STUDY. Increased Detection of Rickettsialpox in a New York City Hospital Following the Anthrax Outbreak of 2001
|
|
|
- Bennett Carroll
- 5 years ago
- Views:
Transcription
1 STUDY Increased Detection of Rickettsialpox in a New York City Hospital Following the Anthrax Outbreak of 2001 Use of Immunohistochemistry for the Rapid Confirmation of Cases in an Era of Bioterrorism Tamara Koss, MD; Eric L. Carter, MD; Marc E. Grossman, MD; David N. Silvers, MD; Asher D. Rabinowitz, MD; Joseph Singleton, Jr, BS; Sherif R. Zaki, MD, PhD; Christopher D. Paddock, MD Background: Rickettsialpox is a self-limited febrile illness with skin lesions that may be mistaken for signs of potentially more serious diseases, such as cutaneous anthrax or chickenpox. The cluster of cutaneous anthrax cases from bioterrorism in October 2001 likely heightened awareness of and concern for cutaneous eschars. Objectives: To apply an immunohistochemical technique on paraffin-embedded skin biopsy specimens for diagnosing rickettsialpox, and to compare the reported incidence of rickettsialpox before, during, and after the cluster of cutaneous anthrax cases. Design: Case series. Setting: Dermatology department in a large tertiary care hospital in New York City. Patients: Eighteen consecutive patients with the clinical diagnosis of rickettsialpox from February 23, 2001, through October 31, Main Outcome Measures: Results of immunohistochemical testing of skin biopsy specimens and of serological testing. Results: Immunohistochemical testing revealed spotted fever group rickettsiae in all 16 eschars and in 5 of the 9 papulovesicles tested. A 4-fold or greater increase in IgG antibody titers reactive with Rickettsia akari was observed in all 9 patients for whom acute and convalescent phase samples were available; 6 patients had single titers indicative of rickettsialpox infection ( 1:64). Of the 18 patients, 9 (50%) presented in the 5 months following the bioterrorism attacks. Conclusions: Rickettsialpox remains endemic in New York City, and the bioterrorism attacks of October 2001 may have led to increased awareness and detection of this disease. Because rickettsialpox may be confused with more serious diseases, such as cutaneous anthrax or chickenpox, clinicians should be familiar with its clinical presentation and diagnostic features. Immunohistochemical staining of skin biopsy specimens, particularly from eschars, is a sensitive technique for confirming the clinical diagnosis. Arch Dermatol. 2003;139: Author affiliations are listed at the end of this article. The authors have no relevant financial interest in this article. RICKETTSIALPOX IS an acute, self-limited, febrile illness caused by Rickettsia akari and transmitted by Liponyssoides sanguineus, a hematophagous mite that infests the common house mouse (Mus musculus). Rickettsialpox begins with the bite of an infected mite, which forms a black eschar. Patients subsequently develop the abrupt onset of high fever, headache, and systemic symptoms, followed by a sparse, disseminated, papulovesicular rash. Rickettsia akari is a member of the spotted fever group of rickettsiae, which also includes Rickettsia rickettsii, the cause of Rocky Mountain spotted fever; Rickettsia conorii, the cause of boutonneuse fever; and Rickettsia africae, the cause of African tick bite fever. 1,2 Rickettsialpox has been described primarily in New York City, but it has also been reported in large cities in the eastern United States (in Massachusetts, Connecticut, Maryland, Ohio, and Pennsylvania) 2-8 and in rural North Carolina, 9 Utah, 8 Russia, 10 Korea, 2 and South Africa. 2,11 The disease has been reported in patients ranging in age from 6 months to 72 years. 1 In the past, the laboratory diagnosis of rickettsialpox was based on testing of paired serum samples to detect a 4-fold increase in antibodies reactive with R akari, a process requiring several weeks. Because patients often do not return for follow-up after the resolution of their illness, convalescent phase serum samples are frequently unavailable for confirma- 1545
2 4 3 No. of New Cases Jan Feb Mar Apr May Jun Jul Aug Sep Oct Nov Dec Jan Feb Mar Apr May Jun Jul Aug Sep Oct Nov Dec Jan Feb Date Figure 1. Rickettsialpox cases from January 1, 2001, through February 28, tory testing. Direct immunofluorescence testing for R rickettsii in fixed, paraffin-embedded tissue was developed initially as a test for Rocky Mountain spotted fever. 12 Because R rickettsii and R akari belong to the spotted fever group of rickettsiae and their antigens have a high level of cross-reactivity, 13 immunofluorescence testing and, more recently, immunohistochemical (IHC) staining using an anti R rickettsii antibody 14,15 have been used successfully to diagnose rickettsialpox using paraffinembedded skin biopsy specimens. More than 800 cases of rickettsialpox have been described, nearly 500 of these in the 3 years after the disease was first identified. 16 Since the 1960s, only single case reports and small case series have been published, and most of these cases have occurred in New York City. 1,9,11,15,17-19 The largest of these series described 13 patients examined during a 10-year period. 11 Rickettsialpox is still endemic in New York City, and an average of 3 to 4 patients are diagnosed annually as having rickettsialpox at our institution. We report a large series of 18 rickettsialpox cases seen in a large tertiary care hospital in New York City from February 23, 2001, through October 31, We used skin biopsy specimens, serological test results, and IHC results to confirm the clinical diagnosis. METHODS Consecutive patients with clinical features suggestive of rickettsialpox were examined at the Department of Dermatology at Columbia-Presbyterian Medical Center, New York City, from February 23, 2001, through October 31, Eleven patients were referred after being evaluated in the emergency department or in outpatient internal medicine clinics, 5 were selfreferred to the dermatology clinic, 1 was seen in the emergency department, and 1 was examined while hospitalized. After obtaining informed consent, skin biopsy specimens of eschars and papulovesicular lesions were obtained using a 2.5- or 3.0-mm punch. Tissue sections were stained with hematoxylin-eosin and evaluated for epidermal changes, necrosis, dermal inflammation, and vascular alterations. Immunohistochemical staining for spotted fever group rickettsiae was performed at the Centers for Disease Control and Prevention using a previously described immunoalkaline phosphatase technique. 14,15 Briefly, a rabbit polyclonal anti R rickettsii antibody was used as the primary antibody; this antibody is known to cross-react with other spotted fever rickettsiae, including R akari. Paired acute and convalescent phase serum specimens were obtained from 9 patients, and a single acute or convalescent phase sample was obtained from 9 patients. These samples were tested for IgG antibody reactive with R akari antigen using an indirect immunofluorescence assay at the Centers for Disease Control and Prevention, as previously described. 11 RESULTS Eighteen patients with laboratory-confirmed rickettsialpox (6 males and 12 females), who ranged in age from 15 months to 73 years, were examined during a 20- month period (Figure 1). The clinical features of the 18 patients diagnosed as having rickettsialpox are shown in Table 1. The presenting complaints for all patients were fever and rash. Of the 18 patients, 17 (94%) presented with the classic triad of an eschar (Figure 2A and B), fever, and papulovesicular rash (Figure 3A and B); all patients had a papulovesicular rash on the trunk and extremities. Only 2 patients (11%) complained of pruritus, and 4 patients (22%) had an enanthema, characterized by small erosions of the palate, tonsils, uvula, tongue, or pharynx. Patients self-reported fever ranged from 38.3 C to 40.6 C (median, 39.3 C). The duration of the rash before presentation ranged from 3 to 9 days (median, 7 days). When the eschar was pointed out to patients during the examination, most did not know how long their eschar had been present, and 5 (28%) were not aware of having an eschar until it was revealed during the physical examination. The most common location of the eschars was around the ankle, as seen in 5 patients (28%). Other locations included the calf, forearm, and back (2 patients, or 11%, for each location); and the chin, neck, chest, upper arm, abdomen, and thigh (1 patient, or 6%, for each location). Sixteen patients (89%) presented with a headache, and 7 (39%) complained of diffuse myalgias. Less common signs and symptoms were lymphadenopathy, gastrointestinal complaints, dizziness, anorexia, sore throat, and arthralgias. Three patients were initially thought to have cutaneous anthrax. Other initial clinical diagnoses included herpesvirus infection, Lyme disease, syphilis, and viral exanthem. Thirteen patients underwent hematologic and 1546
3 Table 1. Comparison of Clinical Characteristics and Diagnostic Results for Rickettsialpox in 4 Reported Case Series* Feature Present Study Kass et al, Rose, Greenberg et al, Papulovesicular eruption 18/18 (100) 13/13 (100) 35/35 (100) 144/144 (100) Necrotic eschar 17/18 (94) 13/13 (100) 29/35 (83) 82/86 (95) Fever 17/18 (94) Common 35/35 (100) 144/144 (100) Headache 16/18 (89) Common 35/35 (100) 130/144 (90) Myalgias or back pain 7/18 (39) Common Often 73/144 (51) Sore throat 7/18 (39) Less frequent Occasionally 6/144 (4) Gastrointestinal symptoms 5/18 (28) 0/13 Occasionally 11/144 (8) Arthralgias 5/18 (28) NR NR NR Enanthema 4/18 (22) 0/13 9/35 (26) 2/144 (1) Lymphadenopathy Regional 3/18 (17) Less frequent Usually Usually Generalized 0/17 0/13 5/35 (14) Uncommon Compatible histopathologic 18/18 (100) 13/13 (100) NR NR features IHC results positive Eschars 16/16 (100) 5/7 (71) ND ND Papules 5/9 (56) 1/10 (10) ND ND Positive serological results 15/18 (83) 9/9 (100) ND ND Abbreviations: IHC, immunohistochemical; ND, not done; NR, not reported. *Data are given as number of patients with the feature/number of patients examined (percentage). Comments in quotations refer to the original authors descriptions in cases in which features were not quantified. A skin biopsy specimen of an eschar showing epidermal and dermal necrosis and a superficial and deep perivascular mononuclear cell infiltrate and/or a skin biopsy specimen of a papulovesicle showing a perivascular mononuclear cell infiltrate and any degree of dermal edema. A 4-fold or greater increase in the serum IgG antibody titer reactive with Rickettsia akari or a single IgG titer of 1:64 or greater. Source biochemical tests during their initial evaluation in the emergency department. Of these 13 patients, 4 (31%) had mild leukopenia, with a white blood cell count ranging from /µl to /µl (normal range, /µl /µl). Two patients (15%) had leukocytosis. One patient had a white blood cell count of /µl, with 6% bands. The 15-month-old child had a markedly elevated white blood cell count of / µl, with 60% neutrophils, and a erythrocyte sedimentation rate of 95 mm/h (normal rate, 0-20 mm/h). Three patients (23%) had mild thrombocytopenia, with a platelet count ranging from /µl to /µl (normal range, /µl /µl). One patient (8%) each had mild transaminase elevations (aspartate aminotransferase level, 63 U/L [normal, U/L]; and alanine aminotransferase level, 128 U/L [normal, 7-41 U/L]), an elevated alkaline phosphatase level (177 U/L [normal, U/L]), and an elevated lactate dehydrogenase level (415 U/L [normal, U/L]). Sixteen patients were diagnosed clinically as having rickettsialpox in the dermatology clinic, and were treated with a 7-day course of doxycycline (100 mg orally twice a day). All but 1 of the patients seemed only mildly ill. One patient had a toxic appearance and vomited several times during her examination in the dermatology clinic; she was hospitalized and treated with intravenous doxycycline (100 mg twice a day) for 3 days before being discharged and treated with oral doxycycline for 5 days. Another patient, the 15-month-old girl, was diagnosed clinically as having rickettsialpox vs an atypical viral exanthem. Because she had a markedly elevated white blood cell count and erythrocyte sedimentation rate, the attending pediatric rheumatologist requested an echocardiogram to rule out atypical mucocutaneous lymph node syndrome. The patient was hospitalized for 2 days and treated with a single dose of intravenous ceftriaxone sodium, 75 mg/kg, and a 7-day course of oral erythromycin, 18 mg/kg per dose every 8 hours. Fever and other systemic symptoms resolved after 24 to 48 hours of antibiotic therapy in all patients. In 12 (86%) of the 14 patients, the papulovesicular eruption had completely resolved by the follow-up visit 1 week after presentation, with only minimal postinflammatory hyperpigmentation. Eschars were seen in 17 of the 18 patients; these healed in 3 to 4 weeks, leaving a small depressed scar in 2 (50%) of the 4 patients seen at the 1-month follow-up visit. A biopsy specimen was obtained from 16 of the 17 eschars. The histopathologic features of the eschars were characterized by variable degrees of epidermal and dermal necrosis (Figure 2C and D). There was a direct correlation between the amount of necrosis in the dermis and epidermis: the more significant the necrosis of the upper portion of the dermis, the greater the degree of epidermal necrosis with ulceration. Ulcerated lesions typically had neutrophils and thrombosed vessels in the ulcer base. The primary pattern of inflammation in all cases was that of a superficial and deep perivascular mononuclear cell infiltrate; 2 lesions had interstitial neutrophils throughout the dermis. None of the eschars showed a leukocytoclastic vasculitis. Papulovesicular lesions showed a spectrum of changes (Figure 3C-E), consisting of variable degrees of papillary dermal edema and a sparse or dense superficial and middermal perivascular mononuclear cell infiltrate. None of the lesions showed epidermal necrosis or leukocytoclastic vasculitis. Immunohistochemical staining revealed spotted fever group rickettsiae in all of the 16 eschars for which biopsy specimens were obtained and in 5 of the 9 pap- 1547
4 A B C D Figure 2. Clinical features of the eschar of rickettsialpox on the abdomen of patient 2 (with associated papulovesicles) (A) and the ankle of patient 10 (B). C, Histopathologic features of a typical eschar showing confluent epidermal necrosis. Engorged blood vessels in the superficial, mid, and deep dermis are surrounded by a dense mononuclear cell infiltrate (hematoxylin-eosin, original magnification 10). D, A higher magnification of the eschar s histopathologic features showing the dense perivascular infiltrate of predominantly mononuclear cells and the dilated vessels containing erythrocytes (hematoxylin-eosin, original magnification 62.5). ules (Table 2). Staining was identified predominantly within the macrophages and mononuclear cells of the perivascular infiltrates associated with these lesions (Figure 4). A 4-fold or greater increase in antibodies reactive with R akari was detected in all 9 patients for whom paired acute and convalescent phase serum samples were available (Table 2). For 9 patients, only 1 serum specimen (acute or convalescent phase) was obtained. Six patients had single elevated titers reactive with R akari. One patient each had an acute phase titer of 1:64, 1:128, 1:256, 1:512, and 1:2048, and 1 patient had a single convalescent phase titer of 1:512. COMMENT The 18 rickettsialpox cases seen in our institution during the 20-month period are noteworthy, because this represents a 3-fold increase in our annual number of cases 1548
5 A D B E C Figure 3. Clinical features of the papulovesicles of rickettsialpox. A, Typical scattered papulovesicles on the back of patient 5. B, Close-up of a papulovesicle. The histopathologic features of papulovesicles show a spectrum of inflammatory changes, ranging from a sparse superficial perivascular mononuclear cell infiltrate (C) to a moderately dense perivascular mononuclear cell infiltrate (D) to severe papillary dermal edema with a moderately dense superficial and middermal perivascular mononuclear cell infiltrate (E) (hematoxylin-eosin, original magnification 25). compared with the previous 5 years. Of our patients, 9 (50%) presented in the 5 months following media reports of the cutaneous anthrax cases in October 2001 (Figure 1). In contrast, there were only 3 rickettsialpox cases in the 5 months preceding the attacks, and we identified only 1 case of rickettsialpox during the corresponding period in 2002 to Immediately following the bioterrorism attacks, clinicians and patients were likely to be more observant and much more concerned about a cutaneous eschar. Several researchers 1,11,17,18 have suggested that rickettsialpox is probably underrecognized and underreported, perhaps because patients with mild disease do not seek medical attention or because clinicians may diagnose patients with rickettsialpox as having chickenpox or other diseases. Alternatively, the true incidence of rickettsialpox in our catchment area may be increasing because of environmental conditions favoring disease transmission (eg, more crowded housing, larger mouse populations, a change in the mite species infesting mice, or the presence of murine diseases that encourage mites to find alternative hosts, such as humans). 1,2,17,21 Our patients clinical presentations are similar to those described in previous historical and contemporary reports (Table 1), with most patients (94%) presenting with the classic triad of fever, eschar, and rash. This presenta- 1549
6 Table 2. Immunohistochemical Staining of Skin Biopsy Specimens and Anti Rickettsia akari Serum Antibodies in 18 Patients With Rickettsialpox Immunohistochemical Staining Patient No./Sex/Age Date of Presentation Lesion Result Phase Anti R akari Antibody Titers (Determined by IFA) 1/M/24 y 2/23/01 Eschar Not identified Acute ND Papule Negative Convalescent 512 2/F/60 y 5/5/01 Eschar Positive Acute 32 Convalescent 512 3/M/48 y 7/23/01 Eschar Positive Acute 32 Convalescent /F/32 y 8/8/01 Eschar Positive Acute 32 Convalescent 512 5/F/29 y 10/9/01 Eschar Positive Acute 32 Convalescent ND 6/F/21 y 10/16/01 Eschar Positive Acute 128 Convalescent 512 7/M/29 y 11/2/01 Eschar Positive Acute 32 Convalescent /F/51 y 11/13/01 Eschar Positive Acute 32 Papule Positive Convalescent /F/15 mo 12/21/01 Eschar ND Acute 256 Convalescent /F/36 y 12/28/01 Eschar Positive Acute 32 Papule Equivocal Convalescent /M/25 y 1/29/02 Eschar Positive Acute 64 Convalescent ND 12/F/55 y 2/5/02 Eschar Positive Acute 128 Papule Positive Convalescent /F/42 y 2/20/02 Eschar Positive Acute 32 Papule Positive Convalescent ND 14/F/25 y 2/23/02 Eschar Positive Acute 512 Convalescent ND 15/M/73 y 3/11/02 Eschar Positive Acute 32 Papule Negative Convalescent ND 16/F/59 y 5/20/02 Eschar Positive Acute 2048 Papule Negative Convalescent ND 17/M/51 y 8/5/02 Eschar Positive Acute 256 Papule Positive Convalescent ND 18/F/59 y 10/31/02 Eschar Positive Acute 128 Papule Positive Convalescent ND Abbreviations: IFA, immunofluorescence assay; ND, not done. Figure 4. Abundant immunohistochemical staining of spotted fever group rickettsiae within the perivascular macrophages and mononuclear cells of an eschar, visualized by using a polyclonal rabbit anti Rickettsia rickettsii antibody (immunoalkaline phosphatase with naphthol fast red substrate and hematoxylin counterstain, original magnification 158). tion should alert clinicians to consider rickettsialpox. Headache was common (89%), and myalgias were seen in more than one third (39%) of our patients. An enanthema of the oral mucosa was present in one fifth (22%) of our patients. Although regional lymphadenopathy was commonly reported when rickettsialpox was first described in the mid to late 1940s, 16,20,22 it was present in only 3 (17%) of our patients. Generalized lymphadenopathy, which was described in a few patients in earlier case series, was not seen in any of our patients (Table 1). In general, routine laboratory test results do not contribute to the diagnosis of rickettsialpox. 1,16 Mild leukopenia and mild thrombocytopenia have been described during the acute phase of the disease 9,11,15,16,20,22 and were seen in approximately one third of the patients we examined. In our series, the most dramatic laboratory abnormalities (a markedly elevated white blood cell count and erythrocyte sedimentation rate) were seen in the youngest patient. The disease most commonly confused with rickettsialpox is chickenpox. 1,2,11,18 Patients with rickettsialpox generally have fewer lesions than patients with chickenpox, and the lesions do not appear in crops. Although rickettsialpox may be rarely associated with pruritus, the pruritus of chickenpox is usually much more severe. In addition, the classic dew drop on a rose petal lesion of 1550
7 chickenpox is morphologically distinct from the erythematous papules, with or without a tiny central vesicle, seen in rickettsialpox. Skin lesions in various stages of evolution (papules, vesicles, and crusts) occur concomitantly in chickenpox, whereas the lesions of rickettsialpox are typically monomorphic. Perhaps the most useful distinguishing feature is the eschar, which is present in nearly all patients with rickettsialpox but not classically associated with chickenpox. Numerous eschar-associated rickettsial diseases may resemble rickettsialpox, including Mediterranean spotted fever, African tick bite fever, Queensland tick typhus, Siberian tick typhus, and scrub typhus. 1,2,20 Rocky Mountain spotted fever is only rarely associated with an eschar. 23,24 The geographic distributions of most of these diseases are helpful for establishing a diagnosis 1,25 (Table 3). The differential diagnosis of a single necrotic eschar also includes cutaneous anthrax, aspergillosis, spider bite, ecthyma gangrenosum, factitial dermatitis, and trauma. 26 Cutaneous anthrax starts as a painless pruritic papule. 26,27 The papule enlarges and develops a central vesicle or bulla, which may have satellite vesicles and which is surrounded by a striking brawny, nonpitting edema that is absent in rickettsialpox. 26,27 The vesicle subsequently ulcerates and is covered by a single, painless, necrotic eschar. (The eschar of rickettsialpox is also painless and may occasionally be pruritic.) Low-grade fever, regional lymphadenopathy, and malaise are common findings, 26,27 but a papulovesicular rash does not occur, which distinguishes this disease clinically from rickettsialpox. No specific histologic features definitively differentiate the eschars of anthrax from those of rickettsialpox, and both diseases share a spectrum of inflammatory changes and dermal and epidermal necrosis. However, marked edema and hemorrhage are generally identified with greater frequency in the lesions of cutaneous anthrax. Other diseases that cause a sparse papulovesicular eruption and that may be confused with rickettsialpox include infectious mononucleosis, several enterovirus infections (such as echovirus types 9 and 16, coxsackievirus A types 9 and 16, and coxsackievirus B type 5), gonococcemia, and eczema vaccinatum. 1,2,17,18 Rickettsialpox is usually a mild self-limited illness that resolves in 6 to 10 days without treatment. 1,2,18 To our knowledge, there are no relapses after infection with R akari and there have been no reported fatalities. 1,2,11 Headache and lassitude may persist for up to 2 weeks after resolution of the fever. Symptoms during the acute illness can occasionally be severe, requiring hospitalization in a few patients. In our series, 3 patients (17%) were hospitalized. The treatment of choice for rickettsialpox is doxycycline, which can dramatically reduce the duration of systemic symptoms (and is also indicated for the treatment of cutaneous anthrax 26,27 ). The recommended dosage of doxycycline is 100 mg orally or intravenously twice a day for 7 days (vs 60 days for cutaneous anthrax associated with bioterrorism 26,27 ). Chloramphenicol may be given to patients who are younger than 8 years or allergic to doxycycline. 1,18 The histopathologic features of our patients eschars (epidermal and dermal necrosis, a superficial and Table 3. Geographic Distribution of Rickettsial Diseases With Eschars That May Be Confused With Rickettsialpox Causative Agent Disease Geographic Distribution Rickettsia conorii Mediterranean spotted fever, boutonneuse fever, and Indian tick typhus Around the Mediterranean Sea, southern Europe, Russia, India, Pakistan, and Africa Rickettsia africae African tick bite fever Sub-Saharan Africa Rickettsia australis Queensland tick Australia typhus Rickettsia sibirica Siberian tick typhus Russia, Siberia, northern China, and Pakistan Rickettsia rickettsii Orientia tsutsugamushi Rocky Mountain spotted fever Scrub typhus United States (especially southeastern and western), Canada, and parts of Central and South America Southeast Asian, Australia, and the South Pacific deep perivascular mononuclear cell infiltrate, and blood vessel thrombosis or necrosis) and papulovesicles (variable papillary dermal edema and a superficial and middermal perivascular mononuclear cell infiltrate) are similar to those described by Kass et al, 11 although we do not use the term lymphocytic vasculitis. The histologic features of rickettsialpox are characteristic, but not diagnostic. Histopathologic analysis of a papulovesicle, however, can help exclude other diseases in the clinical differential diagnosis, such as herpesvirus infections and a tick bite reaction, characterized by multinucleated giant cells and (often) the presence of mouthparts, respectively. In our series, IHC staining of skin biopsy specimens provided the most sensitive method of confirming the diagnosis. This assay was positive for the diagnosis in 21 (84%) of 25 biopsy specimens tested. Biopsy specimens of eschars provided the best sample for evaluation: all eschars were positive for rickettsialpox, compared with only 56% of the papulovesicles. Rickettsialpox should be considered in the differential diagnosis of patients presenting with fever, an eschar, and a papulovesicular eruption, especially in areas where the disease is common, such as New York City. Cutaneous anthrax resulting from natural exposure or acts of bioterrorism is in the differential diagnosis of rickettsialpox; this underscores the importance of clinicians ability to promptly recognize and definitively diagnose rickettsialpox. During the acute phase of rickettsialpox, IHC testing of a skin biopsy specimen from the eschar is the best method for confirming the clinical diagnosis. This test is highly sensitive, requires only 1 patient visit, and may provide results in a few days. Although serological results can be useful in confirming the diagnosis of rickettsialpox, seroconversion may not occur for several weeks and at least 2 patient visits are necessary for the collection of serum samples. Early recognition of the clinical presentation of rickettsialpox and the availability of a sensitive confirmatory IHC test should lead to more rapid and accurate diagnosis and prompt institution of appropriate therapy. 1551
8 Accepted for publication June 25, From the Department of Dermatology, Columbia University College of Physicians & Surgeons, New York, NY (Drs Koss, Carter, Grossman, Silvers, and Rabinowitz); and the Viral and Rickettsial Zoonoses Branch (Mr Singleton and Dr Paddock) and Infectious Disease Pathology Activity (Dr Zaki), the Division of Viral and Rickettsial Diseases, National Center for Infectious Diseases, Centers for Disease Control and Prevention, Atlanta, Ga. Dr Paddock is now with Infectious Disease Pathology Activity, the Division of Viral and Rickettsial Diseases, National Center for Infectious Diseases, Centers for Disease Control and Prevention. This study was supported by the Department of Dermatology, Columbia-Presbyterian Medical Center. We thank Lindy P. Fox, MD, Adam S. Geyer, MD, Joseph M. Obadiah, MD, and Robert R. Walther, MD, for referring their patients with rickettsialpox. Corresponding author and reprints: Tamara Koss, MD, Department of Dermatology, Columbia University College of Physicians & Surgeons, 161 Fort Washington Ave, 12th Floor, New York, NY ( REFERENCES 1. Brettman LR, Lewin S, Holzman RS, et al. Rickettsialpox: report of an outbreak and a contemporary review. Medicine (Baltimore). 1981;60: Boyd AS. Rickettsialpox. Dermatol Clin. 1997;15: Pike G, Cohen S, Murray E. Rickettsialpox: report of serologically proven case occurring in a resident of Boston. N Engl J Med. 1950;243: Rindge M. Connecticut has first rickettsialpox outbreak. Conn Health Bull. 1952; 66: Comer JA, Tzianabos T, Flynn C, Vlahov D, Childs JE. Serologic evidence of rickettsialpox (Rickettsia akari ) infection among intravenous drug users in innercity Baltimore, Maryland. Am J Trop Med Hyg. 1999;60: Hoeprich P, Kent G, Dingle J. Rickettsialpox: report of a serologically proved case in Cleveland. N Engl J Med. 1956;254: LaBocetta A, Israel H, Perri A, Siegel M. Rickettsialpox: report of four apparent cases in Pennsylvania. Am J Med. 1952;13: Lackman D. A review of information on rickettsialpox in the United States. Clin Pediatr. 1963;2: Krusell A, Comer JA, Sexton DJ. Rickettsialpox in North Carolina: a case report. Emerg Infect Dis. 2002;8: Eremeeva ME, Balayeva NM, Ignatovich VF, Raoult D. Proteinic and genomic identification of spotted fever group rickettsiae isolated in the former USSR. J Clin Microbiol. 1993;31: Kass EM, Szaniawski WK, Levy H, Leach J, Srinivasan K, Rives C. Rickettsialpox in a New York City hospital, 1980 to N Engl J Med. 1994;331: Walker DH, Cain BG. A method for specific diagnosis of Rocky Mountain spotted fever on fixed, paraffin-embedded tissue by immunofluorescence. J Infect Dis. 1978;137: Hebert GA, Tzianabos T, Gamble WC, Chappell WA. Development and characterization of high-titered, group-specific fluorescent-antibody reagents for direct identification of rickettsiae in clinical specimens. J Clin Microbiol. 1980;11: Paddock CD, Greer PW, Ferebee TL, et al. Hidden mortality attributable to Rocky Mountain spotted fever: immunohistochemical detection of fatal, serologically unconfirmed disease. J Infect Dis. 1999;179: Sanders S, Di Costanzo D, Leach J, et al. Rickettsialpox in a patient with HIV infection. J Am Acad Dermatol. 2003;48: Rose H. The clinical manifestations and laboratory diagnosis of rickettsialpox. Ann Intern Med. 1949;31: Wong B, Singer C, Armstrong D, Millian SJ. Rickettsialpox: case report and epidemiologic review. JAMA. 1979;242: Heymann WR. Rickettsialpox. Clin Dermatol. 1996;14: Jacobson JM, Desmond EP, Kornblee LV, Hirschman SZ. Positive Weil-Felix reactions in a case of rickettsialpox. Int J Dermatol. 1989;28: Greenberg M, Pellitteri O, Klein I, Huebner R. Rickettsialpox a newly recognized disease, II: clinical observations. JAMA. 1947;133: Krinsky WL. Does epizootic lymphocytic choriomeningitis prime the pump for epidemic rickettsialpox? Rev Infect Dis. 1983;5: Greenberg M, Pellitteri O. Rickettsialpox. Bull N Y Acad Med. 1947;23: Cox GM, Sexton DJ. Photo quiz: Rocky Mountain spotted fever. Clin Infect Dis. 1995;21:315, Walker DH, Gay RM, Valdes-Dapena M. The occurrence of eschars in Rocky Mountain spotted fever. J Am Acad Dermatol. 1981;4: McCalmont C, Zanolli MD. Rickettsial diseases. Dermatol Clin. 1989;7: Carucci JA, McGovern TW, Norton SA, et al. Cutaneous anthrax management algorithm. J Am Acad Dermatol. 2002;47: Swartz MN. Recognition and management of anthrax: an update. N Engl J Med. 2001;345:
African tick typhus. David Mabey
 African tick typhus David Mabey 25 year old English man Holiday in Zimbabwe for 3 months Became unwell on plane home Fever Rash Generalised lymphadenopathy This photo was taken 2 days after onset of symptoms
African tick typhus David Mabey 25 year old English man Holiday in Zimbabwe for 3 months Became unwell on plane home Fever Rash Generalised lymphadenopathy This photo was taken 2 days after onset of symptoms
Laboratory Diagnosis of Endemic
 Laboratory Diagnosis of Endemic Typhus and Rocky Mountain Spotted Fever* L. F. BADGER, M.D. P. A. Surgeon, U. S. Public Health Service, Washington, D. C. THERE is widely scattered throughout the world
Laboratory Diagnosis of Endemic Typhus and Rocky Mountain Spotted Fever* L. F. BADGER, M.D. P. A. Surgeon, U. S. Public Health Service, Washington, D. C. THERE is widely scattered throughout the world
Alberta Health Public Health Notifiable Disease Management Guidelines January 2013
 January 2013 Rickettsial Infections Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) January 2013 January 2013 December
January 2013 Rickettsial Infections Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) January 2013 January 2013 December
WFSICCM SEOUL Managing Scrub Typhus in ICU
 WFSICCM SEOUL 2015 Managing Scrub Typhus in ICU Dr. Shivakumar Iyer Professor & Head Dept of Critical Care Medicine Bharati Vidyapeeth University Medical College, Pune President Indian Society of Critical
WFSICCM SEOUL 2015 Managing Scrub Typhus in ICU Dr. Shivakumar Iyer Professor & Head Dept of Critical Care Medicine Bharati Vidyapeeth University Medical College, Pune President Indian Society of Critical
Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India.
 Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Alberta Health Public Health Notifiable Disease Management Guidelines July 2012
 July 2012 Typhus - Louseborne Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) July 2012 July 2012 October 2005 Case Definition
July 2012 Typhus - Louseborne Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) July 2012 July 2012 October 2005 Case Definition
- Mycoplasma and Ureaplasma. - Rickettsia
 - Mycoplasma and Ureaplasma - Rickettsia Mycoplasma and Ureaplasma Family: Mycoplasmataceae Genus: Mycoplasma Species: M. pneumoniae Species: M. hominis Species: M. genitalium Genus: Ureaplasma Species:
- Mycoplasma and Ureaplasma - Rickettsia Mycoplasma and Ureaplasma Family: Mycoplasmataceae Genus: Mycoplasma Species: M. pneumoniae Species: M. hominis Species: M. genitalium Genus: Ureaplasma Species:
VARICELLA. Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara
 VARICELLA (Chicken pox) Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara Definition : Varicella is a common contagious disease caused
VARICELLA (Chicken pox) Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara Definition : Varicella is a common contagious disease caused
Patricia A. Treadwell, M.D. Professor of Pediatrics
 EXANTHEMS Patricia A. Treadwell, M.D. Professor of Pediatrics Indiana University School of Medicine FACULTY DISCLOSURE I have the following financial relationships with the manufacturer(s) of any commercial
EXANTHEMS Patricia A. Treadwell, M.D. Professor of Pediatrics Indiana University School of Medicine FACULTY DISCLOSURE I have the following financial relationships with the manufacturer(s) of any commercial
Mycoplasmas and other tiny bacteria. Some are disease agents, several have only been recognized over the past few years
 Mycoplasmas and other tiny bacteria Some are disease agents, several have only been recognized over the past few years Mycoplasma biology Tiny, filamentous, pleomorphic, aerobic and anaerobic Filterable
Mycoplasmas and other tiny bacteria Some are disease agents, several have only been recognized over the past few years Mycoplasma biology Tiny, filamentous, pleomorphic, aerobic and anaerobic Filterable
Skin and joint manifestations of
 Australasian Society for Infectious Diseases Skin and joint manifestations of Arboviruses and Rickettsia Dominic Dwyer Dominic Dwyer Centre for Infectious Diseases and Microbiology ICPMR Westmead Hospital
Australasian Society for Infectious Diseases Skin and joint manifestations of Arboviruses and Rickettsia Dominic Dwyer Dominic Dwyer Centre for Infectious Diseases and Microbiology ICPMR Westmead Hospital
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 21 January 1, 29 December 31, 29 Commentary West Nile virus (WNV) is a mosquito-borne virus that
West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 21 January 1, 29 December 31, 29 Commentary West Nile virus (WNV) is a mosquito-borne virus that
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 2009 January 1, 2008 December 31, 2008 Commentary West Nile virus (WNV) is a mosquito-borne virus
West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 2009 January 1, 2008 December 31, 2008 Commentary West Nile virus (WNV) is a mosquito-borne virus
Degos Disease: A Case Report and Review of Literature
 Degos Disease: A Case Report and Review of Literature Monira waked Egyptian Dermatology Online Journal 4 (1): 5, June 2008 Al Houd Al Marsod Hospital Submitted for publication: May 25 th, 2008 Accepted
Degos Disease: A Case Report and Review of Literature Monira waked Egyptian Dermatology Online Journal 4 (1): 5, June 2008 Al Houd Al Marsod Hospital Submitted for publication: May 25 th, 2008 Accepted
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County A Culex quinquefasciatus mosquito on a human finger. Image by James Gathany/ CDC gov/ public domain Maricopa County Department of Public Health Office of Epidemiology
West Nile Virus in Maricopa County A Culex quinquefasciatus mosquito on a human finger. Image by James Gathany/ CDC gov/ public domain Maricopa County Department of Public Health Office of Epidemiology
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Culex larvae found collecting in standing water Image by CDC/James Gathany - License: Public Domain. Maricopa County Department of Public Health Office of Epidemiology
West Nile Virus in Maricopa County Culex larvae found collecting in standing water Image by CDC/James Gathany - License: Public Domain. Maricopa County Department of Public Health Office of Epidemiology
Tickborne Disease Case Investigations
 Massachusetts Department of Public Health Bureau of Infectious Disease and Laboratory Sciences Tickborne Disease Case Investigations Anthony Osinski, MPH May 31, 2018 Factors Associated with Increasing
Massachusetts Department of Public Health Bureau of Infectious Disease and Laboratory Sciences Tickborne Disease Case Investigations Anthony Osinski, MPH May 31, 2018 Factors Associated with Increasing
Technical Bulletin No. 121
 CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 121 January 31, 2014 Lyme Blot, IgG and IgM - Now Performed at CPAL Contact: J. Matthew Groeller, 717.851.1416 Operations Manager, Clinical
CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 121 January 31, 2014 Lyme Blot, IgG and IgM - Now Performed at CPAL Contact: J. Matthew Groeller, 717.851.1416 Operations Manager, Clinical
SELECTED INFECTIONS ACQUIRED DURING TRAVELLING IN NORTH AMERICA. Lin Li, MD August, 2012
 SELECTED INFECTIONS ACQUIRED DURING TRAVELLING IN NORTH AMERICA Lin Li, MD August, 2012 Case 1 32 year old male working in Arizona; on leave back in Singapore Presented to hospital A for fever x (7-10)
SELECTED INFECTIONS ACQUIRED DURING TRAVELLING IN NORTH AMERICA Lin Li, MD August, 2012 Case 1 32 year old male working in Arizona; on leave back in Singapore Presented to hospital A for fever x (7-10)
A. Erythema multiforme and related diseases
 Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
CPC. Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand
 CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
LYME DISEASE Last revised May 30, 2012
 Wisconsin Department of Health Services Division of Public Health Communicable Disease Surveillance Guideline LYME DISEASE Last revised May 30, 2012 I. IDENTIFICATION A. CLINICAL DESCRIPTION: A multi-systemic
Wisconsin Department of Health Services Division of Public Health Communicable Disease Surveillance Guideline LYME DISEASE Last revised May 30, 2012 I. IDENTIFICATION A. CLINICAL DESCRIPTION: A multi-systemic
Elsevier B.V.; この論文は出版社版でありま Right 引用の際には出版社版をご確認ご利用ください This is
 Title Refractory cutaneous lichenoid sarc tranilast. Author(s) Nakahigashi, Kyoko; Kabashima, Kenj Utani, Atsushi; Miyachi, Yoshiki Citation Journal of the American Academy of 63(1): 171-172 Issue Date
Title Refractory cutaneous lichenoid sarc tranilast. Author(s) Nakahigashi, Kyoko; Kabashima, Kenj Utani, Atsushi; Miyachi, Yoshiki Citation Journal of the American Academy of 63(1): 171-172 Issue Date
Uncommon clinical presentations of leprosy: apropos of three cases
 Lepr Rev (2016) 87, 246 251 CASE REPORT Uncommon clinical presentations of leprosy: apropos of three cases RASHMI JINDAL* & NADIA SHIRAZI** *Department of Dermatology, Venereology & Leprosy, Himalayan
Lepr Rev (2016) 87, 246 251 CASE REPORT Uncommon clinical presentations of leprosy: apropos of three cases RASHMI JINDAL* & NADIA SHIRAZI** *Department of Dermatology, Venereology & Leprosy, Himalayan
Update on Lyme Disease Surveillance in Wisconsin for Providers and Laboratories
 Update on Lyme Disease Surveillance in Wisconsin for Providers and Laboratories Christopher Steward Division of Public Health Wisconsin Department of Health Services 04/10/14 Protecting and promoting the
Update on Lyme Disease Surveillance in Wisconsin for Providers and Laboratories Christopher Steward Division of Public Health Wisconsin Department of Health Services 04/10/14 Protecting and promoting the
Scrub typhus cases in a family
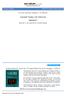 www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS Scrub typhus cases in a family Yasuyuki Taooka, Gen Takezawa ABSTRACT Abstract is not required for Clinical Images International Journal
www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS Scrub typhus cases in a family Yasuyuki Taooka, Gen Takezawa ABSTRACT Abstract is not required for Clinical Images International Journal
Egyptian Dermatology Online Journal Vol. 6 No 1: 14, June 2010
 Wells Syndrome H. Gammaz, H. Amer, A. Adly and S. Mahmoud Egyptian Dermatology Online Journal 6 (1): 14 Al-Haud Al-Marsoud Hospital, Cairo, Egypt e-mail: hananderma@hotmail.com Submitted: April 15, 2010
Wells Syndrome H. Gammaz, H. Amer, A. Adly and S. Mahmoud Egyptian Dermatology Online Journal 6 (1): 14 Al-Haud Al-Marsoud Hospital, Cairo, Egypt e-mail: hananderma@hotmail.com Submitted: April 15, 2010
Increasing Incidence of Rocky Mountain Spotted Fever among the American Indian Population in the United States
 Am. J. Trop. Med. Hyg., 80(4), 2009, pp. 601 605 Copyright 2009 by The American Society of Tropical Medicine and Hygiene Increasing Incidence of Rocky Mountain Spotted Fever among the American Indian Population
Am. J. Trop. Med. Hyg., 80(4), 2009, pp. 601 605 Copyright 2009 by The American Society of Tropical Medicine and Hygiene Increasing Incidence of Rocky Mountain Spotted Fever among the American Indian Population
Citation The Journal of Dermatology, 37(8), available at
 NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
Rickettsial Infections
 Rickettsial Infections COL Mark Kortepeter, MD, MPH Associate Dean for Research Consultant to the Army Surgeon General for Biodefense Uniformed Services University, Bethesda, MD September 2014 UNCLASSIFIED
Rickettsial Infections COL Mark Kortepeter, MD, MPH Associate Dean for Research Consultant to the Army Surgeon General for Biodefense Uniformed Services University, Bethesda, MD September 2014 UNCLASSIFIED
Mike Rossman, MD; Daniel J. Schissel, MD
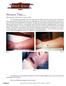 Picture This. Mike Rossman, MD; Daniel J. Schissel, MD You are building relationships with a tribe that primarily inhabits the border region between Iraq and Syria when you are asked to examine a skin
Picture This. Mike Rossman, MD; Daniel J. Schissel, MD You are building relationships with a tribe that primarily inhabits the border region between Iraq and Syria when you are asked to examine a skin
Following the bite of a mosquito infected with CHIKV, most individuals will
 3. CLINICAL 3A. Clinical Presentation of Acute Disease Following the bite of a mosquito infected with CHIKV, most individuals will present with symptomatic disease after an incubation period of 3-7 days
3. CLINICAL 3A. Clinical Presentation of Acute Disease Following the bite of a mosquito infected with CHIKV, most individuals will present with symptomatic disease after an incubation period of 3-7 days
Acute Renal Failure due to Acute Tubular Necrosis caused ACCEPTED. Division of Infectious Diseases, Departments of Internal Medicine 1, Chosun
 JCM Accepts, published online ahead of print on 14 November 2007 J. Clin. Microbiol. doi:10.1128/jcm.01040-07 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions. All
JCM Accepts, published online ahead of print on 14 November 2007 J. Clin. Microbiol. doi:10.1128/jcm.01040-07 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions. All
LESIONS OF THE ORAL CAVITY ORAL CAVITY. Oral Cavity Subsites 4/10/2013 LIPS TEETH GINGIVA ORAL MUCOUS MEMBRANES PALATE TONGUE ORAL LYMPHOID TISSUES
 LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders
 Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Using administrative medical claims data to estimate underreporting of infectious zoonotic diseases
 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 40% Percentage of Yearly Cases 30% 25% 20% 15% 10% 5% 0% January Februar March April May June July August Septem October Novem Decem January Februar March
2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 40% Percentage of Yearly Cases 30% 25% 20% 15% 10% 5% 0% January Februar March April May June July August Septem October Novem Decem January Februar March
Microscopic study of the normal skin in cases of mycosis fungoides
 Microscopic study of the normal skin in cases of mycosis fungoides M. El Darouti, S. Marzook, M. Bosseila, O. Abu Zeid, O. El- Safouri, A. Zayed, A. El-Ramly Egyptian Dermatology Online Journal 2 (1):
Microscopic study of the normal skin in cases of mycosis fungoides M. El Darouti, S. Marzook, M. Bosseila, O. Abu Zeid, O. El- Safouri, A. Zayed, A. El-Ramly Egyptian Dermatology Online Journal 2 (1):
Chapter. Severe Acute Respiratory Syndrome (SARS) Outbreak in a University Hospital in Hong Kong. Epidemiology-University Hospital Experience
 content Chapter Severe Acute Respiratory Syndrome (SARS) Outbreak in a University Hospital in Hong Kong 3 Nelson Lee, Joseph JY Sung Epidemiology-University Hospital Experience Diagnosis of SARS Clinical
content Chapter Severe Acute Respiratory Syndrome (SARS) Outbreak in a University Hospital in Hong Kong 3 Nelson Lee, Joseph JY Sung Epidemiology-University Hospital Experience Diagnosis of SARS Clinical
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
Lyme Disease Surveillance in Wisconsin Christopher Steward Division of Public Health Wisconsin Department of Health Services 04/10/2014
 Lyme Disease Surveillance in Wisconsin Christopher Steward Division of Public Health Wisconsin Department of Health Services 04/10/2014 Protecting and promoting the health and safety of the people of Wisconsin
Lyme Disease Surveillance in Wisconsin Christopher Steward Division of Public Health Wisconsin Department of Health Services 04/10/2014 Protecting and promoting the health and safety of the people of Wisconsin
A comparative trial of Azithromycin versus Doxycycline for the treatment in Rickettsial Fever
 Original article A comparative trial of Azithromycin versus Doxycycline for the treatment in Rickettsial Fever Dr Deo Bhushan, Dr Jadhav Jayashree, DR Nigavekar P V, DR Himanshu Kumar Department of Pediatrics,
Original article A comparative trial of Azithromycin versus Doxycycline for the treatment in Rickettsial Fever Dr Deo Bhushan, Dr Jadhav Jayashree, DR Nigavekar P V, DR Himanshu Kumar Department of Pediatrics,
Case Report Disseminated Herpes Simplex Virus with Fulminant Hepatitis
 Case Reports in Hepatology Volume 2015, Article ID 463825, 4 pages http://dx.doi.org/10.1155/2015/463825 Case Report Disseminated Herpes Simplex Virus with Fulminant Hepatitis Bassam H. Rimawi, 1 Joseph
Case Reports in Hepatology Volume 2015, Article ID 463825, 4 pages http://dx.doi.org/10.1155/2015/463825 Case Report Disseminated Herpes Simplex Virus with Fulminant Hepatitis Bassam H. Rimawi, 1 Joseph
=ﻰﻤاﻤﺤﻠا ﺔﻴﻘﻠﺤﻠا ﺔذﺒاﻨﻠا
 1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
SCRUB TYPHUS PRESENTING AS ATYPICAL PNEUMONIA
 SCRUB TYPHUS PRESENTING AS ATYPICAL PNEUMONIA Sajan Christopher MD, Department of Medicine and K. Sreekanthan MD, Department of Infectious Diseases, Government Medical College, Thiruvananthapuram 695011,
SCRUB TYPHUS PRESENTING AS ATYPICAL PNEUMONIA Sajan Christopher MD, Department of Medicine and K. Sreekanthan MD, Department of Infectious Diseases, Government Medical College, Thiruvananthapuram 695011,
Necrotizing Granulomatous Hepatitis as an Unusual Manifestation of Lyme Disease
 Dig Dis Sci (2007) 52:2629 2632 DOI 10.1007/s10620-006-9405-9 Necrotizing Granulomatous Hepatitis as an Unusual Manifestation of Lyme Disease Antonela C. Zanchi Alan R. Gingold Neil D. Theise Albert D.
Dig Dis Sci (2007) 52:2629 2632 DOI 10.1007/s10620-006-9405-9 Necrotizing Granulomatous Hepatitis as an Unusual Manifestation of Lyme Disease Antonela C. Zanchi Alan R. Gingold Neil D. Theise Albert D.
Gastritis Associated with Epstein-Barr Virus Infection
 CASE REPORT Gastritis Associated with Epstein-Barr Virus Infection Akari Hisamatsu 1, Takayuki Nagai 1, Hitoshi Okawara 1, Hiroshi Nakashima 1, Takako Tasaki 1, Yoshifumi Nakagawa 1, Masahiko Hashinaga
CASE REPORT Gastritis Associated with Epstein-Barr Virus Infection Akari Hisamatsu 1, Takayuki Nagai 1, Hitoshi Okawara 1, Hiroshi Nakashima 1, Takako Tasaki 1, Yoshifumi Nakagawa 1, Masahiko Hashinaga
Lymphomatoid Papulosis 3 Case Reports
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. III (July. 2015), PP 31-35 www.iosrjournals.org Lymphomatoid Papulosis 3 Case Reports
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. III (July. 2015), PP 31-35 www.iosrjournals.org Lymphomatoid Papulosis 3 Case Reports
CASE REPORT ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX
 ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
MELKERSSON-ROSENTHAL SYNDROME AND CROHN S DISEASE
 British Journal of Oral Surgery (1980) 18, 254-258 @ The British Association of Oral Surgeons OOO7-117X/80/00370254$02.00 MELKERSSON-ROSENTHAL SYNDROME AND CROHN S DISEASE N. WORSAAE,~* K. C. CHRISTENSEN,2
British Journal of Oral Surgery (1980) 18, 254-258 @ The British Association of Oral Surgeons OOO7-117X/80/00370254$02.00 MELKERSSON-ROSENTHAL SYNDROME AND CROHN S DISEASE N. WORSAAE,~* K. C. CHRISTENSEN,2
Preliminary evaluation of the INDX R DIP-S-TICKS TM with positive rickettsial samples in Malaysia
 Malaysian J Path01 1993; ls(1): 69-73 Preliminary evaluation of the INDX R DIP-S-TICKS TM with positive rickettsial samples in Malaysia AS KOAY, AIMHLT and YM CHEONG, MBBS, MRCPath Division of Bacteriology,
Malaysian J Path01 1993; ls(1): 69-73 Preliminary evaluation of the INDX R DIP-S-TICKS TM with positive rickettsial samples in Malaysia AS KOAY, AIMHLT and YM CHEONG, MBBS, MRCPath Division of Bacteriology,
Clinicopathologic Self-Assessment
 Clinicopathologic Self-Assessment Handout Symposium (S003), July 27 th 2017 Maija Kiuru MD PhD Assistant Professor, Departments of Dermatology & Pathology University of California Davis CASE 1: History
Clinicopathologic Self-Assessment Handout Symposium (S003), July 27 th 2017 Maija Kiuru MD PhD Assistant Professor, Departments of Dermatology & Pathology University of California Davis CASE 1: History
UC Davis Dermatology Online Journal
 UC Davis Dermatology Online Journal Title Disseminated varicella-zoster virus in an immunocompetent adult Permalink https://escholarship.org/uc/item/3cz2x99b Journal Dermatology Online Journal, 21(3) Authors
UC Davis Dermatology Online Journal Title Disseminated varicella-zoster virus in an immunocompetent adult Permalink https://escholarship.org/uc/item/3cz2x99b Journal Dermatology Online Journal, 21(3) Authors
Viruses: Select Agents and Emerging Pathogens. Patricia Bolívar MS., CLS, PHM
 Viruses: Select Agents and Emerging Pathogens Patricia Bolívar MS., CLS, PHM Objectives Review Select Agent Viruses. Key features to recognize Smallpox virus Update on emerging Viruses of possible pandemic
Viruses: Select Agents and Emerging Pathogens Patricia Bolívar MS., CLS, PHM Objectives Review Select Agent Viruses. Key features to recognize Smallpox virus Update on emerging Viruses of possible pandemic
Department of Medical Microbiology, Faculty of Medicine, University of Malaya, Malaysia; 2
 SEROPREVALENCE OF RICKETSIAL ANTIBODIES AMONG URBAN MALAYSIANS ANTIBODY PREVALENCE OF ORIENTIA TSUTSUGAMUSHI, RICKETTSIA TYPHI AND TT118 SPOTTED FEVER GROUP RICKETTSIAE AMONG MALAYSIAN BLOOD DONORS AND
SEROPREVALENCE OF RICKETSIAL ANTIBODIES AMONG URBAN MALAYSIANS ANTIBODY PREVALENCE OF ORIENTIA TSUTSUGAMUSHI, RICKETTSIA TYPHI AND TT118 SPOTTED FEVER GROUP RICKETTSIAE AMONG MALAYSIAN BLOOD DONORS AND
Future of Pediatrics: Blisters, Hives and Other Tales from the Emergency Room June 14 th, 2016
 A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation. Dermatopathology Specialists Needed. Changing Trends
 Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Infectious Disease SHORT AND CRISP CRAMMER POINTS
 Infectious Disease SHORT AND CRISP CRAMMER POINTS 1 Reservoir of Important Infectious Disease Reservoir Human Rodents Non Living Disease Epidemic typhus, Dracunculiasis, Ancylostomiasis, Trench fever,
Infectious Disease SHORT AND CRISP CRAMMER POINTS 1 Reservoir of Important Infectious Disease Reservoir Human Rodents Non Living Disease Epidemic typhus, Dracunculiasis, Ancylostomiasis, Trench fever,
Fever and rash in children. Haider Arishi MD Consultant, pediatrics and infectious diseases Director, infection control program
 Fever and rash in children Haider Arishi MD Consultant, pediatrics and infectious diseases Director, infection control program objectives To understand importance of fever and rash. To discuss the clinical
Fever and rash in children Haider Arishi MD Consultant, pediatrics and infectious diseases Director, infection control program objectives To understand importance of fever and rash. To discuss the clinical
22 year old QH mare with regionally extensive alopecia and scaling on one front limb and ventral chest (Figure 1 and 2).
 22 year old QH mare with regionally extensive alopecia and scaling on one front limb and ventral chest (Figure 1 and 2). Which of the following is the most likely disease? a. Sterile granuloma complex
22 year old QH mare with regionally extensive alopecia and scaling on one front limb and ventral chest (Figure 1 and 2). Which of the following is the most likely disease? a. Sterile granuloma complex
Didactic Series. Primary HIV Infection. Greg Melcher, M.D. UC Davis AETC 8 Nov 2012
 Didactic Series Primary HIV Infection Greg Melcher, M.D. UC Davis AETC 8 Nov 2012 ACCREDITATION STATEMENT: University of California, San Diego School of Medicine is accredited by the Accreditation Council
Didactic Series Primary HIV Infection Greg Melcher, M.D. UC Davis AETC 8 Nov 2012 ACCREDITATION STATEMENT: University of California, San Diego School of Medicine is accredited by the Accreditation Council
A Rare case of Tubercular Gingivitis Case Report
 Case Report A Rare case of Tubercular Gingivitis Case Report *Dr. Ansh Chugh 1, Dr. Firoz A Hakkim 2, Dr. Rajesh. V 3, Dr. Raghava Sharma 4 1: JUNIOR RESIDENT IN GENERAL MEDICINE 2: SENIOR RESIDENT IN
Case Report A Rare case of Tubercular Gingivitis Case Report *Dr. Ansh Chugh 1, Dr. Firoz A Hakkim 2, Dr. Rajesh. V 3, Dr. Raghava Sharma 4 1: JUNIOR RESIDENT IN GENERAL MEDICINE 2: SENIOR RESIDENT IN
Lyme Disease, an Infectious Diseases Perspective
 Lyme Disease, an Infectious Diseases Perspective Lyme: Pretest 1. The pathognomonic finding of Lyme disease is: 1. An indurated lesion, measuring ~ 2 cm in diameter with a central, necrotic eschar. 2.
Lyme Disease, an Infectious Diseases Perspective Lyme: Pretest 1. The pathognomonic finding of Lyme disease is: 1. An indurated lesion, measuring ~ 2 cm in diameter with a central, necrotic eschar. 2.
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA)
 Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
Kikuchi s disease (necrotizing lymphadenitis) presenting as acneiform eruption
 Journal of the Saudi Society of Dermatology & Dermatologic Surgery (2012) 16, 67 71 King Saud University Journal of the Saudi Society of Dermatology & Dermatologic Surgery www.ksu.edu.sa www.jssdds.org
Journal of the Saudi Society of Dermatology & Dermatologic Surgery (2012) 16, 67 71 King Saud University Journal of the Saudi Society of Dermatology & Dermatologic Surgery www.ksu.edu.sa www.jssdds.org
Spectrum of clinical presentations
 Spectrum of clinical presentations Case History A 7-day-old male patient born full-term via uncomplicated vaginal delivery was seen for multiple erythematous red-brown purpuric lesions that were present
Spectrum of clinical presentations Case History A 7-day-old male patient born full-term via uncomplicated vaginal delivery was seen for multiple erythematous red-brown purpuric lesions that were present
Purpuric drug eruption without leukocytoclastic vasculitis associated with vancomycin
 Asian Pacific Journal of Allergy and Immunology CASE REPORT Purpuric drug eruption without leukocytoclastic vasculitis associated with vancomycin Tamaki Nakamura, 1 Hiroyuki Wakiguchi, 1 Fumiko Okazaki,
Asian Pacific Journal of Allergy and Immunology CASE REPORT Purpuric drug eruption without leukocytoclastic vasculitis associated with vancomycin Tamaki Nakamura, 1 Hiroyuki Wakiguchi, 1 Fumiko Okazaki,
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 34/ Apr 27, 2015 Page 5817
 A STUDY OF CLINICAL AND EPIDEMIOLOGICAL CHARACTERISTICS OF SCRUB TYPHUS IN TERTIARY CARE HOSPITAL IN ANDHRA PRADESH I. V. Ramachandra Rao 1, Kumbha Thulasiram 2, H. V. S. S. Laxman 3 HOW TO CITE THIS ARTICLE:
A STUDY OF CLINICAL AND EPIDEMIOLOGICAL CHARACTERISTICS OF SCRUB TYPHUS IN TERTIARY CARE HOSPITAL IN ANDHRA PRADESH I. V. Ramachandra Rao 1, Kumbha Thulasiram 2, H. V. S. S. Laxman 3 HOW TO CITE THIS ARTICLE:
African tick-bite fever (ATBF), a recently rediscovered. Histologic Features and Immunodetection of African Tick-bite Fever Eschar
 RESEARCH Histologic Features and Immunodetection of African Tick-bite Fever Eschar Hubert Lepidi,* Pierre-Edouard Fournier,* and Didier Raoult* African tick-bite fever (ATBF) is a rickettsiosis caused
RESEARCH Histologic Features and Immunodetection of African Tick-bite Fever Eschar Hubert Lepidi,* Pierre-Edouard Fournier,* and Didier Raoult* African tick-bite fever (ATBF) is a rickettsiosis caused
BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123
 BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123 M55. 4/7 tender lesions on knee, legs and arms. Also iritis/ weight loss/headache, synovitis.?vasculitis. Sarcoidosis. Biopsy from left elbow
BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123 M55. 4/7 tender lesions on knee, legs and arms. Also iritis/ weight loss/headache, synovitis.?vasculitis. Sarcoidosis. Biopsy from left elbow
International Journal of Pharma and Bio Sciences A STUDY OF CLINCAL PROFILE IN DENGUE CASES ABSTRACT
 Research Article Microbiology International Journal of Pharma and Bio Sciences ISSN 0975-6299 A STUDY OF CLINCAL PROFILE IN DENGUE CASES DHANDAPANI E.* 1 AND SUDHA M 2 1 Formerly Professor of Medicine,
Research Article Microbiology International Journal of Pharma and Bio Sciences ISSN 0975-6299 A STUDY OF CLINCAL PROFILE IN DENGUE CASES DHANDAPANI E.* 1 AND SUDHA M 2 1 Formerly Professor of Medicine,
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 2 2013 Article 14 A Case Presentation and Review of Lymphogranuloma Venerum Proctitis Mohammed Bayasi University of Texas Medical Branch, mbayasi@gmail.com
World Journal of Colorectal Surgery Volume 3, Issue 2 2013 Article 14 A Case Presentation and Review of Lymphogranuloma Venerum Proctitis Mohammed Bayasi University of Texas Medical Branch, mbayasi@gmail.com
Spotted Fever Group Rickettsiosis (Including Rocky Mountain Spotted Fever)
 Spotted Fever Group Rickettsiosis (Including Rocky Mountain Spotted Fever) DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail
Spotted Fever Group Rickettsiosis (Including Rocky Mountain Spotted Fever) DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail
Rameshwar Gutte and Uday Khopkar
 Extragenital unilateral lichen sclerosus et atrophicus in a child: a case report Rameshwar Gutte and Uday Khopkar Department of Dermatolgy, Seth GSMC and KEM Hospital, Parel, Mumbai-400012, India Egyptian
Extragenital unilateral lichen sclerosus et atrophicus in a child: a case report Rameshwar Gutte and Uday Khopkar Department of Dermatolgy, Seth GSMC and KEM Hospital, Parel, Mumbai-400012, India Egyptian
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Bacteria: Scarlet fever, Staph infection (sepsis, 4S,toxic shock syndrome), Meningococcemia, typhoid Mycoplasma Rickettsial infection
 Exanthematous Fever objectives FEVER WITH RASH 1 Determine the feature of skin rashes 2 Enumerate the most common causes of skin rashes in children (measles, chicken pox, rubella,erythema infectiosum,
Exanthematous Fever objectives FEVER WITH RASH 1 Determine the feature of skin rashes 2 Enumerate the most common causes of skin rashes in children (measles, chicken pox, rubella,erythema infectiosum,
Hot from the Tropics! Fever in the returned traveler workshop. UHN Conference 2015
 Hot from the Tropics! Fever in the returned traveler workshop UHN Conference 2015 Case 1: General approach to fever in the returning traveller Exercise 1: Location of travel and pathogens 1. Focus on what
Hot from the Tropics! Fever in the returned traveler workshop UHN Conference 2015 Case 1: General approach to fever in the returning traveller Exercise 1: Location of travel and pathogens 1. Focus on what
Rickettsial Diseases in Central India: Proposed Clinical Scoring System for Early Detection of Spotted Fever
 R E S E A R C H P A P E R Rickettsial Diseases in Central India: Proposed Clinical Scoring System for Early Detection of Spotted Fever NARENDRA B RATHI, *AKANKSHA N RATHI, # MICHAEL H GOODMAN, AND # ZUBAIR
R E S E A R C H P A P E R Rickettsial Diseases in Central India: Proposed Clinical Scoring System for Early Detection of Spotted Fever NARENDRA B RATHI, *AKANKSHA N RATHI, # MICHAEL H GOODMAN, AND # ZUBAIR
Hepatitis E Vaccine Clinical Experience. Mrigendra P. Shrestha
 Hepatitis E Vaccine Clinical Experience Mrigendra P. Shrestha 1 Hepatitis E in Nepal 2 Hepatitis E in Nepal Most common type of acute viral hepatitis Occurs in annual rainy season outbreaks Responsible
Hepatitis E Vaccine Clinical Experience Mrigendra P. Shrestha 1 Hepatitis E in Nepal 2 Hepatitis E in Nepal Most common type of acute viral hepatitis Occurs in annual rainy season outbreaks Responsible
Alberta Health and Wellness Public Health Disease Under Surveillance Management Guidelines March 2011
 March 2011 Histoplasmosis Case Definition Confirmed Case Clinical illness [1] with laboratory confirmation of infection: Isolation of Histoplasma capsulatum from an appropriate clinical specimen (tissue
March 2011 Histoplasmosis Case Definition Confirmed Case Clinical illness [1] with laboratory confirmation of infection: Isolation of Histoplasma capsulatum from an appropriate clinical specimen (tissue
Report of Four Volunteers with Primary, Secondary and Tertiary Dengue Infections during a Prospective Cohort Study
 Report of Four Volunteers with Primary, Secondary and Tertiary Dengue Infections during a Prospective Cohort Study Herman Kosasih a, Hadi Yusuf b, Primal Sudjana b, Bachti Alisjahbana b, Suharyono Wuryadi
Report of Four Volunteers with Primary, Secondary and Tertiary Dengue Infections during a Prospective Cohort Study Herman Kosasih a, Hadi Yusuf b, Primal Sudjana b, Bachti Alisjahbana b, Suharyono Wuryadi
Clinicopathologic Self- Assessment S003 AAD 2017
 Clinicopathologic Self- Assessment S003 AAD 2017 Clay J. Cockerell, M.D. Director, Cockerell Dermatopathology Director, Division of Dermatopathology UT Southwestern Medical Center July 2017 No relevant
Clinicopathologic Self- Assessment S003 AAD 2017 Clay J. Cockerell, M.D. Director, Cockerell Dermatopathology Director, Division of Dermatopathology UT Southwestern Medical Center July 2017 No relevant
MEASLES (campak, rubeola, gabak, kerumut) Infectious and Tropical Pediatric Division Department of Child Health, Medical Faculty, University of Sumate
 MEASLES (campak, rubeola, gabak, kerumut) Infectious and Tropical Pediatric Division Department of Child Health, Medical Faculty, University of Sumatera Utara 1 Maculapapular eruption : 1. Measles 2. Atypical
MEASLES (campak, rubeola, gabak, kerumut) Infectious and Tropical Pediatric Division Department of Child Health, Medical Faculty, University of Sumatera Utara 1 Maculapapular eruption : 1. Measles 2. Atypical
ORIGINAL ARTICLE. SEROPREVALENCE OF DENGUE IN TERTIARY CARE CENTRE AT LUCKNOW Shipra Singhal 1, Krati R. Varshney 2, Vineeta Mittal 3, Y. I. Singh 4.
 SEROPREVALENCE OF DENGUE IN TERTIARY CARE CENTRE AT LUCKNOW Shipra Singhal 1, Krati R. Varshney 2, Vineeta Mittal 3, Y. I. Singh 4. 1. Junior Resident, Department of Microbiology, Era s Lucknow Medical
SEROPREVALENCE OF DENGUE IN TERTIARY CARE CENTRE AT LUCKNOW Shipra Singhal 1, Krati R. Varshney 2, Vineeta Mittal 3, Y. I. Singh 4. 1. Junior Resident, Department of Microbiology, Era s Lucknow Medical
Anthrax: An Epidemiologic Perspective. Denise Dietz Public Health Epidemiologist
 Anthrax: An Epidemiologic Perspective Denise Dietz Public Health Epidemiologist Outline Overview of anthrax Explain different types of anthrax Clinical Why a good weapon Epidemiology Bacillus anthracis
Anthrax: An Epidemiologic Perspective Denise Dietz Public Health Epidemiologist Outline Overview of anthrax Explain different types of anthrax Clinical Why a good weapon Epidemiology Bacillus anthracis
THERE IS A GROUP OF PAtients. Defining Urticarial Dermatitis. A Subset of Dermal Hypersensitivity Reaction Pattern
 STUDY Defining Urticarial Dermatitis A Subset of Dermal Hypersensitivity Reaction Pattern Steven Kossard, FACD; Ian Hamann, FACD; Barbara Wilkinson, BSc Background: Urticarial dermatitis may represent
STUDY Defining Urticarial Dermatitis A Subset of Dermal Hypersensitivity Reaction Pattern Steven Kossard, FACD; Ian Hamann, FACD; Barbara Wilkinson, BSc Background: Urticarial dermatitis may represent
STATEMENT FOR MANAGING LYME DISEASE IN NOVA SCOTIA
 INFECTIOUS DISEASES EXPERT GROUP (IDEG) DEPARTMENT OF HEALTH AND WELLNESS STATEMENT FOR MANAGING LYME DISEASE IN NOVA SCOTIA Executive Summary: In 2016, the Public Health Agency of Canada (PHAC) modified
INFECTIOUS DISEASES EXPERT GROUP (IDEG) DEPARTMENT OF HEALTH AND WELLNESS STATEMENT FOR MANAGING LYME DISEASE IN NOVA SCOTIA Executive Summary: In 2016, the Public Health Agency of Canada (PHAC) modified
Seroprevalence of Babesia microti in Individuals with Lyme Disease. Sabino R. Curcio, M.S, MLS(ASCP)
 Seroprevalence of Babesia microti in Individuals with Lyme Disease Sabino R. Curcio, M.S, MLS(ASCP) Lyme Disease Most common vectorborne illness in the United States Caused by the tick-transmitted spirochete
Seroprevalence of Babesia microti in Individuals with Lyme Disease Sabino R. Curcio, M.S, MLS(ASCP) Lyme Disease Most common vectorborne illness in the United States Caused by the tick-transmitted spirochete
manifestations are uncommon. Initial descriptions of the disease (Rosai and Dorfman, 1969) specifically
 Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
SWISS SOCIETY OF NEONATOLOGY. A newborn with a papulonodular rash at birth
 SWISS SOCIETY OF NEONATOLOGY A newborn with a papulonodular rash at birth June 2001 2 Glanzmann R, Neonatal Intensive Care Unit, UKKB Basel, Switzerland Swiss Society of Neonatology, Thomas M Berger, Webmaster
SWISS SOCIETY OF NEONATOLOGY A newborn with a papulonodular rash at birth June 2001 2 Glanzmann R, Neonatal Intensive Care Unit, UKKB Basel, Switzerland Swiss Society of Neonatology, Thomas M Berger, Webmaster
Smallpox Recognition and Vaccination
 Smallpox Recognition and Vaccination Daniel R. Lucey, MD, MPH Georgetown University Medical and Law Centers Senior Scholar, O Neill Law Institute for Global Health Hong Kong Centre for Health Protection
Smallpox Recognition and Vaccination Daniel R. Lucey, MD, MPH Georgetown University Medical and Law Centers Senior Scholar, O Neill Law Institute for Global Health Hong Kong Centre for Health Protection
Challenging Cases in Dermatopathology. Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania
 Challenging Cases in Dermatopathology Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Rosalie Elenitsas
Challenging Cases in Dermatopathology Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Rosalie Elenitsas
Melanoma Update: 8th Edition of AJCC Staging System
 Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Below you will find information about diseases, the risk of contagion, and preventive vaccinations.
 Vaccinations Below you will find information about diseases, the risk of contagion, and preventive vaccinations. DTP - Diphtheria Tetanus Polio Yellow fever Hepatitis A Typhoid fever Cerebrospinal meningitis
Vaccinations Below you will find information about diseases, the risk of contagion, and preventive vaccinations. DTP - Diphtheria Tetanus Polio Yellow fever Hepatitis A Typhoid fever Cerebrospinal meningitis
العصوي الوعاي ي الورام = angiomatosis Bacillary
 1 / 7 BACILLARY ANGIOMATOSIS Epidemiology BA is most commonly seen in patients with acquired immunodeficiency syndrome (AIDS) and a CD4 count less than 50 cells/mm 3, with an incidence of 1.2 cases per
1 / 7 BACILLARY ANGIOMATOSIS Epidemiology BA is most commonly seen in patients with acquired immunodeficiency syndrome (AIDS) and a CD4 count less than 50 cells/mm 3, with an incidence of 1.2 cases per
Name the condition: Canine sterile neutrophilic dermatosis (Sweet s syndrome)
 5-year-old male miniature Schnauzer dog with acute onset of severe macular erythema and multiple tender violaceus plaques all over the body. Which of the following is the most likely diagnosis? 1. Canine
5-year-old male miniature Schnauzer dog with acute onset of severe macular erythema and multiple tender violaceus plaques all over the body. Which of the following is the most likely diagnosis? 1. Canine
West Nile Virus in the Region of Peel 2002
 HUMAN CASE SURVEILLANCE Introduction Human illness caused by mosquito-borne WNV acquired in Peel occurred for the first time in 2002. In 1999, a Peel resident who had traveled to New York City acquired
HUMAN CASE SURVEILLANCE Introduction Human illness caused by mosquito-borne WNV acquired in Peel occurred for the first time in 2002. In 1999, a Peel resident who had traveled to New York City acquired
Lyme disease Overview
 Infectious Disease Epidemiology BMTRY 713 (A. Selassie, DrPH) Lecture 21 Lyme Disease Learning Objectives 1. Describe the agent and vector of Lyme Disease 2. Identify the geographic and temporal patterns
Infectious Disease Epidemiology BMTRY 713 (A. Selassie, DrPH) Lecture 21 Lyme Disease Learning Objectives 1. Describe the agent and vector of Lyme Disease 2. Identify the geographic and temporal patterns
Tick-borne Disease Surveillance
 Tick-borne Disease Surveillance Catherine M. Brown, DVM, MSc, MPH Deputy State Epidemiologist and State Public Health Veterinarian Department of Public Health Bureau of Infectious Disease William A. Hinton
Tick-borne Disease Surveillance Catherine M. Brown, DVM, MSc, MPH Deputy State Epidemiologist and State Public Health Veterinarian Department of Public Health Bureau of Infectious Disease William A. Hinton
