Risk Factors for Infection Following Total Joint Arthroplasty in Rheumatoid Arthritis
|
|
|
- Milo Black
- 5 years ago
- Views:
Transcription
1 Send Orders for Reprints to The Open Rheumatology Journal, 2013, 7, Open Access Risk Factors for Infection Following Total Joint Arthroplasty in Rheumatoid Arthritis Ranjani Somayaji 1, Cheryl Barnabe *,1,2 and Liam Martin 1 1 Department of Medicine, 2 Department of Community Health Sciences, University of Calgary, Calgary, Alberta, Canada Abstract: Objective: Determine risk factors for infection following hip or knee total joint arthroplasty in patients with rheumatoid arthritis. Methods: All rheumatoid arthritis patients with a hip or knee arthroplasty between years 2000 and 2010 were identified from population-based administrative data from the Calgary Zone of Alberta Health Services. Clinical data from patient charts during the hospital admission and during a one year follow-up period were extracted to identify incident infections. Results: We identified 381 eligible procedures performed in 259 patients (72.2% female, mean age 63.3 years, mean body mass index 27.6 kg/m 2 ). Patient comorbidities were hypertension (43.2%), diabetes (10.4%), coronary artery disease (13.9%), smoking (10.8%) and obesity (32%). Few infectious complications occurred: surgical site infections occurred within the first year after 5 procedures (2 joint space infections, 3 deep incisional infections). Infections of non-surgical sites (urinary tract, skin or respiratory, n=4) complicated the hospital admission. The odds ratio for any post-arthroplasty infection was increased in patients using prednisone doses exceeding 15 mg/day (OR 21.0, 95%CI , p=<0.001), underweight patients (OR 6.0, 95%CI , p=0.033) and those with known coronary artery disease (OR 5.1, 95%CI , p=0.017). Types of disease-modifying therapy, age, sex, and other comorbidities were not associated with an increased risk for infection. Conclusions: Steroid doses over 15 mg/day, being underweight and having coronary artery disease were associated with significant increases in the risk of post-arthroplasty infection in rheumatoid arthritis. Maximal tapering of prednisone and comorbidity risk reduction must be addressed in the peri-operative management strategy. Keywords: Rheumatoid arthritis, infections, arthroplasty, administrative data. 1. INTRODUCTION Despite a reduction in the need for total joint arthroplasty (TJA) in the management of end-stage damage of the hip and knee in rheumatoid arthritis (RA) [1-5], many patients still require procedures to restore function and quality of life. It has been suggested that RA patients are at increased risk for post-operative complications such as infection [6], attributed to traditional patient risk factors such as age, smoking status, and obesity, in addition to the risk of immunosuppressive therapies. Post-operative infections cause morbidity, and in the case of prosthetic joint infections the potential need for future revision procedures. Modifiable risk factors should be identified in order to optimize surgical outcomes. A recent systematic review highlights that knowledge of TJA infection risk in RA is actually quite limited [6]. As well, the literature focuses on surgical site and prosthetic joint infections, and neglects the risk for infections of other sites which may complicate the hospital course. The purpose of our study was to determine both the patient and therapeutic risk factors for both surgical site infections in the first year *Address correspondence to this author at the 3330 Hospital Dr. NW, Calgary, AB CANADA T2N 4N1, Canada; Tel: (403) ; Fax: (403) ; ccbarnab@ucalgary.ca post-procedure, and other organ infections occurring during the surgical admission in a population-based RA cohort. 2. METHODS 2.1. Patients Subjects were identified from population-based administrative datasets from the Calgary Zone of Alberta Health Services, Canada from the fiscal years 2000/2001 to the end of fiscal year 2010/2011. These datasets reflect records generated by both trained hospital separation coders and submitted physician billing claims, yielding high accuracy in case identification. This Zone has three tertiary care hospitals where TJA is performed and serves a catchment area of 1.5 million individuals in the province of southern Alberta. We first identified subjects with procedure codes for primary and revision hip or knee TJA (VA.53.LAPN, VG.53.LAPN, VG.53.LAPP) to the end of December 2010 (which allowed for a one year follow-up period for post-operative infection). We then selected the cohort who also had a diagnostic code for RA in any of the years of the study (International Classification of Diseases, 9 th Revision, Clinical Modification (ICD-9-CM) 714.x for fiscal years , or 10th Revision, Canadian Adaptation (ICD-10-CA) M05.x or M06.x for fiscal years ). All diagnoses and procedures were verified at the data extraction stage / Bentham Open
2 120 The Open Rheumatology Journal, 2013, Volume 7 Somayaji et al Data Extraction Age and sex, comorbidities as diagnosed by physicians (including diabetes, hypertension, coronary artery disease), and smoking status were recorded from the pre-operative assessment. The height and weight at the time of surgery were extracted from the chart. Medications, including nonbiologic disease-modifying anti-rheumatic drugs (DMARDs, including methotrexate, sulfasalazine, leflunomide, hydroxychloroquine), and biologic agents (infliximab, adalimumab, etanercept, golimumab, rituximab, abatacept and anakinra) as well as corticosteroid use and dose were noted. For patients receiving a biologic agent, the timing of last dose prior to surgery was recorded. Surgical procedures were recorded as primary hip or knee arthroplasty and revision arthroplasty based on procedure coding and chart review. These procedures included both elective and emergent procedures (i.e. hip arthroplasty following a hip fracture). The duration of disease, level of disease activity and functional level scores are not recorded in the hospital chart and it is not possible to include these data in our analyses Outcomes Surgical site infections (SSI) were characterized in accordance with the Centres for Disease Control criteria [7]. This classification recognizes superficial incisional, deep incisional, and space infections of the joint. We used chart documentation of symptoms and signs of infection to determine the location and severity of infection, antibiotic treatment, or need for re-hospitalization and repeat surgery. This was supported by confirmation of diagnostic imaging results, microbiology testing and outpatient home parenteral therapy program notes. We also extracted details on infections of other sites during the index surgical admission. These data were reviewed by two internal medicine physicians (RS and CB) Independent Variables These were selected based on the existing literature for patient risk factors for infections after TJA. Factors examined included patient sex, age, obesity (body mass index > 30 kg/m 2 ), smoking status (current, past, never), and the three most common comorbid conditions in the cohort (hypertension, diabetes, and coronary artery disease). Therapeutic classes for RA treatment were also examined, including prednisone, non-biologic DMARDs (any) and biologics (any) Statistical Analysis Univariate logistic regression models were constructed to calculate the odds ratio (OR) for any post-arthroplasty infection based on the independent variables above. Our priori research plan indicated that a multivariate model would be constructed however the small number of infectious events limited our ability to do this. All analysis was performed using STATA version 11.2 (College Station, Texas) Ethics Ethics approval was granted by the Conjoint Health Research Ethics Board of the University of Calgary. 3. RESULTS 3.1. Procedures From the administrative data, we identified 420 hip or knee replacement surgeries in RA patients performed over 10 years. Of these, 35 were excluded from further analysis as the diagnosis of RA was not confirmed on chart review, and 4 charts could not be retrieved. The remaining 381 procedures were performed in 259 individuals. The procedures consisted of 137 total hip arthroplasties and 244 total knee arthroplasties. Of these, 345 procedures were done electively, 29 procedures were a revision surgery, and 7 arthroplasties were performed secondary to a fracture Patients The patients demographic data are reported in Table 1. In summary, 72.2% were female, with a mean age of 63.3 years. The mean body mass index was 27.6 kg/m 2, and 32.0% classified as obese. Nearly half of the patients had hypertension (43.2%), followed in frequency by coronary artery disease (13.9%), and diabetes (10.4%). There were 28 (10.8%) current smokers in the cohort. Nine patients had a history of a prior prosthetic joint infection of another joint, with 1 having 2 prior prosthetic joint infections. Table 1. Clinical Characteristics of Study Patients Characteristic Number (%) Female 187 (72.2%) Age, years Smoking Body Mass Index Comorbidity Current Past Never Mean Obese (>30.0) Hypertension Diabetes Coronary artery disease Chronic Obstructive Lung Disease Chronic Renal Failure No comorbid conditions 2 Comorbid conditions mean 63.3 (SD 14.1) 28 (10.8%) 40 (15.4%) 191 (73.8%) 27.6 (7.0) 83 (32.0%) 112 (43.2%) 27 (10.4%) 36 (13.9%) 11 (4.3%) 8 (3.1%) 114 (44.0%) 38 (14.7%) At the time of surgery, 67.5% of patients were being treated with either biologics or non-biologic DMARDs (n = 257/381 procedures) (Table 2). RA treatment varied over the course of the study, with biologic and non-biologic DMARD
3 Risk Factors for Infection Following Total Joint Arthroplasty The Open Rheumatology Journal, 2013, Volume therapy increasing over time (Fig. 1). For 14 of the patients (20.0%) on biologic therapy, this therapy was not held in the pre-operative period. With regards to steroid use, 27.4% of patients were taking between 1 and 15 mg/day of prednisone at the time of surgery, and 1.9% were taking >15 mg/day (Table 2). Nearly all patients (96.8%) received antimicrobial prophylaxis prior to surgery. Fig. (1). Therapy Used by Arthroplasty Patients, by Year of Surgical Procedure. Table 2. Therapy at Time of Surgery Therapeutic Class Number (%) Prednisone DMARDs, Total Exposed Biologics, Total Exposed None mg/day >15 mg/day Methotrexate Hydroxychloroquine Sulfasalazine Leflunomide Combination DMARDs Infliximab Adalimumab Etanercept Golimumab Anakinra 3.3. Surgical Site Infections Abatacept Rituximab 268 (70.7%) 104 (27.4%) 7 (1.9%) 235 (61.2%) 145 (38.1%) 117 (30.7%) 20 (5.3%) 34 (8.9%) 84 (22.1%) 70 (18.4%) 14 (3.7%) 15 (3.9%) 36 (9.5%) 1 (0.3%) 2 (0.5%) 1 (0.3%) 1 (0.3%) Surgical site infections (SSI) were infrequent, only occurring after 5 procedures during the 1 year follow-up period. These included 2 joint space infections, and 3 deep incisional infections. Details of the surgery and infection are found in Table 3. All of these required repeated surgical intervention and prolonged antibiotic courses for resolution Post-Operative Infections Four hospital admissions were complicated by infections of non-surgical sites (urinary tract, skin or respiratory). Specific details on the infection appear in Table Risk Factors for Infection Following Arthroplasty Univariate analysis was used to explore the association between post-arthroplasty infections (pooled) and patient risk factors (Table 4). The odds ratio of any post-arthroplasty infection was increased in patients using prednisone doses exceeding 15 mg/day (odds ratio 21.0, 95%CI , p=<0.001), but not for patients exposed to <15 mg/day. Coronary artery disease was also associated with an increased risk for infection (odds ratio 5.1, 95%CI , p=0.017). Although we were expecting an increased risk of infection in obese patients, it was actually underweight patients (BMI <18.5 kg/m 2 ) who had a significant risk (odds ratio 6.0, 95%CI , p=0.033). DMARDs and biologic therapies, not being on RA treatment, and age, sex, smoking status and other comorbidities of hypertension and diabetes were not associated with an increased risk for infection. 4. DISCUSSION Our retrospective population-based study of 10 years of outcomes of arthroplasty surgery in a Canadian centre shows very few surgical site infections occurring in RA patients. Infections during the hospital course were also rare. In the few cases of infection, a strong association with corticosteroid exposure was apparent, particularly with doses >15 mg/day being associated with a 20-fold increased risk. Other significant risk factors for post-arthroplasty infection were being underweight and a patient history of coronary artery disease. The risk for serious infections in RA is driven by age, disease severity, systemic inflammation and comorbid disease [8]. RA patients are known to be at heightened risk for infection following orthopedic procedures [9-15], plausibly related to the influence of disease factors on surgical healing. To our knowledge, the risk of infection associated with coronary artery disease and low body mass has not been described specifically in orthopedic procedures. Interestingly, a recent study looking at readmissions following arthroplasty found that these factors were associated with an increased risk of readmission, although not necessarily for infections [16]. We believe coronary artery disease and low body mass likely reflect high disease burden in patients with RA, and those with the most severe alterations in immunity. Thus, efforts to effectively manage RA will likely decrease both the need for TJA and surgical risk over time. Modifying and managing RA therapy in the perioperative period is critical in reducing the risk of infection. Chronic corticosteroid exposure is again confirmed in our study to significantly increase the risk for infection,
4 122 The Open Rheumatology Journal, 2013, Volume 7 Somayaji et al. Table 3. Descriptions of Post-Arthroplasty Infections Surgery: Joint and Type Post-Operative Infection: Type and Organism Patient Risk Profile Management Joint Space Infection, Coagulase negative Staph Chronic viral hepatitis Drained seroma, antibiotics; eventual resection with spacer and further revision required Knee arthroplasty, revision Joint Space Infection, S. aureus Prednisone 15 mg/day, coronary artery disease Surgical debridement, antibiotics, revision surgery Deep incisional, S. aureus and Enterococcus Prednisone 10 mg/day, obesity, diabetes, coronary artery disease, hypertension Surgical debridement, prolonged antibiotics Deep incisional, no organism cultured None Wound debridement, removal of hematoma, antibiotics Hip arthroplasty, revision for fracture Deep incisional, Enterococcus faecalis Prednisone 17.5 mg daily, hypertension, diabetes, coronary artery disease, osteomyelitis foot Incision and drainage, prolonged antibiotics Hip arthroplasty, primary Urinary tract Leflunomide and adalimumab, hypertension Antibiotics Hip arthroplasty, primary Urinary tract Prednisone 10 mg/day, age >65 Antibiotics Knee arthroplasty, revision Cellulitis of posterior shin Age >65, coronary artery disease Antibiotics Pneumonia Prednisone 5 mg/day, Leflunomide, age >65 Antibiotics Table 4. Univariate Analysis, Risk Factors for Post-Operative Infection Odds Ratio (95%CI) p Value Age >65 years 2.19 ( ) Female 2.06 ( ) Obesity (BMI >30 kg/m 2 ) 0.24 ( ) Underweight (BMI <18.5 kg/m 2 ) 5.97 ( ) Current Smoker no events - Per Comorbid Condition 1.17 ( ) Hypertension 0.71 ( ) Diabetes 2.36 ( ) Coronary Artery Disease 5.14 ( ) Prednisone Exposure (Any) 3.06 ( ) Prednisone >15 mg/day ( ) DMARD therapy 0.77 ( ) Biologic therapy 0.55 ( ) Not on DMARD or biologic therapy 1.68 ( ) Legend: DMARD disease-modifying anti-rheumatic drug. consistent with the study by Gilson et al, where joint space infections following TJA in patients on anti-tnf therapy were analyzed, with an odds ratio for infection increasing 5 fold for every 5mg/day increase in prednisone dose [17]. The risk for infection conferred by steroids have been further confirmed in studies by Kawakami et al. [18] and Salliot et al. [19]. Corticosteroids impair phagocyte function and suppress cell-mediated immunity [20]. Given the consistency and strength of the association between corticosteroids and infection, this should be the primary target in patient management. In contrast, non-biologic DMARDs to not confer an increased risk of infection, either in our study or many others [17-19, 21-24]. The long half-life of these agents precludes effective discontinuation and resumption without risking flare and worsening of disease control. We do not recommend discontinuation of non-biologic DMARDs
5 Risk Factors for Infection Following Total Joint Arthroplasty The Open Rheumatology Journal, 2013, Volume unless delayed wound healing or infection is experienced in the post-surgical period. The risk of infections conferred by the use of biologic therapies in patients undergoing orthopedic surgery is as yet unresolved in the literature. It is known that tumor necrosis factor-alpha (TNF-alpha), the first widely used target of biologic therapy, plays a critical role in the regulation of inflammatory processes to mount a response to infection [25]. TNF-alpha also plays an important role in wound healing with effects on angiogenesis, fibroblast proliferation, and collagen synthesis [26]. Our study did not show an increased risk of infection post-operatively with biologic use which adds to the body of conflicting literature in this area. Two prospective cohort studies have showed increased infection risk with use of biologics in RA patients undergoing surgeries in contrast to previous case-control and retrospective studies. Giles et al. determined a serious (deep) orthopedic infection rate of 11% and a 4-fold increased risk in patients receiving TNF-alpha inhibitors [22], and Momohara et al. reported a 6.4% superficial or deep postoperative infection rate with a 9-fold increased risk despite discontinuation of therapy pre-operatively [21]. Given the conflicting evidence, there are no standardized guidelines for the management of biologic therapies in the management of patients in the peri-operative period. The American College of Rheumatology suggests that anti-tnf be held for at least 1 week prior to and following surgery [27]. In contrast, the Canadian guidelines are more variable ranging from 1 week 2 months depending on the biologic, nature of the surgery and patient characteristics [28]. In our centre, nurse specialists work alongside physicians in the Biologics Pharmacosurveillance program, with advice on peri-operative management tailored to the patient s current therapy and comorbidities. We acknowledge limitations of our study. We used administrative data to identify all surgical events occurring in our health Zone, with hospital chart review to confirm significant post-operative infectious events in the first year following surgery. It is likely that patients sought care for minor infectious complications outside of the hospital and this would reduce identification of superficial infection. It is expected though that all serious complications and certainly those requiring re-admission to hospital or repeat surgeries would be captured unless the patient migrated to a new health Zone or out of province. Relatively few infection events occurred, and thus the power to detect significant risk factors is reduced. This limitation exists in the majority of the literature surrounding peri-operative infection in RA patients. Additionally, multiple surgeries in individual patients were considered as independent events although one event may affect the next regardless of timing and thus make the statistical assumptions false. However, all of the outcomes occurred in different patients and not in patients with previous prosthetic infections, and thus did not likely alter our results. Finally, disease activity level and function are not captured in the hospital chart, and therefore we cannot comment on the role that these factors played in post-operative infection risk. In summary, we found that the use of corticosteroids increased the risk of post-operative infection in RA patients undergoing large joint arthroplasty especially at doses >15mg/day. Coronary artery disease and being underweight were also associated with post-operative and surgical site infections. DMARDs and biologic therapies did not confer an increased risk of infection in the post-operative period, and the role of comorbidities will need to be studied further to determine their influence of post-operative infection risk. The optimal management of the RA patient in the perioperative period should focus primarily on reduction in corticosteroid use and adherence to recommendations on cessation of biologic therapy. CONFLICT OF INTEREST The authors confirm that this article content has no conflict of interest. ACKNOWLEDGEMENTS Declared none. REFERENCES [1] Massardo L, Gabriel SE, Crowson CS, et al. A population based assessment of the use of orthopedic surgery in patients with rheumatoid arthritis. J Rheumatol 2002; 29(1): 52-6 [2] da Silva E, Doran MF, Crowson CS, et al. Declining use of orthopedic surgery in patients with rheumatoid arthritis? Results of a long-term, population-based assessment. Arthritis Rheum 2003; 49 (2): [3] Louie GH, Ward MM. Changes in the rates of joint surgery among patients with rheumatoid arthritis in California, Ann Rheum Dis 2010; 69(5): [4] Hekmat K, Jacobsson L, Nilsson JA, et al. Decrease in the incidence of total hip arthroplasties in patients with rheumatoid arthritis--results from a well defined population in south Sweden. Arthritis Res Ther 2011; 13(2): R67. [5] Shourt CA, Crowson CS, Gabriel SE, et al. Orthopedic surgery among patients with rheumatoid arthritis : a populationbased study focused on surgery rates, sex, and mortality. J Rheumatol 2012; 39(3): [6] Ravi B, Escott B, Shah PS, et al. A systematic review and metaanalysis comparing complications following total joint arthroplasty for rheumatoid arthritis versus for osteoarthritis. Arthritis Rheum 2012; 64(12): [7] Horan TC, Gaynes RP, Martone WJ, et al. CDC definitions of nosocomial surgical site infections, 1992: a modification of CDC definitions of surgical wound infections. Infect Control Hosp Epidemiol 1992; 13(10): [8] Crowson CS, Hoganson DD, Fitz-Gibbon PD, et al. Development and validation of a risk score for serious infection in patients with rheumatoid arthritis. Arthritis Rheum 2012; 64(9): [9] Bongartz T, Halligan CS, Osmon DR, et al. Incidence and risk factors of prosthetic joint infection after total hip or knee replacement in patients with rheumatoid arthritis. Arthritis Rheum 2008; 59(12): [10] Bengtson S, Knutson K. The infected knee arthroplasty. A 6-year follow-up of 357 cases. Acta Orthop Scand 1991; 62(4): [11] Robertsson O, Knutson K, Lewold S, et al. The Swedish Knee Arthroplasty Register : an update with special emphasis on 41,223 knees operated on in Acta Orthop Scand 2001; 72(5): [12] Wilson MG, Kelley K, Thornhill TS. Infection as a complication of total knee-replacement arthroplasty. Risk factors and treatment in sixty-seven cases. J Bone Joint Surg Am 1990; 72(6): [13] Wymenga AB, van Horn JR, Theeuwes A, et al. Perioperative factors associated with septic arthritis after arthroplasty. Prospective multicenter study of 362 knee and 2,651 hip operations. Acta Orthop Scand 1992; 63(6): [14] Berbari EF, Hanssen AD, Duffy MC, et al. Risk factors for prosthetic joint infection: case-control study. Clin Infect Dis 1998; 27(5):
6 124 The Open Rheumatology Journal, 2013, Volume 7 Somayaji et al. [15] Jamsen E, Huhtala H, Puolakka T, et al. Risk factors for infection after knee arthroplasty. A register-based analysis of 43,149 cases. J Bone Joint Surg Am 2009; 91(1): [16] Saucedo JM, Marecek GS, Wanke TR, et al. Understanding Readmission After Primary Total Hip and Knee Arthroplasty: Who's at Risk? J Arthroplasty 2013 [Epub ahead of print]. [17] Gilson M, Gossec L, Mariette X, et al. Risk factors for total joint arthroplasty infection in patients receiving tumor necrosis factor alpha-blockers: a case-control study. Arthritis Res Ther 2010; 12(4): R145. [18] Kawakami K, Ikari K, Kawamura K, et al. Complications and features after joint surgery in rheumatoid arthritis patients treated with tumour necrosis factor-alpha blockers: perioperative interruption of tumour necrosis factor-alpha blockers decreases complications? Rheumatology (Oxford) 2010; 49(2): [19] Salliot C, Gossec L, Ruyssen-Witrand A, et al. Infections during tumour necrosis factor-alpha blocker therapy for rheumatic diseases in daily practice: a systematic retrospective study of 709 patients. Rheumatology (Oxford) 2007; 46(2): [20] Cutolo M, Seriolo B, Pizzorni C, et al. Use of glucocorticoids and risk of infections. Autoimmun Rev 2008; 8(2): [21] Momohara S, Kawakami K, Iwamoto T, et al. Prosthetic joint infection after total hip or knee arthroplasty in rheumatoid arthritis patients treated with nonbiologic and biologic disease-modifying antirheumatic drugs. Mod Rheumatol 2011; 21(5): [22] Giles JT, Bartlett SJ, Gelber AC, et al. Tumor necrosis factor inhibitor therapy and risk of serious postoperative orthopedic infection in rheumatoid arthritis. Arthritis Rheum 2006; 55(2): [23] Ruyssen-Witrand A, Gossec L, Salliot C, et al. Complication rates of 127 surgical procedures performed in rheumatic patients receiving tumor necrosis factor alpha blockers. Clin Exp Rheumatol 2007; 25(3): [24] den Broeder AA, Creemers MC, Fransen J, et al. Risk factors for surgical site infections and other complications in elective surgery in patients with rheumatoid arthritis with special attention for antitumor necrosis factor: a large retrospective study. J Rheumatol 2007; 34(4): [25] Ellerin T, Rubin RH, Weinblatt ME. Infections and anti-tumor necrosis factor alpha therapy. Arthritis Rheum 2003; 48(11): [26] Busti AJ, Hooper JS, Amaya CJ, et al. Effects of perioperative antiinflammatory and immunomodulating therapy on surgical wound healing. Pharmacotherapy 2005; 25(11): [27] Saag KG, Teng GG, Patkar NM, et al. American College of Rheumatology 2008 recommendations for the use of nonbiologic and biologic disease-modifying antirheumatic drugs in rheumatoid arthritis. Arthritis Rheum 2008; 59(6): [28] Bombardier C, Hazlewood GS, Akhavan P, et al. Canadian Rheumatology Association recommendations for the pharmacological management of rheumatoid arthritis with traditional and biologic disease-modifying antirheumatic drugs: part II safety. J Rheumatol 2012; 39(8): Received: September 18, 2013 Revised: November 30, 2013 Accepted: December 7, 2013 Somayaji et al.; Licensee Bentham Open. This is an open access article licensed under the terms of the Creative Commons Attribution Non-Commercial License ( 3.0/) which permits unrestricted, non-commercial use, distribution and reproduction in any medium, provided the work is properly cited.
Perioperative Medicine:
 Perioperative Medicine: Management of rheumatologic agents Divya Gollapudi, MD May 2016 Medical Operative Consult Clinic Harborview Medical Center Your patient Ms. L is a 55 year-old F w/ h/o RA who presents
Perioperative Medicine: Management of rheumatologic agents Divya Gollapudi, MD May 2016 Medical Operative Consult Clinic Harborview Medical Center Your patient Ms. L is a 55 year-old F w/ h/o RA who presents
2017 PERIOPERATIVE MEDICINE SYMPOSIUM Peri-operative use of immunosuppression in rheumatology patients
 2017 PERIOPERATIVE MEDICINE SYMPOSIUM Peri-operative use of immunosuppression in rheumatology patients Dr Alberta Hoi Rheumatologist MBBS, FRACP, PhD NEW ERA IN MUSCULOSKELETAL MEDICINE New drugs - Biologics,
2017 PERIOPERATIVE MEDICINE SYMPOSIUM Peri-operative use of immunosuppression in rheumatology patients Dr Alberta Hoi Rheumatologist MBBS, FRACP, PhD NEW ERA IN MUSCULOSKELETAL MEDICINE New drugs - Biologics,
Periprosthetic joint infection (PJI) is one of the most
 Bulletin of the Hospital for Joint Diseases 2014;72(4):253-8 253 Periprosthetic Joint Infection in Patients Receiving TNFα Antagonists Nimrod Snir, M.D., Ran Schwarzkopf, M.D., M.Sc., Michael Sobieraj,
Bulletin of the Hospital for Joint Diseases 2014;72(4):253-8 253 Periprosthetic Joint Infection in Patients Receiving TNFα Antagonists Nimrod Snir, M.D., Ran Schwarzkopf, M.D., M.Sc., Michael Sobieraj,
By: For: Division responsible for document: Key words: Name and job title of document author: Name and job title of document author s Line Manager:
 For Use in: By: For: Guidelines for the Management of Interruption of Biologic Therapies for Division responsible for document: Key words: Name and job title of document author: Name and job title of document
For Use in: By: For: Guidelines for the Management of Interruption of Biologic Therapies for Division responsible for document: Key words: Name and job title of document author: Name and job title of document
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Cankaya Ortopedi. Outpatient TKA in Rheumatoid Arthritis. Prof. N. Reha Tandogan, M.D
 IMUKA 2016 Transatlantic Current Concepts in Outpatient Arthroplasty Dr. N. Reha Tandoğan Outpatient TKA in Rheumatoid Arthritis Prof. N. Reha Tandogan, M.D Ortoklinik / Çankaya Orthopaedics, Ankara, Turkey
IMUKA 2016 Transatlantic Current Concepts in Outpatient Arthroplasty Dr. N. Reha Tandoğan Outpatient TKA in Rheumatoid Arthritis Prof. N. Reha Tandogan, M.D Ortoklinik / Çankaya Orthopaedics, Ankara, Turkey
Challenges in Perioperative Medication Management. Learning Objectives. Case 1. » Appropriate use of beta-blockers. Management of diabetes drugs
 Challenges in Perioperative Medication Management Dimitriy Levin, MD Assistant Professor of Medicine University of Colorado Hospital Medicine Group Learning Objectives» Appropriate use of beta-blockers
Challenges in Perioperative Medication Management Dimitriy Levin, MD Assistant Professor of Medicine University of Colorado Hospital Medicine Group Learning Objectives» Appropriate use of beta-blockers
Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty
 Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty A Review of ACS-NSQIP 2006-2012 Arjun Sebastian, M.D., Stephanie Polites, M.D., Kristine Thomsen, B.S., Elizabeth Habermann,
Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty A Review of ACS-NSQIP 2006-2012 Arjun Sebastian, M.D., Stephanie Polites, M.D., Kristine Thomsen, B.S., Elizabeth Habermann,
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: golimumab_simponi 8/2013 2/2018 2/2019 3/2018 Description of Procedure or Service Golimumab (Simponi and
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: golimumab_simponi 8/2013 2/2018 2/2019 3/2018 Description of Procedure or Service Golimumab (Simponi and
Modifiable Risk Factors in Orthopaedic Infections
 Modifiable Risk Factors in Orthopaedic Infections AAOS Patient Safety Committee Burden US Surgical Site Infections (SSI) by the Numbers ~300,000 SSIs/yr (17% of all HAI; second to UTI) 2%-5% of patients
Modifiable Risk Factors in Orthopaedic Infections AAOS Patient Safety Committee Burden US Surgical Site Infections (SSI) by the Numbers ~300,000 SSIs/yr (17% of all HAI; second to UTI) 2%-5% of patients
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Regulatory Status FDA- approved indication: Simponi and Simponi ARIA are tumor necrosis factor (TNF) blockers indicated for the treatment of: (2-3)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 9 Last Review Date: March 16, 2018 Simponi / Simponi
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 9 Last Review Date: March 16, 2018 Simponi / Simponi
The medical treatment of rheumatoid arthritis has been dramatically improved with the
 DOI: 10.5124/jkma.2010.53.10.871 pissn: 1975-8456 eissn: 2093-5951 http://jkma.org Focused Issue of This Month Medical treatment of rheumatoid arthritis (I): Nonsteroidal anti-inflammatory drugs, disease
DOI: 10.5124/jkma.2010.53.10.871 pissn: 1975-8456 eissn: 2093-5951 http://jkma.org Focused Issue of This Month Medical treatment of rheumatoid arthritis (I): Nonsteroidal anti-inflammatory drugs, disease
Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study
 Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study BMJ 2017; 356 doi: https://doi.org/10.1136/bmj.j895 (Published
Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study BMJ 2017; 356 doi: https://doi.org/10.1136/bmj.j895 (Published
Rheumatoid arthritis 2010: Treatment and monitoring
 October 12, 2010 By Yusuf Yazici, MD [1] The significant changes in the way rheumatoid arthritis has been managed include earlier, more aggressive treatment with combination therapy. Significant changes
October 12, 2010 By Yusuf Yazici, MD [1] The significant changes in the way rheumatoid arthritis has been managed include earlier, more aggressive treatment with combination therapy. Significant changes
Synoviocytes. Macrophage. B cell C H R O N I C. Neutrophil. Mast cell I N F L A M M A T I O N. Tissue cell. Endothelial cell. Th1/Th17 IL17 IL22
 DC IL12, IL23 chemokines, ECM, Co-stimulation IL17, IL22 IFNγ ± Macrophage peptidoglycan lipopolysaccharide heat shock proteins Th1/Th17 IL17 IL22 Cell contact, co-stimulation immune complexes acute phase
DC IL12, IL23 chemokines, ECM, Co-stimulation IL17, IL22 IFNγ ± Macrophage peptidoglycan lipopolysaccharide heat shock proteins Th1/Th17 IL17 IL22 Cell contact, co-stimulation immune complexes acute phase
Regulatory Status FDA- approved indication: Simponi and Simponi ARIA are tumor necrosis factor (TNF) blockers indicated for the treatment of:
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 8 Last Review Date: March 17, 2017 Simponi / Simponi
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 8 Last Review Date: March 17, 2017 Simponi / Simponi
Infection Risk After Orthopedic Surgery in Patients With Inflammatory Rheumatic Diseases Treated With Immunosuppressive Drugs
 Arthritis Care & Research Vol. 65, No. 12, December 2013, pp 2032 2040 DOI 10.1002/acr.22077 2013, American College of Rheumatology ORIGINAL ARTICLE Infection Risk After Orthopedic Surgery in Patients
Arthritis Care & Research Vol. 65, No. 12, December 2013, pp 2032 2040 DOI 10.1002/acr.22077 2013, American College of Rheumatology ORIGINAL ARTICLE Infection Risk After Orthopedic Surgery in Patients
Healthcare-associated infection: what the impact is and where the burden falls
 Healthcare-associated infection: what the impact is and where the burden falls E. Tacconelli Dept. Infectious Diseases Catholic University, Rome, Italy Road map Incidence Mortality Lenght of hospitalisation
Healthcare-associated infection: what the impact is and where the burden falls E. Tacconelli Dept. Infectious Diseases Catholic University, Rome, Italy Road map Incidence Mortality Lenght of hospitalisation
Does Using a Laparoscopic Approach to Cholecystectomy Decrease the Risk of Surgical Site Infection?
 ANNALS OF SURGERY Vol. 237, No. 3, 358 362 2003 Lippincott Williams & Wilkins, Inc. Does Using a Laparoscopic Approach to Cholecystectomy Decrease the Risk of Surgical Site Infection? Chesley Richards,
ANNALS OF SURGERY Vol. 237, No. 3, 358 362 2003 Lippincott Williams & Wilkins, Inc. Does Using a Laparoscopic Approach to Cholecystectomy Decrease the Risk of Surgical Site Infection? Chesley Richards,
Certolizumab pegol (Cimzia) for psoriatic arthritis second line
 Certolizumab pegol (Cimzia) for psoriatic arthritis second line This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Certolizumab pegol (Cimzia) for psoriatic arthritis second line This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC
 Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC Update on the Treatment of Rheumatoid Arthritis Sabrina Fallavollita MDCM McGill University Canadian Society of Internal Medicine
Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC Update on the Treatment of Rheumatoid Arthritis Sabrina Fallavollita MDCM McGill University Canadian Society of Internal Medicine
Adherence to Non-Infused Biologic Medications Used to Treat Rheumatoid Arthritis (PDC-RA)
 Adherence to Non-Infused Biologic Medications Used to Treat Rheumatoid Arthritis (PDC-RA) Description The percentage of patients 18 years and older with rheumatoid arthritis (RA) who met the Proportion
Adherence to Non-Infused Biologic Medications Used to Treat Rheumatoid Arthritis (PDC-RA) Description The percentage of patients 18 years and older with rheumatoid arthritis (RA) who met the Proportion
Complication rates of 127 surgical procedures performed in rheumatic patients receiving tumor necrosis factor alpha blockers
 Complication rates of 127 surgical procedures performed in rheumatic patients receiving tumor necrosis factor alpha blockers A. Ruyssen-Witrand, L. Gossec, C. Salliot, M. Luc, M. Duclos, S. Guignard, M.
Complication rates of 127 surgical procedures performed in rheumatic patients receiving tumor necrosis factor alpha blockers A. Ruyssen-Witrand, L. Gossec, C. Salliot, M. Luc, M. Duclos, S. Guignard, M.
The Hospital for Sick Children Technology Assessment at SickKids (TASK)
 The Hospital for Sick Children Technology Assessment at SickKids (TASK) THE USE OF BIOLOGIC RESPONSE MODIFIERS IN POLYARTICULAR-COURSE JUVENILE IDIOPATHIC ARTHRITIS Report No. 2010-01 Date: January 11,
The Hospital for Sick Children Technology Assessment at SickKids (TASK) THE USE OF BIOLOGIC RESPONSE MODIFIERS IN POLYARTICULAR-COURSE JUVENILE IDIOPATHIC ARTHRITIS Report No. 2010-01 Date: January 11,
Amjevita (adalimumab-atto)
 *- Florida Healthy Kids Amjevita (adalimumab-atto) Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2 #* ^ prefilled
*- Florida Healthy Kids Amjevita (adalimumab-atto) Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2 #* ^ prefilled
Malnutrition: An independent Risk Factor for Postoperative Complications
 Malnutrition: An independent Risk Factor for Postoperative Complications Bryan P. Hooks, D.O. University of Pittsburgh-Horizon June 24, 2017 Orthopedic Surgeon-Adult Reconstruction Disclosures: None Objectives:
Malnutrition: An independent Risk Factor for Postoperative Complications Bryan P. Hooks, D.O. University of Pittsburgh-Horizon June 24, 2017 Orthopedic Surgeon-Adult Reconstruction Disclosures: None Objectives:
Effective Health Care Program
 Comparative Effectiveness Review Number 55 Effective Health Care Program Drug Therapy for Rheumatoid Arthritis in Adults: An Update Executive Summary Background Rheumatoid arthritis (RA), which affects
Comparative Effectiveness Review Number 55 Effective Health Care Program Drug Therapy for Rheumatoid Arthritis in Adults: An Update Executive Summary Background Rheumatoid arthritis (RA), which affects
Cimzia. Cimzia (certolizumab pegol) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Section: Prescription Drugs Effective Date: April 1, 2018 Subject: Cimzia Page: 1 of 5 Last Review
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Section: Prescription Drugs Effective Date: April 1, 2018 Subject: Cimzia Page: 1 of 5 Last Review
RHEUMATOID ARTHRITIS DRUGS
 Rheumatology Biologics Criteria from the Exceptional Access Program RHEUMATOID ARTHRITIS DRUGS DRUG NAME BRS REIMBURSED DOSAGE FORM/ STRENGTH Adalimumab Humira 40 mg/0.8 syringe and 40mg/0.8 pen for Anakinra
Rheumatology Biologics Criteria from the Exceptional Access Program RHEUMATOID ARTHRITIS DRUGS DRUG NAME BRS REIMBURSED DOSAGE FORM/ STRENGTH Adalimumab Humira 40 mg/0.8 syringe and 40mg/0.8 pen for Anakinra
Powered by Editorial Manager and ProduXion Manager from Aries Systems Corporation
 Powered by Editorial Manager and ProduXion Manager from Aries Systems Corporation Powered by Editorial Manager and ProduXion Manager from Aries Systems Corporation 1 Original article 2 Risk factors for
Powered by Editorial Manager and ProduXion Manager from Aries Systems Corporation Powered by Editorial Manager and ProduXion Manager from Aries Systems Corporation 1 Original article 2 Risk factors for
Cimzia (certolizumab pegol)
 DRUG POLICY BENEFIT APPLICATION Cimzia (certolizumab pegol) Benefit determinations are based on the applicable contract language in effect at the time the services were rendered. Exclusions, limitations
DRUG POLICY BENEFIT APPLICATION Cimzia (certolizumab pegol) Benefit determinations are based on the applicable contract language in effect at the time the services were rendered. Exclusions, limitations
Coverage Criteria: Express Scripts, Inc. monograph dated 12/15/ months or as otherwise noted by indication
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
Rheumatology Therapeutics: Perioperative DMARD Management, Infection and Malignancy Risks, Vaccination Considerations. Heather Hansen, MD
 Rheumatology Therapeutics: Perioperative DMARD Management, Infection and Malignancy Risks, Vaccination Considerations Heather Hansen, MD Objectives Know Broad Categories of Rheumatoid Arthritis Medications
Rheumatology Therapeutics: Perioperative DMARD Management, Infection and Malignancy Risks, Vaccination Considerations Heather Hansen, MD Objectives Know Broad Categories of Rheumatoid Arthritis Medications
1 P a g e. Systemic Juvenile Idiopathic Arthritis (SJIA) (1.3) Patients 2 years of age and older with active systemic juvenile idiopathic arthritis.
 LENGTH OF AUTHORIZATION: Initial: 3 months for Crohn s or Ulcerative Colitis; 1 year for all other indications. Renewal: 1 year dependent upon medical records supporting response to therapy and review
LENGTH OF AUTHORIZATION: Initial: 3 months for Crohn s or Ulcerative Colitis; 1 year for all other indications. Renewal: 1 year dependent upon medical records supporting response to therapy and review
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: abatacept_orencia 4/2008 2/2018 2/2019 2/2018 Description of Procedure or Service Abatacept (Orencia ), a
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: abatacept_orencia 4/2008 2/2018 2/2019 2/2018 Description of Procedure or Service Abatacept (Orencia ), a
Periprosthetic joint infection: are patients with multiple prosthetic joints at risk?
 Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 6-1-2012 Periprosthetic joint infection: are patients with multiple prosthetic joints at risk? S Mehdi Jafari The
Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 6-1-2012 Periprosthetic joint infection: are patients with multiple prosthetic joints at risk? S Mehdi Jafari The
Gender differences in effectiveness of treatment in rheumatic diseases
 Gender differences in effectiveness of treatment in rheumatic diseases Irene van der Horst-Bruinsma Associate Professor Rheumatology Center of Excellence of Axial Spondyloarthritis ARC/VU University Medical
Gender differences in effectiveness of treatment in rheumatic diseases Irene van der Horst-Bruinsma Associate Professor Rheumatology Center of Excellence of Axial Spondyloarthritis ARC/VU University Medical
C. Assess clinical response after the first three months of treatment.
 Government Health Plan (GHP) of Puerto Rico Authorization Criteria Tumor Necrosis Factor Alpha (TNFα) Adalimumab (Humira ) Managed by MCO Section I. Prior Authorization Criteria A. Physician must submit
Government Health Plan (GHP) of Puerto Rico Authorization Criteria Tumor Necrosis Factor Alpha (TNFα) Adalimumab (Humira ) Managed by MCO Section I. Prior Authorization Criteria A. Physician must submit
Cimzia. Cimzia (certolizumab pegol) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Cimzia Page: 1 of 5 Last Review Date: March 17, 2017 Cimzia Description Cimzia (certolizumab pegol)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Cimzia Page: 1 of 5 Last Review Date: March 17, 2017 Cimzia Description Cimzia (certolizumab pegol)
WHO Surgical Site Infection Prevention Guidelines. Web Appendix 12
 WHO Surgical Site Infection Prevention Guidelines Web Appendix 12 Summary of a systematic review on the perioperative discontinuation of immunosuppressive agents 1. Introduction Immunosuppressive agents
WHO Surgical Site Infection Prevention Guidelines Web Appendix 12 Summary of a systematic review on the perioperative discontinuation of immunosuppressive agents 1. Introduction Immunosuppressive agents
INFLIXIMAB Remicade (infliximab), Inflectra (infliximab-dyyb), Renflexis (infliximab-abda)
 RATIONALE FOR INCLUSION IN PA PROGRAM Background Remicade, Renflexis and Inflectra are tumor necrosis factor (TNFα) blockers. Tumor necrosis factor is an endogenous protein that regulates a number of physiologic
RATIONALE FOR INCLUSION IN PA PROGRAM Background Remicade, Renflexis and Inflectra are tumor necrosis factor (TNFα) blockers. Tumor necrosis factor is an endogenous protein that regulates a number of physiologic
Infections and Biologics
 Overview Infections and Biologics James Galloway What is the risk of infection with biologics? Are some patients at greater risk? Are some drugs safer? Case scenario You recently commenced Judith, a 54
Overview Infections and Biologics James Galloway What is the risk of infection with biologics? Are some patients at greater risk? Are some drugs safer? Case scenario You recently commenced Judith, a 54
ABSTRACT. KEY WORDS antibiotics; prophylaxis; hysterectomy
 Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Center for Evidence-based Policy
 P&T Committee Brief Targeted Immune Modulators: Comparative Drug Class Review Alison Little, MD Center for Evidence-based Policy Oregon Health & Science University 3455 SW US Veterans Hospital Road, SN-4N
P&T Committee Brief Targeted Immune Modulators: Comparative Drug Class Review Alison Little, MD Center for Evidence-based Policy Oregon Health & Science University 3455 SW US Veterans Hospital Road, SN-4N
Fml Limits. Azathioprine (Imuran) 50mg, 75mg, 100mg - $26.85 Cyclosporine, 25mg, 100mg. $ Leflunomide (Arava) 10mg Tablet - $144.
 MEDICATION COVERAGE POLICY PHARMACY AND THERAPEUTICS ADVISORY COMMITTEE POLICY: Rheumatoid Arthritis (RA) P&T DATE: 2/15/2017 CLASS: Rheumatology/Anti-inflammatory Disorders REVIEW HISTORY 2/16, 5/15,
MEDICATION COVERAGE POLICY PHARMACY AND THERAPEUTICS ADVISORY COMMITTEE POLICY: Rheumatoid Arthritis (RA) P&T DATE: 2/15/2017 CLASS: Rheumatology/Anti-inflammatory Disorders REVIEW HISTORY 2/16, 5/15,
Leflunomide Use and the Risk of Interstitial Lung Disease in Rheumatoid Arthritis
 ARTHRITIS & RHEUMATISM Vol. 54, No. 5, May 2006, pp 1435 1439 DOI 10.1002/art.21806 2006, American College of Rheumatology Leflunomide Use and the Risk of Interstitial Lung Disease in Rheumatoid Arthritis
ARTHRITIS & RHEUMATISM Vol. 54, No. 5, May 2006, pp 1435 1439 DOI 10.1002/art.21806 2006, American College of Rheumatology Leflunomide Use and the Risk of Interstitial Lung Disease in Rheumatoid Arthritis
Stelara. Stelara (ustekinumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.90.04 Subject: Stelara Page: 1 of 9 Last Review Date: September 20, 2018 Stelara Description Stelara
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.90.04 Subject: Stelara Page: 1 of 9 Last Review Date: September 20, 2018 Stelara Description Stelara
2017 Medicare STARs Provider Quality Indicators Guide
 2017 Medicare STARs Provider Quality Indicators Guide Medicare STARs Rating Centers for Medicare & Medicaid Services (CMS) created a Five-Star Quality Rating System to help measure the quality in care
2017 Medicare STARs Provider Quality Indicators Guide Medicare STARs Rating Centers for Medicare & Medicaid Services (CMS) created a Five-Star Quality Rating System to help measure the quality in care
Supplementary Online Content
 Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Contributions to health outcomes research Rheumatoid Arthritis. Study objective: Database: Author: Version: Date:
 Contributions to health outcomes research Rheumatoid Arthritis Study objective: Database: Author: Version: Date: Analysis of patient journeys and their resource consumptions in Germany Insurants presenting
Contributions to health outcomes research Rheumatoid Arthritis Study objective: Database: Author: Version: Date: Analysis of patient journeys and their resource consumptions in Germany Insurants presenting
Cimzia. Cimzia (certolizumab pegol) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Subject: Cimzia Page: 1 of 5 Last Review Date: December 8, 2017 Cimzia Description Cimzia (certolizumab
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Subject: Cimzia Page: 1 of 5 Last Review Date: December 8, 2017 Cimzia Description Cimzia (certolizumab
Disclosures. Evidence Based Medicine. Infections in SLE and LN Patients. Aim
 Serious Infection Rates among Patients with Systemic Lupus Erythematosus Receiving Corticosteroids and Immunosuppressants None Disclosures Candace H. Feldman, MD, MPH 1,2 Linda T. Hiraki, MD, SM, ScD 3
Serious Infection Rates among Patients with Systemic Lupus Erythematosus Receiving Corticosteroids and Immunosuppressants None Disclosures Candace H. Feldman, MD, MPH 1,2 Linda T. Hiraki, MD, SM, ScD 3
Treatment of Rheumatoid Arthritis: The Past, the Present and the Future
 Treatment of Rheumatoid Arthritis: The Past, the Present and the Future Lai-Ling Winchow FCP(SA) Cert Rheum(SA) Chris Hani Baragwanath Academic Hospital University of the Witwatersrand Outline of presentation
Treatment of Rheumatoid Arthritis: The Past, the Present and the Future Lai-Ling Winchow FCP(SA) Cert Rheum(SA) Chris Hani Baragwanath Academic Hospital University of the Witwatersrand Outline of presentation
Clinical Policy: Certolizumab (Cimzia) Reference Number: PA.CP.PHAR.247 Effective Date: 01/18 Last Review Date: 08/17 Line of Business: Medicaid
 Clinical Policy: (Cimzia) Reference Number: PA.CP.PHAR.247 Effective Date: 01/18 Last Review Date: 08/17 Line of Business: Medicaid Coding Implications Revision Log Description (Cimzia ) is a tumor necrosis
Clinical Policy: (Cimzia) Reference Number: PA.CP.PHAR.247 Effective Date: 01/18 Last Review Date: 08/17 Line of Business: Medicaid Coding Implications Revision Log Description (Cimzia ) is a tumor necrosis
Summary of Risk Minimization Measures
 Table 6.1.4-1: Summary of Risk Minimization Measures Safety Concern Vaccination Hepatic and renal impairment Combination therapy Elderly Routine Risk Minimization Measures Specific subsection on vaccination
Table 6.1.4-1: Summary of Risk Minimization Measures Safety Concern Vaccination Hepatic and renal impairment Combination therapy Elderly Routine Risk Minimization Measures Specific subsection on vaccination
Proposed Retirement for HEDIS : Disease-Modifying Anti-Rheumatic Drug Therapy for Rheumatoid Arthritis (ART)
 Proposed Retirement for HEDIS 1 2020 2 : Disease-Modifying Anti-Rheumatic Drug Therapy for Rheumatoid Arthritis (ART) NCQA seeks public comment on the proposed retirement of the Disease-Modifying Anti-Rheumatic
Proposed Retirement for HEDIS 1 2020 2 : Disease-Modifying Anti-Rheumatic Drug Therapy for Rheumatoid Arthritis (ART) NCQA seeks public comment on the proposed retirement of the Disease-Modifying Anti-Rheumatic
New Evidence reports on presentations given at EULAR Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis
 New Evidence reports on presentations given at EULAR 2011 Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis Report on EULAR 2011 presentations Anti-TNF failure and response to rituximab
New Evidence reports on presentations given at EULAR 2011 Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis Report on EULAR 2011 presentations Anti-TNF failure and response to rituximab
Key words: rheumatoid arthritis, ankylosing spondylitis, psoriatic arthritis, treatment access
 6, 21...,.,..,..,. - (RA) -,. (AS) (PsA). (Disease-modifying antirheumatic drugs, DMARDs). DMARDs 21. - RA, AS PsA. 21. RA, DMARDs. Leflunomide (Arava)., RA Methotrexate Leflunomid. DMARDs - 5 29. - RA
6, 21...,.,..,..,. - (RA) -,. (AS) (PsA). (Disease-modifying antirheumatic drugs, DMARDs). DMARDs 21. - RA, AS PsA. 21. RA, DMARDs. Leflunomide (Arava)., RA Methotrexate Leflunomid. DMARDs - 5 29. - RA
Simponi / Simponi ARIA (golimumab)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 6 Last Review Date: September 15, 2016 Simponi / Simponi
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 6 Last Review Date: September 15, 2016 Simponi / Simponi
ACTEMRA (TOCILIZUMAB) INJECTION FOR INTRAVENOUS INFUSION
 ACTEMRA (TOCILIZUMAB) INJECTION FOR INTRAVENOUS INFUSION UnitedHealthcare Commercial Medical Benefit Drug Policy Policy Number: 2018D0043I Effective Date: March 1, 2018 Table of Contents Page INSTRUCTIONS
ACTEMRA (TOCILIZUMAB) INJECTION FOR INTRAVENOUS INFUSION UnitedHealthcare Commercial Medical Benefit Drug Policy Policy Number: 2018D0043I Effective Date: March 1, 2018 Table of Contents Page INSTRUCTIONS
Cell-Mediated Immunity and T Lymphocytes
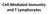 Cell-Mediated Immunity and T Lymphocytes T helper (Th) Cells Peripheral lymhoid tissue thymus Lymphoid stem cell CD8+ CD4+ CD4+ Treg CD8+ CTL + antigen Cytotoxic T lymphocyte CD4+ Th Helper T cell CD4+
Cell-Mediated Immunity and T Lymphocytes T helper (Th) Cells Peripheral lymhoid tissue thymus Lymphoid stem cell CD8+ CD4+ CD4+ Treg CD8+ CTL + antigen Cytotoxic T lymphocyte CD4+ Th Helper T cell CD4+
Isoniazid treatment for latent tuberculosis infection is tolerable for rheumatoid arthritis patients receiving tumor necrosis factor inhibitor therapy
 ORIGINAL ARTICLE 2017 Mar 13. [Epub ahead of print] Isoniazid treatment for latent tuberculosis infection is tolerable for rheumatoid arthritis patients receiving tumor necrosis factor inhibitor therapy
ORIGINAL ARTICLE 2017 Mar 13. [Epub ahead of print] Isoniazid treatment for latent tuberculosis infection is tolerable for rheumatoid arthritis patients receiving tumor necrosis factor inhibitor therapy
HEALTHCARE EFFECTIVENESS DATA AND INFORMATION SET (HEDIS )
 STARS MEASURES 2015 HEALTHCARE EFFECTIVENESS DATA AND INFORMATION SET (HEDIS ) Developed by the National Committee for Quality Assurance (NCQA), HEDIS is the most widely used set of performance measures
STARS MEASURES 2015 HEALTHCARE EFFECTIVENESS DATA AND INFORMATION SET (HEDIS ) Developed by the National Committee for Quality Assurance (NCQA), HEDIS is the most widely used set of performance measures
James R. O Dell, M.D. University of Nebraska Medical Center
 Not everyone in the world needs a biologic: Lessons from TEAR and RACAT James R. O Dell, M.D. University of Nebraska Medical Center Disclosure Declaration James O Dell, MD Advisory Board for Crescendo,
Not everyone in the world needs a biologic: Lessons from TEAR and RACAT James R. O Dell, M.D. University of Nebraska Medical Center Disclosure Declaration James O Dell, MD Advisory Board for Crescendo,
Safety and effectiveness of biologic Disease-Modifying Antirheumatic Drugs in elderly patients with rheumatoid arthritis
 1. Title: Safety and effectiveness of biologic Disease-Modifying Antirheumatic Drugs in elderly patients with rheumatoid arthritis 2. Background: The population of older individuals with rheumatoid arthritis
1. Title: Safety and effectiveness of biologic Disease-Modifying Antirheumatic Drugs in elderly patients with rheumatoid arthritis 2. Background: The population of older individuals with rheumatoid arthritis
Xeljanz (tofacitinib), Xeljanz XR (tofacitinib extended-release)
 Market DC Xeljanz (tofacitinib), Xeljanz XR (tofacitinib extended-release) Override(s) Prior Authorization Quantity Limit Medications Xeljanz (tofacitinib) Approval Duration 1 year Quantity Limit May be
Market DC Xeljanz (tofacitinib), Xeljanz XR (tofacitinib extended-release) Override(s) Prior Authorization Quantity Limit Medications Xeljanz (tofacitinib) Approval Duration 1 year Quantity Limit May be
Skin cancers in patients treated with immunomodulating drugs. Manuelle Viguier, MD, PhD Dermatology department Saint-Louis Hospital Paris, France
 Skin cancers in patients treated with immunomodulating drugs Manuelle Viguier, MD, PhD Dermatology department Saint-Louis Hospital Paris, France Immunomodulating drugs used in Methotrexate Mycophenolate
Skin cancers in patients treated with immunomodulating drugs Manuelle Viguier, MD, PhD Dermatology department Saint-Louis Hospital Paris, France Immunomodulating drugs used in Methotrexate Mycophenolate
Ustekinumab (Stelara) for psoriatic arthritis second line after disease modifying anti rheumatic drugs (DMARDs)
 Ustekinumab (Stelara) for psoriatic arthritis second line after disease modifying anti rheumatic drugs (DMARDs) January 2010 This technology summary is based on information available at the time of research
Ustekinumab (Stelara) for psoriatic arthritis second line after disease modifying anti rheumatic drugs (DMARDs) January 2010 This technology summary is based on information available at the time of research
Adrenocorticotropic hormone gel in patients with refractory rheumatoid arthritis: a case series
 International Journal of Clinical Rheumatology For reprint orders, please contact: reprints@futuremedicine.com Adrenocorticotropic hormone gel in patients with refractory rheumatoid arthritis: a case series
International Journal of Clinical Rheumatology For reprint orders, please contact: reprints@futuremedicine.com Adrenocorticotropic hormone gel in patients with refractory rheumatoid arthritis: a case series
Inflammation, rheumatoid arthritis and cardiovascular disease
 Inflammation, rheumatoid arthritis and cardiovascular disease Yvette Meißner, Pharmacoepidemiology, German Rheumatism Research Centre www. chronische-entzuendung.org Outline I. Cardiovascular disease II.
Inflammation, rheumatoid arthritis and cardiovascular disease Yvette Meißner, Pharmacoepidemiology, German Rheumatism Research Centre www. chronische-entzuendung.org Outline I. Cardiovascular disease II.
Sarcoidosis Case. Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA. WASOG: educational material
 Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Orencia (abatacept) DRUG.00040
 Market DC Orencia (abatacept) DRUG.00040 Override(s) Prior Authorization Quantity Limit Approval Duration 1 year Medications Comments Quantity Limit Orencia (abatacept) - AGP, VA MCD only 4 vials per 28
Market DC Orencia (abatacept) DRUG.00040 Override(s) Prior Authorization Quantity Limit Approval Duration 1 year Medications Comments Quantity Limit Orencia (abatacept) - AGP, VA MCD only 4 vials per 28
Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer
 HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
Supplementary material
 Supplementary material Table S1: Dubois Guidelines for Diagnosis of DrugInduced Lupus 1. Continuous treatment with a known lupusinducing drug for 1month and usually much longer 2. Presenting symptoms:
Supplementary material Table S1: Dubois Guidelines for Diagnosis of DrugInduced Lupus 1. Continuous treatment with a known lupusinducing drug for 1month and usually much longer 2. Presenting symptoms:
The GPs role with biologics for immune-mediated inflammatory diseases David Gardner Rheumatologist GPCME 2015
 The GPs role with biologics for immune-mediated inflammatory diseases David Gardner Rheumatologist GPCME 2015 The views and opinions expressed in the following presentation are those of the presenter and
The GPs role with biologics for immune-mediated inflammatory diseases David Gardner Rheumatologist GPCME 2015 The views and opinions expressed in the following presentation are those of the presenter and
PROVIDER GUIDE Required information on targeted HEDIS and Part D measures
 PROVIDER GUIDE Required information on targeted HEDIS and Part D measures Visit www.atriohp.com/star-ratings-program for full measure descriptions. Contact QI@atriohp.com with any questions. Adult Body
PROVIDER GUIDE Required information on targeted HEDIS and Part D measures Visit www.atriohp.com/star-ratings-program for full measure descriptions. Contact QI@atriohp.com with any questions. Adult Body
Clinical Policy: Anakinra (Kineret) Reference Number: ERX.SPA.135 Effective Date:
 Clinical Policy: (Kineret) Reference Number: ERX.SPA.135 Effective Date: 10.01.16 Last Review Date: 05.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Kineret) Reference Number: ERX.SPA.135 Effective Date: 10.01.16 Last Review Date: 05.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Helpline No:
 ARTHRITIS FOUNDATION Registered Nonprofit Organisation - No. 002-847 NPO Helpline No: 0861 30 30 30 DRUGS AND ARTHRITIS This information leaflet is published by the Arthritis Foundation as part of our
ARTHRITIS FOUNDATION Registered Nonprofit Organisation - No. 002-847 NPO Helpline No: 0861 30 30 30 DRUGS AND ARTHRITIS This information leaflet is published by the Arthritis Foundation as part of our
Abatacept (Orencia) for active rheumatoid arthritis. August 2009
 Abatacept (Orencia) for active rheumatoid arthritis August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Abatacept (Orencia) for active rheumatoid arthritis August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Coccidioidomycosis in Rheumatologic Patients. Susan E. Hoover, MD
 Coccidioidomycosis in Rheumatologic Patients Susan E. Hoover, MD The problem Prevalence of rheumatoid arthritis is 1% Population of Arizona is 6 million At least 150,000 new cocci infections yearly DMARDs
Coccidioidomycosis in Rheumatologic Patients Susan E. Hoover, MD The problem Prevalence of rheumatoid arthritis is 1% Population of Arizona is 6 million At least 150,000 new cocci infections yearly DMARDs
Anti-Tumor Necrosis Factor (Anti-TNF)
 Anti-Tumor Necrosis Factor (Anti-TNF) 110465 Anti-TNF.indd 1 9/20/16 9:01 AM s About your medicine Anti-tumor necrosis factor (anti-tnf) is a type of medicine called biologic agent that targets substance
Anti-Tumor Necrosis Factor (Anti-TNF) 110465 Anti-TNF.indd 1 9/20/16 9:01 AM s About your medicine Anti-tumor necrosis factor (anti-tnf) is a type of medicine called biologic agent that targets substance
Etanercept and Adalimumab Treatment Patterns in Psoriatic Arthritis Patients Enrolled in a Commercial Health Plan
 Adv Ther (2012) 29(8):691 697. DOI 10.1007/s12325-012-0039-3 ORIGINAL RESEARCH Etanercept and Adalimumab Treatment Patterns in Psoriatic Arthritis Patients Enrolled in a Commercial Health Plan Benjamin
Adv Ther (2012) 29(8):691 697. DOI 10.1007/s12325-012-0039-3 ORIGINAL RESEARCH Etanercept and Adalimumab Treatment Patterns in Psoriatic Arthritis Patients Enrolled in a Commercial Health Plan Benjamin
Amjevita (adalimumab-atto) CG-DRUG-64, CG-DRUG-65
 Market DC Amjevita (adalimumab-atto) CG-DRUG-64, CG-DRUG-65 Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2
Market DC Amjevita (adalimumab-atto) CG-DRUG-64, CG-DRUG-65 Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2
The NOF & NBHA Quality Improvement Registry
 In collaboration with CECity The NOF & NBHA Quality Improvement Registry This registry is approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Professionals and GPRO Practices for
In collaboration with CECity The NOF & NBHA Quality Improvement Registry This registry is approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Professionals and GPRO Practices for
Introduction ORIGINAL ARTICLE
 Mod Rheumatol (2007) 17:28 32 Japan College of Rheumatology 2007 DOI 10.1007/s10165-006-0532-0 ORIGINAL ARTICLE Hisashi Yamanaka Yoshiya Tanaka Naoya Sekiguchi Eisuke Inoue Kazuyoshi Saito Hideto Kameda
Mod Rheumatol (2007) 17:28 32 Japan College of Rheumatology 2007 DOI 10.1007/s10165-006-0532-0 ORIGINAL ARTICLE Hisashi Yamanaka Yoshiya Tanaka Naoya Sekiguchi Eisuke Inoue Kazuyoshi Saito Hideto Kameda
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Outcome
 Measure #165 (NQF 0130): Coronary Artery Bypass Graft (CABG): Deep Sternal Wound Infection Rate National Quality Strategy Domain: Effective Clinical Care 2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Measure #165 (NQF 0130): Coronary Artery Bypass Graft (CABG): Deep Sternal Wound Infection Rate National Quality Strategy Domain: Effective Clinical Care 2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
This is a repository copy of Treating active rheumatoid arthritis with Janus kinase inhibitors..
 This is a repository copy of Treating active rheumatoid arthritis with Janus kinase inhibitors.. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/118272/ Version: Accepted
This is a repository copy of Treating active rheumatoid arthritis with Janus kinase inhibitors.. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/118272/ Version: Accepted
Subject: Remicade (Page 1 of 5)
 Subject: Remicade (Page 1 of 5) Objective: I. To ensure that Health Share/Tuality Health Alliance (THA) has a process by which the appropriate utilization of Remicade (Infliximab) for members whose diagnosis
Subject: Remicade (Page 1 of 5) Objective: I. To ensure that Health Share/Tuality Health Alliance (THA) has a process by which the appropriate utilization of Remicade (Infliximab) for members whose diagnosis
Racial and ethnic disparities in surgical amputations following serious. musculoskeletal infections in a diverse New Mexico cohort
 Racial and ethnic disparities in surgical amputations following serious musculoskeletal infections in a diverse New Mexico cohort Martha L. Carvour 1,2,*, Allyssa Chiu 1, Kimberly Page 1 1 Division of
Racial and ethnic disparities in surgical amputations following serious musculoskeletal infections in a diverse New Mexico cohort Martha L. Carvour 1,2,*, Allyssa Chiu 1, Kimberly Page 1 1 Division of
Rheumatoid Arthritis. By: Hadi Esmaily (PharmD., BCCP, MBA) Department of Clinical Pharmacy, Shahid Beheshti Medical University
 Rheumatoid Arthritis By: Hadi Esmaily (PharmD., BCCP, MBA) Department of Clinical Pharmacy, Shahid Beheshti Medical University Introduction RA is a Chronic, Systemic, Inflammatory disorder of unknown etiology
Rheumatoid Arthritis By: Hadi Esmaily (PharmD., BCCP, MBA) Department of Clinical Pharmacy, Shahid Beheshti Medical University Introduction RA is a Chronic, Systemic, Inflammatory disorder of unknown etiology
Pharmacy Medical Necessity Guidelines:
 Pharmacy Medical Necessity Guidelines: Effective: January 1, 2018 Prior Authorization Required Type of Review Care Management Not Covered Type of Review Clinical Review Pharmacy (RX) or Medical (MED) Benefit
Pharmacy Medical Necessity Guidelines: Effective: January 1, 2018 Prior Authorization Required Type of Review Care Management Not Covered Type of Review Clinical Review Pharmacy (RX) or Medical (MED) Benefit
EPO-144 Patients with Morbid Obesity and Congestive Heart Failure Have Longer Operative Time and Room Time in Total Hip Arthroplasty
 SESUG 2016 EPO-144 Patients with Morbid Obesity and Congestive Heart Failure Have Longer Operative Time and Room Time in Total Hip Arthroplasty ABSTRACT Yubo Gao, University of Iowa Hospitals and Clinics,
SESUG 2016 EPO-144 Patients with Morbid Obesity and Congestive Heart Failure Have Longer Operative Time and Room Time in Total Hip Arthroplasty ABSTRACT Yubo Gao, University of Iowa Hospitals and Clinics,
Technology appraisal guidance Published: 22 February 2012 nice.org.uk/guidance/ta247
 Tocilizumab for the treatment of rheumatoid arthritis Technology appraisal guidance Published: 22 February 2012 nice.org.uk/guidance/ta247 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Tocilizumab for the treatment of rheumatoid arthritis Technology appraisal guidance Published: 22 February 2012 nice.org.uk/guidance/ta247 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
(2) 83.3% b/w TST and T-SPOT, (2) 77.4% b/w TST and T-SPOT. 77.7% b/w TST and QFT-GIT. QFT-GIT, 22.2% in T-SPOT. TSPOT vs. TST (> 5 mm) vs.
 Supplementary Table 1. Study characteristics of the included literature Low to moderate TB endemic region Shovman et al. (2009) [21] Minguez et al. (2012) [16], type 35 RA 35 RA 53 Patients with s (RA
Supplementary Table 1. Study characteristics of the included literature Low to moderate TB endemic region Shovman et al. (2009) [21] Minguez et al. (2012) [16], type 35 RA 35 RA 53 Patients with s (RA
Understanding Myositis Medications
 Understanding Myositis Medications 2015 TMA Annual Patient Conference Orlando, Florida Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Disclosures Mallinckrodt: Research Grant Genentech:
Understanding Myositis Medications 2015 TMA Annual Patient Conference Orlando, Florida Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Disclosures Mallinckrodt: Research Grant Genentech:
Arthritis Research UK response: new indicators for inclusion in NICE Quality and Outcomes Framework indicator menu
 February 2015 Arthritis Research UK response: new indicators for inclusion in NICE Quality and Outcomes Framework indicator menu 1. Arthritis Research UK is the charity dedicated to stopping the devastating
February 2015 Arthritis Research UK response: new indicators for inclusion in NICE Quality and Outcomes Framework indicator menu 1. Arthritis Research UK is the charity dedicated to stopping the devastating
