Leishmaniasis. By Joseph Knight, PA-C. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India.
|
|
|
- Cecil Carpenter
- 5 years ago
- Views:
Transcription
1 Leishmaniasis By Joseph Knight, PA-C Objectives 1. Identify the two types of leishmaniasis. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India. 3. Discuss how the leishmaniasis protozoon infects the human body and how it spreads. 4. Describe the two classes of drugs approved by the Food and Drug Administration (FDA) for the treatment of leishmaniasis. 5. Explain why soldiers deployed to areas endemic for leishmaniasis tend to have a lower morbidity rate than do tourists. Introduction United States military activity in the Middle East carries with it not only war wounds, but infections and other diseases which are brought back to the U.S. when troops return. One of the diseases many soldiers may contract while deployed in the Middle East is leishmaniasis. Of 20,000 soldiers that returned to Fort Campbell, Kentucky in late 2003 and early 2004, five percent had skin complaints; of those five percent, twenty-five percent were diagnosed with cutaneous leishmaniasis. 1 It may not be unexpected to see patients with leishmaniasis in the civilian clinical or nursing setting once these soldiers are released from active military service and return to the civilian sector. Civilian travelers to other countries where leishmaniasis is endemic may also return to the U.S. with the disease. The differential diagnosis of any nonhealing ulcer on a patient who has traveled to such an area should include leishmaniasis. Leishmaniasis is an infection cause by protozoa belonging to the genus Leishmania, transmitted to humans by the bite of the female sand fly. The species that mainly affect humans are Leishmania donovani, which causes visceral leishmaniasis (also known as kala-azar, which is Hindi for black sickness or fever), while cutaneous leishmaniasis is caused by Leishmania tropica. Cutaneous leishmaniasis (CL) can reach epidemic proportions in a nonimmune population such as soldiers and tourists, and is maintained endemically in local mammals such as rodents and dogs. In visceral leishmaniasis (VL), parasites replicate in the endothelial system, such as the liver, spleen and bone marrow. The infection can remain asymptomatic or subclinical and can become clinically manifest with an acute, subacute or chronic course. In the classic kalaazar syndrome of VL, patients have potentially life-threatening disease, typically after an incubation period of weeks or months. The syndrome includes fever, marked malnutrition, hepatosplenomegaly and pancytopenia. 2
2 An estimated 12 million cases of visceral and cutaneous leishmaniasis occur worldwide each year 2, with approximately 100,000 deaths a year. 3,4 The cutaneous form of leishmaniasis is the most common, causing 50% to 75% of all new cases, while the visceral form is the most fatal, especially in persons infected with the HIV virus. 5 The number of leishmaniasis cases is increasing, mainly due to man-made environmental changes such as road building, lumbering and dam-building such as is seen in the Amazon rain forest. Continuing migration from rural to urban areas and continuing urbanization worldwide are among the primary causes for the increased exposure to the sand fly. Another risk factor is the movement of large populations into endemic areas. In the city of Kabul, Afghanistan, an estimated 270,000 cases of leishmaniasis occurred in 1996; this with a population of less than 2 million. In India, the resurgence of visceral leishmaniasis has occurred because of deficiencies in the control program. This has seen the emergence of resistant strains of the organism. 3 American troops returning from the Middle East war may unsuspectingly bring quiescent leishmaniasis with them, so it may be seen by clinicians in America whom have never seen a case of leishmaniasis. Life Cycle The life cycle involves a human host and the female sand fly (the vector) which transmits the parasite between vertebrate hosts (see Figure 1 at End of Course). In the vector the parasite develops into a form called the promastigote which reproduces asexually in the vector s gut, then migrates to the pharynx of the insect. Promastigotes are injected into the human host when the sand flea bites. The promastigotes then enter the cells of the human host and change into a form termed the amastigote. The amastigotes then reproduce in the human cell. When the cell is packed with amastigotes, it ruptures, where the amastigotes are then released to infect other cells. The symptoms and pathology of leishmaniasis are a result of the amastigotes killing the human cells. 6 Most infections are transmitted via a sand fly bite, but other potential methods of transmission are congenital, sexual contact, blood transfusion, needle-sharing and organ transplantation. 7 Leishmania tropica and L. major are the two primary causes of cutaneous leishmaniasis, L. tropica resides primarily in the urban areas, while L. major is generally found in the dry desert areas. 9 After two to eight weeks of incubation, an erythematous papule develops at the site of the bite, which eventually evolves into a nodule and then ulcerates and crusts over. Ulcers are typically large and painless. Secondary infection is not uncommon. 8,9,10 Most cutaneous lesions will eventually heal, leaving a depressed, disfiguring scar. Infected persons tend to form immunity to future infection. 11 Mucocutaneous leishmaniasis destroys the tissues of the upper respiratory tract. Lesions in this area usually develop by organisms which travel from other cutaneous sites. The progress of the disease is slow, methodical and destructive. Mucosal disease occurs in 1% to 5% of untreated patients, with lesions developing years or decades after the initial infection; therefore, children are rarely affected. Mucocutaneous leishmaniasis usually presents with respiratory symptoms
3 such as nasopharyngeal congestion which may cause epistaxis. The lesions then infiltrate the nasal mucosa and ulcerate, which will result in scarring and subsequent respiratory difficulty. 13 Visceral leishmaniasis can follow an acute or relatively asymptomatic course but is generally fatal if untreated. 13 The incubation period from time of exposure to the first indications of symptoms is ten days to greater than two years, but is usually three to eight months. Patients present with fever, hepatosplenomegaly and weight loss. 9 Other symptoms may appear, such as weakness, night sweats, anorexia, epistaxis and thinning hair. Since visceral leishmaniasis is becoming an important opportunistic infection in patients with HIV infection, all patients with visceral leishmaniasis should be tested for HIV. 14 Similarly, HIV-positive patients in endemic areas should be evaluated and followed for the development of the visceral form leishmaniasis. 9 Another form of leishmaniasis called viscerotropic is a subset of the visceral form. Viscerotropic leishmaniasis is caused by L. tropica, which is generally considered to be exclusive to the cutaneous form. Viscerotropic leishmaniasis was described by U.S. soldiers in Saudi Arabia during the Desert Storm and Desert Shield operations. Patients developed signs and symptoms of visceral leishmaniasis eight weeks to one year after arrival. Parasites found in bone marrow illustrate the ability of the Leishmania species to express itself in unexpected clinical forms. 15 Case Histories Patient A: A 23-year-old male graduate student in Ohio noted an ulceration on his left middle finger. He had visited the jungles of Panama one month earlier and was bitten by many insects. The ulcer became larger despite the administration of oral erythromycin and dicloxacillin. A month later the student was admitted to a regional hospital with a 2x2 cm indurated ulcer overlying the proximal interphalangeal joint. There was no evidence of lymphatic spread. A biopsy from the edge of the lesion showed an intense lymphohistiocytic infiltrate involving the entire dermis. Cultures for bacteria, fungi and mycobacteria were negative. He was treated with intravenous nafcillin and discharged on oral tetracycline. The lesion persisted, and three weeks later another biopsy was performed. The same histologic picture was seen and again, all cultures were negative. A serum specimen submitted to the Centers for Disease Control for Leishmania antibody testing had a titer of 1:16 by complement fixation (CF) and of 1:16 by indirect immunofluorescent antibody (IFA). The lesion continued to expand with subcutaneous nodules on the back of the hand extending up the arm. Epitrochlear and axillary adenopathy were present. A third biopsy was performed and submitted to Walter Reed Army Hospital for Leishmania culture. Growth of Leishmania braziliensis was reported several weeks later. The patient was treated with 10mg/kg/day sodium stibogluconate intravenously for 21 days. At the beginning of the treatment, the ulceration measured 4.8 cm x 3.5 cm; by the end of therapy the lesion had decreased in size by 75% and was granulating well, while the subcutaneous nodules on the hand and arm had resolved. Three months after the completion of therapy, the ulcer had completely healed with only minimal adenopathy remaining. 16
4 Patient B: A soldier having left Afghanistan approximately three months previously noted fevers of up to 1040 F in December of 2003, along with rigors, sweats, flushing and mild orthostasis in early January of During the course of his illness, the patient experienced fluctuating temperatures and lost 13 pounds of body weight. No leishmanial parasites were noted in lightmicroscopic examinations of cultures of bone marrow and liver-biopsy specimens. No leishmanial DNA was detected by genus-specific polymerase chain reaction (PCR) analysis 17 of the bone-marrow specimen. The findings in the splenic region of a whole-body Positron Emission Tomography (PET) scan were suggestive of lymphoma, and surgical splenectomy was briefly considered. In February, 2004, because of the continuing concern that the patient may have VL, the liver-biopsy specimen was reexamined by light microscopy; one definite and one probable leishmanial parasites were noted. The patient became afebrile after one week of antileishmanial therapy with a lipid formulation of amphotericin B. 18 Patient C: A soldier having left Afghanistan several months previously noted abrupt onset of fevers (maximum 1040 F), myalgias and abdominal pain in December of Unintentional loss of up to 25 pounds of body weight and anorexia accompanied the symptoms. The patient s symptoms worsened during the next six weeks. Leishmanial parasites were not found in lightmicroscopic examinations of the bone marrow and buffy-coat specimens, but were present in liver-biopsy specimens. During February 3 to 17, 2004, the patient was administered six courses of a lipid formulation of amphotericin B. Although his symptoms improved during and after the course of therapy, they worsened in late February. He was rehospitalized on March 5, 2004 with a temperature of 1020 F. Leishmanial parasites and DNA were detected by light-microscopic examination and genus-specific polymerases chain reaction (PCR) of a liver-biopsy specimen, while the test results for a bone-marrow specimen was negative. In addition, the PCR analysis of the liver specimen was positive for Leishmania donovani-l. infantum species complex, whereas the PCR results for the L. major were negative. On March 19th, a 28-day course of antileishmanial therapy was begun with the pentavalent antimonial compound sodium stibogluconate with an intravenous dose of 20mg/kg/day. 18 Treatment Sodium stibugluconate (available in English-speaking countries), and meglumine antimoniate (available in Latin American countries) are both of the pentavalent antimony class, and have been used for the treatment of leishmaniasis for over 50 years. These medications work by inhibiting adenosine triphosphate synthesis. These drugs are not ideal; difficult administration, toxicity and numerous side effects including arthralgias, pancreatitis and drug resistance can present a problem. 6,19 Side-effects usually resolve within a week of cessation of treatment and may not return upon resuming treatment. The lesions start resolving in about 20 days. 8 Dosage is 20 mg/kg/day, either intravenously or by intramuscular injection. Relapse of up to 30% has been reported in Kenya, while increasing resistance is being reported in India. Baseline ECG and blood tests should be done prior to the initiation of therapy. Liver function tests and renal function tests should be done weekly during treatment. 20
5 Systemic antifungal agents such as amphotericin B, ketoconazole and itraconazole are antifungal drugs with antileishmanial activity; however, close monitoring of blood tests is required to preclude severe hepatic, renal and hematological problems. Cure rates of greater than 90% has been shown with the use of amphotericin B; however, its high cost has prevented its use in areas where visceral leishmaniasis is prevalent. The dose is 3-4 mg/kg IV for 5 days. Ketoconazole is given 600 mg/d in three divided doses for 28 days. Itraconazole is given 200mg/d in a single dose for 28 days. 6 Ankylphosphocholine miltefosine is a drug currently undergoing clinical trials. It has produced a 94% cure rate at dosages of about 2.5 mg/kg/d (100 mg daily for 4 weeks) even among patients with antimony-resistant disease. 21,22 Miltefosine was registered for the treatment of visceral leishmaniasis in India in March, , 21 The most effective way to control the disease is to avoid being bitten by the sand fly through the use of insecticides and using bed nets when sleeping. Soldiers deployed to endemic areas tend to show a lower incidence of leishmaniasis infection than do tourists traveling to endemic areas. This may be due to the training soldiers received either before deployment or just after arrival to the war zone. This training includes disease prevention, use of insect repellants and netting and prompt evaluation and treatment by trained military medical personnel. Civilians may not have the training to prevent becoming infected and may not recognize the symptoms once infected. 23 Figure 1 A B A, B: Leishmania tropica amastigotes from an impression smear of a biopsy specimen from a skin lesion. In A, an intact macrophage is practically filled with amastigotes (arrows), several of which have a clearly visible nucleus and kinetoplast; in B, amastigotes are being freed from a rupturing macrophage. Patient had traveled to Egypt, Africa, and the Middle East. Based on culture in NNN medium, followed by isoenzyme analysis, the species was L. tropica.
6 Three Leishmania amastigotes, each with a clearly visible nucleus and kinetoplast, from the same impression smear as in A and B on the previous page. Leishmania mexicana in a biopsy specimen from a skin lesion stained with hematoxylin and eosin. The amastigotes are lining the walls of two vacuoles, a typical arrangement. The species identification was derived from culture followed by isoenzyme analysis. Infection was acquired in Texas.
7 Leishmaniasis is transmitted by the bite of female phlebotomine sandflies. The sandflies inject the infective stage, promastigotes, during blood meals. Promastigotes that reach the puncture wound are phagocytized by macrophages and transform into amastigotes. Amastigotes multiply in infected cells and affect different tissues, depending in part on the Leishmania species. This originates the clinical manifestations of leishmaniasis. Sandflies become infected during blood meals on an infected host when they ingest macrophages infected with amastigotes (, ). In the sandfly's midgut, the parasites differentiate into promastigotes, which multiply and migrate to the proboscis.
8 References 1. Willard RJ, Jeffcoat AM, Benson PM, Walsh DS. Cutaneous leishmaniasis in soldiers from Fort Campbell, Kentucky returning from Operation Iraqi Freedom highlights diagnostic and therapeutic options. J Am Acad Derm. 2005;52(6); Herwaldt BL. Leishmaniasis. Lancet. 1999;354: Dedet JP, Pratlong F. Leishmaniasis. In: Cook GC, Zumla AI, eds. Manson s Tropical Diseases. 21st ed. London, UK. Saunders; 2003: Desjeaux P. Worldwide increasing risk factors for leishmanias. Med Microbiol Immunol. 2001;190(1-2): Desjeaux P. Global control and leishmania HIV coinfection. Clin Dermatol. 1999;17(3): Vidyashankar C. Leishmaniasis. Accessed October 13, Hernandez-PerezJ, Yebra-Banjo M, Jimenez-Martinez E, et al. Visceral leishmaniasis (kalaazar) in solid organ transplantation: report of five cases and review. Clin Infec Dis. 1999;29: Markle WH, Makhoul K. Cutaneous leishmaniasis: recognition and treatment. Am Fam Physician. 2004;69: Batmanis PS, Stone SC. Leishmaniasis in the emergency department. Top Emerg Med. 2003;25(1): Roscoe M. Leishmaniasis: Early diagnosis is the key. JAAPA. 2005;18(7): Magill AJ. Leishmaniasis. In: Strickland GT, ed. Hunters Tropical Medicine and Emerging Infectious Diseases. 8th ed. Philadelphia, PA: WB Saunders; 2000: Murray HW. Kala-azar as an AIDS-related opportunistic infection. AIDS Patient Care STDs. 1999;13(8): Centers for Disease control and Prevention Viscertropic Leishmaniasis in Persons Returning from Operation Desert Storm Available at: Accessed October 13, MMWR Weekly August 23, 1985/34(33); Wortman C, Sweeny G, Houng H-S, et al. Rapid diagnosis of leishmaniasis by fluorgenic polymerase chain reaction. Am J Trop Med Hyg 2001;65: MMWR Weekly. April 2, 2004/53(12); Olliaro PL, Guerin PJ, Gerstl S, et al. Treatment options for visceral leishmaniasis: a systematic review of clinical studies done in India, Lancet Infectious Diseases. 2005; Scope A, Trau H, Anders G, et al. Experience with new world cutaneous leishmaniasis in travelers. J Am Aced Dermatol. 2003;49: Jacobs S. An oral drug for leishmaniasis. N Engl J Med. 2002;347: Jha TK, Sundar S, Thakur CP, et al. Miltefosine, an oral agent, for the treatment of Indian visceral leishmaniasis. N Engl J Med. 1999;341: Hepburn NC. Cutaneous leishmaniasis. Clin Exp Dermatol. 2000;25:
HAEMOFLAGELLATES. Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine
 HAEMOFLAGELLATES Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of Leishmania spp. and Trypanosoma
HAEMOFLAGELLATES Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of Leishmania spp. and Trypanosoma
Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar
 Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar AA 55M presented with sores on left olecranon and umbilical area Umbilical sores present for 3 weeks Left olecranon lesions for 1 week
Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar AA 55M presented with sores on left olecranon and umbilical area Umbilical sores present for 3 weeks Left olecranon lesions for 1 week
Leishmaniasis, Kala Azar(The Black Fever)
 Leishmaniasis, Kala Azar(The Black Fever) By Lawrence Hall Etiologic agent Protist obligate intracellular parasite, Transmission Vectors Phylum: Euglenozoa (genus Leishmania) Over 21 species that infect
Leishmaniasis, Kala Azar(The Black Fever) By Lawrence Hall Etiologic agent Protist obligate intracellular parasite, Transmission Vectors Phylum: Euglenozoa (genus Leishmania) Over 21 species that infect
The Most Common Parasitic Infections In Yemen. Medical Parasitology
 The Most Common Parasitic Infections In Yemen Medical Parasitology ﻓﺎﯾز اﻟﺧوﻻﻧﻲ / د 2 : is a vector-borne disease that transmitted by sandflies and caused by obligate intracellular protozoa of the genus
The Most Common Parasitic Infections In Yemen Medical Parasitology ﻓﺎﯾز اﻟﺧوﻻﻧﻲ / د 2 : is a vector-borne disease that transmitted by sandflies and caused by obligate intracellular protozoa of the genus
BIO Parasitology Spring 2009
 BIO 475 - Parasitology Spring 2009 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 5 Discovery of the Disease In 1924 the Kala-Azar Commission noted that the distribution
BIO 475 - Parasitology Spring 2009 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 5 Discovery of the Disease In 1924 the Kala-Azar Commission noted that the distribution
Leishmaniasis. CDR R.L. Gutierrez Oct 2014
 Leishmaniasis CDR R.L. Gutierrez Oct 2014 Overview Protozoan parasite(s) of tissue and WBCs Many species / Many Syndromes (Cutaneous / Visceral) Pathogen: Location - Old World vs. New World Host: Immune
Leishmaniasis CDR R.L. Gutierrez Oct 2014 Overview Protozoan parasite(s) of tissue and WBCs Many species / Many Syndromes (Cutaneous / Visceral) Pathogen: Location - Old World vs. New World Host: Immune
World Health Organization Department of Communicable Disease Surveillance and Response
 WHO Report on Global Surveillance of Epidemic-prone Infectious Diseases World Health Organization Department of Communicable Disease Surveillance and Response This document has been downloaded from the
WHO Report on Global Surveillance of Epidemic-prone Infectious Diseases World Health Organization Department of Communicable Disease Surveillance and Response This document has been downloaded from the
Leishmaniasis: A forgotten disease among neglected people
 ISPUB.COM The Internet Journal of Health Volume 11 Number 2 Leishmaniasis: A forgotten disease among neglected people Y Homsi, G Makdisi Citation Y Homsi, G Makdisi. Leishmaniasis: A forgotten disease
ISPUB.COM The Internet Journal of Health Volume 11 Number 2 Leishmaniasis: A forgotten disease among neglected people Y Homsi, G Makdisi Citation Y Homsi, G Makdisi. Leishmaniasis: A forgotten disease
~Trichinella Spiralis:
 Musculoskeletal System **Today we are going to talk about the parasites that affect the musculoskeletal system ~Trichinella Spiralis: It s a small nematode that measures to about 2-3mm in length. In general
Musculoskeletal System **Today we are going to talk about the parasites that affect the musculoskeletal system ~Trichinella Spiralis: It s a small nematode that measures to about 2-3mm in length. In general
Visceral leishmaniasis: an endemic disease with global impact
 Visceral leishmaniasis: an endemic disease with global impact Professor Olivier Lortholary, MD, PhD Department of Infectious and Tropical diseases Hôpital Necker-Enfants Malades Université Paris Descartes
Visceral leishmaniasis: an endemic disease with global impact Professor Olivier Lortholary, MD, PhD Department of Infectious and Tropical diseases Hôpital Necker-Enfants Malades Université Paris Descartes
WMLN Case Study. Necrotizing Palate Biopsy Specimen. Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP)
 WMLN Case Study Necrotizing Palate Biopsy Specimen Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP) 44 year old male from Honduras Immigrated to US 12 years ago to WI 4 years ago Seen
WMLN Case Study Necrotizing Palate Biopsy Specimen Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP) 44 year old male from Honduras Immigrated to US 12 years ago to WI 4 years ago Seen
Laboratory diagnosis of Blood and tissue flagellates
 Laboratory diagnosis of Blood and tissue flagellates (Leishmania and trypanosma) Sarah Alharbi Clinical Laboratory department Collage of Applied Medical Sciences King Saud University Leishmania and trypanosma:
Laboratory diagnosis of Blood and tissue flagellates (Leishmania and trypanosma) Sarah Alharbi Clinical Laboratory department Collage of Applied Medical Sciences King Saud University Leishmania and trypanosma:
Protozoa from tissues. Leishmania spp. Naegleria fowleri Toxoplasma gondii Trichomonas vaginalis Trypanosoma spp.
 Protozoa from tissues Leishmania spp. Naegleria fowleri Toxoplasma gondii Trichomonas vaginalis Trypanosoma spp. Leishmaniasis Leishmania infantum, Leishmania donovani, in macrophages of man. Female sandflies:
Protozoa from tissues Leishmania spp. Naegleria fowleri Toxoplasma gondii Trichomonas vaginalis Trypanosoma spp. Leishmaniasis Leishmania infantum, Leishmania donovani, in macrophages of man. Female sandflies:
Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan
 Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan Mamoun Mohammad Al-Athamneh Hiathem Qasem Abu Al-haija Ra ed Smadi Ayman S. Qaqaa Heba
Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan Mamoun Mohammad Al-Athamneh Hiathem Qasem Abu Al-haija Ra ed Smadi Ayman S. Qaqaa Heba
Treatment of Cutaneous Leishmaniasis with Allopurinol and Stibogluconate
 165 Treatment of Cutaneous Leishmaniasis with Allopurinol and S. Martinez, M. Gonzalez, and M. E. Vernaza From the Department of Internal Medicine, University of Cauca, Popayan, and the University Hospital
165 Treatment of Cutaneous Leishmaniasis with Allopurinol and S. Martinez, M. Gonzalez, and M. E. Vernaza From the Department of Internal Medicine, University of Cauca, Popayan, and the University Hospital
Leishmaniasis. MAJ Kris Paolino September 2014
 Leishmaniasis MAJ Kris Paolino September 2014 Thanks to COL (Ret) Kent Kester MAJ Leyi Lin http://www.niaid.nih.gov/topics/leishmaniasis History Sir William Boog Leishman (1865-1926) Matriculated at the
Leishmaniasis MAJ Kris Paolino September 2014 Thanks to COL (Ret) Kent Kester MAJ Leyi Lin http://www.niaid.nih.gov/topics/leishmaniasis History Sir William Boog Leishman (1865-1926) Matriculated at the
2.Trichomonas vaginalis
 2.Trichomonas vaginalis 1. Pathogenic to human &causes vaginitis (trichomoniasis). 2. troph. Is round or pear like in shape, contains 4-6 flagella, all originating from anterior end & only one extend posteriorly.
2.Trichomonas vaginalis 1. Pathogenic to human &causes vaginitis (trichomoniasis). 2. troph. Is round or pear like in shape, contains 4-6 flagella, all originating from anterior end & only one extend posteriorly.
SUMMARY. Cutaneous leishmaniasis with only skin involvement: single to multiple skin ulcers, satellite lesions and nodular lymphangitis.
 SUMMARY Leishmaniasis is a disease affecting predominantly people in the developing countries; 350 million people worldwide are at risk and yearly more than 2 million new cases occur. Leishmaniasis is
SUMMARY Leishmaniasis is a disease affecting predominantly people in the developing countries; 350 million people worldwide are at risk and yearly more than 2 million new cases occur. Leishmaniasis is
Epidemiological Study of Cutaneous Leishmaniasis in Tuz
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 477-483 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.056
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 477-483 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.056
VISERAL LEISHMANIASI S (KALA-AZAR)
 VISERAL LEISHMANIASI S (KALA-AZAR) :OUTLINES DEFINITION. EPIDEMIOLOGY. PARASITE & VECTOR. PATHOLOGY CLINICAL & LIFE CYCLE. PICTURE. COMPLICATIONS. DIAGNOSIS. INVESTIGATIONS. MANAGEMENT TREATMENT S CONTROL.
VISERAL LEISHMANIASI S (KALA-AZAR) :OUTLINES DEFINITION. EPIDEMIOLOGY. PARASITE & VECTOR. PATHOLOGY CLINICAL & LIFE CYCLE. PICTURE. COMPLICATIONS. DIAGNOSIS. INVESTIGATIONS. MANAGEMENT TREATMENT S CONTROL.
Morphological forms of hemoflagellates
 Parasitology Lecture: 1 Hemoflagellates (blood and tissue flagellates) *Classification: - Sub-kingdom: Protozoa -Phylum: Sarcomastigophora -Sub-phylum: Mastigiphora -Class: Zoomastigophora د. رائد *Flagellates
Parasitology Lecture: 1 Hemoflagellates (blood and tissue flagellates) *Classification: - Sub-kingdom: Protozoa -Phylum: Sarcomastigophora -Sub-phylum: Mastigiphora -Class: Zoomastigophora د. رائد *Flagellates
Laboratory investigation of Cutaneous Leishmaniasis in Karachi
 Laboratory investigation of Cutaneous Leishmaniasis in Karachi Pages with reference to book, From 248 To 250 G.M. Rajpar, M.A. Khan, A. Hafiz ( Department of Microbiology, Jinnah Postgraduate Medical Centre,
Laboratory investigation of Cutaneous Leishmaniasis in Karachi Pages with reference to book, From 248 To 250 G.M. Rajpar, M.A. Khan, A. Hafiz ( Department of Microbiology, Jinnah Postgraduate Medical Centre,
Control of leishmaniasis
 SIXTIETH WORLD HEALTH ASSEMBLY A60/10 Provisional agenda item 12.3 22 March 2007 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
SIXTIETH WORLD HEALTH ASSEMBLY A60/10 Provisional agenda item 12.3 22 March 2007 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
Invest in the future, defeat malaria
 Invest in the future, defeat malaria Malaria is caused by parasites from the genus Plasmodium, which are spread to people by infected mosquitoes. There are five species of Plasmodium that can infect humans.
Invest in the future, defeat malaria Malaria is caused by parasites from the genus Plasmodium, which are spread to people by infected mosquitoes. There are five species of Plasmodium that can infect humans.
Antimonial Resistance & Combination therapy in Indian Visceral Leishmaniasis. Shyam Sundar Banaras Hindu University Varanasi, India
 Antimonial Resistance & Combination therapy in Indian Visceral Leishmaniasis Shyam Sundar Banaras Hindu University Varanasi, India History of the Current Epidemic in India & Antimony Resistance 6 Official
Antimonial Resistance & Combination therapy in Indian Visceral Leishmaniasis Shyam Sundar Banaras Hindu University Varanasi, India History of the Current Epidemic in India & Antimony Resistance 6 Official
OPERATION ENDURING FREEDOM
 OPERATION ENDURING FREEDOM Re-Deployment Medical Threat Briefing Name & Unit Prepared by: Office of the Surgeon USAREUR and Europe Regional Medical Command Office of Force Health Protection DSN (314) 370-5680/(314)371-2629
OPERATION ENDURING FREEDOM Re-Deployment Medical Threat Briefing Name & Unit Prepared by: Office of the Surgeon USAREUR and Europe Regional Medical Command Office of Force Health Protection DSN (314) 370-5680/(314)371-2629
Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin
 Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin Department of Dermatology, Pakistan Institute of Medical Sciences,
Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin Department of Dermatology, Pakistan Institute of Medical Sciences,
What is Kala-azar? What are Signs & Symptoms of Kala-Azar?
 What is Kala-azar? Kala-azar is a slow progressing indigenous disease caused by a protozoan parasite of genus Leishmania In India Leishmania donovani is the only parasite causing this disease The parasite
What is Kala-azar? Kala-azar is a slow progressing indigenous disease caused by a protozoan parasite of genus Leishmania In India Leishmania donovani is the only parasite causing this disease The parasite
A Novel Noninvasive Method for Diagnosis of Visceral Leishmaniasis by. rk39 Test in Sputum Samples
 JCM Accepts, published online ahead of print on 0 June 00 J. Clin. Microbiol. doi:0./jcm.00-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
JCM Accepts, published online ahead of print on 0 June 00 J. Clin. Microbiol. doi:0./jcm.00-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças Red Room 17: 00h
 CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000 deaths (6.7%) 310 million at
CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000 deaths (6.7%) 310 million at
Acta Dermatovenerol Croat 2008;16(2):60-64 CLINICAL ARTICLE
 2008;16(2):60-64 CLINICAL ARTICLE Clinical Efficacy of Intramuscular Meglumine Antimoniate Alone and in Combination with Intralesional Meglumine Antimoniate in the Treatment of Old World Cutaneous Leishmaniasis
2008;16(2):60-64 CLINICAL ARTICLE Clinical Efficacy of Intramuscular Meglumine Antimoniate Alone and in Combination with Intralesional Meglumine Antimoniate in the Treatment of Old World Cutaneous Leishmaniasis
Single-Dose Liposomal Amphotericin B in the Treatment of Visceral Leishmaniasis in India: A Multicenter Study
 MAJOR ARTICLE Single-Dose Liposomal Amphotericin B in the Treatment of Visceral Leishmaniasis in India: A Multicenter Study S. Sundar, 1 T. K. Jha, 2 C. P. Thakur, 3 M. Mishra, 4 V. P. Singh, 1 and R.
MAJOR ARTICLE Single-Dose Liposomal Amphotericin B in the Treatment of Visceral Leishmaniasis in India: A Multicenter Study S. Sundar, 1 T. K. Jha, 2 C. P. Thakur, 3 M. Mishra, 4 V. P. Singh, 1 and R.
Visceral childhood leishmaniasis in southern Turkey: experience of twenty years
 The Turkish Journal of Pediatrics 2009; 51: 1-5 Original Visceral childhood leishmaniasis in southern Turkey: experience of twenty years Oğuz Dursun 1, Seyhan Erişir 2, Akif Yeşilipek 3 Divisions of 1
The Turkish Journal of Pediatrics 2009; 51: 1-5 Original Visceral childhood leishmaniasis in southern Turkey: experience of twenty years Oğuz Dursun 1, Seyhan Erişir 2, Akif Yeşilipek 3 Divisions of 1
New insights on leishmaniasis in immunosuppressive conditions
 New insights on leishmaniasis in immunosuppressive conditions Javier Moreno Immunoparasitology Unit WHO Collaborative Center for Leishmaniasis Centro Nacional de Microbiología INSTITUTO DE SALUD CARLOS
New insights on leishmaniasis in immunosuppressive conditions Javier Moreno Immunoparasitology Unit WHO Collaborative Center for Leishmaniasis Centro Nacional de Microbiología INSTITUTO DE SALUD CARLOS
Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar)
 SEA-CD-274 Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar) World Health Organization 2013 All rights reserved. Requests for publications, or for permission to reproduce or translate WHO
SEA-CD-274 Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar) World Health Organization 2013 All rights reserved. Requests for publications, or for permission to reproduce or translate WHO
Leishmaniasis WRAIR- GEIS 'Operational Clinical Infectious Disease' Course
 Leishmaniasis WRAIR- GEIS 'Operational Clinical Infectious Disease' Course UNCLASSIFIED Acknowledgments LTC James E. Moon, MD Chief, Sleep Trials Branch Walter Reed Army Institute of Research CDR Ramiro
Leishmaniasis WRAIR- GEIS 'Operational Clinical Infectious Disease' Course UNCLASSIFIED Acknowledgments LTC James E. Moon, MD Chief, Sleep Trials Branch Walter Reed Army Institute of Research CDR Ramiro
Blood Smears Only 6 October Sample Preparation and Quality Control 15B-K
 NEW YORK STATE Parasitology Proficiency Testing Program Blood Smears Only 6 October 5 The purpose of the New York State Proficiency Testing Program in the category of Parasitology - Blood Smears Only is
NEW YORK STATE Parasitology Proficiency Testing Program Blood Smears Only 6 October 5 The purpose of the New York State Proficiency Testing Program in the category of Parasitology - Blood Smears Only is
OPERATION IRAQI FREEDOM
 Notes/Changes Briefer if service members are completing the health assessment through AKO you may hide/omit/modify slides 25 though 31. They are for use if the service member is filling out the hard copy
Notes/Changes Briefer if service members are completing the health assessment through AKO you may hide/omit/modify slides 25 though 31. They are for use if the service member is filling out the hard copy
Kala-Azar- Treatment Update
 JOURNAL OF ADVANCES IN MEDICINE (JAM) DOI: 10.5958/2319-4324.2016.00002.X REVIEW PAPER Kala-Azar- Treatment Update Anup Singh Associate Professor, Department of Medicine, Institute of Medical Sciences,
JOURNAL OF ADVANCES IN MEDICINE (JAM) DOI: 10.5958/2319-4324.2016.00002.X REVIEW PAPER Kala-Azar- Treatment Update Anup Singh Associate Professor, Department of Medicine, Institute of Medical Sciences,
Original Article Chloroquine in cutaneous leishmaniasis
 Original Article Chloroquine in cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin, Iqbal Sidiqui Department of Dermatology, Pakistan Institute of Medical Sciences, Islamabad Abstract Background Chloroquine
Original Article Chloroquine in cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin, Iqbal Sidiqui Department of Dermatology, Pakistan Institute of Medical Sciences, Islamabad Abstract Background Chloroquine
Short-Course Paromomycin Treatment of Visceral Leishmaniasis in India: 14-Day vs 21-Day Treatment
 MAJOR ARTICLE Short-Course Paromomycin Treatment of Visceral Leishmaniasis in India: 14-Day vs 21-Day Treatment Shyam Sundar, Neha Agrawal, Rakesh Arora, Dipti Agarwal, Madhukar Rai, and Jaya Chakravarty
MAJOR ARTICLE Short-Course Paromomycin Treatment of Visceral Leishmaniasis in India: 14-Day vs 21-Day Treatment Shyam Sundar, Neha Agrawal, Rakesh Arora, Dipti Agarwal, Madhukar Rai, and Jaya Chakravarty
Recommendations for Coping with Leishmaniasis: A Review of Control Strategies. Centro de Convenções de Reboças Red Room 17: 00h
 Recommendations for Coping with Leishmaniasis: A Review of Control Strategies Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000
Recommendations for Coping with Leishmaniasis: A Review of Control Strategies Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000
 Malaria parasites Malaria parasites are micro-organisms that belong to the genus Plasmodium. There are more than 100 species of Plasmodium, which can infect many animal species such as reptiles, birds,
Malaria parasites Malaria parasites are micro-organisms that belong to the genus Plasmodium. There are more than 100 species of Plasmodium, which can infect many animal species such as reptiles, birds,
Therapeutic Options for Visceral Leishmaniasis
 Drugs (2013) 73:1863 1888 DOI 10.1007/s40265-013-0133-0 REVIEW ARTICLE Therapeutic Options for Visceral Leishmaniasis Begoña Monge-Maillo Rogelio López-Vélez Published online: 30 October 2013 Ó The Author(s)
Drugs (2013) 73:1863 1888 DOI 10.1007/s40265-013-0133-0 REVIEW ARTICLE Therapeutic Options for Visceral Leishmaniasis Begoña Monge-Maillo Rogelio López-Vélez Published online: 30 October 2013 Ó The Author(s)
Leishmaniaand Leishmaniasis
 Leishmaniaand Leishmaniasis Methodenseminar SS2014 IRMA SCHABUSSOVA, PhD Institute of Specific Prophylaxis and Tropical Medicine; Medical University Vienna Kinderspitalgasse 15, A-1090 Vienna, Austria
Leishmaniaand Leishmaniasis Methodenseminar SS2014 IRMA SCHABUSSOVA, PhD Institute of Specific Prophylaxis and Tropical Medicine; Medical University Vienna Kinderspitalgasse 15, A-1090 Vienna, Austria
Elimination of VL in the Indian subcontinent is it achievable?
 Elimination of VL in the Indian subcontinent is it achievable? P Das Rajendra Memorial Research Institute, Patna Jorge Alvar DNDi, Geneva Bhawna Sharma DNDi, India Leishmaniasis 350 million at risk worldwide
Elimination of VL in the Indian subcontinent is it achievable? P Das Rajendra Memorial Research Institute, Patna Jorge Alvar DNDi, Geneva Bhawna Sharma DNDi, India Leishmaniasis 350 million at risk worldwide
Flagellates. Dr. Anuluck Junkum PARA
 Flagellates Dr. Anuluck Junkum PARA 317242 Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of pathogenic flagellates Classification of Protozoa Based on locomotive
Flagellates Dr. Anuluck Junkum PARA 317242 Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of pathogenic flagellates Classification of Protozoa Based on locomotive
by author Drug Therapy in African Visceral Leishmaniasis 28th ECCMID Conference, Madrid, Spain 21 April 2018
 Drug Therapy in African Visceral Leishmaniasis 28th ECCMID Conference, Madrid, Spain 21 April 2018 Dr. Monique Wasunna, Director, DNDi Africa Regional Office Presentation Outline 1 2 4 5 Introduction leishmaniasis
Drug Therapy in African Visceral Leishmaniasis 28th ECCMID Conference, Madrid, Spain 21 April 2018 Dr. Monique Wasunna, Director, DNDi Africa Regional Office Presentation Outline 1 2 4 5 Introduction leishmaniasis
Oral miltefosine for Indian post-kala-azar dermal leishmaniasis: a randomised trial
 Tropical Medicine and International Health doi:10.1111/tmi.12015 volume 18 no 1 pp 96 100 january 2013 Oral miltefosine for Indian post-kala-azar dermal leishmaniasis: a randomised trial Shyam Sundar 1,
Tropical Medicine and International Health doi:10.1111/tmi.12015 volume 18 no 1 pp 96 100 january 2013 Oral miltefosine for Indian post-kala-azar dermal leishmaniasis: a randomised trial Shyam Sundar 1,
Kinetoplastids Handout
 Kinetoplastids Handout 1 Kinetoplastids widespread group of flagellated protozoa parasitize virtually all animal groups as well as plants and insects 3 distinct kinetoplastid species cause human disease
Kinetoplastids Handout 1 Kinetoplastids widespread group of flagellated protozoa parasitize virtually all animal groups as well as plants and insects 3 distinct kinetoplastid species cause human disease
Control of leishmaniasis
 EXECUTIVE BOARD EB118/4 118th Session 11 May 2006 Provisional agenda item 5.1 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
EXECUTIVE BOARD EB118/4 118th Session 11 May 2006 Provisional agenda item 5.1 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
Efficacy of Miltefosine in the Treatment of Visceral Leishmaniasis in India After a Decade of Use
 MAJOR ARTICLE Efficacy of Miltefosine in the Treatment of Visceral Leishmaniasis in India After a Decade of Use Shyam Sundar, 1,a Anup Singh, 1,a Madhukar Rai, 1 Vijay K. Prajapati, 1 Avinash K. Singh,
MAJOR ARTICLE Efficacy of Miltefosine in the Treatment of Visceral Leishmaniasis in India After a Decade of Use Shyam Sundar, 1,a Anup Singh, 1,a Madhukar Rai, 1 Vijay K. Prajapati, 1 Avinash K. Singh,
Cutaneous Leishmaniasis : Global overview
 Cutaneous Leishmaniasis : Global overview Meeting of stakeholders for selected Health R&D Demostration Projects, 7-10 May 2014, WHO, Geneva Dr. Daniel Argaw Dagne, NTD/WHO CSR - DDC AFRO Leishmaniasis
Cutaneous Leishmaniasis : Global overview Meeting of stakeholders for selected Health R&D Demostration Projects, 7-10 May 2014, WHO, Geneva Dr. Daniel Argaw Dagne, NTD/WHO CSR - DDC AFRO Leishmaniasis
Blood Smears Only 07 February Sample Preparation and Quality Control 12B A
 NEW YORK STATE Parasitology Proficiency Testing Program Blood Smears Only 07 February 2012 The purpose of the New York State Proficiency Testing Program in the category of Parasitology Blood Smears Only
NEW YORK STATE Parasitology Proficiency Testing Program Blood Smears Only 07 February 2012 The purpose of the New York State Proficiency Testing Program in the category of Parasitology Blood Smears Only
18 : 1. Shyam Sundar, Anup Singh, Arun Shah, Varanasi EPIDEMIOLOGY: DIAGNOSIS OF VL:
 18 : 1 Visceral leishmaniasis-current scenario Visceral leishmaniasis (VL) is a systemic disease that is fatal if left untreated and is caused by an obligate intracellular protozoan parasite of genus leishmania.
18 : 1 Visceral leishmaniasis-current scenario Visceral leishmaniasis (VL) is a systemic disease that is fatal if left untreated and is caused by an obligate intracellular protozoan parasite of genus leishmania.
Necrotizing and suppurative lymphadenitis in Leishmania
 Tropical Medicine and International Health VOLUME I NO. 2 PP 243-250 APRIL 1996 Necrotizing and suppurative lymphadenitis in Leishmania major infections A. Gaafar r, A. Ismai13, A. Y. El Kadaro4, Elsir
Tropical Medicine and International Health VOLUME I NO. 2 PP 243-250 APRIL 1996 Necrotizing and suppurative lymphadenitis in Leishmania major infections A. Gaafar r, A. Ismai13, A. Y. El Kadaro4, Elsir
CUTANEOUS LEISHMANIASIS
 CUTANEOUS LEISHMANIASIS Why are you neglecting me? A WHO initiative to control Cutaneous Leishmaniasis in selected Old World areas This document has been produced as the result of a WHO Informal Consultative
CUTANEOUS LEISHMANIASIS Why are you neglecting me? A WHO initiative to control Cutaneous Leishmaniasis in selected Old World areas This document has been produced as the result of a WHO Informal Consultative
GENUS: LEISHMANIA. Under the genus Leishmania, there are 2 subgenus: SPECIES PARASITIC IN MEN. Under subgenus Leishmania, there are following species:
 GENUS: LEISHMANIA Species parasitic in man: Under the genus Leishmania, there are 2 subgenus: 1. Leishmania 2. Viannia SPECIES PARASITIC IN MEN Under subgenus Leishmania, there are following species: LEISHMANIA
GENUS: LEISHMANIA Species parasitic in man: Under the genus Leishmania, there are 2 subgenus: 1. Leishmania 2. Viannia SPECIES PARASITIC IN MEN Under subgenus Leishmania, there are following species: LEISHMANIA
Departments of Dermatology, Venereology and Leprosy and *Microbiology, Indira Gandhi Medical College, Shimla, India.
 Net Study Comparative efþ cacy of intralesional sodium stibogluconate (SSG) alone and its combination with intramuscular SSG to treat localized cutaneous leishmaniasis: Results of a pilot study Ajeet K.
Net Study Comparative efþ cacy of intralesional sodium stibogluconate (SSG) alone and its combination with intramuscular SSG to treat localized cutaneous leishmaniasis: Results of a pilot study Ajeet K.
POST KALA-AZAR DERMAL LEISHMANIASIS WITH ULCERATION ON FOOT: AN ATYPICAL CASE PRESENTATION SUCCESSFULLY TREATED WITH MILTEFOSINE
 American Journal of Infectious Diseases 10 (2): 50-55, 2014 ISSN: 1553-6203 2014 Science Publication doi:10.3844/ajidsp.2014.50.55 Published Online 10 (2) 2014 (http://www.thescipub.com/ajid.toc) POST
American Journal of Infectious Diseases 10 (2): 50-55, 2014 ISSN: 1553-6203 2014 Science Publication doi:10.3844/ajidsp.2014.50.55 Published Online 10 (2) 2014 (http://www.thescipub.com/ajid.toc) POST
Viral Hepatitis. Background
 Viral Hepatitis Background Hepatitis or inflammation of the liver can be caused by infectious and noninfectious problems. Infectious etiologies include viruses, bacteria, fungi and parasites. Noninfectious
Viral Hepatitis Background Hepatitis or inflammation of the liver can be caused by infectious and noninfectious problems. Infectious etiologies include viruses, bacteria, fungi and parasites. Noninfectious
Parasitic Protozoa, Helminths, and Arthropod Vectors
 PowerPoint Lecture Slides for MICROBIOLOGY ROBERT W. BAUMAN Chapter 23 Parasitic Protozoa, Helminths, and Arthropod Vectors Parasitic Diseases Protozoan and helminthic parasites are emerging as serious
PowerPoint Lecture Slides for MICROBIOLOGY ROBERT W. BAUMAN Chapter 23 Parasitic Protozoa, Helminths, and Arthropod Vectors Parasitic Diseases Protozoan and helminthic parasites are emerging as serious
Phlebotomus argentipes. Amphotericin B has long been recognized as a powerful anti-kala-azar drug
 A STUDY OF EFFICACY AND ADVERSE DRUG REACTIONS OF CONVENTIONAL AMPHOTERICIN B IN THE TREATMENT OF KALA-AZAR Rajesh Kumar Pandey 1, S. N. Singh 2, Bharat Kumar 3, Kashif Shahnawaz 4 HOW TO CITE THIS ARTICLE:
A STUDY OF EFFICACY AND ADVERSE DRUG REACTIONS OF CONVENTIONAL AMPHOTERICIN B IN THE TREATMENT OF KALA-AZAR Rajesh Kumar Pandey 1, S. N. Singh 2, Bharat Kumar 3, Kashif Shahnawaz 4 HOW TO CITE THIS ARTICLE:
Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels
 Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels A M EL Hassan Institute of Endemic Diseases University of Khartoum Introduction PKDL is a VL related
Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels A M EL Hassan Institute of Endemic Diseases University of Khartoum Introduction PKDL is a VL related
PRESENTATION OF INFECTIONS COEXISTENCE IN AN HIV+ PATIENT
 PRESENTATION OF INFECTIONS COEXISTENCE IN AN HIV+ PATIENT Piddubna Anna Sumy State University Department of Infectious Diseases and Epidemiology Sumy Ukraine Patient history Complaints Patient Sex Male
PRESENTATION OF INFECTIONS COEXISTENCE IN AN HIV+ PATIENT Piddubna Anna Sumy State University Department of Infectious Diseases and Epidemiology Sumy Ukraine Patient history Complaints Patient Sex Male
African Trypanosomes
 African Trypanosomes Giemsa-stained blood smear of African trypanosomes viewed under the 100X objective lens. The block arrows denote trypomastigote forms of the African trypanosomes found within the blood
African Trypanosomes Giemsa-stained blood smear of African trypanosomes viewed under the 100X objective lens. The block arrows denote trypomastigote forms of the African trypanosomes found within the blood
Communicable Diseases
 Chapter 23 Communicable Diseases Disease that s spread from one living organism to another or through the environment Infection occurs when pathogens in the body multiply and damage body cells Main Pathogens
Chapter 23 Communicable Diseases Disease that s spread from one living organism to another or through the environment Infection occurs when pathogens in the body multiply and damage body cells Main Pathogens
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT 2 QUALITATIVE AND QUANTITATIVE COMPOSITION
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Pentostam Injection. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Sodium Stibogluconate equivalent to 100 mg pentavalent antimony in each
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Pentostam Injection. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Sodium Stibogluconate equivalent to 100 mg pentavalent antimony in each
Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A Case Report
 J HEALTH POPUL NUTR 2014 Jun;32(2):372-376 ISSN 1606-0997 $ 5.00+0.20 INTERNATIONAL CENTRE FOR DIARRHOEAL DISEASE RESEARCH, BANGLADESH CASE STUDY Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A
J HEALTH POPUL NUTR 2014 Jun;32(2):372-376 ISSN 1606-0997 $ 5.00+0.20 INTERNATIONAL CENTRE FOR DIARRHOEAL DISEASE RESEARCH, BANGLADESH CASE STUDY Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A
EPIDEMIOLOGICAL, CLINICAL AND THERAPEUTIC FEATURES OF PEDIATRIC KALA-AZAR
 EPIDEMIOLOGICAL, CLINICAL AND THERAPEUTIC FEATURES OF PEDIATRIC KALA-AZAR Kadivar Mohammad Rahim 1 and Moslehi Mohammad Ashkan 1 1 Department of Pediatrics, Nemazee Hospital, Shiraz University of Medical
EPIDEMIOLOGICAL, CLINICAL AND THERAPEUTIC FEATURES OF PEDIATRIC KALA-AZAR Kadivar Mohammad Rahim 1 and Moslehi Mohammad Ashkan 1 1 Department of Pediatrics, Nemazee Hospital, Shiraz University of Medical
Research Article Efficacy and Safety of Paromomycin in Treatment of Post-Kala-Azar Dermal Leishmaniasis
 ISRN Parasitology, Article ID 548010, 4 pages http://dx.doi.org/10.1155/2014/548010 Research Article Efficacy and Safety of Paromomycin in Treatment of Post-Kala-Azar Dermal Leishmaniasis Shyam Sundar,
ISRN Parasitology, Article ID 548010, 4 pages http://dx.doi.org/10.1155/2014/548010 Research Article Efficacy and Safety of Paromomycin in Treatment of Post-Kala-Azar Dermal Leishmaniasis Shyam Sundar,
The New England Journal of Medicine
 The New England Journal of Medicine Copyright 22 by the Massachusetts Medical Society VOLUME 347 N OVEMBER 28, 22 NUMBER 22 ORAL MILTEFOSINE FOR INDIAN VISCERAL LEISHMANIASIS SHYAM SUNDAR, M.D., T.K. JHA,
The New England Journal of Medicine Copyright 22 by the Massachusetts Medical Society VOLUME 347 N OVEMBER 28, 22 NUMBER 22 ORAL MILTEFOSINE FOR INDIAN VISCERAL LEISHMANIASIS SHYAM SUNDAR, M.D., T.K. JHA,
Cutaneous Leishmaniasis in a Chinese man returning from the Amazon forest in Brazil
 Hong Kong J. Dermatol. Venereol. (2013) 21, 79-83 Case Report Cutaneous Leishmaniasis in a Chinese man returning from the Amazon forest in Brazil JTHT Yu and SY Wong A 60-year-old man presented with ulcerated
Hong Kong J. Dermatol. Venereol. (2013) 21, 79-83 Case Report Cutaneous Leishmaniasis in a Chinese man returning from the Amazon forest in Brazil JTHT Yu and SY Wong A 60-year-old man presented with ulcerated
- Mycoplasma and Ureaplasma. - Rickettsia
 - Mycoplasma and Ureaplasma - Rickettsia Mycoplasma and Ureaplasma Family: Mycoplasmataceae Genus: Mycoplasma Species: M. pneumoniae Species: M. hominis Species: M. genitalium Genus: Ureaplasma Species:
- Mycoplasma and Ureaplasma - Rickettsia Mycoplasma and Ureaplasma Family: Mycoplasmataceae Genus: Mycoplasma Species: M. pneumoniae Species: M. hominis Species: M. genitalium Genus: Ureaplasma Species:
Fact sheet. Yellow fever
 Fact sheet Key facts is an acute viral haemorrhagic disease transmitted by infected mosquitoes. The yellow in the name refers to the jaundice that affects some patients. Up to 50% of severely affected
Fact sheet Key facts is an acute viral haemorrhagic disease transmitted by infected mosquitoes. The yellow in the name refers to the jaundice that affects some patients. Up to 50% of severely affected
The Struggle with Infectious Disease. Lecture 5
 The Struggle with Infectious Disease Lecture 5 Tropical Diseases Life and infectious disease began in the rift valley/rain forest of Eastern Africa Peoples migrated North to temperate regions Tropical
The Struggle with Infectious Disease Lecture 5 Tropical Diseases Life and infectious disease began in the rift valley/rain forest of Eastern Africa Peoples migrated North to temperate regions Tropical
New Insights into Diagnosing Leishmaniasis
 New Insights into Diagnosing Leishmaniasis Eric Zini Snow meeting, 13 March 2009 Climate Variability and Visceral Leishmaniasis in Europe WHO/TDR, Jan. 2008 Late Eighties Maroli et al., Trop Med Int Health
New Insights into Diagnosing Leishmaniasis Eric Zini Snow meeting, 13 March 2009 Climate Variability and Visceral Leishmaniasis in Europe WHO/TDR, Jan. 2008 Late Eighties Maroli et al., Trop Med Int Health
Prevalence of Cutaneous Leishmaniasis among HIV and Non-HIV Patients attending some Selected Hospitals in Jos Plateau State
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 06 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.706.307
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 06 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.706.307
Leishmaniasis in the WhO european region
 Leishmaniasis in the WhO european region This information leaflet contains six sections and is intended for a generic and public health audience: 1.Leishmaniasis is present in europe. What are the risks
Leishmaniasis in the WhO european region This information leaflet contains six sections and is intended for a generic and public health audience: 1.Leishmaniasis is present in europe. What are the risks
IMMUNE SYSTEM. Biology 2201
 IMMUNE SYSTEM Biology 2201 What is a disease? Other than an injury, any change in the body that interferes with the normal functioning of the body. Two Types of Diseases Non-infectious often called functional
IMMUNE SYSTEM Biology 2201 What is a disease? Other than an injury, any change in the body that interferes with the normal functioning of the body. Two Types of Diseases Non-infectious often called functional
IMMUNE SYSTEM. Biology What is a disease? Other than an injury, any change in the body that interferes with the normal functioning of the body.
 IMMUNE SYSTEM Biology 2201 What is a disease? Other than an injury, any change in the body that interferes with the normal functioning of the body. 1 Two Types of Diseases Non-infectious often called functional
IMMUNE SYSTEM Biology 2201 What is a disease? Other than an injury, any change in the body that interferes with the normal functioning of the body. 1 Two Types of Diseases Non-infectious often called functional
Study Plan: Screening
 Phase 1 with Sporozoite Challenge Open-Label Dose-Escalation Safety, Reactogenicity, Immunogenicity, and Efficacy of the Vaccine Candidate Plasmodium falciparum Malaria Protein (FMP012), an E coli-expressed
Phase 1 with Sporozoite Challenge Open-Label Dose-Escalation Safety, Reactogenicity, Immunogenicity, and Efficacy of the Vaccine Candidate Plasmodium falciparum Malaria Protein (FMP012), an E coli-expressed
Alberta Health Public Health Notifiable Disease Management Guidelines January 2013
 January 2013 Rickettsial Infections Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) January 2013 January 2013 December
January 2013 Rickettsial Infections Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) January 2013 January 2013 December
Immunity and Infection. Chapter 17
 Immunity and Infection Chapter 17 The Chain of Infection Transmitted through a chain of infection (six links) Pathogen: Disease causing microorganism Reservoir: Natural environment of the pathogen Portal
Immunity and Infection Chapter 17 The Chain of Infection Transmitted through a chain of infection (six links) Pathogen: Disease causing microorganism Reservoir: Natural environment of the pathogen Portal
Summary of Cases & Epidemiology Aspects of Leishmaniasis in Thailand
 Summary of Cases & Epidemiology Aspects of Leishmaniasis in Thailand Sukmee T. 1, Mungthin M. 2, Apiwathanasorn C. 3, Leelayoova S. 2 1 Department of Microbiology, Phramongkutklao College of Medicine 2
Summary of Cases & Epidemiology Aspects of Leishmaniasis in Thailand Sukmee T. 1, Mungthin M. 2, Apiwathanasorn C. 3, Leelayoova S. 2 1 Department of Microbiology, Phramongkutklao College of Medicine 2
Disease Transmission Methods
 Disease Transmission Methods In epidemiology, transmission simply means any method by which an infectious agent is spread from one host to another. Knowing the type of pathogen often, but not always, identifies
Disease Transmission Methods In epidemiology, transmission simply means any method by which an infectious agent is spread from one host to another. Knowing the type of pathogen often, but not always, identifies
ISPUB.COM. Cutaneous Leishmaniasis in Iran. C Yazdi, M Narmani, B Sadri INTRODUCTION CASE 1 CASE 2
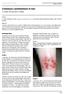 ISPUB.COM The Internet Journal of Infectious Diseases Volume 3 Number 1 Cutaneous Leishmaniasis in Iran C Yazdi, M Narmani, B Sadri Citation C Yazdi, M Narmani, B Sadri. Cutaneous Leishmaniasis in Iran.
ISPUB.COM The Internet Journal of Infectious Diseases Volume 3 Number 1 Cutaneous Leishmaniasis in Iran C Yazdi, M Narmani, B Sadri Citation C Yazdi, M Narmani, B Sadri. Cutaneous Leishmaniasis in Iran.
CASE OF CUTANEOUS LEISHMANIASIS OF THE LID*
 Brit. J. Ophthal. (1965) 49, 542 CASE OF CUTANEOUS LEISHMANIASIS OF THE LID* BY GWYN MORGAN Department ofpathology, Institute of Ophthalmology, University of London THE lid is involved only in about 2
Brit. J. Ophthal. (1965) 49, 542 CASE OF CUTANEOUS LEISHMANIASIS OF THE LID* BY GWYN MORGAN Department ofpathology, Institute of Ophthalmology, University of London THE lid is involved only in about 2
Lecture 7: Mycoses Caused by Dimorphic Fungi, Part I
 BIOL 4849 Medical Mycology Summer 2006 Histoplasmosis Lecture 7: Mycoses Caused by Dimorphic Fungi, Part I u Most common endemic mycotic disease in the United States u Two different varieties (actually
BIOL 4849 Medical Mycology Summer 2006 Histoplasmosis Lecture 7: Mycoses Caused by Dimorphic Fungi, Part I u Most common endemic mycotic disease in the United States u Two different varieties (actually
Series Editors Samuel J. Black, University of Massachusetts, Amherst, MA, US.A. J. Richard Seed, University of North Carolina, Chapel Hill, NC, US.A.
 LEISHMANIA World Class Parasites VOLUME 4 Volumes in the World Class Parasites book series are written for researchers, students and scholars who enjoy reading about excellent research on problems of global
LEISHMANIA World Class Parasites VOLUME 4 Volumes in the World Class Parasites book series are written for researchers, students and scholars who enjoy reading about excellent research on problems of global
Current therapeutics for visceral leischmaniasis. F.Amri
 Current therapeutics for visceral leischmaniasis F.Amri Department of pediatrics Kairouan Intoduction The visceral leischmaniasis is an anthropozoonose caused by a protozoar, the Leishmania infantum The
Current therapeutics for visceral leischmaniasis F.Amri Department of pediatrics Kairouan Intoduction The visceral leischmaniasis is an anthropozoonose caused by a protozoar, the Leishmania infantum The
A RELOOK AT ZIKA VIRAL INFECTION AND ITS LATEST OUTBREAK IN INDIA
 24 th December 2018 A RELOOK AT ZIKA VIRAL INFECTION AND ITS LATEST OUTBREAK IN INDIA BACKGROUND Zika virus infection, which erupted on a large scale in 2015-2016, has infected more than 1.5 million people.
24 th December 2018 A RELOOK AT ZIKA VIRAL INFECTION AND ITS LATEST OUTBREAK IN INDIA BACKGROUND Zika virus infection, which erupted on a large scale in 2015-2016, has infected more than 1.5 million people.
Drug resistance in Indian visceral leishmaniasis
 Tropical Medicine and International Health volume6no11pp849±854november2001 Drug resistance in Indian visceral leishmaniasis Shyam Sundar Kala-azar Medical Research Centre, Banaras Hindu University, Varanasi,
Tropical Medicine and International Health volume6no11pp849±854november2001 Drug resistance in Indian visceral leishmaniasis Shyam Sundar Kala-azar Medical Research Centre, Banaras Hindu University, Varanasi,
African tick typhus. David Mabey
 African tick typhus David Mabey 25 year old English man Holiday in Zimbabwe for 3 months Became unwell on plane home Fever Rash Generalised lymphadenopathy This photo was taken 2 days after onset of symptoms
African tick typhus David Mabey 25 year old English man Holiday in Zimbabwe for 3 months Became unwell on plane home Fever Rash Generalised lymphadenopathy This photo was taken 2 days after onset of symptoms
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
CLINCOPATHOLOGICAL CASE
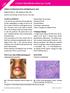 CLINCOPATHOLOGICAL CASE Solitary erythematous firm noduloplaque on nose Hassab El-Naby H., MD, Mosbeh Al Sadat, MD Department of Dermatology, Al-Azhar University, Cairo, Egypt. CLINICAL FINDINGS A 36-year-old
CLINCOPATHOLOGICAL CASE Solitary erythematous firm noduloplaque on nose Hassab El-Naby H., MD, Mosbeh Al Sadat, MD Department of Dermatology, Al-Azhar University, Cairo, Egypt. CLINICAL FINDINGS A 36-year-old
Malaria DR. AFNAN YOUNIS
 Malaria DR. AFNAN YOUNIS Objectives: Epidemiology of malaria Clinical picture Mode of transmission Risk factors Prevention and control Malaria is a life-threatening disease caused by Plasmodium parasites
Malaria DR. AFNAN YOUNIS Objectives: Epidemiology of malaria Clinical picture Mode of transmission Risk factors Prevention and control Malaria is a life-threatening disease caused by Plasmodium parasites
Neglected Diseases (NDs) Landscape in Brazil and South America
 Frontiers in Science on Neglected Diseases 13 th November 2014 Neglected Diseases (NDs) Landscape in Brazil and South America Jeffrey Shaw São Paulo University Biomedical Sciences Institute jeffreyj@usp.br
Frontiers in Science on Neglected Diseases 13 th November 2014 Neglected Diseases (NDs) Landscape in Brazil and South America Jeffrey Shaw São Paulo University Biomedical Sciences Institute jeffreyj@usp.br
Impavido. (miltefosine) New Product Slideshow
 Impavido (miltefosine) New Product Slideshow Introduction Brand name: Impavido Generic name: Miltefosine Pharmacological class: Antileishmanial agent Strength and Formulation: 50mg; hard gel capsules Manufacturer:
Impavido (miltefosine) New Product Slideshow Introduction Brand name: Impavido Generic name: Miltefosine Pharmacological class: Antileishmanial agent Strength and Formulation: 50mg; hard gel capsules Manufacturer:
