Nonspecific Interstitial Pneumonitis: A Common Cause of Pulmonary Disease in the Acquired Immunodeficiency Syndrome
|
|
|
- Solomon Jordan
- 5 years ago
- Views:
Transcription
1 Nonspecific Interstitial Pneumonitis: A Common Cause of Pulmonary Disease in the Acquired Immunodeficiency Syndrome ANTHONY F. SUFFREDINI, M.D.; FREDERICK P. OGNIBENE, M.D.; ERNEST E. LACK, M.D.; J. THAYER SIMMONS, M.D.; MATTHEW BRENNER, M.D.; VEE J. GILL, Ph.D.; H. CLIFFORD LANE, M.D.; ANTHONY S. FAUCI, M.D.; JOSEPH E. PARRILLO, M.D.; HENRY MASUR, M.D.; and JAMES H. SHELHAMER, M.D.; Bethesda, Maryland During a 4.4-year period, nonspecific interstitial pneumonitis was seen in 4 of 0 (38%) patients with the acquired immunodeficiency syndrome and accounted for 32% (48/52) of all episodes of clinical pneumonitis. Diffuse alveolar damage was typically a feature of nonspecific interstitial pneumonitis, but neither lung nor bronchoalveolar lavage detected a pathogen. Of these 4 patients, 3 had no associated pulmonary tumor and had not been exposed to pulmonary toxins, whereas 28 patients had either concurrent pulmonary Kaposi sarcoma, previous experimental therapies, or a history of Pneumocystis pneumonia or drug abuse. Of these 4, 23 had normal chest radiographs. The clinical features of patients with nonspecific interstitial pneumonitis were similar to those of patients with Pneumocystis pneumonia, although histologic findings showed less severe alveolar damage in patients with nonspecific interstitial pneumonitis (p< 0.00). Pathologic evaluation and clinical follow-up suggest that many clinical episodes of pneumonitis in patients with the acquired immunodeficiency syndrome are due to nonspecific interstitial pneumonitis of unknown cause. PULMONARY INFECTION is the most commonly recognized life-threatening disorder in patients with the acquired immunodeficiency syndrome (AIDS), and Pneumocystis carinii is the commonest cause of pneumonia in these patients. Sixty-five percent to eighty percent of patients with AIDS will have at least one episode of Pneumocystis carinii pneumonia (, 2). Other causes of dyspnea, cough, or abnormalities detected through radiography are less common and include cytomegalovirus pneumonia, Kaposi sarcoma, and occasionally fungal or mycobacterial pneumonia. Previous reports suggest that in almost all episodes of pulmonary dysfunction in patients with AIDS, a specific cause can be identified if adequate samples of lung tissue are obtained (, 3). After reviewing the records of 52 episodes of clinical pneumonitis in 0 patients with AIDS, we noted that adequate lung histopathologic specimens frequently showed a nonspecific interstitial inflammatory process but failed to identify a causative infection or tumor. Thirty-two percent of all episodes of pneumonitis in this series appeared to be caused by nonspecific interstitial pneumonitis. Many of these patients had not had previous From the Critical Care Medicine Department, Laboratory of Microbiology, and Radiology Department, Clinical Center, National Institute of Allergy and Infectious Diseases; and Laboratory of Pathology, National Cancer Institute; National Institutes of Health; Bethesda, Maryland. pulmonary infections or a history of drug abuse or exposure to pulmonary toxins that might have explained these findings. Experience with these 52 episodes of pneumonitis suggest that nonspecific interstitial pneumonitis is frequently found in patients with AIDS who have cough, dyspnea, or radiographic evidence of abnormalities. The high frequency of nonspecific interstitial pneumonitis as the cause of either the initial episodes of pneumonitis in patients known to have AIDS (based on extrapulmonary disorders) or as a cause of pneumonitis in patients with a history of other AIDS-related pulmonary disorders has important implications regarding further diagnostic evaluation and therapy. The incidence of interstitial pneumonitis needs to be considered when deciding whether to do an open lung if the results of a are nondiagnostic and when evaluating the appropriateness of empiric antipneumocystis therapy for all patients with AIDS who have pneumonitis. We describe the clinical and radiologic features of nonspecific interstitial pneumonitis and show that this disease is a frequent but usually self-limited cause of pulmonary dysfunction in patients with AIDS. Methods PATIENT POPULATION The histopathologic and microbiologic data obtained from all patients with AIDS who had diagnostic pulmonary procedures at the Clinical Center, National Institutes of Health, between December 982 and May 986 were reviewed. The clinical history, signs, and symptoms of pulmonary disease (fever, cough, sputum production, dyspnea) were recorded for each patient at the time of the procedures. The results of arterial blood gas determinations done no more than hour before each diagnostic procedure were reviewed, and the alveolar-arterial oxygen gradients were calculated. An episode of pneumonitis was defined as the new appearance of any combination of abnormal pulmonary symptoms, signs, or radiographic findings that, in the opinion of one or more of the authors, merited bronchoscope examination. Initial episodes of pneumonitis were those occurring in patients who had not previously had an episode of pneumonitis while being followed for AIDS, and subsequent episodes were those occurring in patients who developed pneumonitis after having had a previously reported AIDS-related episode of the disease. DIAGNOSTIC PROCEDURES Any patient with AIDS who had persistent pulmonary symptoms or an abnormal chest radiograph was referred to the au- Annals of Internal Medicine. 987;07: American College of Physicians 7
2 thors, either before or within 48 hours of the initiation of antimicrobial therapy. Bronchoscopy consisting of bronchoalveolar lung biopsies was done as previously described (4). Bronchoalveolar lavage alone was done if a lung was contraindicated because of the risk of bleeding (platelet counts less than 50 X 0VL unresponsive to transfusion therapy or prothrombin time greater than 5 seconds) or hypoxemia (partial pressure of oxygen less than 00 mm Hg with an inspired oxygen fraction of.0). Transbronchial lung biopsies were done under fluoroscopic guidance, and a mean of four specimens per patient was obtained, with each sample averaging 0. mm to 0.2 mm in largest dimension. A specimen was arbitrarily considered adequate for histologic study if it showed at least 50 alveolar spaces. A nondiagnostic procedure was defined as either a procedure consisting of bronchoalveolar lavage but not lung (because of contraindications to this procedure) that provided a negative microbiologic diagnosis or one that yielded a specimen showing less than 50 alveoli available for histopathologic review. If the bronchoalveolar lavage or lung biopsies or both were nondiagnostic or could not be done and the patient showed substantial clinical deterioration, then an open lung was done. Empiric therapy was never continued for more than 48 hours unless a bronchoscopy or open lung was done. Routine microbiologic evaluation of concentrated lavage included a battery of stains (Gram's, modified toluidine blue for Pneumocystis carinii, wet mount for fungus, fluorochrome for acid-fast bacilli, and direct fluorescent antibody for Legionella) and cultures (routine bacterial, mycobacterial, and fungal cultures and charcoal yeast extract for Legionella). Special stains done routinely on each lung specimen included the Giemsa, periodic acid-schiff, Brown-Brenn, Fite, Gomori's methenamine-silver, and toluidine blue stains (4, 5). RADIOGRAPHIC ANALYSIS AND GALLIUM SCANS All chest radiographs obtained between 24 and 72 hours before the diagnostic procedures were assessed retrospectively as a group by a radiologist who was blinded to the patients' clinical data. The pattern, distribution, and symmetry of the lung infiltrates were graded according to the following scale:, subtle increased perihilar markings; 2, interstitial markings more prominent and extending laterally without evidence of alveolar disease; 3, gross interstitial disease with early alveolar changes; and 4, extensive interstitial-alveolar disease. Gallium 67 citrate scans obtained in patients with nonspecific interstitial pneumonitis within 7 days of their bronchoscopies were reviewed. The scans were graded on a scale of 0 (normal) to 5 (pulmonary uptake greater than liver) (6). HISTOPATHOLOGIC EVALUATION Coded lung histopathologic specimens were reviewed as a group by one pathologist who was blinded to the patients' clinical data. The specimens were graded according to the severity of diffuse alveolar damage on a scale of 0 to 3. A score of 0 indicated no diffuse alveolar damage, and a score of 3, the severest tissue injury. The following five characteristics of tissue injury were each scored individually: alveolar edema and fibrin deposition, hyaline membrane formation, interstitial inflammation, loose interstitial fibrosis, and dense interstitial fibrosis. A total score for each was determined by adding the sum of the scores for each of these five features. In addition, other features of tissue damage, including alveolar macrophages, alveolar hemorrhage, alveolar pneumonitis with neutrophilic infiltration, and interstitial lymphoid aggregates, were each graded on a similar scale of 0 to 3. Nonspecific interstitial pneumonitis was characterized by histologic evidence of diffuse alveolar damage of varying degrees in association with increased numbers of macrophages, alveolar hemorrhage, or lymphoid aggregates and no associated microbial pathogens on the bronchoalveolar lavage stains or culture and on histopathologic tissue sections. Pneumocystis carinii pneumonia was indicated by the presence of at least one cluster of Pneumocystis cysts on the modified toluidine blue stain of the bronchoalveolar lavage pellet or at least one cluster of cysts or both on sections of lung tissue stained with either methenamine silver or toluidine blue. Criteria for diagnosing Kaposi sarcoma included the presence of characteristic strands of spindle cells, extravasated erythrocytes, and hemosiderin deposits on sections of uncrushed pulmonary tissue stained with hematoxylin and eosin (7). Cytomegalovirus pneumonia was defined by the presence of at least one characteristic intranuclear inclusion body in association with some feature of interstitial inflammation. In this study, positive virus cultures of lavage fluid or lung tissue were not considered definitive diagnostic criteria for cytomegalovirus pneumonia (8). Mycobacterial pneumonia was defined by the presence of mycobacterial rods on Fite stain, in association with varying degrees of interstitial inflammation or the presence of aggregates of epithelioid histiocytes, with a positive culture for mycobacteria obtained from bronchoalveolar lavage fluid or lung tissue. Cryptococcus neoformans pneumonia was characterized by the background appearance of interstitial inflammation with encapsulated fungal organisms on periodic acid-schiff or Gomori's methenamine-silver stain or a positive culture for Cryptococcus obtained from the bronchoalveolar lavage fluid or lung tissue (9). STATISTICAL ANALYSIS Descriptive statistics are expressed as mean it SE, and the Student's Mest was used to compare the means between groups. Results We evaluated 04 men and 6 women, ages 23 to 56 years (mean, 36 ± 0.8); 03 men were homosexuals or bisexuals, 2 women and man had a history of transfusion-related AIDS, 2 women had a history of intravenous drug abuse, and 2 women had a history of sexual contact with a bisexual partner or an intravenous drug abuser. All patients were referred to the National Institutes of Health for participation in research protocols involving antiretroviral therapy or treatment for an opportunistic infection or Kaposi sarcoma. The diagnostic procedures used in evaluating the episodes of pneumonitis consisted of bronchoalveolar in 02 episodes, bronchoalveolar lavage alone in 27, bronchoalveolar lavage or either alone or together followed by open lung in 9, or open lung alone in 4. The causes of the initial and subsequent episodes of pneumonitis in the 0 patients are summarized in Table. Infectious and neoplastic manifestations of some of these patients have been previously described (4, 7, 0, ). Nonspecific interstitial pneumonitis occurred in the absence of any recognizable infectious agent in 4 of 0 (38%) patients and accounted for 48 of 52 (32%) episodes of pneumonitis. The data for patients with nonspecific interstitial pneumonitis alone or in association with other pulmonary disorders are shown in Table 2. These patients were divided into those with nonspecific interstitial pneumonitis unassociated with any concurrent neoplasm or pulmonary infection and those with nonspecific interstitial pneumonitis conceivably related to previous opportunistic infections, experimental therapy, or Kaposi sarcoma. All of the patients with nonspecific interstitial pneumonitis (4 patients, 48 episodes) had at least one pulmonary symptom. Cough, the most frequent symptom, 8 July 987 Annals of Internal Medicine Volume 07 Number
3 was documented in 28 of 32 cases, and a temperature greater than 38 C, in 22 of 34 cases. Gallium citrate scans obtained in 7 patients with interstitial pneumonitis were abnormal in 4 (ranging from grades to 4) and normal in 3. The clinical and histopathologic features of the most well-delineated cases of nonspecific interstitial pneumonitis were carefully evaluated (Table 3). Of 3 patients who had had no previous episode of pneumonitis, 2 had presented with extrapulmonary Kaposi sarcoma, and, with central nervous system toxoplasmosis as the initial manifestation of AIDS. When the symptoms of these patients were reviewed, 9 had a nonproductive cough, 3 were dyspneic with exertion, and was asymptomatic. Seven chest radiographs were normal and seven were abnormal, with grades and 2 interstitial infiltrates or diffuse nodules. One radiograph was unavailable for review. In this carefully delineated group, nonspecific interstitial pneumonitis was documented by bronchoalveolar lavage and biopsies in 2 patients and by open lung in. Three patients subsequently had open lung biopsies ( to 0 days after their initial bronchoscopies) that confirmed the initial diagnosis of interstitial pneumonitis in each episode. These patients were followed for 4 to 52 weeks (mean, 20). None of the patients received empiric antibiotic therapy. Patients and 2 subsequently developed Pneumocystis pneumonia (one with concomitant cytomegalovirus pneumonia) 26 and 7 weeks later, respectively. Four additional patients had other subsequent symptomatic pulmonary processes, but bronchoscopic procedures failed to identify a cause; had an open lung 42 weeks after the initial episode of pneumonia that showed Kaposi sarcoma and nonspecific interstitial pneumonitis. Ultimately, of these 3 patients, 7 died due to an infectious or neoplastic process, 4 were lost to follow-up, and 2 are still being followed clinically. Table. Causes of Pneu imonitis in 0 Pa tients v with the Acquired Immunodeficiency Syndrome* Epi sodes Cause Initial Subs equent Total < n( '%) 52 (47) 0 (24) 62 (4) Nonspecific Pneumocystis interstitial pneumonitis 3 (28) 0 (24) 4 (27) Nondiagnostic 0 (9) 9 (22) 9 (2) Kaposi sarcoma n (6) 3 (7) 0 (6) Pneumocystis and cytomegalovirus 3 (3) (2) 4 (3) Cytomegalovirus 2 (2) 3 (7) 5 (3) Bacteria 3 (3) 3 (7) 6 (4) Mycobacteria 2 (2) 2 (5) 4 (3) Cryptococcus 0 (0) (2) Total 0(00) 42(00) () 52(00) * Bronchoalveolar lavage alor le yielded the diaj mosis for seven cases of pneualveolar lavage mocystis pneumonia and 2 cases of bacterial pneu monia; broncho and or op en lung yi elded the diagn osis for the remaining episodes. t Bronchoalveolar lavage don e alone because o f contraindicatic >n to in 7 patients; in 2 patients, specimens were in tadequate. X Concurrent Pneumocystis (: I patient), Crypto coccus ( patie nt), Legionella ( patient), and interstitial pneu monitis (all 7 pati ents). Table 2. Frequency of Association with Possible Causative Processes in Patients with the Acquired Immunodeficiency Syndrome Who Have Nonspecific Interstitial Pneumonitis Associated Pulmonary Disorder Patients Episodes None recognized Concurrent pulmonary Kaposi sarcoma Previous experimental therapy or drug abuse Total n (%) n/(%) 3 (32) 5 (3) 7 (7) 8 (7) 2 (5) 25 (52) 4(00) 48(00) The absence of early pulmonary deterioration during the patients' subsequent clinical courses suggests that bronchoscopy had not failed to detect an opportunistic infection. Patient 4 (Table 3) may have had subclinical pulmonary Kaposi sarcoma on his initial presentation, but this condition was not detected by the initial open lung and was thus not extensive enough to cause diffuse pulmonary dysfunction. In addition to the 3 patients who appeared to have nonspecific interstitial pneumonitis unassociated with an identifiable cause of pneumonitis, there were 28 patients who had presumably the same nonspecific interstitial pneumonitis syndrome, although one or more factors could not be excluded as a possible cause of their episodes of pneumonitis. Nineteen of these patients had received experimental drugs (suramin, alpha interferon, interleukin-2, heteropolyanion tungsten [Rhome-Poulenc, Montreal, Canada]) that are not known to cause interstitial pneumonitis but could have conceivably contributed to this condition. Nine patients were treated with chemotherapy regimens, including bleomycin, for Kaposi sarcoma. Five patients had a history of Pneumocystis pneumonia weeks before the episode of nonspecific interstitial pneumonitis. Two patients were intravenous drug users. Of these 28 patients with interstitial pneumonitis, 6 had open lung biopsies and had an autopsy within 2 weeks of the initial diagnosis; these 7 patients were found to have pulmonary Kaposi sarcoma in addition to nonspecific interstitial pneumonitis. The radiographic and histopathologic findings and the alveolar-arterial oxygen gradients of the patients with interstitial pneumonitis are compared with those of the patients with Pneumocystis pneumonia in Table 4. Twentyone patients who had follow-up bronchoscopies after an initial episode of Pneumocystis pneumonia are included in this comparison. These patients had one to three sequential bronchoscopies consisting of bronchoalveolar lavage and biopsies a mean of weeks after antipneumocystis therapy was initiated. These follow-up bronchoscopic procedures were done for research purposes to show the histologic resolution of the Pneumocystis infection. All 2 patients showed residual nonspecific interstitial pneumonitis on the follow-up lung biopsies, despite histopathologic clearance of the Pneumocystis cysts. The radiographic findings in the patients with nonspecific interstitial pneumonitis of unknown origin showed generally less serious abnormalities than those in the patients with Pneumocystis pneumonia. More than 50% of Suffredini et al. Nonspecific Interstitial Pneumonitis 9
4 Table 3. Clinical Course of 3 Patients with the Acquired Immunodeficiency Syndrome Who Have Nonspecific Interstitial Pneumonitis and No Initial Associated Pulmonary Disorder Patient Diagnostic Procedure Diagnosis of For Initial Episode For Confirmation For Subsequent Episodes Subsequent Episodes Outcome Bronchoalveolar Open lung Bronchoalveolar lavage Pneumocystis and Pulmonary Kaposi * (8) and cytomegalovirus sarcoma and (26) t pneumonia cytomegalovirus pneumonia at autopsy (29)t 2 Bronchoalveolar Open lung Bronchoalveolar lavage Pneumocystis Death due to progressive () and pneumonia Kaposi sarcoma (26) (7) 3 Bronchoalveolar Open lung Nondiagnostic Progressive pulmonary (0) bronchoalveolar infiltrates of unknown lavage (20) origin, lost to follow up (52) 4 Open lung Bronchoalveolar lavage Nonspecific Death due to pulmonary with interstitial Kaposi sarcoma (45) (40) Open lung (42) pneumonitis Kaposi sarcoma and nonspecific interstitial pneumonitis 5 Bronchoalveolar Bronchoalveolar lavage Nonspecific Death due to with interstitial Toxoplasma gondii, (2) pneumonitis nonspecific interstitial pneumonitis at autopsy (6) 6 Bronchoalveolar Bronchoalveolar lavage Nonspecific Death due to fungal and and interstitial cytomegalovirus (6) pneumonitis pneumonia at autopsy (20) 7 Bronchoalveolar 8 Bronchoalveolar 9 Bronchoalveolar 0 Bronchoalveolar Bronchoalveolar 2 Bronchoalveolar 3 Bronchoalveolar * Numbers in parentheses indicate number of days between diagnostic procedure for initial episode of disease and confirmatory procedure. t Numbers in parentheses indicate number of weeks between initial episode and subsequent episode of disease. % Numl Ders in parentheses indicate number of weeks between i nitial episode of disease and outcome. Previous manifestation of AIDS in Patient 5 was opportunistic infection; in all others, Kaposi sarcoma. Chest radiograph clear, cough persists, lost to follow-up (9) Chest radiograph clear, lost to follow-up (5) Lost to follow-up (4) Chest radiograph clear (42) Death due to progressive Kaposi sarcoma (6) Death due to T. gondii, chest radiograph clear (6) Chest radiograph clear, cough persists (6) the patients with nonspecific interstitial pneumonitis had normal radiographs. All of the patients at the time of diagnosis of Kaposi sarcoma of the lung had diffusely abnormal radiographs, although one had presented initially with a normal chest radiograph. Twenty-four percent of the patients with Pneumocystis pneumonia had 0 July 987 Annals of Internal Medicine Volume 07 Number
5 Table 4. Radiographic, Pathologic, and Arterial Blood Gas Findings in Patient Groups with Nonspecific Interstitial Pneumonitis or Pneumocystis carinii Pneumonia Patient Group Radiographic Finding Radiologic and Laboratory Findings Normal Abnormal Diffuse Alveolar Damage Score* Alveolar-Arterial Gradient Interstitial pneumonitis alone Interstitial pneumonitis with Kaposi sarcoma Interstitial pneumonitis with experimental therapy or drug abuse Interstitial pneumonitis after P. carinii pneumonia P. carinii pneumonia n n mm Hg ±0.3f 3.75 ± J 3.45 ± ± ± 4 36 ± 7 34 ± f 37 ± 5 * Determined by adding the sum of the scores for the following five features ui :; ^jury: alveolar edema and fibrin deposition; hyaline membrane formation; interstitial inflammation; loose interstitial fibrosis; and dense interstitial fibrosis. Each feature was graded according to the severity of damage on a scale of 0 to 3; 0 = no damage; 3 = severest damage. tp < 0.00 compared with P. carinii pneumonia. %p < 0.0 compared with P. carinii pneumonia. p < 0.05 compared with P. carinii pneumonia. normal chest radiographs and the remainder had radiographs showing varying degrees of diffuse or unilateral infiltrates. The diffuse alveolar damage score was significantly less in patients with nonspecific interstitial pneumonitis unassociated with infection or tumor than in patients with Pneumocystis pneumonia ( compared with , p < 0.00). However, the score was not different from the score in patients with nonspecific interstitial pneumonitis associated with Kaposi sarcoma or experimental therapies or the score obtained after resolution of Pneumocystis pneumonia. The histopathologic findings in patients with nonspecific interstitial pneumonitis and no associated pulmonary disorder showed interstitial inflammation with lymphocytes and plasma cells and moderate (grades to 2) degrees of edema and fibrin deposition (Figure ). Hyaline membranes, which indicate endothelial-epithelial barrier damage, were present in three patients, and interstitial lymphoid aggregates in three. None of the biopsies or open lung specimens obtained from patients with nonspecific interstitial pneumonitis showed loose or dense fibrosis. In contrast, specimens showed fibroproliferative changes in three of seven patients with nonspecific interstitial pneumonitis and pulmonary Kaposi sarcoma, in 4 of 2 patients with nonspecific interstitial pneumonitis and a history of experimental therapy or drug abuse, in 2 of 2 patients after resolution of Pneumocystis pneumonitis, and in 27 of 60 patients with acute Pneumocystis pneumonia. All patients showed varying degrees of alveolar lining cell hyperplasia and alveolar septal thickening. experimental drug therapies, or chemotherapy. None of these conditions except chemotherapy has been demonstrated to lead to the development of nonspecific interstitial pneumonitis. Clinical follow-up of patients who had had episodes of nonspecific interstitial pneumonitis of unknown origin Discussion Histologic evaluation and clinical follow-up of 52 episodes of pneumonitis in 0 patients with AIDS showed that 32% of the episodes were due to nonspecific interstitial pneumonitis that occurred in the absence of any identifiable infectious pulmonary pathogen. Thirteen of fortyone episodes occurred in patients who had no tumors or exposure to pulmonary toxins and the remaining 28 in patients who had either concurrent pulmonary Kaposi sarcoma, a history of Pneumocystis pneumonia, previous Figure. Transbronchial lung specimen showing characteristic features of nonspecific interstitial pneumonitis. In the field's middle portion, the pulmonary parenchyma shows moderate interstitial inflammation (2 + ) with mononuclear cells in the perivascular area and the lung interstitium. Interstitial edema is noted in the top and bottom left portions of the field. (Hematoxylin and eosin; original magnification, x 220.) Suffredini et al. Nonspecific Interstitial Pneumonitis
6 showed that several developed cytomegalovirus and Pneumocystis pneumonia weeks or months later that appeared as discrete clinical events after the nonspecific interstitial pneumonitis had resolved or stabilized. Histopathologic evaluation and clinical follow-up of these cases suggested that many of the episodes of pneumonitis indicated by clinical and radiologic findings were nonspecific interstitial pneumonitis of unknown cause. The clinical presentation of nonspecific interstitial pneumonitis was quite diverse and indistinguishable from that of identifiable opportunistic infections such as Pneumocystis pneumonia. Most patients presented with fever, cough, and dyspnea that were usually but not invariably mild. Fifty percent of the radiographs and several of the gallium citrate scans were normal. Arterial blood gas analysis showed mild to moderate widening of the alveolar-arterial oxygen gradient. The lung specimens of all of the patients with interstitial pneumonitis showed some histologic abnormalities, including varying degrees of edema, fibrin deposition, and interstitial inflammation with lymphocytes and plasma cells, regardless of the patients' symptoms and chest radiograph results. The inflammatory response was not as severe as that seen with Pneumocystis pneumonia when lung histology was assessed in a blinded fashion. No distinguishing features were apparent that differentiated this interstitial pneumonitis from the nonspecific interstitial pneumonitis that is found in up to 40% of patients who have cancer or have received organ transplants evaluated for diffuse pulmonary infiltrates with biopsies (2, 3). The entity associated with these patients is presumably related to drug toxicities (usually chemotherapeutic agents), radiation therapy effects, oxygen toxicity, occult viral infection, or to the underlying immunosuppressive disease itself (3). None of the patients described in Table 3 had been exposed to any of these pulmonary toxic agents. Our patients with nonspecific interstitial pneumonitis who had had a history of Pneumocystis or previous drug therapy or chemotherapy were evaluated as a separate group. We suspect that some of these patients had AIDSrelated nonspecific interstitial pneumonitis, yet we could not categorically dissociate the potential effect of their previous drug therapy on pulmonary abnormalities. Although bleomycin (used as part of the multidrug chemotherapy regimen for Kaposi sarcoma) has clearly been associated with interstitial pneumonitis in immunocompromised patients, interferon, interleukin-2, heteropolyanion tungsten, or suramin, are not known to have toxic effects on the pulmonary system (3). The interstitial pneumonitis that occurred in patients with concomitant pulmonary Kaposi sarcoma may have been a host response to the tumor or a parallel unrelated process. The cause of nonspecific interstitial pneumonitis in this series could not be determined. The failure of the procedures to yield a diagnosis of opportunistic infections did not likely account for the frequent occurrence of interstitial pneumonitis in our patients, because no patient developed pneumonitis due to identifiable pathogens in the several months after the diagnosis of nonspecific interstitial pneumonitis. The diagnosis of cytomegalovirus pneumonia was limited in our study to those patients whose histologic specimens showed diffuse alveolar damage and characteristic inclusion bodies. Conceivably, either cytomegalovirus could cause pneumonitis in the absence of inclusion bodies, or the sampling techniques that are clinically used could have failed to detect the focal clusters of infected cells. Such a possibility is difficult to prove or disprove. Nonspecific interstitial pneumonitis could also conceivably be caused by human immunodeficiency virus itself, Epstein-Barr virus, other viruses, or noninfectious environmental or therapyassociated toxins. In-situ hybridization studies in the cases of 0 patients included in this analysis failed to show evidence of human immunodeficiency virus genomes (Koenig and associates. Personal communication). Whether nonspecific pneumonitis is caused by the same process that causes inflammatory changes in the myocardium, brain, lymph nodes, spleen, bowel, and other organs in patients with AIDS is, therefore, unknown. Previous reports have described interstitial pneumonitis in patients with AIDS (4-6). Repeated pulmonary infections, drug abuse, or immune complexes were thought to be involved in the pathogenesis of the diffuse alveolar damage. However, 3 of our patients with nonspecific interstitial pneumonitis of unknown cause had no pulmonary opportunistic infections or history of toxin exposure and were not treated with corticosteroids (Table 3). Nonspecific interstitial pneumonitis, in the absence of an identifiable infection, is a common cause of pulmonary symptoms and abnormalities detected on chest radiographs in patients with AIDS. The clinical relevance of this form of interstitial pneumonitis is the similarity of its clinical presentation to that of pulmonary opportunistic infections, especially Pneumocystis carinii pneumonia. Furthermore, the frequent occurrence of nonspecific interstitial pneumonitis in patients with AIDS who have pulmonary dysfunction underscores the need for identifying specific pathogens before initiating potentially toxic antimicrobial therapy. Nonspecific interstitial pneumonitis usually resolves or stabilizes without specific therapy, although subsequent episodes may occur. Its frequent occurrence suggests that it may be a chronic, indolent source of lung injury in patients with AIDS and may contribute to their pulmonary dysfunction. We do not know whether nonspecific interstitial pneumonitis relates in any way to a patient's predisposition to other pulmonary infections or severer acute lung injury. How frequently clinicians will report nonspecific interstitial pneumonitis will depend on the nature of the population of patients with AIDS seen at their hospitals and their clinical threshold for doing lung biopsies. When bronchoalveolar biopsies fail to detect likely etiologic agents in patients with AIDS whose chest radiographs show interstitial disease, clinicians need to recognize that open lung biopsies are not invariably indicated. Further epidemiologic and microbiologic studies are needed to define the cause of this syndrome that may, in fact, be the histopathologic manifes- 2 July 987 Annals of Internal Medicine Volume 07 Number
7 tations of several diverse and unrelated processes. Requests for reprints should be addressed to Anthony F. Suffredeni, M.D.; Critical Care Medicine Department, Room 0-D-48, Clinical Center, National Institutes of Health; Bethesda, MD References. MURRAY JF, FELTON CP, GARAY SM, et al. Pulmonary complications of the acquired immunodeficiency syndrome: report of a National Heart, Lung, and Blood Institute workshop. N Engl J Med. 984;30: CENTERS FOR DISEASE CONTROL. Update: acquired immunodeficiency syndrome United States. MMWR. 986;35: BROADDUS C, DAKE MD, STULBARG MS, et al. Bronchoalveolar lavage and for the diagnosis of pulmonary infections in the acquired immunodeficiency syndrome. Ann Intern Med. 985;02: OGNIBENE FP, SHELHAMER J, GILL V, et al. The diagnosis of Pneumocystis carinii pneumonia in patients with the acquired immunodeficiency syndrome using subsegmental bronchoalveolar lavage. Am Rev Respir Dis. 984;29: GOSEY LL, HOWARD RM, WITEBSKY FG, et al. Advantages of a modified toluidine blue O stain and bronchoalveolar lavage for the diagnosis of Pneumocystis carinii pneumonia. / Clin Microbiol. 985;22: WOOLFENDEN JM, CARRASQUILLO JA, LARSON SM, et al. Acquired immunodeficiency syndrome: Ga-67 citrate imaging. Radiology. 987;62: OGNIBENE FP, STEIS RG, MACHER AM, et al. Kaposi's sarcoma causing pulmonary infiltrates and respiratory failure in the acquired immunodeficiency syndrome. Ann Intern Med. 985;02: CRAIGHEAD, JE. Pulmonary cytomegalovirus infection in the adult. Am J Pathol. 97;63: KATZENSTEIN A-LA, ASKIN FB. Surgical Pathology of Non-neoplastic Lung Disease. Philadelphia: W. B. Saunders Company; 982: KOVACS J A, HIEMENZ JW, MACHER AM, et al. Pneumocystis carinii pneumonia: a comparison between patients with the acquired immunodeficiency syndrome and patients with other immunodeficiencies. Ann Intern Med. 984;00: SHELHAMER JH, OGNIBENE FP, MACHER AM, et al. Persistence of Pneumocystis carinii in lung tissue of acquired immunodeficiency syndrome patients treated for Pneumocystis pneumonia. Am Rev Respir Dis. 984;30: KATZENSTEIN AA, ASKIN FB. Interpretation and significance of pathologic findings in lung. Am J Surg Pathol. 980;4: NASH G. Pathologic features of the lung in the immunocompromised host. Hum Pathol. 982;3: STOVER DE, WHITE DA, ROMANO PA, GELLENE RA, ROBESON WA. Spectrum of pulmonary diseases associated with the acquired immune deficiency syndrome. Am J Med. 985;78: RAMASWAMY G, JAGADHA V, TCHERTKOFF V. Diffuse alveolar damage and interstitial fibrosis in acquired immunodeficiency syndrome patients without concurrent pulmonary infection. Arch Pathol Lab Med. 985;09: BARRIO JL, HARCUP C, BAIER HJ, PITCHENIK AE. Value of repeat fiberoptic bronchoscopies and significance of nondiagnostic bronchoscopic results in patients with the acquired immunodeficiency syndrome. Am Rev Respir Dis. 987;35: Annals of Internal Medicine. 987;07: American College of Physicians \ 3
Pneumocystis. Pneumocystis BIOL Summer Introduction. Mycology. Introduction (cont.) Introduction (cont.)
 Introduction Pneumocystis Disclaimer: This lecture slide presentation is intended solely for educational purposes. Many of the images contained herein are the property of the original owner, as indicated
Introduction Pneumocystis Disclaimer: This lecture slide presentation is intended solely for educational purposes. Many of the images contained herein are the property of the original owner, as indicated
Pneumocystis carinii Pneumonia: Diagnosis
 THE JOURNAL OF INFECTIOUS DISEASES VOL. 157, NO.6. JUNE 1988 1988 by The University of Chicago. All rights reserved. 0022-1899/88/5706-0001$01.00 AIDS COMMENTARY Pneumocystis carinii Pneumonia: Diagnosis
THE JOURNAL OF INFECTIOUS DISEASES VOL. 157, NO.6. JUNE 1988 1988 by The University of Chicago. All rights reserved. 0022-1899/88/5706-0001$01.00 AIDS COMMENTARY Pneumocystis carinii Pneumonia: Diagnosis
11/19/2012. The spectrum of pulmonary diseases in HIV-infected persons is broad.
 The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma
 July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
Chapter 22. Pulmonary Infections
 Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia)
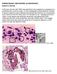 PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia) A 46-year-old man with AIDS was admitted to the hospital for complaints of a persisting fever and dry cough. A chest radiograph showed bilateral
PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia) A 46-year-old man with AIDS was admitted to the hospital for complaints of a persisting fever and dry cough. A chest radiograph showed bilateral
ARDS during Neutropenia. D Mokart DAR IPC GRRRRROH 2010
 ARDS during Neutropenia D Mokart DAR IPC GRRRRROH 2010 Definitions Neutropenia is a decrease in circulating neutrophil white cells in the peripheral blood. neutrophil count of 1,000 1,500 cells/ml = mild
ARDS during Neutropenia D Mokart DAR IPC GRRRRROH 2010 Definitions Neutropenia is a decrease in circulating neutrophil white cells in the peripheral blood. neutrophil count of 1,000 1,500 cells/ml = mild
HYPERSENSITIVITY PNEUMONITIS
 HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
Pneumocystis Pneumonia. Dr. Pradeep kumar II yr Pulmonary Medicine
 Pneumocystis Pneumonia Dr. Pradeep kumar II yr Pulmonary Medicine PNEUMOCYSTIS CARINII PNEUMONIA Pneumocystis carinii pneumonia (PCP), is commonly termed Pneumocystis jiroveci pneumonia, is the 2 nd most
Pneumocystis Pneumonia Dr. Pradeep kumar II yr Pulmonary Medicine PNEUMOCYSTIS CARINII PNEUMONIA Pneumocystis carinii pneumonia (PCP), is commonly termed Pneumocystis jiroveci pneumonia, is the 2 nd most
Clinical Manifestations of HIV
 HIV Symptoms Diane Havlir, MD Professor of Medicine and Chief, HIV/AIDS Division University of California, San Francisco (UCSF) WorldMedSchool; July 2, 2013 1 Clinical Manifestations of HIV! Result from
HIV Symptoms Diane Havlir, MD Professor of Medicine and Chief, HIV/AIDS Division University of California, San Francisco (UCSF) WorldMedSchool; July 2, 2013 1 Clinical Manifestations of HIV! Result from
Immunodeficiencies HIV/AIDS
 Immunodeficiencies HIV/AIDS Immunodeficiencies Due to impaired function of one or more components of the immune or inflammatory responses. Problem may be with: B cells T cells phagocytes or complement
Immunodeficiencies HIV/AIDS Immunodeficiencies Due to impaired function of one or more components of the immune or inflammatory responses. Problem may be with: B cells T cells phagocytes or complement
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
2. Clinical Manifestations (Pediatric HIV Infection)
 Page 1 of 6 HOUSTON ROMANIA SOUTHERN AFRICA MEXICO HOME CONTACT Friday, July 25, 2003 Pediatric HIV Infection by Mark W. Kline, M.D. 1. Introduction 2. Clinical Manifestations 3. Diagnosis 2. Clinical
Page 1 of 6 HOUSTON ROMANIA SOUTHERN AFRICA MEXICO HOME CONTACT Friday, July 25, 2003 Pediatric HIV Infection by Mark W. Kline, M.D. 1. Introduction 2. Clinical Manifestations 3. Diagnosis 2. Clinical
Diagnosis of Pneumocystis carinii
 141 Diagnosis of Pneumocystis carinii Pneumonia in Human Immunodeficiency Virus Infected Patients with Polymerase Chain Reaction: A Blinded Comparison to Standard Methods Juan Torres, 1,a Mitchell Goldman,
141 Diagnosis of Pneumocystis carinii Pneumonia in Human Immunodeficiency Virus Infected Patients with Polymerase Chain Reaction: A Blinded Comparison to Standard Methods Juan Torres, 1,a Mitchell Goldman,
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I. December 5, 2012
 SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
العصوي الوعاي ي الورام = angiomatosis Bacillary
 1 / 7 BACILLARY ANGIOMATOSIS Epidemiology BA is most commonly seen in patients with acquired immunodeficiency syndrome (AIDS) and a CD4 count less than 50 cells/mm 3, with an incidence of 1.2 cases per
1 / 7 BACILLARY ANGIOMATOSIS Epidemiology BA is most commonly seen in patients with acquired immunodeficiency syndrome (AIDS) and a CD4 count less than 50 cells/mm 3, with an incidence of 1.2 cases per
Marc Bazot, MD; Jacques Cadranel, MD; Sylvie Benayoun, MD; Marc Tassart, MD; Jean Michel Bigot, MD; and Marie France Carette, MD
 Primary Pulmonary AIDS-Related Lymphoma* Radiographic and CT Findings Marc Bazot, MD; Jacques Cadranel, MD; Sylvie Benayoun, MD; Marc Tassart, MD; Jean Michel Bigot, MD; and Marie France Carette, MD Study
Primary Pulmonary AIDS-Related Lymphoma* Radiographic and CT Findings Marc Bazot, MD; Jacques Cadranel, MD; Sylvie Benayoun, MD; Marc Tassart, MD; Jean Michel Bigot, MD; and Marie France Carette, MD Study
Fungal Diseases of the Respiratory System
 Fungal Diseases of the Respiratory System Histoplasmosis(cave disease) Dr. Hala Al Daghistani Histoplasmosis is a disease caused by the fungus Histoplasma capsulatum. Histoplasma capsulatum, is usually
Fungal Diseases of the Respiratory System Histoplasmosis(cave disease) Dr. Hala Al Daghistani Histoplasmosis is a disease caused by the fungus Histoplasma capsulatum. Histoplasma capsulatum, is usually
Unit II Problem 2 Pathology: Pneumonia
 Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
A Histological Autopsy Study of the Thyroid gland in HIV infected Adults at the University Teaching Hospital in Lusaka, Zambia
 Original Article A Histological Autopsy Study of the Thyroid gland in HIV infected Adults at the University Teaching Hospital in Lusaka, Zambia 1 1 2 S. Muwowo, V. Mudenda, C. Marimo 1 Department of Pathology
Original Article A Histological Autopsy Study of the Thyroid gland in HIV infected Adults at the University Teaching Hospital in Lusaka, Zambia 1 1 2 S. Muwowo, V. Mudenda, C. Marimo 1 Department of Pathology
Value of Bronchoalveolar Lavage Fluid Cytology in the Diagnosis of Pneumocystis jirovecii Pneumonia: A Review of 30 Cases
 http://dx.doi.org/10.4046/trd.2011.71.5.322 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2011;71:322-327 CopyrightC2011. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
http://dx.doi.org/10.4046/trd.2011.71.5.322 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2011;71:322-327 CopyrightC2011. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection. Masoud Mardani M.D,FIDSA
 Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Nitrofurantoin-Induced Lung Toxicity
 Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
Profile of Tuberculosis Infection among Current HIV+ Patients at the Philippine General Hospital
 Profile of Tuberculosis Infection among Current HIV+ Patients at the Albert B. Albay Jr., MD Jemylyn Garcia, MD Joel Santiaguel, MD UP- TB in the Philippines 6 th leading cause of morbidity and mortality
Profile of Tuberculosis Infection among Current HIV+ Patients at the Albert B. Albay Jr., MD Jemylyn Garcia, MD Joel Santiaguel, MD UP- TB in the Philippines 6 th leading cause of morbidity and mortality
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Inflammation class 2. Inflammation part 2. Rheumatic fever RF. Rheumatic fever - pathogenesis. Hypersensitivity reactions. Rheumatic fever RF
 Inflammation class 2 Inflammation part 2 Rheumatic endocarditis Pneumocystis carinii pneumonia Cytomegalic pneumonia Aspergillosis Actinomycosis Rheumatic fever RF An acute, immunologically mediated multisystem
Inflammation class 2 Inflammation part 2 Rheumatic endocarditis Pneumocystis carinii pneumonia Cytomegalic pneumonia Aspergillosis Actinomycosis Rheumatic fever RF An acute, immunologically mediated multisystem
Outcomes of Moderate-to-Severe Pneumocystis Pneumonia Treated with Adjunctive Steroid in Non-HIV-Infected Patients
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2011, p. 4613 4618 Vol. 55, No. 10 0066-4804/11/$12.00 doi:10.1128/aac.00669-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Outcomes
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2011, p. 4613 4618 Vol. 55, No. 10 0066-4804/11/$12.00 doi:10.1128/aac.00669-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Outcomes
Pneumonia in immunosuppressed patients
 Blackwell Science, LtdOxford, UKRESRespirology1323-77992004 Blackwell Science Asia Pty LtdMarch 20049S1S25S29Original ArticlePneumonia in immunosuppressed patientss Kohno et al. Respirology (2004) 9, S25
Blackwell Science, LtdOxford, UKRESRespirology1323-77992004 Blackwell Science Asia Pty LtdMarch 20049S1S25S29Original ArticlePneumonia in immunosuppressed patientss Kohno et al. Respirology (2004) 9, S25
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage)
 NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage) I. Purpose The adequacy of a sputum specimen is determined
NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage) I. Purpose The adequacy of a sputum specimen is determined
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference. Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2
 June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
Thin-Section CT Findings in 32 Immunocompromised Patients with Cytomegalovirus Pneumonia Who Do Not Have AIDS
 Tomás Franquet 1,2 Kyung S. Lee 3 Nestor L. Müller 1 Received January 27, 2003; accepted after revision April 21, 2003. 1 Department of Radiology, Vancouver Hospital and Health Sciences Center and University
Tomás Franquet 1,2 Kyung S. Lee 3 Nestor L. Müller 1 Received January 27, 2003; accepted after revision April 21, 2003. 1 Department of Radiology, Vancouver Hospital and Health Sciences Center and University
Radiation Pneumonitis Joseph Junewick, MD FACR
 Radiation Pneumonitis Joseph Junewick, MD FACR 03/19/2010 History 16 year old with history of relapsed stage IV-A Hodgkin disease. Prior pulmonary involvement was irradiated. Diagnosis Radiation Pneumonitis
Radiation Pneumonitis Joseph Junewick, MD FACR 03/19/2010 History 16 year old with history of relapsed stage IV-A Hodgkin disease. Prior pulmonary involvement was irradiated. Diagnosis Radiation Pneumonitis
Pathology of Pneumonia
 Pathology of Pneumonia Dr. Atif Ali Bashir Assistant Professor of Pathology College of Medicine Majma ah University Introduction: 5000 sq meters of area.! (olympic track) Filters >10,000 L of air / day!
Pathology of Pneumonia Dr. Atif Ali Bashir Assistant Professor of Pathology College of Medicine Majma ah University Introduction: 5000 sq meters of area.! (olympic track) Filters >10,000 L of air / day!
Immunocompromised patients. Immunocompromised patients. Immunocompromised patients
 Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Judith A. Aberg, MD; Linda M. Mundy, MD; and William G. Powderly, MD
 Pulmonary Cryptococcosis in Patients Without HIV Infection* Judith A. Aberg, MD; Linda M. Mundy, MD; and William G. Powderly, MD Purpose: To further elucidate the diagnostic and therapeutic approaches
Pulmonary Cryptococcosis in Patients Without HIV Infection* Judith A. Aberg, MD; Linda M. Mundy, MD; and William G. Powderly, MD Purpose: To further elucidate the diagnostic and therapeutic approaches
Part I Study Questions
 Part I Study Questions 1. A 59-year-old man with a history of pulmonary embolism diagnosed 2 years ago and treated with warfarin for 6 months is evaluated for progressive dyspnea and bilateral lower extremity
Part I Study Questions 1. A 59-year-old man with a history of pulmonary embolism diagnosed 2 years ago and treated with warfarin for 6 months is evaluated for progressive dyspnea and bilateral lower extremity
No evidence of C4d association with AMR However, C3d and AMR correlated well
 C4d positivity Poor prognostic factor Reversal to C4d negativity did not change prognosis, with current therapy Prognostic factor for CAV Variable time line for CAV/death No correlation with cellular rejection
C4d positivity Poor prognostic factor Reversal to C4d negativity did not change prognosis, with current therapy Prognostic factor for CAV Variable time line for CAV/death No correlation with cellular rejection
Potential etiologies of infection in these patients are diverse, including common and uncommon opportunistic infections.
 In the name of God Principles of post Tx infections 1: Potential etiologies of infection in these patients are diverse, including common and uncommon opportunistic infections. Infection processes can progress
In the name of God Principles of post Tx infections 1: Potential etiologies of infection in these patients are diverse, including common and uncommon opportunistic infections. Infection processes can progress
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
NONE OVERVIEW FINANCIAL DISCLOSURES UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF (UIP) FOR PATHOLOGISTS. IPF = Idiopathic UIP Radiologic UIP Path UIP
 UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
Outline. Cryptococcosis Pneumocystosis Diarrhea. Case Histories: HIV Related- Opportunistic Infections in 2015
 AU Edited: 05/06/15 Case Histories: HIV Related- Opportunistic Infections in 2015 Henry Masur, MD Clinical Professor of Medicine George Washington University School of Medicine Bethesda, Maryland Washington,
AU Edited: 05/06/15 Case Histories: HIV Related- Opportunistic Infections in 2015 Henry Masur, MD Clinical Professor of Medicine George Washington University School of Medicine Bethesda, Maryland Washington,
Α 78-year-old female who presents with a non-resolving pneumonia: what is your diagnosis?
 Evangelia Panagiotidou 1, Serafeim-Chrysovalantis Kotoulas 1, Maria Kilmpasani 2, Nikoleta Pastelli 2, Sofia Akritidou 1, Evangelos Chatzopoulos 1, Vasilis Bikos 1, Vasilios Bagalas 1, Katalin Fekete-Passa
Evangelia Panagiotidou 1, Serafeim-Chrysovalantis Kotoulas 1, Maria Kilmpasani 2, Nikoleta Pastelli 2, Sofia Akritidou 1, Evangelos Chatzopoulos 1, Vasilis Bikos 1, Vasilios Bagalas 1, Katalin Fekete-Passa
Study of systemic fungal infections in renal transplant recipients
 Original Research Article Study of systemic fungal infections in renal transplant recipients N.D. Srinivasaprasad 1*, G. Chandramohan 1, M. Edwin Fernando 2 1 DM (Nephrology), Assistant Professor, 2 DM
Original Research Article Study of systemic fungal infections in renal transplant recipients N.D. Srinivasaprasad 1*, G. Chandramohan 1, M. Edwin Fernando 2 1 DM (Nephrology), Assistant Professor, 2 DM
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
Lung Injury after HCT
 Lung Injury after HCT J. Douglas Rizzo, MD, MS Financial Disclosure None SCS06_1.ppt Background HCT an important therapeutic modality for malignant and non-malignant diseases Pulmonary Toxicity common
Lung Injury after HCT J. Douglas Rizzo, MD, MS Financial Disclosure None SCS06_1.ppt Background HCT an important therapeutic modality for malignant and non-malignant diseases Pulmonary Toxicity common
ECMM Excellence Centers Quality Audit
 ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
Atlas of the Vasculitic Syndromes
 CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Wedge Biopsy for Diffuse Lung Diseases
 Chapter VI Wedge Biopsy for Diffuse Lung Diseases Wedge biopsy via thoracoscopic biopsy or open lung biopsy is occasionally performed to obtain tissue for the diagnosis of a diffuse lung disease. A wedge
Chapter VI Wedge Biopsy for Diffuse Lung Diseases Wedge biopsy via thoracoscopic biopsy or open lung biopsy is occasionally performed to obtain tissue for the diagnosis of a diffuse lung disease. A wedge
Eastern Mediterranean Health Journal, Vol. 14, No. 5,
 Eastern Mediterranean Health Journal, Vol. 14, No. 5, 2008 1217 Case report Inappropriate use of steroid and Pneumocystis jiroveci pneumonia: report of two cases P. Tabarsi, 1 M. Mirsaeidi, 1 M. Amiri,
Eastern Mediterranean Health Journal, Vol. 14, No. 5, 2008 1217 Case report Inappropriate use of steroid and Pneumocystis jiroveci pneumonia: report of two cases P. Tabarsi, 1 M. Mirsaeidi, 1 M. Amiri,
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Leslie Case 4. Prac%cal Approach to Granulomatous Lung Disease. PRE-TEST Which of these images is more likely to have organisms on special stains?
 Leslie Case 4 Prac%cal pproach to Granulomatous Lung Disease Kevin O. Leslie, MD Professor and Consultant Mayo Clinic rizona PRE-TEST have organisms on special stains? PRE-TEST represent infection? PRE-TEST
Leslie Case 4 Prac%cal pproach to Granulomatous Lung Disease Kevin O. Leslie, MD Professor and Consultant Mayo Clinic rizona PRE-TEST have organisms on special stains? PRE-TEST represent infection? PRE-TEST
* MILIARY MOTTLING --
 * MILIARY MOTTLING -- RARE CAUSE DR ARATHI SRINIVASAN FELLOW IN PEDIATRIC HEMATO ONCOLOGY DR A ANDAL DEPARTMENT OF PEDIATRICS DR JULIUS XAVIER SCOTT DEPARTMENT OF PEDIATRIC HEMATO ONCOLOGY KANCHI KAMAKOTI
* MILIARY MOTTLING -- RARE CAUSE DR ARATHI SRINIVASAN FELLOW IN PEDIATRIC HEMATO ONCOLOGY DR A ANDAL DEPARTMENT OF PEDIATRICS DR JULIUS XAVIER SCOTT DEPARTMENT OF PEDIATRIC HEMATO ONCOLOGY KANCHI KAMAKOTI
MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSPLANTATION
 MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSP There are no translations available. MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSPLANTATION
MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSP There are no translations available. MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSPLANTATION
Case Presentations in ILD. Harold R. Collard, MD Department of Medicine University of California San Francisco
 Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
The Pulmonary Pathology of Iatrogenic Immunosuppression. Kevin O. Leslie, M.D. Mayo Clinic Scottsdale
 The Pulmonary Pathology of Iatrogenic Immunosuppression Kevin O. Leslie, M.D. Mayo Clinic Scottsdale The indications for iatrogenic immunosuppression Autoimmune/inflammatory disease Chemotherapy for malignant
The Pulmonary Pathology of Iatrogenic Immunosuppression Kevin O. Leslie, M.D. Mayo Clinic Scottsdale The indications for iatrogenic immunosuppression Autoimmune/inflammatory disease Chemotherapy for malignant
Pulmonary Alveolar Proteinosis
 January 2001 Pulmonary Alveolar Proteinosis Brady Case, Harvard Medical School 1 Our Patient Nelson is a 40 year-old male who presents with a 6 month history of: progressive dyspnea on exertion dry cough
January 2001 Pulmonary Alveolar Proteinosis Brady Case, Harvard Medical School 1 Our Patient Nelson is a 40 year-old male who presents with a 6 month history of: progressive dyspnea on exertion dry cough
MICROBIOLOGICAL TESTING IN PICU
 MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
5/15/2017. What Does HIV/AIDS Look Like in DC in Potpourri of Challenges With Opportunistic Infections
 Potpourri of Challenges With Opportunistic Infections Henry Masur, MD Clinical Professor of Medicine George Washington University Washington, DC FORMATTED: 4/28/217 Learning Objectives After attending
Potpourri of Challenges With Opportunistic Infections Henry Masur, MD Clinical Professor of Medicine George Washington University Washington, DC FORMATTED: 4/28/217 Learning Objectives After attending
2046: Fungal Infection Pre-Infusion Data
 2046: Fungal Infection Pre-Infusion Data Fungal infections are significant opportunistic infections affecting transplant patients. Because these infections are quite serious, it is important to collect
2046: Fungal Infection Pre-Infusion Data Fungal infections are significant opportunistic infections affecting transplant patients. Because these infections are quite serious, it is important to collect
Case of the Day Chest
 Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement
 CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
Bronchoalveolar Lavage and Histopathologic Diagnosis Based on Biopsy
 Idiopathic Pulmonary Fibrosis Bronchoalveolar Lavage and Histopathologic Diagnosis Based on Biopsy JMAJ 46(11): 469 474, 2003 Yukihiko SUGIYAMA Professor, Division of Pulmonary Medicine, Department of
Idiopathic Pulmonary Fibrosis Bronchoalveolar Lavage and Histopathologic Diagnosis Based on Biopsy JMAJ 46(11): 469 474, 2003 Yukihiko SUGIYAMA Professor, Division of Pulmonary Medicine, Department of
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
CD 4 COUNT LEVELS AND PATTERN OF RESPIRATORY COMPLICATIONS IN HIV SEROPOSITIVE PATIENTS IN CALABAR, NIGERIA.
 93 Nigerian Journal of Physiological Sciences 22 (1-2): 93-97 Physiological Society of Nigeria, 2007 Available online/abstracted at http://www.biolineinternational.org.br/njps; www.ajol.info/journals.njps;
93 Nigerian Journal of Physiological Sciences 22 (1-2): 93-97 Physiological Society of Nigeria, 2007 Available online/abstracted at http://www.biolineinternational.org.br/njps; www.ajol.info/journals.njps;
Case Report Rapid Progression of Pulmonary Blastomycosis in an Untreated Patient of Chronic Lymphocytic Leukemia
 Case Reports in Medicine, Article ID 514382, 5 pages http://dx.doi.org/10.1155/2014/514382 Case Report Rapid Progression of Pulmonary Blastomycosis in an Untreated Patient of Chronic Lymphocytic Leukemia
Case Reports in Medicine, Article ID 514382, 5 pages http://dx.doi.org/10.1155/2014/514382 Case Report Rapid Progression of Pulmonary Blastomycosis in an Untreated Patient of Chronic Lymphocytic Leukemia
Respiratory Pathology. Kristine Krafts, M.D.
 Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Index. B Biological factors, 2 Brain stem encephalitis, Burkitt s lymphoma, 83, 105
 Index A Acquired immunodeficiency syndrome (AIDS) abdomen gallbladder complications, 97, 107 109 gastrointestinal complications, 96, 105 106 liver complications, 97, 107 109 neoplasm, 99, 110 111 pancreas
Index A Acquired immunodeficiency syndrome (AIDS) abdomen gallbladder complications, 97, 107 109 gastrointestinal complications, 96, 105 106 liver complications, 97, 107 109 neoplasm, 99, 110 111 pancreas
Clinico-pathological conference
 Genitourin Med 1992;68:11-15 1 1 Clinico-pathological conference Genitourinary Medicine, The London P French University College and Middlesex School of Medicine, The London, Department of Histopathology
Genitourin Med 1992;68:11-15 1 1 Clinico-pathological conference Genitourinary Medicine, The London P French University College and Middlesex School of Medicine, The London, Department of Histopathology
Cytomegalovirus (CMV) Viral Load in Bronchoalveolar Lavage Fluid (BALF) and Plasma to Diagnose Lung Transplant Associated CMV Pneumonia
 Cytomegalovirus (CMV) Viral Load in Bronchoalveolar Lavage Fluid (BALF) and Plasma to Diagnose Lung Transplant Associated CMV Pneumonia I.P. Lodding 1,2, H.H. Schultz 3, J.U. Jensen 1,5, C. Andersen 4,
Cytomegalovirus (CMV) Viral Load in Bronchoalveolar Lavage Fluid (BALF) and Plasma to Diagnose Lung Transplant Associated CMV Pneumonia I.P. Lodding 1,2, H.H. Schultz 3, J.U. Jensen 1,5, C. Andersen 4,
The Lymphatic System. Dr. Ali Ebneshahidi
 The Lymphatic System Dr. Ali Ebneshahidi Functions of The Lymphatic System Lymphatic capillaries reabsorb excessive tissue fluid and transport the fluid through the lymphatic pathway, and ultimately dispose
The Lymphatic System Dr. Ali Ebneshahidi Functions of The Lymphatic System Lymphatic capillaries reabsorb excessive tissue fluid and transport the fluid through the lymphatic pathway, and ultimately dispose
Diagnostic Procedures for Pulmonary Infiltrates in the Compromised Host
 Diagnostic Procedures for Pulmonary Infiltrates in the Compromised Host Michael Douvas, MD Heme/Onc Gerald Donowitz, MD - ID Eric Davis, MD - Pulmonary Disclosure Drs. Davis, Donowitz, and Douvas do not
Diagnostic Procedures for Pulmonary Infiltrates in the Compromised Host Michael Douvas, MD Heme/Onc Gerald Donowitz, MD - ID Eric Davis, MD - Pulmonary Disclosure Drs. Davis, Donowitz, and Douvas do not
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
Pleural effusion as an initial manifestation in a patient with primary pulmonary monoclonal B-cell lymphocyte proliferative disease
 Du et al. Respiratory Research (2018) 19:247 https://doi.org/10.1186/s12931-018-0941-6 LETTER TO THE EDITOR Pleural effusion as an initial manifestation in a patient with primary pulmonary monoclonal B-cell
Du et al. Respiratory Research (2018) 19:247 https://doi.org/10.1186/s12931-018-0941-6 LETTER TO THE EDITOR Pleural effusion as an initial manifestation in a patient with primary pulmonary monoclonal B-cell
Opportunistic infections
 Opportunistic infections Opportunistic infections Decrease in number of CD4 lymphocytes is condition for development of opportunistic infections Risk is started, when number of CD4 lymphocytes drops to
Opportunistic infections Opportunistic infections Decrease in number of CD4 lymphocytes is condition for development of opportunistic infections Risk is started, when number of CD4 lymphocytes drops to
Original Article High-resolution computed tomography features of Pneumocystis jirovecii infection in patients with renal transplant
 Int J Clin Exp Med 2017;10(7):10683-10689 www.ijcem.com /ISSN:1940-5901/IJCEM0050944 Original Article High-resolution computed tomography features of Pneumocystis jirovecii infection in patients with renal
Int J Clin Exp Med 2017;10(7):10683-10689 www.ijcem.com /ISSN:1940-5901/IJCEM0050944 Original Article High-resolution computed tomography features of Pneumocystis jirovecii infection in patients with renal
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
Non-neoplastic Lung Disease II
 Pathobasic Non-neoplastic Lung Disease II Spasenija Savic Prince Pathology Program Systematic approach to surgical lung biopsies with ILD Examples (chronic ILD): Idiopathic interstitial pneumonias: UIP,
Pathobasic Non-neoplastic Lung Disease II Spasenija Savic Prince Pathology Program Systematic approach to surgical lung biopsies with ILD Examples (chronic ILD): Idiopathic interstitial pneumonias: UIP,
Pulmonary Cryptococcosis in an HIV-infected Patient
 Case Report Vol. 28 No. 3 Pulmonary Cryptococcosis:- Wongkulab P, et al. 203 Pulmonary Cryptococcosis in an HIV-infected Patient Panuwat Wongkulab, M.D., Nontakan Nuntachit, M.D., Romanee Chaiwarith, M.D.,
Case Report Vol. 28 No. 3 Pulmonary Cryptococcosis:- Wongkulab P, et al. 203 Pulmonary Cryptococcosis in an HIV-infected Patient Panuwat Wongkulab, M.D., Nontakan Nuntachit, M.D., Romanee Chaiwarith, M.D.,
The Differentiation of Yeast and Yeast-Like Forms in Human Tissues. Introduction. Histochemical Stains Used to Detect Fungi. Histopathologic Diagnoses
 The Differentiation of Yeast and Yeast-Like Forms in Human Tissues Gary W. Procop, MD Chair, Clinical Pathology Staff, Anatomic Pathology Director, Molecular Microbiology, Mycology, and Parasitology Cleveland
The Differentiation of Yeast and Yeast-Like Forms in Human Tissues Gary W. Procop, MD Chair, Clinical Pathology Staff, Anatomic Pathology Director, Molecular Microbiology, Mycology, and Parasitology Cleveland
INTERSTITIAL LUNG DISEASE Dr. Zulqarnain Ashraf
 Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Received February 23, Received revised March 15, Accepted for publication March 16, University of California, Davis, CA, USA
 643990HICXXX10.1177/2324709616643990Journal of Investigative Medicine High Impact Case ReportsNguyen et al case-report2016 Case Report Acute Fibrinous and Organizing Pneumonia Associated With Allogenic
643990HICXXX10.1177/2324709616643990Journal of Investigative Medicine High Impact Case ReportsNguyen et al case-report2016 Case Report Acute Fibrinous and Organizing Pneumonia Associated With Allogenic
Pathology lab 4 DONE BY : MORAD ABU QAMAR
 Pathology lab 4 DONE BY : MORAD ABU QAMAR Chronic interstitial inflammation, lung Certain etiologic agents such as viruses are more likely to lead to chronic inflammation, as seen here in the lung of a
Pathology lab 4 DONE BY : MORAD ABU QAMAR Chronic interstitial inflammation, lung Certain etiologic agents such as viruses are more likely to lead to chronic inflammation, as seen here in the lung of a
Azathioprine-associated Interstitial Pneumonitis
 Azathioprineassociated Interstitial Pneumonitis CARLOS W. M. BEDROSSIAN, M.D., AND BARRY KAHAN, M.D., PH.D. JEFFREY SUSSMAN, M.D., RICHARD H. CONKLIN, PH.D., M.D. Seven renal allograft recipients taking
Azathioprineassociated Interstitial Pneumonitis CARLOS W. M. BEDROSSIAN, M.D., AND BARRY KAHAN, M.D., PH.D. JEFFREY SUSSMAN, M.D., RICHARD H. CONKLIN, PH.D., M.D. Seven renal allograft recipients taking
5/9/2015. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. No, I am not a pulmonologist! Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
HIV related pulmonary infections. A radiologic pictorial review.
 HIV related pulmonary infections. A radiologic pictorial review. Poster No.: C-0836 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Arcalis, P. Trallero, L. Berrocal Morales, S. Medrano, S. 1
HIV related pulmonary infections. A radiologic pictorial review. Poster No.: C-0836 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Arcalis, P. Trallero, L. Berrocal Morales, S. Medrano, S. 1
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids
 Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
A Case of Pediatric Plasma Cell Granuloma
 August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
Test Requested Specimen Ordering Recommendations
 Microbiology Essentials Culture and Sensitivity (C&S) Urine C&S Catheter Surgical (excluding kidney aspirates) Voided Requisition requirements o Specific method of collection MUST be indicated o Indicate
Microbiology Essentials Culture and Sensitivity (C&S) Urine C&S Catheter Surgical (excluding kidney aspirates) Voided Requisition requirements o Specific method of collection MUST be indicated o Indicate
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
Coccidia. Eucoccidioside
 Coccidia Kingdom Sub-Kingdom Phylum Class Order Family Genus Species Protista Protozoa Apicomplexa Sporozoasida Eucoccidioside Sarcocystidae Toxoplasma gondii 1 Toxoplasma gondii (life cycle) Sexual cycle
Coccidia Kingdom Sub-Kingdom Phylum Class Order Family Genus Species Protista Protozoa Apicomplexa Sporozoasida Eucoccidioside Sarcocystidae Toxoplasma gondii 1 Toxoplasma gondii (life cycle) Sexual cycle
