ORIGINAL ARTICLE AFRICAN JOURNAL OF CLINICAL AND EXPERIMENTAL MICROBIOLOGY MAY 2012 ISBN X VOL 13(2)
|
|
|
- Janis Henderson
- 6 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE AFRICAN JOURNAL OF CLINICAL AND EXPERIMENTAL MICROBIOLOGY MAY 2012 ISBN X VOL 13(2) AJCEM/201179/ COPYRIGHT 2012 AFR. J. CLN. EXPER. MICROBIOL 13(2): EVALUATING THE EFFICACY OF TOPICAL SILVER NITRATE AND INTRAMUSCULAR ANTIMONIAL DRUGS IN THE TREATMENT OF CUTANEOUS LEISHMANIASIS IN SOKOTO, NIGERIA 1 Igbineweka O.O., 2 Aghedo F.I., 3 Idusuyi O., 4 Hussain N.A. 1 Brigade Medical Centre, Gingiya Military Barracks, Sokoto¹, Department of Hematology and Blood Transfusion Science, Usmanu Danfodiyu University Teaching Hospital, Sokoto², Department of Pharmacology, Usmanu Danfodiyu University, Sokoto³ Department of Preventive Health, Military Hospital, Lagos 4 Correspondence naahussain@yahoo.co.uk ABSTRACT Background: Cutaneous leishmaniasis (CL) is a disease of public health importance in Nigeria, with high prevalence in the Northwest and Northeastern part of the country. The side effects of antimonial drugs {stibogluconate (SSG) and meglumine antimoniate} in the treatment of CL have often resulted in poor drug adherence and default by patients and possible drug resistance. The increasing default to follow-up and the significant side effects associated with antimonial therapy necessitated the dire need of alternative therapeutic modalities. Thus, this study aimed at comparing the efficacy of topical silver nitrate with the antimonial drugs in the treatment of CL. Methods: A total of 95 patients with clinically diagnosed leishmaniasis and parasitologically proven CL participated in the study after their informed-consent had been obtained. The treatment selection was optional to the participants. Sixty (63.2%) patients received alternative therapy of topical silver nitrate as a single dose while 35(36.8%) patients received antimonial therapy for 21 days at 20mg/kg body weight. Results: On day 30 of treatment, 68 (86.1%) lesions among patients on topical silver nitrate healed completely as compared with only 5 (6.8%) among those on i.m. SSG. There was no improvement in 25 (34.2%) lesions among those on i.m. SSG compared with only 1 (1.2%) lesion among those on topical silver nitrate. Overall, there was a statistically significant difference in the cure rate among patients on silver nitrate as compared with those on i.m. SSG on the 21 st and 30 th days of treatment.(p<0.05). Conclusion: Topical silver nitrate therapy is an effective and better drug treatment for CL among this study population. Keywords: Cutaneous leishmaniasis, efficacy, Silver nitrate, Sodium Stibogluconate, Sokoto INTRODUCTION Leishmaniasis is an infection that is caused by an obligate intracellular protozoa of the genus Leishmania; first described in 1903 by Leishman and Donovan. The natural transmission of Leishmania parasites is carried out by sandflies of the genus Phlebotomus or Lutzomyia (1). These parasites cause three forms of leishmaniasis according to the localization of the parasites in mammalian tissues, notably visceral, cutaneous, and mucosal leishmaniasis. The outcome of infection depends on the species of Leishmania 90
2 parasites and the host s immune response (2). Visceral leishmaniasis (VL) is the most severe form of leishmaniasis involving internal organs such as the spleen and liver and is fatal if left untreated (3). Globally, about 350 million people live in areas of active transmission of Leishmania, with estimated 14 million people directly affected in Africa, Asia, Europe, and America (4). The global burden of leishmaniasis has remained stable for some years, causing a morbidity and mortality loss of 2.4 million Disability Adjusted Life-Years (DALYs) and approximately 70,000 deaths; a significantly high figure ranked among communicable diseases (5,6). Leishmaniasis and Human Immunodeficiency Virus (HIV) co-infection has surged as a major complication of leishmaniasis and has ignited calls for the recognition of leishmaniasis as an Acquired Immunodeficiency Syndrome (AIDS) defining-illness (7). In Africa, particularly Ethiopia and Sudan, it is estimated that 70% of adults with VL also have HIV infection (8). Northern Nigeria is one of the West African endemic CL foci, especially in Sokoto, Gusau, Katsina, Maiduguri and Azare 9. Between 1924 and 1941, the Nigeria health services recorded 131 cases of CL and 5 cases of VL, but there was no indication that these cases were parasitologically confirmed. In 1942, smears of 14 patients from Kano with cutaneous sores were confirmed parasitologically to be leishmaniasis. However, the first case of CL in Nigeria was officially reported in 1944 (9,10). In spite of the initial public health efforts on CL in this region, there is dearth of follow-up data on CL caused by Leishmania tropica and its treatment-induced cure rates. The current management of leishmaniasis are drug treatment of patients, to alleviate disease and vector control to reduce its transmission. Pentavalent antimonials (namely, sodium stibogluconate (SSG) and meglumine antimoniate) are the mainstay of anti-leishmanial therapy (11-13). However, the antimonials have serious adverse effects (such as pancreatitis, hepatotoxicity, and cardiotoxicity) when given intramuscularly (14,16) and are expensive (17). Moreover, the lengthy course of its administration and associated pain often results in low drug adherence, default and ultimately, drug resistance (18,18). Bearing in mind several studies that have shown the high efficacy of colloidal silver as an antimicrobial (20,-23), the topical silver nitrate appears to be the most feasible alternative. Silver is toxic to microorganisms by poisoning respiratory enzymes and components of the microbial electron transport system as well as impairing some DNA function 24,25. Additionally, silver has been shown to interact with structural proteins and preferentially bind with DNA bases to inhibit replication (26,,27). Therefore, in order to achieve effective control of CL, it is pertinent to try other drug-treatment modalities which are painless, tolerable, and of short duration. Hence the focus of this study which compared the efficacy of the topical silver nitrate therapy with the antimonials in the treatment of CL due to L. tropica in Sokoto, Northwest Nigeria. 91
3 MATERIALS AND METHODS Study location and Participants. The study was carried out at 1 Brigade Medical Centre which is located in Gingiya military barracks, Sokoto, Northwest Nigeria. Established in 1984, the medical centre is well staffed, with equipped laboratory and provides curative and preventive services to the soldiers, their families and the civil populace. It is also a designated centre by the Sokoto State Ministry of Health and the Nigerian Ministry of Defence-US Department of Defense (NMOD-USDoD) for the treatment of Leishmaniasis and HIV/AID respectively. Ninety five patients, aged more than 5 years with parasitologically confirmed CL lesions were recruited for the study. The exclusion criteria were pregnancy, breast-feeding mothers, patients who had a major surgery in the previous 3 months, presence of any uncontrolled medical condition; anticipated unavailability for followup; and patients allergic to antimonials and silver nitrate. Ethical issues: The authority of the Medical Centre and State s ethics committee approved the study protocol and the consent form. New and eligible patients attending the clinic for treatment were briefed about the aim and protocol of the study. Patients were enrolled in the study after an informed consent had been given. All medical services provided during the study were free. Participant s Medical History: Prior to the study, a detailed medical and personal history of each participant was taken. These included the duration of symptoms, residence in or travel through a possibly leishmaniasis-endemic area, history of any existing health condition, menstrual and parity history, previous treatments and outcome. A general physical examination was also carried out to assess the location, size of lesions with other characteristics such as infiltration, erythema, scaling and ulceration. Parasitological confirmation: Parasitological confirmation of CL was by microscopic examination of smear and with RIDASCREEN leishmania antibody test kit (R-Biopharm, Germany). Scrapings from the lesion edge were smeared onto a slide, and the slide was dried, fixed with methanol, stained with Giemsa and examined under the microscope at x100 magnification for presence of Leishmania amastigotes. For each, patient, 2 slides were prepared and all positive slides were rechecked and confirmed by at least 2 laboratory scientists. For leishmania antibody testing about 3mls of whole blood was collected from each participant into a clean dry plain blood container and allowed to clot. The blood sample was spun with a bench centrifuge at 5000rpm for 5 minutes and the serum separated into another clean plain container and stored frozen prior to testing at - 20⁰C. The samples were tested using Elisa leishmania antibody kit (R-Biopharm, Germany), using the procedure as described in the manual of the kit. Treatment Procedure Sixty patients had a single dose topical silver nitrate treatment while 35 had daily intramuscular administration of SSG for 21 days using the World Health Organization recommended treatment for CL (28). For intramuscular administration, 20 mg/kg of SSG was administered daily (up to a maximum daily dose of 850 mg) for 21 days (28). For silver nitrate 92
4 treatment, the surface of the each lesion was cleaned with hydrogen peroxide solution and scraped with scalpel blade. The lesion surface was mopped with cotton wool to prevent bleeding; fine granules of silver nitrate were poured into it, covered with water-soaked cotton wool and dressed with plaster for 24 hours. After 24 hours, each lesion was cleaned daily with hydrogen peroxide and covered with Gentamycin-ointment smeared bandage for 21 days. Also, in order to prevent secondary infection, each patient on the topical silver nitrate had 280 mg of intramuscular Gentamycin for 5 days. Treatment efficacy was measured by the percentage of patients cured on 21 st and 30 th day after commencing treatment. Cure is defined as the complete re-epithelialization of the CL lesion, with no evidence of papules, inflammation, or indurations. Data collation and analysis.. The obtained data were analyzed using EPI info computer software package. The results were displayed in tables and Chi square test statistic was used at 95% level of significance. RESULTS A total of 95 patients comprising 74 males (77.9%) and 21 females (22.1%) were recruited for the study as shown in Table 1. Thirty five patients (with a total of 73 lesions) received i.m. SSG while 60 (with a total of 79 lesions) received topical silver nitrate treatment. In both groups, each male patient had an average of 1-2 lesions while each female had an average of 2-5 lesions; thus implying that the lesions were more among females than males. The age range of the patients who had intramuscular SSG was years (mean = 30.5) while that of patients who had topical silver nitrate was years (mean = 32.4). TABLE 1: CHARACTERISTICS OF PATIENTS WITH CUTANEOUS LEISHMANIASIS TREATED WITH INTRAMUSCULAR SSG AND TOPICAL SILVER NITRATE Characteristics Intramuscular SSG (%) Male Female Topical Silver Nitrate (%) Male Female Total (100%) No of Patients 30 (31.6%) 5 (5.3) 44 (46.3) 16 (16.8) 95 No of Lesions 44(28.9) 29(19.1) 41(27%) 38(25%) 152 Mean Age and Range (in years) 30.5 (13-42) 32.4 (16 52) Table 2 showed that the nodular/nodularulcerative lesions were the commonest (constituting 82.1% and 73.4% in i.m. SSG and topical silver nitrate groups respectively). Over two-third lesions were located in the upper limbs in each treatment category (i.m. SSG=65.8%, topical silver nitrate=68.3%).no lesion was seen in the groin, perineum or buttocks in both treatment categories. Table 3 showed the cure rate in each category after 21 st and 30 th day of treatment. On day 21, Sixty five (82.3%) lesions among patients on topical silver nitrate healed completely compared 93
5 with 4 (5.5%) among those on i.m. SSG. There was no improvement in 30 (41%) lesions of patients on i.m. SSG compared with 4 (5.1) among those on topical silver nitrate. On day 30 of treatment, 68 (86.1%) lesions among patients on topical silver nitrate healed completely as compared with only 5 (6.8%) among those on i.m. SSG. Also, there was no improvement in 25 (34.2%) lesions among those on i.m. SSG compared with only 1 (1.2%) lesion among those on topical silver nitrate. There was a statistically significant difference in the cure rate among patients on silver nitrate as compared with those on i.m. SSG on the 21 st and 30 th days of treatment.(p<0.05). Apart from complaints of pain at the site of injections, which was generally greater in the patients who were given i.m SSG, the medications were well-tolerated. For each patient, the results of the post-treatment biochemical and hematological investigations were normal. TABLE 2: CHARACTERISTICS OF THE CUTANEOUS LEISHMANIASIS LESIONS OF THE 95 PATIENTS TREATED Characteristics of Lesions Type of Treatment Intramuscular SSG Topical Silver nitrate (n = 73 lesions) (n = 79 lesions) Mean area of lesion and range (in cm²) 1.8( ) 1.7 ( ) Lesion type (% of lesions) Nodular 32(43.8) 37(46.8) Nodular-ulcerative 28(38.3) 21(26.6) Flat-ulcerative 10(13.7) 13(16.4) Plaque-like 3(4.1) 8(10.1) Lesion site (% of lesion) Shoulder Upper arm Elbow Lower arm Hand Thigh Knee Leg Foot 8(10.9) 10(13.7) 3(4.1) 18(24.7) 9(12.3) 4(5.5) 2(2.7) 13(17.8) 6(8.2) 5(6.3) 14(17.7) 4(5.1) 20(25.3) 11(13.9) 2(2.5) 5(6.3) 15(19) 3(3.8) DISCUSSION There have been several attempts in the past to develop a safe and simply administered drug with a broad spectrum of activity against CL. For example, high cost and painful injections are documented drawbacks of treatment by antimonial compounds(14,15). In addition, the antimonial drugs have been documented to have 80-85% cure rate, recurrent clinical signs and relapses (16). Thus, the dire need to develop effective compounds for the treatment of CL that would be economical, ease of administration and 94
6 could avoid resistance becomes expedient. To surmount this challenge, topical/local treatment of CL lesions seems a logical alternative. Although some forms of topical/local therapy have been in long use in endemic areas by traditional practitioners, they had little if any effect (27). In this study, more than three-quarter of the selected patients were males. The few female participants could be attributed to the exclusion criteria which included pregnant women and breastfeeding mothers. The patients were given the option of choosing a treatment regimen after the informed consent had been obtained and this accounted for the selection of silver nitrate treatment by 60 (63.2%) of the 95 patients. For each treatment regimen, it was observed that the male patients had an average of 1-2 lesions while females had an average of 2-5 lesions; thus implying that the lesions were more among females than males. The reason(s) for this variation cannot be explained since both gender were equally exposed to the vector. Further research to determine this variation is desirable. Also, in both treatment regimen, it was observed that over two-third lesions were located in the upper limbs (i.m. SSG=65.8%, topical silver nitrate=68.3%) and none was seen in the groin, perineum or buttocks. This finding implies that the exposed parts of the body were more accessible to the vector. It is therefore necessary to emphasize the use of protective clothes by the communities; especially while in the farm (or grazing animals); as an important preventive measure against the vector bites. TABLE 3: COMPARISON OF THE CURE RATE AMONG PATIENTS ON INTRAMUSCULAR SSG AND TOPICAL SILVER NITRATE Duration (in days) Cure Rate IM SSG (%) (n=73) Topical Silver Nitrate (%) (n=79) P value Day 21 of treatment Fully healed lesions Improved lesions No change in lesion Worsened lesion 4 (5.5) 39 (53.4) 65 (82.3) 10 (12.7) (34.2) 4 (5.1) 5 (6.8) - Day 30 of treatment Fully healed lesions Improved lesions No change in lesion Worsened lesion 5 (6.8) 43 (58.9) 68 (86.1) 10 (12.7) (28.8) 1 (1.2) 4 (5.4) - More than four-fifth (82.3%) of the lesions among patients on topical silver nitrate and only 5.5% lesions those on i.m. SSG healed completely on the 21 st day of commencing treatment. By the 95
7 30th day, 86.1% of the lesions among those on silver nitrate had healed completely as compared with only 6.8% among those on i.m. SSG. There was a statistically significant difference in the cure rate between patients on silver nitrate and those on i.m. SSG on the 21 st and 30 th days of treatment.(p<0.05). Conclusion: In comparing the efficacy of topical silver nitrate and i.m. SSG in the treatment of CL, this study has shown that a single dose treatment with topical silver nitrate plus topical gentamycin (for secondary infections) was more effective. The study also highlighted the need to educate the community on the use of protective clothing to reduce the bite by the vector. The reasons for the gender variation in the number of CL lesions among this study needs to be further researched. ACKNOWLEDGMENT We are grateful to the management and staff of 1 Brigade Medical Centre, Gingiya Barracks for their facility and cooperation during the period of the study. REFERENCES 1. Mandell GL, Bennett JE, Dolin. In Mandell, Douglas, and Bennett s Principles and practice of infectious diseases. Elsevier, 6 th edn. 2005: Roberts MTM. Current understandings on the immunology of leishmaniasis and recent developments in prevention and treatment. Br. Med.Bull: 2006; 76: Mauel J.. Vaccination Against Leishmania Infections. Current drug targets. immune. Endocr. Metabol. Disord.2002; 2: World Health Organization. Control of Leishmaniasis Report of the secretariat. _4-en.pdf 5. Davies CR, Kaye P, Croft SL, Sundar S. Leishmaniasis: New approaches to disease control. BMJ. 2003; 326: Reithinger R, Dujardin JC, Louzir H, Pirmez C, Alexander B. and Brooker S. Cutaneous Leishmaniasis. Lancet. Infect. Dis. 2007: Singh S. New developments in diagnosis of leishmaniasis. Indian. J. Med. Res.2006;123: Desjeux P. The increase in risk factors for leishmaniasis worldwide. Trans. R. Soc. Trop. Med. Hyg. 2001; 95: Jelliffe RS. Cutaneous Leishmaniasis in Nigeria and the western Sudan. West Afr. Med J. 1995;4: Handmann E. Leishmaniasis: Current status of vaccine development. Clin Microbiol Rev. 2001;14: Berman JD. Human Leishmaniasis: clinical, diagnostic and chemotherapeutic developments in the last ten years. Clin Infect Diseases.1997; 24: Croft SL, Yardley V. Chemotherapy of Leishmaniasis. Curr Pharm Design. 2002; 8: Croft SL, Coombs GH. Leishmaniasis Current chemotherapy and recent advances in the search for novel drugs. Trends Parasitol; 2003; 19: Boelaert M, LeRay D, Van Der Stuyft P. How better drugs could change kala-azar control: lessons from a cost-effectiveness analysis. Trop Med Int Health.2002;7: Aronon NE, Wortman GW, Jackson JE, Gasser RA Jr, Magill JA et al. Safety and efficacy of intravenous sodium stibogluconate in the treatment of leishmaniasis: recent US military experience. Clin Infect Dis.1998; 27:
8 16. Bryceson A. A policy for leishmaniasis with respect to the prevention and control of drug resistance. Trop Med Int Health.2001;6: Dowlati Y. Cutaneous leishmaniasis: clinical aspect. Clin Dermatol; 1996;14: Romero GAS, Guerra MVS, Paes MG, Macedo VO. Comparison of Cutaneous leishmaniasis due to leishmania braziliensis and leismania guyanensis in Brazil: Therapeutic response to meglumine antimonite. Am J Med Hyg.2001; 65: Rojas R, Valderrama L, Valderamma M, Varona MX, Quettette M et al. Resistance to antimony and treatment failure in human leishmaniasis infection. J Infect Dis. 2006;193: Lockman Y, Vardy D, Ohayon D, Elon J. The failure of traditionally used desert plants to act against cutaneous leishmaniasis in experimental animals. Annals of Tropical Medicine and Parasitology.1991; 85: Gunawan C, Teoh WY, Marquis CP, Lifla J, Amal R. Reversible antimicrobial photoswittching in nanosilver. Small.2009;5 (3): Mehrbod P, Motamed N, Tabatabaian M, Soleimani Estyar R, Amini E, Shahidi M, Tavasoti- Kheiri M. In Vitro Antiviral Effect of Nanosilver on Influenza Virus. DARU. 2009;17: Trop M, Novak M, Rodl S, Hellbom B, Kroell W, Goessler W. Silver-coated dressing acticoat caused raised liver enzymes and argyria-like symptoms in burn patient. Journal of Trauma. 2006; 60 (3): Mooney EK. Silver dressings [safety and efficacy reports]. Plast Reconstr Surg; 2006; 117(2): Poon VK, Burd A. In vitro cytotoxity of silver: implication for clinical wound care. Burns; 2004; 30: Dunn K, Edwards-Jones V.. The role of Acticoat TM with nanocrystalline silver in the management of burns. Burns; 2004;30: Reyburn, HA. Guide to the treatment of cutaneous leishmaniasis. Kabul, Afghanistan: World Health Organization
Nanosilver in the treatment of localized cutaneous leishmaniasis caused by Leishmania major (MRHO/IR/75/ER): an in vitro and in vivo study
 DARU Vol. 17, No. 4 2009 285 Nanosilver in the treatment of localized cutaneous leishmaniasis caused by Leishmania major (MRHO/IR/75/ER): an in vitro and in vivo study *1 Mohebali M., 2 Rezayat M.M., 3
DARU Vol. 17, No. 4 2009 285 Nanosilver in the treatment of localized cutaneous leishmaniasis caused by Leishmania major (MRHO/IR/75/ER): an in vitro and in vivo study *1 Mohebali M., 2 Rezayat M.M., 3
Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar
 Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar AA 55M presented with sores on left olecranon and umbilical area Umbilical sores present for 3 weeks Left olecranon lesions for 1 week
Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar AA 55M presented with sores on left olecranon and umbilical area Umbilical sores present for 3 weeks Left olecranon lesions for 1 week
Acta Dermatovenerol Croat 2008;16(2):60-64 CLINICAL ARTICLE
 2008;16(2):60-64 CLINICAL ARTICLE Clinical Efficacy of Intramuscular Meglumine Antimoniate Alone and in Combination with Intralesional Meglumine Antimoniate in the Treatment of Old World Cutaneous Leishmaniasis
2008;16(2):60-64 CLINICAL ARTICLE Clinical Efficacy of Intramuscular Meglumine Antimoniate Alone and in Combination with Intralesional Meglumine Antimoniate in the Treatment of Old World Cutaneous Leishmaniasis
Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin
 Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin Department of Dermatology, Pakistan Institute of Medical Sciences,
Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin Department of Dermatology, Pakistan Institute of Medical Sciences,
HAEMOFLAGELLATES. Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine
 HAEMOFLAGELLATES Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of Leishmania spp. and Trypanosoma
HAEMOFLAGELLATES Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of Leishmania spp. and Trypanosoma
SUMMARY. Cutaneous leishmaniasis with only skin involvement: single to multiple skin ulcers, satellite lesions and nodular lymphangitis.
 SUMMARY Leishmaniasis is a disease affecting predominantly people in the developing countries; 350 million people worldwide are at risk and yearly more than 2 million new cases occur. Leishmaniasis is
SUMMARY Leishmaniasis is a disease affecting predominantly people in the developing countries; 350 million people worldwide are at risk and yearly more than 2 million new cases occur. Leishmaniasis is
Prevalence of Cutaneous Leishmaniasis among HIV and Non-HIV Patients attending some Selected Hospitals in Jos Plateau State
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 06 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.706.307
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 06 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.706.307
Research Article Efficacy and Safety of Paromomycin in Treatment of Post-Kala-Azar Dermal Leishmaniasis
 ISRN Parasitology, Article ID 548010, 4 pages http://dx.doi.org/10.1155/2014/548010 Research Article Efficacy and Safety of Paromomycin in Treatment of Post-Kala-Azar Dermal Leishmaniasis Shyam Sundar,
ISRN Parasitology, Article ID 548010, 4 pages http://dx.doi.org/10.1155/2014/548010 Research Article Efficacy and Safety of Paromomycin in Treatment of Post-Kala-Azar Dermal Leishmaniasis Shyam Sundar,
Evaluation of Thermotherapy for the Treatment of Cutaneous Leishmaniasis in Kabul, Afghanistan: A Randomized Controlled Trial
 MILITARY MEDICINE, 177, 3:345, 2012 Evaluation of Thermotherapy for the Treatment of Cutaneous Leishmaniasis in Kabul, Afghanistan: A Randomized Controlled Trial Najibullah Safi, MD*; COL Gary D. Davis,
MILITARY MEDICINE, 177, 3:345, 2012 Evaluation of Thermotherapy for the Treatment of Cutaneous Leishmaniasis in Kabul, Afghanistan: A Randomized Controlled Trial Najibullah Safi, MD*; COL Gary D. Davis,
Oral miltefosine for Indian post-kala-azar dermal leishmaniasis: a randomised trial
 Tropical Medicine and International Health doi:10.1111/tmi.12015 volume 18 no 1 pp 96 100 january 2013 Oral miltefosine for Indian post-kala-azar dermal leishmaniasis: a randomised trial Shyam Sundar 1,
Tropical Medicine and International Health doi:10.1111/tmi.12015 volume 18 no 1 pp 96 100 january 2013 Oral miltefosine for Indian post-kala-azar dermal leishmaniasis: a randomised trial Shyam Sundar 1,
The Most Common Parasitic Infections In Yemen. Medical Parasitology
 The Most Common Parasitic Infections In Yemen Medical Parasitology ﻓﺎﯾز اﻟﺧوﻻﻧﻲ / د 2 : is a vector-borne disease that transmitted by sandflies and caused by obligate intracellular protozoa of the genus
The Most Common Parasitic Infections In Yemen Medical Parasitology ﻓﺎﯾز اﻟﺧوﻻﻧﻲ / د 2 : is a vector-borne disease that transmitted by sandflies and caused by obligate intracellular protozoa of the genus
World Health Organization Department of Communicable Disease Surveillance and Response
 WHO Report on Global Surveillance of Epidemic-prone Infectious Diseases World Health Organization Department of Communicable Disease Surveillance and Response This document has been downloaded from the
WHO Report on Global Surveillance of Epidemic-prone Infectious Diseases World Health Organization Department of Communicable Disease Surveillance and Response This document has been downloaded from the
Control of leishmaniasis
 SIXTIETH WORLD HEALTH ASSEMBLY A60/10 Provisional agenda item 12.3 22 March 2007 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
SIXTIETH WORLD HEALTH ASSEMBLY A60/10 Provisional agenda item 12.3 22 March 2007 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan
 Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan Mamoun Mohammad Al-Athamneh Hiathem Qasem Abu Al-haija Ra ed Smadi Ayman S. Qaqaa Heba
Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan Mamoun Mohammad Al-Athamneh Hiathem Qasem Abu Al-haija Ra ed Smadi Ayman S. Qaqaa Heba
Antimonial Resistance & Combination therapy in Indian Visceral Leishmaniasis. Shyam Sundar Banaras Hindu University Varanasi, India
 Antimonial Resistance & Combination therapy in Indian Visceral Leishmaniasis Shyam Sundar Banaras Hindu University Varanasi, India History of the Current Epidemic in India & Antimony Resistance 6 Official
Antimonial Resistance & Combination therapy in Indian Visceral Leishmaniasis Shyam Sundar Banaras Hindu University Varanasi, India History of the Current Epidemic in India & Antimony Resistance 6 Official
Leishmaniasis, Kala Azar(The Black Fever)
 Leishmaniasis, Kala Azar(The Black Fever) By Lawrence Hall Etiologic agent Protist obligate intracellular parasite, Transmission Vectors Phylum: Euglenozoa (genus Leishmania) Over 21 species that infect
Leishmaniasis, Kala Azar(The Black Fever) By Lawrence Hall Etiologic agent Protist obligate intracellular parasite, Transmission Vectors Phylum: Euglenozoa (genus Leishmania) Over 21 species that infect
CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças Red Room 17: 00h
 CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000 deaths (6.7%) 310 million at
CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000 deaths (6.7%) 310 million at
by author Drug Therapy in African Visceral Leishmaniasis 28th ECCMID Conference, Madrid, Spain 21 April 2018
 Drug Therapy in African Visceral Leishmaniasis 28th ECCMID Conference, Madrid, Spain 21 April 2018 Dr. Monique Wasunna, Director, DNDi Africa Regional Office Presentation Outline 1 2 4 5 Introduction leishmaniasis
Drug Therapy in African Visceral Leishmaniasis 28th ECCMID Conference, Madrid, Spain 21 April 2018 Dr. Monique Wasunna, Director, DNDi Africa Regional Office Presentation Outline 1 2 4 5 Introduction leishmaniasis
Single-Dose Liposomal Amphotericin B in the Treatment of Visceral Leishmaniasis in India: A Multicenter Study
 MAJOR ARTICLE Single-Dose Liposomal Amphotericin B in the Treatment of Visceral Leishmaniasis in India: A Multicenter Study S. Sundar, 1 T. K. Jha, 2 C. P. Thakur, 3 M. Mishra, 4 V. P. Singh, 1 and R.
MAJOR ARTICLE Single-Dose Liposomal Amphotericin B in the Treatment of Visceral Leishmaniasis in India: A Multicenter Study S. Sundar, 1 T. K. Jha, 2 C. P. Thakur, 3 M. Mishra, 4 V. P. Singh, 1 and R.
Leishmaniasis: A forgotten disease among neglected people
 ISPUB.COM The Internet Journal of Health Volume 11 Number 2 Leishmaniasis: A forgotten disease among neglected people Y Homsi, G Makdisi Citation Y Homsi, G Makdisi. Leishmaniasis: A forgotten disease
ISPUB.COM The Internet Journal of Health Volume 11 Number 2 Leishmaniasis: A forgotten disease among neglected people Y Homsi, G Makdisi Citation Y Homsi, G Makdisi. Leishmaniasis: A forgotten disease
Short-Course Paromomycin Treatment of Visceral Leishmaniasis in India: 14-Day vs 21-Day Treatment
 MAJOR ARTICLE Short-Course Paromomycin Treatment of Visceral Leishmaniasis in India: 14-Day vs 21-Day Treatment Shyam Sundar, Neha Agrawal, Rakesh Arora, Dipti Agarwal, Madhukar Rai, and Jaya Chakravarty
MAJOR ARTICLE Short-Course Paromomycin Treatment of Visceral Leishmaniasis in India: 14-Day vs 21-Day Treatment Shyam Sundar, Neha Agrawal, Rakesh Arora, Dipti Agarwal, Madhukar Rai, and Jaya Chakravarty
Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar)
 SEA-CD-274 Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar) World Health Organization 2013 All rights reserved. Requests for publications, or for permission to reproduce or translate WHO
SEA-CD-274 Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar) World Health Organization 2013 All rights reserved. Requests for publications, or for permission to reproduce or translate WHO
Control of leishmaniasis
 EXECUTIVE BOARD EB118/4 118th Session 11 May 2006 Provisional agenda item 5.1 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
EXECUTIVE BOARD EB118/4 118th Session 11 May 2006 Provisional agenda item 5.1 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
New insights on leishmaniasis in immunosuppressive conditions
 New insights on leishmaniasis in immunosuppressive conditions Javier Moreno Immunoparasitology Unit WHO Collaborative Center for Leishmaniasis Centro Nacional de Microbiología INSTITUTO DE SALUD CARLOS
New insights on leishmaniasis in immunosuppressive conditions Javier Moreno Immunoparasitology Unit WHO Collaborative Center for Leishmaniasis Centro Nacional de Microbiología INSTITUTO DE SALUD CARLOS
Authors Chappuis, François; Alirol, Emilie; Worku, Dagemlidet T; Mueller, Yolanda; Ritmeijer, Koert
 MSF Field Research High mortality among older patients treated with pentavalent antimonials for visceral leishmaniasis in East Africa and rationale for switch to liposomal amphotericin B Item type Article
MSF Field Research High mortality among older patients treated with pentavalent antimonials for visceral leishmaniasis in East Africa and rationale for switch to liposomal amphotericin B Item type Article
Original Article Chloroquine in cutaneous leishmaniasis
 Original Article Chloroquine in cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin, Iqbal Sidiqui Department of Dermatology, Pakistan Institute of Medical Sciences, Islamabad Abstract Background Chloroquine
Original Article Chloroquine in cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin, Iqbal Sidiqui Department of Dermatology, Pakistan Institute of Medical Sciences, Islamabad Abstract Background Chloroquine
DOWNLOAD OR READ : TROPICAL INFECTIOUS DISEASES SECOND EDITION PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : TROPICAL INFECTIOUS DISEASES SECOND EDITION PDF EBOOK EPUB MOBI Page 1 Page 2 tropical infectious diseases second edition tropical infectious diseases second pdf tropical infectious
DOWNLOAD OR READ : TROPICAL INFECTIOUS DISEASES SECOND EDITION PDF EBOOK EPUB MOBI Page 1 Page 2 tropical infectious diseases second edition tropical infectious diseases second pdf tropical infectious
Treatment of Cutaneous Leishmaniasis with Allopurinol and Stibogluconate
 165 Treatment of Cutaneous Leishmaniasis with Allopurinol and S. Martinez, M. Gonzalez, and M. E. Vernaza From the Department of Internal Medicine, University of Cauca, Popayan, and the University Hospital
165 Treatment of Cutaneous Leishmaniasis with Allopurinol and S. Martinez, M. Gonzalez, and M. E. Vernaza From the Department of Internal Medicine, University of Cauca, Popayan, and the University Hospital
Transactions of the Royal Society of Tropical Medicine and Hygiene
 Transactions of the Royal Society of Tropical Medicine and Hygiene 104 (2010) 225 229 Contents lists available at ScienceDirect Transactions of the Royal Society of Tropical Medicine and Hygiene journal
Transactions of the Royal Society of Tropical Medicine and Hygiene 104 (2010) 225 229 Contents lists available at ScienceDirect Transactions of the Royal Society of Tropical Medicine and Hygiene journal
Visceral leishmaniasis: an endemic disease with global impact
 Visceral leishmaniasis: an endemic disease with global impact Professor Olivier Lortholary, MD, PhD Department of Infectious and Tropical diseases Hôpital Necker-Enfants Malades Université Paris Descartes
Visceral leishmaniasis: an endemic disease with global impact Professor Olivier Lortholary, MD, PhD Department of Infectious and Tropical diseases Hôpital Necker-Enfants Malades Université Paris Descartes
Therapeutic Options for Visceral Leishmaniasis
 Drugs (2013) 73:1863 1888 DOI 10.1007/s40265-013-0133-0 REVIEW ARTICLE Therapeutic Options for Visceral Leishmaniasis Begoña Monge-Maillo Rogelio López-Vélez Published online: 30 October 2013 Ó The Author(s)
Drugs (2013) 73:1863 1888 DOI 10.1007/s40265-013-0133-0 REVIEW ARTICLE Therapeutic Options for Visceral Leishmaniasis Begoña Monge-Maillo Rogelio López-Vélez Published online: 30 October 2013 Ó The Author(s)
Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A Case Report
 J HEALTH POPUL NUTR 2014 Jun;32(2):372-376 ISSN 1606-0997 $ 5.00+0.20 INTERNATIONAL CENTRE FOR DIARRHOEAL DISEASE RESEARCH, BANGLADESH CASE STUDY Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A
J HEALTH POPUL NUTR 2014 Jun;32(2):372-376 ISSN 1606-0997 $ 5.00+0.20 INTERNATIONAL CENTRE FOR DIARRHOEAL DISEASE RESEARCH, BANGLADESH CASE STUDY Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A
BIO Parasitology Spring 2009
 BIO 475 - Parasitology Spring 2009 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 5 Discovery of the Disease In 1924 the Kala-Azar Commission noted that the distribution
BIO 475 - Parasitology Spring 2009 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 5 Discovery of the Disease In 1924 the Kala-Azar Commission noted that the distribution
PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia)
 PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia) A 37-year-old woman, who had traveled to New Guinea for several weeks, presented to the medical clinic with fever, chills, and rigors within
PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia) A 37-year-old woman, who had traveled to New Guinea for several weeks, presented to the medical clinic with fever, chills, and rigors within
Laboratory diagnosis of Blood and tissue flagellates
 Laboratory diagnosis of Blood and tissue flagellates (Leishmania and trypanosma) Sarah Alharbi Clinical Laboratory department Collage of Applied Medical Sciences King Saud University Leishmania and trypanosma:
Laboratory diagnosis of Blood and tissue flagellates (Leishmania and trypanosma) Sarah Alharbi Clinical Laboratory department Collage of Applied Medical Sciences King Saud University Leishmania and trypanosma:
Epidemiological Study of Cutaneous Leishmaniasis in Tuz
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 477-483 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.056
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 477-483 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.056
Departments of Dermatology, Venereology and Leprosy and *Microbiology, Indira Gandhi Medical College, Shimla, India.
 Net Study Comparative efþ cacy of intralesional sodium stibogluconate (SSG) alone and its combination with intramuscular SSG to treat localized cutaneous leishmaniasis: Results of a pilot study Ajeet K.
Net Study Comparative efþ cacy of intralesional sodium stibogluconate (SSG) alone and its combination with intramuscular SSG to treat localized cutaneous leishmaniasis: Results of a pilot study Ajeet K.
A Novel Noninvasive Method for Diagnosis of Visceral Leishmaniasis by. rk39 Test in Sputum Samples
 JCM Accepts, published online ahead of print on 0 June 00 J. Clin. Microbiol. doi:0./jcm.00-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
JCM Accepts, published online ahead of print on 0 June 00 J. Clin. Microbiol. doi:0./jcm.00-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
Kala-Azar- Treatment Update
 JOURNAL OF ADVANCES IN MEDICINE (JAM) DOI: 10.5958/2319-4324.2016.00002.X REVIEW PAPER Kala-Azar- Treatment Update Anup Singh Associate Professor, Department of Medicine, Institute of Medical Sciences,
JOURNAL OF ADVANCES IN MEDICINE (JAM) DOI: 10.5958/2319-4324.2016.00002.X REVIEW PAPER Kala-Azar- Treatment Update Anup Singh Associate Professor, Department of Medicine, Institute of Medical Sciences,
Recommendations for Coping with Leishmaniasis: A Review of Control Strategies. Centro de Convenções de Reboças Red Room 17: 00h
 Recommendations for Coping with Leishmaniasis: A Review of Control Strategies Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000
Recommendations for Coping with Leishmaniasis: A Review of Control Strategies Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000
Laboratory investigation of Cutaneous Leishmaniasis in Karachi
 Laboratory investigation of Cutaneous Leishmaniasis in Karachi Pages with reference to book, From 248 To 250 G.M. Rajpar, M.A. Khan, A. Hafiz ( Department of Microbiology, Jinnah Postgraduate Medical Centre,
Laboratory investigation of Cutaneous Leishmaniasis in Karachi Pages with reference to book, From 248 To 250 G.M. Rajpar, M.A. Khan, A. Hafiz ( Department of Microbiology, Jinnah Postgraduate Medical Centre,
Leishmaniasis. By Joseph Knight, PA-C. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India.
 Leishmaniasis By Joseph Knight, PA-C Objectives 1. Identify the two types of leishmaniasis. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India. 3. Discuss how
Leishmaniasis By Joseph Knight, PA-C Objectives 1. Identify the two types of leishmaniasis. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India. 3. Discuss how
Blood Smears Only 6 October Sample Preparation and Quality Control 15B-K
 NEW YORK STATE Parasitology Proficiency Testing Program Blood Smears Only 6 October 5 The purpose of the New York State Proficiency Testing Program in the category of Parasitology - Blood Smears Only is
NEW YORK STATE Parasitology Proficiency Testing Program Blood Smears Only 6 October 5 The purpose of the New York State Proficiency Testing Program in the category of Parasitology - Blood Smears Only is
WMLN Case Study. Necrotizing Palate Biopsy Specimen. Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP)
 WMLN Case Study Necrotizing Palate Biopsy Specimen Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP) 44 year old male from Honduras Immigrated to US 12 years ago to WI 4 years ago Seen
WMLN Case Study Necrotizing Palate Biopsy Specimen Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP) 44 year old male from Honduras Immigrated to US 12 years ago to WI 4 years ago Seen
Buruli ulcer disease. Epidemiology and transmission l Clinical manifestations and diagnosis l Treatment. Chapter 2
 Epidemiology and transmission l Clinical manifestations and diagnosis l Treatment Chapter 2 KEY POINTS Buruli ulcer is an infection caused by an organism called Mycobacterium ulcerans that lives in the
Epidemiology and transmission l Clinical manifestations and diagnosis l Treatment Chapter 2 KEY POINTS Buruli ulcer is an infection caused by an organism called Mycobacterium ulcerans that lives in the
ISPUB.COM. Cutaneous Leishmaniasis in Iran. C Yazdi, M Narmani, B Sadri INTRODUCTION CASE 1 CASE 2
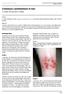 ISPUB.COM The Internet Journal of Infectious Diseases Volume 3 Number 1 Cutaneous Leishmaniasis in Iran C Yazdi, M Narmani, B Sadri Citation C Yazdi, M Narmani, B Sadri. Cutaneous Leishmaniasis in Iran.
ISPUB.COM The Internet Journal of Infectious Diseases Volume 3 Number 1 Cutaneous Leishmaniasis in Iran C Yazdi, M Narmani, B Sadri Citation C Yazdi, M Narmani, B Sadri. Cutaneous Leishmaniasis in Iran.
JMSCR Volume 03 Issue 01 Page January 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Seroprevalence of HBV among HIV Patients and Blood Donors Author Dr. Vedavati B I 1, Dr. Amrutha Kumari B 2, Dr. Venkatesha D 3 Mysore
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Seroprevalence of HBV among HIV Patients and Blood Donors Author Dr. Vedavati B I 1, Dr. Amrutha Kumari B 2, Dr. Venkatesha D 3 Mysore
Children with Visceral Leishmaniasis Presented to Omdurman Emergency Hospital for Children
 Original Article Children with Visceral Leishmaniasis Presented to Omdurman Emergency Hospital for Children Elfakey Walyeldinl, Ahmed Muawial, Mohamed Abdurrahman2 and Suwar M 03 Department of Paediatrics
Original Article Children with Visceral Leishmaniasis Presented to Omdurman Emergency Hospital for Children Elfakey Walyeldinl, Ahmed Muawial, Mohamed Abdurrahman2 and Suwar M 03 Department of Paediatrics
A Comparison of Miltefosine and Sodium. Ritmeijer, K; Dejenie, A; Assefa, Y; Hundie, T B; Mesure, J; Boots, G; den Boer, M; Davidson, R N
 MSF Field Research A Comparison of and Sodium Stibogluconate for Treatment of Visceral Leishmaniasis in an Ethiopian Population with High Prevalence of HIV Infection. Authors Citation Ritmeijer, K; Dejenie,
MSF Field Research A Comparison of and Sodium Stibogluconate for Treatment of Visceral Leishmaniasis in an Ethiopian Population with High Prevalence of HIV Infection. Authors Citation Ritmeijer, K; Dejenie,
Leishmaniasis. CDR R.L. Gutierrez Oct 2014
 Leishmaniasis CDR R.L. Gutierrez Oct 2014 Overview Protozoan parasite(s) of tissue and WBCs Many species / Many Syndromes (Cutaneous / Visceral) Pathogen: Location - Old World vs. New World Host: Immune
Leishmaniasis CDR R.L. Gutierrez Oct 2014 Overview Protozoan parasite(s) of tissue and WBCs Many species / Many Syndromes (Cutaneous / Visceral) Pathogen: Location - Old World vs. New World Host: Immune
Class 9 th Why do we fall ill?
 Class 9 th Why do we fall ill? Health: health is a state of physical, mental and social well being. The health of all individuals is dependent on their physical environment, social environment, and their
Class 9 th Why do we fall ill? Health: health is a state of physical, mental and social well being. The health of all individuals is dependent on their physical environment, social environment, and their
Invest in the future, defeat malaria
 Invest in the future, defeat malaria Malaria is caused by parasites from the genus Plasmodium, which are spread to people by infected mosquitoes. There are five species of Plasmodium that can infect humans.
Invest in the future, defeat malaria Malaria is caused by parasites from the genus Plasmodium, which are spread to people by infected mosquitoes. There are five species of Plasmodium that can infect humans.
Eradication of Guinea Worm in Ethiopia. Ayaan Omar. George Mason University. GCH Health and Environment, Fall 2014, Due: December 3, 2014
 Eradication of Guinea Worm in Ethiopia 1 Eradication of Guinea Worm in Ethiopia Ayaan Omar George Mason University GCH 360-002 - Health and Environment, Fall 2014, Due: December 3, 2014 Introduction Eradication
Eradication of Guinea Worm in Ethiopia 1 Eradication of Guinea Worm in Ethiopia Ayaan Omar George Mason University GCH 360-002 - Health and Environment, Fall 2014, Due: December 3, 2014 Introduction Eradication
Iranian J Parasitol: Vol. 8, No.3, July -Sep 2013, pp Iranian J Parasitol. Open access Journal at ijpa.tums.ac.ir
 Iranian J Parasitol: Vol. 8, No.3, July -Sep 2013, pp.396-401 Iranian J Parasitol Tehran University of Medical Sciences Publication http:// tums.ac.ir Open access Journal at http:// ijpa.tums.ac.ir Iranian
Iranian J Parasitol: Vol. 8, No.3, July -Sep 2013, pp.396-401 Iranian J Parasitol Tehran University of Medical Sciences Publication http:// tums.ac.ir Open access Journal at http:// ijpa.tums.ac.ir Iranian
Cutaneous leishmaniasis: advances in disease pathogenesis, diagnostics and therapeutics
 Clinical dermatology Review article CED Clinical and Experimental Dermatology Cutaneous leishmaniasis: advances in disease pathogenesis, diagnostics and therapeutics M. Ameen Royal Free Hospital, Royal
Clinical dermatology Review article CED Clinical and Experimental Dermatology Cutaneous leishmaniasis: advances in disease pathogenesis, diagnostics and therapeutics M. Ameen Royal Free Hospital, Royal
A comparative study of the effect on healing of ulcer using silver dressing
 International Surgery Journal Khandelwal AK et al. Int Surg J. 2016 May;3(2):768-775 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20160493
International Surgery Journal Khandelwal AK et al. Int Surg J. 2016 May;3(2):768-775 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20160493
Elimination of VL in the Indian subcontinent is it achievable?
 Elimination of VL in the Indian subcontinent is it achievable? P Das Rajendra Memorial Research Institute, Patna Jorge Alvar DNDi, Geneva Bhawna Sharma DNDi, India Leishmaniasis 350 million at risk worldwide
Elimination of VL in the Indian subcontinent is it achievable? P Das Rajendra Memorial Research Institute, Patna Jorge Alvar DNDi, Geneva Bhawna Sharma DNDi, India Leishmaniasis 350 million at risk worldwide
~Trichinella Spiralis:
 Musculoskeletal System **Today we are going to talk about the parasites that affect the musculoskeletal system ~Trichinella Spiralis: It s a small nematode that measures to about 2-3mm in length. In general
Musculoskeletal System **Today we are going to talk about the parasites that affect the musculoskeletal system ~Trichinella Spiralis: It s a small nematode that measures to about 2-3mm in length. In general
VIRAL HEPATITIS: SITUATION ANALYSIS AND PERSPECTIVES IN THE AFRICAN REGION. Report of the Secretariat. CONTENTS Paragraphs BACKGROUND...
 8 April 2014 REGIONAL COMMITTEE FOR AFRICA ORIGINAL: ENGLISH PROGRAMME SUBCOMMITTEE Sixty-fourth session Brazzaville, Republic of Congo, 9 11 June 2014 Provisional agenda item 6 VIRAL HEPATITIS: SITUATION
8 April 2014 REGIONAL COMMITTEE FOR AFRICA ORIGINAL: ENGLISH PROGRAMME SUBCOMMITTEE Sixty-fourth session Brazzaville, Republic of Congo, 9 11 June 2014 Provisional agenda item 6 VIRAL HEPATITIS: SITUATION
What is Kala-azar? What are Signs & Symptoms of Kala-Azar?
 What is Kala-azar? Kala-azar is a slow progressing indigenous disease caused by a protozoan parasite of genus Leishmania In India Leishmania donovani is the only parasite causing this disease The parasite
What is Kala-azar? Kala-azar is a slow progressing indigenous disease caused by a protozoan parasite of genus Leishmania In India Leishmania donovani is the only parasite causing this disease The parasite
VIRAL HEPATITIS: SITUATION ANALYSIS AND PERSPECTIVES IN THE AFRICAN REGION. Report of the Secretariat. CONTENTS Paragraphs BACKGROUND...
 5 November 2014 REGIONAL COMMITTEE FOR AFRICA ORIGINAL: ENGLISH Sixty-fourth session Cotonou, Republic of Benin, 3 7 November 2014 Provisional agenda item 11 VIRAL HEPATITIS: SITUATION ANALYSIS AND PERSPECTIVES
5 November 2014 REGIONAL COMMITTEE FOR AFRICA ORIGINAL: ENGLISH Sixty-fourth session Cotonou, Republic of Benin, 3 7 November 2014 Provisional agenda item 11 VIRAL HEPATITIS: SITUATION ANALYSIS AND PERSPECTIVES
Evaluation of rk28 antigen for serodiagnosis of visceral Leishmaniasis in India
 ORIGINAL ARTICLE TROPICAL AND PARASITIC DISEASES Evaluation of rk8 antigen for serodiagnosis of visceral Leishmaniasis in India M. Vaish, A. Bhatia, S. G. Reed, J. Chakravarty and S. Sundar ) Department
ORIGINAL ARTICLE TROPICAL AND PARASITIC DISEASES Evaluation of rk8 antigen for serodiagnosis of visceral Leishmaniasis in India M. Vaish, A. Bhatia, S. G. Reed, J. Chakravarty and S. Sundar ) Department
Topical effectiveness of different concentrations of nanosilver solution on Leishmania major lesions in Balb/c mice
 J Vector Borne Dis 49, Dec 2012, pp. 249 253 Topical effectiveness of different concentrations of nanosilver solution on Leishmania major lesions in Balb/c mice Mohammad Ali Nilforoushzadeh 1, Leila Shirani-Bidabadi
J Vector Borne Dis 49, Dec 2012, pp. 249 253 Topical effectiveness of different concentrations of nanosilver solution on Leishmania major lesions in Balb/c mice Mohammad Ali Nilforoushzadeh 1, Leila Shirani-Bidabadi
 Malaria parasites Malaria parasites are micro-organisms that belong to the genus Plasmodium. There are more than 100 species of Plasmodium, which can infect many animal species such as reptiles, birds,
Malaria parasites Malaria parasites are micro-organisms that belong to the genus Plasmodium. There are more than 100 species of Plasmodium, which can infect many animal species such as reptiles, birds,
Visceral childhood leishmaniasis in southern Turkey: experience of twenty years
 The Turkish Journal of Pediatrics 2009; 51: 1-5 Original Visceral childhood leishmaniasis in southern Turkey: experience of twenty years Oğuz Dursun 1, Seyhan Erişir 2, Akif Yeşilipek 3 Divisions of 1
The Turkish Journal of Pediatrics 2009; 51: 1-5 Original Visceral childhood leishmaniasis in southern Turkey: experience of twenty years Oğuz Dursun 1, Seyhan Erişir 2, Akif Yeşilipek 3 Divisions of 1
Leishmaniasis. MAJ Kris Paolino September 2014
 Leishmaniasis MAJ Kris Paolino September 2014 Thanks to COL (Ret) Kent Kester MAJ Leyi Lin http://www.niaid.nih.gov/topics/leishmaniasis History Sir William Boog Leishman (1865-1926) Matriculated at the
Leishmaniasis MAJ Kris Paolino September 2014 Thanks to COL (Ret) Kent Kester MAJ Leyi Lin http://www.niaid.nih.gov/topics/leishmaniasis History Sir William Boog Leishman (1865-1926) Matriculated at the
CUTANEOUS LEISHMANIASIS
 CUTANEOUS LEISHMANIASIS Why are you neglecting me? A WHO initiative to control Cutaneous Leishmaniasis in selected Old World areas This document has been produced as the result of a WHO Informal Consultative
CUTANEOUS LEISHMANIASIS Why are you neglecting me? A WHO initiative to control Cutaneous Leishmaniasis in selected Old World areas This document has been produced as the result of a WHO Informal Consultative
Study Plan: Screening
 Phase 1 with Sporozoite Challenge Open-Label Dose-Escalation Safety, Reactogenicity, Immunogenicity, and Efficacy of the Vaccine Candidate Plasmodium falciparum Malaria Protein (FMP012), an E coli-expressed
Phase 1 with Sporozoite Challenge Open-Label Dose-Escalation Safety, Reactogenicity, Immunogenicity, and Efficacy of the Vaccine Candidate Plasmodium falciparum Malaria Protein (FMP012), an E coli-expressed
Efficacy of Miltefosine in the Treatment of Visceral Leishmaniasis in India After a Decade of Use
 MAJOR ARTICLE Efficacy of Miltefosine in the Treatment of Visceral Leishmaniasis in India After a Decade of Use Shyam Sundar, 1,a Anup Singh, 1,a Madhukar Rai, 1 Vijay K. Prajapati, 1 Avinash K. Singh,
MAJOR ARTICLE Efficacy of Miltefosine in the Treatment of Visceral Leishmaniasis in India After a Decade of Use Shyam Sundar, 1,a Anup Singh, 1,a Madhukar Rai, 1 Vijay K. Prajapati, 1 Avinash K. Singh,
Research Methods and Analysis
 Research Methods and Analysis Lecture 9 Analytic Experimental Studies Randomized Study Design Dr. Sayed Bahawaddin Hashemi, MD, MPH, ASCP Experimental Randomized Quasi Randomized Controlled Trial A study
Research Methods and Analysis Lecture 9 Analytic Experimental Studies Randomized Study Design Dr. Sayed Bahawaddin Hashemi, MD, MPH, ASCP Experimental Randomized Quasi Randomized Controlled Trial A study
References for Application for inclusion of paromomycin in the WHO Model List of Essential Medicines
 6 (a) Visceral leishmaniasis disease burden. Desjeux P. Leishmaniasis: current situation and new perspectives. Comp Immunol Microbiol Infect Dis 2004:27:305-18. Sundar S, Murray HW. Availability of miltefosine
6 (a) Visceral leishmaniasis disease burden. Desjeux P. Leishmaniasis: current situation and new perspectives. Comp Immunol Microbiol Infect Dis 2004:27:305-18. Sundar S, Murray HW. Availability of miltefosine
Leishmaniasis impact and treatment access
 REVIEW 10.1111/j.1469-0691.2011.03635.x Leishmaniasis impact and treatment access M. den Boer, D. Argaw, J. Jannin and J. Alvar Leishmaniasis Control Programme, WHO/IDM. Av. Appia, Geneva, Switzerland
REVIEW 10.1111/j.1469-0691.2011.03635.x Leishmaniasis impact and treatment access M. den Boer, D. Argaw, J. Jannin and J. Alvar Leishmaniasis Control Programme, WHO/IDM. Av. Appia, Geneva, Switzerland
Prevalent opportunistic infections associated with HIV-positive children 0-5 years in Benin city, Nigeria
 Malaysian Journal of Microbiology, Vol 4(2) 2008, pp. 11-14 http://dx.doi.org/10.21161/mjm.11508 Prevalent opportunistic infections associated with HIV-positive children 0-5 years in Benin city, Nigeria
Malaysian Journal of Microbiology, Vol 4(2) 2008, pp. 11-14 http://dx.doi.org/10.21161/mjm.11508 Prevalent opportunistic infections associated with HIV-positive children 0-5 years in Benin city, Nigeria
POST KALA-AZAR DERMAL LEISHMANIASIS WITH ULCERATION ON FOOT: AN ATYPICAL CASE PRESENTATION SUCCESSFULLY TREATED WITH MILTEFOSINE
 American Journal of Infectious Diseases 10 (2): 50-55, 2014 ISSN: 1553-6203 2014 Science Publication doi:10.3844/ajidsp.2014.50.55 Published Online 10 (2) 2014 (http://www.thescipub.com/ajid.toc) POST
American Journal of Infectious Diseases 10 (2): 50-55, 2014 ISSN: 1553-6203 2014 Science Publication doi:10.3844/ajidsp.2014.50.55 Published Online 10 (2) 2014 (http://www.thescipub.com/ajid.toc) POST
Communicable Diseases
 Chapter 23 Communicable Diseases Disease that s spread from one living organism to another or through the environment Infection occurs when pathogens in the body multiply and damage body cells Main Pathogens
Chapter 23 Communicable Diseases Disease that s spread from one living organism to another or through the environment Infection occurs when pathogens in the body multiply and damage body cells Main Pathogens
Analytical evaluation of Malaria Research Papers in MEDLINE & SCI during the period of &
 Panigrahi, Mukherjee and Srivastava 1 Analytical evaluation of Malaria Research Papers in & during the period of 1986-9 & 21-5. Panigrahi BK *, Mukherjee T and Srivastava D 28 July 28 Abstract: Vector-borne
Panigrahi, Mukherjee and Srivastava 1 Analytical evaluation of Malaria Research Papers in & during the period of 1986-9 & 21-5. Panigrahi BK *, Mukherjee T and Srivastava D 28 July 28 Abstract: Vector-borne
Safety and immunogenicity of a new Leishmania vaccine candidate ChAd63-KH
 Safety and immunogenicity of a new Leishmania vaccine candidate ChAd63-KH Study Acronym: LEISH2a ClinicalTrials.gov ID: NCT02894008 25th LEAP meeting, 3-5 Sep 2018 Entebbe, Uganda Ahmed M Musa MBBS, DTM
Safety and immunogenicity of a new Leishmania vaccine candidate ChAd63-KH Study Acronym: LEISH2a ClinicalTrials.gov ID: NCT02894008 25th LEAP meeting, 3-5 Sep 2018 Entebbe, Uganda Ahmed M Musa MBBS, DTM
Series Editors Samuel J. Black, University of Massachusetts, Amherst, MA, US.A. J. Richard Seed, University of North Carolina, Chapel Hill, NC, US.A.
 LEISHMANIA World Class Parasites VOLUME 4 Volumes in the World Class Parasites book series are written for researchers, students and scholars who enjoy reading about excellent research on problems of global
LEISHMANIA World Class Parasites VOLUME 4 Volumes in the World Class Parasites book series are written for researchers, students and scholars who enjoy reading about excellent research on problems of global
Phlebotomus argentipes. Amphotericin B has long been recognized as a powerful anti-kala-azar drug
 A STUDY OF EFFICACY AND ADVERSE DRUG REACTIONS OF CONVENTIONAL AMPHOTERICIN B IN THE TREATMENT OF KALA-AZAR Rajesh Kumar Pandey 1, S. N. Singh 2, Bharat Kumar 3, Kashif Shahnawaz 4 HOW TO CITE THIS ARTICLE:
A STUDY OF EFFICACY AND ADVERSE DRUG REACTIONS OF CONVENTIONAL AMPHOTERICIN B IN THE TREATMENT OF KALA-AZAR Rajesh Kumar Pandey 1, S. N. Singh 2, Bharat Kumar 3, Kashif Shahnawaz 4 HOW TO CITE THIS ARTICLE:
Cutaneous Leishmaniasis : Global overview
 Cutaneous Leishmaniasis : Global overview Meeting of stakeholders for selected Health R&D Demostration Projects, 7-10 May 2014, WHO, Geneva Dr. Daniel Argaw Dagne, NTD/WHO CSR - DDC AFRO Leishmaniasis
Cutaneous Leishmaniasis : Global overview Meeting of stakeholders for selected Health R&D Demostration Projects, 7-10 May 2014, WHO, Geneva Dr. Daniel Argaw Dagne, NTD/WHO CSR - DDC AFRO Leishmaniasis
Dr Monique Wasunna MBChB, PhD, DTM&H DNDi Africa Regional office. WorldLeish6 Congress, Toledo Spain
 Phase II Randomized Clinical Trial of the Efficacy and Safety of AmBisome in Combination with SSG or Miltefosine versus Miltefosine Monotherapy for African VL Dr Monique Wasunna MBChB, PhD, DTM&H DNDi
Phase II Randomized Clinical Trial of the Efficacy and Safety of AmBisome in Combination with SSG or Miltefosine versus Miltefosine Monotherapy for African VL Dr Monique Wasunna MBChB, PhD, DTM&H DNDi
CASE OF CUTANEOUS LEISHMANIASIS OF THE LID*
 Brit. J. Ophthal. (1965) 49, 542 CASE OF CUTANEOUS LEISHMANIASIS OF THE LID* BY GWYN MORGAN Department ofpathology, Institute of Ophthalmology, University of London THE lid is involved only in about 2
Brit. J. Ophthal. (1965) 49, 542 CASE OF CUTANEOUS LEISHMANIASIS OF THE LID* BY GWYN MORGAN Department ofpathology, Institute of Ophthalmology, University of London THE lid is involved only in about 2
Fact sheet. Yellow fever
 Fact sheet Key facts is an acute viral haemorrhagic disease transmitted by infected mosquitoes. The yellow in the name refers to the jaundice that affects some patients. Up to 50% of severely affected
Fact sheet Key facts is an acute viral haemorrhagic disease transmitted by infected mosquitoes. The yellow in the name refers to the jaundice that affects some patients. Up to 50% of severely affected
Aperito Journal of Bacteriology, Virology and Parasitology. Therapeutic Potential of Nanoparticulate System for Treatment. of Protozoan Infection
 Aperito Journal of Bacteriology, Virology and Parasitology Received: Sep 19, 2014 Accepted: Oct 08, 2014 Published: Oct 12, 2014 http://dx.doi.org/10.14437/ajbvp-1-102 Editorial Arghya Bandyopadhyay, Aperito
Aperito Journal of Bacteriology, Virology and Parasitology Received: Sep 19, 2014 Accepted: Oct 08, 2014 Published: Oct 12, 2014 http://dx.doi.org/10.14437/ajbvp-1-102 Editorial Arghya Bandyopadhyay, Aperito
AFRICAN JOURNAL OF CLINICAL AND EXPERIMENTAL MICROBIOLOGY SEPTEMBER 2008 ISBN X VOL 9 No 3
 ORIGINAL ARTICLE AFRICAN JOURNAL OF CLINICAL AND EXPERIMENTAL MICROBIOLOGY SEPTEMBER 2008 ISBN 1595-689X VOL 9 No 3 AJCEM/200758/20815 COPYRIGHT 2008 AFR. J. CLN. EXPER. MICROBIOL. 9 (3): 110-114 -http://www.ajol.info/journals/ajcem
ORIGINAL ARTICLE AFRICAN JOURNAL OF CLINICAL AND EXPERIMENTAL MICROBIOLOGY SEPTEMBER 2008 ISBN 1595-689X VOL 9 No 3 AJCEM/200758/20815 COPYRIGHT 2008 AFR. J. CLN. EXPER. MICROBIOL. 9 (3): 110-114 -http://www.ajol.info/journals/ajcem
Aetiology Of Upper Gastrointestinal Bleeding In North- Eastern Nigeria: A Retrospective Endoscopic Study
 ISPUB.COM The Internet Journal of Third World Medicine Volume 8 Number 2 Aetiology Of Upper Gastrointestinal Bleeding In North- Eastern Nigeria: A Retrospective Endoscopic S Mustapha, N Ajayi, A Shehu
ISPUB.COM The Internet Journal of Third World Medicine Volume 8 Number 2 Aetiology Of Upper Gastrointestinal Bleeding In North- Eastern Nigeria: A Retrospective Endoscopic S Mustapha, N Ajayi, A Shehu
Paromomycin for the Treatment of Visceral Leishmaniasis in Sudan: A Randomized, Open-Label, Dose-Finding Study
 Paromomycin for the Treatment of Visceral Leishmaniasis in Sudan: A Randomized, Open-Label, Dose-Finding Study Ahmed M. Musa 1 *, Brima Younis 1, Ahmed Fadlalla 2, Catherine Royce 3, Manica Balasegaram
Paromomycin for the Treatment of Visceral Leishmaniasis in Sudan: A Randomized, Open-Label, Dose-Finding Study Ahmed M. Musa 1 *, Brima Younis 1, Ahmed Fadlalla 2, Catherine Royce 3, Manica Balasegaram
Table of Contents GUIDELINES FOR THE TREATMENT AND PREVENTION OF CUTANEOUS LEISHMANIASIS IN PAKISTAN
 GUIDELINES FOR THE TREATMENT AND PREVENTION OF CUTANEOUS LEISHMANIASIS IN PAKISTAN Table of Contents Acknowledgements 2 Introduction 3 1. Leishmaniasis 4 1.1. Disease incidence 5 1.2. Leishmaniasis in
GUIDELINES FOR THE TREATMENT AND PREVENTION OF CUTANEOUS LEISHMANIASIS IN PAKISTAN Table of Contents Acknowledgements 2 Introduction 3 1. Leishmaniasis 4 1.1. Disease incidence 5 1.2. Leishmaniasis in
Treatment of Disseminated Leishmaniasis With Liposomal Amphotericin B
 MAJOR ARTICLE Treatment of Disseminated Leishmaniasis With Liposomal Amphotericin B Paulo R. L. Machado, 1,2 Maria Elisa A. Rosa, 1 Luís H. Guimarães, 1,2 Fernanda V. O. Prates, 1 Adriano Queiroz, 1,2
MAJOR ARTICLE Treatment of Disseminated Leishmaniasis With Liposomal Amphotericin B Paulo R. L. Machado, 1,2 Maria Elisa A. Rosa, 1 Luís H. Guimarães, 1,2 Fernanda V. O. Prates, 1 Adriano Queiroz, 1,2
DTA3/COFUND Programme Research Project Proforma
 Page 1 General Information Project Code Partner University Faculty/School/Department/Research Centres First supervisor Please provide name and weblink Second supervisor Please provide name and weblink
Page 1 General Information Project Code Partner University Faculty/School/Department/Research Centres First supervisor Please provide name and weblink Second supervisor Please provide name and weblink
Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels
 Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels A M EL Hassan Institute of Endemic Diseases University of Khartoum Introduction PKDL is a VL related
Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels A M EL Hassan Institute of Endemic Diseases University of Khartoum Introduction PKDL is a VL related
Improving the prevention, diagnosis and clinical management of sepsis
 SEVENTIETH WORLD HEALTH ASSEMBLY A70/13 Provisional agenda item 12.2 13 April 2017 Improving the prevention, diagnosis and clinical management of sepsis Report by the Secretariat 1. The Executive Board
SEVENTIETH WORLD HEALTH ASSEMBLY A70/13 Provisional agenda item 12.2 13 April 2017 Improving the prevention, diagnosis and clinical management of sepsis Report by the Secretariat 1. The Executive Board
Downloaded from
 Class IX: Biology Chapter: Why do we fall ill Chapter Notes Key learnings: 1) Our body s well-being is dependent on the proper functioning of its cells and tissues. 2) All our body parts and activities
Class IX: Biology Chapter: Why do we fall ill Chapter Notes Key learnings: 1) Our body s well-being is dependent on the proper functioning of its cells and tissues. 2) All our body parts and activities
Multiple Choice Questions
 Multiple Choice Questions 1. Which one of the following is not a viral disease? (a) Dengue (b) AIDS (c) Typhoid (d) Influenza 2. Which one of the following is not a bacterial disease? (a) Cholera (b) Tuberculosis
Multiple Choice Questions 1. Which one of the following is not a viral disease? (a) Dengue (b) AIDS (c) Typhoid (d) Influenza 2. Which one of the following is not a bacterial disease? (a) Cholera (b) Tuberculosis
Flagellates. Dr. Anuluck Junkum PARA
 Flagellates Dr. Anuluck Junkum PARA 317242 Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of pathogenic flagellates Classification of Protozoa Based on locomotive
Flagellates Dr. Anuluck Junkum PARA 317242 Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of pathogenic flagellates Classification of Protozoa Based on locomotive
VISERAL LEISHMANIASI S (KALA-AZAR)
 VISERAL LEISHMANIASI S (KALA-AZAR) :OUTLINES DEFINITION. EPIDEMIOLOGY. PARASITE & VECTOR. PATHOLOGY CLINICAL & LIFE CYCLE. PICTURE. COMPLICATIONS. DIAGNOSIS. INVESTIGATIONS. MANAGEMENT TREATMENT S CONTROL.
VISERAL LEISHMANIASI S (KALA-AZAR) :OUTLINES DEFINITION. EPIDEMIOLOGY. PARASITE & VECTOR. PATHOLOGY CLINICAL & LIFE CYCLE. PICTURE. COMPLICATIONS. DIAGNOSIS. INVESTIGATIONS. MANAGEMENT TREATMENT S CONTROL.
Response to Treatment in Sputum Smear Positive Pulmonary Tuberculosis Patients In relation to Human Immunodeficiency Virus in Kano, Nigeria.
 Response to Treatment in Sputum Smear Positive Pulmonary Tuberculosis Patients In relation to Human Immunodeficiency Virus in Kano, Nigeria. Yusuf Mohammed, Mukhtar Dauda, Ifeanyi Oyeyi TB/HIV Unit, International
Response to Treatment in Sputum Smear Positive Pulmonary Tuberculosis Patients In relation to Human Immunodeficiency Virus in Kano, Nigeria. Yusuf Mohammed, Mukhtar Dauda, Ifeanyi Oyeyi TB/HIV Unit, International
Protozoa from tissues. Leishmania spp. Naegleria fowleri Toxoplasma gondii Trichomonas vaginalis Trypanosoma spp.
 Protozoa from tissues Leishmania spp. Naegleria fowleri Toxoplasma gondii Trichomonas vaginalis Trypanosoma spp. Leishmaniasis Leishmania infantum, Leishmania donovani, in macrophages of man. Female sandflies:
Protozoa from tissues Leishmania spp. Naegleria fowleri Toxoplasma gondii Trichomonas vaginalis Trypanosoma spp. Leishmaniasis Leishmania infantum, Leishmania donovani, in macrophages of man. Female sandflies:
Application for Inclusion of MILTEFOSINE on WHO Model List of Essential Medicines:
 Application for Inclusion of MILTEFOSINE on WHO Model List of Essential Medicines: Comments re Feb 2011 reviews of the v 2010 application February 23, 2011 1. The application and its review In v 2010,
Application for Inclusion of MILTEFOSINE on WHO Model List of Essential Medicines: Comments re Feb 2011 reviews of the v 2010 application February 23, 2011 1. The application and its review In v 2010,
