T tation remains high and is reported as 38% [l]. The
|
|
|
- Mariah Green
- 6 years ago
- Views:
Transcription
1 Pneumocystis carinii Pneumonia After Heart Transplantation Hideaki Saigenji, MD, Mitsunori Kaneko, MD, Birger Rhenmen, MD, Richard J. Williams, MD, M. Andre Vasu, MD, Timothy B. Icenogle, MD, and Jack G. Copeland, MD Section of Cardiovascular and Thoracic Surgery, Department of Surgery, University of Arizona, Tucson, Arizona Five patients with Pneumocystis carinii pneumonia after heart transplantation are reported. Four had severe clinical symptoms, whereas 1 was asymptomatic. Mechanical ventilatory support was necessary in 1 because of respiratory distress. Pneumocystis carinii infection developed in 4 patients within the first 4 postoperative months, and 1 patient had clinical disease 1 year after transplantation with a recurrence 9 months later. All were treated with trimethoprim-sulfamethoxazole either orally or intravenously (10 to 20 mg * kg-' * day-' of trimethoprim). All patients recovered from infection and received the same drug prophylactically for 2 to 20 months after the infection. All patients are doing well after Pneumocystis carinii infection except 1 who died after an acute myocardial infarction 4 years after infection. We conclude that trimethoprim-sulfamethoxazole is an effective agent for the treatment of Pneumocystis carinii pneumonia after heart transplantation. (Ann Thoruc Surg ) he mortality rate due to infection after heart transplan- T tation remains high and is reported as 38% [l]. The organisms seen after heart transplantation can be universal [2, 31. When diffuse infiltrates in the lung of the immunocompromised host appear in the chest roentgenogram, Pneumocystis curinii infection is the most likely infecting agent [4]. From the beginning of our heart transplant program in March 1979 to March 1988, 159 heart and six heart and lung transplantation procedures were performed. Of this group, Pneumocystis curinii infection developed in 5 patients. This article reports the clinical picture of Pneumocystis curinii pneumonia (PCP) in our series. The problems of diagnosis and treatment of PCP after heart transplantation are also discussed. Material and Methods From March 1979 to March 1988, 158 orthotopic and one heterotopic heart transplantation (HTX) were performed in 139 male and 20 female patients ranging from 2 to 65 years of age. Of those patients, 6 (3 patients in each group) were undergoing a second HTX due to graft failure and graft atherosclerosis. The initial indication for HTX was end-stage heart disease, primary or secondary to ischemic or idiopathic cardiomyopathy. Pneumocystis curinii pneumonia developed in 5 of the 153 heart transplant patients. Accepted for publication March 20, Dr Saigenji's present address is The Second Department of Surgery, Kagoshima University Faculty of Medicine, Sakuragaoka, Kagoshima 890, Japan. Address reprint requests to Dr Copeland, Section of Cardiovascular and Thoracic Surgery, University of Arizona Health Sciences Center, 1501 N Campbell Ave, Tucson, AZ Immunosuppressive regimens for all patients were described in detail previously [2, 3, 51. From 1979 to 1982, immunosuppression consisted of the administration of, and rabbit antithymocyte globulin. From 1983 to 1984, cyclosporin A,, and rabbit antithymocyte globulin were used, and a regimen of cyclosporin A,, and rabbit antithymocyte globulin was followed from 1985 to present. The serum concentration of cyclosporin A 12 hours after the previous dose as measured by radioimmunoassay was maintained at 200 to 250 ng/ml for the first postoperative month and then 100 to 150 ng/ml after the first month. Azathioprine was given at a dose of 2 mg - kg-' - day-' orally and titrated so that a white blood cell count of at least 5 x 109/L (5,OOO/pL) was maintained. Five hundred milligrams of intravenous methylprednisolone was administered intraoperatively, and then 125 mg was given every 12 hours until oral administration was begun. Prednisone was given orally at 1.5 mg * kg-' - day-' and was tapered to 0.5 mg - kg-'.day-' the first month, 0.25 mg. kg-' -day-' at 3 months, and mg - kg-' - day-' at 1 year. In patients suspected of having lung infection after HTX, a transtracheal aspiration was performed in an attempt to isolate the infecting agents. Bronchoscopy and bronchoalveolar lavage were performed under general anesthesia in 1 patient. The specimens obtained by transtracheal aspiration or bronchoalveolar lavage were sent for an immediate Gram stain and KOH preparation for fungi. Cultures for anaerobic and aerobic bacteria, as well as fungi, Legionella, acid-fast bacteria, viruses, mycoplasma, nocardia, and chlamydia were obtained. Part of the specimen was also sent for a silver stain for Pneumocystis curinii and fluorescent antibody stain for Legionella. If by The Society of Thoracic Surgeons /91/$3.50
2 108 SAICENJI ET AL PNEUMOCYSTIS CARINII PNEUMONIA Ann Thorac Surg Table 1. Clinical Pictures Onset of PCP After I m m u n o - Patient Age HTX suppressive No. (y) Sex (mo) Regimens Clinical Pictures 1 25 M 12 Azathioprine, 21 Azathioprine, 2 49 M 2 Cyclosporin A, 3 54 M 4 Cyclosporine A, 4 52 M 2 Cyclosporine A, 5 46 M 2.5 Cyclosporine A, HTX = heart transplantation; M = male; pneumonia; SOB = shortness of breath. Fever, chills, malaise, SOB, Dyspnea, SOB, Asymptomatic Fever, chills, headache, SOB, cough Low grade fever, SOB Chills, SOB, PCP = Pneumocystis carinii no pathogen was found in those specimens, percutaneous transthoracic needle aspiration of the lung under biplane fluoroscopic control was carried out. The specimen from lung aspiration underwent the same tests as those of the transtracheal aspiration. Definite diagnosis of PCP was confirmed by the demonstration of the organism in the lung tissue by transthoracic needle aspiration or in the material obtained from the respiratory tree by transtracheal aspiration or bronchoalveolar lavage. Results Six episodes in 5 of 153 heart transplant patients had confirmed diagnosis of PCP. One patient took azathioprine and, 1 received cyclosporin A and, and 3 patients were given cyclosporin A,, and azathioprine as immunosuppression. Pneumocystis carinii developed in 4 patients from 2 to 4 months after HTX. Patient 1 was proven to have PCP 1 year after transplantation, and this patient had a recurrent PCP 9 months after the initial infection. The patients had various symptoms including fever, chills, shortness of breath, dyspnea without auscultatory finding, and pleuritic pain. One patient had no symptoms (Table 1). Body temperature greater than 37 C was present in 3 patients with the highest recorded temperature being 39.6"C. Respiratory rate ranged from 16 to 32 per minute (mean, 23 per minute). In the laboratory investigations, leukocytosis was present in 4 of 5 patients. Arterial oxygen tension revealed mild to moderate hypoxia (59 to 81 mm Hg; inspired oxygen fraction, 0.21 to 0.4). Arterial carbon dioxide tension tended to show hypocapnia (30 to 34 mm Hg) in all patients (Table 2). Roentgenographic findings of the lungs revealed bilateral diffuse interstitial and alveolar infiltrates in all patients. In 1 patient, a localized nodular infiltrate in the upper left lung was found on the chest roentgenogram at the time of admission. The infiltrate spread rapidly to both lung fields (see Table 2). A random sputum examination showed Pneumocystis Table 2. Laboratory and Radiographic Findings Patient WBC Count Arterial Blood Gas No. (1091~) PO, (mm Hg) PCO, (mm Hg) SaO, PH Radiographic Findings Severe nodular densities 11.2 (FiO, = 0.21) as well as bilateral diffuse interstitial and alveolar infiltrate Bilateral diffuse Localized infiltrate in left lobe at admission, bilateral diffuse interalveolar infiltrate 2 days after admission Bilateral diffuse (FiO, = 0.4) interstitial and alveolar infiltrate Bilateral diffuse (FiO, = 0.4) Bilateral diffuse (Fi02 = 0.4) FiO, = inspired oxygen fraction; = not done; PO, = oxygen tension; PCO, = carbon dioxide tension; SaO, = oxygen saturation; WBC = white blood cell.
3 Ann Thorac Surg SAIGENJI ET AL 109 PNEUMOCYSTIS CARINII PNEUMONIA Table 3. Diagnostic Procedures and Coexisting Infections Patient No. Sputum TTA TNA BAL Coexisting Organisms Nocardia (TTA), Aspergillus (TTA), Streptococcus viridans (TTA) None Neisseria (TTA), Nonehemolytic streptococci (TTA), Herpes simplex (oral swab) Cytomegalovirus (urine) Enterovirus (TTA), cytomegalovirus (BAL) Cytomegalovirus (urine) BAL = bronchoalveolar lavage; = not done; TNA = transthoradc needle aspiration of the lung; lta = transtracheal aspiration; + = positive Pneumocystis carinii in silver stain; - = negative Pneumocystis carinii in silver stain. carinii in 1 patient, but no Pneurnocystis carinii was obtained from transtracheal aspiration in any patient. Pneumocystis carinii was demonstrated in the lung tissue obtained by percutaneous transthoracic needle aspiration in 4 of 5 patients. No Pneumocystis carinii was found in the bronchoalveolar lavage material in 1 patient in whom it was performed. Coexisting infections in the lung or other organs are presented in Table 3. Other pulmonary infection were found in 3 patients. Viral cultures were positive in 4 of the 5 patients, and cytomegalovirus was found in 3 of these 4 patients. Trimethoprim-sulfamethoxazole (TMP-SMX) was given for the treatment of PCP in all patients with a dosage of 10 to 22 mg - kg-' day-' of TMP (160 mg TMP/800 mg SMX). When a patient could not tolerate TMP-SMX orally due to nausea, vomiting, or endotracheal intubation, TMP-SMX with the dosage of 16 to 18 mg - kg-' day-' of TMP (16 mg/ml TMP/80 mg/ml SMX) was administered intravenously. The serum concentration of SMX 1 to 2 hours after the administration of TMP-SMX was examined in 3 patients. The measured serum level ranged between 97 to 193 pg/ml. The side effects identified with this drug were nausea, vomiting, and anorexia. These were present in 4 patients. Patient 4 required mechanical ventilatory support due to the deterioration of respiratory function after the diagnosis of PCP. He was able to be extubated after 2 days of ventilatory support. Clinical symptoms rapidly improved within 2 to 5 days after the beginning of treatment with TMP-SMX; however, radiographic clearing was prolonged an average of 1 month after treatment was initiated. The duration of hospitalization ranged from 5 to 13 days (mean, 10.3 days). All patients prophylactically received TMP-SMX with doses of 4.2 to 5.5 mg - kg-' * day-' of TMP (160 mg TMP/800 mg SMX) for 2 to 20 months after resolution of clinical disease. The only recurrence was in a patient who received only 2 months of postinfection therapy. One patient died 4% years after Pneumocystis carinii infection because of acute myocardial infarction. The remaining 4 patients are doing well from 4 months to 6.5 years after initial Pneumocystis carinii infection (Table 4). Comment Protozoal infection after heart transplantation is infrequent [6, 71, but poses high mortality [8]. The usual organism of protozoal infection is Pneumocystis carinii, and the site of infection is in the lung [9]. From March 1979 to March 1988, 153 patients underwent heart transplantation and 142 of 153 survived at least 1 month after heart transplantation. Pneumocystis carinii pneumonia developed in 5 of the 142 patients (3.5%) surviving more than 1 month, demonstrating the low incidence of PCP. Pneumocystis carinii pneumonia developed in 4 of 5 patients in the early postoperative period (2 to 4 months). Oyer and associates [lo] reported that 87% of all Pneumocystis carinii infections have been diagnosed after the first 3 postoperative months. Most likely, Pneurnocystis carinii infection is opportunistic. All transplanted patients are maintained on immunosuppressive regimens and their resistance to Table 4. Treatment and Prognosis Dose of TMP Dose of SMX Serum Concentration day-') day-') of SMX 1-2 h (mg * kg-'. (mg kg-'. Prophylaxis Patieht After Intake Side Duration Dose No. PO IV PO IV (clg/ml) Effects (mo) (mg. kg-'. day-') Result Abd pain Alive Abd pain, Alive N, V N, V Died" N, V Alive N, V Alive None Alive a Died due to acute myocardial infarction. Abd = abdominal; IV = intravenous administration; N = nausea; = not done; PO = oral intake; SMX = sulfamethoxazole; TMP = trimethoprim; V = vomiting.
4 110 SAIGENJI ET AL PNEUMOCYSTZS CARZNIZ PNEUMONIA Ann Thorac Surg Table 5. Relationship Between lmmunosuppressive Regimen and lncidence of Pneumocystis carinii Pneumonia AZ CsA CsA + Variable + Pred + Pred Pred + AZ Total (1)" 101 (5)" transplantations Survival >1 mo Pneurnocystis carinii 1(3.6%) 1(3.9%) 3 (3.2%) infection a Numbers in parentheses are retransplantations. AZ = azathioprine; CsA = cyclosporin A; Pred =. infection is always reduced in this immunocompromised state. The most aggressive immunosuppression is provided in the early postoperative period and corresponds to the period of the onset of PCP. We have used three different immunosuppressive protocols, but there was no demonstrable difference (x2 analysis) in frequency of PCP among them (Table 5). Definite diagnosis for PCP is confirmed if Pneurnocystis carinii is found in the lung tissue or in the materials from the respiratory tree. Our approach to all transplant patients with fever and any chest roentgenographic abnormality, which might be secondary to infection, is to perform an immediate transtracheal aspiration and to then treat the patient if pathogens are found on stains, cultures, or cytology [ll-131. With transtracheal aspiration, we have had 96% specificity, 70% sensitivity, and 78% accuracy in the diagnosis of pulmonary infections. Although none of these were Pneumocystis, we did reach a diagnosis for 1 patient in our series with a posttranstracheal aspirate sputum (ie, sputum produced immediately after transtracheal aspirate). If early studies (Gram stain, KOH preparation, cytology, Legionella fluorescent antibody) are negative and our patient is toxic or septic or deteriorating clinically or persistently febrile, we proceed immediately to percutaneous transthoracic needle aspiration under fluoroscopic or computed tomographic control. Using this technique, we diagnosed 5 of 6 Pneurnocystis infections and have had 100% specificity, 89% sensitivity, and 91% accuracy with our total series of pulmonary infections. The combination of transtracheal aspiration and transthoracic needle aspiration yielded a sensitivity of 90%, a specificity of loo%, and an accuracy of 91%. In general, we have avoided bronchoscopy in the heart transplant population. Our feeling is that it adds a level of complexity to patient care that is, in most cases, unnecessary and that it may be associated with contaminated cultures by virtue of the transoral approach. Similarly, we have avoided open lung biopsy, an unnecessary and morbid procedure, for cardiac recipients. The diagnostic value of sputum examination is low in our series, but Pitchenik and associates [15] reported that this method was effective in 55% of patients with PCP. Other invasive diagnostic maneuvers such as bronchial brushing, transbronchial lung biopsy, bronchoalveolar lavage, and open lung biopsy have had diagnostic values ranging from 69% to 90% [ Recently, noninvasive methods of diagnosis in PCP have shown promise. Kovacs and co-workers [20] report that 90% of PCP can be diagnosed with indirect immunofluorescence. The characteristic findings on chest radiogram in PCP are bilateral perihilar and basilar infiltrates seen as a diffuse alveolar consolidation without pleural change [4]. All patients in our series have shown these typical changes; however, the initial chest radiographic change in 1 patient was a focal nodular infiltrate. Various atypical radiographic changes in PCP have been reported [21]. These changes include lobular involvement, unilateral predominance, atelectatic-appearing infiltrate, and a pseudonodular pattern. Furthermore, some patients have no abnormalities [22]. Because of the numerous atypical radiographic presentations with PCP, close follow-up and a high level of suspicion are necessary to make diagnosis early. All patients received TMP-SMX (160 mg TMP/800 mg SMX) for the treatment of PCP with the dosage of 10 to 20 mg * kg-' * day-' of TMP. We administer this drug as the initial choice in the treatment of PCP because of fewer reported side effects than pentamidine [23]. Intravenous administration of TMP-SMX with the dosage of 16 to 18 mg * kg-' - day-' of TMP was introduced in those patients who could not tolerate oral administration. The serum concentration of SMX 1 to 2 hours after administration ranged from 97 to 193 pg/ml. Winston and associates [23] reported that the serum levels of SMX were parallel to those of TMP but were about 20 times greater, and a 1.5-hour serum SMX level of at least 100 pg/ml might be used to guide therapy whenever TMP level could not be measured. In 3 patients we were only able to measure the SMX level 1 to 2 hours after TMP-SMX administration. Although 1 patient had a serum level of SMX of 97 pg/ml, the other 2 had levels in excess of 100 pg/ml with our dose regimen. These doses of TMP-SMX were considered high enough to be therapeutic for treatment of PCP. The interaction between TMP-SMX and immunosuppressive regimens is not clear. Though Schafers and colleagues [7] reported that they discontinued use of and azathioprine for the treatment of PCP with TMP-SMX, we found no reason to change the dosages of and azathioprine. Patients receiving azathioprine should be given sulfa with caution as there may be synergistic myelosuppression with these two agents [ll]; however, no one to date has reported pancytopenia, leukopenia, or thrombocytopenia. In all of our heart transplant patients, the dose of cyclosporin A is adjusted daily to keep a serum concentration of 200 to 250 ng/ml for the first postoperative month and 100 to 150 ng/ml after the first month measured by radioimmunoassay. Although it is well known that some kinds of antibiotics affect the serum concentration of cyclosporin A [5], we have not found any adverse interaction between TMP-SMX and cyclosporin A. In all 5 of our patients, the clinical symptoms improved within 2 to 5 days after the beginning of treatment with TMP-SMX; however, radiographic improvement was not
5 Ann Thorac Surg 1991; SAICENJI ET AL 111 DNEUMOCYSTIS CARIN11 PNEUMONIA complete until about 1 month after the beginning of TMP-SMX. Prophylactic continuation of TMP-SMX was given at 4 to 5 mg - kg-' * day-' for 2 to 20 months. Recurrent PCP developed in 1 patient 9 months after initial infection. Although we havqnot determined how long patients must take TMP-SMX prophylactically, we currently recommend continuous therapy for 3 to 6 months after the initial infection with monthly follow-up, because our only recurrence was in a patient treated for 2 months. We do not use this drug permanently, because PCP is considered to be treatable if a recurrence develops. Our retrospective study includes many patients from before the contemporary use of prophylactic TMP-SMX. Although we have been treating cardiac recipients with prophylactic TMP-SMX for 1 year, we have serious reservations and are considering the discontinuation of such therapy. Most important are the toxicities of this therapy: nausea, vomiting, inability to take adequate nutrition or oral medications, and the aforementioned myelotoxicity, especially in the face of ongoing azathioprine treatment. Finally, the low number of Pneumocystis cases in our series (3.5%) and the absence of related mortality may not justify prophylaxis. In summary, Pneumocystis carinii pneumonia developed in 5 of 142 patients who have survived at least 1 month after heart transplantation. All patients recovered from this infection. Trimethoprim-sulfamethoxazole is an effective treatment of this infection in the patients who undergo heart transplantation. References 1. Kaye MP. The registry report. Eighth Annual Meeting of the International Society for Heart Transplantation, Los Angeles, Copeland JG, Mammana RB, Fuller JK, et al. Heart transplantation: four years' experience with conventional immunosuppression. JAMA 1984;251:156%6. 3. Copeland JG, Emery RW, Levinson MM, et al. Cyclosporine: an immunosuppressive panacea? J Thorac Cardiovasc Surg 1986;91: Young LS. Clinical aspects of pneumocystosis in man: epidemiology, clinical manifestations, diagnostic approaches, and sequelae. In: Young LS, ed. Pneumocystis curinii pneumonia. New York: Marcel Dekker, 1984: Copeland JG. Cardiac transplantation. Curr Probl Cardiol 1988;13: Baumgartner WA. Infection in cardiac transplantation. Heart Transplant 1983;3: Schafers HJ, Cremer J, Wahlers T, et al. Pneumocystis curinii pneumonia following heart transplantation. Eur J Cardiothorac Surg 1987;1: Jamieson SW, Oyer PE, Reitz BA, et al. Cardiac transplantation at Stanford. Heart Transplant 1981;1: Mammana RB, Petersen EA, Fuller JK, et al. Pulmonary infections in cardiac transplant patients: modes of diagnosis, complications, and effectiveness of therapy. Ann Thorac Surg 1983;36: Oyer PE, Stinson EB, Bieber CP, Shumway NE. Cardiac transplantation. In: Chatterjee SN, ed. Organ transplantation. Boston: PSG, 1982: Icenogle TB, Copeland JG. Emergency evaluation of the acutely ill heart transplant patient. Boswell Hosp Proc 1987; 13: Ruskin J. Parasitic diseases in the compromised host. In: Rubin RH, Young LS, eds. Clinical approach to infection in the compromised host. 2nd ed. New York: Plenum, 1988: Lau WK, Young LS, Remington JS. Pneumocystis curinii pneumonia: diagnosis by examination of pulmonary secretions. JAMA 1976;236: DeVivo F, Pond GD, Rhenman 8, et al. Transtracheal aspiration and fine needle aspiration biopsy for the diagnosis of pulmonary infection in heart transplant patients. J Thorac Cardiovasc Surg 1988;96:69& Pitchenik AE, Ganjei P, Torres A, et al. Sputum examination for the diagnosis of Pneumocystis curinii pneumonia in the acquired immunodeficiency syndrome. Am Rev Respir Dis 1986;133: Hartman B, Koss M, Hui A, et al. Pneumocystis curinii pneumonia in the acquired immunodeficiency syndrome (AIDS): diagnosis with bronchial brushings, biopsy, and bronchoalveolar lavage. Chest 1985;87: Scheinhorn DJ, Joyner LR, Whitcomb ME. Transbronchial forceps lung biopsy through the fiberoptic bronchoscope in pneumocystis carinii pneumonia. Chest 1974;66: Ognibene FP, Shelhamer J, Gill V, et al. The diagnosis of Pneumocystis curinii pneumonia in patients with the acquired immunodeficiency syndrome using subsegmental bronchoalveolar lavage. Am Rev Respir Dis 1984;129: Peters SG, Prakash UBS. Pneumocystis curinii pneumonia: review of 53 cases. Am J Med 1987;82: Kovacs JA, Ng VL, Masur H, et al. Diagnosis of Pneumocystis curinii pneumonia: improved detection in sputum with use of monoclonal antibodies. N Engl J Med 1988; Doppman JL, Geelhoed GW, de Vita VT. Atypical radiographic feature in Pneumocystis curinii pneumonia. Radiology 1975;114: Israel HL, Gottlieb JE, Schulman ES. Hypoxemia with normal chest roentgenogram due to Pneumocystis carinii pneumonia. Diagnostic errors due to low suspicion of AIDS. Chest 1987;92: Winston DJ, Lau WK, Gale RP, Young LS. Trimethoprimsulfamethoxazole for the treatment of Pneumocystis curinii pneumonia. Ann Intern Med 1980;92:762-9.
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Pneumocystis Pneumonia. Dr. Pradeep kumar II yr Pulmonary Medicine
 Pneumocystis Pneumonia Dr. Pradeep kumar II yr Pulmonary Medicine PNEUMOCYSTIS CARINII PNEUMONIA Pneumocystis carinii pneumonia (PCP), is commonly termed Pneumocystis jiroveci pneumonia, is the 2 nd most
Pneumocystis Pneumonia Dr. Pradeep kumar II yr Pulmonary Medicine PNEUMOCYSTIS CARINII PNEUMONIA Pneumocystis carinii pneumonia (PCP), is commonly termed Pneumocystis jiroveci pneumonia, is the 2 nd most
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids
 Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Community Acquired Pneumonia. Abdullah Alharbi, MD, FCCP
 Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Chapter 22. Pulmonary Infections
 Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement
 CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
Pneumocystis. Pneumocystis BIOL Summer Introduction. Mycology. Introduction (cont.) Introduction (cont.)
 Introduction Pneumocystis Disclaimer: This lecture slide presentation is intended solely for educational purposes. Many of the images contained herein are the property of the original owner, as indicated
Introduction Pneumocystis Disclaimer: This lecture slide presentation is intended solely for educational purposes. Many of the images contained herein are the property of the original owner, as indicated
Antimicrobial Stewardship in Community Acquired Pneumonia
 Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Eastern Mediterranean Health Journal, Vol. 14, No. 5,
 Eastern Mediterranean Health Journal, Vol. 14, No. 5, 2008 1217 Case report Inappropriate use of steroid and Pneumocystis jiroveci pneumonia: report of two cases P. Tabarsi, 1 M. Mirsaeidi, 1 M. Amiri,
Eastern Mediterranean Health Journal, Vol. 14, No. 5, 2008 1217 Case report Inappropriate use of steroid and Pneumocystis jiroveci pneumonia: report of two cases P. Tabarsi, 1 M. Mirsaeidi, 1 M. Amiri,
11/19/2012. The spectrum of pulmonary diseases in HIV-infected persons is broad.
 The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Nitrofurantoin-Induced Lung Toxicity
 Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
The 1-year survival rate approaches 80% for patients
 Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Supplementary Online Content
 Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Immunocompromised patients. Immunocompromised patients. Immunocompromised patients
 Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
2046: Fungal Infection Pre-Infusion Data
 2046: Fungal Infection Pre-Infusion Data Fungal infections are significant opportunistic infections affecting transplant patients. Because these infections are quite serious, it is important to collect
2046: Fungal Infection Pre-Infusion Data Fungal infections are significant opportunistic infections affecting transplant patients. Because these infections are quite serious, it is important to collect
Making the Right Call With. Pneumonia. Community-acquired pneumonia (CAP) is a. Community-Acquired. What exactly is CAP?
 Making the Right Call With Community-Acquired Pneumonia In this article: By Thomas J. Marrie, MD The case of Allyson Allyson, 32, presented to the emergency department with a 48-hour history of anorexia,
Making the Right Call With Community-Acquired Pneumonia In this article: By Thomas J. Marrie, MD The case of Allyson Allyson, 32, presented to the emergency department with a 48-hour history of anorexia,
Trial protocol - NIVAS Study
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
Acute Isolated Pulmonaw Reiection Following Transplantatich of the Heart and Both Lungs: Experimental and Clinical Observations
 Acute Isolated Pulmonaw Reiection Following Transplantatich of the Heart and Both Lungs: Experimental and Clinical Observations D. Novitzky, M.D., D. K. C. Cooper, Ph.D., F.R.C.S., A. G. Rose, Ch.B., M.Med.(Path),
Acute Isolated Pulmonaw Reiection Following Transplantatich of the Heart and Both Lungs: Experimental and Clinical Observations D. Novitzky, M.D., D. K. C. Cooper, Ph.D., F.R.C.S., A. G. Rose, Ch.B., M.Med.(Path),
Invasive Pulmonary Aspergillosis in
 Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Methods ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE
 ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE Li-Hui Soh, Chih-Feng Chian, Wen-Lin Su, Horng-Chin Yan, Wann-Cherng Perng, and Chin-Pyng Wu Background
ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE Li-Hui Soh, Chih-Feng Chian, Wen-Lin Su, Horng-Chin Yan, Wann-Cherng Perng, and Chin-Pyng Wu Background
Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data
 Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data David Ebler, MD David Skarupa, MD Andrew J. Kerwin, MD, FACS Jhun de Villa, MD Michael S. Nussbaum, MD, FACS J.J. Tepas III, MD, FACS
Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data David Ebler, MD David Skarupa, MD Andrew J. Kerwin, MD, FACS Jhun de Villa, MD Michael S. Nussbaum, MD, FACS J.J. Tepas III, MD, FACS
Pneumonia. Definition of pneumonia Infection of the lung parenchyma Usually bacterial
 Pneumonia Definition of pneumonia Infection of the lung parenchyma Usually bacterial Epidemiology of pneumonia Commonest infectious cause of death in the UK and USA Incidence - 5-11 per 1000 per year Worse
Pneumonia Definition of pneumonia Infection of the lung parenchyma Usually bacterial Epidemiology of pneumonia Commonest infectious cause of death in the UK and USA Incidence - 5-11 per 1000 per year Worse
Pneumonia in immunosuppressed patients
 Blackwell Science, LtdOxford, UKRESRespirology1323-77992004 Blackwell Science Asia Pty LtdMarch 20049S1S25S29Original ArticlePneumonia in immunosuppressed patientss Kohno et al. Respirology (2004) 9, S25
Blackwell Science, LtdOxford, UKRESRespirology1323-77992004 Blackwell Science Asia Pty LtdMarch 20049S1S25S29Original ArticlePneumonia in immunosuppressed patientss Kohno et al. Respirology (2004) 9, S25
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia)
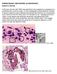 PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia) A 46-year-old man with AIDS was admitted to the hospital for complaints of a persisting fever and dry cough. A chest radiograph showed bilateral
PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia) A 46-year-old man with AIDS was admitted to the hospital for complaints of a persisting fever and dry cough. A chest radiograph showed bilateral
Outcomes of Moderate-to-Severe Pneumocystis Pneumonia Treated with Adjunctive Steroid in Non-HIV-Infected Patients
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2011, p. 4613 4618 Vol. 55, No. 10 0066-4804/11/$12.00 doi:10.1128/aac.00669-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Outcomes
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2011, p. 4613 4618 Vol. 55, No. 10 0066-4804/11/$12.00 doi:10.1128/aac.00669-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Outcomes
MICROBIOLOGICAL TESTING IN PICU
 MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
PULMONARY EMERGENCIES
 EMERGENCIES I. Pneumonia A. Bacterial Pneumonia (most common cause of a focal infiltrate) 1. Epidemiology a. Accounts for up to 10% of hospital admissions in the U.S. b. Most pneumonias are the result
EMERGENCIES I. Pneumonia A. Bacterial Pneumonia (most common cause of a focal infiltrate) 1. Epidemiology a. Accounts for up to 10% of hospital admissions in the U.S. b. Most pneumonias are the result
HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION
 HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health Care Medical
HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health Care Medical
Unit II Problem 2 Pathology: Pneumonia
 Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Medical monitoring: tests available at central hospitals
 medial monitoring: tests available at central hospitals: 1 medical monitoring: tests available at central hospitals Medical monitoring: tests available at central hospitals medial monitoring: tests available
medial monitoring: tests available at central hospitals: 1 medical monitoring: tests available at central hospitals Medical monitoring: tests available at central hospitals medial monitoring: tests available
All I Need Is The Air That I Breathe: A Case Study of Immunotherapy and Severe Pneumonitis
 All I Need Is The Air That I Breathe: A Case Study of Immunotherapy and Severe Pneumonitis Presenter Disclosure Faculty/Speaker: Dr. Brett Finney BSc MD CCFP Relationships with financial sponsors: Grants/Research
All I Need Is The Air That I Breathe: A Case Study of Immunotherapy and Severe Pneumonitis Presenter Disclosure Faculty/Speaker: Dr. Brett Finney BSc MD CCFP Relationships with financial sponsors: Grants/Research
The Pulmonary Pathology of Iatrogenic Immunosuppression. Kevin O. Leslie, M.D. Mayo Clinic Scottsdale
 The Pulmonary Pathology of Iatrogenic Immunosuppression Kevin O. Leslie, M.D. Mayo Clinic Scottsdale The indications for iatrogenic immunosuppression Autoimmune/inflammatory disease Chemotherapy for malignant
The Pulmonary Pathology of Iatrogenic Immunosuppression Kevin O. Leslie, M.D. Mayo Clinic Scottsdale The indications for iatrogenic immunosuppression Autoimmune/inflammatory disease Chemotherapy for malignant
Community-Acquired Pneumonia OBSOLETE 2
 Community-Acquired Pneumonia OBSOLETE 2 Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with respect to appropriate
Community-Acquired Pneumonia OBSOLETE 2 Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with respect to appropriate
PNEUMONIA. I. Background 6 th most common cause of death in U.S. Most common cause of infection related mortality
 Page 1 of 8 September 4, 2001 Donald P. Levine, M.D. University Health Center Suite 5C Office: 577-0348 dlevine@intmed.wayne.edu Assigned reading: pages 153-160; 553-563 PNEUMONIA the most widespread and
Page 1 of 8 September 4, 2001 Donald P. Levine, M.D. University Health Center Suite 5C Office: 577-0348 dlevine@intmed.wayne.edu Assigned reading: pages 153-160; 553-563 PNEUMONIA the most widespread and
Critical Care Nursing Theory. Pneumonia. - Pneumonia is an acute infection of the pulmonary parenchyma
 - is an acute infection of the pulmonary parenchyma - is a common infection encountered by critical care nurses when it complicates the course of a serious illness or leads to acute respiratory distress.
- is an acute infection of the pulmonary parenchyma - is a common infection encountered by critical care nurses when it complicates the course of a serious illness or leads to acute respiratory distress.
clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS*
 clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS* Sanjay R. Patel, MD; Dimitri Karmpaliotis, MD; Najib T. Ayas, MD; Eugene J. Mark, MD; John Wain, MD, FCCP; B. Taylor Thompson,
clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS* Sanjay R. Patel, MD; Dimitri Karmpaliotis, MD; Najib T. Ayas, MD; Eugene J. Mark, MD; John Wain, MD, FCCP; B. Taylor Thompson,
Pneumocystis carinii Pneumonia in Critically Ill Patients with Malignancy: A Descriptive Study
 MAJOR ARTICLE Pneumocystis carinii Pneumonia in Critically Ill Patients with Malignancy: A Descriptive Study J. R. Zahar, 1,a M. Robin, 1 E. Azoulay, 2 F. Fieux, 2 G. Nitenberg, 1 and B. Schlemmer 2 1
MAJOR ARTICLE Pneumocystis carinii Pneumonia in Critically Ill Patients with Malignancy: A Descriptive Study J. R. Zahar, 1,a M. Robin, 1 E. Azoulay, 2 F. Fieux, 2 G. Nitenberg, 1 and B. Schlemmer 2 1
Pneumocystis carinii Pneumonia: Diagnosis
 THE JOURNAL OF INFECTIOUS DISEASES VOL. 157, NO.6. JUNE 1988 1988 by The University of Chicago. All rights reserved. 0022-1899/88/5706-0001$01.00 AIDS COMMENTARY Pneumocystis carinii Pneumonia: Diagnosis
THE JOURNAL OF INFECTIOUS DISEASES VOL. 157, NO.6. JUNE 1988 1988 by The University of Chicago. All rights reserved. 0022-1899/88/5706-0001$01.00 AIDS COMMENTARY Pneumocystis carinii Pneumonia: Diagnosis
PNEUMONIA IN CHILDREN. IAP UG Teaching slides
 PNEUMONIA IN CHILDREN 1 INTRODUCTION 156 million new episodes / yr. worldwide 151 million episodes developing world 95% in developing countries 19% of all deaths in children
PNEUMONIA IN CHILDREN 1 INTRODUCTION 156 million new episodes / yr. worldwide 151 million episodes developing world 95% in developing countries 19% of all deaths in children
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
PEDIATRIC INFLUENZA CLINICAL PRACTICE GUIDELINES
 PEDIATRIC INFLUENZA CLINICAL PRACTICE GUIDELINES DEFINITIONS AND BACKGROUND Uncomplicated influenza illness is characterized by the abrupt onset of constitutional and respiratory signs and symptoms. Signs
PEDIATRIC INFLUENZA CLINICAL PRACTICE GUIDELINES DEFINITIONS AND BACKGROUND Uncomplicated influenza illness is characterized by the abrupt onset of constitutional and respiratory signs and symptoms. Signs
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
General History. 林陳 珠 Female 69 years old 住院期間 : ~ Chief Complaint : sudden loss of conscious 5 minutes in the morning.
 General History 林陳 珠 Female 69 years old 住院期間 : 93.5.8~93.5.15 Chief Complaint : sudden loss of conscious for 2-52 5 minutes in the morning. General History DM under regular medical control for 10 years.
General History 林陳 珠 Female 69 years old 住院期間 : 93.5.8~93.5.15 Chief Complaint : sudden loss of conscious for 2-52 5 minutes in the morning. General History DM under regular medical control for 10 years.
Diagnosis of Pneumocystis carinii
 141 Diagnosis of Pneumocystis carinii Pneumonia in Human Immunodeficiency Virus Infected Patients with Polymerase Chain Reaction: A Blinded Comparison to Standard Methods Juan Torres, 1,a Mitchell Goldman,
141 Diagnosis of Pneumocystis carinii Pneumonia in Human Immunodeficiency Virus Infected Patients with Polymerase Chain Reaction: A Blinded Comparison to Standard Methods Juan Torres, 1,a Mitchell Goldman,
Pneumocystis Pneumonia (PCP): Part 2
 NORTHWEST AIDS EDUCATION AND TRAINING CENTER Pneumocystis Pneumonia (PCP): Part 2 Brian R. Wood, MD Medical Director, NW AETC ECHO Assistant Professor of Medicine, University of Washington Presentation
NORTHWEST AIDS EDUCATION AND TRAINING CENTER Pneumocystis Pneumonia (PCP): Part 2 Brian R. Wood, MD Medical Director, NW AETC ECHO Assistant Professor of Medicine, University of Washington Presentation
Pulmonary Aspergillosis
 May 2005 Pulmonary Aspergillosis Nancy Wei, Harvard Medical School, Year III Overview Pulmonary aspergillosis background information Patient presentations Common radiographic findings for each type of
May 2005 Pulmonary Aspergillosis Nancy Wei, Harvard Medical School, Year III Overview Pulmonary aspergillosis background information Patient presentations Common radiographic findings for each type of
Opportunistic infections
 Opportunistic infections Opportunistic infections Decrease in number of CD4 lymphocytes is condition for development of opportunistic infections Risk is started, when number of CD4 lymphocytes drops to
Opportunistic infections Opportunistic infections Decrease in number of CD4 lymphocytes is condition for development of opportunistic infections Risk is started, when number of CD4 lymphocytes drops to
Bacterial pneumonia with associated pleural empyema pleural effusion
 EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
Carcinoma of the Lung
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
Avian Influenza Clinical Picture, Risk profile & Treatment
 Avian Influenza Clinical Picture, Risk profile & Treatment Jantjie Taljaard Adult ID Unit Tygerberg Academic Hospital University of Stellenbosch jjt@sun.ac.za 083 419 1452 CLINICAL PICTURE The clinical
Avian Influenza Clinical Picture, Risk profile & Treatment Jantjie Taljaard Adult ID Unit Tygerberg Academic Hospital University of Stellenbosch jjt@sun.ac.za 083 419 1452 CLINICAL PICTURE The clinical
Pneumonia. Dr. Rami M Adil Al-Hayali Assistant professor in medicine
 Pneumonia Dr. Rami M Adil Al-Hayali Assistant professor in medicine Definition Pneumonia is an acute respiratory illness caused by an infection of the lung parenchyma, associated with recently developed
Pneumonia Dr. Rami M Adil Al-Hayali Assistant professor in medicine Definition Pneumonia is an acute respiratory illness caused by an infection of the lung parenchyma, associated with recently developed
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage)
 NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage) I. Purpose The adequacy of a sputum specimen is determined
NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage) I. Purpose The adequacy of a sputum specimen is determined
The Utility of Surgical Lung Biopsy in Immunocompromised Children
 The Utility of Surgical Lung Biopsy in Immunocompromised Children Jessica A. Naiditch, MD, Katherine A. Barsness, MD, and David H. Rothstein, MD Objective To determine the utility of lung biopsy in immunocompromised
The Utility of Surgical Lung Biopsy in Immunocompromised Children Jessica A. Naiditch, MD, Katherine A. Barsness, MD, and David H. Rothstein, MD Objective To determine the utility of lung biopsy in immunocompromised
Pneumonia 2017 OMAR PIRZADA
 Pneumonia 2017 OMAR PIRZADA Pneumonia Pneumonia is common 0.5-1% of adults per year, 5-12% presenting to GP with LRTi 22-42% will be admitted to hospital Symptoms and signs Case 1 26 year old man Sudden
Pneumonia 2017 OMAR PIRZADA Pneumonia Pneumonia is common 0.5-1% of adults per year, 5-12% presenting to GP with LRTi 22-42% will be admitted to hospital Symptoms and signs Case 1 26 year old man Sudden
Opportunistic Infections BHIVA Guidelines
 Opportunistic Infections BHIVA Guidelines Mark Nelson David Dockrell Simon Edwards I have.. 1. Read all of the BHIVA guidelines 12% 2. Read some of the BHIVA guidelines in their entirety 3. Browsed some
Opportunistic Infections BHIVA Guidelines Mark Nelson David Dockrell Simon Edwards I have.. 1. Read all of the BHIVA guidelines 12% 2. Read some of the BHIVA guidelines in their entirety 3. Browsed some
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection. Masoud Mardani M.D,FIDSA
 Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules
 Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Diagnosis of Lower Respiratory Tract Infections* What We Have and What Would Be Nice. Robert P. Baughman, MD, FCCP; and Chiara E.
 Diagnosis of Lower Respiratory Tract Infections* What We Have and What Would Be Nice Robert P. Baughman, MD, FCCP; and Chiara E. Conrado, MD Study objectives: To review the various methods used to diagnose
Diagnosis of Lower Respiratory Tract Infections* What We Have and What Would Be Nice Robert P. Baughman, MD, FCCP; and Chiara E. Conrado, MD Study objectives: To review the various methods used to diagnose
Α 78-year-old female who presents with a non-resolving pneumonia: what is your diagnosis?
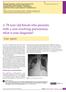 Evangelia Panagiotidou 1, Serafeim-Chrysovalantis Kotoulas 1, Maria Kilmpasani 2, Nikoleta Pastelli 2, Sofia Akritidou 1, Evangelos Chatzopoulos 1, Vasilis Bikos 1, Vasilios Bagalas 1, Katalin Fekete-Passa
Evangelia Panagiotidou 1, Serafeim-Chrysovalantis Kotoulas 1, Maria Kilmpasani 2, Nikoleta Pastelli 2, Sofia Akritidou 1, Evangelos Chatzopoulos 1, Vasilis Bikos 1, Vasilios Bagalas 1, Katalin Fekete-Passa
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Supplementary Material. Mühlethaler et al.
 Supplementary Material. Mühlethaler et al. Bronchoalveolar lavage (BAL) processing and polymerase chain reaction (PCR) methods The BAL procedure was performed following a standardized protocol by an experienced
Supplementary Material. Mühlethaler et al. Bronchoalveolar lavage (BAL) processing and polymerase chain reaction (PCR) methods The BAL procedure was performed following a standardized protocol by an experienced
Diagnostic Procedures for Pulmonary Infiltrates in the Compromised Host
 Diagnostic Procedures for Pulmonary Infiltrates in the Compromised Host Michael Douvas, MD Heme/Onc Gerald Donowitz, MD - ID Eric Davis, MD - Pulmonary Disclosure Drs. Davis, Donowitz, and Douvas do not
Diagnostic Procedures for Pulmonary Infiltrates in the Compromised Host Michael Douvas, MD Heme/Onc Gerald Donowitz, MD - ID Eric Davis, MD - Pulmonary Disclosure Drs. Davis, Donowitz, and Douvas do not
The diagnosis and treatment of cardiac rejection is
 ORIGINAL ARTICLES: CARDIOVASCULAR Routine Surveillance Endomyocardial Biopsy: Late Rejection After Heart Transplantation David A. Heimansohn, MD, Robert J. Robison, MD, John M. Paris III, MD, Robert G.
ORIGINAL ARTICLES: CARDIOVASCULAR Routine Surveillance Endomyocardial Biopsy: Late Rejection After Heart Transplantation David A. Heimansohn, MD, Robert J. Robison, MD, John M. Paris III, MD, Robert G.
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
LONG-TERM RESULTS OF CARDIAC TRANSPLANTATION IN PATIENTS OLDER THAN SIXTY YEARS
 LONG-TERM RESULTS OF CARDIAC TRANSPLANTATION IN PATIENTS OLDER THAN SIXTY YEARS Advanced age has traditionally been a contraindication to cardiac transplantation. We have, however, offered cardiac transplantation
LONG-TERM RESULTS OF CARDIAC TRANSPLANTATION IN PATIENTS OLDER THAN SIXTY YEARS Advanced age has traditionally been a contraindication to cardiac transplantation. We have, however, offered cardiac transplantation
Respiratory Pathology. Kristine Krafts, M.D.
 Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Outline. Cryptococcosis Pneumocystosis Diarrhea. Case Histories: HIV Related- Opportunistic Infections in 2015
 AU Edited: 05/06/15 Case Histories: HIV Related- Opportunistic Infections in 2015 Henry Masur, MD Clinical Professor of Medicine George Washington University School of Medicine Bethesda, Maryland Washington,
AU Edited: 05/06/15 Case Histories: HIV Related- Opportunistic Infections in 2015 Henry Masur, MD Clinical Professor of Medicine George Washington University School of Medicine Bethesda, Maryland Washington,
CASE PRESENTATION VV ECMO
 CASE PRESENTATION VV ECMO Joshua Huelster, MD Fellow in Critical Care Medicine Department of Pulmonary and Critical Care Medicine Hennepin County Medical Center Disclosure There are no conflicts of interest
CASE PRESENTATION VV ECMO Joshua Huelster, MD Fellow in Critical Care Medicine Department of Pulmonary and Critical Care Medicine Hennepin County Medical Center Disclosure There are no conflicts of interest
Antimicrobial Management of Febrile Neutropenic Sepsis
 Antimicrobial Management of Febrile Neutropenic Sepsis Written by: Dr J Joseph, Consultant Haematologist Dr K Gajee, Consultant Microbiologist Amended by: Larissa Claybourn, Antimicrobial Pharmacist Date:
Antimicrobial Management of Febrile Neutropenic Sepsis Written by: Dr J Joseph, Consultant Haematologist Dr K Gajee, Consultant Microbiologist Amended by: Larissa Claybourn, Antimicrobial Pharmacist Date:
Progression pattern of restrictive allograft syndrome after lung transplantation
 http://www.jhltonline.org FEATURED ARTICLES Progression pattern of restrictive allograft syndrome after lung transplantation Masaaki Sato, MD, PhD, a,b David M. Hwang, MD, PhD, a Thomas K. Waddell, MD,
http://www.jhltonline.org FEATURED ARTICLES Progression pattern of restrictive allograft syndrome after lung transplantation Masaaki Sato, MD, PhD, a,b David M. Hwang, MD, PhD, a Thomas K. Waddell, MD,
Nonspecific Interstitial Pneumonitis: A Common Cause of Pulmonary Disease in the Acquired Immunodeficiency Syndrome
 Nonspecific Interstitial Pneumonitis: A Common Cause of Pulmonary Disease in the Acquired Immunodeficiency Syndrome ANTHONY F. SUFFREDINI, M.D.; FREDERICK P. OGNIBENE, M.D.; ERNEST E. LACK, M.D.; J. THAYER
Nonspecific Interstitial Pneumonitis: A Common Cause of Pulmonary Disease in the Acquired Immunodeficiency Syndrome ANTHONY F. SUFFREDINI, M.D.; FREDERICK P. OGNIBENE, M.D.; ERNEST E. LACK, M.D.; J. THAYER
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ
 Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ Art of Good Cooking Good Ingredient Good donor + OK recipient Good technique Good team Good timing Good
Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ Art of Good Cooking Good Ingredient Good donor + OK recipient Good technique Good team Good timing Good
Bronchitis/Pneumonia Core Content Keith Conover, M.D., FACEP /15/02 Clinical Spectrum Chest pain, shoulder pain, neck pain, abdominal pain,
 Bronchitis/Pneumonia Core Content Keith Conover, M.D., FACEP 1.0 10/15/02 Clinical Spectrum Chest pain, shoulder pain, neck pain, abdominal pain, headache Links with smoking, pollen count, FH of asthma
Bronchitis/Pneumonia Core Content Keith Conover, M.D., FACEP 1.0 10/15/02 Clinical Spectrum Chest pain, shoulder pain, neck pain, abdominal pain, headache Links with smoking, pollen count, FH of asthma
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Five patients with AIDS in whom a lower respiratory. was wedged into the segmental bronchus that corresponded
 Thorax 1985;40: 166-170 Early experience and difficulties with bronchoalveolar lavage and transbronchial biopsy in the diagnosis of AIDS associated pneumonia in Britain CR SWINBURN, AL POZNIAK, S SUTHERLAND,
Thorax 1985;40: 166-170 Early experience and difficulties with bronchoalveolar lavage and transbronchial biopsy in the diagnosis of AIDS associated pneumonia in Britain CR SWINBURN, AL POZNIAK, S SUTHERLAND,
Advance Pathology Services, P.C Professional Drive, Suite 3 Cadillac, MI Phone: Fax:
 Advance Pathology Services, P.C. 8865 Professional Drive, Suite 3 Cadillac, MI 49601 Phone: 231-468-2346 Fax: 231-468-2349 Pathology Analysis: Pneumonia and Pulmonary Hemorrhage Cause Death; Clinically
Advance Pathology Services, P.C. 8865 Professional Drive, Suite 3 Cadillac, MI 49601 Phone: 231-468-2346 Fax: 231-468-2349 Pathology Analysis: Pneumonia and Pulmonary Hemorrhage Cause Death; Clinically
Skin Pathway Group Alemtuzumab in Cutaneous Lymphoma
 Skin Pathway Group Alemtuzumab in Cutaneous Lymphoma Indication: Treatment of patients with Cutaneous Lymphoma (Unlicensed use) Disease control prior to Reduced Intensity Conditioning Stem Cell Transplant
Skin Pathway Group Alemtuzumab in Cutaneous Lymphoma Indication: Treatment of patients with Cutaneous Lymphoma (Unlicensed use) Disease control prior to Reduced Intensity Conditioning Stem Cell Transplant
ESCMID Online Lecture Library. by author. CASE PRESENTATION ECCMID clinical grand round May Anat Stern, MD Rambam medical center Haifa, Israel
 CASE PRESENTATION ECCMID clinical grand round May 2014 Anat Stern, MD Rambam medical center Haifa, Israel An 18 years old Female, from Ukraine, diagnosed with acute lymphoblastic leukemia (ALL) in 2003.
CASE PRESENTATION ECCMID clinical grand round May 2014 Anat Stern, MD Rambam medical center Haifa, Israel An 18 years old Female, from Ukraine, diagnosed with acute lymphoblastic leukemia (ALL) in 2003.
Chapter 8. Other Important Tests and Procedures. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
PNEUMONIA IN A PRESUMED IMMUNOCOMPETENT PATIENT
 Dr Marie Bruyneel and Deborah Konopnicki BVIKM/SBMIC November 8th, 2012 PNEUMONIA IN A PRESUMED IMMUNOCOMPETENT PATIENT Men, 54 years Emergency room on end october 2009 Sent by his family doctor for Influenza
Dr Marie Bruyneel and Deborah Konopnicki BVIKM/SBMIC November 8th, 2012 PNEUMONIA IN A PRESUMED IMMUNOCOMPETENT PATIENT Men, 54 years Emergency room on end october 2009 Sent by his family doctor for Influenza
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference. Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2
 June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
Keeping Patients Off the Vent: Bilevel, HFNC, Neither?
 Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
Dr Marie Bruyneel and Deborah Konopnicki. BVIKM/SBMIC November 8th, 2012
 Dr Marie Bruyneel and Deborah Konopnicki BVIKM/SBMIC November 8th, 2012 Men, 54 years Emergency room on end october 2009 Sent by his family doctor for Influenza A H1N1? Viral syndrom, cough, fever 39 (7j)
Dr Marie Bruyneel and Deborah Konopnicki BVIKM/SBMIC November 8th, 2012 Men, 54 years Emergency room on end october 2009 Sent by his family doctor for Influenza A H1N1? Viral syndrom, cough, fever 39 (7j)
ECMM Excellence Centers Quality Audit
 ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
UPDATE IN HOSPITAL MEDICINE
 UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
