 on the surface of HIV-specific
 SUPPLEMENTARY FIGURE LEGEND Supplementary Figure 1. Enhanced detection of CTLA-4 on the surface of HIV-specific CD4 + T cells correlates with intracellular CTLA-4 levels. (a) Comparative CTLA-4 levels
SUPPLEMENTARY FIGURE LEGEND Supplementary Figure 1. Enhanced detection of CTLA-4 on the surface of HIV-specific CD4 + T cells correlates with intracellular CTLA-4 levels. (a) Comparative CTLA-4 levels
& 2004 Nature Publishing Group All rights reserved /04 $
 (2004) 33, 197 204 & 2004 Nature Publishing Group All rights reserved 0268-3369/04 $25.00 www.nature.com/bmt Viral infections Influence of cytomegalovirus (CMV) sero-positivity on CMV infection, lymphocyte
(2004) 33, 197 204 & 2004 Nature Publishing Group All rights reserved 0268-3369/04 $25.00 www.nature.com/bmt Viral infections Influence of cytomegalovirus (CMV) sero-positivity on CMV infection, lymphocyte
Bone Marrow Transplantation and the Potential Role of Iomab-B
 Bone Marrow Transplantation and the Potential Role of Iomab-B Hillard M. Lazarus, MD, FACP Professor of Medicine, Director of Novel Cell Therapy Case Western Reserve University 1 Hematopoietic Cell Transplantation
Bone Marrow Transplantation and the Potential Role of Iomab-B Hillard M. Lazarus, MD, FACP Professor of Medicine, Director of Novel Cell Therapy Case Western Reserve University 1 Hematopoietic Cell Transplantation
Melanoma Bridge Meeting
 Melanoma Bridge Meeting Improving Adoptive Immune Therapy with Genetically Engineered T cells David Stroncek, MD Chief, Cell Processing Section, DTM, CC, NIH 3 December 2015 Adoptive T Cell Therapy: Dose
Melanoma Bridge Meeting Improving Adoptive Immune Therapy with Genetically Engineered T cells David Stroncek, MD Chief, Cell Processing Section, DTM, CC, NIH 3 December 2015 Adoptive T Cell Therapy: Dose
Supplementary Figure 1. Example of gating strategy
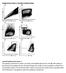 Supplementary Figure 1. Example of gating strategy Legend Supplementary Figure 1: First, gating is performed to include only single cells (singlets) (A) and CD3+ cells (B). After gating on the lymphocyte
Supplementary Figure 1. Example of gating strategy Legend Supplementary Figure 1: First, gating is performed to include only single cells (singlets) (A) and CD3+ cells (B). After gating on the lymphocyte
Diagnosis of CMV infection UPDATE ECIL
 UPDATE ECIL-4 2011 Recommendations for CMV and HHV-6 management in patients with hematological diseases Per Ljungman, Rafael de la Camara, Hermann Einsele, Dan Engelhard, Pierre Reusser, Jan Styczynski,
UPDATE ECIL-4 2011 Recommendations for CMV and HHV-6 management in patients with hematological diseases Per Ljungman, Rafael de la Camara, Hermann Einsele, Dan Engelhard, Pierre Reusser, Jan Styczynski,
PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human
 Anti-CD19-CAR transduced T-cell preparation PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human AB serum (Gemini) and 300 international units/ml IL-2 (Novartis). T cell proliferation
Anti-CD19-CAR transduced T-cell preparation PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human AB serum (Gemini) and 300 international units/ml IL-2 (Novartis). T cell proliferation
Clinical Translation of Immunotherapy using WT1 and CMV specific TCR Gene Transfer
 Clinical Translation of Immunotherapy using WT1 and CMV specific Gene Transfer Dr Emma C Morris Reader, Dept of Immunology, UCL Consultant Haematologist (BMT), UCLH and RFH ISCT, 2/5/211 Gene Transfer
Clinical Translation of Immunotherapy using WT1 and CMV specific Gene Transfer Dr Emma C Morris Reader, Dept of Immunology, UCL Consultant Haematologist (BMT), UCLH and RFH ISCT, 2/5/211 Gene Transfer
Federica Galaverna, 1 Daria Pagliara, 1 Deepa Manwani, 2 Rajni Agarwal-Hashmi, 3 Melissa Aldinger, 4 Franco Locatelli 1
 Administration of Rivogenlecleucel (Rivo-cel, BPX-501) Following αβ T- and B-Cell Depleted Haplo-HSCT in Children With Transfusion-Dependent Thalassemia Federica Galaverna, 1 Daria Pagliara, 1 Deepa Manwani,
Administration of Rivogenlecleucel (Rivo-cel, BPX-501) Following αβ T- and B-Cell Depleted Haplo-HSCT in Children With Transfusion-Dependent Thalassemia Federica Galaverna, 1 Daria Pagliara, 1 Deepa Manwani,
Dr.PSRK.Sastry MD, ECMO
 Peripheral blood stem cell transplantation (Haematopoietic stem cell transplantation) Dr.PSRK.Sastry MD, ECMO Consultant, Medical Oncology Kokilaben Dhirubhai Ambani Hospital Normal hematopoiesis Historical
Peripheral blood stem cell transplantation (Haematopoietic stem cell transplantation) Dr.PSRK.Sastry MD, ECMO Consultant, Medical Oncology Kokilaben Dhirubhai Ambani Hospital Normal hematopoiesis Historical
MUD SCT. Pimjai Niparuck Division of Hematology, Department of Medicine Ramathibodi Hospital, Mahidol University
 MUD SCT Pimjai Niparuck Division of Hematology, Department of Medicine Ramathibodi Hospital, Mahidol University Outlines Optimal match criteria for unrelated adult donors Role of ATG in MUD-SCT Post-transplant
MUD SCT Pimjai Niparuck Division of Hematology, Department of Medicine Ramathibodi Hospital, Mahidol University Outlines Optimal match criteria for unrelated adult donors Role of ATG in MUD-SCT Post-transplant
PUO in the Immunocompromised Host: CMV and beyond
 PUO in the Immunocompromised Host: CMV and beyond PUO in the immunocompromised host: role of viral infections Nature of host defect T cell defects Underlying disease Treatment Nature of clinical presentation
PUO in the Immunocompromised Host: CMV and beyond PUO in the immunocompromised host: role of viral infections Nature of host defect T cell defects Underlying disease Treatment Nature of clinical presentation
T-cell responses, and graft-versus-host disease (GVHD) were associated with late CMV disease or death. After 3 months, Patients
 CLINICAL OBSERVATIONS, INTERVENTIONS, AND THERAPEUTIC TRIALS Late cytomegalovirus disease and mortality in recipients of allogeneic hematopoietic stem cell transplants: importance of viral load and T-cell
CLINICAL OBSERVATIONS, INTERVENTIONS, AND THERAPEUTIC TRIALS Late cytomegalovirus disease and mortality in recipients of allogeneic hematopoietic stem cell transplants: importance of viral load and T-cell
CONTRACTING ORGANIZATION: Johns Hopkins University School of Medicine Baltimore, MD 21205
 AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
Sleeping Beauty: Current applications and future strategies. CAR-TCR Summit 2017 Partow Kebriaei, MD
 Sleeping Beauty: Current applications and future strategies CAR-TCR Summit 2017 Partow Kebriaei, MD Outline Chimeric antigen receptor (CAR) technology Viral versus nonviral vectors Results of current clinical
Sleeping Beauty: Current applications and future strategies CAR-TCR Summit 2017 Partow Kebriaei, MD Outline Chimeric antigen receptor (CAR) technology Viral versus nonviral vectors Results of current clinical
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for Waldenstrom Macroglobulinemia File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem_cell_transplantation_for_waldenstrom_macroglobulinemia
Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for Waldenstrom Macroglobulinemia File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem_cell_transplantation_for_waldenstrom_macroglobulinemia
Human Cytomegalovirus Latency-Associated Proteins Elicit Immune-Suppressive IL-10 Producing CD4 + T Cells
 Human Cytomegalovirus Latency-Associated Proteins Elicit Immune-Suppressive IL-10 Producing CD4 + T Cells Gavin M. Mason, Sarah Jackson, Georgina Okecha, Emma Poole, J. G. Patrick Sissons, John Sinclair,
Human Cytomegalovirus Latency-Associated Proteins Elicit Immune-Suppressive IL-10 Producing CD4 + T Cells Gavin M. Mason, Sarah Jackson, Georgina Okecha, Emma Poole, J. G. Patrick Sissons, John Sinclair,
THERAPEUTIC IMPLICATIONS OF PREPARING AND ADMINISTERING INNATE IMMUNE CELLS. 9:40 am to 10:10 pm Laurence Cooper
 THERAPEUTIC IMPLICATIONS OF PREPARING AND ADMINISTERING INNATE IMMUNE CELLS 9:40 am to 10:10 pm Laurence Cooper ljncooper@ziopharm.com 05-16-2016 Forward-looking statements This presentation contains certain
THERAPEUTIC IMPLICATIONS OF PREPARING AND ADMINISTERING INNATE IMMUNE CELLS 9:40 am to 10:10 pm Laurence Cooper ljncooper@ziopharm.com 05-16-2016 Forward-looking statements This presentation contains certain
TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer
 AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke, Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke, Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
IFN-γ Secretion Assay Detection Kit (PE) human
 Miltenyi Biotec GmbH Friedrich-Ebert-Straße 68 51429 Bergisch Gladbach, Germany Phone +49 2204 8306-0 Fax +49 2204 85197 macs@miltenyibiotec.de Miltenyi Biotec Inc. 12740 Earhart Avenue Auburn CA 95602,
Miltenyi Biotec GmbH Friedrich-Ebert-Straße 68 51429 Bergisch Gladbach, Germany Phone +49 2204 8306-0 Fax +49 2204 85197 macs@miltenyibiotec.de Miltenyi Biotec Inc. 12740 Earhart Avenue Auburn CA 95602,
Children's Hospital of Pittsburgh Annual Progress Report: 2011 Formula Grant
 Children's Hospital of Pittsburgh Annual Progress Report: 2011 Formula Grant Reporting Period July 1, 2012 June 30, 2013 Formula Grant Overview The Children's Hospital of Pittsburgh received $228,401 in
Children's Hospital of Pittsburgh Annual Progress Report: 2011 Formula Grant Reporting Period July 1, 2012 June 30, 2013 Formula Grant Overview The Children's Hospital of Pittsburgh received $228,401 in
Natural Killer Cells: Development, Diversity, and Applications to Human Disease Dr. Michael A. Caligiuri
 Natural Killer Cells: Development, Diversity, November 26, 2008 The Ohio State University Comprehensive Cancer Center The James Cancer Hospital and Solove Research Institute Columbus, Ohio, USA 1 Human
Natural Killer Cells: Development, Diversity, November 26, 2008 The Ohio State University Comprehensive Cancer Center The James Cancer Hospital and Solove Research Institute Columbus, Ohio, USA 1 Human
The Contribution of Homeostatically Expanded Donor CD8 T Cells to Host Reconstitution Following Syngeneic Hematopoietic Cell Transplantation
 University of Miami Scholarly Repository Open Access Dissertations Electronic Theses and Dissertations 2008-07-24 The Contribution of Homeostatically Expanded Donor CD8 T Cells to Host Reconstitution Following
University of Miami Scholarly Repository Open Access Dissertations Electronic Theses and Dissertations 2008-07-24 The Contribution of Homeostatically Expanded Donor CD8 T Cells to Host Reconstitution Following
CMV promotes recipient T-cell immunity following reduced-intensity T-cell depleted HSCT, significantly modulating chimerism status
 Regular Article From www.bloodjournal.org by guest on January 30, 2019. For personal use only. TRANSPLANTATION CMV promotes recipient T-cell immunity following reduced-intensity T-cell depleted HSCT, significantly
Regular Article From www.bloodjournal.org by guest on January 30, 2019. For personal use only. TRANSPLANTATION CMV promotes recipient T-cell immunity following reduced-intensity T-cell depleted HSCT, significantly
What s a Transplant? What s not?
 What s a Transplant? What s not? How to report the difference? Daniel Weisdorf MD University of Minnesota Anti-cancer effects of BMT or PBSCT [HSCT] Kill the cancer Save the patient Restore immunocompetence
What s a Transplant? What s not? How to report the difference? Daniel Weisdorf MD University of Minnesota Anti-cancer effects of BMT or PBSCT [HSCT] Kill the cancer Save the patient Restore immunocompetence
PBMC from each patient were suspended in AIM V medium (Life Technologies) with 5%
 Allogeneic T-cells expressing an anti-cd19 chimeric antigen receptor induce remissions of B-cell malignancies that progress after allogeneic hematopoietic stem cell transplantation without causing graft-versus-host
Allogeneic T-cells expressing an anti-cd19 chimeric antigen receptor induce remissions of B-cell malignancies that progress after allogeneic hematopoietic stem cell transplantation without causing graft-versus-host
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/37178 holds various files of this Leiden University dissertation Author: Bergen, Kees van Title: Characterization and recognition of minor histocompatibility
Cover Page The handle http://hdl.handle.net/1887/37178 holds various files of this Leiden University dissertation Author: Bergen, Kees van Title: Characterization and recognition of minor histocompatibility
3.1 Clinical safety of chimeric or humanized anti-cd25 (ch/anti-cd25)
 3 Results 3.1 Clinical safety of chimeric or humanized anti-cd25 (ch/anti-cd25) Five infusions of monoclonal IL-2 receptor antibody (anti-cd25) were planned according to protocol between day 0 and day
3 Results 3.1 Clinical safety of chimeric or humanized anti-cd25 (ch/anti-cd25) Five infusions of monoclonal IL-2 receptor antibody (anti-cd25) were planned according to protocol between day 0 and day
The National Marrow Donor Program. Graft Sources for Hematopoietic Cell Transplantation. Simon Bostic, URD Transplant Recipient
 1988 199 1992 1994 1996 1998 2 22 24 26 28 21 212 214 216 218 Adult Donors Cord Blood Units The National Donor Program Graft Sources for Hematopoietic Cell Transplantation Dennis L. Confer, MD Chief Medical
1988 199 1992 1994 1996 1998 2 22 24 26 28 21 212 214 216 218 Adult Donors Cord Blood Units The National Donor Program Graft Sources for Hematopoietic Cell Transplantation Dennis L. Confer, MD Chief Medical
Low Avidity CMV + T Cells accumulate in Old Humans
 Supplementary Figure Legends Supplementary Figure 1. CD45RA expressing CMVpp65-specific T cell populations accumulate within HLA-A*0201 and HLA-B*0701 individuals Pooled data showing the size of the NLV/HLA-A*0201-specific
Supplementary Figure Legends Supplementary Figure 1. CD45RA expressing CMVpp65-specific T cell populations accumulate within HLA-A*0201 and HLA-B*0701 individuals Pooled data showing the size of the NLV/HLA-A*0201-specific
Cell-based immunotherapy products for the treatment of blood cancers and inherited blood disorders. Company Presentation June 2016
 Cell-based immunotherapy products for the treatment of blood cancers and inherited blood disorders Company Presentation June 2016 Disclaimer These slides and the accompanying oral presentation contain
Cell-based immunotherapy products for the treatment of blood cancers and inherited blood disorders Company Presentation June 2016 Disclaimer These slides and the accompanying oral presentation contain
Riposta immune versus stato immune
 Riposta immune versus stato immune Russell E. Lewis U.O. Malattie Infettive, Policlinico S. Orsola-Malpighi Dipartimento di Scienze Mediche e Chirurgiche Alma Mater Studiorum Università di Bologna Immunodeficiency
Riposta immune versus stato immune Russell E. Lewis U.O. Malattie Infettive, Policlinico S. Orsola-Malpighi Dipartimento di Scienze Mediche e Chirurgiche Alma Mater Studiorum Università di Bologna Immunodeficiency
SUPPLEMENT Supplementary Figure 1: (A) (B)
 SUPPLEMENT Supplementary Figure 1: CD4 + naïve effector T cells (CD4 effector) were labeled with CFSE, stimulated with α-cd2/cd3/cd28 coated beads (at 2 beads/cell) and cultured alone or cocultured with
SUPPLEMENT Supplementary Figure 1: CD4 + naïve effector T cells (CD4 effector) were labeled with CFSE, stimulated with α-cd2/cd3/cd28 coated beads (at 2 beads/cell) and cultured alone or cocultured with
Tumor Immunology. Wirsma Arif Harahap Surgical Oncology Consultant
 Tumor Immunology Wirsma Arif Harahap Surgical Oncology Consultant 1) Immune responses that develop to cancer cells 2) Escape of cancer cells 3) Therapies: clinical and experimental Cancer cells can be
Tumor Immunology Wirsma Arif Harahap Surgical Oncology Consultant 1) Immune responses that develop to cancer cells 2) Escape of cancer cells 3) Therapies: clinical and experimental Cancer cells can be
Supplementary Figure 1
 Supplementary Figure 1 Identification of IFN-γ-producing CD8 + and CD4 + T cells with naive phenotype by alternative gating and sample-processing strategies. a. Contour 5% probability plots show definition
Supplementary Figure 1 Identification of IFN-γ-producing CD8 + and CD4 + T cells with naive phenotype by alternative gating and sample-processing strategies. a. Contour 5% probability plots show definition
Understanding the role of ex vivo T cell depletion
 Prevention of graftversus-host disease (GVHD) Understanding the role of ex vivo T cell depletion Information for patients undergoing allogeneic stem cell transplantation in AML and their families 2 This
Prevention of graftversus-host disease (GVHD) Understanding the role of ex vivo T cell depletion Information for patients undergoing allogeneic stem cell transplantation in AML and their families 2 This
Clinical Study CMV Serostatus of Donor-Recipient Pairs Influences the Risk of CMV Infection/Reactivation in HSCT Patients
 Bone Marrow Research Volume 22, Article ID 37575, 8 pages doi:.55/22/37575 Clinical Study CMV Serostatus of Donor-Recipient Pairs Influences the Risk of CMV Infection/Reactivation in HSCT Patients Emilia
Bone Marrow Research Volume 22, Article ID 37575, 8 pages doi:.55/22/37575 Clinical Study CMV Serostatus of Donor-Recipient Pairs Influences the Risk of CMV Infection/Reactivation in HSCT Patients Emilia
ASH 2011 aktualijos: MSC TPŠL gydyme. Mindaugas Stoškus VULSK HOTC MRMS
 ASH 2011 aktualijos: MSC TPŠL gydyme Mindaugas Stoškus VULSK HOTC MRMS #3042. Yukiyasu Ozawa et al. Mesenchymal Stem Cells As a Treatment for Steroid-Resistant Acute Graft Versus Host Disease (agvhd);
ASH 2011 aktualijos: MSC TPŠL gydyme Mindaugas Stoškus VULSK HOTC MRMS #3042. Yukiyasu Ozawa et al. Mesenchymal Stem Cells As a Treatment for Steroid-Resistant Acute Graft Versus Host Disease (agvhd);
Transplantation - Challenges for the future. Dr Gordon Cook S t James s Institute of Oncology, Leeds Teaching Hospitals Trust
 Transplantation - Challenges for the future Dr Gordon Cook S t James s Institute of Oncology, Leeds Teaching Hospitals Trust Bone Marrow Transplantation Timeline, 1957-2006 Appelbaum F. N Engl J Med 2007;357:1472-1475
Transplantation - Challenges for the future Dr Gordon Cook S t James s Institute of Oncology, Leeds Teaching Hospitals Trust Bone Marrow Transplantation Timeline, 1957-2006 Appelbaum F. N Engl J Med 2007;357:1472-1475
Allo CTL Protocol Page 1 of 43 Version 0.8 dated August 15th, 2008
 Page 1 of 43 Version 0.8 dated August 15th, 2008 Most Closely HLA Matched Allogeneic Virus Specific Cytotoxic T- Lymphocytes (CTL) to Treat Persistent Reactivation or Infection with Adenovirus, CMV and
Page 1 of 43 Version 0.8 dated August 15th, 2008 Most Closely HLA Matched Allogeneic Virus Specific Cytotoxic T- Lymphocytes (CTL) to Treat Persistent Reactivation or Infection with Adenovirus, CMV and
Michael Grimley 1, Vinod Prasad 2, Joanne Kurtzberg 2, Roy Chemaly 3, Thomas Brundage 4, Chad Wilson 4, Herve Mommeja-Marin 4
 Twice-weekly Brincidofovir (BCV, CMX1) Shows Promising Antiviral Activity in Immunocompromised Transplant Patients with Asymptomatic Adenovirus Viremia Michael Grimley 1, Vinod Prasad, Joanne Kurtzberg,
Twice-weekly Brincidofovir (BCV, CMX1) Shows Promising Antiviral Activity in Immunocompromised Transplant Patients with Asymptomatic Adenovirus Viremia Michael Grimley 1, Vinod Prasad, Joanne Kurtzberg,
5/9/2018. Bone marrow failure diseases (aplastic anemia) can be cured by providing a source of new marrow
 5/9/2018 or Stem Cell Harvest Where we are now, and What s Coming AA MDS International Foundation Indianapolis IN Luke Akard MD May 19, 2018 Infusion Transplant Conditioning Treatment 2-7 days STEM CELL
5/9/2018 or Stem Cell Harvest Where we are now, and What s Coming AA MDS International Foundation Indianapolis IN Luke Akard MD May 19, 2018 Infusion Transplant Conditioning Treatment 2-7 days STEM CELL
